Acute heart failure: Clinical presentation, one-year mortality and prognostic factors
|
|
|
- Gladys Richards
- 6 years ago
- Views:
Transcription
1 The European Journal of Heart Failure 7 (2005) Acute heart failure: Clinical presentation, one-year mortality and prognostic factors Alain Rudiger a, T,1, Veli-Pekka Harjola b,1, Andreas Mqller a, Eero Mattila b, Petrus S7ila b, Markku Nieminen b, Ferenc Follath a a Department of Medicine, University Hospital Zürich, Switzerland b Department of Medicine, Helsinki University Central Hospital, Finland Received 9 August 2004; received in revised form 25 November 2004; accepted 27 January 2005 Abstract Aims: Acute heart failure (HF) is a common but ill-defined clinical entity. We describe patients hospitalised with acute HF in regard of clinical presentation, mortality, and risk factors for an unfavourable outcome. Methods and results: We conducted a prospective study including 312 consecutive patients from two European centers hospitalised with acute HF, defined as new onset or worsening of symptoms and signs of HF within 7 days. The mean age was 73 years and 56% were men. Twenty-eight percent had de-novo acute HF and 72% a decompensation of chronic HF. Coronary heart disease (CHD) was the most frequent underlying heart disease, elevated blood pressure N150 mmhg and acute ischemia being the most important triggers. Four percent of the patients had cardiogenic shock, 13% presented with pulmonary edema. LV-EF was b35%, 35 50% and N50% in 35%, 32% and 33% of the patients, respectively. ICU-treatment was necessary in 39% of the patients. Thirty-day mortality (11%) was increased in the presence of shock or elevated troponin T levels. Twelve-month all-cause mortality (29%) increased in the presence of shock, left ventricular dysfunction, renal insufficiency, CHD, and age. Conclusions: This prospective study shows that despite modern treatment, morbidity and mortality of patients hospitalised with acute HF remain high. D 2005 European Society of Cardiology. Published by Elsevier B.V. All rights reserved. Keywords: Acute heart failure; Cardiogenic shock; Pulmonary oedema; Mortality 1. Introduction Numerous studies have addressed the problem of chronic heart failure (HF) but acute HF has widely been neglected in the past. However, the number of patients suffering from acute heart failure (HF) is increasing, and the prognosis of acute, decompensated HF seems to be poor with a high inhospital and midterm mortality [1 9]. Only little is known about the long-term prognosis and possible risk factors for a fatal outcome in this population [10]. Furthermore, the lack of a generally accepted definition has led to only poorly * Corresponding author. Present address: Wolfson Institute of Biomedical Research, University College London, The Cruciform Building, Gower Street, London WC 1E 6BT. Tel.: ; fax: address: arudiger99@yahoo.de (A. Rudiger). 1 A. Rudiger and V.-P. Harjola contributed equally to this survey. comparable results. In view of new diagnostic and therapeutic options a reassessment of the problem is required [11,12]. The aim of our prospective observation study was to use the same diagnostic criteria for acute HF in two different European centers, and to describe patients with acute HF with regard to clinical presentation, mortality, and risk factors for an unfavourable outcome. 2. Methods 2.1. Study population We conducted a prospective observational study using an identical evaluation protocol in the University Hospital of Zurich, Switzerland (named as center 1 in the following text ), /$ - see front matter D 2005 European Society of Cardiology. Published by Elsevier B.V. All rights reserved. doi: /j.ejheart
2 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) between December 2001 and September 2002, and in the Helsinki University Central Hospital, Finland (center 2) between September 2002 and February Center 1 operates both as tertiary referral hospital and as primary care facility, and center 2 is a tertiary referral hospital. The reference population for the primary care and tertiary referrals for center 1 is 100,000 and 1.5 million inhabitants, and 1.4 million inhabitants for tertiary care in center 2, respectively Diagnosis of acute heart failure Acute HF was diagnosed in the presence of: 1. an underlying heart disease 2. at least two of the following clinical symptoms or signs: dyspnea NYHA III or IV, orthopnea, rales, elevated jugular venous pressure or systolic blood pressure (BP) below 90 mmhg with decreased end-organ perfusion 3. a characteristic chest X-ray (cardiomegaly, venous congestion and/or pulmonary oedema). Importantly, there had to be a rapid onset or significant worsening of HF symptoms within 7 days before admission. The diagnosis of acute HF was made by the physicians in charge of the patient either at the emergency room, at the medical intensive care unit (ICU), or on the ward. In both hospitals all patients admitted to any of the medical wards, including the ICU, the cardiac care unit, and the cardiology clinic, were screened for these diagnostic criteria. At discharge acute HF had to be listed as one of the major diagnoses. Each patient was enrolled only once, even if he/ she was readmitted during the observation period. Patients were excluded from the survey if they were discharged directly from the emergency room and treated as outpatients. Other causes for exclusion were shortness of breath due to pulmonary disease, pulmonary embolism or primary pulmonary hypertension. The characterisation of the patients included age, gender, pre-existing conditions, symptoms and signs on clinical examination. These data were collected by the study team from the patient charts. The results of the following investigations were assessed if available: blood tests, electrocardiogram (ECG), chest X-ray, echocardiogram, coronary angiography. We also evaluated the underlying cardiac disease and possible triggers of acute HF and followed the hospital course. After 12 months the patients or their general physicians were contacted from center 1. In center 2 survival information was obtained from national mortality registry Case definition Patients included in the study were classified in one of the following three categories according to the modified Killip and Kimball classification [13,14]: Cardiogenic shock: Impaired end-organ perfusion with the clinical signs of cold skin, decreased mental performance or oliguria and a systolic BP below 90 mmhg despite adequate treatment with fluids, or need of inotropes or vasopressors. Pulmonary oedema: Dyspnea at rest, rales over all lung fields and chest X-ray compatible with alveolar pulmonary oedema without cardiogenic shock. Congestive HF: Symptoms and signs of HF exclusive of cardiogenic shock or pulmonary oedema. The study population was subdivided into groups of new acute HF and decompensated chronic HF. New (denovo) acute HF was defined as the first manifestation of HF in patients without any previous episode of HF. Decompensated chronic HF was defined as rapid worsening of HF symptoms and signs in patients with pre-existing chronic HF Statistical analysis All data were collected from the patient charts and entered into a computerised database. Median (range), mean (FSD) or percentage were calculated for the overall sample and subgroups. Comparisons were made with the use of the Mann Whitney U test, t-test, Fisher s exact test, or the chisquare test, as appropriate. Survival estimates for all cause mortality were calculated with the method of Kaplan and Meier. The Log Rank test was used to compare the mortality of subgroups. All analyses were performed with the use of SPSS 11.5 for Windows. p-values below 0.05 were taken as significant and all hypothesis testing was two-tailed. 3. Results 3.1. Patient characteristics During the enrolment period, 96 and 216 consecutive patients with acute HF were included into the survey in centers 1 and 2, respectively. Baseline characteristics of the patients are given in Table 1. Fifty-six percent of the patients were men, and they were significantly younger than women (70F12 vs 77F12 years, p below 0.001). Twenty-eight percent of all patients had de-novo acute HF, whereas 72% had decompensation of chronic HF. Seventy-six percent of all patients were admitted to hospital within 3 days from the onset of symptoms. Co-morbidities were common and are shown in Table 2. Coronary heart disease (CHD), valvular heart disease and dilated cardiomyopathy were the three most common underlying heart diseases. In patients with valvular heart disease mitral regurgitation was the most common valve dysfunction and usually mild to moderate. However, 28 patients presented with severe aortic valve dysfunction, 17 had a history of aortic valve replacement, and 5 patients had a tricuspid valve dysfunction. Elevated systolic BP above 150 mmhg, acute ischemia and new atrial fibrillation were the most important triggers for clinical deterioration. Some
