Type 1 diabetes patients with severe non-proliferative retinopathy may benefit from panretinal photocoagulation.
|
|
|
- Amberly Daniella Lynch
- 5 years ago
- Views:
Transcription
1 Type 1 diabetes patients with severe non-proliferative retinopathy may benefit from panretinal photocoagulation. Lövestam-Adrian, Monica; Agardh, Carl-David; Torffvit, Ole; Agardh, Elisabet Published in: Acta Ophthalmologica Scandinavica DOI: /j x Published: Link to publication Citation for published version (APA): Lövestam-Adrian, M., Agardh, C-D., Torffvit, O., & Agardh, E. (2003). Type 1 diabetes patients with severe nonproliferative retinopathy may benefit from panretinal photocoagulation. Acta Ophthalmologica Scandinavica, 81(3), DOI: /j x General rights Copyright and moral rights for the publications made accessible in the public portal are retained by the authors and/or other copyright owners and it is a condition of accessing publications that users recognise and abide by the legal requirements associated with these rights. Users may download and print one copy of any publication from the public portal for the purpose of private study or research. You may not further distribute the material or use it for any profit-making activity or commercial gain You may freely distribute the URL identifying the publication in the public portal Take down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. L UNDUNI VERS I TY PO Box L und
2 Type 1 diabetes patients with severe non-proliferative retinopathy may benefit from panretinal photocoagulation Monica Lo vestam-adrian, 1 Carl-David Agardh, 2 Ole Torffvit 3 and Elisabet Agardh 4 1 Department of Ophthalmology, University Hospital, Lund, Sweden 2 Department of Endocrinology, University Hospital, Malmo, Sweden 3 Department of Medicine, University Hospital, Lund, Sweden 4 Department of Ophthalmology, University Hospital, Malmo, Sweden ABSTRACT. Purpose: To examine whether panretinal photocoagulation for severe nonproliferative retinopathy in type 1 diabetes patients could halt the progression of retinopathy with subsequent vitreous haemorrhages and visual impairment. Methods: During a 10-year follow-up study period of 344 type 1 diabetes patients, 81 subjects went through panretinal photocoagulation. Forty patients were treated for severe non-proliferative retinopathy (age at onset of diabetes 14 8 years, diabetes duration 18 þ 10 years) and 41 for proliferative retinopathy (age at onset years, diabetes duration 22 þ 13 years). One randomly selected eye per patient forms the basis for the study. Metabolic control, systolic and diastolic blood pressure, serum creatinine and urinary albumin levels were measured and analysed yearly during the follow-up period. Results: A total of 35% (14/40) of eyes treated for severe non-proliferative retinopathy developed neovascularizations during a mean time of years. Vitreous haemorrhages were more frequent in eyes with proliferative retinopathy at treatment than in eyes with severe non-proliferative retinopathy (12/41 versus 2/40; p ¼ 0.007). The number of vitrectomies due to vitreous haemorrhages in eyes treated for severe non-proliferative retinopathy tended to be lower (1/40 versus 6/41; p ¼ 0.052). Before photocoagulation, visual acuity (VA) was similar in eyes with severe non-proliferative retinopathy and in those with proliferative retinopathy (1.0, versus 1.0, ; median and range). Visual impairment and blindness tended to develop more often in eyes treated for proliferative retinopathy compared to those treated for severe non-proliferative retinopathy (10/40 versus 4/40; p ¼ 0.056). Eyes with neovascularizations at follow-up were more often visually impaired (VA < 0.5) than eyes without neovascularizations (15/55 versus 1/26; p ¼ 0.016). Conclusion: In type 1 diabetes, panretinal photocoagulation may be beneficial even at the severe non-proliferative retinopathy stage in terms of preventing vitreous haemorrhage, subsequent vitrectomy and visual impairment. Key words: type 1 diabetes severe non-proliferative/ proliferative retinopathy panretinal photocoagulation vitreous haemorrhage vitrectomy Acta Ophthalmol. Scand. 2003: 81: Copyright # Acta Ophthalmol Scand ISSN Introduction Diabetic retinopathy is still a major cause of visual impairment in middleaged people in the Western world (Trautner et al. 1997), despite screening (Porta et al. 1995) and widely accepted guidelines for laser treatment (Diabetic Retinopathy Study Research Group 1981; Early Treatment Diabetic Retinopathy Study Research Group 1985). An analysis of the results from the Early Treatment Diabetic Retinopathy Study (ETDRS) group revealed that panretinal photocoagulation for severe non-proliferative or early proliferative retinopathy reduced the rate of visual impairment in patients with type 2 diabetes, whereas this could not be demonstrated in patients with type 1 diabetes (Ferris 1996). In recent years, a Scandinavian study by Rossing et al. (1998) reported improved visual outcome in type 1 diabetes patients, despite an unchanged incidence of proliferative retinopathy, a finding which could be attributed to more frequent laser treatment. In a previous study of type 1 diabetes patients, we demonstrated that the 10-year incidence of moderate visual impairment was low (8%) and that only two eyes became legally blind (Lo vestam-adrian et al. 2001). The present study of laser treatment approaches aimed to establish whether panretinal photocoagulation in type 1 diabetes patients instituted at 221
3 the severe non-proliferative stage might have a more favourable outcome on vitreous haemorrhages, vitrectomies and visual acuity (VA) in comparison with corresponding laser treatment instituted at the proliferative retinopathy stage. Patients and Methods Patients A total of 81 consecutive type 1 diabetes patients treated with panretinal photocoagulation for severe non-proliferative (n ¼ 40) or proliferative (n ¼ 41) retinopathy, formed the basis for the present study. They represented a subgroup of 452 type 1 diabetes patients examined at the Department of Ophthalmology (Lund) in 1986, out of whom 388 continued to participate in regular eye examinations during the entire 10-year follow-up period (n ¼ 344) or until death (n ¼ 44) (Lo vestam-adrian et al. 2001). Although the time-point for panretinal photocoagulation was not randomly assigned, the numbers of patients in the severe nonproliferative and proliferative groups ended up almost equal. One eye per patient was randomly assigned for this study using a computerbased statistical program (SPSS). Classification of retinopathy Before laser treatment, the classification of retinopathy was based on findings from fundus photographs using a 45 Topcon camera. Three fields per eye were obtained through dilated pupils, nasal, central with stereo pairs, and temporal fields. The retinopathy was characterized as: (1) severe non-proliferative retinopathy, with multiple haemorrhages in four quadrants, venous beading in two quadrants, or intraretinal microvascular abnormalities (IRMA) in one or more quadrants, or (2) proliferative retinopathy, with formation of new vessels and/or vitreous haemorrhages. In addition, the presence or absence of clinically significant macular oedema according to the definition by ETDRS Research Group (1985) was diagnosed according to stereo