Suggestive symptoms and signs of pulmonary thromboembolism in cardiac failure
|
|
|
- Shauna Lynch
- 6 years ago
- Views:
Transcription
1 ARS Medica Tomitana ; 2(22): /arsm Niculescu Zizi1, Ghinea Mihaela Maria2, Niculescu C.2, Grigorian M.1 Suggestive symptoms and signs of pulmonary thromboembolism in cardiac failure 1Faculty of Dental Medicine, University Ovidius of Constanta 2Faculty of Medicine, University Ovidius of Constanta, ABSTRACT Pulmonary thrombembolism can be a complication or it can lead to the onset of heart failure. The early diagnosis of pulmonary thromboembolism may make the difference between life and death. The aim of the study was to determine pulmonary thromboembolism incidence in patients with cardiac failure and to attempt diagnosis optimization. Study group included 150 patients admitted at Medical Clinic II, Emergency Clinical County Hospital Constanta with preexistent known or unknown heart disease, which led to cardiac failure. Patients were suspected with incipient pulmonary thromboembolism. Dyspnea was the most frequently manifested symptom leading to pulmonary thromboembolism suspicion (99%). Pulmonary thromboembolism suggestive dyspnea displayed two forms: sudden onset of dyspnea and increased dyspnea in patients suffering from dyspnea at rest. Thoracic pain was present in approximately 90% of the patients and was manifested in two forms: retrosternal pain, not increasing with respiratory movement, and acute localized thoracic pain, accompanied by hemoptysis and dyspnea; these symptoms suggest pulmonary infarction. Niculescu Zizi Faculty of Medicine, University Ovidius of Constanta University Street, No. 1, Campus B Constanta, Romania ziziniculescu@yahoo.co.uk phone: Pulmonary thromboembolism complicates clinically manifested heart failure or precipitates heart failure onset in patients with latent myocardial dysfunction. Keywords: symptoms and signs, pulmonary tromboembolism, cardiac failure Introduction Clinical practice is frequently confronted with heart failure of known etiology, complicated with pulmonary thromboembolism (PTE), or with cases in which pulmonary thromboembolism has led to acceleration of heart failure onset. Early diagnosis of pulmonary thromboembolism signs in patients whose prognosis is already aggravated by the condition leading to heart failure onset may make the difference between life and death. This is true under the circumstances in which the percentage of death as a result of untreated pulmonary thromboembolism is high, even in patients with no pre-existent heart condition [1, 2]. The aim of the study was to assess incidence of pulmonary thromboembolism in patients with cardiac failure and to attempt diagnosis optimization. 97
2 Material and methods Study group included 150 patients admitted at Medical Clinic II, Emergency Clinical County Hospital Constanţa with preexistent known or unknown heart disease, which led to cardiac failure. Patients were suspected with incipient pulmonary thromboembolism. The prospective study was conducted in the period The study did not include: - patients with massive thromboembolism followed by heart failure - patients with right-sided heart failure secondary to thromboembolic pulmonary hypertension - patients undergoing recent surgery procedure - prolonged bed-ridden patients - patients with recent lower-limb fracture - neoplasm patients Conditions leading to left-sided heart failure were mitral stenosis, complicated or not with atrial fibrillation, arterial hypertension (HTN), ischemic heart disease with left ventricular dysfunction. Conditions complicated with right-sided heart failure were chronic pulmonary heart disease and posterior myocardial infarction. Most patients in the study group suspected with pulmonary thromboembolism presented global heart failure. Conditions leading to cardiac decompensation were: ischemic dilated cardiomyopathy, complicated or not with atrial fibrillation; non-ischemic dilated cardiomyopathy; left-ventricle myocardial infarction with after-effects; and mitral stenosis complicated with atrial fibrillation. Patients in the study group suspected with pulmonary thromboembolism were examined clinically, biologically, and paraclinically in order to establish certain diagnosis of pulmonary thromboembolism. Biological tests consisted of D-dimer dosage or, in certain instances, fibrin monomer qualitative test. The following additional tests were administered to the patients: electrocardiography (ECG), cardio-pulmonary x-ray, echocardiography, pulmonary angiography, pulmonary CT-scan with contrast medium, vascular doppler ultrasound of the lower-extremity veins. Patients undergoing recent surgery (40 days before PTE symptoms onset), bed-ridden patients, patients with recent lower-limb fractures, as well as patients diagnosed with a form of neoplasm were not included in the study group; the reason is that these are high-risk PTE patient groups among the general population, so they could have altered the study results. This study aims to prove the association of cardiac failure and PTE, in the absence of other major PTE risk factors [3,4]. Clinical evaluation: hypothesizing PTE upon patients clinical examination was most important in study group selection and diagnostic strategy approach; it is well-known that, in 90% of cases, PTE suspicion is raised by symptoms such as dyspnea, thoracic pain, or syncope. The monitored parameters are indicated in Table I. Table I. PTE-suggestive symptoms and signs Symptoms Dyspnea Thoracic pain Hemoptysis Syncope Cough Signs Tachypnea ( >20/min) Tachycardia (>100/min) Signs of deep venous thrombosis Fever Cyanosis Radiological changes Atelectasis or infiltrations Pleural effusion Triangular opacity with thoracic wall basis (pulmonary infarction) Hemidiaphragm elevation Hilar artery section ECG changes Right-ventricle overcharge Blood gas changes Hypoxemia Personal pathological Obesity history Smoking History of deep venous thrombosis or PTE Diabetes Most patients in the study group presenting right-sided and global heart failure events manifested, at a given time, intense dyspnea, with no apparent 98
