Preparing for your heart operation
|
|
|
- Cassandra McCoy
- 6 years ago
- Views:
Transcription
1 A lifetime of specialist care Royal Brompton Hospital Preparing for your heart operation
2 Contents Why do I need heart surgery? 3 Types of heart surgery 4 Before coming to hospital 8 What do I need to bring in with me for my stay in hospital? 13 Admission to hospital 15 Recovering from your operation 18 Going home 21 Where can I get more information? 22 This booklet gives you information on preparing for your heart operation. It does not replace the need for personal advice from a healthcare professional. If you need any more information, please contact the cardiac surgery helpline via the hospital switchboard on and ask for bleep
3 Preparing for your heart operation Why do I need heart surgery? People need heart surgery for different reasons. The most common reasons are: Coronary artery disease The coronary arteries supply the heart with blood. In some patients, if fatty material builds up inside the wall of the arteries (atheroma), these arteries become narrowed. If this happens, the blood supply to the heart is reduced and it does not get enough oxygen. This causes chest pain called angina. If the artery becomes totally blocked, the result is a heart attack. Damaged heart valves The heart has four heart valves that control the flow of blood in and out of your heart. Heart valves can get damaged through ageing, rheumatic fever or a heart attack. They may become stiff and their openings narrower or floppy, which may allow blood to flow in the wrong direction. If the valves are damaged, your heart has to work harder to pump blood. Over time, the heart becomes enlarged (bigger) and inefficient. An enlarged heart that does not work well is called heart failure. Symptoms include shortness of breath, tiredness and fluid retention. Enlarged aortic artery The aortic artery is the main artery that carries oxygen-rich blood to the body. The aortic artery can become enlarged and rupture (burst). This abnormality is usually caused by a genetic disorder. 3
4 Types of heart surgery Coronary artery bypass grafting (CABG) What is CABG? Coronary artery bypass grafting (CABG) involves taking a vein or artery from another part of the body, usually the chest or leg, and attaching it to the coronary artery above and below the narrowed area or blockage. This replacement vein or artery is called a graft and allows blood to bypass the narrowing or blockage, improving blood supply to your heart muscle. Heart bypass surgery does not cure the heart disease that caused your arteries to become narrowed or blocked. It is important to follow a healthy lifestyle to help the graft(s) work well and to prevent the narrowing of other arteries. There is more information on how you can improve your lifestyle on page 9 of this booklet. How is CABG carried out? The first step is to collect the vein or artery that is going to be used as the graft. The surgeon then reaches the heart by making a 25cm (10 inches) cut down the middle of the breastbone. An alternative procedure called a minimally invasive operation is available to some patients who have only one blocked coronary artery. Instead of cutting through the breastbone, the surgeon makes a smaller cut in the side of the chest through which the surgery is carried out. Your surgeon will discuss these methods with you and explain which one will be used. What are the advantages of CABG? A successful operation will increase the blood flow to your heart muscle. This will reduce symptoms such as angina (chest pain), shortness of breath and improve your overall quality of 4
5 Preparing for your heart operation life. The surgery also reduces the risk of future heart attacks. At your consultation, your surgeon will always discuss with you what they expect the outcomes to be for you as an individual. What are the risks of CABG? All medical procedures carry some risk. It is important to remember that we would not recommend any procedure if we did not believe the benefits outweigh any risks. The risks will be different for each patient, so we will discuss the risks that apply to you in more detail before the procedure. The risks of CABG surgery include: Atrial fibrillation a fast, irregular heartbeat that usually settles after a few days. It rarely causes a major change to how the heart works or to the patient s overall level of health. Bleeding some patients may need a further operation after surgery to control bleeding. Wound infection this is more common in patients with poorly controlled diabetes or other conditions that make them more vulnerable to infection. If you do get an infection, this can be treated with antibiotics. Renal (kidney) failure this is more common in patients who already have kidney problems and can be treated with dialysis. Stroke this happens when a blood clot develops and travels to the brain, cutting off the oxygen supply. The risk is higher in patients who have had a stroke or transient ischaemic attacks (TIAs, commonly known as mini-strokes). To reduce the risk of stroke, we will give you medications both during and after the operation to slow down the rate at which your blood clots. We may also ask you to wear special stockings after your operation. These have been shown to reduce the risk of clots. Death the risk of not surviving the operation will be higher for patients who are very unwell before the surgery. Your 5
6 surgeon will discuss your risk with you at your consultation. Are there any alternatives to CABG? Drugs will only control the symptoms of your heart disease and will not solve the underlying problem. What will happen if I do not have CABG? Without heart bypass surgery, symptoms such as angina and shortness of breath will get worse and more frequent over time. You will also have a higher risk of having a heart attack. Patients with severe coronary artery disease may have a shorter life expectancy. Heart valve surgery What is heart valve surgery? In heart valve surgery, damaged valves are either repaired or replaced. The valves that most commonly need surgery are the aortic and mitral valves. In some cases it is possible to repair a narrowed valve by simply opening it up (valvotomy). Sometimes a leaking valve can also be repaired, but if it is badly damaged it has to be replaced. There are two types of replacement valves: Mechanical valves made out of metal and plastic. Tissue valves made out of tissue from pigs, cows or from human donors. Heart valve surgery involves making a cut of about 25cm (10 inches) down the middle of the breastbone to access the heart. Some patients are suitable for a minimally invasive operation. This involves making a smaller cut and may lead to quicker recovery times. If a minimally invasive operation is suitable for you, your surgeon will discuss this with you in more detail. 6
