and Transmural Drainage
|
|
|
- Kerry Watts
- 5 years ago
- Views:
Transcription
1 HPB Surgery, 2000, Vol. 11, pp Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under the Harwood Academic Publishers imprint, part of The Gordon and Breach Publishing Group. Printed in Malaysia. Clinical Series Pancreatic Pseudocysts Transpapillary and Transmural Drainage E. DELLA LIBERA a, El S. SIQUEIRA a, M. MORAIS a, M. R. S. ROHR a, Co Q. BRANT J. C. ARDENGH and A. P. FERRARI b,, Fellows of Gastroenterology, Endoscopy Unit; b Director of Endoscopy Unit, Study performed at the Endoscopy Unit of the Division of Gastroenterology of Universidade Federal de So Paulo, So Paulo, Brazil (Received September 1998) Background: Pancreatic pseudocyst endoscopic drainage has been described as a good treatment option, with morbidity and mortality rates that are lower than surgery. The aim of our study is to describe the efficacy of different forms of endoscopic drainage and estimate pseudocyst recurrence rate after short follow up period. Patients and Methods: We studied 30 patients with pancreatic pseudocyst that presented some indication for treatment: persistent abdominal pain, infection or cholestasis. Clinical evaluation was performed with a pain scale, 0 meaning absence of pain and 4 meaning continuous pain. Pseudocysts were first evaluated by abdominal CT scan, and after endoscopic retrograde pancreatography the patients were treated by transpapillary or transmural (cystduodenostomy or cystgastrostomy) drainage. Pseudocyst resolution was documented by serial CT scans. Results: 25/30 patients could be treated. Drainage was successful in 21 (70% in an intention to treat basis). After a mean follow-up of weeks, there was only I (4.2%) recurrence. A total of 6 complications occurred in 37 procedures (16.2%), and all but 2 were managed clinically and/or endoscopically: there was no mortality related to the procedure. Patients submitted to combined drainage needed more procedures than the other groups. There was no difference in the efficacy when we compared the three different drainage methods. Conclusions: We concluded that pancreatic pseudocyst endoscopic drainage is possible in most patients, with high success rate and low morbidity. Keywords: Pancreatic pseudocyst, cystenterostomy, endoscopic drainage, plastic stents INTRODUCTION Pancreatic pseudocysts are collections of pancreatic juice, with high enzymatic concentration, located inside or around the gland, formed as a result of pancreatic inflammation and/or ductal injury [1-3]. They are observed as a complication of acute pancreatitis (16% to 50%), or during the course of chronic pancreatitis, in 20% to 40% of the cases [4, 5]. Most of the pseudocysts secondary to acute pancreatitis resolve spontaneously [6,7] while *Address for correspondence: Rua Pedro de Toledo, 980, cj 66, CEP , So Paulo-SP, Brazil, Tel.: (+5511) , Fax: (+5511) , e-maih Angelo@gastro.epm.br 333
2 334 E.D. LIBERA et al. those associated with chronic, disease are associated with a lower spontaneous resolution rate and more complications [2,8]. Complications include infection, rupture, haemorrhage, biliary compression with or without jaundice, gastrointestinal obstruction, chronic pain, oesophageal varices, leakage with ascites or pleural fluid and pseudoaneurism [8-10]. Indications for drainage include: lesions larger than 4 cm or present longer than six weeks, persistent pain, complications and increased volume documented by imaging test [6, 7, 11]. Complications of surgical treatment occur in 10% to 30%, mortality in 1% to 5% and recurrence in 10% to 20% of the cases [9,12,13]. Percutaneous aspiration is a simple method but associated with frequent recurrence [6, 14]. Percutaneous drainage guided by US or CT is reserved for critically ill patients or for those with infected pseudocyst [15]. Endoscopic drainage has been reported during the last decade with success rates higher than 80% and can be transmural (cystgastrostomy or cystduodenostomy) or transpapillary [11, 12, 16, 17]. Both can be combined although transpallary drainage should be the first option because it s probably associated with a lower complication rate [18]. Endoscopic treatment is reported to have lower morbidity than surgery [5]. This study aimed to evaluate effectiveness and complications of pancreatic pseudocysts endoscopic drainage. MATERIALS AND METHODS Between June 1994 and May 1997, 30 patients referred to our Unit for pancreatic pseudocyst drainage were included in a prospective study. Inclusion criteria were: pancreatic pseudocyst confirmed by abdominal CT, more than 18 years of age, presence of at least one indication for drainage: pseudocyst larger than 4cm present for at least 6 weeks with persistent abdominal pain, progressive increase in size or complication (gastrointestinal or biliary obstruction, infection). Severity of abdominal pain was recorded before the drainage and at the end of the study according to the following score: zero (no pain), 1(sporadic episodes of pain), 2 (weekly episodes), 3 (daily attacks of pain). Size, number, location and relationship of the pseudocyst with the stomach or duodenum were evaluated with CT scan. During endoscopy we always attempted to identify any indentation on gastric or duodenal wall possibly caused by the pseudocyst. Retrograde endoscopic cholangiography was obtained whenever cholestasis was present. According to the findings during ERCP, whenever