Fluoroscope guided epidural needle insertioin in midthoracic region: clinical evaluation of Nagaro's method
|
|
|
- Hector Shelton
- 6 years ago
- Views:
Transcription
1 Clinical Research Article Korean J Anesthesiol 2012 May 62(5): Fluoroscope guided epidural needle insertioin in midthoracic region: clinical evaluation of Nagaro's method Won Joong Kim, Tae Hwa Kim, Hwa Yong Shin, Hyun Kang, Chong Wha Baek, Yong Hun Jung, Young Cheol Woo, Jin Yun Kim, Gill Hoi Koo, and Sun Gyoo Park Department of Anesthesiology and Pain Medicine, College of Medicine, Chung-Ang University, Seoul, Korea Background: In the midthoracic region, a fluroscope guided epidural block has been proposed by using a pedicle as a landmark to show the height of the interlaminar space (Nagaro's method). However, clinical implication of this method was not fully evaluated. We studied the clinical usefulness of a fluoroscope guided thoracic epidural block in the midthoracic region. Methods: Twenty four patients were scheduled to receive an epidural block at the T6-7 intervertebral space. The patients were placed in the prone position. The needle entry point was located at the junction between midline of the pedicle paralleled to the midline of the T7 vertebral body (VB) and the lower border of T7 VB on anteroposterior view of the fluoroscope. The needle touched and walked up the lamina, and the interlaminar space (ILS) was sought near the midline of the VB at the height of the pedicle. Results: The authors could not insert an epidural needle at T6-7 ILS in two patients and it was instead inserted at T5-6 ILS. However, other patients showed easy insertion at T6-7 ILS. The mean inward and upward angulations were 25 o and 55 o respectively. The mean actual depth and calculated depth from skin to thoracic epidural space were 5.1 cm and 6.1 cm respectively. Significant correlation between actual needle depth and body weight, podendal index (kg/ m) or calculated needle depth was noted. Conclusions: The fluorposcope guided epidural block by Nagaro's method was useful in the midthoracic region. However, further study for the caudal shift of needle entry point may be needed. (Korean J Anesthesiol 2012; 62: ) Key Words: Analgesia, Epidural, Fluoroscopy, Thoracic vertebrae. Received: July 13, Revised: September 7, Accepted: September 21, Corresponding author: Young Cheol Woo, M.D., Ph.D., Department of Anesthesiology and Pain Medicine, College of Medicine, Chung-Ang University, 224-1, Heukseok-1dong, Dongjak-gu, Seoul , Korea. Tel: , Fax: , wj12@naver.com This is a thesis for a master's degree. CC This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( creativecommons.org/licenses/by-nc/3.0/), which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright c the Korean Society of Anesthesiologists, 2012
2 Midthoracic epidural block Vol. 62, No. 5, May 2012 Introduction A significant number of patients experience marked pulmonary insufficiency after a thoracotomy, due to severe post operative pain. This post-thoracotomy pain, if not properly controlled, leads to difficulty taking deep breaths and coughing, which are associated with atelectasis, hypoxia, pneumonia, or respiratory distress - conditions interfering with postoperative recovery and lengthening the patients hospital stays [1]. Management of post-thoracotomy pain, therefore, is an impor tant matter, and studies have been conducted for its inve sti gation. Postthoracotomy pain treatment methods using intramuscular or intravascular injection of opioid drugs, as well as intercostal nerve blocks using local anesthetics, are among the techniques studied. The most effective method reported is continuous infusion of local anesthetic into the epidural space [2,3]. A thoracic epidural block is a relatively more difficult procedure than procedures used in other regions, because the spinous process of the thoracic vertebra is longer than that of the lumbar vertebra, and the area through which the needle can approach the epidural space is relatively smaller due to an acute angle and larger distance between the skin and the epidural space. The midthoracic region (T5-8) is the most difficult area when performing a block. Successful placement of the Tuohy needle is known to depend on the patient s physical conditions, anatomic changes in vertebrae, and the anesthesiologist s proficiency, among other factors, resulting in a failure rate of approximately 10% of the Tuohy needle placements attempted blindly by even the most skilled clinicians [4,5]. Another consideration to be made for a thoracic epidural block is the risk of serious neurological complications such as spinal cord injury, possibly resulting from the smaller epidural space in the thoracic region compared to that in the lumbar region, and from the presence of the spinal cord in the direction of the needle s path. Given these difficulties, it is essential that anesthesiologists perform the epidural block in the safest way possible [6]. Until recently, few reliable reports have been presented on fluoroscopice guided epidural blocks performed in the midthoracic region. Nagaro et al. [7] attempted such an epidural block using a paramedian approach, in which, after confirming that the interlaminar space (ILS) is located at the height of the vertebral pedicle in all thoracic vertebrae, they placed the entry point of the needle at the site where the inferior endplate of the targeted vertebral body (VB) meets, in the lateral position, the line parallel to the vertebral column that passes through the midline of the pedicle. They then attempt to locate the ILS from around the midline of the VB at the height of the pedicle [7]. Their study, however, involved only five patients on whom an epidural block was performed in the midthoracic region (T6-7). The results of a study involving such a small number of subjects should be interpreted with caution when performing an epidural block in the midthoracic area. The aim of this study was to evaluate the viability of a C-arm guided epidural block performed in the midthoracic region using a Tuohy needle. The procedure was based on the method reported by Nagaro et al. [7]. Materials and Methods Among the patients scheduled for a thoracotomy with general anesthesia using inhalation anesthetics, 24 patients interested in receiving postoperative pain management were enrolled in the study. Each patient s written consent was collected after obtaining approval from this hospital s insti tutional review board. All candidates were Class 1 or 2 patients according to the ASA physical status classification system; patients for whom the use of the Tuohy needle is prohibited, who had abused drugs within two weeks prior to the thoracic epidural block, or were pregnant were excluded from the study. The subjects age, height, weight, podendal index (PI), sex (sex ratio), and other demographic information are listed in Table 1. The subjects arrived in the operating room unpremedicated and were connected to the ECG, blood pressure meter, and pulse oximeter. They were offered an explanation on how to use the patient controlled epidural analgesia (PCEA). The Tuohy needle (Epidural-set R, Insung Medical, Korea) was placed by an anesthesiologist, using the procedure described as follows. The patients, in an awake state, were instructed to assume the prone position and to place a 10 cm deep pillow under their chest. The pillow was adjusted in such a way that the highest point on the patients back, which would serve as the needle s skin entry point, was highlighted. The patients were also instructed to place both of their arms above their head to ensure that the C-arm fluoroscope would not be inhibited. A paramedian approach, in which the needle punctures the skin on the contralateral side from the operation site, was used. The C-arm guidance AP view was adjusted such that the T7 spinous process would be situated at the midline of the VB and the T7 VB would form a square. The site for needle insertion was then cleansed and sterilized with Betadine R solution and Table 1. Demographic Data Age (yr) Gender (M/ F) Height (cm) Weight (kg) PI (kg/m) 59.4 ± 10.7 (24-77) 16 / ± 8.4 ( ) 62.3 ± 6.8 (52-75) 38.3 ± 3.8 ( ) Values are mean ± SD (minimum-maximum), PI (podendal index) is weight divided by height. 442