3 664 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) Table 1 Baseline characteristics of patients with acute heart failure on hospital admission All (N=312) Center 1 (N=96) Center 2 (N=216) p-valuet Age MeanFSD (year) 73F12 71F13 74F Patients V 65 years no. (%) 84 (26.9) 34 (35.4) 50 (23.1) Patients N75 years no. (%) 147 (47.1) 42 (43.8) 105 (48.6) Male sex no. (%) 176 (56.4) 58 (60.4) 118 (54.6) Symptoms Dyspnea NYHA III or IV no. (%) 286 (94.1) 92 (97.9) 194 (92.4) Orthopnea no. (%) 224 (71.8) 63 (65.6) 161 (74.5) Chest pain CCS 3 or 4 no. (%) 110 (36.4) 29 (30.2) 81 (39.3) Respiration rate (/min) a median (range) 22.0 (10 45) 20.5 (12 45) 24 (10 44) Blood pressure (mmhg) systolic median (range) 140 (70 230) 130 (70 227) 145 (88 230) b0.001 diastolic median (range) 80 (30 170) 78.5 (30 170) 83 (44 140) Heart rate (/min) median (range) 90 (34 180) 93 (52 180) 89 (34 170) Blood tests Creatinine (Amol/l) b median (range) 93 (37 641) 111 (64 506) 85 (37 641) b0.001 Hemoglobin (g/l) median (range) 126 (43 202) 121 (43 161) 129 (62 202) Troponin T positive (z0.1 Ag/l) no. (%) 88 (30.7) 28 (30.8) 60 (30.6) Chest X-ray no. (%) 312 (100) 96 (100) 216 (100) Alveolar infiltrates no. (%) 43 (14.3) 14 (14.7) 29 (14.1) Interstitial congestion no. (%) 83 (27.6) 32 (33.7) 51 (24.8) Pleural effusions no. (%) 136 (50.7) 52 (55.3) 84 (48.3) ECG no. (%) 311 (99.7) 95 (98.9) 216 (100) STEMI no. (%) 23 (7.3) 7 (7.3) 16 (7.4) ACS (without STEMI) no. (%) 55 (17.6) 17 (17.7) 38 (17.6) Echocardiography no. (%) 226 (72.4) 58 (60.4) 168 (77.8) LV-EF c b35% no. (%) 83 (34.9) 32 (50.8) 51 (29.1) LV-EF c 35 49% no. (%) 76 (31.9) 10 (15.9) 66 (37.7) LV-EF c z50% no. (%) 79 (33.2) 21 (33.3) 58 (33.1) Coronary angiography no. (%) 130 (41.7) 32 (33.3) 98 (45.4) NYHA denotes New York Heart Association class, CCS Canadian Cardiac Society class, ECG electrocardiogram, STEMI ST-elevation myocardial infarction, ACS acute coronary syndrome and LV-EF left ventricular ejection fraction. a Respiration rate was documented only in 117 (37.5%) patients. b 1 mg/dl=88.4 cmol/l. c If no echocardiography was performed then LV-EF was taken, if available, from ventriculography. Data shown are the no. (%) of those who underwent LV- EF measurement. T p-value for the comparison between the two centers. patients had more than one underlying cardiac disorder or more than one possible trigger (Table 3). In 25% of the patients acute ischemia was estimated to be the trigger of acute HF. Within this group of patients 29% of patients had a ST-elevation myocardial infarction (STEMI) and the other 71% had an acute coronary syndrome without ST-elevation. Seventy-six percent of the patients had a measurement of the left ventricular ejection fraction (LV-EF) by either echocardiography or ventriculography (Fig. 1). Median LV-EF was lower in patients from center 1 compared to patients from center 2 (34 [11 72]% vs 40 [15 80]%, p=0.042). Patients with a systolic BP N150 mmhg on Table 2 Co-morbidities in patients with acute heart failure All (N=312) Center 1 (N=96) Center 2 (N=216) p-valuet History of Atrial fibrillation no. (%) 91 (29.2) 21 (21.9) 70 (32.4) Elevated blood pressure no. (%) 168 (53.8) 51 (53.1) 117 (54.2) Diabetes mellitus no. (%) 100 (32.1) 25 (26.0) 75 (34.7) Cigarette smoking no. (%) 102 (32.7) 44 (45.8) 58 (26.9) Renal insufficiency Cr-Cl b50 ml/min a no. (%) 109 (41) 50 (52.1) 59 (34.7) Anemia Hemoglobin g/l no. (%) 106 (34.6) 35 (36.5) 71 (33.8) Hemoglobin b100 g/l no. (%) 23 (7.5) 12 (12.5) 11 (5.2) a Cr-Cl denotes creatinine clearance, which was estimated according to the modified Cockcroft and Gault formula [37]. T p-value for the comparison between the two centers.
4 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) Table 3 Underlying heart disease and possible triggers of acute heart failure All (N=312) Center 1 (N=96) Center 2 (N=216) p-valuet Underlying heart disease CHD no. (%) 193 (61.9) 57 (59.4) 136 (63.0) Valvular cardiopathy no. (%) 61 (24.4) 24 (25.5) 37 (23.7) Dilated cardiomyopathy no. (%) 19 (6.1) 2 (2.1) 17 (7.9) Hypertrophic cardiomyopathy no. (%) 4 (1.3) 2 (2.1) 2 (0.9) Myocarditis no. (%) 4 (1.3) 3 (3.1) 1 (0.5) Endocarditis no. (%) 2 (0.6) 1 (1.0) 1 (0.5) Alcoholic cardiopathy no. (%) 2 (0.6) 1 (1.0) 1 (0.5) Pericardial effusion no. (%) 6 (1.9) 5 (5.2) 1 (0.5) HTPL no. (%) 2 (0.6) 2 (2.1) 0 (0) Others no. (%) 21 (6.7) 3 (3.1) 18 (8.3) Trigger Acute ischemia no. (%) 78 (25.0) 24 (25.0) 54 (25.0) 1.0 SBP adm =150 mmhg no. (%) 111 (35.7) 19 (19.8) 92 (42.8) b0.001 SBP adm =180 mmhg no. (%) 37 (11.9) 7 (7.3) 30 (14) New AF no. (%) 47 (15.1) 18 (18.8) 29 (13.4) Symptomatic bradycardia no. (%) 22 (7.1) 3 (3.1) 19 (8.8) Severe valve dysfunction a no. (%) - 15 (15.6) - - CHD denotes coronary heart disease, HTPL heart transplantation, SBP adm systolic blood pressure on admission and AF atrial fibrillation. a Was not assessed in center 2. T p-value for the comparison between the two centers. admission had a higher LV-EF than patients with a systolic BP below 150 mmhg (43 [20 80]% vs 36 [11 73]%, p=0.004). Similarly, LV-EF was higher in patients with a history of elevated BP compared to patients with no history of elevated BP (42 [11 80]% vs 35 [15 73]%, p=0.002). Patients with renal dysfunction (creatinine clearance [Cr- Cl] below 50 ml/min) were older (79F11 vs 69F12, p below 0.001) and had a lower hemoglobin level (117 [58 165]g/l vs 136 [43 180]g/l, p below 0.001) than patients with normal renal function. Patients with diabetes had a higher creatinine level on admission (104 [48 641]Amol/l vs 89 [37 506]Amol/l, p=0.006) than non-diabetics Clinical presentation of acute HF The clinical presentations differed remarkably little between the two centers. Congestive HF with clinical EF >=50% 25.3% no LV-EF 23.7% and radiological signs of decompensation was the predominant presentation of acute HF and occurred in 75 (78%) and 183 (85%) patients from center 1 and center 2, respectively. Pulmonary oedema was diagnosed in 13 (14%) and 28 (13%) patients from center 1 and center 2, respectively. Cardiogenic shock was present in 8 (8.3%) patients from center 1, whereas cardiogenic shock was found in only 5 (2.3%) patients from center 2. Patients with cardiogenic shock had higher troponin levels (0.28 [0 48.3]Ag/l vs 0.03 [0 7.95]Ag/l, p=0.001), higher creatinine levels (115 ([72 436]Amol/l vs 92 [37 641]Amol/l, p=0.04) and a lower LV-EF (27 [11 55]% vs 40 [15 80]%, p=0.005). When patients with shock were excluded from the analysis the following differences between patients with pulmonary oedema and congestive HF were obvious: Patients with pulmonary oedema more often had a history of elevated BP (78% vs 52%, p=0.002) and a trend to higher systolic BP on admission (150 [99 227] mmhg vs 140 [70 230] mmhg, p=0.053). On the other hand patients with congestive HF had higher creatinine levels (109 [44 369]Amol/l vs 90 [37 64]Amol/l, p=0.017) Hospital course EF 35-49% 24.4% EF <35% 26.6% Fig. 1. Distribution of left ventricular ejection fractions (LV-EF) in patients with acute heart failure. ICU-admission was required in 39% of all patients. The median length of ICU stay was 3 days in both centers (range 1 66 and 1 16 for center 1 and 2, respectively). Total length of stay was 11.5 (2 77) days and 8 (1 50) days in center 1 and 2, respectively ( pb0.001). Eight percent of the patients died during the initial hospitalisation, 61% of the patients were discharged home, and 31% of the patients were
5 666 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) Survival Congestive HF (N=258) Pulmonary oedema (N=41) Follow up (days) Cardiogenic shock (N=13) Fig. 2. Kaplan Meier curves for three groups of patients with different presentation of acute heart failure (N=312, Log Rank 0.002). transferred to another hospital or to another department (e.g. cardiac surgery) Follow up The all-cause mortality at 30 days, 12 weeks, and 1 year was 11%, 18%, and 29%, respectively (2 patients from center 1 were lost for 12-month follow up). Thirtyday mortality was influenced by the clinical presentation on admission and was 46% in patients with cardiogenic shock, 9.8% in patients with pulmonary oedema and 8.9% in patients with congestive HF ( p=0.001 shock vs noshock, p=0.774 pulmonary oedema vs congestive HF). Thirty-day mortality was higher in patients with an elevated (z0.1ag/l) troponin T level (21% vs 7.0%; p=0.002). On the other hand, patients with a history of high BP had a lower 30-day mortality than the ones without a history of hypertension (6.5% vs 15%; p=0.016). There was a trend to a higher 30-day mortality in patients requiring ICU-treatment (14% vs 8.4%, p=0.132). One-year survival tended to be better in center 2 with an one-year mortality of 26% vs 37% in center 1 ( p=0.081). Cardiogenic shock (more frequent in center 1) was associated with a substantial all-cause mortality rate of 62% at 12 months, resulting in an odds ratio of 4.1 (95% confidence interval [CI] ). Other risk factors for increased one-year mortality were impaired left ventricular systolic function, renal insufficiency, the presence of CHD, and older age (Figs. 2 5). Odds ratios (95% CI) for LV- EFb35%, Cr-Cl b50 ml/min, the presence of CHD, and age N75years were 2.6 ( ), 2.5 ( ), 1.7 ( ) and 1.7 ( ), respectively. Renal insufficiency and impaired LV-EF remained risk factors for death when patients with cardiogenic shock were excluded from the analysis. No significant differences in one-year survival were found with respect to gender, presence of pulmonary oedema, history of HF, history of elevated BP, underlying Survival.8.7 LV-EF >50% (N=83) LV-EF 35-50% (N=76).6 LV-EF <35% (N=79) Follow up (days) Fig. 3. Kaplan Meier curves for three groups of patients acute heart failure and different left ventricular ejection fractions (N=238, Log Rank 0.001).
