American Epilepsy Society Guidelines
|
|
|
- Alban Silvester Cole
- 5 years ago
- Views:
Transcription
1 Practice guideline update summary: Efficacy and tolerability of the new antiepileptic drugs I: Treatment of new-onset epilepsy Report of the American Epilepsy Society and the Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology Andres M. Kanner, MD 1 ; Eric Ashman, MD 2 ; David Gloss, MD, MPH&TM 3 ; Cynthia Harden, MD 4 ; Blaise Bourgeois, MD 5 ; Jocelyn F. Bautista, MD 6 ; Bassel Abou-Khalil, MD 7 ; Evren Burakgazi-Dalkilic, MD 8 ; Esmeralda Llanas Park, MD 9 ; John Stern, MD 10 ; Deborah Hirtz, MD 11 ; Mark Nespeca, MD 12 ; Barry Gidal, PharmD 13 ; Edward Faught, MD 14 ; and Jacqueline French, MD 15 1 Miller School of Medicine, University of Miami, FL 2 Bronson Neuroscience Center, Bronson Methodist Hospital, Kalamazoo, MI 3 Department of Neurology, Charleston Area Medical Center, Charleston, WV 4 Department of Neurology, Mount Sinai Beth Israel, New York, NY 5 Children s Hospital, Harvard Medical School, Boston, MA 6 Epilepsy Center, Cleveland Clinic Foundation, OH 7 Department of Neurology, Vanderbilt University, Nashville, TN 8 Department of Neurology, Cooper Medical School, Rowan University, Cherry Hill, NJ 9 AMITA Health Medical Group, Hoffman Estates, IL 10 School of Medicine, University of California, Los Angeles 11 School of Medicine, University of Vermont, Burlington 12 Children s Hospital, University of California San Diego School of Medicine 13 School of Pharmacy, University of Wisconsin, Madison 14 School of Medicine, Emory University, Atlanta, GA 15 Department of Neurology, New York University Langone Comprehensive Epilepsy Center, New York Address correspondence and reprint requests to American Academy of Neurology: guidelines@aan.com Approved by the Guideline Development, Dissemination, and Implementation Subcommittee on July 18, 2015; by the Practice Committee on December 2, 2015; by the American Epilepsy Society Board of Directors on January 16, 2018; and by the AAN Institute Board of Directors on April 18, 2018 Objective: To update the 2004 American Academy of Neurology (AAN) guideline for treating new-onset focal or generalized epilepsy (GE) with second- and third-generation antiepileptic drugs (AEDs). Methods: The 2004 AAN criteria was used to systematically review literature (January 2003 to November 2015), classify pertinent studies according to the therapeutic rating scheme, and link recommendations to evidence strength. Results: Several second-generation AEDs are effective for new-onset focal epilepsy. Data are lacking on efficacy in new-onset generalized tonic clonic seizures, juvenile myoclonic epilepsy, or juvenile absence epilepsy, and on efficacy of third-generation AEDs in new-onset epilepsy. Recommendations: Lamotrigine (LTG) should (Level B) and levetiracetam (LEV) and zonisamide (ZNS) may (Level C) be considered in decreasing seizure frequency in adults with new-onset focal epilepsy. LTG should (Level B) and gabapentin (GBP) may (Level C) be considered in decreasing seizure frequency in patients 60 years with new-onset focal epilepsy. Unless there are compelling adverse-effect related concerns, ethosuximide (ETS) or valproic acid (VPA) should be considered before LTG to decrease seizure frequency in treating absence seizures in childhood absence epilepsy (Level B). No high-quality studies suggest clobazam, eslicarbazepine, ezogabine, felbamate, GBP, lacosamide, LEV, LTG, oxcarbazepine, perampanel, pregabalin, rufinamide, tiagabine, topiramate, vigabatrin, or ZNS is effective in treating new-onset epilepsy because no high-quality studies exist in adults of various ages. A recent FDA strategy allows extrapolation of efficacy across populations; therefore, for focal epilepsy, eslicarbazepine and lacosamide (oral only for pediatric use) as add-on or monotherapy in persons 4 years old and perampanel as monotherapy received FDA approval. Epilepsy Currents, Vol. 18, No. 4 (July/August) 2018 pp American Epilepsy Society 260
2 Glossary AAN: American Academy of Neurology AE: adverse events AED: antiepileptic drug CBZ: carbamazepine CBZ-CR: controlled-release carbamazepine CBZ-IR: immediate-release carbamazepine CLB: clobazam ESL: eslicarbazepine ETS: ethosuximide EZG: ezogabine FBM: felbamate GBP: gabapentin GE: generalized epilepsy GTC: generalized tonic clonic JME: juvenile myoclonic epilepsy LCM: lacosamide LEV: levetiracetam LTG: lamotrigine OXC: oxcarbazepine PER: perampanel PGB: pregabalin PHT: phenytoin RCT: randomized controlled trial RFN: rufinamide TGB: tiagabine TPM: topiramate VGB: vigabatrin VPA: valproic acid VPA-ER: extended-release valproic acid ZNS: zonisamide TABLE 1. Summary of the 2004 AAN guideline Level A or B recommendations regarding the use of new AEDs in treatment of new-onset epilepsy AED Monotherapy focal /mixed (focal + IGE) Gabapentin Yes No Lamotrigine Yes Yes Topiramate Yes No Tiagabine No No Oxcarbazepine Yes No Levetiracetam No No Zonisamide No No Childhood absence epilepsy Abbreviations: IGE = idiopathic generalized epilepsy. INTRODUCTION In 2004, the American Academy of Neurology (AAN) and the American Epilepsy Society (AES) published the first evidencebased guidelines on use of 7 second-generation antiepileptic drugs (AEDs) (table 1 shows principal findings). 1,2 A separate guideline on felbamate (FBM) in intractable epilepsy was published (last reaffirmed July 16, 2016). Since the 2004 publications, new studies emerged in the 8 second-generation and 6 newer (third-generation) AEDs (eslicarbazepine [ESL], ezogabine [EZG], lacosamide [LCM], perampanel [PER], pregabalin [PGB], rufinamide [RFN]). The US Food and Drug Administration has since approved 2 older AEDs (clobazam [CLB], vigabatrin [VGB]; in use for decades in Canada, Europe, and Latin America), for treating certain epileptic disorder types in the United States. This update reviews new evidence for efficacy, safety, and tolerability of CLB, VGB, and the 8 second-generation and 6 third-generation AEDs. The 2004 guidelines examine the mechanisms of action, common and serious adverse events (AEs), and pharmacokinetic properties of the second-generation AEDs. 1 3 A companion guideline update examines the evidence in treatment-resistant epilepsy. 4 This article summarizes the guideline findings, conclusions, and recommendations. The complete guideline, including appendices e-1 through e-6 and tables e-1 and e-2, is available as a data supplement at Neurology.org. DESCRIPTION OF THE ANALYTIC PROCESS The AAN and AES convened an expert panel to develop this guideline in accordance with the 2004 AAN process manual. 5 The complete guideline (data supplement) describes the literature search strategy and evidence review process. Recommendations are based on Class I, II, and III studies; Class IV studies are not discussed. ANALYSIS OF EVIDENCE For adults and children with newly diagnosed epilepsy, are CLB, ESL, EZG, FBM, gabapentin (GBP), lamotrigine (LTG), levetiracetam (LEV), LCM, oxcarbazepine (OXC), PER, PGB, RFN, tiagabine (TGB), topiramate (TPM), VGB, and zonisamide (ZNS) effective as monotherapy, and how does their efficacy and tolerability compare with those of older AEDs? The original practice guidelines included studies that enrolled patients with a mixed group of syndromes. 1 With the 2004 criteria, ratings were lowered from Class I to Class II for the 3 LTG studies and the 1 GBP study, and from Class I to Class III for the 2 TPM studies. The 4 OXC studies remain Class I. Thus, GBP and TPM are considered possibly effective (Level C) and LTG probably effective (Level B); the OXC recommendation level remains unchanged (Level A). Monotherapy in adults with new-onset epilepsy with focal epilepsy or unclassified tonic clonic seizures Since the 2004 publications, 2 Class I, 5 Class II, and 2 Class III studies have been published. One study was conducted in patients aged 60 years and one in patients aged 65 years. 261
3 GBP vs LTG vs carbamazepine A Class II double-blind randomized study compared efficacy and tolerability of GBP ( 1,500 mg/d), LTG ( 150 mg/d), and immediate-release carbamazepine (CBZ-IR) ( 600 mg/d) in patients aged 60 years 6 ; the primary outcome was retention in the trial for 12 months on the basis of seizure recurrence or AEs despite dose adjustments. Drug discontinuation was less frequent among patients randomized to LTG than to GBP or CBZ-IR because of better LTG tolerability. The most frequently occurring AEs included a higher occurrence of weight gain and water retention with GBP than with LTG or CBZ, of rash with CBZ than with LTG, and of hyponatremia with CBZ than with GBP. The 3 AEDs did not differ with respect to neurologic AEs. LTG vs controlled-release carbamazepine The differences between LTG and CBZ-IR identified in the study just described were not reproduced in a Class I study comparing LTG efficacy and tolerability ( mg/d) and controlled-release carbamazepine (CBZ-CR) (400 2,000 mg/d) in treating focal epilepsy among patients 65 years. 7 Retention in the trial was the primary outcome and was based on seizure recurrence and AE occurrence. In the trial s final 20 weeks, the seizure-free rates were the same (52% for LTG vs 57% for CBZ- CR). AE occurrence leading to withdrawal was higher for CBZ- CR (14% for LTG vs 25% for CBZ-CR), but this difference did not reach statistical significance. The most common AEs included dizziness, headache, and fatigue with LTG use and rash, headache, dizziness, somnolence, and fatigue with CBZ use. LEV vs CBZ-CR A Class II study compared the efficacy and tolerability of LEV 1,000 3,000 mg/d and CBZ-CR 400 1,200 mg/d. 8 Seizure-free rates were almost identical for LEV and CBZ-CR at 6 months and 1 year. Depression and insomnia occurred significantly more frequently with LEV use and back pain and weight gain with CBZ-CR use. For both AEDs, headache, fatigue, somnolence, and dizziness were the most frequent AEs. ZNS vs CBZ-CR A double-blind Class II study compared efficacy and tolerability of ZNS mg/d and CBZ-CR 600 1,200 mg/d in patients with focal-onset (74%) or unknown (26%) epilepsy. 9 Primary outcome was percentage of patients achieving seizure freedom for 26 weeks. Seizure-free rates for 26 weeks were nearly identical for ZNS and CBZ-CR. Decreased appetite and weight loss occurred more frequently with ZNS use and dizziness with CBZ-CR use. Headache, dizziness, and somnolence were the most frequent AEs in both AEDs. LTG vs GBP vs TPM vs OXC vs carbamazepine Standard and New Antiepileptic Drugs (SANAD)-Arm A is a Class III randomized unblinded trial in children and adults, of whom 89% had focal epilepsy. 