3 cause and despite being administered appropriate therapy for cardiac failure. Severe dyspnea, with sudden onset of persistent polypnea at rest, was often associated with acute, frequently retrosternal, thoracic pain. The fact that cardiac therapy itself, respectively diuretic therapy, might have caused PTE onset by increased blood viscosity was not overlooked [5]. Many patients with right-sided or global heart failure presented non-invasive PTE in varying degrees of dramatic symptoms. Although such medium or brief PTE episodes do not affect right-ventricle function in patients with a previously undamaged heart, in patients with pre-existent heart failure they have caused right-ventricle damage [6]. Most patients with left-sided heart failure, either left ventricle dysfunction or mitral valve pathology, presented pulmonary infarction or in situ embolism clinical features. Results Of the 150 patients aged between 30 and 84, 96 (64%) were men and 54 (36%) were women (Figure 1). The average age for men was 56.8 years and for women 56.3 years, almost equal values. Distribution by age and sex is presented in Table II. Table II. Distribution of the study group by age and sex Age group (years) Males Females > Total The maxium incidence of PTE in heart failure occurs, in men, age range years, and women, years range, actually following the incidence of heart failure. We reported the percentage of men and women to all patients and found p = 0.01 and t = 0.23, meaning that men are statistically significantly correlated with women, in terms of the distribution of the disease (in proportion of 99%), so they follow the same distribution. Patient distribution according to heart failure type is presented in Figure 2. Figure 2. Distribution of cases according to cardiac failure type Figure 1. Distribution of cases according to gender Subgroup with left heart failure and PTE 99
4 suspicion, consisted of 20 patients (13.3%), and they had the following conditions: mitral stenosis complicated with or without atrial fibrillation, ischemic heart disease with left ventricular dysfunction, left ventricular myocardial infarction. There were 12 cases of mitral stenosis, 5 cases of ischemic heart disease and 3 cases of left ventricular myocardial infarction uncomplicated with cardiogenic shock. It is noted that most of this subgoup cases were mitral stenosis (60%). Subgroup of right heart failure and TEP suspicion consisted of 40 patients (26.7%) of the initial sample, of which 38 (95%) were chronic pulmonary heart. Subgroup of global heart failure and suspected to be with TEP also consisted of 90 patients, meaning 60% of the initial batch; from these, 62 had ischemic dilated cardiomyopathy (68.8%), most of them having atrial arrhythmias (atrial fibrillation or atrial flutter). Discussion Suspicion of PTE was initially based on varied symptoms of the patients, sometimes dramatic, marked by syncope and even death, sometimes too little suggestive, consisting of dyspnea and eventualy chest discomfort. Interpretation of the clinical parameters was sometimes difficult because the symptoms and signs given by heart failure itself. All patients had a form of dyspnea (upon exertion and/ or at rest) before the onset of PTE, hemoptysis in a patient with mitral stenosis or with COPD, may be set up only on account of these diseases, and so on. Dyspnea was present in 99% cases, i.e. in almost all initial study group patients, except for 3 patients whose symptoms started with syncope. Dyspnea was the most frequent symptom responsible for PTE suspicion. Dyspnea events varied with each case; assessing its etiology was difficult because most heart failure patients presented dyspnea even before PTE onset. PTE-suggestive dyspnea events were the following: suddenly occurring dyspnea at rest, regardless of patient s posture (clinostatic or orthostatic) and increased dyspnea in a patient with previous episodes of dyspnea at rest and/or dyspnea upon exertion. Isolated dyspnea, sudden apeared, is most often due to a more centrally located PTE, which does not affect the pleura [7]. Often is associated with substernal pain, similar to that of angina pectoris, pain probably due to right ventricular ischemia. Rarely, dyspnea can install gradually, over several weeks, and the diagnosis of PTE is suggested by the absence of other causes of progressive dyspnea. Thoracic pain was present in 135 patients in PTE-suspicion study group, i.e. a rate of approximately 90%. Thoracic pain was manifested in two forms: retrosternal pain, non-aggravated by respiratory movement and acute localized thoracic pain, accompanied by hemoptysis and dyspnea, which suggests pulmonary infarction [8,9]. Chest pain associated with pulmonary embolism is usually sharp and worsens with deep inspiration, cough, and movement, resulting from pleural inflammation in peripheral emboli - pleuritic pain [10,11]. Hemoptysis was present in 72% of the patients, in most cases associated with dyspnea and thoracic pain. Hemoptysis was low, repetitive, with blood red that after a few days became dark brown. Usually it suggests a small embolism, located distally, near the pleura. Syncope was present at PTE onset in 3 cases (2%); in one case, resuscitation was ineffective and patient exitus occurred as a result of massive PTE; two cases beginning in syncope responded to resuscitation, which was followed by lung CT-scan with contrast medium and catheter thromboembolectomy. Syncope is characteristic for central and massive PTE, with severe hemodynamic repercussions. Syncope in the onset of pulmonary embolism can be the result of three possible mechanisms. First, greater than 50% occlusion of the pulmonary vascular tree causes right ventricular failure and impaired left ventricular filling, leading to a reduction in cardiac output, arterial hypotension, reduced cerebral blood flow, and ultimately syncope. The second mechanism of syncope associated with pulmonary embolism is 100
