Familial Dilated Cardiomyopathy Caused by an Alpha-Tropomyosin Mutation
|
|
|
- Gordon Fox
- 5 years ago
- Views:
Transcription
1 Journal of the American College of Cardiology Vol. 55, No. 4, by the American College of Cardiology Foundation ISSN /10/$36.00 Published by Elsevier Inc. doi: /j.jacc QUARTERLY FOCUS ISSUE: HEART FAILURE Familial Dilated Cardiomyopathy Caused by an Alpha-Tropomyosin Mutation The Distinctive Natural History of Sarcomeric Dilated Cardiomyopathy Neal K. Lakdawala, MD,* Lisa Dellefave, MS, CGC, Charles S. Redwood, PHD, Elizabeth Sparks, RNP, Allison L. Cirino, MS, CGC,* Steve Depalma, PHD, Steven D. Colan, MD, Birgit Funke, PHD, Rebekah S. Zimmerman, PHD, Paul Robinson, DPHIL, Hugh Watkins, MD, PHD, Christine E. Seidman, MD,* # J. G. Seidman, PHD, Elizabeth M. McNally, MD, PHD, Carolyn Y. Ho, MD* Boston and Cambridge, Massachusetts; Chicago, Illinois; and Oxford, United Kingdom Objectives Background Methods Results Conclusions We sought to further define the role of sarcomere mutations in dilated cardiomyopathy (DCM) and associated clinical phenotypes. Mutations in several contractile proteins contribute to DCM, but definitive evidence for the roles of most sarcomere genes remains limited by the lack of robust genetic support. Direct sequencing of 6 sarcomere genes was performed on 334 probands with DCM. A novel D230N missense mutation in the gene encoding alpha-tropomyosin (TPM1) was identified. Functional assessment was performed by the use of an in vitro reconstituted sarcomere complex to evaluate ATPase regulation and Ca 2 affinity as correlates of contractility. TPM1 D230N segregated with DCM in 2 large unrelated families. This mutation altered an evolutionarily conserved residue and was absent in 1,000 control chromosomes. In vitro studies demonstrated major inhibitory effects on sarcomere function with reduced Ca 2 sensitivity, maximum activation, and Ca 2 affinity compared with wild-type TPM1. Clinical manifestations ranged from decompensated heart failure or sudden death in those presenting early in life to asymptomatic left ventricular dysfunction in those diagnosed during adulthood. Notably, several affected infants had remarkable improvement. Genetic segregation in 2 unrelated families and functional analyses conclusively establish a pathogenic role for TPM1 mutations in DCM. In vitro results demonstrate contrasting effects of DCM and hypertrophic cardiomyopathy mutations in TPM1, suggesting that specific functional consequences shape cardiac remodeling. Along with previous reports, our data support a distinctive, age-dependent phenotype with sarcomere-associated DCM where presentation early in life is associated with severe, sometimes lethal, disease. These observations have implications for the management of familial DCM. (J Am Coll Cardiol 2010;55:320 9) 2010 by the American College of Cardiology Foundation Dilated cardiomyopathy (DCM) is an important cause of heart failure (HF) and a leading indication for heart transplantation in children (1) and adults (2). During the past decade, there has been increasing recognition of the important contribution of genetic etiologies in causing idiopathic DCM, with family studies suggesting that 30% to 50% of the disease is inherited (3,4). However, clinical manifestations may be highly variable and obscure the identification of familial disease. See page 330 From the *Cardiovascular Division, Brigham and Women s Hospital, Boston, Massachusetts; Department of Medicine, Section of Cardiology, The University of Chicago, Chicago, Illinois; University of Oxford, Oxford, United Kingdom; Department of Genetics, Harvard Medical School, Boston, Massachusetts; Department of Cardiology, Children s Hospital Boston, Boston, Massachusetts; Harvard Medical School Partners Healthcare Center for Personalized Genetic Medicine, Cambridge, Massachusetts; and the #Howard Hughes Medical Institute. Support for these studies comes from grants from the National Institutes of Health (to Drs. Lakdawala, C. E. Seidman, J. G. Seidman, and Ho), Howard Hughes Medical Institute (Dr. C. E. Seidman), the Leducq Foundation (Drs. C. E. Seidman and J. G. Seidman), the Doris Duke Charitable Foundation (Dr. McNally), and the British Heart Foundation (Drs. Redwood, Robinson, and Watkins). Manuscript received August 7, 2009; revised manuscript received October 21, 2009, accepted November 9, 2009.
2 JACC Vol. 55, No. 4, 2010 January 26, 2010:320 9 Lakdawala et al. Tropomyosin Mutations in DCM 321 In contrast to hypertrophic cardiomyopathy (HCM), where sarcomere mutations cause the majority of disease (5), the genetics of DCM are more diverse and not as well defined. Mutations in a broad spectrum of genes have been implicated, including those encoding sarcomere proteins, components of the cytoskeleton, and mitochondrial proteins (3,6). Through comprehensive sequence analyses of sarcomere genes in 334 DCM probands we identified 2 unrelated, multigenerational families with DCM that shared a variant in the gene encoding alpha-tropomyosin (TPM1). Alpha-tropomyosin is an alpha-helical, coiled-coil homodimeric thin filament protein that participates in the Ca 2 regulation of contraction and acto-myosin interaction. Although TPM1 mutations are known causes of HCM, their pathogenicity in DCM has been inconclusive because they have previously been identified only in individual patients (7). We report genetic segregation of a TPM1 mutation and its in vitro functional consequences on sarcomere function. Together these data provide strong evidence that TPM1 mutations are pathogenic in DCM and extend knowledge about the pathogenesis and clinical course associated with sarcomere gene mutations. Methods Genetic analysis. Genomic DNA was isolated from blood by the use of standard methods (6) in probands with DCM. Direct DNA sequence analysis of all coding regions and intron/exon boundaries was performed in 6 sarcomere genes: myosin binding protein-c (MYBPC3); beta-myosin heavy chain (MYH7); cardiac troponin-t (TNNT2); cardiac troponin-i (TNNI3); alpha-tropomyosin (TPM1); and alpha-actin (ACTC1). To calculate the statistical likelihood that a genetic variant was associated with disease, logarithm (base 10) of odds (i.e., LOD) scores were calculated by the use of Vitesse (version 2.0, Bournemouth, Dorset, United Kingdom) for Mac/PC, assuming 80% DCM penetrance at 30 years and an allele frequency Haplotype analysis was performed to determine family relatedness by characterizing flanking single nucleotide polymorphisms in relevant families. Actin tropomyosin-activated myosin ATPase assay. Bacterial expression constructs in pmw172 encoding human wild-type and D230N (mutant) Ala-Ser-alphatropomyosin were created by 2-step polymerase chain reaction site-directed mutagenesis. The Ala-Ser N-terminal addition to TPM1 compensates for the absence of N-terminal acetylation in the bacterially produced peptide (8). Mutant or wild-type Ala-Ser-alpha-tropomyosin were expressed with wild-type troponin I, troponin T, and troponin C in BL21 (DES) plyss Escherichia coli cells and subsequently purified according to established protocols (9). Actin and myosin subfragment-1 (S-1) were obtained from rabbit skeletal muscle by standard procedures (10). Wildtype cardiac troponin complex was reconstituted from individual subunits by the use of stepwise dialysis and gel filtration as previously described (11). Thin filaments were reconstituted at an actin, Ala-Seralpha-tropomyosin, and troponin ratio of 7:1:1, respectively. Assays were performed as previously described with the use of 0.5- mol/l myosin S-1 and thin filaments reconstituted with the use of 3.5- mol/l actin, 0.5- mol/l tropomyosin, and 0.5- mol/l troponin in 50-mmol/l KCl, 5-mmol/l piperazine- N,N=-bis(2-ethanesulfonic acid), 3.87-mmol/l MgCl 2, and 0.25 Abbreviations and Acronyms DCM dilated cardiomyopathy HCM hypertrophic cardiomyopathy HF heart failure LV left ventricular/ ventricle LVIDD left ventricular end-diastolic internal diameter LVEF left ventricular ejection fraction mmol/l dithiothreitol, ph 7.0, at 37 C. The free Ca 2 concentration was set by the use of 1-mmol/l ethylene glycol tetraacetic acid and the appropriate concentration of CaCl 2 as previously described (11). Phosphate release was determined colorimetrically by standard protocols. Measurement of Ca 2 affinity by the use of 2-[4=-(iodoacetamido)aniline]-naphthalene-6-sulfonate (IAANS) troponin. Thin-filament Ca 2 affinity was measured by the use of IAANS label bound to Cys35 of recombinant human troponin C (12); a reporter of Ca 2 binding to the lowaffinity site of troponin C (site II) (12). Thin filaments were reconstituted with 21- mol/l actin, 3- mol/l Ala-Seralpha-tropomyosin, and 3- mol/l IAANS troponin. The final buffer concentration of ethylene glycol tetraacetic acid was 1 mmol/l, and the free Ca 2 concentration was set by use of the appropriate concentration of CaCl 2 as previously described (12). Steady-state fluorescence measurements (excitation 325 nm, emission 455 nm) were made with the use of a RF-1501 spectrofluorometer (Shimadzu, Kyoto, Japan) at 22 C. The change in fluorescence ( F) was monitored as the Ca 2 was titrated with final F values adjusted for the difference in assay mix volume after each incremental addition of 10 mmol/l CaCl 2. The adjusted and normalized F was plotted as a function of Ca 2 concentration and the resultant curves fitted to the Hill equation, a measure of the cooperativity of binding between Ca 2 and the thin filament. Clinical evaluation. Families with apparent familial DCM were recruited for genetic research. Family members were evaluated through history, physical examination, electrocardiography, and echocardiography. Echocardiographic dimensions were represented as z-scores for subjects younger than 16 years of age and left ventricular end-diastolic internal diameter (LVIDD z-score 2.0 was considered enlarged. The left ventricular ejection fraction (LVEF) was calculated by use of the modified Simpson s method. Subjects were considered affected with DCM if they had any of the following: clinical HF with left ventricular (LV) enlargement or systolic dysfunction; asymptomatic LV enlargement, that is, LV dimensions greater than the reference normal dimensions in adults (13) orz-score 2 in children;
3 322 Lakdawala et al. JACC Vol. 55, No. 4, 2010 Tropomyosin Mutations in DCM January 26, 2010:320 9 or asymptomatic LV systolic dysfunction (LVEF 55%). Clinical information on deceased subjects was obtained from their relatives and medical records whenever possible. All subjects provided informed consent in accordance with the guidelines of the University of Chicago and Brigham and Women s Hospital Human Subjects Committees. Statistical analysis. SAS version 9.1 (SAS Institute, Cary, North Carolina) was used to generate Kaplan-Meier curves to describe disease penetrance and event-free survival. Statistically significant differences in Ca 2 affinity and myosin ATPase activity were determined by the use of an unpaired Student t test (InStat, GraphPad Software Inc., La Jolla, California), with significance values defined as p Results Genetic analysis. A total of 334 subjects with DCM underwent sarcomere gene sequence analysis. A guanine to adenine (G A) substitution at residue 688 in the gene encoding alpha-tropomyosin (TPM1) was identified in 2 probands with familial disease (Online Fig. 1). This variant is predicted to substitute a highly conserved, negatively charged aspartate residue (D, position 230) (Online Table 1) with a neutral asparagine (N) on the surface of tropomyosin (Fig. 1) (14). TPM1 D230N segregated with DCM in 2 large Caucasian families (Figs. 2A and 2B). Haplotype analysis was performed by characterizing flanking single nucleotide polymorphisms, which are found to occur at frequencies of 24% and 52%, respectively, in the general population. Disease haplotypes were different in the 2 families (Fig. 2C), indicating that the families were unrelated and that TPM1 D230N arose independently in each family. The TPM1 D230N variant was present in all affected members in families A and B and absent from 21 of 25 unaffected adult family members as well as 1,000 unrelated Caucasian control chromosomes. The combined calculated LOD score was Therefore, we concluded that TPM1 D230N caused DCM in these 2 unrelated families. In vitro alpha-tropomyosin functional studies. To investigate the functional impact of TPM1 D230N, Ca 2 regulation of actin-tropomyosin activated myosin S-1 ATPase was evaluated as an in vitro correlate of contraction. Thin filaments reconstituted with wild-type Ala-Ser-alphatropomyosin had a maximally activated rate of ATP turnover of s 1. The concentration of Ca 2 at half-maximal ATP-turnover (pca 50 ) was (n 5) (Fig. 3A). In contrast, thin filaments reconstituted with D230N Ala-Ser-alpha-tropomyosin produced a lower maximum ATPase turnover rate ( s 1,n 3, p 0.001) and reduced Ca 2 sensitivity (pca , n 3, p 0.05) (Fig. 3A). Filaments reconstituted with a 1:1 mixture of wild-type/d230n Ala-Ser-alphatropomyosin (the expected ratio in situ) also showed a depressed maximally activated rate ( s 1, Figure 1 Molecular Model of Alpha-Tropomyosin Alpha-tropomyosin is an alpha-helical coiled-coil that interacts with actin (violet functional domains) and troponin T (blue). The locations of mutations associated with dilated cardiomyopathy (yellow) and hypertrophic cardiomyopathy (green) are indicated. The D230N mutation is shown in red.
