Cardiac Output (C.O.) Regulation of Cardiac Output
|
|
|
- Caitlin Short
- 6 years ago
- Views:
Transcription
1 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic volume End systolic volume So.. Cardiac output = stroke volume X heat rate. N.B: Cardiac index is the cardiac output per minute per square meter surface area (3.2 L/min/m 2 ). Regulation of Cardiac Output I - Pumping ability of the heart. A. Intrinsic regulation: Is the regulation of pumping ability of the heart without the aid of nerves or hormones., including: 1. Regulation of contractility: a) Effect of Preload. b) Effect of afterload. 2. Regulation of rythmicity.
2 Effect of Preload : Frank-Starling Law: Within limit, the greater the cardiac muscle is streached during cardiac filling the greater will be the force of contraction the greater will be the stroke volume. This curve shows the relation between Cardiac filling (Preload) and the pressure inside ventricles during systole & diastole. a) Diastolic Pressure curve: Till 150 ml, diastolic pressure doesn't increase greatly easy blood flow from atria. More than 150 ml pressure increase rapidly maximum stretch of cardiac fibrous tissue & pericardium. b) Systolic Pressure curve: Till 150 ml, systolic pressure increase rapidly till it reach its maximum. More than 150 ml decrease systolic pressure due to separation of actin & myosine filaments number of cross bridges contraction. Effect Of Afterload : The afterload is the aortic pressure. Ventricle contract isometrically until ventricular pressure is more than aortic pressure isotonic contraction. Within limit, the greater the afterload the greater will be the force of contraction. Excessive increase in aortic pressure decrease cardiac output
3 Intrinsic Regulation of rythmicity: atrial filling stretch S-A node its stimulation heart rat. Q. What is Cardiac Function Curve? This curve shows the relation between right atrial pressure & cardiac output. This curve shows the following: The more the right atrial pressure the more the cardiac output until a plateau is reached. right atrial pressure ventricular filling stretch the ventricle contractility cardiac output. The plateau level is 13 L/minute in normal cardiac curve. plateau level Hyper-effective heart, and plateau level in hypo-effective heart. a) Cause of Hyper-effective heart: 1) Sympathetic stimulation heart rate & cardiac contractility double the plateau level. 2) Hypertrophy of cardiac muscle: Is increase in cardiac muscle mass & its contractility due to increase cardiac overload (as in athletes) double the plateau level Combined 1, 2 (as in marathon runner) plateau up to 40 L/minute b) Causes of Hypo-effective heart: 1) Parasympathetic stimulation or sympathetic inhibition 2) Excessive afterload as in hypertension. 3) Heart disease: Congenital heart disease - Valve disease Cardiac arrhythmia Diseased cardiac muscle as myocarditis
4 B. Extrinsic regulation: It may nervous or hormonal. Nervous regulation of pumping ability : 1. Sympathetic stimulation: Pathway: Vasomotor centre in medulla oblongata Lateral horn cells of upper 4 thoracic segment preganglionic fibers cervical ganglia postganglionic to the heart. Function: 1) heart rate to 200 beat/minute. Sympathetic stimulation noradrenaline release Na permeability & K permeability at S-A nodal membrane prepotential slope heart rate 2) cardiac contraction. Noradrenaline camp in cardiac muscle contractility. 3) Vasodilatation of coronary blood vessels. 2. Parasympathetic stimulation: Pathway: cardiac inhibitory centre dorsal nucleus of the vagus terminal ganglia in the wall of the heart post ganglionic fiber to he atria (Not the ventricle) Function: 1) heart rate may stop atrial beat but not the ventricle that escape from vagal inhibition. Parasympathetic stimulation acetyl choline K permeability in S-A node prepotential slope heart rate. 2) cardiac contractility to lesser extent as it supply atria only. 3) Vasoconstriction of coronary blood vessels. N:B: There are continuous tone from sympathetic & parasympathetic system to the heart but the parasympathetic tone predominate. Nervous regulation affect mainly the heart rate that affect the cardiac output.
5 Q. How does heart rate affect cardiac output? C.O. = S.V. X H.R. In denervated heart: a) Heart rate ( beat/minute) no change in cardiac output. Explanation: heart rate diastolic period cardiac filling S.V. constant C.O. b) Heart rate more than 160 b/min cardiac output. The marked reduction in S.V. can't be compensated by the increase in heart rate C.O. c) Heart rate less than 60 b/min cardiac output. The marked increase in S.V. can not compensate the decrease in heart rate. In intact heart: Sympathetic stimulation heart rate to 200 b/min C.O. Explanation: 1) Sympathetic stimulation heart rate and cardiac contractility. 2) Sympathetic stimulation systolic period allow more time for diastole. Hormonal regulation of pumping ability : Catecholamine & xanthines camp cardiac contractility S.V. C.O. Drugs: a) Digitalis +ve ionotrope C.O. b) Quinidine, hypoxia, hypercapnia & ischemia contractility C.O.
