TRAUMATIC EMERGENCIES
|
|
|
- Diane Wiggins
- 6 years ago
- Views:
Transcription
1 TRAUMATIC EMERGENCIES I. General. A. Follow General Principles/Routine Care protocol unless otherwise indicated. B. Limit scene time for trauma patients, with goal of 15 minutes. C. See Appendix B for Trauma Triage destination procedures. II. Traumatic Hypovolemic Shock. Adult and Pediatric. A. Control hemorrhage. For external hemorrhage, use direct pressure, wound packing, pressure dressings, and tourniquets as necessary: 1. Consider using hemostatic gauze to control bleeding if the pressure dressing does not work. 2. For exsanguinating extremity hemorrhage, consider early use of tourniquets. Mark time applied on the tourniquet(s) and consider Pain Management protocol as necessary, unless patient is in decompensated shock. Contact the Receiving Facility to inform them a tourniquet has been applied. B. Transport patient in the supine position as soon as possible. C. Immobilize as needed (See General Principles, Section VII). D. Keep patient warm by controlling the ambulance temperature and use adjuncts (e.g. heat packs and reflective blankets) when necessary. E. Initiate fluid resuscitation. 1. Adult: a. Large bore I V(s) or IO(s) with warm NS or LR. b. If suspected uncontrolled internal hemorrhage, titrate to a state of relative hypotension with systolic BP of c. If suspected Traumatic Brain Injury (TBI) titrate fluids to maintain systolic BP > 90. d. If hemorrhage is controlled, but signs and symptoms of shock are present, greater amounts of fluids may be infused. 2. Pediatric: a. Large bore IV(s) or IO(s) with warm NS or LR. b. Push 20 ml/kg initially, then c. Titrate infusion rate to restore adequate perfusion (i.e. capillary refill, central and peripheral pulses, appropriate mentation for age). III. CNS and facial trauma. A. Administer O2 at 15 l/nrb mask if patient is breathing adequately on own. If patient is not breathing adequately and has a Traumatic Brain Injury (TBI), ventilate with high flow O2 at 10 breaths/min. for adults, 20 breaths/min. for 24
2 children and 25 breaths/min. for infants. If Increased Intracranial Pressure (IICP) (widening pulse pressure, decreased HR and increased BP, posturing, blown pupil, change in respiratory pattern) is associated with the TBI, ventilate at 20 breaths/min. for adults, 25 breaths/min. for children and 30 breaths/min. for infants. B. Keep pulse oximetry 95%. Intubate PRN. No nasal intubation with significant facial trauma. Follow RSI protocol if needed (Appendix F). Keep EtCO2 level between mmhg for TBI, and between mmhg for TBI with IICP if able to monitor. C. Immobilize as needed (See General Principles, Section VII). D. For partially avulsed teeth, replace if possible if patient is awake. For completely avulsed teeth, rinse with saline, and wrap in gauze soaked with saline. Be alert for potential tooth aspiration. E. Initiate fluid resuscitation. F. For seizures. 1. Adult: a. 1 st choice- May use midazolam, 10 mg for > 40 kg, single dose IM, or b. 2 nd choice- May use midazolam, 0.2 mg/kg of a 5 mg/ml concentration IN, or c. 3 rd choice- May use midazolam, 2 mg increments IV to a maximum dose of 0.1mg/kg or 10 mg (whichever is less), or d. 4 th choice- May use diazepam, 0.2 mg/kg/dose not to exceed 10 mg IV push; may repeat dose once. e. Wait 1-2 minutes between IN/IV doses to evaluate response. 