A review of the management of complex para-pneumonic effusion in adults
|
|
|
- Rosamund Terry
- 6 years ago
- Views:
Transcription
1 Review Article A review of the management of complex para-pneumonic effusion in adults Vikas Koppurapu, Nikhil Meena Department of Internal Medicine, University of Arkansas for Medical Sciences, Little Rock, Arkansas, USA Contributions: (I) Conception and design: All authors; (II) Administrative support: All authors; (III) Provision of study materials or patients: All authors; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Nikhil Meena W Markham St. Slot #555, Little Rock, AR 72205, USA. nkmeena@uams.edu. Abstract: A complex para-pneumonic effusion is a descriptive term for exudative effusions, which complicate or are likely to complicate the anatomy of the pleural space after pneumonia. We performed an online search was performed using the resources PubMed and Google Scholar to provide an update on the management of such effusions based on review of published literature. Search terms including pleural effusion (PE), parapneumonic effusion, and empyema were used. Relevant studies were identified and original articles were studied, compared and summarized. References in these articles were examined for relevance and included where appropriate. Studies involving pediatric patients were excluded. Management of para-pneumonic PE has changed tremendously over the last decade. As we accumulate more evidence in this area, approach to pleural fluid drainage is becoming more specific and guideline based. An example of a practice changing study in this aspect is the Multi-center Intrapleural Streptokinase Trial (MIST) 2 trial which demonstrated that a combination of intra-pleural tpa and DNAse improved outcomes in pleural infections compared to DNase or t-pa alone. More randomized control trials are needed to describe the role of surgical techniques like VATS (video-assisted thoracoscopic surgery) when MIST 2 protocol fails; this combination has revolutionized the management of empyema in recently. Keywords: Pleural effusion (PE); para-pneumonic effusion; empyema; thoracentesis; tube thoracostomy; video assisted thoracoscopic surgery (VATS); decortication Submitted May 07, Accepted for publication May 24, doi: /jtd View this article at: Introduction The pleural sac is the space between the lung (lined by visceral pleura) and the chest wall (lined by the parietal pleura). This space normally contains a thin layer of fluid called the pleural fluid, which functions as a lubricant and assists in reducing friction between the two lining surfaces during respiration. The pleural fluid is produced by the capillaries in parietal pleura and is absorbed by the lymphatics in the parietal pleura, which can under normal circumstances absorb the fluid at rate of about 20 times the rate of production (1). Under certain disease states, the fluid can also enter the pleural cavity from the lung interstitium via the visceral pleura or from the communications across the diaphragm to the peritoneal space (2). A pleural effusion (PE) is said to be present when there is excessive fluid within the pleural space and occurs when the rate of accumulation of the fluid exceeds the rate of drainage. Patients suspected of having PE are evaluated further typically by imaging of the chest like a chest roentgenogram or ultrasound or CT scan to further characterize the effusion. Once the presence of PE is established, the next step to acquire and analyze the pleural fluid (3). Broadly, the effusions are classified as either transudative or exudative (4). Transudative effusions are caused by systemic factors like congestive heart failure (CHF) or nephrotic syndrome which alter the hydrostatic and/or
2 2136 Koppurapu and Meena. Management of complex effusions oncotic forces across the capillaries involved in formation or removal of the pleural fluid (5). Exudative effusions on the other hand are usually caused by local factors like inflammation of pleura or the lungs. Other mechanisms of exudative effusions include impaired lymphatic drainage of the pleural fluid, disruption of thoracic duct and movement of peritoneal fluid through connections across the diaphragm, etc. (6). The most widely used criteria for differentiation of transudative and exudative effusions are the Light s criteria which as follows (4). (I) Pleural fluid protein/serum protein ratio greater than 0.5; (II) Pleural fluid lactate dehydrogenase (LDH)/serum LDH ratio greater than 0.6; (III) Pleural fluid LDH level greater than two-thirds the upper limit of the laboratory s reference range of serum LDH. The effusion is considered to be exudative when one of the three criteria is met. If none of the criteria are met, the effusion is considered to be transudative. Transudative effusions usually respond to medical treatment of the systemic factors contributing to the effusion. However, the exudative effusions can pose a diagnostic and therapeutic challenge, often needing non-surgical/surgical intervention(s) in addition to medical management (6,7). Overview of management of exudative effusions The first step in the management of a new onset PE is a diagnostic thoracentesis or tap (6). Only in few specific circumstances is a tap not warranted, for example if there is a strong suspicion of heart failure as a cause of the effusion(s), then a trial of medical therapy for heart failure can be done prior to a thoracentesis (8). The differentiation between transudative and exudative effusions is made based on the analysis of pleural fluid as explained above. Certain characteristics of the pleural fluid increase the possibility of the effusion being complicated, which include: loculated fluid, ph <7.2, glucose <60 mg/dl, positive gram stain or culture and gross purulence. In the presence of these factors or if the fluid re-accumulates after initial tap, a repeat thoracentesis should be performed (9). If the fluid can t be completely removed, then there are various options available including tube thoracostomy, use of intrapleural fibrinolytics, video assisted thoracoscopic surgery (VATS) and open drainage (OD) (10). Discussing the utility of these various procedures is the crux of this review. Management of parapneumonic effusions Parapneumonic pleural effusion (PPE) refers to a PE associated with a focus of infection in the lungs, which can be bacterial pneumonia, a pulmonary abscess, or infected bronchiectasis (11). It is seen in about 20% of the hospitalized patients with pneumonia (12) and approximately 1 million patients develop PPEs annually in the United States (US) (13). Empyema is said to be present when there is gross purulence or presence of bacteria in the pleural fluid as evidenced by gram stain. It is divided into early (stage I or exudative) and advanced stages (stage II or fibrinopurulent; and stage III or organizing). Also, the presence of thickened parietal pleura on contrast enhanced CT scan is suggestive of empyema (14-16). The rate of parapneumonic empyema related hospitalizations in the US have doubled from 1996 to 2008 and the trend was observed across all age groups (17). Empyema is associated with substantial cost burden and remains an important cause of morbidity and mortality. Early diagnosis, appropriate antimicrobial therapy and adequate drainage of effusion are important in decreasing morbidity and mortality (18). Antibiotic therapy must cover the bacteria implicated in causing pneumonia in that particular setting. Also, anaerobic coverage must be added if there is clinical suspicion or microbiological evidence of involvement of anaerobic bacteria in the infection. The decision to drain the PPE is made based on three important considerations: pleural space anatomy, pleural fluid chemistry and pleural fluid microbiology. A panel developed by the Health and Science Policy Committee of the American College of Chest Physicians classified PPE into four groups based on risk for poor outcome, which is presented in Table 1 at the end of the article (25). Based on the consensus opinion, the panel recommended that patients with category 1 and category 2 risk for poor outcome with PPE may not require drainage; however, drainage was recommended for management of category 3 and 4 PPE. Therapeutic thoracentesis or tube thoracostomy alone may be insufficient treatment for managing most patients with category 3 or 4 PPE. Fibrinolytics, VATS, and surgery are acceptable approaches for managing patients with category 3 and category 4 PPE which do not respond to less invasive drainage methods. The panel however exercised caution while interpreting the above recommendations as some of the studies reviewed has revealed conflicting data (26,27). Though antibiotic therapy alone may be sufficient in
