Sinusitis in Adults UP TO DATE
|
|
|
- Maurice Manning
- 6 years ago
- Views:
Transcription
1 Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy Editor Lee Park, MD Disclosures: Peter H Hwang, MD Grant/Research/Clinical Trial Support: Xoran [Skull base imaging (X-CAT scanner)]. Consultant/Advisory Boards: Medtronic [Sinus surgery (surgical equipment)]; Intersect [Sinus surgery (drug eluting sinus stent)]; Sinuwave [Sinus surgery]; Arthrocare [Sinus surgery]. Anne Getz, MD Nothing to disclose. Daniel G Deschler, MD, FACS Nothing to disclose. Stephen B Calderwood, MD Consultant/Advisory Boards: Pulmatrix [Inhaled antimicrobial products (Not currently released)]. Patent Holder: Vaccine Technologies [Cholera (Cholera vaccines)]. Equity Ownership/Stock Options: PharmAthene [Biodefense (Anthrax)]. Lee Park, MD Employee of UpToDate, Inc. Employment (Spouse): Novartis. Equity Ownership/Stock Options (Spouse): Novartis. Contributor disclosures are reviewed for conflicts of interest by the editorial group. When found, these are addressed by vetting through a multi-level review process, and through requirements for references to be provided to support the content. Appropriately referenced content is required of all authors and must conform to UpToDate standards of evidence. Conflict of interest policy All topics are updated as new evidence becomes available and our peer review process is complete. Literature review current through: May This topic last updated: Feb 26, INTRODUCTION Acute rhinosinusitis (ARS) is defined as symptomatic inflammation of the nasal cavity and paranasal sinuses lasting less than four weeks. The term "rhinosinusitis" is preferred to "sinusitis" since inflammation of the sinuses rarely occurs without concurrent inflammation of the nasal mucosa [1]. The most common etiology of ARS is a viral infection associated with the common cold. Viral rhinosinusitis is complicated by acute bacterial infection in only 0.5 to 2.0 percent of episodes [2]. Uncomplicated acute viral rhinosinusitis (AVRS) typically resolves in 7 to 10 days. Acute bacterial rhinosinusitis (ABRS) may also be a self-limited disease. Rarely, patients with untreated bacterial disease may develop serious complications. (See "Acute sinusitis and rhinosinusitis in adults: Clinical manifestations and diagnosis", section on 'Classification of rhinosinusitis'.). Distinguishing AVRS related to colds and influenza-like illnesses from bacterial infection is a challenge frequently faced by the primary care clinician. Antibiotics are indicated for ABRS, but are ineffective and not recommended for AVRS. Despite the overwhelming prevalence of a viral etiology, however, in the late 1990s, 92 percent of patients in the United Kingdom [3] and 85 to 98 percent of patients in the United States (US) [4] were prescribed an antibiotic when seen for an
2 upper respiratory or sinus infection. Initiatives to limit the use of antibiotics for upper respiratory infections are ongoing in Europe and the United States [5]. This topic will address the treatment of acute rhinosinusitis. The clinical manifestations and diagnosis of acute rhinosinusitis are discussed separately. (See "Acute sinusitis and rhinosinusitis in adults: Clinical manifestations and diagnosis".) APPROACH TO TREATMENT The goals of treatment for acute rhinosinusitis (ARS) are different, depending on whether the source of infection is viral or bacterial. Management of acute viral rhinosinusitis (AVRS) aims to relieve symptoms of nasal obstruction and rhinorrhea; treatment does not shorten the clinical course of the disease. Treatment for acute bacterial rhinosinusitis (ABRS) includes antibiotics to eliminate the infection and prevent complications. Studies suggest that 40 to 69 percent of patients with ABRS may clear their infection spontaneously [6-8]. In most of these studies, however, the diagnosis of acute bacterial infection was not confirmed by sinus aspirate culture, but rather was based upon clinical criteria. The populations studied were therefore likely to include patients with viral infection. Thus, the actual rate of spontaneous resolution of bacterial infection is not certain, but likely to be lower than the reported 40 to 60 percent. It is generally not possible to distinguish AVRS from ABRS in the first 10 days of illness based upon history, examination, or radiologic study. The diagnosis of ABRS is usually clinical, since sinus aspirates for culture are not readily obtainable. ABRS should be suspected in patients presenting with any of the following three features [9]: Persistent symptoms or signs of ARS lasting 10 or more days with no clinical improvement Onset with severe symptoms (fever >39 C or 102 F and purulent nasal discharge or facial pain) lasting at least three consecutive days at the beginning of illness Onset with worsening symptoms following a viral upper respiratory infection that lasted five to six days and was initially improving (See "Acute sinusitis and rhinosinusitis in adults: Clinical manifestations and diagnosis", section on 'Distinguishing bacterial from viral infection'.) Since AVRS is expected to resolve within 10 days and ABRS may also resolve spontaneously within the first 10 days, patients who present with fewer than 10 days of symptoms in general should be managed with supportive care [10]. In a systematic review of 10 trials involving patients with uncomplicated acute sinusitis and a normal immune system, antibiotics slightly shortened the time to cure (number needed to treat for benefit 18) but increased the incidence of adverse effects (number needed to treat for harm 8) [11]. SYMPTOMATIC THERAPY FOR ACUTE RHINOSINUSITIS Acute viral rhinosinusitis (AVRS) is a self-limited process and treatment is aimed at symptom relief. Acute bacterial rhinosinusitis (ABRS) should be treated with antibiotics, but adjunctive therapy for management of symptoms is also indicated. Analgesics Analgesics such as nonsteroidal antiinflammatories andacetaminophen are recommended for pain relief.