2. Pediatric: a. 1 st choice- May use midazolam, 5 mg for kg, single dose IM, or b. 2 nd choice- May use midazolam, 0.2 mg/kg of a 5 mg/ml concentration IN, to a maximum dose of 10 mg, or c. 3 rd choice- May use midazolam, 0.1 mg/kg IV slowly over 2 minutes in no greater than 2 mg increments not to exceed 5 mg, or d. 4 th choice- May use diazepam, 0.2 mg/kg/dose not to exceed 10 mg IV push; may repeat dose once. e. Wait 1-2 minutes between IN/IV doses to evaluate response. IV. Spinal Trauma. A. Assess for neuro deficits in extremities. B. Be prepared to assist ventilations if a high spinal cord injury occurred. C. Keep patient warm by controlling the ambulance temperature and use adjuncts (e.g. heat packs and reflective blankets) when necessary. 25
3 D. Initiate fluid resuscitation. V. Injuries to the Neck. A. Seal open wounds with an occlusive dressing. B. Consider early intubation when signs of expanding hematoma are present. C. Initiate fluid resuscitation. D. Airway obstruction. 1. Keep traumatic tracheostomy open with any appropriate adjunct. 2. Perform a needle/surgical cricothyrotomy if trachea and/or larynx is collapsed or laryngeal edema is obstructing the airway. VI. Injuries to the Eye. A. Protect injured eye; consider use of a rigid shield. B. Cover/bandage unaffected eye. C. Stabilize impaled objects. D. Do not use a pressure dressing to stop fluid leakage or apply pressure to the eye. E. Elevate head if the patient is not hypotensive. F. Chemical burns to the eye: 1. Continuously flush with copious amounts of water or saline solution from inside to outside. 2. Attempt to identify agent if possible, and/or take a picture of the container. G. Consider antiemetic prophylactically. VII. Chest/Abdominal Trauma. A. Assess/monitor quality of breathing. B. Monitor for development of tension pneumothorax. C. Initiate fluid resuscitation. D. ECG monitor enroute. E. Specific injuries. 1. Open chest wounds/tension pneumothorax. a. Monitor and assist ventilations PRN. 26
4 b. Seal with occlusive dressing. Burp dressing if tension pneumothorax develops. c. Perform needle thoracostomy if the patient is hypotensive and has suspected tension pneumothorax. 2. Flail chest. a. Monitor and assist ventilations PRN. b. Monitor for tension pneumothorax. c. Stabilize with tape and bulky dressing. d. Consider intubation PRN. 3. Pulmonary contusion. a. Monitor and assist ventilations PRN. b. Consider use of CPAP if the patient is unable to maintain adequate ventilation. 4. Cardiac tamponade. Consider pericardiocentesis. 5. Abdominal injuries. a. Evisceration: Cover with sterile, moist, occlusive dressing. b. Consider transport with knees flexed/position of comfort. VIII. Musculoskeletal Trauma. A. Dress wounds, monitor perfusion (pulse and/or capillary refill), motor, sensory status before and after splinting. 1. Fractures/Dislocations. a. Splint in the position found. b. If there is severe deformity or the distal extremity is cyanotic or lacks pulses, align with gentle manipulation to achieve return of circulation before splinting. 2. Control hemorrhage. 3. Refer to Pain Management protocol for other considerations. B. Femur, hip or pelvic fracture/dislocation suspected. 1. Stabilize on long backboard. Consider use of scoop stretcher to move the patient. 2. Consider traction device for isolated mid-shaft femur fractures (open or closed). 3. Consider use of pelvic wrap (sheet or commercial device) for stabilization of pelvic fractures. 4. Initiate fluid resuscitation. a. Adult: See Section II.E.1. b. Pediatric: See Section II.E Refer to Pain Management protocol for other considerations. C. Acute low back discomfort without spinal trauma. 1. Consider use of ice/warm packs over area to relieve discomfort. 2. Refer to Pain Management protocol for other considerations. 27
