Pain Management Class Post-Test
|
|
|
- Opal Beasley
- 5 years ago
- Views:
Transcription
1 Name: Date: Unit: Pain Management Class Post-Test 1. Contraindications to regional anesthesia include (circle all that apply): a. Allergy to medication b. Clotting disorders or anticoagulation therapy with elevated PT/PTT/INR, and/or thrombocytopenia c. Spinal abnormalities that prevent catheter insertion d. Active infection without identified source e. Increased intracranial pressure 2. The following is true regarding ambulating a patient with an epidural, interpleural, intrathecal, and nerve block (circle all that apply): a. Check orthostatic blood pressure before ambulation. If SBP <90 mm Hg, and/or patient complains of dizziness, do not ambulate b. Do not ambulate patient with a Bromage Motor Scale <2 c. Licensed staff (PT or RN) must be present to assist in the initial ambulation (2 staff members) d. Ambulate the patient as per order of the Primary Service unless do not ambulate is ordered on the epidural, interpleural, and nerve block infusion orders form e. Do not ambulate any patient with an epidural, interpleural, intrathecal, and nerve block 3. True False Do not use alcohol to cleanse the insertion site because alcohol is neurotoxic. 4. Side effects of epidural, interpleural, intrathecal, or nerve block therapy may include all of the following except: a. Nausea b. Vomiting c. Itching d. Urinary retention e. Numbness f. Respiratory depression g. Urinary tract infection h. Constipation i. Twitching j. Confusion k. Hypotension l. Sedation
2 5. Notify Anesthesia Provide Staff (APS) and stop the infusion if necessary for all of the following except: a. Systolic Blood Pressure <90 mm Hg b. Respiratory rate <10 c. Heart Rate <80 d. Pain Scale >5 and c/o inadequate analgesia e. Sedation Scale (LOS) >4 f. Motor Scale >2 g. Seizure, confusion, complaints of metallic taste, tinnitus h. Side effects unrelieved with ordered medications i. Drip not infusing; disconnected, accidentally removed, leaking epidural catheter, redness, induration, drainage or pain at insertion site. 6. True False When a patient is receiving pain medications via Regional Anesthesia Catheter (R.A.C.) they should not be given sedatives, narcotics, anticoagulants (i.e. Lovenox, Heparin, Coumadin), antiplatlet medications (i.e.., Plavix, Pletal, Ticlid, etc.) aspirin, or additional antiemetics unless approved by Anesthesia Pain Service. 7. Match the tubing: a. Yellow tubing PCA b. Clear tubing Epidural Case Studies Your patient has an epidural in place regulated by a CADD pump. He has had a Total Knee replacement and you are just receiving him from PACU. He is complaining of a severe headache in the occipital region with a pain rating of 10. His vital signs are: B/P 160/90, heart rate 195, regular respirations of 19. His knee pain is rated at a What is your assessment? a. Patient has a subdural bleed b. The Dura was inadvertently punctured during epidural catheter insertion c. The epidural catheter is out of position d. The patient is developing an epidural catheter site infection 9. What is your treatment plan for this assessment? a. Neuro consult b. Page Pain Management Coordinator c. Increase CADD pump rate as per order d. Contact attending surgeon 10. What non-pharmaceutical modalities may help this patient? (Circle all that apply) a. Ambulate b. caffeine intake c. Hydrate d. Heat pack to back of head e. Darken room f. Bedrest (HOB elevation maximum of 30 degrees)
3 11. Anesthesia has decided to do a Blood Patch. What statement(s) is correct regarding this treatment? Circle all that apply a. May use 5-20 ml blood b. Provides a clot over the hole in the Dura to stop CSF leak c. Patient must remain supine for 4 hours after blood patch d. Blood is mixed with pain medication before insertion 12. A patient is Post-op day one, Radical Prostatectomy. Epidural meds are Bupivicaine 0.075% and Fentanyl 5 mcg/ml in 250 ml IV 5 ml/hr per CADD pump. VAS is 2 at rest. BP 124/52 supine, HR 68, RR 14, and Temp The patient is to ambulate for the first time. Your action: a. Assess patient s lower limb neuro status. Patient is able to lift legs off bed but indicates numbness in right thigh. You assist the patient to a sitting position and ask him to hold on to the IV pole as you proceed to ambulate. b. Maintain bedrest. Epidural therapy patients are not permitted to ambulate on post-op day one. c. Obtain an order to DC epidural catheter before ambulation d. Assess the patient s lower limb status including ability to lift legs off bed. There is no numbness or weakness in his legs and patient s BP in the sitting position is 120/ 60. You enlist the assistance of another person for the first ambulation. 13. Your patient is post-op day 3. During rounds the Anesthesia Pain Service writes an order to discontinue the epidural catheter. Darvocet N-100 is ordered Q4-6 hours prn for pain. Your action: a. Do not remove the catheter. Only a member of the Anesthesia Pain Service (APS) can discontinue the catheter b. Delegate the task to a nursing assistant c. Remove the dressing and tape. Cleanse the catheter and site well with alcohol. With the patient in a sitting position, pull on the catheter forcibly since a considerable amount of tension is required to remove the catheter. Apply a 4x4 over the site d. Loosen the tape and dressing carefully so as not to dislodge the catheter. Inspect the site for redness and swelling. Gently pull on the catheter applying steady tension. If resistance is met, stop and notify APS. If the catheter slides out easily, cleanse the site with alcohol and apply a bandaid. Note presence of black tip on catheter 14. Your patient is getting up to a chair at the bedside for the first time. Epidural is at 6ml/hr. BP 110/52 supine. After assisting the patient into a sitting position, you check the BP again. BP 78/38. The patient became diaphoretic and complained of dizziness. Your action: a. Assist the patient back into bed. Place her in a trendelenberg position and prepare a Dopamine drip b. Return the patient into a lying position with a pillow under his/her knees. Open IV s you may administer 500ml Normal saline over 30 minutes. Also consider administer Ephedrine 5-10mg IVP. If BP does not respond to fluids, call the Anesthesia Pain Service. c. Enlist the help of another nurse to get the patient into a chair. Place feet up on a stool and recheck the BP d. Return the patient to bed. Inform him/her you will attempt to get them up later. Reassure him that people experience decreased BP the first day after surgery and Recheck BP again in 30 minutes