4 JACC Vol. 55, No. 4, 2010 January 26, 2010:320 9 Lakdawala et al. Tropomyosin Mutations in DCM 323 Figure 2 Pedigrees and Haplotype Analysis of Families With Autosomal-Dominant DCM Due to D230N Mutation in Alpha-Tropomyosin Pedigrees are shown for 2 unrelated families (family A [A] and family B [B]) with dilated cardiomyopathy (DCM). Squares indicate male family members, circles indicate female family members, solid symbols indicate DCM, open symbols unaffected members, green symbols indicate uncertain clinical status, and slashes indicate deceased members. Genotype results are indicated by ( ) D230N present and ( ) mutation absent. *Sudden cardiac death. (C) Haplotype analysis indicates that the families are unrelated and that the D230N (688G A) TPM1 mutation arose independently in these families. Several family members from each kindred were genotyped at 4 loci in the TPM1 gene (rs , rs , rs , rs ), comprising 4 common haplotypes in Caucasians (A, B, C, D) as described by Hap- Map. The D230N mutation (fam variant) is shown in red with an asterisk.
5 324 Lakdawala et al. JACC Vol. 55, No. 4, 2010 Tropomyosin Mutations in DCM January 26, 2010:320 9 Figure 3 Functional Properties of the D230N Mutation in Alpha-Tropomyosin In vitro functional analyses of the D230N mutant alpha-tropomyosin show that at any activating-level of Ca 2, the D230N mutation resulted in diminished sarcomere function and Ca 2 affinity. (A) Ca 2 sensitivity of thin-filament regulation of actin-tropomyosin activated myosin ATPase activity. Compared with the wild type, maximal ATPase turnover and pca 50 were significantly reduced (p 0.05) in the DCM mutant alpha-tropomyosin (D230N). In contrast, both parameters were significantly increased (p 0.05) in the HCM mutant protein (D175N). (B) Ca 2 binding to the thin filament causes a decrease in spectrofluorescent intensity. The Ca 2 affinity of reconstituted thin filaments containing D230N alpha-tropomyosin DCM mutant was significantly reduced (p 0.001) compared with wild-type alpha-tropomyosin. In contrast the D175N HCM mutant was associated with significantly increased Ca 2 affinity (p 0.05). HCM hypertrophic cardiomyopathy; other abbreviations as in Figure 2. p 0.001) and Ca 2 sensitivity (pca , n 3, p 0.05). The maximally inhibited rate at pca 8.5 ( s 1 ) was not significantly affected by the presence of the mutation. The functional impact of this TPM1 D230N mutation is strikingly different than a TPM1 mutation that causes HCM (D175N) (15). Thin filaments reconstituted with the HCM-mutant protein resulted in regulation with greater Ca 2 -sensitivity (pca , n 3, p 0.05) and increased maximum ATP turnover ( s 1,n 3, p 0.001) relative to wild-type tropomyosin (Fig. 3A). To determine whether the observed decrease in Ca 2 sensitivity of contractility was due to an actual change in Ca 2 affinity rather than an apparent change caused by altered troponin-tropomyosin switching, thin filaments were reconstituted with the use of actin, IAANS-labeled troponin C, and wild-type, D230N, or a 1:1 wild-type/ DCM-mutant mixture tropomyosin. Wild-type thin filaments bound Ca 2 with a pca 50 of with a Hill coefficient (n H ) of (Fig. 3B). In contrast, there was a dramatic decrease in the affinity of filaments containing D230N (pca ; p 0.001), and the Hill
6 JACC Vol. 55, No. 4, 2010 January 26, 2010:320 9 Lakdawala et al. Tropomyosin Mutations in DCM 325 coefficient was also significantly reduced (n H ; p 0.001) (Fig. 3B), indicating decreased cooperativity of Ca 2 binding. Experiments in which we used the 1:1 wild-type/dcm-mutant mixture also showed reduced Ca 2 affinity (pca ) and lower cooperativity (n H p 0.001) (data not shown in figure). In contrast, thin filaments reconstituted with the HCM mutant protein were found to have significantly increased Ca 2 affinity compared with wild-type tropomyosin (pca ; p 0.05), consistent with the increased Ca 2 sensitivity observed in the ATPase assay (Fig. 3B). Clinical features of TPM1 D230N. The clinical manifestations and course of DCM in families A and B are summarized in Table 1. No family members with TPM1 D230N had evidence of cardiac conduction disease, and with one exception, none had evidence of skeletal myopathy. Abnormal cardiac dimensions and contractile parameters were identified in 16 of 20 mutation carriers, indicating a penetrance of 80% for DCM in the 2 families. As seen in Figure 4, the development of DCM occurred over a wide spectrum of ages. However, there were striking differences in clinical course on the basis of age of presentation, with adverse outcomes occurring early in life (Fig. 4). Family A. Family A was notable for severe HF and sudden death in young children. Subjects I-2, III-10, and IV-7 died suddenly at ages 3 years, 13 months, and 5 months, respectively, without previous evidence of heart disease. Two siblings, IV-5 and IV-8, presented with DCM and advanced HF at 5 months of age (LVEF 27% and 29%) and were given the presumptive diagnosis of myocarditis. In IV-5, adenovirus DNA was detected by polymerase chain reaction on endomyocardial biopsy. Both had substantial recovery of LV systolic function and resolution of symptoms after receiving standard medical care at the time of presentation (digoxin and furosemide). Notably IV-8, now age 21 years, participates in marathons. Subjects III-3 and IV-1 developed end-stage HF refractory to medical therapy as teenagers. III-3 presented at age 13 with refractory HF, underwent mitral and tricuspid valve replacement for functional regurgitation, and died weeks later of multisystem organ failure before genetic testing. IV-1 was asymptomatic when diagnosed with DCM at 7 years during family screening but developed severe HF at age 17 years and underwent transplant at 18 years of age. Histologic examination of his explanted heart revealed nonspecific changes consistent with DCM, without myocyte disarray, marked fibrosis, or inflammation to suggest either end-stage HCM or myocarditis. By contrast, 4 mutation carriers who presented in adulthood had mild clinical courses. Subjects III-4, III-7, and III-12 developed mild exercise intolerance in their fifth decade. Clinical studies revealed mild-to-moderate LV systolic dysfunction and enlargement and symptoms resolved with medical management. II-6 was healthy before an inferior myocardial infarction at 71 years. She was subsequently found to have mild LV systolic dysfunction (LVEF 49%) and remains asymptomatic. Four mutation carriers (subjects III-1, IV-4, IV-11, IV-15; ages 54, 16, 22, and 8 years, respectively), had asymptomatic LV systolic dysfunction and/or enlargement. Three adult mutation carriers (III-5, III-13, IV-2), were free of symptoms and had normal LV size and systolic function. Family B. Young members of this family also presented with severe HF. Subject III-1 developed failure to thrive at 10 weeks of age and echocardiography revealed severe LV dilation (LVIDD z-score 15.6) and systolic dysfunction (LVEF 15%). Transplantation was considered, but the subject had substantial recovery with basic medical therapy. By age 8 years, she was asymptomatic with only mild LV systolic dysfunction (LVIDD z-score 1.3, LVEF 46%). At age 20 years, II-6 underwent cardiac transplantation shortly after presenting with refractory HF symptoms and severe LV systolic dysfunction (LVEF 20%). Subject II-7 died of HF at age 12 years, before genetic testing. In addition to DCM, he had congenital cataracts and skeletal muscle weakness. Post-mortem examination demonstrated cardiomegaly with marked endocardial and interstitial fibrosis. Skeletal muscle analyses demonstrated chronic myopathic changes but normal dystrophin staining and no inflammation, evidence of storage disease, tissuespecific atrophy, or fiber type grouping. As in family A, the clinical course of mutation carriers in family B identified in adulthood was far less severe. I-1 had unexplained syncope at age 56 years. Cardiac studies revealed ventricular tachycardia and DCM (LVEF 25%), which improved with medical management. Three other adults (II-2, II-3, and II-4, ages 38, 36, and 33 years, respectively) had asymptomatic LV systolic dysfunction. After an uncomplicated pregnancy, II-4 had a mild further decrease in LVEF from 48% to 39%, improving to 55% with institution of an angiotensin-converting enzyme inhibitor. Discussion We identified a D230N missense mutation in TPM1 as the cause of DCM in 2 unrelated multigenerational families. Unlike previously reported TPM1 variants (E45K, E40K) associated with DCM in isolated subjects (7), we demonstrate that dominant transmission of TPM1 D230N segregates with disease and deleteriously impacts in vitro assays of contractility, providing definitive evidence that TPM1 mutations cause DCM. Furthermore, these functional studies demonstrated that mutations in the same genes have different effects that may influence whether a phenotype of DCM or HCM develops. The clinical profile of these families suggests a pattern for sarcomeric DCM in which clinical outcomes differ dramatically on the basis of age of presentation.
