Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction
|
|
|
- Jason O’Neal’
- 6 years ago
- Views:
Transcription
1 Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction David A. Low 1,2,3*, Ekawat Vichayanrat 2,3, Valeria Iodice 2,3 and Christopher J. Mathias 2,3 1 Research Institute of Sport and Exercise Sciences, Faculty of Science, Liverpool John Moores University, UK 2 Autonomic and Neurovascular Medicine Unit, Faculty of Medicine, Imperial College London at St Mary s Hospital, London, UK 3 Autonomic Unit, National Hospital for Neurology and Neurosurgery, Queen Square/Division of Clinical Neurology, Institute of Neurology, University College London, UK *Corresponding author: Dr David Low Sport and Exercise Sciences Tom Reilly Building Byrom Street Liverpool L3 3AF tel: D.A.Low@ljmu.ac.uk Keywords: Blood pressure, exercise, pressor, Parkinson s disease, hypotension Short Title: Blood pressure during exercise in Parkinson s disease
2 Abstract Aim To clarify the characteristics of hemodynamic responses to exercise and orthostasis in Parkinson's disease patients, especially those with autonomic failure. Methods Clinical audit of supine cycling exercise test data (with active standing tests pre- and postexercise) of Parkinson's patients with autonomic dysfunction. 23 patients (71±7 yr, 7 females) with a confirmed diagnosis of Parkinson's were identified. Results Group mean systolic blood pressure (SBP) fell during pre-exercise standing (-39±29 mmhg, P<0.001, 17 patients had orthostatic hypotension (OH)), while heart rate (HR) increased (+13±7 beats.min-1, P<0.001). SBP (P<0.001) increased during exercise with a wide variation in responses. SBP increased in 13 patients (INC; +30±14 mmhg) and either did not change or decreased in 10 patients (DEC -12±11 mmhg, P<0.001 vs INC). The increase in HR was not different between sub-groups (30±12 vs 25±10 beats.min-1, INC vs. DEC, P=0.29). The size of the pre-exercise stand SBP reduction was greater in DEC vs INC (-64±23 (10 out of 10 had OH) vs -19±16 mmhg (7 out of 13 had OH), respectively, P<0.001). The HR elevation was not different between sub-groups (13±8 vs 13±4 beats.min-1, DEC vs INC, P=0.94). Post-exercise SBP/DBP were lower for both sub-groups compared to pre-exercise and the standing SBP reduction post-exercise was not greater relative to pre-exercise in either sub-group. Conclusion Exercise-induced hypotension can occur in Parkinson's disease patients with autonomic failure with the magnitude of the exercise response being related to the severity of autonomic dysfunction. Exercise does not appear to worsen OH in this sample of Parkinson's patients.
3 Introduction Non-motor features are increasingly recognised in Parkinson s disease, including dysfunction of the autonomic nervous system, which can have a significant impact on quality of life [1]. Cardiovascular autonomic dysfunction can result in precipitous reductions in blood pressure, particularly during various daily activities, such as the upright posture (e.g., orthostatic hypotension), and various symptoms, e.g., cognitive impairment, fatigue and fainting [2]. Cardiovascular autonomic dysfunction (defined as orthostatic hypotension and often referred to as autonomic failure) occurs in ~40% of Parkinson s patients [3], generally in the latter stages of the disease, but it can present in the earlier stages of the disorder in some patients. Exercise is often used as an adjunct therapy in Parkinson s disease. Physical activity/exercise is also a potent stimulus of the autonomic nervous system and can threaten the appropriate maintenance of blood pressure during and/or after exercise however in individuals with compromised autonomic function, e.g., autonomic failure. In contrast to an appropriate pressor response during exercise in healthy individuals, increases in blood pressure can be blunted and/or reductions may even occur (referred to as exercise-induced hypotension) in other neurological disorders, such as Multiple System Atrophy and Pure Autonomic Failure, where autonomic failure is a key diagnostic criteria and clinical features often overlap with Parkinson s disease [4]. Furthermore, exercise can accentuate post-exercise orthostatic hypotension [5]. Analogous to the symptoms that occur during orthostatic hypotension, limited elevations and/or reductions in blood pressure during exercise can cause similar symptoms, such as dizziness, weakness and fatigue. The blood pressure responses to exercise in Parkinson s disease have been scarcely investigated however. The few previous studies that have been conducted have shown that the pressor response to maximal
4 exercise is blunted and that aerobic capacity is reduced in Parkinson s patients [6,7,8]. The integrity of the autonomic nervous system in those studies was not reported however, thus it was unclear if the reduced pressor response in those patients was due to autonomic dysfunction and/or another mechanism(s). In one of our previous studies, relative to aged matched healthy controls, we showed preserved exercise pressor responses in untreated idiopathic Parkinson s patients with intact cardiovascular autonomic function [9]. It is unclear, however, if blood pressure increases appropriately during exercise or if exercise accentuates orthostatic hypotension in Parkinson s disease patients with autonomic dysfunction. The aim of this study was to clarify the characteristics of hemodynamic responses to exercise and orthostasis in Parkinson's disease patients, especially those with autonomic failure.
5 Subjects and Methods We conducted a clinical audit of data from autonomic function exercise tests that are routinely performed in our Units on patients with suspected autonomic dysfunction. Suspected was characterised by the referring clinician and/or the Autonomic Unit consultants surmising that the patient had probable cardiovascular autonomic dysfunction based on the symptoms that they reported, for example, dizziness or visual disturbances and/or paracervical and suboccipital ( coat hanger ) ache while upright, fainting or near fainting episodes, and/or weakness, lethargy or fatigue. We identified records of 23 patients (71 ±7 yr, 7 females) that had a confirmed diagnosis of Parkinson s disease (4.4 ± 3.7 yr) and had completed the exercise test protocol [10]. Patients were on the following medications; dopamine agonists (78%), dopaminergic adjunct therapy (61%, e.g., catechol-o-methyl transferase inhibitors, DOPA decarboxylase inhibitors, monoamine oxidase inhibitors), statins (35%), volume expanders/adrenergic agonists for orthostatic intolerance (30%), proton pump inhibitors for gastrointestinal dysfunction (22%), selective serotonin reuptake inhibitors (26%) and anti-hypertensives (13%). The exercise test protocol involves supine cycling (Lode Angio, Lode B.V., Groningen, Netherlands), e.g., no gravity and orthostatic stress, at 3 incremental stages (25, 50 and 75 watts) for 3 min each [9]. A 5 min active stand test was conducted before and after the exercise protocol to assess orthostatic hypotension and symptoms pre- and post-exercise. Blood pressure and heart rate were intermittently recorded throughout the protocol using upper arm sphgymomanometry (Dinamap Pro 400, GE Healthcare, Chalfont St Giles, UK). ANOVA or paired t tests were performed for comparisons over time within the exercise test and within or between the pre- and post-exercise stand tests. When the ANOVA revealed a
6 significant difference, Tukey's post-hoc testing was performed to determine the location of the specific differences. For any sub-group analyses performed, differences between subgroups were assessed with student's t test or Chi-square where appropriate. Pearson s product correlation was used for studying relationships between variables. Values are presented as means ± SD. Statistical significance was set at a p value of <0.05. Ethical approval was waived as the study did not require ethical approval because it was a retrospective chart review of routine clinical tests.