3 Korean J Anesthesiol Kim, et al. covered with sterile cloths. Using a 25-gauge needle, a local infiltration of 2% lidocaine was performed at the entry point, and a 17-gauge Tuohy needle was advanced through the skin. The needle entry point was located at the junction between midline of the pedicle paralleled to the midline of T7 VB and the lower border of T7 VB on AP view of the fluoroscope (Fig. 1). The Tuohy needle was pushed into the skin to form an angle of approximately 10 o medially until it reached the lamina of the vertebra. The needle was then withdrawn slightly and advanced further medially as well as cephalad until the needle tip was situated in the midline at the height of the pedicle. Assuming the needle would enter the ILS if it did not touch the bone, the needle was further advanced - slowly and using the hanging drop method - until it arrived in the epidural space, at which point the number of times the needle touched the lamina was counted. A contrast agent (Omnipaque R, GE Healthcare, 300 mgi/ml) was administered, with the location of the epidural space confirmed in AP as well as lateral views. Based on the AP views, the angle formed between the inserted needle and the VB midline was measured and then denoted as the inward angulation (IA) (Fig. 2). From the lateral view, the angle between the needle and the line extending to the vertebral body s posterior border was measured and denoted as the upward angulation (UA) (Fig. 3). To investigate the relationships between the locations of the Tuohy needle tip, pedicle, and VB, the shortest distance between the Tuohy needle tip and both pedicles lower borders and the vertebral body s lower border was measured in the AP view, the height of the pedicle and that of the VB were measured, and the ratios (e/a, f/c) were obtained (Fig. 4). The actual needle depth extending from the skin entry point to the epidural space was measured, and the correlation coefficient between the actual depth and patients weight, height, PI, and the calculated depth determined by using the pre-surgical computed tomography (CT) scans was obtained. To obtain the calculated depth, the line linking the epidural space between T6-7 and the spinous process was used (Distance B) (Fig. 5A), and a calculation was performed using the IA and UA, along with the Pythagorean Fig. 2. The figure shows the inward angulation, which represents the angle of the needle to the line of the spinous process on AP view. IA: inward angulation. Fig. 1. This figure shows the interlaminar space, pedicle and ver tebral body on AP radiograph. The needle entry point is the junction between the midline of the pedicle and the lower border of vertebral body. P: pedicle, VB: vertebral body, ML : midline, IE: inferior endplate of vertebral body, NEP: needle entry point. Fig. 3. The figure shows the upward angulation, which represents the angle of the needle to the line made by the posterior border of the vertebral body (white line) on lateral view. UA: upward angulation. 443
4 Midthoracic epidural block Vol. 62, No. 5, May 2012 trigonometric identity (i.e., calculated depth = B / cos [IA] o cos [90 - UA] o ) (Fig. 5B). All measurements were presented as mean and standard deviation. The Shapiro-Wilk test was used for correlation normality tests; additionally, Pearson s correlation was used. Statistical analysis was conducted using SPSS Version 15.0 (SPSS Inc., USA). A P value of < 0.05 was considered statistically significant. Results In 22 of the 24 subjects, the Tuohy needle was inserted into the T6-7 ILS without difficulty. In the other two subjects, the needle was inserted into the T5-6 ILS instead. These two subjects were excluded from all statistical evaluations. Out of the 22 patients, three subjects represented cases in which the needle touched the lamina three times, and four patients represented cases in which the lamina was touched by the needle twice. In the remaining 15 patients, the needle came into contact with the bone once. The IA was 24.8 o ± 5.5 o (minimum value: 12 o, maximum value: 34 o ), and the UA was 54.5 o ± 7.1 o (minimum value: 36 o, maximum value: 70 o ). In most patients, the tip of the needle was found to be situated between the upper half of the height of the T7 pedicle and the inferior border of the T6 VB, on the side of the puncture from the midline. Out of the 22 patients, the needle tip was found to be situated above the T6 VB inferior border in one patient (5%); situated between the T6 VB lower border and the superior Fig. 4. A schematic representation that depicts the projection of a thoracic vertebra (T7) and shows the height of the interlaminar space and epidural needle tip relative to the pedicle and vertebral body. This figure is referred to in Nagaro's study, but ILS cannot be determined on AP view in this study. P: pedicle, VB: vertebral body, ILS: interlaminar space, EN: epidural needle, a: length of pedicle, b: distance from the lower border of the pedicle to the interlaminar space, c: length of vertebral body, d: distance from the lower border of vertebral body to the interlaminar space, e: distance from the lower border of the pedicle to the epidural needle tip, f: distance from the lower border of vertebral body to epidural needle tip. Fig. 6. The figure shows the location of the epidural needle tips (hollow circle and solid circle) with fluoroscope guided epidural block. The hollow square refers to the ipsilateral side of the needle entry point, but the solid square is the contralateral side. Most needle tips are located at the space A and B. A: space between T6 lower border and upper border of the T7 pedicle, B: space between upper border and horizontal midline of the T7 pedicle, C: space between horizontal midline and lower border of the T7 pedicle, ML: midline, P: pedicle. Fig. 5. (A) The midthoracic computed tomography film (transverse plane). B: The distance from the epidural space to skin at the T6-7. (B) Principle of Pythagorean triangle trigonometry. Esti mated depth = B / cos (IA) o cos (90 - UA) o ; B = Distance from the epidural space to skin at the T6-7 (CT transverse plane). IA: Inward anglulation (sagittal plane), UA: upward anglulation (axial plane), EN: epidural needle with paramedian approach. 444