4 15. Your patient is 8 hours post op. He is drowsy but arousable. When awakened he complains of pain with a VAS of 4. Standard epidural solution is infusing at 8ml/hr and Morphine Sulfate 4mg IVP has been given twice over the last 5 hours for breakthrough pain. He is unable to move his legs on command, however, moves is arms freely. No spontaneous movement of either leg is noted. Your action: a. Decrease the epidural solution by 1 hour b. Do nothing, wait until the patient is more awake to better evaluate the lower extremity status c. Stop the epidural infusion and notify Anesthesia Pain Service immediately d. Obtain an order to discontinue the Epidural catheter from the surgical resident so that another pain medication can be ordered 16. The most frequent side effects seen with Epidural therapy are: a. Itching, urinary retention and nausea/vomiting b. Rash, itching, paralysis c. Respiratory depression, hypotension, and nausea/vomiting d. Urinary retention, hematoma at the insertion site, nausea/vomiting 17. Your patient has an epidural solution infusing at 8ml/hr with a VAS 2 at rest and VAS 4 with activity. Temperature Post op day #3. The surgical resident orders to discontinue the epidural therapy and PCA morphine per protocol. Your action is to: a. Discontinue the epidural catheter and initiate the PCA therapy when the equipment is available b. Increase the epidural rate by 1ml and give breakthrough pain medication for the VAS of 4 c. Call for the PCA medication stat and discontinue the epidural when the alternate pain therapy is available and ready to be started d. Call Anesthesia Pain Service to evaluate the patient. If an order to discontinue is obtained from Anesthesia Pain Service, then discontinue the epidural catheter and initiate the PCA as ordered 18. After the epidural catheter is discontinued, charting on the Pain Management Flow Sheet must include: a. Time and date of removal, presence of a tip (blue/black/silver), description of site noting any redness, drainage or swelling, narcotic waste, that is documented by yourself and another nurse b. Waste is documented on the narcotic audit sheet only. Document date and time of catheter removal c. VAS at rest and with activity. Lower extremity sensation and motor strength. Alternative pain management ordered, and the time and date of removal d. Vital signs, including BP sitting and supine, amount of narcotic waste, documented by two nurses, and the date and time of removal 19. When placed correctly, the epidural catheter is : a. In the space between the bony vertebral canal and the dura. This space contain fat, blood vessels, and nerves b. In the lateral horn of the spinal cord c. Through the dura in the cerebral spinal fluid d. Only at the lumbar level
5 20. Your patient is preparing to get out of bed and his epidural catheter becomes tangled in the bed rails. The catheter becomes disconnected. Your action is: a. After wiping each end with alcohol, reconnect the tubing b. You cover the epidural port with a sterile 4x4 gauze and call the anesthesia Pain Service to obtain an order to D/C the catheter c. Reconnect immediately, do not wipe with alcohol because it is neurotoxic d. Cap the epidural port and obtain an alternate pain management therapy order from the surgical resident 21. Your patient is receiving an epidural solution at a rate of 10ml/hr. When doing your hourly vital sign checks, he is found to be lethargic, BP 106/54, HR 64, RR 6. Respirations are shallow and irregular. Your action: a. Decrease the epidural catheter rate to 5ml/hr. Call Respiratory therapy STAT for an oxygen mask set-up. When the patient is more alert, you may resume increasing rate PRN for a VAS >5 b. Stop the epidural infusion. Prepare the dilute narcan solution and call the house officer to obtain the order to administer c. Begin CPR and and ask another nurse to call for the rapid response team d. Stop the epidural infusion, prepare Narcan by diluting and administer 0.1mg IVP q 2-3 minutes: up to 0.4mg maximum, or until the patient responds with a RR > 10 bpm. Notify Anesthesia Pain Service 22. Your patient has a nerve block with Bupivicaine 0.20% running at 8ml/hr s/p a right shoulder rotator cuff repair. She complains of an inability to control her arm. Your action is: a. Turn down the rate to 7ml/hr b. Stop the infusion pump and notify Anesthesia Pain Service immediately c. Remove the catheter d. Explain that this is a normal response and ensure that the patient is safe, perhaps with an arm sling. You may turn the rate down PRN until motor function returns 23. Your patient is POD #2. VAS is 1 at rest and VAS 2-3 with activity, especially coughing or deep breathing. The Epidural solution is infusing at 4ml/hr. The infusion site and system checks are O.K. Vital Signs are stable and no other side effects are noted. Your action: a. Offer breakthrough pain medication when patient is getting ready to ambulate b. No action is necessary. Continue the present Epidural infusion rate c. Increase the epidural to 6ml/hr, prior to ambulating the patient and when patient returns to bed, decrease him/her back to 4ml/hr d. Decrease the epidural to 3ml/hr, and begin the weaning process 24. Your patient is receiving an Epidural infusion at 3 ml/hr. The patient is now restless, confused and disoriented. He is attempting to remove the tape and dressing from his back and had pulled out his IV which was then restarted. His last dose of heparin was approximately 1 hour ago. You action: a. Decrease the epidural rate to 2ml/hr and restrain the patient b. No action necessary c. Increase the epidural rate, the patient appears to be in a great deal of pain d. Stop the infusion and assign a person to stay with the patient. Notify APS
