Outcomes of Acellular Dermal Matrix for Immediate Tissue Expander Reconstruction with Radiotherapy: A Retrospective Cohort Study
|
|
|
- Lily Evans
- 5 years ago
- Views:
Transcription
1 Breast Surgery 5 Outcomes of Acellular Dermal Matrix for Immediate Tissue Expander Reconstruction with Radiotherapy: A Retrospective Cohort Study Aesthetic Surgery Journal 2018, The American Society for Aesthetic Plastic Surgery, Inc. Reprints and permission: journals.permissions@oup.com DOI: /asj/sjy Elizabeth S. Craig, MD; Mark W. Clemens, MD; John C. Koshy, MD; James Wren, BS; Zhang Hong, PhD; Charles Butler, MD; Patrick Garvey, MD; Jesse Selber, MD; and Steven Kronowitz, MD Abstract Background: Despite increasing literature support for the use of acellular dermal matrix (ADM) in expander-based breast reconstruction, the effect of ADM on clinical outcomes in the presence of post-mastectomy radiation therapy (PMRT) has not been well described. Objectives: To analyze the impact ADM plays on clinical outcomes on immediate tissue expander (ITE) reconstruction undergoing PMRT. Methods: We retrospectively reviewed patients who underwent ITE breast reconstruction from 2004 to 2014 at MD Anderson Cancer Center. Patients were categorized into four cohorts: ADM, ADM with PMRT, non-adm, and non-adm with PMRT. Outcomes and complications were compared among cohorts. Results: Over 10 years, 957 patients underwent ITE reconstruction (683 non-adm, 113 non-adm with PMRT, 486 ADM, and 88 ADM with PMRT) with 1370 reconstructions. Overall complication rates for the ADM and non-adm cohorts were 39.0% and 16.7%, respectively (P < 0.001). Within both cohorts, mastectomy skin flap necrosis (MSFN) was the most common complication, followed by infection. ADM use was associated with a significantly higher rate of infections and seromas in both radiated and non-radiated groups; however, when comparing radiated cohorts, the incidence of explantation was significantly lower with the use of ADM. Conclusions: The decision to use ADM for expander-based breast reconstruction should be performed with caution, given higher overall rates of complications, including infections and seromas. There may, however, be a role for ADM in cases requiring PMRT, as the overall incidence of implant failure is lower than non-adm cases Level of Evidence: 3 85 Editorial Decision date: May 10, Two-stage prosthetic breast reconstruction is currently the most common method of reconstruction for breast cancer patients worldwide, and over 68,000 tissue expander-based (TE) reconstructions were performed in the United States in 2016 alone. 1 The ability of ADM to assist with vascularized soft tissue coverage, increase intraoperative fill volumes, secure the pocket, improve breast ptosis, and reinforce the inframammary fold have led to its widespread use. 2 9 ADM has gained popularity for its ability to provide optimal cosmetic results in implant-based reconstruction, 10,11 but the From the Department of Plastic and Reconstructive Surgery, The University of Texas MD Anderson Cancer Center, Houston, TX. Dr Clemens is a Breast Surgery Section Editor for the Aesthetic Surgery Journal. Corresponding Author: Dr Mark Clemens, The University of Texas MD Anderson Cancer Center, 1400 Pressler St., Unit 1488, Houston, TX 77030, USA. mwclemens@mdanderson.org Presented in 2014 at the Texas Society of Plastic Surgeons Annual Meeting in San Antonio, TX
2 2 Aesthetic Surgery Journal aesthetic advantages have been tempered by the controversial data regarding seroma, infection, and other complication rates. 10,12 15 The beneficial impact that PMRT has on decreasing loco-regional recurrence in breast cancer patients has been well documented. 16 In 2004, Kronowitz et al introduced the concept of delayed-immediate and delayed-delayed breast reconstruction, in an effort to preserve the breast footprint and skin envelope in cases in which the risk of PMRT is unknown. 5 However, this has posed a growing challenge to reconstructive surgeons, as the literature is replete with evidence illustrating the deleterious effects of PMRT on expander/ implant-based reconstruction, with complication rates as high as 58.8%. 2,5,12,16 19 In addition, the literature has highlighted the large proportion of patients in this population with unacceptable aesthetic results leading to expander/implant removal While most reconstructive surgeons prefer autologous tissue reconstruction to expander/implant-based reconstruction in patients at risk for PMRT, it is not always feasible. As indications for PMRT continue to grow, understanding the outcomes of ADM in a radiated field becomes critical. The purpose of our study was to examine the impact of ADM with PMRT on clinical outcomes in ITE by performing a retrospective cohort study, which included ADM/non-ADM and PMRT/non-PMRT cohorts. METHODS We retrospectively reviewed a prospectively maintained database of consecutive patients who underwent ITE breast reconstruction from June 2004 to December 2014 at The University of Texas MD Anderson Cancer Center. Patients were categorized into 4 cohorts: ADM, ADM with PMRT, non- ADM, and non-adm with PMRT. Demographic information, comorbidities, perioperative data, operative data, and complications were collected for comparison. The primary outcomes evaluated were seroma (clinically appreciable fluid collection requiring drainage), infection (cellulitis requiring antibiotic treatment), delayed wound healing (incision opening greater than 5 mm), and MSFN (including sloughing, desquamation, and full-thickness loss requiring bedside or operative debridement). The timing of complications was evaluated by comparing both ADM and non-adm groups, as well as PMRT and non-pmrt groups. Patients were excluded from the study if they received pre-mastectomy radiation therapy, or did not reach the endpoint of explantation or implant exchange and were lost to follow-up. This study was approved and carried out under the guidelines of the Institutional Review Board of MD Anderson Cancer Center. Statistical Analysis A univariate analysis was utilized to examine the associations between outcomes and patient characteristic. Patient Table 1. Overall Demographic Information Characteristic characteristics that were found to have both associations and P values less than or equal to 0.25 in the univariate analysis, were then included as independent variables in the multivariate generalized estimation model (GEE). The final multivariate model was determined using a backward-selection algorithm. Multivariate GEE was used to assess the impact of various confounders on patient outcomes. The analyses were performed in SAS 9.2 (SAS Institute, Inc., Cary, NC). The timing of occurrence of complications among the cohorts was compared using a 2-sided Wilcoxon rank sum test, with a P value less than 0.05 considered significant. In order to rule out temporal bias, outcomes between the first and last 5 years of the study were compared, and the rates of overall complications were found to be equivalent. In addition, plastic surgeons and breast surgeons were grouped by the number of cases performed and included in the multivariate analysis to evaluate surgeon technique or experience as potential confounders; however, these were also not found to be significant. Surgical Techniques Total N = 957 patients Age in years, mean ± SD 49.3 ± 10.6 Range BMI, mean ± SD 26.6 ± 10.2 Range Smoker Active 64 (6.7) Previous 185 (19.3) Diabetes 58 (6.1) Peripheral vascular disease 2 (0.2) Overall demographic information of patients included in this study. Tissue expanders were placed in the subpectoral pocket. Reconstructions without ADM involved either partial or total muscle coverage with standard elevation of the serratus anterior and/or rectus fascia. Reconstructions utilizing ADM were performed by securing a sheet of ADM to the inferior border of the pectoralis muscle once it had been released from the chest wall as a pectoralis muscle extension. Intraoperative tissue expansion was performed to tissue tolerance. Drains were placed according to surgeon preference. On average, the length of drains was 10 days (range 7-22 days). Removal of drains was at the discretion of the attending physician and therefore was not standardized across all physicians. In general, drains were removed when output was less than 30 ml for 2 consecutive days