5 the appearance of arrhythmias associated with right ventricular overload. In the third mechanism, the embolism can trigger a vasovagal reflex that leads to neurogenic syncope. However, the contribution of hypoxemia secondary to ventilation or perfusion abnormalities must also be considered and may play an important role in the development of syncope. Moreover, acute pulmonary hypertension may also lead to right-to-left flow across a patent foramen ovale, and thus exacerbate hypoxemia [12,13]. Deep lower-limb venous thrombosis signs were present in 4 patients (2.6%). None showed any personal history of deep venous thrombosis (DVT) or PTE. The association of symptoms and signs is important in clinical practice, assembling the clinical features of frequently encountered PTE syndromes. Patients showed the following symptom and sign associative types suggestive of massive, submassive, and non-massive PTE: Syncope occurred in 3 massive PTE cases (2%); in one case, it was followed by patient death and in 2 cases by resuscitation and subsequent hemodynamic stabilization, after pulmonary CT-scan with contrast medium. Death occurred in one male with ischemic dilated cardiomyopathy and atrial fibrillation; the other 2 cases beginning in syncope were 2 males with chronic obstructive pulmonary disease (COPD) and acute myocardial infarction complicated with PTE. Intense sudden dyspnea followed by collapse was the onset suggesting massive PTE in 12 cases (8%), among which 8 patients with rightsided heart failure (COPD and CPC) and 4 patients with global heart failure (among whom 3 patients with ischemic dilated cardiomyopathy and one patient with mitral stenosis complicated with atrial fibrillation and congestive heart failure). Intense sudden dyspnea often associated with tachycardia ± acute retrosternal pain ± cyanosis ± arterial hypertension; these were the clinical features in 22 patients (15%). Three of the patients manifesting these clinical features also presented signs of deep venous thrombosis (DVP) in a pelvic limb. Sudden dyspnea or aggravation of existing dyspnea associated with acute localized thoracic pain ± hemoptysis ± low-grade fever ± changes in objective lung examination: submatted or matted lung-base, crepitation and/ or sub-crepitation rales, pleural friction rubs at lung base, localized in a certain area; these signs were present in 75 patients (50%). Clinical features were consistent with non-massive PTE (pulmonary infarction). Two patients also presented signs of DVP in a pelvic limb. Increased cardiac failure events occurred in 38 patients (25%): dyspnea on more moderate exertion than before, or dyspnea at rest, in a patient who used to present only dyspnea on exertion; increased or persistent hepatic stasis and edema, despite accurate therapy for cardiac failure. Correlations between significant clinical features and PTE are presented in Table III. Table III. Correlation between PTE-suggestive clinical features and PTE-grade type Clinical syndromes Symptom incidence in study group Possible PTE type Syncope 2% Massive Intense sudden dyspnea, collapse 8% Massive Intense dyspnea, retrosternal thoracic pain, tachicardia, systemic arterial hypotension, cyanosis 15% Massive Sudden dyspnea or aggravated existing dyspnea, acute thoracic localized pain, ± hemoptysis ± low-grade fever Increased cardiac failure events, despite appropriate therapy 50% Non-massive (pulmonary infarction) 25% Non-massive 101
6 Conclusions We can conclude that: pulmonary thromboembolism complicates the evolution of clinically manifested cardiac failure or accelerates cardiac failure onset in patients with latent myocardial dysfunction; PTE-suggestive symptoms are dyspnea, with or without tahipnea, thoracic pain, syncope, hemoptysis; these symptoms occur in isolation or associated; dyspnea was the most frequent symptom responsible for PTE suspicion; forms of PTE-suggestive dyspnea were sudden dyspnea and increased dyspnea in a patient with dyspnea at rest; increased cardiac failure events, despite accurate cardiac failure therapy, were correlated at a high rate (30%) with non-massive PTE; syncope or shock suggests massive PTE, with severe hemodynamic consequences, such as oliguria, cold extremities and/ or signs of acute right-sided cardiac failure. References 1. Stein, P.D., Beemath, A. & Olson, RE. (2005). Trends in the incidence of pulmonary embolism and deep venous thrombosis in hospitalized patients. Am. J. Cardiol. 95(12), DOI: /j.amjcard Gherasim, L., Iliesiu, A. & Gherasim, L. (2004). Tromboembolismul pulmonar. In Medicina Interna Bolile cardiovasculare si metabolice, vol.ii, Part II, (pp ). Bucuresti, Romania: Editura Medicala. 3. Kucher, N. & Golhaber, S.Z. (2005). Management of massive pulmonary embolism. Circulation. 112: e28-e32. DOI: / CIRCULATIONAHA Fedullo, P.E., Auger, W.R., Kerr, K.M. & Rubin, L.J. (2001). Chronic thromboembolic pulmonary hypertension. N. Engl. J. Med. 345(20), DOI: /NEJMra Fedullo, P.F. & Morris, T.A. (2005). Pulmonary Thromboembolism. In: J.F. Murray & J.A. Nadel (Eds.), Textbook of respiratory medicine (section L, chapter 48). 4th ed. Elsevier, W.B Saunders Company. 6. Lang, I.M. (2004). Chronic Thromboembolic Pulmonary Hypertension - Not so rare after all. N. Engl. J. Med. 350, DOI: / NEJMp Stein, P. D., Beemath, A., Matta, F., Weg, J.G., Yusen, R.D., Hales, C.A., & Woodard, P. K. (2007). Clinical Characteristics of Patients with Acute Pulmonary Embolism: Data from PIOPED II. The American Journal of Medicine. 120(10): DOI: /j.amjmed Ouellette, D. & Mosenifar, Z. (2015, October). Pulmonary embolism. Retrieved January 29, 2016, from article/ clinical. 9. Shellhaß, A., Walther, A., Konstantinides, S. & Bötiger, B.W. (2010). The diagnosis and treatment of acute pulmonary embolism. Dtsch. Arztebl. Int. 107(34-35), DOI: / arztebl Agnelli, G. & Becattini, C. (2010). Acute pulmonary embolism. N. Engl. J. Med. 363, DOI: /NEJMra Riedel, M. (2004). Diagnosing pulmonary embolism. Postgrad. Med. J. 80, DOI: /pgmj Castelli, R., Tarsia, P., Tantardini, C., Pantaleo, G., Guariglia, A., Porro, F. (2003). Syncope in patients with pulmonary embolism: comparison between patients with syncope as the presenting symptom of pulmonary embolism and patients with pulmonary embolism without syncope. Vasc. Med. 8(4), DOI: / x03vm510oa 13. Dipaola, F., Cucchi, I., Filardo, N., Carnovali, E., Montano, N., Furlan, R. & Costantino, G. (2006). Syncope as a symptom of non-massive pulmonary embolism: a case report. Intern. Emerg. Med. 1(2), DOI: / BF