10 The clinician chose initial doses, formulation, and titration rate. Primary outcomes were time to treatment failure and time to 12-month remission. For former outcome, LTG outperformed carbamazepine (CBZ), GBP, and TPM and had a nonsignificant advantage over OXC. For the latter outcome, CBZ outperformed GBP and had a nonsignificant advantage over LTG, OXC, and TPM. LTG was noninferior to CBZ for 12-month remission at 2 and 4 years (secondary outcomes). AE intolerability leading to discontinuation was less frequent with GBP and LTG than with OXC and TPM. Although the frequency of tiredness and fatigue was comparable across the AEDs, rash was more frequent with CBZ and OXC; weight gain, dizziness, and ataxia were more frequent with GBP; and psychiatric symptoms, weight loss, and paresthesia were more frequent with TPM. VGB vs CBZ-IR One Class I study 11 and 1 Class III study 12 compared the safety and efficacy of CBZ-IR and VGB. The primary outcome of the Class I study was time to withdrawal due to lack of efficacy or AEs; secondary outcomes included time to 6-month seizure remission, time to first seizure after reaching the initial target dose ( 600 mg/d CBZ-IR and 2 g/d VGB), and AE development. Although there were no differences between the 2 AEDs regarding time to withdrawal due to lack of efficacy, time to 6-month remission was significantly shorter and time to first seizure significantly longer for CBZ-IR than for VGB. VGB was more frequently associated with psychiatric symptoms and weight gain; rash occurred more frequently with CBZ-IR. In the Class III study, there were significantly more patients seizure free on CBZ-IR than VGB. Serious rash occurred with CBZ-IR; VGB was associated with a significantly higher frequency of scintillating visual disturbances and myoclonic jerks. PGB vs LTG In a Class II double-blind study, 13 the primary outcome was the proportion of patients seizure free for 6 continuous months during the efficacy phase. Doses could be adjusted for the first 24 weeks and then were fixed. A majority of patients received PGB 150 mg/d or LTG 100 mg/d when doses were fixed. Secondary outcomes included withdrawal due to lack of efficacy, time to first seizure, and time to seizure freedom after dose escalation. Seizure freedom was achieved by significantly more patients taking LTG than PGB, as LTG use saw a comparatively greater reduction in patients experiencing only secondarily generalized tonic clonic (GTC) seizures. Weight gain occurred more often among patients receiving PGB. Other frequent AEs did not differ in frequency between the 2 AEDs and included headaches, dizziness, somnolence, and fatigue. Moreover, the 2 AEDs differed only slightly in frequency of AE-related withdrawal (8% of those taking PGB vs 7% of those taking LTG). TPM vs phenytoin One Class II double-blind study compared TPM 100 mg/d followed by phenytoin (PHT) (1,000 mg/d load, 300 mg/d maintenance) for preventing seizure recurrence over 28 days. 14 The primary endpoint was time to recurrence of a first focal seizure with altered awareness or GTC seizure (or both) by study day 28, which occurred in 18.9% of patients on TPM and 9.7% on PHT. However, the study could not establish noninferiority. The most frequent AEs included dizziness and somnolence. PHT use saw a higher incidence of rash leading to discontinuation; paresthesia was more common with TPM use. Cognitive AEs 262
4 occurred more frequently among patients on TPM; these led to only 1.5% of such patients withdrawing from the study. Of note, the data from this study apply only to efficacy over 28 days and cannot be generalized to long-term treatment. Conclusions 1. LTG is probably effective in patients aged 60 years with new-onset focal epilepsy (1 Class I study, 1 Class II study). In these 2 studies, LTG was better tolerated than CBZ-IR but not CBZ-CR. 2. GBP is possibly as effective and better tolerated than CBZ-IR in patients aged 60 years with new-onset focal epilepsy (1 Class II study). 3. LEV is possibly as effective as CBZ-CR in patients with new-onset focal epilepsy (1 Class II study). AEs were comparable between the 2 AEDs. Not enough patients experienced unclassified GTC seizures to identify differences between CBZ-CR and LEV. 4. ZNS is possibly as effective as CBZ-CR in patients with new-onset focal epilepsy (1 Class II study). The 2 AEDs had comparable AE frequency. Not enough patients had unclassified GTC seizures to identify differences between CBZ-CR and ZNS. 5. Evidence is insufficient to compare the efficacy of GBP, OXC, and TPM with that of CBZ-IR or CBZ-CR in patients with new-onset or relapsing focal epilepsy or unclassified GTC seizures (1 Class III study). 6. VGB is probably less efficacious than CBZ-IR in new-onset focal epilepsy (a secondary endpoint of 1 Class I study and of 1 Class III study). Not enough patients experienced unclassified GTC seizures to identify differences between VGB and CBZ-IR. Moreover, VGB is associated with increased risk of serious AEs. 7. PGB is possibly less effective than LTG at the study doses, but the PGB dose was lower than typically used for patients with epilepsy (1 Class II study). Data from this study and the 3 LTG studies examined in the 2004 guideline suggest that LTG is probably effective in treating newonset focal epilepsy. 8. It is not possible to determine whether TPM is equivalent to PHT in urgent treatment of new-onset or recurrent focal epilepsy, unclassified GTC seizures, or GE presenting with GTC seizures (1 Class II study). 9. No high-quality studies suggest CLB, ESL, EZG, FBM, GBP, LCM, LEV, LTG, OXC, PER, PGB, RFN, TGB, TPM, VGB, or ZNS is effective in treating new-onset epilepsy. 10. Evidence is insufficient to demonstrate AED efficacy in unclassified GTC seizures (no study had enough patients with this seizure type). Recommendations In patients with new-onset focal epilepsy or unclassified GTC seizures 1. LTG use should be considered to decrease seizure frequency (Level B) 2. LTG use should be considered (Level B) and GBP use may be considered (Level C) to decrease seizure frequency in patients aged 60 years 3. LEV use may be considered to decrease seizure frequency (Level C) 4. ZNS use may be considered to decrease seizure frequency (Level C) 5. VGB use appears to be less efficacious than CBZ-IR use and may not be offered (Level C); furthermore, toxicity profile precludes VGB use as first-line therapy 6. PGB use at 150 mg/d is possibly less efficacious than LTG use at 100 mg/d (Level C) 7. Evidence is insufficient to consider GBP, OXC, or TPM instead of CBZ (Level U) 8. Evidence is insufficient to consider TPM instead of PHT in urgent treatment of new-onset or recurrent focal epilepsy, unclassified GTC seizures, or GE presenting with GTC seizures (Level U) 9. Data are lacking to support or refute use of third-generation AEDs, CLB, FBM, or VGB in treating new-onset epilepsy (Level U) 10. Data are lacking to support or refute use of newer AEDs in treating unclassified GTC seizures (Level U) Monotherapy in children with new-onset epilepsy with either focal epilepsy or unclassified GTC seizures High-dose vs low-dose TPM In 1 Class II study of children and adolescents, 18 the Kaplan- Meier survival analyses for time to next seizure favored the higher dose (400 mg/d), and the probability of seizure freedom was significantly higher among patients randomized to high-dose than low-dose TPM (50 mg/d) (90% and 78%, respectively, at 6 months; 85% and 62%, respectively, at 12 months). AEs occurred in 4% of children taking 50 mg/d and in 14% of those taking 400 mg/d. The most frequent AEs included headache, decreased appetite, weight loss, somnolence, dizziness, paresthesia, and problems with concentration or attention (or both). Conclusions TPM monotherapy at 400 mg/d is possibly more effective than at 50 mg/d in treating children and adolescents with new-onset focal seizures or generalized-onset GTC seizures (1 Class II 263
5 study). The higher dose is associated with more AEs and is not used in these patients in clinical practice. Of note, this study was done for regulatory and not clinical purposes, and the doses used are not clinically relevant. Therefore, the study data are nonapplicable to clinical practice. Recommendation Although the data from this study would suggest that TPM monotherapy is possibly more efficacious at 400 mg/d than at 50 mg/d for treating children and adolescents with new-onset focal epilepsy or generalized-onset GTC seizures (1 Class II study), no recommendations can be made regarding TPM use at the studied doses, particularly in new-onset epilepsy and pediatric patients. Monotherapy in adults and children with new-onset GE or unclassified GTC seizures LTG vs TPM vs valproic acid A Class III multicenter, randomized, open-label, parallel study, SANAD-Arm B, was conducted in 716 outpatient children and adults with seizure disorders (of which almost 90% had focal epilepsy) in whom a clinician regarded valproate the better standard treatment option than carbamazepine. 10 The clinician chose initial doses and formulations. Patients had to have been diagnosed with new-onset epilepsy (87.7% of patients enrolled), have a seizure disorder failing to remit with a previous monotherapy regimen (excluding the AEDs studied in this trial [8.4%]), or have a seizure disorder that was in remission but relapsed after AED discontinuation (3.9%). GE was diagnosed in 63% of patients and focal epilepsy in 7.3%; 27% had unclassified epilepsy. Patients were randomized to LTG, TPM, or valproic acid (VPA); the treating clinician determined the target doses according to everyday practice doses. 19 Primary outcomes were time to treatment failure (defined as AED discontinuation because of seizures or AEs, or both) and time to 1-year remission. VPA outperformed TPM for time to treatment failure but was comparable with LTG. When the analysis was restricted to GE, VPA was superior to LTG and TPM. For time to 1-year remission, VPA was superior to LTG when all patients were included or when analysis was restricted to only those with GE, but VPA did not differ from TPM in either analysis. Weight gain was the most frequent AE leading to treatment failure with VPA, and fatigue and psychiatric and cognitive symptoms were the most common AEs associated with TPM. Rash was the most common AE leading to LTG discontinuation (4%). Conclusion Evidence is insufficient to compare efficacy of LTG and TPM with that of VPA in children and adults with new-onset or relapsing GE (1 Class III study). Monotherapy in adults and adolescents with new-onset focal, GE, or unclassified GTC seizures LEV vs extended-release VPA or CBZ-CR KOMET, a Class III multicenter, randomized, open-label parallel study, compared effectiveness of LEV with that of extendedrelease VPA (VPA-ER) or CBZ-CR in 1,688 outpatient adolescents (aged 16 years) and adults with new-onset epilepsy. 20 GE was diagnosed in 34.8% of patients and focal epilepsy in 64.7%; 2.1% had unclassified epilepsy. The clinician was allowed to choose VPA-ER or CBZ-CR as the better standard treatment option, and patients were then randomized (1:1) to treatment with LEV or 1 of the 2 standard AEDs. Initial target doses were reached over 2 weeks (LEV 1,000 mg/d, VPA-ER 1,000 mg/d, CBZ-CR 600 mg/d), and with seizure occurrence, the clinician could increase the dose to 3,000 mg/d for LEV, 2,000 mg/d for VPA-ER, and 1,600 mg/d for CBZ-CR. Of the patients randomized to standard AEDs, 65.8% treated with VPA-ER had only GE, and 86.5% treated with CBZ-CR had only focal epilepsy. Primary outcomes were time to treatment failure (defined as AED discontinuation caused by seizures or AEs, or both), and LEV was compared with VPA-ER and with CBZ-CR. Time to treatment withdrawal was similar for LEV and VPA-ER; a nonsignificantly longer time to treatment withdrawal occurred with LEV than with CBZ-CR. The 3 drugs were comparable regarding frequency of drug-related AEs and AEs leading to drug discontinuation. The most frequent AEs were weight gain and tremor with VPA, depression with LEV, and rash with CBZ-CR. Headache, fatigue, and dizziness were equally frequent across these AEDs. Conclusion Evidence is insufficient to compare efficacy of CBZ-CR, LEV, and VPA-ER in adolescents and adults with new-onset GE and focal epilepsy (1 Class III study). Childhood absence epilepsy A Class I study compared the efficacy, tolerability, and neuropsychological effects of LTG (12 mg/kg/d), ethosuximide (ETS) (60 mg/kg/d), and VPA (60 mg/kg/d). 