7 Preparing for your heart operation What are the advantages of heart valve surgery? Heart valve surgery should help improve the quality of your life by reducing symptoms such as shortness of breath, blackouts, tiredness, chest pain and fluid retention. It will also reduce the risk of your heart failure developing further and help increase your life expectancy. What are the risks of heart valve surgery? All medical procedures carry some level of risk. However, we would not recommend a procedure if we did not believe the benefits outweigh any risks to your health. Please ask your surgeon if you need more information. These risks will be different for each patient. Your surgeon will discuss the specific risks with you before your operation. The risks of heart valve surgery include: Need for a permanent pacemaker the operation can disrupt the heart s regular rhythm. This will usually return to normal in the days after surgery. Sometimes this does not happen and patients need a permanent pacemaker fitted after surgery to regulate their heart rhythm. Other risks of heart valve surgery are the same as those for heart bypass surgery (CABG) on page 5 of this booklet. Are there any alternatives to heart valve surgery? Drugs can be used to treat the symptoms of your condition, but cannot cure the underlying problem. What will happen if I do not have heart valve surgery? Without heart valve surgery, your symptoms will get worse and more frequent over time. 7
8 Aortic surgery In aortic surgery, the enlarged aortic artery is either replaced or repaired by placing a graft (a synthetic tube) around it to stop it from getting any bigger. What are the advantages of aortic surgery? Aortic surgery will remove the risk of the aortic artery getting any bigger and rupturing (bursting), and will help increase your life expectancy. What are the risks of aortic surgery? All medical procedures carry some level of risk. However, we would not recommend a procedure if we did not believe the benefits outweigh any risks to your health. These risks will be different for each patient. Your surgeon will discuss the specific risks with you at your outpatient appointment before your operation. Before coming to hospital When will I have my operation? Unfortunately we cannot give you a date for your operation immediately. Your surgeon's secretary will contact you to discuss the planned date for your admission and send you a confirmation letter. You can turn down the planned date if you want or need to. However, if you decide to delay the operation, there may be an impact on your health. Once you have a date for your operation, we recommend that you start making travel arrangements for how to get to the hospital on time for your admission. We have accommodation close to the hospital available for families, if needed. However, this must be booked in advance. 8
9 Preparing for your heart operation For more information, please contact the accommodation office on What if my symptoms get worse? If you feel unwell while waiting for your operation, please contact your GP. It may be that your treatment needs to be changed. You should see your GP if you: have unusual swelling in your ankles have a cough and/or are producing phlegm are not able to exercise as much as usual. You should go to accident and emergency (A&E) if your GP cannot see you straight away and you are experiencing any of the following symptoms: angina that is not relieved by rest or controlled by your normal medication unusual chest pain pain in your arms, back or throat shortness of breath that is not relieved by rest fainting or dizzy spells for no reason. Royal Brompton Hospital does not have an A&E department. What can I do to improve my health? Increase your overall level of fitness by walking regularly Increased fitness will help you to recover more quickly after surgery. It also reduces the likelihood of complications after your operation. 9
10 Quit smoking Smoking is one of the main causes of coronary artery disease and it damages your lungs. Patients with strong, healthy lungs tend to recover from surgery much more quickly than those with lung damage. Many patients find that having a heart operation gives them extra motivation to stop smoking. There is plenty of support available to help you give up for good. Please talk to your GP or pharmacist. You can also call SMOKEFREE on or visit them at Control your weight Patients who are overweight are more likely to have complications after their operation and to recover more slowly from surgery. The best way to find out whether you are overweight is to calculate your body mass index (BMI). You can discuss this with your GP, who can also refer you to a local dietitian if needed. Visit your dentist As soon as you know that you need to have heart surgery, visit your dentist to make sure your teeth and gums are as healthy as possible. This is to reduce the risk of infection. Infected gums or teeth can introduce bacteria into the bloodstream, which could cause complications or an infection called endocarditis. We have a separate leaflet on endocarditis. Please ask a member of the nursing team if you would like more information. What appointments and tests will I have before my operation? While you are waiting for a date for your surgery, we will organise other appointments to help make sure you are ready for your operation. Surgical information seminars All patients on the waiting list for heart surgery are invited to a surgical information seminar. During these sessions, a clinical nurse specialist and other healthcare practitioners will give you 10
11 Preparing for your heart operation an idea of what to expect before and after the operation and will also give advice on recovering after surgery. A film of patients talking about having heart surgery is shown during the session, and there will be a chance for you to ask questions. We strongly recommend that you attend a seminar so you are adequately prepared for your surgery. Pre-operative assessment Before coming into hospital for surgery, most patients will need to attend an assessment (health check) at the pre-admission clinic. The assessment is an important part of your preparation for heart surgery. A clinical nurse specialist will contact you by telephone to arrange this. At the pre-operative assessment, some patients will be seen by an anaesthetist (others will see their anaesthetist on arrival at hospital for their surgery). Anaesthetists are specialist doctors who are responsible for providing anaesthesia to patients for operations and procedures. They have a range of skills which include pain management and intensive care. During heart surgery you will have a general anaesthetic to send you to sleep so you don't feel pain while it is carried out. Your anaesthetist will help look after you and will be responsible for you before, during and immediately after your operation. Your anaesthetist will do a pre-operative check where you will be asked about your general health, medical history, previous anaesthetics and operations, allergies and what current medications you are taking. It is important to tell us about allergic reactions you may have had to medicines or other substances (for example latex or specific foods) in the past. Your anaesthetist will examine you, paying particular attention to your heart and lungs, as well as to your mouth and neck. You should tell him/her if you have any loose teeth, caps, crowns or dental bridges. This is to minimise the risk of damage when 11