6 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) Survival.8.7 Creatinineclearance > _ 50ml/min (N=157).6 Creatinineclearance < 50ml/min (N=109) Follow up (days) Fig. 4. Kaplan Meier curves for two groups of patients with acute heart failure and different renal functions (N=266, Log Rank 0.001). CHD, myocardial ischemia, positive troponin level on admission, diabetes, low hemoglobin level on admission or ICU-treatment. 4. Discussion Acute HF can be diagnosed in the presence of an underlying heart disease and the appearance of typical symptoms and signs within 7 days. By using this simple clinical definition, we performed a prospective survey in two European centers. Therewith important insights on presentation, outcome and risk factors for increased short and long-term mortality of patients hospitalised with acute HF have been obtained Clinical presentation of acute HF In the present study 4% of the patients had cardiogenic shock, 13% suffered from pulmonary oedema, and the majority presented with congestive HF severe enough to require hospital admission. Nearly one third had a de-novo acute HF, whereas two thirds had a decompensation of chronic HF. CHD was the leading underlying disease and was present in more than half the patients. The next common etiologies were valvular heart disease and dilated cardiomyopathy. Other underlying cardiopathies, like myocarditis or alcoholic cardiopathy, were rare findings. Elevated BP N150 mmhg, acute myocardial ischemia, atrial fibrillation and severe valve dysfunction were the most frequent factors associated with acute HF in our study. In Presentation: shock vs no shock ( 13/299) LV-EF: <50% vs >_ 50% (159/ 79) LV-EF: <35% vs >_ 35% ( 83/155) Cr-Cl <50ml/min vs Cr-Cl >_ 50ml/min (109/157) Age: >65yrs vs _ < 65yrs (228/ 84) CHD vs no CHD (193/119) Age: >75yrs vs _< 75yrs (147/165) Site: center 1 vs center 2 ( 96/216) Troponin >_ 0.1ug/l vs <0.1ug/l ( 88/199) Diabetes vs no diabetes (100/212) History of HF vs no history of HF (224/ 88) Gender: men vs women (176/136) History of elevated BP vs no hypertension (168/144) Fig. 5. Odds ratios for different risk factors influencing one-year mortality of patients with acute heart failure. The numbers in brackets indicate the number of patients in each group. LV-EF denotes left ventricular ejection fraction, Cr-Cl creatinine clearance, CHD coronary heart disease, HF heart failure and BP blood pressure.
7 668 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) contrast, acute ischemia, new atrial fibrillation and correctable valve disorders are often exclusion criteria in randomised controlled trials investigating new drugs for acute HF [15 18]. In the previous literature, the term acute has been used quite imprecisely and interpreted differently by investigators. Thus, we limited our study population to those with a time span of 7 days or less between the onset or worsening of HF symptoms and admission. More than two thirds of our patients were admitted to hospital within 72 h. About a fourth of our population had a LV-EF b35%, a frequent inclusion criterion in chronic HF trials [19]. Thus, the clinical trials have to be interpreted with respect to their often restricted selection of patients which would exclude the majority of acute HF patients. However, a quarter of all patients presented with a preserved LV systolic function ( LV-EF z50%), which corresponds to previous reports [20 22] Outcome and risk factors The prognostic significance of elevated troponin levels was confirmed in our study, as in a wide variety of studies, especially regarding acute coronary syndrome [23 25]. Interestingly, 30-days survival was improved if the patient had a history of elevated BP. This may be explained by the higher LV-EF in patients with hypertension, an assumption that is supported by recent observations from the EuroHeart Failure Survey [26]. Another explanation might be the use of cardioprotective antihypertensive drugs like ACE-inhibitors or beta blockers in this patient group. However, treatments were not evaluated in this study and further investigations are needed to prove this hypothesis. Twelve-months all-cause mortality was increased by older age, impaired systolic left ventricular function and renal insufficiency. Moreover, the hemodynamic status on admission was the most important risk factor for mortality. Cardiogenic shock was associated with a substantial mortality. The 30-days and 12-month mortality of 46% and 62% in our study are only partly comparable with the ones published in the SHOCK trial which investigated patients with cardiogenic shock as a complication of myocardial infarction [27,28]. In both the control group and the intervention group with early revascularisation, mortality rates were high in SHOCK trial with 56% and 47% after 30 days and 76% and 53% after 1 year, respectively. In contrast to patients with shock, the short- and long-term outcome for hemodynamically stable patients were similar whether the patients had severe congestive HF or pulmonary oedema. This stands in contrast to data on patients with acute coronary syndromes and may be a result of the limited number of patients in our study [29]. Our high all-cause mortality rate at 12 months is comparable to the findings of a study including 150 patients with HF defined by the presence of rales and/or pulmonary vascular congestion on the chest X-ray [30]. In that single center study a mortality rate of 40% after 1 year was reported, and the presence of shock and a depressed LV-EF were negative predictors of in-hospital mortality but did, in contrast to our study, not influence one-year mortality Differences between the study centers In the past, the lack of a uniform definition of acute HF had led to only poorly comparable results. Using identical inclusion criteria, we found very similar and comparable findings in the two study centers. Nevertheless, few differences were present. Cardiogenic shock was more common in center 1, which can be explained by different admission policies between the two centers. Additionally, renal dysfunction was more common in center 1. On the other hand, patients from center 2 had higher BP on admission and better LV-EF. Together, these findings probably explain the longer hospital stay and the trend to a higher 12-month mortality in center Limitations of the study Some of the key clinical signs, that is, respiratory rate, examination of the jugular venous pressure and auscultation findings (third heart sound, rales) were not systematically documented by the physicians in charge of the patients. Some of this inconsistency of data most likely reflects that normal findings were not recorded. The incompleteness of routine medical records and patient charts at least partially illustrates that physicians probably underscore the importance of clinical signs for making the diagnosis and guiding the treatment of heart failure [31,32]. This lack of systematic evaluation of symptoms and signs at baseline is a limitation of our observational study, which, however, reflects real-life practice of performing clinical examination and writing medical reports. Hemodynamic monitoring with right heart catheterisation was performed only when indicated but the results were not collected for this study. B-type natriuretic peptide levels were not measured at the time of the study Comparison with acute HF trials and registries It is often questioned whether randomised clinical trials represent real-life patient populations well enough. With respect to acute HF, this question has largely been unanswered. Thus, we compared the demographic findings of our study with OPTIME, VMAC and LIDO, three recent studies investigating milrinone, nesiritide and levosimendan, respectively, in patients with acute HF [33 35]. In all three studies, patients were explicitly younger and less women were included. All trials excluded patients with, among others, ongoing myocardial ischemia, uncontrolled atrial fibrillation, corrigible valve disorders or severe renal insufficiency. Therefore itts not surprising that mortality was lower in all three trials, both in the treatment groups, as well as, in the control groups.