6 25. Assessment of the Bromage scale includes which of the following? a. Grip strength b. Level of consciousness c. Leg lift d. VAS 26. The major advantage of delivering narcotics via epidural is that they: a. Increase patient alertness b. Reduce pulmonary complications c. Contribute to earlier ambulation d. All of the above 27. True False Itching due to histamine release is inevitable with epidural therapy so all patients are placed on Benadryl IVP every 6 hours for relief 28. True False Pain is subjective. Only the person experiencing it knows how much it really hurts 29. True False Per Policy, only an epidural certified RN can take care of a patient receiving epidural therapy 30. True False If your patient is itching, standard epidural orders allow you to give one ampule (0.4mg) of Narcan IVP undiluted
VAN WERT COUNTY HOSPITAL. Policy/Procedure: Departmental No.: N 11-36A. Issue Date: 7-97 By: Nursing No. of Pages: 6
 VAN WERT COUNTY HOSPITAL Policy/Procedure: Departmental No.: N 11-36A Issue Date: 7-97 By: Nursing No. of Pages: 6 Reviewed: 9-14, 8-11, 8-10 Revised: 9-14 Distribution List: All Nursing Departments Concurrence:
VAN WERT COUNTY HOSPITAL Policy/Procedure: Departmental No.: N 11-36A Issue Date: 7-97 By: Nursing No. of Pages: 6 Reviewed: 9-14, 8-11, 8-10 Revised: 9-14 Distribution List: All Nursing Departments Concurrence:
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa
 CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.84 Subject: Policy: Purpose: Continuous Epidural Analgesia Acute or chronic pain relief provided to a patient
CENTRAL IOWA HEALTHCARE Marshalltown, Iowa CARE OF PATIENT POLICY & PROCEDURES Policy Number: 4.84 Subject: Policy: Purpose: Continuous Epidural Analgesia Acute or chronic pain relief provided to a patient
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Purpose: The goal of epidural anesthesia is to reduce or eliminate pain in the laboring patient.
 Alaska Native Medical Center: Mother Baby Unit Subject: Epidural Anesthesia/PCEA in Laboring Patients Guideline: Epidural Anesthesia in Laboring Patients REVISION DATE: March 2013 REPLACES: L&D Epidural
Alaska Native Medical Center: Mother Baby Unit Subject: Epidural Anesthesia/PCEA in Laboring Patients Guideline: Epidural Anesthesia in Laboring Patients REVISION DATE: March 2013 REPLACES: L&D Epidural
Sarah Reece-Stremtan M.D. Peripheral Nerve Blockade Neuraxial Blocks
 Neuraxial Anesthesia Sarah Reece-Stremtan M.D. Regional Anesthesia Peripheral Nerve Blockade Neuraxial Blocks Placed in the OR under general anesthesia by members of the regional anesthesia team 1 Sensory
Neuraxial Anesthesia Sarah Reece-Stremtan M.D. Regional Anesthesia Peripheral Nerve Blockade Neuraxial Blocks Placed in the OR under general anesthesia by members of the regional anesthesia team 1 Sensory
(Page 1 of 5) Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental Knee Left Total Hip Revision Total Shoulder
 (Page 1 of 5) Allergies/Sensitivities/Reactions: Height: Inches cm Weight: Kg Pounds = Automatic = Physician s option, Check off to Order Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental
(Page 1 of 5) Allergies/Sensitivities/Reactions: Height: Inches cm Weight: Kg Pounds = Automatic = Physician s option, Check off to Order Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental
Physician Orders ADULT: ANES Enhanced Recovery After Surgery (ERAS) Plan
 Initiate Orders Phase Non Categorized R Powerplan Open Care Sets/Protocols/PowerPlans Initiate Powerplan Phase Phase: Anes (ERAS) Pre-insertion Phase, When to Initiate: Other-See Special Instructions,
Initiate Orders Phase Non Categorized R Powerplan Open Care Sets/Protocols/PowerPlans Initiate Powerplan Phase Phase: Anes (ERAS) Pre-insertion Phase, When to Initiate: Other-See Special Instructions,
IR Central Venous Access [ ] Pre Procedure
![IR Central Venous Access [ ] Pre Procedure IR Central Venous Access [ ] Pre Procedure](/thumbs/90/104119758.jpg) IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
Module 10 Troubleshooting Guide
 Module 10 Troubleshooting Guide Your safety and wellbeing are our priority. Issues can occur during your treatment and it is important that you recognize the symptoms. This guide will teach you how to
Module 10 Troubleshooting Guide Your safety and wellbeing are our priority. Issues can occur during your treatment and it is important that you recognize the symptoms. This guide will teach you how to
Epidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal
 Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Epidural Infusions for Pain Relief Including Discharge Advice
 Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
Royal Manchester Children s Hospital Epidural Infusions for Pain Relief Including Discharge Advice Children s Pain Team- Information For Parents and Carers This leaflet aims to provide information for
Pharmacologic Pain Relief: It s Use in Labor. Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Spring, 2016
 Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Spring, 2016 Objectives Recognize common medications used in the management of labor pain
Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Spring, 2016 Objectives Recognize common medications used in the management of labor pain
WHS POSTOPERATIVE POWERPLAN CHANGES
 Medications simplified and standardized to improve safety and effectiveness in the management of pain, itching, nausea/vomiting. Management: o The Anesthesiologist will continue to manage pain in the PACU.