3 Journal of Thoracic Disease, Vol 9, No 7 July Table 1 Classification of PPE based on risk for poor outcome Drainage Category Risk for poor outcome Pleural space anatomy Option Pleural fluid bacteriology Option Pleural fluid chemistry (19-21) And C x ph unknown 1 Very low No (22) And B x culture and gram stain results unknown A 0 minimal, free flowing effusion (<10 mm on lateral decubitus) And C 0 ph >/ Low No And B 0 negative gram stain and cultures (regardless of exposure to antibiotics) A 1 small to moderate, free flowing effusion (>10 mm, but < half of hemithorax) Or B 1 positive gram stain or cultures Or C 1 ph < Moderate Yes (23,24) B 2 pus 4 High Yes A 2 large, free flowing effusion ( half of hemithorax), loculated effusion or effusion with thickened parietal pleura PPE, parapneumonic pleural effusion. certain cases, it remains to be ascertained whether early fluid drainage of complicated effusions has better outcomes compared to conservative therapy alone in such cases (28,29). Regardless, antibiotic therapy is mandatory in all cases of PPE. The following approach is reasonable based on the risk category: (I) Category 1 PPE: medical treatment alone; (II) Category 2 PPE: pleural fluid sampling (via thoracentesis) must be done, with drainage of all free flowing fluid, if a small bore catheter is used; (III) Category 3 and 4 PPE: tube thoracostomy must be performed and clinical status reviewed in 24 hours. If there is incomplete drainage, then intrapleural fibrinolytics must be instituted. After this, if there is incomplete resolution at 72 hours, then surgical drainage is warranted. Tube thoracostomy Tube thoracostomy or chest tube drainage is the least invasive method of draining the pleural fluid after therapeutic thoracentesis. For free flowing fluid which is uniloculated, chest tube drainage usually works well. However, this form of drainage is also frequently used, at least as the initial approach in the management of multiloculated effusions as well. While multiloculated effusions are typically drained using smaller bore catheters to allow placement of multiple tubes, the uniloculated effusions were traditionally drained using large bore catheters to allow thick, viscous fluid to be drained. However, with increasing evidence suggesting that smaller tubes are not associated with inferior outcomes, large bore tubes are falling out of favor. The Multi-center Intrapleural Streptokinase Trial (MIST 1) concluded that there was no significant difference in mortality or need for thoracic surgery among large (15 20 F), medium (10 14 F), or small (<10 F) tubes (30). Also, patients on whom large bore tubes were used complained of significantly higher level of pain. Chest tube insertions for complicated effusions must be done under imaging guidance as the added cost for the procedure is expected to be more than compensated by the increased success of drainage (31). Some studies have shown that performer skills in chest tube insertion may be better in those who undergo training on cadavers and medical simulators compared to the conventional methods of training (32,33). Regular flushes can help maintain the patency of small bore catheters, especially when the fluid is thick. A post procedure CT
4 2138 Koppurapu and Meena. Management of complex effusions scan within 24 hrs is needed to confirm proper placement. Chest tubes are usually left in place until the daily output from the tube falls below 50 ml. Thoracoscopic debridement VATS allows for a safe, effective and relatively less invasive means of drainage of pleural fluid and has the advantage of being able to be converted to thoracotomy if adequate drainage is not achieved. Both debridement and decortication can be performed through VATS. It has also been considered as the gold standard diagnostic procedure for investigation of pleural exudates. In one study, empyema fluid culture positivity with VATS (84.6%) was significantly higher than pre-vats fluid culture (35%). While chest tube drainage alone may be sufficient for early stage empyema, the more advanced stages have a high mortality rate without more advanced methods of drainage. For example, one study evaluated outcomes for different procedures in advanced empyema (defined as stage II or more). The success rate (no death, no additional drainage procedures) with VATS (around 80%) was double the success rate of tube thoracostomy (40%) and was comparable with that of thoracotomy (89%) (34). Common indications for VATS drainage include multiloculated empyema, empyema refractory to tube thoracostomy and presence of pleural peel (35). In one retrospective study, the success rate for drainage of early stage multiloculated empyema was 66%, 95% and 100% in the tube thoracostomy, fibrinolytic therapy and VATS groups, respectively (36). The relatively high success rate and lack of significant morbidity makes VATS a preferred method of drainage. Though the safety and benefit of VATS have been documented beyond doubt in multiple studies, there are no evidence based recommendations on the precise stage and timing for VATS. VATS has revolutionized the management of empyema in the last decade and its role has progressed from a diagnostic purpose to an intermediate procedure for empyemas refractory to medical therapy and as an early drainage procedure for complicated empyemas in order to spare invasive surgery. There is data suggesting improved outcomes with VATS as a primary drainage method compared to chest tube drainage at no significant cost difference. More studies are needed to further establish the benefit of VATS as a primary drainage procedure, especially from the cost perspective and there is a possibility of a paradigm shift in the future in the initial drainage approach for empyema (37). VATS decortication (VATSD) was initially evaluated as a treatment option for early (stage I) empyema. However, recently, several studies have suggested superior outcomes with VATSD compared to Open Decortication (OD) even in advanced stage II and stage III empyema. Still, there is some concern expressed about the ability of VATSD to achieve complete decortication in advanced empyema. In the near future, VATSD can be expected to evolve as the preferred approach for management of even advanced empyema compared to OD. Intrapleural fibrinolytics and DeoxyriboNuclease (DNase) There is conflicting evidence and opinion about the use of fibrinolytics alone to assist in the drainage of complicated effusions. The earlier supposition that intrapleural fibrinolytics improved outcomes, which was based on small trials and case series (38-42) was refuted by a meta-analysis (43) and the MIST 1 trial (44). A Cochrane review of 7 studies recruiting 761 patients did not show any difference in mortality with the use of fibrinolytics. However, it was found that the use of fibrinolytics decreased the need for surgical intervention, except that such a benefit was not shown in the newer MIST 1 trial that was included in the review. A more recent double blinded randomized cross over study showed that intra pleural alteplase (25 mg) was associated with less treatment failure (which was defined as <50% improvement of effusion on CT scan) compared to placebo. The dose range of intrapleural TPA is reported to be between 10 and 100 mg daily with most patients needing 3 to 4 doses (41). Adverse reactions with intra-pleural fibrinolytics include pain, fever and allergic reactions. Intrapleural fibrinolysis is not associated with systemic thrombolysis and one study showed that pleural hemorrhage occurred only in those who were on systemic anticoagulation when receiving intrapleural fibrinolytics. The main component contributing to viscosity of exudative fluid is DNA which led to the use of intrapleural DNase in the management of complicated effusions. The MIST 2 trial which was a double blind randomized study concluded that Intrapleural t-pa-dnase therapy improved fluid drainage in patients with pleural infection and reduced the frequency of surgical referral and the duration of the hospital stay (45). Treatment with DNase alone or t-pa alone was concluded to be ineffective. Another multinational observation study looked at the outcomes in 107 patients who received intrapleural tpa/