7 Results Both systolic (142±18 vs 104±30 mm Hg, P <0.05) and diastolic (78±9 vs 65±14 mm Hg, P <0.05) blood pressure decreased on standing and heart rate increased (65±10 vs 78±10 beats.min -1, P <0.05) in the whole group. 17 of the 23 patients fulfilled the criteria for orthostatic hypotension indicating autonomic failure. 4 out of the other 6 patients (-5±11 mm Hg) displayed reductions in blood pressure during orthostasis. Not all patients (9 out of 23) were able to complete all 3 stages of the exercise protocol due to fatigue or motor dysfunction. There were no differences between those that did and didn t complete the exercise test with regards to pre-exercise supine and head-up tilt blood pressure (both P >0.05) or the peak exercise blood pressure response (P >0.05) or with regards to age or disease duration (both P >0.05). The group mean systolic blood pressure increased during exercise (P <0.05) but there was a wide variation in the responses however (see Figure 1A). A similar trend was evident for diastolic blood pressure (P <0.05). Heart rate increased during exercise (P <0.05, see Figure 1B). Resting supine blood pressure was lower (systolic 134±15 and diastolic 75±11 mm Hg, both P <0.05 vs. pre-exercise supine) and heart rate was higher (69±11 beats.min -1 vs. pre-exercise supine, P <0.05) post-exercise. During postexercise standing, both systolic and diastolic blood pressure decreased and heart rate increased in the whole group (all P <0.05). The same 17 patients that fulfilled the criteria for orthostatic hypotension on pre-exercise standing also met the criteria on post-exercise standing. On further inspection of the blood pressure responses to exercise, systolic blood pressure increased in 13 patients and either did not change or decreased in 10 patients. We therefore further examined these 2 sub-groups that did increase (INC) and those that did
8 not increase or in fact decreased (DEC) systolic blood pressure during exercise. Resting blood pressure was higher in DEC (P <0.05, see Figure 1C). By definition, blood pressure (systolic and diastolic) in the INC group increased during exercise whereas in the DEC group blood pressure was either maintained or reduced (P <0.05 vs INC, see Figure 1C). There were no differences between sub-groups in the elevation in heart rate during exercise (P >0.05, see Figure 1D). The pre- and post-exercise stand data were also re-analysed (see Figure 2). Supine blood pressure was higher in the DEC group (P <0.05 vs INC). There was no difference in supine heart rate between the sub-groups (65±12 vs 65±8 beats.min -1 for INC and DEC, respectively, P >0.05). The size of the pre-exercise stand systolic and diastolic blood pressure reductions were greater in DEC vs INC however (both P <0.05 vs INC, see Figure 2A). The entire DEC group had orthostatic hypotension and 7 of the 13 INC group had orthostatic hypotension (100 vs 54%, respectively, P<0.05). The increase in heart rate during standing was not different between the sub-groups (13±8 vs 13±4 beats.min -1, P >0.05). The magnitude of the change in blood pressure during exercise was also significantly correlated with the magnitude of orthostatic hypotension (R 2 = 0.53, P<0.001). During post-exercise standing blood pressure decreased and the size of the systolic and diastolic blood pressure reductions were greater in DEC vs INC (both P <0.05 vs INC, see Figure 2B). Similar, to pre-exercise, the entire DEC group had orthostatic hypotension and 7 of the 13 INC group had orthostatic hypotension. The increase in heart rate during standing was not different between the sub-groups (12±9 vs 13±7 beats.min -1, P >0.05). The size of the changes in blood pressure were not greater relative to pre-exercise for both sub-groups
9 (all P >0.05). Symptoms were generally more prevalent on post-exercise standing despite smaller reductions in blood pressure however. There was no difference in age (70 ± 7 vs 72 ± 6 yr for INC vs DEC, respectively, P=0.42) or disease duration (3.5 ± 2.7 vs 5.5 ± 4.6 yr for INC vs DEC, respectively, P=0.54) between the sub-groups. There were also no statistical differences in dopaminergic pharmacotherapy between the INC and DEC sub-groups (dopamine agonists; 69 vs 90%, respectively, P>0.05; dopaminergic adjunct therapy; 46 vs 80%, respectively, P>0.05). More patients in the DEC group were on medications for orthostatic intolerance however (8 vs 60%, P <0.05).
10 Discussion The aim of this study was to clarify the characteristics of hemodynamic responses to exercise and orthostasis in Parkinson's disease patients, especially those with autonomic failure. The main findings were that the exercise pressor response is blunted and blood pressure can even decrease during exercise in Parkinson's disease patients with autonomic dysfunction and the extent of the blunting/decrease in blood pressure during exercise is related to the severity of autonomic dysfunction. Furthermore, exercise did not exacerbate orthostatic hypotension in this group of patients. Finally, this is the first study to document reductions in blood pressure, e.g., exercise-induced hypotension, in Parkinson's disease patients with autonomic failure. Cardiovascular autonomic dysfunction is a key non-motor feature of Parkinson's disease. The integrity of cardiovascular autonomic function during exercise in Parkinson's disease has not been thoroughly investigated however. In the few previous studies that have examined the hemodynamic responses to exercise in Parkinson's, the blood pressure responses to maximal exercise were reduced [6,7,8] and the pressor responses to sub-maximal exercise were preserved in Parkinson's patients [9,11]. In the former studies the integrity of autonomic function of the patients was not reported and the reduced blood pressure response may have been a result of the lower aerobic capacity and peak power output achieved. In the latter studies, autonomic function, as assessed using a standard screening protocol or just a head-up tilt test, appeared normal. In the present study 17 of the 23 patients had orthostatic hypotension indicating autonomic failure. 10 of the 23 patients exhibited no change or a reduction in blood pressure during exercise (e.g., the DEC group). All patients in this sub-group displayed orthostatic hypotension and greater reductions in blood pressure on orthostasis relative to the remainder of the patients that exhibited an
11 increase in blood pressure during exercise (e.g., the INC group). OH was present in 7 of the 13 patients of the INC group, however, suggesting that this, e.g., autonomic failure, may not explain the differences in the exercise pressor response between the 2 groups. However, blunted exercise pressor responses were still evident in the INC group given that the definition of this group was simply an increase (of any magnitude) in SBP during exercise, thus, patients who exhibited mild to moderate elevations of blood pressure that are considered sub-normal were included. Furthermore, when examining the whole patient group, the magnitude of the systolic blood pressure change during exercise was also significantly correlated with the magnitude of orthostatic hypotension on pre-exercise standing. These findings strongly suggest that the exercise pressor response (or lack of) in Parkinson s disease patients with autonomic dysfunction is associated with the severity of their cardiovascular autonomic dysfunction, which is consistent with other autonomic failure disorders that display orthostatic and exercise-induced hypotension (e.g., Multiple System Atrophy, Pure Autonomic Failure and Spinal Cord Injury) [4]. Because our primary focus was the examination of the exercise cardiovascular responses in PD patients with suspected autonomic dysfunction we looked to assess those responses first and then further analyse those data (e.g., DEC vs INC) according to the level of autonomic dysfunction rather than start with a comparison of those with and without autonomic failure (e.g., OH). Regardless, if the data are analysed with this latter approach (e.g., those with OH vs. those without OH) then the findings are the same; the blunted/absent pressor responses to exercise are magnified and more prevalent in patients with autonomic failure and the extent of the blunted/absent pressor response is directly related to the severity of autonomic dysfunction/failure (e.g., OH).
12 Generally, autonomic dysfunction presents in the latter stages of Parkinson s disease [12] but it can occur early and even before the hallmark motor dysfunction presents [13]. The proposed mechanisms of cardiovascular autonomic dysfunction in Parkinson s disease generally involve lewy body accumulation and cell loss in various key areas of the autonomic nervous system, such as, autonomic regulatory areas including the hypothalamus, medulla, locus coeruleus and raphe, pre-ganglionic parasympathetic and sympathetic regions including the dorsal vagal motor nuclei of the glossopharyngeal and vagal nerves, autonomic and sympathetic ganglia, as well as post-ganglionic sympathetic denervation [1] that ultimately affect control of blood pressure through baroreflex impairment and loss of sympathetic innervation. The mechanisms for the blunted/absent exercise pressor responses, as well as the more severe cardiovascular autonomic dysfunction/failure, in the DEC group are likely related to impairments in the ability to control cardiac output and/or total peripheral resistance. The similar heart rate responses to orthostasis and exercise in the INC and DEC groups might suggest that the ability to increase/maintain cardiac output was not the likely mechanism contributing to the impaired blood pressure control in the DEC group, consistent with other autonomic failure disorders that display a preserved cardiac output, yet impaired blood pressure, response to exercise [14, 15]. That said, stroke volume (and cardiac output) was not assessed in the present study, cardiac sympathetic denervation is common in Parkinson s disease [1], and an impaired cardiac contractility during exercise has also been reported in PD patients with cardiac sympathetic denervation [11] suggesting that an impaired cardiac output response may have occurred in the DEC group. In contrast, it is possible that the control of total peripheral resistance is impaired in the DEC group.
