Rate-Dependent Effects of Intravenous Lidocaine, Procainamide and Amiodarone on Intraventricular Conduction
|
|
|
- Lester Scott
- 5 years ago
- Views:
Transcription
1 JACC Vol. 6. No. I 179 Rate-Dependent Effects of Intravenous Lidocaine, Procainamide and Amiodarone on Intraventricular Conduction FRED MORADY, MD, FACC, LORENZO A. DICARLO, JR., MD, JEFFREY M. BAERMAN, MD, RYSZARD B. KROL, MD Ann Arbor, Michigan In this study, the duration of the QRS complex during ventricular pacing was used as an index of intraventricular conduction to quantitate the rate-dependent effects of intravenous lidocaine, procainamide and amiodarone. Right ventricular apical pacing (15 to 20 beats) was performed at cycle lengths of 600, 500, 400, 350, 300, 275 and 250 ms, before and 5 minutes after the intravenous administration of lidocaine in 11 patients (serum level 3.2 ± 0.8 JLg/ml [mean ± SD)), procainamide in 14 patients (serum level 8.2 ± 1.9 JLg/ml) and amiodarone in 12 patients (serum level 3.9 ± 1.2 JLg/ml). Electrocardiographic recordings were made at a paper speed of 150 mm/s. QRS duration was measured in a blinded fashion, with reproducibility within 5 %. In the control state, QRS duration was the same at all paced cycle lengths. After lidocaine, procainamide and amiodarone administration, the shortest paced cycle length with complete ventricular capture was 250 ± 0, 275 ± 38 and 264 ± 20 ms, respectively. At a paced cycle length of 600 ms, the increase in QRS duration compared with the control state was 1 ± 2 % with lidocaine (p > 0.05), 21 ± 7% with procainamide (p < 0.001) and 6 ± 6% with amiodarone (p < 0.05). At the shortest paced cycle length with complete capture, the increase in QRS duration compared with the control state was 20 ± 6% with lidocaine (p < 0.001), 42 ± 11 % with procainamide (p < 0.001) and 26 ± 4% with amiodarone (p < 0.001). The acute effects of lidocaine, procainamide and amiodarone on intraventricular conduction are rate-dependent, with the effects of intravenous amiodarone being more similar to those of lidocaine than those of procainamide. Prolongation of conduction occurs at a slower rate with procainamide than with lidocaine or amiodarone. These data suggest that each of these three drugs blocks sodium channels, and that recovery from block is slower with procainamide than with lidocaine or amiodarone. (J Am Coil Cardiol 1985;6:179-85) Lidocaine, procainamide and amiodarone have been shown to block sodium channels in a rate-dependent fashion in isolated muscle preparations (1-4). Depression in the maximal rate of rise of the action potential upstroke by these drugs is accentuated during rapid stimulation because as the rate increases, there is less time for sodium channels to recover from block. Because conduction in ventricular myocardium is dependent predominantly on the fast sodium current, depression of intraventricular conduction by lidocaine, procainamide and amiodarone would also be expected to occur in a rate-dependent fashion. Accordingly, lidocaine From the Division of Cardiology, Department of Internal Medicine, University Hospitals, University of Michigan Medical Center, Ann Arbor, Michigan. Manuscript received December 28, 1985; revised manuscript received February 12, 1985, accepted March 29, Address for reprints: Fred Morady, MD, Division of Cardiology, W , University Hospitals, University of Michigan Medical Center, 1405 East Ann Street, Ann Arbor, Michigan by the American College of Cardiology and procainamide have been found to cause rate-dependent slowing of intraventricular conduction in animal preparations (5,6). However, few studies have investigated the ratedependent effects of these drugs on intraventricular conduction in human subjects. Two studies (7,8) concluded that lidocaine did not have a rate-dependent effect on intraventricular conduction. In a preliminary report (9), the ratedependent effects on QRS duration of intravenous procainamide and lidocaine, and oral amiodarone and mexiletine, were assessed in small numbers of patients (three to five). To date, the rate-dependent effects of intravenous amiodarone on intraventricular conduction in human subjects have not been investigated. In this study, the acute rate-dependent effects on intraventricular conduction of intravenous lidocaine, procainamide and amiodarone were quantitated and compared. The duration of the QRS complex during ventricular pacing was used as an index of intraventricular conduction $3.30