possible, patients were submitted to endoscopic treatment or referred to surgery. Endoscopic drainage was performed in 4 different ways, as follows: Group I-transpapillary drainage (TP)- presence of communication between the main pancreatic duct (MPD) and the pseudocyst, and we were able to cross any stricture and place a pancreatic plastic stent. Group II-cystgastrostomy (CG)-when transpapillary drainage was not possible (absence of communication between the pseudocyst and MPD, or unable to access the MPD) and there was a clear compression on the gastric wall, and the distance between the pseudocyst and the gastric wall was less than I cm measured by CT scan. Group III-cystduodenostomy (CD)- same as described for cystgastrostomy but compression was present on the duodenum. Group IV-combined drainage (CB)-performed whenever the pseudocyst did not heal after a single drainage procedure. Any treatment was repeated whenever necessary. Transpapillary drainage was the first treatment option. The distal end of the stent was located in the MPD, not necessarily inside the pseudocyst. In the presence of a MPD stricture dilation was performed with a passage dilator and the distal end of the stent was position-
3 DRAINAGE OF PSEUDOCYSTS 335 ed proximally to the stricture. Transmural drainage started with pseudocyst puncture trough the gastric or duodenal wall with the tip of a polipectomy snare. After spontaneous-drainage of characteristic fluid, the snare was removed and a guide wire was passed into the snare sheath; then a plastic stent was placed over the wire. Straight or pigtail plastic stents (9 or 10 Fr) were used for transmural drainage, and 5 or 7 Fr plastic pancreatic stents were inserted in transpapillary drainage. Abdominal pain and obstructive symptoms were evaluated clinically and regression of the pseudocyst was confirmed by CT. Once pseudocyst resolution was confirmed the stents were removed and pancreatogram was done to look for possible ductal lesions. An intention to treat analysis was done to evaluate our results. Statistical analysis were done with Fisher test, Student "t" test, X2 and Kruskal-Wallis, whenever appropriate. RESULTS Most of the patients (90%) were male and age ranged from 24 to 64 years (x 38,46 + 9,87 years). Pseudocyst aetiology was alcoholic chronic pancreatitis (ACP) in 26/30 patients (86,7%), abdominal trauma in 2/30 (6,7%) and 2/30 after surgery (6,6%). Three patients with ACP had a history of pseudocyst surgical treatment. Persistent abdominal pain was the most frequent drainage indication (93,4%). Overall 38 pseudocysts was diagnosed: 24 patients with one lesion, 4 patients with 2 and 2 patient with 3. Pseudocyst size ranged from 2 to 20 cm (x 9,14 + 4,93 cm), located in the body (52,6%), head (31,6%) or tail (15,8%). Indentation of the gastric or duodenal wall was identified in 20/30 patients (66,7%), MPD stricture and communication with the pseudocyst in 57,7% and 60% respectively. Fluid was studied in 17 patients and culture was positive in 6 (35%). After ERCP, in 5/30 patients (16,7%) there were no favourable conditions for endoscopic drainage because there was no access to the lesion (transpapillary or transmural). In the 25 remaining patients (83,3%) endoscopic drainage was performed: 8 cases in Group I (ranspapillary), 5 in Group II (cystgastrostomy), 7 in Group III (cystduodenostomy) and 5 in Group IV (combined drainage), total of 37 procedures (14 CG, 7 CD and 16 TP). The average number was of 1.48 procedures per patient and Group IV had more procedures compared with the other groups (p 0,002). Non-obstructed stents were removed after an average of 59,10+28,41 days (range 27 to 120 days). Main pancreatic duct changes (irregularities and strictures) were noted in 2 patients after transpapillary drainage, both had resolution of the pseudocyst without recurrence. Success (regression of the pseudocyst) was obtained in 21/25 (84%) in a per protocol analysis, but a more realistic intention to treat analysis showed that rate to be of 21/30 patients (70%). Pseudocyst regression was different according to drainage group. Better results occurred in Group IV, although such difference was not statistically significant (Tab. I). Twenty one 21 patients were followed from 2 to 124 weeks (x ,82 weeks) and recurrence was diagnosed in only one patient (4,8%), 12 months after CG. He was then submitted to another CG guided by endoscopic ultrasound and he is now asymptomatic. Only 4 patients are taking non-opioid analgesic medication because of abdominal pain, but with clinical score improvement, and CT didn t show pseudocyst recurrence. TABLE Success rate in the different drainage groups Patient N Success rate (%) Transpapillary 8 75 Cystgastrostomy 5 80 Cystduodenostomy 7 85 Combined Analysis for protocol treat intention to 30 70
