Chapter 20. Drugs Affecting Circulation: Antihypertensives, Antianginals, Antithrombotics
|
|
|
- Justin Patrick
- 6 years ago
- Views:
Transcription
1 Chapter 20 Drugs Affecting Circulation: Antihypertensives, Antianginals, Antithrombotics
2 Epidemiology and Etiology of Hypertension Primary: Unknown etiology Secondary: Due to known disease process Adversely affects numerous organs Termed cardiovascular disease (CVD) Diagnosis: Two or more seated BP taken on different days Increased risk of: Left ventricular (LV) hypertrophy, angina, myocardial infarction (MI), heart failure, stroke, peripheral arterial disease (PAD), retinopathy, and renal failure
3 Pathophysiology of Hypertension Arterial blood pressure Product of cardiac output (CO) and total resistance Preload is major factor in systolic blood pressure (SBP) Affects venous capacitance Afterload is major factor in diastolic blood pressure (DBP)
4 Hypertensive Crisis Patient with BP > 180/120 mmhg Hypertensive urgency No signs/symptoms of organ complication Hypertensive emergency Acute, chronic, or progressive organ injury
5 Hypertension Pharmacotherapy First-line agents: Angiotensin-converting enzyme inhibitors (ACEIs) Angiotensin II receptor blockers (ARBs) Calcium channel blockers (CCBs) β Blockers Thiazide-type diuretics
6 Hypertension Pharmacotherapy (cont d) Second-line agents Vasodilators α Blockers α 2 Agonists Antiadrenergics
7 Hypertension Pharmacotherapy (cont d) Angiotensin-converting enzyme inhibitors Suppress renin-angiotensin-aldosterone system Block conversion of angiotensin I to angiotensin II Hemodynamic effect Reduce peripheral arterial resistance (PAR) Increase CO Increase renal blood flow
8 Hypertension Pharmacotherapy (cont d) Indicated for: Hypertension (HTN), heart failure, systolic dysfunction, MI prevention, LV dysfunction, and diabetic neuropathy Generally decrease SBP and DBP 15-25% Most common side effect is dry cough Significant interaction with nonsteroidal antiinflammatory drugs (NSAIDs)
9 Hypertension Pharmacotherapy (cont d) Angiotensin II receptor blockers Angiotensin II type 1 receptor agonists Receptors found in vascular smooth muscle, myocardium, brain, kidney, liver, uterus, adrenal glands Indicated for HTN and treatment of heart failure Slightly weaker than ACEIs Side effects: Orthostatic hypotension, hyperkalemia, neutropenia, nephrotoxicity, and fetotoxicity
10 Hypertension Pharmacotherapy (cont d) Calcium channel blockers Cause coronary and peripheral vasodilation via L- channel blockade Verapamil and diltiazem Negative chronotropic and inotropic effects Long-acting formulations (target circadian rhythm) High incidence of constipation Side effects
11 Hypertension Pharmacotherapy β Blockers Method of action (cont d) Indications Essential HTN, angina, dysrhythmias, MI prevention, chronic heart failure Also: Migraine prophylaxis and alcohol withdrawal May induce bronchospasm and render β-agonist ineffective
12 Hypertension Pharmacotherapy Diuretics (cont d) Five classes Thiazide and thiazide-like agents Loop diuretics K-sparing agents Used for HTN Carbonic anhydrase inhibitors (CAIs) Osmotics Interact with NSAIDs
13 Hypertension Pharmacotherapy (cont d) Potassium-sparing diuretics Weak if used alone Additive effect with thiazides Amiloride (Midamor) and triamterene (Dyrenium) Side effects
14 Hypertension Pharmacotherapy (cont d) Thiazide and thiazide-like diuretics Increase Na and Cl excretion Dose-ceiling effect 2 to 4 weeks to elicit full effect Side effects
15 Hypertension Pharmacotherapy (cont d) Loop diuretics Decrease Na reabsorption at ascending limb of loop of Henle Indicated for chronic heart failure, ascites, renal failure, pulmonary edema, hypercalcemia, hypermagnesemia, syndrome of inappropriate antidiuretic hormone Second-line treatment for management of HTN Cause frequent urination
16 Hypertension Pharmacotherapy Aldosterone antagonists (cont d) Spironolactone (Aldactone) and Eplerenone (Inspra) Spironolactone is weak, often used with other antihypertensives Adverse effects: Impotence, gynecomastia, deep voice, menstrual irregularities, hirsutism, gastrointestinal upset, rash, drowsiness Eplerenone Indicated for HTN and post-mi heart failure Minimal adverse sexual side effects Higher risk of hyperkalemia
17 Hypertension Pharmacotherapy (cont d) Centrally acting adrenergic agents Affect CO and peripheral resistance Negative inotrope/negative chronotrope α 2 Agonists are effective, but riddled with side effects Clonidine transdermal is most effective and least toxic