6 II Venous return. Venous return is affected by: 1. Right atrial pressure (PRA) 2. Mean systemic filling pressure (Psf) 3. Resistance to venous return 1. Right atrial Pressure (PRA): Also called Central venous pressure CVP. Normal value from -2 to +2 mmhge. Average is zero. It is regulated by the balance between pumping ability of the heart & venous return to less than -2 mmhg in case of sever in venous return as in hemorrhage. up to +30 mmhg in serious heart disease. Relation between PRA and venous return is demonstrated in the venous return curve: Venous return curve show the following: PRA more than Zero back pressure against venous return venous return Venous return is zero when PRA reach 7 mmhg PRA below zero venous pressure reaching plateau when PRA is -2 PRA below -2 no further increase in venous return due to collapse of veins entering the chest
7 2. Mean systemic filling pressure (Psf): Is pressure measured in systemic circulation after clamping large vessels at the heart. Normal value -7 mmhg. Importance of Psf: 1) Measure the degree of filling of systemic circulation 2) Affecting Venous return curve as follow: i- Psf shift curve upward to the right ii- Psf shift curve downward to the left. Factor affecting Psf: 1) Blood volume: blood volume Psf. 2) Sympathetic tone: sympathetic tone V.C. Psf 3) Skeletal muscle contraction: compress veins from outside Psf. 3. Resistance to blood flow: Resistance occurs in veins (2/3) and arterioles. resistance to blood flow venous return This curve show effect of different resistance on venous return curve: 1) resistance to 1/2 normal double the venous return. 2) resistance twice decrease venous return to 1/2 normal. N.B. 1) Mean circulatory pressure: is the equilibrated pressure in systemic circulation after one minute of cessation of cardiac blood flow. It is almost equal to Psf (due to small capacity of pulmonary circulation). 2) The most important determinant of venous return is the gradient between Psf & RAP. If RAP = Psf venous return is zero (whatever will be the resistance to blood flow).
8 Relation between C.O. & venous return curve. Right atrial pressure affects both C.O & venous return A steady state is reached at (A) point (intersect between C.O curve & venous return curve. In resting condition: Psf = 7 mmhg PRA = zero Venous return = C.O. = 5 L/min. In muscular exercise: a) venous return due to: i- Psf due to sympathetic V.C. & skeletal muscle contraction. ii- arteriolar vasodilatation peripheral resistance. b) C.O. due to: i- Sympathetic stimulation all properties of the heart hyper-effective heart. The new steady point (B): Psf = 20 mmhg. PRA = up to 2 mmhg Venous return = C.O. = 22 L/min In heart failure: a) C.O. arterial blood pressure glomerular filtration in kidney urine formation blood volume venous return (shifted upward) b) cardiac contractility more in C.O. (shifted downward). The new steady point (C): C.O. = venous return = 3 L/min
9 Variation in C.O. I. Physiological variation: C.O. : Excitement & stress Eating Exercise Environmental temperature Emberyo (Pregnancy)!! C.O. : Standing from lying position Age: The Cardiac index. rise rapidly till it reach maximum at age of 10 year then decline gradually to lower value in age of 80 C.O. not changed by sleep or moderate Environmental temp. II. Pathological variation: C.O. It increase in conditioned associated with decrease peripheral resistance as: 1) Beri beri: thiamine deficiency in diet cellular ability to use nutrient peripheral V.D. peripheral resistance. 2) Anemia: blood viscosity & peripheral V.D. caused by hypoxia peripheral resistance. 3) Arteio-venous fistula: Shunt of blood from large artery to large vein peripheral resistance. 4) Hyperthyroidism: O2 consumption & accumulation of metabolites peripheral V.D. peripheral resistance. C.O. A. pumbing ability: Congenital heart diseas. Valvular heart disaes Myocarditis B. Venous return: blood volume: as hemorrhage Psf venous return Acute Venous dilatation as in anaphylactic shock.