3 Saline irrigation Mechanical irrigation with buffered, physiologic, or hypertonic saline may reduce the need for pain medication and improve overall patient comfort, particularly in patients with frequent sinus infections [12]. The evidence supporting use of saline irrigation is limited, but indicates some decrease in time lost from work and symptom relief with minor adverse effects, including nasal burning and irritation. It is important that irrigants be prepared from sterile or bottled water, as there have been reports of amebic encephalitis due to tap water rinses [13]. Instructions for preparing a rinse solution are shown in a table (table 1). Topical glucocorticoids The theoretic mechanism of action for intranasal glucocorticoids (corticosteroids) is a decrease in mucosal inflammation that allows improved sinus drainage. Studies evaluating topical glucocorticoids should be interpreted with caution, as many studies contain both heterogeneous patient populations (acute, chronic, and/orviral rhinosinusitis) and different treatment regimens (concomitant decongestant, saline irrigation, antibiotic). Studies of topical glucocorticoids have demonstrated some benefit for the relief of symptoms in ARS, both viral and bacterial. A meta-analysis of three studies, involving patients with ARS diagnosed by symptoms and confirmed by radiologic or endoscopic studies, found that use of intranasal steroids, alone or as adjuvant therapy to antibiotics, increased the rate of symptom response compared to placebo (RR 1.11, 95% CI ) [14]. Symptom resolution was greater for patients receiving intranasal glucocorticoids than placebo, and a dose response was observed, comparing mometasone furoate 200 and 400 mcg. When used as an adjunct to antibiotic therapy in the treatment of ABRS, a meta-analysis of placebo-controlled trials suggests that 15 patients would need to be treated with intranasal glucocorticoids to improve clinical symptoms in one patient. One randomized study of patients with ABRS did not demonstrate benefit for intranasal glucocorticoids [15]. Subgroup analysis of this study, however, found that patients with less-severe symptoms did benefit, possibly because thicker nasal secretions and closed ostia in patients with more severe illness limit penetrance of the topical steroids. Intranasal glucocorticoids are likely to be most beneficial for patients with underlying allergic rhinitis. Topical decongestants The use of topical decongestants, such asoxymetazoline, may provide a subjective sense of improved nasal patency. However, there is some concern that topical decongestants themselves may provoke mucosal inflammation, at least in an experimental animal model [16]. If used, topical decongestants should be used sparingly (no more than three consecutive days) to avoid rebound congestion [17]. Topical decongestants are suggested for symptomatic relief in the treatment of AVRS [18]. However, they have little effect as adjunctive therapy to antibiotics in the treatment of ABRS, and 2012 guidelines advise that they are not helpful in patients with ABRS [9]. Oral decongestants Oral decongestants are frequently used to reduce edema and facilitate aeration and drainage. Consistent reports on their efficacy are lacking, however. Some [19,20], but not all [21], studies have demonstrated improved patency of the nasal airway and sinus ostia. One randomized trial compared several oral decongestants (ephedrine sulfate 25 mg, pseudoephedrine HCL 60 mg, phenylephrine HCL 10 mg, and phenylpropanolamine HCL 25 mg) with placebo; only ephedrine was superior to placebo in this trial [22]. Similar to their recommendations against topical formulations, 2012 guidelines advise that oral decongestants are not helpful in patients with ABRS [9].
4 When eustachian tube dysfunction is a significant confounding factor in AVRS, a short course (three to five days) of oral decongestants may be warranted. Oral decongestants should be used with caution in patients with cardiovascular disease, hypertension, or benign prostate hypertrophy due to systemic adverse effects with oral alpha adrenergic preparations [23]. Antihistamines Antihistamines are frequently prescribed for symptom relief due to their drying effects; however, there are no studies investigating their efficacy for this indication [18]. Additionally, over-drying of the mucosa may lead to further discomfort. Antihistamines have side effects (drowsiness, xerostomia), and their use for the treatment of acute sinusitis is not recommended [9]. Mucolytics Mucolytics such as guaifenesin serve to thin secretions and may promote ease of mucus drainage and clearance; however, no published trials exist to definitively support their use [18]. COMMUNITY-ACQUIRED ACUTE BACTERIAL RHINOSINUSITIS For patients who present with 10 or more days of symptoms (purulent rhinorrhea, nasal congestion, and facial pressure), the likelihood of a diagnosis of ABRS is increased. (See "Acute sinusitis and rhinosinusitis in adults: Clinical manifestations and diagnosis", section on 'Distinguishing bacterial from viral infection' and 'Approach to treatment'above.) Observation Patients who are diagnosed with ABRS should be treated with antimicrobial therapy. However, the diagnosis of a bacterial process is often uncertain, and watchful waiting with assurance of follow-up may be appropriate for some patients with milder symptoms. Guidelines from a multidisciplinary expert panel in 2007 recommend that selected patients with symptoms suggestive of mild ABRS (only mild pain and temperature <38.3 C or 101 F) may be managed expectantly [18]. Patients under observation should be treated supportively for relief of symptoms for seven days after the time l, antimicrobial therapy is then initiated. Guidelines from the Infectious Disease Society of America (IDSA) in 2012 recommend that antimicrobial therapy might be withheld for three days in patients with mild symptoms, but initiated promptly thereafter if there is no improvement [9]. Factors such as age, general state of health, and comorbidities should be considered when choosing this option. Patients with moderately severe symptoms who meet clinical criteria for ABRS and patients with severe symptoms regardless of duration of illness should be treated with an antibiotic. Guidelines from the IDSA in 2012 recommend initiation of antibiotic therapy when ABRS is diagnosed by standardized criteria [9]. The rationale is to shorten the duration of illness, relieve symptoms, and prevent recurrent infection or complications. An algorithm for the treatment of acute bacterial rhinosinusitis is shown (algorithm 1). (See 'Antimicrobials' below.)q Antimicrobials Several studies and meta-analyses have addressed the efficacy of systemic antibiotics in the treatment of acute rhinosinusitis (ARS). Given the difficulty in distinguishing viral from bacterial infection, these studies are complicated by heterogeneity in patient symptoms, underlying etiology, and outcomes of treatment. A randomized trial of adult patients (n = 166) presenting to primary care offices who met clinical criteria for acute bacterial rhinosinusitis (ABRS) evaluated whether a 10-day course of amoxicillin, compared to placebo, improved disease-related quality of life as measured by
