Effects of onabotulinumtoxina treatment in patients with and without allodynia: results of the COMPEL study
|
|
|
- Austen McCoy
- 5 years ago
- Views:
Transcription
1 Young et al. The Journal of Headache and Pain (2019) 20:10 The Journal of Headache and Pain RESEARCH ARTICLE Effects of onabotulinumtoxina treatment in patients with and without allodynia: results of the COMPEL study William B. Young 1*, J. Ivan Lopez 2, John F. Rothrock 3, Amelia Orejudos 4, Aubrey Manack Adams 4, Richard B. Lipton 5 and Andrew M. Blumenfeld 6 Open Access Abstract Background: OnabotulinumtoxinA is effective in treating chronic migraine (CM), but there are limited data assessing how allodynia affects preventive treatment responses. This subanalysis of the 108-week, multicenter, open-label COMPEL Study assessed the efficacy and safety of onabotulinumtoxina in people with CM with and without allodynia. Methods: Patients (n = 715) were treated with onabotulinumtoxina 155 U every 12 weeks for 9 treatment cycles. The Allodynia Symptom Checklist was used to identify patients with allodynia (scores 3). The primary outcome for this subanalysis was reduction in monthly headache days from baseline for weeks 105 to 108 in groups with and without allodynia. Other outcomes included assessments of moderate to severe headache days, disability (using the Migraine Disability Assessment [MIDAS] questionnaire), and health-related quality of life (Migraine-Specific Qualityof-Life Questionnaire [MSQ] v2). Adverse events and their relation to treatment were recorded. Results: OnabotulinumtoxinA was associated with a significant mean (SD) reduction in headache day frequency at week 108 relative to baseline in patients with (n = 289) and without (n = 426) allodynia ( 10.8 [7.1] and 12.5 [7.4], respectively; both P < 0.001) that was significantly greater in patients without allodynia (P = betweensubgroup comparison). Moderate to severe headache days were significantly reduced at week 108 in patients with and without allodynia ( 9.6 [6.9] and 10.5 [7.2]; both P < 0.001); reduction was similar between groups. MIDAS scores improved significantly at week 108 ( 53.0 [50.3] and 37.7 [53.0]; both P < 0.001), with a significant between-group difference in favor of those with allodynia (P = 0.005). Similarly, MSQ subscale scores (Role Function Preventive, Role Function Restrictive, Emotional Function) significantly improved at week 108 for patients with and without allodynia: 20.6 (21.9) and 16.9 (20.7), 28.0 (23.3) and 24.7 (22.7), and 27.6 (26.5) and 24.9 (26.1), respectively (all P < 0.001). OnabotulinumtoxinA was well tolerated in patients with and without allodynia. Conclusion: Results indicate that onabotulinumtoxina is associated with reductions from baseline in multiple efficacy outcomes for up to 108 weeks whether or not allodynia is present. The allodynia group showed a smaller treatment response for reduction in headache days, but a similar or greater treatment response for improvement in other measures. No new safety concerns were identified. Keywords: COMPEL, onabotulinumtoxina, Migraine, Allodynia, Disability, Quality of life * Correspondence: William.b.young@jefferson.edu 1 Jefferson Hospital for Neuroscience, 900 Walnut Street, Second Floor, Suite #200, Philadelphia, PA 19107, USA Full list of author information is available at the end of the article The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
2 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 2 of 10 Introduction Chronic migraine (CM) is a debilitating disease occurring in 1.4% to 2.2% of adults globally [1]. It is a distinct primary headache disease defined as headaches occurring on 15 days per month for > 3 months, with migraine features on 8 days per month [2]. People with CM have more allodynia and greater levels of migraine-associated disability than people with episodic migraine [3]. In clinical practice, allodynia, a common condition among people with CM [3, 4], has been associated with a reduced likelihood of a positive response to some acute treatments for migraine [5]. Data from the American Migraine Prevalence and Prevention study demonstrated that individuals with allodynia (defined as a sum score 3 on the Allodynia Symptom Checklist [ASC]) were significantly more likely to have an inadequate response to triptans, nonsteroidal anti-inflammatory drugs, opioids, and barbiturates than those without allodynia [5]. However, it remains unclear whether allodynia also influences response to preventive treatment. The efficacy and safety of onabotulinumtoxina for the prevention of CM was established in the double-blind placebo-controlled Phase III REsearch Evaluating Migraine Prophylaxis Therapy (PREEMPT) trials [6 8] and was further confirmed in the 32-week open-label extension phase [9]. The Chronic Migraine OnabotulinumtoxinA Prolonged Efficacy Open-Label (COMPEL) Study was designed to gather real-world evidence on the long-term management of CM by evaluating the efficacy and safety of onabotulinumtoxina after 9 treatments (108 weeks) [10, 11]. The COMPEL Study demonstrated that treatment with onabotulinumtoxina 155 U was associated with sustained reduction in headache day frequency and migraine-related disability in people with CM over 108 weeks [11]. The COMPEL Study also sought to determine the efficacy of onabotulinumtoxina in specific subgroups of interest that were not specifically assessed in or were excluded from the PREEMPT clinical study program. We undertook this analysis of the COMPEL Study to compare the efficacy and safety of onabotulinumtoxina in patients with CM with and without allodynia at baseline. Methods Primary study design The COMPEL Study (clinicaltrials.gov identifier NCT ) was a multicenter, open-label, prospective study in adult patients with CM across sites in the United States, Australia, and South Korea. The methodology of the COMPEL Study has been published previously and will be only briefly reviewed here for context [10]. OnabotulinumtoxinA (BOTOX ; Allergan plc, Dublin, Ireland) 155 U, with or without concomitant stable oral preventive medication, was administered every 12 weeks for 9 treatment cycles (108 weeks) [10] using the recommended fixed-site, fixed-dose injection paradigm [12]. Adult patients aged 18 years with a diagnosis of CM and with stable comorbidities were eligible for inclusion in the study if they had not previously received onabotulinumtoxina, even if they were taking a stable oral preventive treatment at baseline. We excluded patients who had severe major depressive disorder or suicidal ideation. The study received ethical approval from the institutional review board or independent ethics committee at each site, and we obtained written informed consent from all patients before study enrollment. The primary efficacy measure was the change from baseline in headache days per 28-day period (headache frequency) at 108 weeks (after 9 treatment cycles). The secondary efficacy measures were the change from baseline in headache days at week 60 (after 5 treatment cycles) and the mean change from baseline in the 6-item Headache Impact Test (HIT-6) total score over a 4-week period at weeks 60 and 108. Exploratory outcome measures included, but were not limited to, assessment of the change from baseline in moderate to severe headache days, HIT-6 scores throughout the study, migraine-related disability as assessed by Migraine Disability Assessment questionnaire (MIDAS) scores, and health-related quality of life as assessed by Migraine-Specific Quality-of-Life Questionnaire (MSQ) v2 scores. Moderate to severe headache days were assessed via a daily diary, and HIT-6 and MIDAS scores were assessed at each clinic visit, with higher scores indicating greater disability [13]. The MSQ, which consists of 3 subscales (Role Function Preventive, Role Function Restrictive, and Emotional Function) scored on a 0 to 100 scale, with higher scores indicating greater quality of life [14], was assessed at baseline and at weeks 48, 96, and 108. Safety and tolerability were assessed at each visit for all patients who received 1 onabotulinumtoxina treatment. Patients were withdrawn from the study for safety reasons if they showed any signs of suicidal ideation or became pregnant. Subgroup analysis The subgroups with and without allodynia at baseline were assessed. The ASC was used to identify those with allodynia during the 28-day screening period. We classified patients with an ASC score 3 as having allodynia and those with an ASC score < 3 as not having allodynia at baseline [15, 16]. Statistical analysis As previously reported, for the primary and secondary analyses, including change in headache days and change in HIT-6 scores from baseline, missing data were imputed using a modified last-observation-carried-forward
3 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 3 of 10 method [11]. Observed data were used for the exploratory analyses reported in this manuscript in patients with and without allodynia (headache day frequency, patient-reported outcomes, and safety). Analyses were descriptive and inferential, characterizing trends associated with onabotulinumtoxina treatment over 108 weeks. Differences from baseline for each subgroup (ie, those with and without allodynia) were determined, including only those patients who had data at baseline and at the time point being assessed. The differences between the subgroups (ie, between those with and those without allodynia at baseline) were determined using 2-sided t tests (alpha = 0.05). Results Patient demographics and disposition A total of 716 patients (safety population) were enrolled in the study. Of these patients, 715 received 1 doseof onabotulinumtoxina (analysis population). In the anal-ysis population, 289 patients (40.4%) had allodynia at baseline and 426 (59.6%) did not. Patient demographics at baseline were similar across subgroups, with the exception of sex (Table 1); patients with allodynia were slightly more likely to be women (86.9%) than those without allodynia (83.3%). Clinical characteristics were generally similar across subgroups, with the exception of previous preventive treatment (Table 1); patients with allodynia at baseline were more likely to have previously taken preventive treatment (84.1%) than those without allodynia (78.6%). Among all patients (N = 716), 373 (52.1%) completed the study. Of these patients, 282 had headache day data available for all 5 study visits (including baseline). The most common reasons for study discontinuation were withdrawal of consent (n = 92 [12.8%]), lost to follow-up (n = 82 [11.5%]), lack of efficacy (n = 25 [4.9%]), and adverse events (AEs; n = 25 [3.5%]). Of the 290 patients with allodynia, 157 (54.1%) completed the study compared with 216 (50.7%) of the 426 patients without allodynia. Of the patients with allodynia, a cumulative total of 46 patients (15.9%) discontinued after treatment 2, 85 (29.3%) after treatment 5, and 133 (45.9%) after the final treatment. Of the patients without allodynia, a cumulative total of 85 patients (20.0%) discontinued after treatment 2, 150 (35.2%) after treatment 5, and 210 (49.3%) after the final treatment. Efficacy outcomes Overall efficacy outcomes have been previously published [11] and will be reviewed only briefly here for context. In the analysis population of 715 patients, reductions in headache days were observed from the first assessment (at week 24, after 2 treatment cycles) and continued throughout the 108-week period. By week 108 Table 1 Baseline Patient Demographics and Clinical Characteristics of Patients With and Without Allodynia With Allodynia (n = 289) Without Allodynia (n = 426) Mean (SD) age, y 42.3 (11.3) 43.5 (11.2) Min, max 18,72 18,73 Female, n (%) 251 (86.9) 355 (83.3) Race, n (%) Caucasian 240 (83.0) 341 (80.0) Black 16 (5.5) 25 (5.9) Asian 31 (10.7) 58 (13.6) Native Hawaiian or other Pacific Islander 1 (0.3) 2 (0.5) American Indian or Alaska Native 1 (0.3) 0 (0.0) Mean (SD) BMI, kg/m (6.5) 27.3 (6.4) Mean (SD) age of migraine onset, y 32.2 (13.1) 32.7 (14.1) Mean (SD) time since onset of migraine, y 10.2 (10.5) 10.8 (11.3) Family history of migraine, n (%) 179 (61.7) 270 (63.4) Mean (SD) headache days at baseline 21.7 (4.8) 21.9 (4.9) Mean (SD) moderate to severe headache days at baseline 17.9 (5.6) 17.8 (5.7) Medication use at baseline, n (%)* Previously taken acute medications 288 (99.3) 419 (98.4) Previously taken preventive medications 244 (84.1) 335 (78.6) BMI body mass index *Data were based on the safety population
