Seizures are a common medical emergency,
|
|
|
- Alaina Terry
- 5 years ago
- Views:
Transcription
1 PROGRESSIVE CLINICAL PRACTICE Midazolam Versus Diazepam for the Treatment of Status Epilepticus in Children and Young Adults: A Meta-analysis Jason McMullan, MD, Comilla Sasson, MD, Arthur Pancioli, MD, and Robert Silbergleit, MD Abstract Background: Rapid treatment of status epilepticus (SE) is associated with better outcomes. Diazepam and midazolam are commonly used, but the optimal agent and administration route is unclear. Objectives: The objective was to determine by systematic review if nonintravenous (non-iv) midazolam is as effective as diazepam, by any route, in terminating SE seizures in children and adults. Time to seizure cessation and respiratory complications was examined. Methods: We performed a search of PubMed, Web of Knowledge, Embase, Cochrane Database of Systematic Reviews, Database of Abstracts of Reviews of Effects, American College of Physicians Journal Club, Cochrane Central Register of Controlled Trials, the Cumulative Index to Nursing and Allied Health Literature, and International Pharmaceutical Abstracts for studies published January 1, 1950, through July 4, English language quasi-experimental or randomized controlled trials comparing midazolam and diazepam as first-line treatment for SE, and meeting the Consolidated Standards of Reporting Trials (CONSORT)-based quality measures, were eligible. Two reviewers independently screened studies for inclusion and extracted outcomes data. Administration routes were stratified as non-iv (buccal, intranasal, intramuscular, rectal) or IV. Fixed-effects models generated pooled statistics. Results: Six studies with 774 subjects were included. For seizure cessation, midazolam, by any route, was superior to diazepam, by any route (relative risk [RR] = 1.52; 95% confidence interval [CI] = 1.27 to 1.82). Non-IV midazolam is as effective as IV diazepam (RR = 0.79; 95% CI = 0.19 to 3.36), and buccal midazolam is superior to rectal diazepam in achieving seizure control (RR = 1.54; 95% CI = 1.29 to 1.85). Midazolam was administered faster than diazepam (mean difference = 2.46 minutes; 95% CI = 1.52 to 3.39 minutes) and had similar times between drug administration and seizure cessation. Respiratory complications requiring intervention were similar, regardless of administration route (RR = 1.49; 95% CI = 0.25 to 8.72). Conclusions: Non-IV midazolam, compared to non-iv or IV diazepam, is safe and effective in treating SE. Comparison to lorazepam, evaluation in adults, and prospective confirmation of safety and efficacy is needed. ACADEMIC EMERGENCY MEDICINE 2010; 17: ª 2010 by the Society for Academic Emergency Medicine Keywords: status epilepticus, seizures, benzodiazepines, midazolam, diazepam From the Department of Emergency Medicine, University of Cincinnati (JM, AP), Cincinnati, OH; and the Department of Emergency Medicine, University of Michigan (CS, RS), Ann Arbor, MI. Received October 2, 2009; revision received November 24, 2009; accepted November 25, This work was presented at the Society for Academic Emergency Medicine annual meeting, New Orleans, LA, May 2009, and was awarded Best Fellow Presentation. This publication was supported by an Institutional Clinical and Translational Science Award, NIH NCRR Grant 1UL1RR Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIH. This work was also supported in part by NIH Grant 5U01NS Address for correspondence: Jason McMullan, MD; mcmulljo@ucmail.uc.edu. Reprints will not be available. Seizures are a common medical emergency, accounting for 1% 2% of all emergency department (ED) visits, and status epilepticus (SE) exists in approximately 6% of these encounters. 1 However, the optimal agent and route of administration for the treatment of SE remain unclear. Almost 1 in 10 persons will suffer at least one seizure in their lifetime. 2 While most seizures are self-limited and short, every year 120,000 to 200,000 people have prolonged convulsions or rapidly recurrent convulsions without interval recovery, and these patients in SE have a true medical emergency. 3,4 SE is associated with high morbidity and mortality and contributes to 55,000 deaths each year in the United States. 5 8 Common complications of SE include aspiration, anoxic brain injury, cardiac instability, metabolic and autonomic dysfunction, and direct neuronal damage ª 2010 by the Society for Academic Emergency Medicine ISSN doi: /j x PII ISSN
2 576 McMullan et al. MIDAZOLAM VS. DIAZEPAM IN STATUS SEIZURES Although clinical outcome in SE is primarily determined by the underlying etiology that caused the seizure, persistent seizure activity is associated with worse outcomes across the spectrum of precipitating conditions In otherwise benign epilepsy, refractory SE can still be fatal or result in neuronal injury and chronic brain damage. In SE resulting from acute trauma or stroke, persistent ictal activity is associated with increased secondary neuronal cell death and worse outcomes. 20 Although duration of seizure is associated with higher mortality and worse neurologic recovery in survivors in clinical studies, these data do not provide rigorous proof of causality. However, studies of experimental SE in animal models directly demonstrate that neuronal loss increases with duration of seizure and that kindling effects from persistent seizures are epileptogenic. 19,21 Experimental status models also show that the effectiveness of anticonvulsant medications to terminate seizures rapidly decreases as the time between the start of convulsions and drug administration lengthens. 22 If seizures are not terminated quickly, escalating doses of benzodiazepines are required to achieve seizure cessation, and seizures eventually become entirely refractory to anticonvulsant therapy. 23 Benzodiazepines have been the first-line treatment of SE for the past 30 years, but the optimal drug and the best route of administration for seizure control outside of the hospital setting, or without intravenous (IV) access, remains unclear. Lorazepam is a clinical standard for initial treatment of SE in EDs. 24,25 While shown to be safe for use by paramedics, lorazepam has a relatively short shelf life without refrigeration, limiting its practicality in the prehospital setting. 26 Furthermore, lorazepam is only effective when given IV, and establishing IV access can be challenging, if not impossible, in convulsing patients Diazepam is frequently used for treatment of SE, because it can be delivered either intravenously or rectally. 26,27 However, the effectiveness of diazepam in terminating seizures is thought to be inferior to that of other benzodiazepines, especially when given rectally. 25 Additionally, diazepam is suspected to cause more complications than other benzodiazepines because of the risk for prolonged sedation and respiratory depression. 26,29 Midazolam is rapidly absorbed after intramuscular (IM) injection, does not require refrigeration, and is less expensive than lorazepam. 30 Requiring IV access before benzodiazepine administration may unnecessarily delay treatment of SE, placing the patient at risk, even when done in the ED. Non-IV midazolam administration for treatment of SE is an attractive idea, but there are few studies of its efficacy and safety. 31 A recent Cochrane Review explored benzodiazepine treatment of pediatric SE and included many different medication strategies. 32 Important secondary outcomes, including time required for administration of medication and time to therapeutic effect, were not described, and the review did not include studies addressing out-of-hospital management of SE. This meta-analysis compares the use of non-iv midazolam to that of diazepam in the treatment of seizures. The specific objective was to determine the efficacy, rapidity, and safety of terminating seizures with non-iv midazolam, compared to either IV or non-iv diazepam, as an initial emergency treatment in pediatric and adult patients with SE. METHODS Data Sources and Search Strategy A systematic review of the literature was conducted to identify studies comparing the use of non-iv midazolam to IV or non-iv diazepam in treating SE in pediatric and adult patients. For the purposes of this analysis, seizures lasting longer than 5 minutes are defined as SE, as has been suggested elsewhere. 26,33 The following electronic databases were searched: PubMed, Web of Knowledge, Embase, all evidence-based medicine reviews (includes Cochrane Database of Systematic Reviews, Database of Abstracts of Reviews of Effects, American College of Physicians Journal Club, and Cochrane Central Register of Controlled Trials), the Cumulative Index to Nursing and Allied Health Literature (CINAHL), and International Pharmaceutical Abstracts. All studies published or in press between January 1, 1950, and July 4, 2009, were considered. Only reports published in English were included. The majority of articles were retrieved from PubMed and Web of Knowledge using a Boolean search strategy (Appendix 1). In addition to these automated searches, we conducted a hand search of bibliographies of key articles and abstracts presented at several major scientific conferences in 2006 through These included the annual meetings of the American College of Emergency Physicians, the American Neurological Association, the National Association of EMS Physicians, and the Society for Academic Emergency Medicine. Finally, references of key review articles were hand searched for other relevant articles. Selection Criteria Two reviewers (CS, RS) evaluated each full-text article and determined exclusions based on a priori criteria to ensure the comparability of the groups and to allow for pooling of results. These criteria excluded any study that did not compare diazepam to non-iv administration of midazolam as a first-line treatment for SE, animal studies, any study design other than randomized controlled or quasi-experimental, and any study that used diazepam or midazolam for sedation or prevention of seizures (Figure 1). Initial disagreements between reviewers regarding study inclusion were resolved by consensus. Data Extraction and Quality Assessment Studies that met our preliminary selection criteria were further evaluated by two independent reviewers (CS, JM) using the Consolidated Standards of Reporting Trials (CONSORT) Quality Scale and the Randomized Controlled Trial (RCT) Checklist. 34 The CONSORT Quality Scale has been shown to be useful in determining the methodologic quality of randomized clinical trials in a standardized format. 34 The 30-point scale assigns points for studies that report key concepts on randomization, allocation concealment, repeatability of observations, etc., and serves as a balance to the quality of writing to