8 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) In the EuroHeart failure survey, 11,327 hospitalised patients with diagnosed or suspected acute or chronic HF were investigated in Europe. In comparison to that study, a similar distribution of age and gender was observed in our series. Furthermore, the prevalence of CHD and valvular heart disease, as well as important co-morbidities like diabetes, hypertension and atrial fibrillation were comparable [36]. Nevertheless, 12-week mortality was higher in our study than in the EuroHeart failure survey, i.e. 18% and 14%, respectively. This difference might have occurred by chance only. But importantly, patients with stable HF and even only suspicion of HF were included in EuroHeart failure survey which understandably may result in a lower mortality. Only recently, guidelines for the diagnosis and classification of acute HF have been elaborated by the European Society of Cardiology and will be published later this year. These instructions will allow a uniform patient categorisation in upcoming epidemiological surveys and clinical trials. In conclusion, this realistic assessment of acute HF in two large European hospitals with both central and regional function describes epidemiology, clinical presentation, short- and long-term outcome, and risk factors for increased mortality. These information allow a risk assessment of patients hospitalised with acute HF, and may serve as basis for future trials investigating new therapeutic options. References [1] McMurray J, McDonagh T, Morrison CE, Dargie HJ. Trends in hospitalization for heart failure in Scotland Eur Heart J 1993;14: [2] Cowie MR, Mosterd A, Wood DA, et al. The epidemiology of heart failure. Eur Heart J 1997;18: [3] Cowie MR, Wood DA, Coats AJ, et al. Incidence and aetiology of heart failure: a population-based study. Eur Heart J 1999;20: [4] Brophy JM, Deslauriers G, Boucher B, Rouleau JL. The hospital course and short term prognosis of patients presenting to the emergency room with decompensated congestive heart failure. Can J Cardiol 1993;9: [5] Haldeman GA, Croft JB, Giles WH, Rashidee A. Hospitalization of patients with heart failure: National Hospital Discharge Survey, Am Heart J 1999;137: [6] Jaagosild P, Dawson NV, Thomas C, et al. Outcomes of acute exacerbation of severe congestive heart failure. Arch Intern Med 1998;158: [7] Rame JE, Sheffield MA, Dries DL, et al. Outcome after emergency department discharge with primary diagnosis of heart failure. Am Heart J 2001;142: [8] Levy D, Kenchaiah S, Larson MG, et al. Long-term trends in the incidence of and survival with heart failure. N Engl J Med 2002;347: [9] Jessup M, Brozena S. Heart failure. N Engl J Med 2003;348: [10] Brophy JM, Deslauriers G, Rouleau JL. Long term prognosis of patients presenting to the emergency room with decompensated congestive heart failure. Can J Cardiol 1994;10: [11] Cotter G, Moshkovitz Y, Milovanov O, et al. Acute heart failure: a novel approach to its pathogenesis and treatment. Eur J Heart Fail 2002;4: [12] Felker GM, Adams KF, Konstam MA, O Connor CM, Gheorghiade M. The problem of decompensated heart failure: nomenclature, classification, and risk stratification. Am Heart J 2003;145:S [13] Killip T, Kimball JT. Treatment of myocardial infarction in a coronary care unit: a two year experience with 250 patients. Am J Cardiol 1967;20: [14] Killip T, Kimball JT. A survey of the coronary care unit: concept and results. Prog Cardiovasc Dis 1968;11: [15] Colucci WS, Elkayam U, Horton DP, et al. Intravenous nesiritide, a natriuretic peptide, in the treatment of decompensated congestive heart failure. N Engl J Med 2000;343: [16] Silver MA, Horton DP, Ghali JK, Elkayam U. Effect of nesiritide versus dobutamine on short-term outcomes in the treatment of patients with acutely decompensated heart failure. J Am Coll Cardiol 2002;39: [17] Slawsky MT, Colucci WS, Gottlieb SS, et al. Acute hemodynamic and clinical effects of levosimendan in patients with severe heart failure. Circulation 2000;102: [18] Moiseyev VS, Põder P, Andrejevs N, et al. Safety and efficacy of a novel calcium sensitizer, levosimendan, in patients with left ventricular failure due to an acute myocardial infarction. Eur Heart J 2002;23: [19] Yusuf S, SOLVD investigators. Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med 1991;325: [20] Vasan RS, Benjamin EJ, Levy D. Prevalence, clinical features and prognosis of diastolic heart failure: an epidemiologic perspective. J Am Coll Cardiol 1995;26: [21] Gandhi SK, Powers JC, Nomeir A-M, et al. The pathogenesis of acute pulmonary edema associated with hypertension. N Engl J Med 2001;344: [22] Van Kraaij DJW, van Pol PE, Ruiters AW, et al. Diagnosing diastolic heart failure. Eur J Heart Fail 2002;4: [23] Heidenreich PA, Alloggiamento T, Melsop K, et al. The prognostic value of troponin in patients with non-st-elevation acute coronary syndromes: a meta analysis. J Am Coll Cardiol 2001;38: [24] Ammann P, Maggiorini M, Bertel O, et al. Troponin as a risk factor for mortality in critically ill patients without acute coronary syndromes. J Am Coll Cardiol 2003;41: [25] Steg PG, Dabbous OH, Feldman LJ, et al. Determinants and prognostic impact of heart failure complicating acute coronary syndromes. Circulation 2004;109: [26] Lenzen MJ, Scholte op Reimer WJ, Boersma E, et al. Differences between patients with a preserved and a depressed left ventricular function: a report from the EuroHeart Failure Survey. Eur Heart J 2004;25: [27] Hochman JS, Sleeper LA, Webb JG, et al. Early revascularisation in acute myocardial infarction complicated by cardiogenic shock. N Engl J Med 1999;341: [28] Menon V, Hochman JS. Management of cardiogenic shock complicating acute myocardial infarction. Heart 2002;88: [29] Khot UN, Jia G, Moliterno DJ, et al. Prognostic importance of physical examination for heart failure in non-st-elevation acute coronary syndromes. JAMA 2003;290: [30] Roguin A, Behar D, Ben Ami H, et al. Long-term prognosis of acute pulmonary oedema an ominous outcome. Eur J Heart Fail 2000;2: [31] Stevenson LW, Perloff JK. The limited reliability of physical signs for estimating hemodynamics in chronic heart failure. JAMA 1989;261: [32] Drazner MH, Rame JE, Phil M, Stevenson LW, Dries AL. Prognostic importance of elevated jugular venous pressure and a third heart sound in patients with heart failure. N Engl J Med 2001: [33] Cuffe MS, Califf RM, Adams KF, et al. Short-term intravenous milrinone for acute exacerbation of chronic heart failure. JAMA 2002:
9 670 A. Rudiger et al. / The European Journal of Heart Failure 7 (2005) [34] Young JB, VMAC investigators. Intravenous nesiritide vs nitroglycerin for treatment of decompensated congestive heart failure. JAMA 2002;287: [35] Follath F, Cleland JG, Papp JG, et al. Efficacy and safety of intravenous levosimendan compared with dobutamine in severe lowoutput failure (the LIDO-study): a randomised double-blind trial. Lancet 2002;360: [36] Cleland JG, Swedberg K, Follath F, et al. The EuroHeart failure survey programme a survey on the quality of care among patients with heart failure in Europe. Eur Heart J 2003;24: [37] Cockcroft DW, Gault MH. Prediction of creatinine clearance from serum creatinine. Nephron 1976;16:31 41.
Considerations on the efficacy and safety of levosimendan in ischemic heart failure
 Considerations on the efficacy and safety of levosimendan in ischemic heart failure Markku S. Nieminen, Esa-Pekka Sandell Division of Cardiology, University Central Hospital, Helsinki, Finland Key words:
Considerations on the efficacy and safety of levosimendan in ischemic heart failure Markku S. Nieminen, Esa-Pekka Sandell Division of Cardiology, University Central Hospital, Helsinki, Finland Key words:
Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year
![Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year](/thumbs/76/74263761.jpg) PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
ESC Guidelines for the Diagnosis and Treatment of Acute and Chronic Heart Failure
 Patients t with acute heart failure frequently develop chronic heart failure Patients with chronic heart failure frequently decompensate acutely ESC Guidelines for the Diagnosis and A clinical response
Patients t with acute heart failure frequently develop chronic heart failure Patients with chronic heart failure frequently decompensate acutely ESC Guidelines for the Diagnosis and A clinical response
Diagnosis & Management of Heart Failure. Abena A. Osei-Wusu, M.D. Medical Fiesta
 Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Cardiogenic Shock. Carlos Cafri,, MD
 Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
ACUTE HEART FAILURE. Julie Gorchynski MD, MSc, FACEP, FAAEM. Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014
 ACUTE HEART FAILURE Julie Gorchynski MD, MSc, FACEP, FAAEM Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014 No disclosures Objectives Overview Cases Current Therapy
ACUTE HEART FAILURE Julie Gorchynski MD, MSc, FACEP, FAAEM Department of Emergency Medicine Emergency Residency Program UTHSC, San Antonio TCEP 2014 No disclosures Objectives Overview Cases Current Therapy
Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes?
 Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor
Keynote Address II Managing Acute Heart Failure: What Can We Do to Improve Outcomes? 24 th Annual San Diego Heart Failure Symposium June 1-2, 2018 La Jolla, CA Barry Greenberg, MD Distinguished Professor
Value of echocardiography in chronic dyspnea
 Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Value of echocardiography in chronic dyspnea Jahrestagung Schweizerische Gesellschaft für /Schweizerische Gesellschaft für Pneumologie B. Kaufmann 16.06.2016 Chronic dyspnea Shortness of breath lasting
Heart failure (HF) is a complex clinical syndrome that results in the. impairment of the heart s ability to fill or to pump out blood.
 Introduction: Heart failure (HF) is a complex clinical syndrome that results in the impairment of the heart s ability to fill or to pump out blood. As of 2013, an estimated 5.8 million people in the United
Introduction: Heart failure (HF) is a complex clinical syndrome that results in the impairment of the heart s ability to fill or to pump out blood. As of 2013, an estimated 5.8 million people in the United
HFpEF. April 26, 2018
 HFpEF April 26, 2018 (J Am Coll Cardiol 2017;70:2476 86) HFpEF 50% or more (40-71%) of patients with CHF have preserved LV systolic function. HFpEF is an increasingly frequent hospital discharge. Outcomes
HFpEF April 26, 2018 (J Am Coll Cardiol 2017;70:2476 86) HFpEF 50% or more (40-71%) of patients with CHF have preserved LV systolic function. HFpEF is an increasingly frequent hospital discharge. Outcomes
A Study Conducted At A Tertiary Care Teaching Institute in Chennai, on The Clinical And Etiological Profile Of Patients With Acute Heart Failure.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 12 Ver. VIII (Dec. 2017), PP 27-33 www.iosrjournals.org A Study Conducted At A Tertiary Care
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 12 Ver. VIII (Dec. 2017), PP 27-33 www.iosrjournals.org A Study Conducted At A Tertiary Care
Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT
 Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT Key Messages Heart Failure is Common Heart failure is complex Heart Failure is a major issue for the NHS Heart Failure has a worse prognosis
Charles Spencer MD, FRCP Consultant Cardiologist Mid Staffs NHSFT Key Messages Heart Failure is Common Heart failure is complex Heart Failure is a major issue for the NHS Heart Failure has a worse prognosis
Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment
 ESC 2012 27Aug - 3Sep, 2012, Munich, Germany Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment Marco Metra, MD, FESC Cardiology University
ESC 2012 27Aug - 3Sep, 2012, Munich, Germany Treating the patient with acute heart failure. What do we really know? Principles of acute heart failure treatment Marco Metra, MD, FESC Cardiology University
Heart Failure A Disease for the Internist?