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Chest Pain. Dr. Amitesh Aggarwal. Department of Medicine
 Chest Pain Dr. Amitesh Aggarwal Department of Medicine BACKGROUND Approx 5% of all ED visits 15 % - AMI 25-30 % - Unstable angina 50-55 % - Other conditions Atypical presentations common 2% of patients
Chest Pain Dr. Amitesh Aggarwal Department of Medicine BACKGROUND Approx 5% of all ED visits 15 % - AMI 25-30 % - Unstable angina 50-55 % - Other conditions Atypical presentations common 2% of patients
According to Their Presenting Syndromes*
 Clinical Characteristics of Patients With Acute Pulmonary Embolism Stratified According to Their Presenting Syndromes* Paul D. Stein, MD, FCCP; and Jerald W. Henry, MS Purpose: The purpose of this investigation
Clinical Characteristics of Patients With Acute Pulmonary Embolism Stratified According to Their Presenting Syndromes* Paul D. Stein, MD, FCCP; and Jerald W. Henry, MS Purpose: The purpose of this investigation
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Thrombolysis in PE. Outline. Disclosure. Overview on Pulmonary Embolism. Hot Topics in Emergency Medicine 2012 Midyear Clinical Meeting
 Disclosure Thrombolysis in PE Daniel P. Hays, PharmD, BCPS, FASHP reports no relevant financial relationships. Daniel P. Hays, PharmD, BCPS, FASHP Outline 55 YOF presents to ED with SOB PMH of DVT + noncompliance
Disclosure Thrombolysis in PE Daniel P. Hays, PharmD, BCPS, FASHP reports no relevant financial relationships. Daniel P. Hays, PharmD, BCPS, FASHP Outline 55 YOF presents to ED with SOB PMH of DVT + noncompliance
Cor pulmonale. Dr hamid reza javadi
 1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
October 2017 Pulmonary Embolism
 October 2017 Pulmonary Embolism Prof. Ahmed BaHammam, FRCP, FCCP Professor of Medicine College of Medicine King Saud University 1 Objectives Epidemiology Pathophysiology Diagnosis Massive PE Treatment
October 2017 Pulmonary Embolism Prof. Ahmed BaHammam, FRCP, FCCP Professor of Medicine College of Medicine King Saud University 1 Objectives Epidemiology Pathophysiology Diagnosis Massive PE Treatment
Pathophysiology. Tutorial 3 Hemodynamic Disorders
 Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Pathophysiology Tutorial 3 Hemodynamic Disorders ILOs Recall different causes of thrombosis. Explain different types of embolism and their predisposing factors. Differentiate between hemorrhage types.
Lnformation Coverage Guidance
 Lnformation Coverage Guidance Coverage Indications, Limitations, and/or Medical Necessity Abstract: B-type natriuretic peptide (BNP) is a cardiac neurohormone produced mainly in the left ventricle. It
Lnformation Coverage Guidance Coverage Indications, Limitations, and/or Medical Necessity Abstract: B-type natriuretic peptide (BNP) is a cardiac neurohormone produced mainly in the left ventricle. It
Diagnosis & Management of Heart Failure. Abena A. Osei-Wusu, M.D. Medical Fiesta
 Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Chapter 1. Introduction
 Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
Chapter 1 Introduction Introduction 9 Even though the first reports on venous thromboembolism date back to the 13 th century and the mechanism of acute pulmonary embolism (PE) was unraveled almost 150
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
MATERIALS AND METHODS
 RETROSPECTIVE STUDY OF OPTIMISING THE USE OF COMPUTED TOMOGRAPHY PULMONARY ANGIOGRAPHY (CTPA) FOR THE DIAGNOSIS OF PULMONARY EMBOLISM IN PLACES WITH LIMITED RESOURCES P. V. Kalyan Kumar 1, Ramakrishna
RETROSPECTIVE STUDY OF OPTIMISING THE USE OF COMPUTED TOMOGRAPHY PULMONARY ANGIOGRAPHY (CTPA) FOR THE DIAGNOSIS OF PULMONARY EMBOLISM IN PLACES WITH LIMITED RESOURCES P. V. Kalyan Kumar 1, Ramakrishna
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Pathology of pulmonary vascular disease. Dr.Ashraf Abdelfatah Deyab. Assistant Professor of Pathology Faculty of Medicine Almajma ah University
 Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Pathology of pulmonary vascular disease Dr.Ashraf Abdelfatah Deyab Assistant Professor of Pathology Faculty of Medicine Almajma ah University Pulmonary vascular disease Type of pulmonary circulation: Types
Shock, Hemorrhage and Thrombosis
 Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
Shock, Hemorrhage and Thrombosis 1 Shock Systemic hypoperfusion due to: Reduction in cardiac output Reduction in effective circulating blood volume Hypotension Impaired tissue perfusion Cellular hypoxia
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Epidermiology Early pulmonary embolism
 Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Acute Coronary Syndrome
 ACUTE CORONOARY SYNDROME, ANGINA & ACUTE MYOCARDIAL INFARCTION Administrative Consultant Service 3/17 Acute Coronary Syndrome Acute Coronary Syndrome has evolved as a useful operational term to refer to
ACUTE CORONOARY SYNDROME, ANGINA & ACUTE MYOCARDIAL INFARCTION Administrative Consultant Service 3/17 Acute Coronary Syndrome Acute Coronary Syndrome has evolved as a useful operational term to refer to
Means failure of heart to pump enough blood to satisfy the need of the body.
 Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating)
 Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Pulmonary Embolism..Diagnostic Approach and Algorithm. Tolulope Adesiyun Harvard Medical School, Year III Gillian Lieberman, MD
 Pulmonary Embolism..Diagnostic Approach and Algorithm Tolulope Adesiyun Harvard Medical School, Year III Gillian Lieberman, MD Epidemiology of Pulmonary Embolism Pulmonary Embolus (PE): Thrombus originating
Pulmonary Embolism..Diagnostic Approach and Algorithm Tolulope Adesiyun Harvard Medical School, Year III Gillian Lieberman, MD Epidemiology of Pulmonary Embolism Pulmonary Embolus (PE): Thrombus originating
Chapter 10 Respiratory System J00-J99. Presented by: Jesicca Andrews
 Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Chapter 10 Respiratory System J00-J99 Presented by: Jesicca Andrews 1 Respiratory System 2 Respiratory Infections A respiratory infection cannot be assumed from a laboratory report alone; physician concurrence
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS. 1. Cardiovascular Disease
 THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS 1. Cardiovascular Disease Cardiovascular disease is considered to have developed if there was a definite manifestation
THE FRAMINGHAM STUDY Protocol for data set vr_soe_2009_m_0522 CRITERIA FOR EVENTS 1. Cardiovascular Disease Cardiovascular disease is considered to have developed if there was a definite manifestation
Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks
 Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks 1. What is the most common cause of death in hospitalized patients? 1. Hospital-acquired infection 2. Pulmonary embolism 3. Myocardial infarction
Jessica Bryan, Natalia Evans, Karlyn Henderson, & Whitney Parks 1. What is the most common cause of death in hospitalized patients? 1. Hospital-acquired infection 2. Pulmonary embolism 3. Myocardial infarction
Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg
 Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Rotation: or: Faculty: Coronary Care Unit (CVICU) Dr. Jeff Rottman Drs. Rottman, Salloum, Campbell, Muldowney, Hong, Bagai, Kronenberg Duty Hours: Mon Fri, 7 AM to 7 PM, weekend call shared with consult
Pulmonary Embolism. Supportive module 3 "Basics of diagnosis, treatment and prevention of major pulmonary diseases "
 Supportive module 3 "Basics of diagnosis, treatment and prevention of major pulmonary diseases " Pulmonary Embolism LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky, L. Bogun, L. Martymianova,
Supportive module 3 "Basics of diagnosis, treatment and prevention of major pulmonary diseases " Pulmonary Embolism LECTURE IN INTERNAL MEDICINE FOR IV COURSE STUDENTS M. Yabluchansky, L. Bogun, L. Martymianova,
Clinical Guide - Suspected PE (Reviewed 2006)
 Clinical Guide - Suspected (Reviewed 2006) Principal Developer: B. Geerts Secondary Developers: C. Demers, C. Kearon Background Investigation of patients with suspected pulmonary emboli () remains problematic
Clinical Guide - Suspected (Reviewed 2006) Principal Developer: B. Geerts Secondary Developers: C. Demers, C. Kearon Background Investigation of patients with suspected pulmonary emboli () remains problematic
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT
 PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
PULMONARY EMBOLISM (PE): DIAGNOSIS AND TREATMENT OBJECTIVE: To provide a diagnostic algorithm and treatment options for patients with acute pulmonary embolism (PE). BACKGROUND: Venous thromboembolism (VTE)
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI).
 1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES
 ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Evaluation of Chest Pain in the Primary Care Setting. Joseph Hackler, DO. Disclosures
 Evaluation of Chest Pain in the Primary Care Setting Joseph Hackler, DO Disclosures I have no relevant relationships with commercial interests to disclose. 1 Objectives 1. Discuss the different etiologies
Evaluation of Chest Pain in the Primary Care Setting Joseph Hackler, DO Disclosures I have no relevant relationships with commercial interests to disclose. 1 Objectives 1. Discuss the different etiologies
Disturbance of Circulation Hemodynamic Disorder
 Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
Disturbance of Circulation Hemodynamic Disorder 2/17/2017 By Dr. Hemn Hassan Othman PhD, Pathology Fall 2016 1 Thrombosis Definition: Thrombosis is the formation of solid or semisolid blood clot within
Cardiac Conditions in Sport & Exercise. Cardiac Conditions in Sport. USA - Sudden Cardiac Death (SCD) Dr Anita Green. Sudden Cardiac Death
 Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Ischemic Heart Diseases. Dr. Nabila Hamdi MD, PhD
 Ischemic Heart Diseases Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast the different types of angina regarding their pathogenesis, clinical manifestations and evolution. Discuss myocardial infarct,
Ischemic Heart Diseases Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast the different types of angina regarding their pathogenesis, clinical manifestations and evolution. Discuss myocardial infarct,
Local Coverage Determination (LCD) for Cardiac Catheterization (L29090)
 Local Coverage Determination (LCD) for Cardiac Catheterization (L29090) Contractor Information Contractor Name First Coast Service Options, Inc. Contractor Number 09102 Contractor Type MAC - Part B LCD
Local Coverage Determination (LCD) for Cardiac Catheterization (L29090) Contractor Information Contractor Name First Coast Service Options, Inc. Contractor Number 09102 Contractor Type MAC - Part B LCD
Assessment and Diagnosis of Heart Failure
 Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
Assessment and Diagnosis of Heart Failure Heart failure (HF) is a complex clinical syndrome resulting from any structural or functional impairment of ventricular filling or ejection of blood and is characterized
Heart failure congestive heart failure, or CHF
 Heart failure Heart failure (also called congestive heart failure, or CHF) is a frequent end point of many of the conditions In the United States alone, CHF affects nearly 5 million individuals annually,
Heart failure Heart failure (also called congestive heart failure, or CHF) is a frequent end point of many of the conditions In the United States alone, CHF affects nearly 5 million individuals annually,
Proper Diagnosis of Venous Thromboembolism (VTE)
 Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
Proper Diagnosis of Venous Thromboembolism (VTE) Whal Lee, M.D. Seoul National University Hospital Department of Radiology 2 nd EFORT Asia Symposium, 3 rd November 2010, Taipei DVT - Risk Factors Previous