2 180 MORADY ET AL. JACC Vol. 6, No, I Methods Patients studied. Thirty-seven patients (24 men and 13 women) who underwent electrophysiologic testing because of ventricular tachycardia or unexplained syncope were the subjects of this study. Their mean age (± SO) was 58 ± IS years. Twenty-three patients had coronary artery disease, eight had a dilated cardiomyopathy, one had mitral valve prolapse and five had no identifiable structural heart disease. Pacing protocol. Electrophysiologic testing was performed with the patients in the fasting, un sedated state after informed consent had been obtained, at least four half-lives after discontinuation of all antiarrhythmic drugs. One to three 6F quadripolar electrode catheters were positioned at various locations in the right atrium or ventricle, as clinically indicated. The pacing protocol (outlined later) was performed in the course of electropharmacologic testing in patients who had inducible ventricular tachycardia, or on completion of a normal electrophysiologic study in patients who had unexplained syncope. A quadripolar electrode catheter was positioned in the apex of the right ventricle. Pacing was performed at a current strength of twice diastolic threshold (pulse width 2 ms) with a programmable stimulator (Bloom Associates, Ltd.). In all patients, the pacing threshold was less than I rna. Right ventricular pacing was performed for at least IS to 20 beats at cycle lengths of 600, 500, 400, 350, 300, 275 and 250 rtis'. The last five QRS complexes of each pacing train were recorded on an Electronics for Medicine VRI2 recorder, at a paper speed of 150 mm/s. Electrocardiographic leads Vb land III were recorded. This pacing protocol was performed immediately before and 5 minutes after the administration 'dfiiidocaine in II patients, procainamide in 14 patients and amiodarone in 12 patients. The electrode catheter positioned in the right ventricular apex was not moved in the interim. The following intravenous dosing protocols were used: I) lidocaine: 100 mg over 2 minutes, followed by three 50 mg boluses at 5 minute intervals; a 2 mg/min continuous infusion was started immediately after the initial 100 mg bolus; 2) procainamide: 1 g at a rate of 50 mg/min; and 3) amiodarone: 10 mg/kg at a rate of 50 mg/min. A blood sample for determination of the appropriate serum drug level was drawn after completion of the pacing protocol (10 to 15 minutes). The mean serum levels of lidocaine, procainamide and amiodarone were 3.2 ± 0.8 /Lg/ml (range 1.7 to 4.3),8.2 ± I.9/Lg/ml (range 6.1 to 10.2) and 3.9 ± 1.2/Lg/ml (range 2.1 to 4.8), respectively. Data analysis. The duration of the QRS complex was measured from electrocardiographic lead III which, in all cases, provided the best definition of the onset and termination of the QRS complex. Patients were not included in this study if the onset or termination of the QRS complex was not well defined in any of the three monitored electrocardiographic leads. The duration of the last QRS complex of each paced train was measured in a blinded fashion by one of us (F.M.). Reproducibility, as assessed by independent measurement of the QRS complexes by another one of us (L.O.) was within 5%. All values are expressed as mean ± standard deviation. Statistical analysis was performed with paired or unpaired t test, as appropriate. Results In the control state, there was no significant difference in the QRS duration during ventricular pacing at the various cycle lengths. The shortest cycle length resulting in complete ventricular capture was 260 ± 15 ms. The ratedependent effects of lidocaine, procainamide and amio OFS (ms) 190 l \ 1,, ;, p<o.ol p<o.ool Lidocaine o Control Figure 1. Rate-dependent effects of lidocaine on QRS duration. The mean QRS duration (± 1 SD) is shown before and after lidocaine, during ventricular pacing at cycle lengths of 600 to 250 ms. The number of patients in whom there was complete ventricular capture at each paced cycle length is shown in parentheses below the corresponding cycle length. The mean QRS durations before and after lidocaine at each paced cycle length were compared with a paired t test ~~ZL~~~-L~~~~~~-=~4-~~~~~~ PACED CYCLE LENGTH (ms)
3 JACC Vol. 6, No. I July 1985: MORADY ET AL J pc o Procainamide o Control Figure 2. Rate-dependent effects of procainamide on QRS duration. Format as in Figure I, 200 QRS (ms) PACED CYCLE LENGTH (ms) darone on QRS duration are displayed in Figures I to 6 and Table I, Effects of lidocaine (Fig. 1 and 4). After the administration of lidocaine, at a paced cycle length of 600 ms, there was no change in QRS duration compared with the control state (164 ± 24 versus 162 ± 24 ms, p > 0,05), In all II patients who received lidocaine, there was complete ventricular capture at a paced cycle length of 250 ms, After lidocaine, at a paced cycle length of 250 ms, there was a 21 % increase in QRS duration compared with the control state (194 ± 30 versus 160 ± 24 ms, p < 0.001). Effects of procainamide (Fig. 2 and 5). After procainamide administration, at a paced cycle length of 600 ms, there was a 21 % increase in QRS duration compared with the control state (193 ± 30 versus 160 ± 15 ms, p < 0.00 I). In nine patients, the shortest cycle length resulting in complete ventricular capture was 250 ms, and in five patients, it was 300 or 350 ms (mean 273 ± 12). At the Figure 3. Rate-dependent effects of amiodarone on QRS duration, Format as in Figure L QRS (ms) 190 pc 0.02 pc o Amiodarone o Control l121 PACED CYCLE LENGTH (ms)