5 IX. Amputated Parts. A. Collect parts and debride gross contaminants with saline flush. B. Wrap in sterile saline moistened gauze, place in plastic bag, protect with towel, place on ice. C. Label bag with patient name, date, and time. Send amputated part with patient if available. Note disposition of amputated part on PCR. D. Refer to Pain Management protocol for other considerations. X. Impaled Objects. A. Do not remove unless the airway is compromised. B. Secure the object in place. C. Taser darts will be removed by EMS personnel only if EMS was already dispatched to the scene for a medical/trauma event. XI. Burns. A. Thermal. 1. Consider early intubation PRN, insert an NG/OG tube if patient is intubated. 2. Stop the burning process, irrigate with room-temperature water if necessary. 3. Remove constricting jewelry, and annotate on PCR to whom the jewelry was given. 4. Elevate burned extremities on pillows above level of the heart and monitor distal pulses. 5. Apply dry, sterile non-adherent dressings and/or clean sheets. 6. Keep patient warm. 7. Initiate fluid resuscitation with large bore IV(s) and warmed NS or LR. a. Use the Parkland Formula to calculate IV drip rate as fluid resuscitation in the burn patient is paramount. 4 ml x kg x % of 2 nd and 3 rd degree body surface area burned. b. Half of this calculated total mls will be given in the first 8 hours from the time the patient was burned, so the drip rate per hour must be calculated on that. 8. Refer to Pain Management protocol for other considerations. 9. Consider anxiety relief. a. Diazepam 2-10 mg IV/IO, or b. Midazolam i. Adult: a) 0.2 mg/kg of a 5 mg/ml concentration IN, or b) 2 mg increments IV/IO to a maximum dose of 0.1 mg/kg or 10 mg (whichever is less) or c) 5 mg IM; may repeat once in minutes. ii. Pediatric: a) 0.2 mg/kg of a 5 mg/ml concentration IN, to a maximum dose of 5 mg, or 28
6 b) 0.2 mg/kg IM, to a maximum of 5 mg, or c) 0.1 mg/kg IV slowly over 2 minutes in no greater than 2 mg increments not to exceed 5 mg. d) Contact Mary Bridge Base Station for direction if unsure. 10. Consider transport from the scene to Harborview if burn is: a. > 20% 2 nd or 3 rd degree burns TBSA in any patient, or b. >10% 2 nd or 3 rd degree burns TBSA in patients 8 or > 65 years old, or c. Involving face, hands, feet, genitalia, perineum, or major joints. B. Electrical. 1. Ensure source is deactivated. 2. Apply dry, sterile non-adherent dressings and/or clean sheets. 3. Elevate burned extremities on pillows above level of the heart and monitor distal pulses. 4. Initiate fluid resuscitation with large bore IV(s) and warmed NS or LR. a. Use the Parkland Formula to calculate IV drip rate as fluid resuscitation in the burn patient is paramount. 4 ml x kg x % of 2 nd and 3 rd degree body surface area burned. Electrical injuries use 4 ml for Adults and Pediatrics. b. Half of this calculated total mls will be given in the first 8 hours from the time the patient was burned, so the drip rate per hour must be calculated on that. 5. Intubate PRN, insert an NG/OG tube if patient is intubated. 6. Acquire 12-lead ECG. Monitor ECG/treat dysrhythmias according to AHA Handbook when appropriate. 7. Consider transport from the scene to Harborview if burn is: a. >20% 2 nd or 3 rd degree burns TBSA in any patient, or b. >10% 2 nd or 3 rd degree burns TBSA in patients 8 or > 65 years old, or c. Involving face, hands, feet, genitalia, perineum, or major joints. C. Chemical (Consult Dept. of Transportation Emergency Response Guidebook). 1. Avoid self-contamination. 