photographs of the macula. During follow-up, new vessels as well as the number of vitreous haemorrhages were registered. Photocoagulation All eyes were treated with panretinal photocoagulation, m, seconds, at least 1500 burns/eye, in two to four sessions. The number of laser burns given per eye did not differ between those with severe nonproliferative retinopathy and those with proliferative retinopathy. Eyes with diffuse macular oedema or leakage from central microaneurysms were treated with appropriate focal/grid macular photocoagulation prior to panretinal photocoagulation as described by ETDRS Research Group (1985). Vitrectomy was performed within 3 months in the presence of persistent severe vitreous haemorrhage that obscured visual function. Visual acuity Visual acuity (VA) was tested using Snellen Charts. Three levels of VA were defined: normal or moderately affected VA (VA 0.5), visual impairment (VA ¼ ), and legal blindness (VA 0.1). Medical risk indicators Age, age at onset of diabetes, diabetes duration, HbA 1c, systolic and diastolic blood pressure, serum-creatinine and urinary albumin were registered before photocoagulation and throughout the follow-up period. For each calendar year, a mean value was calculated and from these an overall mean value was obtained. Analytical techniques HbA 1c levels were analysed by ionexchange chromatography using commercially available microcolumns (Bio-Rad, Richmond, California, USA) or by fast liquid chromatography (Kontron Instruments, Milan, Italy). The normal value for both methods is <5.3%. Blood pressure was measured in the supine position using a mercury sphygmomanometer. Diastolic blood pressure was taken at Korotkoff phase V. Urine was collected in polystyrene tubes and stored at 4 for less than 4days before analysis. Urinary albumin concentration was measured with an electroimmunoassay using human albumin (Kabi Vitrum, Stockholm, Sweden) (detection limit 12.5 mg/l) or by turbidimetry with an automated analyser (Cobras Mira, Roche, UK), antibodies (rabbit antihuman albumin) and technique as described by Dakopatts, Copenhagen (detection limit 5 mg/l). Serum creatinine levels were analysed by a kinetic Jaffe reaction or by an enzymatic method (creatinine-hydrolase; EKTA Chem-analyser, Instrument Kodak, New York, NY, USA). The latter method was adjusted to give the same values as the first. Normal values were mmol/l for women and mmol/l for men. Statistics Values are given as mean SD or median and range. Student s two-tailed t-test was used for equal standard deviations and Welch s approximate t-test for unequal standard deviations. Mann Whitney U-test was used for distribution free data and chi-squared test was used for testing categorical variables. Logistic regression analysis with forward stepwise selection was used to establish the independent influence of various risk indicators. All tests were two-tailed and a p-value of 0.05 was considered significant. The statistical analyses were performed using SPSS FOR WINDOWS VERSION 10. Results Photocoagulation and progression of retinopathy The mean times between initiation of treatment and follow-up were similar for both treatment groups ( years for the severe non-proliferative group versus years for the proliferative retinopathy group). A total of 35% (14/40) of eyes treated for severe non-proliferative retinopathy developed neovascularizations during a mean period of years. The majority (8/14) of these included high risk characteristics as defined by the Diabetic Retinopathy Study (DRS) (Diabetic Retinopathy Study Research Group 1981). Vitreous haemorrhages occurred more frequently in eyes treated for proliferative retinopathy than in those treated for severe non-proliferative retinopathy (12/41 versus 2/40; p ¼ 0.007) (Fig. 1). The mean time from initiation of laser treatment to occurrence of vitreous haemorrhages was years. There was a trend towards a lower number of vitrectomies due to vitreous haemorrhage in eyes treated for severe non-proliferative retinopathy than in eyes with proliferative retinopathy at 222
4 Fig. 1. The 10-year cumulative frequency of patients without vitreous haemorrhage throughout the study. Full line: eyes treated for severe nonproliferative retinopathy. Dotted line: eyes treated for proliferative retinopathy. the time of photocoagulation (1/40 versus 6/41; p ¼ 0.052). In all, 80% (32/40) of eyes treated for severe non-proliferative and 68% (28/41) of eyes treated for proliferative retinopathy (NS) had diffuse oedemas or leaking microaneurysms in the centre of the macula and received focal/grid laser photocoagulation prior to panretinal treatment. No eye developed retinal detachment or neovascular glaucoma. Visual acuity Visual acuities prior to laser treatment and at follow-up are shown in Table 1. Before photocoagulation, VA was similar in eyes treated for severe nonproliferative retinopathy and for proliferative retinopathy (median 1.0, range versus median 1.0, range ). Visual impairment and blindness tended to develop more often in eyes treated for proliferative retinopathy compared to those treated for severe non-proliferative retinopathy but the difference was of borderline significance (10/38 versus 4/40; p ¼ 0.056). Visual impairment developed in 1/27 eyes treated for severe non-proliferative retinopathy without progression to proliferative retinopathy. The corresponding figure for those eyes which showed progression to proliferative retinopathy was 3/13. None became legally blind. Table 1. Visual acuity and degree of retinopathy prior to photocoagulation and at follow-up. Visual acuity and degree of retinopathy Visual acuity and degree of retinopathy at follow-up prior to photocoagulation Severe non-proliferative Severe non-proliferative Proliferative retinopathy retinopathy retinopathy retinopathy 0.5 (n ¼ 40) (n ¼ 0) 0.1 (n ¼ 0) Proliferative retinopathy 0.5 (n ¼ 36) (n ¼4 ) (n ¼ 1) 1 Eyes with neovascularizations at follow-up were more often visually impaired (VA < 0.5) than eyes without neovascularizations (15/55 versus 1/26; p ¼ 0.016). At follow-up, the numbers of visually impaired eyes were similar in those treated for diffuse macular oedema or leaking microaneurysms prior to panretinal photocoagulation to those which had not been so treated before panretinal coagulation (12/62 versus 3/19). None of the eyes developed fibrous tissue in the vitreous or neovascular glaucoma. Medical risk indicators The medical risk indicators for development of retinopathy are shown in Table 2. There were no differences in any of the parameters between patients treated for severe non-proliferative retinopathy and patients treated for proliferative retinopathy either before or throughout the observation period. Discussion The risk of development of high risk proliferative retinopathy in nonphotocoagulated eyes with severe nonproliferative retinopathy is high (DRS Research Group 1978; ETDRS Research Group 1991a, 1991b). The 223