4 336 E.D. LIBERA et al. TABLE II groups Frequency of complications (%) in the different Drainage Complications % Transpapillary pancreatitis 2.7 Cystgastrostomy stent proximal migration bleeding* 5.4 Cystduodenostomy perforation duodenal* 2.7 Combined stent proximal migration pneumoperitoneum 5.4 Total 16.2 referred to surgery. Evaluation of abdominal pain in the end of the follow up period identified 17 patients without pain (score zero) and four patients with ACP still complain of some pain. The average abdominal pain score was before and ,64 after treatment (p < 0,001, 95% CI: ). We analysed in an univariate way some factors that could be predictive of a good endoscopic drainage result: gastroduodenal indentation, MPD stricture, communication between the pseudocyst and MPD, age, size of the pseudocyst, cholestasis, presence of multiple lesions, pseudocyst larger than 6cm, serum albumin <3,5 g/dl. Only the presence of gastroduodenal wall indentation seen at endoscopic reached statistical significance (p 0,03). The complications of the 37 procedures occurred after CG (one case of each: bleeding, asymptomatic pneumoperitoneum and proximal stent migration), TP (one case of each: mild pancreatitis and proximal stent migration) and CD (duodenal perforation in one case), total of 6/37 (16.2%) complications (Tab. II). Most complications were benign and managed clinically and/or endoscopically. Two patients (bleeding and perforation) needed surgery (5,4%). There was no mortality related to the procedure. There was no difference between treatment Groups. DISCUSSION There is still a lot of controversy regarding pancreatic pseudocysts treatment, and up to now there is not an ideal way to treat them. There is no consensus in the literature regarding antibiotic use before pseudocyst endoscopic drainage. Some authors [11,13] recommended its use while others [17,18] just indicated it when there are evidences of pseudocyst infection. In this study we only prescribed parenteral antibiotics when there were clinical signs of infection and/or positive cultures, or when we were not able to drain the lesion or the bile duct (when biliary stricture was present). Pseudocyst infection was not among our complications. All 6 patients with a positive pseudocyst fluid culture had resolution without recurrence, and if drainage through the stent is effective, pseudocyst infection doesn t seem to interfere with the result of endoscopic treatment, as observed in this study. Our findings during pancreatograms were similar with those described earlier authors [4, 17,18]. Several complications of transpapillary drainage have been described and they include: stent occlusion (symptomatic or not), stent proximal or distal migration, pseudocyst infection, pseudocyst recurrence or worsening, pancreatitis, pancreatic ducts inflammatory changes and duodenal erosions [12,19-21]. Stent removal or exchange should be done within 4 to 6 weeks due to high occlusion rate after this period [22], up to 100% after 9 weeks [23]. In our study 3 patients needed stent exchange because of occlusion, but none of them presented any symptoms and those were not considered complications. One patient had a transpapillary stent proximal migration and it was not possible to remove it despite pancreatic sphincterotomy and multiple attempts. He is asymptomatic and without pseudocyst recurrence after a 29 month follow up. Some authors had suggested that such complication doesn t have any clinical consequence [12,22]. Distal migration is more common, doesn t cause adverse effects and should not be considered as a complication [22]. There was one case of mild pancreatitis that responded to clinical measures as reported earlier [17, 22].
5 DRAINAGE OF PSEUDOCYSTS 337 Pancreatic stents can induce MPD changes like irregularities and strictures, and also changes in secondary branches, similar those changes found in chronic pancreatitis [19, 24]. They may be asymptomatic and reversible with stent removal or exchange. We noticed morphologic changes on pancreatic ducts after transpapillary drainage in 2 cases, and both were asymptomatic and had no recurrence. We should keep in mind remind that such changes can also be part of the natural history of chronic pancreatitis. Transmural drainage, mainly CG, presents higher risk of complications, specially bleeding [13,14,18]. We had 3 complications after CG (bleeding, pneumoperitoneum and stent migration into the pseudocyst) and one after CD (perforation). Asymptomatic pneumoperitoneum was diagnosed one week after the procedure during a routine CT. Possibly, it was due to a small fistula during CG, maybe secondary to the presence of ascites, even though previous CT scan showed that the distance between gastric wall and the pseudocyst was less than lcm [25]. There was no difference regarding the frequency of complications in the different Groups (Tab. II), although both complications that needed surgery (bleeding and duodenal perforation) occurred after transmural drainage. Endoscopic ultrasound (EUS) allows identification of the best puncture site, specially in cases without a clear gastroduodenal indentation, besides identifying vascular structures between gastric or duodenal wall and the pseudocyst increasing effectiveness and safety of endoscopic drainage [26, 27]. During the study EUS was not available at our institution, and maybe both complications that needed surgery (bleeding and perforation) could be avoided, besides allowing drainage in those cases in which we were unable to identify gastroduodenal compression. More recently we started to perform EUS guided transmural drainage whenever gastric or duodenal wall is not detected during endoscopy [28]. Our success (pseudocyst regression) rate was similar to other published series [12,14,17]. There was no difference among different Groups, suggesting that drainage route had no influence on the results. Our recurrence rate was also comparable to those reported by other authors [11,14]. The only patient that presented pseudocyst recurrence was treated with another endoscopic