4 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 4 of 10 (after 9 treatment cycles), onabotulinumtoxina significantly reduced headache frequency from a mean (SD) baseline of 22.0 (4.8) days by 10.7 (6.4) days (P < ), resulting in 11.3 (7.4) headache days per 28-day period. Similarly, onabotulinumtoxina significantly reduced HIT-6 scores from a baseline score of 64.7 (4.8) by 6.8 (6.6) at week 60 and 7.1 (7.2) at week 108 (P < ). Of the 282 patients who completed the study and had headache day data available for all 5 study visits (including baseline), a slightly greater reduction in headache frequency from baseline ( 11.8 [7.3] days) was noted with onabotulinumtoxina treatment, resulting in a slightly lower number of headache days (9.8 [8.3] days) than in the total analysis population. Patients with versus without allodynia Effect on headache frequency At baseline, patients with allodynia had a mean (SD) of 21.7 [4.8] headache days compared with 21.9 [4.9] headache days in patients without allodynia. OnabotulinumtoxinA significantly reduced the mean (SD) frequency of headache days per 28-day period at week 24 in patients with and without baseline allodynia to 13.8 (8.1) and 14.3 (8.5) days, respectively; at week 60, to 11.8 (7.9) and 11.5 (8.4) days; and at week 108, to 10.5 (8.1) and 9.3 (8.3) days (P <0.001 for all within-group changes from baseline; Additional file 1: Fig. S1A). The change from baseline in headache days at week 24 was 8.4 (6.6) and 7.7 (6.9) days, respectively; at week 60, 9.9 (6.7) and 10.3 (7.3) days; and at week 108, 10.8 (7.1) and 12.5 (7.4) days (Fig. 1a). There was no significant between-group difference in the allodynia subgroups in the mean change in headache frequency from baselineatweek24( 0.7 days; P=0.265) and week 60 (0.4 days; P= 0.532); however, at week 108, there was a statistically significant difference between patients with versus without allodynia at baseline (1.7 days; P= 0.044) in favor of those without baseline allodynia. Similarly, onabotulinumtoxina significantly reduced moderate to severe headache days at week 24 in patients with and without baseline allodynia to 10.7 (7.2) and 11.2 (7.6) days, respectively; at week 60, to 9.1 (6.7) and 8.6 (7.0) days; and at week 108, to 7.7 (6.8) and 7.0 (6.9) days (P < for all within-group changes from baseline; Additional file 1: Figure S1B). The change from baseline in moderate to severe headache days at week 24 was 7.5 (6.1) and 6.7 (6.0) days, respectively; a b Fig. 1 OnabotulinumtoxinA effect on (a) headache days and (b) moderate to severe headache days. *Indicates P < for within-group change from baseline. P values shown in the figure indicate between-subgroup differences in change from baseline; data are observed data
5 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 5 of 10 at week 60, 8.7 (6.1) and 8.9 (6.2) days; and at week 108, 9.6 (6.9) and 10.5 (7.2) days (Fig. 1b). There was no significant between-group difference in change of moderate to severe headache frequency from baseline at any time point. Patient-reported outcomes OnabotulinumtoxinA significantly reduced mean (SD) HIT-6 total scores (with higher scores indicating greater disability) from baseline scores of 65.2 (4.5) and 64.5 (5.1) in patients with and without allodynia, respectively, to 59.2 (6.9) and 58.9 (7.2) for the 28-day period before week 24; to 57.9 (6.7) and 56.6 (7.8) at week 60; and to 56.0 (6.9) and 54.5 (8.3) at week 108. The change from baseline for patients with and without allodynia increased from 5.7 (6.7) and 5.5 (6.2), respectively, at week 24 to 8.4 (7.1) and 9.4 (7.9) at week 108 (P < for all within-group changes from baseline; Fig. 2a). There was no significant between-group difference in the reduction in HIT-6 scores from baseline at any time point. OnabotulinumtoxinA significantly reduced mean (SD) MIDAS total scores (with higher scores indicating greater disability) from baseline scores of 87.4 (58.5) and 71.6 (56.2) for patients with and without allodynia, respectively, to 41.3 (47.3) and 42.3 (52.2) at week 24; 36.2 (44.6) and 29.4 (43.1) at week 60; and 22.7 (25.5) and 26.1 (43.7) at week 108 (P < for all within-group changes from baseline). The change from baseline for patients with and without allodynia increased from 45.4 (57.1) and 29.6 (56.2), respectively, at week 24 to 53.0 (50.3) and 37.7 (53.0) at week 108 (Fig. 2b). There was a statistically significant between-group difference in the change of MIDAS scores from baseline in favor of those with allodynia at week 24 (mean between-group difference, 15.8; P = < 0.001) and at week 108 (mean between group difference, 15.3; P = 0.005). Similarly, MSQ domain scores were significantly increased (improved) at all time points compared with baseline scores regardless of allodynia status. Mean (SD) MSQ Role Function Preventive scores increased from a baseline of 57.0 (22.2) and 62.4 (22.3) for patients with and without allodynia, respectively, to 77.7 (20.4) and 80.9 (20.2) at week 48 and 81.3 (17.0) and 82.3 (19.3) at week 108 (P < for all within-group changes from baseline). The change from baseline for patients with a b Fig. 2 OnabotulinumtoxinA effect on (a) HIT-6 and (b) MIDAS scores. HIT-6 = 6-Item Headache Impact Test; MIDAS = Migraine Disability Assessment questionnaire. *Indicates P < for within-group comparison from baseline. P values shown in the figure indicate betweensubgroup differences in change from baseline; data are observed data
6 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 6 of 10 and without allodynia was similar, with no significant differences at week 48 (19.8 [20.9] and 17.6 [20.6], respectively) or at week 108 (20.6 [21.9] and 16.9 [20.7]; Fig. 3a). Mean (SD) MSQ Role Function Restrictive scores increased from a baseline of 39.2 (18.3) and 44.9 (20.1) for patients with and without allodynia, respectively, to 66.0 (21.7) and 68.3 (22.2) at week 48 and 70.2 (20.7) and 72.8 (21.2) at week 108 (P < for all within-group changes from baseline). The change from baseline for patients with and without allodynia was similar at week 48 (26.5 [22.3] and 21.6 [22.1], respec-tively) and week 108 (28.0 [23.3] and 24.7 [22.7]), with no significant differences at week 108 (Fig. 3b). Mean (SD) MSQ Emotional Function scores increased from a baseline of 46.4 (25.5) and 53.1 (26.2) for patients with and without allodynia, respectively, to 75.1 (25.1) and 78.0 (22.7) at week 48 and 80.1 (20.6) and 81.7 (21.9) at week 108 (P < for all within-group changes from baseline). The mean (SD) change from baseline for patients with and without allodynia was similar, with no significant differences at week 48 (26.7 [26.4] and 22.5 [25.3], respectively) or at week 108 (27.6 [26.5] and 24.9 [26.1]; Fig. 3c). The only significant between-group difference in mean (SD) change from baseline in any MSQ domain was for the change in the Role Function Restrictive domain at week 48 (4.8 [22.2]; P = 0.016; Fig. 3b). Safety and tolerability OnabotulinumtoxinA was well tolerated in both subgroups (Table 2). AEs occurred in 185 patients (63.8%) with allodynia and 251 patients (58.9%) without allodynia. Across the safety population, serious AEs included migraine (n = 6 [0.8%]); suicidal ideation (n = 5 [0.7%]); and noncardiac chest pain, malignant melanoma, and headache (n = 3 [0.4%] for each), with no clear differences observed in patients with and without allodynia. Only 1 serious AE was considered to be treatment-related (generalized rash in a patient without allodynia). Treatment-related AEs occurring in 2% of either subgroup included neck pain, eyelid ptosis, musculoskeletal stiffness, injection site pain, and headache (Table 2). Thirteen patients (1.8%) in the overall population discontinued from the study as a result of treatment-related AEs. Discussion The primary analysis of the COMPEL Study data demonstrated that onabotulinumtoxina 155 U was associated with reductions in headache day frequency and a range of patient-reported outcomes in people with CM over 9 treatment cycles and 108 weeks and with a favorable tolerability profile. These results replicate and extend the findings of the PREEMPT study [6, 8, 9]. Chronic migraine in people with allodynia is typically considered difficult to manage [5], particularly with acute treatments; however, little is known about the effect of allodynia on the response to preventive treatment. The COMPEL data presented herein provide the first analyses over 9 treatment cycles of the efficacy and safety of onabotulinumtoxina in patients with allodynia. Treatment was effective and well tolerated in patients regardless of whether they had allodynia at baseline. OnabotulinumtoxinA treatment resulted in a significantly greater improvement in MIDAS scores in patients with allodynia than in those without allodynia at baseline. Improvement in headache day frequency at week 108 was significantly lower in patients with allodynia compared with those without allodynia. For most other endpoints (eg, HIT-6 and MSQ scores), differences were not significant between those individuals with and without allodynia. Allodynia is associated with sensitization of sensory neurons, first in the trigeminal ganglion within 10 to 20 min of the onset of migraine pain (corresponding to face and scalp pain) and then in the spinal trigeminal nucleus (also known as the trigeminal nucleus caudalis or the trigeminal cervical complex) within 60 to 120 min of the onset of pain [17, 18]. Early administration of acute treatments for migraine is reported to prevent central sensitization, but is relatively ineffective once central sensitization, as expressed by cutaneous allodynia, has occurred [19]. Across a range of drug classes routinely used for the acute treatment of migraine attacks, the presence of allodynia was associated with a greater likelihood of inadequate 2-h (ie, triptans, nonsteroidal anti-inflammatory drugs, opioids, and ergot alkaloids) and 24-h (ie, triptans, nonsteroidal anti-inflammatory drugs, opioids, and barbiturates) pain-free responses [5]. The prevalence of allodynia was lower in our study population (n = 289 [40.4%]) than the prevalence reported in a large group of people with migraine (63.2%) [16] and in a much smaller sample of people with CM (92.5%) [3]. Regardless, in our population, the benefits observed following preventive treatment with onabotulinumtoxina was little influenced by the presence or absence of allodynia at baseline. After onabotulinumtoxina treatment, there was a significant improvement in all efficacy measures at 24, 60 and 108 weeks in patients with and without allodynia compared with baseline. There was a statistically significant between-group reduction in headache frequency in favor of patients without allodynia at week 108, but not at other time points. Furthermore, there was no significant difference in the effect of onabotulinumtoxina on change in moderate to severe headache frequency at any time point, regardless of allodynia status at baseline. These findings suggest that onabotulinumtoxina is capable of attenuating the central sensitization of the sensory neurons associated
7 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 7 of 10 a b c Fig. 3 OnabotulinumtoxinA effect on MSQ (a) Role Function Preventive, (b) Role Function Restrictive, and (c) Emotional Function subscores. MSQ = Migraine-Specific Quality-of-Life Questionnaire. *Indicates P < for within-group comparison from baseline. P values shown in the figure indicate between-subgroup differences in change from baseline; data are observed data with allodynia. However, the role of allodynia on the response to treatment needs to be explored further before definitive conclusions can be drawn. A recent meta-analysis of the treatment of migraine in people presenting to emergency departments, a population that would likely include people with allodynia, proposed that intravenous metoclopramide and prochlor-perazine, and subcutaneous sumatriptan should be offered to patients with acute migraine [20], suggesting that these treatments are effective, even after central sensitization of sensory neurons. Nonetheless, the availability of an effective preventive
