Technical considerations for the fully robotic pancreaticoduodenectomy
|
|
|
- Quentin Casey
- 6 years ago
- Views:
Transcription
1 Surgical Techniques on Pancreatic Surgery Technical considerations for the fully robotic pancreaticoduodenectomy Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He Department of Surgery, The Johns Hopkins Hospital Baltimore, MD 21215, USA Correspondence to: Jin He, MD, PhD. Assistant Professor of Surgery, Department of Surgery, The Johns Hopkins Hospital, 600 N Wolfe Street, Halsted 614, Baltimore, MD 21287, USA. jhe11@jhmi.edu. Abstract: Minimally invasive surgery, including robotic surgery, has become the standard of care for many abdominal procedures. However, the technical complexity associated with pancreaticoduodenectomy (PD) due to the anatomic location and oncologic characteristics of pancreatic tumors has hindered the widespread application of minimally invasive techniques to this procedure. Recent studies have reported that for experienced surgeons, the application of robotic techniques to PD is associated with equivalent oncologic outcomes and rates of complication when compared to an open operation, and may be associated with accelerated surgical recovery. Despite these encouraging results, robotic PD (RPD) is a procedure attempted by a small group of pancreatic surgeons, leading to the great heterogeneity in the techniques used to perform this operation. Herein we describe our technique for fully RPD and demonstrate its execution with a video supplement. Keywords: Pancreaticoduodenectomy (PD); robotic surgery; Whipple procedure Received: 05 April 2017; Accepted: 04 May 2017; Published: 12 June doi: /jovs View this article at: Introduction Pancreaticoduodenectomy (PD), also known as the Whipple, is known to be one of the most challenging and complex abdominal surgical procedures. It remains the only potentially curative procedure for periampullary tumors (1,2). The paramount complexity of this operation can be attributed to the anatomic location of the pancreas within the retroperitoneum, proximity to major visceral vasculature, and the difficult reconstruction required to re-establish gastrointestinal continuity (3-10). In 1994, Gagner and Pomp reported the first successful laparoscopic PD (11-13). Over time, studies have demonstrated the safety and feasibility of laparoscopic pancreatic surgery, as well as reported benefits in terms of postoperative outcomes and equivalent oncologic results when performed by experienced surgeons (14-18). Despite this, only a minority of pancreatic surgeons implemented the laparoscopic approach due to its particular technical challenges, including the difficult nature of the dissection, multiple anastomoses, and steep learning curve. The development of the robotic surgical platform introduced a three-dimensional view and an extended range of motion, effectively overcoming many of factors limiting a laparoscopic approach to the pancreatic head. In 2003, Giulianotti and colleges reported the first series of robotic PD (RPD) (13). In subsequent years, varied robotic approaches RPD were published, including many hybrid applications of the technology (19). Clearly, despite the technological advantages of the robotic approach, there remains a steep learning curve to the mastery of its technical execution by surgeons. Many institutions remain in the early stages of implementing robotic pancreatic surgery, contributing to the wide variability in how these procedures are performed. Despite the variation in RPD techniques, data from high volume centers support that RPD equal results in terms of morbidity and mortality, and associated with decreased intraoperative blood loss and length of stay when compared with open approaches (8). Additionally, other studies have demonstrated RPD is associated with equivalent oncologic outcomes in terms of margin positivity
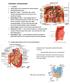