Medications simplified and standardized to improve safety and effectiveness in the management of pain, itching, nausea/vomiting. Management: o The Anesthesiologist will continue to manage pain in the PACU.
Analgesia. The modern approach. Dr. Mark Haworth MB.ChB.DA.MRCA.
 Analgesia The modern approach Dr. Mark Haworth MB.ChB.DA.MRCA. What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) How is pain
Analgesia The modern approach Dr. Mark Haworth MB.ChB.DA.MRCA. What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) How is pain
Going Home with Your Peripheral Nerve Catheter and Pain Relief Pump
 Northwestern Memorial Hospital Patient Education CARE AND TREATMENT If you have any questions about the pain relief pump, please call the Anesthesia Pain Service. Going Home with Your Peripheral Nerve
Northwestern Memorial Hospital Patient Education CARE AND TREATMENT If you have any questions about the pain relief pump, please call the Anesthesia Pain Service. Going Home with Your Peripheral Nerve
PATIENT CARE MANUAL POLICY
 PATIENT CARE MANUAL POLICY NUMBER VII-A-15 PAGE 1 OF 3 APPROVED BY: CATEGORY: Vice President and Senior Operating Officer; Rural Health Services & Professional Practice Lead Body Systems; Central Nervous
PATIENT CARE MANUAL POLICY NUMBER VII-A-15 PAGE 1 OF 3 APPROVED BY: CATEGORY: Vice President and Senior Operating Officer; Rural Health Services & Professional Practice Lead Body Systems; Central Nervous
THERAPY Baclofen Pump Program at Boston Children s Hospital
 BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
PEDIATRIC SPINE SURGERY POST-OP PLAN - Phase:.
 - Phase:. PHYSICIAN S Diagnosis Weight Allergies DETAILS Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert IV to INT when tolerating
- Phase:. PHYSICIAN S Diagnosis Weight Allergies DETAILS Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert IV to INT when tolerating
Title: RN Specialty Practice: RN Procedure: Epidural Catheter Removal. I.D. Number: 1080
 Policies and Procedures Title: EPIDURAL CATHETER REMOVAL RN Specialty Practice: RN Procedure: Epidural Catheter Removal I.D. Number: 1080 Authorization: [X] Former SKtnHR Nursing Practice Committee Source:
Policies and Procedures Title: EPIDURAL CATHETER REMOVAL RN Specialty Practice: RN Procedure: Epidural Catheter Removal I.D. Number: 1080 Authorization: [X] Former SKtnHR Nursing Practice Committee Source:
A Patient s Guide to Pain Management: Pain Pumps
 A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
Discharge Instructions: What to Expect After Lumbar Fusion
 Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
Discharge Instructions: What to Expect After Lumbar Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not take
POST-OP PAIN MANAGEMENT
 POST-OP PAIN MANAGEMENT You re Part of the Team Pain Management After Surgery Having a procedure or surgery to address a health issue can result in post-op (postoperative) pain. This pain can and should
POST-OP PAIN MANAGEMENT You re Part of the Team Pain Management After Surgery Having a procedure or surgery to address a health issue can result in post-op (postoperative) pain. This pain can and should
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
PEDIATRIC SPINE SURGERY POST-OP PLAN - Phase: Pediatric Spine Surgery General Orders
 - Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
- Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
Spinal Anaesthesia and Analgesia. Patient information Leaflet
 Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
Peripheral Nerve Blocks
 Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
Peripheral Nerve Blocks N U R S I N G E D U C A T I O N JPS Acute Pain Service Peripheral nerve blocks are used as part of a multimodal analgesic program which provides the patient with safe and effective
Having an Anaesthetic Your Questions Answered
 PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
Nursing Management Pre /Post Thrombolysis in Stroke
 Craigavon Area Hospital Guidelines for Nursing Management Pre /Post Thrombolysis in Stroke 1. A senior nurse in the stroke unit will be required to monitor the patients condition post Thrombolysis on a
Craigavon Area Hospital Guidelines for Nursing Management Pre /Post Thrombolysis in Stroke 1. A senior nurse in the stroke unit will be required to monitor the patients condition post Thrombolysis on a
Epidurals for pain relief after surgery Information for patients
 Epidurals for pain relief after surgery Information for patients Department of anaesthesia and pain medicine Epidurals for pain relief after surgery This information sheet explains what to expect when
Epidurals for pain relief after surgery Information for patients Department of anaesthesia and pain medicine Epidurals for pain relief after surgery This information sheet explains what to expect when
Lumbar drains. Information for patients Neurosurgery
 Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
Lumbar drains Information for patients Neurosurgery Why do I need drainage of my cerebrospinal fluid (CSF)? The brain and spinal cord are bathed in clear fluid like a baby in the womb. This cerebrospinal
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Having a Regional Anaesthetic Surgery and Critical Care Directorate of Operations
 Having a Regional Anaesthetic Surgery and Critical Care Directorate of Operations Information for patients about spinals, epidurals and nerve blocks. This information leaflet will be given to you by a
Having a Regional Anaesthetic Surgery and Critical Care Directorate of Operations Information for patients about spinals, epidurals and nerve blocks. This information leaflet will be given to you by a
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF)
 Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
Thrombolysis Delivery, Care, and Monitoring. 5 Acute Trusts - 6 Primary Care Trusts Ambulance Trust 4 Local Authorities
 Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Joint Replacement School 2015
 Joint Replacement School 2015 Anaesthetic choices for your hip / knee replacement Presented by the Anaesthetic Department Anaesthetists are doctors who take care of you during your surgery We will visit
Joint Replacement School 2015 Anaesthetic choices for your hip / knee replacement Presented by the Anaesthetic Department Anaesthetists are doctors who take care of you during your surgery We will visit
Your Spinal Anaesthetic
 Your Spinal Anaesthetic This leaflet is for anyone who may have a spinal anaesthetic. hope it will help you prepare and equip you to ask questions. Having a spinal anaesthetic for your operation. This
Your Spinal Anaesthetic This leaflet is for anyone who may have a spinal anaesthetic. hope it will help you prepare and equip you to ask questions. Having a spinal anaesthetic for your operation. This
Obstetrical Anesthesia. Safe Pain Relief for Childbirth
 Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
GEORGETOWN ORTHOPAEDIC SPINE SURGERY. Lumbar Decompression
 Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Lumbar Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Ibuprofen, Motrin, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS FOR 7-10 DAYS BEFORE SURGERY. These medications
Managing Pain and Sickness after Surgery
 Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Hip Hemiarthroplasty Post Op Version 2 4/20/17
 Patient Name: Diagnosis: Allergies with reaction type: Hip Hemiarthroplasty Post Op Version 2 4/20/17 Patient Placement General Diagnosis/Procedure: Preferred Location/Unit Ortho/Neuro PCU ICU General
Patient Name: Diagnosis: Allergies with reaction type: Hip Hemiarthroplasty Post Op Version 2 4/20/17 Patient Placement General Diagnosis/Procedure: Preferred Location/Unit Ortho/Neuro PCU ICU General
Date: I hereby consent to and authorize Chest Medicine Associates and other individuals involved in my care to perform a thoracentesis procedure.