3 Craig et al Table 2. Cohort Demographic Information Characteristic Non-Radiated Radiated P values Non-ADM ADM Non-ADM ADM N = 683 N = 486 N =113 N = 88 Age in years, mean ± SD ± 10.6 Range ± 10.7 Range ± 10.0 Range ± 9.4 Range BMI, mean ± SD ± 13.4 Range ± 5.7 Range ± 5.7 Range ± 5.3 Range Smoker 0.83 Active 42 (6.1) 34 (7.0) 10 (8.8) 4 (4.5) Previous 133 (19.5) 90 (18.5) 23 (20.4) 15 (17.0) Diabetes 44 (6.4) 34 (7.0) 3 (2.7) 0 (0) 0.04 Peripheral vascular disease 0 (0) 3 (0.6) 0 (0) 0 (0) NA Subgroup demographic information (radiated vs non-radiated and non-adm vs ADM). Of note, data for 6 breasts had to be excluded from the ADM-radiated cohort because of missing radiation therapy information, resulting in 88 instead of 94 breasts in the radiated ADM cohort Table 3. Patient Outcomes by ADM Group Characteristic Total Non-Radiated Radiated P value (N = 1376 breasts) Non-ADM ADM Non-ADM ADM Complication 359 (26.1) 106 (15.5) 182 (37.4) 27 (23.9) 42 (47.7) < Dehiscence 55 (4.0) 17 (2.5) 30 (6.2) 3 (2.7) 5 (5.7) Hematoma 25 (1.8) 13 (1.9) 7 (1.4) 2 (1.8) 3 (3.4) 0.83 Infection 108 (7.8) 25 (3.7) 56 (11.5) 13 (11.5) 14 (15.9) < Necrosis 207 (15.0) 45 (6.6) 124 (25.5) 15 (13.3) 21 (23.9) < Seroma 97 (7.0) 26 (3.8) 53 (10.9) 6 (5.3) 12 (13.6) < Explantation 119 (8.6) 40 (5.9) 46 (9.5) 23 (20.4) 10 (11.4) Overall complication rates based on total number of patients included in this study, and based on subgroup. Perioperative antibiotics were administered and, in general, continued postoperatively until all drains were removed. RESULTS One-thousand-three-hundred-seventy-six breast reconstructions in 957 patients with ITE (574 reconstructions performed with ADM, and 796 without ADM) met our inclusion criteria (Table 1). The type of ADM used was divided, as 24.7% of surgeons utilized Surgimend (TEI Biosciences, Boston, MA) and 75.3% utilized Alloderm (LifeCell Corporation, Bridgewater, NJ). The type of mesh used in ADM reconstructions was analyzed against primary outcomes and found to have no influence. Fifteen percent of the entire cohort received PMRT, 27% received neoadjuvant chemotherapy, and 28% received adjuvant chemotherapy. The majority of mastectomies (90.4%) utilized a skin-sparing technique; 6% were nipple sparing. The average follow-up was 210 days (range, ). Demographics were comparable among all groups (Table 2), with the following exceptions. Patients in the ADM without PMRT cohort were older and had a higher incidence of diabetes than patients in the other cohorts (P = and P < 0.001, respectively). Invasive disease and axillary dissections were statistically more prevalent in the cohorts who underwent PMRT than in those who did not. Nipple-sparing mastectomies were statistically more prevalent within the ADM without PMRT cohort (8.8%, P < ). Reconstructions completed with ADM had higher initial TE fill volumes than did those in the non- ADM groups, despite having similar preoperative bra volumes (258 cc versus 152 cc, respectively, P < 0.001)
4 4 Aesthetic Surgery Journal Figure 1. Postoperative complication rates between ADM and total muscle coverage (TMC) compared by timing of radiation therapy. Note that complication differences between ADM and TMC are mainly isolated to the early postoperative phase and more approximate in the long term. Table 4. Explantation Reasons for Explantation Total Non-Radiated Radiated P value N (%) Non-ADM ADM Non-ADM ADM N = 119 N = 40 N = 46 N = 23 N = 10 Complication reason 101 (85%) 32 (80%) 45 (98%) 15 (65%) 9 (90%) 0.29 Necrosis 37 (30.9%) 11 (28%) 17 (37%) 6 (26%) 3 (30%) Infection 57 (46.0%) 19 (48%) 25 (54%) 9 (39%) 4 (40%) Hematoma 2 (1.6%) 2 (5%) 0 (0%) 0 (0%) 0 (0%) Over inflation 5 (4%) 0 (0%) 3 (6%) 0 (0%) 2 (20%) Non-complication reason 18 (15%) 8 (20%) 1 (2%) 8 (35%) 1 (12%) NA Causes of explantation. The table is broken down into explantation due to a complication such as hematoma, etc. or, non-complication reasons such as pain, medical therapy, or patient choice Complications Overall complication rate refers to all measured outcomes with the exception of explantation, which we considered a reconstructive failure and, therefore, reported separately. The incidence of complications (MSFN, infection, hematoma/seroma, dehiscence, and explantation) was reviewed within the cohorts and overall population (Table 3 and Figure 1). When analyzing the cohorts, data for 6 breasts had to be excluded from the radiated-adm cohort due to incomplete radiation treatment data. MSFN was the most common type of complication (Table 3). Higher preoperative bra volume, nipple-sparing mastectomy, PMRT, and the use of ADM were independent risk factors for necrosis. Active smoking was surprisingly not found to be an independent risk factor, but this was 420
5 Craig et al AQ Table 5. Multivariate Overall Complications Characteristics Smoking OR (95% CI) Multivariable GEE model P value Never Ref. - Active 1.72 ( ) Previous 1.30 ( ) 0.18 ADM 3.05 ( ) < PMRT 1.76 ( ) Number of cases done before this surgery <50 Ref. - >= ( ) Multivariate analysis of all demographic variables as indepdnent predictors of overall complications. likely due to insufficient power, as only 6% of our patient population were active smokers. The overall infection rate was 7.8%. Multivariate analysis identified higher bra volume, higher initial expander fill volume, PMRT, and the use of ADM as significant risk factors for infection. For every increase of 100 cc in the initial expander fill volume, the risk of infection increased by 2%. Patients who underwent PMRT were 2 times more likely to have an infection than those who did not. Overall, ADM was associated with an increased risk of infection compared with no ADM [odds ratio (OR) = 1.93, P = 0.01]. Among the patients who did not receive PMRT, the use of ADM increased the chance of having an infection 2 and a half times (OR = 2.48, P = 0.002). For patients reconstructed without ADM, the effect of PMRT alone increased their chance of infection 3 and a half times (Table 4). In contrast, PMRT appeared to have no significant impact on infection rate in patients reconstructed with ADM (P = 0.60). Only 33% of the patients who developed infections had a history of seroma; conversely, 9% had infections prior to being diagnosed with a seroma, but the majority of infections appeared to occur de novo. Seven percent of the patients, overall, developed seromas. Patients reconstructed with ADM who received PMRT had the highest incidence of seroma, at 13.6%, followed by the cohort of patients with ADM but without PMRT at 10.9%. The use of ADM was found to be an independent risk factor for seroma formation (along with higher bra volume), and increased the chance of seroma by threefold (P < ). Smoking, PMRT, and initial expander fill volume were not contributing factors for incidence of seroma. Explantation occurred in 119 patients or 8.6% of the cohort overall. Age, BMI, PMRT, bra volume, intraoperative TE fill volume, nipple-sparing mastectomy, axillary dissection, and invasive disease were significant risk factors for explantation in the univariate analysis. Neither ADM nor PMRT were found to be independent risk factors for explantation overall. However, for patients who underwent PMRT, ADM was associated with fewer explantations and lower odds of explantation when compared with non-adm patients (OR = 0.38, P = 0.04). In fact, the highest rate of explantation occurred in the non-adm with PMRT cohort (20.4%, P = ). Within the non-adm group, PMRT increased the odds of explantation threefold (OR = 3.19, P = 0.002). The main reason for explantation overall was infection (both overall and among cohorts), which occurred in 46% of the explantations, followed by mastectomy skin necrosis, which occurred in 30.9%. Reasons for explantation other than complications comprised only 15% of all explantations and included pain, unsatisfactory aesthetic outcome, TE rupture, and need for/interference with further treatment (Table 4). Multivariate analysis was performed to evaluate the role of preoperative variables in contributing to complications, and identified older age, higher bra volume, smoking, PMRT, and the use of ADM as independent risk factors for overall complication rate (Table 5). Notably, neither the use of either neoadjuvant or adjuvant chemotherapy, nor initial fill was associated with increased overall complication or explantation rates. While controlling for these factors and others, including preoperative bra volume, type of mastectomy, BMI, and smoking status, we were able to note several relationships among ADM, radiation, and the occurrence of complications (Table 6). The timing of these complications occurring did not differ significantly between the ADM/non-ADM and PMRT/ non-pmrt groups. The only differences that were identified were that radiated TEs were explanted much later than non-irradiated TEs (median days vs 56.0 days; P value 0.02) and the timing of seromas (15.0 vs 29.0 days, P value 0.001); mastectomy skin flap necrosis (15.0 vs 10.0 days, P value 0.01) was different between the ADM and non-adm groups, although these differences are not clinically significant. There was no difference in radiated groups in terms of the timing of infection, seroma, or necrosis, or differences between the ADM groups in terms of timing of explantation or seroma occurrence. DISCUSSION While the literature is replete with data regarding the risks and benefits of ADM in ITE reconstructions, we performed the largest retrospective cohort study specifically aimed at assessing the impact of ADM in the setting of PMRT. As expected, the overall complication rate, as well as the incidence of infection and seroma, appeared to be higher in patients undergoing ITE with ADM; however, there were AQ