8 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 8 of 10 Table 2 Summary of Adverse Events Occurring in Patients With and Without Allodynia With Allodynia (n = 290) Without Allodynia (n = 426) AEs, n (%) 1 AE 185 (63.8) 251 (58.9) Serious AE 36 (12.4) 39 (9.2) Discontinuation due to AE 14 (4.8) 18 (4.2) TRAEs, n (%) 1 TRAE 56 (19.3) 75 (17.6) TRAEs occurring in 1% of either subgroup Neck pain 15 (5.2) 14 (3.3) Eyelid ptosis 6 (2.1) 12 (2.8) Musculoskeletal stiffness 6 (2.1) 11 (2.6) Headache 6 (2.1) 6 (1.4) Injection site pain 5 (1.7) 9 (2.1) Facial paresis 4 (1.4) 5 (1.2) Muscular weakness 3 (1.0) 7 (1.6) Migraine 3 (1.0) 4 (0.9) Injection site hematoma 3 (1.0) 1 (0.2) Muscle spasms 3 (1.0) 1 (0.2) Skin tightness 1 (0.3) 6 (1.4) AE adverse event, TRAE treatment-related adverse event treatment will minimize the need for acute treatments in patients with CM. Physicians and patients alike seek preventive treatment that not only reduces headache days but also improves quality of life and reduces migraine-related disability [21]. Therefore, to assess the overall effectiveness of a treatment for CM, it is recommended that in addition to efficacy measures focused on headache frequency, disease-related disability and health-related quality of life should be assessed using validated tools [22]. A > 5 point change in HIT-6 scores is considered clinically meaningful for people with migraine [23]. In our study, onabotulinumtoxina resulted in a > 5 point change from baseline in HIT-6 total scores from week 24 onward, demonstrating a clinically meaningful improvement through week 108 in patients with or without allodynia. Similarly, MIDAS scores were reduced by approximately 40 points by week 60, regardless of allodynia status at baseline. OnabotulinumtoxinA preventive treatment did result in a slightly greater improvement in MIDAS scores in patients with allodynia than in those without allodynia, which was statistically significant at week 108 (P = 0.005); however, both subgroups experienced clinically meaningful improvements. Clinically meaningful differences in MSQ domain scores vary by the specific domain being assessed (Role Function Restrictive domain, 5-point improvement; Role Function Preventive domain, 5- to 8-point improvement; Emotional Function domain, 8- to 10-point improvement) [24]. In our study, regardless of allodynia status at baseline, onabotulinumtoxina treatment was associated with a clinically meaningful increase in all MSQ domain scores. When considered with the results from the other measures of migraine-related disability and quality of life we assessed, these results suggest that the reduction in headache frequency observed in the COMPEL Study would be clinically meaningful to patients with CM and no less so for patients with allodynia at baseline. Others have reported that the presence of allodynia may signal a phenotype resistant to acute treatment for migraine [5, 19, 25], although the benefit of some acute treatments in patients presenting to emergency departments with migraine [20] suggests that the correlation of allodynia with treatment resistance is not clear-cut. Although the effect of onabotulinumtoxina on headache frequency at week 108 was significantly lower in patients with allodynia than in those without allodynia, onabotulinumtoxina reduced moderate to severe headache frequency similarly in both groups. Furthermore, onabotulinumtoxina was at least as effective in patients with allodynia as those without allodynia across a range of secondary efficacy outcomes, suggesting that onabotulinumtoxina is a useful preventive treatment for those patients with CM with allodynia. Study limitations and strengths Open-label studies, although useful to gain additional information once the safety and efficacy profile of an intervention has been clearly established, are subject to inherent limitations, such as the lack of placebo comparison, loss to follow-up, and change in concomitant medication use over the course of the study. These limitations have been discussed more fully in a previous report [11]. Despite the low persistency rates, the treatment benefits we observed at week 24 in this anal-ysis continued to improve up to week 108, and the lack of between-group differences typically persisted, trends that reinforce our conclusions of this subgroup analysis. In addition, fluctuations in headache frequency over time that occur with CM can make the interpretation of results difficult [26]. It is recommended that validated disease-specific tools be used to assess health-related quality of life and disability [22]. Tools such as the HIT-6 and MSQ, which were used in this study, have been validated for use in CM [27, 28], and the MIDAS questionnaire has been validated in migraine [13] and is likely to be valid for use in CM [22], including patients with CM with allodynia. Nonetheless, given the subjective reporting and open-label nature of the study, the results should be interpreted cautiously [22].
9 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 9 of 10 Despite the potential limitations outlined previously, the reduction in headache frequency from baseline in the overall population from the COMPEL Study at week 24 parallels results from the double-blind placebo-controlled phase of the PREEMPT study ( 7.4 days vs 8.4 days, respectively) [8, 11]. Furthermore, results at week 24 for HIT-6 scores and week 48 for MSQ scores are similar to those reported at week 24 (HIT-6, 4.8; Role Function Preventive, ; Role Function Restrictive, ; Emotional Function, ) after the double-blind placebo-controlled phase of the PREEMPT study [8], supporting the relevance oftheresultsfromthecompelstudyand,byextension, this subanalysis of COMPEL data. Conclusions Data from the COMPEL Study support the sustained benefit and safety of onabotulinumtoxina for reducing headache days and disability and improving quality of life for up to 108 weeks (9 treatment cycles) in patients with CM with and without allodynia. The effect of onabotulinumtoxina on headache days at week 108 was significantly lower in patients with allodynia than in those without allodynia. However, the effect on other efficacy measures was similar or greater in those with allodynia versus those without allodynia, despite some reports that patients with allodynia are resistant to acute treatments. No new safety concerns were identified, and onabotulinumtoxina appeared to be well tolerated in patients with and without allodynia at baseline. Additional file Additional file 1: Figure S1. Effect of onabotulinumtoxina on (A) headache frequency and (B) moderate to severe headache frequency in patients with vs without allodynia at baseline. (PDF 15 kb) Abbreviations AE: Adverse event; ASC: Allodynia Symptom Checklist; CM: Chronic migraine; COMPEL: Chronic migraine OnabotulinuMtoxinA Prolonged Efficacy open- Label; HIT-6: 6-item Headache Impact Test; MIDAS: Migraine Disability Assessment questionnaire; MSQ: Migraine-Specific Quality-of-Life Questionnaire v2; PREEMPT: Phase III REsearch Evaluating Migraine Prophylaxis Therapy Acknowledgments This study was sponsored by Allergan plc (Dublin, Ireland). Writing and editorial assistance was provided to the authors by Lee B. Hohaia, PharmD, of Complete Healthcare Communications, LLC (North Wales, PA, USA), a CHC Group company, and was funded by Allergan plc (Dublin, Ireland). All authors met ICMJE authorship criteria. Neither honoraria nor payments were made for authorship. The authors thank the patients for their participation in the study. Principal investigators for the COMPEL Study included Lawrence D. Robbins, MD; Jan L. Brandes, MD; Tamara A. Miller, MD; Roger K. Cady, MD; Jo H. Bonner, MD; Paul K. Winner, DO, FAAN; Marshall C. Freeman, MD; Kathleen B. Mullin, MD; Andrew M. Blumenfeld, MD; Eric J. Eross, DO; Amy A. Gelfand, MD; Ejaz A. Shamim, MD; William B. Young, MD; John F. Rothrock, MD; Stephen H. Landy, MD; J. Ivan Lopez, MD; George R. Nissan, DO; Soma Sahai-Srivastava, MD; Marcia Ribeiro, MD; Maria-Carmen Wilson, MD; Jose M. Casanova, MD, PhD; Laszlo L. Mechtler, MD; Richard J. Stark, MBBS, FRCAP; Andrew H. Evans, MD; John D. O Sullivan, MD, MBBS; Joseph Frasca, MBBS; Min Kyung Chu, MD, PhD; Jeong-Wook Park, MD; ByungKun Kim, MD, PhD; Seong Taek Kim, DDS, MS, PhD; Kwang Soo Lee, MD, MS, PhD; Heui-Soo Moon, MD. Funding This study was sponsored by Allergan plc (Dublin, Ireland). Allergan funded the editorial and writing support and provided support for the study design and the collection, analysis, and interpretation of the data. Other than in their role as authors, employees of Allergan did not have a role in the final decision regarding which data to include in the manuscript or the decision to submit the manuscript for publication. Availability of data and materials Data reported in this manuscript are available within the article and its additional supplementary materials. Additional data from the COMPEL Study (ClinicalTrials.gov identifier NCT ) may be requested at Authors contributions WBY, JIL, and JFR made contributions to the analysis and interpretation of the data, drafting the manuscript, revising critically for important intellectual input, and gave final approval for publication. AO and AMA made substantial contributions to conception and design, analysis and interpretation of data, drafting the manuscript, and revising critically for important intellectual input; they gave final approval for publication of the manuscript and agree to be accountable for appropriate portions of the work. RBL made substantial contributions to the analysis and interpretation of the data, drafting the manuscript, and revising critically for important intellectual input; he gave final approval for publication. AMB made substantial contributions to conception and design, analysis and interpretation of data, drafting the manuscript, and revising critically for important intellectual input; he gave final approval for publication of the manuscript and agrees to be accountable for all aspects of the work. Ethics approval and consent to participate The study received ethical approval from the institutional review board or independent ethics committee at each site, and written informed consent was obtained from patients before study enrollment. Consent for publication Not applicable. Competing interests William B. Young has served on advisory boards for Alder, Allergan, Cipla, Lilly, and Supernus; has consulted for Allergan and Supernus; and has received research support from AGA, Alder, Allergan, Amgen, Autonomic Technology, Cumberland, Dr. Reddy s Laboratories, Eli Lilly, eneura, Merz, and St. Jude Medical. J. Ivan Lopez has no disclosures to report. John F. Rothrock has served on advisory boards and/or has consulted for Allergan, Lilly, Amgen, and Supernus. He also has received funding for travel and speaking from Supernus and has received honoraria from Allergan for participating as a speaker and preceptor at Allergan-sponsored educational programs. His parent institution has received funding from Allergan, Amgen, and Dr. Reddy s Laboratories for clinical research he has conducted. Amelia Orejudos is an employee of Allergan. Aubrey Manack Adams is an employee of Allergan and owns stock in the company. Richard B. Lipton serves on the editorial boards of Neurology and Cephalalgia and as senior advisor to Headache. He has received research support from the National Institutes of Health. He also receives support from the Migraine Research Foundation and the National Headache Foundation. He has reviewed for the National Institute on Aging and National Institute of Neurological Disorders and Stroke, serves as consultant or advisory board member or has received honoraria from Alder, Allergan, Amgen, Autonomic Technologies, Avanir, Biohaven, Biovision, Boston Scientific, Dr. Reddy s Laboratories, Electrocore, Eli Lilly, eneura Therapeutics, GlaxoSmithKline, Merck, Novartis, Pernix, Pfizer, Supernus, Teva, Trigemina, Vector, and Vedanta. He receives royalties from Wolff s Headache (8th Edition, Oxford University Press), Informa, and Wiley. He holds stock options in eneura Therapeutics and Biohaven. Andrew M. Blumenfeld has served on advisory boards for Allergan, Amgen, Alder, Teva, Supernus, Promius, Egalet, and Lilly and has received funding for speaking from Allergan, Amgen, Pernix, Supernus, Depomed, Avanir, and Promius.