 Heart Failure A Disease for the Internist? Dr Chris Davidson Sussex Cardiac Centre BRIGHTON UK Hot Topics in Heart Failure Drug treatments Valsartan / neprilysin inhib Investigations BNP and others Devices
Heart Failure A Disease for the Internist? Dr Chris Davidson Sussex Cardiac Centre BRIGHTON UK Hot Topics in Heart Failure Drug treatments Valsartan / neprilysin inhib Investigations BNP and others Devices
Heart Failure. Cardiac Anatomy. Functions of the Heart. Cardiac Cycle/Hemodynamics. Determinants of Cardiac Output. Cardiac Output
 Cardiac Anatomy Heart Failure Professor Qing ZHANG Department of Cardiology, West China Hospital www.blaufuss.org Cardiac Cycle/Hemodynamics Functions of the Heart Essential functions of the heart to cover
Cardiac Anatomy Heart Failure Professor Qing ZHANG Department of Cardiology, West China Hospital www.blaufuss.org Cardiac Cycle/Hemodynamics Functions of the Heart Essential functions of the heart to cover
Topic Page: congestive heart failure
 Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
Topic Page: congestive heart failure Definition: congestive heart f ailure from Merriam-Webster's Collegiate(R) Dictionary (1930) : heart failure in which the heart is unable to maintain an adequate circulation
Heart Failure Guidelines For your Daily Practice
 Heart Failure Guidelines For your Daily Practice Juan M. Aranda, Jr., MD, FACC, FHFSA Professor of Medicine Director of Heart Failure and Cardiac Transplantation University of Florida College of Medicine
Heart Failure Guidelines For your Daily Practice Juan M. Aranda, Jr., MD, FACC, FHFSA Professor of Medicine Director of Heart Failure and Cardiac Transplantation University of Florida College of Medicine
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
Οξεία Καρδιακή Ανεπάρκεια: Κλινική εικόνα, ταξινόμηση κινδύνου & προγνωστικοί δείκτες
 Οξεία Καρδιακή Ανεπάρκεια: Κλινική εικόνα, ταξινόμηση κινδύνου & προγνωστικοί δείκτες Στράτος Θεοφιλογιαννάκος, MD, PhD Ιατρείο Καρδιακής Ανεπάρκειας, Γ Πανεπιστημιακή Καρδιολογική Κλινική ΑΠΘ, ΠΓΝ Ιπποκράτειο
Οξεία Καρδιακή Ανεπάρκεια: Κλινική εικόνα, ταξινόμηση κινδύνου & προγνωστικοί δείκτες Στράτος Θεοφιλογιαννάκος, MD, PhD Ιατρείο Καρδιακής Ανεπάρκειας, Γ Πανεπιστημιακή Καρδιολογική Κλινική ΑΠΘ, ΠΓΝ Ιπποκράτειο
Οξεία καρδιακή ανεπάρκεια: Ποιες παράμετροι συμβάλλουν στη διαστρωμάτωση κινδύνου των ασθενών;
 Οξεία καρδιακή ανεπάρκεια: Ποιες παράμετροι συμβάλλουν στη διαστρωμάτωση κινδύνου των ασθενών; Γ. Φιλιππάτος, MD, FACC, FESC, FCCP Επ. Καθηγητής Καρδιολογίας Πανεπ. Αθηνών Clinical Outcomes in Patients
Οξεία καρδιακή ανεπάρκεια: Ποιες παράμετροι συμβάλλουν στη διαστρωμάτωση κινδύνου των ασθενών; Γ. Φιλιππάτος, MD, FACC, FESC, FCCP Επ. Καθηγητής Καρδιολογίας Πανεπ. Αθηνών Clinical Outcomes in Patients
Heart Failure in Women: Dr Goh Ping Ping Cardiologist Asian Heart & Vascular Centre
 Heart Failure in Women: More than EF? Dr Goh Ping Ping Cardiologist Asian Heart & Vascular Centre Overview Review pathophysiology as it relates to diagnosis and management Rational approach to workup:
Heart Failure in Women: More than EF? Dr Goh Ping Ping Cardiologist Asian Heart & Vascular Centre Overview Review pathophysiology as it relates to diagnosis and management Rational approach to workup:
AF in the ER: Common Scenarios CASE 1. Fast facts. Diagnosis. Management
 AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
Intravenous Inotropic Support an Overview
 Intravenous Inotropic Support an Overview Shaul Atar, MD Western Galilee Medical Center, Nahariya Affiliated with the Faculty of Medicine of the Galilee, Safed, Israel INOTROPES in Acute HF (not vasopressors)
Intravenous Inotropic Support an Overview Shaul Atar, MD Western Galilee Medical Center, Nahariya Affiliated with the Faculty of Medicine of the Galilee, Safed, Israel INOTROPES in Acute HF (not vasopressors)
IN-HF on line: patient settings (Enrollement period= )
 IN-HF on line: atient settings (Enrollement eriod= 1995-2018) N of centers (total) 187 N of centers (ts. AHF only) 13 N of centers (ts. CHF only) 71 N of centers (both ts. AHF and CHF) 103 N of atients
IN-HF on line: atient settings (Enrollement eriod= 1995-2018) N of centers (total) 187 N of centers (ts. AHF only) 13 N of centers (ts. CHF only) 71 N of centers (both ts. AHF and CHF) 103 N of atients
Reassessing treatment of acute heart failure syndromes: the ADHERE Registry
 European Heart Journal Supplements (2005) 7 (Supplement B), B13 B19 doi:10.1093/eurheartj/sui008 Reassessing treatment of acute heart failure syndromes: the ADHERE Registry Mihai Gheorghiade 1 * and Gerasimos
European Heart Journal Supplements (2005) 7 (Supplement B), B13 B19 doi:10.1093/eurheartj/sui008 Reassessing treatment of acute heart failure syndromes: the ADHERE Registry Mihai Gheorghiade 1 * and Gerasimos
Identification of patients with heart failure and PREserved systolic Function : an Epidemiologic Regional study
 Identification of patients with heart failure and PREserved systolic Function : an Epidemiologic Regional study Dr. Antonio Magaña M.D. (on behalf I-PREFER investigators group) Stockholm, Sweden, August
Identification of patients with heart failure and PREserved systolic Function : an Epidemiologic Regional study Dr. Antonio Magaña M.D. (on behalf I-PREFER investigators group) Stockholm, Sweden, August
Heart Failure with Preserved EF (HFPEF) Epidemiology and management
 Heart Failure with Preserved EF (HFPEF) Epidemiology and management Karl Swedberg Senior Professor of Medicine Sahlgrenska Academy University of Gothenburg Gothenburg, Sweden e-mail: karl.swedberg@gu.se
Heart Failure with Preserved EF (HFPEF) Epidemiology and management Karl Swedberg Senior Professor of Medicine Sahlgrenska Academy University of Gothenburg Gothenburg, Sweden e-mail: karl.swedberg@gu.se
Heart Failure Dr ahmed almutairi Assistant professor internal medicin dept
 Heart Failure Dr ahmed almutairi Assistant professor internal medicin dept (MBBS)(SBMD) Introduction Epidemiology Pathophysiology diastolic/systolic Risk factors Signs and symptoms Classification of HF
Heart Failure Dr ahmed almutairi Assistant professor internal medicin dept (MBBS)(SBMD) Introduction Epidemiology Pathophysiology diastolic/systolic Risk factors Signs and symptoms Classification of HF
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Acute heart failure syndromes: clinical challenges. Pathophysiology. ESC Congress August. Paris, France. Marco Metra
 ESC Congress 2011 27-31 August. Paris, France. Acute heart failure syndromes: clinical challenges. Pathophysiology Marco Metra Cardiology, Dept. Of experimental and applied medicine. University of Brescia.
ESC Congress 2011 27-31 August. Paris, France. Acute heart failure syndromes: clinical challenges. Pathophysiology Marco Metra Cardiology, Dept. Of experimental and applied medicine. University of Brescia.
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes
 Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
Beta-blockers in Patients with Mid-range Left Ventricular Ejection Fraction after AMI Improved Clinical Outcomes Seung-Jae Joo and other KAMIR-NIH investigators Department of Cardiology, Jeju National
My Patient Needs a Stress Test
 My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
My Patient Needs a Stress Test Amy S. Burhanna,, MD, FACC Coastal Cardiology Cape May Court House, New Jersey Absolute and relative contraindications to exercise testing Absolute Acute myocardial infarction
National Horizon Scanning Centre. Irbesartan (Aprovel) for heart failure with preserved systolic function. August 2008
 Irbesartan (Aprovel) for heart failure with preserved systolic function August 2008 This technology summary is based on information available at the time of research and a limited literature search. It
Irbesartan (Aprovel) for heart failure with preserved systolic function August 2008 This technology summary is based on information available at the time of research and a limited literature search. It
CARDIOGENIC SHOCK. Antonio Pesenti. Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI)
 CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
The right heart: the Cinderella of heart failure
 The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
The right heart: the Cinderella of heart failure Piotr Ponikowski, MD, PhD, FESC Medical University, Centre for Heart Disease Clinical Military Hospital Wroclaw, Poland none Disclosure Look into the Heart
HEART FAILURE IN WOMEN. Marian Limacher, MD Division of Cardiovascular Medicine University of Florida
 HEART FAILURE IN WOMEN Marian Limacher, MD Division of Cardiovascular Medicine University of Florida Outline Epidemiology Clinical Overview Why HF is such a challenge State of the Field Heart Failure Adjudication
HEART FAILURE IN WOMEN Marian Limacher, MD Division of Cardiovascular Medicine University of Florida Outline Epidemiology Clinical Overview Why HF is such a challenge State of the Field Heart Failure Adjudication
Tips & tricks on how to treat an acute heart failure patient with low cardiac output and diuretic resistance
 Tips & tricks on how to treat an acute heart failure patient with low cardiac output and diuretic resistance J. Parissis Attikon University Hospital, Athens, Greece Disclosures ALARM investigator received
Tips & tricks on how to treat an acute heart failure patient with low cardiac output and diuretic resistance J. Parissis Attikon University Hospital, Athens, Greece Disclosures ALARM investigator received
Diagnosis is it really Heart Failure?