5 Korean J Anesthesiol Kim, et al. border of the T7 pedicle in six patients (27%); between the superior border and the horizontal midline of the T7 pedicle in 12 patients (55%); between the horizontal midline and the inferior border of the T7 pedicle in three patients (13%); and beyond the vertical midline of the VB in one patient (5%) (Fig. 6). The ratio between the pedicle length (a) and the distance between the inferior border of the pedicle and the needle tip (e) (e/a) was 0.76 ± 0.32 (minimum value: 0.13, maximum value: 1.2), and the ratio between the height of the vertebral body (c) and the distance between the inferior border of the vertebral body and the needle tip (f ) (f/c) was 0.98 ± 0.13 (minimum value: 0.75, maximum value: 1.35) (Fig. 4). The actual depth from the skin entry point to the epidural space was 5.1 cm ± 0.6 cm (minimum value: 4.1 cm, maximum value: 7 cm), and the correlation coefficients between the epidural space s actual depth and the patients weight and PI were and 0.783, respectively; these values were statistically significant (P < 0.01). The distance between the epidural space and the skin measured in the CT scans was 4.3 cm ± 0.6 cm (minimum value: 3.6 cm, maximum value: 6.2 cm). The distance obtained by trigonometry (i.e., the calculated depth) was 6.1 cm ± 1.0 cm. The calculated depth was longer than the actual depth by 0.9 cm ± 0.8 cm; the correlation coefficient between the two values was 0.563, which was significant (P = 0.014). Discussion This study was conducted to evaluate the viability and clinical applicability of a fluoroscope guided thoracic epidural block, based on the method reported by Nagaro et al. [7]. In this study, the inward angulation (IA) was 24.8 o ± 5.5 o, which differed from the figure of 35 o ± 8 o reported by Nagaro et al. [7]. We assumed this difference could be attributed to the location of the needle tip. In the study by Nagaro et al., the needle tips were placed above the vertical midline of the VB in all five patients [7], whereas in this study the needle tip was placed, in most cases, slightly laterally from the vertical midline, on the ipsilateral side of the skin entry point. The upward angulation (UA) in this study, 54.5 o ± 7.1 o, differed slightly from the figure reported by Nagaro et al. [7], 56 o ± 11 o. The UA is critical in determining the distance between the skin and the epidural space. In a study by Yang et al. on the depth of the thoracic epidural space measured from the skin, the distance between the skin and the T6-7 epidural space, measured in the sitting position via a paramedian approach, was 6.16 cm ± 1.25 cm [8], while the distance between the skin entry point and the thoracic epidural space in this study was 5.1 cm ± 0.6 cm. In other words, considering that the patients demographic information (e.g., height, weight, sex) in this study was similar to the information in the study by Yang et al., the approach used in this study appears to have resulted in a larger UA than that obtained by a blind method [8]. In fact, the lateral views showed that in this study there were more cases in which the angle between the needle and the posterior border of the vertebral body was larger than the angle between the midline of the upper and lower ILS and the posterior border of the vertebral body. Based on the method adopted by Nagaro et al., the correlations between the distance from the skin to the epidural space and the patients weight and PI, respectively, were examined. In the epidural block using a median approach, a significant correlation was reported between the patients weight and PI, respectively, and the distance between the skin and the epidural space [9,10]. Located between the skin and the epidural space are several structures, including the subcutaneous tissue, the supraspinous ligament, the interspinous ligament, and the ligamentum flavum. The reported correlation between the patients weight and the depth of the epidural space can be explained by the fact that the subcutaneous tissue is the structure with the highest variability among patients [11]. In a paramedian approach, the angle created between the needle and the skin surface could vary; in addition, deviation of the measurements could increase because the needle tip could likely be placed in ILS on the contralateral side of the entry point. Shim et al. [12] reported that there were no correlations between the patients height, weight and PI, the angle between the skin surface and the needle in the thoracic vertebrae, and the depth of the thoracic epidural space. In the study described here, however, the entry point was determined by fluoroscopy. Thus, the reference entry point was the same for all cases, as was the target location of the needle point. As a result, the IA and UA in this study were consistent to a certain degree, contributing to the significant correlations found between the patients weight, the PI and the depth of needle insertion. In this study, the correlation between the actual depth extending to the thoracic epidural space and the CT-guided calculated depth was also examined. The calculated depth was found to be larger than the actual depth, a finding consistent with the results reported by Kao et al. [13] in a study in which the depth was measured in the lower thoracic region (T10-11), yet contradictory to the results of Lee et al. [14], in whose study the actual depth in the midthoracic region (T7-8) was found to be larger than the calculated depth. The reason why the calculated depth was larger than the actual depth in our study is presumably that the position the patients were instructed to assume (i.e., the prone position, with support from a 10 cm deep pillow) had tightened the skin more than in the supine position where, as in a CT scan, the patients lie on their back, with their arms raised. This prone position, then, had ultimately caused the patients subcutaneous tissue to receive more 445
6 Midthoracic epidural block Vol. 62, No. 5, May 2012 pressure and become more compressed, thus rendering the actual depth smaller when measured. Therefore, an important implication is derived: when advancing the Tuohy needle into the thoracic epidural space, the clinician should expect to find the space in a shallower spot than the calculated depth, and thus should suspect that any further advancing of the needle (i.e., all the way into the estimated depth) could carry the risk of damaging the spinal cord. Nagaro et al. chose the pedicle as the needle s target reference site because they reasoned that they could reduce variability between patients due to the fact that the pedicle is associated with the least amount of anatomical variation and degenerative changes found in individual patients [15]. Using the skeletons of five cadavers, the researchers verified that the caudal edges of the ILS in all thoracic vertebrae, including the midthoracic region, and all lumbar vertebrae, were situated at the height of the pedicle, and that they were all situated at a height half that of the VB or above the VB. From fluoroscope guided AP views, the researchers then determined that the ratio between the length of the pedicle in T7 (a) and the distance between the pedicle s lower border and the ILS caudal edge (b) (b/a) was 0.6 ± 0.1. They also obtained the ratio between the length of the VB (c) and the distance between the VB inferior border and the ILS caudal edge (d) (d/c), which was found to be 0.7 ± 0.1 (Fig. 4). In this study, we originally intended to verify the aforementioned findings in our patients, using a C-arm guide. However, we found it impossible to achieve a clear examination of the ILS caudal edge in the AP views due to the obstruction of fluoroscopy by the long spinous processes of the thoracic vertebrae, the acute angle formed by these, and the organs situated in the mediastinum. Therefore, we chose to calculate the abovementioned ratios using the needle tip placed in the epidural space. According to our calculations, the ratio between the pedicle length and the distance between the pedicle s inferior border and the needle tip was 0.76 ± 0.33, and the ratio between the VB length and the distance between the VB lower border and the needle tip was 0.98 ± These figures