18 Hypertension Pharmacotherapy (cont d) α 1 -Adrenergic antagonists Cause arterial and venous dilation Decrease preload and afterload First-dose phenomenon Initial doses low and at bedtime Indicated for HTN, benign prostatic hyperplasia, heart failure, and Raynaud s vasospasm
19 Hypertension Pharmacotherapy Antiadrenergic agents Second-line drugs (cont d) Reserpine Depletes postganglionic norepinephrine May cause: Sedation, depression, psychosis, peptic ulcers, nasal stuffiness Guanethidine (Ismelin) and Guanadrel (Hylorel) Substitute neurotransmitters May cause orthostatic hypotension, sexual dysfunction, explosive diarrhea
20 Hypertension Pharmacotherapy Vasodilators (cont d) Hydralazine (Apresoline) and minoxidil (Rogaine, Loniten) Second-line treatment for HTN because of side effects Act on vascular smooth muscle to decrease total peripheral resistance May cause reflex tachycardia, renin release, increased CO Often given with β blocker and loop diuretic
21 Epidemiology, Etiology, and Pathophysiology of Angina Chest pain Symptom of myocardial ischemia Imbalance of myocardial O 2 supply and demand May present as: Heavy weight or pressure on chest Burning sensation Shortness of breath (SOB) Pain over sternum, left shoulder, or lower jaw
22 Pharmacotherapy for Angina Nitrates Nitroglycerin dilates coronary arteries and collaterals (mostly venous effect) Indications: Angina, acute MI, HTN Formulations: Oral, IV, ointment, transdermal, translingual, sublingual Sublingual: Q 5 minutes x 3, then seek care Adverse effects: Tachycardia, palpitations, hypotension, dizziness, flushing, headache
23 Pharmacotherapy for Angina (cont d) Ranolazine (Ranexa) Indicated for chronic angina not responding to other medications Shifts energy production from fatty acid oxidation to glucose oxidation (uses less O 2 ) 500 mg BID (maximum, 1 g BID) Contraindicated in hepatic dysfunction
24 Antithrombotic Agents Formation and elimination of acute coronary thrombus Formation initiated by injury to endothelium Platelets adhere to site of injury, release chemicals that cause further aggregation, forming unstable thrombus Eventually forms insoluble fibrin clot Must be removed by fibrinolytic system for homeostasis to be maintained
25 Antithrombotic Agents (cont d) Anticoagulant agents Heparins: Unfractionated heparin and low molecular weight heparin Indicated for venous thromboembolism, pulmonary embolism, atrial fibrillation (AF), disseminated intravascular coagulation (DIC), and peripheral arterial embolism Extracted from porcine intestinal mucosa
26 Antithrombotic Agents (cont d) Anticoagulant agents (cont d) Heparins: Unfractionated heparin and low molecular weight heparin (cont d) Goal: Balance unwanted clotting with risk of hemorrhage Side effects: Bleeding, thrombocytopenia, hyperkalemia, osteoporosis, increased liver enzyme tests (LETs) Antidote: Protamine sulfate
27 Antithrombotic Agents (cont d) Anticoagulant agents (cont d) Direct thrombin inhibitors Desirudin (Iprivask): Indicated for deep vein thrombosis (DVT) Bivalirudin (Angiomax): Indicated for unstable angina Argatroban and lepirudin (Refludan): Used for anticoagulation of patients with heparin-induced thrombocytopenia type 2 (HIT-2) Common adverse side effect: Hemorrhage
28 Antithrombotic Agents (cont d) Anticoagulant agents (cont d) Warfarin (Coumadin) Oral anticoagulant for venous thrombosis, pulmonary embolism (PE), AF, valve replacement, coronary occlusion Daily dosing (delayed onset of 3-5 days) International normalized ratio (INR) is standard for monitoring therapy Hemorrhage is common side effect Many drugs may increase/decrease effects
29 Antithrombotic Agents (cont d) Antiplatelet agents Aspirin Reduces platelet aggregation by inhibition of prostaglandin production Antithrombotic indications: Reduce risk of thrombosis, transient ischemic attack (TIA), or stroke
30 Antithrombotic Agents (cont d) Antiplatelet agents (cont d) Aspirin (cont d) Side effects: Peptic ulcer, renal dysfunction, HTN, tinnitus, pulmonary dysfunction, and bleeding Ibuprofen inhibits pharmacological effect; concurrent NSAID use may cause fatal gastropathy
31 Antithrombotic Agents (cont d) Antiplatelet agents (cont d) Dipyridamole Vasodilator and platelet adhesion inhibitor Indicated as an adjunct to warfarin in prevention of postoperative thromboembolic complications of cardiac valve replacement May potentiate effect of adenosine