21 Study outcomes included freedom from treatment failure after 16 weeks (which could be extended to 20 weeks if necessary) and attention disturbances measured with objective tests (e.g., continuous performance test). Children randomized to ETS and VPA had comparable freedom-from-failure rates, which were significantly higher than the LTG rates. Attention disturbances were significantly more common with VPA than with ETS. These seizure control and cognitive AE differences were maintained at a 12-month follow-up evaluation study. 22 Conclusion LTG is probably not as effective as ETS or VPA for treating absence seizures in children with childhood absence epilepsy (1 Class I study). Attention disturbances are more common with VPA use. Clinical context ETS use is limited to patients with childhood absence epilepsy without associated GTC seizures. Recommendation Unless there are compelling reasons based on AE profile, ETS or VPA use should be considered before LTG use to decrease seizure frequency in treating absence seizures in childhood absence epilepsy (Level B). 264
6 No high-quality studies suggest CLB, ESL, EZG, FBM, GBP, LCM, LEV, LTG, OXC, PER, PGB, RFN, TGB, TPM, VGB, or ZNS is effective in treating new-onset epilepsy. CLINICAL CONTEXT The studies examined here on treating new-onset epilepsy were limited to comparisons between first- and second-generation AEDs (and VGB). Therefore, recommendations can be made related only to those medications and cannot be generalized to comparisons involving other AEDs. The data reviewed apply to treatment of focal epilepsy and limit the ability to make recommendations regarding these drugs for unclassified GTC seizures. The single study wherein the majority of patients had GTC seizures secondary to GE was Class III, so no recommendations can be made regarding the second-generation AEDs (LTG, TPM) used in treating this epilepsy type. The Class I study of children with absence epilepsy suggested that LTG is probably not as effective in this epilepsy type as the 2004 guideline suggests. A recent FDA strategy allows extrapolation of efficacy across populations and granted approval of eslicarbazepine and lacosamide (oral only for pediatric age group) as add-on or monotherapy for focal epilepsy in persons 4 years old and perampanel as monotherapy for focal epilepsy. FBM and VGB are not recommended in new-onset epilepsy for clinical use due to serious AEs, as there are other agents that are both safe and efficacious. RECOMMENDATIONS FOR FUTURE RESEARCH GBP, LEV, LTG, OXC, and ZNS are second-generation AEDs that can be considered for new-onset focal epilepsy. Change from Class I to Class III of 2 TPM studies reviewed in the 2004 guideline 23,24 suggests that TPM may be possibly effective and its efficacy should be reinvestigated in a randomized controlled trial (RCT) with doses commonly used in clinical practice. No data are available on efficacy and tolerability of TGB or any third-generation AEDs and CLB in treating new-onset focal epilepsy. The trial with PGB should be repeated using higher doses to determine whether PGB can be considered efficacious. Among second-generation AEDs, only OXC has evidence from a Class I study suggesting efficacy in new-onset focal epilepsy. 25 No studies exist on efficacy of second-generation AEDs in new-onset GE with GTC seizures in children or adolescents with juvenile absence epilepsy or juvenile myoclonic epilepsy (JME). Data are unavailable about efficacy of third-generation AEDs in new-onset epilepsy in children. The need is clear for RCTs in pediatric patients with newonset epilepsy. No data exist on use of second- and third-generation AEDs, CLB, or VGB in treating adults with new-onset GE with GTC seizures or in JME. Such studies should be included in future research. Third-generation AEDs found equivalent to LTG or to CBZ- CR or VPA (or both CBZ-CR and VPA) for treating new-onset focal epilepsy and GE, respectively, should undergo head-tohead comparisons with third-generation AEDs in double-blind, controlled, parallel studies for efficacy. DISCLAIMER Clinical practice guidelines, practice advisories, systematic reviews and other guidance published by the American Academy of Neurology and its affiliates are assessments of current scientific and clinical information provided as an educational service. The information: 1) should not be considered inclusive of all proper treatments, methods of care, or as a statement of the standard of care; 2) is not continually updated and may not reflect the most recent evidence (new evidence may emerge between the time information is developed and when it is published or read); 3) addresses only the question(s) specifically identified; 4) does not mandate any particular course of medical care; and 5) is not intended to substitute for the independent professional judgment of the treating provider, as the information does not account for individual variation among patients. In all cases, the selected course of action should be considered by the treating provider in the context of treating the individual patient. Use of the information is voluntary. AAN provides this information on an as is basis, and makes no warranty, expressed or implied, regarding the information. AAN specifically disclaims any warranties of merchantability or fitness for a particular use or purpose. AAN assumes no responsibility for any injury or damage to persons or property arising out of or related to any use of this information or for any errors or omissions. CONFLICT OF INTEREST The American Academy of Neurology (AAN) and the American Epilepsy Society (AES) committed to producing independent, critical, and truthful clinical practice guidelines (CPGs). Significant efforts are made to minimize the potential for conflicts of interest to influence the recommendations of this CPG. To the extent possible, the AAN and AES keep separate those who have a financial stake in the success or failure of the products appraised in the CPGs and the developers of the guidelines. Conflict of interest forms were obtained from all authors and reviewed by an oversight committee prior to project initiation. The AAN and AES limit the participation of authors with substantial conflicts of interest. The AAN and AES forbid commercial participation in, or funding of, guideline projects. Drafts of the guideline have been reviewed by at least three AAN committees, three AES committees, a network of neurologists, Neurology peer reviewers, and representatives from related fields. The AAN Guideline Author Conflict of Interest Policy can be viewed at For complete information on this process, access the 2004 AAN process manual. 5 AUTHOR CONTRIBUTIONS Dr. Kanner: study concept and design, acquisition of data, analysis or interpretation of data, drafting/revising the manuscript, critical revision of the manuscript for important intellectual content, study supervision. Dr. Ashman: study concept and design, acquisition of data, analysis or interpretation of data, drafting/revising the manuscript, critical revision of the manuscript for important intellectual content, study supervision. 265
7 Dr. Gloss: acquisition of data, analysis or interpretation of data, drafting/revising the manuscript, critical revision of the manuscript for important intellectual content, study supervision. Dr. Harden: analysis or interpretation of data, drafting/revising the manuscript, critical revision of the manuscript for important intellectual content, study supervision. Dr. Bourgeois: study concept and design, acquisition of data, Dr. Bautista: study concept and design, acquisition of data, Dr. Abou-Khalil: study concept and design, acquisition of data, Dr. Burakgazi-Dalkilic: study concept and design, acquisition of data, Dr. Llanas Park: study concept and design, acquisition of data, Dr. Stern: study concept and design, acquisition of data, analysis or interpretation of data. Dr. Hirtz: study concept and design, acquisition of data, analysis or interpretation of data. Dr. Nespeca: study concept and design, acquisition of data, Dr. Gidal: study concept and design, acquisition of data, analysis or interpretation of data. Dr. Faught: study concept and design, acquisition of data, Dr. French: study concept and design, analysis or interpretation of data, drafting/revising the manuscript, critical revision of the manuscript for important intellectual content, study supervision. STUDY FUNDING This practice guideline was developed with financial support from the American Academy of Neurology (AAN). Authors who serve or served as AAN subcommittee members or methodologists (A.M.K., E.A., D.G., C.H., D.H., and J.F.) were reimbursed by the AAN for expenses related to travel to subcommittee meetings where drafts of manuscripts were reviewed. DISCLOSURES A. Kanner has served on a scientific advisory board for UCB but the honorarium was transferred to the Department of Neurology at the University of Miami, Miller School of Medicine; receives royalties from Psychiatric Aspects of Epilepsy, Treatment of Depression in Neurological Disorders, and Psychiatric Controversies in Epilepsy, and received honoraria from Medscape and as a consultant for Neuropace. E. Ashman receives funding from the American Academy of Neurology (AAN) for travel; has served as associate editor, level of evidence, for Neurology; has performed imaging studies that include MRI, electrophysiology, and electroencephalography in patients who are comatose; and has provided medical reviews and consultations for lawsuits and medical claims as part of his role in the US Air Force. D. Gloss serves as an evidence-based medicine consultant for the AAN. C. Harden receives royalties from UpToDate and Wiley; serves on the speakers bureau for UBC; and has received research support from the National Institute of Neurological Disorders and Stroke (NINDS) of the NIH and the Epilepsy Therapy Project. B. Bourgeois serves on the data and safety monitoring board for a clinical trial conducted by Pfizer Pharmaceuticals, for which he receives honoraria; and receives royalties for The Epilepsy Prescriber s Guide to Antiepileptic Drugs. J. Bautista serves on the National Quality Forum Neurology Steering Committee and the Neurology Endorsement Maintenance Committee and has received research funding from the NIH and NINDS. B. Abou-Khalil has served on but declined honoraria from scientific advisory boards for Sunovion and GlaxoSmithKline; served on the editorial board for Epilepsy Research and Clinical Neurophysiology; and received royalties for Atlas of EEG & Seizure Semiology. His institution received research support from UCB, GlaxoSmithKline, Valeant, Sunovion, Upsher-Smith, Pfizer, Cyberonics, and SK Life Science, from the NIH for the Epilepsy Phenome/Genome Project and from the Human Epilepsy Project. E. Burakgazi-Dalkilic serves on a speakers bureau for Eisai Pharmaceuticals. E. Llanas Park reports no relevant disclosures. J. Stern serves on the scientific advisory board for Sunovion and Lundbeck; serves as an editor for MedLink Neurology; receives royalties for Atlas of EEG Patterns and Atlas of Video-EEG Monitoring; receives honoraria from and serves on the speakers bureaus of UCB, Lundbeck, Eisai, Cyberonics, and Sunovion; and performs clinical practice in epilepsy (50% of his time). D. Hirtz reports no relevant disclosures. M. Nespeca serves on the Scientific Advisory Committee of the Angelman Syndrome Foundation; is a co-investigator for a US Food and Drug Administration funded trial on levetiracetam vs phenobarbital in neonatal seizures and for industry-sponsored trials on everolimus (Novartis) for epilepsy in persons with tuberous sclerosis and on fenfluramine (Zogenix) in Dravet syndrome. B. Gidal serves on scientific advisory boards and speakers bureaus for UCB, Eisai, and Sunovion, for which he receives 266