13 Typically, total peripheral resistance is decreased during dynamic exercise due to the large vasodilation that occurs in the active musculature despite vasoconstriction in other nonactive vascular beds. It is therefore possible that an excessive muscle vasodilation and/or impaired elevations in vascular resistance in quiescent vascular beds (e.g., splanchnic circulation) causes an exacerbated decrease in total peripheral resistance and caused a reduced blood pressure during exercise in the DEC group. Although absolute DBP was not different between the INC and DEC groups during exercise, the change in DBP was significantly different in the DEC group (e.g., an increase in INC and no change in DEC). This hypothesis is consistent with other autonomic failure disorders that display blunted elevations in splanchnic vascular resistance and blood pressure during exercise [14, 15]. Alternatively, it might be a combination of an impaired cardiac output and a blunted total peripheral resistance response is responsible for the blunted exercise pressor response in DEC. A recent study has indicated that both impaired cardiac innervation and total peripheral resistance responses cause OH in PD [16]. Although it is not known whether these findings explain the blunted exercise pressor response in PD patients with autonomic dysfunction, the overlap between the cardiovascular control mechanisms during orthostasis and exercise suggest that this might be likely. Previous studies have shown that exercise exacerbates orthostatic hypotension in autonomic failure disorders [9]. In contrast in the present study, exercise did not accentuate the fall in blood pressure during orthostasis. The reasons for this are unclear but might be related to the lower supine blood pressure prior to standing, thus limiting the potential size of the reduction in blood pressure during orthostasis, the relatively high severity of
14 autonomic dysfunction/failure already evident in this group of patients and/or a specific mechanism related to Parkinsonism as opposed to the other autonomic failure disorders (e.g., Multiple System Atrophy, Pure Autonomic Failure) where exacerbated orthostatic hypotension has previously been documented [9]. Although exercise did not worsen orthostatic hypotension in this sample of Parkinson s patients, it did increase orthostatic symptoms (based on patient reporting; data not presented) which were likely due to the lower pre-standing blood pressure causing blood pressure to fall to symptomatic lower limits quicker and/or a greater peripheral displacement of blood due to the previous exercise bout. In conclusion, these data indicate that exercise-induced hypotension can occur in Parkinson s disease patients with autonomic failure, the magnitude of the exercise blood pressure response in Parkinson s disease patients with autonomic dysfunction is related to the severity of their cardiovascular autonomic dysfunction and exercise does not appear to worsen orthostatic hypotension in this sample of Parkinson s patients but lowers resting blood pressure. These findings have implications for clinicians and their management of Parkinson s patients.
15 References [1] Asahina M, Vichayanrat E, Low DA, Iodice V, Mathias CJ. Autonomic dysfunction in parkinsonian disorders: assessment and pathophysiology. J Neurol Neurosurg Psychiatry. 2013;84: [2] Freeman R, Wieling W, Axelrod FB, Benditt DG, Benarroch E, Biaggioni I, et al. Consensus statement on the definition of orthostatic hypotension, neurally mediated syncope and the postural tachycardia syndrome. Auton Neurosci. 2011;161:46-8. [3] Velseboer DC, de Haan RJ, Wieling W, Goldstein DS, de Bie RM. Prevalence of orthostatic hypotension in Parkinson's disease: A systematic review and meta-analysis. Parkinsonism Relat Disord [4] Low DA, da Nobrega AC, Mathias CJ. Exercise-induced hypotension in autonomic disorders. Auton Neurosci. 2012;171: [5] Smith GD, Mathias CJ. Postural hypotension enhanced by exercise in patients with chronic autonomic failure. Qjm. 1995;88: [6] Reuter I, Engelhardt M, Freiwaldt J, Baas, H. Exercise test in Parkinon s Disease. Clin Auton Res 1999;9: [7] Werner WG, DiFrancisco-Donoghue J, Lamberg EM. Cardiovascular response to treadmill testing in Parkinson disease. J Neurol Phys Ther. 2006;30: [8] DiFrancisco-Donoghue J, Elokda A, Lamberg EM, Bono N, Werner WG. Norepinephrine and cardiovascular responses to maximal exercise in Parkinson's disease on and off medication. Mov Disord. 2009;24: [9] Smith GD, Mathias CJ. Differences in cardiovascular responses to supine exercise and to standing after exercise in two clinical subgroups of Shy-Drager syndrome (multiple system atrophy). J Neurol Neurosurg Psychiatry. 1996;61: [10] Ward CD, Gibb WR. Research diagnostic criteria for Parkinson's disease. Adv Neurol. 1990;53: [11]Nakamura T, Hirayama M, Yamashita F, Uchida K, Hama T, Watanabe H, Sobue G. Lowered cardiac sympathetic nerve performance in response to exercise in Parkinson's disease. Mov Disord. 2010;25: [12] Martinez-Martin P, Schapira AH, Stocchi F, Sethi K, Odin P, MacPhee G, et al. Prevalence of nonmotor symptoms in Parkinson's disease in an international setting; study using nonmotor symptoms questionnaire in 545 patients. Mov Disord. 2007;22: [13] Goldstein DS, Sharabi Y, Karp BI, Bentho O, Saleem A, Pacak K, et al. Cardiac sympathetic denervation preceding motor signs in Parkinson disease. Cleve Clin J Med. 2009;76 Suppl 2:S [14] Smith GD, Watson LP, Pavitt DV, Mathias CJ. Abnormal cardiovascular and catecholamine responses to supine exercise in human subjects with sympathetic dysfunction. J Physiol. 1995;484 ( Pt 1): [15] Chaudhuri KR, Thomaides T, Mathias CJ. Abnormality of superior mesenteric artery blood flow responses in human sympathetic failure. J Physiol. 1992;457: [16] Sobue, G. Role of cardiac sympathetic nerves in preventing orthostatic hypotension in Parkinson's disease. Parkinsonism Relat Disord. 2014; in press.
16 Figure 1. Mean (± 1 SD) blood pressure (upper line systolic, lower line diastolic) and heart rate during exercise for the whole group (A and B, respectively) and for the sub-groups that did (INC) and didn t (DEC) display a pressor response to exercise (C and D). *P<0.05 vs 0 watts, #P<0.05 vs INC. Figure 2. Mean (± 1 SD) absolute systolic and diastolic blood pressure supine prior to 5 min active stand test (left side) and the changes in systolic and diastolic blood pressure during the 5 min active stand test (right side) pre- (upper panel A) and post-exercise (lower panel B) for the sub-groups that did (INC) and didn t (DEC) display a pressor response to exercise. #P<0.05 vs INC.
Exercise Training for PoTS and Syncope
 B 140 120 100 80 60 40 20 0 Blood Pressure (mm Hg) Blood Pressure Heart Rate 60 degree Head Up Tilt Time 140 120 100 80 60 40 20 0 Heart Rate (beats.min -1 ) Exercise Training for PoTS and Syncope C Blood
B 140 120 100 80 60 40 20 0 Blood Pressure (mm Hg) Blood Pressure Heart Rate 60 degree Head Up Tilt Time 140 120 100 80 60 40 20 0 Heart Rate (beats.min -1 ) Exercise Training for PoTS and Syncope C Blood
I ngestion of water increases seated blood pressure (BP) in
 1737 PAPER The effects of water ingestion on orthostatic hypotension in two groups of chronic autonomic failure: multiple system atrophy and pure autonomic failure T M Young, C J Mathias... See end of
1737 PAPER The effects of water ingestion on orthostatic hypotension in two groups of chronic autonomic failure: multiple system atrophy and pure autonomic failure T M Young, C J Mathias... See end of
droxidopa (Northera )
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
:{ic0fp'16. Geriatric Medicine: Blood Pressure Monitoring in the Elderly. Terrie Ginsberg, DO, FACOI
 :{ic0fp'16 ACOFP 53 rd Annual Convention & Scientific Seminars Geriatric Medicine: Blood Pressure Monitoring in the Elderly Terrie Ginsberg, DO, FACOI Blood Pressure Management in the Elderly Terrie B.
:{ic0fp'16 ACOFP 53 rd Annual Convention & Scientific Seminars Geriatric Medicine: Blood Pressure Monitoring in the Elderly Terrie Ginsberg, DO, FACOI Blood Pressure Management in the Elderly Terrie B.
