Arterial calcification frequently accompanies cardiovascular
|
|
|
- Britton Parker
- 5 years ago
- Views:
Transcription
1 Increased Vascular Calcification in Patients Receiving Warfarin Ekamol Tantisattamo, Kum Hyun Han, W. Charles O Neill Objective Matrix gla protein is a vitamin K dependent inhibitor of medial arterial calcification whose synthesis and activity are blocked by warfarin. Warfarin induces arterial calcification in experimental models, but whether this occurs in humans is unclear. This was addressed by examining breast arterial calcification, which is exclusively medial and easily identified on mammograms. Approach and Results Screening mammograms from women with current, past, or future warfarin use were examined for the presence of arterial calcification and compared with mammograms obtained in untreated women matched for age and diabetes mellitus. Women with a serum creatinine >2.0 mg/dl or a history of end-stage renal disease were excluded. In 451 women with mammograms performed after 1 month of warfarin therapy, the prevalence of arterial calcification was 50% greater than in 451 untreated women (39.0% versus 25.9%; P<0.0001). However, in 159 mammograms performed before warfarin therapy, the prevalence of arterial calcification was not increased (26.4% versus 25.8%). The increased prevalence varied with duration of treatment, from 25.0% for <1 year to 74.4% for >5 years. In a multivariable logistic model, only age and duration of warfarin, but not the period of time after stopping warfarin, were significant determinants of arterial calcification in women with current or past warfarin use. Conclusions The prevalence of breast arterial calcification is increased in women with current or past warfarin use independent of other risk factors and conditions predating warfarin use. This effect appears to be cumulative and may be irreversible. (Arterioscler Thromb Vasc Biol. 2015;35: DOI: /ATVBAHA ) Key Words: anticoagulation matrix proteins vascular calcification Arterial calcification frequently accompanies cardiovascular disease and portends poorer outcomes. 1 4 Calcification occurs either within atherosclerotic plaques (neointimal calcification) or within the muscular layer unrelated to atheromatous disease (medial calcification). While neointimal calcification may merely be a marker of atherosclerotic burden, medial calcification seems to be directly pathogenic by decreasing vascular compliance. 5,6 The medial form is associated with advanced age, diabetes mellitus, advanced chronic kidney disease, and rare genetic disorders. 7 See accompanying editorial on page 9 The pathophysiology of arterial calcification is complex and involves factors that either promote or inhibit the process. One key inhibitor is matrix gla protein (MGP), a vitamin K dependent protein synthesized by vascular smooth muscle. 8 Absence of MGP leads to extensive and fatal medial calcification in mice 9 and is also associated with arterial calcification in humans. 10,11 Warfarin reduces γ-carboxylation of vascular MGP 8 and induces medial arterial calcification in rats both ex vivo and in vivo. 8,12 Whether warfarin also promotes atherosclerotic calcification is unknown. The role of MGP has led to concern that warfarin therapy may increase vascular calcification, but studies to date have been small or limited to specific populations and have yielded conflicting results Furthermore, the imaging used does not distinguish between medial and atherosclerotic calcification, and the abundance of atherosclerotic calcification at the sites studied could obscure effects on medial calcification. The results were also not fully controlled for effects of underlying cardiovascular disease that is often present in patients receiving warfarin. Calcification of breast arteries is exclusively medial, 18,19 easily detected on mammograms, and correlates with arterial calcification in the extremities. 20 Routine screening mammography therefore provides a unique opportunity to examine the effect of warfarin on medial arterial calcification in a large cohort. Materials and Methods Materials and Methods are available in the online-only Data Supplement. Results The computerized search yielded women with screening mammograms, of whom 637 were identified as having received warfarin. Of these, the duration of warfarin was <1 Received on: July 25, 2014; final version accepted on: September 28, From the Renal Division, Department of Medicine, Emory University School of Medicine, Atlanta, GA (E.T., K.H.H., C.O.N.); and Department of Internal Medicine, Inje University College of Medicine, Ilsan Paik Hospital, Goyang, Korea (K.H.H). The online-only Data Supplement is available with this article at Correspondence to W. Charles O Neill, MD, Emory University, Renal Division WMB 338, 1639 Pierce Dr, Atlanta, GA woneill@emory.edu 2014 American Heart Association, Inc. Arterioscler Thromb Vasc Biol is available at DOI: /ATVBAHA
2 238 Arterioscler Thromb Vasc Biol January 2015 Nonstandard Abbreviations and Acronyms BAC MGP breast arterial calcification matrix gla protein month in 100, 38 had a history of end-stage renal disease, 28 had a serum creatinine 2.0, and 20 had no documented warfarin use. The characteristics of the remaining 451 women and the matched controls are shown in Table 1. The use of hydroxymethylglutaryl CoA reductase inhibitors (statins) was twice as prevalent in the warfarin group, probably reflecting the greater prevalence of underlying cardiovascular disease. There were significant, but quantitatively small differences in the serum concentrations of creatinine, calcium, low-density lipoprotein, high-density lipoprotein, and triglycerides that did not fit a particular pattern. In 90% of the patients, the indication for anticoagulation was either atrial fibrillation or deep venous thrombosis with or without pulmonary embolus. Mechanical heart valves (4.7%) and left ventricular thrombus (2.9%) accounted for most of the remainder. Slightly more than half of the patients were receiving warfarin at the time of the mammogram. The remaining 44% had discontinued the warfarin at a mean of 2.7 years before the mammogram with a range of 3 days to 8.5 years. Two separate courses of warfarin were prescribed in 11% of the patients, and the mean interval between treatments was 2.7 years with a maximum of 19 years. Mammograms performed before warfarin therapy were available in 159 women, who were matched to a different set of controls. The characteristics of this group are shown in Table 2. This includes 98 women in the previous cohort who also had mammograms after starting warfarin but with different matched controls because of the differences in age. Serum concentrations of creatinine and phosphorus were slightly higher and high-density lipoprotein slightly lower in the warfarin group. There were no significant differences between the patients with mammograms performed after warfarin therapy (Table 1) and patients with mammograms performed before treatment (Table 2), except for a lower use of statins in the former. Arterial calcification was identified as thin linear opacities along the edges of vessels, and mammograms were scored as positive only if calcification was present on both sides of 1 vessel (Figure 1, top). This calcification is easily distinguished from other forms of calcification (Figure 1, middle and bottom), and in the rare cases of uncertainty, the mammogram was scored as negative. In mammograms performed after initiation of warfarin therapy, the prevalence of arterial calcification was 50% greater than in the control mammograms Table 1. Characteristics of Women With Mammograms Performed After 1 Month of Warfarin Therapy and Untreated Controls Warfarin Untreated P Value n Age, y 68.2±0.6 (36 95) 67.9±0.6 (36 96) 1.00 Diabetes mellitus, % Race, % White Black Other Unknown Serum values, mg/dl Creatinine 0.91±0.01 ( ) 0.86±0.01 ( ) Calcium 9.29±0.03 ( ) 9.39±0.02 ( ) Phosphorus 3.56±0.05 ( ; 277) 3.43±0.06 ( ; 183) LDL cholesterol 98±2 (8 247; 386) 107±2 (15 236; 406) HDL cholesterol 56±1 (19 120; 394) 59±1 (20 126; 409) Triglycerides 124±4 (28 727; 396) 113±3 (27 458; 409) Statin use, % < Indication*, % AF 41.9 DVT/PE 47.5 Other 17.5 Warfarin duration, y ( ) Current therapy, % 56 Range and number of subjects if less than total are given in parentheses. AF indicates atrial fibrillation; DVT, deep venous thrombosis; HDL, high-density lipoprotein; LDL, lowdensity lipoprotein; and PE, pulmonary embolus. *Some patients had >1 indication.