4 182 MORADY ET AL. JACC Vol. 6, No. I CONTROL LIDOCAINE 800ms 800ms 250ms 250ms Figure 4. Typical example of the rate-dependent effect of lidocaine on QRS duration. The last two or three paced complexes of a train of 15 to 20 stimuli are shown. In the control state, QRS duration was 153 ms at a paced cycle length of 600 and 250 ms. After lidocaine administration (serum level 3.4 ILgiml), the QRS duration was unchanged at a paced length of 600 ms, but increased by 22% to 187 ms at a paced cycle length of 250 ms. i.illl 11111:: 1;1"lli!:!::IIIIIIIIIII!I!II!111::II!III: lil!lii1!ll;ii!i':!":r!i!i.i l::!ii:llllli!illll::. 1II'I!IIII! ~200msshortest paced cycle length resulting in complete ventricular capture, there was a 41 % increase in QRS duration compared with the control state (232 ± 37 versus 164 ± 25 ms, p < 0.(01). Effects of amiodarone (Fig. 3 and 6). After amiodarone administration, at a paced cycle length of 600 ms, there was a 6% increase in QRS duration compared with the control state (160 ± 26 versus 152 ± 29 ms, p < 0.05). In eight patients, the shortest paced cycle length resulting in complete ventricular capture was 250 ms, and in three patients, it was 275 or 300 ms (mean 262 ± 21). At the shortest paced cycle length resulting in complete ventricular capture, there was a 26% increase in QRS duration compared with the control state (190 ± 38 versus ISO ± 28 ms, p < 0.(01). Comparison of drug effects (Table 1). At a paced cycle length of 600 ms, the increase in QRS duration compared with the control state after procainamide was significantly greater than after lidocaine or amiodarone (p < for both), and the increase after amiodarone was significantly greater than that after lidocaine (p < 0.001). At the shortest paced cycle length resulting in complete ventricular capture, the increase in QRS duration compared with the control state was significantly greater after procainamide than after lidocaine or amiodarone (p < for both), and the increase after amiodarone was significantly greater than that after lidocaine (p < 0.05). Discussion The results of this study indicate that intravenous lidocaine, procainamide and amiodarone all acutely prolong intraventricular conduction in a rate-dependent manner. Because sodium channel blockade is reflected by intraventric- CONTROL PROCAINAMIDE 600 ms 600 ms Figure S. Typical example of the rate-dependent effect of procainamide on QRS duration. In the control state, QRS duration was 167 ms and was not rate-dependent. After procainamide administration (serum level 7.9 ILgiml), QRS duration in 275 ms 300 ms ~\r'\r~\f 'V\J\;l creased by 20% to 200 ms at a paced cycle length of 600 ms, and by 36% to 227 ms at a paced cycle length of 300 ms. At paced cycle lengths shorter than 300 ms, there was 2: I ventricular capture ' !'III': ms~
5 JACC Vol. 6, No. I July 1985: MORADY ET AL. 183 CONTROL AMIODARONE 600 ms 600 ms Figure 6. A typical example of the rate-dependent effect of intravenous amiodarone on QRS duration. In the control state, QRS duration was 173 ms at a paced cycle length of 600 and 250 ms. After amiodarone administration (serum level 3.8 J,Lg/ml), QRS duration increased by 12% to 193 ms at a paced cycle length of 600 ms, and by 31 % to 227 ms at a paced cycle length of 275 ms. At a paced cycle length of 250 ms, there was 2: I ventricular capture. 250 ms 275 ms ryv-- vvv 73ms -"\ V lilllllllllllllllllllllllllllllllllllllllllllllllllilliiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiiii!i11i1i1i1iiiii '-200ms~ ular conduction, these findings are consistent with rate-dependent sodium channel blockade found previously (1-4) to occur in vitro in response to lidocaine, procainamide and amiodarone. Results of prior studies. In a preliminary report (9), the rate-dependent effects on QRS duration of intravenous procainamide and lidocaine and oral amiodarone and mexiletine were tested in groups of three to five patients each. With each drug, the QRS duration at a short ventricular pacing cycle length (290 ± 34 ms) was 10 to 12% greater than at a ventricular pacing cycle length of 500 ms. When the results of our study were analyzed in a similar fashion, intravenous lidocaine, procainamide and amiodarone were found to increase the QRS duration at a ventricular pacing cycle length of 300 ms to a value 10 to 11 % greater than at a cycle length of 500 ms. Our results therefore confirm these preliminary observations; however, they also highlight the contrasting effects of the three drugs since the study compared pre- and post-drug QRS duration at various pacing Table 1. Percent Change in QRS Duration After Lidocaine, Procainamide and Amiodarone Administration at a Ventricular Paced Cycle Length of 600 ms and at the Shortest Paced Cycle Length Resulting in Complete Ventricular Capture Lidocaine Procainamide Amiodarone (II patients) (14 patients) (12 patients) Percent change in QRS Paced CL 600 ms (A) I ± 2 (B) 21 ± 7 (C) 6 ± 6 Shortest paced CL (D) 20 ± 6 (E) 42 ± II (F) 26 ± 4 with complete capture Shortest paced CL with (G) 250 ± 0 (H) 275 ± 38 (I) 264 ± 20 complete capture (ms) p Values p < = D vs. A, E vs. B, F vs. C, B vs. A, B vs. C, C vs. A, E vs. D, E vs. F; p < 0.01 = H vs. G; P < 0.05 = F vs. D; P > 0.05 = H vs. I, I vs. G. Values are expressed as mean ± SD. CL = cycle length. cycle lengths, rather than only QRS duration at long and short pacing cycle lengths after drug administration. Effects of lidocaine. Lidocaine administration had little or no measurable effect on intraventricular conduction at a cycle length of 600 ms; depression of intraventricular conduction by lidocaine was manifest only at the more rapid pacing rates. In contrast, two prior studies (7,8) of the effects of lidocaine on