8 honoraria; performs clinical practice in epilepsy (20% of his time); and has provided expert testimony, prepared an affidavit, and acted as a witness in the legal proceeding of Activis v Depomed. E. Faught serves on the scientific advisory boards of Eisai, Lundbeck, SK Life Science, Supernus, Sunovion, and UCB; has received research support from Brain Sentinel, UCB, the Centers for Disease Control and Prevention, University of Alabama at Birmingham, and the Epilepsy Consortium; and has acted as a witness in legal proceedings for Rushton Stakley. J. French receives New York University salary support from the Epilepsy Foundation and for consulting work on behalf of the Epilepsy Study Consortium for Eisai, GlaxoSmithKline, Novartis, Pfizer, Sunovion, UCB, and Upsher Smith; has received research grants from Eisai Medical Research, Lundbeck, Pfizer, Sunovion, and UCB; has received grants from the Epilepsy Research Foundation, Epilepsy Study Consortium, Epilepsy Therapy Project, and the NINDS of the NIH; serves on the editorial boards of Lancet Neurology, Neurology Today, and Epileptic Disorders; serves as scientific officer for the Epilepsy Foundation for which New York University receives salary support; and has received travel reimbursement related to research, advisory meetings, or presentation of results at scientific meetings from the Epilepsy Study Consortium, the Epilepsy Foundation, Eisai, GlaxoSmithKline, Pfizer, UCB, and Upsher-Smith. References 1. French JA, Kanner AM, Bautista J, et al. Efficacy and tolerability of the new antiepileptic drugs I: treatment of new-onset epilepsy. Neurology 2004;62: French JA, Kanner AM, Bautista J, et al. Efficacy and tolerability of the new antiepileptic drugs II: treatment of refractory epilepsy. Neurology 2004;62: French J, Smith M, Faught E, Brown L. Practice advisory: the use of felbamate in the treatment of patients with intractable epilepsy: report of the Quality Standards Subcommittee of the American Academy of Neurology and the American Epilepsy Society. Neurology 1999;52: Kanner AM, Ashman E, Gloss D, et al.; on behalf of the American Academy of Neurology and American Epilepsy Society. Practice guideline update: Efficacy and tolerability of the new antiepileptic drugs I: Treatment of new-onset epilepsy. Report of the Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology and the American Epilepsy Society. In development. 5. American Academy of Neurology. Clinical Practice Guidelines Process Manual, 2004 ed. St. Paul, MN: The American Academy of Neurology; Published Accessed January 30, Rowan AJ, Ramsay RE, Collins JF, et al.; VA Cooperative Study 428 Group. New onset geriatric epilepsy: a randomized study of gabapentin, lamotrigine, and carbamazepine. Neurology 2005;64: Saetre E, Perucca E, Isojärvi J, Gjerstad L; LAM Study Group. An international multicenter randomized double-blind controlled trial of lamotrigine and sustained-release carbamazepine in the treatment of newly diagnosed epilepsy in the elderly. Epilepsia 2007;48: Brodie MJ, Perucca E, Ryvlin P, Ben-Menachem E, Meencke HJ; Levetiracetam Monotherapy Study Group. Comparison of levetiracetam and controlled-release carbamazepine in newly diagnosed epilepsy. Neurology 2007;68: Baulac M, Brodie MJ, Patten A, Segieth J, Giorgi L. Efficacy and tolerability of zonisamide versus controlled-release carbamazepine for newly diagnosed partial epilepsy: a phase 3, randomised, doubleblind, non-inferiority trial. Lancet Neurol 2012;11: Marson AG, Al-Kharusi AM, Alwaidh M, et al; SANAD Study Group The SANAD study of effectiveness of carbamazepine, gabapentin, lamotrigine, oxcarbazepine, or topiramate for treatment of partial epilepsy: an unblinded randomised controlled trial. Lancet 2007;369: Chadwick D. Safety and efficacy of vigabatrin and carbamazepine in newly diagnosed epilepsy: a multicentre randomised doubleblind study. Vigabatrin European Monotherapy Study Group. Lancet 1999;354: Kälviäinen R, Aikiä M, Saukkonen AM, Mervaala E, Riekkinen PJ Sr. Vigabatrin vs carbamazepine monotherapy in patients with newly diagnosed epilepsy. A randomized, controlled study. Arch Neurol 1995;52: Kwan P, Brodie MJ, Kälviäinen R, Yurkewicz J, Weaver J, Knapp LE. Efficacy and safety of pregabalin versus lamotrigine in patients with newly diagnosed partial seizures: a phase 3, double-blind, randomised, parallel-group trial. Lancet 2011;10: Ramsay E, Faught E, Krumholz A, et al.; CAPSS-272 Study Group. Efficacy, tolerability, and safety of rapid initiation of topiramate versus phenytoin in patients with new-onset epilepsy: a randomized double-blind clinical trial. Epilepsia 2010;51: Brodie MJ, Overstall PW, Giorgi L. Multicentre, double-blind, randomised comparison between lamotrigine and carbamazepine in elderly patients with newly diagnosed epilepsy. The UK Lamotrigine Elderly Study Group. Epilepsy Res 1999;37: Brodie MJ, Richens A, Yuen AW. Double-blind comparison of lamotrigine and carbamazepine in newly diagnosed epilepsy. UK Lamotrigine/Carbamazepine Monotherapy Trial Group. Lancet 1995;345: Steiner TJ, Dellaportas CL, Findley LJ, et al. Lamotrigine monotherapy in newly diagnosed untreated epilepsy: a double-blind comparison with phenytoin. Epilepsia 1999;40: Glauser TA, Dlugos DJ, Dodson WE, Grinspan A, Wang S, Wu SC; EPMN-106/INT-28 Investigators. Topiramate monotherapy in newly diagnosed epilepsy in children and adolescents. J Child Neurol 2007;22: Marson AG, Al-Kharusi AM, Alwaidh M, et al.; SANAD Study Group. The SANAD study of effectiveness of valproate, lamotrigine, or topiramate for generalised and unclassifiable epilepsy: an unblinded randomised controlled trial. Lancet 2007; 369: Trinka E, Marson AG, Van Paesschen W, et al.; KOMET Study Group. KOMET: an unblinded, randomized, two parallel-group, stratified trial comparing the effectiveness of levetiracetam with controlledrelease carbamazepine and extended-release sodium valproate as monotherapy in patients with newly diagnosed epilepsy. J Neurol Neurosurg Psychiatry, 2013;84: Glauser TA, Cnaan A, Shinnar S, et al.; Childhood Absence Epilepsy Study Group. Ethosuximide, valproic acid, and lamotrigine in childhood absence epilepsy. N Engl J Med 2010;362: Glauser TA, Cnaan A, Shinnar S, et al.; Childhood Absence Epilepsy Study Team. Ethosuximide, valproic acid, and lamotrigine in child- 267
9 hood absence epilepsy: initial monotherapy outcomes at 12 months. Epilepsia 2013;54: Gilliam FG, Veloso F, Bomhof MA, et al. A dose-comparison trial of topiramate as monotherapy in recently diagnosed partial epilepsy. Neurology 2003;60: Privitera MD, Brodie MJ, Mattson RH, et al.; EPMN 105 Study Group. Topiramate, carbamazepine and valproate monotherapy: doubleblind comparison in newly diagnosed epilepsy. Acta Neurol Scand 2003;107: Guerreiro MM, Vigonius U, Pohlmann H, et al. A double-blind controlled clinical trial of oxcarbazepine versus phenytoin in children and adolescents with epilepsy. Epilepsy Res 1997;27:
2018 American Academy of Neurology
 Practice Guideline Update Efficacy and Tolerability of the New Antiepileptic Drugs I: Treatment of New-Onset Epilepsy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of
Practice Guideline Update Efficacy and Tolerability of the New Antiepileptic Drugs I: Treatment of New-Onset Epilepsy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of
2018 American Academy of Neurology
 Practice Guideline Update Efficacy and Tolerability of the New Antiepileptic Drugs II: Treatment-Resistant Epilepsy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of the
Practice Guideline Update Efficacy and Tolerability of the New Antiepileptic Drugs II: Treatment-Resistant Epilepsy Report by: Guideline Development, Dissemination, and Implementation Subcommittee of the
Published Ahead of Print on June 13, 2018 as /WNL
 SPECIAL ARTICLE Published Ahead of Print on June 13, 2018 as 10.1212/WNL.0000000000005756 Practice guideline update summary: Efficacy and tolerability of the new antiepileptic drugs II: Treatment-resistant
SPECIAL ARTICLE Published Ahead of Print on June 13, 2018 as 10.1212/WNL.0000000000005756 Practice guideline update summary: Efficacy and tolerability of the new antiepileptic drugs II: Treatment-resistant
Zonisamide Should Be Considered a First-Line Antiepileptic Drug for Patients with Newly Diagnosed Partial Epilepsy
 Current Literature In Clinical Science Zonisamide Should Be Considered a First-Line Antiepileptic Drug for Patients with Newly Diagnosed Partial Epilepsy Efficacy and Tolerability of Zonisamide Versus
Current Literature In Clinical Science Zonisamide Should Be Considered a First-Line Antiepileptic Drug for Patients with Newly Diagnosed Partial Epilepsy Efficacy and Tolerability of Zonisamide Versus
Update in Clinical Guidelines in Epilepsy
 Why We Need Clinical Guidelines? Clinician needs advice! Update in Clinical Guidelines in Epilepsy Charcrin Nabangchang, M.D. Phramongkutklao College of Medicine Tiamkao S, Neurology Asia2013 Why We Need
Why We Need Clinical Guidelines? Clinician needs advice! Update in Clinical Guidelines in Epilepsy Charcrin Nabangchang, M.D. Phramongkutklao College of Medicine Tiamkao S, Neurology Asia2013 Why We Need
AED Treatment Approaches. David Spencer, MD Director, OHSU Epilepsy Center Professor, Department of Neurology
 AED Treatment Approaches David Spencer, MD Director, OHSU Epilepsy Center Professor, Department of Neurology Audience Response Keypads Please utilize the keypad at your table to answer questions throughout
AED Treatment Approaches David Spencer, MD Director, OHSU Epilepsy Center Professor, Department of Neurology Audience Response Keypads Please utilize the keypad at your table to answer questions throughout
Epilepsia, 45(5): , 2004 Blackwell Publishing, Inc. C 2004 International League Against Epilepsy. C 2004 AAN Enterprises, Inc.