12 inserting breathing tubes and monitor probes once you have been anaesthetised. It is also important to tell your anaesthetist if you have any pain or stiffness when you move your neck. When the assessment is finished and the anaesthetist has your test results (see below), he/she will explain what will happen during your surgery, and tell you about the risks and benefits of having it. He/she will also discuss any choices you might have regarding your anaesthetic. MRSA (methicillin resistant staphylococcus aureus) swabs This test is to check whether you have MRSA bacteria on your skin or in your nose. This is a routine test for all patients admitted to the hospital. It is an important test that helps to stop the spread of MRSA (sometimes referred to as a superbug ). Electrocardiogram (ECG) An electrocardiogram is a simple, painless test which measures the electrical activity of your heart through electrodes (sticky patches) placed on your chest. Blood tests Blood tests can help us to check different areas of your general health. If you have a blood test your nurse can explain what we are checking for. Chest X-ray An X-ray lets us look at your lungs, as well as the size and shape of your heart. Echocardiogram (echo) An echocardiogram is a test that uses sound waves to build up a moving picture of the heart. It is similar to the ultrasound scan used in pregnancy and is extremely safe. It allows us to learn more about the function and structure of your heart valves and chambers. We attach electrodes to your chest to monitor your heart and take the echo with a small hand-held recorder. 12
13 Preparing for your heart operation Ultrasound, computerised tomography (CT) or magnetic resonance imaging (MRI) scan All of these scans let us look at your heart and lungs in more detail. Your doctor or nurse will explain which scan you are having and why. Carotid doppler This is an ultrasound scan of the arteries in your neck (the carotid arteries). It allows us to examine the arteries for any signs of narrowing or blockage. Lung function tests If you smoke, have recently quit, or have a chronic lung problem, such as chronic obstructive pulmonary disease (COPD) or asthma, you may need to have a lung function test to check how well your lungs are working. It is a simple and painless test where you simply breathe into a mouthpiece. What do I need to bring in with me for my stay in hospital? Toiletries Toothbrush and toothpaste Shampoo, liquid soap and shower gel Deodorant Shaving equipment for men Hairbrush/comb Disposable flannels and clean towels will be provided daily by the hospital. Clothing The clothing you bring should be light and comfortable. Avoid tight, elasticated, restrictive clothing, particularly at the ankles. 13
14 Front-buttoning tops are recommended as it will be difficult to pull clothing over your head because of your wound. Female patients will need to bring in at least two bras. They should be non-wired and front fastening. It is important that your bras are the correct size. If you attend the preadmission clinic, you will be measured as part of your assessment. If not, please go to a lingerie department/shop and get measured so that you bring/buy the right size bra. Footwear Bring a pair of slippers that fit well and cover the whole of the foot. Avoid backless slippers and shoes. Non-slip socks will be provided. Medication Please bring in all the medications you take, in their original boxes. This is so your doctor can accurately prescribe the medication you require for your stay in hospital. Valuables We recommend that you do not bring any valuables or large sums of money with you. Glasses, dentures and hearing aids If you wear dentures, bring a plastic denture pot with a secure fitting lid. If you wear glasses, bring a hard glasses case. If you wear a hearing aid, bring the storage box for your hearing aids so these can be securely looked after while you are in theatre. Ear plugs and eye mask Ear plugs and eye masks are optional, but you could find them useful to help block out the noise/light that is inevitable in a ward environment at night. 14
15 Preparing for your heart operation Storage for your belongings You will have your own locker at your bedside to store your belongings. While you are having your operation, we will lock your belongings in a secure locked cupboard until you return to the ward. Devices You will be able to use a mobile phone, laptop or MP3 player. There is access to free wifi on all wards. Ask your nurse for the password. Please bring earphones with you so that you don t disturb other patients. Admission to hospital It is very important that you do not shave or remove hair from your chest, arms, legs or groin before coming into hospital. This is because shaving may damage the skin and increase the risk of infection. We will prepare your skin for surgery while you are in hospital. What will happen on the day of my admission and surgery? Most patients will be admitted on the morning of the day of their surgery. Some patients will need to be admitted the day before surgery. You will be told about this when you are given a date for your operation. You will be asked to shower at home before coming in for surgery, using an antimicrobial hair and body wash, which will be given to you at your pre-admission assessment. If you are admitted for surgery the day before your operation, you will be asked to shower the evening before, and morning of, your surgery on the ward. 15
16 Your surgeon will discuss the operation with you at your preadmission assessment or on the ward if you are admitted the day before surgery. The surgeon will then ask you to sign a consent form to show that you understand the information and agree to have the operation. If you have any more questions about the operation, please discuss these with your surgeon. You will not be able to eat or drink anything for six hours before your operation as the anaesthetic must be given on an empty stomach. You may take regular medication, as advised by your anaesthetist, with a small sip of water right up to the time of your surgery if necessary. It is normal to be anxious before your surgery. You may be given a sedative medication ( pre-med ), which will help you to relax. When it is time for your operation, you will be taken on a bed or chair to the anaesthetic room. A friend or relative is welcome to stay with you until this time. What will happen once I am in the anaesthetic room? Once you arrive in the operating department, an assistant who works with the anaesthetist will check your details and paperwork again. You will then be brought into the anaesthetic room. We will connect you to a heart monitor and place a probe clip on your finger to measure your pulse and oxygen levels. You will be given oxygen to breathe through a mask and the anaesthetist will then insert a cannular (tube) into a vein in your arm. You will be given anaesthetic drugs by injection through the cannula in your arm or vein to send you to sleep. Many patients do not remember anything after this, but some are aware of the anaesthetist injecting a local anaesthetic into their wrist. This is so we can insert a small tube (cannula) into your artery to monitor your blood pressure. Once you are deeply anaesthetised, a breathing tube will be 16