7 326 Lakdawala et al. JACC Vol. 55, No. 4, 2010 Tropomyosin Mutations in DCM January 26, 2010:320 9 Clinical Table 1Characteristics Clinical Characteristics of Affected Family of Affected Members Family onmembers the Basison of the Severity Basisof ofclinical SeverityPresentation of Clinical Presentation Family Pedigree Age at Diagnosis* NYHA functional class II Current Age or Age at Death D230N Sex Clinical Features LVEF (%) LVIDD (cm)/(z-score) Comments A I-2 3 yrs NA F SCD No symptoms before SCD. No autopsy performed. A III-3 13 yrs 13 yrs NA F NYHA IV HF death Died of multisystem organ failure during HF hospitalization. A III months 13 months NA M SCD No symptoms before SCD. Autopsy notable for LV dilation. A IV-1 7 yrs 26 yrs M NYHA IV Txp A IV-5 5 months 28 yrs F NYHA IV with improvement Diagnosed during family screening and became progressively symptomatic culminating in cardiac transplantation at 18 yrs (13.2) Severe HF as an infant with improvement after medical therapy (LVEF now 50%). A IV-7 6 months 6 months NA F SCD SCD at age 6 months without previous symptoms. Autopsy reported LV dilation. A IV-8 5 months 21 yrs F NYHA IV with improvement (15.2) Severe HF as an infant with improvement after medical therapy (LVEF now 58%). B I-1 56 yrs 64 yrs F VT Presented with symptomatic VT and severe DCM, which improved with medical therapy (LVEF now 40%). B II-6 20 yrs 24 yrs M NYHA IV Txp 20 Cardiac transplantation at age 20 yrs. B II-7 9 yrs 12 yrs NA M NYHA IV HF death Presented with DCM at 9 yrs and died of HF at 12 yrs. Also had congenital cataracts and skeletal weakness. B III-1 10 weeks 8 yrs F NYHA IV (15.6) Severe HF as an infant with improvement after medical therapy (LVEF now 46%). NYHA functional class II A II-4 71 yrs F NYHA I Asymptomatic. Mildly reduced LVEF identified after myocardial infarction at 71 yrs. A III-1 54 yrs 57 yrs F NYHA I Asymptomatic but LVEF decreased during follow-up from 52% to 40%. A III-4 47 yrs 53 yrs M NYHA II Minimal exercise intolerance developed at age 48 yrs. A III-5 53 yrs F NYHA I Asymptomatic without evidence of LV enlargement or dysfunction. A III-7 45 yrs 50 yrs M NYHA II Minimal exercise intolerance developed at age 47 yrs. A III yrs 44 yrs F NYHA II Palpitations and mild LV enlargement/systolic dysfunction without exercise limitation. A III yrs F NYHA I Asymptomatic without evidence of LV enlargement or dysfunction. A IV-2 23 yrs F NYHA I Asymptomatic without evidence of LV enlargement or dysfunction. A IV-4 16 yrs 19 yrs F NYHA I Asymptomatic with mild LV enlargement. A IV yrs 24 yrs M NYHA I Asymptomatic but LVEF decreased during follow-up from 50% to 40%. A IV-15 8 yrs 11 yrs F NYHA I Asymptomatic with mildly reduced LVEF. B II-2 30 yrs 38 yrs M NYHA I Asymptomatic with mildly reduced LVEF. B II-3 32 yrs 36 yrs M NYHA I Asymptomatic but moderately reduced LVEF that decreased during follow-up from 42% to 35% with concomitant 5-mm increase in LVIDD. B II-4 31 yrs 34 yrs F NYHA I Asymptomatic but LVEF decreased after pregnancy from 48% to 39%, normalizing with medical therapy (55%). *No age provided for subjects without evidence of DCM. Age at death. DCM dilated cardiomyopathy; HF heart failure; LV left ventricular/ventricle; LVEF left ventricular ejection fraction; LVIDD left ventricular end-diastolic diameter z-score calculated for children age 16 yrs; NA not available; NYHA New York Heart Association functional class; SCD sudden cardiac death; Txp cardiac transplantation; VT ventricular tachycardia. Divergent functional consequences of sarcomere mutations may shape different patterns of cardiac remodeling. Sarcomere mutations were initially characterized as the cause of HCM but, as demonstrated in this study, can also cause DCM (6,16). The molecular mechanisms that determine whether a dilated or hypertrophic phenotype
8 JACC Vol. 55, No. 4, 2010 January 26, 2010:320 9 Lakdawala et al. Tropomyosin Mutations in DCM 327 Figure 4 Clinical Outcomes in Carriers of the D230N Alpha-Tropomyosin Mutation The presence of TPM1 D230N is associated with a high risk for developing DCM but over a wide spectrum of ages, ranging from infancy to the sixth decade (black curve). DCM includes both symptomatic and asymptomatic left ventricular systolic dilation and/or dysfunction. Severe clinical outcomes, cardiac death, and transplantation (Txp) were confined to young family members and distinctly absent from those presenting in adulthood (red curve). *Subjects who experienced cardiac death before genotyping were assumed to be mutation carriers (G ). Abbreviations as in Figure 2. develops have not been clearly elucidated. Mutation location does not appear to be critical. As shown in Figure 1, mutations that cause HCM and DCM are closely interspersed and in the same functional domains in tropomyosin. However, the in vitro functional consequences of these mutations differ. Consistent with previous reports evaluating DCM mutations in thin filament proteins (12), our results demonstrate that D230N alters Ca 2 regulation in tropomyosin by reducing Ca 2 sensitivity, maximum activation, and Ca 2 affinity. Experimental models in which the investigators used mechanically loaded cardiac muscle fibers (17) have also shown a Ca 2 -desensitizing effect of thin filament mutations. Collectively, these DCM mutations are predicted to produce a muscle intrinsically capable of producing less force at any activating Ca 2 concentration. Left ventricular dilation may represent a compensatory mechanism to maintain stroke volume in the setting of reduced contractility as the result of decreased force production and/or Ca 2 affinity associated with the TPM1 mutation. Activation of the neurohormonal axis may also occur, culminating in progressive cardiac failure. Notably, these functional changes are opposite to those observed for sarcomere mutations that ultimately give rise to HCM in which Ca 2 sensitivity is enhanced and predicted to increase contractility (12). Figure 3 illustrates this contrast. Maximum ATPase activity, Ca 2 sensitivity, and Ca 2 affinity are decreased with the D230N DCM TPM1 mutation but increased with the D175N HCM TPM1 mutation. Moreover, previous biophysical studies in which the investigators examined the thick filament demonstrated a similar pattern. Force generation and ATPase activity are decreased in myosin heavy-chain mutations associated with DCM but increased in HCM-associated mutations (18). Collectively these results suggest that fundamental differences in the functional consequences of sarcomere mutations may underlie the very disparate patterns of remodeling observed in DCM and HCM, despite an apparently common genetic etiology. We postulate that sarcomere mutations that compromise force generation may lead to a dilated phenotype, whereas a hypertrophic phenotype may arise from mutations that increase force generation. A distinctive age-dependent phenotypic profile of sarcomere mutation DCM. Consistent with previous descriptions of DCM caused by sarcomere mutations, the clinical profiles of our families differ from both HCM caused by sarcomere mutations and DCM of other genetic etiologies, neither of which are characterized by severe disease in early childhood (19,20). As illustrated in Figure 4, marked age-dependent differences in outcomes were observed in our 2 families with TPM1 mutations. Presentation early in life, from infancy to adolescence, was not uncommon and was associated with severe, sometimes lethal outcomes, including sudden cardiac death and refractory HF leading to death or transplantation. In contrast, a mild course was observed in relatives diagnosed as adults. The pattern of severe childhood but mild adult-onset disease seen with the TPM1 D230N mutation is similar to that reported with 2 other sarcomere genes, MYH7 and
9 328 Lakdawala et al. JACC Vol. 55, No. 4, 2010 Tropomyosin Mutations in DCM January 26, 2010:320 9 TNNT2 (6,16,21). Affected members of these families also demonstrated marked LV dysfunction and HF very early in life, with either striking recovery or progression to death or transplantation, whereas those identified in adulthood generally had mild disease. This clinical profile differs meaningfully from that observed in other genetic causes of DCM, such as that caused by lamin A/C or phospholamban mutations where manifestations typically do not develop until adulthood and are progressive (19,22). The mechanisms underlying the different clinical course in children and adults have not been defined; however, recognizing this pattern as a feature of sarcomere mutation DCM is important for appropriate family evaluation and intervention. Moreover, although early presentation with DCM was typically severe, there was potential for remarkable improvement because 3 of 5 affected infants with the TPM1 mutation had striking recovery of LV function. We speculate that the underlying TPM1 mutation may confer susceptibility to myocardial injury due to viral infections (e.g., myocarditis) or systemic illness that could account for the initially dramatic clinical presentations. Factors leading to the marked improvement in a subset of these children are less clear and unlikely to be related solely to receiving basic medical therapy. However, further elucidation of the mechanisms that allowed recovery in this primary genetic cardiomyopathy may provide important insights regarding the pathogenesis and management of more common secondary forms of DCM and HF. Conclusions and Clinical Implications We present robust evidence that mutations in TPM1 cause DCM and further characterization of disease pathogenesis and clinical course. In vitro functional studies provide insight into the phenotypic development of cardiomyopathy. Although sarcomere mutations are a common cause of both HCM and DCM, the functional consequences appear markedly different in these 2 diseases, with opposite effects on Ca 2 affinity, sensitivity, and contractility. These fundamental differences may play an important role in shaping the type of cardiac remodeling that arises. The pattern emerging in these and other DCM families suggests that sarcomere mutations may result in a distinctive, age-dependent clinical profile. Early presentation is associated with severe, sometimes-lethal disease, although with potential for substantial recovery. In contrast, presentation in adulthood is generally benign. These observations have several important clinical implications. In pediatriconset HF, inherited causes of cardiomyopathy often are overlooked in favor of a presumptive diagnosis of myocarditis (23), particularly if there is dramatic clinical improvement. However, in these 2 families, childhood disease was caused by the TPM1 mutation. This finding highlights the importance of considering genetic etiologies in new-onset DCM in children and the need to consider at-risk family members. Furthermore, these findings have relevance for screening families with DCM. Current guidelines for family screening in HCM recommend that formal evaluation typically begins in adolescence (24). However, the severe disease manifestations observed in young children with DCM suggest that the identification of a sarcomere mutation should prompt aggressive screening for DCM in all first degree relatives, beginning early in life. Acknowledgments The authors are grateful for the participation of these families. Reprint requests and correspondence: Dr. Carolyn Y. Ho, Brigham and Women s Hospital, 75 Francis Street, Boston, Massachusetts cho@partners.org. REFERENCES 1. Boucek MM, Aurora P, Edwards LB, et al. Registry of the International Society for Heart and Lung Transplantation: tenth official pediatric heart transplantation report J Heart Lung Transplant 2007;26: Taylor DO, Edwards LB, Boucek MM, et al. Registry of the International Society for Heart and Lung Transplantation: twentyfourth official adult heart transplant report J Heart Lung Transplant 2007;26: Burkett EL, Hershberger RE. Clinical and genetic issues in familial dilated cardiomyopathy. J Am Coll Cardiol 2005;45: Mahon NG, Murphy RT, MacRae CA, Caforio AL, Elliott PM, McKenna WJ. Echocardiographic evaluation in asymptomatic relatives of patients with dilated cardiomyopathy reveals preclinical disease. Ann Intern Med 2005;143: Ho CY, Seidman CE. A contemporary approach to hypertrophic cardiomyopathy. Circulation 2006;113:e Kamisago M, Sharma SD, DePalma SR, et al. Mutations in sarcomere protein genes as a cause of dilated cardiomyopathy. N Engl J Med 2000;343: Olson TM, Kishimoto NY, Whitby FG, Michels VV. Mutations that alter the surface charge of alpha-tropomyosin are associated with dilated cardiomyopathy. J Mol Cell Cardiol 2001;33: Monteiro PB, Lataro RC, Ferro JA, Reinach Fde C. Functional alpha-tropomyosin produced in Escherichia coli. A dipeptide extension can substitute the amino-terminal acetyl group. J Biol Chem 1994; 269: Redwood C, Lohmann K, Bing W, et al. Investigation of a truncated cardiac troponin T that causes familial hypertrophic cardiomyopathy: Ca(2 ) regulatory properties of reconstituted thin filaments depend on the ratio of mutant to wild-type protein. Circ Res 2000;86: Pardee JD, Spudich JA. Purification of muscle actin. Methods Enzymol 1982;85 Pt B: Robinson P, Mirza M, Knott A, et al. Alterations in thin filament regulation induced by a human cardiac troponin T mutant that causes dilated cardiomyopathy are distinct from those induced by troponin T mutants that cause hypertrophic cardiomyopathy. J Biol Chem 2002; 277: Robinson P, Griffiths PJ, Watkins H, Redwood CS. Dilated and hypertrophic cardiomyopathy mutations in troponin and {alpha}- tropomyosin have opposing effects on the calcium affinity of cardiac thin filaments. Circ Res 2007;101: Lang RM, Bierig M, Devereux RB, et al. Recommendations for chamber quantification: a report from the American Society of Echocardiography s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr 2005;18: Whitby FG, Phillips GN Jr. Crystal structure of tropomyosin at 7 Angstroms resolution. Proteins 2000;38:49 59.