intraventricular conduction in human subjects concluded that this drug did not have rate-dependent effects on conduction. However, the dose of lidocaine administered in these prior studies was only 50 to 150 mg and may not have yielded an adequate serum drug level. In addition, in these studies, intraventricular conduction was assessed by measurement of QRS duration during atrial pacing. The assessment of rate-dependent effects was therefore limited by the occurrence of atrioventricular nodal Wenckebach block. The use of ventricular pacing in our study avoided this limitation and allowed the attainment of more rapid rates than is possible with atrial pacing. Effects of procainamide. In contrast to the effects of lidocaine, procainamide slowed conduction to a significant degree (21%), even at a paced cycle of 600 ms. This suggests that there is more rapid recovery of blocked sodium channels with lidocaine than with procainarnide, such that at an interstimulus interval of 600 ms, recovery of sodium channels blocked by lidocaine is complete or nearly complete and no measurable prolongation of intraventricular conduction is observed. These findings are compatible with the results of in vitro studies (2) indicating that the recovery half-time of sodium channels blocked by lidocaine is 140 ms, whereas the corresponding recovery half-time in the case of procainamide is 1.8 seconds. These findings also explain why procainamide increases QRS duration during sinus rhythm whereas lidocaine does not (10), even though both drugs block sodium channels. Effects of intravenous amiodarone. The acute rate-dependent effects of intravenous arniodarone on intraventric-
6 184 MORADY ET AL. JACC Vol. 6. No. I ular conduction were intermediate to the effects of lidocaine and procainamide, with mild prolongation (6%) at a paced cycle length of 600 ms, and a maximal prolongation of 26% at the more rapid stimulation rates. The acute effects of intravenous amiodarone more closely resembled the effects of lidocaine than those of procainamide. In contrast, in vitro studies (4) have indicated that the time constant for recovery of sodium channels from amiodarone blockade is long (1.8 seconds), suggesting that significant prolongation of intraventricular conduction should occur at a paced cycle length of 600 ms. There are three possible explanations for this apparent discrepancy. First, although the serum amiodarone level in every patient tested with this drug was within or above the range of serum levels reported to be "therapeutic" for intravenous amiodarone (2 to 3 p,g/ml) (11) because the pacing protocol was performed only 5 minutes after completion of the amiodarone infusion, there may not have been adequate time for amiodarone to move from the intravascular into the tissue compartment. Second, because sodium channel blockade caused by admiodarone administration is both rate-dependent and voltage-dependent (4), the discrepancy may be attributed to voltage differences between the intact heart and isolated muscle preparations. Finally, there may be a difference between the rate-dependent effects of amiodarone in animals and human subjects. Intravenous amiodarone in treatment of ventricular tachycardia. There has been disagreement regarding the acute efficacy of intravenous amiodarone for the treatment of ventricular tachycardia. Some studies (11-16) reported that intravenously administered amiodarone is efficacious in the acute suppression of both spontaneous and induced ventricular tachycardia and ventricular premature depolarizations. However, other studies (17, 18) concluded that intravenous amiodarone has no acute antiarrhythmic effects on ventricular arrhythmias. Although some investigators (4) concluded that amiodarone has primary effects on the myocardial action potential which could account for its antiarrhythmic effects, others (19,20) found that the antiarrhythmic effects of amiodarone may be mediated by a disturbance in thyroid metabolism. The results of our study suggest that amiodarone does have a direct depressant effect on conduction through ventricular myocardium. This effect occurred acutely and cannot be explained by an alteration in thyroid metabolism. Intravenous amiodarone has little or no acute effect on ventricular refractoriness (15,16,18,21). Therefore, rate-dependent effects of amiodarone on intraventricular conduction may provide a potential mechanism of action by which intravenous amiodarone suppresses ventricular arrhythmias. No comments were made in this study on the relation between QRS duration during sinus rhythm, presence of bundle branch block or duration of HV interval and ratedependent effects on conduction because very few patients studied had bundle branch block or a prolonged HV interval. Conclusions. Lidocaine, procainamide and amiodarone all acutely prolong intraventricular conduction in a ratedependent fashion. The findings of this study provide in vivo corroboration of in vitro data indicating that each of these drugs blocks sodium channels. The rate-dependent response to these drugs suggests that recovery of blocked sodium channels occurs most rapidly with lidocaine, and least rapidly with procainamide. We express our gratitude to Lisa Hackbarth for her