NIH Public Access Author Manuscript Am J Med. Author manuscript; available in PMC 2007 November 8.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Med. 2007 October ; 120(10): 871 879. Clinical Characteristics of Patients with Acute Pulmonary Embolism: Data from PIOPED II
NIH Public Access Author Manuscript Published in final edited form as: Am J Med. 2007 October ; 120(10): 871 879. Clinical Characteristics of Patients with Acute Pulmonary Embolism: Data from PIOPED II
Cardiac Pathology & Rehabilitation
 Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Radiology of the respiratory/cardiac diseases (part 2)
 Cardiology Cycle - Lecture 6 436 Teams Radiology of the respiratory/cardiac diseases (part 2) Objectives Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Leena Alwakeel Aroob Alhuthail
Cardiology Cycle - Lecture 6 436 Teams Radiology of the respiratory/cardiac diseases (part 2) Objectives Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Leena Alwakeel Aroob Alhuthail
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Process Measure: Screening for Adult Obstructive Sleep Apnea
 Process Measure: Screening for Adult Obstructive Sleep Apnea Measure Description Description Type of Measure All patients aged 18 years and older at high risk for obstructive sleep apnea (OSA) with documentation
Process Measure: Screening for Adult Obstructive Sleep Apnea Measure Description Description Type of Measure All patients aged 18 years and older at high risk for obstructive sleep apnea (OSA) with documentation
Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year
![Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year Protocol Identifier Subject Identifier Visit Description. [Y] Yes [N] No. [Y] Yes [N] N. If Yes, admission date and time: Day Month Year](/thumbs/76/74263761.jpg) PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
PAST MEDICAL HISTORY Has the subject had a prior episode of heart failure? o Does the subject have a prior history of exposure to cardiotoxins, such as anthracyclines? URGENT HEART FAILURE VISIT Did heart
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
ΚΑΡΔΙΟΛΟΓΟΣ EUROPEAN ACCREDITATION IN TRANSTHORACIC AND TRANSESOPHAGEAL ECHOCARDIOGRAPHY
 1 ΚΑΡΔΙΟΛΟΓΟΣ EUROPEAN ACCREDITATION IN TRANSTHORACIC AND TRANSESOPHAGEAL ECHOCARDIOGRAPHY 2 Constrictive pericarditis (CP) is characterized by impaired ventricular filling due to a stiffened or noncompliant
1 ΚΑΡΔΙΟΛΟΓΟΣ EUROPEAN ACCREDITATION IN TRANSTHORACIC AND TRANSESOPHAGEAL ECHOCARDIOGRAPHY 2 Constrictive pericarditis (CP) is characterized by impaired ventricular filling due to a stiffened or noncompliant
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Listing Form: Heart or Cardiovascular Impairments. Medical Provider:
 Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Proper Completion of a Death Certificate"
 Proper Completion of a Death Certificate" Pennsylvania Department of Health Bureau of Health Statistics and Research Division of Statistical Registries Division of Vital Records Why should you care? 1.
Proper Completion of a Death Certificate" Pennsylvania Department of Health Bureau of Health Statistics and Research Division of Statistical Registries Division of Vital Records Why should you care? 1.
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Heart Failure. Cardiac Anatomy. Functions of the Heart. Cardiac Cycle/Hemodynamics. Determinants of Cardiac Output. Cardiac Output
 Cardiac Anatomy Heart Failure Professor Qing ZHANG Department of Cardiology, West China Hospital www.blaufuss.org Cardiac Cycle/Hemodynamics Functions of the Heart Essential functions of the heart to cover
Cardiac Anatomy Heart Failure Professor Qing ZHANG Department of Cardiology, West China Hospital www.blaufuss.org Cardiac Cycle/Hemodynamics Functions of the Heart Essential functions of the heart to cover
Heart Disorders. Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8. Overview Heart Disorders Vascular Disorders
 Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
2/4/2011. Nathan Kerner, M.D.
 Nathan Kerner, M.D. Definition Elevated pressures - cut off usually >40 mmhg pulmonary artery systolic pressure (PASP) Usually associated with elevated pulmonary vascular resistance (PVR) measured in dynessec/cm
Nathan Kerner, M.D. Definition Elevated pressures - cut off usually >40 mmhg pulmonary artery systolic pressure (PASP) Usually associated with elevated pulmonary vascular resistance (PVR) measured in dynessec/cm
Pulmonary Embolism Is it the Greatest Danger in Deep Vein Thrombosis?
 Difficult issues in Deep Vein Thrombosis: Pulmonary Embolism Is it the Greatest Danger in Deep Vein Thrombosis? Raluca Dulgheru; C Gherghinescu; B Dorobat; H Muresan; R Darabont; M Cinteza; D Vinereanu
Difficult issues in Deep Vein Thrombosis: Pulmonary Embolism Is it the Greatest Danger in Deep Vein Thrombosis? Raluca Dulgheru; C Gherghinescu; B Dorobat; H Muresan; R Darabont; M Cinteza; D Vinereanu
SPECIAL PATHOPHYSIOLOGY SHOCK
 SPECIAL PATHOPHYSIOLOGY SHOCK 1. How do we call blood pressure values below the reference range? 1.Hypovolemia. 2. Hypothermia. 3. Hypooncia. 4. Hypoosmia. 5. Hypotension. 2. What is acute circulatory
SPECIAL PATHOPHYSIOLOGY SHOCK 1. How do we call blood pressure values below the reference range? 1.Hypovolemia. 2. Hypothermia. 3. Hypooncia. 4. Hypoosmia. 5. Hypotension. 2. What is acute circulatory
Radiologic Features of The Pulmonary Embolus
 January 2003 Radiologic Features of The Pulmonary Embolus Travis McGlothin HMSIII Mr. J is a 51 y.o. male who presented to the BIDMC ED w/ acute onset of: Lft. Hemiparesis slurred speech mild dyspnea mild
January 2003 Radiologic Features of The Pulmonary Embolus Travis McGlothin HMSIII Mr. J is a 51 y.o. male who presented to the BIDMC ED w/ acute onset of: Lft. Hemiparesis slurred speech mild dyspnea mild
Severe pulmonary embolism: surgical aspects. Oliver Reuthebuch Clinic for Cardiac Surgery University Hospital Basel Switzerland
 Severe pulmonary embolism: surgical aspects Oliver Reuthebuch Clinic for Cardiac Surgery University Hospital Basel Switzerland Severe pulmonary embolism Acute pulmonary embolism Chronic pulmonary thromboembolism
Severe pulmonary embolism: surgical aspects Oliver Reuthebuch Clinic for Cardiac Surgery University Hospital Basel Switzerland Severe pulmonary embolism Acute pulmonary embolism Chronic pulmonary thromboembolism
A Diagnostic Dilemma saved by sound
 A Diagnostic Dilemma saved by sound Dr Syam Ravindranath MBBS DNB, Dr Ash Mukherjee FCEM FACEM We p r e s e n t a d i a g n o s t i c a l l y c h a l l e n g i n g s c e n a r i o in a 59 y e a r old f
A Diagnostic Dilemma saved by sound Dr Syam Ravindranath MBBS DNB, Dr Ash Mukherjee FCEM FACEM We p r e s e n t a d i a g n o s t i c a l l y c h a l l e n g i n g s c e n a r i o in a 59 y e a r old f