2. Remove all clothing. 3. Remove constricting jewelry, and annotate on PCR to whom the jewelry was given. 4. Dry powder; brush off if needed. 5. Flush copiously with water. 6. Elevate burned extremities on pillows above level of the heart and monitor distal pulses. Avoid spreading contamination on adjacent tissue. 7. Attempt to identify chemical if possible, and/or take a picture of the container. 8. Intubate PRN, insert an NG/OG tube if patient is intubated. 9. Consider transport from the scene to Harborview if burn is: a. > 20% 2 nd or 3 rd degree burns TBSA in any patient, or b. >10% 2 nd or 3 rd degree burns TBSA in patients 8 or > 65 years old, or c. Involving face, hands, feet, genitalia, perineum, or major joints. 29
7 XII. Crush Injury Syndrome (CIS)/Traumatic Rhabdomyolysis (TR). It is imperative that patients be pretreated before extrication or movement, therefore assessment of extremities (in the position found) for symptoms of CIS/TR must be accomplished initially. A patient pinned or entrapped with at least one major limb having arterial circulatory compromise for at least 4 hours should be considered for CIS/TR. Patients with CIS/TR may not survive if treatment is not initiated before removal from the situation. A. Manage airway as indicated. If RSI is necessary, do not use succinylcholine; consider vecuronium 0.1 mg/kg IV/IO or rocuronium 1 mg/kg IV/IO. B. Administer O2 with NRB mask at LPM. C. Give albuterol 2.5 mg in 3 ml NS SVN continuously. D. Administer IV: 1000 ml NS with sodium bicarbonate 100 meq (label bag) mixed in. Volume replacement and pre-alkalization should take place immediately after CIS identified. Set drip rate to infuse at 1500 ml/hour. E. Monitor ECG/treat dysrhythmias according to AHA Handbook when appropriate. F. Stabilize excitable cardiac tissue with calcium gluconate 10%, 3 g IV/IO or calcium chloride 10%, 1000 mg (1g) IV/IO push over 5 minutes. Consider 2 nd dose after 20 minutes. Don t mix in the same IV line as the bicarb drip. G. Consider midazolam 2 mg increments IV/IO to a maximum dose of 0.1 mg/kg or 10 mg for sedation. H. Refer to Pain Management protocol for other considerations. I. If prolonged extrication (longer than 4 hours), consult Base Station for other medication considerations. J. For pediatric patients contact MBCH for treatment regimen. 30
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
Utah EMS Protocol Guidelines: Trauma
 Utah EMS Protocol Guidelines: Trauma Version 1 / November 1, 2013 Trauma Patient Care Guidelines These guidelines were created to provide direction for each level of certified provider in caring for trauma
Utah EMS Protocol Guidelines: Trauma Version 1 / November 1, 2013 Trauma Patient Care Guidelines These guidelines were created to provide direction for each level of certified provider in caring for trauma
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
PEDIATRIC TRAUMA EMERGENCIES
 PEDIATRIC TRAUMA EMERGENCIES Last Revised: January 2015 1 PEDIATRIC COMA SCALE Indicator Eye Opening Spontaneous 4 To verbal stimuli 3 To pain only 2 No response 1 Verbal Response Oriented, appropriate
PEDIATRIC TRAUMA EMERGENCIES Last Revised: January 2015 1 PEDIATRIC COMA SCALE Indicator Eye Opening Spontaneous 4 To verbal stimuli 3 To pain only 2 No response 1 Verbal Response Oriented, appropriate
Chapter 28. Objectives. Objectives 01/09/2013. Bleeding and Soft-Tissue Trauma
 Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
NOTE If it is necessary to perform abdominal thrusts, expose the abdominal area prior to pressing on the abdomen.