3 ACAD EMERG MED June 2010, Vol. 17, No Citations: 62 PubMed, 124 Web of Knowledge, 15 Embase, 20 All EBM reviews, 16 CINAHL, 14 International Pharm Abstracts 157 Articles excluded after screening of titles and abstracts 30 Articles excluded for: not RCT (6), not including original data (5), no comparison group (7), not being acute status epilepticus (7), and for not comparing the two medications (5) 44 Potentially relevant articles for full text review 14 Full text articles screened in detail CONSORT Checklist for quality applied 8 Articles excluded for not meeting quality criteria (CONSORT score <20) 6 Articles included for pooled analysis Figure 1. Search strategy for articles reviewed for meta-analysis. CONSORT = Consolidated Standards of Reporting Trials; CINAHL = Cumulative Index to Nursing and Allied Health Literature; EBM = evidence-based medicine; RCT = randomized controlled trial. judge the strength and validity of findings. An a priori threshold score of at least 20 was established for inclusion. The RCT Checklist serves as a way to abstract data on specific interventions and to further assess key components of study design. The following variables were extracted from the studies: type of study design, definition of SE, types of complications reported, absolute numbers of patients in the diazepam and the midazolam groups that had seizure activity terminated, route of administration, and dosage of drug administered. Data Analysis Study inclusion agreement between investigators was evaluated by kappa statistics. Pooled risk ratios were determined using both the Mantel-Haenszel fixed effects and DerSimonian and Laird random-effects models. 35 Data were stratified into two subgroups, one comparing IV diazepam versus non-iv midazolam, and the other comparing non-iv diazepam to non-iv midazolam. Where study data were available, we assessed the mean differences in times between initial assessment and drug administration and between drug administration and cessation of seizure activity based on route of administration. A fixed-effects model was used to pool times across studies. Heterogeneity within the group was assessed using Cochran s Q-test and I 2 statistic, which measures the degree of variation among studies. 36 Begg s test and a visual inspection of the funnel plot were conducted to evaluate publication bias. All statistical tests were twosided. Stata version 10.0 (StataCorp., College Station, TX) and Review Manager 5.0 (RevMan, Copenhagen, Denmark; The Nordic Cochrane Centre, The Cochrane Collaboration, 2008) were used to conduct the analyses. A meta-influence analysis was conducted to statistically omit one study at a time to determine the effect on the overall pooled estimate. A sensitivity analysis was performed to assess the effect of removing the most influential study from the pooled subgroup results. RESULTS Search and Study Characteristics The initial literature search yielded 251 references, of which 44 met preliminary selection criteria for inclusion within the meta-analysis (Figure 1). Four authors were contacted to clarify the comparability of groups, to obtain more data, or to clarify definitions of SE. Thirtyeight articles were excluded because trial design was not randomized or controlled (n =6); data included were not original (n =5); there was no comparison group (n =7); acute SE was not described (n =7); the two drugs chosen for this review were not utilized (n =5); and the CONSORT score was <20 (n =8). 34 The kappa for interrater reliability for inclusion into the study was The characteristics of the six studies included studies containing 774 subjects are shown in Table 1, and all are RCTs. Although the intent of our analysis was to include all age groups, all of the studies meeting the selection criteria happened to be studies of children and young adults. Five studies included children only; one study included children and adults; however, the oldest subject was 22 years old. 42 Routes of medication administration included IV and rectal (PR) diazepam and buccal, intranasal (IN), and IM midazolam. Dosing of medications varied slightly among studies: diazepam mg kg IV or 0.5 mg kg PR or midazolam 0.2 mg kg IM and IN or 0.5 mg kg buccal. One study used fixed doses of PR diazepam (10 mg) and buccal midazolam (10 mg). 42 The determination of seizure cessation was clinically based and used varying definitions based on time until convulsion stoppage and or absence of seizure recurrence. Some studies included prolonged simple partial or focal convulsions. 37,39,41,42 Despite these clinical and methodologic differences, there was no significant statistical heterogeneity in pooled analysis of all included studies (I 2 = 0%, Figure 2). Seizure Cessation Midazolam, by any route, was superior to diazepam, by any route, in achieving seizure cessation in pooled analysis (relative risk [RR] = 1.52; 95% confidence interval [CI] = 1.27 to 1.82, n=6, number needed to treat [NNT] = 7; Figure 2). Three studies of 146 subjects compared IM or IN midazolam to IV diazepam. In pooled analysis, there
4 578 McMullan et al. MIDAZOLAM VS. DIAZEPAM IN STATUS SEIZURES Table 1 Characteristics of Included Studies Study, yr n Age Range Diazepam Dose Route Midazolam Dose Route Definition of Status Chamberlain et al., months 18 yr 0.3 mg kg IV 0.2 mg kg IM Seizing >10 minutes Lahat et al., months 5 yr 0.3 mg kg IV 0.2 mg kg IN Seizing >10 minutes Mahmoudian et al., months 15 yr 0.2 mg kg IV 0.2 mg kg IN Seizing at arrival to ED McIntyre et al., months 15 yr 0.5 mg kg PR 0.5 mg kg buccal Seizing at arrival to ED Mpimbaza et al., months 12 yr 0.5 mg kg PR 0.5 mg kg buccal Seizing at arrival to ED or >5 minutes Scott et al., yr 10 mg PR 10 mg buccal Seizing >5 minutes CONSORT = Consolidated Standards of Reporting Trials; IM = intramuscular; IN = intranasal; IV = intravenous; PR = per rectum. Figure 2. Diazepam versus midazolam in failure to achieve seizure cessation (all routes of administration). IV = intravenous; IM = intramuscular; IN = intranasal; M-H = Mantel-Haenszel; PR = per rectum. Figure 3. IV diazepam versus non-iv midazolam in failure to achieve seizure cessation. IV = intravenous; IM = intramuscular; IN = intranasal; M-H = Mantel-Haenszel. is no apparent difference between non-iv midazolam and IV diazepam in achieving seizure cessation (RR = 0.79; 95% CI = 0.19 to 3.26; Figure 3). Statistical heterogeneity of this subgroup of studies was very low (I 2 = 0%). Three studies of 628 subjects compared rectal diazepam to buccal midazolam. Buccal midazolam is more successful in achieving seizure cessation (RR = 1.54; 95% CI = 1.29 to 1.85; I 2 = 0%; NNT = 6). Time to Administration and Time to Seizure Cessation Early treatment of SE is likely to be most successful and relies on the time intervals of seizure onset to medical contact, medical contact to drug administration, and drug administration to therapeutic effect. These time intervals are separately evaluated when reported by individual studies. No studies reliably report the time from seizure onset to medical contact. Two 37,38 studies demonstrate non-iv midazolam was administered 2.46 minutes (95% CI = 1.52 to 3.39 minutes) quicker than IV diazepam to seizing patients. Non-IV midazolam and IV diazepam were similar in the time between drug administration and seizure cessation in three studies (mean difference = 0.68 minutes, 95% CI = )0.03 to 1.39 minutes). Respiratory Complications Respiratory complications were rarely reported. In five studies of 750 subjects only five instances of respiratory depression requiring intubation or ventilatory support (0.7%) were described, and these all came from a single study of non-iv benzodiazepines. 40 There is no apparent difference between the safety of midazolam and diazepam (RR = 1.49; 95% CI = 0.25 to 8.72; Figure 4). Causes of respiratory depression were
5 ACAD EMERG MED June 2010, Vol. 17, No Definition of Success CONSORT Score Trial Design Nongeneralized Seizures Included? History of Fever (%) No seizure activity within 5 minutes 23 Randomized Yes (11 partial motor) Randomized No No seizure activity within 5 minutes; up to 10 minutes considered delayed success History of Prior Seizures (%) No seizure activity within 10 minutes 22 Randomized Yes (6 simple partial) No seizure activity within 10 minutes and 27 Randomized Yes (5 partial included were no recurrent seizure within 1 hour protocol violations) No seizure activity within 10 minutes and 28 Randomized Yes (61 focal) 72 4 no recurrent seizure within 1 hour Seizure cessation within 10 minutes 26 Randomized Yes (17 complex partial, 10 myoclonic) Figure 4. Respiratory complications requiring intervention (assisted ventilations, endotracheal intubation). IV = intravenous; IM = intramuscular; IN = intranasal; M-H = Mantel-Haenszel; PR = per rectum. described as multifactorial, but further detail was not provided. Sensitivity Analysis For each outcome, removing individual studies did not affect pooled risk ratios or measurements of statistical heterogeneity. There is also no apparent bias introduced by dose of medication, length of seizure required for inclusion, or inclusion of nongeneralized seizures. Outcomes were also analyzed using a random-effects model, with no meaningful effect on the results. A more broad pooled analysis including the eight studies with CONSORT scores between 15 and 19 yields similar results to all outcomes: 27,43 49 overall success (RR = 1.50; 95% CI = 1.30 to 1.73, n=14), IV diazepam versus non-iv midazolam (RR = 0.90; 95% CI = 0.48 to 1.68, n=5), or PR diazepam versus buccal midazolam (RR = 1.51; 95% CI = 1.26 to 1.80, n=4). Midazolam appears to be associated with fewer respiratory complications in this expanded group (RR = 1.74; 95% CI = 1.23 to 2.46, n=13, I 2 = 69%); however, this result is biased by a single study, 46 and exclusion resulted in no safety difference between the two medications (RR = 1.31; 95% CI = 0.88 to 1.95, n=12, I 2 = 0%). Visual inspection of funnel plots shows no obvious signal of asymmetry, which suggests lack of significant publication bias; this is limited due to the small numbers of studies included. Begg s test was marginal, but not statistically significant (p = ). DISCUSSION This pooled meta-analysis of all published data from 774 subjects in six studies supports the use of midazolam by non-iv routes as a favorable alternative to diazepam in the initial treatment of SE. Midazolam, by any route, achieved seizure cessation more often than diazepam, by any route (RR = 1.52; 95% CI = 1.27 to 1.82). This finding is even more apparent when comparing non-iv administration of diazepam and midazolam. The superior efficacy of midazolam compared to diazepam likely reflects more favorable pharmacokinetics. Erratic absorption of rectal diazepam often results in low or delayed plasma peak drug concentrations, whereas IM and IN midazolam have a more consistent and higher bioavailability of 87 and 55%, respectively, with a short time to peak concentration. 29 Rapidity of seizure cessation is also a clinically important measure of performance that depends on both the speed of administration and the onset of action. Earlier termination of seizure reduces the risk of complications due to convulsions, reduces neuronal injury, and is associated with decreased mortality. Rapid termination may also prevent kindling effects, where seizures become more refractory to treatment and risk of recurrence increases as the duration of convulsions increases. 19 Reliance on the IV route for benzodiazepine administration can be an important obstacle to rapid treatment of SE, because of difficulty or delay in obtaining IV access in a convulsing patient. As a result, our
6 580 McMullan et al. MIDAZOLAM VS. DIAZEPAM IN STATUS SEIZURES meta-analysis appears to favor non-iv midazolam, as its time to administration was more than 2 minutes faster and seizure cessation less than 45 seconds slower than that of IV diazepam. Respiratory depression is an expected and accepted side effect of benzodiazepine medications, and this meta-analysis suggests that midazolam is as safe as diazepam with regard to respiratory complications. Overall, 0.8% (3 375) of pediatric patients in this analysis receiving diazepam experienced complications, which is much less than the 10.3% previously observed with diazepam in a trial of the prehospital treatment of SE in adults. 26 Midazolam was associated with risk of respiratory complications in children similar to that found with diazepam (0.5%, 2 375). Respiratory depression in patients treated for SE can be a complication of either continued seizures or an adverse medication effect. At least in the prehospital setting, failure to treat seizures is associated with much higher rates of respiratory complications. Twenty-two percent of placebo-treated patients in a prehospital trial of SE suffered a respiratory complication related to ongoing seizure. 26 Current clinical practice does not reflect the findings that non-iv midazolam is a safe and effective treatment for SE. There are no consensus guidelines addressing prehospital treatment of SE, and many large agencies rely solely on diazepam or allow only restricted use of midazolam. Published professional guidelines for SE management rely on lorazepam or diazepam and emphasize IV administration Only the Royal College of General Practitioners acknowledges the role of buccal midazolam for use in the prehospital environment, but even in that guideline rectal diazepam is preferred. 52 Recent surveys of parents and practitioners show a growing acceptance of IN and buccal midazolam over PR diazepam, but widespread adoption has not yet occurred. 