HOSPICE DIAGNOSIS DETERMINATION ASSESSMENT
|
|
|
- Cody McCoy
- 5 years ago
- Views:
Transcription
1 Patient Name: MR #: Date: Objective documentation is required to support hospice admission. This worksheet is intended to gather information on both the severity and trajectory of the patient s condition from the medical record and admission assessment to confirm admission criteria is met and to determine primary diagnosis and prognosis group. 1. List all pertinent diagnoses found in the medical record. 2. Complete form. 3. Return to this page and designate each diagnosis appropriately following assessment and collaboration with the attending physician/and medical director. Only 1 Diagnosis is marked as primary (first on claim). Multiple diagnoses may be directly related to primary diagnosis or indirectly related but equally affecting prognosis. All other diagnoses, not determined as affecting prognosis, will be considered unrelated. DIAGNOSIS PER MEDICAL RECORD ICD 10 CODE ACTIVE SYMPTOMS YES NO PRIMARY RELATED TO UNRELATED DIAGNOSIS PROGNOSIS COMORBIDITY Information received from physician/facility/family, about current condition that has resulted in a referral to hospice. Give a general review of the past 6 months. (Directions: Check all that Apply) PART I: Decline in Clinical Status Guidelines: Increasing emergency room visits, hospitalizations/physician s visits related to diagnosis. Explain: Recurrent or intractable infections such as pneumonia, sepsis or upper urinary tract. Explain: Progressive Nutritional Decline: (Not related to reversible causes such as depression or diuretics) Weight Loss or Weight Gain Most Recent/Admit Weight: Date of Weight: Prior Weight: 3 months: 6 months: % of Change: Factors Related to Weight Change: Decreasing Anthropomorphic Measurement Rt. Arm: Lt. Arm: Date of Measure: Abdominal Girth: Thigh (Rt. or Lt.): Decreasing Albumin or Cholesterol Levels Albumin Level: Date: Past Level: Pre-Albumin Level: Date: Past Level: Cholesterol Level: Date: Past Level: Dysphagia leading to recurrent aspiration and/or inadequate oral intake documented by: Decreasing food portions or consumption. Has not responded to enteral nutritional support, despite adequate caloric intake due to intolerance or other complications supporting not reasonable to expect prolonged life. Other intake pattern issues: Form 10P 2/ BRIGGS, Des Moines, IA Unauthorized copying or use violates copyright law. PRINTED IN U.S.A. Page 1 of 6
2 BMI score on admission: ( is considered at risk) Height (in) BMI Wgt. (lbs.) 4'10" 4'11" 5'0" 5'1" 5'2" 5'3" 5'4" 5'5" 5'6" 5'7" Progressively Worsening Signs and Symptoms: General Symptoms: Dyspnea with increasing respiratory rate. Oxygen usage: Pulse Ox level at rest: Pulse Ox level after exertion: Cough, intractable or other: Nausea/vomiting poorly responsive to treatment: Diarrhea, intractable: Pain requiring increasing doses of major analgesics with long-term usage. Describe: Other: General Signs: Decline in systolic blood pressure to below 90 or progressive postural hypotension: Ascites or another progressive edema: Venous, arterial or lymphatic obstruction due to local progression or metastatic disease. Pleural/pericardial effusion: Progressive weakness (Give objective description): Change in level of consciousness: Laboratory Results: (When available lab testing is not required to establish hospice eligibility.) Decreasing po2 or increasing pco2: Increasing calcium, creatinine, BUN or liver function studies: Increasing tumor markers (e.g. CEA, PSA): Progressive changes in sodium/potassium level: Other: *** Obtain copies of all available dietary records, laboratory records, radiology records, radiology reports, etc. *** Page 2 of '8" '9" '10" '11" 72 6'0" 73 6'1" 74 6'2" 75 6'3" 76 6'4" 12
3 PART II: Non-Disease Specific Baseline Guidelines: (both must be met) 1. Palliative Performance Scale (PPS)* Admission Score: Performance Score of <70% in general and less than <40-50% for some disease specific guidelines. PPS Ambulation Activity & Evidence of Level Disease Progression Self-Care Intake Level Conscious Level 80% Full Normal Activity with Effort Full Normal Full 70% Reduced Unable to work normal job/ Full Normal or Reduced Full Significant evidence of disease 60% Reduced Unable to do hobby/housework Occasional Assistance Same Full or Confused 50% Mainly Sit/Lie Unable to do any work Considerable Assistance Same Full or Confused 40% Mainly in Bed Unable to do most activities Mainly Assisted Same Full or Drowsy +/- Confusion 30% Totally in Bed Unable to do any activities Total Care Reduced Same % Totally in Bed Unable to do any activities Total Care Minimal/Sips Same 10% Totally in Bed Unable to do any activities Total Care Mouth Care Drowsy or Coma 0% Death 2. Dependance on assistance for two or more activities of daily living (ADLs) Feeding Transfer Ambulation Bathing Continence Dressing Karnofsky Performance Status Scale* Admission Score: The lower the Karnofsky score, the worse the survival for most serious illnesses. Able to carry on normal activity and to work; no special care needed. Unable to work; able to live at home and care for most personal needs; varying amount of assistance needed. Unable to care of self; requires equivalent of institutional or hospital care; disease may be progressing rapidly. 100 Normal no complaints; no evidence of disease. 90 Able to carry on normal activity; minor signs or symptoms of disease. 80 Normal activity with effort; some signs or symptoms of disease. 70 Cares for self; unable to carry on normal activity or to do active work. 60 Requires occasional assistance, but is able to care for most of his personal needs. 50 Requires considerable assistance and frequent medical care. 40 Disabled; requires special care and assistance. 30 Severely disabled; hospital admission is indicated although death not imminent. Very sick; hospital admission necessary; active supportive treatment necessary. 10 Moribund; fatal processes progressing rapidly. 0 Dead Disease Specific Guidelines: Note: These guidelines are to be used in conjunction with the Non-disease specific baseline guidelines described in Part I and Part II. Documentation should paint a picture for the reviewer to clearly see why the patient is appropriate for hospice care and the level of care provided, i.e., routine home, continuous home, inpatient respite or general inpatient. The records should include observations and data, not merely conclusions. During the initial assessment for hospice appropriateness, complete the disease specific guideline for each pertinent diagnosis identified in medical records. CANCER Type and Location of Cancer Diagnosis Identified in Medical Record: Note: Certain cancers with poor prognoses (e.g. small cell lung cancer, brain cancer and pancreatic cancer) may be hospice eligible without fulfilling the other criteria in this section. Class III or IV per medical record Distant Metastasis: Progressed from earlier stage with: Continuous decline despite treatment Patient declines further disease directed therapy Page 3 of 6