excellent secretarial assistance. References I. Hondeghem L, Katzung BG. Test of a model of antiarrhythmic drug action: effects of quinidine and lidocaine on myocardial conduction. Circulation 1980;61: Courtney KR. Interval-dependent effects of small antiarrhythmic drugs on excitability of guinea-pig myocardium. J Mol Cell Cardiol 1980; 12: Ehring GR, Hondeghem LM. Structural similarities and cardiac electrophysiological differences between lidocaine and procainamide. Proc West Pharmacol Soc 1980;23: Mason W, Hondeghem LM, Katzung BG. Amiodarone blocks inactivated cardiac sodium channels. Ptlugers Arch 1983;396: Man RYK, Dresel PE. A specific effect of lidocaine and tocainide on ventricular conduction of mid-range extrasystoles. J Cardiovasc Pharmacol 1979;1: Wald RW, Waxman MB, Downar E. The effect of antiarrhythmic drugs on depressed conduction and unidirectional block in sheep Purkinje fibers. Circ Res 1980;46: Rosen KM, Lau SH, Weiss MB, Damato AN. The effect of lidocaine on atrioventricular and intraventricular conduction in man. Am J Cardiol 1970;25: Bekheit S, Murtagh JG, Morton P, Fletcher E. Effect of lignocaine on conducting system of human heart. Br Heart J 1973;35: Mercer AB, Foster JR, Simpson RJ, Gettes LS. Use-dependency of antiarrhythmic drugs in the human heart (abstr). Circulation 1983;68 (suppl III):III Surawicz B, Lasseter KC. Effect of drugs on the electrocardiogram. Prog Cardiovasc Dis 1970;13: II. Mostow ND, Rakita L, Vrobel TR, Noon D, Blumer J. Amiodarone: intravenous loading for rapid suppression of complex ventricular arrhythmias. J Am Coli Cardiol 1984;4: Hoogenhuyze DV, Burg PVD, de Wilde A, Reeme WJ, Krauss XH. Acute effects of intravenous amiodarone in patients with complex ventricular dysrhythmias (abstr). Am J Cardiol 1982;49: Holt P, Curry P, Way B, Holt D. Intravenous amiodarone: an effective antiarrhythmic agent (abstr). Am J Cardiol 1982;49: Morady F, Scheinman MM, Shen E, Shapiro W, Sung R, DiCarlo L. Intravenous amiodarone in the acute treatment of recurrent symptomatic ventricular tachycardia. Am J Cardiol 1983;51: Hariman RJ, Gomes JAC, Kang PS, EI-Sherif N. Effects of intravenous amiodarone in patients with inducible repetitive ventricular responses and ventricular tachycardia. Am Heart J 1984; I 07: Saksena S, Rothbart ST, Shah Y, Cappello G. Clinical efficacy and electropharmacology of continuous intravenous amiodarone infusion and chronic oral amiodarone in refractory ventricular tachycardia. Am J Cardiol 1984;54: Nademanee K, Feld G, Hendrickson J, Intarachot V, Kannan R, Singh B. Does intravenous amiodarone shorten the latency of the onset of
7 JACC Vol. 6, No. July 1985: MORADY ET AL. 185 antiarrhythmic action of oral amiodarone in ventricular dysrhythmias? (abstr). J Am Coli Cardiol 1983;1: Wellens HJJ, Brugada P, Abdollah H, Dassen WR. A comparison of the electrophysiologic effects of intravenous and oral amiodarone in the same patient. Circulation 1984;69: Nademanee K, Singh BN, Phil D, et at. Pharmacokinetic significance of serum reverse T 3 levels during amiodarone treatment: a potential method for monitoring chronic drug therapy. Circulation 1982; 66: Singh BN, Nademanee K. Amiodarone and thyroid function: clinical implications during antiarrhythmic therapy. Am Heart J 1983;106: Singh BN. Amiodarone: historical development and pharmacologic profile. Am Heart J 1983;106:
The Effect of Rate on Prolongation of Ventricular Refractoriness by Quinidine in Humans
 The Effect of Rate on Prolongation of Ventricular Refractoriness by Quinidine in Humans SHIMON ROSENHECK, JOAO SOUSA, HUGH CALKINS, ALAN H. KADISH, and FRED MORADY From the Division of Cardiology, Department
The Effect of Rate on Prolongation of Ventricular Refractoriness by Quinidine in Humans SHIMON ROSENHECK, JOAO SOUSA, HUGH CALKINS, ALAN H. KADISH, and FRED MORADY From the Division of Cardiology, Department
Effects of intravenous amiodarone on ventricular refractoriness, intraventricular conduction, and ventricular tachycardia induction
 Europace (2000) 2, 207 215 doi:10.1053/eupc.2000.0099, available online at http://www.idealibrary.com on Effects of intravenous amiodarone on ventricular refractoriness, intraventricular conduction, and
Europace (2000) 2, 207 215 doi:10.1053/eupc.2000.0099, available online at http://www.idealibrary.com on Effects of intravenous amiodarone on ventricular refractoriness, intraventricular conduction, and
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Acute and Chronic Effects of Amiodarone on Ventricular Refractoriness, Intraventricular Conduction and Ventricular Tachycardia Induction
 148 JACC Vol 7. No I January 1986148-57 Acute and Chronic Effects of Amiodarone on Ventricular Refractoriness, Intraventricular Conduction and Ventricular Tachycardia Induction FRED MORADY, MD, FACC, LORENZO
148 JACC Vol 7. No I January 1986148-57 Acute and Chronic Effects of Amiodarone on Ventricular Refractoriness, Intraventricular Conduction and Ventricular Tachycardia Induction FRED MORADY, MD, FACC, LORENZO
Predicting Ventricular Tachycardia Cycle Length After Procainamide by Assessing Cycle Length-Dependent Changes in Paced QRS Duration