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
OUTLINE SHEET 5.4 PRIMARY SURVEY
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
Nassau Regional Emergency Medical Services. Advanced Life Support Pediatric Protocol Manual
 Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Aviation Rescue Swimmer Course
 Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
BASE HOSPITAL PROTOCOL INDEX
 BASE HOSPITAL PROTOCOL INDEX 1. EPIC-Kids Algorithm 2. EPIC-Adult-Algorithm 3. External Hemorrhage Control Protocol 4. Spinal Motion Restriction 1-15; 01-16 Airway/Breathing O 2 sat
BASE HOSPITAL PROTOCOL INDEX 1. EPIC-Kids Algorithm 2. EPIC-Adult-Algorithm 3. External Hemorrhage Control Protocol 4. Spinal Motion Restriction 1-15; 01-16 Airway/Breathing O 2 sat
EmergencyKT: Management of Thermal Injury in Adult Patients
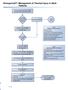 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) REQUEST EMT-P RESPONSE DO NOT DELAY TRANSPORT
 PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) 1. Basic Life Support airway management procedures are initiated. 2. Endotracheal Intubation is indicated under any of the following conditions:
PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) 1. Basic Life Support airway management procedures are initiated. 2. Endotracheal Intubation is indicated under any of the following conditions:
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Pre-hospital Trauma Life Support. Rattiya Banjungam Emergency Physician, Khon Kaen Hospital
 Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
Pre-hospital Trauma Life Support Rattiya Banjungam Emergency Physician, Khon Kaen Hospital Golden principles of Prehospital Trauma Care Golden Hour There is a golden hour if you are critically injured,
 International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES
 INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Mesa County EMS Protocol Test 2016
 Mesa County EMS Protocol Test 2016 1. Which of the following is incorrect? a. Each EMS and Fire agency should have protocols in place for evaluation of personnel involved in fire suppression operations
Mesa County EMS Protocol Test 2016 1. Which of the following is incorrect? a. Each EMS and Fire agency should have protocols in place for evaluation of personnel involved in fire suppression operations
Frontline First Aid 2012 Emergency Care Manual Treatments
 Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
3. The signs of Compartment Syndrome are listed in the General Crush Protocol. a. True b. False
 Schoolcraft Medical Control Authority (MCA) Protocol and Procedures Test, February 2015, Version 1 MFR/EMT/SPECIALIST/PARAMEDIC 1. Schoolcraft County Medical Control Protocols and Procedures can be found
Schoolcraft Medical Control Authority (MCA) Protocol and Procedures Test, February 2015, Version 1 MFR/EMT/SPECIALIST/PARAMEDIC 1. Schoolcraft County Medical Control Protocols and Procedures can be found
Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System
 1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
ADULT TRAUMA EMERGENCIES
 ADULT TRAUMA EMERGENCIES Last Revised: May 2017 1 GLASGOW COMA SCALE Indicator Response Score Eye Opening Spontaneous 4 To voice 3 To pain 2 None 1 Verbal Response Oriented 5 Confused 4 Inappropriate words
ADULT TRAUMA EMERGENCIES Last Revised: May 2017 1 GLASGOW COMA SCALE Indicator Response Score Eye Opening Spontaneous 4 To voice 3 To pain 2 None 1 Verbal Response Oriented 5 Confused 4 Inappropriate words
Name: Level of license: Date: Agency(ies):
 Schoolcraft County Medical Control Authority (MCA) Protocol and Procedures Test, October 2013 version 1.0 Name: Level of license: Date: Agency(ies): 1. EMS agencies within the Medical Control Authority
Schoolcraft County Medical Control Authority (MCA) Protocol and Procedures Test, October 2013 version 1.0 Name: Level of license: Date: Agency(ies): 1. EMS agencies within the Medical Control Authority
Does Patient Meet LERN Criteria?
 ROUTINE TRAUMA CARE Ensure scene safety & BSI precautions Assess the MECHANISM OF INJURY (MOI) / Scene Size Up / Need for Additional Resources 1 / MCI? Assess for and begin treating LIFE THREATENING injuries
ROUTINE TRAUMA CARE Ensure scene safety & BSI precautions Assess the MECHANISM OF INJURY (MOI) / Scene Size Up / Need for Additional Resources 1 / MCI? Assess for and begin treating LIFE THREATENING injuries
68W COMBAT MEDIC POCKET GUIDE
 GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
EMS System for Metropolitan Oklahoma City and Tulsa 2018 Medical Control Board Treatment Protocols
 EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Hypotension / Shock. Adult Medical Section Protocols. Protocol 30
 Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Z19.2 Cross Reference to Patient Care Maps & Clinical Care Procedures
 2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
DENVER METRO EMS PROTOCOLS: JULY 2013 UPDATE
 DENVER METRO EMS PROTOCOLS: JULY 2013 UPDATE NEW FOR JULY 2013 New: 0121 Procedure Protocol: Bougie-Assisted surgical cricothyroidotomy protocol New: 7010 Droperidol (Inapsine) protocol New: 5056 suspected
DENVER METRO EMS PROTOCOLS: JULY 2013 UPDATE NEW FOR JULY 2013 New: 0121 Procedure Protocol: Bougie-Assisted surgical cricothyroidotomy protocol New: 7010 Droperidol (Inapsine) protocol New: 5056 suspected