2 Page 2 of 5 Journal of Visualized Surgery, 2017 Figure 1 Fully robotic pancreaticoduodenectomy (Whipple procedure) (22). and adequate lymphadenectomy when compared with open techniques (20,21). Although the equivalency of RPD to established open techniques has been demonstrated, the robotic approach associated with extended operative times. Here we describe our technique for RPD, share our tips to facilitate the key steps of the procedure, and demonstrate its operative execution in the accompanying video (Figure 1). Patient selection Video 1. Fully robotic pancreaticoduodenectomy (Whipple procedure) Daniel Galvez, Rebecca Sorber, Ammar A. Javed, Jin He* Department of Surgery, The Johns Hopkins Hospital Baltimore, MD, USA Available online: Careful patient selection is the critical first step in the successful application of the robotic approach to PD. The potential for conversion to an open approach is relatively high, with an overall conversion rate 17.8% in a recent review (8). While the decision to convert to an open procedure intra-operatively is a reflection of good surgical judgment, there exists a significant expenditure of resources associated with an aborted robotic procedure. This technique should be applied scrupulously with good preoperative as well as intraoperative judgment if it is to benefit outcomes and prove to be cost effective. The patient s body habitus, prior abdominal surgery, and etiology of the patient s disease should be considered strongly. At experienced centers, RPD can be safely and effectively applied to a wide range of benign and malignant lesions of the pancreatic head and neck with varying degrees of vascular involvement (23-25). However, for those surgeons and institutions in the early stages of incorporating RPD into their practice, it is helpful to apply the technique first to small benign and premalignant pancreatic lesions, as these operations tend to be more anatomically straightforward and with minimal risk of vascular invasion (26). Due to these considerations, high quality imaging in the form of a pancreas protocol CT or MRI is required as part of the preoperative workup to determine resectability, as well as identify any aberrant vasculature. Clinical summary The patient in this video was a 68-year-old obese male who presented with several months of indigestion, weight loss and newly diagnosed diabetes mellitus. Subsequent imaging demonstrated a 3.2 cm 2.3 cm mass in the head of the pancreas with associated dilatation of the main pancreatic duct to 5 mm. The mass was noted to abut the portal vein. Furthermore, the patient was noted to have an accessory right hepatic artery originating from the celiac axis. Endoscopic ultrasound and fine needle biopsy diagnosis of pancreatic ductal adenocarcinoma. Preoperative workup included a high quality abdominal CT scan showing resectable cancer and no evidence of distant metastases. Like other patients presenting with resectable disease at our institution, this patient was enrolled in a clinical trial which he received a combination of cyclophosphamide, nivolumab and a study vaccine in the neoadjuvant setting. The patient underwent RPD and had an uneventful recovery. On postoperative day (POD) 1, the nasogastric tube was removed and the patient was started on sips of water and ice chips. Deep vein thrombosis prophylaxis was initiated and maintained throughout the hospital course. On POD 2 the Foley catheter was removed and he was able to void spontaneously. By POD 4, he was tolerating a regular diet with pancreatic enzyme supplementation. His JP drains were removed on POD 5 and 6. The average length of stay for a RPD at our institution is 7 days. Setup For maximum effectiveness and optimal outcomes after RPD, the importance of a surgical team (i.e., anesthesiologist, bedside assistant, scrub tech and circulator) with robotics experience cannot be overstated. We routinely place a nasogastric tube to decompress the stomach. After induction of general anesthesia, the patient was placed in a supine and split leg position. A 15 mmhg pneumoperitoneum is established using a Veress needle or a Hasson technique. A 12 mm trocar was placed at the umbilical site and the robotic camera was introduced for abdominal exploration to rule out gross carcinomatosis, liver metastasis and extensive intraabdominal adhesions. If
3 Journal of Visualized Surgery, 2017 Page 3 of 5 Figure 2 Trocar placement. no prohibitive anatomy or pathology was identified, four 8 mm robotic trocars were placed (Figure 2) under direct visual guidance. After placement of all trocars, the da Vinci Xi system was docked from the patient s left side, with the assistant at the bedside to facilitate instrument exchange. Exposure and dissection In general, we perform the dissection starting with the bile duct, followed by the stomach, pancreas and jejunum. A robotic vessel sealer was used to divide the ligamentum teres and falciform ligament. This viable tissue flap may be used later to cover biliary anastomosis and the gastroduodenal artery (GDA) stump. We entered the lesser sac by dividing the gastro-colic ligament on the greater