 Epilepsia, 45(5):410 423, 2004 Blackwell Publishing, Inc. C 2004 International League Against Epilepsy C 2004 AAN Enterprises, Inc. Efficacy and Tolerability of the New Antiepileptic Drugs, II: Treatment
Epilepsia, 45(5):410 423, 2004 Blackwell Publishing, Inc. C 2004 International League Against Epilepsy C 2004 AAN Enterprises, Inc. Efficacy and Tolerability of the New Antiepileptic Drugs, II: Treatment
Children Are Not Just Small Adults Choosing AEDs in Children
 Children Are Not Just Small Adults Choosing AEDs in Children Natrujee Wiwattanadittakun, MD Neurology division, Department of Pediatrics, Chiang Mai University Hospital, Chiang Mai University 20 th July,
Children Are Not Just Small Adults Choosing AEDs in Children Natrujee Wiwattanadittakun, MD Neurology division, Department of Pediatrics, Chiang Mai University Hospital, Chiang Mai University 20 th July,
Difficult to treat childhood epilepsy: Lessons from clinical case scenario
 Difficult to treat childhood epilepsy: Lessons from clinical case scenario Surachai Likasitwattanakul, M.D. Department of Pediatrics Faculty of Medicine, Siriraj Hospital Natural history of Epilepsy Untreated
Difficult to treat childhood epilepsy: Lessons from clinical case scenario Surachai Likasitwattanakul, M.D. Department of Pediatrics Faculty of Medicine, Siriraj Hospital Natural history of Epilepsy Untreated
Monotherapy in Newly Diagnosed Epilepsy: Levetiracetam Versus Standard Anticonvulsants
 Monotherapy in Newly Diagnosed Epilepsy: Levetiracetam Versus Standard Anticonvulsants Current Literature In Clinical Science KOMET: An Unblinded, Randomised, Two Parallel-Group, Stratified Trial Comparing
Monotherapy in Newly Diagnosed Epilepsy: Levetiracetam Versus Standard Anticonvulsants Current Literature In Clinical Science KOMET: An Unblinded, Randomised, Two Parallel-Group, Stratified Trial Comparing
Pharmacological Treatment of Non-Lesional Epilepsy December 8, 2013
 Pharmacological Treatment of Non-Lesional Epilepsy December 8, 2013 Michael Privitera, MD Professor of Neurology University of Cincinnati, Neuroscience Institute American Epilepsy Society Annual Meeting
Pharmacological Treatment of Non-Lesional Epilepsy December 8, 2013 Michael Privitera, MD Professor of Neurology University of Cincinnati, Neuroscience Institute American Epilepsy Society Annual Meeting
AEDs in 2011: A Critical Comparative Review December 3, 2011
 AEDs in 2011: A Critical Comparative Review December 3, 2011 Selim R. Benbadis, M.D. University of South Florida Tampa, FL American Epilepsy Society Annual Meeting Disclosure Speakers bureau Consultant
AEDs in 2011: A Critical Comparative Review December 3, 2011 Selim R. Benbadis, M.D. University of South Florida Tampa, FL American Epilepsy Society Annual Meeting Disclosure Speakers bureau Consultant
MONOTHERAPY IS PREferred
 Monotherapy in Epilepsy Role of the Newer Antiepileptic Drugs Blanca Vazquez, MD NEUROLOGICAL REVIEW Background: Monotherapy is the goal for pharmacological treatment of epilepsy. Well-controlled trials
Monotherapy in Epilepsy Role of the Newer Antiepileptic Drugs Blanca Vazquez, MD NEUROLOGICAL REVIEW Background: Monotherapy is the goal for pharmacological treatment of epilepsy. Well-controlled trials
ORIGINAL CONTRIBUTION. Comparative Effectiveness of 10 Antiepileptic Drugs in Older Adults With Epilepsy
 ORIGINAL CONTRIBUTION Comparative Effectiveness of 10 Antiepileptic Drugs in Older Adults With Epilepsy Hiba Arif, MD; Richard Buchsbaum; Joanna Pierro, BA; Michael Whalen, BA; Jessica Sims, MD; Stanley
ORIGINAL CONTRIBUTION Comparative Effectiveness of 10 Antiepileptic Drugs in Older Adults With Epilepsy Hiba Arif, MD; Richard Buchsbaum; Joanna Pierro, BA; Michael Whalen, BA; Jessica Sims, MD; Stanley
Pharmacy Medical Necessity Guidelines: Anticonvulsants/Mood Stabilizers
 Pharmacy Medical Necessity Guidelines: Anticonvulsants/Mood Stabilizers Effective: December 18, 2017 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review
Pharmacy Medical Necessity Guidelines: Anticonvulsants/Mood Stabilizers Effective: December 18, 2017 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review
Drug Choice in New-Onset Epilepsy December 6, 2013
 Drug Choice in New-Onset Epilepsy December 6, 2013 Tracy A. Glauser, M.D. Director, Comprehensive Epilepsy Center Cincinnati Children s Hospital Medical Center American Epilepsy Society Annual Meeting
Drug Choice in New-Onset Epilepsy December 6, 2013 Tracy A. Glauser, M.D. Director, Comprehensive Epilepsy Center Cincinnati Children s Hospital Medical Center American Epilepsy Society Annual Meeting
Therapeutic strategies in the choice of antiepileptic drugs
 Acta neurol. belg., 2002, 102, 6-10 Original articles Therapeutic strategies in the choice of antiepileptic drugs V. DE BORCHGRAVE, V. DELVAUX, M. DE TOURCHANINOFF, J.M. DUBRU, S. GHARIANI, Th. GRISAR,
Acta neurol. belg., 2002, 102, 6-10 Original articles Therapeutic strategies in the choice of antiepileptic drugs V. DE BORCHGRAVE, V. DELVAUX, M. DE TOURCHANINOFF, J.M. DUBRU, S. GHARIANI, Th. GRISAR,
Tailoring therapy to optimize care for Epilepsy. Dr Tim Wehner National Hospital for Neurology and Neurosurgery London, UK For discussion only
 Tailoring therapy to optimize care for Epilepsy Dr Tim Wehner National Hospital for Neurology and Neurosurgery London, UK For discussion only Disclosures Session (travel expenses) sponsored by Pfizer Premature
Tailoring therapy to optimize care for Epilepsy Dr Tim Wehner National Hospital for Neurology and Neurosurgery London, UK For discussion only Disclosures Session (travel expenses) sponsored by Pfizer Premature
Disclosure. Learning Objectives
 Linda D. Leary, M.D. Associate Clinical Professor of Pediatrics & Neurology South Texas Comprehensive Epilepsy Center UT Health Science Center San Antonio Disclosure Linda D. Leary, M.D. discloses the
Linda D. Leary, M.D. Associate Clinical Professor of Pediatrics & Neurology South Texas Comprehensive Epilepsy Center UT Health Science Center San Antonio Disclosure Linda D. Leary, M.D. discloses the
Newer AEDs compared to LVT as adjunctive treatments for uncontrolled focal epilepsy. Dr. Yotin Chinvarun. M.D. Ph.D.
 Newer AEDs compared to LVT as adjunctive treatments for uncontrolled focal epilepsy Dr. Yotin Chinvarun. M.D. Ph.D. Chronology of antiepileptic drug introduction over the past 150 years 20 15 10 Perampanel
Newer AEDs compared to LVT as adjunctive treatments for uncontrolled focal epilepsy Dr. Yotin Chinvarun. M.D. Ph.D. Chronology of antiepileptic drug introduction over the past 150 years 20 15 10 Perampanel
Efficacy and tolerability of the new antiepileptic drugs I: Treatment of new onset epilepsy
 Special Article CME Efficacy and tolerability of the new antiepileptic drugs I: Treatment of new onset epilepsy Report of the Therapeutics and Technology Assessment Subcommittee and Quality Standards Subcommittee
Special Article CME Efficacy and tolerability of the new antiepileptic drugs I: Treatment of new onset epilepsy Report of the Therapeutics and Technology Assessment Subcommittee and Quality Standards Subcommittee
Treatment of epilepsy in adults
 Treatment of epilepsy in adults Review 33 Treatment of epilepsy in adults S B Gunatilake 1, A Arasalingam 2 Sri Lanka Journal of Neurology, 2012, 1, 33-38 Case vignettes 1. A 60-year old patient with long
Treatment of epilepsy in adults Review 33 Treatment of epilepsy in adults S B Gunatilake 1, A Arasalingam 2 Sri Lanka Journal of Neurology, 2012, 1, 33-38 Case vignettes 1. A 60-year old patient with long
AN UPDATE ON ANTIEPILEPTIC AGENTS: FOCUS ON AN UPDATE ON ANTIEPILEPTIC AGENTS: FOCUS ON SECOND GENERATION TREATMENT OPTIONS
 Volume 24, Issue 1 October 2008 AN UPDATE ON ANTIEPILEPTIC AGENTS: FOCUS ON SECOND GENERATION TREATMENT OPTIONS Jason Richey, Pharm.D. Candidate Epilepsy is a neurological disorder characterized by sudden
Volume 24, Issue 1 October 2008 AN UPDATE ON ANTIEPILEPTIC AGENTS: FOCUS ON SECOND GENERATION TREATMENT OPTIONS Jason Richey, Pharm.D. Candidate Epilepsy is a neurological disorder characterized by sudden
Efficacy and tolerability of the new antiepileptic drugs II: Treatment of refractory epilepsy
 Special Article Efficacy and tolerability of the new antiepileptic drugs II: Treatment of refractory epilepsy Report of the Therapeutics and Technology Assessment Subcommittee and Quality Standards Subcommittee
Special Article Efficacy and tolerability of the new antiepileptic drugs II: Treatment of refractory epilepsy Report of the Therapeutics and Technology Assessment Subcommittee and Quality Standards Subcommittee
ARTICLES Monotherapy in adults and elderly persons
 ARTICLES Monotherapy in adults and elderly persons Edward Faught, MD Address correspondence and reprint requests to Dr. Edward Faught, Department of Neurology, University of Alabama at Birmingham Epilepsy
ARTICLES Monotherapy in adults and elderly persons Edward Faught, MD Address correspondence and reprint requests to Dr. Edward Faught, Department of Neurology, University of Alabama at Birmingham Epilepsy
Treatment outcome after failure of a first antiepileptic drug
 Treatment outcome after failure of a first antiepileptic drug Laura J. Bonnett, PhD Catrin Tudur Smith, PhD Sarah Donegan, PhD Anthony G. Marson, PhD Correspondence to Prof. Marson: A.G.Marson@liverpool.ac.uk
Treatment outcome after failure of a first antiepileptic drug Laura J. Bonnett, PhD Catrin Tudur Smith, PhD Sarah Donegan, PhD Anthony G. Marson, PhD Correspondence to Prof. Marson: A.G.Marson@liverpool.ac.uk
Epilepsy T.I.A. Cataplexy. Nonepileptic seizure. syncope. Dystonia. Epilepsy & other attack disorders Overview
 : Clinical presentation and management Markus Reuber Professor of Clinical Neurology Academic Neurology Unit University of Sheffield, Royal Hallamshire Hospital. Is it epilepsy? Overview Common attack
: Clinical presentation and management Markus Reuber Professor of Clinical Neurology Academic Neurology Unit University of Sheffield, Royal Hallamshire Hospital. Is it epilepsy? Overview Common attack
New AEDs in Uncontrolled seizures
 New AEDs in Uncontrolled seizures Uncontrolled seizures/epilepsy Intractable epilepsy, Refractory epilepsy, Pharmacoresistant epilepsy Dr. Suthida Yenjun Traditionally, referred to therapeutic failure
New AEDs in Uncontrolled seizures Uncontrolled seizures/epilepsy Intractable epilepsy, Refractory epilepsy, Pharmacoresistant epilepsy Dr. Suthida Yenjun Traditionally, referred to therapeutic failure
7/31/09. New AEDs. AEDs. Dr. Yotin Chinvarun M.D. Ph.D. Comprehensive Epilepsy and Sleep disorder Program PMK hospital. 1 st genera*on AEDs
 Dr. Yotin Chinvarun M.D. Ph.D. Comprehensive Epilepsy and Sleep disorder Program PMK hospital New AEDs AEDs NEW OLD Pregabalin Pregabalin 1 st genera*on AEDs Phenytoin Carbamazepine Valproate Phenobarbital
Dr. Yotin Chinvarun M.D. Ph.D. Comprehensive Epilepsy and Sleep disorder Program PMK hospital New AEDs AEDs NEW OLD Pregabalin Pregabalin 1 st genera*on AEDs Phenytoin Carbamazepine Valproate Phenobarbital
CLINICIAN INTERVIEW AS i M: When you examine a clinical trial in new- onset epilepsy, how relevant are the results to your daily clinical practice?
 FROM CLINICAL TRIALS TO CLINICAL PRACTICE: TRANSLATING EPILEPSY RESEARCH INTO PATIENT CARE Interview with Jacqueline A. French, MD Dr Jacqueline A. French is a Professor in the Department of Neurology
FROM CLINICAL TRIALS TO CLINICAL PRACTICE: TRANSLATING EPILEPSY RESEARCH INTO PATIENT CARE Interview with Jacqueline A. French, MD Dr Jacqueline A. French is a Professor in the Department of Neurology
Staging of Seizures According to Current Classification Systems December 10, 2013
 Staging of Seizures According to Current Classification Systems December 10, 2013 Elinor Ben-Menachem, M.D.,Ph.D, Instituet of Clinical Neuroscience and Physiology, Sahlgren Academy, Goteborg University,
Staging of Seizures According to Current Classification Systems December 10, 2013 Elinor Ben-Menachem, M.D.,Ph.D, Instituet of Clinical Neuroscience and Physiology, Sahlgren Academy, Goteborg University,
Ernie Somerville Prince of Wales Hospital EPILEPSY
 Ernie Somerville Prince of Wales Hospital EPILEPSY Overview Classification New and old anti-epileptic drugs (AEDs) Neuropsychiatric side-effects Limbic encephalitis Non-drug therapies Therapeutic wishlist
Ernie Somerville Prince of Wales Hospital EPILEPSY Overview Classification New and old anti-epileptic drugs (AEDs) Neuropsychiatric side-effects Limbic encephalitis Non-drug therapies Therapeutic wishlist
Optimizing Antiepileptic Drug Therapy in Refractory Epilepsy
 15 Optimizing Antiepileptic Drug Therapy in Refractory Epilepsy Nicholas P. Poolos Department of Neurology and UW Regional Epilepsy Center, University of Washington, Seattle, WA, USA Introduction: When
15 Optimizing Antiepileptic Drug Therapy in Refractory Epilepsy Nicholas P. Poolos Department of Neurology and UW Regional Epilepsy Center, University of Washington, Seattle, WA, USA Introduction: When
Epilepsy management What, when and how?