17 Preparing for your heart operation inserted through your mouth and into your airway, and you will have a catheter fitted. What happens after my operation? Immediately after your operation you will be taken to the adult intensive care unit (AICU) or to the recovery unit. You will be connected to a monitor to check your heart rate, blood pressure and blood oxygen levels. A nurse will be with you at all times. At first, we will keep you asleep so that we can make sure your heart is working well and that there is no major bleeding from the wound. We will then turn off the anaesthetic and allow you to wake up gradually. You will become aware that the tube helping you to breathe is still in your mouth. As soon as we are happy that you can breathe strongly enough on your own, a nurse will remove the tube. Several drips will provide you with the fluid, medications and pain relief you need. You will also have a catheter in your bladder. This means that you do not have to worry about going to the toilet. You will also have some chest drains in place after your operation. These remove blood, fluid and air that may collect in the chest after surgery. The drains are removed once they have finished draining all the fluid. When can my friends and family visit me? Your friends and family can visit you as soon as you are well enough. You are likely to be very tired after your operation and we suggest that you only have two visitors at a time. To reduce the risk of infection in hospital, visitors should always wash their hands before and after visiting you and use the hand cleansing gels which are at the end of every bed and at the entrance to the ward. Please ask your friends and family not to visit you if they are feeling unwell. 17
18 Recovering from your operation When will I move back to the ward? Most patients are well enough to move back to the high dependency unit (HDU) on the day after their operation. Some patients take longer to recover than others and need to stay a little longer on the intensive care unit. What will happen when I am back on the ward? Once you are back on the ward you should recover quickly. Most drips and drains will be removed within two or three days of the operation and each day you should notice an improvement in how you feel. Most patients pass through the following stages during their recovery. Remember that every patient is different and so this is just a guide: Stage one (generally day one) HDU You will still be connected to some drips and tubes. A nurse or physiotherapist will help you sit in a chair and spend some of the day out of bed. You will be able to eat and drink small amounts. Stage two (generally day two) return to the ward We will remove most of your drips and tubes. If you have had heart bypass surgery with a vein from your leg, we will remove the bandage from your leg. Your nurse or physiotherapist will encourage you to take regular short walks around the ward. Your nurse will help you with personal hygiene, if needed. You will be able to dress in your own clothing. 18
19 Preparing for your heart operation Stage three (generally days three to four) You will be able to walk longer distances. You will be able to have a shower a nurse can help if needed. You should have a better appetite. Stage four (generally day five) You should be able to climb stairs. If your mobility is limited, or you are worried about climbing stairs, a physiotherapist will help you with this. Plans for your return home will be finalised including support from social services, if needed. Stage five (generally days six to seven) You will go home. What pain relief will I receive after my operation? Good pain relief is important for your recovery. Our aim is to control your pain so that you can do the exercises your physiotherapist gives you and so that you can gradually move and walk around comfortably. Throughout your stay in hospital we will ask you to score your pain on a scale of zero to 10. Zero being no pain and 10 being unbearable pain. Please do not feel you need to give a brave answer. If you give us an honest answer, it helps us make sure that you have the correct level of pain relief. There are many different pain relief methods available. Before your operation, your anaesthetist will discuss this with you and together you will decide on which methods are best for you. 19
20 Options include: Patient controlled analgesia (PCA) This is a method that allows you to control your own pain relief. A pump containing medication (normally morphine) is connected to a cannula (a small plastic tube) that is inserted into one of your veins. When you are in pain, you press a button that delivers a safe, pre-set amount of medication. There is no risk of addiction or overdosing. Most patients receive pain relief in this way after their operation. Tablets or liquid Once you are eating and drinking again, you will be given this type of pain medication throughout the day. Tablets or liquid can be used along with PCA. They usually take about 30 minutes to work. Suppositories If you are having problems swallowing or are feeling sick after your operation we can give you suppositories. These are waxy pellets placed into your back passage (rectum). They dissolve and the medication is then easily passed into your body. What happens if I have problems with pain? Please rest assured that we will do everything we can to control any pain you have following your operation. We have specialist pain management nurses who will be happy to see you if you are finding that your pain is a problem. How long will I need to take pain relief medication for? You will need to take pain relief medication for the first few weeks after your operation. We have a separate leaflet about managing your pain at home. Please ask us if you would like more information. 20
21 Preparing for your heart operation Going home When will I go home? Different patients take different amounts of time to recover after heart surgery. It is difficult to predict exactly when you will go home, but most patients are ready a week after their operation. What will happen before I am discharged home? We know that being discharged from hospital after an operation can be both a happy and a worrying time. Our staff will do everything they can to make you feel prepared. Different members of our team will discuss with you what to do to help your recovery back at home. We will give you a twoweek supply of your medication and a copy of your discharge letter that we also post to your GP. We have a separate leaflet on returning home after your heart operation. We will give you a copy of this when you are recovering from your operation in hospital. If you do not receive a copy, please let us know. Will transport be arranged to take me home? We can only arrange hospital transport for patients who are in medical need and cannot get to and from our hospitals in any other way. Unless you have a medical need for hospital transport, you will be asked to make your own arrangements. You will not be able to drive for at least six weeks after your operation, so please arrange for someone to take you home. If you are planning to use public transport, please make sure that someone is able to travel with you. Parking Royal Brompton Hospital has no parking for patients and relatives. 21