5 Journal of Thoracic Disease, Vol 9, No 7 July DNase. Treatment success at 30 days, volume of pleural fluid drained, improvement in radiographic pleural opacity and inflammatory markers, need for surgery, and adverse events were the measured outcomes. Over 90% of the patients were successfully managed with intrapleural tpa/dnase and did not need surgical intervention. Majority of the patients received tpa/dnase more than 24 hours after failing antibiotics and tube thoracostomy. Fluid drained increased from a median of 250 ml in the 24 hours preceding commencement of intrapleural therapy to 2,475 ml in the 72 hours following treatment initiation (P<0.05). There was a corresponding decrease in pleural opacity and C-reactive protein. Adverse events included pain and non-fatal bleeding. With these recent studies, it is reasonable to conclude that intrapleural tpa/dnase is a safe and effective drainage option (unlike tpa alone which had conflicting evidence) especially as a rescue therapy for patients who do not respond to initial conservative management with antibiotics and chest tube drainage (46). While, it is clear that tpa/dnaase is helpful, the exact dosing may still need to be determined so as to have maximal beneficence and minimal complications. OD Advanced stages of empyema are characterized by deposition of fibrin on the pleural surfaces and formation of pleural peel, which can limit re-expansion of the lung leading to significant symptoms. In such late stages, decortication/total pleurectomy is usually needed to allow the re-expansion of the lung. The invasive option is usually reserved for patients whose exercise tolerance and quality of life remain limited for over six months due to the fibrotic changes in the pleura. Though OD was traditionally used for these advanced empyemas, new evidence suggests better outcomes with VATSD, which is taking over OD as the initial procedure of choice for such empyemas (47). One study analyzed the predicting factors for conversion thoracotomy and OD following VATS. Factors studied included age, sex, presence of bacteria, presence of gram-positive and gram-negative organisms, and time interval between onset of symptoms and surgery, as well as different etiologic groups (postpneumonic, postoperative, posttraumatic, postembolic, tuberculosis). It was found that delayed referral (>2 weeks) and presence of gram-negative microorganisms were the only significant predictors for conversion thoracotomy in a multivariate analysis (48). Conclusions Management of complex pleural effusion remains ever changing. VATS debridement if fibrinolytics fail seems to have the best outcome. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Light RW. Disorders of the pleura. Harrison s principles of Internal Medicine. 19th edition. McGraw Hill, 2015: Porcel JM, Light RW. Diagnostic approach to pleural effusion in adults. Am Fam Physician 2006;73: Saguil A, Wyrick K, Hallgren J. Diagnostic approach to pleural effusion. Am Fam Physician 2014;90: Light RW, Macgregor MI, Luchsinger PC, et al. Pleural effusions: the diagnostic separation of transudates and exudates. Ann Intern Med 1972;77: Chetty KG. Transudative pleural effusions. Clin Chest Med 1985;6: Sahn SA. The differential diagnosis of pleural effusions. West J Med 1982;137: Light RW. Diagnostic principles in pleural disease. Eur Respir J 1997;10: Light RW. Clinical practice. Pleural effusion. N Engl J Med 2002;346: Light RW, Rodriguez RM. Management of parapneumonic effusions. Clin Chest Med 1998;19: Na MJ, Dikensoy O, Light RW. New trends in the diagnosis and treatment in parapneumonic effusion and empyema. Tuberk Toraks 2008;56: Ferreiro L, San José ME, Valdés L. Management of Parapneumonic Pleural Effusion in Adults. Arch Bronconeumol 2015;51: Porcel JM, Light RW. Parapneumonic pleural effusions and empyema in adults: current practice. Rev Clin Esp 2009;209: Sahn SA. Diagnosis and management of parapneumonic effusions and empyema. Clin Infect Dis 2007;45:
6 2140 Koppurapu and Meena. Management of complex effusions 14. Waite RJ, Carbonneau RJ, Balikian JP, et al. Parietal pleural changes in empyema: appearances at CT. Radiology 1990;175: Aquino SL, Webb WR, Gushiken BJ. Pleural exudates and transudates: diagnosis with contrast-enhanced CT. Radiology 1994;192: Kirsch E, Gückel C, Kaim A, et al. The findings and value of computed tomography in pleural empyema. Rofo 1994;161: Grijalva CG, Zhu Y, Nuorti JP, et al. Emergence of parapneumonic empyema in the USA. Thorax 2011;66: Ashbaugh DG. Empyema thoracis. Factors influencing morbidity and mortality. Chest 1991;99: Heffner JE, Brown LK, Barbieri C, et al. Pleural fluid chemical analysis in parapneumonic effusions. A metaanalysis. Am J Respir Crit Care Med 1995;151: Lesho EP, Roth BJ. Is ph paper an acceptable, low-cost alternative to the blood gas analyzer for determining pleural fluid ph? Chest 1997;112: Cheng DS, Rodriguez RM, Rogers J, et al. Comparison of pleural fluid ph values obtained using blood gas machine, ph meter, and ph indicator strip. Chest 1998;114: Light RW, Girard WM, Jenkinson SG, et al. Parapneumonic effusions. Am J Med 1980;69: Ferguson AD, Prescott RJ, Selkon JB, et al. The clinical course and management of thoracic empyema. QJM 1996;89: Himelman RB, Callen PW. The prognostic value of loculations in parapneumonic pleural effusions. Chest 1986;90: Colice GL, Curtis A, Deslauriers J, et al. Medical and surgical treatment of parapneumonic effusions: an evidence-based guideline. Chest 2000;118: Wait MA, Sharma S, Hohn J, et al. A randomized trial of empyema therapy. Chest 1997;111: Angelillo Mackinlay TA, Lyons GA, Chimondeguy DJ, et al. VATS debridement versus thoracotomy in the treatment of loculated postpneumonia empyema. Ann Thorac Surg 1996;61: Berger HA, Morganroth ML. Immediate drainage is not required for all patients with complicated parapneumonic effusions. Chest 1990;97: Lim TK. Management of parapneumonic pleural effusion. Curr Opin Pulm Med 2001;7: Rahman NM, Maskell NA, Davies CW, et al. The relationship between chest tube size and clinical outcome in pleural infection. Chest 2010;137: Moulton JS. Image-guided management of complicated pleural fluid collections. Radiol Clin North Am 2000;38: Chung TN, Kim SW, You JS, et al. Tube thoracostomy training with a medical simulator is associated with faster, more successful performance of the procedure. Clin Exp Emerg Med 2016;3: Takayesu JK, Peak D, Stearns D. Cadaver-based training is superior to simulation training for cricothyrotomy and tube thoracostomy. Intern Emerg Med 2017;12: Wozniak CJ, Paull DE, Moezzi JE, et al. Choice of first intervention is related to outcomes in the management of empyema. Ann Thorac Surg 2009;87: ; discussion Luh SP, Chou MC, Wang LS, et al. Video-assisted thoracoscopic surgery in the treatment of complicated parapneumonic effusions or empyemas: outcome of 234 patients. Chest 2005;127: Metin M, Yeginsu A, Sayar A, et al. Treatment of multiloculated empyema thoracis using minimally invasive methods. Singapore Med J 2010;51: Zahid I, Nagendran M, Routledge T, et al. Comparison of video-assisted thoracoscopic surgery and open surgery in the management of primary empyema. Curr Opin Pulm Med 2011;17: Davies RJ, Traill ZC, Gleeson FV. Randomised controlled trial of intrapleural streptokinase in community acquired pleural infection. Thorax 1997;52: Bouros D, Schiza S, Tzanakis N, et al. Intrapleural urokinase versus normal saline in the treatment of complicated parapneumonic effusions and empyema. A randomized, double-blind study. Am J Respir Crit Care Med 1999;159: Diacon AH, Theron J, Schuurmans MM, et al. Intrapleural streptokinase for empyema and complicated parapneumonic effusions. Am J Respir Crit Care Med 2004;170: Thommi G, Nair CK, Aronow WS, et al. Efficacy and safety of intrapleural instillation of alteplase in the management of complicated pleural effusion or empyema. Am J Ther 2007;14: Tuncozgur B, Ustunsoy H, Sivrikoz MC, et al. Intrapleural urokinase in the management of parapneumonic empyema: a randomised controlled trial. Int J Clin Pract 2001;55: Tokuda Y, Matsushima D, Stein GH, et al. Intrapleural fibrinolytic agents for empyema and complicated parapneumonic effusions: a meta-analysis. Chest
7 Journal of Thoracic Disease, Vol 9, No 7 July ;129: Maskell NA, Davies CW, Nunn AJ, et al. U.K. Controlled trial of intrapleural streptokinase for pleural infection. N Engl J Med 2005;352: Rahman NM, Maskell NA, West A, et al. Intrapleural use of tissue plasminogen activator and DNase in pleural infection. N Engl J Med 2011;365: Piccolo F, Pitman N, Bhatnagar R, et al. Intrapleural tissue plasminogen activator and deoxyribonuclease for pleural infection. An effective and safe alternative to surgery. Ann Am Thorac Soc 2014;11: Shahin Y, Duffy J, Beggs D, et al. Surgical management of primary empyema of the pleural cavity: outcome of 81 patients. Interact Cardiovasc Thorac Surg 2010;10: Lardinois D, Gock M, Pezzetta E, et al. Delayed referral and gram-negative organisms increase the conversion thoracotomy rate in patients undergoing video-assisted thoracoscopic surgery for empyema. Ann Thorac Surg 2005;79: Cite this article as: Koppurapu V, Meena N. A review of the management of complex para-pneumonic effusion in adults. J Thorac Dis 2017;9(7): doi: /jtd
Modern Approaches to Empyema
 Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
aacp consensus statement
 aacp consensus statement Medical and Surgical Treatment of Parapneumonic Effusions* An Evidence-Based Guideline Gene L. Colice, MD, FCCP; Anne Curtis, MD; Jean Deslauriers, MD; John Heffner, MD, FCCP;
aacp consensus statement Medical and Surgical Treatment of Parapneumonic Effusions* An Evidence-Based Guideline Gene L. Colice, MD, FCCP; Anne Curtis, MD; Jean Deslauriers, MD; John Heffner, MD, FCCP;
Alper Toker, MD. VATS decortication. Istanbul University, Istanbul Medical School Department of Thoracic Surgery
 VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
EMPYEMA. Catheter Based Treatment vs. VATS. UCHSC Department of Surgery Grand Rounds August 27 th, Jeremy Hedges, M.D.
 EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
Treatment of multiloculated empyema thoracis using minimally invasive methods
 O r i g i n a l A r t i c l e Singapore Med J 2010; 51(3) : 242 Treatment of multiloculated empyema thoracis using minimally invasive methods Metin M, Yeginsu A, Sayar A, Alzafer S, Solak O, Ozgul A, Erkorkmaz
O r i g i n a l A r t i c l e Singapore Med J 2010; 51(3) : 242 Treatment of multiloculated empyema thoracis using minimally invasive methods Metin M, Yeginsu A, Sayar A, Alzafer S, Solak O, Ozgul A, Erkorkmaz
Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children. Saeed Al Hindi, MD, CABS, FRCSI*
 Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Best timing for surgical intervention of empyema. Supervisor: Intern:
 Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
Outcomes & Clinical Trials Update: Empyema & NEC
 Outcomes & Clinical Trials Update: Empyema & NEC American Pediatric Surgical Association Outcomes & Clinical Trials Committee Fizan Abdullah, Chair Saleem Islam, Vice Chair Gudrun Aspelund Catherine C.
Outcomes & Clinical Trials Update: Empyema & NEC American Pediatric Surgical Association Outcomes & Clinical Trials Committee Fizan Abdullah, Chair Saleem Islam, Vice Chair Gudrun Aspelund Catherine C.
Post Pneumonic Empyema: Is There Still a Role for Surgery?
 Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
Parapneumonic effusions are a common problem
 Proceeding S.Z.P.G.M.I. vol: 20(2): pp. 9-3, 200. Intrapleural Streptokinase in Management of Complicated Parapneumonic Effusion and Empyema Kamran Hameed, Ahmad Hasan Banjer, Mohammad Abdul-Aziz Siddiqui
Proceeding S.Z.P.G.M.I. vol: 20(2): pp. 9-3, 200. Intrapleural Streptokinase in Management of Complicated Parapneumonic Effusion and Empyema Kamran Hameed, Ahmad Hasan Banjer, Mohammad Abdul-Aziz Siddiqui
Surgical decortication as the first-line treatment for pleural empyema
 Shin et al General Thoracic Surgical decortication as the first-line treatment for pleural empyema Jung Ar Shin, MD, a Yoon Soo Chang, MD, PhD, a Tae Hoon Kim, MD, PhD, b Seok Jin Haam, MD, c Hyung Jung
Shin et al General Thoracic Surgical decortication as the first-line treatment for pleural empyema Jung Ar Shin, MD, a Yoon Soo Chang, MD, PhD, a Tae Hoon Kim, MD, PhD, b Seok Jin Haam, MD, c Hyung Jung
Posttraumatic Empyema Thoracis
 Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20,
 Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME
 VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME Paolo Claudio Cassina, MD a Markus Hauser, MD, FCCP b Ludger Hillejan, MD a Dieter Greschuchna, MD a
VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME Paolo Claudio Cassina, MD a Markus Hauser, MD, FCCP b Ludger Hillejan, MD a Dieter Greschuchna, MD a
A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion
 Original Article A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion Che-Chia Chang 1,2, Tzu-Ping Chen 1, Chi-Hsiao Yeh 1, Pin-Fu Huang 1,
Original Article A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion Che-Chia Chang 1,2, Tzu-Ping Chen 1, Chi-Hsiao Yeh 1, Pin-Fu Huang 1,
Fibrinolytic Therapy in Complicated Parapneumonic Effusions and Empyema
 Fibrinolytic Therapy in Complicated Parapneumonic Effusions and Empyema MS Barthwal Pulmonologist and Medical Specialist, Department of Respiratory Medicine, Military Hospital (Cardio Thoracic Center),
Fibrinolytic Therapy in Complicated Parapneumonic Effusions and Empyema MS Barthwal Pulmonologist and Medical Specialist, Department of Respiratory Medicine, Military Hospital (Cardio Thoracic Center),
Case Report Intrapleural administration of DNase alone for pleural empyema
 Int J Clin Exp Med 2015;8(11):22011-22015 www.ijcem.com /ISSN:1940-5901/IJCEM0016173 Case Report Intrapleural administration of DNase alone for pleural empyema Vladimir Bobek 1,2,3, Andrzej Majewski 4,
Int J Clin Exp Med 2015;8(11):22011-22015 www.ijcem.com /ISSN:1940-5901/IJCEM0016173 Case Report Intrapleural administration of DNase alone for pleural empyema Vladimir Bobek 1,2,3, Andrzej Majewski 4,
Intrapleural Fibrinolytic Therapy in Complicated Parapneumonic Effusion and Empyema: Present Status
 Review Article Intrapleural Fibrinolytic Therapy in Complicated Parapneumonic Effusion and Empyema: Present Status Col (Dr) M.S. Barthwal Department of Pulmonary Medicine, Military Hospital, Namkum, Ranchi,
Review Article Intrapleural Fibrinolytic Therapy in Complicated Parapneumonic Effusion and Empyema: Present Status Col (Dr) M.S. Barthwal Department of Pulmonary Medicine, Military Hospital, Namkum, Ranchi,
Pleural Fluid Analysis: Back to Basics
 Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
APPROACH TO PLEURAL EFFUSIONS. Raed Alalawi, MD, FCCP
 APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
Surgery should be the first line of treatment for empyemaresp_1677
 202..207 PRO/CON DEBATE Surgery should be the first line of treatment for empyemaresp_1677 IOANNIS E. PETRAKIS, 1 JOHN E. HEFFNER 2 * AND JEFFREY S. KLEIN 3 1 Department of General and Thoracic Surgery,
202..207 PRO/CON DEBATE Surgery should be the first line of treatment for empyemaresp_1677 IOANNIS E. PETRAKIS, 1 JOHN E. HEFFNER 2 * AND JEFFREY S. KLEIN 3 1 Department of General and Thoracic Surgery,
@ERSpublications Does pleural irrigation improve pleural fluid drainage and resolution of sepsis in pleural infection?