were slightly larger than those obtained by Nagaro et al., presumably because the needle tip in our study was placed into the epidural space, slightly toward the cranial side rather than toward the ILS caudal edge. In the majority of the 22 patients participating in this study, the needle tip was found to be placed somewhere between horizontal midline of the T7 pedicle and the T6 VB inferior border. The ratio between the pedicle length (a) and the distance between the pedicle s lower border and the needle tip (e) (e/a) was, on average, 0.76, indicating that in most patients, the interlaminar space began in the upper half part of the pedicle. However, since the minimum value was 0.13, caution is required when the needle is pushed in toward the lamina; such a first trial could lead to a penetration into the ILS. The maximum value, on the other hand, was 1.2, indicating that in certain cases the ILS began above the lower border of the VB in the upper level along the thoracic vertebrae. The approach adopted by Nagaro et al. appears to offer a clearer guideline on the needle entry point and target site than that suggested by the blind method. In their approach, the IA and UA, also appear to be more consistent. The use of fluoroscopy enables clinicians to approach the epidural space at a particular angle, as well as to confirm the placement of the needle inside the epidural space when assisted by the use of contrast agents. This technique helps prevent complications resulting from epidural blocks, such as spinal cord injury. In the study described here, insertion of the Tuohy needle into the desired site was unsuccessful in two patients. Nevertheless, the needle was introduced safely into the epidural space in the upper level of the thoracic vertebrae. As a result, a 100% Tuohy needle insertion rate was accomplished. Several features of our study differ from those reported by Nagaro et al. For example, we carried out needle insertion in the prone position, not the lateral position. Inserting a Tuohy needle in the prone position has several merits. First, the prone position helps clinicians obtain C-arm guidance AP and lateral views with greater ease. Second, it is easier for the patients to maintain the same position throughout the procedure, without moving; it is also easier for the clinician to secure his or her visual field. Third, when verifying the thoracic level via fluoroscopy, the prone position makes it easier to count the bones (i.e., counting from T1 in the caudal direction). Lastly, when inserting the needle into the skin, the prone position helps reduce what is known as the dimpling of the skin. Based on the results of this study, we suggest two ways to complement the method adopted by Nagaro et al. First, shifting the skin entry point slightly in the caudal direction would likely help the clinician locate the thoracic epidural space, since their method employs a larger UA, whereby the needle tends to approach the ILS at an acute angle instead of approaching it parallel to the lamina, and as a result increases the likelihood of failing to locate the epidural space. In this study, our attempt to insert the needle into the ILS between T6-7 failed in two patients; the insertion was accomplished in the space between T5-6 instead. The failure is presumably attributable to a UA that was larger than appropriate, in which case the needle tends to touch the lamina and then penetrate into ILS of the upper-level vertebra rather than the intended space. If the insertion must be accomplished in the ILS between T6-7, the skin entry point should be shifted toward the caudal edge, thereby reducing the UA. Second, achieving a greater flexion of the thoracic vertebrae would enable clinicians to locate the thoracic epidural space 446
7 Korean J Anesthesiol Kim, et al. with greater ease. In fact, not only the UA of the needle in the midthoracic region but also the degree of thoracic flexion, as well as the presence of osteophytes, influence the anesthesiologists attempts to locate the thoracic epidural space. While it is more difficult than increasing the flexion of either the lumbar spine or the cervical vertebrae, accomplishing a greater flexion of the thoracic vertebrae, such as by increasing the depth of pillow beyond 10 cm, as used in this study, would facilitate the attempt to locate the thoracic epidural space. In one of the 22 patients in our study, the UA was found to be 70 o, showing a considerable difference from the average UA of 55 o. The reason why the needle could penetrate into the epidural space despite such a large difference in UA was presumably the height of the interlaminar space. In conclusion, the epidural block performed in the midthoracic region as described by Nagaro et al. is a clinically easy and safe procedure. We recommend further research on an alternative method in which the needle is inserted from a skin entry point that is situated slightly toward the caudal edge. References 1. De Cosmo G, Aceto P, Gualtieri E, Congedo E. Analgesia in thoracic surgery: review. Minerva Anesthesiol 2009; 75: Sawchuk CW, Ong B, Unruh HW, Horan TA, Greengrass R. Thoracic versus lumbar epidural fentanyl for postthoracotomy pain. Ann Thorac Surg 1993; 55: Lomessy A, Magnin C, Viale JP, Motin J, Cohen R. Clinical advantages of fentanyl given epidurally for postoperative analgesia. Anesthesiology 1984; 61: Hood DD, Dewan DM. Anesthetic and obstetric outcome in morbidly obese parturients. Anesthesiology 1993; 79: Konrad C, Schüpfer G, Wietlisbach M, Gerber H. Learning manual skills in anesthesiology: Is there a recommended number of cases for anesthetic procedures? Anesth Analg 1998; 86: Giebler RM, Scherer RU, Peters J. Incidence of neurologic complications related to thoracic epidural catheterization. Anesthesiology 1997; 86: Nagaro T, Yorozuya T, Kamei M, Kii N, Arai T, Abe S. Fluoroscopically guided epidural block in the thoracic and lumbar regions. Reg Anesth Pain Med 2006; 31: Yang MK, Kim DH, Kim KW. A depth of the Tuohy needle in thoracic epidural anesthesia. Korean J Anesthesiol 1994; 27: Han KR, Choi HR, Hyun HS, Kwak NK, Kim C. A clinical measure of the skin to cervical epidural space depth in the Korean adults. J Korean Pain Soc 1999; 12: Song ZH, Kang YS, Chun TW, Cho KH. Distance from skin in the lumbar epidural space in Korean adult male. Korean J Anesthesiol 1994; 27: Palmer SK, Abram SE, Maitra AM, von Colditz JH. Distance from the skin to the lumbar epidural space in an obstetric population. Anesth Analg 1983; 62: Shim JC, Lee ME, Kim DW. Predicting factors for the distance from skin to the epidural space with the paramedian epidural approach. J Korean Pain Soc 1996; 9: Kao MC, Tsai SK, Chang WK, Liu HT, Hsieh YC, Hu JS, et al. Prediction of the distance from skin to epidural space for low-thoracic epidural catheter insertion by computed tomography. Br J Anaesth 2004; 92: Lee SJ, Choi SH, Kim MS, Shin YS. Prediction of the distance from skin to midthoracic epidural space by computed tomography. Korean J Anesthesiol 2005; 48: Kricun ME. Imaging modalities in spinal disorder. Philadelphia, WB Saunders. 1988, pp
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion
 Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Pain Physician 2011; 14:195-210 ISSN 1533-3159 Technical Report Alternative Approach To Needle Placement In Cervical Spinal Cord Stimulator Insertion Jie Zhu, MD 1,2, Frank J. E. Falco, MD 1, 2, C. Obi
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
The goal of this article is to describe the. Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation.
 Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
Pain Physician 2011; 14:45-53 ISSN 1533-3159 Technique Alternative Approach To Needle Placement In Spinal Cord Stimulator Trial/Implantation Jie Zhu, MD 1, Frank Falco, MD 1,2, C. Obi Onyewu, MD 1, Youssef
mild Devices Kit - Instructions for Use
 INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
INDICATION FOR USE The Vertos mild Devices are specialized surgical instruments intended to be used to perform lumbar decompressive procedures for the treatment of various spinal conditions. CONTENTS AND
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Computed Tomography (CT) Simulated Fluoroscopy-Guided Transdiscal Approach in Transcrural Celiac Plexus Block
 Brief Report Korean J Pain 2013 October; Vol. 26, No. 4: 396-400 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.4.396 Computed Tomography (CT) Simulated Fluoroscopy-Guided Transdiscal
Brief Report Korean J Pain 2013 October; Vol. 26, No. 4: 396-400 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.4.396 Computed Tomography (CT) Simulated Fluoroscopy-Guided Transdiscal
Christopher Ciarallo, MD Denver Health/Children s Hospital Colorado CRASH 2016
 Distribution of the vertebral level of the intercristal line by ultrasonography Christopher Ciarallo, MD Denver Health/Children s Hospital Colorado CRASH 2016 Korean J Anesthesiol. 2014 Sep;67(3):181 5
Distribution of the vertebral level of the intercristal line by ultrasonography Christopher Ciarallo, MD Denver Health/Children s Hospital Colorado CRASH 2016 Korean J Anesthesiol. 2014 Sep;67(3):181 5
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Percutaneous Vertebroplasty: Indications, Technique, and Results Sequence of Operations
 Percutaneous Vertebroplasty: Indications, Technique, and Results Sequence of Operations Technique: Sequence of Operations Materials Dual Guidance Local Anesthesia Puncture Vertebral Body Biopsy Vertebral
Percutaneous Vertebroplasty: Indications, Technique, and Results Sequence of Operations Technique: Sequence of Operations Materials Dual Guidance Local Anesthesia Puncture Vertebral Body Biopsy Vertebral
Introduction to ultrasound of the lumbar spine a systematic approach. Dr Anja U. Mitchell Copenhagen University Hospital Herlev Helsinki
 Introduction to ultrasound of the lumbar spine a systematic approach Dr Anja U. Mitchell Copenhagen University Hospital Herlev Helsinki 22.11.12 Applications Identify vertebral level Midline identification
Introduction to ultrasound of the lumbar spine a systematic approach Dr Anja U. Mitchell Copenhagen University Hospital Herlev Helsinki 22.11.12 Applications Identify vertebral level Midline identification
Ultrasound and central neuraxial blocks [Editorial]
![Ultrasound and central neuraxial blocks [Editorial] Ultrasound and central neuraxial blocks [Editorial]](/thumbs/90/103053049.jpg) Loughborough University Institutional Repository Ultrasound and central neuraxial blocks [Editorial] This item was submitted to Loughborough University's Institutional Repository by the/an author. Citation:
Loughborough University Institutional Repository Ultrasound and central neuraxial blocks [Editorial] This item was submitted to Loughborough University's Institutional Repository by the/an author. Citation:
I. Chien, I.C. Lu, F.Y. Wang, et al airway management [9]. An examination of a patient s back for spinal landmarks was reported to be a better predict
![I. Chien, I.C. Lu, F.Y. Wang, et al airway management [9]. An examination of a patient s back for spinal landmarks was reported to be a better predict I. Chien, I.C. Lu, F.Y. Wang, et al airway management [9]. An examination of a patient s back for spinal landmarks was reported to be a better predict](/thumbs/92/108339438.jpg) SPINAL PROCESS LANDMARK AS A PREDICTING FACTOR FOR DIFFICULT EPIDURAL BLOCK: A PROSPECTIVE STUDY IN TAIWANESE PATIENTS I Chien, I-Chen Lu, Fu-Yuan Wang, Lee-Ying Soo, Kwong-Leung Yu, and Chao-Shun Tang
SPINAL PROCESS LANDMARK AS A PREDICTING FACTOR FOR DIFFICULT EPIDURAL BLOCK: A PROSPECTIVE STUDY IN TAIWANESE PATIENTS I Chien, I-Chen Lu, Fu-Yuan Wang, Lee-Ying Soo, Kwong-Leung Yu, and Chao-Shun Tang
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
Technical Note NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE FLUOROSCOPIC VIEWS DURING CERVICAL RADIOFREQUENCY NEUROTOMY.
 Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
Technical Note Interventional Pain Management Reports ISSN 2575-9841 Volume 2, Number 4, pp127-131 2018, American Society of Interventional Pain Physicians NEEDLE TIP DEPTH ASSESSMENT ON FORAMINAL OBLIQUE
David S. Warner, M.D., Editor. Ultrasonography of the Adult Thoracic and Lumbar Spine for Central Neuraxial Blockade
 REVIEW ARTICLE David S. Warner, M.D., Editor Ultrasonography of the Adult Thoracic and Lumbar Spine for Central Neuraxial Blockade Ki Jinn Chin, F.R.C.P.C.,* Manoj Kumar Karmakar, M.D., Philip Peng, F.R.C.P.C.
REVIEW ARTICLE David S. Warner, M.D., Editor Ultrasonography of the Adult Thoracic and Lumbar Spine for Central Neuraxial Blockade Ki Jinn Chin, F.R.C.P.C.,* Manoj Kumar Karmakar, M.D., Philip Peng, F.R.C.P.C.
Ultrasound-guided Pulsed Radiofrequency of the Third Occipital Nerve
 Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Case Report Korean J Pain 2013 April; Vol. 26, No. 2: 186-190 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.2.186 Ultrasound-guided Pulsed Radiofrequency of the Third Occipital
Limitations: The Epidrum cannot be used to confirm whether the needle has entered the vascular space without fluoroscopy.
 Pain Physician 2016; 19:131-138 ISSN 1533-3159 Randomized Trial False Loss of Resistance in Cervical Epidural Injection: The Loss of Resistance Technique Compared with the Epidrum Guidance in Locating
Pain Physician 2016; 19:131-138 ISSN 1533-3159 Randomized Trial False Loss of Resistance in Cervical Epidural Injection: The Loss of Resistance Technique Compared with the Epidrum Guidance in Locating
THE VERTEBRAL COLUMN. Average adult length: In male: about 70 cms. In female: about 65 cms.
 THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
ASJ. Magnification Error in Digital Radiographs of the Cervical Spine Against Magnetic Resonance Imaging Measurements. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Dorsal Fixation of the Thoracic and Lumbar Spine Techniques
 Pedicle, Facet, Cortical, and Translaminar Screw Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Dorsal Fixation of the Thoracic and Lumbar
Pedicle, Facet, Cortical, and Translaminar Screw Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Dorsal Fixation of the Thoracic and Lumbar
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT
 US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
US-GUIDED INTRA-ARTICULAR INJECTION TECHNIQUE OF FACETS JOINT www.ecografieinfiltrazioni.it Dott. Luca Di Sante LBP is a major cause of disability, the exact pathogenesis of acute LBP remains unclear The
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Origin of lumbar spinal roots and their relationship to intervertebral discs
 Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
A New Anterior Approach for Fluoroscopy-guided Suprascapular Nerve Block
 Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
Original Article Korean J Pain 2012 July; Vol. 25, No. 3: 168-172 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.3.168 A New Anterior Approach for Fluoroscopy-guided Suprascapular
UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS. Surgical Technique
 UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS Surgical Technique Joint Spine Sports Med MySpine Surgical Technique Joint Spine Sports Med 2 INTRODUCTION MySpine is a patient matched, pedicle targeted technology
UNIQUE ANATOMIES PATIENT-MATCHED SOLUTIONS Surgical Technique Joint Spine Sports Med MySpine Surgical Technique Joint Spine Sports Med 2 INTRODUCTION MySpine is a patient matched, pedicle targeted technology
Thoracic and Lumbar Spine Anatomy.
 Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
Confirmation with Epidurogram Necessary?
 Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES
 REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
The Effects of Posture on Neck Flexion Angle While Using a Smartphone according to Duration
 J Korean Soc Phys Med, 2016; 11(3): 35-39 http://dx.doi.org/10.13066/kspm.2016.11.3.35 Online ISSN: 2287-7215 Print ISSN: 1975-311X Research Article Open Access The Effects of Posture on Neck Flexion Angle
J Korean Soc Phys Med, 2016; 11(3): 35-39 http://dx.doi.org/10.13066/kspm.2016.11.3.35 Online ISSN: 2287-7215 Print ISSN: 1975-311X Research Article Open Access The Effects of Posture on Neck Flexion Angle
The Most Reliable Spinal Solution
 MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
MFG : 09.02.20 REV : 1 4CIS VANE introduces you the reliable pedicle screw The Most Reliable Spinal Solution Non-slip threaded joint Ergonomic design Wedged trapezoid thread Superior locking mechanism
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D.
 Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
Corresponding Author:
 Palpate Intercristal Line CORRECTLY: Not Transgress TOO High: Can Be TOO Close To Conus Medullaris Deepak Gupta *, David H. Rustom ** and Shushovan Chakrabortty *** The Intercristal Line (ICL) is an imaginary
Palpate Intercristal Line CORRECTLY: Not Transgress TOO High: Can Be TOO Close To Conus Medullaris Deepak Gupta *, David H. Rustom ** and Shushovan Chakrabortty *** The Intercristal Line (ICL) is an imaginary
A survey of dental treatment under general anesthesia in a Korean university hospital pediatric dental clinic
 Original Article pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2016;16(3):203-208 http://dx.doi.org/10.17245/jdapm.2016.16.3.203 A survey of dental treatment under general anesthesia in a Korean
Original Article pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2016;16(3):203-208 http://dx.doi.org/10.17245/jdapm.2016.16.3.203 A survey of dental treatment under general anesthesia in a Korean
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
The vault bones Frontal Parietals Occiput Temporals Sphenoid Ethmoid
 The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
Original Article Clinics in Orthopedic Surgery 2016;8:
 Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Original Article Clinics in Orthopedic Surgery 2016;8:71-77 http://dx.doi.org/10.4055/cios.2016.8.1.71 More than 5-Year Follow-up Results of Two- Level and Three-Level Posterior Fixations of Thoracolumbar
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
Outline. Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures
 C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Thoracic epidural analgesia is an effective acute pain management
 REGIONAL ANESTHESIA AND ACUTE PAIN ORIGINAL ARTICLE Evaluation of Ultrasound-Assisted Thoracic Epidural Placement in Patients Undergoing Upper Abdominal and Thoracic Surgery A Randomized, Double-Blind
REGIONAL ANESTHESIA AND ACUTE PAIN ORIGINAL ARTICLE Evaluation of Ultrasound-Assisted Thoracic Epidural Placement in Patients Undergoing Upper Abdominal and Thoracic Surgery A Randomized, Double-Blind
Transitioning to the Suboccipital Triangle. Suboccipital Triangle
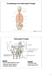 Transitioning to the Suboccipital Triangle Syllabus p. 14-15 Suboccipital Triangle Borders -Rectus capitis posterior major -Obliquus capitis superior -Obliquus capitis inferior Contents -Vertebral artery
Transitioning to the Suboccipital Triangle Syllabus p. 14-15 Suboccipital Triangle Borders -Rectus capitis posterior major -Obliquus capitis superior -Obliquus capitis inferior Contents -Vertebral artery
An approach to neuraxial anaesthesia for the severely scoliotic spine
 British Journal of Anaesthesia 111 (5): 807 11 (2013) Advance Access publication 9 May 2013. doi:10.1093/bja/aet161 An approach to neuraxial anaesthesia for the severely scoliotic spine C. Bowens 1 *,
British Journal of Anaesthesia 111 (5): 807 11 (2013) Advance Access publication 9 May 2013. doi:10.1093/bja/aet161 An approach to neuraxial anaesthesia for the severely scoliotic spine C. Bowens 1 *,
Clinical Effectiveness of Ultrasound-guided Costotransverse Joint Injection in Thoracic Back Pain Patients
 Brief Report Korean J Pain 2016 July; Vol. 29, No. 3: 197-201 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.3.197 Clinical Effectiveness of Ultrasound-guided Costotransverse Joint
Brief Report Korean J Pain 2016 July; Vol. 29, No. 3: 197-201 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2016.29.3.197 Clinical Effectiveness of Ultrasound-guided Costotransverse Joint
SURGICAL REMOVAL OF A LOOPED AND KNOTTED EPIDURAL CATHETER IN A POSTPARTUM PATIENT
 SURGICAL REMOVAL OF A LOOPED AND KNOTTED EPIDURAL CATHETER IN A POSTPARTUM PATIENT - A Case Report - O. AL-KAYED *, F. AL-BOUTI **, AND M.O. ABABNEH *** Summary We report a case of unsuccessful removal
SURGICAL REMOVAL OF A LOOPED AND KNOTTED EPIDURAL CATHETER IN A POSTPARTUM PATIENT - A Case Report - O. AL-KAYED *, F. AL-BOUTI **, AND M.O. ABABNEH *** Summary We report a case of unsuccessful removal
Continuous Spinal Anaesthesia
 Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
2012 CPT Changes Affecting Radiology REVISIONS
 2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
O bstetric patients present unique challenges. Pre-Procedure Neuraxial Ultrasound in Obstetric Anesthesia
 Pre-Procedure Neuraxial Ultrasound in Obstetric Anesthesia Manuel C. Vallejo ABSTRACT Aim of review: To determine the current state of pre-procedure neuraxial ultrasound in obstetric anesthesia practice.