5 a symptom score [24]. There was no difference between groups at day 3, the primary specified outcome, or at day 10, although there was greater symptom improvement reported by the amoxicillin group at day 7. All patients were also offered symptomatic treatment for relief of pain, fever, cough, and nasal congestion. A 2008 meta-analysis based upon individual patient data (n = 2547) from nine randomized trials found that 15 patients with rhinosinusitis would need to be treated with antibiotics before one additional patient would be cured [25]. Clinical signs and symptoms did not define a patient subgroup that was more likely to benefit from treatment or distinguish viral from bacterial infection. A 2012 meta-analysis of 13 randomized trials in adults with ABRS (n = 2878) found that 13 patients (95% CI 9-22) would need to be treated with antibiotics for one to benefit [9]. A 2008 meta-analysis pooled results from 17 randomized trials in which acute sinusitis was variably diagnosed (the majority by clinical criteria, but also imaging, microbiology, and inflammatory markers) [7]. There was variability in choice of antibiotic, use of ancillary therapy, and inclusion of children (three studies). Compared to placebo, antibiotics were associated with a higher rate of cure or symptom improvement at 7 to 15 days (OR 1.64, 95% CI ), but the magnitude of effect was moderate (cure or improvement in 77 percent with antibiotics versus 68 percent with placebo). The 9 percent difference in cure/improvement rate with antibiotic therapy was at the expense of an 8 percent increase in adverse effects, mostly gastrointestinal (30 versus 22 percent for placebotreated patients). A meta-analysis that analyzed data from five trials comparing antibiotics to placebo, defining failure as lack of cure or improvement at 7 to 15 days follow-up, found an increased response rate for antibiotics (RR 0.66, 95% CI ) [26]. Eighty percent of the participants not treated with antibiotics and 90 percent of the antibiotic group improved within two weeks. No one antibiotic was superior to another in the review of 51 studies comparing antibiotics. Choice of antibiotic When antibiotics are administered, treatment is most often initiated empirically. Although culture-guided therapy is optimal, obtaining suitable cultures requires endoscopy or antral puncture and is generally reserved for patients with complications. (See "Acute sinusitis and rhinosinusitis in adults: Clinical manifestations and diagnosis", section on 'Diagnostic tests'.) Most comparative studies of antibiotics for the treatment of ABRS do not involve patients with culture-defined infection and therefore include patients who meet predefined clinical criteria but who may not have bacterial infection. The significant rate of spontaneous recovery in mixed populations of AVRS and ABRS decreases the ability of studies to differentiate between lesseffective and more-effective antibiotics (the apparent response to less-effective antibiotics is greater than would be seen in a more strictly defined ABRS population; conversely, the relative effectiveness of more appropriate antibiotics is diminished). Thus, the finding in multiple studies of equivalent effectiveness among antibiotics is called into some question [8,26-30]. Amoxicillin has been recommended as a first-line agent in the past because of its narrow spectrum and relative low cost. However, there is increasing emergence of antimicrobial resistance among respiratory pathogens, including pneumococci and H. influenzae. Resistance rates vary regionally, with the prevalence of H. influenzae resistance ranging from 27 to 43
6 percent in the US [9]. Additionally, the introduction of routine conjugated pneumococcal vaccination in children has changed the spectrum of bacterial infection. In both adults and children, the percentage of ABRS due to S. pneumoniae has decreased while the proportion of ABRS due to H. influenzae has increased. The addition of clavulanate to amoxicillin improves coverage for ampicillin-resistant H. influenzae as well as M. catarrhalis. While evidence is stronger in children than adults to support use of amoxicillin-clavulanateinstead of amoxicillin, the IDSA 2012 guidelines makes the following recommendations regarding antimicrobial treatment of ABRS in adults [9]: Amoxicillin-clavulanate rather than amoxicillin is recommended as empiric therapy for nonpenicillin allergic adults. Amoxicillin-clavulanate is also preferred to a respiratory fluoroquinolone as initial empiric therapy. The dose of amoxicillin-clavulanate for most patients would be either 500 mg/125 mg orally three times daily or 875 mg/125mg orally twice daily. High-dose amoxicillin-clavulanate (2 g orally twice daily) is recommended in geographic regions with rates of penicillin-nonsusceptible S. pneumonia exceeding 10 percent and for patients who meet any of the following criteria: 65 years and older, recently hospitalized, treated with an antibiotic in the previous month, or immunocompromised. Doxycycline is a reasonable alternative for first-line therapy and can be used in patients with penicillin allergy. A respiratory flulone (levofloxacin or moxifloxacin) is another option for penicillin-allergic patients. Macrolides (clarithromycin or azithromycin), trimethoprim-sulfamethoxazole, and secondor third-generation cephalosporins are not recommended for empiric therapy because of high rates of resistance of S. pneumoniae (and of H. influenzae for trimethoprimsulfamethoxazole). Routine coverage for S. aureus or methicillin-resistant S. aureus (MRSA) is not indicated at this time. Despite the prevalence of staphylococcal colonization in the middle meatus in health adults, S. aureus remains an uncommon cause of ABRS [31]. Local and regional histograms of bacterial resistance should be referenced to understand resistance trends in the local community. The recommendation to treat with amoxicillin-clavulanate rather than a respiratory fluoroquinolone is based upon studies showing equivalent effectiveness in patients with culturedocumented infection [32] and a need to limit the overuse of fluoroquinolones in an effort to slow the development of resistance to this antibiotic class. Pregnant patients can be treated with amoxicillin-clavulanate (class B); pregnant patients who are penicillin-allergic would need to be treated withazithromycin (class B), as doxycycline (class D) and fluoroquinolones (class C) are not options in pregnancy. Duration for initial treatment The IDSA guidelines advise a 5 to 7 day course of antibiotics (rather than 10 to 14 days) in adults. In one meta-analysis of 12 randomized trials of ABRS in adults, no difference was noted in response rates or relapse rates comparing short courses (3 to 7 days) and longer courses (6 to 10 days) of antibiotics [33]. Rates of adverse events were lower for 5 day compared with 10 day courses. However, there was heterogeneity in the trials in terms of symptom duration and use of adjunctive medications. Studies of antimicrobial response, based
