Practical guidelines on the management and prevention of the diabetic foot 2011
|
|
|
- Hester Fleming
- 6 years ago
- Views:
Transcription
1 DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): Published online in Wiley Online Library (wileyonlinelibrary.com).2253 IWGDF GUIDELINES Practical guidelines on the management and prevention of the diabetic foot 2011 K. Bakker 1 * J. Apelqvist 2 N. C. Schaper 3 on behalf of the International Working Group on the Diabetic Foot Editorial Board 1 IWGDF, Heemstede, The Netherlands 2 Department of Endocrinology, University Hospital of Malmö, Sweden 3 Division of Endocrinology, MUMC+, CARIM and CAPHRI Institute, Maastricht, The Netherlands *Correspondence to: K. Bakker, International Working Group on the Diabetic Foot, Heemsteedse Dreef 90, 2102 KN, Heemstede, The Netherlands. karel.bakker@hetnet.nl Prepared by the International Working Group on the Diabetic Foot. Keywords Introduction management; guidelines; diabetic foot Foot complications are among the most serious and costly complications of diabetes mellitus. Amputation of the lower extremity or part of it is usually preceded by a foot ulcer. A strategy that includes prevention, patient and staff education, multidisciplinary treatment of foot ulcers, and close monitoring can reduce amputation rates by 49 85%. Therefore, several countries and organizations, such as the World Health Organization and the International Diabetes Federation, have set goals to reduce the rate of amputations by up to 50%. The basic principles of prevention and treatment described in these guidelines are based on the International Consensus on the Diabetic Foot. Depending on local circumstances, these principles have to be translated for local use, taking into account regional differences in socio-economics, accessibility to health care, and cultural factors. These practical guidelines are aimed at healthcare workers involved in the care of people with diabetes. For more details and information on treatment by specialists in foot care, the reader is referred to the International Consensus document. Pathophysiology Received: 18 October 2011 Accepted: 18 October 2011 Although the spectrum of foot lesions varies in different regions of the world, the pathways to ulceration are probably identical in most patients. Diabetic foot lesions frequently result from two or more risk factors occurring together. In the majority of patients, diabetic peripheral neuropathy plays a central role: up to 50% of people with diabetes with type 2 diabetes have neuropathy and at-risk feet. Neuropathy leads to an insensitive and sometimes deformed foot, often with an abnormal walking pattern. In people with neuropathy, minor trauma caused, for example, by ill-fitting shoes, walking barefoot, or an acute injury can precipitate a chronic ulcer. Loss of sensation, foot deformities, and limited joint mobility can result in abnormal biomechanical loading of the foot. Thickened skin (callus) forms as a result. This leads to a further increase of the abnormal loading and, often, subcutaneous haemorrhage. Whatever the primary cause, the patient continues walking on the insensitive foot, impairing subsequent healing (Figure 1). Peripheral vascular disease, usually in conjunction with minor trauma, may result in a Copyright 2012 John Wiley & Sons, Ltd.
2 K. Bakker et al. 226 and standing up, and their shoes and socks should also be inspected. Identification of the at-risk foot After examination of the foot, each patient can be assigned to a risk category, which should guide the subsequent management (Figure 2). Figure 1. Illustration of ulcer due to repetitive stress painful, purely ischaemic foot ulcer. However, in patients with both neuropathy and ischaemia (neuroischaemic ulcer), symptoms may be absent, despite severe peripheral ischaemia. Microangiopathy should not be accepted as a primary cause of an ulcer. Progression of risk categories Sensory neuropathy and/or foot deformities or bony prominences and/or signs of peripheral ischemia and/ or previous ulcer or amputation Sensory neuropathy Non-sensory neuropathy Cornerstones of foot management There are five key elements that underpin foot management: Regular inspection and examination of the at-risk foot Identification of the at-risk foot Education of patient, family, and healthcare providers Appropriate footwear Treatment of nonulcerative pathology Regular inspection and examination All people with diabetes should be examined at least once a year for potential foot problems. Patients with demonstrated risk factor(s) should be examined more often every 1 6 months. The absence of symptoms does not mean that the feet are healthy; the patient might have neuropathy, peripheral vascular disease, or even an ulcer without any complaints. The patient s feet should be examined with the patient lying down Copyright 2012 John Wiley & Sons, Ltd. Figure 2. Areas at risk Diabetes Metab Res Rev 2012; 28(Suppl 1):
3 Management and Prevention of the Diabetic Foot 227 Education for patients, family, and healthcare providers Education, presented in a structured and organized manner, plays an important role in the prevention of foot problems. The aim is to enhance motivation and skills. People with diabetes should learn how to recognize potential foot problems and be aware of the steps they need to take in response. The educator must demonstrate the skills, such as how to cut nails appropriately. Education should be provided in several sessions over time, preferably using a mixture of methods. It is essential to evaluate whether the person with diabetes has understood the messages, is motivated to act, and has sufficient self-care skills. An example of instructions for the high-risk patient and family is given in the succeeding part of this article. Furthermore, physicians and other healthcare professionals should receive periodic education to improve care for high-risk individuals. Items that should be covered when instructing the high-risk patient are as follows: Daily feet inspection, including areas between the toes The need for another person with skills to inspect feet, should the people with diabetes be unable to do so. (If vision is impaired, people with diabetes should not attempt their own foot care.) Regular washing of feet with careful drying, especially between the toes Water temperature, which should always be below 37 C Not using a heater or a hot-water bottle to warm ones feet Avoidance of barefoot walking indoors or outdoors and of wearing of shoes without socks Chemical agents or plasters to remove corns and calluses, which should not be used Daily inspection and palpation of the inside of the shoes Not wearing tight shoes or shoes with rough edges and uneven seams Use of lubricating oils or creams for dry skin, but not between the toes Daily change of socks Wearing of stocking with seams