10 Young et al. The Journal of Headache and Pain (2019) 20:10 Page 10 of 10 Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Jefferson Hospital for Neuroscience, 900 Walnut Street, Second Floor, Suite #200, Philadelphia, PA 19107, USA. 2 University of South Alabama College of Medicine, Mobile, AL, USA. 3 George Washington School of Medicine, Washington, DC, USA. 4 Allergan plc, Irvine, CA, USA. 5 Montefiore Headache Center, Department of Neurology, Department of Epidemiology and Population Health, Albert Einstein College of Medicine, Bronx, NY, USA. 6 Headache Center of Southern California, The Neurology Center, Carlsbad, CA, USA. Received: 1 October 2018 Accepted: 19 December 2018 References 1. Natoli JL, Manack A, Dean B, Butler Q, Turkel CC, Stovner L, Lipton RB (2010) Global prevalence of chronic migraine: a systematic review. Cephalalgia 30: Headache Classification Committee of the International Headache Society (2018) The international classification of headache disorders, 3rd edition. Cephalalgia 38: Benatto MT, Florencio LL, Carvalho GF, Dach F, Bigal ME, Chaves TC, Bevilaqua-Grossi D (2017) Cutaneous allodynia is more frequent in chronic migraine, and its presence and severity seems to be more associated with the duration of the disease. Arq Neuropsiquiatr 75: / X Chen N, Zhang J, Wang P, Guo J, Zhou M, He L (2015) Functional alterations of pain processing pathway in migraine patients with cutaneous allodynia. Pain Med 16: Lipton RB, Munjal S, Buse DC, Bennett A, Fanning KM, Burstein R, Reed ML (2017) Allodynia is associated with initial and sustained response to acute migraine treatment: results from the American Migraine Prevalence and Prevention Study. Headache 57: Aurora SK, Dodick DW, Turkel CC, DeGryse RE, Silberstein SD, Lipton RB, Diener HC, Brin MF (2010) OnabotulinumtoxinA for treatment of chronic migraine: results from the double-blind, randomized, placebo-controlled phase of the PREEMPT 1 trial. Cephalalgia 30: / Diener HC, Dodick DW, Aurora SK, Turkel CC, DeGryse RE, Lipton RB, Silberstein SD, Brin MF (2010) OnabotulinumtoxinA for treatment of chronic migraine: results from the double-blind, randomized, placebo-controlled phase of the PREEMPT 2 trial. Cephalalgia 30: / Dodick DW, Turkel CC, DeGryse RE, Aurora SK, Silberstein SD, Lipton RB, Diener HC, Brin MF (2010) OnabotulinumtoxinA for treatment of chronic migraine: pooled results from the double-blind, randomized, placebocontrolled phases of the PREEMPT clinical program. Headache 50: Aurora SK, Winner P, Freeman MC, Spierings EL, Heiring JO, DeGryse RE, VanDenburgh AM, Nolan ME, Turkel CC (2011) OnabotulinumtoxinA for treatment of chronic migraine: pooled analyses of the 56-week PREEMPT clinical program. Headache 51: Blumenfeld AM, Aurora SK, Laranjo K, Papapetropoulos S (2015) Unmet clinical needs in chronic migraine: rationale for study and design of COMPEL, an open-label, multicenter study of the long-term efficacy, safety, and tolerability of onabotulinumtoxina for headache prophylaxis in adults with chronic migraine. BMC Neurol 15: Blumenfeld AM, Stark RJ, Freeman MC, Orejudos A, Manack Adams A (2018) Long-term study of the efficacy and safety of onabotulinumtoxina for the prevention of chronic migraine: COMPEL study. J Headache Pain 19: BOTOX for injection, for intramuscular, intradetrusor, or intradermal use (onabotulinumtoxina). Full Prescribing Information, Allergan plc, Irvine, CA, Stewart W, Lipton R, Dowson A, Sawyer J (2001) Development and testing of the migraine disability assessment (MIDAS) questionnaire to assess headache-related disability. Neurology 56:S20 S28. WNL.56.suppl_1.S Martin BC, Pathak DS, Sharfman MI, Adelman JU, Taylor F, Kwong WJ, Jhingran P (2000) Validity and reliability of the migraine-specific quality of life questionnaire (MSQ version 2.1). Headache 40: /j x 15. Bigal ME, Ashina S, Burstein R, Reed ML, Buse D, Serrano D, Lipton RB, AMPP Group (2008) Prevalence and characteristics of allodynia in headache sufferers: a population study. Neurology 70: /01.wnl b1 16. Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML, Serrano D, Stewart WF, American Migraine Prevalence Prevention Advisory Group (2008) Cutaneous allodynia in the migraine population. Ann Neurol 63: Burstein R, Jakubowski M, Garcia-Nicas E, Kainz V, Bajwa Z, Hargreaves R, Becerra L, Borsook D (2010) Thalamic sensitization transforms localized pain into widespread allodynia. Ann Neurol 68: Burstein R, Jakubowski M, Rauch SD (2011) The science of migraine. J Vestib Res 21: Burstein R, Collins B, Jakubowski M (2004) Defeating migraine pain with triptans: a race against the development of cutaneous allodynia. Ann Neurol 55: Orr SL, Friedman BW, Christie S, Minen MT, Bamford C, Kelley NE, Tepper D (2016) Management of adults with acute migraine in the emergency department: the American Headache Society evidence assessment of parenteral pharmacotherapies. Headache 56: Silberstein S, Lipton R, Dodick D, Freitag F, Mathew N, Brandes J, Bigal M, Ascher S, Morein J, Wright P, Greenberg S, Hulihan J (2009) Topiramate treatment of chronic migraine: a randomized, placebo-controlled trial of quality of life and other efficacy measures. Headache 49: doi.org/ /j x 22. Silberstein S, Tfelt-Hansen P, Dodick DW, Limmroth V, Lipton RB, Pascual J, Wang SJ (2008) Guidelines for controlled trials of prophylactic treatment of chronic migraine in adults. Cephalalgia 28: x 23. Dodick DW, Turkel CC, DeGryse RE, Diener HC, Lipton RB, Aurora SK, Nolan ME, Silberstein SD (2015) Assessing clinically meaningful treatment effects in controlled trials: chronic migraine as an example. J Pain 16: doi.org/ /j.jpain Cole JC, Lin P, Rupnow MF (2009) Minimal important differences in the migraine-specific quality of life questionnaire (MSQ) version. Cephalalgia 29: Lipton RB, Munjal S, Buse DC, Fanning KM, Bennett A, Reed ML (2016) Predicting inadequate response to acute migraine medication: results from the American Migraine Prevalence and Prevention (AMPP) study. Headache 56: Serrano D, Lipton RB, Scher AI, Reed ML, Stewart WBF, Adams AM, Buse DC (2017) Fluctuations in episodic and chronic migraine status over the course of 1 year: implications for diagnosis, treatment and clinical trial design. J Headache Pain 18: Rendas-Baum R, Yang M, Varon SF, Bloudek LM, DeGryse RE, Kosinski M (2014) Validation of the Headache Impact Test (HIT-6) in patients with chronic migraine. Health Qual Life Outcomes 12: /s Rendas-Baum R, Bloudek LM, Maglinte GA, Varon SF (2013) The psychometric properties of the migraine-specific quality of life questionnaire version 2.1 (MSQ) in chronic migraine patients. Qual Life Res 22:
Effects of onabotulinumtoxina treatment in chronic migraine patients with and without daily headache at baseline: results from the COMPEL Study
 Young et al. The Journal of Headache and Pain (2019) 20:12 https://doi.org/10.1186/s10194-018-0953-0 The Journal of Headache and Pain RESEARCH ARTICLE Effects of onabotulinumtoxina treatment in chronic
Young et al. The Journal of Headache and Pain (2019) 20:12 https://doi.org/10.1186/s10194-018-0953-0 The Journal of Headache and Pain RESEARCH ARTICLE Effects of onabotulinumtoxina treatment in chronic
Richard B. Lipton, 1 Joel Saper, 2 Messoud Ashina, 3 David Biondi, 4 Suman Bhattacharya, 4 Joe Hirman, 5 Barbara Schaeffler, 4 Roger Cady 4
 A Phase 3, Randomized, Double-blind, Placebo-Controlled Study to Evaluate the Efficacy and Safety of for the Preventive Treatment of Chronic Migraine: Results of the PROMISE-2 (PRevention Of Migraine via
A Phase 3, Randomized, Double-blind, Placebo-Controlled Study to Evaluate the Efficacy and Safety of for the Preventive Treatment of Chronic Migraine: Results of the PROMISE-2 (PRevention Of Migraine via
Triptans: Nonresponse, Recurrence, and Serious AEs for Many Patients
 Efficacy, Safety, and Tolerability of Rimegepant 75 mg, an Oral CGRP Receptor Antagonist, for the Acute Treatment of Migraine: Results from a Phase 3, Double-Blind, Randomized, Placebo-Controlled Trial,
Efficacy, Safety, and Tolerability of Rimegepant 75 mg, an Oral CGRP Receptor Antagonist, for the Acute Treatment of Migraine: Results from a Phase 3, Double-Blind, Randomized, Placebo-Controlled Trial,
Promius Pharma, a subsidiary of Dr. Reddy s Laboratories, Princeton, NJ; 2 Vedanta Research, Chapel Hill, NC; 3
 Triptan Use and Discontinuation Among a Population Sample of Persons with Migraine: Results from Migraine in America Symptoms and Treatment (MAST) Study Aftab Alam, MBBS, MS, MBA 1 ; Sagar Munjal, MD 1
Triptan Use and Discontinuation Among a Population Sample of Persons with Migraine: Results from Migraine in America Symptoms and Treatment (MAST) Study Aftab Alam, MBBS, MS, MBA 1 ; Sagar Munjal, MD 1
Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse
 DOI 10.1186/s40064-015-1386-8 RESEARCH Open Access Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse Fayyaz Ahmed *, Hassan
DOI 10.1186/s40064-015-1386-8 RESEARCH Open Access Does analgesic overuse matter? Response to OnabotulinumtoxinA in patients with chronic migraine with or without medication overuse Fayyaz Ahmed *, Hassan
RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE
 RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE Gretchen E. Tietjen, MD University of Toledo Toledo, Ohio Learning objectives At the conclusion of this presentation, participants should be able to: 1. Understand
RISK FACTORS AND PROGNOSIS OF CHRONIC MIGRAINE Gretchen E. Tietjen, MD University of Toledo Toledo, Ohio Learning objectives At the conclusion of this presentation, participants should be able to: 1. Understand
Joel R. Saper, 1 Richard B. Lipton, 2 David B. Kudrow, 3 Joe Hirman, 4 David W. Dodick, 5 Stephen Silberstein, 6 George Chakhava, 7 Jeff Smith 8
 Primary Results of PROMISE-1 (PRevention Of Migraine via Intravenous eptinezumab Safety and Efficacy 1) Trial: a Phase 3, Randomized, Double-blind, Placebo-Controlled Study to Evaluate the Efficacy and
Primary Results of PROMISE-1 (PRevention Of Migraine via Intravenous eptinezumab Safety and Efficacy 1) Trial: a Phase 3, Randomized, Double-blind, Placebo-Controlled Study to Evaluate the Efficacy and
Per cent of patients with chronic migraine who responded per onabotulinumtoxina treatment cycle: PREEMPT
 Migraine 1 Department of Neurology, Thomas Jefferson University, Philadelphia, Pennsylvania, USA 2 Department of Neurology, Mayo Clinic Arizona, Phoenix, Arizona, USA 3 Department of Neurology and Neurological
Migraine 1 Department of Neurology, Thomas Jefferson University, Philadelphia, Pennsylvania, USA 2 Department of Neurology, Mayo Clinic Arizona, Phoenix, Arizona, USA 3 Department of Neurology and Neurological
abstract n engl j med 377;22 nejm.org November 30,
 The new england journal of medicine established in 1812 November 30, 2017 vol. 377 no. 22 for the Preventive Treatment of Chronic Migraine Stephen D. Silberstein, M.D., David W. Dodick, M.D., Marcelo E.