32 Antithrombotic Agents (cont d) Antiplatelet agents (cont d) Clopidogrel (Plavix) Platelet aggregation inhibitor Indications: History of MI, stroke, PAD, acute coronary syndrome Slightly more effective than aspirin (except for stroke prophylaxis) Metabolized by liver Steady state in 3 to 7 days 75 mg QD (plus aspirin) 300-mg loading dose for acute coronary syndrome (ACS)
33 Antithrombotic Agents (cont d) Antiplatelet agents (cont d) Ticlopidine Platelet aggregation inhibitor Indicated for stroke More effective than aspirin Steady state in 14 to 21 days Metabolized by liver Risk of life-threatening blood dyscrasias Use only if aspirin/clopidogrel are unacceptable
34 Antithrombotic Agents (cont d) Antiplatelet agents (cont d) Cilostazol and pentoxifylline Cause vasodilation and inhibition of platelet aggregation Indicated for PAD pain Clinical benefits may take up to 12 weeks Transient adverse effects: Headache, diarrhea, dizziness, palpitations 100 mg BID on an empty stomach
35 Antithrombotic Agents (cont d) Antiplatelet agents (cont d) Glycoprotein IIb/IIIa inhibitors Indicated for ACS Abciximab (ReoPro) is drug of choice Not available in oral formulation (ineffective) Bleeding is most common adverse side effect
36 Antithrombotic Agents (cont d) Thrombolytic agents Indicated for PE, ischemic stroke, and acute ST segment elevation MI Agents: Streptokinase (second line), alteplase, reteplase, and tenecteplase Therapy should begin within 12 hours of symptoms
37 Antithrombotic Agents (cont d) Thrombolytic agents (cont d) Contraindications: Internal bleeding, aortic dissection, head injury or stroke in last 3 months, HTN, anticoagulant use Bleeding is most common adverse effect Gastrointestinal, genitourinary, respiratory tract, retroperitoneal, intracranial
Chapter 10 Worksheet Blood Pressure and Antithrombotic Agents
 Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
7/7/ CHD/MI LVH and LV dysfunction Dysrrhythmias Stroke PVD Renal insufficiency and failure Retinopathy. Normal <120 Prehypertension
 Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Section 3, Lecture 2
 59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Nitroglycerin and Heparin Drip Interfacility Protocols
 Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs
 Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Hypertension (JNC-8)
 Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Index. Hematol Oncol Clin N Am 19 (2005) Note: Page numbers of article titles are in boldface type.
 Hematol Oncol Clin N Am 19 (2005) 203 208 Index Note: Page numbers of article titles are in boldface type. A Abciximab, as an antiplatelet agent, 93 94 Acute coronary syndromes, use of antiplatelet drugs
Hematol Oncol Clin N Am 19 (2005) 203 208 Index Note: Page numbers of article titles are in boldface type. A Abciximab, as an antiplatelet agent, 93 94 Acute coronary syndromes, use of antiplatelet drugs
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood:
 Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Antihypertensives. Antihypertensive Classes. RAAS Inhibitors. Renin-Angiotensin Cascade. Angiotensin Receptors. Approaches to Hypertension Treatment
 Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Treatment of T Angina reatment of By Ali Alalawi
 Treatment of Angina By Ali Alalawi Determinants of Oxygen Demand Need to improve ratio of: Coronary blood flow / cardiac work Or Cardiac O2 Supply / Cardiac Requirement Coronary Circulation vs Other Circulation
Treatment of Angina By Ali Alalawi Determinants of Oxygen Demand Need to improve ratio of: Coronary blood flow / cardiac work Or Cardiac O2 Supply / Cardiac Requirement Coronary Circulation vs Other Circulation
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Angina Pectoris. Edward JN Ishac, Ph.D. Smith Building, Room
 Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari
![Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari Pharmacology I [PHL 313] Diuretics. Dr. Mohammad Nazam Ansari](/thumbs/90/104323364.jpg) Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
Pharmacology I [PHL 313] Diuretics Dr. Mohammad Nazam Ansari Renal Pharmacology Kidneys: Each adult kidney weighs 125-170g in males and 115-155g in females, represent 0.5% of total body weight, but receive
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
CHAPTER-I MYOCARDIAL INFARCTION