10 JACC Vol. 55, No. 4, 2010 January 26, 2010:320 9 Lakdawala et al. Tropomyosin Mutations in DCM Thierfelder L, Watkins H, MacRae C, et al. Alpha-tropomyosin and cardiac troponin T mutations cause familial hypertrophic cardiomyopathy: a disease of the sarcomere. Cell 1994;77: Mogensen J, Murphy RT, Shaw T, et al. Severe disease expression of cardiac troponin C and T mutations in patients with idiopathic dilated cardiomyopathy. J Am Coll Cardiol 2004;44: Morimoto S, Lu QW, Harada K, et al. Ca(2 )-desensitizing effect of a deletion mutation Delta K210 in cardiac troponin T that causes familial dilated cardiomyopathy. Proc Natl Acad Sci U S A 2002;99: Debold EP, Schmitt JP, Patlak JB, et al. Hypertrophic and dilated cardiomyopathy mutations differentially affect the molecular force generation of mouse alpha-cardiac myosin in the laser trap assay. Am J Physiol Heart Circ Physiol 2007;293:H Pasotti M, Klersy C, Pilotto A, et al. Long-term outcome and risk stratification in dilated cardiolaminopathies. J Am Coll Cardiol 2008; 52: Maron BJ, Casey SA, Poliac LC, Gohman TE, Almquist AK, Aeppli DM. Clinical course of hypertrophic cardiomyopathy in a regional United States cohort. JAMA 1999;281: Villard E, Duboscq-Bidot L, Charron P, et al. Mutation screening in dilated cardiomyopathy: prominent role of the beta myosin heavy chain gene. Eur Heart J 2005;26: Schmitt JP, Kamisago M, Asahi M, et al. Dilated cardiomyopathy and heart failure caused by a mutation in phospholamban. Science 2003; 299: Towbin JA, Lowe AM, Colan SD, et al. Incidence, causes, and outcomes of dilated cardiomyopathy in children. JAMA 2006;296: Hershberger RE, Lindenfeld J, Mestroni L, Seidman CE, Taylor MR, Towbin JA. Genetic evaluation of cardiomyopathy a Heart Failure Society of America practice guideline. J Card Fail 2009;15: Key Words: cardiomyopathy y heart failure y genetics. APPENDIX For a supplemental figure and table, please see the online version of this article.
2011 HCM Guideline Data Supplements
 Data Supplement 1. Genetics Table Study Name/Author (Citation) Aim of Study Quality of life and psychological distress quality of life and in mutation psychological carriers: a crosssectional distress
Data Supplement 1. Genetics Table Study Name/Author (Citation) Aim of Study Quality of life and psychological distress quality of life and in mutation psychological carriers: a crosssectional distress
Familial DilatedCardiomyopathy Georgios K Efthimiadis, MD
 Familial DilatedCardiomyopathy Georgios K Efthimiadis, MD Dilated Cardiomyopathy Dilated LV/RV, reduced EF, in the absence of CAD valvulopathy pericardial disease Prevalence:40/100.000 persons Natural
Familial DilatedCardiomyopathy Georgios K Efthimiadis, MD Dilated Cardiomyopathy Dilated LV/RV, reduced EF, in the absence of CAD valvulopathy pericardial disease Prevalence:40/100.000 persons Natural
Hypertrophic Cardiomyopathy
 Hypertrophic Cardiomyopathy From Genetics to ECHO Alexandra A Frogoudaki Second Cardiology Department ATTIKON University Hospital Athens University Athens, Greece EUROECHO 2010, Copenhagen, 11/12/2010
Hypertrophic Cardiomyopathy From Genetics to ECHO Alexandra A Frogoudaki Second Cardiology Department ATTIKON University Hospital Athens University Athens, Greece EUROECHO 2010, Copenhagen, 11/12/2010
Clinical Genetics in Cardiomyopathies
 Clinical Genetics in Cardiomyopathies Γεώργιος Κ Ευθυμιάδης Αναπληρωτής Καθηγητής Καρδιολογίας ΑΠΘ No conflict of interest Genetic terms Proband: The first individual diagnosed in a family Mutation: A
Clinical Genetics in Cardiomyopathies Γεώργιος Κ Ευθυμιάδης Αναπληρωτής Καθηγητής Καρδιολογίας ΑΠΘ No conflict of interest Genetic terms Proband: The first individual diagnosed in a family Mutation: A
Hypertrophic Cardiomyopathy: beyond gradient and wall thickness
 Hypertrophic Cardiomyopathy: beyond gradient and wall thickness Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School no disclosures special thanks to A. Baggish 1 Hypertrophic
Hypertrophic Cardiomyopathy: beyond gradient and wall thickness Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School no disclosures special thanks to A. Baggish 1 Hypertrophic
Left ventricular non-compaction: the New Cardiomyopathy on the Block
 Left ventricular non-compaction: the New Cardiomyopathy on the Block Aamir Jeewa MB BCh, FAAP, FRCPC Section Head, Cardiomyopathy & Heart Function Program The Hospital for Sick Children Assistant Professor
Left ventricular non-compaction: the New Cardiomyopathy on the Block Aamir Jeewa MB BCh, FAAP, FRCPC Section Head, Cardiomyopathy & Heart Function Program The Hospital for Sick Children Assistant Professor
Definition and classification of the cardiomyopathies. Georgios K Efthimiadis Ass Prof of Cardiology
 Definition and classification of the cardiomyopathies Georgios K Efthimiadis Ass Prof of Cardiology Historical Context WHO: 1980 classification "heart muscle diseases of unknown cause" WHO 1995 classification
Definition and classification of the cardiomyopathies Georgios K Efthimiadis Ass Prof of Cardiology Historical Context WHO: 1980 classification "heart muscle diseases of unknown cause" WHO 1995 classification
Genotype Positive/ Phenotype Negative: Is It a Disease?