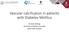
3 Tantisattamo et al Warfarin and Vascular Calcification 239 Table 2. Characteristics of Women With Mammograms Performed Before Initiation of Warfarin Therapy and Untreated Controls (39.0% versus 25.9%; P<0.0001). However, the prevalence of arterial calcification in mammograms performed before warfarin therapy was not increased compared with matched controls (26.4% versus 25.8%) and did not differ from the control group for mammograms performed after warfarin therapy. These data are displayed graphically in Figure 2. The effect of warfarin was dependent on the duration of therapy (Figure 3), with a nonsignificant 25% increase in the prevalence of arterial calcification after <1 year (mean duration, 0.48±0.02), a 67% increase between 1 and 5 years (mean duration, 2.7±0.1), and a 74% increase beyond 5 years (mean duration, 11.4±0.5). In the 20% of patients receiving warfarin for 6 months, the prevalence of arterial calcification was not increased (24% versus 27%). In patients who had discontinued Warfarin Untreated P Value n Age, y (40 88) (40 88) 1.00 Diabetes mellitus, % Race, % White Black Other Unknown Serum values, mg/dl Creatinine ( ) ( ) Calcium ( ) ( ) 0.46 Phosphorus ( ; 84) ( ; 55) 0.04 LDL cholesterol 103±3 (27 322; 136) 108±3 (40 195; 134) 0.24 HDL cholesterol 56±1 (15 100; 137) 59±1 (24 114; 135) Triglycerides 121±6 (28 463; 139) 113±5 (33 485; 135) 0.31 Statin use, % Indication*, % AF 43.4 DVT/PE 47.2 Other 12.6 Years before warfarin ( ) Range and number of subjects if less than total are given in parentheses. AF indicates atrial fibrillation; DVT, deep venous thrombosis; HDL, high-density lipoprotein; LDL, low-density lipoprotein; and PE: pulmonary embolus. *Some patients had >1 indication. warfarin before the mammogram, the prevalence of arterial calcification was still increased compared with the controls (28.8% versus 22.2%), although this was not statistically significant. However, many of these patients had received a short course of warfarin compared with the life-long therapy in most of the subjects receiving warfarin at the time of the mammogram. To determine whether the greater use of a hydroxymethylglutaryl CoA reductase inhibitors in the warfarin-treated patients affected the results, subjects were analyzed separately based on the use of this medication. In the 125 warfarin-treated subjects using statins, the prevalence of breast arterial calcification (BAC) was 46.4% versus 32.0% in the non-warfarin controls matched for age and diabetes mellitus. In the 326 Figure 1. Breast calcification. A, Dual linear calcifications indicative of arterial calcification. Insets, Enlargements of heavy (top) and light (bottom) calcifications. B, Linear calcifications representing calcification of ductal fluid. Inset, Enlargement of calcifications. C, Nonlinear, nonvascular calcifications. Inset, Enlargement of a calcification.
4 240 Arterioscler Thromb Vasc Biol January 2015 Figure 2. Prevalence of breast arterial calcification on mammograms performed during or after warfarin therapy (n=451) and before warfarin therapy (n=159) compared with control patients (no warfarin therapy) matched for age and diabetes mellitus status. *P< vs no warfarin. warfarin-treated subjects not using statins, the prevalence of BAC was 36.2% compared with 23.6% in the non-warfarin controls matched for age and diabetes mellitus. The percent increase in BAC associated with warfarin was similar in each group (45% versus 53%). Subjects using statins were significantly older than those not using statins (73 versus 66). Mammograms performed before and after starting warfarin were available in 98 women, but the duration of warfarin therapy was only 1.05±0.12 years. The prevalence of BAC increased from 28% to 30% because of the development of new BAC in 2 patients, who were treated with warfarin for 4.2 and 5.4 years. Among the 14 patients receiving warfarin for 2 years, this represented an incidence of 14%. Based on the time between mammograms in this group (4.6±0.3 years) and the linear relationship between age and prevalence of BAC after age 50 in all the non-warfarin controls (1.5% per year; data not shown), this is twice the expected incidence. However, the data lack statistical significance because of the small numbers. Figure 4 shows the prevalence of BAC in different groups based on age or diabetes mellitus. Calcification was much less common in women aged <60 years, but the increase associated with warfarin was much greater (400%) compared with women aged 60 years(41%). The increase was also greater Figure 3. Effect of warfarin duration on breast arterial calcification. Control patients (no warfarin therapy) were matched for age and diabetes mellitus status. The number of patients is given in parentheses. *P=0.009; **P= Figure 4. Effect of warfarin on breast arterial calcification based on age and diabetes mellitus compared with control patients (no warfarin therapy) matched for age and diabetes mellitus status. The number of patients is given in parentheses. in non-diabetics compared to diabetics (60% versus 34%). In a logistic model that included age, diabetes mellitus, warfarin duration, and warfarin-free duration, only age and the duration of warfarin therapy were significant determinants of BAC (Table 3). Race, serum creatinine, serum calcium, and statin use were not determinants in either the warfarin subjects or the untreated controls (not shown). Serum lipids showed no significant effect when added to the model. In the simplest model, age (odds ratio, 1.08; P< ), warfarin duration (odds ratio, 1.05; P=0.0057), and atrial fibrillation (odds ratio, 1.73; P=0.023) were significant determinants of BAC. Radiographs of a lower extremity (knee or below) performed within 2 years of the mammogram were available in 248 of the women. Among women with BAC, the prevalence of arterial calcification visible on lower extremity radiographs was 40% compared with only 18% in those without BAC (P=0.0006). The quantity of radiographs was insufficient to analyze the effect of warfarin. Discussion Warfarin use was associated with a 50% greater prevalence of BAC in women undergoing screening mammography. The effect was particularly large in women aged <60 years, who exhibited a 5-fold increase. This association of warfarin with medial arterial calcification is consistent with inhibition of MGP, a vitamin K dependent inhibitor of vascular calcification that is synthesized by vascular smooth muscle 8 and whose action is blocked by warfarin, resulting in arterial calcification ex vivo and in vivo in animals. 8,12 The effect of warfarin could not be explained by other known risk factors for medial arterial calcification because the control subjects were matched for age and diabetes mellitus, and subjects with serum creatinine >2 or a history of end-stage renal disease were excluded. Although serum creatinine was significantly greater in the warfarin subjects, likely reflecting underlying cardiovascular disease, the difference was small and unlikely to have influenced the results. Serum creatinine was not a significant determinant of arterial calcification in either the warfarin group or the control group, and our previous studies have shown only a
5 Tantisattamo et al Warfarin and Vascular Calcification 241 Table 3. Multivariable Logistic Regression Model for Breast Arterial Calcification in Patients Receiving Warfarin Odds Ratio 95% Confidence Interval P Value Age, y < Diabetes mellitus Race (white vs nonwhite) Indication (AF vs non-af) Warfarin duration, y Warfarin-free duration, y Serum creatinine, mg/dl Serum calcium, mg/dl Statin use AF indicates atrial fibrillation. small, nonsignificant increase in BAC in stage 3 chronic kidney disease. 21 Because cardiovascular disease is common in patients requiring anticoagulation, it was important to establish that underlying disease was not responsible for the increased prevalence of BAC. In particular, there is the real possibility that vascular calcification or other ectopic calcification could lead to atrial fibrillation and subsequent warfarin therapy. Although there were some significant differences in serum lipid values between the warfarin and non-warfarin patients, they were small and did not fit an atherosclerotic risk profile. It is possible that the greater use of statins in this group could have influenced these values. Importantly, none of the differences in lipid values showed an effect on BAC in regression models. Statin use was substantially greater in the warfarin group, most likely related to an increased prevalence of cardiovascular disease. Although BAC was more prevalent in those using statins, probably explained by the greater age, statin use did not correlate with calcification. Further evidence that the increased calcification associated with warfarin was not due to underlying cardiovascular disease came from examining mammograms performed before the start of warfarin therapy. Because the vast majority of these were performed within a year before warfarin therapy, they should reflect the underlying state of vascular calcification. The prevalence of arterial calcification in these mammograms was almost identical to that in mammograms from matched controls and to the prevalence in the controls for the mammograms performed after initiation of warfarin. This demonstrates that the increased prevalence associated with warfarin use is not because of patient characteristics that predated warfarin use and is directly related to the anticoagulation. Data on incidence of BAC was available in only a small number of women, most of whom received warfarin for only brief periods. Although not statistically significant, the results show a 2-fold increase in incidence after 2 years of warfarin, consistent with the increase in prevalence found for the corresponding duration of warfarin therapy. The increased prevalence of BAC varied directly with the duration of warfarin therapy, providing further evidence that it is due to the warfarin. Although not significant, the small increase in prevalence seen with durations under 1 year suggests that warfarin might influence calcification within that time frame. Beyond 5 years, the further increase in prevalence was small, despite durations up to 39 years, suggesting that some patients are resistant to the effect of warfarin. Because only prevalence was determined, it is possible that the extent of calcification continued to increase. There was no increase in the prevalence of arterial calcification in patients receiving warfarin for 6 months. This suggests that standard therapy for uncomplicated deep venous thrombosis does not promote vascular calcification. In a substantial number of subjects, warfarin was discontinued before the mammogram, but this period without warfarin did not influence the prevalence of arterial calcification, suggesting that the effect of warfarin persists after therapy and raising the possibility that it is irreversible. Other studies have suggested an effect of warfarin on calcification of coronary 13,15 and femoral 16 arteries, but no significant effect on coronary artery calcification was found in another study. 14 Because these sites exhibit both atherosclerotic and medial calcification, an effect limited to medial calcification may be difficult to discern. An increase in cardiac valve calcification has also been noted in patients receiving warfarin. 15,22 The cohorts in most of these prior studies were small, and although traditional risk factors for underlying cardiovascular disease may have been controlled, additional factors may apply specifically to vascular calcification. Furthermore, because only patients currently receiving warfarin were studied, the effect of past warfarin treatment and potential reversibility were not addressed. Previous data suggest that BAC is a marker of calcification in other arterial beds. It predicts cardiovascular disease in the general population 2,23 and correlates with calcification in peripheral arteries in patients with end-stage renal disease. 20 The correlation with calcification of peripheral arteries in the current data indicates that this is also true in the general population. We have also shown that BAC is strongly associated with critical limb ischemia in end-stage renal disease patients, 24 which is consistent with the finding that calcification of peripheral arteries predicts critical limb ischemia in patients with peripheral arterial disease. 4 An increase in medial calcification may therefore explain the failure of warfarin to improve outcomes in peripheral arterial disease. 25 Furthermore, warfarin use is associated with calciphylaxis, 17 a particularly serious complication of vascular calcification. Although this suggests that the increased BAC with warfarin likely reflects generalized medial calcification and could have clinical consequences, further studies will be required to confirm this. The mechanism by which warfarin increases medial arterial calcification is presumably related to impaired gamma carboxylation of MGP, an important inhibitor of vascular calcification that is synthesized by vascular smooth muscle. 8 Absence of this protein in mice results in severe medial arterial calcification, 9 and calcification is also seen when it is absent in humans. 10,11 The carboxylation of MGP, which is probably required for activity, 26,27 is blocked by warfarin, 8 resulting in arterial calcification in vivo 12 and ex vivo. 8 MGP is a highly insoluble protein that adheres to the vascular matrix. Thus, persistence after synthesis may explain why short courses of warfarin (<6 months) were not associated with increased BAC.