The new england journal of medicine established in 1812 November 30, 2017 vol. 377 no. 22 for the Preventive Treatment of Chronic Migraine Stephen D. Silberstein, M.D., David W. Dodick, M.D., Marcelo E.
Defining the Differences Between Episodic Migraine and Chronic Migraine
 Curr Pain Headache Rep (2012) 16:86 92 DOI 10.1007/s11916-011-0233-z CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Defining the Differences Between Episodic Migraine and Chronic Migraine Zaza Katsarava
Curr Pain Headache Rep (2012) 16:86 92 DOI 10.1007/s11916-011-0233-z CHRONIC DAILY HEADACHE (SJ WANG, SECTION EDITOR) Defining the Differences Between Episodic Migraine and Chronic Migraine Zaza Katsarava
David W. Dodick M.D. Professor Director of Headache Medicine Department of Neurology Mayo Clinic Phoenix Arizona USA
 Headache Masters School 2013 in Asia Sunday March 24, 2013 Procedural Medicine Workshop Onabotulinumtoxin A: Evidence, Injection Technique, and Mechanism of Action David W. Dodick M.D. Professor Director
Headache Masters School 2013 in Asia Sunday March 24, 2013 Procedural Medicine Workshop Onabotulinumtoxin A: Evidence, Injection Technique, and Mechanism of Action David W. Dodick M.D. Professor Director
OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with the PREEMPT paradigm
 Pedraza et al. SpringerPlus (2015) 4:176 DOI 10.1186/s40064-015-0957-z a SpringerOpen Journal RESEARCH Open Access OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with
Pedraza et al. SpringerPlus (2015) 4:176 DOI 10.1186/s40064-015-0957-z a SpringerOpen Journal RESEARCH Open Access OnabotulinumtoxinA treatment for chronic migraine: experience in 52 patients treated with
1/25/2018 ARE CGRP ANTAGONISTS ANY BETTER THAN CURRENT EVIDENCE BASED TREATMENTS? Disclosures: Objectives: Headache Division
 ARE CGRP ANTAGONISTS ANY BETTER THAN CURRENT EVIDENCE BASED TREATMENTS? Lawrence C Newman, MD, FAHS, FAAN Clinical Professor of Neurology Disclosures: Advisory Board: Alder, Allergan, Amgen, Lilly, Supernus,
ARE CGRP ANTAGONISTS ANY BETTER THAN CURRENT EVIDENCE BASED TREATMENTS? Lawrence C Newman, MD, FAHS, FAAN Clinical Professor of Neurology Disclosures: Advisory Board: Alder, Allergan, Amgen, Lilly, Supernus,
2 nd Resubmission. 13 January 2017
 2 nd Resubmission botulinum toxin A, 50 Allergan units, 100 Allergan units, 200 Allergan units, powder for solution for injection (Botox ) SMC No. (692/11) Allergan Limited 13 January 2017 The Scottish
2 nd Resubmission botulinum toxin A, 50 Allergan units, 100 Allergan units, 200 Allergan units, powder for solution for injection (Botox ) SMC No. (692/11) Allergan Limited 13 January 2017 The Scottish
OnabotulinumtoxinA in the treatment of patients with chronic migraine: clinical evidence and experience
 731521TAN0010.1177/1756285617731521Therapeutic Advances in Neurological DisordersC-C Chiang and AJ Starling research-article2017 Therapeutic Advances in Neurological Disorders Review OnabotulinumtoxinA
731521TAN0010.1177/1756285617731521Therapeutic Advances in Neurological DisordersC-C Chiang and AJ Starling research-article2017 Therapeutic Advances in Neurological Disorders Review OnabotulinumtoxinA
Calcitonin Gene-Related Peptide (CGRP) Inhibitors as Preventive Treatments for Patients with Episodic or Chronic Migraine: Effectiveness and Value
 Calcitonin Gene-Related Peptide (CGRP) Inhibitors as Preventive Treatments for Patients with Episodic or Chronic Migraine: Effectiveness and Value Background Draft Background and Scope December 4, 2017
Calcitonin Gene-Related Peptide (CGRP) Inhibitors as Preventive Treatments for Patients with Episodic or Chronic Migraine: Effectiveness and Value Background Draft Background and Scope December 4, 2017
medications. This was an openlabel study consisting of patients with migraines who historically failed to respond to oral triptan
 J Headache Pain (2007) 8:13 18 DOI 10.1007/s10194-007-0354-7 ORIGINAL Seymour Diamond Fred G. Freitag Alexander Feoktistov George Nissan Sumatriptan 6 mg subcutaneous as an effective migraine treatment
J Headache Pain (2007) 8:13 18 DOI 10.1007/s10194-007-0354-7 ORIGINAL Seymour Diamond Fred G. Freitag Alexander Feoktistov George Nissan Sumatriptan 6 mg subcutaneous as an effective migraine treatment
OnabotulinumtoxinA 155 U in medication overuse headache: a two years prospective study
 OnabotulinumtoxinA 155 U in medication overuse headache: a two years prospective study The Harvard community has made this article openly available. Please share how this access benefits you. Your story
OnabotulinumtoxinA 155 U in medication overuse headache: a two years prospective study The Harvard community has made this article openly available. Please share how this access benefits you. Your story
A two years open-label prospective study of OnabotulinumtoxinA 195 U in medication overuse headache: a real-world experience
 Negro et al. The Journal of Headache and Pain (2016) 17:1 DOI 10.1186/s10194-016-0591-3 RESEARCH ARTICLE A two years open-label prospective study of OnabotulinumtoxinA 195 U in medication overuse headache:
Negro et al. The Journal of Headache and Pain (2016) 17:1 DOI 10.1186/s10194-016-0591-3 RESEARCH ARTICLE A two years open-label prospective study of OnabotulinumtoxinA 195 U in medication overuse headache:
Research Submission. Accepted for publication December 14, 2004.
 Research Submission Botulinum Toxin Type A for the Prophylaxis of Chronic Daily Headache: Subgroup Analysis of Patients Not Receiving Other Prophylactic Medications: A Randomized Double-Blind, Placebo-Controlled
Research Submission Botulinum Toxin Type A for the Prophylaxis of Chronic Daily Headache: Subgroup Analysis of Patients Not Receiving Other Prophylactic Medications: A Randomized Double-Blind, Placebo-Controlled
Topiramate plus nortriptyline in the preventive treatment of migraine: a controlled study for nonresponders
 J Headache Pain (2012) 13:53 59 DOI 10.1007/s10194-011-0395-4 ORIGINAL Topiramate plus nortriptyline in the preventive treatment of migraine: a controlled study for nonresponders Abouch Valenty Krymchantowski
J Headache Pain (2012) 13:53 59 DOI 10.1007/s10194-011-0395-4 ORIGINAL Topiramate plus nortriptyline in the preventive treatment of migraine: a controlled study for nonresponders Abouch Valenty Krymchantowski
NEXT GENERATION MIGRAINE THERAPIES. Saturday, April 6, 2019 Sheraton San Diego Hotel & Marina-Bay Tower San Diego, California
 Saturday, April 6, 2019 Sheraton San Diego Hotel & Marina-Bay Tower San Diego, California Saturday, May 18, 2019 Westin Galleria Dallas Dallas, Texas Saturday, June 8, 2019 Marriott Marquis New York New
Saturday, April 6, 2019 Sheraton San Diego Hotel & Marina-Bay Tower San Diego, California Saturday, May 18, 2019 Westin Galleria Dallas Dallas, Texas Saturday, June 8, 2019 Marriott Marquis New York New
10/17/2017 CHRONIC MIGRAINES BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES PATIENT CASE EPIDEMIOLOGY EPIDEMIOLOGY
 BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
BOTOX: TO INJECT OR NOT INJECT? IN CHRONIC MIGRAINE PROPHYLAXIS OBJECTIVES JENNIFER SHIN, PHARMD PGY2 AMBULATORY CARE PHARMACY RESIDENT COMMUNITYCARE HEALTH CENTERS PHARMACOTHERAPY ROUNDS OCTOBER 20, 2017
Botulinum toxin type A for the prevention of headaches in adults with chronic migraine
 Botulinum toxin type A for the prevention of headaches in adults with chronic migraine Issued: June 2012 guidance.nice.org.uk/ta260 NICE has accredited the process used by the Centre for Health Technology
Botulinum toxin type A for the prevention of headaches in adults with chronic migraine Issued: June 2012 guidance.nice.org.uk/ta260 NICE has accredited the process used by the Centre for Health Technology
8-May-2018 ICER OPEN COMMENT PERIOD ON CGRP INHIBITORS FOR MIGRAINE. Submitted electronically to:
 8-May-2018 ICER OPEN COMMENT PERIOD ON CGRP INHIBITORS FOR MIGRAINE Submitted electronically to: publiccomments@icer-review.org Steven D. Pearson, MD, President Institute for Clinical and Economic Review
8-May-2018 ICER OPEN COMMENT PERIOD ON CGRP INHIBITORS FOR MIGRAINE Submitted electronically to: publiccomments@icer-review.org Steven D. Pearson, MD, President Institute for Clinical and Economic Review
Disclosure. Learning Objectives 11/10/2017. The Best and Most Interesting Research from Last Year Cephalalgia
 The Best and Most Interesting Research from Last Year Cephalalgia David W. Dodick, M.D. Department of Neurology Mayo Clinic Scottsdale Arizona Disclosure Consulting services: Acorda, Allergan, Amgen, Alder,
The Best and Most Interesting Research from Last Year Cephalalgia David W. Dodick, M.D. Department of Neurology Mayo Clinic Scottsdale Arizona Disclosure Consulting services: Acorda, Allergan, Amgen, Alder,
Mark W. Green, MD, FAAN
 Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
Comorbidities of Migraine
 Comorbidities of Migraine Richard B. Lipton, MD Edwin S Lowe Professor and Vice Chair of Neurology Director, Montefiore Headache Center Albert Einstein College of Medicine Overview What is comorbidity?