6 6 Aesthetic Surgery Journal Table 6. Multivariate Everything 535 Non-Radiated Irradiated Non-ADM ADM Non-ADM ADM Irradiated vs Non-Irradiated ADM Non-ADM Radiated vs ADM Radiated Overall complication Ref 3.16 ( ) 1.95 ( ) 4.61 ( ) OR = 1.52 ( ) OR = 2.36 ( ) 540 P < P = P < P = 0.10 P = Dehiscence Ref 2.46 ( ) 1.07 ( ) 2.26 ( ) Infection Ref 2.68 ( ) 3.23 ( ) 3.67 ( ) P = 0.01 P = 0.91 P = P = P = P = P = P = 0.60 P = 0.77 Necrosis Ref 4.99 ( ) 2.76 ( ) 4.01 ( ) P =< P = P < P = 0.48 P = Seroma Ref 3.19 ( ) 1.59 ( ) 4.17 ( ) P < P = P = P = 0.57 P = 0.08 Explantation Ref 1.90 ( ) 3.19 ( ) 1.22 ( ) OR = 0.64 ( ) OR = 0.38 ( ) P = 0.04 P = P = 0.69 P = 0.34 P = Multivariate analysis examining the role of ADM and radiation on overall complications, dehiscence, infection, necrosis, seroma, and explantation. Odds ratios (OR) were not performed if statistical significance was not present. The non-adm and non-radiated cohort was used as a point of reference for OR determinations. OR reported as OR (95% CI) fewer expander failures in the PMRT who utilized ADM. In fact, the use of ADM appeared to play a protective role in preventing re-operation and explantation in patients undergoing PMRT (Figure 2). The overall complication rate of 26% in our study is slightly higher than that reported in the literature; however, this is likely due to the significantly larger sample of irradiated patients, a known risk factor for negative outcomes. 22,23 Similar to previous reports, we found a higher complication rate in the ADM cohort than in the non-adm cohort. In addition to age, BMI, PMRT, and smoking, risk factors previously reported in the literature, bra volume was found to be an independent risk factor for complications. While both BMI and bra volume were found to be significant variables in the univariate analysis, only bra volume was found to be significant in the multivariate analysis. Bra volume may, therefore, be a more specific indicator for breast-related outcomes, as a large BMI does not always correspond with large breast size. 5,24 The MSFN rate in both ADM and non-adm patients is greater than that reported in the literature. 10,22,23 However, it should be noted that for a given bra volume, both ADM cohorts (irradiated and non-irradiated) had intraoperative fill volumes that were 100 cc higher on average than those of the non-adm cohorts. While ADM allows for a greater intraoperative fill volume, this advantage can place additional pressure on thin, ischemic flaps, contributing to higher rates of MSFN. Judicious clinical assessment of skin viability, and perhaps the use of SPY can offer additional assistance in determining tissue tolerance to fill volumes. PMRT was also found to be a significant risk factor for MSFN, and this may be secondary to more aggressive mastectomies being performed in the setting of advanced disease (as indicated by the need for PMRT). Other contributing risk factors to mastectomy skin necrosis bra volume and the nipple-sparing technique are fixed variables and should therefore be included in preoperative discussions with the patients. Both PMRT and ADM were found to be significant risk factors for infections; however, other factors may have either over- or underreported the true incidence of infection. It should be noted that we have a red breast clinic at our institution where patients with suspected infections undergo immediate ultrasonographic evaluation, an infectious disease consult, and drainage of any fluid collection by interventional radiology as part of a standard protocol. Our approach to diagnosing and treating cellulitis with intravenous antibiotics likely differs from that of other practices and might lead to the overestimation of the true incidence of infection, particularly in our ADM patients. However, given that infection is the leading cause of explantation, it is possible that our aggressive approach might also increase our ability to salvage reconstructions. Explantations occurred in 8.6% of our patient population, the majority of which was in irradiated patients treated without ADM. Radiation is a known risk factor for AQ3
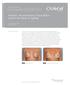
7 Craig et al 7 A B C D Figure 2. Example of prosthetic reconstruction of the radiated breast with acellular dermal matrix. Patient is a 41-year-old female who required bilateral skin-sparing mastectomy and tissue expander reconstruction with ADM as a pectoralis major extension for soft tissue support. (A, B, C) Appearance of skin 6 months following 3D conformal 50 gy external beam radiation therapy with incision and internal mammary boost. Patient received device exchange and one round of autologous fat grafting. (D) Appearance of incisions (E) at 1 month of the right non-radiated breast (F) and slower healing of the left radiated breast. Implant choice was a shaped gel extra projection 650 ml implant on the right breast and a 700 ml implant on the left breast. Postoperative course was uncomplicated with no further revisions, (G, H, I) appearance at 2 years postoperatively and (J) by 3D surface imaging (taken with 3dMD LLC Camera Systems, Atlanta, GA). 690
8 8 Aesthetic Surgery Journal 695 E F G H Figure 2. Continued 745 infection, but its impact on ADM is relatively unknown. 23 The effect of radiation on patients reconstructed without ADM was profound, increasing the infection rate 3 times. Similarly, the explantation rate of patients reconstructed without ADM who underwent PMRT was 3 times higher than that of non-adm patients who did not undergo PMRT (20.4% vs 5.9%, respectively). In contrast, patients reconstructed with ADM experienced no difference in infection or seroma rate in response to radiation. Radiation therapy is a known risk factor for complications in non-adm 800
9 Craig et al 9 I J Figure 2. Continued reconstructions; however, studies are just beginning to report the effects of radiation on ADM reconstructions. An evidence-based review performed by Clemens and Kronowitz suggests a potentially protective effect of ADM in the setting of PMRT, with decreased cellular infiltrates and decreased capsular contracture rates. 6,15,19,21,25,27 32 Seth et al published a case-control series in 2012 with 592 ITE reconstructions and found no significant increase in complication rate following PMRT in patients reconstructed with ADM. 33 This is in contrast to the observed threefold increase in complication rate experienced by the non-adm group following PMRT (P = 0.003). Unfortunately, a contrast analysis was not performed between the irradiated ADM and non-adm groups to evaluate how ADM reconstructions behave with respect to traditional techniques in the setting of radiation. In addition, the ADM and non- ADM cohorts had varying demographic profiles that may have confounded their outcomes. While this study lends support to previously reported data, questions still remain regarding the true impact of PMRT on ADM in breast reconstruction, how this compares to traditional techniques, and how this influences patient selection criteria. Our data support the conclusions by other authors that ADM plays a protective role in irradiated patients by limiting explantation. 23,26 Among these, our study is the largest study to date using cohort comparisons to illustrate the impact of ADM on patients undergoing PMRT We theorize that ADM has a higher infection and seroma rate prior to its incorporation. Use of antibiotics, aggressive treatment of red breasts, and prolonged use of drains are imperative for promoting incorporation. Once incorporated, the ADM may serve as an additional vascularized layer over the TE, protecting it from bacterial contamination. Patients without ADM do not experience an incorporation period, and therefore have initially lower infection and seroma rates. However, in the setting of radiation, non-adm patients do not have the advantage of an additional vascularized ADM layer and are thus more susceptible to bacterial contamination, leading to higher explantation rates. In 2012, Nahabedian published the following indications for ADM: women with A to D cup size breasts, regardless of age, who are not morbidly obese, have not had prior radiation, and are not active smokers. 14 Similarly, Ganske et al described changes in their patient selection criteria and postoperative management that played a critical role in the success of their implant-based reconstructions with ADM. 4 Intraoperative tailoring of the ADM to eliminate folding and dead space, aggressive mastectomy skin flap excision and debridement, and more conservative drain removal thresholds successfully decreased their complication rates to those equivalent to their non-adm reconstructions. 12 We recognize that our study has limitations. This is a retrospective review and is subject to type II error. Capsular contracture rates were not included in our study or data collection because it was reported in a subjective and inconsistent manner. Our incidence of PMRT may be low compared to other studies; however, this may in part be explained by the relatively high incidence of prophylactic