22 There are three disabled parking spaces on the Sydney Street site, which are available on a first-come-first-served basis and are limited to stays of four hours. There is metered parking on the streets around the Sydney Street site, which varies from a maximum stay of between two and four hours. If you are dropping someone off who is being admitted for surgery or picking someone up who has had heart surgery, the parking attendant will allow you to park in front of the main entrance of the hospital for 15 minutes, if there is space available. Alternatively, you may be asked to park in one of the metered bays on the street until a space becomes available. Where can I get more information? Please call us if you have any questions about coming into hospital, your surgery, or recovering after the operation. You can call our 24-hour cardiac surgery helpline through the main hospital switchboard on , and ask for bleep If you have concerns about any aspect of the service you have received in hospital and feel unable to talk to those people responsible for your care, call the Patient Advice and Liaison Service (PALS) on or pals@rbht.nhs.uk. This is a confidential service. 22
23 23 Preparing for your heart operation
24 Royal Brompton Hospital Sydney Street London SW3 6NP tel: textphone: (18001) Harefield Hospital Hill End Road Harefield Middlesex UB9 6JH tel: textphone: (18001) Website: Brosurteki bilginin Turkçe tercumesi için tedavi goruyor oldugunuz bolume bas vurunuz. Bolum personeli tercumenin gerçeklesmesini en kisa zamanda ayarlacaktir. Royal Brompton & Harefield NHS Foundation Trust January 2018
A lifetime of specialist care. Having a CT coronary angiography scan
 A lifetime of specialist care Having a CT coronary angiography scan Contents What is a CT coronary angiography scan? 3 What are the benefits? 3 Are there any alternatives? 3 What happens if I don t have
A lifetime of specialist care Having a CT coronary angiography scan Contents What is a CT coronary angiography scan? 3 What are the benefits? 3 Are there any alternatives? 3 What happens if I don t have
After your angiogram or angioplasty
 A lifetime of specialist care Royal Brompton Hospital After your angiogram or angioplasty Contents A diagram of the coronary arteries 3 After your angiogram 4 After your angioplasty and stent 4 Going back
A lifetime of specialist care Royal Brompton Hospital After your angiogram or angioplasty Contents A diagram of the coronary arteries 3 After your angiogram 4 After your angioplasty and stent 4 Going back
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
A lifetime of specialist care. Cardiomyopathy day case clinic
 A lifetime of specialist care Cardiomyopathy day case clinic Contents Cardiomyopathy day case clinic 3 What does the clinic team do? 3 Where do I need to go? 4 What should I bring? 4 Family history 4 What
A lifetime of specialist care Cardiomyopathy day case clinic Contents Cardiomyopathy day case clinic 3 What does the clinic team do? 3 Where do I need to go? 4 What should I bring? 4 Family history 4 What
A lifetime of specialist care. Systematic assessment of refractory asthma (SARA)
 A lifetime of specialist care Systematic assessment of refractory asthma (SARA) Contents Introduction 3 What do I need to know? 3 What should I bring? 4 Visiting hours, facilities and dietary requirements
A lifetime of specialist care Systematic assessment of refractory asthma (SARA) Contents Introduction 3 What do I need to know? 3 What should I bring? 4 Visiting hours, facilities and dietary requirements
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Physiotherapy at home
 Royal Brompton & Harefield NHS Foundation Trust Physiotherapy at home Contents Introduction 1 Exercise is necessary to 2 What type of exercise should I do? 2 How long should I walk for? 2 At home 3 Guidelines
Royal Brompton & Harefield NHS Foundation Trust Physiotherapy at home Contents Introduction 1 Exercise is necessary to 2 What type of exercise should I do? 2 How long should I walk for? 2 At home 3 Guidelines
You and your anaesthetic Information to help patients prepare for an anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia explained and www.youranaesthetic.info This leaflet gives basic information to help
You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia explained and www.youranaesthetic.info This leaflet gives basic information to help
You and your anaesthetic. Information to help patients prepare for an anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic This leaflet gives basic information to help you prepare for your anaesthetic. It has been written by patients, patient
You and your anaesthetic Information to help patients prepare for an anaesthetic This leaflet gives basic information to help you prepare for your anaesthetic. It has been written by patients, patient
You and your anaesthetic Information to help patients prepare for an anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia Explained and www.youranaesthetic.info This leaflet gives basic information to help
You and your anaesthetic Information to help patients prepare for an anaesthetic You can find out more from Anaesthesia Explained and www.youranaesthetic.info This leaflet gives basic information to help
Transcatheter Aortic Valve Implantation (TAVI) PROOF. Patient Information leaflet. Lancashire Cardiac Centre
 Transcatheter Aortic Valve Implantation (TAVI) Patient Information leaflet Lancashire Cardiac Centre Welcome to the Lancashire Cardiac Centre During your admission you will be admitted to Ward 37. Ward
Transcatheter Aortic Valve Implantation (TAVI) Patient Information leaflet Lancashire Cardiac Centre Welcome to the Lancashire Cardiac Centre During your admission you will be admitted to Ward 37. Ward
You and your anaesthetic
 Questions you may like to ask your anaesthetist Q Who will give my anaesthetic? Q Do I have to have a general anaesthetic? Q What type of anaesthetic do you recommend? Q Have you often used this type of
Questions you may like to ask your anaesthetist Q Who will give my anaesthetic? Q Do I have to have a general anaesthetic? Q What type of anaesthetic do you recommend? Q Have you often used this type of
Information about Your Anaesthetic and Pain Control After Surgery
 Information about Your Anaesthetic and Pain Control After Surgery Information for patients Specialist Support If you require this leaflet in another language, large print or another format, please contact
Information about Your Anaesthetic and Pain Control After Surgery Information for patients Specialist Support If you require this leaflet in another language, large print or another format, please contact
Aortic valve replacement. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Aortic replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in
Aortic replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in
Patient information. You and Your Anaesthetic Information to help you prepare for anaesthetic. Anaesthesia Directorate PIF 344/ V5
 Patient information You and Your Anaesthetic Information to help you prepare for anaesthetic Anaesthesia Directorate PIF 344/ V5 Types of anaesthesia Anaesthesia stops you feeling pain and other sensations.
Patient information You and Your Anaesthetic Information to help you prepare for anaesthetic Anaesthesia Directorate PIF 344/ V5 Types of anaesthesia Anaesthesia stops you feeling pain and other sensations.