drainage, as already described [14, 18]. Comparative evaluation of abdominal pain score before and after drainage showed statistically significant improvement. Asymptomatic patients were mainly those in alcohol abstinence, and probably this an important factor for good clinical response during long follow up. In conclusion, we believe that pancreatic pseudocyst endoscopic drainage is possible in most patients, with high success rate and low morbidity. Most complications can be clinically and/or endoscopically managed. Transpapillary drainage should be tried before transmural drainage, because it is associated with low morbidity. Patients that are successfully drained have important clinical improvement and recurrence is uncommon, specially for those that stay in alcohol abstinence. Acknowledgments This study was financially supported by Fundao de Amparo h Pesquisa do Estado de Sao Paulo (FAPESP), process # 93/ References [1] Bourliere, M. and Sarles, H. (1989). Pancreatic cysts and pseudocysts associated with acute and chronic pancreatitis. Dig. Dis. Sci., 34, [2] Sahel, J. (1991). Endoscopic drainage of pancreatic cysts. Endoscopy, 23, [3] Banks, P. A. (1997). Practice guidelines in acute pancreatitis. Am. J. Gastroenterol, 92, [4] Barthet, M., Bugallo, M., Moreira, L. S., Bastid, C., Sastre, B. and Sahel, J. (1993). Management of cysts and pseudocysts complicating chronic pancreatitis. The retrospective study of 143 patients. Gastroenterol Clin. Biol., 17,
6 338 E.D. LIBERA et al. [5] Lawson, J. M. and Baillie, J. (1995). Endoscopic therapy goes pancreatic pseudocysts. Gastrointest Endosc Clin. N. Am., 5, [6] Grace, P. A. and Williamson, R. C. N. (1993). Modern management of pancreatic pseudocysts. Br. J. Surg., 80, [7] Huibregtse, K. and Smits, M. E. (1994). Endoscopic management of diseases of the pancreas. Am. J. Gastroenterol, 89, $66-$77. [8] Bradley III, E. L. (1989). Complications of chronic pancreatitis. Surg. Clin. N. Am., 69, [9] Adams, D. B. and Anderson, M. C. (1992). Changing concepts in the surgical management of pancreatic pseudocysts. Am. Surg., 58, [10] Yeo, C. J., Bastidas, J. A., Lynch-Nyhan, A., Fishman, E. K., Zinner, M. J. and Cameron, J. L. (1990). The natural history of pancreatic pseudocysts documented by computed tomography. Surg. Gynecol Obstet, 170, [11] Catalano, M. F., Geenen, J. E., Schmaiz, M. J., Johnson, G. K., Dean, R. S. and Hogan, W. J. (1995). Treatment of pancreatic pseudocysts with ductal communication by transpapillary pancreatic duct endoprosthesis. Gastrointest Endosc, 42, [12] Smits, M. E., Rauws, E. A. J., Tytgat, G. N. J. and Huibregtse, K. (1995). The efficacy of endoscopic treatment of pancreatic pseudocysts. Gastrointest Endosc, 42, [13] Kozarek, R. A. (1997). Endoscopic treatment of pancreatic pseudocysts. Gastrointest Endosc Clin. N. Am., 7, [14] Cremer, M., Deviere, J. and Engelholm, L. (1989). Endoscopic management of cysts and pseudocysts in chronic pancreatitis: long-term follow-up after 7 years of experience. Gastrointest Endosc, 35, 1-9. [15] Servant, E., DeStefano, A., Weiner, T. M. and Jaques, P. F. (1992). Long term results of percutaneous catheter drainage of pancreatic pseudocysts. Surg. Gynecol Obstet, 175, [16] Kozarek, R. A., Ball, T. J., Patterson, D. J., Freeny, P. C., Ryan, J. A. and Traverso, W. (1991). Endoscopic transpapillary therapy goes disrupted pancreatic duct and peripancreatic fluid collections. Gastroenterology, 100, [17] Barthet, M., Sahel, J., Bertei, C. B. and Bernard, J. P. (1995). Endoscopic transpapillary drainage of pancreatic pseudocysts. Gastrointest Endosc, 42, [18] Binmoeller, K. F., Seifert, H., Walter, A. and Soehendra, N. (1995). Transpapillary and transmural drainage of pancreatic pseudocytes. Gastrointest Endosc, 42, [19] Sherman, S., Alvarez, C., Robert, M., Ashley, S. W., Reber, H. A. and Lehman, G. A. (1993). Polyethylene pancreatic duct stent-induced changes in the normal dog pancreas. Gastrointest Endosc, 39, [20] Ponchon, T., Bory, R. M., Hedelius, F., Roubein, L. D., Paliard, P., Napoleon, B. and Chavaillon, A. (1995). Endoscopic stenting goes pain relief in chronic pancreatitis: results of the standardized protocol. Gastrointest Endosc, 42, [21] Smits, M. E., Badiga, S. M., Rauws, E. A. J., Tytgat, G. N. J. and Huibregtse, K. (1995). Long-term results of pancreatic stents in chronic pancreatitis. Gastrointest Endosc, 42, [22] Siegel, J. and Veerappan, A. (1991). Endoscopic management of pancreatic disorders: potential risks of pancreatic prostheses. Endoscopy, 23, [23] Ikenberry, S. O., Sherman, S. and Hawes, R. H. (1994). The occlusion rate of pancreatic stents. Gastrointest Endosc, 40, [24] Kozarek, R. A. (1990). Pancreatic stents can induce ductal changes consistent with chronic pancreatitis. Gastrointest Endosc, 36, [25] Della Libera, E. and Ferrari, A. P. (1997). Asymptomatic pneumoperitoneum after endoscopic treatment of pseudocysts. Endoscopy, 29, [26] Binmoeller, K. and Soehendra, N. (1995). Endoscopic ultrasonography in the diagnosis and treatment of pancreatic pseudocysts. Gastrointest Endosc Clin. N. Am., 5, [27] Chan, A. T., Heller, S. J., Vam Dam, J., Carr-Locke, D. L. and Banks, P. A. (1996). Endoscopic cystgastrostomy: roll of endoscopic ultrasonography. Am. J. Gastroenterol, 91, [28] Ardengh, J. C., Della Libera, E. and Ferrari, A. P. (1998). Endosonography-guided drainage of pancreatic pseudocyst without gastric or duodenal compression. Endoscopy, 30, $71-2.