10 10 Aesthetic Surgery Journal mastectomies (31.4%). In addition, the non-adm group comprised both partial and total muscle coverage. One could argue that partial muscle coverage places patients at greater risk for bacterial contamination and explantation as compared to total muscle coverage. However, only a few patients had partial muscle coverage and are believed to not have significantly impacted this group as a whole. In addition, there was some variability in the timing of drain removal and duration of antibiotics in our group practice that could potentially impact seroma and infection rates, although with 1367 reconstructions, we believe these small differences were likely inconsequential. Patients who completed PMRT at outside institutions were included in this study, allowing some variability in radiation dosing treatments. Again, the majority of patients received their treatment at our institution, making any patients treated outside the institution negligible in such a large cohort. CONCLUSIONS The key to success in breast reconstruction is patient selection and patient education. With the introduction of ADM, we now have another tool to consider and evaluate its utility in each patient. The data presented in the current study can be used to further guide patient selection, and educate patients about their risk profile for complications when using ADM. The decision to use ADM for expander-based breast reconstruction should be performed with caution, given higher overall rates of complications, including infections and seromas. There may, however, be a role for ADM in cases requiring PMRT, as the overall incidence of implant failure is lower than non-adm cases. The choice to use ADM should be individualized, with particular attention paid to the risk factors presented in our study. Disclosures Dr Patrick Garvey was a consultant for LifeCell Corporation. Dr Jesse Selber was a consultant for TEI Biosciences and Mentor Worldwide. The other authors declared no potential conflicts of interest with respect to the research, authorship, and publication of this article. Funding The authors received no financial support for the research, authorship, and publication of this article. REFERENCES 1. American Society of Plastic Surgeons Plastic Surgery Statistics Report. American Society of Plastic Surgeons website, News/Statistics/2016/2016-plastic-surgery-statisticsreport.pdf. Accessed September 1, Antony AK, McCarthy CM, Cordeiro PG, et al. Acellular human dermis implantation in 153 immediate two-stage tissue expander breast reconstructions: determining the incidence and significant predictors of complications. Plast Reconstr Surg. 2010;125(6): Basu CB, Leong M, Hicks MJ. Acellular cadaveric dermis decreases the inflammatory response in capsule formation in reconstructive breast surgery. Plast Reconstr Surg. 2010;126(6): Berry T, Brooks S, Sydow N, et al. Complication rates of radiation on tissue expander and autologous tissue breast reconstruction. Ann Surg Oncol. 2010;17: Brooks S, Djohan R, Tendulkar R, Nutter B, Lyons J, Dietz J. Risk factors for complications of radiation therapy on tissue expander breast reconstructions. Breast J. 2012;18(1): Chun YS, Verma K, Rosen H, et al. Implant-based breast reconstruction using acellular dermal matrix and the risk of postoperative complications. Plast Reconstr Surg. 2010;125(2): Clemens MW, Kronowitz SJ. Acellular dermal matrix in irradiated tissue expander/implant-based breast reconstruction: evidence-based review. Plast Reconstr Surg. 2012;130(5):27S-34S. 8. Colwell AS, Tessler O, Lin AM, et al. Breast reconstruction following nipple-sparing mastectomy: predictors of complications, reconstruction outcomes, and 5-year trends. Plast Reconstr Surg. 2014;133(3): Cordeiro PG, Snell L, Heerdt A, McCarthy C. Immediate tissue expander/implant breast reconstruction after salvage mastectomy for cancer recurrence following lumpectomy/ irradiation. Plast Resconstr Surg. 2010;129(2): Cowen D, Gross E, Rouannet P, et al. Immediate post-mastectomy breast reconstruction followed by radiotherapy: risk factors for complications. Breast Cancer Res Treat. 2010;121(3): Forsberg CG, Kelly DA, Wood BC, et al. Aesthetic outcomes of acellular dermal matrix in tissue expander/ implant-based breast reconstruction. Ann Plast Surg. 2014;72(6):S116-S Ganske I, Verma K, Rosen H, Eriksson E, Chun YS. Minimizing complications with the use of acellular dermal matrix for immediate implant-based breast reconstruction. Ann Plast Surg. 2013;71(5): Glasberg SB, Light D. AlloDerm and Strattice in breast reconstruction: a comparison and techniques for optimizing outcomes. Plast Reconstr Surg. 2012;129(6): Gurunluoglu R, Gurunluoglu A, Williams SA, Tebockhorst S. Current trends in breast reconstruction: survey of American Society of Plastic Surgeons Ann Plast Surg. 2013;70(1): Hanna KR, DeGeorge BR Jr, Mericli AF, Lin KY, Drake DB. Comparison study of two types of expander-based breast reconstruction. Ann Plast Surg. 2013;70(1): Ho A, Cordeiro P, Disa J, et al. Long-term outcomes in breast cancer patients undergoing immediate 2-stage expander/implant reconstruction and postmastectomy radiation. Cancer. 2012;118(9): Ho G, Nguyen TJ, Shahabi A, Hwang BH, Chan LS, Wong AK. A systematic review and meta-analysis of complications associated with acellular dermal matrix-assisted breast reconstruction. Ann Plast Surg. 2012;68(4): AQ
11 Craig et al Hubenak JR, Zhang Q, Branch CD, Kronowitz SJ. Mechanisms of injury to normal tissue after radiotherapy: a review. Plast Reconstr Surg. 2014;133(1):49e-56e. 19. Israeli Ro, Feingold R. Acellular dermal matrix in breast reconstruction in the setting of radiotherapy. Aesthet Surg J. 2011;31(7S):51S-64S. 20. Jhaveri JD, Rush SC, Kostroff K, et al. Clinical outcomes of postmastectomy radiation therapy after immediate breast reconstruction. Int J Radiat Oncol Biol Phys. 2008;72(3): Kim JY, Davila AA, Persing S, et al. A meta-analysis of human acellular dermis and submuscular tissue expander breast reconstruction. Plast Reconstr Surg. 2012;129(1): Komorowska-Timek E, Oberg KC, Timek TA, Gridley DS, Miles DA. The effect of AlloDerm envelopes on periprosthetic capsule formation with and without radiation. Plast Reconstr Surg. 2009;123(3): Kronowitz SJ. Current status of implant-based breast reconstruction in patients receiving postmastectomy radiation therapy. Plast Reconstr Surg. 2012;130(4):513e-523e. 24. Kronowitz SJ, Hunt KK, Kuerer HM, et al. Delayedimmediate breast reconstruction. Plast Reconstr Surg. 2004;113(6): McCarthy CM, Lee CN, Halvorson EG, et al. The use of acellular dermal matrices in two-stage expander/implant reconstruction: a multicenter, blinded, randomized controlled trial. Plast Reconstr Surg. 2012;130(5):57S-66S. 26. Lam TC, Hsieh F, Boyages J. The effects of postmastectomy adjuvant radiotherapy on immediate two-stage prosthetic breast reconstruction: a systematic review. Plast Reconstr Surg. 2013;132(3): Moyer HR, Pinell-White X, Losken A. The effect of radiation on acellular dermal matrix and capsule formation in breast reconstruction: clinical outcomes and histologic analysis. Plast Reconstr Surg. 2014;133(2): Nahabedian MY. Acellular dermal matrices in primary breast reconstruction: principles, concepts, and indications. Plast Reconstr Surg. 2012;130(5S-2):44S-53S. 29. Nahabedian MY. AlloDerm performance in the setting of prosthetic breast surgery, infection, and irradiation. Plast Reconstr Surg. 2009;124(6): Parks JW, Hammond SE, Walsh WA, Adams RL, Chandler RG, Luce EA. Human acellular dermis versus no acellular dermis in tissue expansion breast reconstruction. Plast Reconstr Surg. 2012;130(4): Rawlani V, Buck DW 2nd, Johnson SA, Heyer KS, Kim JY. Tissue expander breast reconstruction using prehydrated human acellular dermis. Ann Plast Surg. 2011;66(6): Sbitany H, Sandeen SN, Amalfi AN, Davenport MS, Langstein HN. Acellular dermis-assisted prosthetic breast reconstruction versus complete submuscular coverage: a head-to-head comparison of outcomes. Plast Reconstr Surg. 2009;124(6): Seth AK, Hirsch EM, Fine NA, Kim JY. Utility of acellular dermis-assisted breast reconstruction in the setting of radiation: a comparative analysis. Plast Reconstr Surg. 2012;130(4): Spear SL, Parikh PM, Reisin E, Menon NG. Acellular dermis-assisted breast reconstruction. Aesthetic Plast Surg. 2008;32(3): Spear SL, Seruya M, Rao SS, et al. Two-stage prosthetic breast reconstruction using AlloDerm including outcomes of different timings of radiotherapy. Plast Reconstr Surg. 2012;130(1): Vardanian AJ, Clayton JL, Roostaeian J, et al. Comparison of implant-based immediate breast reconstruction with and without acellular dermal matrix. Plast Reconstr Surg. 2011;128(5):403e-410e. 37. Weichman KE, Wilson SC, Weinstein AL, et al. The use of acellular dermal matrix in immediate two-stage tissue expander breast reconstruction. Plast Reconstr Surg. 2012;129(5): Zienowicz RJ, Karacaoglu E. Implant-based breast reconstruction with allograft. Plast Reconstr Surg. 2007;120(2):
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm
 Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm Minh-Doan Nguyen, MD, PhD, a Chen Chen, MS, b Salih Colakoğlu, MD, b Donald J. Morris, MD, b Adam M.
Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm Minh-Doan Nguyen, MD, PhD, a Chen Chen, MS, b Salih Colakoğlu, MD, b Donald J. Morris, MD, b Adam M.
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION
 NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
Radiation Therapy And Expander-Implant Breast Reconstruction: Analysis Of Timing And Complications
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2013 Radiation Therapy And Expander-Implant Breast Reconstruction:
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2013 Radiation Therapy And Expander-Implant Breast Reconstruction:
Prepectoral breast reconstruction and radiotherapy a closer look
 Original Article Prepectoral breast reconstruction and radiotherapy a closer look Steven Sigalove Scottsdale Center for Plastic Surgery, Scottsdale, AZ, USA Correspondence to: Steven Sigalove, MD, FACS.
Original Article Prepectoral breast reconstruction and radiotherapy a closer look Steven Sigalove Scottsdale Center for Plastic Surgery, Scottsdale, AZ, USA Correspondence to: Steven Sigalove, MD, FACS.
Allograft Based Breast Reconstruction: Opportunity for a Second Look
 Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position
 Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Acellular Dermal Matrix in Primary Breast Reconstruction
 Supplemental Article Acellular Dermal Matrix in Primary Breast Reconstruction Hani Sbitany, MD; and Howard N. Langstein, MD Traditional implant-based breast reconstruction is relatively simple to perform
Supplemental Article Acellular Dermal Matrix in Primary Breast Reconstruction Hani Sbitany, MD; and Howard N. Langstein, MD Traditional implant-based breast reconstruction is relatively simple to perform
The Effect of Acellular Dermal Matrix in Implant-Based Immediate Breast Reconstruction with Latissimus Dorsi Flap
 ORIGINAL ARTICLE https://doi.org/10.14730/.2017.23.1.17 Arch Aesthetic Plast Surg 2017;23(1):17-23 pissn: 2234-0831 eissn: 2288-9337 The Effect Acellular Dermal Matrix in Implant-Based Immediate Breast
ORIGINAL ARTICLE https://doi.org/10.14730/.2017.23.1.17 Arch Aesthetic Plast Surg 2017;23(1):17-23 pissn: 2234-0831 eissn: 2288-9337 The Effect Acellular Dermal Matrix in Implant-Based Immediate Breast
Current perspectives on radiation therapy in autologous and prosthetic breast reconstruction
 Review Article Current perspectives on radiation therapy in autologous and prosthetic breast reconstruction Mark W. Clemens, Steven J. Kronowitz Department of Plastic Surgery, The University of Texas M.D.
Review Article Current perspectives on radiation therapy in autologous and prosthetic breast reconstruction Mark W. Clemens, Steven J. Kronowitz Department of Plastic Surgery, The University of Texas M.D.
The picture can't be displayed. None. The picture can't be displayed. The picture can't be displayed. Overall N= 564
 Predictors and Timing for Successful Radiated Breast Reconstruction Mark W. Clemens, MD FACS Associate Professor MD Anderson Cancer Center None Disclosure Kaiser Permanente 2018 Plastic Surgery Symposium
Predictors and Timing for Successful Radiated Breast Reconstruction Mark W. Clemens, MD FACS Associate Professor MD Anderson Cancer Center None Disclosure Kaiser Permanente 2018 Plastic Surgery Symposium
Acellular Dermal Matrix in Reconstructive Breast Surgery: Survey of Current Practice among Plastic Surgeons
 Acellular Dermal Matrix in Reconstructive Breast Surgery: Survey of Current Practice among Plastic Surgeons The Harvard community has made this article openly available. Please share how this access benefits
Acellular Dermal Matrix in Reconstructive Breast Surgery: Survey of Current Practice among Plastic Surgeons The Harvard community has made this article openly available. Please share how this access benefits
MASTECTOMY AND IMMEDIATE BREAST RECONSTRUCTION IN INVASIVE CARCINOMA
 MASTECTOMY AND IMMEDIATE BREAST RECONSTRUCTION IN INVASIVE CARCINOMA Node-postive breast cancer Delayed-immediate reconstruction versus delayed reconstruction DBCG RT Recon-Protocol Tine Engberg Damsgaard
MASTECTOMY AND IMMEDIATE BREAST RECONSTRUCTION IN INVASIVE CARCINOMA Node-postive breast cancer Delayed-immediate reconstruction versus delayed reconstruction DBCG RT Recon-Protocol Tine Engberg Damsgaard
A Comparative Study of CG CryoDerm and AlloDerm in Direct-to-Implant Immediate Breast Reconstruction
 A Comparative Study of CG CryoDerm and AlloDerm in Direct-to-Implant Immediate Breast Reconstruction Original Article Jun Ho Lee 1, Ki Rin Park 1, Tae Gon Kim 1, Ju-Ho Ha 1, Kyu-Jin Chung 1, Yong-Ha Kim
A Comparative Study of CG CryoDerm and AlloDerm in Direct-to-Implant Immediate Breast Reconstruction Original Article Jun Ho Lee 1, Ki Rin Park 1, Tae Gon Kim 1, Ju-Ho Ha 1, Kyu-Jin Chung 1, Yong-Ha Kim
Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts
 Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Breast Surgery Reduction Mammaplasty and Mastopexy in Previously Irradiated Breasts Scott L. Spear, MD; Samir S. Rao, MD; Ketan M. Patel, MD; and Maurice Y. Nahabedian, MD The combination of lumpectomy
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER
 BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: September 2013 The recommendations contained in this guideline are a consensus of the Alberta Provincial
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: September 2013 The recommendations contained in this guideline are a consensus of the Alberta Provincial
Clinically significant capsular contracture is BREAST
 BREAST Acellular Dermal Matrix Assisted Direct-to-Implant Breast Reconstruction and Capsular Contracture: A 13-Year Experience C. Andrew Salzberg, M.D. Andrew Y. Ashikari, M.D. Colleen Berry, A.R.N.P.,
BREAST Acellular Dermal Matrix Assisted Direct-to-Implant Breast Reconstruction and Capsular Contracture: A 13-Year Experience C. Andrew Salzberg, M.D. Andrew Y. Ashikari, M.D. Colleen Berry, A.R.N.P.,
The Case FOR Oncoplastic Surgery in Small Breasts. Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA
 The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
AN AUDIT OF ACELLULAR DERMAL MATRIX (ADM) ASSISTED BREAST RECONSTRUCTION PROCEDURES ARE ANTIBIOTICS UNAVOIDABLE?