D. Pre-Hospital Trauma Triage and Bypass Algorithm
 D. Pre-Hospital Trauma Triage and Bypass Algorithm Hospital bypass is defined as transporting the patient to the nearest hospital that has the appropriate level of care for the patient s suspected severity
D. Pre-Hospital Trauma Triage and Bypass Algorithm Hospital bypass is defined as transporting the patient to the nearest hospital that has the appropriate level of care for the patient s suspected severity
MICHIGAN. Table of Contents. State Protocols. Adult Treatment Protocols
 MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
Trauma Registry Documentation December 16, 2014
 Trauma Registry Documentation December 16, 2014 The State of Florida now requires ALL Acute Care hospitals to submit data to the statetrauma Registry. Although Baptist Health hospitals are NOT Trauma Centers
Trauma Registry Documentation December 16, 2014 The State of Florida now requires ALL Acute Care hospitals to submit data to the statetrauma Registry. Although Baptist Health hospitals are NOT Trauma Centers
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
The following equipment and supplies shall be maintained at a minimum. Agencies should consider typical or expected usage for optimal inventory
 The following equipment and supplies shall be maintained at a minimum. Agencies should consider typical or expected usage for optimal inventory A. ALL BLS AND ALS RESPONSE AND/OR TRANSPORT UNITS Transport
The following equipment and supplies shall be maintained at a minimum. Agencies should consider typical or expected usage for optimal inventory A. ALL BLS AND ALS RESPONSE AND/OR TRANSPORT UNITS Transport
INTUBATION/RSI. PURPOSE: A. To facilitate secure, definitive control of the airway by endotracheal intubation in an expeditious and safe manner
 Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
CHANGES FOR DECEMBER 2008 PREHOSPITAL CARE MANUAL
 CHANGES FOR DECEMBER 2008 PREHOSPITAL CARE MANUAL Item Changed Airway Management Procedure Oral Intubation Procedure Tube Confirmation and Monitoring Procedure C10 Chest Pain/ACS M2 Allergic Reaction/Anaphylaxis
CHANGES FOR DECEMBER 2008 PREHOSPITAL CARE MANUAL Item Changed Airway Management Procedure Oral Intubation Procedure Tube Confirmation and Monitoring Procedure C10 Chest Pain/ACS M2 Allergic Reaction/Anaphylaxis
Animal Bites & Stings (PEDIATRIC)
 Animal Bites & Stings 1 ABC s Oxygen (as needed) Bandage & mmobilization site Cold packs can be applied for comfort NTRMAT V of LR Treat for hypotension/shock (if present) ARAMC Note and treat signs of:
Animal Bites & Stings 1 ABC s Oxygen (as needed) Bandage & mmobilization site Cold packs can be applied for comfort NTRMAT V of LR Treat for hypotension/shock (if present) ARAMC Note and treat signs of:
ITLS Advanced Pre-Test Annotated Key 8 th Edition
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Rapid Sequence Induction
 Rapid Sequence Induction Virtual simultaneous administration, after preoxygenation, of a potent sedative agent and a rapidly acting neuromuscular blocking agent to facilitate rapid tracheal intubation
Rapid Sequence Induction Virtual simultaneous administration, after preoxygenation, of a potent sedative agent and a rapidly acting neuromuscular blocking agent to facilitate rapid tracheal intubation
EMS System for Metropolitan Oklahoma City and Tulsa 2019 Medical Control Board Treatment Protocols
 EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 14G PATIENT PRIORITIZATION While each patient will receive the best possible EMS care in a humane and ethical manner, proper patient
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
ADMINISTRATIVE REQUIREMENT MANUAL EFFECTIVE DATE
 PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition)
 2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
Verde Valley Medical Center Orientation Manual and Treatment Guidelines Changes
 Verde Valley Medical Center Orientation Manual and Treatment Guidelines 2017 Changes Description Page Change Why Orientation Manual changes Verde Valley Provider agencies Application for Medical Direction
Verde Valley Medical Center Orientation Manual and Treatment Guidelines 2017 Changes Description Page Change Why Orientation Manual changes Verde Valley Provider agencies Application for Medical Direction
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies)
 SLO County Emergency Medical Services Agency Bulletin 2012-09 PLEASE POST Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies) July
SLO County Emergency Medical Services Agency Bulletin 2012-09 PLEASE POST Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies) July
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow,
 1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents
 Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents Approved/ Revised Effective BLS Adult Nerve Agent/Organophosphate Poisoning Antidote
Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents Approved/ Revised Effective BLS Adult Nerve Agent/Organophosphate Poisoning Antidote
Module I. Disasters and their Effects on the Population: Key Concepts
 PRE COURSE EXAM Place an x by the correct answer(s) on the answer sheet. Module I. Disasters and their Effects on the Population: Key Concepts 1. Which of the following best defines an event as a disaster?
