Adult Extracorporeal Life Support (ECLS) Family Guide
|
|
|
- Philomena Cummings
- 6 years ago
- Views:
Transcription
1 Adult Extracorporeal Life Support (ECLS) Family Guide Notice: This information is considered for general use only. It should not be used instead of medical advice and care. If you have a specific health concern or care need, you should talk with your doctor. Rev. 4/15.
2 Dear family members and friends, We realize that this is a very hard time for you. Having a loved one in the intensive care unit is stressful for everyone. Be assured, there will be many people available to help you through this difficult time. This booklet was created in hopes of answering some of your questions about ECLS and what will be happening with your loved one. We hope you find this information helpful. We want you to feel comfortable in asking us questions and expressing your concerns. As you think of things, you may want to write them down. We are here for you as well as your loved one. Sincerely, The Nebraska Medicine ECLS Team
3 GLOSSARY As you review this booklet, refer back to these pages for explanation of words you may not recognize. Always feel free to ask the team any questions you have. ECLS Extracorporeal Life Support (ECLS) ECMO Extracorporeal Membrane Oxygenation. This is a form of ECLS. Extracorporeal means that the blood circulates outside of the body with the help of a machine. ACT Activated Clotting Time. This is a blood test that tells us how long it takes for the blood to clot. We check this periodically. Antibiotic A medicine that destroys or slows the growth of bacteria or germs. Used to prevent or get rid of an infection. Arterial blood gas (ABG) test A small amount of blood that is drawn from an artery and tested to find out the amount of oxygen and carbon dioxide it contains. Bronchoscopy In this procedure a camera is placed to examine the lungs and also to take samples of lung tissue and sputum. Cannulae These are plastic tubes that the surgeons place into the blood vessels that lead to the heart.the ECLS Circuit attaches to these cannulae. Cannulation The process of placing the cannulae into the blood vessels. This will be performed surgically or by percutaneous method.
4 Percutaneous Cannulation The cannulae are placed like an IV. There is no surgical incision made. Chest tube A tube placed into the space between the lung and chest wall that removes air or fluid. It is used to treat a collapsed lung (pneumothorax) or to remove fluid around the lung (pleural effusion). Decannulation The process of removing the cannulae from the blood vessels. Depending on the blood vessels used it may be possible to pull out a cannula like an IV or it might require an operation. Dobhoff tube This is a tube that is inserted through the nose to a part of the intestines. This tube allows us to give nutrition and calories to the patient. ECLS flow This is the amount of blood that is being moved through the ECLS circuit per minute. This relates to how much support the patient is receiving. ECLS team This team is made up of specially trained nurses, respiratory therapists, nutritionists, pharmacists, perfusionists, surgeons and physicians. EEG (Electroencephalogram) Recording of the electrical activity of the brain. ET (Endotracheal tube) A tube placed in the windpipe that is connected to a ventilator. Heparin A drug used to prevent blood from clotting. LVAD (left ventricular assist device) This is a device that will assist the left side of the heart when it is failing. More information will be given to you if your family member is waiting for this device.
5 Oxygenator This is the artificial lung where carbon dioxide is removed and oxygen is added. Nasogastric (NG) tube A feeding tube that is passed through the nose and into the stomach. Platelets Cells in the blood that help stop bleeding by helping to form clots. Platelets are damaged and used up by the ECLS circuit. They are regularly monitored and replaced. RVAD (right ventricular assist device) This is a device that will assist the right side of the heart when it is failing. Tracheostomy A tube that is placed directly into the neck that leads to the lungs. This tube takes the place of the endotracheal tube that is placed in the mouth. The tracheostomy tube helps to protect the larynx, decreases the risk of infecting the lungs with germs from the mouth, is more comfortable for patients and allows easier management of the ventilator. Urgent/Emergent ECLS In many circumstances ECLS is initiated in patients who are extremely unstable and may be close to a cardiac arrest. Ventilator Breathing machine used to deliver oxygen to the lungs through a tube in the windpipe. It pushes air in and out of the lungs. Wean When the patient has shown improvement, we will decrease the support from the ECLS circuit and monitor how the patient s heart and/or lungs are functioning.
6 What is ECLS? ECLS stand for Extracorporeal Life Support. You may also hear the term ECMO which stands for Extracorporeal Membrane Oxygenation. ECLS is a broader term that includes ECMO. ECLS is a special procedure that takes over the work of the heart and/or lungs when they are too sick to properly support the body. ECLS allows the heart and/or lungs time to rest and heal. ECLS does not cure these organs, but allows them time to rest. ECLS is very similar to the machine used for open-heart operations. While those patients are on the machine for only hours, ECLS patients can be on the machine from days to even weeks. During ECLS, patients may appear to be better but you need to know that the person is still very sick and needs the ECLS machine for life support. Who needs ECLS? Patients who are considered for ECLS have severe heart and/or lung failure. They are not responding to standard medical treatments and unlikely to survive without exceptional treatment (ECLS). Often the breathing machine (ventilator) is in use with high settings and/ or a large amount of heart medicine is in use to maintain the blood pressure. The patients must have a reversible illness and good brain function for ECLS to have a chance of success. Most of our patients are sent to us from other hospitals. Many patients who are referred to us for ECLS do not actually receive this treatment. Once they are at our hospital our team will do a full evaluation of the patient s needs. Many will improve without the need for ECLS.