4 DEMENTIA, END STAGE Type of Dementia Identified in Medical Record: (This guide is for Alzheimer s Type of Dementia, not multi-focus Dementia.) 1. Should show all the following characteristics: Stage 7 FAST Unable to bathe without assistance Unable to ambulate without assistance Urinary and fecal incontinence Unable to dress without assistance No consistent meaningful communication Alzheimer s Dementia Functional Decline* FAST Classification Admission Score: FAST Scale Stage Characteristics 1. Normal Adult No functional decline. 2. Normal Older Adult Personal awareness of some functional decline. 3. Early Alzheimer s Noticeable deficits in demanding job situations. 4. Mild Alzheimer s Requires assistance in complicated tasks such as handling finances. 5. Moderate Alzheimer s Requires assistance in choosing proper attire. 6. Moderately Severe Alzheimer s Requires assistance dressing, bathing and toileting. Experiences urinary and fecal incontinence. 7. Severe Alzheimer s A. Ability to speak limited to six words D. Inability to sit without lateral support B. Ability to speak limited to single word E. Inability to smile C. Loss of ambulation F. Inability to hold head up 2. Should have life-threatening complication within past 12 months: Aspiration Pneumonia Pyelonephritis or other upper UTI or Septicemia Decubitus Ulcer, stage 3-4 Fever, recurrent after antibiotics 10% weight loss over prior 6 months or Albumin Level <2.5 gm/dl CARDIOVASCULAR DISEASE, END STAGE Cardiac Diagnoses in Medical Records: Patient must have #1 and either #2 or #3 present: 1. CHF with a NYHA Class IV Symptoms and has declined invasive treatments. The Stages of Heart Failure NYHA Classification Class Level at Admission: Class Patient Symptoms Class I (Mild) No limitation of physical activity. Ordinary physical activity does not cause undue fatigue, palpitation or dyspnea (shortness of breath). Class II (Mild) Slight limitation of physical activity. Comfortable at rest, but ordinary physical activity results in fatigue, palpitation or dyspnea. Class III (Moderate) Marked limitation of physical activity. Comfortable at rest, but less than ordinary activity causes fatigue, palpitation or dyspnea. Class IV (Severe) Unable to carry out any physical activity without discomfort, such as; fatigue, dyspnea or angina. Symptoms of cardiac insufficiency at rest. If any physical activity is undertaken, discomfort is increased. 2. The patient: May have symptoms of congestive failure and/or angina at rest. CHF may be documented by Echo showing EF of Patient s EF: Date: Has an inability to carry out minimal physical activity without dyspnea or angina increasing. 3. Patient is optimally treated with: (Or they have a medical reason why they cannot be.) Diuretics: ACE inhibitors: Vasodilators: Nitrates: Other: PASP Level: Additional Supportive Documentation: (Supportive of Pulmonary Hypertension) Treatment resistant symptomatic supraventricular or ventricular arrhythmias: History of cardiac arrest or resuscitation History of unexplained syncope Brain embolism or secondary CVA of cardiac origin Concomitant HIV disease *Note: If no CHF: Other end-stage cardiac information to support end-stage must be clearly available in the medical record. Page 4 of 6
5 PULMONARY DISEASE, END STAGE Pulmonary Diagnoses in Medical Records: (1 and 2 should be present and 3-5 documented will lend support.) 1. Severe chronic lung disease as documented by disabling dyspnea at rest, poorly or unresponsive to bronchodilators resulting in decreased functional capacity, e.g., bed to chair existence, fatigue and cough. FEV1 after bronchodilator <30% of predicted. Patient %: Progression as evidenced by: Increasing visits to emergency room Hospitalization for pulmonary infections and/or respiratory failure Increased home physician visits Objectively documented with decrease in FEV 1 >40 ml/year 2. Hypoxemia at rest on room air, as evidenced with po2 55% or Oxygen saturation 88% or Hypercapnia with pco2 50 mmhg 3. Right heart failure (RHF) secondary to pulmonary disease (Cor pulmonale) (Not secondary to left heart disease or valvulopathy Any Valve Disease.) 4. Unintentional weight loss >10% over prior 6 months 5. Resting Tachycardia >100 bpm Pulse at rest on admission: LIVER DISEASE, END STAGE Liver diagnoses in Medical Records: (Patients waiting for transplants can be admitted for service) (1 and 2 should be present and 3 documented will lend support.) 1. End stage liver disease demonstrated with PT prolonged more than 5 seconds or INR >1.5 and Serum albumin < One or more of the following conditions: Ascites, refractory to treatment or patient non-compliance Hepatorenal syndrome: (elevated creatinine and BUN with oliguria <400 cc per day and urine sodium <10 meq/l History of recurrent variceal bleeding despite intensive therapy 3. Additional supportive documentation may include: Progressive malnutrition Muscle wasting with reduced strength and endurance Continued active alcoholism (>80 gm ethanol/day) RENAL DISEASE, END STAGE History of spontaneous bacterial peritonitis Hepatic encephalopathy, refractory to treatment Hepatocellular Carcinoma Hepatitis B surface antigen positive Hepatitis C refractory to interferon treatment Renal Diagnoses in Medical Records: 1 and either 2 or 3 should be present. 1. Patient is not seeking dialysis/transplant or is discontinuing dialysis 2. Creatinine clearance is <10 cc/min (< cc/min for patient with diabetes) 3. Serum creatinine >8.0 mg/dl (>6.0 mg/dl for patient with diabetes) Other supportive documentation includes: Acute Renal Failure with: Mechanical Ventilation Immunosuppression/AIDS Malignancy in another organ Albumin <3.5 gm/dl Chronic lung disease Cachexia Advanced cardiac disease Platelet count <,000 Advanced liver disease Disseminated intravascular coagulation Sepsis GI bleeding Chronic Renal Failure with: Uremia (GFR < is typical) Pt. level: Oliguria of <400 cc/ hrs Intractable hyperkalemia of >7.0 not responsive to treatment Uremic pericarditis Hepatorenal syndrome Intractable fluid overload, not responding to treatment Page 5 of 6
6 STROKE & COMA, END STAGE Patients will be considered to be in the terminal stage of stroke or coma if they meet the following: PPS <40% Inability to maintain hydration Weight loss of 10% in 6 months or 7.5% in the last 3 months Serum albumin 2.5 Current history of pulmonary aspiration not respon sive to speech language pathology intervention Sequential calorie counts documenting inadequate caloric/fluid intake Dysphagia severe enough to prevent the patient from receiving food and fluids necessary to sustain life, in a patient who declines or does not receive artificial nutrition and hydration. Comatose Patient with 3 of the following on the 3rd day: Abnormal brain stem response Doll s Eyes (no natural movement of eyes) Absent verbal responses Absent withdrawal response to pain Serum creatinine >1.5 gm/dl Documentation of the following factors, in the context of progressive clinical decline, within the past 12 months will support eligibility: Aspiration Pneumonia Date: Refractory stage 3-4 decubitus ulcers Upper urinary tract infection (pyelonephritis) Fever recurrent after antibiotics Sepsis Additional information about Diagnostic Imaging Factors can support poor prognosis after a stroke. ALS, END STAGE ALS must demonstrate either 1 or 2 below 1. Critically impaired breathing capacity with the following in the past 12 months: Significant dyspnea at rest Vital capacity less than 30% Patient declines artificial ventilation External ventilation may be used for comfort measures only 2. Rapid disease progression: Progressed to wheelchair or bed-bound Progressed to barely intelligible speech Progressed from normal to pureed diet Progressed from independent to assisted with all activities of daily living And critical nutritional impairment Oral intake of nutrients and fluids insufficient to sustain life Continuous weight loss Dehydration or hypovolemia Absence of artificial feeding methods sufficient to sustain life, but not for relieving hunger 3. In Addition: Life-threatening complications in the past 12 months: Recurrent aspiration pneumonia with or without tube feedings Upper urinary tract infection (pyelonephritis) Sepsis Recurrent fever after antibiotic therapy HIV Disease 1. CD4+ Count < cells/mcl or persistent viral load >100,000 copies/ml plus one of the following: CNS lymphoma Persistent body wasting (10% body mass) Mycobacterium avium complex (MAC) bacteremia, untreated or unresponsive Progressive multifocal leukoencephalopathy Systemic Lymphoma Visceral Kaposi Sarcoma, unresponsive Renal Failure in the absence of dialysis Crypotosporidium Infection Toxoplasmosis Additional supportive documentation: PPS score of 50% Chronic diarrhea for >1 year Active substance abuse >50 years old Absence of or resistance to drug therapy CHF, symptomatic at rest Advanced liver disease For other neurological diagnoses, not addressed in the disease specific guidelines, (such as Multiple Sclerosis, Parkinson s, Huntington s), describe any specific symptoms to support a <6 month predicted prognosis: Nurse Signature: Date: Page 6 of 6 HIV, END STAGE