Pre-Procedure Neuraxial Ultrasound in Obstetric Anesthesia Manuel C. Vallejo ABSTRACT Aim of review: To determine the current state of pre-procedure neuraxial ultrasound in obstetric anesthesia practice.
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Epidural anaesthesia and analgesia
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Epidural anaesthesia and analgesia Author : Matthew Gurney Categories : Vets Date : June 1, 2009 Matthew Gurney discusses
Comprasion of Effectiveness of CT vs C-arm Guided Percutaneous Radiofrequency Lumbar Facet Rhizotomy
 Original Article Korean J Pain 2010 June; Vol. 23, No. 2: 137-141 pissn 2005-9159 eissn 2093-0569 DOI:10.3344/kjp.2010.23.2.137 Comprasion of Effectiveness of CT vs C-arm Guided Percutaneous Radiofrequency
Original Article Korean J Pain 2010 June; Vol. 23, No. 2: 137-141 pissn 2005-9159 eissn 2093-0569 DOI:10.3344/kjp.2010.23.2.137 Comprasion of Effectiveness of CT vs C-arm Guided Percutaneous Radiofrequency
The value of Tuffier s line for neonatal neuraxial procedures. Department of Anatomy, School of Medicine, Faculty of Health Sciences,
 The value of Tuffier s line for neonatal neuraxial procedures Albert van Schoor 1, MC Bosman 1, and AT Bosenberg 2, Original article 1 Department of Anatomy, School of Medicine, Faculty of Health Sciences,
The value of Tuffier s line for neonatal neuraxial procedures Albert van Schoor 1, MC Bosman 1, and AT Bosenberg 2, Original article 1 Department of Anatomy, School of Medicine, Faculty of Health Sciences,
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
SURGICAL TECHNIQUE MANUAL. InterFuse T
 1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Citation for published version (APA): Eijkelkamp, M. F. (2002). On the development of an artificial intervertebral disc s.n.
 University of Groningen On the development of an artificial intervertebral disc Eijkelkamp, Marcus Franciscus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
University of Groningen On the development of an artificial intervertebral disc Eijkelkamp, Marcus Franciscus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
Infraclavicular brachial plexus blocks aim at the
 REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives
 1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
LESSON ASSIGNMENT. Positioning for Exams of the Spine. After completing this lesson, you should be able to identify:
 LESSON ASSIGNMENT LESSON 4 Positioning for Exams of the Spine. LESSON ASSIGNMENT Paragraphs 4-1 through 4-15. LESSON OBJECTIVES After completing this lesson, you should be able to identify: 4-1. Identify
LESSON ASSIGNMENT LESSON 4 Positioning for Exams of the Spine. LESSON ASSIGNMENT Paragraphs 4-1 through 4-15. LESSON OBJECTIVES After completing this lesson, you should be able to identify: 4-1. Identify
Technique Guide. StenoFix. Interspinous distraction after surgical decompression.
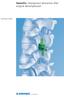 Technique Guide StenoFix. Interspinous distraction after surgical decompression. Table of Contents Introduction StenoFix 2 Indications and Contraindications 4 Surgical Technique Preoperative Planning
Technique Guide StenoFix. Interspinous distraction after surgical decompression. Table of Contents Introduction StenoFix 2 Indications and Contraindications 4 Surgical Technique Preoperative Planning
Contralateral Oblique View Is Superior to the Lateral View for Lumbar Epidural Access
 Pain Medicine 2016; 17: 839 850 doi: 10.1093/pm/pnv031 Contralateral Oblique View Is Superior to the Lateral View for Lumbar Epidural Access Jatinder S. Gill, MD,* Jyotsna V. Nagda, MD,* Musa M. Aner,
Pain Medicine 2016; 17: 839 850 doi: 10.1093/pm/pnv031 Contralateral Oblique View Is Superior to the Lateral View for Lumbar Epidural Access Jatinder S. Gill, MD,* Jyotsna V. Nagda, MD,* Musa M. Aner,
Feasibility study of real-time three-/four-dimensional ultrasound for epidural catheter insertion
 British Journal of Anaesthesia 107 (3): 438 45 (2011) Advance Access publication 9 June 2011. doi:10.1093/bja/aer157 REGIONAL ANAESTHESIA Feasibility study of real-time three-/four-dimensional ultrasound
British Journal of Anaesthesia 107 (3): 438 45 (2011) Advance Access publication 9 June 2011. doi:10.1093/bja/aer157 REGIONAL ANAESTHESIA Feasibility study of real-time three-/four-dimensional ultrasound
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study
 Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
A morphometric study of the Pedicles of dry human typical lumbar vertebrae
 Original article: A morphometric of the Pedicles of dry human typical lumbar vertebrae Dhaval K. Patil 1 *, Pritha S. Bhuiyan 2 1Resident, Department of Anatomy, Seth G S Medical College, Parel, Mumbai-400012,
Original article: A morphometric of the Pedicles of dry human typical lumbar vertebrae Dhaval K. Patil 1 *, Pritha S. Bhuiyan 2 1Resident, Department of Anatomy, Seth G S Medical College, Parel, Mumbai-400012,
J Korean Soc Spine Surg 2016 Sep;23(3): Originally published online September 30, 2016;
 Journal of Korean Society of Spine Surgery Multifocal Extensive Spinal Tuberculosis Accompanying Isolated Involvement of Posterior Elements - A Case Report - Dong-Eun Shin, M.D., Sang-June Lee, M.D., Young
Journal of Korean Society of Spine Surgery Multifocal Extensive Spinal Tuberculosis Accompanying Isolated Involvement of Posterior Elements - A Case Report - Dong-Eun Shin, M.D., Sang-June Lee, M.D., Young
ORIGINAL PAPER. Department of Orthopedic Surgery,Nagoya University Graduate School of Medicine,Nagoya,Japan 2
 Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Eldor Epidural Kit (CSEN 68) Epidural catheter technique
 Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Lumbar Facet Joint Interventions
 Krishna Poddar, Rachit Gulati PRACTITIONERS SECTION 10.5005/jp-journals-10046-0063 1 Krishna Poddar, 2 Rachit Gulati ABSTRACT Facet joints or zygapophyseal joints are paired synovial joints in the vertebrae