7 Some of the reasons that adults go on ECLS at our institution are: Pneumonia from lung infections ARDS- acute respiratory distress syndrome PE- pulmonary embolus MI- myocardial infarction (heart attack) Heart failure Heart arrhythmias After difficult heart operations After heart or lung transplantation What is emergent/urgent ECLS? This is an emergency ECLS response. We may receive a call from the Emergency Department, any of the Intensive Care Units, or Catheterization Labs. The patient is extremely unstable and may be close to cardiac arrest. The ECLS team will make the decision about going on bypass in these situations. These patients generally have their ECLS cannulae placed in the artery and vein in their groin. This is the fastest access.
8 How does ECLS work? Cannulae are placed in blood vessels in the patient s neck, chest and/or groin. They can be placed surgically, or they can be placed percutaneously. The ECLS surgeon will determine which method is required. These cannulae allow blood to be removed from the body and pumped back in and are attached to tubing that goes to the ECLS machine. The ECLS machine makes the blood flow through the tubing by the turning motion of the pump. How fast the blood goes depends on how fast the pump turns. This flow number may be high at the beginning meaning the machine is doing most of the work. As your loved one gets better, the flow may slowly be decreased because less support is needed. The amount of time this takes depends on how the heart and lungs heal. Depending on the requirements, oxygen may be added and carbon dioxide removed by an artificial lung (oxygenator). The blood is then warmed to body temperature and given back to your loved one through the tubing. If an oxygenator is used you may notice that the blood coming from your loved one will be dark because it contains little oxygen. The blood going back in will be bright red because it carries lots of oxygen. The blood is taken
9 out and given back at the same speed so your loved one s body doesn t miss the blood going through the tubing. Are there different types of ECLS? Yes. ECLS can be used for heart and lung support or for lung support only. The terms VA and VV refer to the blood vessels used in the treatment. Sometimes a person may start with one form of ECLS and need to be switched to another. VA ECMO: If the patient needs heart and/or lung support they will be placed on VA or VenoArterial ECMO. This is the type of bypass that is most like the system used in the operating room for heart operations. A cannula will be placed in a large artery and another cannula in a large vein. VV ECMO: If the patient needs lung support only they will be placed on VV or VenoVenous ECMO. The cannulae will be placed in large veins. Occasionally one cannula may be sufficient for VV ECMO. RVAD: If the patient needs support of the right side of the heart an RVAD or Right Ventricular Assist Device may be utilized. A cannula will be placed in a large vein and another in the pulmonary artery. This form of ECLS may be used in conjunction with an LVAD or Left Ventricular Assist Device or in conjunction with ECMO. RVAD/ECMO: If the patient needs support of the right side of the heart and the lungs an RVAD or Right Ventricular Assist Device may be utilized. A cannula will be placed in a large vein and another in the pulmonary artery. This form of ECLS may be used in conjunction with an LVAD or Left Ventricular Assist Device. This support requires the addition of an oxygenator (artificial lung) to the RVAD.
10 ECLS is an evolving field and there are other types of support that we may utilize now and in the future. What are the goals and what is the success? By taking over the work of the sick organ - heart and/or lungs, ECLS provides time for these organs to rest and heal. ECLS does not heal the organs. It only allows time for them to rest. ECLS will be used only after all other medical measures have been attempted. When the heart and/or lungs have healed, then the patient will be taken off ECLS. This can takes days to weeks in the adult patient. Some patients may be able to transition from ECLS to an LVAD, which is a long-term pump that lives inside the body. Before an LVAD is placed patients undergo extensive evaluations to ensure this is a suitable treatment. Some patients who are on the waiting list for a heart or lung transplant may receive these organs and be taken off ECLS. Patients undergo extensive evaluations before listing for heart or lung transplantation. ECLS is only utilized in extremely ill patients as a last resort. For all patients treated with ECLS, approximately 50 percent will survive. This risk varies depending on the underlying disease and the overall health of the patient. However, the risk of dying without ECLS is significantly greater than the risk of dying with it.
11 What are the risks? The risk of dying without ECLS is significantly greater than the risk of dying with it. The most common risk with ECLS is bleeding. This is because we continuously run a medication called heparin. It is very important that clots do not form in the ECLS circuit. Heparin thins the blood to prevent this. Bleeding can occur anywhere in the body while the patient is on heparin. Adults most commonly bleed from where the cannulae were placed. The most dangerous bleeding may occur in or around the brain. We are constantly monitoring for signs of bleeding and steps will be taken to slow any bleeding that happens including stopping heparin. If the bleeding increases, your loved one may need surgery. If there is too much bleeding, ECLS may need to be stopped. Clots may form in the circuit. Air bubbles may also enter the circuit. These may clog the circuit or get into the blood from the tubes and cause organ damage. This can even be fatal. Many safety measures are taken so this won t happen. Although every safety measure is taken, any part of the ECLS circuit can fail, rupture or malfunction. The ECMO Specialists are specially trained if this should occur. Patients on ECLS are at risk for having infections especially of the lungs and the blood stream. A risk of infection arises any time a tube is placed in the body, especially in a blood vessel. We are constantly monitoring for signs of infection. Antibiotics will be given if needed.