 ORIGINAL ARTICLE RESPIRATORY INFECTIONS Pleural irrigation trial (PIT): a randomised controlled trial of pleural irrigation with normal saline versus standard care in patients with pleural infection Clare
ORIGINAL ARTICLE RESPIRATORY INFECTIONS Pleural irrigation trial (PIT): a randomised controlled trial of pleural irrigation with normal saline versus standard care in patients with pleural infection Clare
Guidelines/Guidance/CAP/ Hospitalized Child. PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014
 Guidelines/Guidance/CAP/ Hospitalized Child PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014 CAP in Children: Epi Greatest cause of death in children worldwide Estimated > 2 M deaths in children In developed
Guidelines/Guidance/CAP/ Hospitalized Child PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014 CAP in Children: Epi Greatest cause of death in children worldwide Estimated > 2 M deaths in children In developed
Pleural infection. CME Respiratory medicine. Investigations. Clinical features. Chest x-ray. Pleural ultrasound
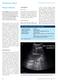 Clinical Medicine 2012, Vol 12, No 1: 82 6 Pleural infection John M Wrightson, clinical research fellow and respiratory specialist registrar, Oxford Pleural Unit, Churchill Hospital, Oxford and NIHR Oxford
Clinical Medicine 2012, Vol 12, No 1: 82 6 Pleural infection John M Wrightson, clinical research fellow and respiratory specialist registrar, Oxford Pleural Unit, Churchill Hospital, Oxford and NIHR Oxford
Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip*
 Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip* Dong-sheng Cheng, MD; R. Michael Rodriguez, MD; Jeffrey Rogers, RRT; Marvin Wagster; DanielL. Starnes,
Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip* Dong-sheng Cheng, MD; R. Michael Rodriguez, MD; Jeffrey Rogers, RRT; Marvin Wagster; DanielL. Starnes,
Complicated parapneumonic effusion and empyema thoracis: Microbiologic and therapeutic aspects
 Respiratory Medicine (2006) 100, 286 291 Complicated parapneumonic effusion and empyema thoracis: Microbiologic and therapeutic aspects Duygu Ozol, Sibel Oktem, Erturk Erdinc Department of Chest Disease,
Respiratory Medicine (2006) 100, 286 291 Complicated parapneumonic effusion and empyema thoracis: Microbiologic and therapeutic aspects Duygu Ozol, Sibel Oktem, Erturk Erdinc Department of Chest Disease,
Advances in the Management of Empyema
 Advances in the Management of Empyema RCP Update in Respiratory Medicine 26 th January 2017 Najib M Rahman Associate Professor of Respiratory Medicine University of Oxford najib.rahman@ndm.ox.ac.uk Financial
Advances in the Management of Empyema RCP Update in Respiratory Medicine 26 th January 2017 Najib M Rahman Associate Professor of Respiratory Medicine University of Oxford najib.rahman@ndm.ox.ac.uk Financial
The use of thrombolytics in the management of complex pleural fluid collections
 Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA
 MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
Trust Guideline for the management of Parapneumonic Effusion in children
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
Factors predictive of the failure of medical treatment in patients with pleural infection
 ORIGINAL ARTICLE Korean J Intern Med 2014;29:603-612 Factors predictive of the failure of medical treatment in patients with pleural infection Sung-Kyoung Kim 1, Chul Ung Kang 2, So Hyang Song 1, Deog
ORIGINAL ARTICLE Korean J Intern Med 2014;29:603-612 Factors predictive of the failure of medical treatment in patients with pleural infection Sung-Kyoung Kim 1, Chul Ung Kang 2, So Hyang Song 1, Deog
Surgical treatment of empyema in children
 Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
Clinical Medicine Insights: Circulatory, Respiratory and Pulmonary Medicine. Empyema Thoracis. Ala Eldin H. Ahmed 1,2 and Tariq E.
 Clinical Medicine Insights: Circulatory, Respiratory and Pulmonary Medicine REVIEW Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Empyema Thoracis Ala Eldin
Clinical Medicine Insights: Circulatory, Respiratory and Pulmonary Medicine REVIEW Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Empyema Thoracis Ala Eldin
Top Tips for Pleural Disease in 2012
 Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Empyema Thoracis* Therapeutic Management and Outcome
 Empyema Thoracis* Therapeutic Management and Outcome Gregory P. LeMense, MD; Charlie Strange, MD, FCCP; and Steven A. Sahn, MD, FCCP Study objective: We evaluated treatment and outcome of patients with
Empyema Thoracis* Therapeutic Management and Outcome Gregory P. LeMense, MD; Charlie Strange, MD, FCCP; and Steven A. Sahn, MD, FCCP Study objective: We evaluated treatment and outcome of patients with
Management of Pleural Empyema Using VATS with Jet-Lavage System
 Journal of Surgery 2018; 6(5): 135-139 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20180605.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Management of Pleural Empyema Using VATS
Journal of Surgery 2018; 6(5): 135-139 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20180605.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Management of Pleural Empyema Using VATS
Malignant Effusions. Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital
 Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Contemporary outcomes of surgical management of complex thoracic infections
 Original Article Contemporary outcomes of surgical management of complex thoracic infections Ian C. Bostock 1, Fariha Sheikh 1, Timothy M. Millington 1,2, David J. Finley 1,2, Joseph D. Phillips 1,2 1
Original Article Contemporary outcomes of surgical management of complex thoracic infections Ian C. Bostock 1, Fariha Sheikh 1, Timothy M. Millington 1,2, David J. Finley 1,2, Joseph D. Phillips 1,2 1
Review Article Management of Infectious Processes of the Pleural Space: A Review
 Pulmonary Medicine Volume 2012, Article ID 816502, 10 pages doi:10.1155/2012/816502 Review Article Management of Infectious Processes of the Pleural Space: A Review Ankur Girdhar, Adil Shujaat, and Abubakr
Pulmonary Medicine Volume 2012, Article ID 816502, 10 pages doi:10.1155/2012/816502 Review Article Management of Infectious Processes of the Pleural Space: A Review Ankur Girdhar, Adil Shujaat, and Abubakr
Tissue Plasminogen Activator for the Treatment of Parapneumonic Effusions in Pediatric Patients
 Tissue Plasminogen Activator for the Treatment of Parapneumonic Effusions in Pediatric Patients Emily N. Israel 1,2 and Allison B. Blackmer 1,2, * 1 Department of Pharmacy Services, University of Michigan
Tissue Plasminogen Activator for the Treatment of Parapneumonic Effusions in Pediatric Patients Emily N. Israel 1,2 and Allison B. Blackmer 1,2, * 1 Department of Pharmacy Services, University of Michigan
Diagnosis and Management of Parapneumonic Effusions and Empyema
 CLINICAL PRACTICE Ellie J. C. Goldstein, Section Editor INVITED ARTICLE Diagnosis and Management of Parapneumonic Effusions and Empyema Steve A. Sahn Division of Pulmonary, Critical Care, Allergy, and
CLINICAL PRACTICE Ellie J. C. Goldstein, Section Editor INVITED ARTICLE Diagnosis and Management of Parapneumonic Effusions and Empyema Steve A. Sahn Division of Pulmonary, Critical Care, Allergy, and
EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC CHANGES
 Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Guideline for management of children & adolescents with pleural empyema
 CHILD AND ADOLESCENT HEALTH SERVICE PRINCESS MARGARET HOSPITAL FOR CHILDREN Guideline for management of children & adolescents with pleural empyema This guideline provides an evidence-based framework for
CHILD AND ADOLESCENT HEALTH SERVICE PRINCESS MARGARET HOSPITAL FOR CHILDREN Guideline for management of children & adolescents with pleural empyema This guideline provides an evidence-based framework for
Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase
 European Journal of Cardio-thoracic Surgery 26 (2004) 503 507 www.elsevier.com/locate/ejcts Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase Gülşen Ekingen*,
European Journal of Cardio-thoracic Surgery 26 (2004) 503 507 www.elsevier.com/locate/ejcts Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase Gülşen Ekingen*,
Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy?
 Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy? Daniel T. L. Chan, MBBS, Alan D. L. Sihoe, FRCSEd, FCCP, Shun Chan, MBBS, Dickson S. F. Tsang, MBBS,
Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy? Daniel T. L. Chan, MBBS, Alan D. L. Sihoe, FRCSEd, FCCP, Shun Chan, MBBS, Dickson S. F. Tsang, MBBS,
Thoraxdrainage SGP Jahresversammlung 2016, Lausanne
 Thoraxdrainage SGP Jahresversammlung 2016, Lausanne Dr. med. Lukas Kern a bit of history (incomplete.) a bit of physiology (basic ) indication data guidelines a bit of history (incomplete.) a bit of physiology
Thoraxdrainage SGP Jahresversammlung 2016, Lausanne Dr. med. Lukas Kern a bit of history (incomplete.) a bit of physiology (basic ) indication data guidelines a bit of history (incomplete.) a bit of physiology
Manejo Práctico del Derrame Pleural
 Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases
 Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Thoracotomy and decortication in empyema: Clinical spectrum and outcome
 Original Article Thoracotomy and decortication in empyema: Clinical spectrum and outcome Shrestha KP*, Adhikari S**, Pokhrel DP*** *Associate Professor, **DM Resident, ***Professor NAMS ABSTRACT INTRODUCTION:
Original Article Thoracotomy and decortication in empyema: Clinical spectrum and outcome Shrestha KP*, Adhikari S**, Pokhrel DP*** *Associate Professor, **DM Resident, ***Professor NAMS ABSTRACT INTRODUCTION:
Effectiveness and Risks Associated With Intrapleural Alteplase by Means of Tube Thoracostomy
 Effectiveness and Risks Associated With Intrapleural Alteplase by Means of Tube Thoracostomy Sharon Ben-Or, MD, Richard H. Feins, MD, Nirmal K. Veeramachaneni, MD, and Benjamin E. Haithcock, MD Division
Effectiveness and Risks Associated With Intrapleural Alteplase by Means of Tube Thoracostomy Sharon Ben-Or, MD, Richard H. Feins, MD, Nirmal K. Veeramachaneni, MD, and Benjamin E. Haithcock, MD Division
Complicated parapneumonic effusion and empyema thoracis: microbiology and predictors of adverse outcomes
 O R I G I N A L A R T I C L E KY Tsang WS Leung Veronica L Chan Alsa WL Lin CM Chu Key words Empyema, pleural; Fibrinolytic agents; Guidelines; Pleural effusion; Pneumonia; Thoracic cavity Hong Kong Med
O R I G I N A L A R T I C L E KY Tsang WS Leung Veronica L Chan Alsa WL Lin CM Chu Key words Empyema, pleural; Fibrinolytic agents; Guidelines; Pleural effusion; Pneumonia; Thoracic cavity Hong Kong Med
Accepted Manuscript. Current State of the Art for the Surgical Management of empyema thoracis. K. Robert Shen, M.D.
 Accepted Manuscript Current State of the Art for the Surgical Management of empyema thoracis K. Robert Shen, M.D. PII: S0022-5223(18)32919-2 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.006 Reference:
Accepted Manuscript Current State of the Art for the Surgical Management of empyema thoracis K. Robert Shen, M.D. PII: S0022-5223(18)32919-2 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.006 Reference:
Treatment of Loculated Pleural Effusions with Transcatheter Intracavitary Urokinase
 941 Treatment of Loculated Pleural Effusions with Transcatheter Intracavitary Urokinase Jeffrey S. Moulton1 Surgical thoracostomy tube placement and radiologically guided catheter drainage Patrick Timothy
941 Treatment of Loculated Pleural Effusions with Transcatheter Intracavitary Urokinase Jeffrey S. Moulton1 Surgical thoracostomy tube placement and radiologically guided catheter drainage Patrick Timothy
Immediate Drainage Is Not Required for All Patients with Complicated Parapneumonic Effusions*
 Immediate Drainage Is Not Required for All Patients with Complicated Parapneumonic Effusions* Herbert A. Berger; M.D.;t and Melvin L. Morganroth, M.D., F.C.C.P.t We retrospectively investigated if the
Immediate Drainage Is Not Required for All Patients with Complicated Parapneumonic Effusions* Herbert A. Berger; M.D.;t and Melvin L. Morganroth, M.D., F.C.C.P.t We retrospectively investigated if the
Pleural fluid analysis
 Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Intrapleural catheter drainage followed by pleurodesis is the
 ORIGINAL ARTICLE Intrapleural Urokinase for the Treatment of Loculated Malignant Pleural Effusions and Trapped Lungs in Medically Inoperable Cancer Patients Li-Han Hsu, MD,* Thomas C. Soong, MD, An-Chen
ORIGINAL ARTICLE Intrapleural Urokinase for the Treatment of Loculated Malignant Pleural Effusions and Trapped Lungs in Medically Inoperable Cancer Patients Li-Han Hsu, MD,* Thomas C. Soong, MD, An-Chen
Role of routine computed tomography in paediatric pleural empyema
 c Additional Methods data are published online only at http:// thorax.bmj.com/content/vol63/ issue10 1 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London, UK;
c Additional Methods data are published online only at http:// thorax.bmj.com/content/vol63/ issue10 1 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London, UK;
Interventional radiology treatment of empyema and lung abscesses
 PAEDIATRIC RESPIRATORY REVIEWS (2008) 9, 77 84 CME ARTICLE Interventional radiology treatment of empyema and lung abscesses Mark J. Hogan* and Brian D. Coley Nationwide Children s Hospital and The Ohio
PAEDIATRIC RESPIRATORY REVIEWS (2008) 9, 77 84 CME ARTICLE Interventional radiology treatment of empyema and lung abscesses Mark J. Hogan* and Brian D. Coley Nationwide Children s Hospital and The Ohio
Empyema in Australia (and related Soapbox topics)
 Empyema in Australia (and related Soapbox topics) Adam Jaffe School of Women s and Children s Health, Sydney Children s Hospital Introduction Relatively rare < 1% pneumonias empyema Strachan R, Jaffé A.
Empyema in Australia (and related Soapbox topics) Adam Jaffe School of Women s and Children s Health, Sydney Children s Hospital Introduction Relatively rare < 1% pneumonias empyema Strachan R, Jaffé A.