 ESC Congress Munich - 25-29 August 2012 Heart Failure with Preserved Ejection Fraction From Bench to Bedside Diagnosis is it really Heart Failure? Prof. Burkert Pieske Department of Cardiology Med.University
ESC Congress Munich - 25-29 August 2012 Heart Failure with Preserved Ejection Fraction From Bench to Bedside Diagnosis is it really Heart Failure? Prof. Burkert Pieske Department of Cardiology Med.University
Heart Failure Background, recognition, diagnosis and management
 Heart Failure Background, recognition, diagnosis and management Speaker bureau: Novartis At the conclusion of this activity, participants will be able to: Recognize signs and symptoms of heart failure
Heart Failure Background, recognition, diagnosis and management Speaker bureau: Novartis At the conclusion of this activity, participants will be able to: Recognize signs and symptoms of heart failure
Heart Failure A Team Approach Background, recognition, diagnosis and management
 Heart Failure A Team Approach Background, recognition, diagnosis and management Speaker bureau: Novartis At the conclusion of this activity, participants will be able to: Recognize signs and symptoms of
Heart Failure A Team Approach Background, recognition, diagnosis and management Speaker bureau: Novartis At the conclusion of this activity, participants will be able to: Recognize signs and symptoms of
Nora Goldschlager, M.D. SFGH Division of Cardiology UCSF
 CLASSIFICATION OF HEART FAILURE Nora Goldschlager, M.D. SFGH Division of Cardiology UCSF DISCLOSURES: NONE CLASSIFICATION C OF HEART FAILURE NYHA I IV New paradigm Stage A: Pts at high risk of developing
CLASSIFICATION OF HEART FAILURE Nora Goldschlager, M.D. SFGH Division of Cardiology UCSF DISCLOSURES: NONE CLASSIFICATION C OF HEART FAILURE NYHA I IV New paradigm Stage A: Pts at high risk of developing
LCZ696 A First-in-Class Angiotensin Receptor Neprilysin Inhibitor
 The Angiotensin Receptor Neprilysin Inhibitor LCZ696 in Heart Failure with Preserved Ejection Fraction The Prospective comparison of ARNI with ARB on Management Of heart failure with preserved ejection
The Angiotensin Receptor Neprilysin Inhibitor LCZ696 in Heart Failure with Preserved Ejection Fraction The Prospective comparison of ARNI with ARB on Management Of heart failure with preserved ejection
Acute heart failure syndromes: the Cinderella of heart failure research
 European Heart Journal Supplements (2005) 7 (Supplement B), B8 B12 doi:10.1093/eurheartj/sui007 Acute heart failure syndromes: the Cinderella of heart failure research Faiez Zannad 1,2,3 * 1 INSERM, Centre
European Heart Journal Supplements (2005) 7 (Supplement B), B8 B12 doi:10.1093/eurheartj/sui007 Acute heart failure syndromes: the Cinderella of heart failure research Faiez Zannad 1,2,3 * 1 INSERM, Centre
Trials Enrolled subjects Findings Fox et al. 2014, SIGNIFY 1
 Appendix 5 (as supplied by the authors): Published trials on the effect of ivabradine on outcomes including mortality in patients with different cardiovascular diseases Trials Enrolled subjects Findings
Appendix 5 (as supplied by the authors): Published trials on the effect of ivabradine on outcomes including mortality in patients with different cardiovascular diseases Trials Enrolled subjects Findings
Medical Management of Acute Heart Failure
 Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό
 Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό Diastolic HF DD: Diastolic Dysfunction DHF: Diastolic HF HFpEF: HF with preserved EF DD Pathophysiologic condition: impaired relaxation, LV compliance, LV filling
Μαρία Μπόνου Διευθύντρια ΕΣΥ, ΓΝΑ Λαϊκό Diastolic HF DD: Diastolic Dysfunction DHF: Diastolic HF HFpEF: HF with preserved EF DD Pathophysiologic condition: impaired relaxation, LV compliance, LV filling
Clinical Phenotypes and In-hospital Management and Prognosis in Diabetic versus Non-diabetic Patients with Acute Heart Failure in ALARM-HF Registry
 Clinical Phenotypes and In-hospital Management and Prognosis in Diabetic versus Non-diabetic Patients with Acute Heart Failure in ALARM-HF Registry J T. Parissis, A. Mebazaa, V. Bistola, I. Ikonomidis,
Clinical Phenotypes and In-hospital Management and Prognosis in Diabetic versus Non-diabetic Patients with Acute Heart Failure in ALARM-HF Registry J T. Parissis, A. Mebazaa, V. Bistola, I. Ikonomidis,
Assessment and Diagnosis of Heart Failure
 Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM ID NUMBER: FORM NAME: H F A DATE: 10/01/2015 VERSION: D CONTACT YEAR NUMBER: FORM SEQUENCE NUMBER: General Instructions: The Heart Failure Hospital Record
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM ID NUMBER: FORM NAME: H F A DATE: 10/01/2015 VERSION: D CONTACT YEAR NUMBER: FORM SEQUENCE NUMBER: General Instructions: The Heart Failure Hospital Record
Introduction to Heart Failure. Mauricio Velez, M.D. Transplant Cardiologist APACVS 2018 April 5-7 Miami, FL
 Introduction to Heart Failure Mauricio Velez, M.D. Transplant Cardiologist APACVS 2018 April 5-7 Miami, FL Disclosures No relevant financial relationships to disclose Objectives and Outline Define heart
Introduction to Heart Failure Mauricio Velez, M.D. Transplant Cardiologist APACVS 2018 April 5-7 Miami, FL Disclosures No relevant financial relationships to disclose Objectives and Outline Define heart
Heart Failure. Guillaume Jondeau Hôpital Bichat, Paris, France
 Heart Failure Guillaume Jondeau Hôpital Bichat, Paris, France Epidemiology Importance of PEF Europe I-PREFER study. Abstract: 2835 Prevalence of HF Preserved LV systolic Function older (65 vs 62 y, p
Heart Failure Guillaume Jondeau Hôpital Bichat, Paris, France Epidemiology Importance of PEF Europe I-PREFER study. Abstract: 2835 Prevalence of HF Preserved LV systolic Function older (65 vs 62 y, p
The benefit of treatment with -blockers in heart failure is
 Heart Rate and Cardiac Rhythm Relationships With Bisoprolol Benefit in Chronic Heart Failure in CIBIS II Trial Philippe Lechat, MD, PhD; Jean-Sébastien Hulot, MD; Sylvie Escolano, MD, PhD; Alain Mallet,
Heart Rate and Cardiac Rhythm Relationships With Bisoprolol Benefit in Chronic Heart Failure in CIBIS II Trial Philippe Lechat, MD, PhD; Jean-Sébastien Hulot, MD; Sylvie Escolano, MD, PhD; Alain Mallet,
How to define the target population?
 Heart Failure 2011 22-24 May. Gothenburg, Sweden Mortality or morbidity as target in acute heart failure trials How to define the target population? Marco Metra, Brescia The Burden of Acute HF Acute HF
Heart Failure 2011 22-24 May. Gothenburg, Sweden Mortality or morbidity as target in acute heart failure trials How to define the target population? Marco Metra, Brescia The Burden of Acute HF Acute HF
Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft
 Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft M. Buerke, K. Krohe, M. Russ, C. Schneider, H. Lemm, R. Prondzinsky, I. Friedrich,
Hemodynamic improvement upon levosimendan treatment in low cardiac output patients following coronary artery bypass graft M. Buerke, K. Krohe, M. Russ, C. Schneider, H. Lemm, R. Prondzinsky, I. Friedrich,
Management of Acute Heart Failure
 Management of Acute Heart Failure Uri Elkayam, MD Professor of Medicine University of Southern California School of Medicine Los Angeles, California elkayam@usc.edu ADHF Treatments Goals.2 Improve symptoms.
Management of Acute Heart Failure Uri Elkayam, MD Professor of Medicine University of Southern California School of Medicine Los Angeles, California elkayam@usc.edu ADHF Treatments Goals.2 Improve symptoms.