12 There is a risk for limb complications resulting from poor blood flow or oxygen delivery to the limbs. This is most common in patients with VA ECMO on the side with the arterial cannula but can affect any extremity. Patients requiring ECLS are extremely sick and their organs may start to fail due to inadequate blood supply or oxygen. The brain is the biggest concern for this. Other organs frequently affected are the kidneys and liver. Blood and blood products are needed often while on ECLS. The risks of getting blood transfusions are well known and our blood bank does many tests to make sure the blood is as safe as possible. However no test is 100 percent accurate. Who will be managing ECLS and taking care of my loved one? The ECLS team includes a large group of people from different specialties. Intensive care physicians (called intensivists) and cardiothoracic surgeons are frequently at the core of the team. Other members include nurses caring for your loved one, a respiratory therapist who takes care of the breathing machine and specialists who operate the ECLS machine. The team may ask other specialists to assist them including cardiologists (heart), neurologists (brain), pulmonologists (lungs), nephrologists (kidneys), infectious disease experts, nutritionists, pharmacists, physiotherapists etc. Each day members of the team will come to the bedside to talk about how your loved one is doing and the plan of care. These sessions are called rounds. We encourage you to take part in rounds by sharing your insights, questions and concerns. We
13 expect you to have questions about the care, and want to hear them. There are also people who are there to take care of you and your family. Ask your loved one s nurse to call the social worker if you need help dealing with issues like a place to stay, meal tickets, parking passes or have emotional needs. A chaplain and palliative care services are available. What happens during those days/weeks? A small subset of patients may not be on the ventilator when ECLS is initiated and may be able to remain off the ventilator. Most patients, however, will have already been placed on the ventilator. After ECLS is started, if possible, the ventilator is turned down to rest settings. This means we will decrease the oxygen levels and the amount of pressure used to keep the lungs inflated. This allows the lungs to rest. The patient s lungs will continue to be suctioned. After ECLS is started it may be possible to decrease the heart medications required to maintain the blood pressure thus allowing the heart to rest. The first couple of days on the ventilator frequently require the patient to be well sedated and even chemically paralyzed. We do this so that we can decrease the amount of oxygen their body uses. As soon as possible we will stop the paralyzing medication and let the patient wake up. We will ask them to squeeze our hands or move their feet. If they are comfortable we will try to allow them to remain awake and will treat their pain and anxiety.
14 For some patients it may be possible, over time, to remove them from the ventilator (extubate). Others may require a tracheostomy to be placed. The patient will receive a chest x-ray every morning. We will draw blood for labs routinely throughout the day. Sometimes a special procedure such as a heart catheterization, or a CT scan is required. We will take the patient to those areas of the hospital where these tests are performed. The ECLS Specialist and bedside nurse will always be with the patient during these road trips. These trips require careful planning due to the critical nature of the patient and the cumbersome nature of the machinery. Are they in pain? We try to make sure that your loved one is not in pain. They will be kept sedated with drugs such as morphine, lorazepan, and propofol. If possible we will wake the patient at least every day to make sure that they are ok. We will ask them to squeeze our hand or follow a command. Once they have done this we will continue with the pain medications. We encourage you to talk to your loved one. They may be able to hear you even if they cannot respond. Most patients do not remember this time in their lives. Some have been able to recall dreams or moments during this time. What kind of medications are used? Many types of medications are given while the patient is on ELCS. The following list is what you might see or hear most frequently. It is not a complete list. morphine/fentanyl These are used for pain.
15 lorazepam/versed/propofol/dexmedetomidine These are sedatives. They help decrease anxiety. atracurium This is a drug that paralyzes the muscles. We use this with critically ill patients to help reduce the amount of oxygen that their body uses. Once the patient is stable we will try and discontinue this drug. furosemide (Lasix) This medication helps to increase the urine output. vancomycin, gentamycin, cefazolin These are all antibiotics. There are many different antibiotics that may be used. pantoprazole This medication helps to protect the stomach against ulcers. dopamine, dobutamine, norepinephrine, epinephrine, vasopressin These medications are used to help increase the blood pressure. heparin This is the medication that thins the blood. It will take longer for the blood to form a clot. The ECLS Specialist monitors the level of clotting. The heparin dose will be increased or decreased based on the clotting time and the patient s condition. What about nutrition? While on ECLS your loved one will usually be fed through a tube that is placed through the nose or mouth to the intestines. The food we give through this tube is similar to Ensure or other liquid drinks like this. This fluid is delivered directly to the intestines. If we are unable to place the tube or your loved one does not tolerate being fed in this manner, we will use nutrition through the veins (Total Parenteral Nutrition- TPN). TPN will be given through an IV to the patient, or through the ECLS circuit. The amount of calories required is assessed several times a week.
16 What happens if the kidneys fail? If the patient s kidneys are unable to produce enough urine or function properly then we will help them with dialysis. Frequently the patient s kidney function returns in time and they do not require long term dialysis. What will my loved one look like on ECLS? The cannulae in the neck and the large amount of tubing in the ECLS circuit may be upsetting to look at. You may notice a breathing tube (endotracheal tube or ET tube) going into your loved one s mouth or nose. This will be attached to a breathing machine, which helps keep the lungs inflated. They will be attached to other routine monitoring equipment. Your loved one s head and body may look puffy. The puffiness (edema) is often seen in the eyelids and may limit how much they can open their eyes. The puffiness (edema) is generally caused by the therapies needed to support your loved one. How do you know if they will get better? We are watching for improvements every day. We will look at all aspects of heart and lung function. This would include blood pressure, chest x-rays, pulmonary mechanics (how much air is in the lungs, how easily they fill with air with each breath) blood gases, ECLS flow and many more. We will do what we call a wean from ECLS. If your loved one is on ECLS for lung support we will turn up the ventilator and cap off the oxygenators in the ECLS circuit. This will require the patient s lungs to do all the work. If the patient s condition remains good then
17 we will consider removing the patient from ECLS. If your loved one is on ECLS for heart support we will turn the ventilator to appropriate settings and reduce the ECLS flow. We will be watching the patient s blood pressure. We may have to add medications to help keep the blood pressure in an appropriate range. If everything looks good then we will consider removing ECLS at this time. If your loved one does not do well during the wean, ECLS is continued. The physician and staff taking care of your loved one will explain what we are looking at during these weans. The final trial is with ECLS removed. What happens once they are ready to come off ECLS? When it has been decided that the patient is ready to come off ECLS we will cut the circuit away from the cannulae. The ECLS cannulae will be removed (decannulated). This may require an operation. Your loved one may remain on a ventilator until they are able to breathe on their own again. This is different for every patient. It may take days or weeks. As the lungs improve, weaning from the ventilator will start. Physical therapy will start early and patients frequently require rehabilitation before going home. It is very important for us as well as your family member to be seen by our team a few times after they go home. We will schedule appointments for this. This is to make sure that everything is going as it should.