Anaesthesia and pain (Daycase Patient) Patient information Leaflet
 Anaesthesia and pain (Daycase Patient) Patient information Leaflet February 2018 INTRODUCTION Welcome to Tameside Hospital, this leaflet gives basic information to help you prepare for your anaesthetic,
Anaesthesia and pain (Daycase Patient) Patient information Leaflet February 2018 INTRODUCTION Welcome to Tameside Hospital, this leaflet gives basic information to help you prepare for your anaesthetic,
Your anaesthetic for major surgery
 Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts
 Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you.
 Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
Mitral valve surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Mitral valve surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Mitral valve surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
The pillars defining our quality care. We Care!
 The pillars defining our quality care We Care! 1 What is Anaesthesia? Anaesthesia stops you feeling pain and other sensations. It can be given in various ways and does not always make you unconscious.
The pillars defining our quality care We Care! 1 What is Anaesthesia? Anaesthesia stops you feeling pain and other sensations. It can be given in various ways and does not always make you unconscious.
You and your anaesthe c
 You and your anaesthe c Information to help patients prepare for an anaesthetic This leaflet gives basic information to help you prepare for your anaesthetic. Some types of anaesthesia Anaesthesia stops
You and your anaesthe c Information to help patients prepare for an anaesthetic This leaflet gives basic information to help you prepare for your anaesthetic. Some types of anaesthesia Anaesthesia stops
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Having an Anaesthetic Your Questions Answered
 PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
Inguinal hernias may be present from birth but may not become evident until later in life. They are usually more common in men.
 This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
Anaesthetic choices for hip or knee replacement
 Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
Anaesthetic choices for hip or knee replacement Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an operation to replace a hip
Transcatheter Aortic Valve Implant (TAVI) Sussex Cardiac Centre
 Transcatheter Aortic Valve Implant (TAVI) Sussex Cardiac Centre Information for patients and carers Contents Valvular heart disease 3 What are the symptoms 3 Transcatheter aortic valve implantation 4 What
Transcatheter Aortic Valve Implant (TAVI) Sussex Cardiac Centre Information for patients and carers Contents Valvular heart disease 3 What are the symptoms 3 Transcatheter aortic valve implantation 4 What
You and your anaesthetic
 You and your anaesthetic Information to help patients prepare for an anaesthetic This leaflet gives basic information to help you prepare for your anaesthetic. It has been written by patients, patient
You and your anaesthetic Information to help patients prepare for an anaesthetic This leaflet gives basic information to help you prepare for your anaesthetic. It has been written by patients, patient
Your visit to theatre
 Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft
 Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet
 Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
WEB device for treating brain (intracranial) aneurysms
 WEB device for treating brain (intracranial) aneurysms This leaflet explains more about the WEB device, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
WEB device for treating brain (intracranial) aneurysms This leaflet explains more about the WEB device, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
Femoropopliteal/distal. bypass grafts. Vascular Surgery Patient Information Leaflet
 Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation
 Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Mitral Regurgitation
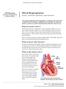 UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
Carotid Endarterectomy
 Information for patients Carotid Endarterectomy Northern General Hospital You have been diagnosed as having Carotid Artery Disease and need an operation called a Carotid Endarterectomy. This leaflet explains
Information for patients Carotid Endarterectomy Northern General Hospital You have been diagnosed as having Carotid Artery Disease and need an operation called a Carotid Endarterectomy. This leaflet explains
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Your Anaesthetic Explained
 Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Information for patients, parents and guardians. Your child s doctor has recommended that your child has a procedure called an ablation.
 Having an ablation Information for patients, parents and guardians Your child s doctor has recommended that your child has a procedure called an ablation. An ablation is a treatment for an abnormal heartbeat.
Having an ablation Information for patients, parents and guardians Your child s doctor has recommended that your child has a procedure called an ablation. An ablation is a treatment for an abnormal heartbeat.
Cheltenham General Hospital
 Page 1 of 5 Coronary angioplasty Introduction This leaflet provides information for patients undergoing coronary angioplasty also known as PCI (Percutaneous Coronary Intervention). What is coronary artery
Page 1 of 5 Coronary angioplasty Introduction This leaflet provides information for patients undergoing coronary angioplasty also known as PCI (Percutaneous Coronary Intervention). What is coronary artery
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
ARTERIAL BYPASS GRAFTS IN THE LEG
 The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
You and Your Anaesthetic
 York Teaching Hospital NHS Foundation Trust You and Your Anaesthetic Information to help patients prepare for an anaesthetic Anaesthetics Department For more information, please contact: The Anaesthetic
York Teaching Hospital NHS Foundation Trust You and Your Anaesthetic Information to help patients prepare for an anaesthetic Anaesthetics Department For more information, please contact: The Anaesthetic
Deep brain stimulation
 About insertion of a deep brain stimulator The deep brain stimulator sends electrical impulses to the brain interrupting the abnormal signals that are causing the symptoms. The impulses are adjusted by
About insertion of a deep brain stimulator The deep brain stimulator sends electrical impulses to the brain interrupting the abnormal signals that are causing the symptoms. The impulses are adjusted by
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request.
 Information for inpatients This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Med/304.1 (2012) Page 1 of 8
Information for inpatients This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Med/304.1 (2012) Page 1 of 8
Nephrostomy. Radiology Department. Patient information leaflet
 Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
Nephrostomy Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a nephrostomy. It explains what is involved and the possible risks. The benefits and risks
Oesophageal Stent insertion
 Oesophageal Stent insertion What is an Oesophageal Stent? Patients with a blockage in their oesophagus or stomach that cannot be relieved by an operation may be offered the option of having an oesophageal
Oesophageal Stent insertion What is an Oesophageal Stent? Patients with a blockage in their oesophagus or stomach that cannot be relieved by an operation may be offered the option of having an oesophageal
If you have any further questions, please speak to a doctor or nurse caring for you.
