WRITER TRISTAN WALKER TABLE OF CONTENTS. The Basics of cardiac pharmacology 2007
|
|
|
- Douglas Cole
- 5 years ago
- Views:
Transcription
1 WRITER TRISTAN WALKER TABLE OF CONTENTS 1. WHAT ARE THE MAJOR CLASSES OF CARDIAC DRUGS? HOW DO THEY WORK? CONSIDERATIONS FOR THE PEDIATRIC PATIENT SUMMARY TABLE...10 REFERENCES
2 1. What are the major classes of cardiac drugs? There are 7 classes of drugs grouped according to their physiologic actions 1. Inotropic Drugs a. Digitalis Glycosides b. Sympathomimetic Amines c. Phosphodiesterase Inhibitors 2. Vasodilator Drugs a. Angiotensin-Converting Enzyme Inhibitors b. Angiotensin II type 1 Receptor Antagonists c. Direct-acting vasodilators d. Calcium Channel Blockers e. Organic Nitrates 3. Anti-adrenergic Drugs a. Central adrenergic inhibitors b. Sympathetic Nerve Ending Antagonists c. Peripheral Alpha-adrenergic receptor antagonists d. Beta-adrenergic receptor antagonists 4. Anti-arrhythmic Drugs a. Class I Anti-arrhythmics i. Class IA Anti-arrhythmics ii. Class IB Anti-arrhythmics iii. Class IC Anti-arrhythmics b. Class II Anti-arrhythmics c. Class III Anti-arrhythmics d. Class IV Anti-arrhythmics e. Adenosine 5. Diuretics a. Loop Diuretics b. Thiazide Diuretucs c. Potassium-sparing Diuretics 6. Ant-thrombotic Drugs a. Platelet inhibitors b. Anti-coagulant Drugs 7. Lipid regulating Drugs a. HMG CoA Reductase Inhibitors b. Bile Acid Binding Agents c. Niacin d. Fibrates 2
3 2. How do they work? 1. Inotropic Drugs Inotropic drugs work by increasing the force of ventricular contraction, for indication impaired myocardial systolic function. Although each drug in this group work through a different mechanism they generally all work through to improve cardiac contraction by increasing intracellular calcium concentration. When the intracellular calcium is increased the cardiac actin / myosin interactions are augmented resulting in increased stroke volume and cardiac output for each ventricular filling. a. Digitalis Glycosides (Digoxin) Digoxin is perhaps one the most commonly used cardiac glycoside, and has been studied extensively. Digoxin works by inhibiting the sarcolemma Na-K ATPase activity which results in an increase in the intra-cellular Na concentration. This results in an increase in transsarcolemma sodium gradient and increases the Na/Ca exchange. The end result is that the intracellular Ca concentration is increased, which means that more Ca is available to the contractile proteins. The myocardial response results in increased contractility and increased cardiac output. Similarly the increased intra-cellular sodium concentration delays repolarization and therefore decreases both sinus rate and AV conduction. b. Sympathomimetic Amines Adrenergic agonists mimic the effect of the sympathetic nervous system. Stimulation of the Beta1-adrenergic receptors in the heart results in positive inotropic (increases contractility), chronotropic (increases heart rate), dromotropic (increases rate of conduction through AV node) and lusitropic (increases relaxation of myocardium during diastole) effects. The effects of the beta1 agonists are mediated by G-coupled protein stimulation which stimulates adenylyl cyclase and generates camp. The G-coupled protein stimulation ultimately results in the activation of camp-dependent protein kinases and the phosphorylation of key regulatory proteins in the cardiac myocytes. Care must be taken when prescribing these drugs in a pediatric setting. Several factors must be taken into consideration including: Loading conditions, volume status and responsiveness of peripheral vasculature. This can be especially tricky in critically ill infants and children. Furthermore, the exact titration of these drugs is further complicated by the fact that there are age dependent changes in receptor-effector coupling, kinase activities, substrate availability, phosphatase activity and camp hydrolysis by phosphodiesterases. These factors contribute to age related variability in responsiveness to the adrenergic agonists. Examples of Sympathomimetic Amines: Drug Name Notes Dopamine Dopamine is an endogenous catecholamine precursor of epinephrine which is capable of directly and indirectly increasing blood pressure. Dopamine is administered as a continuous infusion. Dopamine has specific dopaminergic (DA) receptor effects at low concentrations, Beta1 receptor effects (positive inotropy and chronotropy) at moderate concentrations, and Alpha1 receptor effects (vasoconstriction) at high concentrations. Dopamine also causes renal vasodilation (controvercial). Dobutamine Dobutamine affects mainly the beta 1 adrenergic receptors. In children, Dobutamine increases the contractility and heart rate, thereby improving cardiac output. As a result, systemic vascular resistance may decline (secondary vasodilation). Dobutamine does not dilate renal vasculature. Dobutamine is often used in conjunction with Dopamine, considering the balancing effects on peripheral vascular resistance. 3