7 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report
 CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) Endosonographic imaging of pancreatic pseudocysts before endoscopic transmural drainage Fockens, P.; Johnson, T.G.; van Dullemen, H.M.; Huibregtse, K.; Tytgat, G.N.J.
UvA-DARE (Digital Academic Repository) Endosonographic imaging of pancreatic pseudocysts before endoscopic transmural drainage Fockens, P.; Johnson, T.G.; van Dullemen, H.M.; Huibregtse, K.; Tytgat, G.N.J.
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic Stents
 Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
Gastroenterology Research and Practice Volume 2015, Article ID 365457, 6 pages http://dx.doi.org/10.1155/2015/365457 Research Article Risk Factors for Migration, Fracture, and Dislocation of Pancreatic
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Endoscopic Therapy of Chronic Pancreatitis
 AMERICAN SOCIETY FOR GASTROINTESTINAL ENDOSCOPY Endoscopic Therapy of Chronic Pancreatitis Chronic pancreatitis is an inflammatory process characterized by destruction of pancreatic parenchyma and ductal
AMERICAN SOCIETY FOR GASTROINTESTINAL ENDOSCOPY Endoscopic Therapy of Chronic Pancreatitis Chronic pancreatitis is an inflammatory process characterized by destruction of pancreatic parenchyma and ductal
Acute Pancreatitis: A Case Report
 Diagnostic and Therapeutic Endoscopy, Vol. 4, pp. 155-160 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) Amsterdam
Diagnostic and Therapeutic Endoscopy, Vol. 4, pp. 155-160 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) Amsterdam
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY?
 Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
Endoscopy 2006 Update and Live Demonstration Berlin, 04. 05. Mai 2006 CHRONIC PANCREATITIS CONSERVATIVE TREATMENT, ENDOSCOPY OR SURGERY? J. F. Riemann A. Rosenbaum Medizinische Klinik C, Klinikum Ludwigshafen
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Synchronous Hepatic Cryotherapy and Resection
 HPB Surgery, 2000, Vol. 11, pp. 379-382 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 2000, Vol. 11, pp. 379-382 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
Endoscopic treatment for chronic pancreatitis: indications, technique, results
 J Hepatobiliary Pancreat Sci (2010) 17:770 775 DOI 10.1007/s00534-009-0182-7 TOPICS Chronic pancreatitis: current treatment strategies Endoscopic treatment for chronic pancreatitis: indications, technique,
J Hepatobiliary Pancreat Sci (2010) 17:770 775 DOI 10.1007/s00534-009-0182-7 TOPICS Chronic pancreatitis: current treatment strategies Endoscopic treatment for chronic pancreatitis: indications, technique,
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
SURGERY? COMMON BILE DUCT STONES ERCP OR. Room 759. Maryland
 HPB INTERNATIONAL 277 alter the natural history of the disease, and delay or prevent the development or cirrhosis. Data from our unit as well as others suggests that to be the case. The current series,
HPB INTERNATIONAL 277 alter the natural history of the disease, and delay or prevent the development or cirrhosis. Data from our unit as well as others suggests that to be the case. The current series,
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis. William H. Nealon M.D.