Pleural Effusion. Exudative pleural effusion - Involve an increase in capillary permeability and impaired pleural fluid resorption
 Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Paediatric Empyema: A Case Report and Literature Review
 Case reports Paediatric Empyema: A Case Report and Literature Review S. J. PARSONS, E. FENTON, M. WILLIAMS Department of Paediatrics, Royal Hobart Hospital, Hobart, TASMANIA ABSTRACT Objective: To present
Case reports Paediatric Empyema: A Case Report and Literature Review S. J. PARSONS, E. FENTON, M. WILLIAMS Department of Paediatrics, Royal Hobart Hospital, Hobart, TASMANIA ABSTRACT Objective: To present
Current medical management of pleural infection
 REVIEW Current medical management of pleural infection Demosthenes Bouros, Argyris Tzouvelekis & Katerina M Antoniou Author for correspondence Democritus University of Thrace, Department of Pneumonology
REVIEW Current medical management of pleural infection Demosthenes Bouros, Argyris Tzouvelekis & Katerina M Antoniou Author for correspondence Democritus University of Thrace, Department of Pneumonology
Infection of the pleural space with the formation of. Effects of Streptokinase and Deoxyribonuclease on Viscosity of Human Surgical and Empyema Pus*
 Effects of Streptokinase and Deoxyribonuclease on Viscosity of Human Surgical and Empyema Pus* Graham Simpson, MD; David Roomes, MB, ChB; and Mal Heron, PhD Study objective: To investigate the effects
Effects of Streptokinase and Deoxyribonuclease on Viscosity of Human Surgical and Empyema Pus* Graham Simpson, MD; David Roomes, MB, ChB; and Mal Heron, PhD Study objective: To investigate the effects
Management of pleural infection in adults: British Thoracic Society pleural disease guideline 2010
 1 Oxford Centre for Respiratory Medicine, Churchill Hospital Site, Oxford Radcliffe Hospital, Oxford, UK 2 Department of Respiratory Medicine, Royal Berkshire Hospital, Reading, UK Correspondence to Dr
1 Oxford Centre for Respiratory Medicine, Churchill Hospital Site, Oxford Radcliffe Hospital, Oxford, UK 2 Department of Respiratory Medicine, Royal Berkshire Hospital, Reading, UK Correspondence to Dr
Use of Fibrinolytics in Abdominal and Pleural Collections
 264 Use of Fibrinolytics in Abdominal and Pleural Collections Anuradha S. Shenoy-Bhangle, MD 1 DebraA.Gervais,MD 1,2 1 Abdominal Imaging and Intervention, Department of Radiology, Massachusetts General
264 Use of Fibrinolytics in Abdominal and Pleural Collections Anuradha S. Shenoy-Bhangle, MD 1 DebraA.Gervais,MD 1,2 1 Abdominal Imaging and Intervention, Department of Radiology, Massachusetts General
Use of fibrinolytic agents in the management of complicated parapneumonic effusions and empyemas
 Thorax 1998;53(Suppl 2):S65 S72 Use of fibrinolytic agents in the management of complicated parapneumonic effusions and empyemas Steven A Sahn Division of Pulmonary and Critical Care Medicine, Allergy
Thorax 1998;53(Suppl 2):S65 S72 Use of fibrinolytic agents in the management of complicated parapneumonic effusions and empyemas Steven A Sahn Division of Pulmonary and Critical Care Medicine, Allergy
Surgical versus non-surgical management for pleural empyema(protocol)
 Cochrane Database of Systematic Reviews Surgical versus non-surgical management for pleural empyema(protocol) ChinTY,ReddenMD,HsuCCT,vanDrielML ChinTY,ReddenMD,HsuCCT,vanDrielML. Surgical versus non-surgical
Cochrane Database of Systematic Reviews Surgical versus non-surgical management for pleural empyema(protocol) ChinTY,ReddenMD,HsuCCT,vanDrielML ChinTY,ReddenMD,HsuCCT,vanDrielML. Surgical versus non-surgical
REVIEW ARTICLE. Pleural infection-current diagnosis and management
 REVIEW ARTICLE Pleural infection-current diagnosis and management Andrew Rosenstengel, YC Gary Lee Clinical Pleural Fellow, Respiratory Dept, Sir Charles Gairdner Hospital, Perth WA 6009, Australia ABSTRACT
REVIEW ARTICLE Pleural infection-current diagnosis and management Andrew Rosenstengel, YC Gary Lee Clinical Pleural Fellow, Respiratory Dept, Sir Charles Gairdner Hospital, Perth WA 6009, Australia ABSTRACT
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY
 V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Pleural empyema Abduyeva F.M., MD, PhD
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Pleural empyema Abduyeva F.M., MD, PhD
Atypical Pleural Fluid Profiles in Tuberculous Pleural Effusion: Sequential Changes Compared with Parapneumonic and Malignant Pleural Effusions
 ORIGINAL ARTICLE Atypical Pleural Fluid Profiles in Tuberculous Pleural Effusion: Sequential Changes Compared with Parapneumonic and Malignant Pleural Effusions Chang Ho Kim, So Yeon Lee, Yong Dae Lee,
ORIGINAL ARTICLE Atypical Pleural Fluid Profiles in Tuberculous Pleural Effusion: Sequential Changes Compared with Parapneumonic and Malignant Pleural Effusions Chang Ho Kim, So Yeon Lee, Yong Dae Lee,
Serous fluids. Dr. Mohamed Saad Daoud
 Serous fluids 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition 2 The closed cavities of the body namely, the pleural, pericardial, and peritoneal
Serous fluids 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition 2 The closed cavities of the body namely, the pleural, pericardial, and peritoneal
BGS Autumn The wet lung - Pleural effusions. Nick Maskell. BGS Autumn Meeting November 2017
 The wet lung - Pleural effusions BGS Autumn Meeting November 2017 Nick Maskell Professor of Respiratory Medicine Bristol University, Bristol Conflicts of interest Prof Maskell has sat on advisory boards
The wet lung - Pleural effusions BGS Autumn Meeting November 2017 Nick Maskell Professor of Respiratory Medicine Bristol University, Bristol Conflicts of interest Prof Maskell has sat on advisory boards
Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients. J Porcel, P Vázquez, M Vives, A Nogués, M Falguera, A Manonelles
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 3 Number 1 Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients J Porcel, P Vázquez, M Vives, A Nogués, M Falguera,
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 3 Number 1 Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients J Porcel, P Vázquez, M Vives, A Nogués, M Falguera,
Causes of pleural effusion and its imaging approach in pediatrics. M. Mearadji International Foundation for Pediatric Imaging Aid
 Causes of pleural effusion and its imaging approach in pediatrics M. Mearadji International Foundation for Pediatric Imaging Aid Pleural fluid A tiny amount of fluid in the pleural cavity is physiological.
Causes of pleural effusion and its imaging approach in pediatrics M. Mearadji International Foundation for Pediatric Imaging Aid Pleural fluid A tiny amount of fluid in the pleural cavity is physiological.
Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA) Lung Infection
 Short Communication TheScientificWorldJOURNAL (2009) 9, 723 728 ISSN 1537-744X; DOI 10.1100/tsw.2009.91 Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA)
Short Communication TheScientificWorldJOURNAL (2009) 9, 723 728 ISSN 1537-744X; DOI 10.1100/tsw.2009.91 Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA)
Outcome and mortality analysis in complicated parapneumonic effusion and empyema
 International Journal of Clinical Trials Arivudainambi VP. Int J Clin Trials. 2017 Nov;4(4):176-183 http://www.ijclinicaltrials.com pissn 2349-3240 eissn 2349-3259 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3259.ijct20174208
International Journal of Clinical Trials Arivudainambi VP. Int J Clin Trials. 2017 Nov;4(4):176-183 http://www.ijclinicaltrials.com pissn 2349-3240 eissn 2349-3259 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3259.ijct20174208
New trends in the diagnosis and treatment in parapneumonic effusion and empyema
 New trends in the diagnosis and treatment in parapneumonic effusion and empyema Moon Jun NA 1,2, Öner DİKENSOY 3, Richard W. LIGHT 1 1 Division of Allergy, Pulmonary, and Critical Care Medicine of Vanderbilt
New trends in the diagnosis and treatment in parapneumonic effusion and empyema Moon Jun NA 1,2, Öner DİKENSOY 3, Richard W. LIGHT 1 1 Division of Allergy, Pulmonary, and Critical Care Medicine of Vanderbilt
Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS AND FACTORS ASSOCIATED WITH ITS OCCURRENCE
 Original Articles Incidence of Pneumothorax After Thoracentesis and Factors Associated with Its Occurrence 77 Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS
Original Articles Incidence of Pneumothorax After Thoracentesis and Factors Associated with Its Occurrence 77 Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS
Indwelling Pleural Catheters in Malignant and Non-Malignant Disease
 Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings
 Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Clinical Importance of Angiogenic Cytokines, Fibrinolytic Activity and Effusion Size in Parapneumonic Effusions
 Clinical Importance of Angiogenic Cytokines, Fibrinolytic Activity and Effusion Size in Parapneumonic Effusions Chi-Li Chung 1,2, Shih-Hsin Hsiao 1, George Hsiao 3, Joen-Rong Sheu 3, Wei-Lin Chen 3, Shi-Chuan
Clinical Importance of Angiogenic Cytokines, Fibrinolytic Activity and Effusion Size in Parapneumonic Effusions Chi-Li Chung 1,2, Shih-Hsin Hsiao 1, George Hsiao 3, Joen-Rong Sheu 3, Wei-Lin Chen 3, Shi-Chuan
Treatment of Complicated Pleural Effusions in 2013
 Treatment of Complicated Pleural Effusions in 2013 Rahul Bhatnagar, MB ChB, MRCP a,b, Nick A. Maskell, DM, FRCP b,c, * KEYWORDS Complicated pleural effusions Pleural effusions Pleural infections Lung infections
Treatment of Complicated Pleural Effusions in 2013 Rahul Bhatnagar, MB ChB, MRCP a,b, Nick A. Maskell, DM, FRCP b,c, * KEYWORDS Complicated pleural effusions Pleural effusions Pleural infections Lung infections
THE USE OF PLEURAL FLUID CHOLESTEROL IN IDENTIFYING THE TYPE OF PLEURAL EFFUSION
 THE USE OF PLEURAL FLUID CHOLESTEROL IN IDENTIFYING THE TYPE OF PLEURAL EFFUSION Hyacinth D. Jumalon, MD, DPCP West Visayas State University Medical Center Iloilo City Region VI introduction - The first
THE USE OF PLEURAL FLUID CHOLESTEROL IN IDENTIFYING THE TYPE OF PLEURAL EFFUSION Hyacinth D. Jumalon, MD, DPCP West Visayas State University Medical Center Iloilo City Region VI introduction - The first
PLEURAL DISEASES. (Pleural effusion & empyema) Menaldi Rasmin
 PLEURAL DISEASES (Pleural effusion & empyema) Menaldi Rasmin Department of Pulmonology & Respiratory Medicine Faculty of Medicine, University of Indonesia Introduction Pleural effusion is the most common
PLEURAL DISEASES (Pleural effusion & empyema) Menaldi Rasmin Department of Pulmonology & Respiratory Medicine Faculty of Medicine, University of Indonesia Introduction Pleural effusion is the most common
Treatment approaches for empyema in children
 PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 164 170 CME REVIEW Treatment approaches for empyema in children Samatha Sonnappa 1, * and Adam Jaffe 2 1 Portex Respiratory Unit, Great Ormond Street Hospital and
PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 164 170 CME REVIEW Treatment approaches for empyema in children Samatha Sonnappa 1, * and Adam Jaffe 2 1 Portex Respiratory Unit, Great Ormond Street Hospital and
Alfonso Fiorelli 1, Francesco Caronia 2, Aldo Prencipe 3, Mario Santini 1, Brendon Stiles 4. Evidenced-Based Clinical Problem Solving Article
 Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions
 ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions
 Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Review of video-assisted thoracoscopy in children
 Review Article Review of video-assisted thoracoscopy in children S N Oak, S V Parelkar, K V SatishKumar, R Pathak, B H Ramesh, S Sudhir, M Keshav Department of Pediatric Surgery, TNMC and BYL Nair Hospital,
Review Article Review of video-assisted thoracoscopy in children S N Oak, S V Parelkar, K V SatishKumar, R Pathak, B H Ramesh, S Sudhir, M Keshav Department of Pediatric Surgery, TNMC and BYL Nair Hospital,
Pleural Diseases. Dr Matthew J Knight Consultant Respiratory Physician
 Pleural Diseases Dr Matthew J Knight Consultant Respiratory Physician What do you need to know? What do you need to know? Pleura- normal anatomy and physiology Pleural effusions Causes and investigations
Pleural Diseases Dr Matthew J Knight Consultant Respiratory Physician What do you need to know? What do you need to know? Pleura- normal anatomy and physiology Pleural effusions Causes and investigations
Pleural fluid. creatinine - urinothorax haematocrit -haemothorax bilirubin gut perforation. Fluid samples 1st Plain Universal ( cell count)
 Examination Purpose of test Sample 17725 Fluid Profile (appearance, culture, WBC differential, ph, total protein, glucose, amylase, triglyceride, albumin, HDL) Peritoneal/ascitic and pleural fluid are
Examination Purpose of test Sample 17725 Fluid Profile (appearance, culture, WBC differential, ph, total protein, glucose, amylase, triglyceride, albumin, HDL) Peritoneal/ascitic and pleural fluid are
Risk factors for complicated parapneumonic effusion and empyema on presentation to hospital with community-acquired pneumonia
 See Editorial, p 556Royal Infirmary of Edinburgh, Edinburgh, Scotland, UK Correspondence to: Dr J D Chalmers, Department of Respiratory Medicine, Royal Infirmary of Edinburgh, 51 Little France Crescent,
See Editorial, p 556Royal Infirmary of Edinburgh, Edinburgh, Scotland, UK Correspondence to: Dr J D Chalmers, Department of Respiratory Medicine, Royal Infirmary of Edinburgh, 51 Little France Crescent,
Pleural Disease. Disclosure. Normal Pleural Anatomy. Outline. Pleural Fluid Origins: Transudates. Pleural Fluid Origins: Exudates
 Disclosure Pleural Disease Anne L Fuhlbrigge MD MS Clinical Director Division of Pulmonary and Critical Care Medicine Brigham and Women s Hospital Channing Laboratory Harvard Medical School Boston, MA
Disclosure Pleural Disease Anne L Fuhlbrigge MD MS Clinical Director Division of Pulmonary and Critical Care Medicine Brigham and Women s Hospital Channing Laboratory Harvard Medical School Boston, MA
TOTAL CHOLESTEROL ANALYSIS FOR DIFFERENTIATING EXUDATES AND TRANSUDATES IN PLEURAL FLUIDS
 INDONESIAN JOURNAL OF CLINICAL PATHOLOGY AND MEDICAL LABORATORY Majalah Patologi Klinik Indonesia dan Laboratorium Medik Page 136 2018 March; 24(2): 136-140 p-issn 0854-4263 e-issn 2477-4685 Available
INDONESIAN JOURNAL OF CLINICAL PATHOLOGY AND MEDICAL LABORATORY Majalah Patologi Klinik Indonesia dan Laboratorium Medik Page 136 2018 March; 24(2): 136-140 p-issn 0854-4263 e-issn 2477-4685 Available
Pleural Empyema Joseph Junewick, MD FACR
 Pleural Empyema Joseph Junewick, MD FACR 03/19/2010 History Teenager with persistent fever and cough. Pneumonia diagnosed 1 week ago. Diagnosis Pleural Empyema Additional Clinical Surgery-Clear fluid with
Pleural Empyema Joseph Junewick, MD FACR 03/19/2010 History Teenager with persistent fever and cough. Pneumonia diagnosed 1 week ago. Diagnosis Pleural Empyema Additional Clinical Surgery-Clear fluid with