4 Isoproterenol Isoproterenol is a synthetic catecholamine that is selective in Beta receptor agonism. Administration will result in the stimulation of both the Beta1 receptors found primarily in the myocardium as well as the peripheral Beta2 receptors. Administration of Isoproterenol increases cardiac contractility and heart rate via the Beta1 receptor stimulation, while reducing systemic vascular resistance as a result from the Beta2 stimulation. Isoproterenol reduces pulmonary vascular resistance and can help patients with pulmonary hypertension. Adverse side-effects include sinus tachycardia and arrhythmias and because of this patients must be monitored closely. c. Phosphodiesterase Inhibitors Are drugs that control the degradation of intracellular camp. With increased intracellular camp levels the sarcoplasmic calcium concentration increases, resulting in increased cardiac muscle contractility (positive inotropy), with little effect on chronotropy. In the vasculature increased camp levels associate with smooth muscle relaxation and vasodilation. Examples of Phosphodiesterase Inhibitors Drug Name Notes Milrinone Milrinone is a potent and selective Phosphodiesterase Inhibitor. Generally Milrinone tends to be better tolerated in the pediatric population than Amrinone, but may cause significant hypotension due to the vasodilating effect on peripheral vasculature. It can also cause thrombocytopenia with prolonged use. Dobutamine is often preferred to Milrinone in neonates, due to its better side effect profile. Amrinone A relatively weak and non-selective phosphodiesterase inhibitor. Long term oral therapy is associated with significant toxic effects. Not used often in pediatrics. A comparison of the different types of Inotropic drugs Class Type Examples Predominant Agonist Effect Inotropic Digitalis Glycosides Sympathomimetic Amines Phosphodiesterase Inhibitors Digoxin n/a Increases intracellular Ca. Contractility After load Heart Rate Dopamine, Beta1=DA1>Alpha Dobutamine, Beta1 ( ) Isoproterenol, Beta1=Beta2 Epinephrine, Beta1=Beta2=Alpha Norepinephrine Beta1=Alpha Amrinone, Milrinone n/a ( ) Increases camp, intracellular Ca and vasodilate 4
5 2. Vasodilator Drugs Initial vasoconstriction is a mechanism used by the body to compensate for falling cardiac output. This vasoconstriction is mainly mediated by norepinephrine and angiotensin II. Venous constriction may ultimately result in pulmonary congestion as the pulmonary capillary hydrostatic pressure rises. Venous constriction can also result in an increase in the resistance against which the left ventricle must contract and thereby impedes cardiac output. Thus, vasodilator drugs are given to mediate the increased constriction and reduced the unwanted side effects of the compensatory mechanisms at work. These drugs can act to reduce elevated blood pressure and are therefore anti-hypertensives. Each of the vasodilator drugs work at specific vascular sites, and some (ACE inhibitors, alpha-blockers and sodium nitroprusside) are able to work on both sides of the circulation. 3. Anti-adrenergic Drugs Normally stimulation of a sympathetic nerve results in norepinephrine being released and stimulating alpha or beta receptors. Generally - each drug works by interfering with the sympathetic nervous system 4. Anti-arrhythmic Drugs a) Although a number of different classification systems exist, these drugs are commonly separated into four groups (Classes I through IV) based on their mechanism of action, and then there are those that do not fall into this classification scheme and are simply named (such as Adenosine) The main reason to use these drugs is to abolish the mechanisms by which tachyarrhythmias occur. b) Class I Anti-arrhythmics Block the fast sodium channel responsible for phase 0 depolarization of the action potential Further divided into three subtypes based on the degree of sodium channel blockade and the effect of the drug on the cell s