 The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
Chronic pancreatitis is a fibroinflammatory disease of the
 Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
Session 2C: Pancreaticobiliary Disease CHRONIC PANCREATITIS: WHEN TO SCOPE? Gregory A. Coté, MD, MS Chronic pancreatitis is a fibroinflammatory disease of the pancreas that presents with several distinct
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
Morning Report. Allison Haden, MD October 1, 2002
 Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
Therapeutic EUS: today & tomorrow Pietro Fusaroli
 Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
An Intra-Hepatic Pancreatic Pseudocyst Successfully Treated by Endoscopic Transpapillary Drainage Alone
 CASE REPORT An Intra-Hepatic Pancreatic Pseudocyst Successfully Treated by Endoscopic Transpapillary Drainage Alone Deepak Kumar Bhasin, Surinder Singh Rana, Vijant Singh Chandail, Mohit Nanda, Nikhil
CASE REPORT An Intra-Hepatic Pancreatic Pseudocyst Successfully Treated by Endoscopic Transpapillary Drainage Alone Deepak Kumar Bhasin, Surinder Singh Rana, Vijant Singh Chandail, Mohit Nanda, Nikhil
Outcome of pancreatic ascites in patients with tropical calcific pancreatitis managed using a uniform treatment protocol
 Indian J Gastroenterol 2009(May June):28(3):102 106 CASE SERIES Outcome of pancreatic ascites in patients with tropical calcific pancreatitis managed using a uniform treatment protocol Prakash Kurumboor
Indian J Gastroenterol 2009(May June):28(3):102 106 CASE SERIES Outcome of pancreatic ascites in patients with tropical calcific pancreatitis managed using a uniform treatment protocol Prakash Kurumboor
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Case Report Spontaneous Intramural Duodenal Hematoma: Pancreatitis, Obstructive Jaundice, and Upper Intestinal Obstruction
 Case Reports in Surgery Volume 2016, Article ID 5321081, 4 pages http://dx.doi.org/10.1155/2016/5321081 Case Report Spontaneous Intramural Duodenal Hematoma: Pancreatitis, Obstructive Jaundice, and Upper
Case Reports in Surgery Volume 2016, Article ID 5321081, 4 pages http://dx.doi.org/10.1155/2016/5321081 Case Report Spontaneous Intramural Duodenal Hematoma: Pancreatitis, Obstructive Jaundice, and Upper
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas
 ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser
 16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013
 Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Title. region. Author(s) Citation Surgery, 145(3), pp ; Issue Date
 NAOSITE: Nagasaki University's Ac Title Author(s) Huge pancreatic pseudocyst migratin region. Tajima, Yoshitsugu; Mishima, Takehi Taiichiro; Adachi, Tomohiko; Tsuneo Citation Surgery, 145(3), pp.341-342;
NAOSITE: Nagasaki University's Ac Title Author(s) Huge pancreatic pseudocyst migratin region. Tajima, Yoshitsugu; Mishima, Takehi Taiichiro; Adachi, Tomohiko; Tsuneo Citation Surgery, 145(3), pp.341-342;
Case Report Acute Obstructive Suppurative Pancreatic Ductitis in an Asymptomatic Patient
 Case Reports in Medicine Volume 2015, Article ID 919452, 4 pages http://dx.doi.org/10.1155/2015/919452 Case Report Acute Obstructive Suppurative Pancreatic Ductitis in an Asymptomatic Patient Eisha Wali,
Case Reports in Medicine Volume 2015, Article ID 919452, 4 pages http://dx.doi.org/10.1155/2015/919452 Case Report Acute Obstructive Suppurative Pancreatic Ductitis in an Asymptomatic Patient Eisha Wali,
Complex pancreatico- duodenal injuries. Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University
 Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
M. Ellrichmann; C. Jürgensen; A. Arlt; A. Fritscher-Ravens
 Randomized multicenter study on pancreatic duct stenting in disrupted or obstructed ducts in context with endoscopic treatment of pancreatic pseudocysts. M. Ellrichmann; C. Jürgensen; A. Arlt; A. Fritscher-Ravens
Randomized multicenter study on pancreatic duct stenting in disrupted or obstructed ducts in context with endoscopic treatment of pancreatic pseudocysts. M. Ellrichmann; C. Jürgensen; A. Arlt; A. Fritscher-Ravens
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Does it matter what we drain?
 Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Clinical outcomes and nonendoscopic interventions after minor papilla endotherapy in patients with symptomatic pancreas divisum
 ORIGINAL ARTICLE: Clinical Endoscopy Clinical outcomes and nonendoscopic interventions after minor papilla endotherapy in patients with symptomatic pancreas divisum Lyssa N. Chacko, MD, Yang K. Chen, MD,
ORIGINAL ARTICLE: Clinical Endoscopy Clinical outcomes and nonendoscopic interventions after minor papilla endotherapy in patients with symptomatic pancreas divisum Lyssa N. Chacko, MD, Yang K. Chen, MD,
Magnetic resonance cholangiopancreatography (MRCP) is an imaging. technique that is able to non-invasively assess bile and pancreatic ducts,
 SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
SECRETIN AUGMENTED MRCP Riccardo MANFREDI, MD, MBA, FESGAR Magnetic resonance cholangiopancreatography (MRCP) is an imaging technique that is able to non-invasively assess bile and pancreatic ducts, in
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
7/11/2017. We re gonna help a lot of people today. Biliary/Pancreatic Endoscopy. AGS July 1-2, Kenneth M. Sigman, MD
 Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience
 Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Case Reports in Surgery Volume 2013, Article ID 821032, 4 pages http://dx.doi.org/10.1155/2013/821032 Case Report Uncommon Mixed Type I and II Choledochal Cyst: An Indonesian Experience Fransisca J. Siahaya,
Spontaneous Regression of Pancreatic. Pseudocyst Mimicking a Submucosal. Tumor of the Stomach with Upper. Gastrointestinal Bleeding.