18 What happens if they do not get better? There is the chance that despite our best efforts, your loved one will not improve. We will talk to you frequently about the condition of your loved one. If the ECLS team feels that we have done everything possible for your loved one, but they are not getting better or are getting worse, they will sit down and talk with your family. Resources are available to you to help support your family during this difficult time. What about bridge to LVAD patients, or patients on the transplant waiting list? A select group of patients that have heart failure may be treated with a long term pump placed inside the body (LVAD). We will place these patients on ECLS until they are well enough to have the LVAD placed. The heart failure/lvad team will evaluate these patients before and after they are placed on ECLS. If your loved one is an LVAD candidate, more information will be given to you by the heart failure service. A select group of patients may be on the heart or lung transplant waiting list and require ECLS due to deterioration in their condition. They may still be candidates for transplantation. After transplantation the goal would be to discontinue ECLS though this may not always be possible. If your loved one is a transplant candidate, more information will be given to you by the transplant service. When can we visit and how can we help? After ECLS has started, and once the patient is stabilized, you will be able to visit.
19 All of our adult patients are managed in the ICU. You will be given the policies of the unit by the clerk or nurse taking care of your loved one. We will always try and let you come in as much as possible. Call at any time, day or night, to check on your loved one. We are always happy to talk to you and answer questions. Family plays an important part in recovery. While on ECMO, there are some things you can do to help: We encourage you to talk to your loved one and hold their hands. They may not be able to respond back to you but they may be able to hear you. Bring photographs, blankets, etc. Make tapes of you reading stories, singing songs, or talking. Bring them in or send them if you cannot be with your loved one right away. Children can draw or color pictures to be placed at the bedside or choose a small toy to send. Some units will let children visit. Ask the nurse. We do encourage you to rest, eat well and take care of yourselves. Getting sick yourself will not help either of you. Your family member may be off work for a long period of time. If there are any forms to be completed please let us know.
20 Notice: This information is considered for general use only. It should not be used instead of medical advice and care. If you have a specific health concern or care need, you should talk with your doctor. Rev. 4/15.
Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program
 PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
ECMO Extracorporeal Membrane Oxygenation
 ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
WELCOME. Welcome to the Children s Hospital PICU (Pediatric Intensive Care Unit). We consider it a privilege to care for your child and your family.
 ECMO FAMILY GUIDE WELCOME Welcome to the Children s Hospital PICU (Pediatric Intensive Care Unit). We consider it a privilege to care for your child and your family. This book was created to give you the
ECMO FAMILY GUIDE WELCOME Welcome to the Children s Hospital PICU (Pediatric Intensive Care Unit). We consider it a privilege to care for your child and your family. This book was created to give you the
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
About Your Ventricular Assist Device (VAD) Surgery
 About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
What You Need to Know about a Kidney Transplant
 Page 1 of 5 What You Need to Know about a Kidney Transplant This information will help you understand the risks, benefits and possible complications involved in a kidney transplant. Please read it carefully.
Page 1 of 5 What You Need to Know about a Kidney Transplant This information will help you understand the risks, benefits and possible complications involved in a kidney transplant. Please read it carefully.
Acute Respiratory Failure
 Acute Respiratory Failure For family, friends and caregivers of a patient with acute respiratory failure in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information
Acute Respiratory Failure For family, friends and caregivers of a patient with acute respiratory failure in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Thoracic Diagnostic Assessment Program. Patient information for. Last revised: November
 Thoracic Diagnostic Assessment Program Patient information for Last revised: November 2016 1 A list of your tests and appointments Diagnostic tests 2 3 4 Specialist appointments Doctor: Specialty: Notes:
Thoracic Diagnostic Assessment Program Patient information for Last revised: November 2016 1 A list of your tests and appointments Diagnostic tests 2 3 4 Specialist appointments Doctor: Specialty: Notes:
Esophagectomy Surgery
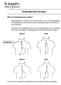 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Transplant Surgery. Patient Education Guide to Your Kidney/Pancreas Transplant Page 9-1. For a kidney/pancreas transplant. Before Your Surgery
 Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Giving your heart strength. Ventricular Assist Device.
 Giving your heart strength. Ventricular Assist Device. 1 National leader in Ventricular Assist Devices Although you may be nervous when considering heart surgery, you can rest assured knowing that UR Medicine
Giving your heart strength. Ventricular Assist Device. 1 National leader in Ventricular Assist Devices Although you may be nervous when considering heart surgery, you can rest assured knowing that UR Medicine
Intensive Care Diary. information. Radnor Ward. Salisbury NHS Foundation Trust
 information Intensive Care Diary Radnor Ward Salisbury NHS Foundation Trust Contents The purpose of your diary Intensive Care Diary Admission Day - What happened? Why am I here? Visitor s Blog / World
information Intensive Care Diary Radnor Ward Salisbury NHS Foundation Trust Contents The purpose of your diary Intensive Care Diary Admission Day - What happened? Why am I here? Visitor s Blog / World
Informed Consent for Liver Transplant Patients
 Informed Consent for Liver Transplant Patients Evaluation Process You will be evaluated with consultations, lab tests and various procedures to determine the medical appropriateness of liver transplant.