Alzheimer s Disease, Dementia, Related Disorders
 Alzheimer s Disease, Dementia, Related Disorders Stage 7 on the FAST Scale signifies the threshold of activity limitation that would support a six-month prognosis. The FAST Scale does not address the impact
Alzheimer s Disease, Dementia, Related Disorders Stage 7 on the FAST Scale signifies the threshold of activity limitation that would support a six-month prognosis. The FAST Scale does not address the impact
Table of Contents: Amyotrophic Lateral Sclerosis (ALS)
 Guidelines for Hospice Admission Amyotrophic Lateral Sclerosis (ALS) Cancer Cerebral Vascular Accident / Stroke or Coma Dementia / Alzheimer s Failure to Thrive Adults Heart Disease / CHF HIV Disease Huntington
Guidelines for Hospice Admission Amyotrophic Lateral Sclerosis (ALS) Cancer Cerebral Vascular Accident / Stroke or Coma Dementia / Alzheimer s Failure to Thrive Adults Heart Disease / CHF HIV Disease Huntington
Determining Eligibility for Hospice Care
 Determining Eligibility for Hospice Care Main Number: 203 739-8300 Toll Free Number: 888 357-3334 www.regionalhospicect.org Many people may not understand all that Regional Hospice can offer or they are
Determining Eligibility for Hospice Care Main Number: 203 739-8300 Toll Free Number: 888 357-3334 www.regionalhospicect.org Many people may not understand all that Regional Hospice can offer or they are
Objectives 2/11/2016 HOSPICE 101
 HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
Hospice Eligibility August 2018
 Hospice Eligibility August 2018 Objectives Identify who can make a hospice referral Review hospice eligibility and disease-specific prognostic indicators Review Open Access philosophy Who Can Make A Referral
Hospice Eligibility August 2018 Objectives Identify who can make a hospice referral Review hospice eligibility and disease-specific prognostic indicators Review Open Access philosophy Who Can Make A Referral
Hospice Admission Guidelines
 Hospice Admission Guidelines www.hospiceheart.org Community Hospice Patients are eligible for hospice care when their physician determines the patient has a life expectancy of six (6) months or less. The
Hospice Admission Guidelines www.hospiceheart.org Community Hospice Patients are eligible for hospice care when their physician determines the patient has a life expectancy of six (6) months or less. The
PHYSICIAN REFERENCE GUIDE FOR HOSPICE ELIGIBILITY. Office: (850) Fax: (850)
 PHYSICIAN REFERENCE GUIDE FOR HOSPICE ELIGIBILITY www.regencyhospice.com Office: (850) 478-2695 Fax: (850) 478-9481 OUR MISSION The mission of Curo Health Services, and its hospice affiliates, is to honor
PHYSICIAN REFERENCE GUIDE FOR HOSPICE ELIGIBILITY www.regencyhospice.com Office: (850) 478-2695 Fax: (850) 478-9481 OUR MISSION The mission of Curo Health Services, and its hospice affiliates, is to honor
Hospice. Quick Reference Guide for Determining Eligibility for Hospice Care
 Hospice Quick Reference Guide for Determining Eligibility for Hospice Care Hospice is a comprehensive service available to patients and their families who have a life expectancy of six months or less.
Hospice Quick Reference Guide for Determining Eligibility for Hospice Care Hospice is a comprehensive service available to patients and their families who have a life expectancy of six months or less.
Hospice & Palliative Care Referral Guidelines. (901)
 Hospice & Palliative Care Referral Guidelines Issued 2010 (901) 516-1600 www.methodisthealth.org Give us time to help your patients. Unfortunately, few patients and families receive the full benefit of
Hospice & Palliative Care Referral Guidelines Issued 2010 (901) 516-1600 www.methodisthealth.org Give us time to help your patients. Unfortunately, few patients and families receive the full benefit of
Hospice Eligibility Job Aid. Introduction/Importance
 Introduction/Importance Hospice care is a benefit under various insurance programs. Most hospice care in the United States is provided through Medicare. To be eligible to elect hospice care under Medicare
Introduction/Importance Hospice care is a benefit under various insurance programs. Most hospice care in the United States is provided through Medicare. To be eligible to elect hospice care under Medicare
Community and Mental Health Services. Palliative Care. Criteria and
 Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
How to Estimate a Six-Month Prognosis. Hospice by the Bay Physicians
 Dear Colleague: Your local nonprofit, Hospice by the Bay, is here to help you, the referring physician: 1) determine hospice eligibility in terminally ill patients, 2) have the hospice conversation with
Dear Colleague: Your local nonprofit, Hospice by the Bay, is here to help you, the referring physician: 1) determine hospice eligibility in terminally ill patients, 2) have the hospice conversation with
Legislation POLST. Palliative and Hospice Care: End of Life Decisions. Palliative and Hospice Care End of Life Decisions John F. Bertagnolli, Jr, DO
 Palliative and Hospice Care End of Life Decisions John F. Bertagnolli, Jr, DO Legislation On 12/21/11 Gov. Christie signed legislation that enables patients to indicate their preferences regarding life
Palliative and Hospice Care End of Life Decisions John F. Bertagnolli, Jr, DO Legislation On 12/21/11 Gov. Christie signed legislation that enables patients to indicate their preferences regarding life
Specialist Palliative Care Service Referral Criteria and Guidance
 Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
Contractor Information. LCD Information. Local Coverage Determination (LCD): Hospice Determining Terminal Status (L34538) Document Information
 Local Coverage Determination (LCD): Hospice Determining Terminal Status (L34538) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website. Contractor Information
Local Coverage Determination (LCD): Hospice Determining Terminal Status (L34538) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website. Contractor Information
Eligibility Toolkit hosparus.org A non-profit hospice care provider
 Eligibility Toolkit 1-800-264-0521 hosparus.org A non-profit hospice care provider Our goal in partnering with you is to help residents/ patients live the rest of their lives as they wish, and to be comfortable
Eligibility Toolkit 1-800-264-0521 hosparus.org A non-profit hospice care provider Our goal in partnering with you is to help residents/ patients live the rest of their lives as they wish, and to be comfortable
Specialist Palliative Care Referral for Patients
 Specialist Palliative Care Referral for Patients This guideline covers referrals for patients with progressive terminal illness, whether due to cancer or other disease. For many patients in the late stages
Specialist Palliative Care Referral for Patients This guideline covers referrals for patients with progressive terminal illness, whether due to cancer or other disease. For many patients in the late stages
LCD for HOSPICE -- Determining Terminal Status (L13653)