54,55 This analysis, in conjunction with previously published systematic reviews, 32,56 may inform the development of future evidence-based guidelines. However, further prospective clinical trials are ultimately needed to confirm the efficacy and safety of non-iv midazolam in the treatment of patients with SE, especially in the adult population. LIMITATIONS As with all meta-analyses, the primary limitations of this study are those of the source data. The studies included here are relatively small and contained differences in treatments, routes of medication administration, medication doses, outcome definitions, and inclusion criteria. However, the pooled results demonstrated low statistical heterogeneity, suggesting that comparisons are valid. Given the small numbers of studies included, the visual inspection of the funnel plot and measure of statistical heterogeneity should be interpreted with caution A minimal I 2 does not guarantee homogeneity, but does provide evidence that there was no observed heterogeneity. Our finding of I 2 = 0% is consistent with many previously published Cochrane reviews. 36 Adults were virtually unrepresented in the included studies, and extrapolation of these results to the adult population should be done with caution. Future trials specifically targeting adult populations are required to confirm these findings. Studies also used differing definitions of adverse events, which were infrequent. However, this analysis is underpowered to detect differences in complication rates. Although a rigorous search strategy was employed, we did not attempt to identify or analyze non English language studies. Comparisons with other anticonvulsants are lacking and were not identified or included in this meta-analysis. Despite these limitations, the effects identified here appear robust given the magnitude of the findings and the rather small CIs. Prospective confirmatory investigation, however, is warranted. CONCLUSIONS Published data support the efficacy and safety of nonintravenous routes of administration for midazolam, when compared to diazepam administered via any route in treating patients with status epilepticus, in the doses studied. Midazolam has characteristics that may make it an optimal choice for the treatment of seizing patients. References 1. Huff JS, Morris DL, Kothari RU, Gibbs MA. Emergency department management of patients with seizures: a multicenter study. Acad Emerg Med. 2001; 8: Epilepsy Foundation. Epilepsy and Seizure Statistics. Available at: org/about/statistics.cfm. Accessed Feb 28, Shinnar S, Berg AT, Moshe SL, Shinnar R. How long do new-onset seizures in children last? Ann Neurol. 2001; 49: Theodore WH, Porter RJ, Albert P, et al. The secondarily generalized tonic-clonic seizure: a videotape analysis. Neurology. 1994; 44: DeLorenzo RJ, Hauser WA, Towne AR, et al. A prospective, population-based epidemiologic study of status epilepticus in Richmond, Virginia. Neurology. 1996; 46: Hauser WA. Status epilepticus: epidemiologic considerations. Neurology. 1990; 40(5 Suppl 2): Towne AR, Pellock JM, Ko D, DeLorenzo RJ. Determinants of mortality in status epilepticus. Epilepsia. 1994; 35: Claassen J, Lokin JK, Fitzsimmons BF, Mendelsohn FA, Mayer SA. Predictors of functional disability and mortality after status epilepticus. Neurology. 2002; 58: Meldrum BS, Horton RW. Physiology of status epilepticus in primates. Arch Neurol. 1973; 28: Lothman E. The biochemical basis and pathophysiology of status epilepticus. Neurology. 1990; 40(5 Suppl 2): Aminoff MJ, Simon RP. Status epilepticus. Causes, clinical features and consequences in 98 patients. Am J Med. 1980; 69:
7 ACAD EMERG MED June 2010, Vol. 17, No Bayne LL, Simon RP. Systemic and pulmonary vascular pressures during generalized seizures in sheep. Ann Neurol. 1981; 10: White PT, Grant P, Mosier J, Craig A. Changes in cerebral dynamics associated with seizures. Neurology. 1961; 11(4 Pt 1): Boggs JG, Painter JA, DeLorenzo RJ. Analysis of electrocardiographic changes in status epilepticus. Epilepsy Res. 1993; 14: Boggs JG, Marmarou A, Agnew JP, et al. Hemodynamic monitoring prior to and at the time of death in status epilepticus. Epilepsy Res. 1998; 31: Haut SR, Veliskova J, Moshe SL. Susceptibility of immature and adult brains to seizure effects. Lancet Neurol. 2004; 3: Maegaki Y, Kurozawa Y, Hanaki K, Ohno K. Risk factors for fatality and neurological sequelae after status epilepticus in children. Neuropediatrics. 2005; 36: Waterhouse EJ, Garnett LK, Towne AR, et al. Prospective population-based study of intermittent and continuous convulsive status epilepticus in Richmond, Virginia. Epilepsia. 1999; 40: Morimoto K, Fahnestock M, Racine RJ. Kindling and status epilepticus models of epilepsy: rewiring the brain. Prog Neurobiol. 2004; 73: Towne AR. Epidemiology and outcomes of status epilepticus in the elderly. Int Rev Neurobiol. 2007; 81: Holmes GL. Seizure-induced neuronal injury: animal data. Neurology. 2002; 59(9 Suppl 5):S Goodkin HP, Liu X, Holmes GL. Diazepam terminates brief but not prolonged seizures in young, naive rats. Epilepsia. 2003; 44: Jones DM, Esmaeil N, Maren S, Macdonald RL. Characterization of pharmacoresistance to benzodiazepines in the rat Li-pilocarpine model of status epilepticus. Epilepsy Res. 2002; 50: Henry JC, Holloway R. Review: Lorazepam provides the best control for status epilepticus [review]. ACP J Club. 2006; 144: Prasad K, Al-Roomi K, Krishnan PR, Sequeira R. Anticonvulsant therapy for status epilepticus. Cochrane Database Syst Rev. 2005; (4):CD Alldredge BK, Gelb AM, Isaacs SM, et al. A comparison of lorazepam, diazepam, and placebo for the treatment of out-of-hospital status epilepticus. N Engl J Med. 2001; 345: Rainbow J, Browne GJ, Lam LT. Controlling seizures in the prehospital setting: diazepam or midazolam? J Paediatr Child Health. 2002; 38: Vilke GM, Sharieff GQ, Marino A, Gerhart AE, Chan TC. Midazolam for the treatment of out-ofhospital pediatric seizures. Prehosp Emerg Care. 2002; 6: Rey E, Treluyer JM, Pons G. Pharmacokinetic optimization of benzodiazepine therapy for acute seizures. Focus on delivery routes. Clin Pharmacokinet. 1999; 36: Bebin M, Bleck TP. New anticonvulsant drugs. Focus on flunarizine, fosphenytoin, midazolam and stiripentol. Drugs. 1994; 48: Fountain NB, Adams RE. Midazolam treatment of acute and refractory status epilepticus. Clin Neuropharmacol. 1999; 22: Appleton R, Macleod S, Martland T. Drug management for acute tonic-clonic convulsions including convulsive status epilepticus in children. Cochrane Database Syst Rev. 2008; (3):CD Lowenstein DH, Bleck T, Macdonald RL. It s time to revise the definition of status epilepticus. Epilepsia. 1999; 40: Huwiler-Muntener K, Juni P, Junker C, Egger M. Quality of reporting of randomized trials as a measure of methodologic quality. JAMA. 2002; 287: DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986; 7: Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003; 327: Chamberlain JM, Altieri MA, Futterman C, Young GM, Ochsenschlager DW, Waisman Y. A prospective, randomized study comparing intramuscular midazolam with intravenous diazepam for the treatment of seizures in children. Pediatr Emerg Care. 1997; 13: Lahat E, Goldman M, Barr J, Bistritzer T, Berkovitch M. Comparison of intranasal midazolam with intravenous diazepam for treating febrile seizures in children: prospective randomised study. BMJ. 2000; 321: Mahmoudian T, Zadeh MM. Comparison of intranasal midazolam with intravenous diazepam for treating acute seizures in children. Epilepsy Behav. 2004; 5: McIntyre J, Robertson S, Norris E, et al. Safety and efficacy of buccal midazolam versus rectal diazepam for emergency treatment of seizures in children: a randomised controlled trial. Lancet. 2005; 366: Mpimbaza A, Ndeezi G, Staedke S, Rosenthal PJ, Byarugaba J. Comparison of buccal midazolam with rectal diazepam in the treatment of prolonged seizures in Ugandan children: a randomized clinical trial. Pediatrics. 2008; 121:e Scott RC, Besag FM, Neville BG. Buccal midazolam and rectal diazepam for treatment of prolonged seizures in childhood and adolescence: a randomised trial. Lancet. 1999; 353: Baysun S, Aydin OF, Atmaca E, Gurer YK. A comparison of buccal midazolam and rectal diazepam for the acute treatment of seizures. Clin Pediatr (Phila). 2005; 44: Bhattacharyya M, Kalra V, Gulati S. Intranasal midazolam vs. rectal diazepam in acute childhood seizures. Pediatr Neurol. 2006; 34: Fisgin T, Gurer Y, Tezic T, et al. Effects of intranasal midazolam and rectal diazepam on acute convulsions in children: prospective randomized study. J Child Neurol. 2002; 17: Holsti M, Sill BL, Firth SD, Filloux FM, Joyce SM, Furnival RA. Prehospital intranasal midazolam for the treatment of pediatric seizures. Pediatr Emerg Care. 2007; 23:
8 582 McMullan et al. MIDAZOLAM VS. DIAZEPAM IN STATUS SEIZURES 47. Shah I, Deshmukh CT. Intramuscular midazolam vs. intravenous diazepam for acute seizures. Indian J Pediatr. 2005; 72: Talukdar B, Chakrabarty B. Efficacy of buccal midazolam compared to intravenous diazepam in controlling convulsions in children: a randomized controlled trial. Brain Dev. 2008; 31: Warden CR, Frederick C. Midazolam and diazepam for pediatric seizures in the prehospital setting. Prehosp Emerg Care. 2006; 10: Meierkord H, Boon P, Engelsen B, et al. EFNS guideline on the management of status epilepticus. Eur J Neurol. 2006; 13: Appleton R, Choonara I, Martland T, Phillips B, Scott R, Whitehouse W. The treatment of convulsive status epilepticus in children. The Status Epilepticus Working Party, Members of the Status Epilepticus Working Party. Arch Dis Child. 2000; 83: Stokes T, Shaw EJ, Juarez-Garcia A, Camosso-Stefinovic J, Baker R. Clinical Guidelines and Evidence Review for the Epilepsies: Diagnosis and Management in Adults and Children in Primary and Secondary Care. London, England: Royal College of General Practitioners, Scottish Intercollegiate Guidelines Network. Diagnosis and Management of Epilepsy in Adults: A National Clinical Guideline. Edinburgh, Scotland: Scottish Intercollegiate Guidelines Network, de Haan GJ, van der Geest P, Doelman G, Bertram E, Edelbroek P. A comparison of midazolam nasal spray and diazepam rectal solution for the residential treatment of seizure exacerbations. Epilepsia. 2010; 51: Klimach VJ. The community use of rescue medication for prolonged epileptic seizures in children. Seizure. 2009; 18: Sofou K, Kristjansdottir R, Papachatzakis NE, Ahmadzadeh A, Uvebrant P. Management of prolonged seizures and status epilepticus in childhood: a systematic review. J Child Neurol. 2009; 24: Lau J, Ioannidis JP, Terrin N, Schmid CH, Olkin I. The case of the misleading funnel plot. BMJ. 2006; 333: Tang JL, Liu JL. Misleading funnel plot for detection of bias in meta-analysis. J Clin Epidemiol. 2000; 53: Terrin N, Schmid CH, Lau J. In an empirical evaluation of the funnel plot, researchers could not visually identify publication bias. J Clin Epidemiol. 2005; 58: PICO: In pediatric and adult patients with status epilepticus, is the administration of non-intravenous midazolam versus any route of diazepam more effective in ceasing seizures? Exclusion Criteria 1. Any study that does not compare diazepam to midazolam as a first-line treatment for status epilepticus. 2. Animal studies. 3. Studies that are not randomized controlled trials or quasi-experimental studies. 4. Any study that uses diazepam or midazolam as sedation, or prevention of seizures. Search Strategy PubMed (62) 26 pulled for full text ( Seizures [MeSH] OR status epilepticus [MeSH) AND ( diazepam [MeSH Terms] OR diazepam [All Fields]) AND ( midazolam [MeSH Terms] OR midazolam [All Fields]) EMBASE (15, all duplicates) All EBM Reviews (Cochrane, ACP Journal Club) (20 titles, 13 full texts pulled) CINAHL (16, all duplicates) International Pharmaceutical Abstracts (14, all duplicates) Web of Knowledge (124) (5 full texts) Hand search of review article bibliographies: all duplicates TOTAL FULL TEXTS REVIEWED = 44 Total INCLUDED = 6 Stratified by buccal versus intranasal versus intramuscular midazolam and rectal versus intravenous diazepam Appendix B: Funnel Plot Appendix A: Boolean Search Strategy Date of Original Search: August 20, 2008 Search updated July 4, 2009 Funnel plot for Figure 2 (diazepam vs. midazolam in failure to achieve seizure cessation). Kendall s rank correlation (Begg s test) = 0.77, p = As a comparison, the linear correlation (Egger s Test) = 0.27, p = 0.24.