 2006 17 128-132 Spontaneous Regression of Pancreatic Pseudocyst Mimicking a Submucosal Tumor of the Stomach with Upper Gastrointestinal Bleeding Report of a Case Kuo-Chih Tseng, Yu-Hsi Hsieh, Chang-An
2006 17 128-132 Spontaneous Regression of Pancreatic Pseudocyst Mimicking a Submucosal Tumor of the Stomach with Upper Gastrointestinal Bleeding Report of a Case Kuo-Chih Tseng, Yu-Hsi Hsieh, Chang-An
SOD (Sphincter of Oddi Dysfunction)
 SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
Efficacy of Endotherapy in the Treatment of Pain Associated With Chronic Pancreatitis: A Systematic Review and Meta-Analysis
 ORIGINAL ARTICLE Efficacy of Endotherapy in the Treatment of Pain Associated With Chronic Pancreatitis: A Systematic Review and Meta-Analysis 1 Mikram Jafri, 2 Amit Sachdev, 3 Javed Sadiq, 2 David Lee,
ORIGINAL ARTICLE Efficacy of Endotherapy in the Treatment of Pain Associated With Chronic Pancreatitis: A Systematic Review and Meta-Analysis 1 Mikram Jafri, 2 Amit Sachdev, 3 Javed Sadiq, 2 David Lee,
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Treatment of chronic calcific pancreatitis endoscopy versus surgery
 Treatment of chronic calcific pancreatitis endoscopy versus surgery 35 - year old ladypresented to LPC Mumbai with intermittent abdominal pain. Pain was intermittent, colicky, more in epigastrium and periumbilical
Treatment of chronic calcific pancreatitis endoscopy versus surgery 35 - year old ladypresented to LPC Mumbai with intermittent abdominal pain. Pain was intermittent, colicky, more in epigastrium and periumbilical
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Research Article Endoscopic Closure for EUS and ERCP Related Duodenal Perforation by Endoclips
 Gastroenterology Research and Practice Volume 2016, Article ID 1051597, 5 pages http://dx.doi.org/10.1155/2016/1051597 Research Article Endoscopic Closure for EUS and ERCP Related Duodenal Perforation
Gastroenterology Research and Practice Volume 2016, Article ID 1051597, 5 pages http://dx.doi.org/10.1155/2016/1051597 Research Article Endoscopic Closure for EUS and ERCP Related Duodenal Perforation
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1157 1161 LIVER, PANCREAS, AND BILIARY TRACT Delayed and Unsuccessful Endoscopic Retrograde Cholangiopancreatography Are Associated With Worse Outcomes
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1157 1161 LIVER, PANCREAS, AND BILIARY TRACT Delayed and Unsuccessful Endoscopic Retrograde Cholangiopancreatography Are Associated With Worse Outcomes
CPT 2014 Overview of GI Changes
 CPT 2014 Overview of GI Changes The following table is a listing of the new,, and deleted codes in the Esophagus/Endoscopy section effective January 1, 2014. The table lists the CPT code, a brief description
CPT 2014 Overview of GI Changes The following table is a listing of the new,, and deleted codes in the Esophagus/Endoscopy section effective January 1, 2014. The table lists the CPT code, a brief description
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Endoscopic Ultrasound-Guided Pancreatic Duct Intervention
 FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
Evaluation and Management of Refractory Biliary Stricture. J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc.
 Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver Function Tests
 Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
Article Efficacy of Pancreatic Endotherapy in Pancreatic Ascites and Pleural Effusion
 Article Efficacy of Pancreatic Endotherapy in Pancreatic Ascites and Pleural Effusion Sudhir Gupta, Nitin Gaikwad *, Amol Samarth, Niraj Sawalakhe and Tushar Sankalecha Department of Gastroenterology,
Article Efficacy of Pancreatic Endotherapy in Pancreatic Ascites and Pleural Effusion Sudhir Gupta, Nitin Gaikwad *, Amol Samarth, Niraj Sawalakhe and Tushar Sankalecha Department of Gastroenterology,
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
cholangiopancreatography
 1250 Hepatopancreatic-Biliary Unit, Academic Medical Centre, University of Amsterdam, The Netherlands P H P Davids J Ringers E A J Rauws L Th de Wit K Huibregtse M N van der Heyde G N J Tytgat Correspondence
1250 Hepatopancreatic-Biliary Unit, Academic Medical Centre, University of Amsterdam, The Netherlands P H P Davids J Ringers E A J Rauws L Th de Wit K Huibregtse M N van der Heyde G N J Tytgat Correspondence
Pancreatitis is the most common and potentially serious ENDOSCOPY CORNER
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:834 839 ENDOSCOPY CORNER Short 5Fr vs Long 3Fr Pancreatic Stents in Patients at Risk for Post-Endoscopic Retrograde Cholangiopancreatography Pancreatitis
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:834 839 ENDOSCOPY CORNER Short 5Fr vs Long 3Fr Pancreatic Stents in Patients at Risk for Post-Endoscopic Retrograde Cholangiopancreatography Pancreatitis
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Endoscopic transluminal drainage of pancreatic pseudocyst and pancreatic necrosectomy Removing dead tissue from
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Endoscopic transluminal drainage of pancreatic pseudocyst and pancreatic necrosectomy Removing dead tissue from
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
ABDOMINAL WALL HAEMATOMA COMPLICATING LAPAROSCOPIC CHOLECYSTECTOMY