 Consent for Surgical and Medical Treatment Patient Name: ----------- Date: --------------- Patient Number: _ Treatment Location: Chest Medicine Associates Date of Birth: ~~ I hereby consent to and authorize
Consent for Surgical and Medical Treatment Patient Name: ----------- Date: --------------- Patient Number: _ Treatment Location: Chest Medicine Associates Date of Birth: ~~ I hereby consent to and authorize
Pain Module. Opioid-RelatedRespiratory Depression (ORRD)
 Pain Module Opioid-RelatedRespiratory Depression (ORRD) Characteristics of patients who are at higher risk for Opioid- Related Respiratory Depression (ORRD) Sleep apnea or sleep disorder diagnosis : typically
Pain Module Opioid-RelatedRespiratory Depression (ORRD) Characteristics of patients who are at higher risk for Opioid- Related Respiratory Depression (ORRD) Sleep apnea or sleep disorder diagnosis : typically
Optimize vent weaning and SBT outcomes. Identify underlying causes for SBT failures. Role SBT and weaning protocol have in respiratory care
 Optimize vent weaning and SBT outcomes Identify underlying causes for SBT failures Role SBT and weaning protocol have in respiratory care Lower risk of developing complications Lower risk of VAP, other
Optimize vent weaning and SBT outcomes Identify underlying causes for SBT failures Role SBT and weaning protocol have in respiratory care Lower risk of developing complications Lower risk of VAP, other
Children's (Pediatric) PICC Line Placement
 Scan for mobile link. Children's (Pediatric) PICC Line Placement A peripherally inserted central catheter (PICC line) is most often used to deliver medication over a long period. The doctor or nurse inserts
Scan for mobile link. Children's (Pediatric) PICC Line Placement A peripherally inserted central catheter (PICC line) is most often used to deliver medication over a long period. The doctor or nurse inserts
PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE
 1 PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE 2 Table of Contents page# Learning Objectives 3 Concepts of Pain Relief 4 Introduction to PCA 4 Definition of terms used with IV PCA 6 Opioids used with
1 PATIENT CONTROLLED ANALGESIA LEARNING PACKAGE 2 Table of Contents page# Learning Objectives 3 Concepts of Pain Relief 4 Introduction to PCA 4 Definition of terms used with IV PCA 6 Opioids used with
THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery
 THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery Clearance: Prior to surgery you will need surgical clearance from your Primary Care Physician and/ or Cardiologist, if recommended.
THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery Clearance: Prior to surgery you will need surgical clearance from your Primary Care Physician and/ or Cardiologist, if recommended.
Spinal anaesthesia for hip and knee joint replacement surgery. Trauma and Orthopaedics Patient Information Leaflet
 Spinal anaesthesia for hip and knee joint replacement surgery Trauma and Orthopaedics Patient Information Leaflet Spinal anaesthesia for hip and knee joint replacement surgery For many operations patients
Spinal anaesthesia for hip and knee joint replacement surgery Trauma and Orthopaedics Patient Information Leaflet Spinal anaesthesia for hip and knee joint replacement surgery For many operations patients
Thrombolysis Assessment
 Thrombolysis Assessment Brief Clinical Summary of symptom onset of arrival of patient of assessment BP GCS BM If BM
Thrombolysis Assessment Brief Clinical Summary of symptom onset of arrival of patient of assessment BP GCS BM If BM
Understanding your risk of blood clots from hospital to home and how Bevyxxa may help
 Understanding your risk of blood clots from hospital to home and how Bevyxxa may help People who take Bevyxxa and have medicine injected into their spinal and epidural area, or have a spinal puncture,
Understanding your risk of blood clots from hospital to home and how Bevyxxa may help People who take Bevyxxa and have medicine injected into their spinal and epidural area, or have a spinal puncture,
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs
 Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Fracture Surgery. Post-Operative Care. And. Rehabilitation Protocol
 PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
Your Anaesthetic Explained
 Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Thyroid or Parathyroid Surgery
 PATIENT EDUCATION patienteducation.osumc.edu This handout gives you information about what to expect before, during and after your surgery. If you have questions, ask your nurse or doctor for more information.
PATIENT EDUCATION patienteducation.osumc.edu This handout gives you information about what to expect before, during and after your surgery. If you have questions, ask your nurse or doctor for more information.