Cardiovascular Images
 Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Cardiovascular Images Pulmonary Embolism Diagnosed From Right Heart Changes Seen After Exercise Stress Echocardiography Brian C. Case, MD; Micheas Zemedkun, MD; Amarin Sangkharat, MD; Allen J. Taylor,
Evaluation of a diagnostic pathway in heart failure in primary care, using electrocardiography and brain natriuretic peptide guided echocardiography
 Evaluation of a diagnostic pathway in heart failure in primary care, using electrocardiography and brain natriuretic peptide guided echocardiography Rebecka Karlsson Pardeep Jhund 1 Material and methods
Evaluation of a diagnostic pathway in heart failure in primary care, using electrocardiography and brain natriuretic peptide guided echocardiography Rebecka Karlsson Pardeep Jhund 1 Material and methods
Percutaneous Mitral Valve Repair: What Can We Treat and What Should We Treat
 Percutaneous Mitral Valve Repair: What Can We Treat and What Should We Treat Innovative Procedures, Devices & State of the Art Care for Arrhythmias, Heart Failure & Structural Heart Disease October 8-10,
Percutaneous Mitral Valve Repair: What Can We Treat and What Should We Treat Innovative Procedures, Devices & State of the Art Care for Arrhythmias, Heart Failure & Structural Heart Disease October 8-10,
Relationship between cardiac dysfunction, HF and HF rendered asymptomatic
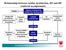 Relationship between cardiac dysfunction, HF and HF rendered asymptomatic NORMAL CARDIAC DYSFUNCTION CORRECTED OR RESOLVED Therapy CAN be withdrawn without recurrence of symptoms Transient Heart Failure
Relationship between cardiac dysfunction, HF and HF rendered asymptomatic NORMAL CARDIAC DYSFUNCTION CORRECTED OR RESOLVED Therapy CAN be withdrawn without recurrence of symptoms Transient Heart Failure
Mortality as an Efficacy or Safety Endpoint : Lessons Learned from the Heart Failure Trials
 Mortality as an Efficacy or Safety Endpoint : Lessons Learned from the Heart Failure Trials Christopher M. O Connor, MD Professor of Medicine Director, Duke Heart Center Acting Chief, Division of Cardiology
Mortality as an Efficacy or Safety Endpoint : Lessons Learned from the Heart Failure Trials Christopher M. O Connor, MD Professor of Medicine Director, Duke Heart Center Acting Chief, Division of Cardiology
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT
 NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
NCAP NATIONAL CARDIAC AUDIT PROGR AMME NATIONAL HEART FAILURE AUDIT 2016/17 SUMMARY REPORT CONTENTS PATIENTS ADMITTED WITH HEART FAILURE...4 Demographics... 4 Trends in Symptoms... 4 Causes and Comorbidities
Objectives. Systolic Heart Failure: Definitions. Heart Failure: Historical Perspective 2/7/2009
 Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
Objectives Diastolic Heart Failure and Indications for Echocardiography in the Asian Population Damon M. Kwan, MD UCSF Asian Heart & Vascular Symposium 02.07.09 Define diastolic heart failure and differentiate
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient
 Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
Left Ventricular Diastolic Dysfunction in South Indian Essential Hypertensive Patient Dr. Peersab.M. Pinjar 1, Dr Praveenkumar Devarbahvi 1 and Dr Vasudeva Murthy.C.R 2, Dr.S.S.Bhat 1, Dr.Jayaraj S G 1
Cardiogenic shock: Current management
 Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Cardiogenic shock: Current management Janine Pöss Universitätsklinikum des Saarlandes Klinik für Innere Medizin III Kardiologie, Angiologie und internistische Intensivmedizin Homburg/Saar I have nothing
Pearls in Acute Heart Failure Management
 Pearls in Acute Heart Failure Management Best Practices Juan M. Aranda Jr., M.D. Professor of Medicine Medical Director of Heart Failure/ Transplant Program University of Florida College of Medicine Disclosures:
Pearls in Acute Heart Failure Management Best Practices Juan M. Aranda Jr., M.D. Professor of Medicine Medical Director of Heart Failure/ Transplant Program University of Florida College of Medicine Disclosures:
State of the Art: acute heart failure Is it just congestion?
 ESC CONGRESS 2017 Barcelona, 26. 30. August 2017 State of the Art: acute heart failure Is it just congestion? S.B. Felix, FESC Klinik für Innere Medizin B Ernst-Moritz-Arndt-Universität Greifswald 1456
ESC CONGRESS 2017 Barcelona, 26. 30. August 2017 State of the Art: acute heart failure Is it just congestion? S.B. Felix, FESC Klinik für Innere Medizin B Ernst-Moritz-Arndt-Universität Greifswald 1456
HEART FAILURE. Study day November 2018 Sarah Briggs
 HEART FAILURE Study day November 2018 Sarah Briggs Overview and Introduction This course is an introduction and overview of heart failure. Normal heart function and basic pathophysiology of heart failure
HEART FAILURE Study day November 2018 Sarah Briggs Overview and Introduction This course is an introduction and overview of heart failure. Normal heart function and basic pathophysiology of heart failure
Disclosure Information : No conflict of interest
 Intravenous nicorandil improves symptoms and left ventricular diastolic function immediately in patients with acute heart failure : a randomized, controlled trial M. Shigekiyo, K. Harada, A. Okada, N.
Intravenous nicorandil improves symptoms and left ventricular diastolic function immediately in patients with acute heart failure : a randomized, controlled trial M. Shigekiyo, K. Harada, A. Okada, N.
Influence of diabetes on the survival of patients hospitalized with heart failure: A 12-year study
 The European Journal of Heart Failure 7 (005) 59 www.elsevier.com/locate/heafai Influence of diabetes on the survival of patients hospitalized with heart failure: A 1-year study Abstract Alfonso Varela-Roman,
The European Journal of Heart Failure 7 (005) 59 www.elsevier.com/locate/heafai Influence of diabetes on the survival of patients hospitalized with heart failure: A 1-year study Abstract Alfonso Varela-Roman,
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency
 Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart failure
 HOT TOPIC Cardiology Journal 2010, Vol. 17, No. 6, pp. 543 548 Copyright 2010 Via Medica ISSN 1897 5593 Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart
HOT TOPIC Cardiology Journal 2010, Vol. 17, No. 6, pp. 543 548 Copyright 2010 Via Medica ISSN 1897 5593 Comparison of clinical trials evaluating cardiac resynchronization therapy in mild to moderate heart
Dobutamine-induced increase in heart rate is blunted by ivabradine treatment in patients with acutely decompensated heart failure
 Dobutamine-induced increase in heart rate is blunted by ivabradine treatment in patients with acutely decompensated heart failure Yuksel Cavusoglu, KU Mert, A Nadir, F Mutlu, E Gencer, T Ulus, A Birdane
Dobutamine-induced increase in heart rate is blunted by ivabradine treatment in patients with acutely decompensated heart failure Yuksel Cavusoglu, KU Mert, A Nadir, F Mutlu, E Gencer, T Ulus, A Birdane
Pivotal Role of Renal Function in Acute Heart failure
 Pivotal Role of Renal Function in Acute Heart failure Doron Aronson MD, FESC Department of Cardiology RAMBAM Health Care Campus Haifa, Israel Classification and definitions of cardiorenal syndromes CRS
Pivotal Role of Renal Function in Acute Heart failure Doron Aronson MD, FESC Department of Cardiology RAMBAM Health Care Campus Haifa, Israel Classification and definitions of cardiorenal syndromes CRS
NT-proBNP: Evidence-based application in primary care
 NT-proBNP: Evidence-based application in primary care Associate Professor Rob Doughty The University of Auckland, Auckland City Hospital, Auckland Heart Group NT-proBNP: Evidence in Primary Care The problem
NT-proBNP: Evidence-based application in primary care Associate Professor Rob Doughty The University of Auckland, Auckland City Hospital, Auckland Heart Group NT-proBNP: Evidence in Primary Care The problem
Copeptin in heart failure: Associations with clinical characteristics and prognosis
 Copeptin in heart failure: Associations with clinical characteristics and prognosis D. Berliner, N. Deubner, W. Fenske, S. Brenner, G. Güder, B. Allolio, R. Jahns, G. Ertl, CE. Angermann, S. Störk for
Copeptin in heart failure: Associations with clinical characteristics and prognosis D. Berliner, N. Deubner, W. Fenske, S. Brenner, G. Güder, B. Allolio, R. Jahns, G. Ertl, CE. Angermann, S. Störk for
Acute heart Failure. Critical cardiac care: update Markku S. Nieminen Helsinki, Finland. M S Nieminen, AHF ,ESC Stockholm
 Acute heart Failure Critical cardiac care: update 2010 Markku S. Nieminen Helsinki, Finland M S Nieminen, AHF 300810,ESC Stockholm Acute heart Failure Critical cardiac care: update 2010 Markku S. Nieminen
Acute heart Failure Critical cardiac care: update 2010 Markku S. Nieminen Helsinki, Finland M S Nieminen, AHF 300810,ESC Stockholm Acute heart Failure Critical cardiac care: update 2010 Markku S. Nieminen
Prevention of Atrial Fibrillation and Heart Failure in the Hypertensive Patient
 Prevention of Atrial Fibrillation and Heart Failure in the Hypertensive Patient The Issue of Primary Prevention of A.Fib. (and Heart Failure) and not the Prevention of Recurrent A.Fib. after Electroconversion
Prevention of Atrial Fibrillation and Heart Failure in the Hypertensive Patient The Issue of Primary Prevention of A.Fib. (and Heart Failure) and not the Prevention of Recurrent A.Fib. after Electroconversion
New CHF Patient in my Office: What Should I Do?
 New CHF Patient in my Office: What Should I Do? Joseph Mishkin MD FACC Advanced Heart Failure, Transplantation and Mechanical Circulatory Support No disclosures Disclosures Clinical Presentation 38 year
New CHF Patient in my Office: What Should I Do? Joseph Mishkin MD FACC Advanced Heart Failure, Transplantation and Mechanical Circulatory Support No disclosures Disclosures Clinical Presentation 38 year
The Who, How and When of Advanced Heart Failure Therapies. Disclosures. What is Advanced Heart Failure?