 LCD for HOSPICE -- Determining Terminal Status (L13653) Contractor Information Contractor Name Cahaba GBA, LLC - Midwest Contractor Number 00011 Contractor Type RHHI LCD ID Number L13653 LCD Information
LCD for HOSPICE -- Determining Terminal Status (L13653) Contractor Information Contractor Name Cahaba GBA, LLC - Midwest Contractor Number 00011 Contractor Type RHHI LCD ID Number L13653 LCD Information
HOSPICE IN A POCKET steinhospice.org. 3rd Edition. Indications for Hospice Referrals
 HOSPICE IN A POCKET 3rd Edition Indications for Hospice Referrals 1-800-625-5269 steinhospice.org Thank you for allowing Stein Hospice to be an extension of your services to the patients who turn to you
HOSPICE IN A POCKET 3rd Edition Indications for Hospice Referrals 1-800-625-5269 steinhospice.org Thank you for allowing Stein Hospice to be an extension of your services to the patients who turn to you
GUIDELINES. for Hospice Admission
 GUIDELINES for Hospice Admission 124555_GuidelinesCover.indd 1 12/30/14 9:36 AM Table of Contents Hospice basics 10 Questions to Ask Dementia Amyotrophic Lateral Sclerosis (ALS) Cancer Cerebral Vascular
GUIDELINES for Hospice Admission 124555_GuidelinesCover.indd 1 12/30/14 9:36 AM Table of Contents Hospice basics 10 Questions to Ask Dementia Amyotrophic Lateral Sclerosis (ALS) Cancer Cerebral Vascular
Hospice Eligibility. Jeanette S. Ross MD, AGSF, FAAHPM
 Hospice Eligibility Jeanette S. Ross MD, AGSF, FAAHPM Objectives To define the Medicare Hospice benefit an describe the basic services To identify the medical criteria for Hospice eligibility as it applies
Hospice Eligibility Jeanette S. Ross MD, AGSF, FAAHPM Objectives To define the Medicare Hospice benefit an describe the basic services To identify the medical criteria for Hospice eligibility as it applies
Medicare hospice benefit. Katherine Dietrich, DO HMDC FACP CPE
 Medicare hospice benefit Katherine Dietrich, DO HMDC FACP CPE Disclosures Hospice Compassus Medical Director Billings MT Which of the following is correct about the Medicare Hospice Benefit? A. Once a
Medicare hospice benefit Katherine Dietrich, DO HMDC FACP CPE Disclosures Hospice Compassus Medical Director Billings MT Which of the following is correct about the Medicare Hospice Benefit? A. Once a
Course Handouts & Post Test
 STROKE/COMA: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Post Test To download presentation
STROKE/COMA: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Post Test To download presentation
Pike County. Determining Hospice Eligibility A guide to aide physicians in the important role they play in referring patients to hospice care.
 Determining Hospice Eligibility A guide to aide physicians in the important role they play in referring patients to hospice care. Pike County Hospice Caring for our Communities since 1993 Pike County Hospice
Determining Hospice Eligibility A guide to aide physicians in the important role they play in referring patients to hospice care. Pike County Hospice Caring for our Communities since 1993 Pike County Hospice
Clinical Policy: Hospice Services Reference Number: PA.CP.MP.54
 Clinical Policy: Reference Number: PA.CP.MP.54 Effective Date: 01/18 Last Review Date: 10/17 Coding Implications Revision Log Description Medical necessity for hospice services. Policy It is the policy
Clinical Policy: Reference Number: PA.CP.MP.54 Effective Date: 01/18 Last Review Date: 10/17 Coding Implications Revision Log Description Medical necessity for hospice services. Policy It is the policy
GUIDELINES: Referral Guidelines to Nelson Tasman Hospice Service including Clinical Criteria for Patients
 GUIDELINES: Referral Guidelines to Nelson Tasman Hospice Service including Clinical Criteria for Patients Overview Admission to the hospice service is NOT diagnosis specific and includes all patients with
GUIDELINES: Referral Guidelines to Nelson Tasman Hospice Service including Clinical Criteria for Patients Overview Admission to the hospice service is NOT diagnosis specific and includes all patients with
Clinical Policy: Hospice Services Reference Number: CP.MP.54
 Clinical Policy: Reference Number: CP.MP.54 Effective Date: 05/13 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.54 Effective Date: 05/13 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Hospice Approach to Caring Ellen M. Brown M.D.
 Hospice Approach to Caring Ellen M. Brown M.D. bjectives By the conclusion of this session, attendees will be able to: Explain the hospice philosophy and goals Understand what is covered by the hospice
Hospice Approach to Caring Ellen M. Brown M.D. bjectives By the conclusion of this session, attendees will be able to: Explain the hospice philosophy and goals Understand what is covered by the hospice
Course Handouts & Post Test
 End Stage Liver Disease (ESLD) End Stage Renal Disease (ESRD) Disease Trajectory and Hospice Eligibility Terri Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc. & Hospice Education
End Stage Liver Disease (ESLD) End Stage Renal Disease (ESRD) Disease Trajectory and Hospice Eligibility Terri Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc. & Hospice Education
Transitions Guidelines: Chronic Illness Management. Revised 2016
 Transitions Guidelines: Chronic Illness Management Revised 2016 1 Table of Contents Introduction Transitions Program Pillars General Principles Regarding Admission Cancer Cirrhosis Congestive Heart Failure
Transitions Guidelines: Chronic Illness Management Revised 2016 1 Table of Contents Introduction Transitions Program Pillars General Principles Regarding Admission Cancer Cirrhosis Congestive Heart Failure
Three triggers that suggest that patients could benefit from a hospice palliative care approach
 Why is it important to identify people nearing the end of life? About 1% of the population dies each year. Although some deaths are unexpected, many more in fact can be predicted. This is inherently difficult,
Why is it important to identify people nearing the end of life? About 1% of the population dies each year. Although some deaths are unexpected, many more in fact can be predicted. This is inherently difficult,
Compliant Hospice Admission
 Compliant Hospice Admission DETERMINING ELIGIBILITY AND PROGNOSIS Gail Austin Cooney MD HMDC FAAHPM Chief Medical Officer Access TrustBridge Health gcooney@trustbridge.com 1 Conflict of Interest Disclosure
Compliant Hospice Admission DETERMINING ELIGIBILITY AND PROGNOSIS Gail Austin Cooney MD HMDC FAAHPM Chief Medical Officer Access TrustBridge Health gcooney@trustbridge.com 1 Conflict of Interest Disclosure
Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov ( )
 Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov (1920-1992) Objectives Palliative care versus hospice care. Admission guidelines to hospice services. Having the
Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov (1920-1992) Objectives Palliative care versus hospice care. Admission guidelines to hospice services. Having the
HIV: Disease Trajectory and Hospice Eligibility
 HIV: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources/HEN Course Materials & Disclosure Course materials including handout(s) and conflict
HIV: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources/HEN Course Materials & Disclosure Course materials including handout(s) and conflict
Renal Care and Liver Disease: Disease Trajectory and Hospice Eligibility
 Renal Care and Liver Disease: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources/HEN Course Materials & Disclosure Course materials including
Renal Care and Liver Disease: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources/HEN Course Materials & Disclosure Course materials including
So let s go through each disease then and understand some of the established prognostic factors starting with COPD.