inside out or preferably without any seams Never wearing tight or knee-high socks. Cutting nails straight across (Figure 3) Corns and calluses, which should be cut by a healthcare provider Patient awareness of the need to ensure that feet are examined regularly by a healthcare provider Notifying the healthcare provider at once if a blister, cut, scratch, or sore has developed Appropriate footwear Inappropriate footwear is a major cause of ulceration. Appropriate footwear should be used both indoors and outdoors and should be adapted to the altered biomechanics and deformities essential for prevention. Patients without loss of protective sensation can select off-the-shelf footwear by themselves. In patients with neuropathy and/or ischaemia, extra care must be taken when fitting footwear particularly when foot deformities are also present. The shoe should not be too tight or too loose (Figure 4). The inside of the shoe should be 1 2 cm longer than the foot itself. The internal width should be equal to the width of the foot at the site of the metatarsal phalangeal joints, and the height should allow enough room for the toes. The fit must be evaluated with the patient in standing position, preferably at the end of the day. If the fit is too tight because of deformities or if there are signs of abnormal loading of the foot (e.g. hyperaemia, callus, ulceration), patients should be referred for special footwear (advice and/or construction), including insoles and orthoses. Figure 3. How to cut nails Figure 4. Internal width of the shoe
4 228 K. Bakker et al. Treatment of nonulcerative pathology In a high-risk patient, callus and nail and skin pathology should be treated regularly, preferably by a trained foot care specialist. If possible, foot deformities should be treated nonsurgically (e.g. with an orthosis). Foot ulcers A standardized and consistent strategy for evaluating wounds is essential and will guide further therapy. The following items must be addressed. Cause Ill-fitting shoes are the most frequent cause of ulceration, even in patients with pure ischaemic ulcers. Therefore, shoes should be examined meticulously in all patients. Type Most ulcers can be classified as neuropathic, ischaemic, or neuro-ischaemic. This will guide further therapy. Assessment of the vascular tree is essential in the management of a foot ulcer. If one or more pedal pulses are absent, or if an ulcer does not improve despite optimal treatment, more extensive vascular evaluation should be performed. As a first step, the ankle brachial pressure can be measured. An ankle brachial pressure index less than 0.9 is a sign of peripheral arterial disease. However, ankle pressure might be falsely elevated because of calcification of the arteries. Preferably, other tests, such as measurements of toe pressure or transcutaneous pressure of oxygen (TcPo 2 ), should be used. Figure 5 gives an estimate of the chance of healing using the tests. If a major amputation is being contemplated, the option of revascularization should be considered first. Noninvasive evaluation and estimate of probability of healing: Site and depth Neuropathic ulcers frequently occur on the plantar surface of the foot or in areas overlying a bony deformity. Ischaemic and neuro-ischaemic ulcers are more common on the tips of the toes or the lateral border of the foot. The depth of an ulcer can be difficult to determine because of the presence of overlying callus or necrosis. Therefore, neuropathic ulcers with callus and necrosis should be debrided as soon as possible. This debridement should not be performed in ischaemic or neuro-ischaemic ulcers without signs of infection. In neuropathic ulcers, debridement can usually be performed without (general) anaesthesia. Signs of infection Infection of the foot in a person with diabetes presents a serious threat to the affected limb and should be evaluated and treated promptly. Infection is diagnosed by the presence of signs and/or symptoms of inflammation, but these may be blunted by neuropathy or ischemia, and systemic findings (e.g. fever, increased white blood count) are often absent. Infections should be classified as mild (superficial with minimal cellulitis), moderate (deeper or more extensive), or severe (accompanied by systemic signs of sepsis). If not properly treated, infection can spread to underlying tissues, including the bone. Patients with a diabetic foot infection should be assessed for the presence of osteomyelitis. When there is a deep wound overlying the bone, especially if it is longstanding and it is possible to touch the bone with a sterile probe, osteomyelitis is likely. Properly obtained specimens for Gram stain and culture of deep tissue are advised; avoid superficial swabs. Mild (superficial and limited) infection is usually caused by aerobic Gram-positive cocci, especially Staphylococcus aureus. Chronic infections and infections that are more severe are often polymicrobial with aerobic Gram-negative rods and anaerobes. Ulcer treatment If treatment is based on the principles outlined in the succeeding part of this article, healing can be achieved in the majority of patients. Optimum wound care cannot compensate for continuing trauma to the wound bed or for ischaemia or infection. Patients with an ulcer deeper than the subcutaneous tissues should be treated intensively, and, depending on local resources and infrastructure, hospitalization must be considered. Principles of ulcer treatment Figure 5. A schematic estimate of the probability of healing of foot ulcers and minor amputations in relation to ankle blood pressure, toe blood pressure, and transcutaneous oxygen pressure (TcPo 2 ) based on selected reports Relief of pressure and protection of the ulcer Mechanical off-loading the cornerstone in ulcers with increased biomechanical stress
5 Management and Prevention of the Diabetic Foot 229 Total contact casting or other casting techniques preferable in the management of plantar ulcers Temporary footwear Individually moulded insoles and fitted shoes Non-weight bearing limitation of standing and walking crutches, etc. Restoration of skin perfusion Peripheral arterial disease is the most important factor relating to the outcome of a diabetic foot ulcer. Healing will be severely impaired in diabetic patients with a foot ulcer in case of symptoms or signs of ischemia, an ankle brachial pressure index <0.6, toe pressures <50 mmhg, or TcPo 2 <30 mmhg. In these patients, revascularization should always be considered. The benefits of pharmacological treatment to improve perfusion have not been established Emphasis should be placed on cardiovascular risk reduction (cessation of smoking, treatment of hypertension and dyslipidaemia, use of aspirin) Treatment of infection Superficial ulcer with skin infection Cleanse, debride all necrotic tissue and surrounding callus Start empiric oral