7 upon sinus aspirate cultures in children, indicate bacterial eradication within 72 hours for appropriate antimicrobial treatment [34], supporting a shorter antibiotic course than has traditionally been advised. Systemic glucocorticoids A systematic review and meta-analysis of four randomized trials in adults with acute sinusitis (n = 1008) found that systemic glucocorticoids plus antibiotic, compared with antibiotic plus placebo or, in one trial, a nonsteroidal anti-inflammatory, resulted in improved symptom control at days three to seven (risk ratio, RR 1.4, 95% CI ) [35]. Radiologic findings consistent with acute sinusitis were part of the diagnostic criteria in three studies. These data are limited by the potential for attrition bias and the lack of long-term followup on the effects of steroids. In a subsequent randomized trial, oral prednisolone 30 mg daily for seven days was not more effective than placebo in reducing facial pain or pressure on day seven for adult patients with clinically diagnosed acute rhinosinusitis [36]. Unlike topical glucocorticoids, systemic glucocorticoids possess a significant side effect profile, including hyperglycemia, hypertension, increased appetite, mood changes, and insomnia, as well as effects on bone metabolism and cataract formation with more chronic exposure. We suggest not using systemic glucocorticoids in the outpatient treatment of acute rhinosinusitis pending the availability of additional data from higher-quality trials. (See "Major side effects of systemic glucocorticoids".) Treatment failure Patients with ABRS are expected to show some response to empiric antimicrobial therapy after three to five days. An alternative treatment strategy is indicated for patients with ABRS who fail to show some improvement in that time frame, or in whom symptoms worsen after at least two to three days of therapy. Experimental evidence indicates bacterial eradication by day three [37,38] and studies have correlated clinical and bacteriologic response [39]. Although older adults or those with multiple morbidities may take longer to resolve infection, such individuals should also show some symptom improvement within five days of initiating antimicrobial therapy for ABRS [9]. Reasons for treatment failure include resistant pathogens, inadequate dosing, structural abnormalities, or a noninfectious etiology. Patients who fail first-line therapy require alternative antibiotic selection. Ideally, an endoscopically-guided culture could be performed to redirect antibiotic therapy, although this is often impractical. Options for second-line therapy provide a broader spectrum of activity and/or a different class of agent. Guidelines from the IDSA recommend the following options for empiric second-line treatment. If improvement is seen within 3 to 5 days of initiation of therapy, a total course duration of 7 to 10 days is recommended: Amoxicillin-clavulanate 2000 mg/125 mg orally twice daily Levofloxacin 500 mg orally once daily Moxifloxacin 400 mg orally once daily Patients with severe infection requiring hospitalization could be treated with one of the following: a respiratory fluoroquinolone (levofloxacin ormoxifloxacin in doses above, either orally or intravenously) or intravenousampicillin-sulbactam 1.5 to 3.0 g every six hours, ceftriaxone 1 to 2 g every 24 hours, or cefotaxime 2 g every four to six hours. Although specific recommendations from the IDSA are not available, we suggest that intravenous antibiotics be given until there is
8 clear evidence of patient response, at which time the patient could be discharged on an oral antibiotic with similar activity to complete a 10-day course. If there is no response to intravenous antibiotics within 48 hours of hospitalization, a CT scan should be performed to verify the diagnosis and to evaluate for suppurative complications (eg, orbital cellulitis, intracranial abscess) and an ENT consultation requested to obtain sinus cultures and for consideration of the need for surgical intervention. A CT scan of the sinuses is indicated if symptoms worsen or fail to improve. For patients who have failed to respond to both first- and second-line therapy, sinus cultures should be obtained either by direct aspirate or endoscopy of the middle meatus; nasopharyngeal cultures are not reliable. Relapse after treatment Recurrence of symptoms within two weeks of response to initial treatment usually represents inadequate eradication of infection. Patients who had a good response to initial therapy and who have mild symptoms of relapse can be treated with a longer course of the same antibiotic. Patients who had only minimal symptom response with the initial antibiotic or whose relapse is moderate to severe, however, are more likely to have organisms resistant to the initial empiric antibiotic and would require a change in the drug selected. The recommended duration of antibiotic treatment for relapse has not been addressed by published guidelines. The treatment duration should be guided by the goal of full resolution of symptoms. If symptoms persist despite a repeat 7- to 10-day course of antibiotics, referral to an otolaryngologist is warranted. Patients who had only minimal symptom response with the initial antibiotic or whose relapse is moderate to severe, however, are more likely to have organisms resistant to the initial empiric antibiotic and would require a change in the drug selected. (See 'Treatment failure' above.) INDICATIONS FOR SPECIALTY REFERRAL Early referral is essential for patients whose symptoms indicate the need for urgent endoscopy or surgical biopsy, or for diagnostic testing (imaging or immunologic testing) that couldn t be performed where they have initially presented. Such patients include those with severe infection (high persistent fever, orbital edema, severe headache, visual disturbance, altered mental status, or meningeal signs), those in whom fungal sinusitis or granulomatous disease is suspected, and those with nosocomial infection. Patients with identified anatomic defects causing obstruction require referral for surgery. Patients who are immunocompromised or are found to have unusual or resistant pathogens might benefit from consultation with an infectious disease specialist. Additionally, referral is indicated for patients with ABRS who have failed to respond to first- and second-line antimicrobial therapy. The 2012 IDSA guidelines have developed consensus recommendations about indications for less-urgent specialty referral as follows: Multiple recurrent episodes of ABRS (three to four episodes per year) Chronic rhinosinusitis (with or without polyps or asthma) with recurrent exacerbations of ABRS Patients with allergic rhinitis who may be candidates for immunotherapy SURGERY There is no indication for surgery in patients with uncomplicated ABRS. However, surgery may be emergently indicated in patients experiencing extra-sinus complications of ABRS,