 Okay, I am Dr. David Hui from the Department of Palliative Care from The University of Texas MD Anderson Cancer Center and we are going to talk about Prognostication in Advanced Diseases, Part II. So in
Okay, I am Dr. David Hui from the Department of Palliative Care from The University of Texas MD Anderson Cancer Center and we are going to talk about Prognostication in Advanced Diseases, Part II. So in
J6 Hospice Nursing Documentation
 J6 Nursing Documentation Supporting Terminal Prognosis 1536_0415 Today s Presenters Corrinne Ball, RN, CPC, CAC, CACO Provider Outreach and Education Consultant 2 Disclaimer National Government Services,
J6 Nursing Documentation Supporting Terminal Prognosis 1536_0415 Today s Presenters Corrinne Ball, RN, CPC, CAC, CACO Provider Outreach and Education Consultant 2 Disclaimer National Government Services,
Primary Palliative Care
 Primary Palliative Care Amanda Overstreet, DO October 20, 2017 No financial disclosures Objectives Discuss palliative care and how it differs from hospice Explore how to manage patients goals and expectations
Primary Palliative Care Amanda Overstreet, DO October 20, 2017 No financial disclosures Objectives Discuss palliative care and how it differs from hospice Explore how to manage patients goals and expectations
Hospice and Palliative Care for the Elderly
 Hospice and Palliative Care for the Elderly Stephan Stellmacher, DO FACP Internal Medicine Hospice and Palliative Care Medicine Hospice vs. Palliative care + Palliative care seeks to relieve suffering
Hospice and Palliative Care for the Elderly Stephan Stellmacher, DO FACP Internal Medicine Hospice and Palliative Care Medicine Hospice vs. Palliative care + Palliative care seeks to relieve suffering
Guideline for Estimating Length of Survival in Palliative Patients
 http://pal 11 ative. into Cornelius Woelk MD, CCFP Medical Director of Palliative Care Regional Health Authority - Central Manitoba 385 Main Street Winkler, Manitoba, Canada R6W 1J2 Ph: 204-325-4312 Fax:
http://pal 11 ative. into Cornelius Woelk MD, CCFP Medical Director of Palliative Care Regional Health Authority - Central Manitoba 385 Main Street Winkler, Manitoba, Canada R6W 1J2 Ph: 204-325-4312 Fax:
Understanding THE SYMPTOMS YOU SEE
 Understanding THE SYMPTOMS YOU SEE Z Human existence is rich with experiences that weave a completed quilt called life. As the quilt nears completion, there is no set calendar as to its final, beautiful
Understanding THE SYMPTOMS YOU SEE Z Human existence is rich with experiences that weave a completed quilt called life. As the quilt nears completion, there is no set calendar as to its final, beautiful
11/2/2011 DOWNLOAD THE HANDOUTS OBJECTIVES. Determining Terminal Status: Dementia Due to Alzheimer s Disease and Related Disorders
 Determining Terminal Status: Dementia Due to Alzheimer s Disease and Related Disorders Joy Barry, RN, MEd, LNC Weatherbee Resources, Inc. Hospice Education Network, Inc. DOWNLOAD THE HANDOUTS Click on
Determining Terminal Status: Dementia Due to Alzheimer s Disease and Related Disorders Joy Barry, RN, MEd, LNC Weatherbee Resources, Inc. Hospice Education Network, Inc. DOWNLOAD THE HANDOUTS Click on
5/3/2012 PRESENTATION GOALS RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT
 RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT Presented by Carrie Black Bourassa, LRT, RRT PRESENTATION GOALS Define palliative care Define hospice care Discuss pulmonary hospice
RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT Presented by Carrie Black Bourassa, LRT, RRT PRESENTATION GOALS Define palliative care Define hospice care Discuss pulmonary hospice
Course Handouts & Disclosure
 COPD: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Disclosure To download presentation
COPD: Disease Trajectory and Hospice Eligibility Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Disclosure To download presentation
Clinical Policy: Hospice Services Reference Number: CA.CP.MP.54
 Clinical Policy: Reference Number: CA.CP.MP.54 Effective Date: 05/13 Last Review Date: 01/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CA.CP.MP.54 Effective Date: 05/13 Last Review Date: 01/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
HIV: Disease Trajectory and Hospice Eligibility
 HIV: Disease Trajectory and Hospice Eligibility Terri L. Maxwell, PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc Hospice Education Network Inc Course Handouts & Post Test To download presentation
HIV: Disease Trajectory and Hospice Eligibility Terri L. Maxwell, PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc Hospice Education Network Inc Course Handouts & Post Test To download presentation
Discussing Prognosis. David Ross Russell MD ProHealth Physicians Inc.