antibiotic therapy targeted at S. aureus and streptococci Deep (potentially limb-threatening) infection Urgently evaluate for surgical drainage to remove necrotic tissue, including infected bone, and drain abscesses Consider need for arterial revascularization Initiate empiric, parenteral broad-spectrum antibiotic therapy aimed at Gram-positive and Gramnegative bacteria, including anaerobes Metabolic control and treatment of comorbidity Optimal diabetes control, if necessary with insulin (blood glucose <8 mmol/l or <140 mg/dl) Treatment of oedema and malnutrition Local wound care Frequent wound inspection Frequent wound debridement (with scalpel) Control of exudate and maintenance of moist environment Consideration of negative pressure therapy in postoperative wounds The following treatments are not established in routine management: Biological active products (collagen, growth factors, bio-engineered tissue) in neuropathic ulcers Systemic hyperbaric oxygen treatment Silver or other anti-microbial agents containing dressings Note: footbaths are contra-indicated as they induce maceration of the skin. Education for patient and relatives Instruction should be given on appropriate selfcare and how to recognize and report signs and symptoms of (worsening) infection fever, changes under local wound conditions, or hyperglycaemia Determining the cause and preventing recurrence The cause of the ulceration should be determined to reduce the chance of recurrences. Ulcers on contralateral foot should be prevented and heel protection provided during periods of bed rest. Once the episode is over, the patient should be included in a comprehensive foot care programme with life-long observation Organization Effective organization requires systems and guidelines for education, screening, risk reduction, treatment, and auditing. Local variations in resources and staffing will often determine the ways in which care is provided. Ideally, a foot care programme should provide the following: Education for patients, carers and healthcare staff in hospitals, primary health care, and the community A system to detect all people who are at risk, with annual foot examination of all known patients Measures to reduce risk, such as podiatry and appropriate footwear Prompt and effective treatment Auditing of all aspects of the service to ensure that local practice meets accepted standards of care An overall structure that is designed to meet the needs of patients requiring chronic care rather than simply responding to acute problems when they occur In all countries, at least three levels of foot care management are needed: Level 1 General practitioner, podiatrist, and diabetic nurse Level 2 Diabetologist, surgeon (general and/or vascular and/or orthopaedic), podiatrist, and diabetic nurse Level 3 Specialized foot centre with multiple disciplines specialized in diabetic foot care Setting up a multidisciplinary foot care team has been found to be accompanied by a drop in the number of amputations. If it is not possible to create a full team from the outset, this should be built up step by step, introducing the various different disciplines at different stages. This team must work in both primary and secondary care settings. Ideally, a foot care team would consist of a diabetologist, surgeon, podiatrist, orthotist, educator, and plaster technician, in close collaboration with an orthopaedic, podiatric and/or vascular surgeon, and dermatologist.
6 230 K. Bakker et al. Addendum Sensory foot examination Neuropathy can be detected using the 10-g (5.07 Semmes Weinstein) monofilament, tuning fork (128 Hz), and/or cotton wisp. Semmes Weinstein monofilament Sensory examination should be carried out in a quiet and relaxed setting. First, apply the monofilament on the patient s hands (or elbow or forehead) so that he or she knows what to expect. The patient must not be able to see whether or where the examiner applies the filament. The three sites to be tested on both feet are indicated in Figure 6. Apply the monofilament perpendicular to the skin surface (Figure 7(A)). Apply sufficient force to cause the filament to bend or buckle (Figure 7(B)). The total duration of the approach skin contact and removal of the filament should be approximately 2 s. Apply the filament along the perimeter of, not on, an ulcer site, callus, scar, or necrotic tissue. Do not allow the filament to slide across the skin or make repetitive contact at the test site. Press the filament to the skin and ask the patient whether they feel the pressure applied ( yes / no ) and, next, where they feel the pressure ( left foot / right foot ). Repeat this application twice at the same site, but alternate this with at least one mock application in which no filament is applied (total three questions per site). Protective sensation is present at each site if the patient correctly answers two out of three applications. Protective sensation is absent with two out of three incorrect answers the patient is then considered to be at risk of ulceration. Encourage the patients during testing by giving positive feedback. The healthcare provider should be aware of the possible loss of buckling force of the monofilament if used for too long. Figure 7. Application of the monofilaments Tuning fork The sensory examination should be carried out in a quiet and relaxed setting. First, apply the tuning fork on the patient s wrists (or elbow or clavicle) so that he or she knows what to expect. The patient must not be able to see whether or where the examiner applies the tuning fork. The tuning fork is applied on a bony part on the dorsal side of the distal phalanx of the first toe. The tuning fork should be applied perpendicularly with constant pressure (Figure 8). Repeat this application twice, but alternate this with at least one mock application in which the tuning fork is not vibrating. Figure 6. Sites to be tested with monofilaments Figure 8. How to use a tuning fork
7 Management and Prevention of the Diabetic Foot 231 The test is positive if the patient correctly answers at least two of three applications and negative ( at risk for ulceration ) with two of three incorrect answers. If the patient is unable to sense the vibrations on the big toe, the test is repeated more proximally (malleolus, tibial tuberositas). Encourage the patient during testing by giving positive feedback. Easy-to-use foot screening assessment sheet for clinical examination The foot is at risk if any of the items given are present Deformity or bony prominences Skin not intact (ulcer) Neuropathy Monofilament undetectable Tuning fork undetectable Cotton wool undetectable Abnormal pressure, callus Loss of joint mobility Foot pulses Tibial posterior artery absent Dorsal pedal artery absent Discoloration on dependency Any others Previous ulcer Amputation Inappropriate footwear Conflict of Interest None declared.