Informed Consent for Liver Transplant Patients Evaluation Process You will be evaluated with consultations, lab tests and various procedures to determine the medical appropriateness of liver transplant.
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
For family, friends and caregivers of a patient with pneumonia in the Medical Surgical Intensive Care Unit (MSICU)
 Form: D-5206 Pneumonia For family, friends and caregivers of a patient with pneumonia in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Form: D-5206 Pneumonia For family, friends and caregivers of a patient with pneumonia in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
A VIDEO SERIES. living WELL. with kidney failure KIDNEY TRANSPLANT
 A VIDEO SERIES living WELL with kidney failure KIDNEY TRANSPLANT Contents 2 Introduction 3 What will I learn? 5 Who is on my healthcare team? 6 What is kidney failure? 6 What treatments are available
A VIDEO SERIES living WELL with kidney failure KIDNEY TRANSPLANT Contents 2 Introduction 3 What will I learn? 5 Who is on my healthcare team? 6 What is kidney failure? 6 What treatments are available
UW MEDICINE PATIENT EDUCATION. Hemodialysis. A treatment option for kidney disease. Treatment Options for Kidney Disease
 UW MEDICINE PATIENT EDUCATION Hemodialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and care of blood access. 2. Understand the purpose and basic principles of hemodialysis.
UW MEDICINE PATIENT EDUCATION Hemodialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and care of blood access. 2. Understand the purpose and basic principles of hemodialysis.
Subtotal and Total Gastrectomy
 DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
Clinic Procedures. After your heart transplant. Lab Tests
 UW MEDICINE PATIENT EDUCATION Clinic Procedures After your heart transplant We hope your new heart puts you on the road to a productive, healthy, and happy life. To be sure you and your heart are doing
UW MEDICINE PATIENT EDUCATION Clinic Procedures After your heart transplant We hope your new heart puts you on the road to a productive, healthy, and happy life. To be sure you and your heart are doing
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
A VIDEO SERIES. living WELL. with kidney failure WHAT IS KIDNEY FAILURE?
 A VIDEO SERIES living WELL with kidney failure WHAT IS KIDNEY FAILURE? Contents 2 Introduction 11 What is a kidney transplant? 3 What will I learn? 12 What role do diet and medi- 5 Who is on my 7 healthcare
A VIDEO SERIES living WELL with kidney failure WHAT IS KIDNEY FAILURE? Contents 2 Introduction 11 What is a kidney transplant? 3 What will I learn? 12 What role do diet and medi- 5 Who is on my 7 healthcare
Retroperineal Lymph Node Dissection (RPLND)
 Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Surgery. Patient Education Transplant Services. For a kidney/pancreas transplant
 Patient Education Surgery For a kidney/pancreas transplant By the time you have surgery, you may have been waiting for some time. It will help to read this section before surgery so you will know what
Patient Education Surgery For a kidney/pancreas transplant By the time you have surgery, you may have been waiting for some time. It will help to read this section before surgery so you will know what
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Is a LVAD the Right Treatment for Me? Decision Aid
 Is a LVAD the Right Treatment for Me? Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand what the LVAD treatment
Is a LVAD the Right Treatment for Me? Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand what the LVAD treatment
Pacemaker and AV Node Ablation Patient Information
 Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Emphysema. Lungs The lungs help us breathe in oxygen and breathe out carbon dioxide. Everyone is born with 2 lungs: a right lung and a left lung.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects millions of people worldwide. Emphysema involves damage to the air sacs in the lungs. This makes
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects millions of people worldwide. Emphysema involves damage to the air sacs in the lungs. This makes
LUNG SURGERY. Treatment for Lung Problems
 LUNG SURGERY Treatment for Lung Problems When You Need Lung Surgery Your doctor is recommending surgery for your lung problem. Surgery alone may treat your problem. Or you may need other treatments as
LUNG SURGERY Treatment for Lung Problems When You Need Lung Surgery Your doctor is recommending surgery for your lung problem. Surgery alone may treat your problem. Or you may need other treatments as
Treatment Options Not Not access
 Treatment Options Treatment options for Chronic Kidney Disease (CKD) CKD is a permanent condition. Treatment will: Help the patient feel better Not cure the disease Not make the kidneys start working again
Treatment Options Treatment options for Chronic Kidney Disease (CKD) CKD is a permanent condition. Treatment will: Help the patient feel better Not cure the disease Not make the kidneys start working again
Pneumonia. Trachea , The Patient Education Institute, Inc. id Last reviewed: 11/11/2017 1
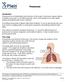 Pneumonia Introduction Pneumonia is an inflammation and infection of the lungs. Pneumonia causes millions of deaths every year. It can affect anybody, but is more dangerous to older adults, babies and
Pneumonia Introduction Pneumonia is an inflammation and infection of the lungs. Pneumonia causes millions of deaths every year. It can affect anybody, but is more dangerous to older adults, babies and
What You Need to Know about a Heart Transplant
 Page 1 of 8 What You Need to Know about a Heart Transplant This information will help you understand the risks, benefits, and possible complications involved in a heart transplant. Please read it carefully.
Page 1 of 8 What You Need to Know about a Heart Transplant This information will help you understand the risks, benefits, and possible complications involved in a heart transplant. Please read it carefully.