Cardiology. Objectives. Chapter
 1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
1:44 M age 1121 Chapter Cardiology Objectives art 1: Cardiovascular natomy and hysiology, ECG Monitoring, and Dysrhythmia nalysis (begins on p. 1127) fter reading art 1 of this chapter, you should be able
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency
 Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Impedance Cardiography (ICG) Application of ICG in Intensive Care and Emergency Aim of haemodynamic monitoring in ICU and ED Detection and therapy of insufficient organ perfusion Answers to common cardiovascular
Case N 1. Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds. Courtesy Dr Van den Homberg-Tanzania
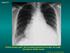 Case N 1 Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds Courtesy Dr Van den Homberg-Tanzania Case N 1 Enlargment of cardiac silhouette. Notice the symetry
Case N 1 Anterior thoracic paint with increasing dyspnea for few days. No cough. Decrease of cardiac sounds Courtesy Dr Van den Homberg-Tanzania Case N 1 Enlargment of cardiac silhouette. Notice the symetry
Peripartum Cardiomyopathy. Lavanya Rai Manipal
 Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
Peripartum Cardiomyopathy Lavanya Rai Manipal Definition - PPCM - Dilated cardiomyopathy of unknown cause resulting in cardiac failure that occurs in the peripartum period in women without any preexisting
SPECIAL PATHOPHYSIOLOGY CARDIO-VASCULAR SYSTEM
 1. Myocardia lischemia is mainly a result of: 1.Coronary hypoxemia. 2. Coronary artery disease (CAD). 3. Acute coronaritis. 4. Coronary anemia. 5. Heart remodelling. SPECIAL PATHOPHYSIOLOGY CARDIO-VASCULAR
1. Myocardia lischemia is mainly a result of: 1.Coronary hypoxemia. 2. Coronary artery disease (CAD). 3. Acute coronaritis. 4. Coronary anemia. 5. Heart remodelling. SPECIAL PATHOPHYSIOLOGY CARDIO-VASCULAR
University Journal of Medicine and Medical Specialities
 University Journal of Medicine and Medical Specialities Volume 1 Issue 1 2015 An unusual case of SADDLE Pulmonary Thrombo Embolism Boopathirajan P Jayanthi R Stanley Medical College Abstract: Pulmonary
University Journal of Medicine and Medical Specialities Volume 1 Issue 1 2015 An unusual case of SADDLE Pulmonary Thrombo Embolism Boopathirajan P Jayanthi R Stanley Medical College Abstract: Pulmonary
Pulmonary Embolism. Pulmonary Embolism. Pulmonary Embolism. PE - Clinical
 Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
Pulmonary embolus - a practical approach to investigation and treatment Sam Janes Wellcome Senior Fellow and Respiratory Physician, University College London Background Diagnosis Treatment Common: 50 cases
Pre Hospital and Initial Management of Acute Coronary Syndrome
 Pre Hospital and Initial Management of Acute Coronary Syndrome Dr. Muhammad Fadil, SpJP 3rd SymCARD 2013 Classification of ACS ESC Guidelines for the management of Acute Coronary Syndrome in patients without
Pre Hospital and Initial Management of Acute Coronary Syndrome Dr. Muhammad Fadil, SpJP 3rd SymCARD 2013 Classification of ACS ESC Guidelines for the management of Acute Coronary Syndrome in patients without
Disclosures. Objectives
 BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
BRIGHAM AND WOMEN S HOSPITAL Treatment of Massive and Submassive Pulmonary Embolism Gregory Piazza, MD, MS Assistant Professor of Medicine Harvard Medical School Staff Physician, Cardiovascular Division
L: Cardiovascular. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 107
 L: Cardiovascular Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 107 Major Competency Area: L Cardiovascular Competency: L-1 Cardiovascular Nursing Date: January
L: Cardiovascular Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 107 Major Competency Area: L Cardiovascular Competency: L-1 Cardiovascular Nursing Date: January
HEMODYNAMIC DISORDERS
 HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
HEMODYNAMIC DISORDERS Normal fluid homeostasis requires vessel wall integrity as well as maintenance of intravascular pressure and osmolarity within certain physiologic ranges. Increases in vascular volume
Acute Coronary Syndromes Unstable Angina Non ST segment Elevation MI (NSTEMI) ST segment Elevation MI (STEMI)
 Leanna R. Miller, RN, MN, CCRN-CSC, PCCN-CMC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Evaluate common abnormalities that mimic myocardial infarction. Identify
Leanna R. Miller, RN, MN, CCRN-CSC, PCCN-CMC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Evaluate common abnormalities that mimic myocardial infarction. Identify
Objectives. Pulmonary Vascular Changes in Heart Disease. Pressure, Flow, Resistance. Pressure, Flow, Resistance FETAL CIRCULATION
 Objectives Pulmonary Vascular Changes in Heart Disease To review the normal physiology of the pulmonary circulation To define pulmonary hypertension, its causes especially related to heart disease, and
Objectives Pulmonary Vascular Changes in Heart Disease To review the normal physiology of the pulmonary circulation To define pulmonary hypertension, its causes especially related to heart disease, and
Single Center 4 year series of 114 consecutive patients treated for massive and submassive PE. Mark Goodwin, MD
 Single Center 4 year series of 114 consecutive patients treated for massive and submassive PE Mark Goodwin, MD Disclosure Speaker name:... I have the following potential conflicts of interest to report:
Single Center 4 year series of 114 consecutive patients treated for massive and submassive PE Mark Goodwin, MD Disclosure Speaker name:... I have the following potential conflicts of interest to report:
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
Abstract Clinical and paraclinical studies on myocardial and endocardial diseases in dog
 Abstract The doctoral thesis entitled Clinical and paraclinical studies on myocardial and endocardial diseases in dog was motivated by the study of the most frequent cardiopathies in dogs, which involves
Abstract The doctoral thesis entitled Clinical and paraclinical studies on myocardial and endocardial diseases in dog was motivated by the study of the most frequent cardiopathies in dogs, which involves
9 : , Fogarty 89% 9 : , Table 1. (Tel : )
 : 7-83, 2000 187 5 17 11 10 6 7 62. 6 8 1 1 8 12.8 8 6 5 1 3 7 6 5 Fogarty 3 8% 6 : 7-83, 2000 187 5 17 11 10 7 (Tel : 05-366-1111) 21-0811 117-1 1 27 2000 6 1 73 10 13.7% 6 7 62. 1 6 6.2 6 8 1 1 8 6 5
: 7-83, 2000 187 5 17 11 10 6 7 62. 6 8 1 1 8 12.8 8 6 5 1 3 7 6 5 Fogarty 3 8% 6 : 7-83, 2000 187 5 17 11 10 7 (Tel : 05-366-1111) 21-0811 117-1 1 27 2000 6 1 73 10 13.7% 6 7 62. 1 6 6.2 6 8 1 1 8 6 5
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
Unilateral pulmonary oedema, a forgotten presentation.