5 Table 2. Comparison of patient characteristics between those with severe non-proliferative and those with proliferative retinopathy. Severe non-proliferative retinopathy (n ¼ 40) Proliferative retinopathy (n ¼ 41) Age at onset (years) Diabetes duration (years) HbA 1c (%) SBP (mmhg) DBP (mmhg) Urinary albumin (mgl 1 ) 72 (0 9350) 86 (0 5375) Serum creatinine (mmol 1 ) 69 (51 651) 74(51 748) Insulin dose (Ukg 1 ) Values are given as mean SD and as median and range. The values given are the mean values for all measurements during the observation period. SBP ¼ systolic blood pressure; DBP ¼ diastolic blood pressure. ETDRS reported a 44% risk within 3 years (ETDRS Research Group 1991a). In the present study, despite panretinal photocoagulation for severe non-proliferative retinopathy, 35% of eyes developed new vessels within 3 years and 57% of those showed signs of high risk proliferative retinopathy. This is comparable to the ETDRS study, in which 20% of treated eyes developed high risk proliferative retinopathy (ETDRS Research Group 1991a) and demonstrates the progressive nature of severe non-proliferative retinopathy and risk of visual impairment due to vitreous haemorrhage. The occurrence of vitreous haemorrhage (29%) in eyes with proliferative retinopathy at the time of treatment was similar to the frequency reported by Vander et al. (1991). Most of the vitreous haemorrhages occurred within the first 3 years after photocoagulation and thereafter the frequency declined. Vitreous haemorrhage is the most frequent cause of visual loss (ETDRS Research Group 1999) and as we were able to demonstrate that, despite the development of neovascularizations, vitreous haemorrhages could be avoided in most cases treated for severe nonproliferative retinopathy, our study indicates that early panretinal photocoagulation may be beneficial at this early stage. The frequency of visually impaired eyes was 14% (11/81), representing a range similar to that found by the (1991a) ETDRS No 9, where 12% of eyes were found to be visually impaired (< 20/40). We have not used the same criteria for more severely affected vision. It should be mentioned, however, that the ETDRS found that 5% of eyes had VA of <20/100 after 4years of follow-up (ETDRS Research Group 1991a), compared to the 2% (2/81) of eyes with VA 0.1 found in our study. Visual acuity outcome is dependent on macular function. In the present study, it was better among those in whom panretinal photocoagulation was instituted at the severe non-proliferative stage than among those in whom panretinal photocoagulation was instituted at the proliferative stage. The number of eyes that received focal and/or grid laser photocoagulation did not differ, indicating that exudative oedema occurred to similar extents in both groups. There were no other obvious reasons for visual loss, such as fibrous tissue in the vitreous or neovascular glaucoma in either of the groups. However, the possibility that ischaemic maculopathy had an influence on VA cannot be excluded and this could contribute to the slightly higher number of visually impaired eyes in the proliferative retinopathy group. A previous study has shown that when comparing treatment outcome between type 1 and type 2 diabetes patients, patients with type 2 diabetes seem to benefit most from early treatment (i.e. treatment at the severe nonproliferative retinopathy stage) (Ferris 1996). These patients showed a 50% reduction in the rate of visual loss after early photocoagulation, in contrast to patients with type 1 diabetes, in whom no improvement in the rate of visual loss was seen. In our study of type 1 diabetes patients, laser treatment for severe non-proliferative retinopathy seemed to be beneficial. The results may be partly explained by the fact that all our cases received treatment for exudative macular oedema prior to panretinal photocoagulation. In the ETDRS, eyes assigned to deferral of panretinal treatment did not receive any focal photocoagulation for macular oedema, until the positive results of macular treatment were released (ETDRS Research Group 1985). Furthermore, early treatment in our study referred only to eyes with severe non-proliferative retinopathy, whereas the early treatment group in the ETDRS also included eyes with early proliferative retinopathy. The ETDRS stated that early panretinal photocoagulation should be considered but not immediately recommended, given its side effects of decreased peripheral and night vision (Frank 1975; Buckley et al. 1992). In cases where no early treatment was given, a maximum follow-up period of 2 3 months in patients with severe nonproliferative retinopathy was recommended. In our study, we showed that early laser treatment resulted in fewer vitreous haemorrhages and, possibly, fewer visually impaired eyes but side effects such as visual field defects, impaired night vision and contrast sensitivity were not studied. However, the psychological implications of, for example, frequent examinations, should also be taken into account. In a study comparing psychiatric symptomatology in patients with and without proliferative diabetic retinopathy, a strong correlation was seen between negative life events and recently diagnosed proliferative retinopathy. No such correlation was seen in patients treated with panretinal photocoagulation once the outcome was stabilized (Jacobson et al. 1985). Stabilization of diabetic retinopathy is probably more rapidly achieved at the severe nonproliferative stage and as the recommended follow-up time can be extended in properly treated patients (ETDRS Research Group 1991a), early panretinal photocoagulation might be psychologically beneficial. Increased levels of baseline HbA 1c (Klein et al. 1994a; Davis et al. 1998) are associated with higher risks of developing more severe levels of retinopathy. In the present study, we found no differences in metabolic control between patients with severe 224
6 non-proliferative and proliferative retinopathy before photocoagulation or during the follow-up period. The present study used the mean of all HbA 1c values obtained during the observation period, thus reflecting the influence of longterm metabolic control, whereas only baseline values were used for analyses in the other studies (Klein et al. 1994a; Davis et al. 1998). In addition, neither blood pressure nor signs of nephropathy, both risk factors for retinopathy (Klein et al. 1989, 1993), differed between patients with severe non-proliferative or proliferative retinopathy. However, the lack of statistical significance in our study may well be due to the small numbers of patients. The logistic regression analysis revealed no independent risk indicators predicting the development of new vessels in patients treated for severe non-proliferative retinopathy. This is in disagreement with other studies, which found progression of retinopathy to be determined by medical risk indicators such as metabolic control and hypertension (Klein et al. 1988, 1994b; Lloyd et al. 1995). In summary, in this study of type 1 diabetes patients, treatment with panretinal photocoagulation for severe non-proliferative or proliferative retinopathy (in groups where age at onset and duration of diabetes, metabolic control and blood pressure levels were comparable) reduced the frequency of vitreous haemorrhages and vitrectomies in the severe non-proliferative group. The results indicate that panretinal photocoagulation might be beneficial as early as the severe non-proliferative retinopathy stage in type 1 diabetes patients. Acknowledgements This study was supported by grants from the Swedish Medical Research Council K98 19X A, the Medical Faculty of Lund University, Skane County Council Foundation