 Genotype Positive/ Phenotype Negative: Is It a Disease? Michelle Michels MD, PhD Center of Inherited Cardiovascular Diseases Erasmus MC, Rotterdam, the Netherlands No disclosures What is phenotype negative
Genotype Positive/ Phenotype Negative: Is It a Disease? Michelle Michels MD, PhD Center of Inherited Cardiovascular Diseases Erasmus MC, Rotterdam, the Netherlands No disclosures What is phenotype negative
Corporate Medical Policy
 Corporate Medical Policy Genetic Testing for Predisposition to Inherited Hypertrophic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_predisposition_to_inherited_hypertrophic_cardiomyopathy
Corporate Medical Policy Genetic Testing for Predisposition to Inherited Hypertrophic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_predisposition_to_inherited_hypertrophic_cardiomyopathy
in Familial Dilated Cardiomyopathy
 Familial Dilated Cardiomyopathy y Clinical and Genetic et Issues in Familial Dilated Cardiomyopathy College of Medicine, Chungbuk National University Kyung-Kuk Hwang Contents Definition (criteria) Clinical
Familial Dilated Cardiomyopathy y Clinical and Genetic et Issues in Familial Dilated Cardiomyopathy College of Medicine, Chungbuk National University Kyung-Kuk Hwang Contents Definition (criteria) Clinical
Preventing Sudden Death in Young Athletes. Outline. Scope of the Problem. Causes of SCD in Young Athletes. Sudden death in the young athlete
 Preventing Sudden Death in Young Athletes Ronn E. Tanel, MD Director, Pediatric Arrhythmia Service UCSF Children s Hospital Associate Professor of Pediatrics UCSF School of Medicine Outline Sudden death
Preventing Sudden Death in Young Athletes Ronn E. Tanel, MD Director, Pediatric Arrhythmia Service UCSF Children s Hospital Associate Professor of Pediatrics UCSF School of Medicine Outline Sudden death
Inherited Arrhythmia Syndromes
 Inherited Arrhythmia Syndromes When to perform Genetic testing? Arthur AM Wilde February 4, 2017 Which pts should undergo genetic testing? SCD victims with a likely diagnosis Pts diagnosed with an inherited
Inherited Arrhythmia Syndromes When to perform Genetic testing? Arthur AM Wilde February 4, 2017 Which pts should undergo genetic testing? SCD victims with a likely diagnosis Pts diagnosed with an inherited
Cardiomyopathy. ACOI IM Board Review 2018 Martin C. Burke DO, FACOI
 Cardiomyopathy ACOI IM Board Review 2018 Martin C. Burke DO, FACOI No Disclosures Cardiomyopathies Definition: diseases of heart muscle 1980 WHO: unknown causes Not clinically relevant 1995 WHO: diseases
Cardiomyopathy ACOI IM Board Review 2018 Martin C. Burke DO, FACOI No Disclosures Cardiomyopathies Definition: diseases of heart muscle 1980 WHO: unknown causes Not clinically relevant 1995 WHO: diseases
Genetic Cardiomyopathies
 2017 HFCT Annual Scientific Meeting The Heart Failure Crosstalk Genetic Cardiomyopathies Teerapat Yingchoncharoen M.D. Ramathibodi Hospital Cardiomyopathy Group of diseases of the myocardium associated
2017 HFCT Annual Scientific Meeting The Heart Failure Crosstalk Genetic Cardiomyopathies Teerapat Yingchoncharoen M.D. Ramathibodi Hospital Cardiomyopathy Group of diseases of the myocardium associated
How NOT to miss Hypertrophic Cardiomyopathy? Adaya Weissler-Snir, MD University Health Network, University of Toronto
 How NOT to miss Hypertrophic Cardiomyopathy? Adaya Weissler-Snir, MD University Health Network, University of Toronto Introduction Hypertrophic cardiomyopathy is the most common genetic cardiomyopathy,
How NOT to miss Hypertrophic Cardiomyopathy? Adaya Weissler-Snir, MD University Health Network, University of Toronto Introduction Hypertrophic cardiomyopathy is the most common genetic cardiomyopathy,
Clinical Policy Title: Genetic testing for hereditary cardiomyopathy
 Clinical Policy Title: Genetic testing for hereditary cardiomyopathy Clinical Policy Number: 02.01.21 Effective Date: October 1, 2016 Initial Review Date: August 17, 2016 Most Recent Review Date: August
Clinical Policy Title: Genetic testing for hereditary cardiomyopathy Clinical Policy Number: 02.01.21 Effective Date: October 1, 2016 Initial Review Date: August 17, 2016 Most Recent Review Date: August
Genetic Screening and Double Mutation in Japanese Patients With Hypertrophic Cardiomyopathy
 Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGIAL ARTICLE Molecular Cardiology Genetic Screening and Double Mutation in Japanese Patients With Hypertrophic
Circulation Journal Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp ORIGIAL ARTICLE Molecular Cardiology Genetic Screening and Double Mutation in Japanese Patients With Hypertrophic
Idiopathic restrictive cardiomyopathy is part of the clinical expression of cardiac troponin I mutations
 Idiopathic restrictive cardiomyopathy is part of the clinical expression of cardiac troponin I mutations See the related Commentary beginning on page 175. Jens Mogensen, 1 Toru Kubo, 1,2 Mauricio Duque,
Idiopathic restrictive cardiomyopathy is part of the clinical expression of cardiac troponin I mutations See the related Commentary beginning on page 175. Jens Mogensen, 1 Toru Kubo, 1,2 Mauricio Duque,
Restrictive Cardiomyopathy
 ESC Congress 2011, Paris Imaging Unusual Causes of Cardiomyopathy Restrictive Cardiomyopathy Kazuaki Tanabe, MD, PhD Professor of Medicine Chair, Division of Cardiology Izumo, Japan I Have No Disclosures
ESC Congress 2011, Paris Imaging Unusual Causes of Cardiomyopathy Restrictive Cardiomyopathy Kazuaki Tanabe, MD, PhD Professor of Medicine Chair, Division of Cardiology Izumo, Japan I Have No Disclosures
Treatment of Hypertrophic Cardiomyopathy in Bruce B. Reid, MD
 Treatment of Hypertrophic Cardiomyopathy in 2017 Bruce B. Reid, MD Disclosures I have no conflicts of interest to disclose I will not be discussing any off label medications and/or devices Objectives 1)
Treatment of Hypertrophic Cardiomyopathy in 2017 Bruce B. Reid, MD Disclosures I have no conflicts of interest to disclose I will not be discussing any off label medications and/or devices Objectives 1)
Cardiovascular Topics
 146 CARDIOVASCULAR JOURNAL OF AFRICA Vol 18, No. 3, May/June 2007 Cardiovascular Topics Long-term follow-up of R403W MYH7 and R92W TNNT2 HCM families: mutations determine left ventricular dimensions but
146 CARDIOVASCULAR JOURNAL OF AFRICA Vol 18, No. 3, May/June 2007 Cardiovascular Topics Long-term follow-up of R403W MYH7 and R92W TNNT2 HCM families: mutations determine left ventricular dimensions but
Mutations and Disease Mutations in the Myosin Gene
 Biological Sciences Initiative HHMI Mutations and Disease Mutations in the Myosin Gene Goals Explore how mutations can lead to disease using the myosin gene as a model system. Explore how changes in the
Biological Sciences Initiative HHMI Mutations and Disease Mutations in the Myosin Gene Goals Explore how mutations can lead to disease using the myosin gene as a model system. Explore how changes in the
Update in Cardiomyopathies: Their New Classifications and Importance of Mixed Phenotypes
 Update in Cardiomyopathies: Their New Classifications and Importance of Mixed Phenotypes Andre Keren MD Hadassah-Hebrew University Hospital, Jerusalem Cesarea, 2008 f o s r a es e y t hi 0 a 5 p t o rs
Update in Cardiomyopathies: Their New Classifications and Importance of Mixed Phenotypes Andre Keren MD Hadassah-Hebrew University Hospital, Jerusalem Cesarea, 2008 f o s r a es e y t hi 0 a 5 p t o rs
Clinical Policy Title: Genetic testing for hereditary cardiomyopathy
 Clinical Policy Title: Genetic testing for hereditary cardiomyopathy Clinical Policy Number: 02.01.24 Effective Date: October 1, 2016 Initial Review Date: August 17, 2016 Most Recent Review Date: August
Clinical Policy Title: Genetic testing for hereditary cardiomyopathy Clinical Policy Number: 02.01.24 Effective Date: October 1, 2016 Initial Review Date: August 17, 2016 Most Recent Review Date: August
4/11/2017. Cardiomyopathy. John Steuter, MD Bryan Heart. Disclosures. No Conflicts. Cardiomyopathy. WHO Classification
 Cardiomyopathy John Steuter, MD Bryan Heart Disclosures No Conflicts Cardiomyopathy WHO Classification Anatomy & physiology of the LV 1. Dilated Enlarged Systolic dysfunction 2. Hypertrophic Thickened
Cardiomyopathy John Steuter, MD Bryan Heart Disclosures No Conflicts Cardiomyopathy WHO Classification Anatomy & physiology of the LV 1. Dilated Enlarged Systolic dysfunction 2. Hypertrophic Thickened
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers MANAGEMENT
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers MANAGEMENT
Contribution of genetics for sudden death risk stratification in dilated cardiomyopathy
 Contribution of genetics for sudden death risk stratification in dilated cardiomyopathy Pr Philippe Charron Centre de Référence pour les maladies cardiaques héréditaires (1) Hôpital Ambroise Paré, Boulogne
Contribution of genetics for sudden death risk stratification in dilated cardiomyopathy Pr Philippe Charron Centre de Référence pour les maladies cardiaques héréditaires (1) Hôpital Ambroise Paré, Boulogne
Journal of the American College of Cardiology Vol. 38, No. 2, by the American College of Cardiology ISSN /01/$20.
 Journal of the American College of Cardiology Vol. 38, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(01)01386-9 CLINICAL
Journal of the American College of Cardiology Vol. 38, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(01)01386-9 CLINICAL
In Vivo Animal Models of Heart Disease. Why Animal Models of Disease? Timothy A Hacker, PhD Department of Medicine University of Wisconsin-Madison
 In Vivo Animal Models of Heart Disease Timothy A Hacker, PhD Department of Medicine University of Wisconsin-Madison Why Animal Models of Disease? Heart Failure (HF) Leading cause of morbidity and mortality
In Vivo Animal Models of Heart Disease Timothy A Hacker, PhD Department of Medicine University of Wisconsin-Madison Why Animal Models of Disease? Heart Failure (HF) Leading cause of morbidity and mortality
Declaration of conflict of interest. I have nothing to disclose.
 Declaration of conflict of interest I have nothing to disclose. Left Bundle branch block in HF: DO GENETICS MATTER? Silvia Giuliana Priori Cardiovascular Genetics, Langone Medical Center, New York University
Declaration of conflict of interest I have nothing to disclose. Left Bundle branch block in HF: DO GENETICS MATTER? Silvia Giuliana Priori Cardiovascular Genetics, Langone Medical Center, New York University
ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above) YES (Proceed to Stage II)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: TNNT2, LMNA HGNC ID: 11949, 6636 ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition?
Stage I: Rule-Out Dashboard GENE/GENE PANEL: TNNT2, LMNA HGNC ID: 11949, 6636 ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition?