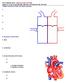
10 Cardiac Work Output Stroke work output: Is the amount of energy converted to work by the heart during each heart beat. Minute work output: is the total amount of energy that the heart converts in one minute. Minute work output = Stroke work output X heart rate/min. This work has two forms: 1. External work: Is the work performed to pump stroke volume against the mean arterial blood pressure (volume-pressure work). External work of Lt. ventricle = stroke volume X mean systemic blood pressure. External work of Rt. ventricle = stroke volume X mean pulmonary blood pressure 2. Kinetic work: Is the work performed by the heart to give velocity to the blood in the vascular system. The kinetic work is only 1% of the total work so it can be neglected. Volume Pressure Curve of Lt ventricle. Phase I: (filling phase) It represent the period of ventricular filling during diastole At (A) point the end diastolic volume is 115 ml. & mitral valve close Phase II: (Isometric contraction phase) Ventricle is closed chamber pressure but constant volume at point (B), EDV not changed & aortic valve open. Phase III: (Ejection phase) More in pressure due to ventricular systole but decrease in volume. At (C) point, End systolic volum = 45 ml & aortic valve closes.
11 Phase IV: (Isometric relaxation phase) The ventricle is closed chamber in pressure but constant volume At (D) point ESV = 45 & mitral valve opens Factor Affecting External work output: 1. Preload: mean Lt atrial pressure EDV and pressure from point A to A Provide after load is constant Ejection start at the same point (B = B) Provide that contractility is constant, so initial point of relaxation (C) Fall on contractility line. Conclusion: area of volume pressure curve external work output of Lt ventricle 2. Afterload: aortic pressure point at which ejection occurs (B) Provide contractility is constant, so initial point of relaxation move up to fall on contractility line Conclusion: stroke volume but external work due to area of volume pressure curve 3. Change in contractility: contractility the slope of contractility line area of volume pressure curve external work output & vise versa NB: Minute work output is affected by preload, afterload, contractility + heart rate. Sympathetic stimulation to the heart: a) venous return preload. b) mean arterial blood pressure afterload c) cardiac contractility. d) heart rate a, b, c & d minute work output of the heart.
During exercise the heart rate is 190 bpm and the stroke volume is 115 ml/beat. What is the cardiac output?
 The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
-12. -Ensherah Mokheemer - ABDULLAH ZREQAT. -Faisal Mohammad. 1 P a g e
 -12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
-12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
Heart Pump and Cardiac Cycle. Faisal I. Mohammed, MD, PhD
 Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiac Output MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Cardiac output and Venous Return. Faisal I. Mohammed, MD, PhD
 Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
Cardiac output and Venous Return Faisal I. Mohammed, MD, PhD 1 Objectives Define cardiac output and venous return Describe the methods of measurement of CO Outline the factors that regulate cardiac output
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
From PV loop to Starling curve. S Magder Division of Critical Care, McGill University Health Centre
 From PV loop to Starling curve S Magder Division of Critical Care, McGill University Health Centre Otto Frank 1890 s Frank-Starling Relationship ( The Law of the Heart ) The greater the initial stretch
From PV loop to Starling curve S Magder Division of Critical Care, McGill University Health Centre Otto Frank 1890 s Frank-Starling Relationship ( The Law of the Heart ) The greater the initial stretch
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
AS Level OCR Cardiovascular System
 AS Level OCR Cardiovascular System Learning Objectives The link between the Cardiac Cycle and the Conduction system of the heart. The relationship between Stroke volume, Heart rate and Cardiac Output.
AS Level OCR Cardiovascular System Learning Objectives The link between the Cardiac Cycle and the Conduction system of the heart. The relationship between Stroke volume, Heart rate and Cardiac Output.
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System: The Heart
 Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
SIKLUS JANTUNG. Rahmatina B. Herman
 SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Cardiac Output (CO) Definitions. Cardiac Output and venous return. Dr Badri Paudel GMC. Cardiac Output. Venous Return
 Cardiac Output and venous return Dr Badri Paudel GMC Definitions Cardiac Output The quantity of blood pumped into the aorta each minute measured in milliliters (ml) per minute (min) or liters (L) per minute
Cardiac Output and venous return Dr Badri Paudel GMC Definitions Cardiac Output The quantity of blood pumped into the aorta each minute measured in milliliters (ml) per minute (min) or liters (L) per minute
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
IP: Regulation of Cardiac Output
 ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp , , , I. Major Functions of the Circulatory System
 P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
TOPIC : Cardiogenic Shock
 University of Ferrara Department of Morphology, Surgery and Experimental Medicine. Section of Anaesthesia and Intensive Care Medicine TOPIC : Cardiogenic Shock What is shock? Shock is a condition of inadequate
University of Ferrara Department of Morphology, Surgery and Experimental Medicine. Section of Anaesthesia and Intensive Care Medicine TOPIC : Cardiogenic Shock What is shock? Shock is a condition of inadequate
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006
 SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
Properties of Pressure
 OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Anaesthesia. Update in. An Introduction to Cardiovascular Physiology. James Rogers Correspondence
 Update in Anaesthesia Originally published in Update in Anaesthesia, edition 10 (1999) An Introduction to Cardiovascular Physiology Correspondence Email: James.Rogers@nbt.nhs.uk INTRODUCTION The cardiovascular
Update in Anaesthesia Originally published in Update in Anaesthesia, edition 10 (1999) An Introduction to Cardiovascular Physiology Correspondence Email: James.Rogers@nbt.nhs.uk INTRODUCTION The cardiovascular
The Cardiovascular System
 Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
DESCRIBE THE FACTORS AFFECTING CARDIAC OUTPUT.