6 242 Arterioscler Thromb Vasc Biol January 2015 Although the results provide strong evidence that warfarin promotes vascular calcification, prospective studies will be required to confirm this. The results of this study are necessarily restricted to women, and although it is likely that the findings can be extrapolated to other arterial beds, this will also need to be confirmed. The inability to quantify BAC limits the sensitivity of the analyses, but it does not diminish the findings. Most likely, the effect of warfarin is underestimated because worsening of existing calcifications would not be recognized in this nonquantitative analysis. An effect of anticoagulation on vascular calcification independent of the mechanism of warfarin action cannot be ruled out by the findings of this study, although there is no precedent for this. Unfortunately, the paucity of warfarinnaïve patients treated with other anticoagulants prevented such an analysis, and future studies will be required to address this issue. None. Disclosures References 1. Budoff MJ, Shaw LJ, Liu ST, Weinstein SR, Mosler TP, Tseng PH, Flores FR, Callister TQ, Raggi P, Berman DS. Long-term prognosis associated with coronary calcification: observations from a registry of 25,253 patients. J Am Coll Cardiol. 2007;49: Kemmeren JM, van Noord PAH, Beijerinck D, Fracheboud J, Banga JD, van der Graaf Y. Arterial calcification found on breast cancer screening mammograms and cardiovascular mortality in women. The DOM project. Am J Epidemiol. 1998; Lehto S, Niskanen L, Suhonen M, Rönnemaa T, Laakso M. Medial artery calcification. A neglected harbinger of cardiovascular complications in non-insulin-dependent diabetes mellitus. Arterioscler Thromb Vasc Biol. 1996;16: Guzman RJ, Brinkley DM, Schumacher PM, Donahue RM, Beavers H, Qin X. Tibial artery calcification as a marker of amputation risk in patients with peripheral arterial disease. J Am Coll Cardiol. 2008;51: Allison MA, Hiatt WR, Hirsch AT, Coll JR, Criqui MH. A high anklebrachial index is associated with increased cardiovascular disease morbidity and lower quality of life. J Am Coll Cardiol. 2008;51: Cecelja M, Chowienczyk P. Role of arterial stiffness in cardiovascular disease. JRSM Cardiovasc Dis. 2012;1:. 7. Lau WL, Ix JH. Clinical detection, risk factors, and cardiovascular consequences of medial arterial calcification: a pattern of vascular injury associated with aberrant mineral metabolism. Semin Nephrol. 2013;33: Lomashvili KA, Wang X, Wallin R, O Neill WC. Matrix Gla protein metabolism in vascular smooth muscle and role in uremic vascular calcification. J Biol Chem. 2011;286: Luo G, Ducy P, McKee MD, Pinero GJ, Loyer E, Behringer RR, Karsenty G. Spontaneous calcification of arteries and cartilage in mice lacking matrix GLA protein. Nature. 1997;386: Meier M, Weng LP, Alexandrakis E, Rüschoff J, Goeckenjan G. Tracheobronchial stenosis in Keutel syndrome. Eur Respir J. 2001;17: Munroe PB, Olgunturk RO, Fryns JP, Van Maldergem L, Ziereisen F, Yuksel B, Gardiner RM, Chung E. Mutations in the gene encoding the human matrix Gla protein cause Keutel syndrome. Nat Genet. 1999;21: Price PA, Faus SA, Williamson MK. Warfarin causes rapid calcification of the elastic lamellae in rat arteries and heart valves. Arterioscler Thromb Vasc Biol. 1998;18: Weijs B, Blaauw Y, Rennenberg RJ, Schurgers LJ, Timmermans CC, Pison L, Nieuwlaat R, Hofstra L, Kroon AA, Wildberger J, Crijns HJ. Patients using vitamin K antagonists show increased levels of coronary calcification: an observational study in low-risk atrial fibrillation patients. Eur Heart J. 2011;32: Villines TC, O Malley PG, Feuerstein IM, Thomas S, Taylor AJ. Does prolonged warfarin exposure potentiate coronary calcification in humans? Results of the warfarin and coronary calcification study. Calcif Tissue Int. 2009;85: Koos R, Mahnken AH, Mühlenbruch G, Brandenburg V, Pflueger B, Wildberger JE, Kühl HP. Relation of oral anticoagulation to cardiac valvular and coronary calcium assessed by multislice spiral computed tomography. Am J Cardiol. 2005;96: Rennenberg RJ, van Varik BJ, Schurgers LJ, Hamulyak K, Ten Cate H, Leiner T, Vermeer C, de Leeuw PW, Kroon AA. Chronic coumarin treatment is associated with increased extracoronary arterial calcification in humans. Blood. 2010;115: Hayashi M, Takamatsu I, Kanno Y, Yoshida T, Abe T, Sato Y; Japanese Calciphylaxis Study Group. A case-control study of calciphylaxis in Japanese end-stage renal disease patients. Nephrol Dial Transplant. 2012;27: Nielsen BB, Holm NV. Calcification in breast arteries. The frequency and severity of arterial calcification in female breast tissue without malignant changes. Acta Pathol Microbiol Immunol Scand A. 1985;93: O Neill WC, Adams AL. Breast arterial calcification in chronic kidney disease: absence of smooth muscle apoptosis and osteogenic transdifferentiation. Kidney Int. 2014;85: Duhn V, D Orsi ET, Johnson S, D Orsi CJ, Adams AL, O Neill WC. Breast arterial calcification: a marker of medial vascular calcification in chronic kidney disease. Clin J Am Soc Nephrol. 2011;6: Hassan NA, D Orsi ET, D Orsi CJ, O Neill WC. The risk for medial arterial calcification in CKD. Clin J Am Soc Nephrol. 2012;7: Koos R, Krueger T, Westenfeld R, Kühl HP, Brandenburg V, Mahnken AH, Stanzel S, Vermeer C, Cranenburg EC, Floege J, Kelm M, Schurgers LJ. Relation of circulating matrix gla-protein and anticoagulation status in patients with aortic valve calcification. Thromb Haemost. 2009;101: Iribarren C, Go AS, Tolstykh I, Sidney S, Johnston SC, Spring DB. Breast vascular calcification and risk of coronary heart disease, stroke, and heart failure. J Womens Health. 2004; Abou-Hassan N, Tantisattamo, E, D Orsi, ET, O Neill WC. The clinical significance of medial arterial calcification in end-stage renal disease [published online ahead of print May 28, 2014]. Kidney Int. doi: /ki Investigators WAVET. Oral anticoagulant and antiplatelet therapy and peripheral arterial disease. N Engl J Med. 2007;357: Romberg RW, Werness PG, Riggs BL, Mann KG. Inhibition of hydroxyapatite crystal growth by bone-specific and other calcium-binding proteins. Biochemistry. 1986;25: Schurgers LJ, Spronk HM, Skepper JN, Hackeng TM, Shanahan CM, Vermeer C, Weissberg PL, Proudfoot D. Post-translational modifications regulate matrix Gla protein function: importance for inhibition of vascular smooth muscle cell calcification. J Thromb Haemost. 2007;5: Significance The association of warfarin with breast arterial calcification strongly suggests that it promotes medial arterial calcification. This is critically important because of the widespread use of this anticoagulant and the fact that many of the patients treated with warfarin either already have underlying cardiovascular disease or are at risk for it.
Arterial calcification is common in cardiovascular disease
 Increased Peripheral Arterial Calcification in Patients Receiving Kum Hyun Han, MD; W. Charles O Neill, MD Background- Matrix Gla protein is a vitamin K dependent inhibitor of vascular calcification. use
Increased Peripheral Arterial Calcification in Patients Receiving Kum Hyun Han, MD; W. Charles O Neill, MD Background- Matrix Gla protein is a vitamin K dependent inhibitor of vascular calcification. use
Stefanos K. Roumeliotis. Department of Nephrology, Medical School Democritus University of Thrace, Alexandroupolis, Greece. Stefanos K.
 Department of Nephrology, Medical School Democritus University of Thrace, Alexandroupolis, Greece Passive, degenerative accumulation process of Ca ++ /P +++ without treatment options Active, complex, condition:
Department of Nephrology, Medical School Democritus University of Thrace, Alexandroupolis, Greece Passive, degenerative accumulation process of Ca ++ /P +++ without treatment options Active, complex, condition:
Review Series Immunodiagnostic Systems Limited. Matrix Gla-Protein Overview
 Matrix Gla-Protein: Overview Review Series Immunodiagnostic Systems Limited 1 Introduction In recent years, the insights into the pathogenesis of Vascular Calcification (VC) have changed significantly.
Matrix Gla-Protein: Overview Review Series Immunodiagnostic Systems Limited 1 Introduction In recent years, the insights into the pathogenesis of Vascular Calcification (VC) have changed significantly.
Matrix Gla protein is associated with coronary artery calcification as assessed by electron-beam computed tomography
 2004 Schattauer GmbH, Stuttgart Cell Signaling and Vessel Remodeling Matrix Gla protein is associated with coronary artery calcification as assessed by electron-beam computed tomography Shuichi Jono 1,Yuji
2004 Schattauer GmbH, Stuttgart Cell Signaling and Vessel Remodeling Matrix Gla protein is associated with coronary artery calcification as assessed by electron-beam computed tomography Shuichi Jono 1,Yuji
Declaration of conflict of interest
 Declaration of conflict of interest Inhibitors of vascular calcification what have we learned from animal models Ralf Westenfeld Department of Cardiology Heinrich-Heine-University Düsseldorf Do you know
Declaration of conflict of interest Inhibitors of vascular calcification what have we learned from animal models Ralf Westenfeld Department of Cardiology Heinrich-Heine-University Düsseldorf Do you know
Vitamin K deficiency in CKD patients: a modifiable risk factor for vascular calcification?
 http://www.kidney-international.org & 2009 International Society of Nephrology deficiency in CKD patients: a modifiable risk factor for vascular calcification? Thilo Krueger 1, Ralf Westenfeld 2, Markus
http://www.kidney-international.org & 2009 International Society of Nephrology deficiency in CKD patients: a modifiable risk factor for vascular calcification? Thilo Krueger 1, Ralf Westenfeld 2, Markus
Vascular calcification in patients with Diabetes Mellitus. Dr Jamie Bellinge University of Western Australia Royal Perth Hospital
 Vascular calcification in patients with Diabetes Mellitus Dr Jamie Bellinge University of Western Australia Royal Perth Hospital Risk of cardiovascular disease Cardiovascular disease; - Stroke - Coronary
Vascular calcification in patients with Diabetes Mellitus Dr Jamie Bellinge University of Western Australia Royal Perth Hospital Risk of cardiovascular disease Cardiovascular disease; - Stroke - Coronary
Declaration of conflict of interest. Nothing to disclose
 Declaration of conflict of interest Nothing to disclose Strategies for prevention and regression of vascular calcification: new treatment options? Leon J Schurgers, PhD Department of Biochemistry Maastricht
Declaration of conflict of interest Nothing to disclose Strategies for prevention and regression of vascular calcification: new treatment options? Leon J Schurgers, PhD Department of Biochemistry Maastricht
Research Article The Impact of Warfarin on Patients with End Stage Renal Disease
 Advances in Vascular Medicine, Article ID 542034, 4 pages http://dx.doi.org/10.1155/2014/542034 Research Article The Impact of Warfarin on Patients with End Stage Renal Disease Anahita Dua, 1 Sapan S.
Advances in Vascular Medicine, Article ID 542034, 4 pages http://dx.doi.org/10.1155/2014/542034 Research Article The Impact of Warfarin on Patients with End Stage Renal Disease Anahita Dua, 1 Sapan S.
Calcium scores and matrix Gla protein levels: association with vitamin K status
 DOI: 10.1111/j.1365-2362.2010.02275.x ORIGINAL ARTICLE Calcium scores and matrix Gla protein levels: association with vitamin K status Roger J. M. W. Rennenberg *, Peter W. de Leeuw *, Alphons G. H. Kessels,
DOI: 10.1111/j.1365-2362.2010.02275.x ORIGINAL ARTICLE Calcium scores and matrix Gla protein levels: association with vitamin K status Roger J. M. W. Rennenberg *, Peter W. de Leeuw *, Alphons G. H. Kessels,
Breast Arterial Calcification: A Marker of Medial Vascular Calcification in Chronic Kidney Disease
 Article Breast Arterial Calcification: A Marker of Medial Vascular Calcification in Chronic Kidney Disease Valerie Duhn,* Ellen T. D Orsi, Samuel Johnson,* Carl J. D Orsi, Amy L. Adams, and W. Charles
Article Breast Arterial Calcification: A Marker of Medial Vascular Calcification in Chronic Kidney Disease Valerie Duhn,* Ellen T. D Orsi, Samuel Johnson,* Carl J. D Orsi, Amy L. Adams, and W. Charles
Breast arterial calcification in chronic kidney disease: absence of smooth muscle apoptosis and osteogenic transdifferentiation
 http://www.kidney-international.org & 2013 International Society of Nephrology see commentary on page 501 Breast arterial calcification in chronic kidney disease: absence of smooth muscle apoptosis and
http://www.kidney-international.org & 2013 International Society of Nephrology see commentary on page 501 Breast arterial calcification in chronic kidney disease: absence of smooth muscle apoptosis and
The Role of Vitamin K in Soft-Tissue Calcification 1
 THEMATIC REVIEW SERIES: VITAMIN K The Role of Vitamin K in Soft-Tissue Calcification 1 Elke Theuwissen,* Egbert Smit, and Cees Vermeer VitaK, Maastricht University, Maastricht, the Netherlands ABSTRACT
THEMATIC REVIEW SERIES: VITAMIN K The Role of Vitamin K in Soft-Tissue Calcification 1 Elke Theuwissen,* Egbert Smit, and Cees Vermeer VitaK, Maastricht University, Maastricht, the Netherlands ABSTRACT
Epicardial coronary artery calcification (CAC) occurs in
 Matrix Gla Protein Is Associated With Risk Factors for Atherosclerosis but not With Coronary Artery Calcification Christopher J. O Donnell, M. Kyla Shea, Paul A. Price, David R. Gagnon, Peter W.F. Wilson,
Matrix Gla Protein Is Associated With Risk Factors for Atherosclerosis but not With Coronary Artery Calcification Christopher J. O Donnell, M. Kyla Shea, Paul A. Price, David R. Gagnon, Peter W.F. Wilson,
Dementia. Inhibition of vascular calcification
 FLEMENGHO Dementia Inhibition of vascular calcification Role of matrix Gla protein Yan-Ping Liu, Fang-Fei Wei, Cees Vermeer, and Jan A. Staessen, Research Unit Hypertension and Cardiovascular Epidemiology,
FLEMENGHO Dementia Inhibition of vascular calcification Role of matrix Gla protein Yan-Ping Liu, Fang-Fei Wei, Cees Vermeer, and Jan A. Staessen, Research Unit Hypertension and Cardiovascular Epidemiology,
Apixaban for Atrial Fibrillation in Patients with End-Stage Renal Disease on Dialysis
 Apixaban for Atrial Fibrillation in Patients with End-Stage Renal Disease on Dialysis Caitlin Reedholm, PharmD PGY1 Pharmacy Resident St. David s South Austin Medical Center November 2, 2018 Abbreviations
Apixaban for Atrial Fibrillation in Patients with End-Stage Renal Disease on Dialysis Caitlin Reedholm, PharmD PGY1 Pharmacy Resident St. David s South Austin Medical Center November 2, 2018 Abbreviations
Condition Congestive heart failure I11.0; I13.0; I13.2; I42.0; I50 CO3C Left ventricular dysfunction I50.1; I50.9 E11 1; E11 9
 Comparative effectiveness and safety of non-vitamin K antagonists oral anticoagulants (OACs) and warfarin in daily clinical practice: A propensity weighted nationwide cohort study. Supplementary material
Comparative effectiveness and safety of non-vitamin K antagonists oral anticoagulants (OACs) and warfarin in daily clinical practice: A propensity weighted nationwide cohort study. Supplementary material
Antithrombotics in Stroke management
 Antithrombotics in Stroke management Faculty: Robert Beveridge Relationships with commercial interests: Grants/Research Support: N/A Speakers Bureau/Honoraria: Astra Zeneca, Bayer, Boerhinger Ingelheim,
Antithrombotics in Stroke management Faculty: Robert Beveridge Relationships with commercial interests: Grants/Research Support: N/A Speakers Bureau/Honoraria: Astra Zeneca, Bayer, Boerhinger Ingelheim,
NEW MK-7 SELECT INTRODUCTION
 NEW MK-7 SELECT INTRODUCTION As we have all known for several years now, the presence of optimal amounts of vitamin D is essential for maintaining optimal bone health and bone calcification, as noted by
NEW MK-7 SELECT INTRODUCTION As we have all known for several years now, the presence of optimal amounts of vitamin D is essential for maintaining optimal bone health and bone calcification, as noted by
Coronary Artery Calcification
 Coronary Artery Calcification Julianna M. Czum, MD OBJECTIVES CORONARY ARTERY CALCIFICATION Julianna M. Czum, MD Dartmouth-Hitchcock Medical Center 1. To review the clinical significance of coronary heart
Coronary Artery Calcification Julianna M. Czum, MD OBJECTIVES CORONARY ARTERY CALCIFICATION Julianna M. Czum, MD Dartmouth-Hitchcock Medical Center 1. To review the clinical significance of coronary heart
Uncarboxylated matrix Gla protein (ucmgp) is associated with coronary artery calcification in haemodialysis patients
 2009 Schattauer GmbH, Stuttgart Cardiovascular Biology and Cell Signalling Uncarboxylated matrix Gla protein (ucmgp) is associated with coronary artery calcification in haemodialysis patients Ellen C.
2009 Schattauer GmbH, Stuttgart Cardiovascular Biology and Cell Signalling Uncarboxylated matrix Gla protein (ucmgp) is associated with coronary artery calcification in haemodialysis patients Ellen C.
Financial Disclosures. Coronary Artery Calcification. Objectives. Coronary Artery Calcium 6/6/2018. Heart Disease Statistics At-a-Glace 2017
 Coronary Artery Calcification Dharmendra A. Patel, MD MPH Director, Echocardiography Laboratory Associate Program Director Cardiovascular Disease Fellowship Program Erlanger Heart and Lung Institute UT
Coronary Artery Calcification Dharmendra A. Patel, MD MPH Director, Echocardiography Laboratory Associate Program Director Cardiovascular Disease Fellowship Program Erlanger Heart and Lung Institute UT
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Olesen JB, Lip GYH, Kamper A-L, et al. Stroke and bleeding
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Olesen JB, Lip GYH, Kamper A-L, et al. Stroke and bleeding
Supplementary Online Content
 Supplementary Online Content Lin Y-S, Chen Y-L, Chen T-H, et al. Comparison of Clinical Outcomes Among Patients With Atrial Fibrillation or Atrial Flutter Stratified by CHA 2 DS 2 -VASc Score. JAMA Netw
Supplementary Online Content Lin Y-S, Chen Y-L, Chen T-H, et al. Comparison of Clinical Outcomes Among Patients With Atrial Fibrillation or Atrial Flutter Stratified by CHA 2 DS 2 -VASc Score. JAMA Netw
Vitamin K intake and calcifications in breast arteries
 CHAPTER 7 Vitamin K intake and calcifications in breast arteries Angela H.E.M. Maas, Yvonne T. van der Schouw David Beijerinck, Jan J.M. Deurenberg, Willem P.Th.M. Mali Diederick E. Grobbee, Yolanda van
CHAPTER 7 Vitamin K intake and calcifications in breast arteries Angela H.E.M. Maas, Yvonne T. van der Schouw David Beijerinck, Jan J.M. Deurenberg, Willem P.Th.M. Mali Diederick E. Grobbee, Yolanda van
Management of Patients with Atrial Fibrillation Undergoing Coronary Artery Stenting 경북대의전원내과조용근
 Management of Patients with Atrial Fibrillation Undergoing Coronary Artery Stenting 경북대의전원내과조용근 Case (2011, 5) 74-years old gentleman Exertional chest pain Warfarin with good INR control Ex-smoker, social(?)
Management of Patients with Atrial Fibrillation Undergoing Coronary Artery Stenting 경북대의전원내과조용근 Case (2011, 5) 74-years old gentleman Exertional chest pain Warfarin with good INR control Ex-smoker, social(?)
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Solomon SD, Uno H, Lewis EF, et al. Erythropoietic response
Chronic Kidney Disease as cardiovascular risk predictor Evidence based clinical management. Fabio Mazza
 Chronic Kidney Disease as cardiovascular risk predictor Evidence based clinical management Fabio Mazza CKD (Chronic Kidney Disease) is an ever-increasing clinical condition marked by a progressive reduction
Chronic Kidney Disease as cardiovascular risk predictor Evidence based clinical management Fabio Mazza CKD (Chronic Kidney Disease) is an ever-increasing clinical condition marked by a progressive reduction
KCS Congress: Impact through collaboration
 Stroke Prevention in Atrial Fibrillation (SPAF) in Kenya Elijah N. Ogola FACC University of Nairobi Kenya Cardiac Society Annual Scientific Congress Mombasa 28 th June 1 st July 2017 KCS Congress: Impact
Stroke Prevention in Atrial Fibrillation (SPAF) in Kenya Elijah N. Ogola FACC University of Nairobi Kenya Cardiac Society Annual Scientific Congress Mombasa 28 th June 1 st July 2017 KCS Congress: Impact
Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis
 ORIGINAL ARTICLE Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis Masaki Ohya 1, Haruhisa Otani 2,KeigoKimura 3, Yasushi Saika 4, Ryoichi Fujii 4, Susumu
ORIGINAL ARTICLE Improved Assessment of Aortic Calcification in Japanese Patients Undergoing Maintenance Hemodialysis Masaki Ohya 1, Haruhisa Otani 2,KeigoKimura 3, Yasushi Saika 4, Ryoichi Fujii 4, Susumu
Supplementary Appendix
 Supplementary Appendix Increased Risk of Atrial Fibrillation and Thromboembolism in Patients with Severe Psoriasis: a Nationwide Population-based Study Tae-Min Rhee, MD 1, Ji Hyun Lee, MD 2, Eue-Keun Choi,
Supplementary Appendix Increased Risk of Atrial Fibrillation and Thromboembolism in Patients with Severe Psoriasis: a Nationwide Population-based Study Tae-Min Rhee, MD 1, Ji Hyun Lee, MD 2, Eue-Keun Choi,
Diabetes and the heart: mechanisms of cardiac injury, hypertension and heart failure. SAGLB.DIA u Date of approval: November 2017
 Diabetes and the heart: mechanisms of cardiac injury, hypertension and heart failure SAGLB.DIA.17.08.0968u Date of approval: November 2017 Abbreviations ACS: acute coronary syndrome AGE: advanced glycoxidation
Diabetes and the heart: mechanisms of cardiac injury, hypertension and heart failure SAGLB.DIA.17.08.0968u Date of approval: November 2017 Abbreviations ACS: acute coronary syndrome AGE: advanced glycoxidation
LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC
![LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC LDL cholesterol (p = 0.40). However, higher levels of HDL cholesterol (> or =1.5 mmol/l [60 mg/dl]) were associated with less progression of CAC](/thumbs/88/116891773.jpg) Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
Am J Cardiol (2004);94:729-32 Relation of degree of physical activity to coronary artery calcium score in asymptomatic individuals with multiple metabolic risk factors M. Y. Desai, et al. Ciccarone Preventive
Chapter 4: Cardiovascular Disease in Patients with CKD
 Chapter 4: Cardiovascular Disease in Patients with CKD The prevalence of cardiovascular disease (CVD) was 65.8% among patients aged 66 and older who had chronic kidney disease (CKD), compared to 31.9%
Chapter 4: Cardiovascular Disease in Patients with CKD The prevalence of cardiovascular disease (CVD) was 65.8% among patients aged 66 and older who had chronic kidney disease (CKD), compared to 31.9%
Effects of Kidney Disease on Cardiovascular Morbidity and Mortality
 Effects of Kidney Disease on Cardiovascular Morbidity and Mortality Joachim H. Ix, MD, MAS Assistant Professor in Residence Division of Nephrology University of California San Diego, and Veterans Affairs
Effects of Kidney Disease on Cardiovascular Morbidity and Mortality Joachim H. Ix, MD, MAS Assistant Professor in Residence Division of Nephrology University of California San Diego, and Veterans Affairs
Cardiovascular Mortality: General Population vs ESRD Dialysis Patients
 Cardiovascular Mortality: General Population vs ESRD Dialysis Patients Annual CVD Mortality (%) 100 10 1 0.1 0.01 0.001 25-34 35-44 45-54 55-64 66-74 75-84 >85 Age (years) GP Male GP Female GP Black GP
Cardiovascular Mortality: General Population vs ESRD Dialysis Patients Annual CVD Mortality (%) 100 10 1 0.1 0.01 0.001 25-34 35-44 45-54 55-64 66-74 75-84 >85 Age (years) GP Male GP Female GP Black GP
Circulating matrix Gla protein in patients with vascular pathology
 Human & Veterinary Medicine International Journal of the Bioflux Society OPEN ACCESS Research Article Circulating matrix Gla protein in patients with vascular pathology 1 Ciprian N. Silaghi, 1 Simona R.
Human & Veterinary Medicine International Journal of the Bioflux Society OPEN ACCESS Research Article Circulating matrix Gla protein in patients with vascular pathology 1 Ciprian N. Silaghi, 1 Simona R.
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
MODULE 1: Stroke Prevention in Atrial Fibrillation Benjamin Bell, MD, FRCPC
 MODULE 1: Stroke Prevention in Atrial Fibrillation Benjamin Bell, MD, FRCPC Specialty: General Internal Medicine Lecturer, Department of Medicine University of Toronto Staff Physician, General Internal
MODULE 1: Stroke Prevention in Atrial Fibrillation Benjamin Bell, MD, FRCPC Specialty: General Internal Medicine Lecturer, Department of Medicine University of Toronto Staff Physician, General Internal
Ischemic Heart and Cerebrovascular Disease. Harold E. Lebovitz, MD, FACE Kathmandu November 2010
 Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Impact of menaquinone-4 supplementation on coronary artery calcification and arterial stiffness: an open label single arm study
 Ikari et al. Nutrition Journal (2016) 15:53 DOI 10.1186/s12937-016-0175-8 RESEARCH Open Access Impact of menaquinone-4 supplementation on coronary artery calcification and arterial stiffness: an open label
Ikari et al. Nutrition Journal (2016) 15:53 DOI 10.1186/s12937-016-0175-8 RESEARCH Open Access Impact of menaquinone-4 supplementation on coronary artery calcification and arterial stiffness: an open label
CLINICAL OUTCOME Vs SURROGATE MARKER
 CLINICAL OUTCOME Vs SURROGATE MARKER Statin Real Experience Dr. Mostafa Sherif Senior Medical Manager Pfizer Egypt & Sudan Objective Difference between Clinical outcome and surrogate marker Proper Clinical
CLINICAL OUTCOME Vs SURROGATE MARKER Statin Real Experience Dr. Mostafa Sherif Senior Medical Manager Pfizer Egypt & Sudan Objective Difference between Clinical outcome and surrogate marker Proper Clinical
Updates in Anticoagulation for Atrial Fibrillation and Venous Thromboembolism
 Disclosures Updates in Anticoagulation for Atrial Fibrillation and Venous Thromboembolism No financial conflicts of interest Member of the ABIM Focused- Practice in Hospital Medicine Self Examination Process
Disclosures Updates in Anticoagulation for Atrial Fibrillation and Venous Thromboembolism No financial conflicts of interest Member of the ABIM Focused- Practice in Hospital Medicine Self Examination Process
For unclear reasons, only about 40% of patients with calcific aortic stenosis also have coronary
 Αθηροσκλήρωση και ασβεστοποιός στένωση της αορτικής βαλβίδας. Οµοιότητες και διαφορές Ν. Μεζίλης Κλινική «Άγιος Λουκάς» Ασβεστοποιός στένωση της αορτικής βαλβίδας: Μία ακόµα µορφή αθηρωµάτωσης; Some observations
Αθηροσκλήρωση και ασβεστοποιός στένωση της αορτικής βαλβίδας. Οµοιότητες και διαφορές Ν. Μεζίλης Κλινική «Άγιος Λουκάς» Ασβεστοποιός στένωση της αορτικής βαλβίδας: Μία ακόµα µορφή αθηρωµάτωσης; Some observations
Case Study: Chris Arden. Peripheral Arterial Disease
 Case Study: Chris Arden Peripheral Arterial Disease Patient Presentation Diane is a 65-year-old retired school teacher She complains of left calf pain when walking 50 metres; the pain goes away after she
Case Study: Chris Arden Peripheral Arterial Disease Patient Presentation Diane is a 65-year-old retired school teacher She complains of left calf pain when walking 50 metres; the pain goes away after she
In Whom and When Should Atrial Fibrillation Ablation be Considered?
 In Whom and When Should Atrial Fibrillation Ablation be Considered? Christian de Chillou, MD, PhD Department of Cardiology University Hospital Nancy, France ESC 2010 Stockholm, August 30. 2010 2 In Whom?
In Whom and When Should Atrial Fibrillation Ablation be Considered? Christian de Chillou, MD, PhD Department of Cardiology University Hospital Nancy, France ESC 2010 Stockholm, August 30. 2010 2 In Whom?
Left Atrial Appendage Closure Devices. Atrial Fibrillation 10/11/2017
 Left Atrial Appendage Closure Devices Emile Daoud, MD Chief, Cardiac Electrophysiology Wexner Medical Center, The Ohio State University Atrial Fibrillation 1 Adjusted Annual Stroke Risk Using CHA 2 DS
Left Atrial Appendage Closure Devices Emile Daoud, MD Chief, Cardiac Electrophysiology Wexner Medical Center, The Ohio State University Atrial Fibrillation 1 Adjusted Annual Stroke Risk Using CHA 2 DS
Dual Antiplatelet Therapy Made Practical
 Dual Antiplatelet Therapy Made Practical David Parra, Pharm.D., FCCP, BCPS Clinical Pharmacy Program Manager in Cardiology/Anticoagulation VISN 8 Pharmacy Benefits Management Clinical Associate Professor
Dual Antiplatelet Therapy Made Practical David Parra, Pharm.D., FCCP, BCPS Clinical Pharmacy Program Manager in Cardiology/Anticoagulation VISN 8 Pharmacy Benefits Management Clinical Associate Professor
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL 1 Supplemental Table 1. ICD codes Diagnoses, surgical procedures, and pharmacotherapy used for defining the study population, comorbidity, and outcomes Study population Atrial fibrillation
SUPPLEMENTAL MATERIAL 1 Supplemental Table 1. ICD codes Diagnoses, surgical procedures, and pharmacotherapy used for defining the study population, comorbidity, and outcomes Study population Atrial fibrillation
Lipid Management 2013 Statin Benefit Groups
 Clinical Integration Steering Committee Clinical Integration Chronic Disease Management Work Group Lipid Management 2013 Statin Benefit Groups Approved by Board Chair Signature Name (Please Print) Date
Clinical Integration Steering Committee Clinical Integration Chronic Disease Management Work Group Lipid Management 2013 Statin Benefit Groups Approved by Board Chair Signature Name (Please Print) Date
Anticoagulation, atrial fibrillation in elderly patients with chronic kidney disease
 Anticoagulation, atrial fibrillation in elderly patients with chronic kidney disease Zbigniew Heleniak M.D. Ph.D. Department of Nephrology, Transplantology and Internal Medicine Medical University of Gdansk
Anticoagulation, atrial fibrillation in elderly patients with chronic kidney disease Zbigniew Heleniak M.D. Ph.D. Department of Nephrology, Transplantology and Internal Medicine Medical University of Gdansk
Bone Markers and Vascular Calcification in CKD-MBD
 Bone Markers and Vascular Calcification in CKD-MBD Pierre Delanaye, MD, PhD Department of Nephrology, Dialysis, Transplantation CHU Sart Tilman University of Liège BELGIUM Bone Markers and Vascular Calcification
Bone Markers and Vascular Calcification in CKD-MBD Pierre Delanaye, MD, PhD Department of Nephrology, Dialysis, Transplantation CHU Sart Tilman University of Liège BELGIUM Bone Markers and Vascular Calcification
Evaluate Risk of Stroke & Bleeding in AF Patients
 XV World Congress of Arrhythmias, Beijing, China - 17-20 September, 2015 Evaluate Risk of Stroke & Bleeding in AF Patients Antonio Raviele, MD, FESC, FHRS President ALFA Alliance to Fight Atrial fibrillation
XV World Congress of Arrhythmias, Beijing, China - 17-20 September, 2015 Evaluate Risk of Stroke & Bleeding in AF Patients Antonio Raviele, MD, FESC, FHRS President ALFA Alliance to Fight Atrial fibrillation
Bayer submits application for marketing approval of rivaroxaban for patients with coronary or peripheral artery disease to European Medicines Agency
 Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Bayer submits application for marketing approval of rivaroxaban for patients
Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Bayer submits application for marketing approval of rivaroxaban for patients
Update on Lipid Management in Cardiovascular Disease: How to Understand and Implement the New ACC/AHA Guidelines
 Update on Lipid Management in Cardiovascular Disease: How to Understand and Implement the New ACC/AHA Guidelines Paul Mahoney, MD Sentara Cardiology Specialists Lipid Management in Cardiovascular Disease
Update on Lipid Management in Cardiovascular Disease: How to Understand and Implement the New ACC/AHA Guidelines Paul Mahoney, MD Sentara Cardiology Specialists Lipid Management in Cardiovascular Disease
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK?
 VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
Bayer s rivaroxaban submitted to U.S. FDA for approval in patients with coronary and/or peripheral artery disease
 Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Bayer s rivaroxaban submitted to U.S. FDA for approval in patients with coronary
Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Bayer s rivaroxaban submitted to U.S. FDA for approval in patients with coronary
Chapter 1 Introduction
 Chapter 1 Introduction There are several disorders which carry an increased risk of thrombosis, clots that interfere with normal circulation, including: venous thromboembolism (VTE), comprising both deep
Chapter 1 Introduction There are several disorders which carry an increased risk of thrombosis, clots that interfere with normal circulation, including: venous thromboembolism (VTE), comprising both deep
Supplementary Online Content
 Supplementary Online Content Inohara T, Xian Y, Liang L, et al. Association of intracerebral hemorrhage among patients taking non vitamin K antagonist vs vitamin K antagonist oral anticoagulants with in-hospital
Supplementary Online Content Inohara T, Xian Y, Liang L, et al. Association of intracerebral hemorrhage among patients taking non vitamin K antagonist vs vitamin K antagonist oral anticoagulants with in-hospital
Do Not Cite. Draft for Work Group Review.
 Defect Free Acute Inpatient Ischemic Stroke Measure Bundle Measure Description Percentage of patients aged 18 years and older with a diagnosis of ischemic stroke OR transient ischemic attack who were admitted
Defect Free Acute Inpatient Ischemic Stroke Measure Bundle Measure Description Percentage of patients aged 18 years and older with a diagnosis of ischemic stroke OR transient ischemic attack who were admitted
Results from RE-COVER RE-COVER II RE-MEDY RE-SONATE EXECUTIVE SUMMARY
 Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
Assessment of the safety and efficacy of dabigatran etexilate (Pradaxa ) in the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) and the prevention of recurrent DVT and PE Results from
Disclosures. Diabetes and Cardiovascular Risk Management. Learning Objectives. Atherosclerotic Cardiovascular Disease
 Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
The Changing Landscape of Managing Patients with PAD- Update on the Evidence and Practice of Care in Patients with Peripheral Artery Disease
 Interventional Cardiology and Cath Labs The Changing Landscape of Managing Patients with PAD- Update on the Evidence and Practice of Care in Patients with Peripheral Artery Disease Manesh R. Patel MD Chief,
Interventional Cardiology and Cath Labs The Changing Landscape of Managing Patients with PAD- Update on the Evidence and Practice of Care in Patients with Peripheral Artery Disease Manesh R. Patel MD Chief,
 1. Prevalence and prognostic significance of incidental cardiac troponin T elevation in ambulatory patients with stable coronary artery disease: data from the Heart and Soul study Hsieh, B.P., et al. Am
1. Prevalence and prognostic significance of incidental cardiac troponin T elevation in ambulatory patients with stable coronary artery disease: data from the Heart and Soul study Hsieh, B.P., et al. Am
6 th ACC-SHA Joint Meeting Jeddah, Saudi Arabia
 6 th ACC-SHA Joint Meeting Jeddah, Saudi Arabia October 31 st - November 1 st, 2015 NOACS vs. Coumadin in Atrial Fibrillation: Is It Worth to Switch? Raed Sweidan, MD, FACC Consultant and Head of Cardiac
6 th ACC-SHA Joint Meeting Jeddah, Saudi Arabia October 31 st - November 1 st, 2015 NOACS vs. Coumadin in Atrial Fibrillation: Is It Worth to Switch? Raed Sweidan, MD, FACC Consultant and Head of Cardiac
3/23/2017. Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate Europace Oct;14(10): Epub 2012 Aug 24.
 Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Arteriosclerosis & Atherosclerosis
 Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017
 Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Angelika Cyganska, PharmD Austin T. Wilson, MS, PharmD Candidate 2017 Explain the efficacy and safety of triple therapy, in regards to thromboembolic and bleeding risk Summarize the guideline recommendations
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
RAPID Phase III Perspectives from the Medical Device Industry
 RAPID Phase III Perspectives from the Medical Device Industry Megan M. Brandt Vice President, Quality and Regulatory Affairs Cardiovascular Systems, Inc. St. Paul, MN PAD and Critical Limb Ischemia: Disease
RAPID Phase III Perspectives from the Medical Device Industry Megan M. Brandt Vice President, Quality and Regulatory Affairs Cardiovascular Systems, Inc. St. Paul, MN PAD and Critical Limb Ischemia: Disease
Familial hypercholesterolaemia in children and adolescents
 Familial hypercholesterolaemia in children and adolescents Rationale and recommendations for early identification and treatment European Atherosclerosis Society Consensus Panel Slide deck adapted from:
Familial hypercholesterolaemia in children and adolescents Rationale and recommendations for early identification and treatment European Atherosclerosis Society Consensus Panel Slide deck adapted from:
SUPPLEMENTAL MATERIALS
 SUPPLEMENTAL MATERIALS Table S1: Variables included in the propensity-score matching Table S1.1: Components of the CHA 2DS 2Vasc score Table S2: Crude event rates in the compared AF patient cohorts Table
SUPPLEMENTAL MATERIALS Table S1: Variables included in the propensity-score matching Table S1.1: Components of the CHA 2DS 2Vasc score Table S2: Crude event rates in the compared AF patient cohorts Table
Coronary Artery Calcium to Predict All-Cause Mortality in Elderly Men and Women
 Journal of the American College of Cardiology Vol. 52, No. 1, 28 28 by the American College of Cardiology Foundation ISSN 735-197/8/$34. Published by Elsevier Inc. doi:1.116/j.jacc.28.4.4 CLINICAL RESEARCH
Journal of the American College of Cardiology Vol. 52, No. 1, 28 28 by the American College of Cardiology Foundation ISSN 735-197/8/$34. Published by Elsevier Inc. doi:1.116/j.jacc.28.4.4 CLINICAL RESEARCH
Supplementary Online Content
 Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
Supplementary Online Content Kavousi M, Leening MJG, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines
New Guidelines in Dyslipidemia Management
 The Fourth IAS-OSLA Course on Lipid Metabolism and Cardiovascular Risk Muscat, Oman, February 2018 New Guidelines in Dyslipidemia Management Dr. Khalid Al-Waili, MD, FRCPC, DABCL Senior Consultant Medical
The Fourth IAS-OSLA Course on Lipid Metabolism and Cardiovascular Risk Muscat, Oman, February 2018 New Guidelines in Dyslipidemia Management Dr. Khalid Al-Waili, MD, FRCPC, DABCL Senior Consultant Medical
A: Epidemiology update. Evidence that LDL-C and CRP identify different high-risk groups
 A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
A: Epidemiology update Evidence that LDL-C and CRP identify different high-risk groups Women (n = 27,939; mean age 54.7 years) who were free of symptomatic cardiovascular (CV) disease at baseline were
Chapter 4: Cardiovascular Disease in Patients With CKD
 Chapter 4: Cardiovascular Disease in Patients With CKD The prevalence of cardiovascular disease is 68.8% among patients aged 66 and older who have CKD, compared to 34.1% among those who do not have CKD
Chapter 4: Cardiovascular Disease in Patients With CKD The prevalence of cardiovascular disease is 68.8% among patients aged 66 and older who have CKD, compared to 34.1% among those who do not have CKD
Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance
 CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
Stratificazione del rischio, corretto bilancio tra ischemia e bleeding: il beneficio clinico netto
 Fibrillazione atriale: rischio tromboembolico, Venezia - 27/28 Novembre 2015 Stratificazione del rischio, corretto bilancio tra ischemia e bleeding: il beneficio clinico netto Antonio Raviele, MD, FESC,
Fibrillazione atriale: rischio tromboembolico, Venezia - 27/28 Novembre 2015 Stratificazione del rischio, corretto bilancio tra ischemia e bleeding: il beneficio clinico netto Antonio Raviele, MD, FESC,
Combining Coronary Artery Calcium Scanning with SPECT/PET Myocardial Perfusion Imaging