 Surgical Removal of a Paraganglioma of the Temporal Bone This leaflet explains more about surgery for the removal of a paraganglioma of the temporal bone, including the benefits, risks and any alternatives
Surgical Removal of a Paraganglioma of the Temporal Bone This leaflet explains more about surgery for the removal of a paraganglioma of the temporal bone, including the benefits, risks and any alternatives
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Transcatheter Aortic Valve Implant (TAVI)
 Transcatheter Aortic Valve Implant (TAVI) Sussex Cardiac Centre Information for Patients and Carers Contents Advice pre and post transcatheter aortic valve implant 2 Valvular heart disease 3 What are the
Transcatheter Aortic Valve Implant (TAVI) Sussex Cardiac Centre Information for Patients and Carers Contents Advice pre and post transcatheter aortic valve implant 2 Valvular heart disease 3 What are the
AN INFORMATION LEAFLET
 LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
About general anaesthesia Day Surgery Unit Patient Information Leaflet
 About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
About general anaesthesia Day Surgery Unit Patient Information Leaflet Originator: Nahla Farid - Consultant Anaesthetist Date: November 2011 Version: 1 Date for Review: November 2014 DGOH Ref No: DGOH/PIL/00560
Pacemaker and AV Node Ablation Patient Information
 Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Ultrafiltration. A guide for patients undergoing ultrafiltration for the treatment of heart failure
 Ultrafiltration A guide for patients undergoing ultrafiltration for the treatment of heart failure Dr Sue Ellery Consultant Cardiologist Patient Information What is heart failure? 3 What is the treatment
Ultrafiltration A guide for patients undergoing ultrafiltration for the treatment of heart failure Dr Sue Ellery Consultant Cardiologist Patient Information What is heart failure? 3 What is the treatment
Repair of Hydrocele. Patient Information. Day Surgery. Ward 3, Leigh Infirmary
 Repair of Hydrocele Patient Information Day Surgery Ward 3, Leigh Infirmary Author ID: LS Leaflet Number: SW3.002 Version: 5 Name of Leaflet: Repair of Hydrocele Date Produced: August 2017 Review Date:
Repair of Hydrocele Patient Information Day Surgery Ward 3, Leigh Infirmary Author ID: LS Leaflet Number: SW3.002 Version: 5 Name of Leaflet: Repair of Hydrocele Date Produced: August 2017 Review Date:
Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute
 Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having an Abdominal Aortic Aneurysm (AAA) and it has
Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having an Abdominal Aortic Aneurysm (AAA) and it has
Home intravenous and intramuscular antibiotics
 Home intravenous and intramuscular antibiotics Children s Community Nursing Service 0161 206 2370 All Rights Reserved 2018. Document for issue as handout. This booklet has been given to you because your
Home intravenous and intramuscular antibiotics Children s Community Nursing Service 0161 206 2370 All Rights Reserved 2018. Document for issue as handout. This booklet has been given to you because your
Your surgeon will order pre-operative testing before you have surgery.
 Tests You May Need Prior to Surgery Your surgeon will order pre-operative testing before you have surgery. These tests give your surgeon valuable information regarding your current health condition. Below
Tests You May Need Prior to Surgery Your surgeon will order pre-operative testing before you have surgery. These tests give your surgeon valuable information regarding your current health condition. Below
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Crossover bypass graft surgery Vascular Surgery Patient Information Leaflet
 Crossover bypass graft surgery Vascular Surgery Patient Information Leaflet Crossover bypass graft surgery Information for patients from the Vascular Surgery Service This leaflet tells you about the operation
Crossover bypass graft surgery Vascular Surgery Patient Information Leaflet Crossover bypass graft surgery Information for patients from the Vascular Surgery Service This leaflet tells you about the operation
Having a diagnostic catheter angiogram
 Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Hydrocele repair. Information for parents and carers
 Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Antegrade Ureteric Stent
 Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
Antegrade Ureteric Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as an antegrade ureteric stent. It explains what is involved and the possible
Laparoscopic Cholecystectomy
 Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Varicose Veins Operation. Patient Information Leaflet
 Varicose Veins Operation Patient Information Leaflet April 2017 1 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the leaky
Varicose Veins Operation Patient Information Leaflet April 2017 1 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the leaky
Patient Information. A guide to your anaesthetic
 Patient Information A guide to your anaesthetic This booklet has been produced to answer your questions and to help ease your mind about the anaesthetic you are to have. Contents Page 1. What is anaesthesia?
Patient Information A guide to your anaesthetic This booklet has been produced to answer your questions and to help ease your mind about the anaesthetic you are to have. Contents Page 1. What is anaesthesia?