Comorbidities of Migraine Richard B. Lipton, MD Edwin S Lowe Professor and Vice Chair of Neurology Director, Montefiore Headache Center Albert Einstein College of Medicine Overview What is comorbidity?
Expert Opinion. OnabotulinumtoxinA for Chronic Migrainehead_2071 CLINICAL HISTORY. Andrew Blumenfeld, MD; Randolph W. Evans, MD
 142..148 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.02081.x Published by Wiley Periodicals, Inc. Expert Opinion OnabotulinumtoxinA for Chronic Migrainehead_2071
142..148 Headache 2011 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2011.02081.x Published by Wiley Periodicals, Inc. Expert Opinion OnabotulinumtoxinA for Chronic Migrainehead_2071
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 CGRP Page 1 of 13 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
CGRP Page 1 of 13 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
Chronic Migraine: Epidemiology and Disease Burden
 Curr Pain Headache Rep (2011) 15:70 78 DOI 10.1007/s11916-010-0157-z Chronic Migraine: Epidemiology and Disease Burden Aubrey N. Manack & Dawn C. Buse & Richard B. Lipton Published online: 10 November
Curr Pain Headache Rep (2011) 15:70 78 DOI 10.1007/s11916-010-0157-z Chronic Migraine: Epidemiology and Disease Burden Aubrey N. Manack & Dawn C. Buse & Richard B. Lipton Published online: 10 November
The Journal of Headache and Pain
 Schwedt et al. The Journal of Headache and Pain (2018) 19:38 https://doi.org/10.1186/s10194-018-0865-z The Journal of Headache and Pain RESEARCH ARTICLE Open Access Factors associated with acute medication
Schwedt et al. The Journal of Headache and Pain (2018) 19:38 https://doi.org/10.1186/s10194-018-0865-z The Journal of Headache and Pain RESEARCH ARTICLE Open Access Factors associated with acute medication
Clinical Trials. Hans-Christoph Diener Senior Professor of Clinical Neuroscienes Medical Faculty University Duisburg-Essen Germany
 Clinical Trials Hans-Christoph Diener Senior Professor of Clinical Neuroscienes Medical Faculty University Duisburg-Essen Germany Conflict of Interest Statement German Research Council German Ministry
Clinical Trials Hans-Christoph Diener Senior Professor of Clinical Neuroscienes Medical Faculty University Duisburg-Essen Germany Conflict of Interest Statement German Research Council German Ministry
MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache
 MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache Measure Description Percentage of patients age 12 years and older with a diagnosis of migraine who were prescribed a guideline recommended
MEASURE #1: MEDICATION PRESCRIBED FOR ACUTE MIGRAINE ATTACK Headache Measure Description Percentage of patients age 12 years and older with a diagnosis of migraine who were prescribed a guideline recommended
A Multi-Center Double-Blind Pilot Comparison of OnabotulinumtoxinA and Topiramate for the Prophylactic Treatment of Chronic Migrainehead_
 Headache 2010 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2010.01796.x Published by Wiley Periodicals, Inc. Research Submission A Multi-Center Double-Blind Pilot Comparison of OnabotulinumtoxinA
Headache 2010 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2010.01796.x Published by Wiley Periodicals, Inc. Research Submission A Multi-Center Double-Blind Pilot Comparison of OnabotulinumtoxinA
Giorgio Sandrini Armando Perrotta Cristina Tassorelli Paola Torelli Filippo Brighina Grazia Sances Giuseppe Nappi
 J Headache Pain (2011) 12:427 433 DOI 10.1007/s10194-011-0339-z ORIGINAL Botulinum toxin type-a in the prophylactic treatment of medication-overuse headache: a multicenter, double-blind, randomized, placebo-controlled,
J Headache Pain (2011) 12:427 433 DOI 10.1007/s10194-011-0339-z ORIGINAL Botulinum toxin type-a in the prophylactic treatment of medication-overuse headache: a multicenter, double-blind, randomized, placebo-controlled,
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Patient Reported Outcome High Priority
 Quality ID #435: Quality of Life Assessment For Patients With Primary Headache Disorders National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Patient Reported Functional Outcomes
Quality ID #435: Quality of Life Assessment For Patients With Primary Headache Disorders National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Patient Reported Functional Outcomes
ISSN doi: /head.13327
 Headache VC 18 The Authors Headache: The Journal Head and Face Pain published by Wiley Periodicals, Inc. on behalf American Headache Society ISSN 17-8748 doi:.1111/head.13327 Research Submission Use Most
Headache VC 18 The Authors Headache: The Journal Head and Face Pain published by Wiley Periodicals, Inc. on behalf American Headache Society ISSN 17-8748 doi:.1111/head.13327 Research Submission Use Most
6/20/2018. Chronic Migraine versus Chronic Pain: Similarities and Differences. Disclosure (36 months) Clinical Differences/Background
 Chronic Migraine versus Chronic Pain: Similarities and Differences Clinical Differences/Background David W. Dodick, M.D. Professor Department of Neurology Mayo Clinic Phoenix Arizona Disclosure (36 months)
Chronic Migraine versus Chronic Pain: Similarities and Differences Clinical Differences/Background David W. Dodick, M.D. Professor Department of Neurology Mayo Clinic Phoenix Arizona Disclosure (36 months)
Research Submission. ISSN doi: /head Published by Wiley Periodicals, Inc. Headache 2013 American Headache Society
 Headache 2013 American Headache Society ISSN 0017-8748 doi: 10.1111/head.12150 Published by Wiley Periodicals, Inc. Research Submission Sex Differences in the Prevalence, Symptoms, and Associated Features
Headache 2013 American Headache Society ISSN 0017-8748 doi: 10.1111/head.12150 Published by Wiley Periodicals, Inc. Research Submission Sex Differences in the Prevalence, Symptoms, and Associated Features
What is the Effectiveness of OnabotulinumtoxinA (Botox ) in Reducing the Number of Chronic Migraines (CM) in Patients Years Old?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 What is the Effectiveness of OnabotulinumtoxinA
Harold G. Wolff Lecture Award Winner
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01217.x Published by Wiley Periodicals, Inc. Harold G. Wolff Lecture Award Winner
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01217.x Published by Wiley Periodicals, Inc. Harold G. Wolff Lecture Award Winner
A multicenter, prospective, single arm, open label, observational study of stms for migraine prevention (ESPOUSE Study)
 Original Article A multicenter, prospective, single arm, open label, observational study of stms for migraine prevention (ESPOUSE Study) Cephalalgia 2018, Vol. 38(6) 1038 1048! International Headache Society
Original Article A multicenter, prospective, single arm, open label, observational study of stms for migraine prevention (ESPOUSE Study) Cephalalgia 2018, Vol. 38(6) 1038 1048! International Headache Society
A single-center retrospective study of onabotulinumtoxina for treatment of 245 chronic migraine patients: survey results of a realworld
 https://doi.org/10.1007/s13760-018-0978-9 ORIGINAL ARTICLE A single-center retrospective study of onabotulinumtoxina for treatment of 245 chronic migraine patients: survey results of a realworld experience
https://doi.org/10.1007/s13760-018-0978-9 ORIGINAL ARTICLE A single-center retrospective study of onabotulinumtoxina for treatment of 245 chronic migraine patients: survey results of a realworld experience
Technology appraisal guidance Published: 27 June 2012 nice.org.uk/guidance/ta260
 Botulinum toxin type A for the prevention ention of headaches in adults with chronic migraine Technology appraisal guidance Published: 27 June 2012 nice.org.uk/guidance/ta260 NICE 2018. All rights reserved.
Botulinum toxin type A for the prevention ention of headaches in adults with chronic migraine Technology appraisal guidance Published: 27 June 2012 nice.org.uk/guidance/ta260 NICE 2018. All rights reserved.