Helen Gelly, MD, FUHM, FCCWS
 Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Model of Care for the Diabetic Foot National Clinical Programme for Diabetes Clinical Strategy and Programme Division 2018 Revision number Document drafted by National Clinical Programme for Diabetes Working
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Diabetic Foot Services. Ketan Dhatariya Elsie Bertram Diabetes Centre Norfolk & Norwich University Hospital
 Diabetic Foot Services Ketan Dhatariya Elsie Bertram Diabetes Centre Norfolk & Norwich University Hospital Objectives 1. Background 2. Foot Screening 3. First line management ulceration 4. Management
Diabetic Foot Services Ketan Dhatariya Elsie Bertram Diabetes Centre Norfolk & Norwich University Hospital Objectives 1. Background 2. Foot Screening 3. First line management ulceration 4. Management
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers. Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT
 Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
How can DIABETES affect my FEET? Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
How can DIABETES affect my FEET? By: Emma Howard Specialist Podiatrist and Team Leader, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how
a health care guide Care of your high-risk feet
 a health care guide Care of your high-risk feet Why is it important? Certain medical conditions for example, diabetes, rheumatoid arthritis and circulation disorders can place your feet at high risk of
a health care guide Care of your high-risk feet Why is it important? Certain medical conditions for example, diabetes, rheumatoid arthritis and circulation disorders can place your feet at high risk of
Diabetes - Foot Care
 Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Diabetes - Foot Care Introduction People with diabetes are more likely than others to have problems with their feet. These problems can lead to dangerous infections of the foot. Recognizing and treating
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems
 Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
The Diabetic Foot Latest Statistics
 The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
Podiatry in Practice. Alan M. Singer, DPM, FACFAS
 Podiatry in Practice Alan M. Singer, DPM, FACFAS Podiatry in Practice Alan Singer, D.P.M. UNIVERSITY PODIATRY GROUP Onychomycosis Anti-fungals Onychocryptosis (Ingrown Nails) Ingrown Nails Partial Nail
Podiatry in Practice Alan M. Singer, DPM, FACFAS Podiatry in Practice Alan Singer, D.P.M. UNIVERSITY PODIATRY GROUP Onychomycosis Anti-fungals Onychocryptosis (Ingrown Nails) Ingrown Nails Partial Nail
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme
 Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
LOOKING AFTER YOUR FEET
 LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
LOOKING AFTER YOUR FEET Looking after your feet Diabetes can affect the nerves and blood supply to the feet. Over years, the nerve endings to the feet can be affected by high blood glucose levels, and
Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide
 Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide Diabetes, Obesity & Nutrition Strategic Clinical Network Version 1.0 Acknowledgement This healthcare provider s guide has been adapted from
Diabetes Foot Care Clinical Pathway Healthcare Provider s Guide Diabetes, Obesity & Nutrition Strategic Clinical Network Version 1.0 Acknowledgement This healthcare provider s guide has been adapted from
Aetiology Macroangiopathy occurs mainly distally ie Popliteal artery There is arterial wall calcification Microangiopathy is less common
 DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
Preventing Foot Ulcers in the Neuropathic Diabetic Foot. Glossary of Terms
 Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Rapid Foot Screening
 GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
Front line management of the Diabetic Foot
 Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Screening for diabetic foot complications
 Screening for diabetic foot complications Classifying risk of ulceration 4 Normal sensation, palpable pulses, no deformity Evidence of neuropathy, absence of pedal pulse(s) Evidence of neuropathy, absence
Screening for diabetic foot complications Classifying risk of ulceration 4 Normal sensation, palpable pulses, no deformity Evidence of neuropathy, absence of pedal pulse(s) Evidence of neuropathy, absence
The Diabetic foot. diabetic. foot. the
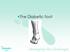 The Diabetic Some basic facts. Diabetes is on increase. Foot ulcers occur in 12% to 25% of people with diabetes. Diabetics who have had a ulcer are more likely to have a re occurrence. Diabetes is biggest
The Diabetic Some basic facts. Diabetes is on increase. Foot ulcers occur in 12% to 25% of people with diabetes. Diabetics who have had a ulcer are more likely to have a re occurrence. Diabetes is biggest
DIABETES AND FOOTCARE
 DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
DIABETES AND FOOTCARE Self-Care and Treatment for Healthy Feet Don t Take Your Feet for Granted Every day, you depend on your feet to keep you moving. But when you have diabetes, your feet need special
Administer 60 Second Foot Screen Tool*
 Basic Foot Care Screen and Self Care Education Toolkit - Central West Diabetes egional Coordination Centre 2012 Foot Care Screening Flow Map Administer 60 Second Foot Screen Tool* Client Education Throughout
Basic Foot Care Screen and Self Care Education Toolkit - Central West Diabetes egional Coordination Centre 2012 Foot Care Screening Flow Map Administer 60 Second Foot Screen Tool* Client Education Throughout
Practical advice when treating feet
 Practical advice when treating feet Helen Mandic Clinical Lead Podiatrist in Health Promotion and Student Mentor Department of Podiatry and Foot Health Dawlish Hospital Falls Prevention The Role of the
Practical advice when treating feet Helen Mandic Clinical Lead Podiatrist in Health Promotion and Student Mentor Department of Podiatry and Foot Health Dawlish Hospital Falls Prevention The Role of the
Patient Product Information
 Patient Product Information REGEN-D 150 (India's First Recombinant Human Epidermal Growth Factor (rhegf) Gel for Diabetic Foot Ulcers) Generic name: [Recombinant Human Epidermal Growth Factor (rhegf)]
Patient Product Information REGEN-D 150 (India's First Recombinant Human Epidermal Growth Factor (rhegf) Gel for Diabetic Foot Ulcers) Generic name: [Recombinant Human Epidermal Growth Factor (rhegf)]
Assessment and Management of Wounds In Diabetes. Maria Mousley Northamptonshire NHS Foundation Trust
 Assessment and Management of Wounds In Diabetes Maria Mousley Northamptonshire NHS Foundation Trust Background At least 61000 people with diabetes in England have a foot ulcer at any given time There are
Assessment and Management of Wounds In Diabetes Maria Mousley Northamptonshire NHS Foundation Trust Background At least 61000 people with diabetes in England have a foot ulcer at any given time There are
Model of care for the diabetic foot
 Model of care for the diabetic foot Item type Authors Citation Publisher Report National Diabetes Programme Working Group National Diabetes Programme Working Group. Model of care for the diabetic foot.
Model of care for the diabetic foot Item type Authors Citation Publisher Report National Diabetes Programme Working Group National Diabetes Programme Working Group. Model of care for the diabetic foot.
People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy.
 Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Our Vision NADA BoD Strategic Planning Session -
 Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
Who we are NADA is a not-for-profit members-led organization established in 1995 as a result of the rising rates of diabetes among First Nations, Inuit and Métis Peoples in Canada Our Vision - 2016 NADA
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Type 2 diabetes: prevention and management of foot problems
 Type 2 diabetes: prevention and management of foot problems NICE guideline Revised version Second draft for consultation, August 2003 If you wish to comment on the recommendations, please make your comments
Type 2 diabetes: prevention and management of foot problems NICE guideline Revised version Second draft for consultation, August 2003 If you wish to comment on the recommendations, please make your comments
AGONY FEET. The. of the. Prevention and management of diabetic foot ulcers
 The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
You have high risk feet
 You have high risk feet diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY. Emergency Department
You have high risk feet diabetes information and advice leaflet Emergency Action Plan FOOT ATTACK? If your foot is red, swollen or if you have skin breakdown RING 07786250788 IMMEDIATELY. Emergency Department
1 of :19
 1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetes Manual. Foot Care
 Diabetes Manual Foot Care Diabetes Service, Country Health SA April 2013 Authors/Reviewers Jane Giles, Advanced Clinical Practice Consultant, RN CDE Diabetes Service, Country Health SA Kate Visentin, Clinical
Diabetes Manual Foot Care Diabetes Service, Country Health SA April 2013 Authors/Reviewers Jane Giles, Advanced Clinical Practice Consultant, RN CDE Diabetes Service, Country Health SA Kate Visentin, Clinical
Diabetes-Diabetes Mellitus About one in five people with diabetes will enter the hospital for foot problems. DIABETIC FOOT PROBLEMS by Robert
 Diabetes-Diabetes Mellitus About one in five people with diabetes will enter the hospital for foot problems. DIABETIC FOOT PROBLEMS by Robert Frykberg, DPM Foot problems are leading causes of hospitalization
Diabetes-Diabetes Mellitus About one in five people with diabetes will enter the hospital for foot problems. DIABETIC FOOT PROBLEMS by Robert Frykberg, DPM Foot problems are leading causes of hospitalization
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
A Guide for People With Diabetes. Take Care of Your Feet for a
 A Guide for People With Diabetes Take Care of Your Feet for a You can take care of your feet! Do you want to avoid serious foot problems that can lead to a toe, foot, or leg amputation? Take Care of Your
A Guide for People With Diabetes Take Care of Your Feet for a You can take care of your feet! Do you want to avoid serious foot problems that can lead to a toe, foot, or leg amputation? Take Care of Your
This document is available, on request, in accessible formats, including Braille, CD, audio cassette and minority languages.
 Diabetic Foot Care Cover:Layout 1 18/12/08 14:35 Page 1 email: info@northerntrust.hscni.net This document is available, on request, in accessible formats, including Braille, CD, audio cassette and minority
Diabetic Foot Care Cover:Layout 1 18/12/08 14:35 Page 1 email: info@northerntrust.hscni.net This document is available, on request, in accessible formats, including Braille, CD, audio cassette and minority
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Diabetes Mellitus and the Associated Complications
 Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Diabetic Feet. Juanita Muller
 Diabetic Feet Juanita Muller Mr RR 69 year old male CHARCOT ARTHROPATHY Diabetic Feet Callus Acute injury and ulceration Infection Osteomylitis Chronic ulceration Ischaemic necrosis Charcot s arthropathy
Diabetic Feet Juanita Muller Mr RR 69 year old male CHARCOT ARTHROPATHY Diabetic Feet Callus Acute injury and ulceration Infection Osteomylitis Chronic ulceration Ischaemic necrosis Charcot s arthropathy
Foot protection for people with diabetes a focus on prevention
 Foot protection for people with diabetes a focus on prevention Presentation by Mike Townson Independent Podiatry Consultant. Facilitated by Angela Farrell Neubourg Pharma UK Ltd. Foot Assessment training
Foot protection for people with diabetes a focus on prevention Presentation by Mike Townson Independent Podiatry Consultant. Facilitated by Angela Farrell Neubourg Pharma UK Ltd. Foot Assessment training
Peripheral Neuropathy
 Peripheral Neuropathy Neuropathy affects 30-50% of patient population with diabetes and this prevalence tends to increase proportionally with duration of diabetes and dependant on control. Often presents
Peripheral Neuropathy Neuropathy affects 30-50% of patient population with diabetes and this prevalence tends to increase proportionally with duration of diabetes and dependant on control. Often presents
10/19/2017. Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI. Consultant with J&J-Depuy-Synthesis
 Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
of :07
 he diabetic foot ulcer - management and outcomes of 6 3-12-2012 11:07 The diabetic foot ulcer - management and outcomes Impaired perfusion Infection Extent and depth Condition of the ulcer Site Sensation
he diabetic foot ulcer - management and outcomes of 6 3-12-2012 11:07 The diabetic foot ulcer - management and outcomes Impaired perfusion Infection Extent and depth Condition of the ulcer Site Sensation
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Diabetic Foot Pathophysiology. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetes is a serious disease that can develop from lack of insulin production in the body or due to
 Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
Page 1 The Diabetic Foot Definition Diabetes is a serious disease that can develop from lack of insulin production in the body or due to the inability of the body's insulin to perform its normal everyday
How to Fight Diabetes and Win. Taking Care of. Your Feet
 How to Fight Diabetes and Win Taking Care of Your Feet TAKING CARE OF YOUR FEET Developing a good foot care plan is very important when you have diabetes. Diabetes and Your Feet Diabetes affects many areas
How to Fight Diabetes and Win Taking Care of Your Feet TAKING CARE OF YOUR FEET Developing a good foot care plan is very important when you have diabetes. Diabetes and Your Feet Diabetes affects many areas
Advice for rheumatoid patients at risk of developing foot related problems
 Advice for rheumatoid patients at risk of developing foot related problems Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Advice for rheumatoid patients at risk of developing foot related problems Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast,
Diabetes Foot and Skin Care. Diabetes and the feet. Foot problems: Major cause of morbidity and mortality
 Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY CLINICAL GUIDELINES TABLE OF CONTENTS. Diabetes Mellitus and Podiatric Care 2
 NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY 2012-2013 CLINICAL GUIDELINES TABLE OF CONTENTS CONDITION PAGE(S) Diabetes Mellitus and Podiatric Care 2 Fractures 3-4 Heel Pain (Posterior) Retrocalcaneal
NORTHEAST OHIO NEIGHBORHOOD HEALTH SERVICES, INC. PODIATRY 2012-2013 CLINICAL GUIDELINES TABLE OF CONTENTS CONDITION PAGE(S) Diabetes Mellitus and Podiatric Care 2 Fractures 3-4 Heel Pain (Posterior) Retrocalcaneal
Advice for People with Diabetes
 General Foot Health Advice for People with Diabetes Podiatry - Diabetic Neuropathy Diabetic Neuropathy Diabetic Neuropathy is a term used to describe nerve damage which most commonly affects the leg and
General Foot Health Advice for People with Diabetes Podiatry - Diabetic Neuropathy Diabetic Neuropathy Diabetic Neuropathy is a term used to describe nerve damage which most commonly affects the leg and
Thames Valley Strategic Clincal Network (TVSCN) Diabetes Footcare Pathway from average to excellent
 Thames Valley Strategic Clincal Network (TVSCN) Diabetes Footcare Pathway from average to excellent Prepared by the TV SCN Diabetic Foot Reference Group October 2015 Version 1.6 1 Thames Valley Diabetes
Thames Valley Strategic Clincal Network (TVSCN) Diabetes Footcare Pathway from average to excellent Prepared by the TV SCN Diabetic Foot Reference Group October 2015 Version 1.6 1 Thames Valley Diabetes
University of Huddersfield Repository
 University of Huddersfield Repository Newton, Veronica and Roberts, Peter Foot Inspection or Foot Assessment? Original Citation Newton, Veronica and Roberts, Peter (2011) Foot Inspection or Foot Assessment?