Krishna Poddar, Rachit Gulati PRACTITIONERS SECTION 10.5005/jp-journals-10046-0063 1 Krishna Poddar, 2 Rachit Gulati ABSTRACT Facet joints or zygapophyseal joints are paired synovial joints in the vertebrae
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW
 INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
TECHNICAL BROCHURE. Capture Facet Fixation System
 TECHNICAL BROCHURE Capture Facet Fixation System Table of Contents Product Overview...2 Instruments...4 Capture Facet Screw Surgical Technique Patient Preparation and Positioning...6 Guide Pin Placement...7
TECHNICAL BROCHURE Capture Facet Fixation System Table of Contents Product Overview...2 Instruments...4 Capture Facet Screw Surgical Technique Patient Preparation and Positioning...6 Guide Pin Placement...7
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Lumbar Puncture. Practical Skills Teaching. Year 3 Medical Students MB BCh
 Lumbar Puncture Practical Skills Teaching Year 3 Medical Students MB BCh 2012-2013 Contents Introduction to workshop... 3 Overall Session Aim... 4 Intended learning objectives... 4 Workshop Structure Guidance
Lumbar Puncture Practical Skills Teaching Year 3 Medical Students MB BCh 2012-2013 Contents Introduction to workshop... 3 Overall Session Aim... 4 Intended learning objectives... 4 Workshop Structure Guidance
THE benefits of pediatric regional anesthesia are many, Ultrasound Imaging for Regional Anesthesia in Infants, Children, and Adolescents
 REVIEW ARTICLES Anesthesiology 2010; 112:719 28 Copyright 2010, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins David S. Warner, M.D., Editor Ultrasound Imaging for Regional
REVIEW ARTICLES Anesthesiology 2010; 112:719 28 Copyright 2010, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins David S. Warner, M.D., Editor Ultrasound Imaging for Regional
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Sonographically Guided Lumbar Spine Procedures
 SOUND JUDGMENT Sonographically Guided Lumbar Spine Procedures David A. Provenzano, MD, Samer Narouze, MD, PhD Invited paper Videos online at www.jultrasoundmed.org The Sound Judgment Series consists of
SOUND JUDGMENT Sonographically Guided Lumbar Spine Procedures David A. Provenzano, MD, Samer Narouze, MD, PhD Invited paper Videos online at www.jultrasoundmed.org The Sound Judgment Series consists of
ACP. Anterior Cervical Plate System SURGICAL TECHNIQUE
 ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
ACP Anterior Cervical Plate System SURGICAL TECHNIQUE ACP TABLE OF CONTENTS INTRODUCTION 4 INDICATIONS AND CONTRAINDICATIONS 5 WARNINGS AND PRECAUTIONS 6 IMPLANT DESCRIPTION 7 INSTRUMENTS 10 SURGICAL
Hinged Laminoplasty System surgical technique
 BlackbirdTM Hls Hinged Laminoplasty System surgical technique Blackbird TM Hls The ChoiceSpine Blackbird Hinged Laminoplasty System (HLS) design eliminates fitting plates through trial and error bending.
BlackbirdTM Hls Hinged Laminoplasty System surgical technique Blackbird TM Hls The ChoiceSpine Blackbird Hinged Laminoplasty System (HLS) design eliminates fitting plates through trial and error bending.
Alamo T Transforaminal Lumbar Interbody System Surgical Technique
 Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
The sacrum is a complex anatomical structure.
 A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
The Effects of Nursing Intervention on Pain Control during Chemoport Needle Insertion
 Vol.128 (Healthcare and Nursing 2016), pp.169-173 http://dx.doi.org/10.14257/astl.2016. The Effects of Nursing Intervention on Pain Control during Chemoport Needle Insertion Jin Hee Shin 1, Mee Lan Park²,
Vol.128 (Healthcare and Nursing 2016), pp.169-173 http://dx.doi.org/10.14257/astl.2016. The Effects of Nursing Intervention on Pain Control during Chemoport Needle Insertion Jin Hee Shin 1, Mee Lan Park²,
Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol and sevoflurane
 Clinical Research Article Korean J Anesthesiol 2011 January 60(1): 36-40 DOI: 10.4097/kjae.2011.60.1.36 Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol
Clinical Research Article Korean J Anesthesiol 2011 January 60(1): 36-40 DOI: 10.4097/kjae.2011.60.1.36 Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol
100 Interpace Parkway Parsippany, NJ
 100 Interpace Parkway Parsippany, NJ 07054 www.biometspine.com 800-526-2579 All trademarks are the property of Biomet, Inc. or one of its subsidiaries, unless otherwise indicated. Rx Only. 2009 EBI, LLC.
100 Interpace Parkway Parsippany, NJ 07054 www.biometspine.com 800-526-2579 All trademarks are the property of Biomet, Inc. or one of its subsidiaries, unless otherwise indicated. Rx Only. 2009 EBI, LLC.
The Language of Anatomy. (Anatomical Terminology)
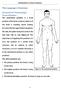 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
STANDARDIZED PROCEDURE LUMBAR PUNCTURE (Adult, Peds)
 I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
I. Definition The lumbar puncture (LP) may assist in the diagnosis of meningitis, encephalitis, metastatic carcinomas, brain tumors, leukemia, demyelinating conditions, brain or spinal cord abscesses,
Original Article The spread of spinal anesthesia in term parturient: effect of hip/shoulder width ratio and vertebral column length
 Int J Clin Exp Med 2016;9(11):21562-21567 www.ijcem.com /ISSN:1940-5901/IJCEM0028307 Original Article The spread of spinal anesthesia in term parturient: effect of hip/shoulder width ratio and vertebral
Int J Clin Exp Med 2016;9(11):21562-21567 www.ijcem.com /ISSN:1940-5901/IJCEM0028307 Original Article The spread of spinal anesthesia in term parturient: effect of hip/shoulder width ratio and vertebral
Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused by Paravertebral Block
 Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 33-37 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.33 Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused
Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 33-37 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.33 Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused
