TRAINING NEONATOLOGY SILVANA PARIS
|
|
|
- Elwin Watts
- 5 years ago
- Views:
Transcription
1 TRAINING ON NEONATOLOGY SILVANA PARIS
2 RESUSCITATION IN DELIVERY ROOM
3 INTRODUCTION
4 THE GLOBAL RESUSCITATION BURDEN IN NEWBORN
5 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS NEED RESUSCITATION 5% MODERATE RESUSCITATION AND 1% (1,3 MILLION) EXTENSIVE RESUSCITATION OPTIMAL RESUSCITATION METHODS MAY SUBSTANTIALLY REDUCE MORTALITY
6 INTERVENTIONS IN TERM OR NEAR TERM NEWBORN IN THE DELIVERY ROOM INTERVENTION Assess baby s response to birth Keep baby warm Position, clear airway, stimulate to breathe by drying Give oxygen only if necessary FREQUENCY Establish effective ventilation bag & mask ventilation endotracheal intubate Provide chest compressions Adrenaline Volume expansion 3 5/100 1/100-1/700 < 1/1000 6/ /12000
7 P-BSL P-ALS
8 P-BLS PEDIATRIC BASIC LIFE SUPPORT P-ALS PEDIATRIC ADVANCED LIFE SUPPORT
9 DEFINITION Basic Life Support Has been defined like a method for the preservation of life by the initial establishment of and /or maintenance of airway, breathing and circulation, in case of emergency care For every step it is need EVALUATION ACTION
10 BLS/ALS SEQUENCE CHECK FOR A AIRWAYS B BREATHING BLS ALS C CIRCULATION D DRUGS/DEFIBRILLATION
11 GENERAL PRINCIPLES OF NEONATAL RESUSCITATION
12 A PERSON SKILLLED IN RESUSCITATION OF THE NEWBORN SHOULD BE PRESENT AT THE DELIVERY OF ALL HGH-RISK INFANTS THERE IS NO TIME FOR INDECISION, YET AN INCORRECT DECISION CAN BE TRAGIC SUCCESSFUL PERFORMANCE IN THIS SITUATION INVOLVES KNOWLEDGE OF PERINATAL PHYSIOLOGY AND PRINCIPLES OF RESUSCITATION
13 GOALS OF RESUSCITATION
14 EXPANSION OF THE LUNGS (A AIRWAYS) BY CLEARING THE UPPER ARIWAY AND ENSURING A PATENT ROUTE TO THE TRACHEA ALVEOLAR VENTILATION (B BREATHING) INCREASING THE ARTERIAL PO2 BY PROVIDING OXYGEN IF NECESSARY ADEQUATE CARDIAC OUT (C CIRCULATION) MINIMIZE THE OXYGEN CONSUMPTION BY REDUCING HEAT LOSSES IN THE IMMEDIATE POSTPARTUM PERIOD
15 STAFF FOR NEONATAL RESUSCITATION MEDICAL OFFICERS NEONATAL INTENSIVE CARE NURSES MIDWIVES
16 PHYSIOLOGY
17 FETAL-NEONATAL CIRCOLATION
18 ADULT BLOOD CIRCULATION The heart pumps blood into two closed circuits the systemic circulation and the pulmonary circulation with each beat. The two circuits are arranged in series: The output of one becomes the input of the other The left side of the heart is the pump for the systemic circulation; In systemic tissues, exchange of nutrients and gases occur at capillary bed level. Blood unloads oxygen and picks up carbon dioxide from tissues The right side of the heart is the pump for the pulmonary circulation; it receives all the dark red, deoxygenated blood returning from the systemic circulation. Blood ejected from the right ventricle into the pulmonary arteries that carry it to the right and left lungs. Gas exchange occurs across these capillaries, and newly oxygenated blood enters venules and progressively larger veins The freshly oxygenated blood flows into four pulmonary veins and return to the left atrium of the heart.
19 ADULT BLOOD CIRCULATION
20 FETAL CIRCULATION Placenta Umbilical Vein Fetal Portal Vein Inferior Cave Vein SHUNT Ductus Venosus Right Atrium Left Atrium SHUNT Right Ventricle Left Ventricle FORAMEN OVALE Pulmonary Artery SHUNT Ductus Aorta Arteriosus Aorta Systemic Circulation
21 Image from
22 THE PHYSIOLOGICAL CHANGES DURING TRANSITION FROM FETAL LIFE TO NEONATAL LIFE
23 CIRCULATORY CHANGES When cord is clamped and placenta is no longer part of system LEFT HEART PRESSURE INCREASE RIGHT HEART PRESSURE DROPS SHUNTS CLOSE EXPANSION OF THE LUNGS ESTABLISHMENT OF AFFECTIVE AIR EXCHANGE
24 POSTNATAL CIRCULATION IMAGE FORM OXFORD JOURNAL.ORG
25 PRE-POST NATAL CIRCULATION IMAGES FROM
26 THE CHANGE FROM FETAL TO POSTNATAL CIRCULATION HAPPENS VERY QUICKLY CHANGES ARE INITIATED BY BABY S FIRST BREATH FORAMEN OVALE DUCTUS ARTERIOUSUS DUCTUS VENOSUS CLOSES SHORTLY AFTER BIRTH, FUSES COMPLETELY IN FIRST YEAR CLOSES SOON AFTER BIRTH, BECOMES LIGAMENTUM ARTERIOUSUM IN ABOUT 3 MONTHS LIGAMENTUM VENOSUM UMBILICAL ARTERIES MEDIAL UMBILICAL LIGAMENTS UMBILICAL VEIN LIGAMENTUM TERES
27 WHEN THE INFANT IS BORN A CONTINUAL PROCESS OF EVALUATION AND EVENTUALLY RESUSCITATION BEGINS
28 NO ASPHYXIA APGAR OF 8 TO 10 ROUTINE CARE
29 MILD ASPHYXIA APGAR SCORE OF 5 TO 7 INFANTS MILD DEPRESSED THE GOAL IS TO INDUCE THE BABY TO TAKE A SPONTANEOUS BREATH TO ACHIEVE LUNG EXPANSION AND ESTABLISH A FUNCTIONAL RESIDUAL CAPACITY (FRC) STIMULATION OXYGEN IF IT IS NEED
30 MODERATE ASPHYXIA APGAR SCORE OF 3 TO 4 HEART RATE < 100 BEATS /min > 60 BEATS/ min (DESPITE STIMULATION AND FACIAL OXYGEN) BAG AND MASK VENTILATION SHOULD BE STARTED
31 SEVERE ASPHYXIA APGAR SCORE OF 0 TO 2 THESE INFANTS REQUIRE IMMEDIATE AND VIGOROUS RESUSCITATION THIS PROCESS REQUIRES AT LEAST THREE TRAINED PEOPLE WORKING TOGETHER SWIFTLY AND EFFICIENTLY
32 SEVERE ASPHYXIA APGAR SCORE OF 0 TO 2 HR <60/min (DESPITE THE BAG VENTILATION) START CHEST COMPRESS AND DRUGS IF IT IS NEED
33 EXENTIAL RESUSCITATION DRUGS ADRENALINE 1:10,000 VOLUME EXPANDERS: NORMAL SALINE / (BLOOD O-NEG) NALOXONE
34 ILCOR/AHA RESUSCITATION ALGORHYTM A Airways Initial steps of stabilisation (assess the airways, positioning, stimulating, dry and provide warmth) B Breathing C CirculatIon D Drugs Ventilation (including bag-mask or bag -tube ventilation) Chest compressions Medications or volume expansion
35 RESUSCITATION ALGORHYTM A B C D BIRTH Term Gestation? Amniotic fluid clear? Breathing or crying? Good muscle tone? Color pink? NO No Evaluate respirations, heart rate and color Apneic or HR<100 HR>1000 Provide positive pressure ventilation HR < 60 HR > 60 Continue positive pressure ventilation Administer chest compression HR < 60 Administer Adrenaline and/or Volume expander Yes Provide routine care Dry Provide warmth Clear airway if needed Breathing > 100 but cyanotic cyanotic Consider Supplementary O2 Persistent cyanosis Tracheal intubation may be considered at several steps A-B 30 SEC C -D 30 SEC
36 CESSATION OF RESUSCITATION If after 20 minutes of resuscitation the baby is Not breathing and pulse is absent cease efforts Explain to the mother that the baby has died, and give it to her to hold if she wishes
37 POST RESUSCITATION CARE
38 REPORT AND RECORD EVENTS ACCURATELY NEWBORNS INTUBATED AND EXTUBATED AT DELIVERY REQUIRES OBSERVATION FOR AT LEAST 2 HOURS NEWBORNS WHO RECEIVED NALOXONE AT BIRTH REQUIRE OBSERVATION FOR AT LEAST 4 HOURS NEWBORNS WHO REQUIRED RESUSCITATION ARE AT RISK MONITOR VITAL SIGNS AND HYPOGLYCAEMIA, CONSIDER NEED FOR ANTIBIOTICS INSERT AN OROGASTRIC TUBE (SIZE 8 FG) TO ASPIRATE AND DECOMPRESS THE STOMACH OF ANY NEWBORN THAT REQUIRED PROLONGED VENTILATION
39 NEONATAL RESUSCITATION DRUGS
40 ADRENALINE 1:10,000 SOLUTION ADRENALINE 1:10,000 solution = 0.1ml contains 10mcg of adrenaline Dose: ml/kg of 1:10,000 IV Repeat intravenously, when indicated at 3-minute cycle Flush 1 ml Normal Saline after each intravenous administration It is indicated when the heart rate remains <60 after 30 seconds of adequate ventilation and chest compressions solution administered via the endotracheal route until the intravenous route is established
41 VOLUME EXPANDERS I NORMAL SALINE Dose: 10ml/kg IV Slow push over 5-10 minutes (optimally via free-flowing umbilical venous catheter) It is indicated in an infant where there is suspected blood loss or the infant appears pale, poor perfusion, weak pulse and has not responded adequately to other resuscitative measures EMERGENCY O-NEG BLOOD it is indicated for emergency transfusion in the setting of massive blood loss
42 NALOXONE 0.4mg/ml SOLUTION NALOXONE Dose: 0.1mg/kg of a 0.4mg/ml solution IM/IV It is indicated to reversal of respiratory depression in a newly born infant whose mother received narcotics within 4 hours of birth. It is important to establish and maintain adequate ventilation and circulation before administration of naloxone DO NOT administer Naloxone to infants born to women suspected of narcotic dependence. This may cause abrupt withdrawal and seizures
43 Correct position of the head for ventilation <neutral position> FROM WHO POCKET BOOK
44 Fitting mask over face right size and position mask held mask too mask too of mask too low small large right wrong wrong wrong FROM WHO POCKET BOOK
45 Inadequate seal If you hear air escaping from the mask, form a better seal. The most common leak is between the nose and the cheeks. FROM WHO POCKET BOOK
46 Ventilating a neonate with bag and mask Pull the jaw forward towards the mask with the third finger of the hand holding the mask Do not hyperextend the neck FROM WHO POCKET BOOK
47 KEY TO SUCCESSFUL RESUSCITATION ANTICIPATE (EQUIPMENT) BE PREPARED (RECOGNIZE RISK FACTORS) KNOW WHAT TO DO (BE GENTLE AND FAST) IN WHAT ORDER (ABCD SUPPORT) BE ABLE TO WORK QUICKLY IN COORDINATION DOCUMENT/RECORD MAINTAIN HYGIENE REMEMBER MOTHER
48 ILCOR Guidelines Newborn Resuscitation Changes from Timing the first 60 seconds only Progression to the next step following initial evaluation is defined by heart rate and respiration For babies born at term it is best to begin resuscitation with air rather than 100% oxygen Evidence does not support or refute routine endotracheal suctioning of infants born through meconium-stained amniotic fluid, even when the newborn is depressed Chest compression - ventilation ratio 3:1 unless the arrest is known to be of cardiac etiology. Then higher ratio should be considered (15:2) Hypothermia in moderate to severe HIE
49 THNKS FOR ATTENTION
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
and the beat goes on: developing a heart and vascular system
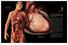 HEARTCHAPTER1.qxp 7/15/05 10:22 AM Page 4 this integrated system of heart, blood, and vessels is known as the cardiovascular system. CHAPTER 1 and the beat goes on: developing a heart and vascular system
HEARTCHAPTER1.qxp 7/15/05 10:22 AM Page 4 this integrated system of heart, blood, and vessels is known as the cardiovascular system. CHAPTER 1 and the beat goes on: developing a heart and vascular system
PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني
 Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Development of Blood Vessels and Fetal Circulation *
 OpenStax-CNX module: m46610 1 Development of Blood Vessels and Fetal Circulation * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the
OpenStax-CNX module: m46610 1 Development of Blood Vessels and Fetal Circulation * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the
Neonatal/Pediatric Cardiopulmonary Care
 Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Cardiovascular System Blood Vessels
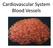 Cardiovascular System Blood Vessels Structure of Blood Vessels The three layers (tunics) Tunica intima composed of simple squamous epithelium Tunica media sheets of smooth muscle Contraction vasoconstriction
Cardiovascular System Blood Vessels Structure of Blood Vessels The three layers (tunics) Tunica intima composed of simple squamous epithelium Tunica media sheets of smooth muscle Contraction vasoconstriction
The Physiology of the Fetal Cardiovascular System
 The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
The Physiology of the Fetal Cardiovascular System Jeff Vergales, MD, MS Department of Pediatrics Division of Pediatric Cardiology jvergales@virginia.edu Disclosures I serve as the medical director for
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
Neonatal Resuscitation
 Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
Neonatal Resuscitation High Risk Deliveries A person trained in neonatal resuscitation is usually called to be present for the following deliveries: 1. Antepartum factors Maternal diabetes Pregnancy induced
Neonatal Resuscitation in What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011
 Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Blood Vessels. Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels. Veins carry blood toward the heart
 C H A P T E R Blood Vessels 20 Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels The site of exchange of molecules between blood and tissue fluid Veins
C H A P T E R Blood Vessels 20 Types of Blood Vessels Arteries carry blood away from the heart Capillaries smallest blood vessels The site of exchange of molecules between blood and tissue fluid Veins
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
THE CIRCULATORY SYSTEM
 Biology 30S THE CIRCULATORY SYSTEM Name: This module adapted from bblearn.merlin.mb.ca 1 Introduction to Circulation The first organ to form, and the last organ to die. The heart is the pump of life. The
Biology 30S THE CIRCULATORY SYSTEM Name: This module adapted from bblearn.merlin.mb.ca 1 Introduction to Circulation The first organ to form, and the last organ to die. The heart is the pump of life. The
table of contents pediatric treatment guidelines
 table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
NEONATOLOGY Healthy newborn. Neonatal sequelaes
 NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Pedi-Cap CO 2 detector
 Pedi-Cap CO 2 detector Presentation redeveloped for this program by Rosemarie Boland from an original presentation by Johnston, Adams & Stewart, (2006) Background Clinical methods of endotracheal tube
Pedi-Cap CO 2 detector Presentation redeveloped for this program by Rosemarie Boland from an original presentation by Johnston, Adams & Stewart, (2006) Background Clinical methods of endotracheal tube
Development of the Heart *
 OpenStax-CNX module: m46673 1 Development of the Heart * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will
OpenStax-CNX module: m46673 1 Development of the Heart * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will
PIAF study: Placental insufficiency and aortic isthmus flow Jean-Claude Fouron, MD
 Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Dear colleagues, I would like to thank you very sincerely for agreeing to participate in our multicentre study on the clinical significance of recording fetal aortic isthmus flow during placental circulatory
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
Circulatory System Review
 Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
Stabilization and Transportation guidelines for Neonates and infants with Heart disease:
 Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
Stabilization and Transportation guidelines for Neonates and infants with Heart disease: Background: Referral Pediatric Cardiac Units, frequently receive neonates and infants referred and transported from
Pediatric Advanced Life Support Overview Judy Haluka BS, RCIS, EMT-P
 Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Nassau Regional Emergency Medical Services. Advanced Life Support Pediatric Protocol Manual
 Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Steven Ringer MD PhD April 5, 2011
 Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
And Then There Were Two. Renae Buehner RNC, BSN Avera McKennan Labor and Delivery Unit Supervisor, Lead OB Flight RN
 And Then There Were Two Renae Buehner RNC, BSN Avera McKennan Labor and Delivery Unit Supervisor, Lead OB Flight RN Disclosures I have none She s coming in hot Assisting the maternal patient in a safe
And Then There Were Two Renae Buehner RNC, BSN Avera McKennan Labor and Delivery Unit Supervisor, Lead OB Flight RN Disclosures I have none She s coming in hot Assisting the maternal patient in a safe
Resuscitation efforts for Mom & Baby
 Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY
 Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen
 Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
1 Pediatric Advanced Life Support Science Update What s New for 2010? 3 CPR. 4 4 Steps of BLS Survey 5 CPR 6 CPR.
 1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
TOPIC 6: HUMAN HEALTH AND PHYSIOLOGY
 TOPIC 6: HUMAN HEALTH AND PHYSIOLOGY 6.2 Transport System/Circulatory Draw and label a diagram of the heart showing the four chambers, associated blood vessels, valves and the route of blood through the
TOPIC 6: HUMAN HEALTH AND PHYSIOLOGY 6.2 Transport System/Circulatory Draw and label a diagram of the heart showing the four chambers, associated blood vessels, valves and the route of blood through the
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Patent ductus arteriosus (PDA)
 Patent ductus arteriosus (PDA) Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 This information sheet explains about the congenital (present at birth) heart condition
Patent ductus arteriosus (PDA) Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 This information sheet explains about the congenital (present at birth) heart condition
New Zealand Data Sheet. Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml
 CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
A. Incorrect! Think of a therapy that reduces prostaglandin synthesis. B. Incorrect! Think of a therapy that reduces prostaglandin synthesis.
 USMLE Step 1 - Problem Drill 02: Embryology Question No. 1 of 10 1. A premature infant is born with a patent ductus arteriosis. Which of the following treatments may be used as part of the treatment regimen?
USMLE Step 1 - Problem Drill 02: Embryology Question No. 1 of 10 1. A premature infant is born with a patent ductus arteriosis. Which of the following treatments may be used as part of the treatment regimen?
A SYNOPSIS BY ILCOR PEDIATRIC TASK FORCE. Pediatric Basic Life Support, Pediatric Advanced Life Support and Neonatal Resuscitation 2015
 Vol. 2 - No.4 October - December 2015 83 Vol. 2 - No.4 October - December 2015 84 There is new evidence that when treating pediatric septic shock in specific settings, the use of restricted volume of isotonic
Vol. 2 - No.4 October - December 2015 83 Vol. 2 - No.4 October - December 2015 84 There is new evidence that when treating pediatric septic shock in specific settings, the use of restricted volume of isotonic
ISPUB.COM. The Use of LMA in Newborn Resuscitation. R Vadhera INTRODUCTION VENTILATION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 1 Number 4 The Use of LMA in Newborn Resuscitation R Vadhera Citation R Vadhera. The Use of LMA in Newborn Resuscitation. The Internet Journal of
ISPUB.COM The Internet Journal of Anesthesiology Volume 1 Number 4 The Use of LMA in Newborn Resuscitation R Vadhera Citation R Vadhera. The Use of LMA in Newborn Resuscitation. The Internet Journal of
DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5
 DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5 REVIEW OF CARDIAC ANATOMY Heart 4 chambers Base and apex Valves Pericardial sac 3 layers: epi, myo, endo cardium Major blood vessels Aorta and its
DEVELOPMENT OF THE CIRCULATORY SYSTEM L E C T U R E 5 REVIEW OF CARDIAC ANATOMY Heart 4 chambers Base and apex Valves Pericardial sac 3 layers: epi, myo, endo cardium Major blood vessels Aorta and its
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Resuscitation Checklist
 Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
The assessment helps decide if the patient is an emergency, priority or non-urgent case.
 Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
June 2011 Bill Streett-Training Section Chief
 Capnography 102 June 2011 Bill Streett-Training Section Chief Terminology Capnography: the measurement and numerical display of end-tidal CO2 concentration, at the patient s airway, during a respiratory
Capnography 102 June 2011 Bill Streett-Training Section Chief Terminology Capnography: the measurement and numerical display of end-tidal CO2 concentration, at the patient s airway, during a respiratory
1
 1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Cardiac Emergencies. Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington
 Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
These signs should lead to the administration of high concentrations of
 Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
ACoRN Workbook 2012 Update
 ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
Pediatrics 1 Neonatal Resuscitation Pediatric Assessment Airway Management. Neonatology. Topics. EMT Paramedic / Critical Refresher Session # 22
 EMT Paramedic / Critical Refresher Session # 22 Pediatrics 1 Neonatal Resuscitation Pediatric Assessment Airway Management 1 Neonatology 2 Topics Newborns & Neonates High Risk Newborn Patients APGAR Scoring
EMT Paramedic / Critical Refresher Session # 22 Pediatrics 1 Neonatal Resuscitation Pediatric Assessment Airway Management 1 Neonatology 2 Topics Newborns & Neonates High Risk Newborn Patients APGAR Scoring
2. General Cardiac Arrest Protocol Medical Newborn/Neonatal. Protocol 8-3 Resuscitation 4. Medical Supraventricular
 PEDIATRIC CARDIAC SECTION: Pediatric Cardiovascular Emergencies REVISED: 06/2017 Section 8 1. Cardiac Arrest Unknown Rhythm (i.e. Protocol 8-1 BLS) 2. General Cardiac Arrest Protocol 8-2 3. Medical Newborn/Neonatal
PEDIATRIC CARDIAC SECTION: Pediatric Cardiovascular Emergencies REVISED: 06/2017 Section 8 1. Cardiac Arrest Unknown Rhythm (i.e. Protocol 8-1 BLS) 2. General Cardiac Arrest Protocol 8-2 3. Medical Newborn/Neonatal
Pediatric Code Blue. Goals of Resuscitation. Focus Conference November Ensure organ perfusion
 Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Circulatory System Notes
 Circulatory System Notes Functions of Circulatory System A. Transports B. Transports C. Transports D. Transports E. of fluids F. G. Regulate temperature H. Blood clotting Characteristics of various blood
Circulatory System Notes Functions of Circulatory System A. Transports B. Transports C. Transports D. Transports E. of fluids F. G. Regulate temperature H. Blood clotting Characteristics of various blood
Skeletal muscle. Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
 Regional blood flow Skeletal muscle Extreme increases during exercises Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
Regional blood flow Skeletal muscle Extreme increases during exercises Flow increases and decreases with each muscular contraction - as a result of compression of the blood vessels by contracted muscle
Circulatory System. and. Respiratory System. Ari Min, Yerim Lee and Min Ji Song THE HEART LUNGS. Monday, May 23, 2011
 Human Anatomy Circulatory System and THE HEART Respiratory System LUNGS Ari Min, Yerim Lee and Min Ji Song Purpose of the Circulatory System Function of circulatory system: exchange gases with cardiovascular
Human Anatomy Circulatory System and THE HEART Respiratory System LUNGS Ari Min, Yerim Lee and Min Ji Song Purpose of the Circulatory System Function of circulatory system: exchange gases with cardiovascular
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
Today s objectives:! - Learn BASICS of circulatory system (Heart, different veins and arteries)! - Appreciate effects and treatment for
 Today s objectives:! - Learn BASICS of circulatory system (Heart, different veins and arteries)! - Appreciate effects and treatment for hyperlipidemia! Agenda! - Review objectives for 6.2! - Video of circulatory
Today s objectives:! - Learn BASICS of circulatory system (Heart, different veins and arteries)! - Appreciate effects and treatment for hyperlipidemia! Agenda! - Review objectives for 6.2! - Video of circulatory
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
NRP 2018 Current Issues Seminar Science behind NRP. Myra Wyckoff, MD, FAAP Marya Strand, MD, MS, FAAP
 NRP 2018 Current Issues Seminar Science behind NRP Myra Wyckoff, MD, FAAP Marya Strand, MD, MS, FAAP Faculty Disclosure Information In the past 12 months, we have had no relevant financial relationships
NRP 2018 Current Issues Seminar Science behind NRP Myra Wyckoff, MD, FAAP Marya Strand, MD, MS, FAAP Faculty Disclosure Information In the past 12 months, we have had no relevant financial relationships
Birth Asphyxia - Summary of the previous meeting and protocol overview
 Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
10RC2 - Berger. Resuscitation of the newborn
 10RC2 - Berger Resuscitation of the newborn Thomas M. Berger Neonatal and Paediatric Intensive Care Unit Children s Hospital of Lucerne Lucerne, Switzerland Introduction The respiratory and cardiovascular
10RC2 - Berger Resuscitation of the newborn Thomas M. Berger Neonatal and Paediatric Intensive Care Unit Children s Hospital of Lucerne Lucerne, Switzerland Introduction The respiratory and cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS
 CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
Paediatric Resuscitation. EMS Rounds Gurinder Sangha MD Paediatric Emergency Fellow June 18, 2009
 Paediatric Resuscitation EMS Rounds Gurinder Sangha MD Paediatric Emergency Fellow June 18, 2009 Essentials of Resuscitation Airway Breathing Circulation AIRWAY Differences in Paediatric Airway Shorter
Paediatric Resuscitation EMS Rounds Gurinder Sangha MD Paediatric Emergency Fellow June 18, 2009 Essentials of Resuscitation Airway Breathing Circulation AIRWAY Differences in Paediatric Airway Shorter
Circulation: Chapter 25. Cardiac Output. The Mammalian Heart Fig Right side of the heart
 Circulation: Chapter 25 1. Limits of Diffusion A. Small organisms use diffusion B. rapid over small distances 2. Most animals have circulatory systems A. Blood B. Pump (Heart) or propulsive structures
Circulation: Chapter 25 1. Limits of Diffusion A. Small organisms use diffusion B. rapid over small distances 2. Most animals have circulatory systems A. Blood B. Pump (Heart) or propulsive structures
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
The Circulatory System
 The Circulatory System answers to worksheet will either be on the presentation or video By: Lanya King, Geianah Shaw,and Heidi Puerta The Functions of the Circulatory System Respiration- delivers oxygen
The Circulatory System answers to worksheet will either be on the presentation or video By: Lanya King, Geianah Shaw,and Heidi Puerta The Functions of the Circulatory System Respiration- delivers oxygen
Spleen. Vertebrate hearts Pericardial cavity division in coelum. Vessel walls. Endocardium = endothelium of blood vessels. Artery elastic tissue
 Spleen White pulp macrophages, monocyte storage Red pulp - (RBC) storage, and prod n (in nonmammals) Vertebrate hearts Pericardial cavity division in coelum Endocardium = endothelium of blood vessels Fig.
Spleen White pulp macrophages, monocyte storage Red pulp - (RBC) storage, and prod n (in nonmammals) Vertebrate hearts Pericardial cavity division in coelum Endocardium = endothelium of blood vessels Fig.
RESUSCITATION AT BIRTH
 ` 1 VITED ARTICLE RESUSCITATION AT BIRTH R Joseph ABSTRACT Birth asphyxia is frequent and often severe, occurring in about 10% and 1% respectively of all births; in a third it is unexpected. Delivery rooms
` 1 VITED ARTICLE RESUSCITATION AT BIRTH R Joseph ABSTRACT Birth asphyxia is frequent and often severe, occurring in about 10% and 1% respectively of all births; in a third it is unexpected. Delivery rooms
Cardiovascular System
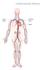 Cardiovascular System Cardiovascular System - Function The cardiovascular system transports, from one part of the body to another: nutrients, oxygen, ions, proteins, hormones and other signaling molecules,
Cardiovascular System Cardiovascular System - Function The cardiovascular system transports, from one part of the body to another: nutrients, oxygen, ions, proteins, hormones and other signaling molecules,
PALS Case Scenario Testing Checklist Respiratory Case Scenario 1 Upper Airway Obstruction
 Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Large Arteries of Heart
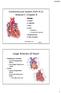 Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
ILCOR ADVISORY STATEMENT: RESUSCITATION OF THE NEWLY BORN INFANT. An Advisory Statement From the Pediatric Working Group of the
 ILCOR ADVISORY STATEMENT: RESUSCITATION OF THE NEWLY BORN INFANT An Advisory Statement From the Pediatric Working Group of the International Liaison Committee on Resuscitation John Kattwinkel, MD* ; Susan
ILCOR ADVISORY STATEMENT: RESUSCITATION OF THE NEWLY BORN INFANT An Advisory Statement From the Pediatric Working Group of the International Liaison Committee on Resuscitation John Kattwinkel, MD* ; Susan
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
Contents. Page 1. Homework 11 Chapter Blood Vessels Due: Week 6 Lec 11
 Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Managing Compromised and Weak Calves at Birth
 University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln Range Beef Cow Symposium Animal Science Department 11-2015 Managing Compromised and Weak Calves at Birth Franklyn Garry
University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln Range Beef Cow Symposium Animal Science Department 11-2015 Managing Compromised and Weak Calves at Birth Franklyn Garry
Introduction (1 of 3)
 Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
ADMISSION/DISCHARGE FORM FOR INFANTS BORN IN 2019 DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