NMDOH digital library; keywords searched: pre-hospital, benzodiazepine, emergency medical technician, treatment of seizures, status epilepticus.
 Background Literature Review and Recommendations Administration of Benzodiazepines by EMT -I in the pre-hospital setting EMS Bureau Protocol Review Steering Committee Status epilepticus is a recognized
Background Literature Review and Recommendations Administration of Benzodiazepines by EMT -I in the pre-hospital setting EMS Bureau Protocol Review Steering Committee Status epilepticus is a recognized
Controlling seizures in children: diazepam or midazolam? Systematic review
 Hong Kong Journal of Emergency Medicine Controlling seizures in children: diazepam or midazolam? Systematic review D Doshi Introduction: Diazepam is commonly used to treat acute childhood seizures, but
Hong Kong Journal of Emergency Medicine Controlling seizures in children: diazepam or midazolam? Systematic review D Doshi Introduction: Diazepam is commonly used to treat acute childhood seizures, but
PROTOCOL. Francesco Brigo, Luigi Giuseppe Bongiovanni
 COMMON REFERENCE-BASED INDIRECT COMPARISON META-ANALYSIS OF INTRAVENOUS VALPROATE VERSUS INTRAVENOUS PHENOBARBITONE IN GENERALIZED CONVULSIVE STATUS EPILEPTICUS PROTOCOL Francesco Brigo, Luigi Giuseppe
COMMON REFERENCE-BASED INDIRECT COMPARISON META-ANALYSIS OF INTRAVENOUS VALPROATE VERSUS INTRAVENOUS PHENOBARBITONE IN GENERALIZED CONVULSIVE STATUS EPILEPTICUS PROTOCOL Francesco Brigo, Luigi Giuseppe
Stop the Status: Improving Outcomes in Pediatric Epilepsy Syndromes. Michelle Welborn, PharmD ICE Alliance
 Stop the Status: Improving Outcomes in Pediatric Epilepsy Syndromes Michelle Welborn, PharmD ICE Alliance Overview Seizures and Epilepsy Syndromes Seizure Emergencies Febrile Seizures Critical Population
Stop the Status: Improving Outcomes in Pediatric Epilepsy Syndromes Michelle Welborn, PharmD ICE Alliance Overview Seizures and Epilepsy Syndromes Seizure Emergencies Febrile Seizures Critical Population
A Shot in the Arm for Prehospital Status Epilepticus: The RAMPART Study
 Current Literature In Clinical Science A Shot in the Arm for Prehospital Status Epilepticus: The RAMPART Study Intramuscular Versus Intravenous Therapy for Prehospital Status Epilepticus. Silbergleit R,
Current Literature In Clinical Science A Shot in the Arm for Prehospital Status Epilepticus: The RAMPART Study Intramuscular Versus Intravenous Therapy for Prehospital Status Epilepticus. Silbergleit R,
A Comparison of Buccal Midazolam and Intravenous Diazepam for the Acute Treatment of Seizures in Children
 Original Article Iran J Pediatr Sep 2012; Vol 22 (No 3), Pp: 303-308 A Comparison of Buccal Midazolam and Intravenous Diazepam for the Acute Treatment of Seizures in Children Seyed-Hassan Tonekaboni 1,2,
Original Article Iran J Pediatr Sep 2012; Vol 22 (No 3), Pp: 303-308 A Comparison of Buccal Midazolam and Intravenous Diazepam for the Acute Treatment of Seizures in Children Seyed-Hassan Tonekaboni 1,2,
Inappropriate emergency management of status epilepticus in children contributes to need for intensive care
 1584 PAPER Inappropriate emergency management of status epilepticus in children contributes to need for intensive care R F M Chin, L Verhulst, B G R Neville, M J Peters, R C Scott... See end of article
1584 PAPER Inappropriate emergency management of status epilepticus in children contributes to need for intensive care R F M Chin, L Verhulst, B G R Neville, M J Peters, R C Scott... See end of article
Journal of Child Neurology
 Journal of Child Neurology http://jcn.sagepub.com Management of Prolonged s and Status Epilepticus in Childhood: A Systematic Review Kalliopi Sofou, Ragnhildur Kristjánsdóttir, Nikolaos E. Papachatzakis,
Journal of Child Neurology http://jcn.sagepub.com Management of Prolonged s and Status Epilepticus in Childhood: A Systematic Review Kalliopi Sofou, Ragnhildur Kristjánsdóttir, Nikolaos E. Papachatzakis,
Accounting for Repeat Enrollments During an Emergency Clinical Trial: The Rapid Anticonvulsant Medications Prior to Arrival Trial (RAMPART)
 RESEARCH METHODS &STATISTICS Accounting for Repeat Enrollments During an Emergency Clinical Trial: The Rapid Anticonvulsant Medications Prior to Arrival Trial (RAMPART) William J. Meurer, MD, MS, Robert
RESEARCH METHODS &STATISTICS Accounting for Repeat Enrollments During an Emergency Clinical Trial: The Rapid Anticonvulsant Medications Prior to Arrival Trial (RAMPART) William J. Meurer, MD, MS, Robert
Intranasal Midazolam Versus Intravenous Diazepam for the Treatment of Acute Seizures in Paediatric Patients
 Intranasal Midazolam Versus Intravenous Diazepam for the Treatment of Acute Seizures in Paediatric Patients Pooja Garg, R S Sethi, Aradhna Kankane, OS Chaurasia, Anuj Shamsher Sethi Department of Peadiatrics,
Intranasal Midazolam Versus Intravenous Diazepam for the Treatment of Acute Seizures in Paediatric Patients Pooja Garg, R S Sethi, Aradhna Kankane, OS Chaurasia, Anuj Shamsher Sethi Department of Peadiatrics,
Early termination of prolonged epileptic
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e Early termination of prolonged epileptic seizures in response to intravenous administration of benzodiazepines by paramedics in the prehospital setting
T h e n e w e ngl a nd j o u r na l o f m e dic i n e Early termination of prolonged epileptic seizures in response to intravenous administration of benzodiazepines by paramedics in the prehospital setting
1. What is the comparative efficacy of IV lorazepam and IV diazepam for the treatment of febrile seizures in children (less than 12 years of age)?