 Epilepsy management What, when and how? J Helen Cross UCL-Institute of Child Health, Great Ormond Street Hospital for Children, London, & National Centre for Young People with Epilepsy, Lingfield, UK What
Epilepsy management What, when and how? J Helen Cross UCL-Institute of Child Health, Great Ormond Street Hospital for Children, London, & National Centre for Young People with Epilepsy, Lingfield, UK What
How to choose/use anti-epileptic drugs wisely? Dr. Chusak Limotai, MD., M.Sc., CSCN(C)
 How to choose/use anti-epileptic drugs wisely? Dr. Chusak Limotai, MD., M.Sc., CSCN(C) Talk overview When to start treatment? Which drug? Monotherapy Combining AEDs (Rational polytherapy) Old AEDs versus
How to choose/use anti-epileptic drugs wisely? Dr. Chusak Limotai, MD., M.Sc., CSCN(C) Talk overview When to start treatment? Which drug? Monotherapy Combining AEDs (Rational polytherapy) Old AEDs versus
Efficacy of Levetiracetam: A Review of Three Pivotal Clinical Trials
 Epilepsia, 42(Suppl. 4):31 35, 2001 Blackwell Science, Inc. International League Against Epilepsy Efficacy of : A Review of Three Pivotal Clinical Trials Michael Privitera University of Cincinnati Medical
Epilepsia, 42(Suppl. 4):31 35, 2001 Blackwell Science, Inc. International League Against Epilepsy Efficacy of : A Review of Three Pivotal Clinical Trials Michael Privitera University of Cincinnati Medical
11/7/2018 EPILEPSY UPDATE. Dr.Ram Sankaraneni. Disclosures. Speaker bureau LivaNova
 EPILEPSY UPDATE Dr.Ram Sankaraneni Disclosures Speaker bureau LivaNova 1 Outline New onset Seizure Investigations in patients with epilepsy Medical management of epilepsy Non Pharmacological options in
EPILEPSY UPDATE Dr.Ram Sankaraneni Disclosures Speaker bureau LivaNova 1 Outline New onset Seizure Investigations in patients with epilepsy Medical management of epilepsy Non Pharmacological options in
TITLE: Pharmacological Treatments in Patients with Epilepsy: Guidelines
 TITLE: Pharmacological Treatments in Patients with Epilepsy: Guidelines DATE: 01 April 2011 RESEARCH QUESTION What are the evidence-based guidelines for pharmacological treatments in patients with epilepsy?
TITLE: Pharmacological Treatments in Patients with Epilepsy: Guidelines DATE: 01 April 2011 RESEARCH QUESTION What are the evidence-based guidelines for pharmacological treatments in patients with epilepsy?
Lacosamide (Vimpat) for partial-onset epilepsy monotherapy. December 2011
 Lacosamide (Vimpat) for partial-onset epilepsy monotherapy This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a
Lacosamide (Vimpat) for partial-onset epilepsy monotherapy This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a
Understanding and Managing Epilepsy
 Page 1 Understanding and Managing Epilepsy Jacquelyn L. Bainbridge, Pharm.D., FCCP Associate Professor University of Colorado Denver School of Pharmacy & Department of Neurology Supported by an educational
Page 1 Understanding and Managing Epilepsy Jacquelyn L. Bainbridge, Pharm.D., FCCP Associate Professor University of Colorado Denver School of Pharmacy & Department of Neurology Supported by an educational
Seizure control with antiepileptic drug therapy in 517 consecutive adult outpatients at the Kork Epilepsy Centre
 Original article Epileptic Disord 2012; 14 (4): 379-87 Seizure control with antiepileptic drug therapy in 517 consecutive adult outpatients at the Kork Epilepsy Centre Bernhard J Steinhoff, Anke Maren
Original article Epileptic Disord 2012; 14 (4): 379-87 Seizure control with antiepileptic drug therapy in 517 consecutive adult outpatients at the Kork Epilepsy Centre Bernhard J Steinhoff, Anke Maren
APPENDIX S. Removed sections from original guideline. 1.1 Pharmacological treatment Introduction
 00 0 APPENDIX S Removed sections from original guideline. Pharmacological treatment.. Introduction The evidence base for the newer AEDs (gabapentin, lamotrigine, levetiracetam, oxcarbazepine, tiagabine,
00 0 APPENDIX S Removed sections from original guideline. Pharmacological treatment.. Introduction The evidence base for the newer AEDs (gabapentin, lamotrigine, levetiracetam, oxcarbazepine, tiagabine,
Appendix M Health Economic Evidence Extractions
 Appendix M Health Economic Evidence Extractions Which AEDs are clinically effective and cost-effective for people with focal epilepsy with or without secondary generalisation seizures? Frew E, Sandercock
Appendix M Health Economic Evidence Extractions Which AEDs are clinically effective and cost-effective for people with focal epilepsy with or without secondary generalisation seizures? Frew E, Sandercock
Evidence for a rapid action of levetiracetam compared to topiramate in refractory partial epilepsy
 Seizure (2006) 15, 112 116 www.elsevier.com/locate/yseiz Evidence for a rapid action of levetiracetam compared to topiramate in refractory partial epilepsy Luigi M. Specchio a,e, *, Giovanni Boero b,e,
Seizure (2006) 15, 112 116 www.elsevier.com/locate/yseiz Evidence for a rapid action of levetiracetam compared to topiramate in refractory partial epilepsy Luigi M. Specchio a,e, *, Giovanni Boero b,e,
levetiracetam 250,500,750 and 1000mg tablets and levetiracetam oral solution 100mg/1ml (Keppra ) (No. 397/07) UCB Pharma Ltd
 Scottish Medicines Consortium Resubmission levetiracetam 250,500,750 and 1000mg tablets and levetiracetam oral solution 100mg/1ml (Keppra ) (No. 397/07) UCB Pharma Ltd 11 January 2008 The Scottish Medicines
Scottish Medicines Consortium Resubmission levetiracetam 250,500,750 and 1000mg tablets and levetiracetam oral solution 100mg/1ml (Keppra ) (No. 397/07) UCB Pharma Ltd 11 January 2008 The Scottish Medicines
Topics. A. Simple partial seizures
 Management of Partial Epilepsy: Focus on Sodium Valproate Asia Pacific Epilepsy Meeting 8 Associate Professor Somsak Tiamkao Division of Neurology, Department of Medicine Srinagarind Epilepsy Research
Management of Partial Epilepsy: Focus on Sodium Valproate Asia Pacific Epilepsy Meeting 8 Associate Professor Somsak Tiamkao Division of Neurology, Department of Medicine Srinagarind Epilepsy Research
Topics. What are Prediction Factors? Seizure type Etiologies Frequency of seizures Response to first AED Genetic?
 Early Recognition and Management of Refractory Epilepsy Topics How to predict who developed refractory epilepsy Associate Professor Somsak Tiamkao Division of Neurology, Department of Medicine Faculty
Early Recognition and Management of Refractory Epilepsy Topics How to predict who developed refractory epilepsy Associate Professor Somsak Tiamkao Division of Neurology, Department of Medicine Faculty
BIBLIOGRAPHIC REFERENCE TABLE FOR SODIUM VALPROATE IN CHILDHOOD EPILEPSY
 BIBLIOGRAPHIC REFERENCE TABLE FOR SODIUM VALPROATE IN CHILDHOOD EPILEPSY Bibliographic Marson AG et al. for (Review). The Cochrane 2000 De Silva M et al. Romised or for childhood. Lancet, 1996; 347: 709-713
BIBLIOGRAPHIC REFERENCE TABLE FOR SODIUM VALPROATE IN CHILDHOOD EPILEPSY Bibliographic Marson AG et al. for (Review). The Cochrane 2000 De Silva M et al. Romised or for childhood. Lancet, 1996; 347: 709-713
Antiepileptics. Medications Comment Quantity Limit Carbamazepine. May be subject Preferred to quantity limit Epitol
 Market DC Antiepileptics Override(s) Approval Duration Prior Authorization 1 year Step Therapy Quantity Limit *Indiana Medicaid See State Specific Mandate below *Maryland Medicaid See State Specific Mandate
Market DC Antiepileptics Override(s) Approval Duration Prior Authorization 1 year Step Therapy Quantity Limit *Indiana Medicaid See State Specific Mandate below *Maryland Medicaid See State Specific Mandate
Opinion 24 July 2013
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 24 July 2013 FYCOMPA 2 mg, film-coated tablet B/7 (CIP: 34009 267 760 0 8) B/28 (CIP: 34009 268 447 4 5) FYCOMPA 4
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 24 July 2013 FYCOMPA 2 mg, film-coated tablet B/7 (CIP: 34009 267 760 0 8) B/28 (CIP: 34009 268 447 4 5) FYCOMPA 4
Stay, Hit, or Fold? What Do You Do If the Treatment May Be as Bad as the Problem Results of a Q-PULSE Survey
 It s Current Epilepsy Resources and Updates Stay, Hit, or Fold? What Do You Do If the Treatment May Be as Bad as the Problem Results of a Q-PULSE Survey Chad Carlson, MD Associate Professor of Neurology,
It s Current Epilepsy Resources and Updates Stay, Hit, or Fold? What Do You Do If the Treatment May Be as Bad as the Problem Results of a Q-PULSE Survey Chad Carlson, MD Associate Professor of Neurology,
Scottish Medicines Consortium
 Scottish Medicines Consortium levetiracetam, 250, 500, 750 and 1000mg tablets and levetiracetam oral solution 100mg/ml (Keppra ) No. (394/07) UCB Pharma Limited 10 August 2007 The Scottish Medicines Consortium
Scottish Medicines Consortium levetiracetam, 250, 500, 750 and 1000mg tablets and levetiracetam oral solution 100mg/ml (Keppra ) No. (394/07) UCB Pharma Limited 10 August 2007 The Scottish Medicines Consortium
SODIUM CHANNEL BLOCKERS IN THE 21 ST CENTURY. Professor Martin J Brodie University of Glasgow Glasgow, Scotland
 IN THE 21 ST CENTURY Professor Martin J Brodie University of Glasgow Glasgow, Scotland Eisai SODIUM CHANNEL BLOCKERS Declaration of interests UCB Pharma GlaxoSmithKline Lundbeck Takeda Advisory board,
IN THE 21 ST CENTURY Professor Martin J Brodie University of Glasgow Glasgow, Scotland Eisai SODIUM CHANNEL BLOCKERS Declaration of interests UCB Pharma GlaxoSmithKline Lundbeck Takeda Advisory board,
Epilepsy for the General Internist
 Epilepsy for the General Internist William O. Tatum DO, FAAN, FACNS Professor of Neurology Mayo College of Medicine Senior Consultant, Mayo Clinic Florida Director, Epilepsy Center and Monitoring Unit
Epilepsy for the General Internist William O. Tatum DO, FAAN, FACNS Professor of Neurology Mayo College of Medicine Senior Consultant, Mayo Clinic Florida Director, Epilepsy Center and Monitoring Unit
Levetiracetam monotherapy in juvenile myoclonic epilepsy
 Seizure (2008) 17, 64 68 www.elsevier.com/locate/yseiz Levetiracetam monotherapy in juvenile myoclonic epilepsy Deron V. Sharpe *, Anup D. Patel, Bassel Abou-Khalil, Gerald M. Fenichel Vanderbilt University
Seizure (2008) 17, 64 68 www.elsevier.com/locate/yseiz Levetiracetam monotherapy in juvenile myoclonic epilepsy Deron V. Sharpe *, Anup D. Patel, Bassel Abou-Khalil, Gerald M. Fenichel Vanderbilt University
The Epilepsy Prescriber s Guide to Antiepileptic Drugs
 The Epilepsy Prescriber s Guide to Antiepileptic Drugs The Epilepsy Prescriber s Guide to Antiepileptic Drugs Philip N. Patsalos FRCPath, PhD Professor of Clinical Pharmacology and Consultant Clinical
The Epilepsy Prescriber s Guide to Antiepileptic Drugs The Epilepsy Prescriber s Guide to Antiepileptic Drugs Philip N. Patsalos FRCPath, PhD Professor of Clinical Pharmacology and Consultant Clinical
APPENDIX K Pharmacological Management
 1 2 3 4 APPENDIX K Pharmacological Management Table 1 AED options by seizure type Table 1 AED options by seizure type Seizure type First-line AEDs Adjunctive AEDs Generalised tonic clonic Lamotrigine Oxcarbazepine
1 2 3 4 APPENDIX K Pharmacological Management Table 1 AED options by seizure type Table 1 AED options by seizure type Seizure type First-line AEDs Adjunctive AEDs Generalised tonic clonic Lamotrigine Oxcarbazepine
eslicarbazepine acetate 800mg tablet (Zebinix) SMC No. (592/09) Eisai Ltd
 eslicarbazepine acetate 800mg tablet (Zebinix) SMC No. (592/09) Eisai Ltd 8 October 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises NHS Boards
eslicarbazepine acetate 800mg tablet (Zebinix) SMC No. (592/09) Eisai Ltd 8 October 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises NHS Boards
8/30/10. How to use Antiepileptic drugs properly. 3nd generation AEDs. Introduction. Introduction. Introduction. AEDs. Dr.Yotin Chinvarun M.D., Ph.D.