 DESCRIBE THE FACTORS AFFECTING CARDIAC OUTPUT. BY: DISHA PRAKASH I MBBS, ROLL NO: 16M069 OBJECTIVES OF LEARNING Terminology and conceptual understanding of Cardiac Output. Factors regulating Cardiac Output.
DESCRIBE THE FACTORS AFFECTING CARDIAC OUTPUT. BY: DISHA PRAKASH I MBBS, ROLL NO: 16M069 OBJECTIVES OF LEARNING Terminology and conceptual understanding of Cardiac Output. Factors regulating Cardiac Output.
Cardiac Output 1 Fox Chapter 14 part 1
 Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #12 Understanding Preload and Afterload
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #12 Understanding Preload and Afterload Cardiac output (CO) represents the volume of blood that is delivered
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #12 Understanding Preload and Afterload Cardiac output (CO) represents the volume of blood that is delivered
Cardiac Output. Graphics are used with permission of: adam.com ( Benjamin Cummings Publishing Co (
 Interactive Physiology Cardiac Output Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.aw.com/bc) Page 1. Introduction Cardiac output is
Interactive Physiology Cardiac Output Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.aw.com/bc) Page 1. Introduction Cardiac output is
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
CARDIAC OUTPUT,VENOUS RETURN AND THEIR REGULATION. DR.HAROON RASHID. OBJECTIVES
 CARDIAC OUTPUT,VENOUS RETURN AND THEIR REGULATION. DR.HAROON RASHID. OBJECTIVES Define Stroke volume, Cardiac output Venous return,& identity their normal values. Describe control (intrinsic & extrinsic)
CARDIAC OUTPUT,VENOUS RETURN AND THEIR REGULATION. DR.HAROON RASHID. OBJECTIVES Define Stroke volume, Cardiac output Venous return,& identity their normal values. Describe control (intrinsic & extrinsic)
The circulatory system
 Introduction to Physiology (Course # 72336) 1 הלב עקרונות בסיסיים (הכנה למעבדת לב) Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
Introduction to Physiology (Course # 72336) 1 הלב עקרונות בסיסיים (הכנה למעבדת לב) Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
Approximately the size of your fist Location. Pericardial physiology
 Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Cardiovascular System
 Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition
 TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
I. Cardiac Output Chapter 14
 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Introduction to Physiology (Course # 72336) 1. Adi Mizrahi Textbook Chapter 12
 Introduction to Physiology (Course # 72336) 1 עקרונות בסיסיים (הכנה למעבדת לב) הלב Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
Introduction to Physiology (Course # 72336) 1 עקרונות בסיסיים (הכנה למעבדת לב) הלב Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
Circulation: Chapter 25. Cardiac Output. The Mammalian Heart Fig Right side of the heart
 Circulation: Chapter 25 1. Limits of Diffusion A. Small organisms use diffusion B. rapid over small distances 2. Most animals have circulatory systems A. Blood B. Pump (Heart) or propulsive structures
Circulation: Chapter 25 1. Limits of Diffusion A. Small organisms use diffusion B. rapid over small distances 2. Most animals have circulatory systems A. Blood B. Pump (Heart) or propulsive structures
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
THE CARDIOVASCULAR SYSTEM
 THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
Circulation. Sinoatrial (SA) Node. Atrioventricular (AV) Node. Cardiac Conduction System. Cardiac Conduction System. Linked to the nervous system
 Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Chapter 18 - Heart. I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity)
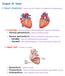 Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Cardiac Cycle MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Cardiac Properties MCQ
 Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
The Heart. C h a p t e r. PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris
 C h a p t e r 20 The Heart PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings Introduction
C h a p t e r 20 The Heart PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings Introduction
BME 5742 Bio-Systems Modeling and Control. Lecture 41 Heart & Blood Circulation Heart Function Basics
 BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
CHAPTER 4: The cardiovascular system
 CHAPTER 4: The cardiovascular system Question - text book page 52 Why does the human body need a double circulatory system? There are two circulatory systems with quite distinct functions The pulmonary
CHAPTER 4: The cardiovascular system Question - text book page 52 Why does the human body need a double circulatory system? There are two circulatory systems with quite distinct functions The pulmonary
ADVANCED ASSESSMENT Cardiovascular System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Cardiovascular System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Cardiovascular System AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Cardiovascular System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Cardiovascular System AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Topics to be Covered. Cardiac Measurements. Distribution of Blood Volume. Distribution of Pulmonary Ventilation & Blood Flow
 Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM
 Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Why would epidural analgesia cause these symptoms? How would increasing the blood volume change venous pressure (VP)?