University of Huddersfield Repository Newton, Veronica and Roberts, Peter Foot Inspection or Foot Assessment? Original Citation Newton, Veronica and Roberts, Peter (2011) Foot Inspection or Foot Assessment?
Patient & Family Guide. Diabetic Foot Ulcer.
 Patient & Family Guide Diabetic Foot Ulcer 2018 www.nshealth.ca Diabetic Foot Ulcer What is a diabetic foot ulcer? The term foot ulcer is used to describe an open sore that happens below the ankle and
Patient & Family Guide Diabetic Foot Ulcer 2018 www.nshealth.ca Diabetic Foot Ulcer What is a diabetic foot ulcer? The term foot ulcer is used to describe an open sore that happens below the ankle and
AIM OF MASTERCLASS. Overview of the diabetic foot disease. Modern approach to management
 AIM OF MASTERCLASS Overview of the diabetic foot disease Modern approach to management DIABETIC FOOT DISEASE THROUGHOUT THE WORLD, THERE IS AN AMPUTATION EVERY 20 SECONDS MOST OF THESE AMPUTATIONS ARE
AIM OF MASTERCLASS Overview of the diabetic foot disease Modern approach to management DIABETIC FOOT DISEASE THROUGHOUT THE WORLD, THERE IS AN AMPUTATION EVERY 20 SECONDS MOST OF THESE AMPUTATIONS ARE
UNIT FOUR LESSON 11 OUTLINE
 UNIT FOUR LESSON 11 OUTLINE Tell participants: Taking care of your feet is an important part of diabetes management. Diabetes is the leading cause of amputations of the lower limbs. In Kentucky, there
UNIT FOUR LESSON 11 OUTLINE Tell participants: Taking care of your feet is an important part of diabetes management. Diabetes is the leading cause of amputations of the lower limbs. In Kentucky, there
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT
 Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
Foot Care. Taking steps towards good FOR AT-RISK FEET. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a LOW RISK of developing serious problems,
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a LOW RISK of developing serious problems,
Lesser toe sequential repair
 Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014
 Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014 Dr. Michael Yan, MD, CCFP Clinical Lecturer, Department of Family Medicine, University of
Happy Feet: Feeling good about diabe.c foot screening! Family Medicine Forum 2014, Quebec City November 14, 2014 Dr. Michael Yan, MD, CCFP Clinical Lecturer, Department of Family Medicine, University of
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Project I - Background Worksheet. Team Members: Kira Brown, Paige Fallu. Clinical problem Diabetic Foot Ulcers
 Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
Project I - Background Worksheet Team Members: Kira Brown, Paige Fallu Clinical problem Diabetic Foot Ulcers 1) Strategic Focus based on the Strategic focus powerpoint presentation and readings a. Team
Rapid Recovery Hyperbarics 9439 Archibald Ave. Suite 104 Rancho Cucamonga CA,
 Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
National Aboriginal Diabetes Association
 National Aboriginal Diabetes Association 2015 To increase awareness of diabetes and foot care management Disclaimer: This presentation is offered as educational information and shall not be used as a substitute
National Aboriginal Diabetes Association 2015 To increase awareness of diabetes and foot care management Disclaimer: This presentation is offered as educational information and shall not be used as a substitute
A guide to diabetes footcare. Department of Podiatry. patientinformation
 Department of Podiatry patientinformation Hearing about your experience of our services is very important as it means we can pass compliments to our staff and make improvements where necessary. Tell us
Department of Podiatry patientinformation Hearing about your experience of our services is very important as it means we can pass compliments to our staff and make improvements where necessary. Tell us
Leg Ulcer Case Study
 Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Leg Ulcer Case Study Wound Healing Community Outreach Service Mrs Ivy Hurtzalot, a 71-year-old lady, presents to her general practitioner with an ulcer on her right medial malleolus. Ivy reveals that the
Putting feet first: national minimum skills framework
 In partnership with Putting feet first: national minimum skills framework The national minimum skills framework for commissioning of footcare services for people with diabetes Revised March 2011 This report
In partnership with Putting feet first: national minimum skills framework The national minimum skills framework for commissioning of footcare services for people with diabetes Revised March 2011 This report
My Diabetic Patient Has No Pulses; What Should I Do?
 Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
Emily Malgor, MD Assistant Professor of Surgery University of Oklahoma, Oklahoma City My Diabetic Patient Has No Pulses; What Should I Do? There are no disclosures. Background Diabetes affects 387 million
Integumentary Physical Therapy 피부계물리치료학
 Integumentary Physical Therapy 피부계물리치료학 Dong-Ryul Lee, PT, Ph.D. Movement Impairment Specialist & Performance Enhancement Specialist Neurofeedback, Robotics & Virtual Reality Research Specialites: NeuroRehabilitation
Integumentary Physical Therapy 피부계물리치료학 Dong-Ryul Lee, PT, Ph.D. Movement Impairment Specialist & Performance Enhancement Specialist Neurofeedback, Robotics & Virtual Reality Research Specialites: NeuroRehabilitation
Renal Foot Care. Christian Pankhurst
 Renal Foot Care Christian Pankhurst The consequences of poor management of the renal foot are considerable: prolonged ulceration and ill health, gangrene and amputation, depression and death. The health
Renal Foot Care Christian Pankhurst The consequences of poor management of the renal foot are considerable: prolonged ulceration and ill health, gangrene and amputation, depression and death. The health
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
THE DIABETIC FOOT. Nicola Kilburn Diabetes Specialist Podiatrist
 THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
THE DIABETIC FOOT Nicola Kilburn Diabetes Specialist Podiatrist Diabetic foot disease is associated with significant morbidity and mortality. Foot screening is effective in identifying an individuals risk
Podiatric Medicine: Best Foot Forward. Dr. Kevin J. DeAngelis, DPM Brandywine Family Foot Care 213 Reeceville Rd. Suite 13 Coatesville, PA
 Podiatric Medicine: Best Foot Forward Dr. Kevin J. DeAngelis, DPM Brandywine Family Foot Care 213 Reeceville Rd. Suite 13 Coatesville, PA What is a Podiatrist? Specially trained physician specializing
Podiatric Medicine: Best Foot Forward Dr. Kevin J. DeAngelis, DPM Brandywine Family Foot Care 213 Reeceville Rd. Suite 13 Coatesville, PA What is a Podiatrist? Specially trained physician specializing
A new classification of the diabetic ischaemic foot promotes a modern approach to treatment. Michael Edmonds King s College Hospital London
 A new classification of the diabetic ischaemic foot promotes a modern approach to treatment Michael Edmonds King s College Hospital London Disclosure Speaker name: Michael Edmonds... I have the following
A new classification of the diabetic ischaemic foot promotes a modern approach to treatment Michael Edmonds King s College Hospital London Disclosure Speaker name: Michael Edmonds... I have the following
Multidisciplinary diabetic foot project - Samoa
 Multidisciplinary diabetic foot project - Samoa The World Health Organization and the International Diabetes Federation have stated that up to 85 percent of diabetic lower extremity amputations are preventable
Multidisciplinary diabetic foot project - Samoa The World Health Organization and the International Diabetes Federation have stated that up to 85 percent of diabetic lower extremity amputations are preventable
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
HOW TO SPOT A FOOT ATTACK PREVENTING SERIOUS FOOT PROBLEMS
 HOW TO SPOT A FOOT ATTACK PREVENTING SERIOUS FOOT PROBLEMS Your foot check has shown that there is a high risk that you could develop serious foot problems 2 YOUR FEET MATTER If you ve been given this
HOW TO SPOT A FOOT ATTACK PREVENTING SERIOUS FOOT PROBLEMS Your foot check has shown that there is a high risk that you could develop serious foot problems 2 YOUR FEET MATTER If you ve been given this
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR
 ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
Diabetes Footcare Pathway from average to excellent
 Thames Valley Strategic Clincal Network Diabetes Footcare Pathway from average to excellent Prepared by the TV SCN Diabetic Foot Reference Group November 2015 Thames Valley Diabetic Footcare Pathway, Version
Thames Valley Strategic Clincal Network Diabetes Footcare Pathway from average to excellent Prepared by the TV SCN Diabetic Foot Reference Group November 2015 Thames Valley Diabetic Footcare Pathway, Version
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Clinical Guideline for: Diagnosis and Management of Charcot Foot
 Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Northumbria Healthcare NHS Foundation Trust. Preparing For Foot and Ankle Surgery. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Preparing For Foot and Ankle Surgery Issued by the Orthopaedic Department This leaflet gives you information about what is involved in foot and ankle surgery.
Northumbria Healthcare NHS Foundation Trust Preparing For Foot and Ankle Surgery Issued by the Orthopaedic Department This leaflet gives you information about what is involved in foot and ankle surgery.
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Contents. The Diabetic Foot 3. Essentials of Diabetic Foot Care 5. Numbness in Feet, But No Diabetes? Here s What Else It Could Be 7
 Contents The Diabetic Foot 3 Essentials of Diabetic Foot Care 5 Numbness in Feet, But No Diabetes? Here s What Else It Could Be 7 Proper Shoes For Diabetics 9 How to Treat and Prevent a Diabetic Foot Ulcer
Contents The Diabetic Foot 3 Essentials of Diabetic Foot Care 5 Numbness in Feet, But No Diabetes? Here s What Else It Could Be 7 Proper Shoes For Diabetics 9 How to Treat and Prevent a Diabetic Foot Ulcer
Diabetic Foot Problems
 http://www.medicine-on-line.com Diabetic foot disease: 1/12 Diabetic Foot Problems Author: Affiliation: Rebecca Wong BN, MSc(Health Care) Prince of Wales Hospital, Hong Kong SAR Introduction Diabetes Mellitus
http://www.medicine-on-line.com Diabetic foot disease: 1/12 Diabetic Foot Problems Author: Affiliation: Rebecca Wong BN, MSc(Health Care) Prince of Wales Hospital, Hong Kong SAR Introduction Diabetes Mellitus
Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태
 Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태 DMF Protocol VIPS approach V : Vascular I : infection P : Pressure off S : specific wound care Ulcer/Pressure off& Biomechanics PVD vs Peripheral neuropathy NP
Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태 DMF Protocol VIPS approach V : Vascular I : infection P : Pressure off S : specific wound care Ulcer/Pressure off& Biomechanics PVD vs Peripheral neuropathy NP