Treatment choices for someone with Stage 5 kidney disease are:
 Information for patients about advanced kidney disease Dialysis and non-dialysis treatments DOCUMENT PREPARED FOR This information is to help you understand some key issues about dialysis; it is designed
Information for patients about advanced kidney disease Dialysis and non-dialysis treatments DOCUMENT PREPARED FOR This information is to help you understand some key issues about dialysis; it is designed
Iowa Methodist Medical Center Transplant Center. Informed Consent for Kidney Transplant Recipient
 Iowa Methodist Transplant Center Iowa Methodist Medical Center Transplant Center 1215 Pleasant Street, Suite 506 Des Moines, IA 50309 515-241-4044 Phone 515-241-4100 Fax Iowa Methodist Medical Center Transplant
Iowa Methodist Transplant Center Iowa Methodist Medical Center Transplant Center 1215 Pleasant Street, Suite 506 Des Moines, IA 50309 515-241-4044 Phone 515-241-4100 Fax Iowa Methodist Medical Center Transplant
Thoracoscopy for Lung Cancer
 Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Type 2 Diabetes. Care for your body today for a healthier tomorrow
 Type 2 Diabetes Care for your body today for a healthier tomorrow Understanding diabetes You may already know that having diabetes means you have too much sugar in your blood. Why do you have high blood
Type 2 Diabetes Care for your body today for a healthier tomorrow Understanding diabetes You may already know that having diabetes means you have too much sugar in your blood. Why do you have high blood
UW MEDICINE REGIONAL HEART CENTER HEART TRANSPLANT. Orientation Class at University of Washington Medical Center
 UW MEDICINE REGIONAL HEART CENTER HEART TRANSPLANT Orientation Class at University of Washington Medical Center OVERVIEW This slideshow explains: Your Transplant Evaluation Transplant Listing Heart Transplant
UW MEDICINE REGIONAL HEART CENTER HEART TRANSPLANT Orientation Class at University of Washington Medical Center OVERVIEW This slideshow explains: Your Transplant Evaluation Transplant Listing Heart Transplant
Gastroscopy Instructions
 Patient information Gastroscopy Instructions i Important pre operative information for all patients. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Patient information Gastroscopy Instructions i Important pre operative information for all patients. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
E09 PEG. Expires end of March 2018 VITALITY.CO.UK
 VITALITY.CO.UK E09 PEG Expires end of March 2018 You can get more information and share your experiences at www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org eidohealthcare.com
VITALITY.CO.UK E09 PEG Expires end of March 2018 You can get more information and share your experiences at www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org eidohealthcare.com
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Coronary angioplasty and stents
 Tests and Procedures Coronary angioplasty and stents By Mayo Clinic Staff Coronary angioplasty (AN-jee-o-plas-tee), also called percutaneous coronary intervention, is a procedure used to open clogged heart
Tests and Procedures Coronary angioplasty and stents By Mayo Clinic Staff Coronary angioplasty (AN-jee-o-plas-tee), also called percutaneous coronary intervention, is a procedure used to open clogged heart
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs
 Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Lung Surgery: Thoracoscopy
 Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Talking with your doctors about palliative care Dr. Mary Anne Huggins and Barbara Pidcock
 Talking with your doctors about palliative care Dr. Mary Anne Huggins and Barbara Pidcock You will have appointments with your family doctor, and with specialists. It will help you if you write your brief
Talking with your doctors about palliative care Dr. Mary Anne Huggins and Barbara Pidcock You will have appointments with your family doctor, and with specialists. It will help you if you write your brief
Getting Knowledge About Kidney Disease
 Last Reviewed Getting Knowledge About Kidney Disease Have you been told that you have late stage kidney disease? Choose Your Lifestyle On Dialysis There are two kinds of dialysis. Dialysis can be done
Last Reviewed Getting Knowledge About Kidney Disease Have you been told that you have late stage kidney disease? Choose Your Lifestyle On Dialysis There are two kinds of dialysis. Dialysis can be done
Ventricular Assist Devices (VAD)
 Patient & Family Guide 2018 Ventricular Assist Devices (VAD) Aussi disponible en français : Dispositifs d assistance ventriculaire (DAV) (FF85-1853) www.nshealth.ca Ventricular Assist Devices (VAD) How
Patient & Family Guide 2018 Ventricular Assist Devices (VAD) Aussi disponible en français : Dispositifs d assistance ventriculaire (DAV) (FF85-1853) www.nshealth.ca Ventricular Assist Devices (VAD) How
Heart catheterization for adults with congenital heart disease
 Heart catheterization for adults with congenital heart disease What is a heart catheterization? It is a procedure that provides details about your heart function and circulation. It helps your doctor make
Heart catheterization for adults with congenital heart disease What is a heart catheterization? It is a procedure that provides details about your heart function and circulation. It helps your doctor make
Gastroscopy instructions
 Golden Jubilee National Hospital NHS National Waiting Times Centre Gastroscopy instructions Pre operative patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Golden Jubilee National Hospital NHS National Waiting Times Centre Gastroscopy instructions Pre operative patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Transarterial Chemoembolization (TACE)
 Transarterial Chemoembolization (TACE) Princess Margaret Know what to expect Read this booklet to learn: What TACE is...1 How TACE works...2 The benefits of TACE...3 The risks and side effects of TACE...3
Transarterial Chemoembolization (TACE) Princess Margaret Know what to expect Read this booklet to learn: What TACE is...1 How TACE works...2 The benefits of TACE...3 The risks and side effects of TACE...3
Lung Cancer Resection
 Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Golden Jubilee National Hospital Cardiac catheterisation or coronary angioplasty/stenting
 Golden Jubilee National Hospital NHS National Waiting Times Centre Cardiac catheterisation or coronary angioplasty/stenting Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000
Golden Jubilee National Hospital NHS National Waiting Times Centre Cardiac catheterisation or coronary angioplasty/stenting Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000
Glossary. Anesthesiologist A doctor who puts you or parts of your body to sleep during surgery.