 CASE 12 A 25-year-old pregnant woman is in labor at the hospital. She has no medical problems and has had no complications with this pregnancy. She is in the active phase of labor, feeling intense contractions,
CASE 12 A 25-year-old pregnant woman is in labor at the hospital. She has no medical problems and has had no complications with this pregnancy. She is in the active phase of labor, feeling intense contractions,
Heart. Structure Physiology of blood pressure and heartbeat
 Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
The Cardiovascular System
 11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
Major Function of the Cardiovascular System. Transportation. Structures of the Cardiovascular System. Heart - muscular pump
 Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co.
 Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
Cardiovascular Physiology: Cardiovascular (CV) adjustment during exercise:
 Cardiovascular Physiology: Cardiovascular (CV) adjustment during exercise: By Dr Dler Gallaly (Lecturer) PhD in Medical Physiology- Dept. of Physiology, College of Medicine, HMU- Erbil- Iraq. 2016 / 2017
Cardiovascular Physiology: Cardiovascular (CV) adjustment during exercise: By Dr Dler Gallaly (Lecturer) PhD in Medical Physiology- Dept. of Physiology, College of Medicine, HMU- Erbil- Iraq. 2016 / 2017
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Chapter 6: The Cardiovascular System and Its Control
 Part II: Cardiovascular and Respiratory Function (6 th Edition) Why do we need cardiorespiratory systems? As organisms became more complex, lost touch with the environment---beyond simple diffusion! Chapter
Part II: Cardiovascular and Respiratory Function (6 th Edition) Why do we need cardiorespiratory systems? As organisms became more complex, lost touch with the environment---beyond simple diffusion! Chapter
THE HEART Dr. Ali Ebneshahidi
 THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
Physiology of Circulation. Dr. Hiwa Shafiq 16/12/2018
 Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Circulatory system ( 循环系统 )
 Circulatory system ( 循环系统 ) Circulatory system: heart + blood vessels Function: nutrient transportation and metabolites returning Blood: carrier Heart: pump Blood vessels: route, substance communications
Circulatory system ( 循环系统 ) Circulatory system: heart + blood vessels Function: nutrient transportation and metabolites returning Blood: carrier Heart: pump Blood vessels: route, substance communications
Lecture 13: The Cardiovascular System ref: Cardiovascular Physiology, D. Mohrman and L. Heller, 4th ed. McGraw-Hill (1997)
 Lecture 13: The Cardiovascular System ref: Cardiovascular Physiology, D. Mohrman and L. Heller, 4th ed. McGraw-Hill (1997) Blood Heart Blood Vessels Arteries - capillaries - Veins Ventilation-Perfusion
Lecture 13: The Cardiovascular System ref: Cardiovascular Physiology, D. Mohrman and L. Heller, 4th ed. McGraw-Hill (1997) Blood Heart Blood Vessels Arteries - capillaries - Veins Ventilation-Perfusion
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5
 BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5 1. Heart Functions a. Generates pressure that propels blood thru blood vessels. (Tissue perfusion.) b. Separates oxygenated
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5 1. Heart Functions a. Generates pressure that propels blood thru blood vessels. (Tissue perfusion.) b. Separates oxygenated
- what other structures, besides the heart, does the mediastinum contain?
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) An Introduction to the Cardiovascular System - read the paragraphs under this heading on page 580 The Heart is a Four Chambered Organ describe
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) An Introduction to the Cardiovascular System - read the paragraphs under this heading on page 580 The Heart is a Four Chambered Organ describe
The Circulatory System. The Heart, Blood Vessels, Blood Types
 The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
Unit 10 ~ Learning Guide
 Unit 10 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 10 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Practice Exercises for the Cardiovascular System
 Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
Responses to Changes in Posture QUESTIONS. Case PHYSIOLOGY CASES AND PROBLEMS
 64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