 CHAPTER-I MYOCARDIAL INFARCTION Definition A myocardial infarction, more commonly known as MI or acute myocardial infarction (AMI) or heart attack is a condition where there is interruption of blood supply
CHAPTER-I MYOCARDIAL INFARCTION Definition A myocardial infarction, more commonly known as MI or acute myocardial infarction (AMI) or heart attack is a condition where there is interruption of blood supply
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Hemostasis and Blood Forming Organs
 Hemostasis and Blood Forming Organs Subcommittee: Williams, Patricia B. (Chair) pbwillia@umich.edu McMillan, David dcmcmillan@unmc.edu Dobrydneva, Yuliya dobrydy@evms.edu DEFEROXAMINE FERROUS SULFATE ferrous
Hemostasis and Blood Forming Organs Subcommittee: Williams, Patricia B. (Chair) pbwillia@umich.edu McMillan, David dcmcmillan@unmc.edu Dobrydneva, Yuliya dobrydy@evms.edu DEFEROXAMINE FERROUS SULFATE ferrous
ANGINA PECTORIS. angina pectoris is a symptom of myocardial ischemia in the absence of infarction
 Pharmacology Ezra Levy, Pharm.D. ANGINA PECTORIS A. Definition angina pectoris is a symptom of myocardial ischemia in the absence of infarction angina usually implies severe chest pain or discomfort during
Pharmacology Ezra Levy, Pharm.D. ANGINA PECTORIS A. Definition angina pectoris is a symptom of myocardial ischemia in the absence of infarction angina usually implies severe chest pain or discomfort during
Anginal pain is a result of an imbalance between myocardial oxygen supply and demand. Pharmacological management is aimed at prevention of myocardial
 Angina Anginal pain is a result of an imbalance between myocardial oxygen supply and demand. Pharmacological management is aimed at prevention of myocardial ischemia and pain as well as prevention of myocardial
Angina Anginal pain is a result of an imbalance between myocardial oxygen supply and demand. Pharmacological management is aimed at prevention of myocardial ischemia and pain as well as prevention of myocardial
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Anticoagulants. Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT
 Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Acute coronary syndromes
 Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Acute coronary syndromes 1 Acute coronary syndromes Acute coronary syndromes results primarily from diminished myocardial blood flow secondary to an occlusive or partially occlusive coronary artery thrombus.
Blood Thinner Agent. Done by: Meznah Al-mutairi Pharm.D Candidate PNU Collage of Pharmacy
 Blood Thinner Agent Done by: Meznah Al-mutairi Pharm.D Candidate PNU Collage of Pharmacy Outline: Blood thinner agent definition. anticoagulants drugs. Thrombolytics. Blood thinner agent Therapeutic interference
Blood Thinner Agent Done by: Meznah Al-mutairi Pharm.D Candidate PNU Collage of Pharmacy Outline: Blood thinner agent definition. anticoagulants drugs. Thrombolytics. Blood thinner agent Therapeutic interference
LXIV: DRUGS: 4. RAS BLOCKADE
 LXIV: DRUGS: 4. RAS BLOCKADE ACE Inhibitors Components of RAS Actions of Angiotensin i II Indications for ACEIs Contraindications RAS blockade in hypertension RAS blockade in CAD RAS blockade in HF Limitations
LXIV: DRUGS: 4. RAS BLOCKADE ACE Inhibitors Components of RAS Actions of Angiotensin i II Indications for ACEIs Contraindications RAS blockade in hypertension RAS blockade in CAD RAS blockade in HF Limitations
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Chapter 21. Diuretic Agents. Mosby items and derived items 2008, 2002 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
M2 TEACHING UNDERSTANDING PHARMACOLOGY
 M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
Management of Hypertension
 Clinical Practice Guidelines Management of Hypertension Definition and classification of blood pressure levels (mmhg) Category Systolic Diastolic Normal
Clinical Practice Guidelines Management of Hypertension Definition and classification of blood pressure levels (mmhg) Category Systolic Diastolic Normal
Hypertensives Emergency and Urgency
 Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
Oral Anticoagulant Drugs
 Oral Anticoagulant Drugs Spoiled sweet clover caused hemorrhage in cattle(1930s). Substance identified as bishydroxycoumarin. Initially used as rodenticides, still very effective, more than strychnine.
Oral Anticoagulant Drugs Spoiled sweet clover caused hemorrhage in cattle(1930s). Substance identified as bishydroxycoumarin. Initially used as rodenticides, still very effective, more than strychnine.