 Introduction How to use Antiepileptic drugs properly Modern treatment of seizures started in 1850 with the introduction of bromides, based on the theory that epilepsy was caused by an excessive sex drive
Introduction How to use Antiepileptic drugs properly Modern treatment of seizures started in 1850 with the introduction of bromides, based on the theory that epilepsy was caused by an excessive sex drive
Epilepsy: problems of diagnosis and recommended treatment Nicola Cooper MRCP and Morgan Feely MD, FRCP, FRCP(I)
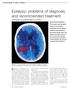 Epilepsy: problems of diagnosis and recommended treatment Nicola Cooper MRCP and Morgan Feely MD, FRCP, FRCP(I) VM Our series Prescribing in gives practical advice for successful management of the special
Epilepsy: problems of diagnosis and recommended treatment Nicola Cooper MRCP and Morgan Feely MD, FRCP, FRCP(I) VM Our series Prescribing in gives practical advice for successful management of the special
New generation antiepileptic drugs: what do they offer in terms of improved tolerability and safety?
 Therapeutic Advances in Drug Safety Review New generation antiepileptic drugs: what do they offer in terms of improved tolerability and safety? Ther Adv Drug Saf (2011) 2(4) 141 158 DOI: 10.1177/ 2042098611411127!
Therapeutic Advances in Drug Safety Review New generation antiepileptic drugs: what do they offer in terms of improved tolerability and safety? Ther Adv Drug Saf (2011) 2(4) 141 158 DOI: 10.1177/ 2042098611411127!
Chronic Management of Idiopathic Generalized epilepsies (IGE) Hassan S.Hosny M.D. Prof of Neurology, Cairo University
 Chronic Management of Idiopathic Generalized epilepsies (IGE) Hassan S.Hosny M.D. Prof of Neurology, Cairo University Sanaa 2009 Points of Discussion Prevalence compared to focal epilepsy Adult form Status
Chronic Management of Idiopathic Generalized epilepsies (IGE) Hassan S.Hosny M.D. Prof of Neurology, Cairo University Sanaa 2009 Points of Discussion Prevalence compared to focal epilepsy Adult form Status
For patients with epilepsy and the neurologists who treat them, the primary goal
 38 Practical Neurology October 2008 A specialist answers the common question, My patient is seizure-free now what do I do? By Carl W. Bazil, MD, PhD For patients with epilepsy and the neurologists who
38 Practical Neurology October 2008 A specialist answers the common question, My patient is seizure-free now what do I do? By Carl W. Bazil, MD, PhD For patients with epilepsy and the neurologists who
Network meta-analysis of pharmacological interventions in the treatment of epilepsy
 APPENDIX O Network meta-analysis of pharmacological interventions in the treatment of epilepsy 0 0. Introduction The results of conventional meta-analyses of direct evidence alone (as presented in the
APPENDIX O Network meta-analysis of pharmacological interventions in the treatment of epilepsy 0 0. Introduction The results of conventional meta-analyses of direct evidence alone (as presented in the
Epilepsy. Annual Incidence. Adult Epilepsy Update
 Adult Epilepsy Update Annual Incidence J. Layne Moore, MD, MPH Associate Professor Department of Neurology and Pharmacy Director, Division of Epilepsy The Ohio State University Used by permission Health
Adult Epilepsy Update Annual Incidence J. Layne Moore, MD, MPH Associate Professor Department of Neurology and Pharmacy Director, Division of Epilepsy The Ohio State University Used by permission Health
London, 07 August 2006 Product name: Keppra Procedure No. EMEA/H/C/277/II/63 SCIENTIFIC DISCUSSION
 London, 07 August 2006 Product name: Keppra Procedure No. EMEA/H/C/277/II/63 SCIENTIFIC DISCUSSION 1/15 EMEA 2006 1. Introduction Epilepsy is one of the most common and challenging neurological disorders.
London, 07 August 2006 Product name: Keppra Procedure No. EMEA/H/C/277/II/63 SCIENTIFIC DISCUSSION 1/15 EMEA 2006 1. Introduction Epilepsy is one of the most common and challenging neurological disorders.
Research Article Efficacy and Safety of Levetiracetam and Carbamazepine as Monotherapy in Partial Seizures
 Hindawi Publishing Corporation Epilepsy Research and Treatment Volume 2015, Article ID 415082, 6 pages http://dx.doi.org/10.1155/2015/415082 Research Article Efficacy and Safety of Levetiracetam and Carbamazepine
Hindawi Publishing Corporation Epilepsy Research and Treatment Volume 2015, Article ID 415082, 6 pages http://dx.doi.org/10.1155/2015/415082 Research Article Efficacy and Safety of Levetiracetam and Carbamazepine
Updated advice for nurses who care for patients with epilepsy
 NICE BULLETIN Updated advice for nurses who care for patients with epilepsy NICE provided the content for this booklet which is independent of any company or product advertised NICE BULLETIN Updated advice
NICE BULLETIN Updated advice for nurses who care for patients with epilepsy NICE provided the content for this booklet which is independent of any company or product advertised NICE BULLETIN Updated advice
Neuromuscular Disease(2) Epilepsy. Department of Pediatrics Soochow University Affiliated Children s Hospital
 Neuromuscular Disease(2) Epilepsy Department of Pediatrics Soochow University Affiliated Children s Hospital Seizures (p130) Main contents: 1) Emphasize the clinical features of epileptic seizure and epilepsy.
Neuromuscular Disease(2) Epilepsy Department of Pediatrics Soochow University Affiliated Children s Hospital Seizures (p130) Main contents: 1) Emphasize the clinical features of epileptic seizure and epilepsy.
Evidence-Based Guideline: Management of an Unprovoked First Seizure in Adults
 It s Current Epilepsy Resources and Updates Evidence-Based Guideline: Management of an Unprovoked First Seizure in Adults Report of the Guideline Development Subcommittee of the American Academy of Neurology
It s Current Epilepsy Resources and Updates Evidence-Based Guideline: Management of an Unprovoked First Seizure in Adults Report of the Guideline Development Subcommittee of the American Academy of Neurology
Introduction to seizures and epilepsy
 Introduction to seizures and epilepsy Selim R. Benbadis, M.D. Professor Departments of Neurology & Neurosurgery Director, Comprehensive Epilepsy Program Symptomatic seizures Head injury (trauma) Stroke
Introduction to seizures and epilepsy Selim R. Benbadis, M.D. Professor Departments of Neurology & Neurosurgery Director, Comprehensive Epilepsy Program Symptomatic seizures Head injury (trauma) Stroke
Epilepsy and EEG in Clinical Practice
 Mayo School of Professional Development Epilepsy and EEG in Clinical Practice November 10-12, 2016 Hard Rock Hotel at Universal Orlando Orlando, FL Course Directors Jeffrey Britton, MD and William Tatum,
Mayo School of Professional Development Epilepsy and EEG in Clinical Practice November 10-12, 2016 Hard Rock Hotel at Universal Orlando Orlando, FL Course Directors Jeffrey Britton, MD and William Tatum,
Epilepsy Martin J Brodie, Steven C Schachter, Patrick Kwan Fourth edition
 Fast Facts Fast Facts: Epilepsy Martin J Brodie, Steven C Schachter, Patrick Kwan Fourth edition Fast Facts Fast Facts: Epilepsy Fourth edition Martin J Brodie MB ChB MRCP MD FRCP Director, Epilepsy Unit
Fast Facts Fast Facts: Epilepsy Martin J Brodie, Steven C Schachter, Patrick Kwan Fourth edition Fast Facts Fast Facts: Epilepsy Fourth edition Martin J Brodie MB ChB MRCP MD FRCP Director, Epilepsy Unit
Epilepsy Therapy Symposium What You Need to Know to Get Your Patients Into the 65% Group
 Epilepsy Therapy Symposium What You Need to Know to Get Your Patients Into the 65% Group Symposium Co-Chairs: Cynthia Harden, M.D. and Jerry Shih, M.D. Saturday, December 5, 215 Convention Center Grand
Epilepsy Therapy Symposium What You Need to Know to Get Your Patients Into the 65% Group Symposium Co-Chairs: Cynthia Harden, M.D. and Jerry Shih, M.D. Saturday, December 5, 215 Convention Center Grand
Levetiracetam in patients with generalised epilepsy and myoclonic seizures: An open label study
 Seizure (2006) 15, 214 218 www.elsevier.com/locate/yseiz CASE REPORT Levetiracetam in patients with generalised epilepsy and myoclonic seizures: An open label study Angelo Labate a,b, Eleonora Colosimo
Seizure (2006) 15, 214 218 www.elsevier.com/locate/yseiz CASE REPORT Levetiracetam in patients with generalised epilepsy and myoclonic seizures: An open label study Angelo Labate a,b, Eleonora Colosimo
Disclosures. AED Options. Epilepsy Pharmacotherapy: Treatment Considerations with Older AEDs
 Epilepsy Pharmacotherapy: Treatment Considerations with Older AEDs BARRY E. GIDAL, PHARMD PROFESSOR SCHOOL OF PHARMACY & DEPT. OF NEUROLOGY Disclosures Speaking honoraria: UCB, Eisai, Sunovion Consultant:
Epilepsy Pharmacotherapy: Treatment Considerations with Older AEDs BARRY E. GIDAL, PHARMD PROFESSOR SCHOOL OF PHARMACY & DEPT. OF NEUROLOGY Disclosures Speaking honoraria: UCB, Eisai, Sunovion Consultant:
Review of Anticonvulsant Medications: Traditional and Alternative Uses. Andrea Michel, PharmD, CACP
 Review of Anticonvulsant Medications: Traditional and Alternative Uses Andrea Michel, PharmD, CACP Objectives Review epidemiology of epilepsy Classify types of seizures Discuss non-pharmacologic and pharmacologic
Review of Anticonvulsant Medications: Traditional and Alternative Uses Andrea Michel, PharmD, CACP Objectives Review epidemiology of epilepsy Classify types of seizures Discuss non-pharmacologic and pharmacologic
Seizure outcome after switching antiepileptic drugs: A matched, prospective study.