 Title: The Use of Lorazepam for Febrile Seizures in Children Date: 25 January 2008 Context and policy issues: Febrile seizures are the most common form of childhood seizures, affecting approximately 2
Title: The Use of Lorazepam for Febrile Seizures in Children Date: 25 January 2008 Context and policy issues: Febrile seizures are the most common form of childhood seizures, affecting approximately 2
A bs tr ac t. n engl j med 366;7 nejm.org february 16,
 The new england journal of medicine established in 1812 february 16, 2012 vol. 366 no. 7 Intramuscular versus Intravenous Therapy for Prehospital Status Epilepticus Robert Silbergleit, M.D., Valerie Durkalski,
The new england journal of medicine established in 1812 february 16, 2012 vol. 366 no. 7 Intramuscular versus Intravenous Therapy for Prehospital Status Epilepticus Robert Silbergleit, M.D., Valerie Durkalski,
Intranasal Midazolam Compared with Intravenous Diazepam in Patients Suffering from Acute Seizure: A Randomized Clinical Trial
 Original Article Iran J Pediatr Mar 2012; Vol 22 (No 1), Pp: 1-8 Intranasal Midazolam Compared with Intravenous Diazepam in Patients Suffering from Acute Seizure: A Randomized Clinical Trial Mohsen Javadzadeh
Original Article Iran J Pediatr Mar 2012; Vol 22 (No 1), Pp: 1-8 Intranasal Midazolam Compared with Intravenous Diazepam in Patients Suffering from Acute Seizure: A Randomized Clinical Trial Mohsen Javadzadeh
ARTICLE. Intranasal Midazolam vs Rectal Diazepam for the Home Treatment of Acute Seizures in Pediatric Patients With Epilepsy
 JOURNAL CLUB ARTICLE Intranasal Midazolam vs Rectal Diazepam for the Home Treatment of Acute Seizures in Pediatric Patients With Epilepsy Maija Holsti, MD, MPH; Nanette Dudley, MD; Jeff Schunk, MD; Kathleen
JOURNAL CLUB ARTICLE Intranasal Midazolam vs Rectal Diazepam for the Home Treatment of Acute Seizures in Pediatric Patients With Epilepsy Maija Holsti, MD, MPH; Nanette Dudley, MD; Jeff Schunk, MD; Kathleen
First Line Therapy in Acute Seizure Management. William Dalsey, MD, FACEP
 First Line Therapy in Acute Seizure Management Case Presentation A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
First Line Therapy in Acute Seizure Management Case Presentation A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
Outline. What is a seizure? What is epilepsy? Updates in Seizure Management Terminology, Triage & Treatment
 Outline Updates in Seizure Management Terminology, Triage & Treatment Joseph Sullivan, MD! Terminology! Videos of different types of seizures! Diagnostic evaluation! Treatment options! Acute! Maintenance
Outline Updates in Seizure Management Terminology, Triage & Treatment Joseph Sullivan, MD! Terminology! Videos of different types of seizures! Diagnostic evaluation! Treatment options! Acute! Maintenance
Simple Protocol & Bayesian Design: Established Status Epilepticus Treatment Trial (ESETT)
 Simple Protocol & Bayesian Design: Established Status Epilepticus Treatment Trial (ESETT) Jaideep Kapur on behalf of ESETT invertigator University of Virginia Status epilepticus is a condition resulting
Simple Protocol & Bayesian Design: Established Status Epilepticus Treatment Trial (ESETT) Jaideep Kapur on behalf of ESETT invertigator University of Virginia Status epilepticus is a condition resulting
Midazolam for seizures: Buccal administration
 Midazolam for seizures: Buccal administration Rationale Buccal Midazolam is a convenient and efficient method used to treat prolonged seizures and status epilepticus in children. It can be used in hospital
Midazolam for seizures: Buccal administration Rationale Buccal Midazolam is a convenient and efficient method used to treat prolonged seizures and status epilepticus in children. It can be used in hospital
JPPT Brief Review Article
 Brief Review Article Treatment of Acute Seizures: Is Intranasal Midazolam a Viable Option? Lesley K. Humphries, PharmD 1 and Lea S. Eiland, PharmD 2,3 1 Department of Pharmacy, Rockingham Memorial Hospital,
Brief Review Article Treatment of Acute Seizures: Is Intranasal Midazolam a Viable Option? Lesley K. Humphries, PharmD 1 and Lea S. Eiland, PharmD 2,3 1 Department of Pharmacy, Rockingham Memorial Hospital,
Original article. Epileptic Disord 2013; 15 (3):
 Original article Epileptic Disord 2013; 15 (3): 314-23 A common reference-based indirect comparison meta-analysis of intravenous valproate versus intravenous phenobarbitone for convulsive status epilepticus
Original article Epileptic Disord 2013; 15 (3): 314-23 A common reference-based indirect comparison meta-analysis of intravenous valproate versus intravenous phenobarbitone for convulsive status epilepticus
Lieven Lagae Department of Paediatric Neurology Leuven University Leuven, Belgium. Management of acute seizure settings from infancy to adolescence
 Lieven Lagae Department of Paediatric Neurology Leuven University Leuven, Belgium Management of acute seizure settings from infancy to adolescence Consequences of prolonged seizures Acute morbidity and
Lieven Lagae Department of Paediatric Neurology Leuven University Leuven, Belgium Management of acute seizure settings from infancy to adolescence Consequences of prolonged seizures Acute morbidity and
What Are the Best Non-IV Parenteral Options for a Seizing Patient? William C. Dalsey, MD, MBA, FACEP
 What Are the Best Non-IV Parenteral Options for a Seizing Patient? A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
What Are the Best Non-IV Parenteral Options for a Seizing Patient? A 32-year old male intravenous drug user was brought to the ED having had a witnessed generalized tonic-clonic seizure 10 minutes prior
Department of Clinical Pharmacy, University of Colorado, Skaggs School of Pharmacy and Pharmaceutical Sciences, Aurora, CO 6
 American Epilepsy Society Guideline Evidence-Based Guideline: Treatment of Convulsive Status Epilepticus in Children and Adults: Report of the Guideline Committee of the American Epilepsy Society Tracy
American Epilepsy Society Guideline Evidence-Based Guideline: Treatment of Convulsive Status Epilepticus in Children and Adults: Report of the Guideline Committee of the American Epilepsy Society Tracy
National Essential Medicine List Primary Health Care Medication Review Process Component: Emergencies and injuries
 1. Executive Summary National Essential Medicine List Primary Health Care Medication Review Process Component: Emergencies and injuries Date: 31 August2017 Medicine (INN):Midazolam, buccal (repeat dose)
1. Executive Summary National Essential Medicine List Primary Health Care Medication Review Process Component: Emergencies and injuries Date: 31 August2017 Medicine (INN):Midazolam, buccal (repeat dose)
Status Epilepticus: Implications Outside the Neuro-ICU
 Status Epilepticus: Implications Outside the Neuro-ICU Jeffrey M Singh MD Critical Care and Neurocritical Care Toronto Western Hospital October 31 st, 2014 Disclosures I (unfortunately) have no disclosures
Status Epilepticus: Implications Outside the Neuro-ICU Jeffrey M Singh MD Critical Care and Neurocritical Care Toronto Western Hospital October 31 st, 2014 Disclosures I (unfortunately) have no disclosures
Cochrane Pregnancy and Childbirth Group Methodological Guidelines
 Cochrane Pregnancy and Childbirth Group Methodological Guidelines [Prepared by Simon Gates: July 2009, updated July 2012] These guidelines are intended to aid quality and consistency across the reviews
Cochrane Pregnancy and Childbirth Group Methodological Guidelines [Prepared by Simon Gates: July 2009, updated July 2012] These guidelines are intended to aid quality and consistency across the reviews
PROSPERO International prospective register of systematic reviews
 PROSPERO International prospective register of systematic reviews Closed reduction methods for acute anterior shoulder dislocation [Cochrane Protocol] Kanthan Theivendran, Raj Thakrar, Subodh Deshmukh,
PROSPERO International prospective register of systematic reviews Closed reduction methods for acute anterior shoulder dislocation [Cochrane Protocol] Kanthan Theivendran, Raj Thakrar, Subodh Deshmukh,
WHOLE LOTTA SHAKIN GOIN ON
 WHOLE LOTTA SHAKIN GOIN ON ADAM M. YATES, MD FACEP ASSOCIATE CHIEF OF EMERGENCY SERVICES UPMC MERCY SEIZURE DEFINITIONS Partial(focal) only involves part of the brain General Involves entire brain Simple
WHOLE LOTTA SHAKIN GOIN ON ADAM M. YATES, MD FACEP ASSOCIATE CHIEF OF EMERGENCY SERVICES UPMC MERCY SEIZURE DEFINITIONS Partial(focal) only involves part of the brain General Involves entire brain Simple
Rescue medications. What are rescue medications? Ideal rescue medication. Why use rescue medications?
 Rescue medications Out-of-hospital treatment of prolonged seizures or acute repetitive seizures What are rescue medications? Medicines used to terminate a prolonged seizure or acute repetitive seizures
Rescue medications Out-of-hospital treatment of prolonged seizures or acute repetitive seizures What are rescue medications? Medicines used to terminate a prolonged seizure or acute repetitive seizures
Database of Abstracts of Reviews of Effects (DARE) Produced by the Centre for Reviews and Dissemination Copyright 2017 University of York.
 A comparison of the cost-effectiveness of five strategies for the prevention of non-steroidal anti-inflammatory drug-induced gastrointestinal toxicity: a systematic review with economic modelling Brown
A comparison of the cost-effectiveness of five strategies for the prevention of non-steroidal anti-inflammatory drug-induced gastrointestinal toxicity: a systematic review with economic modelling Brown
Intramuscular midazolam versus intravenous lorazepam in the pre-hospital treatment of status epilepticus (the RAMPART trial) Project Summary
 Intramuscular midazolam versus intravenous lorazepam in the pre-hospital treatment of status epilepticus (the RAMPART trial) Project Summary Trial Principal Investigator: Robert Silbergleit, MD Co-principal
Intramuscular midazolam versus intravenous lorazepam in the pre-hospital treatment of status epilepticus (the RAMPART trial) Project Summary Trial Principal Investigator: Robert Silbergleit, MD Co-principal
A prospective randomised study on intranasal midazolam versus rectal diazepam for acute seizures in children
 Original article A prospective randomised study on intranasal midazolam versus rectal diazepam for acute seizures in children 1Dr Rajwanti K. Vaswani*, 2 DrAshishkumar M. Banpurkar 1Professor, Department
Original article A prospective randomised study on intranasal midazolam versus rectal diazepam for acute seizures in children 1Dr Rajwanti K. Vaswani*, 2 DrAshishkumar M. Banpurkar 1Professor, Department
Choice of axis, tests for funnel plot asymmetry, and methods to adjust for publication bias
 Technical appendix Choice of axis, tests for funnel plot asymmetry, and methods to adjust for publication bias Choice of axis in funnel plots Funnel plots were first used in educational research and psychology,
Technical appendix Choice of axis, tests for funnel plot asymmetry, and methods to adjust for publication bias Choice of axis in funnel plots Funnel plots were first used in educational research and psychology,
Q9. In adults and children with convulsive epilepsy in remission, when should treatment be discontinued?
 updated 2012 When to discontinue antiepileptic drug treatment in adults and children Q9. In adults and children with convulsive epilepsy in remission, when should treatment be discontinued? Background
updated 2012 When to discontinue antiepileptic drug treatment in adults and children Q9. In adults and children with convulsive epilepsy in remission, when should treatment be discontinued? Background
Alotaibi, Khalid Nijr (2017) Convulsive status epilepticus in children. PhD thesis, University of Nottingham.
 Alotaibi, Khalid Nijr (2017) Convulsive status epilepticus in children. PhD thesis, University of Nottingham. Access from the University of Nottingham repository: http://eprints.nottingham.ac.uk/38829/1/khalid%20final%20thesis%20nov%202016.pdf
Alotaibi, Khalid Nijr (2017) Convulsive status epilepticus in children. PhD thesis, University of Nottingham. Access from the University of Nottingham repository: http://eprints.nottingham.ac.uk/38829/1/khalid%20final%20thesis%20nov%202016.pdf
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist.
 Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
A Systematic Review and Meta-Analysis of Pre-Transfusion Hemoglobin Thresholds for Allogeneic Red Blood Cell Transfusions
 A Systematic Review and Meta-Analysis of Pre-Transfusion Hemoglobin Thresholds for Allogeneic Red Blood Cell Transfusions Authors: Lesley J.J. Soril 1,2, MSc; Laura E. Leggett 1,2, MSc; Joseph Ahn, MSc
A Systematic Review and Meta-Analysis of Pre-Transfusion Hemoglobin Thresholds for Allogeneic Red Blood Cell Transfusions Authors: Lesley J.J. Soril 1,2, MSc; Laura E. Leggett 1,2, MSc; Joseph Ahn, MSc
National Essential Medicine List Primary Healthcare Medication Review Process Component: Emergencies and injuries
 National Essential Medicine List Primary Healthcare Medication Review Process Component: Emergencies and injuries 1. Executive Summary Date: 31 August 2017 Medicine (INN): Midazolam, IM Medicine (ATC):
National Essential Medicine List Primary Healthcare Medication Review Process Component: Emergencies and injuries 1. Executive Summary Date: 31 August 2017 Medicine (INN): Midazolam, IM Medicine (ATC):
abstract ARTICLE BACKGROUND AND OBJECTIVES: Convulsive seizures account for 15% of pediatric air transports.
 Seizure Treatment in Children Transported to Tertiary Care: Recommendation Adherence and Outcomes Heather M. Siefkes, MD, MSCI, a, b Maija Holsti, MD, MPH, c Denise Morita, MD, d Lawrence J. Cook, PhD,
Seizure Treatment in Children Transported to Tertiary Care: Recommendation Adherence and Outcomes Heather M. Siefkes, MD, MSCI, a, b Maija Holsti, MD, MPH, c Denise Morita, MD, d Lawrence J. Cook, PhD,
Hope for New Treatments for Acute Repetitive Seizures
 Current Literature In Clinical Science Hope for New Treatments for Acute Repetitive Seizures A Double-Blind, Randomized, Placebo-Controlled Trial of a Diazepam Auto-Injector Administered by Caregivers
Current Literature In Clinical Science Hope for New Treatments for Acute Repetitive Seizures A Double-Blind, Randomized, Placebo-Controlled Trial of a Diazepam Auto-Injector Administered by Caregivers
Treatment adherence and outcomes in the management of convulsive status epilepticus in the emergency room
 Original article Epileptic Disord 2007; 9 (1): 43-50 Treatment adherence and outcomes in the management of convulsive status epilepticus in the emergency room Taim Muayqil, Brian H. Rowe, S. Nizam Ahmed
Original article Epileptic Disord 2007; 9 (1): 43-50 Treatment adherence and outcomes in the management of convulsive status epilepticus in the emergency room Taim Muayqil, Brian H. Rowe, S. Nizam Ahmed
Buccal Midazolam versus Intravenous Diazepam in Prolonged Seizures in Children
 Original Article DOI: 10.17354/ijss/2015/306 Buccal Midazolam versus Intravenous Diazepam in Prolonged Seizures in Children Rohit Khandelwal 1, Leeni Mehta Khandelwal 2, Karnail Singh 3 1 Assistant Professor,
Original Article DOI: 10.17354/ijss/2015/306 Buccal Midazolam versus Intravenous Diazepam in Prolonged Seizures in Children Rohit Khandelwal 1, Leeni Mehta Khandelwal 2, Karnail Singh 3 1 Assistant Professor,
Meta-analyses: analyses:
 Meta-analyses: analyses: how do they help, and when can they not? Lee Hooper Senior Lecturer in research synthesis & nutrition l.hooper@uea.ac.uk 01603 591268 Aims Systematic Reviews Discuss the scientific
Meta-analyses: analyses: how do they help, and when can they not? Lee Hooper Senior Lecturer in research synthesis & nutrition l.hooper@uea.ac.uk 01603 591268 Aims Systematic Reviews Discuss the scientific
MINDFULNESS-BASED INTERVENTIONS IN EPILEPSY
 03 March 2016; v.1 MINDFULNESS-BASED INTERVENTIONS IN EPILEPSY AIM This review aimed to evaluate the effectiveness of mindfulness as a therapeutic intervention for people with epilepsy. METHODS Criteria
03 March 2016; v.1 MINDFULNESS-BASED INTERVENTIONS IN EPILEPSY AIM This review aimed to evaluate the effectiveness of mindfulness as a therapeutic intervention for people with epilepsy. METHODS Criteria
Refractory Status Epilepticus in Children: What are the Options?
 Refractory Status Epilepticus in Children: What are the Options? Weng Man Lam, PharmD, BCPS, BCPPS PICU Clinical Pharmacy Specialist Memorial Hermann Texas Medical Center November 11, 2017 Objectives 1.
Refractory Status Epilepticus in Children: What are the Options? Weng Man Lam, PharmD, BCPS, BCPPS PICU Clinical Pharmacy Specialist Memorial Hermann Texas Medical Center November 11, 2017 Objectives 1.
PROSPERO International prospective register of systematic reviews
 PROSPERO International prospective register of systematic reviews High-dose chemotherapy followed by autologous haematopoietic cell transplantation for children, adolescents and young adults with first
PROSPERO International prospective register of systematic reviews High-dose chemotherapy followed by autologous haematopoietic cell transplantation for children, adolescents and young adults with first
Duration of refractory status epilepticus and outcome: Loss of prognostic utility after several hours
 FULL-LENGTH ORIGINAL RESEARCH Duration of refractory status epilepticus and outcome: Loss of prognostic utility after several hours *Frank W. Drislane, yandrew S. Blum, zmaria R. Lopez, xshiva Gautam,
FULL-LENGTH ORIGINAL RESEARCH Duration of refractory status epilepticus and outcome: Loss of prognostic utility after several hours *Frank W. Drislane, yandrew S. Blum, zmaria R. Lopez, xshiva Gautam,
TITLE: Patient-Controlled Analgesia for Acute Injury Transfers: A Review of the Clinical Effectiveness, Safety, and Guidelines
 TITLE: Patient-Controlled Analgesia for Acute Injury Transfers: A Review of the Clinical Effectiveness, Safety, and Guidelines DATE: 11 August 2014 CONTEXT AND POLICY ISSUES Patient-controlled analgesia
TITLE: Patient-Controlled Analgesia for Acute Injury Transfers: A Review of the Clinical Effectiveness, Safety, and Guidelines DATE: 11 August 2014 CONTEXT AND POLICY ISSUES Patient-controlled analgesia
Seizure remission in adults with long-standing intractable epilepsy: An extended follow-up
 Epilepsy Research (2010) xxx, xxx xxx journal homepage: www.elsevier.com/locate/epilepsyres Seizure remission in adults with long-standing intractable epilepsy: An extended follow-up Hyunmi Choi a,, Gary
Epilepsy Research (2010) xxx, xxx xxx journal homepage: www.elsevier.com/locate/epilepsyres Seizure remission in adults with long-standing intractable epilepsy: An extended follow-up Hyunmi Choi a,, Gary
2008 EAGLES PRESENTATION. Intranasal Versed Usage in an Urban Fire Based EMS System: PARAMEDIC PERCEPTION OF UTILITY
 2008 EAGLES PRESENTATION Intranasal Versed Usage in an Urban Fire Based EMS System: PARAMEDIC PERCEPTION OF UTILITY CFD EMS OVERVIEW CFD EMS OVERVIEW CFD EMS OVERVIEW All ALS EMS System Two EMT-Ps on each
2008 EAGLES PRESENTATION Intranasal Versed Usage in an Urban Fire Based EMS System: PARAMEDIC PERCEPTION OF UTILITY CFD EMS OVERVIEW CFD EMS OVERVIEW CFD EMS OVERVIEW All ALS EMS System Two EMT-Ps on each
Alectinib Versus Crizotinib for Previously Untreated Alk-positive Advanced Non-small Cell Lung Cancer : A Meta-Analysis
 Showa Univ J Med Sci 30 2, 309 315, June 2018 Original Alectinib Versus Crizotinib for Previously Untreated Alk-positive Advanced Non-small Cell Lung Cancer : A Meta-Analysis Ryo MANABE 1, Koichi ANDO
Showa Univ J Med Sci 30 2, 309 315, June 2018 Original Alectinib Versus Crizotinib for Previously Untreated Alk-positive Advanced Non-small Cell Lung Cancer : A Meta-Analysis Ryo MANABE 1, Koichi ANDO
Using Number Needed to Treat to Interpret Treatment Effect
 Continuing Medical Education 20 Using Number Needed to Treat to Interpret Treatment Effect Der-Shin Ke Abstract- Evidence-based medicine (EBM) has rapidly emerged as a new paradigm in medicine worldwide.
Continuing Medical Education 20 Using Number Needed to Treat to Interpret Treatment Effect Der-Shin Ke Abstract- Evidence-based medicine (EBM) has rapidly emerged as a new paradigm in medicine worldwide.
Challenges in the Design and Analysis of Non-Inferiority Trials: A Case Study. Key Points from FDA Guidance
 Challenges in the Design and Analysis of Non-Inferiority Trials: A Case Study Valerie Durkalski NETT Statistical and Data Management Center (NINDS U01 NS059041) Division of Biostatistics & Epidemiology
Challenges in the Design and Analysis of Non-Inferiority Trials: A Case Study Valerie Durkalski NETT Statistical and Data Management Center (NINDS U01 NS059041) Division of Biostatistics & Epidemiology
ESETT ELIGIBILITY OVERVIEW. James Chamberlain, MD
 ESETT ELIGIBILITY OVERVIEW James Chamberlain, MD Eligibility Age Convulsive Status Benzos Not excluded Eligibility Age 2 years to < 18 years (Pediatric) 18 years to 65 years (Adult) > 65 years (Geriatric)
ESETT ELIGIBILITY OVERVIEW James Chamberlain, MD Eligibility Age Convulsive Status Benzos Not excluded Eligibility Age 2 years to < 18 years (Pediatric) 18 years to 65 years (Adult) > 65 years (Geriatric)
Title: What is the role of pre-operative PET/PET-CT in the management of patients with
 Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
What the s wrong with this person?