 39 Predicting Ventricular Tachycardia Cycle Length After Procainamide by Assessing Cycle Length-Dependent Changes in Paced QRS Duration Francis E. Marchlinski, MD, Alfred E. Buxton, MD, Mark E. Josephson,
39 Predicting Ventricular Tachycardia Cycle Length After Procainamide by Assessing Cycle Length-Dependent Changes in Paced QRS Duration Francis E. Marchlinski, MD, Alfred E. Buxton, MD, Mark E. Josephson,
Reversion of ventricular tachycardia by pacemaker stimulation
 British Heart Journal, 1971, 33, 922-927. Reversion of ventricular tachycardia by pacemaker stimulation M. A. Bennett and B. L. Pentecost From the General Hospital, Birmingham 4 Reversion of ventricular
British Heart Journal, 1971, 33, 922-927. Reversion of ventricular tachycardia by pacemaker stimulation M. A. Bennett and B. L. Pentecost From the General Hospital, Birmingham 4 Reversion of ventricular
Ventricular ectopic activity after premature atrial beats
 British Heart Journal, 1977, 39, 1033-1037 Ventricular ectopic activity after premature atrial beats in acute myocardial infarction1 R. J. MYERBURG, R. J. SUNG, G. GERSTENBLITH, STEPHEN M. MALLON, AND
British Heart Journal, 1977, 39, 1033-1037 Ventricular ectopic activity after premature atrial beats in acute myocardial infarction1 R. J. MYERBURG, R. J. SUNG, G. GERSTENBLITH, STEPHEN M. MALLON, AND
Results of Catheter Ablation of Ventricular Tachycardia Using Direct Current Shocks
 Results of Catheter Ablation of Ventricular Tachycardia Using Direct Current Shocks FRED MORADY, MELVIN M. SCHEINMAN, JERRY C. GRIFFIN, JOHN M. HERRE, and WILLIAM H. KOU From the Divisions of Cardiology,
Results of Catheter Ablation of Ventricular Tachycardia Using Direct Current Shocks FRED MORADY, MELVIN M. SCHEINMAN, JERRY C. GRIFFIN, JOHN M. HERRE, and WILLIAM H. KOU From the Divisions of Cardiology,
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular Nodal Reentrant Tachycardia
 645 Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular dal Reentrant Tachycardia S. ADAM STRICKBERGER, M.D., EMILE DAOUD, M.D., MARK
645 Effects of Partial and Complete Ablation of the Slow Pathway on Fast Pathway Properties in Patients with Atrioventricular dal Reentrant Tachycardia S. ADAM STRICKBERGER, M.D., EMILE DAOUD, M.D., MARK
COMPLEX CASE STUDY INNOVATIVE COLLECTIONS. Case presentation
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways
 Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Atrioventricular (AV) Nodal Reentry Associated with 2:1 Infra-His Conduction Block during Tachycardia in a Patient with AV Nodal Triple Pathways Haruhiko ABE, M.D., Takashi OHKITA, M.D., Masasuke FUJITA,
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
CLINICAL INVESTIGATIONS. Methods
 CLINICAL INVESTIGATIONS Jpn Circ J 2001; 65: 702 706 Correlation Between the Effective Refractory Period and Activation-Recovery Interval Calculated From the Intracardiac Unipolar Electrogram of Humans
CLINICAL INVESTIGATIONS Jpn Circ J 2001; 65: 702 706 Correlation Between the Effective Refractory Period and Activation-Recovery Interval Calculated From the Intracardiac Unipolar Electrogram of Humans
Paroxysmal Nonreentrant Supraventricular Tachycardia Due to Simultaneous Fast and Slow Pathway Conduction in Dual Atrioventricular Node Pathways
 456 lacc Vol. 10, No.2 DIAGNOSTIC STUDIES Paroxysmal Nonreentrant Supraventricular Tachycardia Due to Simultaneous Fast and Slow Pathway Conduction in Dual Atrioventricular Node Pathways SUNG SOON KIM,
456 lacc Vol. 10, No.2 DIAGNOSTIC STUDIES Paroxysmal Nonreentrant Supraventricular Tachycardia Due to Simultaneous Fast and Slow Pathway Conduction in Dual Atrioventricular Node Pathways SUNG SOON KIM,
Transcoronary Chemical Ablation of Atrioventricular Conduction
 757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract
 191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Erdem DiRER,1 MD, Murat OZDEMIR, MD, U. Kemal TEZCAN, MD, Sinan AYDOGDU, MD, Sule KORKMAZ, MD, Yalcim SOZUTEK, MD, and Emine KUTUK, MD
 Can Isolated, Symptomatic, Frequent Ventricular Premature Depolarizations be a Predictor of an Inducible Ventricular Tachycardia? Treatment by Radiofrequency Catheter Ablation Erdem DiRER,1 MD, Murat OZDEMIR,
Can Isolated, Symptomatic, Frequent Ventricular Premature Depolarizations be a Predictor of an Inducible Ventricular Tachycardia? Treatment by Radiofrequency Catheter Ablation Erdem DiRER,1 MD, Murat OZDEMIR,
Nature of the Gap Phenomenon in Man
 Nature of the Gap Phenomenon in Man By Delon Wu, Pablo Denes, Ramesh Dhingra, and Kenneth M. Rosen BSTRCT The atrioventricular (V) gap phenomenon occurs when the effective refractory period of a distal
Nature of the Gap Phenomenon in Man By Delon Wu, Pablo Denes, Ramesh Dhingra, and Kenneth M. Rosen BSTRCT The atrioventricular (V) gap phenomenon occurs when the effective refractory period of a distal
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
were inserted into the right femoral vein and positioned system and intracardiac recordings were displayed
 CASE REPORTS Termination of Ventricular Tachycardia by Carotid Sinus Massage DAVID S. HESS, M.D., TIMOTHY HANLON, M.D., MELVIN SCHEINMAN, M.D., ROGER BUDGE, M.D., AND JAWAHAR DESAI, M.D. SUMMARY Intracardiac
CASE REPORTS Termination of Ventricular Tachycardia by Carotid Sinus Massage DAVID S. HESS, M.D., TIMOTHY HANLON, M.D., MELVIN SCHEINMAN, M.D., ROGER BUDGE, M.D., AND JAWAHAR DESAI, M.D. SUMMARY Intracardiac