9 including orbital abscess, epidural abscess, meningitis, and brain abscess. Surgical debridement is also indicated for the treatment of acute invasive fungal rhinosinusitis, a condition for which mortality rates remain high despite timely debridement and systemic antifungal therapy. (See "Fungal rhinosinusitis".) Indications for surgery in patients with chronic rhinosinusitis are discussed separately. (See "Management of chronic rhinosinusitis", section on 'Indications for surgery'.) INFORMATION FOR PATIENTS UpToDate offers two types of patient education materials, The Basics and Beyond the Basics. The Basics patient education pieces are written in plain language, at the 5 th to 6 th grade reading level, and they answer the four or five key questions a patient might have about a given condition. These articles are best for patients who want a general overview and who prefer short, easy-to-read materials. Beyond the Basics patient education pieces are longer, more sophisticated, and more detailed. These articles are written at the 10 th to 12 th grade reading level and are best for patients who want in-depth information and are comfortable with some medical jargon. Here are the patient education articles that are relevant to this topic. We encourage you to print or these topics to your patients. (You can also locate patient education articles on a variety of subjects by searching on patient info and the keyword(s) of interest.) Basics topics (see "Patient information: Sinusitis in adults (The Basics)" and "Patient information: What you should know about antibiotics (The Basics)") Beyond the basics topics (see "Patient information: Acute sinusitis (sinus infection) (Beyond the Basics)") SUMMARY AND RECOMMENDATIONS It is generally not possible to distinguish viral from bacterial acute rhinosinusitis (ARS) in the first 10 days of illness. Acute bacterial rhinosinusitis (ABRS) should be suspected in patients presenting with any of the following three features: 1) persistent symptoms or signs of ARS lasting 10 or more days with no clinical improvement; 2) onset with severe symptoms (fever >39 C or 102 F and purulent nasal discharge or facial pain) lasting at least three consecutive days at the beginning of illness; 3) onset with worsening symptoms following a viral upper respiratory infection that lasted five to six days and was initially improving. Management of acute viral rhinosinusitis (AVRS) aims to relieve symptoms of nasal obstruction and rhinorrhea; treatment for ABRS includes antibiotics to eliminate the infection and prevent complications. (See 'Approach to treatment'above.) AVRS is expected to resolve within 10 days; ABRS may also resolve spontaneously within the first 10 days. Patients who present with fewer than 10 days of symptoms, in the absence of high fever or symptoms suggesting complicated illness, should be managed with supportive care. We suggest mild analgesics, saline nasal irrigation, and fluid (Grade 2C). We suggest treatment with intranasal glucocorticoids (Grade 2B). Decongestants may be useful when eustachian tube dysfunction is a factor for patients with AVRS, but are not likely to be helpful for patients with ABRS and have adverse side effects. We suggest not treating symptoms with antihistamines (Grade 2C). (See 'Symptomatic therapy for acute rhinosinusitis'above.)
10 We recommend treatment with an antibiotic for patients whose clinical symptoms meet criteria for ABRS (algorithm 1) (Grade 1B). In light of increasing microbial resistance to antibiotics, we suggest initial empiric treatment with amoxicillin-clavulanate rather than macrolides (clarithromycin or azithromycin), trimethoprim-sulfamethoxazole, or oral secondor third-generation cephalosporins (Grade 2B). For most patients, amoxicillin-clavulanate (either 500mg/125 mg orally three times daily or 875 mg/125 mg orally twice daily) should be given for five to seven days. Doxycycline is a reasonable alternative for first-line therapy and can be used in patients with penicillin allergy. A respiratory fluoroquinolone (levofloxacin or moxifloxacin) is another option for penicillin-allergic patients. (See 'Choice of antibiotic' above and 'Duration for initial treatment' above.) Local and regional histograms of bacterial resistance should be referenced to understand resistance trends in the local community. (See 'Choice of antibiotic' above.) Patients with ABRS are expected to show some response to empiric antimicrobial therapy after three to five days. An alternative treatment strategy is indicated for patients with ABRS who fail to show some improvement in that time frame, or in whom symptoms worsen after at least two to three days of therapy. Options for second-line empiric therapy include highdose amoxicillin-clavulanate (2000 mg/125 mg orally twice daily) or a respiratory fluoroquinolone (levofloxacin 500 mg orally once daily or moxifloxacin 400 mg orally once daily). (See'Treatment failure' above.) Specialty referral on an urgent basis is indicated for patients with severe infection (high persistent fever, orbital edema, severe headache, visual disturbance, altered mental status, or meningeal signs), those in whom fungal sinusitis or granulomatous disease is suspected, and those with nosocomial infection. Referral is also indicated for patients with obstructive anatomic defects, immunocompromise, resistant pathogens, or failure to respond to first- and second-line antimicrobial therapy. (See 'Indications for specialty referral' above.) There is no indication for surgery in patients with uncomplicated ABRS. However, surgery may be emergently indicated in patients experiencing extra-sinus complications of ABRS, including orbital abscess, epidural abscess, meningitis, and brain abscess. (See'Surgery' above.)
Prefe f rred d t e t rm: : rhi h no n s o inu n s u iti t s
 HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Diagnosis and Treatment of Respiratory Illness in Children and Adults
 Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis
 Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
Update on Rhinosinusitis 2013 AAP Guidelines Review
 Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
ب ه نام خد ا فارماکوویژیالنس و عوارض ناخواسته داروها آذر ماه 1396
 ب ه نام خد ا فارماکوویژیالنس و عوارض ناخواسته داروها آذر ماه 1396 Upper Respiratory Tract Infections Z. Sahraei Pharm. D., Ph.D. Infectious Disease Clinical Pharmacist Rhinosinusitis Definition Acute rhinosinusitis
ب ه نام خد ا فارماکوویژیالنس و عوارض ناخواسته داروها آذر ماه 1396 Upper Respiratory Tract Infections Z. Sahraei Pharm. D., Ph.D. Infectious Disease Clinical Pharmacist Rhinosinusitis Definition Acute rhinosinusitis
Sinusitis & its complication. MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University
 Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
SINUSITIS/RHINOSINUSITIS
 1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Sinusitis/Rhinosinusitis SINUSITIS/RHINOSINUSITIS
 1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
High dose amoxicillin for sinusitis
 High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
Choosing an appropriate antimicrobial agent. 3) the spectrum of potential pathogens
 Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
CLINICAL PRACTICE GUIDELINE
 This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
Acute Bacterial Sinusitis: The latest treatment recommendations. Objectives Having completed the learning activities, the participant will be able to:
 Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief.
 Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
4/7/13 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC
 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
Measure #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
+ Conflict of interest. + Sinus and Nasal Anatomy. + What is your diagnosis? 1) Allergic Rhinitis. 2) Non-Allergic rhinitis. 3) Chronic Rhinosinusitis
 Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
Section Editor Mark D Aronson, MD
 1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
IDSA Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in Children and Adults
 Clinical Infectious Diseases Advance Access published March 20, 2012 IDSA GUIDELINES IDSA Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in Children and Adults Anthony W. Chow, 1 Michael
Clinical Infectious Diseases Advance Access published March 20, 2012 IDSA GUIDELINES IDSA Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in Children and Adults Anthony W. Chow, 1 Michael
27/11/2012. Parainfuenza 1, 2 3 Rhinovirus Coronavirus Adenovirus Respiratory syncytial virus (RSV) Chlamydophila pneumoniae Mycoplasma pneumonite
 8 «Evidence-based Medicine-» 27/11/2012,,,, : :,,,,,,,, (30%-50%) () (5%-10%) (40%-50%) 20% Infuenza A B Parainfuenza 1, 2 3 Rhinovirus Coronavirus Adenovirus Respiratory syncytial virus (RSV) Chlamydophila
8 «Evidence-based Medicine-» 27/11/2012,,,, : :,,,,,,,, (30%-50%) () (5%-10%) (40%-50%) 20% Infuenza A B Parainfuenza 1, 2 3 Rhinovirus Coronavirus Adenovirus Respiratory syncytial virus (RSV) Chlamydophila
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
MANAGEMENT of BACTERIAL RHINOSINUSITIS
 MANAGEMENT of BACTERIAL RHINOSINUSITIS Jennifer Le, PharmD Assistant Professor of Pharmacy Practice, College of Pharmacy, Western University of Health Sciences Martin S. Lipsky, MD Dean and Professor of
MANAGEMENT of BACTERIAL RHINOSINUSITIS Jennifer Le, PharmD Assistant Professor of Pharmacy Practice, College of Pharmacy, Western University of Health Sciences Martin S. Lipsky, MD Dean and Professor of
Respiratory tract infections. Krzysztof Buczkowski
 Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
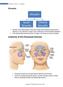 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
Background. Background. AAP (2013) Guidelines. Background 4/19/2016
 Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Maximum Medical Therapy of Chronic Rhinosinusitis. Riyadh Alhedaithy R5 ENT Resident, Combined KSUF and SB. 30/12/2015
 Maximum Medical Therapy of Chronic Rhinosinusitis Riyadh Alhedaithy R5 ENT Resident, Combined KSUF and SB. 30/12/2015 ARTICLE REVIEW INTRODUCTION Chronic rhinosinusitis (CRS) is a common, debilitating,
Maximum Medical Therapy of Chronic Rhinosinusitis Riyadh Alhedaithy R5 ENT Resident, Combined KSUF and SB. 30/12/2015 ARTICLE REVIEW INTRODUCTION Chronic rhinosinusitis (CRS) is a common, debilitating,
Diagnosis and Treatment of Respiratory Illness in Children and Adults Guideline
 Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD)
 Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
PIDS AND RESPIRATORY DISORDERS
 PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
UPPER RESPIRATORY TRACT INFECTIONS. IAP UG Teaching slides
 UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
Quality ID #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
Executive summary of recommendations
 MOH LINIL PRTIE GUIELINES 2/2010 Management of Rhinosinusitis and llergic Rhinitis cademy of Medicine, Singapore hapter of Otorhinolaryngologists ollege of Surgeons, Singapore ollege of Family Physicians,
MOH LINIL PRTIE GUIELINES 2/2010 Management of Rhinosinusitis and llergic Rhinitis cademy of Medicine, Singapore hapter of Otorhinolaryngologists ollege of Surgeons, Singapore ollege of Family Physicians,
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older)
 2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
USAID Health Care Improvement Project. pneumonia) respiratory infections through improved case management (amb/hosp)
 Improvement objective: : decrease morbidity and mortality due to acute upper (rhinitis, sinusitis, pharyngitis) and lower (bronchitis, pneumonia) respiratory infections through improved case management
Improvement objective: : decrease morbidity and mortality due to acute upper (rhinitis, sinusitis, pharyngitis) and lower (bronchitis, pneumonia) respiratory infections through improved case management
Clinical Practice Guideline: Tonsillectomy in Children, Baugh et al Otolaryngology Head and Neck Surgery, 2011 J and: 144 (1 supplement) S1 30.
 Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Pediatric ENT Guidelines Jane Cooper, FNP, CORLN References: Clinical Practice Guideline: Tympanostomy tubes in children, Rosenfeld et al., American Academy of Otolaryngology Head and Neck Surgery Foundation
Sinusitis. Disclosures. What are sinuses? STEVEN E DAVIS, MD. Consultant and speaker, Novartis Research: Intersect ENT
 Sinusitis STEVEN E DAVIS, MD Disclosures Consultant and speaker, Novartis Research: Intersect ENT What are sinuses? Stedman s medical dictionary 25 th edition 1. a channel for the passage of blood or lymph,
Sinusitis STEVEN E DAVIS, MD Disclosures Consultant and speaker, Novartis Research: Intersect ENT What are sinuses? Stedman s medical dictionary 25 th edition 1. a channel for the passage of blood or lymph,
Phototherapy in Allergic Rhinitis
 Phototherapy in Allergic Rhinitis Rhinology Chair KSU KAUH Ibrahim AlAwadh 18\1\2017 MBBS, SB & KSUF Resident, ORL-H&N Background: Endonasal phototherapy can relieve the symptoms of allergic rhinitis
Phototherapy in Allergic Rhinitis Rhinology Chair KSU KAUH Ibrahim AlAwadh 18\1\2017 MBBS, SB & KSUF Resident, ORL-H&N Background: Endonasal phototherapy can relieve the symptoms of allergic rhinitis
Disclaimers. Topical Therapy. The Problem. Topical Therapy for Chronic Rhinosinusitis No Disclosures
 Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
ANTIBIOTICS ACUTE RHINOSINUSITIS IN CHILDREN
 MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
Clinical Practice Guideline: Asthma
 Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Clinical Practice Guideline for the Diagnosis and Management of Acute Bacterial Sinusitis in Children Aged 1 to 18 Years
 Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE Clinical Practice Guideline for the Diagnosis and Management
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children CLINICAL PRACTICE GUIDELINE Clinical Practice Guideline for the Diagnosis and Management
Treatment & Management of Acute Sinusitis in the Primary Care Setting
 University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
Antibiotics, Expectorants, and Cough Suppressants. Center For Cardiac Fitness Pulmonary Rehab The Miriam Hospital
 Antibiotics, Expectorants, and Cough Suppressants Center For Cardiac Fitness Pulmonary Rehab The Miriam Hospital Objectives Review the mechanism of action (MOA), dosing, benefits, and various options for:
Antibiotics, Expectorants, and Cough Suppressants Center For Cardiac Fitness Pulmonary Rehab The Miriam Hospital Objectives Review the mechanism of action (MOA), dosing, benefits, and various options for:
Middleton Chapter 43 (pages ) Rhinosinusitis and Nasal Polyps Prepared by: Malika Gupta, MD
 FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Will sulfamethoxazole treat sinus infection
 Will sulfamethoxazole treat sinus infection Find information about which conditions Sulfamethoxazole- Trimethoprim by a Fungus; Bacterial Infection of Heart Valve; Sinus Irritation and Congestion. Bactrim
Will sulfamethoxazole treat sinus infection Find information about which conditions Sulfamethoxazole- Trimethoprim by a Fungus; Bacterial Infection of Heart Valve; Sinus Irritation and Congestion. Bactrim
Allergy, Asthma & Clinical Immunology 2011, 7:2
 Allergy, Asthma & Clinical Immunology This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Canadian
Allergy, Asthma & Clinical Immunology This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. Canadian
13.2 Elements for a Public Summary
 13.2 Elements for a Public Summary 13.2.1 Overview of disease epidemiology The common cold is one of the most prevalent diseases in humans and is the most common condition for which family doctors are
13.2 Elements for a Public Summary 13.2.1 Overview of disease epidemiology The common cold is one of the most prevalent diseases in humans and is the most common condition for which family doctors are
General Surgery >>>>>[[ sheet # 4]]
![General Surgery >>>>>[[ sheet # 4]] General Surgery >>>>>[[ sheet # 4]]](/thumbs/82/86768776.jpg) General Surgery 11-3-2014 >>>>>[[ sheet # 4]] *Note *: this sheet includes the slides and extra notes >> and what the dr were mentioned are in the bold font Acute Rhinosinusitis Sinusitis commonly used
General Surgery 11-3-2014 >>>>>[[ sheet # 4]] *Note *: this sheet includes the slides and extra notes >> and what the dr were mentioned are in the bold font Acute Rhinosinusitis Sinusitis commonly used
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Corporate Medical Policy Septoplasty
 Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Respiratory Infections
 Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Respiratory System Virology
 Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
Respiratory System Virology Common Cold: Rhinitis. A benign self limited syndrome caused by several families of viruses. The most frequent acute illness in industrialized world. Mild URT illness involving:
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Acute Otitis Media. These podcasts are designed to give medical students an overview of key topics in pediatrics. The
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Acute Otitis Media. These podcasts are designed to give medical students an overview of key topics in pediatrics. The
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 4 January 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 4 January 2012 Examination of the dossier for a medicinal product included for a 5-year period starting on 7 January
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 4 January 2012 Examination of the dossier for a medicinal product included for a 5-year period starting on 7 January
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Infections of the head, neck, and lower respiratory tract
 Infections of the head, neck, and lower respiratory tract Infections of the upper respiratory tract Common 25% bacteria antibiotics 75% viruses Diagnosis on clinical grounds Nonspecific infections of the
Infections of the head, neck, and lower respiratory tract Infections of the upper respiratory tract Common 25% bacteria antibiotics 75% viruses Diagnosis on clinical grounds Nonspecific infections of the
Current Trend in URTI
 Current Trend in URTI Dr Chow Chun Kuen Specialist in Otorhinolaryngology Upper respiratory tract infection Nonspecific Most common cause of physician visits & sick leaves Acute infection of noes, sinuses,
Current Trend in URTI Dr Chow Chun Kuen Specialist in Otorhinolaryngology Upper respiratory tract infection Nonspecific Most common cause of physician visits & sick leaves Acute infection of noes, sinuses,
NECK MASS. Clinical history and examination: Document detail history of mass. Imaging: US or CT of neck
 ENT ENT Referral Referral Guidelines Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment
ENT ENT Referral Referral Guidelines Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment
COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN
 ١ ٢ COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN Dr mostafavi SN Pediatric Infectious Disease Department Isfahan University of Medical Sciences Case 1 ٣ An 18 month old infant brought with high
١ ٢ COMMON UPPER RESPIRATORY TRACT INFECTIONS IN CHILDREN Dr mostafavi SN Pediatric Infectious Disease Department Isfahan University of Medical Sciences Case 1 ٣ An 18 month old infant brought with high
Chronic Rhinosinusitis-Treatment
 Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center
 Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center Kathy Peters is a 63 y.o. patient that presents to your urgent care office today with a history
Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center Kathy Peters is a 63 y.o. patient that presents to your urgent care office today with a history
Objectives. Pneumonia. Pneumonia. Epidemiology. Prevalence 1/7/2012. Community-Acquired Pneumonia in infants and children
 Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
Objectives Community-Acquired in infants and children Review of Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America - 2011 Sabah Charania,
Anatomically, lower respiratory tract is directly connected with the upper one. Ideally, when both specialists manage
 ISSN: 0975-766X CODEN: IJPTFI Available Online through Research Article www.ijptonline.com MANAGEMENT FEATURES OF PATIENT WITH BRONCHIAL ASTHMA AND ACUTE EXACERBATION OF CHRONIC SINUSITIS BY VACUUM DRAINAGE
ISSN: 0975-766X CODEN: IJPTFI Available Online through Research Article www.ijptonline.com MANAGEMENT FEATURES OF PATIENT WITH BRONCHIAL ASTHMA AND ACUTE EXACERBATION OF CHRONIC SINUSITIS BY VACUUM DRAINAGE
Dr Conroy Wong. Professor Richard Beasley. Dr Sarah Mooney. Professor Innes Asher
 Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
A Winter Free of Cold Understanding the Common Cold and Flu. Camille Aizarani, MD Family Medicine Specialist
 A Winter Free of Cold Understanding the Common Cold and Flu Camille Aizarani, MD Family Medicine Specialist Outline Introduction Is it a cold or flu? The Common Cold Symptoms of Common Cold Tansmission
A Winter Free of Cold Understanding the Common Cold and Flu Camille Aizarani, MD Family Medicine Specialist Outline Introduction Is it a cold or flu? The Common Cold Symptoms of Common Cold Tansmission
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
Definition. Otitis Media with effusion (OME)
 Otitis Media. 1 Dr,wegdan saeed ALFHAL 2 Definition Acute Otitis Media (AOM) acute onset of symptoms, evidence of a middle ear effusion, and signs or symptoms of middle ear inflammation. Otitis Media with
Otitis Media. 1 Dr,wegdan saeed ALFHAL 2 Definition Acute Otitis Media (AOM) acute onset of symptoms, evidence of a middle ear effusion, and signs or symptoms of middle ear inflammation. Otitis Media with
Seasonal Allergic Rhinitis (Hay Fever)
 Seasonal Allergic Rhinitis (Hay Fever) Link to prescribing guidance: http://www.enhertsccg.nhs.uk/ear-nose-and-oropharynx Clinical Presentation Link to CKS NICE guidance: https://cks.nice.org.uk/allergicrhinitis
Seasonal Allergic Rhinitis (Hay Fever) Link to prescribing guidance: http://www.enhertsccg.nhs.uk/ear-nose-and-oropharynx Clinical Presentation Link to CKS NICE guidance: https://cks.nice.org.uk/allergicrhinitis
Commen Nose Diseases
 Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
What causes abnormal secretions?