for Research and Development and Crown Princess Margareta s Committee for the Blind. References Buckley S, Jenkins L & Benjamin L (1992): Field loss after panretinal photocoagulation with diode and argon lasers. Doc Ophthalmol 82: Davis MD, Fisher MR & Gangnon RE et al. (1998): Risk factors for high risk proliferative diabetic retinopathy and severe visual loss., Report No. 18. Invest Ophthalmol Vis Sci 39: Diabetic Retinopathy Study Research Group (1978): Photocoagulation treatment of proliferative diabetic retinopathy. DRS Report No. 2. Ophthalmology 85: Diabetic Retinopathy Study Research Group (1981): Photocoagulation treatment of proliferative diabetic retinopathy: clinical applications of Diabetic Retinopathy Study (DRS) findings. DRS Report No. 8. Ophthalmology 88: Research Group (1985): Photocoagulation for diabetic macular oedema. ETDRS Report No. 1. Arch Ophthalmol 103: Research Group (1991a): Early photocoagulation for diabetic retinopathy. ETDRS Report No. 9. Ophthalmology 98: Research Group (1991b): Fundus photographic risk factors for progression of diabetic retinopathy. ETDRS Report No. 12. Ophthalmology 98: Research Group (1999): Causes of severe visual loss in the Early Treatment Diabetic Retinopathy Study. ETDRS Report No. 24. Am J Ophthalmol 127: Ferris F (1996): Early photocoagulation in patients with either type 1 or type 2 diabetes. Trans Am Ophthalmol Soc 94: Frank RN (1975): Visual field and electroretinography following extensive photocoagulation. Arch Ophthalmol 93: Jacobson AM, Rand LI & Hauser ST (1985): Psychological stress and glycaemic control: a comparison of patients with and without proliferative diabetic retinopathy. Psychosom Med 47: Klein R, Klein BEK, Moss SE & Cruickshank KJ (1994a): Relationship of hyperglycaemia to the longterm incidence and progression of diabetic retinopathy. Arch Intern Med 154: Klein R, Klein BEK, Moss SE & Cruickshank KJ (1994b): The Wisconsin epidemiologic study of diabetic retinopathy. XIV. Ten-year incidence and progression of diabetic retinopathy. Arch Ophthalmol 112: Klein R, Klein BEK, Moss SE, Davis MD & DeMets DL (1988): Glycosylated haemoglobin predicts the incidence and progression of diabetic retinopathy. JAMA 260: Klein R, Klein BEK, Moss SE, Davis MD & DeMets DL (1989): Is blood pressure a predictor of the incidence or progression of diabetic retinopathy? Arch Intern Med 149: Klein R, Moss SE & Klein BEK (1993): Is gross proteinuria a risk factor for the incidence of proliferative diabetic retinopathy? Ophthalmology 100: Lloyd CE, Klein R, Maser RE, Kuller LH, Becker DJ & Orchard TJ (1995): The Pittsburgh Epidemiology of Diabetes Complications (EDC) Study. J Diabetes Complications 9: Lo vestam-adrian M, Agardh C-D, Torffvit O & Agardh E (2001): Diabetic retinopathy, visual acuity and medical risk indicators. A continuous 10-year follow-up study in type 1 diabetic patients under routine care. J Diabetes Complications 15: Porta M, Tomalino MG, Santoro F et al. (1995): Diabetic retinopathy as a cause of blindness in the province of Turin, Northwest Italy, in Diabetic Med 12: Rossing K, Jacobsen P, Rossing P, Lauritzen E, Lund-Andersen H & Parving HH (1998): Improved visual function in IDDM patients with unchanged cumulative incidence of sight-threatening diabetic retinopathy. Diabetes Care 21: Trautner C, Icks A, Haastert B, Plum B & Berger M (1997): Incidence of blindness in relation to diabetes. Diabetes Care 20: Vander JF, Duker JS, Benson WE, Brown GC, McNamara JA & Rosenstein RB (1991): Longterm stability and visual outcome after favourable initial response of proliferative diabetic retinopathy to panretinal photocoagulation. Ophthalmology 98 (10): Received on April 12th, Accepted on December 23rd, Correspondence: Dr Monica Lo vestam-adrian Department of Ophthalmology University Hospital Lund SE Lund Sweden Tel: þ Fax: þ monica.lovestam_adrian@oft.lu.se 225
Visual prognosis after panretinal photocoagulation for. Proliferative diabetic retinopathy (PDR)
 Visual prognosis after panretinal photocoagulation for proliferative diabetic retinopathy Toke Bek 1 and Mogens Erlandsen 2 1 Department of Ophthalmology, A rhus University Hospital, A rhus, Denmark 2
Visual prognosis after panretinal photocoagulation for proliferative diabetic retinopathy Toke Bek 1 and Mogens Erlandsen 2 1 Department of Ophthalmology, A rhus University Hospital, A rhus, Denmark 2
The retinal renin-angiotensin system: implications for therapy in diabetic retinopathy
 (2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
(2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diabetic Management beyond traditional risk factors and LDL-C control: Can we improve macro and microvascular risks?
 Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Diabetes Care 24: , 2001
 Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
Andrew J. Barkmeier, MD; Benjamin P. Nicholson, MA; Levent Akduman, MD
 c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
Diabetic and the Eye: An Introduction
 Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy
 European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
INTRODUCTION AND SYMPTOMS
 CHAPTER 1 INTRODUCTION AND SYMPTOMS Introduction of Diabetic Retinopathy Diabetic retinopathy (DR) is a potentially blinding complication of diabetes. It is defined as presence of one or more definite
CHAPTER 1 INTRODUCTION AND SYMPTOMS Introduction of Diabetic Retinopathy Diabetic retinopathy (DR) is a potentially blinding complication of diabetes. It is defined as presence of one or more definite
Factors Associated with Visual Outcome after Photocoagulation for Diabetic Retinopathy
 Investigative Ophthalmology & Visual Science, Vol. 30, No. 1, January 1989 Copyright Association for Research in Vision and Ophthalmology Factors Associated with Visual Outcome after Photocoagulation for
Investigative Ophthalmology & Visual Science, Vol. 30, No. 1, January 1989 Copyright Association for Research in Vision and Ophthalmology Factors Associated with Visual Outcome after Photocoagulation for
Abnormalities of the retinal veins are. loops and reduplications in diabetic retinopathy. Prevalence, distribution, and pattern of development
 Venous loops and reduplications in diabetic retinopathy Prevalence, distribution, and pattern of development Toke Bek Department of Ophthalmology, Århus University Hospital, DK-8000 Århus C, Denmark ABSTRACT.
Venous loops and reduplications in diabetic retinopathy Prevalence, distribution, and pattern of development Toke Bek Department of Ophthalmology, Århus University Hospital, DK-8000 Århus C, Denmark ABSTRACT.
Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
Impact of changes in metabolic control on progression to photocoagulation for clinically significant macular oedema:a 20 year study of type 1 diabetes
 Downloaded from orbit.dtu.dk on: Jan 05, 2019 Impact of changes in metabolic control on progression to photocoagulation for clinically significant macular oedema:a 20 year study of type 1 diabetes Sander,
Downloaded from orbit.dtu.dk on: Jan 05, 2019 Impact of changes in metabolic control on progression to photocoagulation for clinically significant macular oedema:a 20 year study of type 1 diabetes Sander,
Increased mortality after fracture of the surgical neck of the humerus: a case-control study of 253 patients with a 12-year follow-up.