 Journal Of Harmonized Research (JOHR) Journal Of Harmonized Research in Medical & Health Sci. 4(1), 2017, 12-16 ISSN 2395 6046 Original Research Article AN AUDIT OF ACELLULAR DERMAL MATRIX (ADM) ASSISTED
Journal Of Harmonized Research (JOHR) Journal Of Harmonized Research in Medical & Health Sci. 4(1), 2017, 12-16 ISSN 2395 6046 Original Research Article AN AUDIT OF ACELLULAR DERMAL MATRIX (ADM) ASSISTED
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
The use of postmastectomy radiation therapy (PMRT) to prevent
 NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Oncoplastic and Reconstructive Surgery
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons
 Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
San Antonio Breast Cancer Symposium 2010: Highlights from a Surgical Perspective. Disclosures
 San Antonio Breast Cancer Symposium 2010: Highlights from a Surgical Perspective January 18, 2011 Association of Northern California Oncologists Steven Chen, MD, MBA Chief, Breast Surgery University of
San Antonio Breast Cancer Symposium 2010: Highlights from a Surgical Perspective January 18, 2011 Association of Northern California Oncologists Steven Chen, MD, MBA Chief, Breast Surgery University of
Two-stage prepectoral breast reconstruction
 Original Article Two-stage prepectoral breast reconstruction Maurice Y. Nahabedian 1, Steven R. Jacobson 2 1 National Center for Plastic Surgery, McLean, VA, USA; 2 Jacobson Plastic Surgery, Rochester,
Original Article Two-stage prepectoral breast reconstruction Maurice Y. Nahabedian 1, Steven R. Jacobson 2 1 National Center for Plastic Surgery, McLean, VA, USA; 2 Jacobson Plastic Surgery, Rochester,
PROS AND CONS OF IMMEDIATE PROSTHETIC IMPLANTS VS USE OF EXPANDER FOR POST MASTECTOMY BREAST RECONSTRUCTIONS
 PROS AND CONS OF IMMEDIATE PROSTHETIC IMPLANTS VS USE OF EXPANDER FOR POST MASTECTOMY BREAST Dr Tienie van Rooyen Mediclinic Kloof Hospital Pretoria IMMEDIATE Since 1990 s Skin sparing mastectomies proven
PROS AND CONS OF IMMEDIATE PROSTHETIC IMPLANTS VS USE OF EXPANDER FOR POST MASTECTOMY BREAST Dr Tienie van Rooyen Mediclinic Kloof Hospital Pretoria IMMEDIATE Since 1990 s Skin sparing mastectomies proven
Nipple-Sparing Mastectomy via an Inframammary Fold Incision with Implant- Based Reconstruction in Patients with Prior Cosmetic Breast Surgery
 Breast Surgery Nipple-Sparing Mastectomy via an Inframammary Fold Incision with Implant- Based Reconstruction in Patients with Prior Cosmetic Breast Surgery Aesthetic Surgery Journal 2015, Vol 35(5) 548
Breast Surgery Nipple-Sparing Mastectomy via an Inframammary Fold Incision with Implant- Based Reconstruction in Patients with Prior Cosmetic Breast Surgery Aesthetic Surgery Journal 2015, Vol 35(5) 548
Pre-pectoral Breast Reconstruction in Nipple Sparing Mastectomy
 September 2017 Issue 9 Pre-pectoral Breast Reconstruction in Nipple Sparing Mastectomy Aldona J. Spiegel, MD Director and Founder of the Center for Breast Restoration at the Institute for Reconstructive
September 2017 Issue 9 Pre-pectoral Breast Reconstruction in Nipple Sparing Mastectomy Aldona J. Spiegel, MD Director and Founder of the Center for Breast Restoration at the Institute for Reconstructive
Tissue Reinforcement in Implant-based Breast Reconstruction
 Tissue Reinforcement in Implant-based Breast Reconstruction The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published
Tissue Reinforcement in Implant-based Breast Reconstruction The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published
A short-term follow-up of implant based breast reconstruction using a titanium-coated polypropylene mesh (TiLoop Ò Bra)
 Available online at www.sciencedirect.com EJSO xx (2012) 1e6 www.ejso.com A short-term follow-up of implant based breast reconstruction using a titanium-coated polypropylene mesh (TiLoop Ò Bra) M. Dieterich
Available online at www.sciencedirect.com EJSO xx (2012) 1e6 www.ejso.com A short-term follow-up of implant based breast reconstruction using a titanium-coated polypropylene mesh (TiLoop Ò Bra) M. Dieterich
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy. Zhang Jin, Ph.D MD
 How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
MAASTRO- CLINIC More than just an institute for radiotherapy Patientcare research training & education
 MAASTRO- CLINIC More than just an institute for radiotherapy Patientcare research training & education Breast reconstruction: Before or after post mastectomy radiotherapy? Prof. dr. Liesbeth Boersma May
MAASTRO- CLINIC More than just an institute for radiotherapy Patientcare research training & education Breast reconstruction: Before or after post mastectomy radiotherapy? Prof. dr. Liesbeth Boersma May
Current perspectives on radiation therapy in autologous and prosthetic breast. Won Park, M.D. Department of Radiation Oncology Samsung Medical Center
 Current perspectives on radiation therapy in autologous and prosthetic breast Won Park, M.D. Department of Radiation Oncology Samsung Medical Center DBCG 82 b & c Overgaard et al Radiot Oncol 2007 1152
Current perspectives on radiation therapy in autologous and prosthetic breast Won Park, M.D. Department of Radiation Oncology Samsung Medical Center DBCG 82 b & c Overgaard et al Radiot Oncol 2007 1152
Capsular Contracture Rate in a Low-Risk Population After Primary Augmentation Mammaplasty
 Capsular Contracture Rate in a Low-Risk Population After Primary Augmentation Mammaplasty Andrew L. Blount, Matthew D. Martin, Kyle D. Lineberry, Nicolas Kettaneh, David R. Alfonso Breast Surgery Capsular
Capsular Contracture Rate in a Low-Risk Population After Primary Augmentation Mammaplasty Andrew L. Blount, Matthew D. Martin, Kyle D. Lineberry, Nicolas Kettaneh, David R. Alfonso Breast Surgery Capsular
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation. Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS
 Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
As the prevalence of breast cancer has increased. Breast. Is Sterile Better Than Aseptic? Comparing the Microbiology of Acellular Dermal Matrices
 Original Article Breast Is Sterile Better Than Aseptic? Comparing the Microbiology of Acellular Dermal Matrices Gabriel M. Klein, MD* Ahmed E. Nasser, MD* Brett T. Phillips, MD, MBA Robert P. Gersch, PhD
Original Article Breast Is Sterile Better Than Aseptic? Comparing the Microbiology of Acellular Dermal Matrices Gabriel M. Klein, MD* Ahmed E. Nasser, MD* Brett T. Phillips, MD, MBA Robert P. Gersch, PhD
Prophylactic Mastectomy & Reconstructive Implications
 Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
SINGLE-STAGE BREAST RECONSTRUCTION WITH WISE PATTERN AND INFERIOR AUTODERM FLAP FOR MAMMARY HYPERTROPHY
 Volume 4 Number 1 PLSTI SURGRY Pulse News 35 SINGL-STG RST RONSTRUTION WITH WIS PTTRN N INRIOR UTORM LP OR MMMRY HYPRTROPHY Jaime S. Schwartz, M reast reconstruction with prosthetic devices has become
Volume 4 Number 1 PLSTI SURGRY Pulse News 35 SINGL-STG RST RONSTRUTION WITH WIS PTTRN N INRIOR UTORM LP OR MMMRY HYPRTROPHY Jaime S. Schwartz, M reast reconstruction with prosthetic devices has become
Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review
 Research Article http://www.alliedacademies.org/advanced-surgical-research/ Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review Gurnam Virdi* Department of surgery, Queen Elizabeth
Research Article http://www.alliedacademies.org/advanced-surgical-research/ Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review Gurnam Virdi* Department of surgery, Queen Elizabeth
The success of breast conservation protocols BREAST. Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy
 BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
Breast Reconstruction in Women Under 30: A 10-Year Experience
 ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
Plastic Reconstructive Aspects after Mastectomy
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Plastic Reconstructive Aspects after Mastectomy Plastic Reconstructive Aspects after Mastectomy Version 2002: Brunnert Version
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Plastic Reconstructive Aspects after Mastectomy Plastic Reconstructive Aspects after Mastectomy Version 2002: Brunnert Version
Tackling challenging revision breast augmentation cases
 the BREAST Careful preoperative consultations can reduce the need for revision breast surgery. Second Time Around Tackling challenging revision breast augmentation cases By Adam D. Schaffner, MD, FACS
the BREAST Careful preoperative consultations can reduce the need for revision breast surgery. Second Time Around Tackling challenging revision breast augmentation cases By Adam D. Schaffner, MD, FACS