 Ketamine for Prehospital Management of Excited Delirium Syndrome: Is it all just a bunch of hype?!? Financial Disclosure Asa M. Margolis, DO, MPH, MS, FACEP Assistant Professor Division of Special Operation
Ketamine for Prehospital Management of Excited Delirium Syndrome: Is it all just a bunch of hype?!? Financial Disclosure Asa M. Margolis, DO, MPH, MS, FACEP Assistant Professor Division of Special Operation
A COMMON REFERENCE-BASED INDIRECT COMPARISON META-ANALYSIS OF ESLICARBAZEPINE VERSUS LACOSAMIDE AS ADD ON TREATMENTS FOR FOCAL EPILEPSY PROTOCOL
 A COMMON REFERENCE-BASED INDIRECT COMPARISON META-ANALYSIS OF ESLICARBAZEPINE VERSUS LACOSAMIDE AS ADD ON TREATMENTS FOR FOCAL EPILEPSY PROTOCOL Francesco Brigo 1,2 1 Department of Neurological and Movement
A COMMON REFERENCE-BASED INDIRECT COMPARISON META-ANALYSIS OF ESLICARBAZEPINE VERSUS LACOSAMIDE AS ADD ON TREATMENTS FOR FOCAL EPILEPSY PROTOCOL Francesco Brigo 1,2 1 Department of Neurological and Movement
Peer Reviewed Title: Journal Issue: Author: Publication Date: Permalink: Author Bio: Keywords:
 Peer Reviewed Title: Prehospital Care for the Adult and Pediatric Seizure Patient: Current Evidence Based Recommendations Journal Issue: Western Journal of Emergency Medicine: Integrating Emergency Care
Peer Reviewed Title: Prehospital Care for the Adult and Pediatric Seizure Patient: Current Evidence Based Recommendations Journal Issue: Western Journal of Emergency Medicine: Integrating Emergency Care
Status Epilepticus in Children
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
CrackCast Episode 18 Seizures
 CrackCast Episode 18 Seizures Episode overview: 1) Define status epilepticus 2) List the doses of common medications used for status epilepticus 3) List 10 differential diagnoses for seizures 4) List 10
CrackCast Episode 18 Seizures Episode overview: 1) Define status epilepticus 2) List the doses of common medications used for status epilepticus 3) List 10 differential diagnoses for seizures 4) List 10
Cochrane Breast Cancer Group
 Cochrane Breast Cancer Group Version and date: V3.2, September 2013 Intervention Cochrane Protocol checklist for authors This checklist is designed to help you (the authors) complete your Cochrane Protocol.
Cochrane Breast Cancer Group Version and date: V3.2, September 2013 Intervention Cochrane Protocol checklist for authors This checklist is designed to help you (the authors) complete your Cochrane Protocol.
Efficacy of postoperative epidural analgesia Block B M, Liu S S, Rowlingson A J, Cowan A R, Cowan J A, Wu C L
 Efficacy of postoperative epidural analgesia Block B M, Liu S S, Rowlingson A J, Cowan A R, Cowan J A, Wu C L CRD summary This review evaluated the efficacy of post-operative epidural analgesia. The authors
Efficacy of postoperative epidural analgesia Block B M, Liu S S, Rowlingson A J, Cowan A R, Cowan J A, Wu C L CRD summary This review evaluated the efficacy of post-operative epidural analgesia. The authors
Background: Traditional rehabilitation after total joint replacement aims to improve the muscle strength of lower limbs,
 REVIEWING THE EFFECTIVENESS OF BALANCE TRAINING BEFORE AND AFTER TOTAL KNEE AND TOTAL HIP REPLACEMENT: PROTOCOL FOR A SYSTEMATIC RE- VIEW AND META-ANALYSIS Background: Traditional rehabilitation after
REVIEWING THE EFFECTIVENESS OF BALANCE TRAINING BEFORE AND AFTER TOTAL KNEE AND TOTAL HIP REPLACEMENT: PROTOCOL FOR A SYSTEMATIC RE- VIEW AND META-ANALYSIS Background: Traditional rehabilitation after
Administrating Medications with the MAD Device
 Disclosures Administrating Medications with the MAD Device Nothing to disclose 2015 VSHP Spring Seminar April 18, 2015 Megan Davis Hoesly, PharmD, BCPS Sentara Virginia Beach General Hospital Clinical
Disclosures Administrating Medications with the MAD Device Nothing to disclose 2015 VSHP Spring Seminar April 18, 2015 Megan Davis Hoesly, PharmD, BCPS Sentara Virginia Beach General Hospital Clinical
RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION?
 RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION? MR. Salehi Omrani MD¹, MR. Edraki MD 2, M. Alizadeh MD 3 Abstract: Objective Febrile convulsion is the most common
RESEARCH ARTICLE IS LUMBAR PUNCTURE ALWAYS NECESSARY IN THE FEBRILE CHILD WITH CONVULSION? MR. Salehi Omrani MD¹, MR. Edraki MD 2, M. Alizadeh MD 3 Abstract: Objective Febrile convulsion is the most common
Systematic Reviews. Simon Gates 8 March 2007
 Systematic Reviews Simon Gates 8 March 2007 Contents Reviewing of research Why we need reviews Traditional narrative reviews Systematic reviews Components of systematic reviews Conclusions Key reference
Systematic Reviews Simon Gates 8 March 2007 Contents Reviewing of research Why we need reviews Traditional narrative reviews Systematic reviews Components of systematic reviews Conclusions Key reference
Pediatric 9-1-1: Show Me the Evidence!
 Pediatric 9-1-1: Show Me the Evidence! Toni Gross, MD, MPH Phoenix Children s Hospital Division of Emergency Medicine National Association of EMS Physicians, Pediatric Committee Chair Overview EMS history
Pediatric 9-1-1: Show Me the Evidence! Toni Gross, MD, MPH Phoenix Children s Hospital Division of Emergency Medicine National Association of EMS Physicians, Pediatric Committee Chair Overview EMS history
Personalizing Drug Delivery
 Personalizing Drug Delivery Emilio Perucca, M.D, Ph.D. Clinical Pharmacology unit, University of Pavia & C. Mondino National Neurological Institute, Pavia, Italy Washington, December 7, 2013 1 American
Personalizing Drug Delivery Emilio Perucca, M.D, Ph.D. Clinical Pharmacology unit, University of Pavia & C. Mondino National Neurological Institute, Pavia, Italy Washington, December 7, 2013 1 American
Phenytoin, Levetiracetam, and Pregabalin in the Acute Management of Refractory Status Epilepticus in Patients with Brain Tumors
 Neurocrit Care (2012) 16:109 113 DOI 10.1007/s12028-011-9626-4 ORIGINAL ARTICLE Phenytoin, Levetiracetam, and Pregabalin in the Acute Management of Refractory Status Epilepticus in Patients with Brain
Neurocrit Care (2012) 16:109 113 DOI 10.1007/s12028-011-9626-4 ORIGINAL ARTICLE Phenytoin, Levetiracetam, and Pregabalin in the Acute Management of Refractory Status Epilepticus in Patients with Brain
First line management of prolonged convulsive seizures in children and adults good practice points
 First line management of prolonged convulsive seizures in children and adults good practice points Liesbeth De Waele 1*, Paul Boon 2, Berten Ceulemans 3, Bernard Dan 4, Anna Jansen 5, Benjamin Legros 6,
First line management of prolonged convulsive seizures in children and adults good practice points Liesbeth De Waele 1*, Paul Boon 2, Berten Ceulemans 3, Bernard Dan 4, Anna Jansen 5, Benjamin Legros 6,
Downloaded from jssu.ssu.ac.ir at 0:37 IRST on Sunday February 17th 2019
 -2384 2 *. : 4 :. 2 / 4 3 6/. ( /) : 6 /4. 6. 00 92 6. 0 :. :. 0 :. International league Against Epilepsy (ILAE) First Unprovoked Seizure (FUS) 24 () (2) 20.. 2 3-4. (). : -* - 0 626024: 0 626024 : E-mial:
-2384 2 *. : 4 :. 2 / 4 3 6/. ( /) : 6 /4. 6. 00 92 6. 0 :. :. 0 :. International league Against Epilepsy (ILAE) First Unprovoked Seizure (FUS) 24 () (2) 20.. 2 3-4. (). : -* - 0 626024: 0 626024 : E-mial:
Monitor and treat respiratory depression and sedation with supportive emergency measures.
 Versed (midazolam), Nasal Administration of Purpose: Versed (midazolam) is a short-acting benzodiazepine medication that is administered intra-nasally to control status epilepticus, a common life-threatening
Versed (midazolam), Nasal Administration of Purpose: Versed (midazolam) is a short-acting benzodiazepine medication that is administered intra-nasally to control status epilepticus, a common life-threatening
Allergen immunotherapy for the treatment of allergic rhinitis and/or asthma
 ril 2014 Allergen immunotherapy for the treatment of allergic rhinitis and/or asthma FINAL COMPREHENSIVE RESEARCH PLAN June 2015 Study Team: Systematic Review Unit FINAL COMPREHENSIVE RESEARCH PLAN: Systematic
ril 2014 Allergen immunotherapy for the treatment of allergic rhinitis and/or asthma FINAL COMPREHENSIVE RESEARCH PLAN June 2015 Study Team: Systematic Review Unit FINAL COMPREHENSIVE RESEARCH PLAN: Systematic
Systematic Reviews and Meta- Analysis in Kidney Transplantation
 Systematic Reviews and Meta- Analysis in Kidney Transplantation Greg Knoll MD MSc Associate Professor of Medicine Medical Director, Kidney Transplantation University of Ottawa and The Ottawa Hospital KRESCENT
Systematic Reviews and Meta- Analysis in Kidney Transplantation Greg Knoll MD MSc Associate Professor of Medicine Medical Director, Kidney Transplantation University of Ottawa and The Ottawa Hospital KRESCENT
Status Epilepticus: A refresher. Objectives
 Status Epilepticus: A refresher Ruben D. Villanueva, Pharm.D., BCPS OU Medical Center Trauma ICU Pharmacist Objectives Define seizures, convulsive and non convulsive status epilepticus, and refractory
Status Epilepticus: A refresher Ruben D. Villanueva, Pharm.D., BCPS OU Medical Center Trauma ICU Pharmacist Objectives Define seizures, convulsive and non convulsive status epilepticus, and refractory
The fitting child. Dr Chris Bird MRCPCH DTMH, Locum consultant, Paediatric Emergency Medicine
 The fitting child Dr Chris Bird MRCPCH DTMH, Locum consultant, Paediatric Emergency Medicine What I am not Detail from The Neurologist, Jose Perez The sacred disease Epilepsy comes from the ancient Greek
The fitting child Dr Chris Bird MRCPCH DTMH, Locum consultant, Paediatric Emergency Medicine What I am not Detail from The Neurologist, Jose Perez The sacred disease Epilepsy comes from the ancient Greek
Established Status Epilepticus Treatment Trial (ESETT)
 Established Status Epilepticus Treatment Trial (ESETT) A multicenter, randomized, blinded, comparative effectiveness study of fosphenytoin, valproic acid, or levetiracetam in the emergency department treatment
Established Status Epilepticus Treatment Trial (ESETT) A multicenter, randomized, blinded, comparative effectiveness study of fosphenytoin, valproic acid, or levetiracetam in the emergency department treatment
p ผศ.นพ.ร งสรรค ช ยเสว ก ล คณะแพทยศาสตร ศ ร ราชพยาบาล
 Natural Course and Prognosis of Epilepsy p ผศ.นพ.ร งสรรค ช ยเสว ก ล คณะแพทยศาสตร ศ ร ราชพยาบาล Introduction Prognosis of epilepsy generally means probability of being seizure-free after starting treatment
Natural Course and Prognosis of Epilepsy p ผศ.นพ.ร งสรรค ช ยเสว ก ล คณะแพทยศาสตร ศ ร ราชพยาบาล Introduction Prognosis of epilepsy generally means probability of being seizure-free after starting treatment
Authors' objectives To evaluate the efficacy of intravenous immunoglobulin (IVIG) for neurologic conditions.