Northera (droxidopa)
 Northera (droxidopa) Policy Number: 5.01.657 Last Review: 07/2018 Origination: 07/2018 Next Review: 07/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Northera
Northera (droxidopa) Policy Number: 5.01.657 Last Review: 07/2018 Origination: 07/2018 Next Review: 07/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Northera
Treatment of orthostatic hypotension in Multiple System Atrophy New Clinical Studies
 Treatment of orthostatic hypotension in Multiple System Atrophy New Clinical Studies Cyndya A. Shibao, M.D., F.A.H.A. Assistant Professor of Medicine Division of Clinical Pharmacology Disclosure Lundbeck
Treatment of orthostatic hypotension in Multiple System Atrophy New Clinical Studies Cyndya A. Shibao, M.D., F.A.H.A. Assistant Professor of Medicine Division of Clinical Pharmacology Disclosure Lundbeck
Contempo GIMSI Cosa cambia alla luce della letteratura in tema di terapia farmacologica
 Contempo GIMSI 2015-2017 Cosa cambia alla luce della letteratura in tema di terapia farmacologica Dott.ssa Diana Solari Centro Aritmologico e Sincope Unit, Lavagna www.gimsi.it POST 2 (Prevention of Syncope
Contempo GIMSI 2015-2017 Cosa cambia alla luce della letteratura in tema di terapia farmacologica Dott.ssa Diana Solari Centro Aritmologico e Sincope Unit, Lavagna www.gimsi.it POST 2 (Prevention of Syncope
POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE
 POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE POTS Irritable heart syndrome. Soldier s heart. Effort syndrome. Vasoregulatory asthenia. Neurocirculatory asthenia. Anxiety neurosis.
POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE POTS Irritable heart syndrome. Soldier s heart. Effort syndrome. Vasoregulatory asthenia. Neurocirculatory asthenia. Anxiety neurosis.
ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 1 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE Emilia-Lidia
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 1 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE Emilia-Lidia
L-dihydroxyphenylserine (Droxidopa) in the treatment of orthostatic hypotension
 Clin Auton Res (8) 8[Suppl ]:5 9 DOI.7/s86-7-5-z ARTICLE Christopher J. Mathias L-dihydroxyphenylserine (Droxidopa) in the treatment of orthostatic hypotension The European experience Received: 5 October
Clin Auton Res (8) 8[Suppl ]:5 9 DOI.7/s86-7-5-z ARTICLE Christopher J. Mathias L-dihydroxyphenylserine (Droxidopa) in the treatment of orthostatic hypotension The European experience Received: 5 October
HRV in Diabetes and Other Disorders
 HRV in Diabetes and Other Disorders Roy Freeman, MD Center for Autonomic and Peripheral Nerve Disorders Beth Israel Deaconess Medical Center Harvard Medical School Control Propranolol Atropine Wheeler
HRV in Diabetes and Other Disorders Roy Freeman, MD Center for Autonomic and Peripheral Nerve Disorders Beth Israel Deaconess Medical Center Harvard Medical School Control Propranolol Atropine Wheeler
6/13/2017 PROFESSOR CHRISTOPHER J MATHIAS. Non-motor features in PD AUTONOMIC NERVOUS SYSTEM. Motor. Non-Motor CLINICAL AUTONOMIC MANIFESTATIONS
 PRFESSR CRISTPER J MATIAS Autonomic & Neurovascular Medicine Centre and The Joint ypermobility Unit, ospital of St John & St Elizabeth, St Johns Wood, London Autonomic Dysfunction in Parkinsons Disease:
PRFESSR CRISTPER J MATIAS Autonomic & Neurovascular Medicine Centre and The Joint ypermobility Unit, ospital of St John & St Elizabeth, St Johns Wood, London Autonomic Dysfunction in Parkinsons Disease:
INTRODUCTION POTS is: Poorly understood Rarely considered SIGNIFICANT morbidity Appropriate initial diagnosis & care will expedite management of POTS
 Learning objectives At the end of this presentation the learner should: Define POTS & identify the various etiologies of POTS Be able to differentiate POTS from other causes of orthostatic intolerance
Learning objectives At the end of this presentation the learner should: Define POTS & identify the various etiologies of POTS Be able to differentiate POTS from other causes of orthostatic intolerance
Clinical Study Nondipping in Parkinson s Disease
 SAGE-Hindawi Access to Research Parkinson s Disease Volume 2011, Article ID 897586, 5 pages doi:10.4061/2011/897586 Clinical Study Nondipping in Parkinson s Disease Sita Sommer, 1 Billur Aral-Becher, 1
SAGE-Hindawi Access to Research Parkinson s Disease Volume 2011, Article ID 897586, 5 pages doi:10.4061/2011/897586 Clinical Study Nondipping in Parkinson s Disease Sita Sommer, 1 Billur Aral-Becher, 1
Multiple choice questions: ANSWERS
 Multiple choice questions: ANSWERS Chapter 1. Redefining Parkinson s disease 1. Common non-motor features that precede the motor findings in Parkinson s disease (PD) include all of the following except?
Multiple choice questions: ANSWERS Chapter 1. Redefining Parkinson s disease 1. Common non-motor features that precede the motor findings in Parkinson s disease (PD) include all of the following except?
CIC Edizioni Internazionali
 Comparison of active standing test, head-up tilt test and 24-h ambulatory heart rate and blood pressure monitoring in diagnosing postural tachycardia Mojca Kirbiš, MD a,b Anton Grad, MD, PhD c Bernard
Comparison of active standing test, head-up tilt test and 24-h ambulatory heart rate and blood pressure monitoring in diagnosing postural tachycardia Mojca Kirbiš, MD a,b Anton Grad, MD, PhD c Bernard
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Adamec I., Klepac N., Milivojević I., Radić B., Habek M. (2012) Sick sinus syndrome and orthostatic hypotension in Parkinson's disease. Acta Neurologica Belgica, 112 (3).
Središnja medicinska knjižnica Adamec I., Klepac N., Milivojević I., Radić B., Habek M. (2012) Sick sinus syndrome and orthostatic hypotension in Parkinson's disease. Acta Neurologica Belgica, 112 (3).
L-dihydroxyphenylserine (Droxidopa): a new therapy for neurogenic orthostatic hypotension
 Clin Auton Res (2008) 18[Suppl 1]:19 24 DOI 10.1007/s10286-007-1002-2 ARTICLE Horacio Kaufmann L-dihydroxyphenylserine (Droxidopa): a new therapy for neurogenic orthostatic hypotension The US experience
Clin Auton Res (2008) 18[Suppl 1]:19 24 DOI 10.1007/s10286-007-1002-2 ARTICLE Horacio Kaufmann L-dihydroxyphenylserine (Droxidopa): a new therapy for neurogenic orthostatic hypotension The US experience
Tilt Table Testing. Dr. Prateek Suri
 Tilt Table Testing Dr. Prateek Suri Background Syncope is very commonly seen in the population Among the various causes of syncope vasovagal syncope is the most common cause There is an absence of a gold
Tilt Table Testing Dr. Prateek Suri Background Syncope is very commonly seen in the population Among the various causes of syncope vasovagal syncope is the most common cause There is an absence of a gold
CARDIOVASCULAR DYSFUNCTION IN PARKINSONIAN DISORDERS
 CARDIOVASCULAR DYSFUNCTION IN PARKINSONIAN DISORDERS Christopher J. Mathias Neurovascular Medicine Unit, Division of Neuroscience & Psychological Medicine, Imperial College School of Medicine at St Mary
CARDIOVASCULAR DYSFUNCTION IN PARKINSONIAN DISORDERS Christopher J. Mathias Neurovascular Medicine Unit, Division of Neuroscience & Psychological Medicine, Imperial College School of Medicine at St Mary
Pyridostigmine in the Treatment of Postural Orthostatic Tachycardia: A Single-Center Experience
 Pyridostigmine in the Treatment of Postural Orthostatic Tachycardia: A Single-Center Experience KHALIL KANJWAL, M.D.,* BEVERLY KARABIN, PH.D.,* MUJEEB SHEIKH, M.D.,* LAWRENCE ELMER, M.D., PH.D., YOUSUF
Pyridostigmine in the Treatment of Postural Orthostatic Tachycardia: A Single-Center Experience KHALIL KANJWAL, M.D.,* BEVERLY KARABIN, PH.D.,* MUJEEB SHEIKH, M.D.,* LAWRENCE ELMER, M.D., PH.D., YOUSUF
Clinical Studies 129
 Clinical Studies 129 Syncope in migraine. The population-based CAMERA study Roland D. Thijs, 1* Mark C. Kruit, 2* Mark A. van Buchem, 2 Michel D. Ferrari, 1 Lenore J. Launer, 3,4 and J. Gert van Dijk
Clinical Studies 129 Syncope in migraine. The population-based CAMERA study Roland D. Thijs, 1* Mark C. Kruit, 2* Mark A. van Buchem, 2 Michel D. Ferrari, 1 Lenore J. Launer, 3,4 and J. Gert van Dijk
NORTHERA (droxidopa) oral capsule
 NORTHERA (droxidopa) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
NORTHERA (droxidopa) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
Premotor PD: autonomic failure
 Premotor PD: autonomic failure Division of Neurobiology Department of Neurology Medical University of Innsbruck Non-motor symptoms in PD Autonomic OH, constipation, impotence, urinary incontinence or retention,
Premotor PD: autonomic failure Division of Neurobiology Department of Neurology Medical University of Innsbruck Non-motor symptoms in PD Autonomic OH, constipation, impotence, urinary incontinence or retention,
Diagnosing and Treating Neurogenic Orthostatic Hypotension: A Case Study
 Diagnosing and Treating Neurogenic Orthostatic Hypotension: A Case Study Learning Objectives: Illustrate how to accurately diagnose noh Employ scales and questionnaires in combination with cardiovascular
Diagnosing and Treating Neurogenic Orthostatic Hypotension: A Case Study Learning Objectives: Illustrate how to accurately diagnose noh Employ scales and questionnaires in combination with cardiovascular
Indications and Uses of Testing. Laboratory Testing of Autonomic Function. Generalized Autonomic Failure. Benign Disorders 12/30/2012.