Managing IHD and acute Myocardial Infarction
 Managing IHD and acute Myocardial Infarction In Ireland- 1 out of every 10 deaths ( 22% of all premature deaths) in 2006 were due to CVD 30,000 15,000 0 1998 1999 2000 2001 2002 2003 2004 2005 2006 Source
Managing IHD and acute Myocardial Infarction In Ireland- 1 out of every 10 deaths ( 22% of all premature deaths) in 2006 were due to CVD 30,000 15,000 0 1998 1999 2000 2001 2002 2003 2004 2005 2006 Source
Introduction. Factors affecting blood pressure: 1-COP = HR X SV mainly affect SBP. 2-TPR = diameter of arterioles X viscosity of blood affect DBP
 Introduction Hypertension is a persistent elevation of blood pressure above 140 / 90 mmhg for more than three sitting. (0ptimal level
Introduction Hypertension is a persistent elevation of blood pressure above 140 / 90 mmhg for more than three sitting. (0ptimal level
sympatholytics sympatholytics sympatholytics
 sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
Low Efficacy Diuretics. Potassium sparing diuretics. Carbonic anhydrase inhibitors. Osmotic diuretics. Miscellaneous
 University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Low Efficacy Diuretics 1. Potassium sparing diuretics 2. Carbonic anhydrase inhibitors 3. Osmotic diuretics 4. Miscellaneous
University of Al Qadisiyah College of Pharmacy Dr. Bassim I Mohammad, MBChB, MSc, Ph.D Low Efficacy Diuretics 1. Potassium sparing diuretics 2. Carbonic anhydrase inhibitors 3. Osmotic diuretics 4. Miscellaneous
Hypertension diagnosis (see detail document) Diabetic. Target less than 130/80mmHg
 Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Hypertension diagnosis (see detail document) Non-diabetic Diabetic Very elderly (older than 80 years) Target less than 140/90mmHg Target less than 130/80mmHg Consider SBP target less than 150mmHg Non-diabetic
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina
 Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Medicine Dr. Omed Lecture 2 Stable and Unstable Angina Risk stratification in stable angina. High Risk; *post infarct angina, *poor effort tolerance, *ischemia at low workload, *left main or three vessel
Prof dr Aleksandar Raskovic DIRECT VASODILATORS
 Prof dr Aleksandar Raskovic DIRECT VASODILATORS Direct vasodilators Minoxidil (one of the most powerful peripheral arterial dilators) Opening of KATP channels, efflux of K, lose of Ca and smooth muscle
Prof dr Aleksandar Raskovic DIRECT VASODILATORS Direct vasodilators Minoxidil (one of the most powerful peripheral arterial dilators) Opening of KATP channels, efflux of K, lose of Ca and smooth muscle
Fundamentals of Pharmacology for Veterinary Technicians Chapter 8
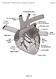 Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
Management of Hypertension. Ahmed El Hawary MD Suez Canal University
 Management of Hypertension Ahmed El Hawary MD Suez Canal University Minimal vs. Optimal Care Resources more than science affect type of care and level of management. what is possible (minimal care) and
Management of Hypertension Ahmed El Hawary MD Suez Canal University Minimal vs. Optimal Care Resources more than science affect type of care and level of management. what is possible (minimal care) and
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
CCRN Review Cardiovascular
 CCRN Review Cardiovascular Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Angina Definition discomfort that occurs when oxygen demand
CCRN Review Cardiovascular Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Angina Definition discomfort that occurs when oxygen demand
Pharmacology. Drugs affecting the Cardiovascular system (Antianginal Drugs)
 Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Heart failure. Failure? blood supply insufficient for body needs. CHF = congestive heart failure. increased blood volume, interstitial fluid
 Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
New Antithrombotic and Antiplatelet Drugs in CAD : (Factor Xa inhibitors, Direct Thrombin inhibitors and Prasugrel)
 New Antithrombotic and Antiplatelet Drugs in CAD : (Factor Xa inhibitors, Direct Thrombin inhibitors and Prasugrel) Limitations and Advantages of UFH and LMWH Biological limitations of UFH : 1. immune-mediated
New Antithrombotic and Antiplatelet Drugs in CAD : (Factor Xa inhibitors, Direct Thrombin inhibitors and Prasugrel) Limitations and Advantages of UFH and LMWH Biological limitations of UFH : 1. immune-mediated
Hypertension. Penny Mosley MRPharmS
 Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Antihypertensives. Diagnostic category
 Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
Categories of HTN. Overview of Hypertension. Types of Hypertension
 Categories of HTN Overview of Hypertension Normal SBP 100 Quick review of the Basics: What is
Categories of HTN Overview of Hypertension Normal SBP 100 Quick review of the Basics: What is
Coronary Heart Disease. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Coronary Heart Disease Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives Define coronary heart disease (CHD). Identify the causes and risk factors of CHD Discuss the pathophysiological
Coronary Heart Disease Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives Define coronary heart disease (CHD). Identify the causes and risk factors of CHD Discuss the pathophysiological
Angina pectoris due to coronary atherosclerosis : Atenolol is indicated for the long term management of patients with angina pectoris.
 Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Beta 1 Beta blockers A - Propranolol,
 Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
ISCHEMIC HEART DISEASE (IHD)
 ISCHEMIC HEART DISEASE (IHD) 1 Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU DEFINITIONS IHD: O2 or blood supply to myocardium resulting from coronary
ISCHEMIC HEART DISEASE (IHD) 1 Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU DEFINITIONS IHD: O2 or blood supply to myocardium resulting from coronary
Heart Failure. Dr. Alia Shatanawi
 Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Nanik Hatsakorzian Pharm.D/MPH
 Pharm.D/MPH 2014 1 Therapeutics FDA indication & Dosing Clinical Pearls Anticoagulants Heparin Antiphospholipid antibody syndrome Cerebral thromboembolism Prosthetic heart valve Acute coronary syndrome
Pharm.D/MPH 2014 1 Therapeutics FDA indication & Dosing Clinical Pearls Anticoagulants Heparin Antiphospholipid antibody syndrome Cerebral thromboembolism Prosthetic heart valve Acute coronary syndrome
CARDIAC REHABILITATION PROGRAMME:- MEDICATION
 CARDIAC REHABILITATION PROGRAMME:- MEDICATION AIM OF THIS SESSION Understand the reasons for taking your medications, Discuss the common side effects associated with these medications - knowing when to
CARDIAC REHABILITATION PROGRAMME:- MEDICATION AIM OF THIS SESSION Understand the reasons for taking your medications, Discuss the common side effects associated with these medications - knowing when to
Objectives. Treatment of ACS. Early Invasive Strategy. UA/NSTEMI General Concepts. UA/NSTEMI Initial Therapy/Antithrombotic
 Objectives Treatment of ACS Michael P. Gulseth, Pharm. D., BCPS Pharmacotherapy II Spring 2006 Define early invasive strategy and what patients typically receive this approach Compare/contrast the medications
Objectives Treatment of ACS Michael P. Gulseth, Pharm. D., BCPS Pharmacotherapy II Spring 2006 Define early invasive strategy and what patients typically receive this approach Compare/contrast the medications
Managing Hypertension in the Perioperative Arena
 Managing Hypertension in the Perioperative Arena Optimizing Perioperative Management Strategies for Hypertension in the Cardiac Surgical Patient Objectives: Treatment of hypertensive emergencies. ALBERT
Managing Hypertension in the Perioperative Arena Optimizing Perioperative Management Strategies for Hypertension in the Cardiac Surgical Patient Objectives: Treatment of hypertensive emergencies. ALBERT
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI
 DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
FACTOR Xa AND PAR-1 BLOCKER : ATLAS-2, APPRAISE-2 & TRACER TRIALS
 New Horizons In Atherothrombosis Treatment 2012 순환기춘계학술대회 FACTOR Xa AND PAR-1 BLOCKER : ATLAS-2, APPRAISE-2 & TRACER TRIALS Division of Cardiology, Jeonbuk National University Medical School Jei Keon Chae,
New Horizons In Atherothrombosis Treatment 2012 순환기춘계학술대회 FACTOR Xa AND PAR-1 BLOCKER : ATLAS-2, APPRAISE-2 & TRACER TRIALS Division of Cardiology, Jeonbuk National University Medical School Jei Keon Chae,
Byvalson. (nebivolol, valsartan) New Product Slideshow
 Byvalson (nebivolol, valsartan) New Product Slideshow Introduction Brand name: Byvalson Generic name: Nebivolol, valsartan Pharmacological class: Beta-blocker + angiotensin II receptor blocker (ARB) Strength
Byvalson (nebivolol, valsartan) New Product Slideshow Introduction Brand name: Byvalson Generic name: Nebivolol, valsartan Pharmacological class: Beta-blocker + angiotensin II receptor blocker (ARB) Strength
Cardiovascular Pharmacotherapy
 Cardiovascular Pharmacotherapy Overview Mechanism of cardiovascular drugs Indications and clinical use in cardiology Renin-Angiotensin Inhibitors: Angiotensin-Converting Enzyme Inhibitors, Angiotensin
Cardiovascular Pharmacotherapy Overview Mechanism of cardiovascular drugs Indications and clinical use in cardiology Renin-Angiotensin Inhibitors: Angiotensin-Converting Enzyme Inhibitors, Angiotensin
Pharmacotherapy of Angina Pectoris
 Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Chapter / Section / Drug
 2 Cardiovascular System 2.1 Positive inotropic drugs Digoxin Digoxin specific antibody ( DigiFab ) 2.2 Diuretics 2.2.1 Thiazides and related diuretics Indapamide (1 st Line) Bendroflumethiazide Metolazone
2 Cardiovascular System 2.1 Positive inotropic drugs Digoxin Digoxin specific antibody ( DigiFab ) 2.2 Diuretics 2.2.1 Thiazides and related diuretics Indapamide (1 st Line) Bendroflumethiazide Metolazone
- Mohammad Sinnokrot. -Ensherah Mokheemer. - Malik Al-Zohlof. 1 P a g e
 -1 - Mohammad Sinnokrot -Ensherah Mokheemer - Malik Al-Zohlof 1 P a g e Introduction Two of the most important problems you will face as a doctor are coagulation and bleeding, normally they are in balance,
-1 - Mohammad Sinnokrot -Ensherah Mokheemer - Malik Al-Zohlof 1 P a g e Introduction Two of the most important problems you will face as a doctor are coagulation and bleeding, normally they are in balance,
Heart Failure Clinician Guide JANUARY 2018
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2018 Introduction This evidence-based guideline summary is based on the 2018 National Heart Failure Guideline.