 HPB Surgery, 1994, Vol. 7, pp. 291-296 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
HPB Surgery, 1994, Vol. 7, pp. 291-296 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Title. CitationSurgical Endoscopy, 26(6): Issue Date Doc URL. Rights. Type. File Information. surgery
 Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Department of Internal Medicine, Saitama Citizens Medical Center, Saitama , Japan
 Case Reports in Cardiology Volume 2016, Article ID 8790347, 5 pages http://dx.doi.org/10.1155/2016/8790347 Case Report GuideLiner Catheter Use for Percutaneous Intervention Involving Anomalous Origin of
Case Reports in Cardiology Volume 2016, Article ID 8790347, 5 pages http://dx.doi.org/10.1155/2016/8790347 Case Report GuideLiner Catheter Use for Percutaneous Intervention Involving Anomalous Origin of
Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
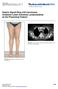 Clinical Image TheScientificWorldJOURNAL (2007) 7, 1189 1192 ISSN 1537-744X; DOI 10.1100/tsw.2007.199 Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
Clinical Image TheScientificWorldJOURNAL (2007) 7, 1189 1192 ISSN 1537-744X; DOI 10.1100/tsw.2007.199 Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
6/17/2016. ERCP in June 26, Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates
 ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
Overview. Doumit S. BouHaidar, MD ACG/VGS/ODSGNA Regional Postgraduate Course Copyright American College of Gastroenterology 1
 Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
Acute Pancreatitis. Falk Symposium 161 Dresden
 Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Title: Insertion of fully covered self-expanding. metal stents in benign biliary diseases. Rev
 Title: Insertion of fully covered self-expanding metal stents in benign biliary diseases Authors: Mariana Omodeo, Ignacio Malaga, Dante Manazzoni, Cecilia Curvale, Julio de Maria, Martín Alejandro Guidi,
Title: Insertion of fully covered self-expanding metal stents in benign biliary diseases Authors: Mariana Omodeo, Ignacio Malaga, Dante Manazzoni, Cecilia Curvale, Julio de Maria, Martín Alejandro Guidi,
Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage
 Shimane J. Med. Sci., Vol.34 pp.73-80, 2017 73 Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage Ahmed SELIM 1,2), Nobuhiko FUKUBA 1), Ichiro MORIYAMA 3), Hiroki
Shimane J. Med. Sci., Vol.34 pp.73-80, 2017 73 Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage Ahmed SELIM 1,2), Nobuhiko FUKUBA 1), Ichiro MORIYAMA 3), Hiroki
ORIGINAL PAPERS. R. Insertion of fully covered self-expanding metal stents in benign biliary diseases. ABSTRACT MATERIALS AND METHODS INTRODUCTION
 ORIGINAL PAPERS Insertion of fully covered self-expanding metal stents in benign biliary diseases Mariana Omodeo, Ignacio Málaga, Dante Manazzoni, Cecilia Curvale, Julio de María, Martín Guidi and Raúl
ORIGINAL PAPERS Insertion of fully covered self-expanding metal stents in benign biliary diseases Mariana Omodeo, Ignacio Málaga, Dante Manazzoni, Cecilia Curvale, Julio de María, Martín Guidi and Raúl
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Case Report Heterotopic Pancreas within the Proximal Hepatic Duct, Containing Intraductal Papillary Mucinous Neoplasm
 Case Reports in Surgery Volume 2015, Article ID 816960, 4 pages http://dx.doi.org/10.1155/2015/816960 Case Report Heterotopic Pancreas within the Proximal Hepatic Duct, Containing Intraductal Papillary
Case Reports in Surgery Volume 2015, Article ID 816960, 4 pages http://dx.doi.org/10.1155/2015/816960 Case Report Heterotopic Pancreas within the Proximal Hepatic Duct, Containing Intraductal Papillary
FAST TRACK MANAGEMENT OF PANCREATIC CANCER
 FAST TRACK MANAGEMENT OF PANCREATIC CANCER Jawad Ahmad Consultant Hepatobiliary Surgeon University Hospital Coventry and Warwickshire NHS Trust Part 1. Fast Track Surgery for Pancreatic Cancer Part 2.
FAST TRACK MANAGEMENT OF PANCREATIC CANCER Jawad Ahmad Consultant Hepatobiliary Surgeon University Hospital Coventry and Warwickshire NHS Trust Part 1. Fast Track Surgery for Pancreatic Cancer Part 2.
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
New developments in diagnosis and non-surgical treatment of chronic pancreatitis
 bs_bs_banner doi:10.1111/jgh.12250 NUTRITIONAL FACTORS IN PANCREATOBILIARY DISORDERS New developments in diagnosis and non-surgical treatment of chronic pancreatitis Kazuo Inui, Junji Yoshino, Hironao
bs_bs_banner doi:10.1111/jgh.12250 NUTRITIONAL FACTORS IN PANCREATOBILIARY DISORDERS New developments in diagnosis and non-surgical treatment of chronic pancreatitis Kazuo Inui, Junji Yoshino, Hironao
Y A L E S C H O O L O F M E D I C I N E. This is a CME accredited activity. The presenters and there are no conflicts of interest.
 This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Transluminal endoscopic necrosectomy after acute pancreatitis: a multicentre study with long-term follow-up (the GEPARD Study)
 See Commentary, p 1180 1 Department of Internal Medicine, Oldenburg Municipal Hospital, Oldenburg, Germany; 2 Central Interdisciplinary Endoscopy Unit, Department of Gastroenterology, Charité Medical University
See Commentary, p 1180 1 Department of Internal Medicine, Oldenburg Municipal Hospital, Oldenburg, Germany; 2 Central Interdisciplinary Endoscopy Unit, Department of Gastroenterology, Charité Medical University