 1-Glossary Glossary Acute rejection A type of rejection that occurs when immune cells from your body attack the transplanted organ(s). Acute rejection may occur at any time after a transplant. But it usually
1-Glossary Glossary Acute rejection A type of rejection that occurs when immune cells from your body attack the transplanted organ(s). Acute rejection may occur at any time after a transplant. But it usually
Colonic (Large Intestine) Manometry
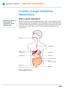 Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Having a gastroscopy A guide for patients and their carers
 Having a gastroscopy A guide for patients and their carers Contents Welcome to the integrated procedures unit....1 Why do I need a gastroscopy?...1 What is the benefit of a gastroscopy?...2 Are there any
Having a gastroscopy A guide for patients and their carers Contents Welcome to the integrated procedures unit....1 Why do I need a gastroscopy?...1 What is the benefit of a gastroscopy?...2 Are there any
Arch Angiography. Exceptional healthcare, personally delivered
 Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Insertion of a Haemodialysis Catheter
 Insertion of a Haemodialysis Catheter Exceptional healthcare, personally delivered Introduction This leaflet is about the procedure required to put in a temporary dialysis catheter. It is intended to give
Insertion of a Haemodialysis Catheter Exceptional healthcare, personally delivered Introduction This leaflet is about the procedure required to put in a temporary dialysis catheter. It is intended to give
California Cardiovascular Consultants Medical Associates
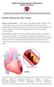 Patient information: Heart Attack What is a heart attack? A heart attack, also called myocardial infarction, or MI, is what happens when one of the arteries that supply blood to the heart gets blocked.
Patient information: Heart Attack What is a heart attack? A heart attack, also called myocardial infarction, or MI, is what happens when one of the arteries that supply blood to the heart gets blocked.
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
Heart Disease. Signs and Symptoms
 Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
ANGIOPLASTY AND STENTING
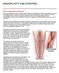 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
Having CT Enterography Information for Patients
 Having CT Enterography Information for Patients In this leaflet: Introduction 2 What is CT Enterography?.....2 How does it work?. 2 Are there any risks?.3 Are there any alternatives to CT Enterography?..3
Having CT Enterography Information for Patients In this leaflet: Introduction 2 What is CT Enterography?.....2 How does it work?. 2 Are there any risks?.3 Are there any alternatives to CT Enterography?..3
Haemodialysis. Patient Information. Working together for better patient information. Health & care information you can trust. The Information Standard
 Haemodialysis Patient Information Health & care information you can trust The Information Standard Certified Member Working together for better patient information Haemodialysis (HD) helps to remove the
Haemodialysis Patient Information Health & care information you can trust The Information Standard Certified Member Working together for better patient information Haemodialysis (HD) helps to remove the
Kidney Disease Treatment Options
 Page 1 Fact sheet The kidneys play a number of important roles in your body such as: extracting excess water to make urine (wee) controlling your blood pressure filtering waste products and toxins from
Page 1 Fact sheet The kidneys play a number of important roles in your body such as: extracting excess water to make urine (wee) controlling your blood pressure filtering waste products and toxins from
PERCUTANEOUS BILIARY DRAINAGE
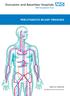 PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
CORONARY ARTERY PROCEDURES
 CORONARY ARTERY PROCEDURES Cardiac Catheterization, Stenting, and Bypass Surgery Coronary Artery Disease Your doctor has told you that you may have coronary artery disease (CAD). Having CAD means that
CORONARY ARTERY PROCEDURES Cardiac Catheterization, Stenting, and Bypass Surgery Coronary Artery Disease Your doctor has told you that you may have coronary artery disease (CAD). Having CAD means that
Epidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal
 Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
Information for patients pidurals and spinals: information about their operation for anyone who may benefit from an epidural or spinal This leaflet has been made using information from the Royal College
KIDNEY TRANSPLANT - A TREATMENT OPTION
 KIDNEY TRANSPLANT - A TREATMENT OPTION Page 1/5 WHAT IS A KIDNEY TRANSPLANT? When kidney failure becomes very advanced, your kidneys are so damaged they can no longer do their job. A transplant is a treatment
KIDNEY TRANSPLANT - A TREATMENT OPTION Page 1/5 WHAT IS A KIDNEY TRANSPLANT? When kidney failure becomes very advanced, your kidneys are so damaged they can no longer do their job. A transplant is a treatment
Transcatheter Aortic Valve Implantation:
 Transcatheter Aortic Valve Implantation: Information for Patients and Families FD.635.D356.PHC (R.May-18) cover1 Transcatheter Aortic Valve Implantation: Information for Patients and Families Previously
Transcatheter Aortic Valve Implantation: Information for Patients and Families FD.635.D356.PHC (R.May-18) cover1 Transcatheter Aortic Valve Implantation: Information for Patients and Families Previously
Sinclair Community College, Division of Allied Health Technologies
 Sinclair Community College, Division of Allied Health Technologies Health Promotion for Community Health Workers Cardiovascular disease, stroke, and cancer Class #9 Heart Failure (date) Course Objectives:
Sinclair Community College, Division of Allied Health Technologies Health Promotion for Community Health Workers Cardiovascular disease, stroke, and cancer Class #9 Heart Failure (date) Course Objectives:
Advice to patients having an angioplasty
 What is an angioplasty? Advice to patients having an angioplasty An angioplasty is an x ray procedure to open a narrowed or blocked artery in order to improve blood flow. It involves inserting a long tube
What is an angioplasty? Advice to patients having an angioplasty An angioplasty is an x ray procedure to open a narrowed or blocked artery in order to improve blood flow. It involves inserting a long tube
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Closing your Patent Ductus Arteriosus (PDA)