curvature of the stomach, exposing the pancreas. Once the superior and inferior borders of the pancreas were delineated, dissection of the porta hepatis was performed. We dissected the cystic duct and artery within Calot s triangle. After confirming the critical view, we double clipped them with Hem-o-lock clips and transected them with the robotic scissor. We isolated the common hepatic duct and transected it above the confluence of the cystic and common bile duct. Of note, the aberrant anatomy of the hepatic artery should be considered here to avoid injury on a replaced right or accessory right hepatic artery, as was the case in our patient. We routinely perform portal lymphadenectomy, which helps skeletonize the proper hepatic artery and portal vein. Once isolated, we traced the proper hepatic to the common hepatic artery. The root of the right gastric artery was identified, clipped and transected with the vessel sealer. Next, the GDA takeoff from the hepatic artery was isolated. The GDA was test clamped to ensure adequate hepatic perfusion via the common hepatic artery. Once adequate perfusion was confirmed, the GDA was ligated with a 2-0 silk tie, double clipped with Hem-o-lock clips, and transected with scissors. The vessel sealer was used to take the omentum down from the greater and lesser curves of the stomach. An Endo-GIA stapler was used to divide the stomach approximately 5 cm proximal to the pylorus. The choice of a green or black staple cartridge depends on the thickness of the stomach. We continued the dissection to mobilize the hepatic artery away from the portal vein along the superior edge of the pancreas. During this part of the portal vein dissection, care should be taken to avoid uncontrolled division of the superior pancreaticoduodenal vein on the lateral side of the portal vein. Dissection was continued along the inferior edge of pancreas. With the portal vein dissected out above the pancreas, the superior mesenteric vein (SMV) could be easily identified. A retropancreatic tunnel on top of the portal vein was carefully created with blunt dissection. We used an umbilical tape to suspend the pancreatic neck to avoid injury to the portal vein during the transection of the pancreatic neck. We continued the sharp dissection to mobilize the pancreatic neck and head off the portal vein. Dissection was continued along the SMV. The first tributary to the SMV is the gastrocolic trunk of Henle, which drains the right gastroepiploic vein and the right superior colic vein. The Henle trunk was carefully dissected out, clipped and transected with scissors. Once the SMV was isolated, the omentum and transverse colon were free from the head of the pancreas. The Kocher maneuver was performed to mobilize the pancreatic head and duodenum from the retroperitoneum. The inferior vena cava and the abdominal aorta were exposed. The left renal vein often located across the ventral side of the aorta was carefully identified. The root of the superior mesenteric artery (SMA) was above the left renal vein and needed to be very carefully preserved. The ligament of Treitz can often be divided on the right side of the root of mesentery if the patient has minimal amount of intra-abdominal fat. When the patient is obese, it is easier to identify the ligament of Treitz at its normal position and divide it before the Kocher maneuver. After the first portion of the jejunum was pulled to the right upper quadrant, it was transected using an Endo-GIA stapler. The vessel sealer was used to divide the mesentery along the jejunum until the uncinate of the pancreas.
4 Page 4 of 5 Journal of Visualized Surgery, 2017 The transection of the uncinate along the right side of the SMA was the most challenging part. The current robotic vessel sealer is bulky and not suitable for fine dissection. When the tumor is not involving the uncinate, the vessel sealer can be used to divide the tissue along the right side of SMA. If the tumor is close to the uncinate, we often use combination of hook cautery and bipolar Maryland clamp to transect the tissue along the SMA. The inferior pancreaticoduodenal artery was identified, isolated, clipped and transected with the vessel sealer. The dissection along the SMA was performed from caudal to cephalad direction. In this particular case, the accessory right hepatic artery was identified as coming from the celiac axis and preserved. Finally, the gallbladder was taken down from the liver cystic plate using the hook cautery. A large Endo-Catch bag was used to