 Combining Coronary Artery Calcium Scanning with SPECT/PET Myocardial Perfusion Imaging Daniel S. Berman, MD Director, Cardiac Imaging Cedars-Sinai Heart Institute Professor of Medicine and Imaging Cedars-Sinai
Combining Coronary Artery Calcium Scanning with SPECT/PET Myocardial Perfusion Imaging Daniel S. Berman, MD Director, Cardiac Imaging Cedars-Sinai Heart Institute Professor of Medicine and Imaging Cedars-Sinai
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients. David Liff MD Oklahoma Heart Institute Vascular Center
 DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
Cardiac Ischemia (is-kē-mē-uh)
 Chapter 21 Cardiac Ischemia (is-kē-mē-uh) By: Alejandra & Lindsay I. Cardiac Ischemia =the most common cause of death in Western Culture ~35% of deaths. -Suddenly from acute coronary occlusion or fibrillation
Chapter 21 Cardiac Ischemia (is-kē-mē-uh) By: Alejandra & Lindsay I. Cardiac Ischemia =the most common cause of death in Western Culture ~35% of deaths. -Suddenly from acute coronary occlusion or fibrillation
Manuel Castellá Cardiovascular Surgery Hospital Clínic, Universidad de
 When not to exclude the LAA Manuel Castellá Cardiovascular Surgery Hospital Clínic, Universidad de Barcelona mcaste@clinic.ub.es @mcastellamd Normal hearts Patient in sinus rhythm Patient in AF (with
When not to exclude the LAA Manuel Castellá Cardiovascular Surgery Hospital Clínic, Universidad de Barcelona mcaste@clinic.ub.es @mcastellamd Normal hearts Patient in sinus rhythm Patient in AF (with
Asif Serajian DO FACC FSCAI
 Anticoagulation and Antiplatelet update: A case based approach Asif Serajian DO FACC FSCAI No disclosures relevant to this talk Objectives 1. Discuss the indication for antiplatelet therapy for cardiac
Anticoagulation and Antiplatelet update: A case based approach Asif Serajian DO FACC FSCAI No disclosures relevant to this talk Objectives 1. Discuss the indication for antiplatelet therapy for cardiac
Primary Prevention of Stroke
 Primary Prevention of Stroke Dr Chris Ellis Cardiologist Green Lane CVS Service, Auckland City Hospital & Auckland Heart Group, Mercy Hospital, Auckland 67 Pages Long, 735 References 29 Sub-Headings for
Primary Prevention of Stroke Dr Chris Ellis Cardiologist Green Lane CVS Service, Auckland City Hospital & Auckland Heart Group, Mercy Hospital, Auckland 67 Pages Long, 735 References 29 Sub-Headings for
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors
 Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
Autonomic nervous system, inflammation and preclinical carotid atherosclerosis in depressed subjects with coronary risk factors Carmine Pizzi 1 ; Lamberto Manzoli 2, Stefano Mancini 3 ; Gigliola Bedetti
Fasting or non fasting?
 Vascular harmony Robert Chilton Professor of Medicine University of Texas Health Science Center Director of Cardiac Catheterization labs Director of clinical proteomics Which is best to measure Lower continues
Vascular harmony Robert Chilton Professor of Medicine University of Texas Health Science Center Director of Cardiac Catheterization labs Director of clinical proteomics Which is best to measure Lower continues
Antiplatelet and Anti-Thrombotic Therapy. Ivan Anderson, MD RIHVH Cardiology
 Antiplatelet and Anti-Thrombotic Therapy Ivan Anderson, MD RIHVH Cardiology Outline Anti-thrombotic therapy Risk stratification of stroke with atrial fibrillation DVT and PE treatment Pharmacology Anti-platelet
Antiplatelet and Anti-Thrombotic Therapy Ivan Anderson, MD RIHVH Cardiology Outline Anti-thrombotic therapy Risk stratification of stroke with atrial fibrillation DVT and PE treatment Pharmacology Anti-platelet
Practical Considerations for Using Oral Anticoagulants in Patients with Chronic Kidney Disease
 Practical Considerations for Using Oral Anticoagulants in Patients with Chronic Kidney Disease Cyrille K. Cornelio, Pharm.D. PGY2 Cardiology Pharmacy Resident The University of Oklahoma College of Pharmacy
Practical Considerations for Using Oral Anticoagulants in Patients with Chronic Kidney Disease Cyrille K. Cornelio, Pharm.D. PGY2 Cardiology Pharmacy Resident The University of Oklahoma College of Pharmacy
The Framingham Coronary Heart Disease Risk Score
 Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Advances in Anticoagulation
 May 18, 2017 Advances in Anticoagulation Wei Ling Lau, MD Assistant Professor, Nephrology University of California, Irvine Talk Outline High stroke risk in CKD population Warfarin off-target effects on
May 18, 2017 Advances in Anticoagulation Wei Ling Lau, MD Assistant Professor, Nephrology University of California, Irvine Talk Outline High stroke risk in CKD population Warfarin off-target effects on
TAVR in patients with. End-Stage CKD or in Renal Replacement Therapy:
 TAVR in patients with End-Stage CKD or in Renal Replacement Therapy: Special Considerations and Prevention of early Valve Failure Antonios Chalapas, MD, PhD, FESC THV & Hygeia Hospital Heart Team Athens,
TAVR in patients with End-Stage CKD or in Renal Replacement Therapy: Special Considerations and Prevention of early Valve Failure Antonios Chalapas, MD, PhD, FESC THV & Hygeia Hospital Heart Team Athens,
Aortic Root Calcification: A Possible Imaging Biomarker of Coronary Atherosclerosis
 Published online: January 8, 216 216 S. Karger AG, Basel 2235 8676/16/34 167$39.5/ Mini-Review Aortic Root Calcification: A Possible Imaging Biomarker of Coronary Hussein Nafakhi a Hasan A. Al-Nafakh b
Published online: January 8, 216 216 S. Karger AG, Basel 2235 8676/16/34 167$39.5/ Mini-Review Aortic Root Calcification: A Possible Imaging Biomarker of Coronary Hussein Nafakhi a Hasan A. Al-Nafakh b
The CARI Guidelines Caring for Australasians with Renal Impairment. Serum phosphate GUIDELINES
 Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Serum phosphate GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
Date written: August 2005 Final submission: October 2005 Author: Carmel Hawley Serum phosphate GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Oral Anticoagulants Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Oral Anticoagulant - Bevyxxa (betrixaban), Eliquis (apixaban), Pradaxa (dabigatran),
Oral Anticoagulants Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Oral Anticoagulant - Bevyxxa (betrixaban), Eliquis (apixaban), Pradaxa (dabigatran),
2013 ACC AHA LIPID GUIDELINE JAY S. FONTE, MD
 2013 ACC AHA LIPID GUIDELINE JAY S. FONTE, MD How do you interpret my blood test results? What are our targets for these tests? Before the ACC/AHA Lipid Guidelines A1c:
2013 ACC AHA LIPID GUIDELINE JAY S. FONTE, MD How do you interpret my blood test results? What are our targets for these tests? Before the ACC/AHA Lipid Guidelines A1c:
We have recently proposed the hypothesis that arterial
 Osteoprotegerin Inhibits Artery Calcification Induced by Warfarin and by Vitamin D Paul A. Price, Helen H. June, Jessica R. Buckley, Matthew K. Williamson Abstract The present experiments were carried
Osteoprotegerin Inhibits Artery Calcification Induced by Warfarin and by Vitamin D Paul A. Price, Helen H. June, Jessica R. Buckley, Matthew K. Williamson Abstract The present experiments were carried
Performance and Quality Measures 1. NQF Measure Number. Coronary Artery Disease Measure Set
 Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Left atrium appendage closure: A new technique for patients at high hemorrhagic risk
 Left atrium appendage closure: A new technique for patients at high hemorrhagic risk Victoria Martin Yuste MD PhD ITC. Cardiology Department. Hospital Clinic. Barcelona SITE. Barcelona, Juin-9-2013 NON
Left atrium appendage closure: A new technique for patients at high hemorrhagic risk Victoria Martin Yuste MD PhD ITC. Cardiology Department. Hospital Clinic. Barcelona SITE. Barcelona, Juin-9-2013 NON
MPS and Calcium Score in asymptomatic patient F. Mut, J. Vitola
 MPS and Calcium Score in asymptomatic patient F. Mut, J. Vitola Nuclear Medicine Service, Asociacion Española Montevideo, Uruguay Quanta Diagnostico Nuclear Curitiba, Brazil Clinical history Male 63 y.o.,
MPS and Calcium Score in asymptomatic patient F. Mut, J. Vitola Nuclear Medicine Service, Asociacion Española Montevideo, Uruguay Quanta Diagnostico Nuclear Curitiba, Brazil Clinical history Male 63 y.o.,