 Indications and Uses of Testing Laboratory Testing of Autonomic Function Conditions of generalized autonomic failure Help define the degree of autonomic dysfunction and distinguish more benign from life
Indications and Uses of Testing Laboratory Testing of Autonomic Function Conditions of generalized autonomic failure Help define the degree of autonomic dysfunction and distinguish more benign from life
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES
 SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
Neurogenic orthostatic hypotension (NOH) results from
 Norepinephrine Precursor Therapy in Neurogenic Orthostatic Hypotension Horacio Kaufmann, MD; Daniela Saadia, MD; Andrei Voustianiouk, PhD; David S. Goldstein, MD, PhD; Courtney Holmes, CMT; Melvin D. Yahr,
Norepinephrine Precursor Therapy in Neurogenic Orthostatic Hypotension Horacio Kaufmann, MD; Daniela Saadia, MD; Andrei Voustianiouk, PhD; David S. Goldstein, MD, PhD; Courtney Holmes, CMT; Melvin D. Yahr,
AUTONOMIC FUNCTION IS A HIGH PRIORITY
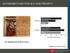 AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
Sistema Nervoso Vegetativo Vademecum per la diagnosi differenziale
 Sistema Nervoso Vegetativo Vademecum per la diagnosi differenziale Pietro Cortelli IRCCS Istituto delle Scienze Neurologiche di Bologna DIBINEM, Alma Mater Studiorum - Università di Bologna Anatomo-Functional
Sistema Nervoso Vegetativo Vademecum per la diagnosi differenziale Pietro Cortelli IRCCS Istituto delle Scienze Neurologiche di Bologna DIBINEM, Alma Mater Studiorum - Università di Bologna Anatomo-Functional
Findings from the 2015 HRS Expert Consensus Document on Postural Tachycardia Syndrome (POTS) and Inappropriate Sinus Tachycardia (IST)
 Findings from the 2015 HRS Expert Consensus Document on Postural Tachycardia Syndrome (POTS) and Inappropriate Sinus Tachycardia (IST) Ahmad Hersi, MBBS, MSc, FRCPC Professor of Cardiac Sciences Consultant
Findings from the 2015 HRS Expert Consensus Document on Postural Tachycardia Syndrome (POTS) and Inappropriate Sinus Tachycardia (IST) Ahmad Hersi, MBBS, MSc, FRCPC Professor of Cardiac Sciences Consultant
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
F indings or symptoms of autonomic dysfunction are
 1407 PAPER Age and duration related changes in muscle sympathetic nerve activity in Parkinson s disease K Shindo, H Watanabe, H Tanaka, K Ohashi, T Nagasaka, S Tsunoda, Z Shiozawa... See end of article
1407 PAPER Age and duration related changes in muscle sympathetic nerve activity in Parkinson s disease K Shindo, H Watanabe, H Tanaka, K Ohashi, T Nagasaka, S Tsunoda, Z Shiozawa... See end of article
Do Now pg What is the fight or flight response? 2. Give an example of when this response would kick in.
 Do Now pg 81 1. What is the fight or flight response? 2. Give an example of when this response would kick in. Autonomic Nervous System The portion of the PNS that functions independently (autonomously)
Do Now pg 81 1. What is the fight or flight response? 2. Give an example of when this response would kick in. Autonomic Nervous System The portion of the PNS that functions independently (autonomously)
Pheochromocytoma: Effects of Catecholamines
 36 PHYSIOLOGY CASES AND PROBLEMS Case 8 Pheochromocytoma: Effects of Catecholamines Helen Ames is a 51-year-old homemaker who experienced what she thought were severe menopausal symptoms. These awful "attacks"
36 PHYSIOLOGY CASES AND PROBLEMS Case 8 Pheochromocytoma: Effects of Catecholamines Helen Ames is a 51-year-old homemaker who experienced what she thought were severe menopausal symptoms. These awful "attacks"
T. Laitinen Departments of Physiology and Clinical Physiology, University of Kuopio and Kuopio University Hospital, Kuopio, Finland
 AUTONOMOUS NEURAL REGULATION T. Laitinen Departments of Physiology and Clinical Physiology, University of Kuopio and Kuopio University Hospital, Kuopio, Finland Keywords: Autonomic nervous system, sympathetic
AUTONOMOUS NEURAL REGULATION T. Laitinen Departments of Physiology and Clinical Physiology, University of Kuopio and Kuopio University Hospital, Kuopio, Finland Keywords: Autonomic nervous system, sympathetic
Neurocardiogenic syncope
 Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Integrated analysis of droxidopa trials for neurogenic orthostatic hypotension
 Biaggioni et al. BMC Neurology (2017) 17:90 DOI 10.1186/s12883-017-0867-5 RESEARCH ARTICLE Open Access Integrated analysis of droxidopa trials for neurogenic orthostatic hypotension Italo Biaggioni 1*,
Biaggioni et al. BMC Neurology (2017) 17:90 DOI 10.1186/s12883-017-0867-5 RESEARCH ARTICLE Open Access Integrated analysis of droxidopa trials for neurogenic orthostatic hypotension Italo Biaggioni 1*,
Note: At the end of the instructions, you will find a table which must be filled in to complete the exercise.
 Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
The Exercise Pressor Reflex
 The Exercise Pressor Reflex Dr. James P. Fisher School of Sport, Exercise & Rehabilitation Sciences College of Life & Environmental Sciences University of Birmingham, UK Copenhagen, 2018 Based on work
The Exercise Pressor Reflex Dr. James P. Fisher School of Sport, Exercise & Rehabilitation Sciences College of Life & Environmental Sciences University of Birmingham, UK Copenhagen, 2018 Based on work
LU:research Institutional Repository of Lund University
 LU:research Institutional Repository of Lund University This is an author produced version of a paper published in International journal of geriatric psychiatry. This paper has been peer-reviewed but does
LU:research Institutional Repository of Lund University This is an author produced version of a paper published in International journal of geriatric psychiatry. This paper has been peer-reviewed but does
III./3.1. Movement disorders with akinetic rigid symptoms
 III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
Introduction to Autonomic
 Part 2 Autonomic Pharmacology 3 Introduction to Autonomic Pharmacology FUNCTIONS OF THE AUTONOMIC NERVOUS SYSTEM The autonomic nervous system (Figure 3 1) is composed of the sympathetic and parasympathetic
Part 2 Autonomic Pharmacology 3 Introduction to Autonomic Pharmacology FUNCTIONS OF THE AUTONOMIC NERVOUS SYSTEM The autonomic nervous system (Figure 3 1) is composed of the sympathetic and parasympathetic
Desmopressin In The Treatment of Postural Orthostatic Tachycardia
 The Journal of Innovations in Cardiac Rhythm Management, 6 (2015), 2222 2226 DOI: 10.19102/icrm. 2015.061202 PHARMACOLOGICAL THERAPY RESEARCH ARTICLE Desmopressin In The Treatment of Postural Orthostatic
The Journal of Innovations in Cardiac Rhythm Management, 6 (2015), 2222 2226 DOI: 10.19102/icrm. 2015.061202 PHARMACOLOGICAL THERAPY RESEARCH ARTICLE Desmopressin In The Treatment of Postural Orthostatic
Cardiovagal Baroreflex Sensitivity in Parkinson s Disease and Multiple-System Atrophy
 JCN Open Access pissn 173-5 / eissn 5-513 / J Clin Neurol 1 ORIGINAL ARTICLE Cardiovagal Baroreflex Sensitivity in Parkinson s Disease and Multiple-System Atrophy Sankanika Roy a Ashok Kumar Jaryal a Achal
JCN Open Access pissn 173-5 / eissn 5-513 / J Clin Neurol 1 ORIGINAL ARTICLE Cardiovagal Baroreflex Sensitivity in Parkinson s Disease and Multiple-System Atrophy Sankanika Roy a Ashok Kumar Jaryal a Achal
Pharmacologic Treatment of Parkinson s Disease. Nicholas J. Silvestri, M.D. Assistant Professor of Neurology
 + Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Assistant Professor of Neurology + Overview n Brief review of Parkinson s disease (PD) n Clinical manifestations n Pathophysiology
+ Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Assistant Professor of Neurology + Overview n Brief review of Parkinson s disease (PD) n Clinical manifestations n Pathophysiology
Influence of Age, Hypertension or Myocardial Infarction on Cardiovascular Responses to Changes in Body Position
 Influence of Age, Hypertension or Myocardial Infarction on Cardiovascular Responses to Changes in Body Position A population-based study in 30-, 50- and 60-year-old men BY ANNA HOFSTEN UPPSALA UNIVERSITY
Influence of Age, Hypertension or Myocardial Infarction on Cardiovascular Responses to Changes in Body Position A population-based study in 30-, 50- and 60-year-old men BY ANNA HOFSTEN UPPSALA UNIVERSITY
Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study
 Original Article DOI: 10.17354/ijss/2016/16 Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study M Usharani 1, K Chandini 2 1 Professor and Head, Department of Physiology,
Original Article DOI: 10.17354/ijss/2016/16 Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study M Usharani 1, K Chandini 2 1 Professor and Head, Department of Physiology,
Pharmacologic Treatment of Parkinson s Disease. Nicholas J. Silvestri, M.D. Associate Professor of Neurology
 + Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Associate Professor of Neurology + Disclosures n NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT + Learning
+ Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Associate Professor of Neurology + Disclosures n NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT + Learning
Northera (droxidopa) Preliminary Findings From Study 301 in Symptomatic Neurogenic Orthostatic Hypotension. September 2010
 Northera (droxidopa) Preliminary Findings From Study 301 in Symptomatic Neurogenic Orthostatic Hypotension September 2010 1 2004-2010 Chelsea Therapeutics, Inc. This presentation is being provided for
Northera (droxidopa) Preliminary Findings From Study 301 in Symptomatic Neurogenic Orthostatic Hypotension September 2010 1 2004-2010 Chelsea Therapeutics, Inc. This presentation is being provided for
Integrated Cardiopulmonary Pharmacology Third Edition
 Integrated Cardiopulmonary Pharmacology Third Edition Chapter 3 Pharmacology of the Autonomic Nervous System Multimedia Directory Slide 19 Slide 37 Slide 38 Slide 39 Slide 40 Slide 41 Slide 42 Slide 43
Integrated Cardiopulmonary Pharmacology Third Edition Chapter 3 Pharmacology of the Autonomic Nervous System Multimedia Directory Slide 19 Slide 37 Slide 38 Slide 39 Slide 40 Slide 41 Slide 42 Slide 43
The magnitude and duration of ambulatory blood pressure reduction following acute exercise
 Journal of Human Hypertension (1999) 13, 361 366 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE The magnitude and duration of ambulatory
Journal of Human Hypertension (1999) 13, 361 366 1999 Stockton Press. All rights reserved 0950-9240/99 $12.00 http://www.stockton-press.co.uk/jhh ORIGINAL ARTICLE The magnitude and duration of ambulatory
Autonomic nervous system
 Autonomic nervous system Key notes Autonomic: an independent system that runs on its own The ANS is a visceral and involuntary sensory and motor system The visceral motor fibers in the autonomic nerves
Autonomic nervous system Key notes Autonomic: an independent system that runs on its own The ANS is a visceral and involuntary sensory and motor system The visceral motor fibers in the autonomic nerves
JMD. Cardiovascular Autonomic Dysfunction in Mild and Advanced Parkinson s Disease ORIGINAL ARTICLE
 http://dx.doi.org/10.14802/jmd.16001 / J Mov Disord 2016;9(2):97-103 pissn 2005-940X / eissn 2093-4939 ORIGINAL ARTICLE Cardiovascular Autonomic Dysfunction in Mild and Advanced Parkinson s Disease Joong-Seok
http://dx.doi.org/10.14802/jmd.16001 / J Mov Disord 2016;9(2):97-103 pissn 2005-940X / eissn 2093-4939 ORIGINAL ARTICLE Cardiovascular Autonomic Dysfunction in Mild and Advanced Parkinson s Disease Joong-Seok
Rehabilitation for Postural Tachycardia Syndrome (POTS)
 Rehabilitation for Postural Tachycardia Syndrome (POTS) Satish R Raj MD MSCI FACC FHRS FRCPC Associate Professor of Cardiac Sciences University of Calgary Adjunct Associate Professor of Medicine Autonomic
Rehabilitation for Postural Tachycardia Syndrome (POTS) Satish R Raj MD MSCI FACC FHRS FRCPC Associate Professor of Cardiac Sciences University of Calgary Adjunct Associate Professor of Medicine Autonomic
Ganglionic Blockers. Ganglion- blocking agents competitively block the action of
 Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Blood Pressure and its Regulation
 Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Exercise Associated collapse. ACSM Team Physician Course Part II 2/4/2017 Jerrad Zimmerman MD
 Exercise Associated collapse ACSM Team Physician Course Part II 2/4/2017 Jerrad Zimmerman MD Exercise Associated Collapse Characterized by collapse after completion of an intense exercise event in the
Exercise Associated collapse ACSM Team Physician Course Part II 2/4/2017 Jerrad Zimmerman MD Exercise Associated Collapse Characterized by collapse after completion of an intense exercise event in the
EHA Physiology: Challenges and Solutions Lab 1 Heart Rate Response to Baroreceptor Feedback
 Group No. Date: Computer 5 Names: EHA Physiology: Challenges and Solutions Lab 1 Heart Rate Response to Baroreceptor Feedback One of the homeostatic mechanisms of the human body serves to maintain a fairly
Group No. Date: Computer 5 Names: EHA Physiology: Challenges and Solutions Lab 1 Heart Rate Response to Baroreceptor Feedback One of the homeostatic mechanisms of the human body serves to maintain a fairly
SYNCOPE. Sanjay P. Singh, MD Chairman & Professor, Department of Neurology. Syncope
 SYNCOPE Sanjay P. Singh, MD Chairman & Professor, Department of Neurology. Syncope Syncope is a clinical syndrome characterized by transient loss of consciousness (TLOC) and postural tone that is most
SYNCOPE Sanjay P. Singh, MD Chairman & Professor, Department of Neurology. Syncope Syncope is a clinical syndrome characterized by transient loss of consciousness (TLOC) and postural tone that is most
P ure autonomic failure (PAF) is a sporadic idiopathic
 PAPER Progression and prognosis in pure autonomic failure (): comparison with multiple system atrophy N Mabuchi, M Hirayama, Y Koike, H Watanabe, H Ito, R Kobayashi, K Hamada, G Sobue... See end of article
PAPER Progression and prognosis in pure autonomic failure (): comparison with multiple system atrophy N Mabuchi, M Hirayama, Y Koike, H Watanabe, H Ito, R Kobayashi, K Hamada, G Sobue... See end of article
Pa t h w a y s. Pa r k i n s o n s. MacMahon D.G. Thomas S. Fletcher P. Lee M. 2006
 Pathways bolt 16/6/06 20:38 Page 1 Pa t h w a y s A PARADIGM FOR DISEASE MANAGEMENT IN Pa r k i n s o n s Disease MacMahon D.G. Thomas S. Fletcher P. Lee M. 2006 Clinical diagnosis Pa r k i n s o n s disease
Pathways bolt 16/6/06 20:38 Page 1 Pa t h w a y s A PARADIGM FOR DISEASE MANAGEMENT IN Pa r k i n s o n s Disease MacMahon D.G. Thomas S. Fletcher P. Lee M. 2006 Clinical diagnosis Pa r k i n s o n s disease
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
Orthostatic Hypotension (Postural Hypotension)
 Orthostatic Hypotension (Postural Hypotension) Authors: SCIRE Community Team Reviewed by: Darryl Caves, PT Last updated: April 9, 2018 Changes to blood pressure control after spinal cord injury (SCI) may
Orthostatic Hypotension (Postural Hypotension) Authors: SCIRE Community Team Reviewed by: Darryl Caves, PT Last updated: April 9, 2018 Changes to blood pressure control after spinal cord injury (SCI) may
Immediate Effect of Intermittent Cervical Traction in Supine versus Sitting Position on Heart Rate and Blood Pressure in Healthy Young Individuals
 www.jmscr.igmpublication.org Impact Factor-1.1147 ISSN (e)-2347-176x Immediate Effect of Intermittent Cervical Traction in Supine versus Sitting Position on Heart Rate and Blood Pressure in Healthy Young
www.jmscr.igmpublication.org Impact Factor-1.1147 ISSN (e)-2347-176x Immediate Effect of Intermittent Cervical Traction in Supine versus Sitting Position on Heart Rate and Blood Pressure in Healthy Young
1. INTRODUCTION. National Hospital for Neurology & Neurosurgery, London
 RATE OF CHANGE IN CEREBRAL OXYGENATION AND BLOOD PRESSURE IN RESPONSE TO PASSIVE CHANGES IN POSTURE: A COMPARISON BETWEEN PURE AUTONOMIC FAILURE PATIENTS AND CONTROLS Ilias Tachtsidis, Clare E. Elwell,
RATE OF CHANGE IN CEREBRAL OXYGENATION AND BLOOD PRESSURE IN RESPONSE TO PASSIVE CHANGES IN POSTURE: A COMPARISON BETWEEN PURE AUTONOMIC FAILURE PATIENTS AND CONTROLS Ilias Tachtsidis, Clare E. Elwell,
Spinal Cord (2014), 1 5. & 2014 International Spinal Cord Society All rights reserved /14
 (214), 1 5 & 214 International Society All rights reserved 1362-4393/14 www.nature.com/sc ORIGINAL ARTICLE Electrical stimulation-evoked contractions blunt orthostatic hypotension in sub-acute spinal cord-injured
(214), 1 5 & 214 International Society All rights reserved 1362-4393/14 www.nature.com/sc ORIGINAL ARTICLE Electrical stimulation-evoked contractions blunt orthostatic hypotension in sub-acute spinal cord-injured
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
This work was supported by the VA RR&D Service: Grants # B4162C and B4723H
 Jill M. Wecht, EdD Associate Professor of Medicine and Rehabilitation Medicine; the Mount Sinai School of Medicine Career Development 2; VA Rehabilitation Research & Development Service This work was supported
Jill M. Wecht, EdD Associate Professor of Medicine and Rehabilitation Medicine; the Mount Sinai School of Medicine Career Development 2; VA Rehabilitation Research & Development Service This work was supported
The postural tachycardia syndrome (POTS) is characterized
 Sympathetic Nerve Activity in Response to Hypotensive Stress in the Postural Tachycardia Syndrome Istvan Bonyhay, MD, PhD; Roy Freeman, MD Background Increased central sympathetic activity and/or deficient
Sympathetic Nerve Activity in Response to Hypotensive Stress in the Postural Tachycardia Syndrome Istvan Bonyhay, MD, PhD; Roy Freeman, MD Background Increased central sympathetic activity and/or deficient
Program Highlights. Michael Pourfar, MD Co-Director, Center for Neuromodulation New York University Langone Medical Center New York, New York
 Program Highlights David Swope, MD Associate Professor of Neurology Mount Sinai Health System New York, New York Michael Pourfar, MD Co-Director, Center for Neuromodulation New York University Langone
Program Highlights David Swope, MD Associate Professor of Neurology Mount Sinai Health System New York, New York Michael Pourfar, MD Co-Director, Center for Neuromodulation New York University Langone
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD
 AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
Blood pressure fluctuation and hypertension in patients with Parkinson s disease
 Blood pressure fluctuation and hypertension in patients with Parkinson s disease Tetsuro Tsukamoto 1, Yoshimi Kitano 2 & Sadako Kuno 3 1 Department of Neurology, Numazu Rehabilitation Hospital, 2510-22
Blood pressure fluctuation and hypertension in patients with Parkinson s disease Tetsuro Tsukamoto 1, Yoshimi Kitano 2 & Sadako Kuno 3 1 Department of Neurology, Numazu Rehabilitation Hospital, 2510-22
Orthostatic Hypotension
 Orthostatic Hypotension http://suntechmed.web4.hubspot.com/portals/41365/images/bloodpressuredoctor.jpg Orthostatic (postural) hypotension is an excessive fall in BP when an upright position is assumed.
Orthostatic Hypotension http://suntechmed.web4.hubspot.com/portals/41365/images/bloodpressuredoctor.jpg Orthostatic (postural) hypotension is an excessive fall in BP when an upright position is assumed.