Comments on the Draft Evidence Report: Migraine Treatment: Effectiveness and Value
 May 8, 2018 Via Electronic Mail Steven Pearson, MD Institute for Clinical and Economic Review Two Liberty Square, Ninth Floor Boston, MA 02109 RE: Comments on the Draft Evidence Report: Migraine Treatment:
May 8, 2018 Via Electronic Mail Steven Pearson, MD Institute for Clinical and Economic Review Two Liberty Square, Ninth Floor Boston, MA 02109 RE: Comments on the Draft Evidence Report: Migraine Treatment:
Get ahead of the ACHE: Monoclonal Antibodies in Migraine Prevention
 Get ahead of the ACHE: Monoclonal Antibodies in Migraine Prevention Amanda Janisch, PharmD PGY2 Ambulatory Care Pharmacy Resident MCHS SWMN, Mankato, MN 2018 MFMER slide-1 Disclosures No financial interest
Get ahead of the ACHE: Monoclonal Antibodies in Migraine Prevention Amanda Janisch, PharmD PGY2 Ambulatory Care Pharmacy Resident MCHS SWMN, Mankato, MN 2018 MFMER slide-1 Disclosures No financial interest
Transforming Treatment for Migraine. 16 th Annual Needham Healthcare Conference April 4, 2017
 Transforming Treatment for Migraine 16 th Annual Needham Healthcare Conference April 4, 2017 Forward Looking Statements This presentation and the accompanying commentary contain certain forward-looking
Transforming Treatment for Migraine 16 th Annual Needham Healthcare Conference April 4, 2017 Forward Looking Statements This presentation and the accompanying commentary contain certain forward-looking
10/13/17. Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD
 Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Christy M. Jackson, MD Director, Dalessio Headache Center Scripps Clinic, La Jolla Clinical Professor, Neurosciences UCSD } Depomed Consultant 2014 to present } Avanir Consultant 2014 to present } Amgen
Supplementary Online Content
 Supplementary Online Content Dodick DW, Silberstein SD, Bigal ME, et al. Effect of Fremanezumab Compared With Placebo for Prevention of Episodic Migraine: A Randomized Clinical Trial. JAMA. doi:10.1001/jama.2018.4853
Supplementary Online Content Dodick DW, Silberstein SD, Bigal ME, et al. Effect of Fremanezumab Compared With Placebo for Prevention of Episodic Migraine: A Randomized Clinical Trial. JAMA. doi:10.1001/jama.2018.4853
Committed to Transforming the Treatment Paradigm for Migraine Prevention
 Committed to Transforming the Treatment Paradigm for Migraine Prevention 36th Annual J.P. Morgan Healthcare Conference January 8, 2018 Forward-Looking Statements This presentation and the accompanying
Committed to Transforming the Treatment Paradigm for Migraine Prevention 36th Annual J.P. Morgan Healthcare Conference January 8, 2018 Forward-Looking Statements This presentation and the accompanying
Quality ID #435: Quality of Life Assessment For Patients With Primary Headache Disorders National Quality Strategy Domain: Effective Clinical Care
 Quality ID #435: Quality of Life Assessment For Patients With Primary Headache Disorders National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Quality ID #435: Quality of Life Assessment For Patients With Primary Headache Disorders National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
A new questionnaire for assessment of adverse events associated with triptans: methods of assessment influence the results. Preliminary results
 J Headache Pain (2004) 5:S112 S116 DOI 10.1007/s10194-004-0123-4 Michele Feleppa Fred D. Sheftell Luciana Ciannella Amedeo D Alessio Giancarlo Apice Nino N. Capobianco Donato M.T. Saracino Walter Di Iorio
J Headache Pain (2004) 5:S112 S116 DOI 10.1007/s10194-004-0123-4 Michele Feleppa Fred D. Sheftell Luciana Ciannella Amedeo D Alessio Giancarlo Apice Nino N. Capobianco Donato M.T. Saracino Walter Di Iorio
Despite the widespread use of triptans ... REPORTS... Almotriptan: A Review of Pharmacology, Clinical Efficacy, and Tolerability
 ... REPORTS... Almotriptan: A Review of Pharmacology, Clinical Efficacy, and Tolerability Randal L. Von Seggern, PharmD, BCPS Abstract Objective: This article summarizes preclinical and clinical data for
... REPORTS... Almotriptan: A Review of Pharmacology, Clinical Efficacy, and Tolerability Randal L. Von Seggern, PharmD, BCPS Abstract Objective: This article summarizes preclinical and clinical data for
National Institute for Health and Clinical Excellence. Single Technology Appraisal (STA)
 National Institute for Health and Clinical Excellence Comment 1: the draft remit Single Technology Appraisal (STA) Botulinum toxin type A for the prophylaxis of headaches in adults with chronic migraine
National Institute for Health and Clinical Excellence Comment 1: the draft remit Single Technology Appraisal (STA) Botulinum toxin type A for the prophylaxis of headaches in adults with chronic migraine
Inpatient Treatment of Status Migraine With Dihydroergotamine in Children and Adolescents
 Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
Headache 2008 the Authors Journal compilation 2008 American Headache Society ISSN 0017-8748 doi: 10.1111/j.1526-4610.2008.01293.x Published by Wiley Periodicals, Inc. Brief Communication Inpatient Treatment
PROMISE 2 Top-Line Data Results January 8, 2018
 PROMISE 2 Top-Line Data Results January 8, 2018 Forward-Looking Statements This presentation and the accompanying commentary contains certain forward-looking statements within the meaning of Section 27A
PROMISE 2 Top-Line Data Results January 8, 2018 Forward-Looking Statements This presentation and the accompanying commentary contains certain forward-looking statements within the meaning of Section 27A
Faculty Disclosures. Learning Objectives. Acute Treatment Strategies
 WWW.AMERICANHEADACHESOCIETY.ORG Acute Treatment Strategies Content developed by: Lawrence C. Newman, MD, FAHS Donna Gutterman, PharmD Faculty Disclosures LAWRENCE C. NEWMAN, MD, FAHS Dr. Newman has received
WWW.AMERICANHEADACHESOCIETY.ORG Acute Treatment Strategies Content developed by: Lawrence C. Newman, MD, FAHS Donna Gutterman, PharmD Faculty Disclosures LAWRENCE C. NEWMAN, MD, FAHS Dr. Newman has received
Topiramate intervention to prevent transformation of episodic migraine: The topiramate INTREPID study
 Cephalalgia OnlineFirst, published on May 17, 2010 as doi:10.1177/0333102410372427 Original Article Topiramate intervention to prevent transformation of episodic migraine: The topiramate INTREPID study
Cephalalgia OnlineFirst, published on May 17, 2010 as doi:10.1177/0333102410372427 Original Article Topiramate intervention to prevent transformation of episodic migraine: The topiramate INTREPID study
Editorial Team Conflict of Interest Statements
 Editorial Team Conflict of Interest Statements Editor in Chief David Dodick Advisory board/consultant: Allergan, Amgen, Alder, Arteaus, Pfizer, Colucid, Merck, ENeura, NuPathe, Eli Lilly, Autonomic Technologies,
Editorial Team Conflict of Interest Statements Editor in Chief David Dodick Advisory board/consultant: Allergan, Amgen, Alder, Arteaus, Pfizer, Colucid, Merck, ENeura, NuPathe, Eli Lilly, Autonomic Technologies,
Views and Perspectives
 Headache ISSN 0017-8748 VC 2017 Allergan plc. Headache published by Wiley Periodicals, Inc. doi: 10.1111/head.13074 on behalf of American Headache Society Published by Wiley Periodicals, Inc. Views and
Headache ISSN 0017-8748 VC 2017 Allergan plc. Headache published by Wiley Periodicals, Inc. doi: 10.1111/head.13074 on behalf of American Headache Society Published by Wiley Periodicals, Inc. Views and
Overuse of barbiturate and opioid containing medications for primary headache disorders Description
 Measure Title Overuse of barbiturate and opioid containing medications for primary headache disorders Description Percentage of s age 12 years and older with a diagnosis of primary headache who were prescribed
Measure Title Overuse of barbiturate and opioid containing medications for primary headache disorders Description Percentage of s age 12 years and older with a diagnosis of primary headache who were prescribed
Study No.:MPX Title: Rationale: Phase: IIB Study Period: Study Design: Centres: Indication: Treatment: Objectives:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Therapeutic Advances in Neurological Disorders
 499788TAN6510.1177/1756285613499788Therapeutic Advances in Neurological DisordersS Landy, R Hoagland 2013499788 Therapeutic Advances in Neurological Disorders Original Research Sumatriptan/naproxen sodium
499788TAN6510.1177/1756285613499788Therapeutic Advances in Neurological DisordersS Landy, R Hoagland 2013499788 Therapeutic Advances in Neurological Disorders Original Research Sumatriptan/naproxen sodium
Hareendran et al. Health and Quality of Life Outcomes (2017) 15:224 DOI /s
 Hareendran et al. Health and Quality of Life Outcomes (2017) 15:224 DOI 10.1186/s12955-017-0799-1 RESEARCH Open Access Development and exploration of the content validity of a patient-reported outcome
Hareendran et al. Health and Quality of Life Outcomes (2017) 15:224 DOI 10.1186/s12955-017-0799-1 RESEARCH Open Access Development and exploration of the content validity of a patient-reported outcome
Improving the detection of chronic migraine: Development and validation of Identify Chronic Migraine (ID-CM)
 Original Article Improving the detection of chronic migraine: Development and validation of Identify Chronic Migraine (ID-CM) Cephalalgia 2016, Vol. 36(3) 203 215! International Headache Society 2015 Reprints
Original Article Improving the detection of chronic migraine: Development and validation of Identify Chronic Migraine (ID-CM) Cephalalgia 2016, Vol. 36(3) 203 215! International Headache Society 2015 Reprints
JEADV SHORT REPORT. Abstract
 DOI: 1.1111/jdv.13216 JEADV SHORT REPORT HiSCR (Hidradenitis Suppurativa Clinical Response): a novel clinical endpoint to evaluate therapeutic outcomes in patients with hidradenitis suppurativa from the
DOI: 1.1111/jdv.13216 JEADV SHORT REPORT HiSCR (Hidradenitis Suppurativa Clinical Response): a novel clinical endpoint to evaluate therapeutic outcomes in patients with hidradenitis suppurativa from the
December 21, https://www.womenshealth.gov/publications/our-publications/fact-sheet/migraine.html#i 2
 Steven Pearson, MD Institute for Clinical and Economic Review 2 Liberty Square, Ninth Floor Boston, MA 02109 Dear Dr. Pearson: December 21, 2017 The Alliance for the Adoption of Innovations in Medicine
Steven Pearson, MD Institute for Clinical and Economic Review 2 Liberty Square, Ninth Floor Boston, MA 02109 Dear Dr. Pearson: December 21, 2017 The Alliance for the Adoption of Innovations in Medicine
6/20/2018 PROCEDURAL TREATMENTS FOR HEADACHE. Case study: Emily. Diary
 Headache severity (Scale 0 10) Topiramate started on July 20, D/C July 29 Amitriptyline initiated, D/C on Sep 23 PROCEDURAL TREATMENTS FOR HEADACHE Andrew M. Blumenfeld Director of the Headache Center
Headache severity (Scale 0 10) Topiramate started on July 20, D/C July 29 Amitriptyline initiated, D/C on Sep 23 PROCEDURAL TREATMENTS FOR HEADACHE Andrew M. Blumenfeld Director of the Headache Center
Committed to Transforming the Treatment Paradigm for Migraine Prevention
 June 14, 2018 Committed to Transforming the Treatment Paradigm for Migraine Prevention September 6, 2018 Forward-Looking Statements This presentation and the accompanying commentary contains certain forward-looking
June 14, 2018 Committed to Transforming the Treatment Paradigm for Migraine Prevention September 6, 2018 Forward-Looking Statements This presentation and the accompanying commentary contains certain forward-looking
Andrew Michael Blumenfeld, M.D.