PRE COURSE EXAM Place an x by the correct answer(s) on the answer sheet. Module I. Disasters and their Effects on the Population: Key Concepts 1. Which of the following best defines an event as a disaster?
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments
 ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
Pediatric Prehospital Treatment Protocols
 Pediatric Prehospital Treatment Protocols COUNTY EMS AGENCY Updated: July 17, 20 18 Pediatric Primary Survey 1 Pediatric PEA 2 Pediatric Asystole 3 Pediatric V-Fib/Pulseless V-Tach 4 Neonatal Resuscitation
Pediatric Prehospital Treatment Protocols COUNTY EMS AGENCY Updated: July 17, 20 18 Pediatric Primary Survey 1 Pediatric PEA 2 Pediatric Asystole 3 Pediatric V-Fib/Pulseless V-Tach 4 Neonatal Resuscitation
Resuscitation Checklist
 Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
Resuscitation Checklist Actions if multiple responders are on scene Is resuscitation appropriate? Conditions incompatible with life Advanced decision in place Based on the information available, the senior
IRECA BLS Challenge 2015 Scenario 1
 Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
FIRST AID WRITTEN EXAM. Team Name: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. a. TRUE b. FALSE
 2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
5/2/2018. Notice. Putting Humpty Dumpty Back Together Again
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
SAN JOAQUIN COUNTY EMERGENCY MEDICAL SERVICES
 EMS Agency SAN JOAQUIN COUNTY EMERGENCY MEDICAL SERVICES Pediatric Advanced Life Support Policies Emergency Medical Services TITLE: Pediatric Routine Medical Care EMS Policy No. 5800 Pediatric Routine
EMS Agency SAN JOAQUIN COUNTY EMERGENCY MEDICAL SERVICES Pediatric Advanced Life Support Policies Emergency Medical Services TITLE: Pediatric Routine Medical Care EMS Policy No. 5800 Pediatric Routine
Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA THE PREHOSPITAL APPROACH TO CHEST INJURY MANAGEMENT
 Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA Chest injuries are significant contributors to death from major trauma and can be difficult to assess adequately in the pre-hospital
Aurora Health Care EMS Continuing Education Spring 2011 Packet THORACIC TRAUMA Chest injuries are significant contributors to death from major trauma and can be difficult to assess adequately in the pre-hospital
The Primary Survey. C. Clay Cothren, MD FACS. Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado
 The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS
 EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director ALLERGIC REACTION/ANAPHYLAXIS ADULT BLS TREATMENT
EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director ALLERGIC REACTION/ANAPHYLAXIS ADULT BLS TREATMENT
County of Santa Clara Emergency Medical Services System
 County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
Combined CFRN and CTRN Detailed Content Outline
 Clinical items (primarily category, Assessment (15-20%), 1. General principles of transport nursing practice 19 31 A. Transport physiology 1. Physiologic stressors of transport 2. Effects of altitude on
Clinical items (primarily category, Assessment (15-20%), 1. General principles of transport nursing practice 19 31 A. Transport physiology 1. Physiologic stressors of transport 2. Effects of altitude on
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
McCann Technical School 70 Hodges Cross Road North Adams, MA Medical Assisting Program