Managing Hypertrophic Cardiomyopathy with Imaging. Gisela C. Mueller University of Michigan Department of Radiology
 Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
2, 6, 3, 7, 8, 9, 10, 5
 A novel regulatory element in cardiac muscle troponin T. Striated muscle contraction is regulated by the position of tropomyosin on actin. That position, in turn, is regulated by the troponin complex (troponin
A novel regulatory element in cardiac muscle troponin T. Striated muscle contraction is regulated by the position of tropomyosin on actin. That position, in turn, is regulated by the troponin complex (troponin
Citation for published version (APA): Christiaans, I. (2010). Hypertrophic cardiomyopathy: towards an optimal strategy
 UvA-DARE (Digital Academic Repository) Hypertrophic cardiomyopathy: towards an optimal strategy Christiaans, I. Link to publication Citation for published version (APA): Christiaans, I. (2010). Hypertrophic
UvA-DARE (Digital Academic Repository) Hypertrophic cardiomyopathy: towards an optimal strategy Christiaans, I. Link to publication Citation for published version (APA): Christiaans, I. (2010). Hypertrophic
1. Cardiomyocytes and nonmyocyte. 2. Extracellular Matrix 3. Vessels שאלה 1. Pathobiology of Heart Failure Molecular and Cellular Mechanism
 Pathobiology of Heart Failure Molecular and Cellular Mechanism Jonathan Leor Neufeld Cardiac Research Institute Tel-Aviv University Sheba Medical Center, Tel-Hashomer שאלה 1 התא הנפוץ ביותר (75%~) בלב
Pathobiology of Heart Failure Molecular and Cellular Mechanism Jonathan Leor Neufeld Cardiac Research Institute Tel-Aviv University Sheba Medical Center, Tel-Hashomer שאלה 1 התא הנפוץ ביותר (75%~) בלב
Genetic testing in Cardiomyopathies
 Genetic testing in Cardiomyopathies Silvia Giuliana Priori Cardiovascular Genetics, Langone Medical Center, New York University School of Medicine, New York, USA and Molecular Cardiology, IRCCS Fondazione
Genetic testing in Cardiomyopathies Silvia Giuliana Priori Cardiovascular Genetics, Langone Medical Center, New York University School of Medicine, New York, USA and Molecular Cardiology, IRCCS Fondazione
YES NO UNKNOWN. Stage I: Rule-Out Dashboard Secondary Findings in Adults ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS
 Stage I: Rule-Out Dashboard HGNC ID: 11949, 6636, 2928 OMIM ID: 191045, 150330, 302045 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource, such as a practice guideline or systematic review, for
Stage I: Rule-Out Dashboard HGNC ID: 11949, 6636, 2928 OMIM ID: 191045, 150330, 302045 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource, such as a practice guideline or systematic review, for
Pioneering Precision Cardiovascular Medicine. (NASDAQ: MYOK) Corporate Presentation March 2018
 Pioneering Precision Cardiovascular Medicine (NASDAQ: MYOK) Corporate Presentation March 2018 Forward-Looking Statements Statements we make in this presentation may include statements which are not historical
Pioneering Precision Cardiovascular Medicine (NASDAQ: MYOK) Corporate Presentation March 2018 Forward-Looking Statements Statements we make in this presentation may include statements which are not historical
Investigating the family after a sudden cardiac death. Dr Catherine Mercer Consultant Clinical Geneticist, Wessex
 Investigating the family after a sudden cardiac death Dr Catherine Mercer Consultant Clinical Geneticist, Wessex Sudden adult deaths subdivided Sudden Adult Death Sudden Cardiac Death Sudden Arrhythmic
Investigating the family after a sudden cardiac death Dr Catherine Mercer Consultant Clinical Geneticist, Wessex Sudden adult deaths subdivided Sudden Adult Death Sudden Cardiac Death Sudden Arrhythmic
Cardiac Sarcoidosis. Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar
 Cardiac Sarcoidosis Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar Introduction Multisystem granulomatous disease of unknown etiology characterized by noncaseating granulomas in
Cardiac Sarcoidosis Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar Introduction Multisystem granulomatous disease of unknown etiology characterized by noncaseating granulomas in
Εμφύτευση απινιδωτών για πρωτογενή πρόληψη σε ασθενείς που δεν περιλαμβάνονται στις κλινικές μελέτες
 Εμφύτευση απινιδωτών για πρωτογενή πρόληψη σε ασθενείς που δεν περιλαμβάνονται στις κλινικές μελέτες Δημήτριος M. Κωνσταντίνου Ειδικός Καρδιολόγος, MD, MSc, PhD, CCDS Πανεπιστημιακός Υπότροφος Dr. Konstantinou
Εμφύτευση απινιδωτών για πρωτογενή πρόληψη σε ασθενείς που δεν περιλαμβάνονται στις κλινικές μελέτες Δημήτριος M. Κωνσταντίνου Ειδικός Καρδιολόγος, MD, MSc, PhD, CCDS Πανεπιστημιακός Υπότροφος Dr. Konstantinou
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association
 Genetic Testing for Predisposition to Page 1 of 12 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Genetic Testing for Predisposition to Inherited Hypertrophic
Genetic Testing for Predisposition to Page 1 of 12 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association Title: Genetic Testing for Predisposition to Inherited Hypertrophic
Hypertrophic Cardiomyopathy
 Hypertrophic Cardiomyopathy A Presentation for the MUD meeting January, 2018 Reviewed by Bill Rooney MD VP/Medical Director 1 https://commons.wikimedia.org/wiki/file:blausen_0166_cardiomyopathy_hypertrophic.p
Hypertrophic Cardiomyopathy A Presentation for the MUD meeting January, 2018 Reviewed by Bill Rooney MD VP/Medical Director 1 https://commons.wikimedia.org/wiki/file:blausen_0166_cardiomyopathy_hypertrophic.p
Risk prediction in inherited conditions Laminopathies
 Risk prediction in inherited conditions Laminopathies Karim Wahbi Cochin hospital, Paris karim.wahbi@aphp.fr Risk prediction in laminopathies Current approach for risk stratification A new score to predict
Risk prediction in inherited conditions Laminopathies Karim Wahbi Cochin hospital, Paris karim.wahbi@aphp.fr Risk prediction in laminopathies Current approach for risk stratification A new score to predict
Ventricular Tachycardia Ablation. Saverio Iacopino, MD, FACC, FESC
 Ventricular Tachycardia Ablation Saverio Iacopino, MD, FACC, FESC ü Ventricular arrhythmias, both symptomatic and asymptomatic, are common, but syncope and SCD are infrequent initial manifestations of
Ventricular Tachycardia Ablation Saverio Iacopino, MD, FACC, FESC ü Ventricular arrhythmias, both symptomatic and asymptomatic, are common, but syncope and SCD are infrequent initial manifestations of
Hypertrophic Cardiomyopathy: Patient Management in 2018
 Hypertrophic Cardiomyopathy: Patient Management in 2018 Mackram F. Eleid, MD Giornate Cardiologeche Torinesi October 26, 2018 2018 MFMER slide-1 Disclosures No relevant financial relationships to disclose
Hypertrophic Cardiomyopathy: Patient Management in 2018 Mackram F. Eleid, MD Giornate Cardiologeche Torinesi October 26, 2018 2018 MFMER slide-1 Disclosures No relevant financial relationships to disclose
Case 1: Clinical history
 United State Canadian Specialty Conference Pediatric Pathology February 26, 2011 David Parham, MD University of Oklahoma Case 1 Case 1: Clinical history 2 year, 3 month old African American male admitted
United State Canadian Specialty Conference Pediatric Pathology February 26, 2011 David Parham, MD University of Oklahoma Case 1 Case 1: Clinical history 2 year, 3 month old African American male admitted
Arrhythmogenic Cardiomyopathy cases. Δέσποινα Παρχαρίδου Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογική κλινική ΑΧΕΠΑ
 Arrhythmogenic Cardiomyopathy cases Δέσποινα Παρχαρίδου Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογική κλινική ΑΧΕΠΑ Definition ARVD (Arrhythmogenic Right Ventricular Dysplasia) Progressive loss of
Arrhythmogenic Cardiomyopathy cases Δέσποινα Παρχαρίδου Καρδιολόγος Επιστημονικός Συνεργάτης Α Καρδιολογική κλινική ΑΧΕΠΑ Definition ARVD (Arrhythmogenic Right Ventricular Dysplasia) Progressive loss of
Cardiomyopathy in Fabry s disease
 Cardiomyopathy in Fabry s disease Herzinsuffizienzlunch Basel, 11.09.2018 Christiane Gruner Kardiologie, UniversitätsSpital Zürich Content Background / epidemiology Differential diagnosis Clinical presentations
Cardiomyopathy in Fabry s disease Herzinsuffizienzlunch Basel, 11.09.2018 Christiane Gruner Kardiologie, UniversitätsSpital Zürich Content Background / epidemiology Differential diagnosis Clinical presentations
University of Groningen. Inherited Cardiomyopathies Spaendonck-Zwarts, Karin Yvon van
 University of Groningen Inherited Cardiomyopathies Spaendonck-Zwarts, Karin Yvon van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
University of Groningen Inherited Cardiomyopathies Spaendonck-Zwarts, Karin Yvon van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
D ilated cardiomyopathy is a primary myocardial disorder
 757 CARDIOVASCULAR MEDICINE Progression of familial and non-familial dilated cardiomyopathy: long term follow up V V Michels, D J Driscoll, F A Miller, T M Olson, E J Atkinson, C L Olswold, D J Schaid...
757 CARDIOVASCULAR MEDICINE Progression of familial and non-familial dilated cardiomyopathy: long term follow up V V Michels, D J Driscoll, F A Miller, T M Olson, E J Atkinson, C L Olswold, D J Schaid...
Cardiomyopathies. Andre Keren, MD
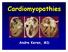 Cardiomyopathies Andre Keren, MD Cardiomyopathies Heart muscle disease of unknown etiology Elliott P et al. Eur Heart J 2008;29:270-276 Definition of Cardiomyopathies Elliott P et al. Eur Heart J 2008;29:270-276
Cardiomyopathies Andre Keren, MD Cardiomyopathies Heart muscle disease of unknown etiology Elliott P et al. Eur Heart J 2008;29:270-276 Definition of Cardiomyopathies Elliott P et al. Eur Heart J 2008;29:270-276
The State of the Molecular Autopsy for Sudden Death in the Young
 The State of the Molecular Autopsy for Sudden Death in the Young Michael J. Ackerman, MD, PhD Windland Smith Rice Cardiovascular Genomics Research Professor Professor of Medicine, Pediatrics, and Pharmacology
The State of the Molecular Autopsy for Sudden Death in the Young Michael J. Ackerman, MD, PhD Windland Smith Rice Cardiovascular Genomics Research Professor Professor of Medicine, Pediatrics, and Pharmacology
Research Article Cardiac Troponin T (TNNT2) Mutations in Chinese Dilated Cardiomyopathy Patients
 BioMed Research International, Article ID 907360, 7 pages http://dx.doi.org/10.1155/2014/907360 Research Article Cardiac Troponin T (TNNT2) Mutations in Chinese Dilated Cardiomyopathy Patients Xiaoping
BioMed Research International, Article ID 907360, 7 pages http://dx.doi.org/10.1155/2014/907360 Research Article Cardiac Troponin T (TNNT2) Mutations in Chinese Dilated Cardiomyopathy Patients Xiaoping
UvA-DARE (Digital Academic Repository) Genetic basis of hypertrophic cardiomyopathy Bos, J.M. Link to publication
 UvA-DARE (Digital Academic Repository) Genetic basis of hypertrophic cardiomyopathy Bos, J.M. Link to publication Citation for published version (APA): Bos, J. M. (2010). Genetic basis of hypertrophic
UvA-DARE (Digital Academic Repository) Genetic basis of hypertrophic cardiomyopathy Bos, J.M. Link to publication Citation for published version (APA): Bos, J. M. (2010). Genetic basis of hypertrophic
Steel vs Alcohol. Or Neither. Management of Hypertrophic Cardiomyopathy. Josh Doll, MD January 24, 2015
 Steel vs Alcohol Or Neither Management of Hypertrophic Cardiomyopathy Josh Doll, MD January 24, 2015 47yo Male, Mr. L Severe progressive dyspnea on exertion and weight gain Previous avid Cross-Fit participant
Steel vs Alcohol Or Neither Management of Hypertrophic Cardiomyopathy Josh Doll, MD January 24, 2015 47yo Male, Mr. L Severe progressive dyspnea on exertion and weight gain Previous avid Cross-Fit participant
HCM GENETIC OR CLINICAL FAMILY SCREENING?