retrieve the Whipple specimen. hepatic duct were larger than 5 mm in diameter, we would choose the running PDS suture for this anastomosis. Lastly, the jejunum on the left side of the mesenteric root was identified for GJ anastomosis. We performed an antecolic side-to-side isoperistaltic GJ utilizing a 60 mm blue load Endo-GIA stapler. In order to achieve a tensionfree GJ anastomosis, it may be necessary to divide the omentum for obese patients. The enterotomy site was closed with 3-0 V-Loc in 2 layers in a running fashion. In this case, the GJ anastomosis was covered with an omental flap and the ligamentum teres flap was utilized to cover the GDA stump. We routinely use two 19-French Blake drains through the existing lateral robotic port sites. We find it helpful to have a systematic convention in which the right-sided drain was positioned posterior to the PJ anastomosis and the leftsided drain anterior to the PJ anastomosis. Reconstruction After the specimen was removed from the peri-umbilical port site, we re-established the pneumoperitoneum. Hemostasis was confirmed before the reconstruction. The order of anastomoses performed during the RPD was the same as that in the open procedure, in which the pancreaticojejunostomy (PJ) was performed first, followed by the hepaticojejunostomy (HJ), and finally the gastrojejunostomy (GJ). We performed a retrocolic standard end-to-side PJ in 2 layers. The posterior edge of the pancreatic neck was secured to the bowel with a running 3-0 V-Loc suture. A pin-hole enterotomy was made next to the pancreatic duct. The duct-to-mucosa anastomosis was performed using 5-0 PDS sutures applied in an interrupted fashion. The caliber of the main pancreatic duct dictates the number of sutures on the PJ and the size of a pancreatic stent. We routinely use pediatric feeding tube as pancreatic stent to across the duct-to-mucosa anastomosis. In general, 4 6 interrupted sutures are sufficient to secure the duct-to-mucosa anastomosis. The PJ was finished with a second anterior line of running 3-0 V-Loc suture between the pancreas and jejunum. Approximately 5 cm distal to the PJ, an end-to-side HJ was created. The 5-0 PDS sutures were placed in an interrupted fashion to secure the hepatic duct to jejunum. In this case, a total of 12 interrupted sutures were placed to form the HJ. The number of sutures should be dictated by the caliber of the dilated CBD. If the diameter of the Tips, tricks and pitfalls Selection of anatomically and pathologically favorable candidate patients is key for successful execution of RPD, especially for those new to the technique. Once isolated, the GDA should be test clamped prior to division to assess hepatic perfusion via the common hepatic artery alone; if adequacy of flow is in question, a Doppler may be introduced for further confirmation. Following retro-pancreatic tunneling, an umbilical tape is passed through the tunnel and used to retract the gland anteriorly to facilitate a controlled pancreatic division. To prevent excess blood loss during final mobilization, care should be taken to actively identify the inferior pancreaticoduodenal vein on the anterior surface of the PV as well as small branches of SMA perfusing the specimen. We perform a 2 layer end to side PJ: the pancreatic neck is secured to the bowel with a running 3-0 V-Loc suture and the pancreatic duct is secured to the jejunal mucosa with 4 6 interrupted 5-0 PDS sutures. The HJ is completed in an end to side fashion with interrupted 5-0 PDS sutures; the number of sutures is dictated by the caliber of the dilated CBD. The tissue flap created on division of the ligamentum teres at the beginning of the case may be utilized for protection of the GDA stump. Acknowledgements None.
5 Journal of Visualized Surgery, 2017 Page 5 of 5 Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Dai R, Turley RS, Blazer DG. Contemporary review of minimally invasive pancreaticoduodenectomy. World J Gastrointest Surg 2016;8: He J, Ahuja N, Makary MA, et al resected periampullary adenocarcinomas at a single institution: trends over three decades. HPB (Oxford) 2014;16: Doula C, Kostakis ID, Damaskos C, et al. Comparison Between Minimally Invasive and Open Pancreaticoduodenectomy: A Systematic Review. Surg Laparosc Endosc Percutan Tech 2016;26: Joyce D, Morris-Stiff G, Falk GA, et al. Robotic surgery of the pancreas. World J Gastroenterol 2014;20: Memeo R, Sangiuolo F, de Blasi V, et al. Robotic pancreaticoduodenectomy and distal pancreatectomy: State of the art. J Visc Surg 