 Closing your Patent Ductus Arteriosus (PDA) Information for patients and families Read this booklet to learn: what a PDA is why it should be closed what to expect with this procedure what follow-up care
Closing your Patent Ductus Arteriosus (PDA) Information for patients and families Read this booklet to learn: what a PDA is why it should be closed what to expect with this procedure what follow-up care
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Your anaesthetic for major surgery
 Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Transjugular Liver Biopsy UHB is a no smoking Trust
 Transjugular Liver Biopsy UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction, benefits and alternatives
Transjugular Liver Biopsy UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Introduction, benefits and alternatives
If You Have Head or Neck Cancer
 EASY READING If You Have Head or Neck Cancer What is head and neck cancer? Cancer can start any place in the body. Cancer that starts in the head and neck can have many names. It depends on where the cancer
EASY READING If You Have Head or Neck Cancer What is head and neck cancer? Cancer can start any place in the body. Cancer that starts in the head and neck can have many names. It depends on where the cancer
DIABETES AND CHRONIC KIDNEY DISEASE
 DIABETES AND CHRONIC KIDNEY DISEASE Stage 5 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
DIABETES AND CHRONIC KIDNEY DISEASE Stage 5 www.kidney.org National Kidney Foundation's Kidney Disease Outcomes Quality Initiative Did you know that the National Kidney Foundation's Kidney Disease Outcomes
LVAD, RVAD, BiVAD, Total Artificial Heart
 UW MEDICINE PATIENT EDUCATION Mechanical Circulatory Support (MCS) Surgery: LVAD, RVAD, BiVAD, Total Artificial Heart Your follow-up care This handout explains follow-up care after your mechanical circulatory
UW MEDICINE PATIENT EDUCATION Mechanical Circulatory Support (MCS) Surgery: LVAD, RVAD, BiVAD, Total Artificial Heart Your follow-up care This handout explains follow-up care after your mechanical circulatory
Having a radiologically inserted gastrostomy. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Having a radiologically inserted gastrostomy An information guide Having a radiologically inserted gastrostomy Introduction This leaflet
Having a PEG tube inserted Information for patients and carers
 Sunderland Day Case Centre Endoscopy Having a PEG tube inserted Information for patients and carers www.medway.nhs.uk Checklist Things to remember before your procedure Read the booklet carefully. Fill
Sunderland Day Case Centre Endoscopy Having a PEG tube inserted Information for patients and carers www.medway.nhs.uk Checklist Things to remember before your procedure Read the booklet carefully. Fill
About general anaesthesia Day Surgery Unit Patient Information Leaflet
 About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
ICD Implantation Patient Information
 Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
more intense treatments are needed to get rid of the infection.
 What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
Computerised Tomography (CT) Coronary Angiogram
 Computerised Tomography (CT) Coronary Angiogram Radiology Department Patient information leaflet This leaflet tells you about having a CT Coronary Angiogram (CTCA) scan. It explains what is involved and
Computerised Tomography (CT) Coronary Angiogram Radiology Department Patient information leaflet This leaflet tells you about having a CT Coronary Angiogram (CTCA) scan. It explains what is involved and
Thrombolysis and thrombectomy
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Thrombolysis and thrombectomy This information sheet explains about how a blood is diagnosed and the various forms
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Thrombolysis and thrombectomy This information sheet explains about how a blood is diagnosed and the various forms
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft
 Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
PNEUMONIA. Your Treatment and Recovery
 PNEUMONIA Your Treatment and Recovery Understanding Pneumonia Symptoms of Pneumonia Do you feel feverish and tired, with a cough that won t go away? If so, you may have pneumonia. This is a lung infection
PNEUMONIA Your Treatment and Recovery Understanding Pneumonia Symptoms of Pneumonia Do you feel feverish and tired, with a cough that won t go away? If so, you may have pneumonia. This is a lung infection
For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU)
 Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Anaesthetic choices for hip or knee replacement
 Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
CT Guided Lung Biopsy. A guide for patients undergoing biopsy
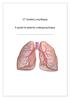 CT Guided Lung Biopsy A guide for patients undergoing biopsy Introduction The aim of this booklet is to: Answer your questions about CT guided lung biopsy Explain why you need the test Describe what is
CT Guided Lung Biopsy A guide for patients undergoing biopsy Introduction The aim of this booklet is to: Answer your questions about CT guided lung biopsy Explain why you need the test Describe what is
Patient Information. Preventing and treating blood clots
 Patient Information Preventing and treating blood clots 1_Clexane_Patient_Booklet_AW05.indd 1 8/04/2016 11:26 a The information provided in this document is for patients prescribed CLEXANE, and should
Patient Information Preventing and treating blood clots 1_Clexane_Patient_Booklet_AW05.indd 1 8/04/2016 11:26 a The information provided in this document is for patients prescribed CLEXANE, and should
Computerised Tomography Pulmonary Angiography (CTPA)
 Computerised Tomography Pulmonary Angiography (CTPA) Radiology Department Patient information leaflet This leaflet tells you about having a CT Pulmonary Angiography (CTPA) scan. If you have any questions
Computerised Tomography Pulmonary Angiography (CTPA) Radiology Department Patient information leaflet This leaflet tells you about having a CT Pulmonary Angiography (CTPA) scan. If you have any questions
ECLS as Bridge to Transplant
 ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
RADIATION THERAPY RADIATION THERAPY. In this section, you will learn about:
 RADIATION THERAPY RADIATION THERAPY In this section, you will learn about: How radiation therapy works What to expect from your CT planning appointment What to expect from your treatments Your radiation
RADIATION THERAPY RADIATION THERAPY In this section, you will learn about: How radiation therapy works What to expect from your CT planning appointment What to expect from your treatments Your radiation
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