Pharmacotherapy of Angina Pectoris
 Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Pharmacotherapy of Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
TREATMENT OF HYPERTENSION
 TREATMENT OF HYPERTENSION Aim of treatment BP Goals Main items of treatment Lifestyle modification When to start drug Rx Pharmacological therapy 1. Relief of symptoms 2. Prevention of complications and
TREATMENT OF HYPERTENSION Aim of treatment BP Goals Main items of treatment Lifestyle modification When to start drug Rx Pharmacological therapy 1. Relief of symptoms 2. Prevention of complications and
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005
 VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
VA/DoD Clinical Practice Guideline for the Diagnosis and Management of Hypertension - Pocket Guide Update 2004 Revision July 2005 1 Any adult in the health care system 2 Obtain blood pressure (BP) (Reliable,
Agents for Peripheral Vascular Disease & Thrombosis
 Agents for Peripheral Vascular Disease & Thrombosis Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus
Agents for Peripheral Vascular Disease & Thrombosis Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus
Agents for Peripheral Vascular Disease & Thrombosis
 Agents for Peripheral Vascular Disease & Thrombosis Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus
Agents for Peripheral Vascular Disease & Thrombosis Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus
Role of Clopidogrel in Acute Coronary Syndromes. Hossam Kandil,, MD. Professor of Cardiology Cairo University
 Role of Clopidogrel in Acute Coronary Syndromes Hossam Kandil,, MD Professor of Cardiology Cairo University ACS Treatment Strategies Reperfusion/Revascularization Therapy Thrombolysis PCI (with/ without
Role of Clopidogrel in Acute Coronary Syndromes Hossam Kandil,, MD Professor of Cardiology Cairo University ACS Treatment Strategies Reperfusion/Revascularization Therapy Thrombolysis PCI (with/ without
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL 1 Supplemental Table 1. ICD codes Diagnoses, surgical procedures, and pharmacotherapy used for defining the study population, comorbidity, and outcomes Study population Atrial fibrillation
SUPPLEMENTAL MATERIAL 1 Supplemental Table 1. ICD codes Diagnoses, surgical procedures, and pharmacotherapy used for defining the study population, comorbidity, and outcomes Study population Atrial fibrillation
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Chapter 10. Learning Objectives. Learning Objectives 9/11/2012. Congestive Heart Failure
 Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Heart Failure Clinician Guide JANUARY 2016
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Heart Failure Clinician Guide JANUARY 2016 Introduction This evidence-based guideline summary is based on the 2016 National Heart Failure Guideline.
Protocols for the Management of Cardiac Conditions. By Pam Bayles, RN, BSN
 Protocols for the Management of Cardiac Conditions By Pam Bayles, RN, BSN Deaths in Thousands 1,000 800 600 400 200 0 00 10 20 30 40 50 60 70 80 90 00 06 Years Deaths from diseases of the heart (United
Protocols for the Management of Cardiac Conditions By Pam Bayles, RN, BSN Deaths in Thousands 1,000 800 600 400 200 0 00 10 20 30 40 50 60 70 80 90 00 06 Years Deaths from diseases of the heart (United
Diagnosis and Management of Acute Myocardial Infarction
 Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Nursing Process Focus: Patients Receiving Heparin
 Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC. Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Obtain complete heath history including allergies, drug history and possible drug Assess baseline coagulation studies and CBC. Assess for history of bleeding disorders, GI bleeding, cerebral bleed, recent
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
SBP in range of 120 to 140 :no progression or regression of CAD. Sipahi et al., 2006
 Management of Hypertension in Patients with CAD M. Mohsen Ibrahim, MD Cardiology Department- Cairo University 1. What is the optimal BP in patients with hypertension and CAD? 2. What is the minimum safe
Management of Hypertension in Patients with CAD M. Mohsen Ibrahim, MD Cardiology Department- Cairo University 1. What is the optimal BP in patients with hypertension and CAD? 2. What is the minimum safe
Beta-blockers. Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol.