2016;153: Memeo R, Tzedakis S, de Blasi V, et al. Robotic Pancreaticoduodenectomy: Operative Steps (With Video). Surg Laparosc Endosc Percutan Tech 2016;26:e Parisi A, Desiderio J, Trastulli S, et al. Robotic pyloruspreserving pancreaticoduodenectomy: Technical considerations. Int J Surg 2015;21 Suppl 1:S Wang M, Cai H, Meng L, et al. Minimally invasive pancreaticoduodenectomy: A comprehensive review. Int J Surg 2016;35: Zeh HJ, 3rd, Bartlett DL, Moser AJ. Robotic-assisted major pancreatic resection. Adv Surg 2011;45: Zhang YH, Zhang CW, Hu ZM, et al. Pancreatic cancer: Open or minimally invasive surgery? World J Gastroenterol 2016;22: Baker EH, Ross SW, Seshadri R, et al. Robotic pancreaticoduodenectomy for pancreatic adenocarcinoma: role in 2014 and beyond. J Gastrointest Oncol 2015;6: Liao CH, Wu YT, Liu YY, et al. Systemic Review of the Feasibility and Advantage of Minimally Invasive Pancreaticoduodenectomy. World J Surg 2016;40: Wright GP, Zureikat AH. Development of Minimally Invasive Pancreatic Surgery: an Evidence-Based Systematic Review of Laparoscopic Versus Robotic Approaches. J Gastrointest Surg 2016;20: Coratti A, Di Marino M, Coratti F, et al. Initial Experience With Robotic Pancreatic Surgery: Technical Feasibility and Oncological Implications. Surg Laparosc Endosc Percutan Tech 2016;26: Croner RS. Robotic Pancreatic Resections: Feasibility and Advantages. Indian J Surg 2015;77: Peng L, Lin S, Li Y, et al. Systematic review and metaanalysis of robotic versus open pancreaticoduodenectomy. Surg Endosc [Epub ahead of print]. 17. Place TL, Nau P, Mezhir JJ. Minimally invasive pancreatectomy for cancer: a critical review of the current literature. J Gastrointest Surg 2015;19: Zureikat AH, Postlewait LM, Liu Y, et al. A Multiinstitutional Comparison of Perioperative Outcomes of Robotic and Open Pancreaticoduodenectomy. Ann Surg 2016;264: Narula VK, Mikami DJ, Melvin WS. Robotic and laparoscopic pancreaticoduodenectomy: a hybrid approach. Pancreas 2010;39: Corcione F, Pirozzi F, Cuccurullo D, et al. Laparoscopic pancreaticoduodenectomy: experience of 22 cases. Surg Endosc 2013;27: Walsh RM, Chalikonda S. How I Do It: Hybrid Laparoscopic and Robotic Pancreaticoduodenectomy. J Gastrointest Surg 2016;20: Galvez D, Sorber R, Javed AA, et al. Fully robotic pancreaticoduodenectomy (Whipple procedure). Asvide 2017;4:244. Available online: articles/ Adam MA, Choudhury K, Dinan MA, et al. Minimally Invasive Versus Open Pancreaticoduodenectomy for Cancer: Practice Patterns and Short-term Outcomes Among 7061 Patients. Ann Surg 2015;262: Baker EH, Ross SW, Seshadri R, et al. Robotic pancreaticoduodenectomy: comparison of complications and cost to the open approach. Int J Med Robot 2016;12: Piedimonte S, Wang Y, Bergman S, et al. Early experience with robotic pancreatic surgery in a Canadian institution. Can J Surg 2015;58: Boone BA, Zenati M, Hogg ME, et al. Assessment of quality outcomes for robotic pancreaticoduodenectomy: identification of the learning curve. JAMA Surg 2015;150: doi: /jovs Cite this article as: Galvez D, Sorber R, Javed AA, He J. Technical considerations for the fully robotic pancreaticoduodenectomy..
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP
 ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Outcomes of robotic surgery for pancreatic ductal adenocarcinoma
 Original Article Outcomes of robotic surgery for pancreatic ductal adenocarcinoma Qian Zhan 1,2, Xiaxing Deng 1,2, Yuanchi Weng 1,2, Jiabin Jin 1,2, Zhichong Wu 1,2, Hongwei Li 1,2, Baiyong Shen 1,2, Chenghong
Original Article Outcomes of robotic surgery for pancreatic ductal adenocarcinoma Qian Zhan 1,2, Xiaxing Deng 1,2, Yuanchi Weng 1,2, Jiabin Jin 1,2, Zhichong Wu 1,2, Hongwei Li 1,2, Baiyong Shen 1,2, Chenghong
Anatomy of the SMALL INTESTINE. Dr. Noman Ullah Wazir PMC
 Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
The first total laparoscopic pancreatoduodenectomy in Poland
 Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
Case report Videosurgery Andrzej Budzyński 1, Anna Zub-Pokrowiecka 1, Anna Zychowicz 1, Michał Pędziwiatr 1, Mateusz Wierdak 2, Maciej Matłok 1, Małgorzata Zając 1 12 nd Department of General Surgery,
Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer
 Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer
 Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS
 BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer
 Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
To describe the liver. To list main structures in porta hepatis.
 GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
Ruijin robotic thoracic surgery: S segmentectomy of the left upper lobe
 Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Case Report Page 1 of 5 Ruijin robotic thoracic surgery: S 1+2+3 segmentectomy of the left upper lobe Han Wu, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Hailei Du, Dingpei Han, Kai Chen,
Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer
 Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection
 Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Small Plicae Circularis. Short Closely packed together. Sparse, completely absent at distal part Lymphoid Nodule
 Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Intestines Differences Between Jejunum and Ileum Types Jejunum Ileum Color Deeper red Paler pink Calibre Bigger Smaller Thickness of wall Thick and Heavy Thin and Lighter Vascularity Highly vascularised
Nasogastric tube. Stomach. Pylorus. Duodenum 1. Duodenum 2. Duodenum 3. Duodenum 4
 Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Duodenum retroperitoneal
 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Surgical Management of Pancreatic Cancer
 I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
Surface Anatomy. Location Shape Weight Role of Five Surfaces Borders Fissures Lobes Peritoneal Lig
 The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
3/28/2012. Periampullary Tumors. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Eric K. Nakakura Ko Olina, HI
 Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass
 Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass 51(2023) Table 1 Laboratory data on admission Fig. 2 Percutaneous transhepatic cholangiogram shows tapering obstruction
Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass 51(2023) Table 1 Laboratory data on admission Fig. 2 Percutaneous transhepatic cholangiogram shows tapering obstruction
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Pancreas and Biliary System
 Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Lecture 02 Anatomy of the LIVER
 Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Uniportal video-assisted thoracic surgery for complicated pulmonary resections
 Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Review Article on Thoracic Surgery Uniportal video-assisted thoracic surgery for complicated pulmonary resections Ding-Pei Han, Jie Xiang, Run-Sen Jin, Yan-Xia Hu, He-Cheng Li Jiaotong University School
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
6 th August 2018 Day 1 - Gallbladder & Bile duct Topic
 Venue: Sterling Hospital Auditorium, Sterling Hospitals, Gurukul Road Ahmedabad, Gujarat 6 th August 2018 Day 1 - Gallbladder & Bile duct Registration(8:00am-8:15am) Inauguration(8:15am-8:30am) Welcome
Venue: Sterling Hospital Auditorium, Sterling Hospitals, Gurukul Road Ahmedabad, Gujarat 6 th August 2018 Day 1 - Gallbladder & Bile duct Registration(8:00am-8:15am) Inauguration(8:15am-8:30am) Welcome
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Cholecystectomy. Sarah Forsyth
 Cholecystectomy Sarah Forsyth History of Cholecystectomy First open cholecystectomy 1882 by Carl Langenbuch in Germany First lap cholecystectomy 1987, Philip Mouret (Gynaecologist) in Lyon, France 1990,
Cholecystectomy Sarah Forsyth History of Cholecystectomy First open cholecystectomy 1882 by Carl Langenbuch in Germany First lap cholecystectomy 1987, Philip Mouret (Gynaecologist) in Lyon, France 1990,
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Li Yang, Diancai Zhang, Fengyuan Li, Xiang Ma. Introduction
 Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Original Article on Gastrointestinal Surgery Simultaneous laparoscopic distal gastrectomy (uncut Roux-en-Y anastomosis), right hemi-colectomy and radical rectectomy (Dixon) in a synchronous triple primary
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Laparoscopic extended right hemicolectomy with D3
 Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Surgical Technique Page 1 of 11 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Weixian Hu, Jiabin Zheng, Yong Li Department of General Surgery, Guangdong General Hospital, Guangdong
Mauro Podda 1, Salomone Di Saverio 2, Adolfo Pisanu 1
 Editorial Page 1 of 5 Exploring the feasibility and effectiveness of robotic-assisted pancreaticoduodenectomy with modified Blumgart pancreaticojejunostomy: a look beyond the technology Mauro Podda 1,
Editorial Page 1 of 5 Exploring the feasibility and effectiveness of robotic-assisted pancreaticoduodenectomy with modified Blumgart pancreaticojejunostomy: a look beyond the technology Mauro Podda 1,
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Chapter 2. Simple Nephrectomy. Please Give Three Tips for Laparoscopic Simple Nephrectomy. Dr. de la Rosette
 Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe
 Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Laparoscopic Whipple procedure: review of the literature
 J Hepatobiliary Pancreat Surg (2009) 16:726 730 DOI 10.1007/s00534-009-0142-2 TOPICS Evolution and challenge in endoscopic HBP surgery Laparoscopic Whipple procedure: review of the literature Michel Gagner
J Hepatobiliary Pancreat Surg (2009) 16:726 730 DOI 10.1007/s00534-009-0142-2 TOPICS Evolution and challenge in endoscopic HBP surgery Laparoscopic Whipple procedure: review of the literature Michel Gagner
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Prevalence of anatomical variations of cystic artery in South Indian cadavers
 International Journal of Research in Medical Sciences Tejaswi HL et al. Int J Res Med Sci. 2013 Nov;1(4):424-428 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20131122
International Journal of Research in Medical Sciences Tejaswi HL et al. Int J Res Med Sci. 2013 Nov;1(4):424-428 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20131122
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 )
 Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
Robotic Surgery for Upper Tract Urothelial Carcinoma. Li-Ming Su, MD
 Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
Robotic Surgery for Upper Tract Urothelial Carcinoma Li-Ming Su, MD David A. Cofrin Professor of Urology, Associate Chairman of Clinical Affairs, Chief, Division of Robotic and Minimally Invasive Urologic
-12. -Renad Habahbeh. -Dr Mohammad mohtasib
 -12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
-12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
1. Epidemiology of Esophageal Cancer 2. Operative Strategies 3. Minimally Invasive Esophagectomy 4. Video
 Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Dr. Zahiri. In the name of God
 Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
Clinical Anatomy of the Biliary Apparatus: Relations & Variations
 Clinical Anatomy of the Biliary Apparatus: Relations & Variations Handout download: http://www.oucom.ohiou.edu/dbms-witmer/gs-rpac.htm 27 March 2007 Lawrence M. Witmer, PhD Professor of Anatomy Department
Clinical Anatomy of the Biliary Apparatus: Relations & Variations Handout download: http://www.oucom.ohiou.edu/dbms-witmer/gs-rpac.htm 27 March 2007 Lawrence M. Witmer, PhD Professor of Anatomy Department
Robotic-Assisted Pancreatoduodenectomy
 Curr Surg Rep (2013) 1:98 105 DOI 10.1007/s40137-013-0017-y MINIMALLY INVASIVE PANCREATIC SURGERY (MG HOUSE, SECTION EDITOR) Robotic-Assisted Pancreatoduodenectomy Mohammad Khreiss Herbert J. Zeh Brian
Curr Surg Rep (2013) 1:98 105 DOI 10.1007/s40137-013-0017-y MINIMALLY INVASIVE PANCREATIC SURGERY (MG HOUSE, SECTION EDITOR) Robotic-Assisted Pancreatoduodenectomy Mohammad Khreiss Herbert J. Zeh Brian
7/11/17. The Surgeon s Operative Report: Tools and Tips to Enhance Abstraction. Stopwoundinfection.com. Impact to Healthcare
 1. Scott, R. Douglas. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. March 2009. http://www.cdc.gov/hai/pdfs/hai/scott_costpaper.pdf. 2.
1. Scott, R. Douglas. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. March 2009. http://www.cdc.gov/hai/pdfs/hai/scott_costpaper.pdf. 2.