 Discussing Prognosis David Ross Russell MD ProHealth Physicians Inc. Prognosis- peeling back the layers Not a new Science Psalm 39 LORD, make me to know mine end, and the measure of my days. Hippocrates
Discussing Prognosis David Ross Russell MD ProHealth Physicians Inc. Prognosis- peeling back the layers Not a new Science Psalm 39 LORD, make me to know mine end, and the measure of my days. Hippocrates
End of Life with Dementia Sue Quist RN, CHPN
 End of Life with Dementia Sue Quist RN, CHPN Objectives: Describe the Medicare hospice benefit and services. Discuss the Medicare admission criteria for hospice patients with dementia due to Alzheimer
End of Life with Dementia Sue Quist RN, CHPN Objectives: Describe the Medicare hospice benefit and services. Discuss the Medicare admission criteria for hospice patients with dementia due to Alzheimer
SCALES SCALES SCALES. Performance Scales WHAT SHOULD THE RAINBOW FISH DO WITH ALL OF THESE SCALES?? KPS FAST ECOG PPS NYHA MRI ALSFRS
 SCALES SCALES SCALES WHAT SHOULD THE RAINBOW FISH DO WITH ALL OF THESE SCALES?? Karen L. Cross, MD, FAAHPM Performance Scales KPS FAST ECOG PPS NYHA MRI ALSFRS PPS = 30, 40, or 50 ECOG = 2, 3, or 4 NYHA
SCALES SCALES SCALES WHAT SHOULD THE RAINBOW FISH DO WITH ALL OF THESE SCALES?? Karen L. Cross, MD, FAAHPM Performance Scales KPS FAST ECOG PPS NYHA MRI ALSFRS PPS = 30, 40, or 50 ECOG = 2, 3, or 4 NYHA
Local Coverage Determination for Hospice - Liver Disease (L31536)
 Page 1 of 5 Centers for Medicare & Medicaid Services Print Message: If you are experiencing issues printing this page, then please click Return to Previous Page and select the 'Need a PDF?' button. You
Page 1 of 5 Centers for Medicare & Medicaid Services Print Message: If you are experiencing issues printing this page, then please click Return to Previous Page and select the 'Need a PDF?' button. You
HOSPICE 101. Another choice for patients facing a terminal prognosis. De Anna Looper, RN, CHPN, CHPCA. Carrefour Associates L.L.C.
 HOSPICE 101 Another choice for patients facing a terminal prognosis. De Anna Looper, RN, CHPN, CHPCA Senior Vice President of Clinical Operations Carrefour Associates L.L.C. HOSPICE 101 Patients and their
HOSPICE 101 Another choice for patients facing a terminal prognosis. De Anna Looper, RN, CHPN, CHPCA Senior Vice President of Clinical Operations Carrefour Associates L.L.C. HOSPICE 101 Patients and their
HPS ALLIANCE MEMBERS ONLY HOSPICE WEBINAR SERIES
 HPS ALLIANCE MEMBERS ONLY HOSPICE WEBINAR SERIES - 2019 PRESENTER(S): LESLIE HEAGY, RN, COS-C & MELINDA A. GABOURY, COS-C Documenting to support the Hospice Terminal Prognosis February 15, 2019 DOCUMENTING
HPS ALLIANCE MEMBERS ONLY HOSPICE WEBINAR SERIES - 2019 PRESENTER(S): LESLIE HEAGY, RN, COS-C & MELINDA A. GABOURY, COS-C Documenting to support the Hospice Terminal Prognosis February 15, 2019 DOCUMENTING
For The Critters Present
 For The Critters Present Be sure to Sepsis Sepsis secondary to UTI Bacteremia SIRS secondary to infection For More Info-Contact Your Documentation Specialist Pat Spadaro, R.N. 6796 Rosanne Garofano, R.N.
For The Critters Present Be sure to Sepsis Sepsis secondary to UTI Bacteremia SIRS secondary to infection For More Info-Contact Your Documentation Specialist Pat Spadaro, R.N. 6796 Rosanne Garofano, R.N.
Definitions in Palliative Care
 Definitions in Palliative Care Palliative care is specialist care provided for all people living with, and dying from a terminal condition and for whom the primary goal is quality of life. Palliative Care
Definitions in Palliative Care Palliative care is specialist care provided for all people living with, and dying from a terminal condition and for whom the primary goal is quality of life. Palliative Care
Hospice Palliative Scales Part I By James L. Holly, MD Your Life Your Health The Examiner May 10, 2012
 Hospice Palliative Scales Part I By James L. Holly, MD Your Life Your Health The Examiner May 10, 2012 One of the most important aspects of Patient-Centered Medical Home is the systematic discussion of
Hospice Palliative Scales Part I By James L. Holly, MD Your Life Your Health The Examiner May 10, 2012 One of the most important aspects of Patient-Centered Medical Home is the systematic discussion of
TRAJECTORY OF ILLNESS IN END OF LIFE CARE
 TRAJECTORY OF ILLNESS IN END OF LIFE CARE By Dr Helen Fryer OBJECTIVES To be aware of the three commonest trajectories of decline in the UK To understand the challenges faced in delivering effective Palliative
TRAJECTORY OF ILLNESS IN END OF LIFE CARE By Dr Helen Fryer OBJECTIVES To be aware of the three commonest trajectories of decline in the UK To understand the challenges faced in delivering effective Palliative
LCD for Hospice - Determining Terminal Status (L25678) Contractor Information. Contractor Name National Government Services, Inc.
 1 of 25 4/18/2008 1:46 PM LCD for Hospice - Determining Terminal Status (L25678) Contractor Information Contractor Name National Government Services, Inc. Contractor Number 00180 00450 00454 Contractor
1 of 25 4/18/2008 1:46 PM LCD for Hospice - Determining Terminal Status (L25678) Contractor Information Contractor Name National Government Services, Inc. Contractor Number 00180 00450 00454 Contractor
Nursing Process Focus: Patients Receiving Dextran 40 (Gentran 40)
 Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
LCD for Hospice - Determining Terminal Status (L25678) Contractor Information. Contractor Name National Government Services, Inc.
 Page 1 of 27 LCD for Hospice - Determining Terminal Status (L25678) Contractor Information Contractor Name National Government Services, Inc. Contractor Number 00180 00450 00454 Contractor Type RHHI LCD
Page 1 of 27 LCD for Hospice - Determining Terminal Status (L25678) Contractor Information Contractor Name National Government Services, Inc. Contractor Number 00180 00450 00454 Contractor Type RHHI LCD
CHF for Clinician. AtHomeCare.com
 CHF for Clinician AtHomeCare.com CONTACT INFORMATION FOR CLIENTS Client s Name: SOC Date: Case Manager s Name: Phone #: Physician s Name: Phone: Emergency Contact Person s Name: Phone Number: MISSION STATEMENT
CHF for Clinician AtHomeCare.com CONTACT INFORMATION FOR CLIENTS Client s Name: SOC Date: Case Manager s Name: Phone #: Physician s Name: Phone: Emergency Contact Person s Name: Phone Number: MISSION STATEMENT
11/11/2014. Deanna Speer BSN, CHPN Debbie Brand APRN, FNP-C. Describe the scope of palliative care as differentiated from hospice care.