Faculty. Joseph Friedman, MD
 Faculty Claire Henchcliffe, MD, DPhil Associate Professor of Neurology Weill Cornell Medical College Associate Attending Neurologist New York-Presbyterian Hospital Director of the Parkinson s Institute
Faculty Claire Henchcliffe, MD, DPhil Associate Professor of Neurology Weill Cornell Medical College Associate Attending Neurologist New York-Presbyterian Hospital Director of the Parkinson s Institute
Hypotensive susceptibility and antihypertensive drugs Diana Solari Santa Margherita Ligure, 7 aprile 2016
 Hypotensive susceptibility and antihypertensive drugs Diana Solari Santa Margherita Ligure, 7 aprile 2016 Arrhythmologic Center, Department of Cardiology, Lavagna SYNCOPE AND ANTIHYPERTENSIVE DRUGS Many
Hypotensive susceptibility and antihypertensive drugs Diana Solari Santa Margherita Ligure, 7 aprile 2016 Arrhythmologic Center, Department of Cardiology, Lavagna SYNCOPE AND ANTIHYPERTENSIVE DRUGS Many
Ivabradine in Inappropriate Sinus Tachycardia
 UNIVERSITA DEGLI STUDI DI MILANO I.R.C.C.S POLICLINICO SAN DONATO CENTRO PER LO STUDIO E LA TERAPIA DELLLE MALATTIE CARDIOVASCOLARI E. MALAN Ivabradine in Inappropriate Sinus Tachycardia Riccardo Cappato,
UNIVERSITA DEGLI STUDI DI MILANO I.R.C.C.S POLICLINICO SAN DONATO CENTRO PER LO STUDIO E LA TERAPIA DELLLE MALATTIE CARDIOVASCOLARI E. MALAN Ivabradine in Inappropriate Sinus Tachycardia Riccardo Cappato,
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Northera) Reference Number: CP.PMN.17 Effective Date: 08.01.16 Last Review Date: 11.18 Line of Business: Commercial, Medicaid Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Northera) Reference Number: CP.PMN.17 Effective Date: 08.01.16 Last Review Date: 11.18 Line of Business: Commercial, Medicaid Revision Log See Important Reminder at the end of this policy
European Commission approves ONGENTYS (opicapone) a novel treatment for Parkinson s disease patients with motor fluctuations
 July 6, 2016 European Commission approves ONGENTYS (opicapone) a novel treatment for Parkinson s disease patients with motor fluctuations Porto, 5 July 2016 BIAL announced that the medicinal product ONGENTYS
July 6, 2016 European Commission approves ONGENTYS (opicapone) a novel treatment for Parkinson s disease patients with motor fluctuations Porto, 5 July 2016 BIAL announced that the medicinal product ONGENTYS
Autonomic Dysfunction
 Autonomic Dysfunction Unique anatomy PRE-GANGLIONIC POST-GANGLIONIC PRE-GANGLIONIC POST-GANGLIONIC Bradbury-Eggleston Postural hypotension with cardiovascular, GI, urogenital, thermoregulatory, sudomotor
Autonomic Dysfunction Unique anatomy PRE-GANGLIONIC POST-GANGLIONIC PRE-GANGLIONIC POST-GANGLIONIC Bradbury-Eggleston Postural hypotension with cardiovascular, GI, urogenital, thermoregulatory, sudomotor
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1)
 I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
An Update on the Physiology of Mild Traumatic Brain Injury. Barry Willer PhD Grand Rounds Psychiatry 2017
 An Update on the Physiology of Mild Traumatic Brain Injury Barry Willer PhD Grand Rounds Psychiatry 2017 Disclosures The Buffalo Sabres Foundation Robert Rich Family Foundation PUCCS Foundation NFL Charities
An Update on the Physiology of Mild Traumatic Brain Injury Barry Willer PhD Grand Rounds Psychiatry 2017 Disclosures The Buffalo Sabres Foundation Robert Rich Family Foundation PUCCS Foundation NFL Charities
Use of Methylphenidate in the Treatment of Patients Suffering From Refractory Postural Tachycardia Syndrome
 American Journal of Therapeutics 0, 000 000 (2010) Use of Methylphenidate in the Treatment of Patients Suffering From Refractory Postural Tachycardia Syndrome Khalil Kanjwal, MD, 1 Bilal Saeed, MD, 2 Beverly
American Journal of Therapeutics 0, 000 000 (2010) Use of Methylphenidate in the Treatment of Patients Suffering From Refractory Postural Tachycardia Syndrome Khalil Kanjwal, MD, 1 Bilal Saeed, MD, 2 Beverly
Orthostatic Intolerance (OI) In the Young. (orthostasis = standing) (OI= Can t remain standing)
 Orthostatic Intolerance (OI) In the Young (orthostasis = standing) (OI= Can t remain standing) Gravitational Blood Distribution in Man and Beast Unconstrained Pooling Causes Rapid Loss of BP Circulatory
Orthostatic Intolerance (OI) In the Young (orthostasis = standing) (OI= Can t remain standing) Gravitational Blood Distribution in Man and Beast Unconstrained Pooling Causes Rapid Loss of BP Circulatory
Neurogenic orthostatic hypotension: the very basics
 Clin Auton Res (2017) 27:39 43 DOI 10.1007/s10286-017-0437-3 EDITORIAL Neurogenic orthostatic hypotension: the very basics Horacio Kaufmann 1 Jose-Alberto Palma 1 Received: 7 June 2017 / Accepted: 8 June
Clin Auton Res (2017) 27:39 43 DOI 10.1007/s10286-017-0437-3 EDITORIAL Neurogenic orthostatic hypotension: the very basics Horacio Kaufmann 1 Jose-Alberto Palma 1 Received: 7 June 2017 / Accepted: 8 June
Evaluation and Management of Parkinson s Disease in the Older Patient
 Evaluation and Management of Parkinson s Disease in the Older Patient David A. Hinkle, MD, PhD Comprehensive Movement Disorders Clinic Pittsburgh Institute for Neurodegenerative Diseases University of
Evaluation and Management of Parkinson s Disease in the Older Patient David A. Hinkle, MD, PhD Comprehensive Movement Disorders Clinic Pittsburgh Institute for Neurodegenerative Diseases University of
Alcohol consumption may be linked to syncopal events.
 Alcohol Potentiates Orthostatic Hypotension Implications for Alcohol-Related Syncope Krzysztof Narkiewicz, MD, PhD; Ryan L. Cooley, MD; Virend K. Somers, MD, PhD Background Alcohol consumption may be linked
Alcohol Potentiates Orthostatic Hypotension Implications for Alcohol-Related Syncope Krzysztof Narkiewicz, MD, PhD; Ryan L. Cooley, MD; Virend K. Somers, MD, PhD Background Alcohol consumption may be linked
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
Hypotension Focus: It s not ACS or HF, but it will be on the PANRE. Question #1. Question #2. Andrea Applegate, PA-C
 Hypotension Focus: It s not ACS or HF, but it will be on the PANRE Andrea Applegate, PA-C Question #1 Which of the following pains is associated with orthostatic hypotension? A. toe box pain B. coat hanger
Hypotension Focus: It s not ACS or HF, but it will be on the PANRE Andrea Applegate, PA-C Question #1 Which of the following pains is associated with orthostatic hypotension? A. toe box pain B. coat hanger
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Movement Disorders: A Brief Overview
 Movement Disorders: A Brief Overview Albert Hung, MD, PhD Massachusetts General Hospital Harvard Medical School August 17, 2006 Cardinal Features of Parkinsonism Tremor Rigidity Bradykinesia Postural imbalance
Movement Disorders: A Brief Overview Albert Hung, MD, PhD Massachusetts General Hospital Harvard Medical School August 17, 2006 Cardinal Features of Parkinsonism Tremor Rigidity Bradykinesia Postural imbalance
Prior Authorization with Quantity Limit Program Summary
 Gocovri (amantadine) Prior Authorization with Quantity Limit Program Summary This prior authorization applies to Commercial, NetResults A series, SourceRx and Health Insurance Marketplace formularies.
Gocovri (amantadine) Prior Authorization with Quantity Limit Program Summary This prior authorization applies to Commercial, NetResults A series, SourceRx and Health Insurance Marketplace formularies.
Dizziness, postural hypotension and postural blackouts: Two cases suggesting multiple system atrophy
 Dizziness, postural hypotension and postural blackouts: Two cases suggesting multiple system atrophy Dr Rahul Chakor, Associate Prof and Head Dept of Neurology, Dr Anand Soni, Senior Resident, T N Medical
Dizziness, postural hypotension and postural blackouts: Two cases suggesting multiple system atrophy Dr Rahul Chakor, Associate Prof and Head Dept of Neurology, Dr Anand Soni, Senior Resident, T N Medical
Evaluation of non-motor symptoms in Parkinson s Disease: An underestimated necessity
 HIPPOKRATIA 2013, 17, 3: 214-219 ORIGINAL ARTICLE Evaluation of non-motor symptoms in Parkinson s Disease: An underestimated necessity Bostantjopoulou S 1, Katsarou Z 2, Karakasis C 1,Peitsidou E 1, Milioni
HIPPOKRATIA 2013, 17, 3: 214-219 ORIGINAL ARTICLE Evaluation of non-motor symptoms in Parkinson s Disease: An underestimated necessity Bostantjopoulou S 1, Katsarou Z 2, Karakasis C 1,Peitsidou E 1, Milioni
Cardiovascular Physiology: Cardiovascular (CV) adjustment during exercise:
 Cardiovascular Physiology: Cardiovascular (CV) adjustment during exercise: By Dr Dler Gallaly (Lecturer) PhD in Medical Physiology- Dept. of Physiology, College of Medicine, HMU- Erbil- Iraq. 2016 / 2017
Cardiovascular Physiology: Cardiovascular (CV) adjustment during exercise: By Dr Dler Gallaly (Lecturer) PhD in Medical Physiology- Dept. of Physiology, College of Medicine, HMU- Erbil- Iraq. 2016 / 2017
Adrenal Medulla. Amelyn R. Rafael, M.D.
 Adrenal Medulla Amelyn R. Rafael, M.D. Adrenal Medulla Exodermal in origin Cells derived from the sympathogonia of the primitive neuroectoderm A sympathetic ganglion in which the post-ganglionic cells
Adrenal Medulla Amelyn R. Rafael, M.D. Adrenal Medulla Exodermal in origin Cells derived from the sympathogonia of the primitive neuroectoderm A sympathetic ganglion in which the post-ganglionic cells