 Increased mortality after fracture of the surgical neck of the humerus: a case-control study of 253 patients with a 12-year follow-up. Olsson, Christian; Petersson, Claes; Nordquist, Anders Published in:
Increased mortality after fracture of the surgical neck of the humerus: a case-control study of 253 patients with a 12-year follow-up. Olsson, Christian; Petersson, Claes; Nordquist, Anders Published in:
A New Model for Assessment of Change in Visual Function in Diabetes
 A New Model for Assessment of Change in Visual Function in Diabetes HELLGREN, KARL-JOHAN 2014 Link to publication Citation for published version (APA): Hellgren, K-J. (2014). A New Model for Assessment
A New Model for Assessment of Change in Visual Function in Diabetes HELLGREN, KARL-JOHAN 2014 Link to publication Citation for published version (APA): Hellgren, K-J. (2014). A New Model for Assessment
Proliferative retinopathy and proteinuria predict mortality rate in type 1 diabetic patients from Fyn County, Denmark
 Diabetologia (2008) 51:583 588 DOI 10.1007/s00125-008-0953-8 ARTICLE Proliferative retinopathy and proteinuria predict mortality rate in type 1 diabetic patients from Fyn County, Denmark J. Grauslund &
Diabetologia (2008) 51:583 588 DOI 10.1007/s00125-008-0953-8 ARTICLE Proliferative retinopathy and proteinuria predict mortality rate in type 1 diabetic patients from Fyn County, Denmark J. Grauslund &
The Natural History of Diabetic Retinopathy and How Primary Care Makes A Difference
 The Natural History of Diabetic Retinopathy and How Primary Care Makes A Difference We will discuss - How exactly does blood sugar control affect retinopathy? - What are other factors that we measure in
The Natural History of Diabetic Retinopathy and How Primary Care Makes A Difference We will discuss - How exactly does blood sugar control affect retinopathy? - What are other factors that we measure in
Fundus Fluorescein Angiography in Diabetic Retinopathy: Correlation of Angiographic Findings to the Clinical Maculopathy Abstract: Purpose:
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XII (Feb. 2016), PP 80-88 www.iosrjournals.org Fundus Fluorescein Angiography in Diabetic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XII (Feb. 2016), PP 80-88 www.iosrjournals.org Fundus Fluorescein Angiography in Diabetic
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient
 Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Optic Disc Cupping: Four Year Follow-up from the WESDR
 Investigative Ophthalmology & Visual Science, Vol. 30, o., February 989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Four Year Follow-up from the WER Barbara E. K.
Investigative Ophthalmology & Visual Science, Vol. 30, o., February 989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Four Year Follow-up from the WER Barbara E. K.
CLINICAL SCIENCES. Results After Lens Extraction in Patients With Diabetic Retinopathy. Early Treatment Diabetic Retinopathy Study Report Number 25
 CLINICAL SCIENCES Results After Lens Extraction in Patients With Diabetic Retinopathy Early Treatment Diabetic Retinopathy Study Report Number 25 Emily Y. Chew, MD; William E. Benson, MD; Nancy A. Remaley,
CLINICAL SCIENCES Results After Lens Extraction in Patients With Diabetic Retinopathy Early Treatment Diabetic Retinopathy Study Report Number 25 Emily Y. Chew, MD; William E. Benson, MD; Nancy A. Remaley,
Efficacy of principle-guided laser treatment in diabetic retinopathy.
 Biomedical Research 2017; 28 (6): 2566-2570 ISSN 0970-938X www.biomedres.info Efficacy of 4-2-1 principle-guided laser treatment in diabetic retinopathy. Ding Xu 1, Chun-Xia Li 2, Chun Zhao 1, Wan-Cheng
Biomedical Research 2017; 28 (6): 2566-2570 ISSN 0970-938X www.biomedres.info Efficacy of 4-2-1 principle-guided laser treatment in diabetic retinopathy. Ding Xu 1, Chun-Xia Li 2, Chun Zhao 1, Wan-Cheng
Diabetic Retinopatathy
 Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
DIABETIC RETINOPATHY
 DIABETIC RETINOPATHY C. L. B. Canny, MD FRCSC Diabetic retinopathy is the most serious eye manifestation of diabetes and is responsible for most of the blindness caused by diabetes. Diabetic retinopathy
DIABETIC RETINOPATHY C. L. B. Canny, MD FRCSC Diabetic retinopathy is the most serious eye manifestation of diabetes and is responsible for most of the blindness caused by diabetes. Diabetic retinopathy
Diabetic retinopathy (DR) was first PROCEEDINGS DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT
 DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT Diabetic retinopathy (DR) is characterized by the development of retinal microaneurysms, hemorrhages, deposits of leaked lipoproteins (hard exudates),
DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT Diabetic retinopathy (DR) is characterized by the development of retinal microaneurysms, hemorrhages, deposits of leaked lipoproteins (hard exudates),
Medical Retina 2011 Nicholas Lee
 Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
RANZCO Screening and Referral Pathway for Diabetic Retinopathy #
 RANZCO Screening and Referral Pathway for Diabetic Retinopathy # Patient Presents a. Screen for Diabetic Retinopathy every 2 years b. Begin screening at diagnosis of Diabetes * Clinical Modifi ers Yearly
RANZCO Screening and Referral Pathway for Diabetic Retinopathy # Patient Presents a. Screen for Diabetic Retinopathy every 2 years b. Begin screening at diagnosis of Diabetes * Clinical Modifi ers Yearly
Diabetes, particularly diabetic retinopathy, is
 Chapter 14 Vision Disorders in Diabetes Ronald Klein, MD, MPH, and Barbara E.K. Klein, MD, MPH SUMMARY Diabetes, particularly diabetic retinopathy, is the leading cause of new cases of blindness in people
Chapter 14 Vision Disorders in Diabetes Ronald Klein, MD, MPH, and Barbara E.K. Klein, MD, MPH SUMMARY Diabetes, particularly diabetic retinopathy, is the leading cause of new cases of blindness in people
Optic Disc Cupping: Prevalence Findings from the WESDR
 Investigative Ophthalmology & Visual Science, Vol., o. 2, February 1989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Prevalence Findings from the WER Barbara E. K.
Investigative Ophthalmology & Visual Science, Vol., o. 2, February 1989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Prevalence Findings from the WER Barbara E. K.
In its initial report, the Early Treatment Diabetic Retinopathy. A Severity Scale for Diabetic Macular Edema Developed from ETDRS Data
 A Severity Scale for Diabetic Macular Edema Developed from ETDRS Data Ronald E. Gangnon, 1,2 Matthew D. Davis, 3 Larry D. Hubbard, 3 Lloyd M. Aiello, 4 Emily Y. Chew, 5 Frederick L. Ferris III, 5 Marian
A Severity Scale for Diabetic Macular Edema Developed from ETDRS Data Ronald E. Gangnon, 1,2 Matthew D. Davis, 3 Larry D. Hubbard, 3 Lloyd M. Aiello, 4 Emily Y. Chew, 5 Frederick L. Ferris III, 5 Marian
Microaneurysms in the development of diabetic retinopathy (UKPDS 42)
 Diabetologia (1999) 42: 1107±1112 Ó Springer-Verlag 1999 Microaneurysms in the development of diabetic retinopathy (UKPDS 42) E.M. Kohner 1, I. M. Stratton 2, S. J. Aldington 3, R. C. Turner 2, D. R. Matthews
Diabetologia (1999) 42: 1107±1112 Ó Springer-Verlag 1999 Microaneurysms in the development of diabetic retinopathy (UKPDS 42) E.M. Kohner 1, I. M. Stratton 2, S. J. Aldington 3, R. C. Turner 2, D. R. Matthews
Diabetic Retinopathy
 Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Retinopathy in a diabetic population
 Kathmandu University Medical Journal (2007), Vol. 5, No. 2, Issue 18, 204-209 Retinopathy in a diabetic population Shrestha S 1, Malla OK 2, Karki DB 3, Byanju RN 4 2 Fellow of NAMS, 3 Professor, NAMS,
Kathmandu University Medical Journal (2007), Vol. 5, No. 2, Issue 18, 204-209 Retinopathy in a diabetic population Shrestha S 1, Malla OK 2, Karki DB 3, Byanju RN 4 2 Fellow of NAMS, 3 Professor, NAMS,
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
Diabetic Retinopathy Screening in Hong Kong. Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong
 Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Longitudinal Studies of Incidence and Progression of Diabetic Retinopathy Assessed by Retinal Photography in Pima Indians
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Longitudinal Studies of Incidence and Progression of Diabetic Retinopathy Assessed by Retinal Photography in Pima Indians
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Longitudinal Studies of Incidence and Progression of Diabetic Retinopathy Assessed by Retinal Photography in Pima Indians
Effect of Ruboxistaurin on Blood Retinal Barrier Permeability in Relation to Severity of Leakage in Diabetic Macular Edema
 Effect of Ruboxistaurin on Blood Retinal Barrier in Relation to Severity of Leakage in Diabetic Macular Edema The Harvard community has made this article openly available. Please share how this access
Effect of Ruboxistaurin on Blood Retinal Barrier in Relation to Severity of Leakage in Diabetic Macular Edema The Harvard community has made this article openly available. Please share how this access
Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic
 Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic 25.6 million adults 11.3% of the adult population 10.9 million adults 65 years and older 26.9% of this age population 79 million people are Pre-diabetic!!
Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic 25.6 million adults 11.3% of the adult population 10.9 million adults 65 years and older 26.9% of this age population 79 million people are Pre-diabetic!!
Treatment of Diabetic Macular Edema without Intravitreal injections
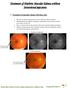 Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
7Progression and regression:
 7Progression and regression: Distinct developmental patterns of diabetic retinopathy in patients with type 2 diabetes treated in the Diabetes Care System West-Friesland, the Netherlands Hata Zavrelova,
7Progression and regression: Distinct developmental patterns of diabetic retinopathy in patients with type 2 diabetes treated in the Diabetes Care System West-Friesland, the Netherlands Hata Zavrelova,
DIABETIC RETINOPATHY AMONG TYPE 2 DIABETIC PATIENTS PRESENTING WITH MICROALBUMINURIA
 ORIGINAL ARTICLE DIABETIC RETINOPATHY AMONG TYPE 2 DIABETIC PATIENTS PRESENTING WITH MICROALBUMINURIA Arshad Hussain 1, Iqbal Wahid 2, Danish Ali Khan 3 ABSTRACT INTRODUCTION: Diabetes mellitus is becoming
ORIGINAL ARTICLE DIABETIC RETINOPATHY AMONG TYPE 2 DIABETIC PATIENTS PRESENTING WITH MICROALBUMINURIA Arshad Hussain 1, Iqbal Wahid 2, Danish Ali Khan 3 ABSTRACT INTRODUCTION: Diabetes mellitus is becoming
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
Charles Darwin University
 Charles Darwin University Area-under-the-HbA1c-curve above the normal range and the prediction of microvascular outcomes an analysis of data from the Diabetes Control and Complications Trial Maple-Brown,
Charles Darwin University Area-under-the-HbA1c-curve above the normal range and the prediction of microvascular outcomes an analysis of data from the Diabetes Control and Complications Trial Maple-Brown,
Schatz, Patrik; Skarin, Angelika; Lavaque, Alejandro J; Lima, Luiz H; Arevalo, Jose Fernando
 Preservation of macular structure and function after intravitreal aflibercept for choroidal neovascularization associated with serpiginous choroiditis. Schatz, Patrik; Skarin, Angelika; Lavaque, Alejandro
Preservation of macular structure and function after intravitreal aflibercept for choroidal neovascularization associated with serpiginous choroiditis. Schatz, Patrik; Skarin, Angelika; Lavaque, Alejandro
FREQUENCY OF DIABETIC RETINOPATHY IN A TERTIARY CARE HOSPITAL USING DIGITAL RETINAL IMAGING TECHNOLOGY
 ORIGINAL ARTICLE FREQUENCY OF DIABETIC RETINOPATHY IN A TERTIARY CARE HOSPITAL USING DIGITAL RETINAL IMAGING TECHNOLOGY INTRODUCTION As more and more people are being affected with diabetes and with poor
ORIGINAL ARTICLE FREQUENCY OF DIABETIC RETINOPATHY IN A TERTIARY CARE HOSPITAL USING DIGITAL RETINAL IMAGING TECHNOLOGY INTRODUCTION As more and more people are being affected with diabetes and with poor
Central Mersey Diabetic Retinopathy Screening Programme. Referring patients for Diabetic Retinopathy Screening
 Central Mersey Diabetic Retinopathy Screening Programme Referring patients for Diabetic Retinopathy Screening Information for GPs in Halton & St Helens, Knowsley and Warrington PCT Version: June 2008 Review
Central Mersey Diabetic Retinopathy Screening Programme Referring patients for Diabetic Retinopathy Screening Information for GPs in Halton & St Helens, Knowsley and Warrington PCT Version: June 2008 Review
Diabetic Retinopathy
 Diabetic Retinopathy Introduction People with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina that is caused by diabetes.
Diabetic Retinopathy Introduction People with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina that is caused by diabetes.
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation
 Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic Retinopathy Screening Programme
 (2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
(2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
Risk Factors for High-Risk Proliferative Diabetic Retinopathy and Severe Visual Loss: Early Treatment Diabetic Retinopathy Study Report #18
 Risk Factors for High-Risk Proliferative Diabetic Retinopathy and Severe Visual Loss: Early Treatment Diabetic Retinopathy Study Report #18 Matthew D. Davis, 1 Marian R. Fisher, 1 Ronald E. Gangnon, 1
Risk Factors for High-Risk Proliferative Diabetic Retinopathy and Severe Visual Loss: Early Treatment Diabetic Retinopathy Study Report #18 Matthew D. Davis, 1 Marian R. Fisher, 1 Ronald E. Gangnon, 1
A LOOK INSIDE DIABETIC EYE DISEASE
 A LOOK INSIDE DIABETIC EYE DISEASE JILL M. DILLON, O.D. DEPARTMENT OF OPHTHALMOLOGY/OPTOMETRY MARSHFIELD CLINIC 1 FINANCIAL DISCLOSURES I have no financial interest or relationships to disclose. Any references
A LOOK INSIDE DIABETIC EYE DISEASE JILL M. DILLON, O.D. DEPARTMENT OF OPHTHALMOLOGY/OPTOMETRY MARSHFIELD CLINIC 1 FINANCIAL DISCLOSURES I have no financial interest or relationships to disclose. Any references
Ten recommendations for Osteoarthritis and Cartilage (OAC) manuscript preparation, common for all types of studies.