 Deanna Speer BSN, CHPN Debbie Brand APRN, FNP-C Describe the scope of palliative care as differentiated from hospice care. Recognize indicators of prognosis in advanced, serious illness. Demonstrate skills
Deanna Speer BSN, CHPN Debbie Brand APRN, FNP-C Describe the scope of palliative care as differentiated from hospice care. Recognize indicators of prognosis in advanced, serious illness. Demonstrate skills
Supplementary Online Content
 Supplementary Online Content Rhee C, Jones TM, Hamad Y, et al; Centers for Disease Control and Prevention (CDC) Prevention Epicenters Program. Prevalence, underlying causes, and preventability of sepsis-associated
Supplementary Online Content Rhee C, Jones TM, Hamad Y, et al; Centers for Disease Control and Prevention (CDC) Prevention Epicenters Program. Prevalence, underlying causes, and preventability of sepsis-associated
ANAMORELIN FOR CACHEXIA. Series 20 CASE REPORT FORM
 1 ANAMORELIN FOR CACHEXIA Series 20 CASE REPORT FORM Palliative Care Clinical Studies Collaborative (PaCCSC) RAPID Pharmacovigilance in Palliative Care The case report form (CRF) is to be completed in
1 ANAMORELIN FOR CACHEXIA Series 20 CASE REPORT FORM Palliative Care Clinical Studies Collaborative (PaCCSC) RAPID Pharmacovigilance in Palliative Care The case report form (CRF) is to be completed in
Symptoms Assess symptoms and needs across all domains. Screen using Edmonton Symptom Assessment System (ESAS) for: Pain Nausea Depression
 A Palliative Care Approach for Primary Care Integrating a palliative care approach earlier in the disease trajectory improves the quality of living and dying, and relieves suffering for patients and families
A Palliative Care Approach for Primary Care Integrating a palliative care approach earlier in the disease trajectory improves the quality of living and dying, and relieves suffering for patients and families
IEHP UM Subcommittee Approved Authorization Guidelines My Path (A Palliative Care Approach)
 UM_OTH 09 IEHP UM Subcommittee Approved Authorization Guidelines I. Policy: A. Inland Empire Health Plan (IEHP), in accordance with Senate Bill (SB) 1004, is dedicated to creating a community/home-based
UM_OTH 09 IEHP UM Subcommittee Approved Authorization Guidelines I. Policy: A. Inland Empire Health Plan (IEHP), in accordance with Senate Bill (SB) 1004, is dedicated to creating a community/home-based
Painting a Picture of Eligibility Through Documentation
 2017 ALL RIGHTS RESERVED R&C HEALTHCARE SOLUTIONS Painting a Picture of Eligibility Through Documentation CHARLENE ROSS, MBA, MSN, RN C ONSULTANT/EDUCATOR R &C HEALTHCARE SOLUTIONS & HOSPICE FUNDAMENTALS
2017 ALL RIGHTS RESERVED R&C HEALTHCARE SOLUTIONS Painting a Picture of Eligibility Through Documentation CHARLENE ROSS, MBA, MSN, RN C ONSULTANT/EDUCATOR R &C HEALTHCARE SOLUTIONS & HOSPICE FUNDAMENTALS
Chronic Hepatic Disease
 Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Chronic Hepatic Disease 10 th Leading Cause of Death Liver Functions Energy Metabolism Protein Synthesis Solubilization, Transport, and Storage Protects and Clears drugs, damaged cells Causes of Liver
Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC NPSS Asheville, NC
 Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC 2017 NPSS Asheville, NC Objectives Understand the importance of documenting to the highest specificity Understand
Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC 2017 NPSS Asheville, NC Objectives Understand the importance of documenting to the highest specificity Understand
Cardiorenal and Renocardiac Syndrome
 And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
Course Handouts & Disclosure
 ALS: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc Hospice Education Network Inc Course Handouts & Disclosure To download presentation
ALS: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc Hospice Education Network Inc Course Handouts & Disclosure To download presentation
National Medical Policy
 National Medical Policy Subject: Policy Number: Hospice Care NMP238 Effective Date*: September 2005 Updated: September 2007, January 2011 This National Medical Policy is subject to the terms in the IMPORTANT
National Medical Policy Subject: Policy Number: Hospice Care NMP238 Effective Date*: September 2005 Updated: September 2007, January 2011 This National Medical Policy is subject to the terms in the IMPORTANT
The Failing Heart in Primary Care
 The Failing Heart in Primary Care Hamid Ikram How fares the Heart Failure Epidemic? 4357 patients, 57% women, mean age 74 years HFSA 2010 Practice Guideline (3.1) Heart Failure Prevention A careful and
The Failing Heart in Primary Care Hamid Ikram How fares the Heart Failure Epidemic? 4357 patients, 57% women, mean age 74 years HFSA 2010 Practice Guideline (3.1) Heart Failure Prevention A careful and
CareFirst Hospice. Health care for the end of life. CareFirst
 Hospice Health care for the end of life 1 What is Hospice? Hospice is a philosophy- When a person in end stages of an illness can no longer receive, or wants to receive, life sustaining treatment, he or
Hospice Health care for the end of life 1 What is Hospice? Hospice is a philosophy- When a person in end stages of an illness can no longer receive, or wants to receive, life sustaining treatment, he or
James W. Castillo II, MD Medical Director of the Palliative Care Consultation Service Valley Baptist Health System
 End of Life Issues in Stroke James W. Castillo II, MD Medical Director of the Palliative Care Consultation Service Valley Baptist Health System Conflict Disclosure Information James W. Castillo II, MD
End of Life Issues in Stroke James W. Castillo II, MD Medical Director of the Palliative Care Consultation Service Valley Baptist Health System Conflict Disclosure Information James W. Castillo II, MD
A Palliative Approach in Caring for the Person and Family Living with Dementia Hospice and Palliative Nurses Association (HPNA) Online Education
 A Palliative Approach in Caring for the Person and Family Living with Dementia Anne Carr, GNP BC Anne Mahler, GCNS BC, ACHPN Created May 2017 Disclosures Anne Carr and Anne Mahler have no real or perceived
A Palliative Approach in Caring for the Person and Family Living with Dementia Anne Carr, GNP BC Anne Mahler, GCNS BC, ACHPN Created May 2017 Disclosures Anne Carr and Anne Mahler have no real or perceived
TEMPLATE CASE REPORT FORM. Rapid Response Pharmacovigilance in Palliative Care
 TEMPLATE CASE REPORT FORM Rapid Response Pharmacovigilance in Palliative Care The case report form is to be completed in compliance with PaCCSC Standard Operating Procedures 1 Staff email: Participant
TEMPLATE CASE REPORT FORM Rapid Response Pharmacovigilance in Palliative Care The case report form is to be completed in compliance with PaCCSC Standard Operating Procedures 1 Staff email: Participant
CCRN Review - Renal. CCRN Review - Renal 10/16/2014. CCRN Review Renal. Sodium Critical Value < 120 meq/l > 160 meq/l
 CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
Chapter Goal. Learning Objectives 9/12/2012. Chapter 36. Geriatrics. Use assessment findings to formulate management plan for geriatric patients
 Chapter 36 Geriatrics Chapter Goal Use assessment findings to formulate management plan for geriatric patients Learning Objectives Describe dependent & independent living environments Identify local resources
Chapter 36 Geriatrics Chapter Goal Use assessment findings to formulate management plan for geriatric patients Learning Objectives Describe dependent & independent living environments Identify local resources
Ontario s Referral and Listing Criteria for Adult Heart Transplantation