 Unilateral pulmonary oedema, a forgotten presentation. Poster No.: C-2146 Congress: ECR 2018 Type: Educational Exhibit Authors: C. A. Arboleda Vallejo, M. I. carvajal, M. Perez ; Medellin, 1 2 1 1 2 Antioquia/CO,
Unilateral pulmonary oedema, a forgotten presentation. Poster No.: C-2146 Congress: ECR 2018 Type: Educational Exhibit Authors: C. A. Arboleda Vallejo, M. I. carvajal, M. Perez ; Medellin, 1 2 1 1 2 Antioquia/CO,
Difficulties of timely diagnosis of the Pulmonary Embolism of patients with chronic obstructive lung disease: possibility MSCT.
 Difficulties of timely diagnosis of the Pulmonary Embolism of patients with chronic obstructive lung disease: possibility MSCT. Poster No.: C-2618 Congress: ECR 2012 Type: Scientific Exhibit Authors: I.
Difficulties of timely diagnosis of the Pulmonary Embolism of patients with chronic obstructive lung disease: possibility MSCT. Poster No.: C-2618 Congress: ECR 2012 Type: Scientific Exhibit Authors: I.
2
 1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
On Referral to our Unit
 Case Presentation By Samah Ibrahim Abdel Meguid Idris, MD Internal Medicine & Nephrology Consultant Head of Hemodialysis Unit Ahmed Maher Hospital, Alexandria Patient Data MEA 27-year-old male patient
Case Presentation By Samah Ibrahim Abdel Meguid Idris, MD Internal Medicine & Nephrology Consultant Head of Hemodialysis Unit Ahmed Maher Hospital, Alexandria Patient Data MEA 27-year-old male patient
Is it HF secondary to rheumatic heart disease???
 Is it HF secondary to rheumatic heart disease??? Is mitral regurg. Is complication of CHF??? Cardiomyopathy Definition The term cardiomyopathy is purely descriptive, meaning disease of the heart muscle
Is it HF secondary to rheumatic heart disease??? Is mitral regurg. Is complication of CHF??? Cardiomyopathy Definition The term cardiomyopathy is purely descriptive, meaning disease of the heart muscle
Pericardial diseases
 Pericardial diseases Anatomy of the pericardium Consists of parietal and visceral membranes. The space between them(pericardial space is normally filled by a lymph like fluid. The fluid s normal quantity
Pericardial diseases Anatomy of the pericardium Consists of parietal and visceral membranes. The space between them(pericardial space is normally filled by a lymph like fluid. The fluid s normal quantity
CHAPTER X - SECONDARY PULMONARY HYPERTENSION CHRONIC PULMONARY THROMBOEMBOLISM (HTP). PULMONARY THROMBENDARTERECTOMY
 CHAPTER X - SECONDARY PULMONARY HYPERTENSION CHRONIC PULMONARY THROMBOEMBOLISM (HTP). PULMONARY THROMBENDARTERECTOMY Walter KLEPETKO, PhD, VIENNA - AUSTRIA Marian GASPAR, PhD, TIMISOARA 10. 1. Definition.
CHAPTER X - SECONDARY PULMONARY HYPERTENSION CHRONIC PULMONARY THROMBOEMBOLISM (HTP). PULMONARY THROMBENDARTERECTOMY Walter KLEPETKO, PhD, VIENNA - AUSTRIA Marian GASPAR, PhD, TIMISOARA 10. 1. Definition.
Appendix to Gibson et al. Application of a decision rule and a D-dimer assay in the
 Appendix to Gibson et al. Application of a decision rule and a D-dimer assay in the diagnosis of pulmonary embolism (Thromb Haemost 2010; 103.4) Case 1 You are paged by an emergency room physician, who
Appendix to Gibson et al. Application of a decision rule and a D-dimer assay in the diagnosis of pulmonary embolism (Thromb Haemost 2010; 103.4) Case 1 You are paged by an emergency room physician, who
Congestive Heart Failure Patient Profile. Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption
 Congestive Heart Failure Patient Profile Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption Chief Complaint - SOB - When asked: Increasing difficulty
Congestive Heart Failure Patient Profile Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption Chief Complaint - SOB - When asked: Increasing difficulty
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
7. Echocardiography Appropriate Use Criteria (by Indication)
 Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
PE and DVT. Dr Anzo William Adiga WatsApp or Call Medical Officer/RHEMA MEDICAL GROUP
 PE and DVT Dr Anzo William Adiga WatsApp or Call +256777363201 Medical Officer/RHEMA MEDICAL GROUP OBJECTIVES DEFINE DVT AND P.E PATHOPHYSIOLOGY OF DVT CLINICAL PRESENTATION OF DVT/PE INVESTIGATE DVT MANAGEMENT
PE and DVT Dr Anzo William Adiga WatsApp or Call +256777363201 Medical Officer/RHEMA MEDICAL GROUP OBJECTIVES DEFINE DVT AND P.E PATHOPHYSIOLOGY OF DVT CLINICAL PRESENTATION OF DVT/PE INVESTIGATE DVT MANAGEMENT