 HCM GENETIC OR CLINICAL FAMILY SCREENING? Division of Inherited Cardiac Diseases Heart Center for the Young and Athletes A Dpt of Cardiology University of Athens GENETICS IN HCM DIAGNOSIS GENETIC RECOMFIRMATION
HCM GENETIC OR CLINICAL FAMILY SCREENING? Division of Inherited Cardiac Diseases Heart Center for the Young and Athletes A Dpt of Cardiology University of Athens GENETICS IN HCM DIAGNOSIS GENETIC RECOMFIRMATION
Methods We thoroughly searched these genes to find the mutations in 38 probands of unrelated families with familial HCM.
 Progress in Cardiology Different expressivity of a ventricular essential myosin light chain gene Ala57Gly mutation in familial hypertrophic cardiomyopathy Won-Ha Lee, PhD, a Tae Hong Hwang, MS, a Akinori
Progress in Cardiology Different expressivity of a ventricular essential myosin light chain gene Ala57Gly mutation in familial hypertrophic cardiomyopathy Won-Ha Lee, PhD, a Tae Hong Hwang, MS, a Akinori
Underwriting Inherited or Acquired Cardiomyopathies
 19 Underwriting Inherited or Acquired Cardiomyopathies Andrea Di Lenarda, Patrizia Marocco, Giulia Barbati *, Marco Merlo*, Marco Anzini*, Andrea Perkan*, Francesca Cettolo*, Bruno Pinamonti*, Gianfranco
19 Underwriting Inherited or Acquired Cardiomyopathies Andrea Di Lenarda, Patrizia Marocco, Giulia Barbati *, Marco Merlo*, Marco Anzini*, Andrea Perkan*, Francesca Cettolo*, Bruno Pinamonti*, Gianfranco
What s new in Hypertrophic Cardiomyopathy?
 What s new in Hypertrophic Cardiomyopathy? Dr Andris Ellims HCM Clinic @ The Alfred Hypertrophic Cardiomyopathy = otherwise unexplained LV hypertrophy* 1 in 500 prevalence most common inherited cardiovascular
What s new in Hypertrophic Cardiomyopathy? Dr Andris Ellims HCM Clinic @ The Alfred Hypertrophic Cardiomyopathy = otherwise unexplained LV hypertrophy* 1 in 500 prevalence most common inherited cardiovascular
Cardiomyopathy. Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement
 Cardiomyopathy Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement Nebraska Home Office Life Underwriters Association March 20, 2018 1 Cardiomyopathy A myocardial disorder in which
Cardiomyopathy Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement Nebraska Home Office Life Underwriters Association March 20, 2018 1 Cardiomyopathy A myocardial disorder in which
Πρόληψη του ΑΚΘ σε ασθενείς με μη-ισχαιμική μυοκαρδιοπάθεια:
 Πρόληψη του ΑΚΘ σε ασθενείς με μη-ισχαιμική μυοκαρδιοπάθεια: Νεώτερα δεδομένα στη διαστρωμάτωση κινδύνου Εμμ. Μ. Κανουπάκης MD, PhD, FESC Πανεπιστημιακό Νοσοκομείο Ηρακλείου NIDCM Presence of LV dilatation
Πρόληψη του ΑΚΘ σε ασθενείς με μη-ισχαιμική μυοκαρδιοπάθεια: Νεώτερα δεδομένα στη διαστρωμάτωση κινδύνου Εμμ. Μ. Κανουπάκης MD, PhD, FESC Πανεπιστημιακό Νοσοκομείο Ηρακλείου NIDCM Presence of LV dilatation
HST.161 Molecular Biology and Genetics in Modern Medicine Fall 2007
 MIT OpenCourseWare http://ocw.mit.edu HST.161 Molecular Biology and Genetics in Modern Medicine Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms.
MIT OpenCourseWare http://ocw.mit.edu HST.161 Molecular Biology and Genetics in Modern Medicine Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms.
A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH
 A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH 1* Paul Leeson, PhD, FRCP and 1 Adam J. Lewandowski, DPhil 1 Oxford Cardiovascular Clinical Research Facility, Division of Cardiovascular Medicine,
A NEW RISK FACTOR FOR EARLY HEART FAILURE: PRETERM BIRTH 1* Paul Leeson, PhD, FRCP and 1 Adam J. Lewandowski, DPhil 1 Oxford Cardiovascular Clinical Research Facility, Division of Cardiovascular Medicine,
Pathophysiology: Heart Failure
 Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations
 Sports Cardiology Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations Domenico Corrado, MD, PhD Inherited Arrhytmogenic Cardiomyopathy Unit Department of Cardiac, Thoracic and
Sports Cardiology Sudden Cardiac Death in Sports: Causes and Current Screening Recommendations Domenico Corrado, MD, PhD Inherited Arrhytmogenic Cardiomyopathy Unit Department of Cardiac, Thoracic and
Thin Filament Mutations: Developing an Integrative Approach to a Complex Disorder
 This Review is part of a thematic series on The Molecular Basis for Familial Hypertrophic Cardiomyopathy, which includes the following articles: A Personal History: Identifying the Sarcomeric Genes As
This Review is part of a thematic series on The Molecular Basis for Familial Hypertrophic Cardiomyopathy, which includes the following articles: A Personal History: Identifying the Sarcomeric Genes As
The Athlete s Heart. Role of Echo. Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University
 The Athlete s Heart Role of Echo Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. Disclosures Grant support (to institution) for Core
The Athlete s Heart Role of Echo Neil J. Weissman, MD MedStar Health Research Institute & Professor of Medicine Georgetown University Washington, D.C. Disclosures Grant support (to institution) for Core
Cardiomyopathies with Mixed and Inapparent Morphological Features in Cardiac Troponin I3 Mutation
 ase Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean irculation Journal ardiomyopathies with Mixed and Inapparent Morphological Features in ardiac Troponin I3 Mutation Dae-Won Sohn, MD 1, Hyung-Kwan
ase Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean irculation Journal ardiomyopathies with Mixed and Inapparent Morphological Features in ardiac Troponin I3 Mutation Dae-Won Sohn, MD 1, Hyung-Kwan
Journal of the American College of Cardiology Vol. 46, No. 9, by the American College of Cardiology Foundation ISSN /05/$30.
 Journal of the American College of Cardiology Vol. 46, No. 9, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.05.087
Journal of the American College of Cardiology Vol. 46, No. 9, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.05.087
The diseases hypertrophic cardiomyopathy (HCM) and
 Dilated and Hypertrophic Cardiomyopathy Mutations in Troponin and -Tropomyosin Have Opposing Effects on the Calcium Affinity of Cardiac Thin Filaments Paul Robinson, Peter J. Griffiths, Hugh Watkins, Charles
Dilated and Hypertrophic Cardiomyopathy Mutations in Troponin and -Tropomyosin Have Opposing Effects on the Calcium Affinity of Cardiac Thin Filaments Paul Robinson, Peter J. Griffiths, Hugh Watkins, Charles
SEMINAIRES IRIS. Sudden cardiac death in the adult. Gian Battista Chierchia. Heart Rhythm Management Center, UZ Brussel. 20% 25% Cancers !
 Sudden cardiac death in the adult Gian Battista Chierchia. Heart Rhythm Management Center, UZ Brussel.! " # $ % Cancers National Vital Statistics Report, Vol 49 (11), Oct. 12, 2001. 20% 25% State-specific
Sudden cardiac death in the adult Gian Battista Chierchia. Heart Rhythm Management Center, UZ Brussel.! " # $ % Cancers National Vital Statistics Report, Vol 49 (11), Oct. 12, 2001. 20% 25% State-specific
Echo assessment of the failing heart
 Echo assessment of the failing heart Mark K. Friedberg, MD The Labatt Family Heart Center The Hospital for Sick Children Toronto, Ontario, Canada Cardiac function- definitions Cardiovascular function:
Echo assessment of the failing heart Mark K. Friedberg, MD The Labatt Family Heart Center The Hospital for Sick Children Toronto, Ontario, Canada Cardiac function- definitions Cardiovascular function:
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT JANUARY 24, 2012
 IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
ESSENTIAL MESSAGES FROM ESC GUIDELINES
 ESSENTIAL MESSAGES FROM ESC GUIDELINES Committee for Practice Guidelines To improve the quality of clinical practice and patient care in Europe HCM GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF HYPERTROPHIC
ESSENTIAL MESSAGES FROM ESC GUIDELINES Committee for Practice Guidelines To improve the quality of clinical practice and patient care in Europe HCM GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF HYPERTROPHIC
Key determinants of pathogenicity
 Key determinants of pathogenicity Session 6: Determining pathogenicity and genotype-phenotype correlation J. Peter van Tintelen MD PhD Clinical geneticist Academic Medical Center Amsterdam, the Netherlands
Key determinants of pathogenicity Session 6: Determining pathogenicity and genotype-phenotype correlation J. Peter van Tintelen MD PhD Clinical geneticist Academic Medical Center Amsterdam, the Netherlands
Tetralogy of Fallot Latest data in risk stratification and replacement of pulmonic valve
 Tetralogy of Fallot Latest data in risk stratification and replacement of pulmonic valve Alexandra A Frogoudaki Adult Congenital Heart Clinic Second Cardiology Department ATTIKON University Hospital No
Tetralogy of Fallot Latest data in risk stratification and replacement of pulmonic valve Alexandra A Frogoudaki Adult Congenital Heart Clinic Second Cardiology Department ATTIKON University Hospital No
U N I V E R S I T Ä T S M E D I Z I N B E R L I N CBF KARDIOLOGIE
 U N I V E R S I T Ä T S M E D I Z I N B E R L I N I have nothing to disclose. Case 2 A Case of acute heart failure 54 year old female Patient with acute heart failure and ventricular tachycardia 53 year
U N I V E R S I T Ä T S M E D I Z I N B E R L I N I have nothing to disclose. Case 2 A Case of acute heart failure 54 year old female Patient with acute heart failure and ventricular tachycardia 53 year
Athlete s Heart vs. Cardiomyopathy