refractory period c) Class II Anti-arrhythmics Beta-adrenergic receptor blockers d) Class III Anti-arrhythmics These drugs significantly prolong the action potential with little effect on the rise of phase 0 depolarization The mechanism of action is through blocking the repolarizing potassium current during the phase 2 and phase 3 of the action potential e) Class IV Anti-arrhythmics Block the slow L-type calcium channel f) Adenosine An endogenous nucleoside with a very short half life Most effective drug for the elimination of re-entrant PSVT Binds to specific adenosine receptors and activates potassium channels. When the potassium channels are activated the inward potassium current hyperpolarizes the cell membrane and thereby suppresses spontaneous depolarization of the SA node as well as slows conduction through the AV node. 5
6 5. Diuretics Most often used to treat heart failure and hypertension and are considered to be the mainstay of anti-congestive therapy. With heart failure there is an enhanced renal re-absorption of sodium and water which results in peripheral edema and pulmonary congestion. Diuretics are used to relieve the congestive symptoms associated with the excess fluid in the extra-cellular space. The clinical response to a diuretic depends on how efficiently salt and water is delivered to the renal tubule. a) Loop Diuretics This type of diuretic works at the loop of Henle. At the loop of Henle the loop diuretics inhibit chloride-sodium-potassium co-transport in the thick ascending limb. This results in a reduction of the reabsorbed chloride, sodium and potassium, as well as a net increase in the excretion of free water. b) Thiazide Diuretics These work by inhibiting the sodium and chloride transport in the distal convoluted tubule of the nephron. c) Potassium Sparing Diuretics The potassium sparing diuretics are anti-congestive, i.e they increase the loss of water without sacrificing potassium. d) Osmotic Diuretics The osmotic diuretics are reserved for the acute setting. These are generally used in patients with severe circulatory congestion with limited renal output. 6. Anti-thrombotic Drugs Modulation of the platelet function and the coagulation pathway helps to control the pathogenesis associated with such cardiovascular disorders as unstable angina and acute myocardial infarction as well as such disorders as venous thrombosis, thrombi associated with atrial fibrillation, dilated cardiomyopathy or mechanical prosthetic heart valves 7. Lipid regulating Drugs Help to modulate the pathogenesis of atherosclerosis Drugs that improve lipid outcomes are cardioprotective and inhibit the progression of atherosclerosis 6
7 3. Considerations for the pediatric patient Oral administration of drugs is the most common method used in children. Neonates, compared with infants and older children have less acid secretion in the stomach for the first few weeks after birth. GI transit time is more rapid for the first 5 years of childhood and this can affect the absorption of drugs administered in a sustained release preparation Drug distribution Drugs are distributed from the plasma to different organs on the basis of their affinity for tissues with high water or lipid content. For example in premature infants water represents 85% of BW whereas in the 1 year old child it represents 60%. When the percentage of extra-cellular water is high, as it would be in a neonate patient, a drug must be given in a larger dose n a milligram per kilogram basis to achieve the same serum concentration The amount of body water changes with development Age Extra-cellular Water (%) Total Body Water (%) Premature Infant Full term infant month old child year old child Adolescent Drug Metabolism Predominantly done in the liver 2 major pathways: Phase 1: metabolize substances and consist of the mixed function oxidase system, the cyp450 system and the N-demethylation pathways. Premature and full term neonates have 50 to 75% of these enzymes compared to levels in infants. This means that drugs metabolized by these systems may have a higher serum concentration for the same relative dose in neonates as compared to infants Phase 2: reactions conjugate endogenous compounds or specific drugs and their metabolites into water soluble entities by glucuronidation, or acetylation. These are usually adequate to metabolize most drugs and endogenous compounds by 1 to 2 weeks after birth in full term infants Doses of certain drugs must be adjusted accordingly in the first few weeks of neonatal life or else the neonate may be predisposed to drug toxicity Drug elimination The primary route of drug elimination of drugs is via the kidney. Drug elimination can also occur via the biliary, GI and respiratory tracts to a lesser degree. There is decreased renal elimination in neonates which must be accounted for when dosing Rx. 7