 Ontario s Referral and Listing Criteria for Adult Heart Transplantation Version 3.0 Trillium Gift of Life Network Adult Heart Transplantation Referral & Listing Criteria PATIENT REFERRAL CRITERIA: The
Ontario s Referral and Listing Criteria for Adult Heart Transplantation Version 3.0 Trillium Gift of Life Network Adult Heart Transplantation Referral & Listing Criteria PATIENT REFERRAL CRITERIA: The
Midazolam for Agitation - Baseline
 Midazolam for Agitation - Baseline Staff email Participant ID Date of Baseline w D-M-Y H:M Initials of person entering data Demographics Gender Male Female Age Weight (kg) Height (cm) Page 1 Primary life
Midazolam for Agitation - Baseline Staff email Participant ID Date of Baseline w D-M-Y H:M Initials of person entering data Demographics Gender Male Female Age Weight (kg) Height (cm) Page 1 Primary life
SN Visit Note. Vital Signs. Blood Sugar. Oxygen. Allergies. Pain Assessment. Visit Date: Episode Date: Patient Name: Patient ID:
 Patient Name: Patient ID: Visit Date: Episode Date: SN Visit Note Vital Signs Not ed Temperature: Pulse Apical: Reg Irreg Resp: / min Pulse Radial: Reg Irreg B/P (L) B/P (R) Sitting: / Sitting: / Standing:
Patient Name: Patient ID: Visit Date: Episode Date: SN Visit Note Vital Signs Not ed Temperature: Pulse Apical: Reg Irreg Resp: / min Pulse Radial: Reg Irreg B/P (L) B/P (R) Sitting: / Sitting: / Standing:
Talking to Patients about Living (and Dying) When They Are Dying
 Talking to Patients about Living (and Dying) When They Are Dying Andy Robinson, MD Palliative Medicine Colorado Permanente Medical Group February 4, 2017 Disclosures Nothing to disclose Objectives Increase
Talking to Patients about Living (and Dying) When They Are Dying Andy Robinson, MD Palliative Medicine Colorado Permanente Medical Group February 4, 2017 Disclosures Nothing to disclose Objectives Increase
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
ACOFP 55th Annual Convention & Scientific Seminars. How Complicated is Your Panel? Effective Risk Coding in Primary Care. Alison Mancuso, DO, FACOFP
 8 ACOFP 55th Annual Convention & Scientific Seminars How Complicated is Your Panel? Effective Risk Coding in Primary Care Alison Mancuso, DO, FACOFP How Complicated is Your Panel?: Effective Risk Coding
8 ACOFP 55th Annual Convention & Scientific Seminars How Complicated is Your Panel? Effective Risk Coding in Primary Care Alison Mancuso, DO, FACOFP How Complicated is Your Panel?: Effective Risk Coding
Palliative Care In Respirology: Who s job is it, anyway?! Everyones!
 Palliative Care In Respirology: Who s job is it, anyway?! Everyones! Dr. Shalini Nayar MD Respiratory Medicine Palliative Medicine Clinical Assistant Professor, Dept of Medicine, UBC Canadian Cancer Society
Palliative Care In Respirology: Who s job is it, anyway?! Everyones! Dr. Shalini Nayar MD Respiratory Medicine Palliative Medicine Clinical Assistant Professor, Dept of Medicine, UBC Canadian Cancer Society
Local Coverage Determination for Hospice Alzheimer's Disease &Related Disorders (L31539)
 Page 1 of 6 Centers for Medicare & Medicaid Services Print Message: If you are experiencing issues printing this page, then please click Return to Previous Page and select the 'Need a PDF?' button. You
Page 1 of 6 Centers for Medicare & Medicaid Services Print Message: If you are experiencing issues printing this page, then please click Return to Previous Page and select the 'Need a PDF?' button. You
Exercise Prescription for Patients with CHF
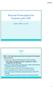 Exercise Prescription for Patients with CHF LESLIE AYRES, PT, DPT Goals After viewing this presentation the physical therapist will be able to: Discuss and understand the diagnosis of CHF including: Clinical
Exercise Prescription for Patients with CHF LESLIE AYRES, PT, DPT Goals After viewing this presentation the physical therapist will be able to: Discuss and understand the diagnosis of CHF including: Clinical
UH Case Medical Center Adult Inpatient Telemetry Admission, Transfer and Discharge Guidelines
 UH Case Medical Center Adult Inpatient Telemetry Admission, Transfer and Discharge Guidelines STATEMENT OF PURPOSE: To facilitate appropriate geo-location placement of patients who require telemetry monitoring
UH Case Medical Center Adult Inpatient Telemetry Admission, Transfer and Discharge Guidelines STATEMENT OF PURPOSE: To facilitate appropriate geo-location placement of patients who require telemetry monitoring
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Liver failure &portal hypertension
 Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
4. Which survey program does your facility use to get your program designated by the state?
 TRAUMA SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and
TRAUMA SURVEY Please complete one survey for each TCD designation you have in your facility. There would be a maximum of three surveys completed if your facility was designated as a trauma, stroke and
APACHE II: A Severity of Disease Classification System Standard Operating Procedure for Accurate Calculations
 BACKGROUND APACHE II: A Severity of Disease Classification System Standard Operating Procedure for Accurate Calculations The APACHE prognostic scoring system was developed in 1981 at the George Washington
BACKGROUND APACHE II: A Severity of Disease Classification System Standard Operating Procedure for Accurate Calculations The APACHE prognostic scoring system was developed in 1981 at the George Washington
2. To provide an ethical, moral and practical framework for decision-making during a public health emergency.
 November 2010 TABLE TOP EXERCISE PARTICIPANT GUIDE When Routine Critical Care Resources Are Not Available Time expectations for each session: SECTION ACTIVITY TIME I Introduction 5 minutes II Exercise
November 2010 TABLE TOP EXERCISE PARTICIPANT GUIDE When Routine Critical Care Resources Are Not Available Time expectations for each session: SECTION ACTIVITY TIME I Introduction 5 minutes II Exercise
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS
 REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
Hospice Documentation Strategies
 HOSPICE DOCUMENTATION REQUIREMENTS: Hospice Documentation Strategies The hospice clinical record must support the plan of care and frequencies of visits along with the findings of the comprehensive assessment
HOSPICE DOCUMENTATION REQUIREMENTS: Hospice Documentation Strategies The hospice clinical record must support the plan of care and frequencies of visits along with the findings of the comprehensive assessment
Hospice 101: A Primer for the PCP/Hospitalist. John Thompson, II DO, DABFM, HMDC
 Hospice 101: A Primer for the PCP/Hospitalist John Thompson, II DO, DABFM, HMDC Objectives: Understand the difference between Hospice and Palliative Medicine. Have a general understanding of hospice criteria
Hospice 101: A Primer for the PCP/Hospitalist John Thompson, II DO, DABFM, HMDC Objectives: Understand the difference between Hospice and Palliative Medicine. Have a general understanding of hospice criteria
Cardiac Pathology & Rehabilitation
 Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
March Hospice Fundamentals All Rights Reserved 1. What We ll Cover
 The Clinicians Connection to Documentation: Using the PPS, FAST, BMI, MAC and NYHA What We ll Cover Common scaling and measurement tools Importance of tools in supporting eligibility Effective use Common
The Clinicians Connection to Documentation: Using the PPS, FAST, BMI, MAC and NYHA What We ll Cover Common scaling and measurement tools Importance of tools in supporting eligibility Effective use Common