VENTRICULAR TACHYCARDIA WITH HEMODYNAMIC INSTABILITY REFRACTORY TO CARDIOVERSION: A CASE REPORT
 VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
VENTRCULAR TACHYCARDA WTH HEMODYNAMC NSTABLTY REFRACTORY TO CARDOVERSON: A CASE REPORT Chun-Jen Chou, 1 Chee-Siong Lee, 2,3 and Wen-Ter Lai 2,3 1 Department of Emergency Medicine, Kaohsiung Municipal Hsiao-Kang
Bernard Belhassen, MD; Roman Fish, MD; Sami Viskin, MD; Aharon Glick, MD; Michael Glikson, MD; Michael Eldar, MD
 www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
Journal of the American College of Cardiology Vol. 33, No. 3, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 3, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00614-7 A Technique
Journal of the American College of Cardiology Vol. 33, No. 3, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00614-7 A Technique
Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm
 Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm AMAN CHUGH, MEHMET OZAYDIN, CHRISTOPH SCHARF, STEVE W.K. LAI, BURR HALL, PETER CHEUNG, FRANK PELOSI, JR, BRADLEY
Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm AMAN CHUGH, MEHMET OZAYDIN, CHRISTOPH SCHARF, STEVE W.K. LAI, BURR HALL, PETER CHEUNG, FRANK PELOSI, JR, BRADLEY
Premature Ventricular Depolarization
 Premature Ventricular Depolarization By CESAR A. CACERES, M.D. A DIFFERENCE has been observed in certain instances between the onset of QRS in intracavitary and surface limb leads. Simultaneous tracings
Premature Ventricular Depolarization By CESAR A. CACERES, M.D. A DIFFERENCE has been observed in certain instances between the onset of QRS in intracavitary and surface limb leads. Simultaneous tracings
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Introduction. Circulation
 Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Introduction Circulation 1- Systemic (general) circulation 2- Pulmonary circulation carries oxygenated blood to all parts of the body carries deoxygenated blood to the lungs From Lt. ventricle aorta From
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Arrival of excitation at right ventricular apical endocardium in Wolff-Parkinson-White syndrome type A, with and without right bundle-branch block'
 British Heart Journal, 973, 35, 594-600. Arrival of excitation at right ventricular apical endocardium in Wolff-Parkinson-White syndrome type A, with and without right bundle-branch block' Cesar A. Castillo,
British Heart Journal, 973, 35, 594-600. Arrival of excitation at right ventricular apical endocardium in Wolff-Parkinson-White syndrome type A, with and without right bundle-branch block' Cesar A. Castillo,
Lecture outline. Electrical properties of the heart. Automaticity. Excitability. Refractoriness. The ABCs of ECGs Back to Basics Part I
 Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
Lecture outline The ABCs of ECGs Back to Basics Part I Meg Sleeper VMD, DACVIM (cardiology) University of Florida Veterinary School Electrical properties of the heart Action potentials Normal intracardiac
ECG. Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13
 ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
Prolongation of conduction time during premature stimulation in the human atrium is primarily caused by local stimulus response latency
 European Heart Journal (1995) 16, 1920-1924 Prolongation of conduction time during premature stimulation in the human atrium is primarily caused by local stimulus response latency B. S. KOLLER, P. E. KARASIK,
European Heart Journal (1995) 16, 1920-1924 Prolongation of conduction time during premature stimulation in the human atrium is primarily caused by local stimulus response latency B. S. KOLLER, P. E. KARASIK,
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Bundle of His Recordings in Congenital Complete Heart Block
 Bundle of His Recordings in Congenital Complete Heart Block By DAVID T. KELLY, M.B., SIDNEY J. BRODSKY, M.D., M. MIROWSKI, M.D., L. JEROME KROVETZ, M.D., PH.D., AND RIcHARD D. RowE, M.D. SUMMARY Six children,
Bundle of His Recordings in Congenital Complete Heart Block By DAVID T. KELLY, M.B., SIDNEY J. BRODSKY, M.D., M. MIROWSKI, M.D., L. JEROME KROVETZ, M.D., PH.D., AND RIcHARD D. RowE, M.D. SUMMARY Six children,
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Differentiating Junctional Tachycardia and Atrioventricular Node Re-Entry Tachycardia Based on Response to Atrial Extrastimulus Pacing
 Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
The Electrocardiogram
 The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
The Electrocardiogram Chapters 11 and 13 AUTUMN WEDAN AND NATASHA MCDOUGAL The Normal Electrocardiogram P-wave Generated when the atria depolarizes QRS-Complex Ventricles depolarizing before a contraction
Journal of the American College of Cardiology Vol. 36, No. 2, by the American College of Cardiology ISSN /00/$20.
 Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
Journal of the American College of Cardiology Vol. 36, No. 2, 2000 2000 by the American College of Cardiology ISSN 0735-1097/00/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)00770-1 Diagnostic
Are there low risk patients in Brugada syndrome?