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Anatomy: Know Your Abdomen
 Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Pathways of Regional Spread in Pancreatic Cancer
 Pathways of Regional Spread in Pancreatic Cancer 12 Chusilp Charnsangavej, M.D. Regional spread of pancreatic ductal adenocarcinoma is common at the time of diagnosis, and it is often associated with poor
Pathways of Regional Spread in Pancreatic Cancer 12 Chusilp Charnsangavej, M.D. Regional spread of pancreatic ductal adenocarcinoma is common at the time of diagnosis, and it is often associated with poor
Left-sided approach for suprapancreatic lymph node dissection in laparoscopy-assisted distal gastrectomy without duodenal transection
 Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Robotic-assisted McKeown esophagectomy
 Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
I patients with nonendocrine pancreas carcinoma
 LYMPH NODE INVOLVEMENT IN CARCINOMA OF THE HEAD OF THE PANCREAS AREA ANTONIO L. CUBILLA, MD,* JOSEPH FORTNER, MD,+~ AND PATRICK J. FITZGERALD, MD*~ A prospective study to determine the lymph node involvement
LYMPH NODE INVOLVEMENT IN CARCINOMA OF THE HEAD OF THE PANCREAS AREA ANTONIO L. CUBILLA, MD,* JOSEPH FORTNER, MD,+~ AND PATRICK J. FITZGERALD, MD*~ A prospective study to determine the lymph node involvement
Abdomen and Retroperitoneum Ultrasound Protocols
 Abdomen and Retroperitoneum Ultrasound Protocols Reviewed By: Anna Ellermeier, MD Last Reviewed: March 2018 Contact: (866) 761-4200, Option 1 **NOTE for all examinations: 1. If documenting possible flow
Abdomen and Retroperitoneum Ultrasound Protocols Reviewed By: Anna Ellermeier, MD Last Reviewed: March 2018 Contact: (866) 761-4200, Option 1 **NOTE for all examinations: 1. If documenting possible flow
Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer
 Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
WHICH LYMPH NODES SHOULD BE
 Y.K.: 82 Y.O. WOMAN WITH ANEMIA No GI symptoms. Chronic AF taking coumadin: INR=2.1. HCT=24. Anemia persists despite Rx. Colonoscopy: tumor in ascending colon. Bx: adenocarcinoma. Rx: Laparoscopic right
Y.K.: 82 Y.O. WOMAN WITH ANEMIA No GI symptoms. Chronic AF taking coumadin: INR=2.1. HCT=24. Anemia persists despite Rx. Colonoscopy: tumor in ascending colon. Bx: adenocarcinoma. Rx: Laparoscopic right
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Thoracoscopic S 6 segmentectomy: tricks to know
 Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Laparoscopic extended right hemicolectomy with D3 lymphadenectomy
 Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
Surgical Technique Page 1 of 10 Laparoscopic extended right hemicolectomy with D3 lymphadenectomy Yong Li General Surgery, Guangdong General Hospital and Guangdong Academy of Medical Sciences, Guangzhou
1 Right & left Hepatic ducts Gastric Impression of spleen
 Pancreatic Model 1 Right & left Hepatic ducts 14 Gastric Impression of spleen 2 Common hepatic duct 15 Renal Impression of spleen 3 Cystic Duct 16 Colic Impression of spleen 4 Common Bile Duct 17 Splenic
Pancreatic Model 1 Right & left Hepatic ducts 14 Gastric Impression of spleen 2 Common hepatic duct 15 Renal Impression of spleen 3 Cystic Duct 16 Colic Impression of spleen 4 Common Bile Duct 17 Splenic
Classification of nodal stations in gastric cancer
 Review Article Classification of nodal stations in gastric cancer Fausto Rosa 1, Guido Costamagna 2, Giovanni Battista Doglietto 1, Sergio Alfieri 1 1 Department of Digestive Surgery, 2 Department of Digestive
Review Article Classification of nodal stations in gastric cancer Fausto Rosa 1, Guido Costamagna 2, Giovanni Battista Doglietto 1, Sergio Alfieri 1 1 Department of Digestive Surgery, 2 Department of Digestive
Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus. Anji Wall, Zuliang Feng & Willie Melvin. Journal of Robotic Surgery
 Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus Anji Wall, Zuliang Feng & Willie Melvin Journal of Robotic Surgery ISSN 1863-2483 Volume 8 Number 2 J Robotic Surg (2014) 8:169-171
Robotic-assisted Roux-en-Y gastric bypass in a patient with situs inversus Anji Wall, Zuliang Feng & Willie Melvin Journal of Robotic Surgery ISSN 1863-2483 Volume 8 Number 2 J Robotic Surg (2014) 8:169-171
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
The jejunum and the Ileum. Prof. Oluwadiya KS
 The jejunum and the Ileum Prof. Oluwadiya KS www.oluwadiya.siteled.com Introduction Introduction The small intestine (SI) comprises of the duodenum, jejunum and the ileum The jejunum is the second part
The jejunum and the Ileum Prof. Oluwadiya KS www.oluwadiya.siteled.com Introduction Introduction The small intestine (SI) comprises of the duodenum, jejunum and the ileum The jejunum is the second part
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
SAGES Society of American Gastrointestinal and Endoscopic Surgeons http://www.sages.org Guidelines for Laparoscopic Resection of Curable Colon and Rectal Cancer Author : SAGES Webmaster PREAMBLE The following