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks
 Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft
 Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
Skin sparing mastectomy: Technique and suggested methods of reconstruction
 Journal of the Egyptian National Cancer Institute (2014) 26, 153 159 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Skin
Journal of the Egyptian National Cancer Institute (2014) 26, 153 159 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Skin
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni
 SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
The biplanar oncoplastic technique case series: a 2-year review
 Original Article The biplanar oncoplastic technique case series: a 2-year review Alexander J. Kaminsky 1, Ketan M. Patel 2, Costanza Cocilovo 1, Maurice Y. Nahabedian 2, Reza Miraliakbari 3 1 INOVA Fairfax
Original Article The biplanar oncoplastic technique case series: a 2-year review Alexander J. Kaminsky 1, Ketan M. Patel 2, Costanza Cocilovo 1, Maurice Y. Nahabedian 2, Reza Miraliakbari 3 1 INOVA Fairfax
complicanze in chirurgia senologica ricostruttiva Tecniche per la prevenzione delle complicanze nelle mastectomie conservative
 Il trattamento delle complicanze in chirurgia senologica ricostruttiva Tecniche per la prevenzione delle complicanze nelle mastectomie conservative Dr. Christian Rizzetto UOC Chirurgia Senologica - Breast
Il trattamento delle complicanze in chirurgia senologica ricostruttiva Tecniche per la prevenzione delle complicanze nelle mastectomie conservative Dr. Christian Rizzetto UOC Chirurgia Senologica - Breast
The role of fat grafting in prepectoral breast reconstruction
 Surgical Technique The role of fat grafting in prepectoral breast reconstruction Halley Darrach, Franca Kraenzlin, Nima Khavanin, Karan Chopra, Justin M. Sacks Department of Plastic and Reconstructive
Surgical Technique The role of fat grafting in prepectoral breast reconstruction Halley Darrach, Franca Kraenzlin, Nima Khavanin, Karan Chopra, Justin M. Sacks Department of Plastic and Reconstructive
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
F ORUM. Is One-Stage Breast Augmentation With Mastopexy Safe and Effective? A Review of 186 Primary Cases
 Is One-Stage Breast Augmentation With Mastopexy Safe and Effective? A Review of 186 Primary Cases W. Grant Stevens, MD; David A. Stoker, MD; Mark E. Freeman, MD; Suzanne M. Quardt, MD; Elliot M. Hirsch,
Is One-Stage Breast Augmentation With Mastopexy Safe and Effective? A Review of 186 Primary Cases W. Grant Stevens, MD; David A. Stoker, MD; Mark E. Freeman, MD; Suzanne M. Quardt, MD; Elliot M. Hirsch,
Breast reconstruction following conservative mastectomies: predictors of complications and outcomes
 Review Article Breast reconstruction following conservative mastectomies: predictors of complications and outcomes Sophocles H. Voineskos 1,2, Simon G. Frank 3, Peter G. Cordeiro 3 1 Division of Plastic
Review Article Breast reconstruction following conservative mastectomies: predictors of complications and outcomes Sophocles H. Voineskos 1,2, Simon G. Frank 3, Peter G. Cordeiro 3 1 Division of Plastic
The cosmetic result of immediate mastectomy
 Esther February 14, 20147:45 PM 19:45 4 Color Fig(s): F1-3 Art: GOX-D-14-00014 Ideas and Innovations Breast Immediate Single-stage Endoscopic Latissimus Dorsi Breast and Nipple Reconstruction AQ2 Joaquim
Esther February 14, 20147:45 PM 19:45 4 Color Fig(s): F1-3 Art: GOX-D-14-00014 Ideas and Innovations Breast Immediate Single-stage Endoscopic Latissimus Dorsi Breast and Nipple Reconstruction AQ2 Joaquim
ARTICLE COVERSHEET SERVER-BASED
 ARTICLE COVERSHEET LWW_CONDENSED-FLA(7.75X10.75) SERVER-BASED Template version : 8.1 Revised: 08/23/2012 Article :SAP22670 Creator : jteves Date : Saturday September 8th 2012 Time : 05:19:34 Number of
ARTICLE COVERSHEET LWW_CONDENSED-FLA(7.75X10.75) SERVER-BASED Template version : 8.1 Revised: 08/23/2012 Article :SAP22670 Creator : jteves Date : Saturday September 8th 2012 Time : 05:19:34 Number of
Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps
 BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
Positive Margin Re-Excision Following Immediate Autologous Breast Reconstruction: Morbidity, Cosmetic Outcome, and Oncologic Significance
 Breast Surgery Preliminary Report Positive Margin Re-Excision Following Immediate Autologous Breast Reconstruction: Morbidity, Cosmetic Outcome, and Oncologic Significance Aesthetic Surgery Journal 2017,
Breast Surgery Preliminary Report Positive Margin Re-Excision Following Immediate Autologous Breast Reconstruction: Morbidity, Cosmetic Outcome, and Oncologic Significance Aesthetic Surgery Journal 2017,
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy
 Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction
 Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Porcine Acellular Peritoneal Matrix in Immediate Breast Reconstruction: A Multicenter, Prospective, Single-Arm Trial.
 BREAST Porcine Acellular Peritoneal Matrix in Immediate Breast Reconstruction: A Multicenter, Prospective, Single-Arm Trial Downloaded from https://journals.lww.com/plasreconsurg by jwaj/ss93nyufrwsa7+5b5vziqu6wjijpvebiwz2h1+urwvkxr8buwdlbm24ib0ef6jtjgezj35mn43+kfemwfghpapetcfe9xzrly5+altkvsb2srjqfp1wqazazaeek4hfbhxlkoq=
BREAST Porcine Acellular Peritoneal Matrix in Immediate Breast Reconstruction: A Multicenter, Prospective, Single-Arm Trial Downloaded from https://journals.lww.com/plasreconsurg by jwaj/ss93nyufrwsa7+5b5vziqu6wjijpvebiwz2h1+urwvkxr8buwdlbm24ib0ef6jtjgezj35mn43+kfemwfghpapetcfe9xzrly5+altkvsb2srjqfp1wqazazaeek4hfbhxlkoq=
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Bilateral Reduction Mammaplasty as an Oncoplastic Technique for the Management of Early-Stage Breast Cancer in Women with Macromastia
 Bilateral Reduction Mammaplasty as an Oncoplastic Technique for the Management of Early-Stage Breast Cancer in Women with Macromastia Russell E. Ettinger, MD, a Shailesh Agarwal, MD, a Paul H. Izenberg,
Bilateral Reduction Mammaplasty as an Oncoplastic Technique for the Management of Early-Stage Breast Cancer in Women with Macromastia Russell E. Ettinger, MD, a Shailesh Agarwal, MD, a Paul H. Izenberg,
Goals of Care. Restore shape and function after cancer
 Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Strattice Reconstructive Tissue Matrix used in the repair of rippling
 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty?
 Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty? Michele A. Shermak, MD, Jessie Mallalieu, PA-C, and David Chang, PhD, MPH, MBA The Johns Hopkins Medical Institutions, Division
Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty? Michele A. Shermak, MD, Jessie Mallalieu, PA-C, and David Chang, PhD, MPH, MBA The Johns Hopkins Medical Institutions, Division
PAPER. Impact of Chemotherapy on Postoperative Complications After Mastectomy and Immediate Breast Reconstruction
 PAPER Impact of Chemotherapy on Postoperative Complications After Mastectomy and Immediate Breast Reconstruction Anne Warren Peled, MD; Kaoru Itakura, BA; Robert D. Foster, MD; Debby Hamolsky, RN, MS;
PAPER Impact of Chemotherapy on Postoperative Complications After Mastectomy and Immediate Breast Reconstruction Anne Warren Peled, MD; Kaoru Itakura, BA; Robert D. Foster, MD; Debby Hamolsky, RN, MS;
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER
 Page 1 of 44 BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: February, 2017 The recommendations contained in this guideline are a consensus of the
Page 1 of 44 BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: February, 2017 The recommendations contained in this guideline are a consensus of the
The decision to repair a partial mastectomy CME. State of the Art and Science in Postmastectomy Breast Reconstruction.
 CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
INNOVATIVE RECONSTRUCTIVE STRATEGIES IN BREAST CANCER SURGERY
 INNOVATIVE RECONSTRUCTIVE STRATEGIES IN BREAST CANCER SURGERY Jane L. Kakkis, MD, MPH Breast Surgeon, Director Orange Coast Memorial Medical Center, Fountain Valley, CA USA WHEN RADIATION IS NECESSARY
INNOVATIVE RECONSTRUCTIVE STRATEGIES IN BREAST CANCER SURGERY Jane L. Kakkis, MD, MPH Breast Surgeon, Director Orange Coast Memorial Medical Center, Fountain Valley, CA USA WHEN RADIATION IS NECESSARY
AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION
 CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
Symmastia is an uncommon but very deforming BREAST. The Neosubpectoral Pocket for the Correction of Symmastia.