 The Neurology Center of Southern California 6010 Hidden Valley Road, Suite 200, Carlsbad, California 92011 9850 Genesee Ave, Suite 470, La Jolla, CA, 92037 1955 Citracado Pkwy, Suite 102, Escondido, CA
The Neurology Center of Southern California 6010 Hidden Valley Road, Suite 200, Carlsbad, California 92011 9850 Genesee Ave, Suite 470, La Jolla, CA, 92037 1955 Citracado Pkwy, Suite 102, Escondido, CA
Paradigm for Migraine Patients
 June Transforming 14, 2018 the Prevention Treatment Paradigm for Migraine Patients January 2019 Forward-Looking Statements This presentation and the accompanying commentary contains certain forward-looking
June Transforming 14, 2018 the Prevention Treatment Paradigm for Migraine Patients January 2019 Forward-Looking Statements This presentation and the accompanying commentary contains certain forward-looking
Proposed Project Scope. OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice
 Proposed Project Scope OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice May 2018 1. BACKGROUND AND RATIONALE Migraine is a common, debilitating
Proposed Project Scope OPTIMAL USE OnabotulinumtoxinA for the Prevention of Chronic Migraine Clinical Evidence, Policies and Practice May 2018 1. BACKGROUND AND RATIONALE Migraine is a common, debilitating
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 CGRP Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
CGRP Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: CGRP (calcitonin gene-related peptide) Prime Therapeutics will review Prior Authorization requests
UNDERSTANDING CHRONIC MIGRAINE. Learn about diagnosis, management, and treatment options for this headache condition
 UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
UNDERSTANDING CHRONIC MIGRAINE Learn about diagnosis, management, and treatment options for this headache condition 1 What We re Going to Cover Today The symptoms and phases of migraine Differences between
PROGRAM SYLLABUS. Jointly provided by Potomac Center for Medical Education and Rockpointe
 PROGRAM SYLLABUS Jointly provided by Potomac Center for Medical Education and Rockpointe This activity is supported by an educational grant from Lilly. For further information concerning Lilly grant funding
PROGRAM SYLLABUS Jointly provided by Potomac Center for Medical Education and Rockpointe This activity is supported by an educational grant from Lilly. For further information concerning Lilly grant funding
Comparison of dynamic (brush) and static (pressure) mechanical allodynia in migraine
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology July 2006 Comparison of dynamic (brush) and static (pressure) mechanical allodynia in
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology July 2006 Comparison of dynamic (brush) and static (pressure) mechanical allodynia in
Migraine is a highly prevalent and debilitating
 A Migraine Disease Management Program in the Primary Care Setting: Impact on Patient Quality of Life and Productivity Loss Winghan Jacqueline Kwong, PharmD, PhD, Stephen H. Landy, MD, Jill Braverman-Panza,
A Migraine Disease Management Program in the Primary Care Setting: Impact on Patient Quality of Life and Productivity Loss Winghan Jacqueline Kwong, PharmD, PhD, Stephen H. Landy, MD, Jill Braverman-Panza,
PDFlib PLOP: PDF Linearization, Optimization, Protection. Page inserted by evaluation version
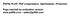 PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com Headache 2008 the Authors Journal compilation 2008 American Headache Society
PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com Headache 2008 the Authors Journal compilation 2008 American Headache Society
Validation of the Headache Impact Test (HIT-6) in patients with chronic migraine
 Rendas-Baum et al. Health and Quality of Life Outcomes 2014, 12:117 RESEARCH Open Access Validation of the Headache Impact Test (HIT-6) in patients with chronic migraine Regina Rendas-Baum 1*, Min Yang
Rendas-Baum et al. Health and Quality of Life Outcomes 2014, 12:117 RESEARCH Open Access Validation of the Headache Impact Test (HIT-6) in patients with chronic migraine Regina Rendas-Baum 1*, Min Yang
INDIVIDUAL STUDY TABLE REFERRING TO PART OF THE DOSSIER Volume: Page:
 SYNOPSIS Protocol No.: TOPMAT-MIG-303 EudraCT No.: 2005-000321-29 Title of Study: A double-blind, randomised, placebo-controlled, multicentre study to investigate the efficacy and tolerability of in prolonged
SYNOPSIS Protocol No.: TOPMAT-MIG-303 EudraCT No.: 2005-000321-29 Title of Study: A double-blind, randomised, placebo-controlled, multicentre study to investigate the efficacy and tolerability of in prolonged
Effectiveness of Pharmacological Treatments in Imploding vs. Exploding Headaches
 Effectiveness of Pharmacological Treatments in Imploding vs. Exploding Headaches Item Type Thesis Authors Hunt, Megan Publisher The University of Arizona. Rights Copyright is held by the author. Digital
Effectiveness of Pharmacological Treatments in Imploding vs. Exploding Headaches Item Type Thesis Authors Hunt, Megan Publisher The University of Arizona. Rights Copyright is held by the author. Digital
Early onset of efficacy with erenumab in patients with episodic and chronic migraine
 Schwedt et al. The Journal of Headache and Pain (2018) 19:92 https://doi.org/10.1186/s10194-018-0923-6 The Journal of Headache and Pain RESEARCH ARTICLE Early onset of efficacy with erenumab in patients
Schwedt et al. The Journal of Headache and Pain (2018) 19:92 https://doi.org/10.1186/s10194-018-0923-6 The Journal of Headache and Pain RESEARCH ARTICLE Early onset of efficacy with erenumab in patients
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Emgality) Reference Number: CP.PHAR.## Effective Date: 11.13.18 Last Review Date: 02.19 Line of Business: Commercial, TBD HIM*, Medicaid Revision Log See Important Reminder at the end
Clinical Policy: (Emgality) Reference Number: CP.PHAR.## Effective Date: 11.13.18 Last Review Date: 02.19 Line of Business: Commercial, TBD HIM*, Medicaid Revision Log See Important Reminder at the end
Sociodemographic and comorbidity profiles of chronic migraine and episodic migraine sufferers
 1 Department of Neurology, Albert Einstein College of Medicine, Bronx, New York, USA; 2 Montefiore Headache Center, Bronx, New York, USA; 3 Allergan, Irvine, California, USA 4 Vedanta Research, Chapel
1 Department of Neurology, Albert Einstein College of Medicine, Bronx, New York, USA; 2 Montefiore Headache Center, Bronx, New York, USA; 3 Allergan, Irvine, California, USA 4 Vedanta Research, Chapel
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
Identification of negative predictors of pain-free response to triptans: Analysis of the eletriptan database
 doi:10.1111/j.1468-2982.2007.01457.x Identification of negative predictors of pain-free response to triptans: Analysis of the eletriptan database H-C Diener 1, DW Dodick 2, PJ Goadsby 3, RB Lipton 4, M
doi:10.1111/j.1468-2982.2007.01457.x Identification of negative predictors of pain-free response to triptans: Analysis of the eletriptan database H-C Diener 1, DW Dodick 2, PJ Goadsby 3, RB Lipton 4, M
8/6/18. Patient Experience. effective management of Chronic Migraine and Occipital Neuralgia in the Post 9/11 Combat Veteran
 8//8 Patient Experience Validation of practice based evidence for effective management of Chronic Migraine and Occipital Neuralgia in the Post 9/ Combat Veteran Karen Williams,MSN, RN, FNP-BC Neurology/Headache
8//8 Patient Experience Validation of practice based evidence for effective management of Chronic Migraine and Occipital Neuralgia in the Post 9/ Combat Veteran Karen Williams,MSN, RN, FNP-BC Neurology/Headache
Daily Oxymetazoline Cream Demonstrates High and Sustained Efficacy in Patients With Persistent Erythema of Rosacea Through 52 Weeks of Treatment
 Accepted Manuscript Daily Oxymetazoline Cream Demonstrates High and Sustained Efficacy in Patients With Persistent Erythema of Rosacea Through 52 Weeks of Treatment Michael H. Gold, MD, FAAD, Mark Lebwohl,
Accepted Manuscript Daily Oxymetazoline Cream Demonstrates High and Sustained Efficacy in Patients With Persistent Erythema of Rosacea Through 52 Weeks of Treatment Michael H. Gold, MD, FAAD, Mark Lebwohl,
Novartis announces Phase III STRIVE data published in NEJM demonstrating significant and sustained efficacy of erenumab in migraine prevention
 Novartis International AG Novartis Global Communications CH-4002 Basel Switzerland http://www.novartis.com MEDIA RELEASE COMMUNIQUE AUX MEDIAS MEDIENMITTEILUNG Novartis announces Phase III STRIVE data
Novartis International AG Novartis Global Communications CH-4002 Basel Switzerland http://www.novartis.com MEDIA RELEASE COMMUNIQUE AUX MEDIAS MEDIENMITTEILUNG Novartis announces Phase III STRIVE data
Migraine much more than just a headache
 Migraine much more than just a headache Session hosted by Teva UK Limited PUU4 11:15 12:15 UK/NHSS/18/0021b Date of Preparation: August 2018 The views expressed in this presentation are those of the speaker
Migraine much more than just a headache Session hosted by Teva UK Limited PUU4 11:15 12:15 UK/NHSS/18/0021b Date of Preparation: August 2018 The views expressed in this presentation are those of the speaker
Andrew M. Blumenfeld 1*, Sheena K. Aurora 2*, Karen Laranjo 3 and Spyros Papapetropoulos 4
 Blumenfeld et al. BMC Neurology (2015) 15:100 DOI 10.1186/s12883-015-0353-x STUDY PROTOCOL Unmet clinical needs in chronic migraine: Rationale for study and design of COMPEL, an open-label, multicenter
Blumenfeld et al. BMC Neurology (2015) 15:100 DOI 10.1186/s12883-015-0353-x STUDY PROTOCOL Unmet clinical needs in chronic migraine: Rationale for study and design of COMPEL, an open-label, multicenter
The use of combination therapies in the acute management of migraine
 REVIEW The use of combination therapies in the acute management of migraine Abouch Valenty Krymchantowski Headache Center of Rio, Rio de Janeiro, Brazil; Outpatient Headache Unit of the Instituto de Neurologia
REVIEW The use of combination therapies in the acute management of migraine Abouch Valenty Krymchantowski Headache Center of Rio, Rio de Janeiro, Brazil; Outpatient Headache Unit of the Instituto de Neurologia
Utilization and Safety of OnabotulinumtoxinA for the Prophylactic. Treatment of Chronic Migraine from an Observational Study in.
 Utilization and Safety of OnabotulinumtoxinA for the Prophylactic Treatment of Chronic Migraine from an Observational Study in Europe Running Title: Utilization and Safety of OnabotulinumtoxinA for Chronic
Utilization and Safety of OnabotulinumtoxinA for the Prophylactic Treatment of Chronic Migraine from an Observational Study in Europe Running Title: Utilization and Safety of OnabotulinumtoxinA for Chronic
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache
 MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
Faculty Disclosures. Learning Objectives
 WWW.AMERICANHEADACHESOCIETY.ORG Pathophysiology Content developed by: Andrew C. Charles, MD, FAHS, Peter J. Goadsby, MD, PhD, FAHS Donna Gutterman, PharmD Faculty Disclosures ANDREW C. CHARLES, MD, FAHS
WWW.AMERICANHEADACHESOCIETY.ORG Pathophysiology Content developed by: Andrew C. Charles, MD, FAHS, Peter J. Goadsby, MD, PhD, FAHS Donna Gutterman, PharmD Faculty Disclosures ANDREW C. CHARLES, MD, FAHS