 Ten recommendations for Osteoarthritis and Cartilage (OAC) manuscript preparation, common for all types of studies. Ranstam, Jonas; Lohmander, L Stefan Published in: Osteoarthritis and Cartilage DOI: 10.1016/j.joca.2011.07.007
Ten recommendations for Osteoarthritis and Cartilage (OAC) manuscript preparation, common for all types of studies. Ranstam, Jonas; Lohmander, L Stefan Published in: Osteoarthritis and Cartilage DOI: 10.1016/j.joca.2011.07.007
Diabetic Retinopathy Frequently Asked Questions
 Diabetic Retinopathy Frequently Asked Questions Q.Who is at risk of diabetic retinopathy? Diabetic retinopathy is a highly vascularised eye complication of both insulin dependent and non-insulin dependent
Diabetic Retinopathy Frequently Asked Questions Q.Who is at risk of diabetic retinopathy? Diabetic retinopathy is a highly vascularised eye complication of both insulin dependent and non-insulin dependent
Slide notes: The major chronic complications of diabetes mellitus are described here. Among these, microvascular complications have an important
 1 2 The major chronic complications of diabetes mellitus are described here. Among these, microvascular complications have an important role. They comprise microangiopathy, diabetic retinopathy, diabetic
1 2 The major chronic complications of diabetes mellitus are described here. Among these, microvascular complications have an important role. They comprise microangiopathy, diabetic retinopathy, diabetic
Treatment of diabetic maculopathy by
 Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Understanding Diabetic Retinopathy
 Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Clinical Trials in Diabetic Retinopathy. Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D.
 1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
End-of-life care in oxygen-dependent COPD and cancer: a national population-based study.
 End-of-life care in oxygen-dependent COPD and cancer: a national population-based study. Ahmadi, Zainab; Lundström, Staffan; Janson, Christer; Strang, Peter; Emtner, Margareta; Currow, David C; Ekström,
End-of-life care in oxygen-dependent COPD and cancer: a national population-based study. Ahmadi, Zainab; Lundström, Staffan; Janson, Christer; Strang, Peter; Emtner, Margareta; Currow, David C; Ekström,
Retinal vessel calibre and micro- and macrovascular complications in type 1 diabetes
 Diabetologia (2009) 52:2213 2217 DOI 10.1007/s00125-009-1459-8 SHORT COMMUNICATION Retinal vessel calibre and micro- and macrovascular complications in type 1 diabetes J. Grauslund & L. Hodgson & R. Kawasaki
Diabetologia (2009) 52:2213 2217 DOI 10.1007/s00125-009-1459-8 SHORT COMMUNICATION Retinal vessel calibre and micro- and macrovascular complications in type 1 diabetes J. Grauslund & L. Hodgson & R. Kawasaki
Influence of pregnancy on long-term progression of retinopathy in patients with type 1 diabetes
 Diabetologia (2008) 51:1041 1045 DOI 10.1007/s00125-008-0994-z ARTICLE Influence of pregnancy on long-term progression of retinopathy in patients with type 1 diabetes C. S. Arun & R. Taylor Received: 31
Diabetologia (2008) 51:1041 1045 DOI 10.1007/s00125-008-0994-z ARTICLE Influence of pregnancy on long-term progression of retinopathy in patients with type 1 diabetes C. S. Arun & R. Taylor Received: 31
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Brampton Hurontario Street Brampton, ON L6Y 0P6
 Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
X-Plain Diabetic Retinopathy Reference Summary
 X-Plain Diabetic Retinopathy Reference Summary Introduction Patients with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina
X-Plain Diabetic Retinopathy Reference Summary Introduction Patients with diabetes are more likely to have eye problems that can lead to blindness. Diabetic retinopathy is a disease of the eye s retina
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington
 Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
MAGNITUDE OF DIABETIC EYE DISEASE IN INDIA
 Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
The prevalence of retinopathy in subjects with and without type 2 diabetes mellitus
 The prevalence of retinopathy in subjects with and without type 2 diabetes mellitus Eydis Olafsdottir, 1,2,3 Dan K. G. Andersson, 4 Inger Dedorsson 3 and Einar Stefa nsson 1,2 1 Department of Ophthalmology,
The prevalence of retinopathy in subjects with and without type 2 diabetes mellitus Eydis Olafsdottir, 1,2,3 Dan K. G. Andersson, 4 Inger Dedorsson 3 and Einar Stefa nsson 1,2 1 Department of Ophthalmology,
FRANZCO, MD, MBBS. Royal Darwin Hospital
 Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Association between symptoms of depression and glycaemic control may be unstable across gender Pouwer, François; Snoek, F.J.
 Tilburg University Association between symptoms of depression and glycaemic control may be unstable across gender Pouwer, François; Snoek, F.J. Published in: Diabetic Medicine: Journal of Diabetes UK Publication
Tilburg University Association between symptoms of depression and glycaemic control may be unstable across gender Pouwer, François; Snoek, F.J. Published in: Diabetic Medicine: Journal of Diabetes UK Publication
Macular function assessed with mferg before and after panretinal photocoagulation in patients with proliferative diabetic retinopathy.
 Macular function assessed with mferg before and after panretinal photocoagulation in patients with proliferative diabetic retinopathy. Lövestam Adrian, Monica; Andréasson, Sten; Ponjavic, Vesna Published
Macular function assessed with mferg before and after panretinal photocoagulation in patients with proliferative diabetic retinopathy. Lövestam Adrian, Monica; Andréasson, Sten; Ponjavic, Vesna Published
Management of diabetic eye disease: an overview
 Peter Blows Photographic screening for diabetic eye disease can identify patients who will benefit from laser treatment. BOTSWANA MANAGEMENT Management of diabetic eye disease: an overview Laser for DR
Peter Blows Photographic screening for diabetic eye disease can identify patients who will benefit from laser treatment. BOTSWANA MANAGEMENT Management of diabetic eye disease: an overview Laser for DR
Diabetic Retinopathy A Presentation for the Public
 Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Prevalence of diabetic retinopathy in diabetics of rural population belonging to Ramanagara and Chikkaballapura districts of Karnataka
 International Journal of Scientific and Research Publications, Volume 5, Issue 3, March 215 1 ISSN 225-3153 Prevalence of diabetic retinopathy in diabetics of rural population belonging to Ramanagara and
International Journal of Scientific and Research Publications, Volume 5, Issue 3, March 215 1 ISSN 225-3153 Prevalence of diabetic retinopathy in diabetics of rural population belonging to Ramanagara and
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA
 Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
Vitrectomy Combined with Phacoemulsification and Intraocular Lens Implantation for Diabetic Macular Edema
 Vitrectomy Combined with Phacoemulsification and Intraocular Lens Implantation for Diabetic Macular Edema Kentaro Amino* and Hidenobu Tanihara *Amino Eye Clinic, Shimonoseki, Yamaguchi Prefecture, Japan;