 The Who, How and When of Advanced Heart Failure Therapies 9 th Annual Dartmouth Conference on Advances in Heart Failure Therapies Dartmouth-Hitchcock Medical Center Lebanon, NH May 20, 2013 Joseph G. Rogers,
The Who, How and When of Advanced Heart Failure Therapies 9 th Annual Dartmouth Conference on Advances in Heart Failure Therapies Dartmouth-Hitchcock Medical Center Lebanon, NH May 20, 2013 Joseph G. Rogers,
Rikshospitalet, University of Oslo
 Rikshospitalet, University of Oslo Preventing heart failure by preventing coronary artery disease progression European Society of Cardiology Dyslipidemia 29.08.2010 Objectives The trends in cardiovascular
Rikshospitalet, University of Oslo Preventing heart failure by preventing coronary artery disease progression European Society of Cardiology Dyslipidemia 29.08.2010 Objectives The trends in cardiovascular
Clinical Presentation of Heart Failure Patients Admitted in National Institute of Cardiovascular Diseases, Dhaka
 J MEDICINE 2014; 15 : 18-22 Clinical Presentation of Heart Failure Patients Admitted in National Institute of Cardiovascular Diseases, Dhaka MD. TOUFIQUR RAHMAN, 1 AAS MAJUMDER, 2 AFZALUR RAHMAN, 3 ABDUL
J MEDICINE 2014; 15 : 18-22 Clinical Presentation of Heart Failure Patients Admitted in National Institute of Cardiovascular Diseases, Dhaka MD. TOUFIQUR RAHMAN, 1 AAS MAJUMDER, 2 AFZALUR RAHMAN, 3 ABDUL
The Failing Heart in Primary Care
 The Failing Heart in Primary Care Hamid Ikram How fares the Heart Failure Epidemic? 4357 patients, 57% women, mean age 74 years HFSA 2010 Practice Guideline (3.1) Heart Failure Prevention A careful and
The Failing Heart in Primary Care Hamid Ikram How fares the Heart Failure Epidemic? 4357 patients, 57% women, mean age 74 years HFSA 2010 Practice Guideline (3.1) Heart Failure Prevention A careful and
The ACC 50 th Annual Scientific Session
 Special Report The ACC 50 th Annual Scientific Session Part One From March 18 to 21, 2001, physicians from around the world gathered to learn, to teach and to discuss at the American College of Cardiology
Special Report The ACC 50 th Annual Scientific Session Part One From March 18 to 21, 2001, physicians from around the world gathered to learn, to teach and to discuss at the American College of Cardiology
Pathophysiology: Heart Failure
 Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Synopsis. Study title. Investigational Product Indication Design of clinical trial. Number of trial sites Duration of clinical trial / Timetable
 Synopsis Study title Investigational Product Indication Design of clinical trial Number of trial sites Duration of clinical trial / Timetable Repetitive levosimendan infusions for patients with advanced
Synopsis Study title Investigational Product Indication Design of clinical trial Number of trial sites Duration of clinical trial / Timetable Repetitive levosimendan infusions for patients with advanced
5 Important Things to Know About Heart Failure. Kia Afshar, MD
 5 Important Things to Know About Heart Failure Kia Afshar, MD Disclosures I have no conflicts of interest to disclose I will not be discussing any off label medications and/or devices Objectives 1) Understand
5 Important Things to Know About Heart Failure Kia Afshar, MD Disclosures I have no conflicts of interest to disclose I will not be discussing any off label medications and/or devices Objectives 1) Understand
ACUTE HEART FAILURE in the ED. Pr. Samir Nouira Emergency Department Fattouma Bourguiba University Hospital Monastir Tunisia
 ACUTE HEART FAILURE in the ED Pr. Samir Nouira Emergency Department Fattouma Bourguiba University Hospital Monastir Tunisia ACUTE HEART FAILURE 80% Acute Heart Failure Syndrome Sensitivity Specificity
ACUTE HEART FAILURE in the ED Pr. Samir Nouira Emergency Department Fattouma Bourguiba University Hospital Monastir Tunisia ACUTE HEART FAILURE 80% Acute Heart Failure Syndrome Sensitivity Specificity
Management of acute decompensated heart failure and cardiogenic shock. Arintaya Phrommintikul Department of Medicine CMU
 Management of acute decompensated heart failure and cardiogenic shock Arintaya Phrommintikul Department of Medicine CMU Acute heart failure: spectrum Case 64 y/o M with Hx of non-ischemic DCM (LVEF=25-30%)
Management of acute decompensated heart failure and cardiogenic shock Arintaya Phrommintikul Department of Medicine CMU Acute heart failure: spectrum Case 64 y/o M with Hx of non-ischemic DCM (LVEF=25-30%)
Using Lung Ultrasound to Diagnose and Manage Acute Heart Failure
 Using Lung Ultrasound to Diagnose and Manage Acute Heart Failure Jennifer Martindale, MD Assistant Professor Department of Emergency Medicine SUNY Downstate/Kings County Hospital Brooklyn, NY What is acute
Using Lung Ultrasound to Diagnose and Manage Acute Heart Failure Jennifer Martindale, MD Assistant Professor Department of Emergency Medicine SUNY Downstate/Kings County Hospital Brooklyn, NY What is acute
Peripartum Cardiomyopathy. Lavanya Rai Manipal
 Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
Patient characteristics Intervention Comparison Length of followup
 ISCHAEMIA TESTING CHAPTER TESTING FOR MYCOCARDIAL ISCHAEMIA VERSUS NOT TESTING FOR MYOCARDIAL ISCHAEMIA Ref ID: 4154 Reference Wienbergen H, Kai GA, Schiele R et al. Actual clinical practice exercise ing
ISCHAEMIA TESTING CHAPTER TESTING FOR MYCOCARDIAL ISCHAEMIA VERSUS NOT TESTING FOR MYOCARDIAL ISCHAEMIA Ref ID: 4154 Reference Wienbergen H, Kai GA, Schiele R et al. Actual clinical practice exercise ing
Innovation therapy in Heart Failure
 Innovation therapy in Heart Failure P. Laothavorn September 2015 Topics of discussion Basic Knowledge about heart failure Standard therapy New emerging therapy References: standard Therapy in Heart Failure
Innovation therapy in Heart Failure P. Laothavorn September 2015 Topics of discussion Basic Knowledge about heart failure Standard therapy New emerging therapy References: standard Therapy in Heart Failure
Stopping the Revolving Door of ADHF
 Stopping the Revolving Door of ADHF Ileana L. Piña, MD, MPH Professor of Medicine and Epidemiology/Population Health Associate Chief for Academic Affairs -- Cardiology Montefiore-Einstein Medical Center
Stopping the Revolving Door of ADHF Ileana L. Piña, MD, MPH Professor of Medicine and Epidemiology/Population Health Associate Chief for Academic Affairs -- Cardiology Montefiore-Einstein Medical Center
Heart Failure Management. Waleed AlHabeeb, MD, MHA Assistant Professor of Medicine Consultant Heart Failure Cardiologist
 Heart Failure Management Waleed AlHabeeb, MD, MHA Assistant Professor of Medicine Consultant Heart Failure Cardiologist Heart failure prevalence is expected to continue to increase¹ 21 MILLION ADULTS WORLDWIDE
Heart Failure Management Waleed AlHabeeb, MD, MHA Assistant Professor of Medicine Consultant Heart Failure Cardiologist Heart failure prevalence is expected to continue to increase¹ 21 MILLION ADULTS WORLDWIDE
Online Appendix (JACC )
 Beta blockers in Heart Failure Collaborative Group Online Appendix (JACC013117-0413) Heart rate, heart rhythm and prognostic effect of beta-blockers in heart failure: individual-patient data meta-analysis
Beta blockers in Heart Failure Collaborative Group Online Appendix (JACC013117-0413) Heart rate, heart rhythm and prognostic effect of beta-blockers in heart failure: individual-patient data meta-analysis
Right Ventricular Systolic Dysfunction is common in Hypertensive Heart Failure: A Prospective Study in Sub-Saharan Africa
 Right Ventricular Systolic Dysfunction is common in Hypertensive Heart Failure: A Prospective Study in Sub-Saharan Africa 1 Ojji Dike B, Lecour Sandrine, Atherton John J, Blauwet Lori A, Alfa Jacob, Sliwa
Right Ventricular Systolic Dysfunction is common in Hypertensive Heart Failure: A Prospective Study in Sub-Saharan Africa 1 Ojji Dike B, Lecour Sandrine, Atherton John J, Blauwet Lori A, Alfa Jacob, Sliwa
21/06/2018. MEASURING PERFORMANCE (AUDIT AND QUALITY IMPROVEMENT) Towards Reducing Inequity. What should we be measuring?
 MEASURING PERFORMANCE (AUDIT AND QUALITY IMPROVEMENT) Towards Reducing Inequity Dr Raewyn Fisher Cardiologist Director of Waikato Integrated Heart Failure Service What should we be measuring? At risk,
MEASURING PERFORMANCE (AUDIT AND QUALITY IMPROVEMENT) Towards Reducing Inequity Dr Raewyn Fisher Cardiologist Director of Waikato Integrated Heart Failure Service What should we be measuring? At risk,
Practical Points in Cardiorenal Syndrome
 Practical Points in Cardiorenal Syndrome Vichai Senthong, MD. Cardiovascular Unit, Faculty of Medicine Khon Kaen university HFCT Annual Scientific Meeting June 16, 2017, Eastin Grand Sathorn Hotel, Bangkok
Practical Points in Cardiorenal Syndrome Vichai Senthong, MD. Cardiovascular Unit, Faculty of Medicine Khon Kaen university HFCT Annual Scientific Meeting June 16, 2017, Eastin Grand Sathorn Hotel, Bangkok