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 8-2016 Seizure outcome after switching antiepileptic drugs: A matched, prospective study.
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 8-2016 Seizure outcome after switching antiepileptic drugs: A matched, prospective study.
Management of Epilepsy in Primary Care and the Community. Carrie Burke, Epilepsy Specialist Nurse
 Management of Epilepsy in Primary Care and the Community Carrie Burke, Epilepsy Specialist Nurse Epilepsy & Seizures Epilepsy is a common neurological disorder characterised by recurring seizures (NICE,
Management of Epilepsy in Primary Care and the Community Carrie Burke, Epilepsy Specialist Nurse Epilepsy & Seizures Epilepsy is a common neurological disorder characterised by recurring seizures (NICE,
The Selection of Antiepileptic Drugs for the Treatment of Epilepsy in Children and Adults
 The Selection of Antiepileptic Drugs for the Treatment of Epilepsy in Children and Adults Jorge J. Asconape, MD KEYWORDS Epilepsy Seizures Antiepileptic drugs Epilepsy is one of the most common chronic
The Selection of Antiepileptic Drugs for the Treatment of Epilepsy in Children and Adults Jorge J. Asconape, MD KEYWORDS Epilepsy Seizures Antiepileptic drugs Epilepsy is one of the most common chronic
Epilepsy: pharmacological treatment by seizure type. Clinical audit tool. Implementing NICE guidance
 Epilepsy: pharmacological treatment by seizure type Clinical audit tool Implementing NICE guidance 2012 NICE clinical guideline 137 Clinical audit tool: Epilepsy (2012) Page 1 of 25 This clinical audit
Epilepsy: pharmacological treatment by seizure type Clinical audit tool Implementing NICE guidance 2012 NICE clinical guideline 137 Clinical audit tool: Epilepsy (2012) Page 1 of 25 This clinical audit
Improving trial methodology: Examples from epilepsy. Tony Marson University of Liverpool
 Improving trial methodology: Examples from epilepsy Tony Marson University of Liverpool This talk Examples of trial methodology research Focus on epilepsy but Examples are relevant to any field Epilepsy
Improving trial methodology: Examples from epilepsy Tony Marson University of Liverpool This talk Examples of trial methodology research Focus on epilepsy but Examples are relevant to any field Epilepsy
Pohlmann-Eden et al. BMC Neurology (2016) 16:149 DOI /s
 Pohlmann-Eden et al. BMC Neurology (16) 16:149 DOI.1186/s12883-16-663-7 RESEARCH ARTICLE Open Access Comparative effectiveness of levetiracetam, valproate and carbamazepine among elderly patients with
Pohlmann-Eden et al. BMC Neurology (16) 16:149 DOI.1186/s12883-16-663-7 RESEARCH ARTICLE Open Access Comparative effectiveness of levetiracetam, valproate and carbamazepine among elderly patients with
2 nd Line Treatments for Dravet. Eric BJ Ségal, MD Northeast Regional Epilepsy Group
 2 nd Line Treatments for Dravet Eric BJ Ségal, MD Northeast Regional Epilepsy Group Disclosures Accepted honoraria from Greenwich Pharmaceuticals, Zogenix, Eisai, Lundbeck, Lineagen. Overview Evidence
2 nd Line Treatments for Dravet Eric BJ Ségal, MD Northeast Regional Epilepsy Group Disclosures Accepted honoraria from Greenwich Pharmaceuticals, Zogenix, Eisai, Lundbeck, Lineagen. Overview Evidence
Seizures in Children: Laboratory
 Article neurology Seizures in Children: Laboratory Diagnosis and Management Philippe Major, MD,* Elizabeth A. Thiele, MD, PhD* Objectives After completing this article, readers should be able to: 1. Formulate
Article neurology Seizures in Children: Laboratory Diagnosis and Management Philippe Major, MD,* Elizabeth A. Thiele, MD, PhD* Objectives After completing this article, readers should be able to: 1. Formulate
Objective: To provide evidence-based recommendations for treatment of adults with an unprovoked first seizure.
 SPECIAL ARTICLE Evidence-based guideline: Management of an unprovoked first seizure in adults Report of the Guideline Development Subcommittee of the American Academy of Neurology and the American Epilepsy
SPECIAL ARTICLE Evidence-based guideline: Management of an unprovoked first seizure in adults Report of the Guideline Development Subcommittee of the American Academy of Neurology and the American Epilepsy
New antiepileptic drugs
 Chapter 29 New antiepileptic drugs J.W. SANDER UCL Institute of Neurology, University College London, National Hospital for Neurology and Neurosurgery, Queen Square, London, and Epilepsy Society, Chalfont
Chapter 29 New antiepileptic drugs J.W. SANDER UCL Institute of Neurology, University College London, National Hospital for Neurology and Neurosurgery, Queen Square, London, and Epilepsy Society, Chalfont
LMMG New Medicine Recommendation
 LMMG New Medicine Recommendation Oxcarbazepine (Trileptal ) for the treatment of epilepsy LMMG Recommendation: Amber 0: Oxcarbazepine (Trileptal ) is recommended for use as monotherapy or adjunctive therapy
LMMG New Medicine Recommendation Oxcarbazepine (Trileptal ) for the treatment of epilepsy LMMG Recommendation: Amber 0: Oxcarbazepine (Trileptal ) is recommended for use as monotherapy or adjunctive therapy
Long-term effect of antiepileptic drug switch on serum lipids and C-reactive protein.
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 5-1-2016 Long-term effect of antiepileptic drug switch on serum lipids and C-reactive
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 5-1-2016 Long-term effect of antiepileptic drug switch on serum lipids and C-reactive
New Drug Evaluation: brivaracetam [tablet and solution, oral; solution, intravenous]
![New Drug Evaluation: brivaracetam [tablet and solution, oral; solution, intravenous] New Drug Evaluation: brivaracetam [tablet and solution, oral; solution, intravenous]](/thumbs/77/75213643.jpg) Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Seizure medications An overview
 Seizure medications An overview Andrew Zillgitt, DO Staff Neurologist Comprehensive Epilepsy Center Department of Neurology Henry Ford Hospital None Disclosures Objectives A lot to review!!!!! Look at
Seizure medications An overview Andrew Zillgitt, DO Staff Neurologist Comprehensive Epilepsy Center Department of Neurology Henry Ford Hospital None Disclosures Objectives A lot to review!!!!! Look at
TRANSPARENCY COMMITTEE OPINION. 19 July 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 19 July 2006 Keppra 250 mg, film-coated tablets Box of 60 tablets (CIP code: 356 013-6) Keppra 500 mg, film-coated
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 19 July 2006 Keppra 250 mg, film-coated tablets Box of 60 tablets (CIP code: 356 013-6) Keppra 500 mg, film-coated
Epilepsy 101. Overview of Treatment Kathryn A. O Hara RN. American Epilepsy Society
 Epilepsy 101 Overview of Treatment Kathryn A. O Hara RN American Epilepsy Society Objectives Describe the main treatment options for epilepsy Identify factors essential in the selection of appropriate
Epilepsy 101 Overview of Treatment Kathryn A. O Hara RN American Epilepsy Society Objectives Describe the main treatment options for epilepsy Identify factors essential in the selection of appropriate
Prescribing and Monitoring Anti-Epileptic Drugs
 Prescribing and Monitoring Anti-Epileptic Drugs Mark Granner, MD Clinical Professor and Vice Chair for Clinical Programs Director, Iowa Comprehensive Epilepsy Program Department of Neurology University
Prescribing and Monitoring Anti-Epileptic Drugs Mark Granner, MD Clinical Professor and Vice Chair for Clinical Programs Director, Iowa Comprehensive Epilepsy Program Department of Neurology University
New Medicines Profile
 New Medicines Profile February 2010 Issue No. 10/02 Eslicarbazepine Concise evaluated information to support the managed entry of new medicines in the NHS Brand Name, (Manufacturer): Zebinix (Eisai Limited)
New Medicines Profile February 2010 Issue No. 10/02 Eslicarbazepine Concise evaluated information to support the managed entry of new medicines in the NHS Brand Name, (Manufacturer): Zebinix (Eisai Limited)
Advances in the diagnosis and management of epilepsy in adults
 n DRUG REVIEW Advances in the diagnosis and management of epilepsy in adults Diego Kaski MRCP, PhD and Charles Cockerell MD, FRCP SPL This drug review looks at the key issues in diagnosing epilepsy, initiating
n DRUG REVIEW Advances in the diagnosis and management of epilepsy in adults Diego Kaski MRCP, PhD and Charles Cockerell MD, FRCP SPL This drug review looks at the key issues in diagnosing epilepsy, initiating
p ผศ.นพ.ร งสรรค ช ยเสว ก ล คณะแพทยศาสตร ศ ร ราชพยาบาล
 Natural Course and Prognosis of Epilepsy p ผศ.นพ.ร งสรรค ช ยเสว ก ล คณะแพทยศาสตร ศ ร ราชพยาบาล Introduction Prognosis of epilepsy generally means probability of being seizure-free after starting treatment
Natural Course and Prognosis of Epilepsy p ผศ.นพ.ร งสรรค ช ยเสว ก ล คณะแพทยศาสตร ศ ร ราชพยาบาล Introduction Prognosis of epilepsy generally means probability of being seizure-free after starting treatment
EPILEPSY: SPECTRUM OF CHANGE WITH AGE. Gail D. Anderson, Ph.D.
 EPILEPSY: SPECTRUM OF CHANGE WITH AGE Gail D. Anderson, Ph.D. Incidence: 0.5% - 1.0% of U.S. population Peak incidence of onset: first 2 years of life, ages 5-7 years, early puberty and elderly. 125,000
EPILEPSY: SPECTRUM OF CHANGE WITH AGE Gail D. Anderson, Ph.D. Incidence: 0.5% - 1.0% of U.S. population Peak incidence of onset: first 2 years of life, ages 5-7 years, early puberty and elderly. 125,000
Refractory epilepsy: treatment with new antiepileptic drugs
 Seizure 2000; 9: 51 57 doi: 10.1053/seiz.1999.0348, available online at http://www.idealibrary.com on Refractory epilepsy: treatment with new antiepileptic drugs P. K. DATTA & P. M. CRAWFORD Department
Seizure 2000; 9: 51 57 doi: 10.1053/seiz.1999.0348, available online at http://www.idealibrary.com on Refractory epilepsy: treatment with new antiepileptic drugs P. K. DATTA & P. M. CRAWFORD Department