All about your anaesthetic
 Patient information leaflet All about your anaesthetic Spinal anaesthesia and 3 associated risks For patients having a surgical procedure at a Care UK independent diagnostic and treatment centre This
Patient information leaflet All about your anaesthetic Spinal anaesthesia and 3 associated risks For patients having a surgical procedure at a Care UK independent diagnostic and treatment centre This
Annual Pain Competency
 Annual Pain Competency 2016 Revised for RBMC Please call Professional Development at X4196 or X5947 if you have any questions The learner will be able to: Objectives Explain pain scales & appropriate use
Annual Pain Competency 2016 Revised for RBMC Please call Professional Development at X4196 or X5947 if you have any questions The learner will be able to: Objectives Explain pain scales & appropriate use
Prof A Pourazar Immunohematologist
 Prof A Pourazar Immunohematologist What is plasma? Plasma is part of blood. It is the liquid that supports the circulation of red blood cells, white blood cells and platelets. Plasma is mainly water and
Prof A Pourazar Immunohematologist What is plasma? Plasma is part of blood. It is the liquid that supports the circulation of red blood cells, white blood cells and platelets. Plasma is mainly water and
Thoracic Epidural Injection
 Thoracic Epidural Injection 1 Introduction Before you agree to have your lumbar epidural, it is sensible to know all you can about it. This means knowing why you may need the epidural, what the procedure
Thoracic Epidural Injection 1 Introduction Before you agree to have your lumbar epidural, it is sensible to know all you can about it. This means knowing why you may need the epidural, what the procedure
Your spinal anaesthetic
 Your spinal anaesthetic This booklet is for anyone who may have a spinal anaesthetic. We hope it will help you prepare and equip you to ask questions. This booklet explains what to expect when you have
Your spinal anaesthetic This booklet is for anyone who may have a spinal anaesthetic. We hope it will help you prepare and equip you to ask questions. This booklet explains what to expect when you have
You and your anaesthetic Information to help patients prepare for an anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia Explained and www.youranaesthetic.info This leaflet gives basic information to help
You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia Explained and www.youranaesthetic.info This leaflet gives basic information to help
(30689) PROT Pain PCA Adult Patient Controlled Analgesia
 Diagnosis Allergies Nursing Assess and Document PCA: 1. Assess and document pain rating, sedation level and respiratory rate every 2 hours; assess and document pain rating, sedation level and respiratory
Diagnosis Allergies Nursing Assess and Document PCA: 1. Assess and document pain rating, sedation level and respiratory rate every 2 hours; assess and document pain rating, sedation level and respiratory
Discharge Instructions What to Expect After Cervical Fusion
 Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
Discharge Instructions What to Expect After Cervical Fusion Incision Care You may shower 72 hours after you have been discharged from the hospital unless otherwise stated by Dr. Valente. Please do not
Chapter 16 Moving and Positioning Patients
 Chapter 16 Moving and Positioning Patients Terminology Related to Movement Contractures Shortening and tightening of muscles due to disuse Dorsiflexion Bending of the foot in an upward direction Plantar
Chapter 16 Moving and Positioning Patients Terminology Related to Movement Contractures Shortening and tightening of muscles due to disuse Dorsiflexion Bending of the foot in an upward direction Plantar
You and your anaesthetic
 Questions you may like to ask your anaesthetist Q Who will give my anaesthetic? Q Do I have to have a general anaesthetic? Q What type of anaesthetic do you recommend? Q Have you often used this type of
Questions you may like to ask your anaesthetist Q Who will give my anaesthetic? Q Do I have to have a general anaesthetic? Q What type of anaesthetic do you recommend? Q Have you often used this type of
DOCUMENT CONTROL PAGE
 DOCUMENT CONTROL PAGE Title Title: GUIDELINES FOR THE MANAGEMENT OF CONTINUOUS EPIDURAL INFUSION IN CHILDREN Version: 3 Reference Number: Supersedes Supersedes: All previous versions (1998, 2007) Description
DOCUMENT CONTROL PAGE Title Title: GUIDELINES FOR THE MANAGEMENT OF CONTINUOUS EPIDURAL INFUSION IN CHILDREN Version: 3 Reference Number: Supersedes Supersedes: All previous versions (1998, 2007) Description
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery. Updated Jan 2017
 Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
Thank you for choosing Saint Joseph s Hospital Health Center for your spine surgery Updated Jan 2017 This class is designed to give you some basic, important information about spine surgery We will cover
ISPUB.COM. Epidural For Pain Control After Surgery. A Kowalski, O Wenker WHAT IS AN EPIDURAL? WHY SHOULD I HAVE AN EPIDURAL?
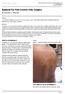 ISPUB.COM The Internet Journal of Pain, Symptom Control and Palliative Care Volume 2 Number 1 A Kowalski, O Wenker Citation A Kowalski, O Wenker.. The Internet Journal of Pain, Symptom Control and Palliative
ISPUB.COM The Internet Journal of Pain, Symptom Control and Palliative Care Volume 2 Number 1 A Kowalski, O Wenker Citation A Kowalski, O Wenker.. The Internet Journal of Pain, Symptom Control and Palliative
Paravertebral policy. The Acute pain Management Dept, UCLH
 UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
UCLH PARAVERTEBRAL BLOCK (ADULTS) POLICY Paravertebral policy. The Acute pain Management Dept, UCLH DEFINITION A Paravertebral block is a method of providing effective analgesia using a local anaesthetic.
Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
What is a catheter? What do I need to learn about catheter care?