 Athlete s Heart vs. Cardiomyopathy Linda D. Gillam, MD, MPH, FASE Chair, Department of Cardiovascular Medicine Medical Director, Cardiovascular Service Line Former Team Cardiologist to the New York Jets
Athlete s Heart vs. Cardiomyopathy Linda D. Gillam, MD, MPH, FASE Chair, Department of Cardiovascular Medicine Medical Director, Cardiovascular Service Line Former Team Cardiologist to the New York Jets
Hypertrophic Cardiomyopathy
 019-CardioCase:019-CardioCase 4/16/07 1:39 PM Page 19 Hypertrophic Cardiomyopathy Abdullah Alshehri, MD; and Andrew Ignaszewski, MD, FRCPC CardioCase presentation Presley s check-up Presley, 37, discovered
019-CardioCase:019-CardioCase 4/16/07 1:39 PM Page 19 Hypertrophic Cardiomyopathy Abdullah Alshehri, MD; and Andrew Ignaszewski, MD, FRCPC CardioCase presentation Presley s check-up Presley, 37, discovered
Hypertrophic cardiomyopathy: from molecular and genetic mechanisms to clinical management
 European Heart Journal Supplements (2001) 3 (Supplement L), L43 L50 Hypertrophic cardiomyopathy: from molecular and genetic mechanisms to clinical management Department of Cardiovascular Medicine, University
European Heart Journal Supplements (2001) 3 (Supplement L), L43 L50 Hypertrophic cardiomyopathy: from molecular and genetic mechanisms to clinical management Department of Cardiovascular Medicine, University
The Causes of Heart Failure
 The Causes of Heart Failure Andy Birchall HFSN Right heart failure LVSD - HFREF Valve regurgitation or stenosis Dropsy CCF congestive cardiac failure Cor pulmonale Pulmonary hypertension HFPEF LVF Definitions
The Causes of Heart Failure Andy Birchall HFSN Right heart failure LVSD - HFREF Valve regurgitation or stenosis Dropsy CCF congestive cardiac failure Cor pulmonale Pulmonary hypertension HFPEF LVF Definitions
Cardiac Issues in the Adolescent Athlete. Sean Levchuck, M.D. St. Francis Hospital- The Heart Center
 Cardiac Issues in the Adolescent Athlete Sean Levchuck, M.D. St. Francis Hospital- The Heart Center Sudden Cardiac Death Incidence is.6-6.2 % per 100,000 children in the US 20-25 % of the deaths occur
Cardiac Issues in the Adolescent Athlete Sean Levchuck, M.D. St. Francis Hospital- The Heart Center Sudden Cardiac Death Incidence is.6-6.2 % per 100,000 children in the US 20-25 % of the deaths occur
The Genetics of Cardiomyopathy CE Seidman, MD
 The Genetics of Cardiomyopathy CE Seidman, MD Cardiomyopathies arise as primary and enigmatic disorders of the myocardium or secondary to established cardiovascular disease, such as chronic ischemia, hypertension,
The Genetics of Cardiomyopathy CE Seidman, MD Cardiomyopathies arise as primary and enigmatic disorders of the myocardium or secondary to established cardiovascular disease, such as chronic ischemia, hypertension,
Hypertrophic Cardiomyopathy: basics and management
 Hypertrophic Cardiomyopathy: basics and management Bette Kim, MD Program Director, Cardiomyopathy Program Director, Roosevelt Hospital Echocardiography Lab Assistant Professor of Clinical Medicine Mount
Hypertrophic Cardiomyopathy: basics and management Bette Kim, MD Program Director, Cardiomyopathy Program Director, Roosevelt Hospital Echocardiography Lab Assistant Professor of Clinical Medicine Mount
DIAGNOSIS AND MANAGEMENT OF ARRHYTHMOGENIC CARDIOMYOPATHY. David SIU MD ( 蕭頌華醫生 ) Division of Cardiology The University of Hong Kong
 APHRS Summit 2018 in conjunction with HKCC Heart Rhythm Refresher Course DIAGNOSIS AND MANAGEMENT OF ARRHYTHMOGENIC CARDIOMYOPATHY David SIU MD ( 蕭頌華醫生 ) Division of Cardiology The University of Hong Kong
APHRS Summit 2018 in conjunction with HKCC Heart Rhythm Refresher Course DIAGNOSIS AND MANAGEMENT OF ARRHYTHMOGENIC CARDIOMYOPATHY David SIU MD ( 蕭頌華醫生 ) Division of Cardiology The University of Hong Kong
HYPERTROPHIC CARDIOMYOPATHY RISK STRATIFICATION WHAT IS NEW?
 HYPERTROPHIC CARDIOMYOPATHY RISK STRATIFICATION WHAT IS NEW? Division of Inherited Cardiac Diseases Heart Center for the Young and Athletes A Dpt of Cardiology University of Athens LANCET 2013 ESC HCM
HYPERTROPHIC CARDIOMYOPATHY RISK STRATIFICATION WHAT IS NEW? Division of Inherited Cardiac Diseases Heart Center for the Young and Athletes A Dpt of Cardiology University of Athens LANCET 2013 ESC HCM
Clinical Utilization and Function of Tissue Doppler Imaging in Detecting Congenital Cardiomyopathies
 618221JDMXXX10.1177/8756479315618221Journal of Diagnostic Medical SonographyAlexander research-article2015 Literature Review Clinical Utilization and Function of Tissue Doppler Imaging in Detecting Congenital
618221JDMXXX10.1177/8756479315618221Journal of Diagnostic Medical SonographyAlexander research-article2015 Literature Review Clinical Utilization and Function of Tissue Doppler Imaging in Detecting Congenital
Sports Participation in Patients with Inherited Diseases of the Aorta
 Sports Participation in Patients with Inherited Diseases of the Aorta Yonatan Buber, MD Adult Congenital Heart Service Leviev Heart Center Safra Childrens Hospital Disclosures None Patient Presentation
Sports Participation in Patients with Inherited Diseases of the Aorta Yonatan Buber, MD Adult Congenital Heart Service Leviev Heart Center Safra Childrens Hospital Disclosures None Patient Presentation
CT for Myocardial Characterization of Cardiomyopathy. Byoung Wook Choi, Yonsei University Severance Hospital, Seoul, Korea
 CT for Myocardial Characterization of Cardiomyopathy Byoung Wook Choi, Yonsei University Severance Hospital, Seoul, Korea Cardiomyopathy Elliott P et al. Eur Heart J 2008;29:270-276 The European Society
CT for Myocardial Characterization of Cardiomyopathy Byoung Wook Choi, Yonsei University Severance Hospital, Seoul, Korea Cardiomyopathy Elliott P et al. Eur Heart J 2008;29:270-276 The European Society
Outline. Pathophysiology: Heart Failure. Heart Failure. Heart Failure: Definitions. Etiologies. Etiologies
 Outline Pathophysiology: Mat Maurer, MD Irving Assistant Professor of Medicine Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology : Definitions An inability of the
Outline Pathophysiology: Mat Maurer, MD Irving Assistant Professor of Medicine Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology : Definitions An inability of the
HFpEF. April 26, 2018
 HFpEF April 26, 2018 (J Am Coll Cardiol 2017;70:2476 86) HFpEF 50% or more (40-71%) of patients with CHF have preserved LV systolic function. HFpEF is an increasingly frequent hospital discharge. Outcomes
HFpEF April 26, 2018 (J Am Coll Cardiol 2017;70:2476 86) HFpEF 50% or more (40-71%) of patients with CHF have preserved LV systolic function. HFpEF is an increasingly frequent hospital discharge. Outcomes
CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE. Dr. Bahar Naghavi
 2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
Cardiomyopathy. Cardiomyopathies HOCM. Hypertrophic Obstructive Cardiomyopathy. Systolic Anterior Movement (SAM) of Mitral Valve (Venturi Effect) Cine
 Jens Bremerich Radiology University Hospital Basel Hypertrophic Obstructive Cine VENC Cine (5m/s) Modified Bernoulli Equation: P (in mmhg) = 4 x (Vmax)2 Vmax= 4.2 m/s, P = 70mm Hg Hydrodynamica 738 HOCM
Jens Bremerich Radiology University Hospital Basel Hypertrophic Obstructive Cine VENC Cine (5m/s) Modified Bernoulli Equation: P (in mmhg) = 4 x (Vmax)2 Vmax= 4.2 m/s, P = 70mm Hg Hydrodynamica 738 HOCM
MYOSIN BINDING PROTEIN C GENE (MYBPC3) MUTATIONS IN HYPERTROPHIC CARDIOMYOPATHY
 MYOSIN BINDING PROTEIN C GENE (MYBPC3) MUTATIONS IN HYPERTROPHIC CARDIOMYOPATHY Summary of the PhD Thesis Tímea Tóth Graduate School of Clinical Medicine University of Szeged Supervisor: Róbert Sepp, MD,
MYOSIN BINDING PROTEIN C GENE (MYBPC3) MUTATIONS IN HYPERTROPHIC CARDIOMYOPATHY Summary of the PhD Thesis Tímea Tóth Graduate School of Clinical Medicine University of Szeged Supervisor: Róbert Sepp, MD,
Response of Right Ventricular Size to Treatment with Cardiac Resynchronization Therapy and the Risk of Ventricular Tachyarrhythmias in MADIT-CRT
 Response of Right Ventricular Size to Treatment with Cardiac Resynchronization Therapy and the Risk of Ventricular Tachyarrhythmias in MADIT-CRT Heart Rhythm Society (May 11, 2012) Colin L. Doyle, BA,*
Response of Right Ventricular Size to Treatment with Cardiac Resynchronization Therapy and the Risk of Ventricular Tachyarrhythmias in MADIT-CRT Heart Rhythm Society (May 11, 2012) Colin L. Doyle, BA,*
Is it HF secondary to rheumatic heart disease???
 Is it HF secondary to rheumatic heart disease??? Is mitral regurg. Is complication of CHF??? Cardiomyopathy Definition The term cardiomyopathy is purely descriptive, meaning disease of the heart muscle
Is it HF secondary to rheumatic heart disease??? Is mitral regurg. Is complication of CHF??? Cardiomyopathy Definition The term cardiomyopathy is purely descriptive, meaning disease of the heart muscle
Risk Factors for Sudden cardiac Death
 Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
Risk Factors for Sudden cardiac Death A. Arenal Arrhythmias in competitive sports Disclosure Conflict of interest Advisory board: Medtronic, Boston Scientific Research grants: Medtronic, Boston Scientific,
ARVC when TO IMPLANT THE ASYMPTOMATIC PERSON
 EUROPACE 2011 INHERITED ELECTRICAL CARDIAC DISORDERS ARVC when TO IMPLANT THE ASYMPTOMATIC PERSON June 26 th 2011 Robert Lemery MD CONFLICTS of INTEREST None ASYMPTOMATIC ARVC 1. ECG 2. ASYMPTOMATIC PVC
EUROPACE 2011 INHERITED ELECTRICAL CARDIAC DISORDERS ARVC when TO IMPLANT THE ASYMPTOMATIC PERSON June 26 th 2011 Robert Lemery MD CONFLICTS of INTEREST None ASYMPTOMATIC ARVC 1. ECG 2. ASYMPTOMATIC PVC