8 Development of the kidney in children Age GFR (ml/min/1.73m2) Full term neonate month month month years Max tubular secretion (mg/min/1.73) Usual therapeutic and toxic serum drug concentrations Cardiovascular agent Therapeutic level Toxic level Digoxin 0.5 to 2 ng/ml >3 ng/ml Lidocaine 2 to 5 µg/ml >6 µg/ml Quinidine 1 το 5 µg/ml >7 µg/ml Procainamide 4 το 10 µg/ml >10 µg/ml 8
9 9
10 4. Summary Table Class How do they work? Type Examples Inotropic Increase the force of the ventricular contraction when myocardial systolic function is impaired Digitalis Glycosides Digoxin Generally all drugs in this class improve cardiac contraction by increasing intracellular calcium concentration via various mechanisms Sympathomimetic Amines Dopamine, Dobutamine, Increased calcium serves to augment actin and Isoproterenol, Epinephrine, myosin interactions in the cardiac muscle and Norepinephrine thereby serves to increase the stroke volume and cardiac output for each ventricular filling. Phosphodiesterase Inhibitors Amrinone, Milrinone Vasodilator Mediate the increased constriction and reduced the unwanted effects of the compensatory mechanisms at work in the heart. Act to reduce blood pressure and are therefore anti-hypertensives Each of the vasodilator drugs work at specific vascular sites, and some are able to work on both sides of the circulation. Anti-Adrenergic Normally stimulation of a sympathetic nerve results in norepinephrine being released and stimulating alpha or beta receptors. Generally - each drug works by interfering with the sympathetic nervous system Angiotensin-Converting Enzyme Inhibitors Angiotensin II type 1 Receptor Antagonists Direct-acting vasodilators Calcium Channel Blockers Organic Nitrates Central adrenergic inhibitors Sympathetic Nerve Ending Antagonists Peripheral Alpha-adrenergic receptor antagonists Beta-adrenergic receptor antagonists - Enalapril, Captopril - Losartan - Digoxin - Verapamil - Nitroprusside Salbutamol (Beta 2 blocker) Prazosin (Alpha 1 blocker) 10
11 Anti-Arrhythmic Although a number of different classification systems exist, these drugs are commonly separated into four groups (Classes I through IV) based on their mechanism of action. The main reason to use these drugs is to abolish the mechanisms by which tacharrhythmias occur. Class I Anti-arrhythmics Block the fast sodium channel responsible for phase 0 depolarization of the action potential Further divided into three subtypes based on the degree of sodium channel blockade and the effect of the drug on the cell s refractory period o Class IA (medium blockade) o Class IB (minimal blockade) o Class IC (maximal blockade) 1A Procainamide 1B Lidocaine 1C - Propafenone Class II Anti-arrhythmics Beta-adrenergic receptor blockers Class III Anti-arrhythmics These drugs significantly prolong the action potential with little effect on the rise of phase 0 depolarization The mechanism of action is through blocking the repolarizing potassium current during the phase 2 and phase 3 of the action potential Propranolol Amiodarone Class IV Anti-arrhythmics Block the slow L-type calcium channel Verapamil 11
12 Diuretics Most often used to treat heart failure and hypertension and are used to relive the congestive symptoms associated with the excess fluid in the extra-cellular space Anti-thrombotic Drugs Lipid regulating Drugs Modulation of the platelet function and the coagulation pathway helps to control the pathogenesis associated with such cardiovascular disorders as unstable angina and acute myocardial infarction as well as such disorders as venous thrombosis, thrombi associated with atrial fibrillation, dilated cardiomyopathy or mechanical prosthetic heart valves improve lipid outcomes are cardio-protective and inhibit the progression of atherosclerosis Adenosine An endogenous nucleoside with a very short half life Most effective drug for the elimination of reentrant PSVT Binds to specific adenosine receptors and activates potassium channels. When the potassium channels are activated the inward potassium current hyperpolarizes the cell membrane and thereby suppresses spontaneous depolarization of the SA node as well as slows conduction through the AV node. Loop Diuretics Thiazide Diuretics Potassium-sparing Diuretics Platelet inhibitors Anti-coagulant Drugs HMG CoA Reductase Inhibitors Bile Acid Binding Agents Niacin Fibrates Adenosine Furosemide Hydrochlorothiazide Spironolactone Tissue Plasminogen Activator Warfarin, Heparin 12