 Use of intravenous immunoglobulin for treatment of neurologic conditions: a systematic review Fergusson D, Hutton B, Sharma M, Tinmouth A, Wilson K, Cameron D W, Hebert P C CRD summary This review assessed
Use of intravenous immunoglobulin for treatment of neurologic conditions: a systematic review Fergusson D, Hutton B, Sharma M, Tinmouth A, Wilson K, Cameron D W, Hebert P C CRD summary This review assessed
Systematic review with multiple treatment comparison metaanalysis. on interventions for hepatic encephalopathy
 Systematic review with multiple treatment comparison metaanalysis on interventions for hepatic encephalopathy Hepatic encephalopathy (HE) is a reversible neuropsychiatric syndrome associated with severe
Systematic review with multiple treatment comparison metaanalysis on interventions for hepatic encephalopathy Hepatic encephalopathy (HE) is a reversible neuropsychiatric syndrome associated with severe
Can t Stop the Seizing!
 Can t Stop the Seizing! Joseph Miller, MD, MS MCEP Critical Care March, 2019 Objectives Describe the importance of time to treatment Delineate treatment based on best evidence Describe novel diagnostic
Can t Stop the Seizing! Joseph Miller, MD, MS MCEP Critical Care March, 2019 Objectives Describe the importance of time to treatment Delineate treatment based on best evidence Describe novel diagnostic
FEBRILE SEIZURES. IAP UG Teaching slides
 FEBRILE SEIZURES 1 DEFINITION Febrile seizures are seizures that occur between the age of 6 and 60 months with a temperature of 38 C or higher, that are not the result of central nervous system infection
FEBRILE SEIZURES 1 DEFINITION Febrile seizures are seizures that occur between the age of 6 and 60 months with a temperature of 38 C or higher, that are not the result of central nervous system infection
Pain Rating Scale GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care.
 GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care. 2. Presentation Pain may be present in many different conditions. Management of pain in the field can help to reduce suffering, make transport
GG. PAIN MANAGEMENT (NEW 10) 1. Initiate General Patient Care. 2. Presentation Pain may be present in many different conditions. Management of pain in the field can help to reduce suffering, make transport
Influence of blinding on treatment effect size estimate in randomized controlled trials of oral health interventions
 Saltaji et al. BMC Medical Research Methodology (218) 18:42 https://doi.org/1.1186/s12874-18-491- RESEARCH ARTICLE Open Access Influence of blinding on treatment effect size estimate in randomized controlled
Saltaji et al. BMC Medical Research Methodology (218) 18:42 https://doi.org/1.1186/s12874-18-491- RESEARCH ARTICLE Open Access Influence of blinding on treatment effect size estimate in randomized controlled
Critical Thinking A tour through the science of neuroscience
 Critical Thinking A tour through the science of neuroscience NEBM 10032/5 Publication Bias Emily S Sena Centre for Clinical Brain Sciences, University of Edinburgh slides at @CAMARADES_ Bias Biases in
Critical Thinking A tour through the science of neuroscience NEBM 10032/5 Publication Bias Emily S Sena Centre for Clinical Brain Sciences, University of Edinburgh slides at @CAMARADES_ Bias Biases in
Antiepileptics Audit
 Antiepileptics Audit Dr Kate Marley Dr Lucy Potter Dr Melanie Brooks Dr Averil Fountain CNS Sue Croft External Reviewer: Dr A Nicolson Consultant Neurologist c CURRENT GUIDANCE 4.1 GENERAL PRINCIPLES Anti-epileptic
Antiepileptics Audit Dr Kate Marley Dr Lucy Potter Dr Melanie Brooks Dr Averil Fountain CNS Sue Croft External Reviewer: Dr A Nicolson Consultant Neurologist c CURRENT GUIDANCE 4.1 GENERAL PRINCIPLES Anti-epileptic
A comparison of lorazepam and diazepam as initial therapy in convulsive status epilepticus
 Q J Med 2002; 95:225 231 A comparison of lorazepam and diazepam as initial therapy in convulsive status epilepticus H.R. COCK 1 and A.H.V. SCHAPIRA 1,2 From the 1 Department of Clinical and Experimental
Q J Med 2002; 95:225 231 A comparison of lorazepam and diazepam as initial therapy in convulsive status epilepticus H.R. COCK 1 and A.H.V. SCHAPIRA 1,2 From the 1 Department of Clinical and Experimental
Clinical Policy Title: Cardiac rehabilitation
 Clinical Policy Title: Cardiac rehabilitation Clinical Policy Number: 04.02.02 Effective Date: September 1, 2013 Initial Review Date: February 19, 2013 Most Recent Review Date: February 6, 2018 Next Review
Clinical Policy Title: Cardiac rehabilitation Clinical Policy Number: 04.02.02 Effective Date: September 1, 2013 Initial Review Date: February 19, 2013 Most Recent Review Date: February 6, 2018 Next Review
Citation Characteristics of Research Published in Emergency Medicine Versus Other Scientific Journals
 ORIGINAL CONTRIBUTION Citation Characteristics of Research Published in Emergency Medicine Versus Other Scientific From the Division of Emergency Medicine, University of California, San Francisco, CA *
ORIGINAL CONTRIBUTION Citation Characteristics of Research Published in Emergency Medicine Versus Other Scientific From the Division of Emergency Medicine, University of California, San Francisco, CA *
Evidence based urology in practice: heterogeneity in a systematic review meta-analysis. Health Services Research Unit, University of Aberdeen, UK
 Version 6, 12/10/2009 Evidence based urology in practice: heterogeneity in a systematic review meta-analysis Mari Imamura 1, Jonathan Cook 2, Sara MacLennan 1, James N Dow 1 and Philipp Dahm 3 for the
Version 6, 12/10/2009 Evidence based urology in practice: heterogeneity in a systematic review meta-analysis Mari Imamura 1, Jonathan Cook 2, Sara MacLennan 1, James N Dow 1 and Philipp Dahm 3 for the
SAGE-547 for super-refractory status epilepticus
 NIHR Innovation Observatory Evidence Briefing: April 2017 SAGE-547 for super-refractory status epilepticus NIHRIO (HSRIC) ID: 10866 NICE ID: 8456 Status epilepticus is a single epileptic seizure lasting
NIHR Innovation Observatory Evidence Briefing: April 2017 SAGE-547 for super-refractory status epilepticus NIHRIO (HSRIC) ID: 10866 NICE ID: 8456 Status epilepticus is a single epileptic seizure lasting
Evaluating the results of a Systematic Review/Meta- Analysis
 Open Access Publication Evaluating the results of a Systematic Review/Meta- Analysis by Michael Turlik, DPM 1 The Foot and Ankle Online Journal 2 (7): 5 This is the second of two articles discussing the
Open Access Publication Evaluating the results of a Systematic Review/Meta- Analysis by Michael Turlik, DPM 1 The Foot and Ankle Online Journal 2 (7): 5 This is the second of two articles discussing the
Management of Complex Febrile Seizures
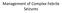 Management of Complex Febrile Seizures An 13 month old girl presents to the ED after having a shaking episode at home. Mom describes shaking of both arms and legs, lasting 20 minutes. The child has no
Management of Complex Febrile Seizures An 13 month old girl presents to the ED after having a shaking episode at home. Mom describes shaking of both arms and legs, lasting 20 minutes. The child has no
GABA A Receptor Trafficking during Status Epilepticus December 4, 2010
 GABA A Receptor Trafficking during Status Epilepticus December 4, 2010 Howard P. Goodkin, MD, PhD The Shure Associate Professor of Pediatric Neurology University of Virginia Charlottesville, VA American
GABA A Receptor Trafficking during Status Epilepticus December 4, 2010 Howard P. Goodkin, MD, PhD The Shure Associate Professor of Pediatric Neurology University of Virginia Charlottesville, VA American
Cochrane Central Register of Controlled Trials (CENTRAL) (The Cochrane Library)
 A systematic review of smoking cessation and relapse prevention interventions in parents of babies admitted to a neonatal unit (after delivery) Divya Nelson, Sarah Gentry, Caitlin Notley, Henry White,
A systematic review of smoking cessation and relapse prevention interventions in parents of babies admitted to a neonatal unit (after delivery) Divya Nelson, Sarah Gentry, Caitlin Notley, Henry White,
The QUOROM Statement: revised recommendations for improving the quality of reports of systematic reviews
 The QUOROM Statement: revised recommendations for improving the quality of reports of systematic reviews David Moher 1, Alessandro Liberati 2, Douglas G Altman 3, Jennifer Tetzlaff 1 for the QUOROM Group
The QUOROM Statement: revised recommendations for improving the quality of reports of systematic reviews David Moher 1, Alessandro Liberati 2, Douglas G Altman 3, Jennifer Tetzlaff 1 for the QUOROM Group
The Management of Refractory Status Epilepticus: An Update
 Epilepsia, 47(Suppl. 1):35 40, 2006 Blackwell Publishing, Inc. C International League Against Epilepsy The Management of Refractory Status Epilepticus: An Update Daniel H. Lowenstein Department of Neurology,
Epilepsia, 47(Suppl. 1):35 40, 2006 Blackwell Publishing, Inc. C International League Against Epilepsy The Management of Refractory Status Epilepticus: An Update Daniel H. Lowenstein Department of Neurology,
Supplementary Online Content
 Supplementary Online Content Wu HY, Peng YS, Chiang CK, et al. Diagnostic performance of random urine samples using albumin concentration vs ratio of albumin to creatinine for microalbuminuria screening
Supplementary Online Content Wu HY, Peng YS, Chiang CK, et al. Diagnostic performance of random urine samples using albumin concentration vs ratio of albumin to creatinine for microalbuminuria screening
Systematic Review of RCTs of Haemophilus influenzae Type b Conjugate Vaccines: Efficacy and immunogenicity
 Supplementary text 1 Systematic Review of RCTs of Haemophilus influenzae Type b Conjugate Vaccines: Efficacy and immunogenicity Review protocol Pippa Scott, Shelagh Redmond, Nicola Low and Matthias Egger
Supplementary text 1 Systematic Review of RCTs of Haemophilus influenzae Type b Conjugate Vaccines: Efficacy and immunogenicity Review protocol Pippa Scott, Shelagh Redmond, Nicola Low and Matthias Egger