 Post-Nasal Drip Glands in your nose and throat continually produce mucus (one to two quarts a day). Mucus moistens and cleans the nasal membranes, humidifies air, traps and clears inhaled foreign matter,
Post-Nasal Drip Glands in your nose and throat continually produce mucus (one to two quarts a day). Mucus moistens and cleans the nasal membranes, humidifies air, traps and clears inhaled foreign matter,
continuing education for pharmacists
 continuing education for pharmacists Common Cold, Sinusitis, Influenza: The Diseases, Prevention, Treatment Volume XXX, No. 11 Mona T. Thompson, R.Ph., PharmD Dr. Mona T. Thompson has no relevant financial
continuing education for pharmacists Common Cold, Sinusitis, Influenza: The Diseases, Prevention, Treatment Volume XXX, No. 11 Mona T. Thompson, R.Ph., PharmD Dr. Mona T. Thompson has no relevant financial
Management of Common Respiratory Disorders in Children. Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children. Disclosures. Roadmap 6/10/2016
 Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
Management of Common Respiratory Disorders in Children Whitney Pressler, MD Pediatric Brown Bag Series Webinar June 14, 2016 Disclosures I have no financial relationships to disclose I will not be discussing
DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS. Dr. Ziyad Al-Abduljabbar
 DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS Dr. Ziyad Al-Abduljabbar International Forum of Allergy & Rhinology, Vol. 5, No. 9, September 2015 INTRODUCTION
DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS Dr. Ziyad Al-Abduljabbar International Forum of Allergy & Rhinology, Vol. 5, No. 9, September 2015 INTRODUCTION
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o
 A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting]
![Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting] Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting]](/thumbs/83/87318178.jpg) Clinical Pearls Infectious Diseases Pritish K. Tosh, MD MN ACP Nov 7, 2014 [Answers and discussion slides will be posted after the meeting] Case 1 A 33-year-old male with diffuse large B-cell lymphoma
Clinical Pearls Infectious Diseases Pritish K. Tosh, MD MN ACP Nov 7, 2014 [Answers and discussion slides will be posted after the meeting] Case 1 A 33-year-old male with diffuse large B-cell lymphoma
This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy.
 This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/92131/
This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/92131/
The child with a troublesome cough. Dr Marco Zampoli Paediatric Pulmonology Red Cross War Memorial Children s Hospital GP Refresher Course 2012
 The child with a troublesome cough Dr Marco Zampoli Paediatric Pulmonology Red Cross War Memorial Children s Hospital GP Refresher Course 2012 Cough is the most common symptom in children Inability to
The child with a troublesome cough Dr Marco Zampoli Paediatric Pulmonology Red Cross War Memorial Children s Hospital GP Refresher Course 2012 Cough is the most common symptom in children Inability to
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
ENT Referral Guidelines
 ENT Referral Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment of patients with cancerous
ENT Referral Guidelines Austin Health ENT Clinic holds fortnightly multidisciplinary meetings with Plastics/ Maxillary Facial and Oncology units to discuss and plan the treatment of patients with cancerous
Chronic obstructive pulmonary disease (acute exacerbation): antimicrobial prescribing
 National Institute for Health and Care Excellence Final Chronic obstructive pulmonary disease (acute exacerbation): antimicrobial prescribing Evidence review December 2018 Contents Disclaimer The recommendations
National Institute for Health and Care Excellence Final Chronic obstructive pulmonary disease (acute exacerbation): antimicrobial prescribing Evidence review December 2018 Contents Disclaimer The recommendations
Sinus Surgery. Middle Meatus
 Sinus Surgery Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus surgery is also yours. This
Sinus Surgery Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus surgery is also yours. This
NOVEMBER 2016 DRUG ANTIBIOTICS ACUTE RHINOSINUSITIS IN ADULTS
 NOVEMBER 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
NOVEMBER 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
AMERICAN ACADEMY OF PEDIATRICS. Clinical Practice Guideline: Management of Sinusitis
 AMERICAN ACADEMY OF PEDIATRICS Subcommittee on Management of Sinusitis and Committee on Quality Improvement Clinical Practice Guideline: Management of Sinusitis ABSTRACT. This clinical practice guideline
AMERICAN ACADEMY OF PEDIATRICS Subcommittee on Management of Sinusitis and Committee on Quality Improvement Clinical Practice Guideline: Management of Sinusitis ABSTRACT. This clinical practice guideline
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