13 13
14 References 1. Lilly, L.S. and Harvard Medical School., Pathophysiology of heart disease : a collaborative project of medical students and faculty. 2003, Philadelphia: Lippincott Williams & Wilkins. 2. Rudolph, A.M., R.K. Kamei, and K.J. Overby, Rudolph's fundamentals of pediatrics. 2002, New York: McGraw-Hill, Medical Pub. Division. 3. Allen, H.D., F.H. Adams, and A.J. Moss, Moss and Adams' heart disease in infants, children, and adolescents : including the fetus and young adult. 2001, Philadelphia, PA: Lippincott Williams and Wilkins. 14
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Drugs Used in Heart Failure. Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia
 Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
Fundamentals of Pharmacology for Veterinary Technicians Chapter 8
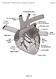 Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Heart failure. Failure? blood supply insufficient for body needs. CHF = congestive heart failure. increased blood volume, interstitial fluid
 Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Heart Failure. Dr. Alia Shatanawi
 Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
POSITIVE INOTROPIC AGENTS
 POSITIVE INOTROPIC AGENTS Positively inotropic agents increase the strength of contraction of heart muscle (myocardial contractility). Drugs of this group include: Cardioactive inotropes (digoxin, digitoxin);
POSITIVE INOTROPIC AGENTS Positively inotropic agents increase the strength of contraction of heart muscle (myocardial contractility). Drugs of this group include: Cardioactive inotropes (digoxin, digitoxin);
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood:
 Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Dysrhythmias. Dysrythmias & Anti-Dysrhythmics. EKG Parameters. Dysrhythmias. Components of an ECG Wave. Dysrhythmias
 Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
7/21/2017. Learning Objectives. Current Cardiovascular Pharmacology. Epinephrine. Cardiotonic Agents. Epinephrine. Epinephrine. Arthur Jones, EdD, RRT
 Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Chapter 2 ~ Cardiovascular system
 Chapter 2 ~ Cardiovascular System: General Section 1 of 6 Chapter 2 ~ Cardiovascular system 2.1 Positive inotropic drugs 2.1.1 Cardiac glycosides DIGOXIN 2.2 Diuretics Elixir 50micrograms in 1ml Injection
Chapter 2 ~ Cardiovascular System: General Section 1 of 6 Chapter 2 ~ Cardiovascular system 2.1 Positive inotropic drugs 2.1.1 Cardiac glycosides DIGOXIN 2.2 Diuretics Elixir 50micrograms in 1ml Injection
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS)
 DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
Chapter 10 Worksheet Blood Pressure and Antithrombotic Agents
 Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Beta 1 Beta blockers A - Propranolol,
 Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
Pharma Lecture 3 Beta blockers that we are most interested in are the ones that target Beta 1 receptors. Beta blockers A - Propranolol, it s a non-selective competitive antagonist of beta 1 and beta 2
Congestive Heart Failure
 Congestive Heart Failure (CHF) Congestive Heart Failure - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@vcu.edu Heart failure:
Congestive Heart Failure (CHF) Congestive Heart Failure - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@vcu.edu Heart failure:
Atrial fibrillation in the ICU
 Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Chapter 14. Agents used in Cardiac Arrhythmias
 Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Δακτυλίτιδα και Ινότροπα Φάρμακα στην Καρδιακή Ανεπάρκεια. Ι.Κανονίδης
 Δακτυλίτιδα και Ινότροπα Φάρμακα στην Καρδιακή Ανεπάρκεια Ι.Κανονίδης Cardiac Glycosides Chronic Congestive Heart Failure DIGOXIN Na-K ATPase Na + K + Na-Ca Exchange Na + Ca ++ Ca ++ K + Na + Myofilaments
Δακτυλίτιδα και Ινότροπα Φάρμακα στην Καρδιακή Ανεπάρκεια Ι.Κανονίδης Cardiac Glycosides Chronic Congestive Heart Failure DIGOXIN Na-K ATPase Na + K + Na-Ca Exchange Na + Ca ++ Ca ++ K + Na + Myofilaments
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis.
 Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
Potassium regulation. -Kidney is a major regulator for potassium Homeostasis. Normal potassium intake, distribution, and output from the body. Effects of severe hyperkalemia Partial depolarization of cell
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients. Keliana O Mara, PharmD August 4, 2018
 The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
Chapter 10. Learning Objectives. Learning Objectives 9/11/2012. Congestive Heart Failure
 Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
Chapter 10 Congestive Heart Failure Learning Objectives Explain concept of polypharmacy in treatment of congestive heart failure Explain function of diuretics Learning Objectives Discuss drugs used for
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Intravenous Infusions
 Intravenous Infusions 1) An IV insulin infusion can be used for patients: a) with out of control diabetes b) with DKA (Diabetic Ketoacidosis) c) after a heart attack 2) Hyperglycemia is an adaptive response
Intravenous Infusions 1) An IV insulin infusion can be used for patients: a) with out of control diabetes b) with DKA (Diabetic Ketoacidosis) c) after a heart attack 2) Hyperglycemia is an adaptive response
Vasoactive Medications. Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis
 Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Cardiovascular drugs
 chapter 13 Cardiovascular drugs Cardiovascular drugs act on the heart or blood vessels to control the cardiovascular system. They are used to treat a variety of conditions from hypertension to chronic
chapter 13 Cardiovascular drugs Cardiovascular drugs act on the heart or blood vessels to control the cardiovascular system. They are used to treat a variety of conditions from hypertension to chronic
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
Antihypertensives. Antihypertensive Classes. RAAS Inhibitors. Renin-Angiotensin Cascade. Angiotensin Receptors. Approaches to Hypertension Treatment
 Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
CONGESTIVE CARDIAC FAILURE. Dr.T.Rajathilagam, M.D., S.R.M. Medical College
 CONGESTIVE CARDIAC FAILURE Dr.T.Rajathilagam, M.D., S.R.M. Medical College HEART FUNCTIONS Your heart is an amazing powerhouse that pumps and circulates 5 or 6 gallons of blood each minute through your
CONGESTIVE CARDIAC FAILURE Dr.T.Rajathilagam, M.D., S.R.M. Medical College HEART FUNCTIONS Your heart is an amazing powerhouse that pumps and circulates 5 or 6 gallons of blood each minute through your
Cardiac Properties MCQ
 Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D.
 Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Leading Causes of Death in the U.S. Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Blood flow at rest and exercise
 Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Medical Management of Acutely Decompensated Heart Failure. William T. Abraham, MD Director, Division of Cardiovascular Medicine
 Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
Cardiovascular Physiology and Pharmacology
 Cardiovascular Physiology and Pharmacology Peter Paal Perioperative Medicine, Barts Heart Centre St. Bartholomew s Hospital, Barts Healt NHS Queen Mary University of London and Department of Anaesthesiology
Cardiovascular Physiology and Pharmacology Peter Paal Perioperative Medicine, Barts Heart Centre St. Bartholomew s Hospital, Barts Healt NHS Queen Mary University of London and Department of Anaesthesiology
Drug Therapy of Heart Failure. Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014
 Drug Therapy of Heart Failure Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Drug Therapy of Heart Failure Definition of Heart Failure Causes Classifications
Drug Therapy of Heart Failure Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Drug Therapy of Heart Failure Definition of Heart Failure Causes Classifications
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Hypertension. Penny Mosley MRPharmS
 Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Hypertension Penny Mosley MRPharmS Outline of presentation Introduction to hypertension Physiological control of arterial blood pressure What determines our bp? What determines the heart rate? What determines
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs
 Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
The Cardiovascular System
 Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Beta-blockers. Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol.
 Drugs of CVS Beta-blockers Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol. Atenolol.cardioselective Propranolol, nonselective Bisoprolol, cardioselective Metoprolol Carvedilol, alpha
Drugs of CVS Beta-blockers Atenolol. Propranolol. Bisoprolol. Metoprolol. Labetalol. Carvedilol. Atenolol.cardioselective Propranolol, nonselective Bisoprolol, cardioselective Metoprolol Carvedilol, alpha
Chapter / Section / Drug
 2 Cardiovascular System 2.1 Positive inotropic drugs Digoxin Digoxin specific antibody ( DigiFab ) 2.2 Diuretics 2.2.1 Thiazides and related diuretics Indapamide (1 st Line) Bendroflumethiazide Metolazone
2 Cardiovascular System 2.1 Positive inotropic drugs Digoxin Digoxin specific antibody ( DigiFab ) 2.2 Diuretics 2.2.1 Thiazides and related diuretics Indapamide (1 st Line) Bendroflumethiazide Metolazone
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
Diagnosis & Management of Heart Failure. Abena A. Osei-Wusu, M.D. Medical Fiesta
 Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Diagnosis & Management of Heart Failure Abena A. Osei-Wusu, M.D. Medical Fiesta Learning Objectives: 1) Become familiar with pathogenesis of congestive heart failure. 2) Discuss clinical manifestations
Angina pectoris due to coronary atherosclerosis : Atenolol is indicated for the long term management of patients with angina pectoris.
 Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Table 1. Diuretics. Drugs Mechanisms of Action Indications Adverse Drug Effects. Table 2. Electrolyte Modifiers.
 Table 1. Diuretics. hydrochlorothiazide 23 furosemide 23 triamterene 23 Inhibits sodium reabsorption at the distal convoluted tubule Inhibits sodium reabsorption at the loop of Henle Competitive inhibitor
Table 1. Diuretics. hydrochlorothiazide 23 furosemide 23 triamterene 23 Inhibits sodium reabsorption at the distal convoluted tubule Inhibits sodium reabsorption at the loop of Henle Competitive inhibitor
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Images have been removed from the PowerPoint slides in this handout due to copyright restrictions.
 Heart Failure Heart Failure Introduction and History AHA 2015 Statistics About 6 million Americans 870,000 new cases each year 1 in 9 deaths related to HF Almost 1 million hospitalizations each year (cost
Heart Failure Heart Failure Introduction and History AHA 2015 Statistics About 6 million Americans 870,000 new cases each year 1 in 9 deaths related to HF Almost 1 million hospitalizations each year (cost
Milrinone. wen-3177v02 Page 1 of 8
 Milrinone Lactate Injection Rx only DESCRIPTION Milrinone Lactate Injection, is a member of a new class of bipyridine inotropic/vasodilator agents with phosphodiesterase inhibitor activity, distinct from
Milrinone Lactate Injection Rx only DESCRIPTION Milrinone Lactate Injection, is a member of a new class of bipyridine inotropic/vasodilator agents with phosphodiesterase inhibitor activity, distinct from
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
During exercise the heart rate is 190 bpm and the stroke volume is 115 ml/beat. What is the cardiac output?
 The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
PRINCIPLES OF DIURETIC ACTIONS:
 DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
DIURETIC: A drug that increases excretion of solutes Increased urine volume is secondary All clinically useful diuretics act by blocking Na + reabsorption Has the highest EC to IC ratio = always more sodium
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pharmacology - Problem Drill 11: Vasoactive Agents
 Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
B. 14 Antidysrhythmic drugs. a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification
 B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
The adrenergic drugs affect receptors that are stimulated by norepinephrine or epinephrine. Some adrenergic drugs act directly on the adrenergic
 Adrenergic drugs The adrenergic drugs affect receptors that are stimulated by norepinephrine or epinephrine. Some adrenergic drugs act directly on the adrenergic receptor (adrenoceptor) by activating it
Adrenergic drugs The adrenergic drugs affect receptors that are stimulated by norepinephrine or epinephrine. Some adrenergic drugs act directly on the adrenergic receptor (adrenoceptor) by activating it
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
PITTMed Cardiology. Pharmacology Modules. Learning Objectives. Site Contents. Fall 2018
 PITTMed Cardiology Fall 2018 Site Contents Pharmacology Modules Please complete the following modules during the first week of class: Adrenergics Cholinergics Adrenergic Drugs in Cardiology Hypercalcemia
PITTMed Cardiology Fall 2018 Site Contents Pharmacology Modules Please complete the following modules during the first week of class: Adrenergics Cholinergics Adrenergic Drugs in Cardiology Hypercalcemia
Staging and Treating Patients with Heart Failure Henry Green, III, DVM, DACVIM Purdue University West Lafayette, IN
 Staging and Treating Patients with Heart Failure Henry Green, III, DVM, DACVIM Purdue University West Lafayette, IN There are many different diseases that can cause signs of congestive heart failure(chf)
Staging and Treating Patients with Heart Failure Henry Green, III, DVM, DACVIM Purdue University West Lafayette, IN There are many different diseases that can cause signs of congestive heart failure(chf)
Improving Transition of Care in Congestive Heart Failure. Mark J. Gloth, DO, MBA. Vice President, Chief Medical Officer HCR ManorCare
 Improving Transition of Care in Congestive Heart Failure Mark J. Gloth, DO, MBA. Vice President, Chief Medical Officer HCR ManorCare Heart Failure Fastest growing clinical cardiac disease in the United
Improving Transition of Care in Congestive Heart Failure Mark J. Gloth, DO, MBA. Vice President, Chief Medical Officer HCR ManorCare Heart Failure Fastest growing clinical cardiac disease in the United
Medical Management of Acute Heart Failure
 Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Critical Care Medicine and Trauma Medical Management of Acute Heart Failure Mary O. Gray, MD, FAHA Associate Professor of Medicine University of California, San Francisco Staff Cardiologist and Training
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Review of Cardiac Mechanics & Pharmacology 10/23/2016. Brent Dunworth, CRNA, MSN, MBA 1. Learning Objectives
 Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition
 TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες. Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο
 Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο Όλες οι κοιλιακές αρρσθμίες δεν είναι ίδιες Υπάρτοσν διαθορές ζηον πληθυσμό, ηον μηχανισμό
Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο Όλες οι κοιλιακές αρρσθμίες δεν είναι ίδιες Υπάρτοσν διαθορές ζηον πληθυσμό, ηον μηχανισμό
Physiology ( 14 questions )
 CVS Theory exam questions - Soul Batch - Physiology ( 14 questions ) 1- Which of the following increases the circulatory filling pressure but not resistance? A- Endothelin B- Aldosterone C- Calcium D-
CVS Theory exam questions - Soul Batch - Physiology ( 14 questions ) 1- Which of the following increases the circulatory filling pressure but not resistance? A- Endothelin B- Aldosterone C- Calcium D-
Myocardial Infarction: Left Ventricular Failure
 CARDIOVASCULAR PHYSIOLOGY 93 Case 17 Myocardial Infarction: Left Ventricular Failure Marvin Zimmerman is a 52-year-old construction manager who is significantly overweight. Despite his physician's repeated
CARDIOVASCULAR PHYSIOLOGY 93 Case 17 Myocardial Infarction: Left Ventricular Failure Marvin Zimmerman is a 52-year-old construction manager who is significantly overweight. Despite his physician's repeated
a)-catecholamines // these are compounds which have the catechol nucleus as adrenaline, noradrenaline, isoprenaline, dopamine, dobutamine
 1 Adrenergic or sympathetic agonist: Are classified according to: I)- according to the chemical structure a)-catecholamines // these are compounds which have the catechol nucleus as adrenaline, noradrenaline,
1 Adrenergic or sympathetic agonist: Are classified according to: I)- according to the chemical structure a)-catecholamines // these are compounds which have the catechol nucleus as adrenaline, noradrenaline,
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Swans and Pressors. Vanderbilt Surgery Summer School Ricky Shinall
 Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall Shock, Swans, Pressors in 15 minutes 4 Reasons for Shock 4 Swan numbers to know 7 Pressors =15 things to know 4 Reasons for Shock Not enough
Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall Shock, Swans, Pressors in 15 minutes 4 Reasons for Shock 4 Swan numbers to know 7 Pressors =15 things to know 4 Reasons for Shock Not enough
Swans and Pressors. Vanderbilt Surgery Summer School Ricky Shinall
 Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall SHOCK Hypotension SHOCK Hypotension SHOCK=Reduction of systemic tissue perfusion, resulting in decreased oxygen delivery to the tissues.
Swans and Pressors Vanderbilt Surgery Summer School Ricky Shinall SHOCK Hypotension SHOCK Hypotension SHOCK=Reduction of systemic tissue perfusion, resulting in decreased oxygen delivery to the tissues.
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
M2 TEACHING UNDERSTANDING PHARMACOLOGY
 M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
M2 TEACHING UNDERSTANDING PHARMACOLOGY USING CVS SYSTEM AS AN EXAMPLE NIGEL FONG 2 JAN 2014 TODAY S OBJECTIVE Pharmacology often seems like an endless list of mechanisms and side effects to memorize. To
Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic
![Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic](/thumbs/90/103241154.jpg) Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