Vitrectomy Combined with Phacoemulsification and Intraocular Lens Implantation for Diabetic Macular Edema Kentaro Amino* and Hidenobu Tanihara *Amino Eye Clinic, Shimonoseki, Yamaguchi Prefecture, Japan;
Front Line Diabetic Retinopathy What Not to Miss and Why
 Front Line Diabetic Retinopathy What Not to Miss and Why David M Brown MD FACS Clinical Professor of Ophthalmology Blanton Eye Institute, Houston Methodist Hospital Baylor College of Medicine Retina Consultants
Front Line Diabetic Retinopathy What Not to Miss and Why David M Brown MD FACS Clinical Professor of Ophthalmology Blanton Eye Institute, Houston Methodist Hospital Baylor College of Medicine Retina Consultants
Diabetic Eye Disease
 Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Abstract. Introduction. Original paper. Comparison of screening for diabetic retinopathy by non-specialists and specialists
 Comparison of screening for diabetic retinopathy by non-specialists and specialists Effectiveness of screening for diabetic retinopathy by nonspecialist doctors: the importance of physician-ophthalmologist
Comparison of screening for diabetic retinopathy by non-specialists and specialists Effectiveness of screening for diabetic retinopathy by nonspecialist doctors: the importance of physician-ophthalmologist
Diabetic Retinopathy in Primary Care
 Diabetic Retinopathy in Primary Care Epidemiology Diabetes is one of the most serious challenges to health care world rld-wide. According to recent projections it will affect 239 million people e by 2010-
Diabetic Retinopathy in Primary Care Epidemiology Diabetes is one of the most serious challenges to health care world rld-wide. According to recent projections it will affect 239 million people e by 2010-
PROCEEDINGS THE IMPORTANCE OF ENDOTHELIAL DAMAGE: DIABETIC RETINOPATHY* Massimo Porta, MD, PhD ABSTRACT
 THE IMPORTANCE OF ENDOTHELIAL DAMAGE: DIABETIC RETINOPATHY* Massimo Porta, MD, PhD ABSTRACT Diabetic retinopathy is the leading cause of blindness in adults of working age in industrialized countries and
THE IMPORTANCE OF ENDOTHELIAL DAMAGE: DIABETIC RETINOPATHY* Massimo Porta, MD, PhD ABSTRACT Diabetic retinopathy is the leading cause of blindness in adults of working age in industrialized countries and
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Puschmann, Andreas; Dickson, Dennis W; Englund, Elisabet; Wszolek, Zbigniew K; Ross, Owen A
 CHCHD2 and Parkinson's disease Puschmann, Andreas; Dickson, Dennis W; Englund, Elisabet; Wszolek, Zbigniew K; Ross, Owen A Published in: Lancet Neurology DOI: 10.1016/S1474-4422(15)00095-2 2015 Link to
CHCHD2 and Parkinson's disease Puschmann, Andreas; Dickson, Dennis W; Englund, Elisabet; Wszolek, Zbigniew K; Ross, Owen A Published in: Lancet Neurology DOI: 10.1016/S1474-4422(15)00095-2 2015 Link to
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Control of Systemic Factors Can Preserve Vision in Diabetic Retinopathy
 dmcjuly05_cme_dr 7/28/05 9:19 AM Page 38 Control of Systemic Factors Can Preserve Vision in Diabetic Retinopathy Jointly sponsored by The Dulaney Foundation and Diabetic Microvascular Complications Today.
dmcjuly05_cme_dr 7/28/05 9:19 AM Page 38 Control of Systemic Factors Can Preserve Vision in Diabetic Retinopathy Jointly sponsored by The Dulaney Foundation and Diabetic Microvascular Complications Today.
Progression of diabetic retinopathy after cataract extraction
 BritishlournalofOphthalmology, 1991,75,547-551 Ophthalmology Department, Kaplan Hospital, Rehovot, affiliated with the Hebrew University-Hadassah Medical School, Jerusalem, Israel A Pollock S Dotan M Oliver
BritishlournalofOphthalmology, 1991,75,547-551 Ophthalmology Department, Kaplan Hospital, Rehovot, affiliated with the Hebrew University-Hadassah Medical School, Jerusalem, Israel A Pollock S Dotan M Oliver
Diabetic retinopathy in Victoria, Australia: the Visual Impairment Project
 Br J Ophthalmol 2000;84:865 870 865 Centre for Eye Research Australia, University of Melbourne, Melbourne, Australia R McKay C A McCarty H R Taylor Correspondence to: Cathy McCarty, Centre for Eye Research
Br J Ophthalmol 2000;84:865 870 865 Centre for Eye Research Australia, University of Melbourne, Melbourne, Australia R McKay C A McCarty H R Taylor Correspondence to: Cathy McCarty, Centre for Eye Research
Cronfa - Swansea University Open Access Repository
 Cronfa - Swansea University Open Access Repository This is an author produced version of a paper published in : Expert review of endocrinology & diabetes Cronfa URL for this paper: http://cronfa.swan.ac.uk/record/cronfa25942
Cronfa - Swansea University Open Access Repository This is an author produced version of a paper published in : Expert review of endocrinology & diabetes Cronfa URL for this paper: http://cronfa.swan.ac.uk/record/cronfa25942
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Obstructive sleep apnoea and retinopathy in patients with type 2 diabetes Altaf, Quratul-ain; Dodson, Paul; Ali, Asad; Raymond, Neil T; Wharton, Helen; Hampshire- Bancroft, Rachel; Shah, Mirriam; Shepherd,
Obstructive sleep apnoea and retinopathy in patients with type 2 diabetes Altaf, Quratul-ain; Dodson, Paul; Ali, Asad; Raymond, Neil T; Wharton, Helen; Hampshire- Bancroft, Rachel; Shah, Mirriam; Shepherd,
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
The Relationship among COPD Severity, Inhaled Corticosteroid Use, and the Risk of Pneumonia.
 The Relationship among COPD Severity, Inhaled Corticosteroid Use, and the Risk of Pneumonia. Rennard, Stephen I; Sin, Donald D; Tashkin, Donald P; Calverley, Peter M; Radner, Finn Published in: Annals
The Relationship among COPD Severity, Inhaled Corticosteroid Use, and the Risk of Pneumonia. Rennard, Stephen I; Sin, Donald D; Tashkin, Donald P; Calverley, Peter M; Radner, Finn Published in: Annals
Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus
 Original article: Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus 1Dr Apoorva*, 2 Dr Sabhia Jan 1Senior Resident, 2
Original article: Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus 1Dr Apoorva*, 2 Dr Sabhia Jan 1Senior Resident, 2
Use of eye care services by people with diabetes: the Melbourne Visual Impairment Project
 410 Department of Ophthalmology, University of Melbourne, Melbourne, Australia C A McCarty C W Lloyd-Smith P M Livingston Y L Stanislavsky H R Taylor Victorian WorkCover Authority, Melbourne, Australia
410 Department of Ophthalmology, University of Melbourne, Melbourne, Australia C A McCarty C W Lloyd-Smith P M Livingston Y L Stanislavsky H R Taylor Victorian WorkCover Authority, Melbourne, Australia
Outline. Preventing & Treating Diabetes Related Blindness. Eye Care Center Doctors. Justin Kanoff, MD. Eye Care Center of Northern Colorado
 Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
MATERIALS AND METHODS
 Automated Detection of Diabetic Retinopathy in a Fundus Photographic Screening Population Nicolai Larsen, 1,2 Jannik Godt, 3 Michael Grunkin, 3 Henrik Lund-Andersen, 1,2 and Michael Larsen 1 PURPOSE. To
Automated Detection of Diabetic Retinopathy in a Fundus Photographic Screening Population Nicolai Larsen, 1,2 Jannik Godt, 3 Michael Grunkin, 3 Henrik Lund-Andersen, 1,2 and Michael Larsen 1 PURPOSE. To