 Drugs of CVS Beta-blockers Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol. Atenolol.cardioselective Propranolol, nonselective Bisoprolol, cardioselective Metoprolol Carvedilol, alpha
Drugs of CVS Beta-blockers Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol. Atenolol.cardioselective Propranolol, nonselective Bisoprolol, cardioselective Metoprolol Carvedilol, alpha
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Heart Failure. Dr. William Vosik. January, 2012
 Heart Failure Dr. William Vosik January, 2012 Questions for clinicians to ask Is this heart failure? What is the underlying cause? What are the associated disease processes? Which evidence-based treatment
Heart Failure Dr. William Vosik January, 2012 Questions for clinicians to ask Is this heart failure? What is the underlying cause? What are the associated disease processes? Which evidence-based treatment
Table 1. Diuretics. Drugs Mechanisms of Action Indications Adverse Drug Effects. Table 2. Electrolyte Modifiers.
 Table 1. Diuretics. hydrochlorothiazide 23 furosemide 23 triamterene 23 Inhibits sodium reabsorption at the distal convoluted tubule Inhibits sodium reabsorption at the loop of Henle Competitive inhibitor
Table 1. Diuretics. hydrochlorothiazide 23 furosemide 23 triamterene 23 Inhibits sodium reabsorption at the distal convoluted tubule Inhibits sodium reabsorption at the loop of Henle Competitive inhibitor
When the learner has completed this module, she/he will be able to:
 Thrombolytics and Myocardial Infarction WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017
Thrombolytics and Myocardial Infarction WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017
Dental Management Considerations for Patients on Antithrombotic Therapy
 Dental Management Considerations for Patients on Antithrombotic Therapy Warfarin and Antiplatelet Joel J. Napeñas DDS FDSRCS(Ed) Program Director General Practice Residency Program Department of Oral Medicine
Dental Management Considerations for Patients on Antithrombotic Therapy Warfarin and Antiplatelet Joel J. Napeñas DDS FDSRCS(Ed) Program Director General Practice Residency Program Department of Oral Medicine
Cardiovascular System
 Therapeutic Agents for the Lecture 04 Therapeutic Agents for the Cardiovascular System Cardiovascular System Chapter 18 1 Anatomy of the Cardiovascular System OBJECTIVES Describe the major components of
Therapeutic Agents for the Lecture 04 Therapeutic Agents for the Cardiovascular System Cardiovascular System Chapter 18 1 Anatomy of the Cardiovascular System OBJECTIVES Describe the major components of
Diuretic Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Blood Pressure Management in Acute Ischemic Stroke
 Blood Pressure Management in Acute Ischemic Stroke Kimberly Clark, PharmD, BCCCP Clinical Pharmacy Specialist Critical Care, Greenville Health System Adjunct Assistant Professor, South Carolina College
Blood Pressure Management in Acute Ischemic Stroke Kimberly Clark, PharmD, BCCCP Clinical Pharmacy Specialist Critical Care, Greenville Health System Adjunct Assistant Professor, South Carolina College
Estimated 5.7 million Americans with HF. 915, 000 new HF cases annually, HF incidence approaches
 Heart Failure: Management of a Chronic Disease Jenny Bauerly RN, CHFN, APRN-BC Heart Failure (HF) Definition A complex clinical syndrome that can result from any structural or functional cardiac disorder
Heart Failure: Management of a Chronic Disease Jenny Bauerly RN, CHFN, APRN-BC Heart Failure (HF) Definition A complex clinical syndrome that can result from any structural or functional cardiac disorder
hypertension Head of prevention and control of CVD disease office Ministry of heath
 hypertension t. Samavat MD,Cadiologist,MPH Head of prevention and control of CVD disease office Ministry of heath RECOMMENDATIONS FOR HYPERTENSION DIAGNOSIS, ASSESSMENT, AND TREATMENT Definition of hypertension
hypertension t. Samavat MD,Cadiologist,MPH Head of prevention and control of CVD disease office Ministry of heath RECOMMENDATIONS FOR HYPERTENSION DIAGNOSIS, ASSESSMENT, AND TREATMENT Definition of hypertension
Angina Pectoris Dr. Shariq Syed
 Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Cardiorenal and Renocardiac Syndrome
 And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
And Renocardiac Syndrome A Vicious Cycle Cardiorenal and Renocardiac Syndrome Type 1 (acute) Acute HF results in acute kidney injury Type 2 Chronic cardiac dysfunction (eg, chronic HF) causes progressive