 MA 104 MEDICAL SOCIAL SCIENCE 4 Credits Fall Semester Part IV FIRST RESPONDER Syllabus McCann Technical School 70 Hodges Cross Road North Adams, MA 01247 Medical Assisting Program INSTRUCTORS: Laurie Tuper,
MA 104 MEDICAL SOCIAL SCIENCE 4 Credits Fall Semester Part IV FIRST RESPONDER Syllabus McCann Technical School 70 Hodges Cross Road North Adams, MA 01247 Medical Assisting Program INSTRUCTORS: Laurie Tuper,
Advanced Assessment and Treatment of Trauma
 Advanced Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls
Advanced Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls
Alix Casler, M.D., F.A.A.P. Orlando, FL
 Alix Casler, M.D., F.A.A.P. Orlando, FL Emergencies in the School Setting Initial triage Basics of History and Exam Specific Scenarios Initial Assessment and Triage First steps in evaluating a potential
Alix Casler, M.D., F.A.A.P. Orlando, FL Emergencies in the School Setting Initial triage Basics of History and Exam Specific Scenarios Initial Assessment and Triage First steps in evaluating a potential
Musculoskeletal Trauma. Lesson Goal. Lesson Objectives 9/10/2012. Recognize and manage patients with musculoskeletal trauma
 Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
MEDICAL CONTROL POLICY STATEMENT/ADVISORY. Re: Spinal Injury Assessment & Spinal Precautions Procedure
 MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
Trauma Alert Step 2 Additions
 Trauma Alert Step 2 Additions MANGLED, DEGLOVED OR PULSELESS EXTREMITY PELVIC INJURY WITH HIGH-RISK MECHANISM OF INJURY Many thanks to Paramedic FTO Justin Bramlette for assembling this training presentation
Trauma Alert Step 2 Additions MANGLED, DEGLOVED OR PULSELESS EXTREMITY PELVIC INJURY WITH HIGH-RISK MECHANISM OF INJURY Many thanks to Paramedic FTO Justin Bramlette for assembling this training presentation
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
PARAMEDIC PROVIDER AUTHORIZED STOCK
 Monterey County EMS System Policy Policy Number: 4010 Effective Date: 7/1/2018 Review Date: 6/30/2021 I. PURPOSE PARAMEDIC PROVIDER AUTHORIZED STOCK A. To establish equipment standards for paramedic service
Monterey County EMS System Policy Policy Number: 4010 Effective Date: 7/1/2018 Review Date: 6/30/2021 I. PURPOSE PARAMEDIC PROVIDER AUTHORIZED STOCK A. To establish equipment standards for paramedic service
Airway Management. Teeradej Kuptanon, MD
 Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Portage County EMS Patient Care Guidelines. Routine Trauma Care
 Portage County EMS Patient Care Guidelines Routine Trauma Care Priorities Chief Complaint LOPQRST AS/PN AMPL Initial Exam Rapid Trauma Assessment Detailed Focused Exam Data Goals of Therapy Monitoring
Portage County EMS Patient Care Guidelines Routine Trauma Care Priorities Chief Complaint LOPQRST AS/PN AMPL Initial Exam Rapid Trauma Assessment Detailed Focused Exam Data Goals of Therapy Monitoring
Portage County EMS Patient Care Guidelines. Routine Trauma Care
 Portage County EMS Patient Care Guidelines Routine Trauma Care Priorities Chief Complaint LOPQRST AS/PN AMPL Initial Exam Rapid Trauma Assessment Detailed Focused Exam Data Goals of Therapy Monitoring
Portage County EMS Patient Care Guidelines Routine Trauma Care Priorities Chief Complaint LOPQRST AS/PN AMPL Initial Exam Rapid Trauma Assessment Detailed Focused Exam Data Goals of Therapy Monitoring
Advanced Resuscitation - Child
 C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