Femoropopliteal bypass graft
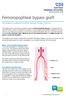 Femoropopliteal bypass graft Information for patients from the Vascular Surgery Service This leaflet tells you about the operation known as femoropopliteal bypass; it explains what is involved before,
Femoropopliteal bypass graft Information for patients from the Vascular Surgery Service This leaflet tells you about the operation known as femoropopliteal bypass; it explains what is involved before,
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Laparotomy for large retroperitoneal mass:
 Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for Patients having Total Knee Replacement Surgery
 Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Arch Angiography. Exceptional healthcare, personally delivered
 Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Femoral endarterectomy
 Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Knee joint arthroscopy
 Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Sedation explained. Information for patients. First Edition
 Sedation explained Information for patients First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet explains what sedation is, how it works and when you may need it. It also explains the benefits and
Sedation explained Information for patients First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet explains what sedation is, how it works and when you may need it. It also explains the benefits and
Gynaecology Department Patient Information Leaflet
 Laparoscopy Gynaecology Department Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called a laparoscopy. It explains what the operation involves, why it is
Laparoscopy Gynaecology Department Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called a laparoscopy. It explains what the operation involves, why it is
KIDNEY TRANSPLANT - A TREATMENT OPTION
 KIDNEY TRANSPLANT - A TREATMENT OPTION Page 1/5 WHAT IS A KIDNEY TRANSPLANT? When kidney failure becomes very advanced, your kidneys are so damaged they can no longer do their job. A transplant is a treatment
KIDNEY TRANSPLANT - A TREATMENT OPTION Page 1/5 WHAT IS A KIDNEY TRANSPLANT? When kidney failure becomes very advanced, your kidneys are so damaged they can no longer do their job. A transplant is a treatment
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Enhanced Recovery After Surgery (ERAS) Diary
 Cardiac Surgery Enhanced Recovery After Surgery (ERAS) Diary Patient s Name: Options available If you d like a large print, audio, Braille or a translated version of this leaflet then please call: 01253
Cardiac Surgery Enhanced Recovery After Surgery (ERAS) Diary Patient s Name: Options available If you d like a large print, audio, Braille or a translated version of this leaflet then please call: 01253
Arthroscopy of the ankle. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Arthroscopy of the ankle Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Arthroscopy of the ankle Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Varicoceles can cause various problems, including subfertility.
 This leaflet has been provided to help answer some of the questions you or those who care for you may have about percutaneous abscess drainage. It is not meant to replace the consultation between you and
This leaflet has been provided to help answer some of the questions you or those who care for you may have about percutaneous abscess drainage. It is not meant to replace the consultation between you and
Endovascular Aneurysm Repair (EVAR)
 Endovascular Aneurysm Repair (EVAR) Exceptional healthcare, personally delivered You have been diagnosed with an abdominal aortic aneurysm (AAA). This means that the main artery in your abdomen (the aorta)
Endovascular Aneurysm Repair (EVAR) Exceptional healthcare, personally delivered You have been diagnosed with an abdominal aortic aneurysm (AAA). This means that the main artery in your abdomen (the aorta)
Robotic-assisted lingual tonsillectomy for sleep apnoea
 Robotic-assisted lingual tonsillectomy for sleep apnoea You have been given this leaflet because you have been referred for a robotic-assisted lingual tonsillectomy for sleep apnoea. This leaflet offers
Robotic-assisted lingual tonsillectomy for sleep apnoea You have been given this leaflet because you have been referred for a robotic-assisted lingual tonsillectomy for sleep apnoea. This leaflet offers
This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation.
 Page 1 of 5 Your anaesthetic Introduction This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation. Who is an anaesthetist? Anaesthetists
Page 1 of 5 Your anaesthetic Introduction This leaflet provides information for patients due to have an operation or procedure with general anaesthetic and/or sedation. Who is an anaesthetist? Anaesthetists
Catheter Ablation for Supra-ventricular Tachycardia
 Additional Notes Our mission To provide the excellent care we would expect for our families. The Royal Bournemouth Hospital, Castle Lane East, Bournemouth, Dorset, BH7 7DW The Bournemouth Hospital Charity
Additional Notes Our mission To provide the excellent care we would expect for our families. The Royal Bournemouth Hospital, Castle Lane East, Bournemouth, Dorset, BH7 7DW The Bournemouth Hospital Charity
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Your child s general anaesthetic for dental treatment
 Questions you may like to ask your anaesthetist Q Who will give my child s anaesthetic? Q Is this the only type of anaesthetic possible for dental treatment? Q Have you often used this type of anaesthetic?
Questions you may like to ask your anaesthetist Q Who will give my child s anaesthetic? Q Is this the only type of anaesthetic possible for dental treatment? Q Have you often used this type of anaesthetic?
Endoscopy Unit Pyloric and Duodenal Stent insertion
 Endoscopy Unit Pyloric and Duodenal Stent insertion Information for patients Your doctor has recommended that you have a Pyloric or Duodenal Stent Insertion. This leaflet will explain the procedure and
Endoscopy Unit Pyloric and Duodenal Stent insertion Information for patients Your doctor has recommended that you have a Pyloric or Duodenal Stent Insertion. This leaflet will explain the procedure and
Superior vena cava stent
 Radiology department Superior vena cava stent Introduction This leaflet tells you about the procedure known as superior vena cava (SVC) stent insertion. It explains what is involved and what the benefits
Radiology department Superior vena cava stent Introduction This leaflet tells you about the procedure known as superior vena cava (SVC) stent insertion. It explains what is involved and what the benefits
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
Mr Sanjeev Sarin MS FRCS. Aortic Aneurysms Patient Information Sheet
 Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Laser Trans Urethral Resection of Prostate (TURP)
 Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Having MR Small Bowel (MR Enterography)
 Having MR Small Bowel (MR Enterography) Information for Patients In this leaflet: Introduction 2 What is an MR Small Bowel?..2 What do I need to do to before my scan?....2 Where do I go when I arrive at
Having MR Small Bowel (MR Enterography) Information for Patients In this leaflet: Introduction 2 What is an MR Small Bowel?..2 What do I need to do to before my scan?....2 Where do I go when I arrive at
Patient Information Coronary Angiogram
 Patient Information Coronary Angiogram Cardiac Suite Cardiology Department What is a coronary angiogram? A coronary angiogram is an invasive investigation to detect signs of heart disease, such as narrowing
Patient Information Coronary Angiogram Cardiac Suite Cardiology Department What is a coronary angiogram? A coronary angiogram is an invasive investigation to detect signs of heart disease, such as narrowing
Having a ureteric stent inserted
 Having a ureteric stent inserted This leaflet explains more about having a ureteric stent inserted. It describes the benefits, risks, alternatives and what you can expect when you come to hospital. If
Having a ureteric stent inserted This leaflet explains more about having a ureteric stent inserted. It describes the benefits, risks, alternatives and what you can expect when you come to hospital. If