 Catheter care What is a catheter? A catheter is a tube that drains urine from your child s body. The catheter is connected to tubing and a bag to collect the urine. Catheters come in different sizes and
Catheter care What is a catheter? A catheter is a tube that drains urine from your child s body. The catheter is connected to tubing and a bag to collect the urine. Catheters come in different sizes and
Pain Management: Epidural Steroid Injections
 A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Pain Management: Epidural Steroid Injections 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from
Physician s Order Form. Physician s Order Form. Telemetry/Progressive Care Orders. Continued on next page. >>>>>>> Continued on next page.
 DATE: TIME: DATE TIME INTRAVENOS FLID and MEDICATION Status: Admit to Telemetry Admit to Progressive Care nit Transfer to Progressive Care nit Note: Discontinue Previous Orders Transfer to Telemetry nit
DATE: TIME: DATE TIME INTRAVENOS FLID and MEDICATION Status: Admit to Telemetry Admit to Progressive Care nit Transfer to Progressive Care nit Note: Discontinue Previous Orders Transfer to Telemetry nit
Pharmacologic Pain Relief: It s Use in Labor
 Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Fall, 2016 Objectives Recognize common medications used in the management of labor pain
Pharmacologic Pain Relief: It s Use in Labor Linda Robinson MSN, RNC Clinical Nurse Specialist, Northwest Hospital Fall, 2016 Objectives Recognize common medications used in the management of labor pain
TRANSURETHRAL RESECTION OF THE PROSTATE
 TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
TRANSURETHRAL RESECTION OF THE PROSTATE A discussion of the operation and the pre and post operative care You and your doctor have considered the possibility that you have a transurethral resection of
Before and After Your Surgery
 UW MEDICINE PATIENT EDUCATION Before and After Your Surgery Artificial urinary sphincter or male urethral sling surgery This handout explains how to prepare for and what to expect after artificial urinary
UW MEDICINE PATIENT EDUCATION Before and After Your Surgery Artificial urinary sphincter or male urethral sling surgery This handout explains how to prepare for and what to expect after artificial urinary
PHYSICIAN'S ORDERS Mark in for desired orders. If is blank, order is inactive. VENTILATOR SEDATION / ANALGESIC / DELIRIUM ORDER
 Nursing Daily awakenings PHYSICIAN'S ORDERS Mark in for desired orders. If is blank, order is inactive. VENTILATOR SEDATION / ANALGESIC / DELIRIUM ORDER Do not perform daily awakenings: Rationale: Daily
Nursing Daily awakenings PHYSICIAN'S ORDERS Mark in for desired orders. If is blank, order is inactive. VENTILATOR SEDATION / ANALGESIC / DELIRIUM ORDER Do not perform daily awakenings: Rationale: Daily
LONG TERM CARE FACILITY ADMIT ORDERS
 Page 1 of 7 LONG TERM CARE FACILITY ADMIT ORDERS ADMISSION: Admit patient to Skilled Nursing Facility: Admit patient to Acute Rehabilitation Facility: Admit patient to Subacute Rehabilitation Facility:
Page 1 of 7 LONG TERM CARE FACILITY ADMIT ORDERS ADMISSION: Admit patient to Skilled Nursing Facility: Admit patient to Acute Rehabilitation Facility: Admit patient to Subacute Rehabilitation Facility:
Information about Your Anaesthetic and Pain Control After Surgery
 Information about Your Anaesthetic and Pain Control After Surgery Information for patients Specialist Support If you require this leaflet in another language, large print or another format, please contact
Information about Your Anaesthetic and Pain Control After Surgery Information for patients Specialist Support If you require this leaflet in another language, large print or another format, please contact
ID Number: To maintain consistent standards for monitoring CSF drainage and the patients neurological status.
 Policies & Procedures Title: Cerebrospinal Fluid (CSF) Drainage LUMBAR - Post Thoraco-aortic Aneurysm - Management of drainage system - Spinal pressure monitoring - Care of patient - Assisting with removal
Policies & Procedures Title: Cerebrospinal Fluid (CSF) Drainage LUMBAR - Post Thoraco-aortic Aneurysm - Management of drainage system - Spinal pressure monitoring - Care of patient - Assisting with removal
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR
 GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
GUIDELINES FOR PERIPHERAL NERVE / PLEXUS BLOCK CATHETER MANAGEMENT DEPARTMENT OF ANAESTHESIOLOGY AND INTENSIVE CARE HOSPITAL KUALA LUMPUR INTRODUCTION Regional block provides superior pain relief, compared
Anaesthetic choices for hip or knee replacement
 Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
Anaesthesia and pain (Daycase Patient) Patient information Leaflet
 Anaesthesia and pain (Daycase Patient) Patient information Leaflet February 2018 INTRODUCTION Welcome to Tameside Hospital, this leaflet gives basic information to help you prepare for your anaesthetic,
Anaesthesia and pain (Daycase Patient) Patient information Leaflet February 2018 INTRODUCTION Welcome to Tameside Hospital, this leaflet gives basic information to help you prepare for your anaesthetic,
Tips for Successful Venipuncture
 Page 1 of 5 Patient Positioning Have patient lie or sit down. Never draw blood on a patient who is standing. Make the patient as comfortable as you possibly can. Always watch and ask patient if he/she
Page 1 of 5 Patient Positioning Have patient lie or sit down. Never draw blood on a patient who is standing. Make the patient as comfortable as you possibly can. Always watch and ask patient if he/she
You and your anaesthetic Information to help patients prepare for an anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia explained and www.youranaesthetic.info This leaflet gives basic information to help
You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia explained and www.youranaesthetic.info This leaflet gives basic information to help
Proof 2. CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery /
 CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery / Proof 2 Addressograph/Plaque Cancer Assessment Clinic (CAC) Date: yyaa mm dj Day
CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery / Proof 2 Addressograph/Plaque Cancer Assessment Clinic (CAC) Date: yyaa mm dj Day
Lumbar Fusion. Reference Guide for PACU CLINICAL PATHWAY. All patient variances to the pathway are to be circled and addressed in the progress notes.
 Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Reference Guide for PACU Lumbar Fusion CLINICAL PATHWAY All patient variances to the pathway are to be circled and addressed in the progress notes. This Clinical Pathway is intended to assist in clinical
Physician Orders ADULT: Kidney-Panc/PancTransplant Post Op Plan
 Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase T;N, Phase: Kidney-Panc/Panc Transp Post Op Phase, When to Initiate: Kidney-Panc/Panc Transp Post Op Phase Vital Signs Vital
Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase T;N, Phase: Kidney-Panc/Panc Transp Post Op Phase, When to Initiate: Kidney-Panc/Panc Transp Post Op Phase Vital Signs Vital
Pain Relief Options for Labor. Providing you with quality care, information and support
 Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
TOTAL KNEE ARTHROPLASTY (Total Knee Replacement) The Knee Joint
 (Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
(Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
Welcome to the Royal Orthopaedic Hospital (ROH). For further information please visit
 Produced: May 2015 Ref: 259v01 Review: May 2017 Author: Theatres, Anaesthetics and Critical Care Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Your Anaesthetic Welcome to the Royal
Produced: May 2015 Ref: 259v01 Review: May 2017 Author: Theatres, Anaesthetics and Critical Care Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Your Anaesthetic Welcome to the Royal
SURGICAL NEURAXIAL ANALGESIA/ANESTHESIA EPIDURAL/PARAVERTEBRAL/ INTRATHECAL/PERIPHERAL REGIONAL, INTERMITTENT OR CONTINUOUS
 KINGSTON GENERAL HOSPITAL SURGICAL NEURAXIAL ANALGESIA/ANESTHESIA: EPIDURAL/PARAVERTEBRAL/ INTRATHECAL/PERIPHERAL REGIONAL, INTERMITTENT OR CONTINUOUS ANALGESIA/ANESTHESIA LEARNING GUIDE Prepared by: Nursing
KINGSTON GENERAL HOSPITAL SURGICAL NEURAXIAL ANALGESIA/ANESTHESIA: EPIDURAL/PARAVERTEBRAL/ INTRATHECAL/PERIPHERAL REGIONAL, INTERMITTENT OR CONTINUOUS ANALGESIA/ANESTHESIA LEARNING GUIDE Prepared by: Nursing
Dr. Clark s Frequently Asked Questions
 Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
Myelogram and Lumbar Puncture: Pre and Post Procedure Details
 Myelogram and Lumbar Puncture: Pre and Post Procedure Details (Revised October 2011) 1) Patients should be well hydrated. No solid food after midnight but clear liquids in the a.m. 2) Patients who take
Myelogram and Lumbar Puncture: Pre and Post Procedure Details (Revised October 2011) 1) Patients should be well hydrated. No solid food after midnight but clear liquids in the a.m. 2) Patients who take
IV Acetaminophen Pain Study for Neurosurgery Post Op Non ICU Admit Plan Begin Immediately/PACU
 Post Op Non ICU Admit Plan Begin Immediately/PACU PHYSICIAN S Weight Allergies Admit/Discharge/Transfer Request Patient Bed Requested Location: 3W, Pt Status: Inpatient (LOS > 2 midnights) Patient Condition
Post Op Non ICU Admit Plan Begin Immediately/PACU PHYSICIAN S Weight Allergies Admit/Discharge/Transfer Request Patient Bed Requested Location: 3W, Pt Status: Inpatient (LOS > 2 midnights) Patient Condition
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Your Spinal Anaesthetic Information for Patients
 Your Spinal Anaesthetic Information for Patients This leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients, patient representatives and
Your Spinal Anaesthetic Information for Patients This leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients, patient representatives and
The Surgical Patient. Objectives:
 The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
ANAESTHESIA & PAIN MANAGEMENT FOR KNEE REPLACEMENT
 BEFORE SURGERY ANAESTHESIA & PAIN MANAGEMENT FOR KNEE REPLACEMENT FASTING INSTRUCTIONS No food for 6 hours before your operation. It is okay to drink clear fluids up to 2 hours before surgery (water, clear
BEFORE SURGERY ANAESTHESIA & PAIN MANAGEMENT FOR KNEE REPLACEMENT FASTING INSTRUCTIONS No food for 6 hours before your operation. It is okay to drink clear fluids up to 2 hours before surgery (water, clear
Your Nerve Block & Home Pump For Hip Surgery
 Your Nerve Block & Home Pump For Hip Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 3/10 Why? To Help Control Postoperative Pain at Home A pump connected to
Your Nerve Block & Home Pump For Hip Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 3/10 Why? To Help Control Postoperative Pain at Home A pump connected to
Home Care Services HomeMed MedEQUIP Michigan Visiting Care Michigan Visiting Nurses Wheelchair Seating Service PROCEDURE
 UNIVERSITY OF MICHIGAN HOSPITALS AND HEALTH CENTERS UMHHC-HCS: 253.054 First Approved Date: 3/2010 Home Care Services HomeMed MedEQUIP Michigan Visiting Care Michigan Visiting Nurses Wheelchair Seating
UNIVERSITY OF MICHIGAN HOSPITALS AND HEALTH CENTERS UMHHC-HCS: 253.054 First Approved Date: 3/2010 Home Care Services HomeMed MedEQUIP Michigan Visiting Care Michigan Visiting Nurses Wheelchair Seating