 BREAST The Neosubpectoral Pocket for the Correction of Symmastia Scott L. Spear, M.D. Joseph H. Dayan, M.D. David Bogue, M.D. Mark W. Clemens, M.D. Michael Newman, M.D. Steven Teitelbaum, M.D. G. Patrick
BREAST The Neosubpectoral Pocket for the Correction of Symmastia Scott L. Spear, M.D. Joseph H. Dayan, M.D. David Bogue, M.D. Mark W. Clemens, M.D. Michael Newman, M.D. Steven Teitelbaum, M.D. G. Patrick
Lipofilling of the Breast Does Not Increase the Risk of Recurrence of Breast Cancer: A Matched Controlled Study
 BREAST of the Breast Does Not Increase the Risk of Recurrence of Breast Cancer: A Matched Controlled Study Steven J. Kronowitz, M.D. Cosman Camilo Mandujano, M.D. Jun Liu, M.D., Ph.D. Henry M. Kuerer,
BREAST of the Breast Does Not Increase the Risk of Recurrence of Breast Cancer: A Matched Controlled Study Steven J. Kronowitz, M.D. Cosman Camilo Mandujano, M.D. Jun Liu, M.D., Ph.D. Henry M. Kuerer,
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Controversy regarding the safety of silicone gelfilled
 Featured Operative Technique The Neopectoral Pocket in Revisionary reast Surgery G. Patrick Maxwell, MD; and Allen Gabriel, MD ontroversy regarding the safety of silicone gelfilled breast implants, which
Featured Operative Technique The Neopectoral Pocket in Revisionary reast Surgery G. Patrick Maxwell, MD; and Allen Gabriel, MD ontroversy regarding the safety of silicone gelfilled breast implants, which
Why Do Patients Seek Revisionary Breast Surgery?
 Breast Surgery Why Do Patients Seek Revisionary Breast Surgery? Navanjun S. Grewal, MD; and Jack Fisher, MD In 2011, according to the American Society for Aesthetic Plastic Surgery (ASAPS), 316 848 American
Breast Surgery Why Do Patients Seek Revisionary Breast Surgery? Navanjun S. Grewal, MD; and Jack Fisher, MD In 2011, according to the American Society for Aesthetic Plastic Surgery (ASAPS), 316 848 American
Francesco Gargano, MD, Frank Ciminello, MD. Correspondence: Objective: Methods:
 eplasty: Vol. 9 a Francesco Gargano, MD,, PhD Frank Ciminello, MD a b Miami, FL, 33155; Miami Children's Hospital,, UMDNJ Plastic Surgery cdepartm Correspondence: francescogargano@hotmail.com Objective:
eplasty: Vol. 9 a Francesco Gargano, MD,, PhD Frank Ciminello, MD a b Miami, FL, 33155; Miami Children's Hospital,, UMDNJ Plastic Surgery cdepartm Correspondence: francescogargano@hotmail.com Objective:
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Updates in Breast Care. Truth or Hype. History of Breast Cancer Surgery. Dr Karen Barbosa 5/3/2017 4/20/2017
 Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
Updates in Breast Care Dr Karen Barbosa 4/20/2017 Truth or Hype Princess Bust Developer Sears, Roebuck and Co. 1897 Promised to make the breast round, firm and beautiful History of Breast Cancer Surgery
Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop
 Aesth Plast Surg (2011) 35:333 340 DOI 10.1007/s00266-010-9612-9 ORIGINAL ARTICLE Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop André Auersvald Luiz Augusto Auersvald Received: 28 April
Aesth Plast Surg (2011) 35:333 340 DOI 10.1007/s00266-010-9612-9 ORIGINAL ARTICLE Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop André Auersvald Luiz Augusto Auersvald Received: 28 April
The American Cancer Society estimates that CME. ASPS Clinical Practice Guideline Summary on Breast Reconstruction with Expanders and Implants
 CME ASPS Clinical Practice Guideline Summary on Breast Reconstruction with Expanders and Implants Amy Alderman, M.D., M.P.H. Karol Gutowski, M.D. Amy Ahuja, M.P.H. Diedra Gray, M.P.H. Postmastectomy Expander/Implant
CME ASPS Clinical Practice Guideline Summary on Breast Reconstruction with Expanders and Implants Amy Alderman, M.D., M.P.H. Karol Gutowski, M.D. Amy Ahuja, M.P.H. Diedra Gray, M.P.H. Postmastectomy Expander/Implant
Breast Reconstruction. Westmead Breast Cancer Institute
 Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
Nipple Sparing Mastectomy: Tips & Tricks. Rebecca Nelson, MD MSc FRCSC Plastic & Reconstructive Surgeon, Burnaby Hospital
 Nipple Sparing Mastectomy: Tips & Tricks Rebecca Nelson, MD MSc FRCSC Plastic & Reconstructive Surgeon, Burnaby Hospital Nipple Sparing Mastectomy (NSM) Introduction & Technique Safety Evidence Indications/Contraindications
Nipple Sparing Mastectomy: Tips & Tricks Rebecca Nelson, MD MSc FRCSC Plastic & Reconstructive Surgeon, Burnaby Hospital Nipple Sparing Mastectomy (NSM) Introduction & Technique Safety Evidence Indications/Contraindications
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C. Your Guide To BREAST RECONSTRUCTION
 Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Breast Cancer after Augmentation: Oncologic and Reconstructive Considerations among Women Undergoing Mastectomy.
 BREAST Breast Cancer after Augmentation: Oncologic and Reconstructive Considerations among Women Undergoing Mastectomy Eugenia H. Cho, B.S. Ronnie L. Shammas, B.S. Brett T. Phillips, M.D., M.B.A. Rachel
BREAST Breast Cancer after Augmentation: Oncologic and Reconstructive Considerations among Women Undergoing Mastectomy Eugenia H. Cho, B.S. Ronnie L. Shammas, B.S. Brett T. Phillips, M.D., M.B.A. Rachel
Repeating Conservative Surgery after Ipsilateral Breast Tumor Reappearance: Criteria for Selecting the Best Candidates
 Ann Surg Oncol (2012) 19:3771 3776 DOI 10.1245/s10434-012-2404-5 ORIGINAL ARTICLE BREAST ONCOLOGY Repeating Conservative Surgery after Ipsilateral Breast Tumor Reappearance: Criteria for Selecting the
Ann Surg Oncol (2012) 19:3771 3776 DOI 10.1245/s10434-012-2404-5 ORIGINAL ARTICLE BREAST ONCOLOGY Repeating Conservative Surgery after Ipsilateral Breast Tumor Reappearance: Criteria for Selecting the
 This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction
 CLINICAL PAPER Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction Ximena A. Pinell-White, MD, Keli Kolegraff, MD, and Grant W. Carlson, MD Background: Contralateral
CLINICAL PAPER Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction Ximena A. Pinell-White, MD, Keli Kolegraff, MD, and Grant W. Carlson, MD Background: Contralateral
Impact of different type of cancer treatment on the effectiveness of breast reconstruction
 Perspective Impact of different type of cancer treatment on the effectiveness of breast reconstruction Joanna Szloch, Elżbieta Marczyk, Marta Kołodziej-Rzepa, Andrzej L. Komorowski Department of Surgical
Perspective Impact of different type of cancer treatment on the effectiveness of breast reconstruction Joanna Szloch, Elżbieta Marczyk, Marta Kołodziej-Rzepa, Andrzej L. Komorowski Department of Surgical
Prevention of Implant Malposition in Inframammary Augmentation Mammaplasty
 Prevention of Implant Malposition in Inframammary Augmentation Mammaplasty Yoon Ji Kim, Yang Woo Kim, Young Woo Cheon Department of Plastic and Reconstructive Surgery, Gachon University Gil Medical Center,
Prevention of Implant Malposition in Inframammary Augmentation Mammaplasty Yoon Ji Kim, Yang Woo Kim, Young Woo Cheon Department of Plastic and Reconstructive Surgery, Gachon University Gil Medical Center,
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
Motiva Implant Matrix Silicone Breast Implants Summary of Clinical Data 5-Year Follow Up
 Motiva Implant Matrix Silicone Breast Implants Summary of Clinical Data 5-Year Follow Up October 21 - February 216 Motiva Implant Matrix Silicone Breast Implants Prospective Clinical Evaluation: 5-Year
Motiva Implant Matrix Silicone Breast Implants Summary of Clinical Data 5-Year Follow Up October 21 - February 216 Motiva Implant Matrix Silicone Breast Implants Prospective Clinical Evaluation: 5-Year