 Are there low risk patients in Brugada syndrome? Pedro Brugada MD, PhD Andrea Sarkozy MD Risk stratification in Brugada syndrome In the last years risk stratification in Brugada syndrome has become the
Are there low risk patients in Brugada syndrome? Pedro Brugada MD, PhD Andrea Sarkozy MD Risk stratification in Brugada syndrome In the last years risk stratification in Brugada syndrome has become the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Mechanism of Ventricular Tachycardia Termination by Pacing at Left Ventricular Sites in Patients with Coronary Artery Disease
 Journal of Interventional Cardiac Electrophysiology 6, 35 41, 2002 C 2002 Kluwer Academic Publishers. Manufactured in The Netherlands. Mechanism of Ventricular Tachycardia Termination by Pacing at Left
Journal of Interventional Cardiac Electrophysiology 6, 35 41, 2002 C 2002 Kluwer Academic Publishers. Manufactured in The Netherlands. Mechanism of Ventricular Tachycardia Termination by Pacing at Left
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties
 www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 «Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
and fibrillation in pre-excitation (Wolff-Parkinson-
 British Heart Journal, 973, 35, 8ii-8i6. Factors regulating ventricular rates during atrial flutter and fibrillation in pre-excitation (Wolff-Parkinson- White) syndrome Agustin Castellanos, Jr., Robert
British Heart Journal, 973, 35, 8ii-8i6. Factors regulating ventricular rates during atrial flutter and fibrillation in pre-excitation (Wolff-Parkinson- White) syndrome Agustin Castellanos, Jr., Robert
Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia
 www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
www.ipej.org 149 Case Report Coexistence of Atrioventricular Nodal Reentrant Tachycardia and Idiopathic Left Ventricular Outflow-Tract Tachycardia Majid Haghjoo, M.D, Arash Arya, M.D, Mohammadreza Dehghani,
Cardiac Arrhythmias Simulated by Concealed Bundle of His Extrasystoles in the Dog
 Cardiac Arrhythmias Simulated by Concealed Bundle of His Extrasystoles in the Dog By Anthony N. Da ma to, Sun H. Lau, and Gustavus Bobb ABSTRACT In 0 open-chest intact dog hearts, multiple close bipolar
Cardiac Arrhythmias Simulated by Concealed Bundle of His Extrasystoles in the Dog By Anthony N. Da ma to, Sun H. Lau, and Gustavus Bobb ABSTRACT In 0 open-chest intact dog hearts, multiple close bipolar
A Case of Alternating Bundle Branch Block in Combination With Intra-Hisian Block
 A Case of Alternating Bundle Branch Block in Combination With IntraHisian Block Yukie OGURA, 1 MD, Junichi KATO, 1 MD, Yuji OGAWA, 1 MD, Takahiro SHIOKOSHI, 1 MD, Toru KITAOKA, 1 MD, Takahide SUZUKI, 1
A Case of Alternating Bundle Branch Block in Combination With IntraHisian Block Yukie OGURA, 1 MD, Junichi KATO, 1 MD, Yuji OGAWA, 1 MD, Takahiro SHIOKOSHI, 1 MD, Toru KITAOKA, 1 MD, Takahide SUZUKI, 1
Effect of an increase in coronary perfusion on transmural. ventricular repolarization
 Effect of an increase in coronary perfusion on transmural ventricular repolarization Yan-Zhou Zhang 1, MD, PhD, Ben He 1, MD, Le-Xin Wang 2, MD, PhD. From: 1 Department of Cardiology, Renji Hospital, Medical
Effect of an increase in coronary perfusion on transmural ventricular repolarization Yan-Zhou Zhang 1, MD, PhD, Ben He 1, MD, Le-Xin Wang 2, MD, PhD. From: 1 Department of Cardiology, Renji Hospital, Medical
V. TACHYCARDIAS Rapid rhythm abnormalities
 V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
V. TACHYCARDIAS Rapid rhythm abnormalities Tachyarrhythmias currently account for up to 350,000 deaths annually in the US. In addition to these clearly dangerous rhythm disturbances, other forms of more
Cardiac Dysrhythmias and Sports
 Sudden unexpected death during athletic participation is the overriding consideration in advising individuals with dysrhythmias about participation in sports. The incidence of sudden death is 1 to 2 per
Sudden unexpected death during athletic participation is the overriding consideration in advising individuals with dysrhythmias about participation in sports. The incidence of sudden death is 1 to 2 per
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
at least 4 8 hours per week
 ECG IN ATHLETS An athlete is defined as an individual who engages in regular exercise or training for sport or general fitness, typically with a premium on performance, and often engaged in individual
ECG IN ATHLETS An athlete is defined as an individual who engages in regular exercise or training for sport or general fitness, typically with a premium on performance, and often engaged in individual
Chapter 14. Agents used in Cardiac Arrhythmias
 Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction
 Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction The Use of Competitive Atrial Pacing By ROBERT M. EASLEY, JR., M.D., AND SIDNEY GOLDSTEIN, M.D. SUMMARY A
Differentiation of Ventricular Tachycardia from Junctional Tachycardia with Aberrant Conduction The Use of Competitive Atrial Pacing By ROBERT M. EASLEY, JR., M.D., AND SIDNEY GOLDSTEIN, M.D. SUMMARY A
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 13.01.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Medicine. Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract
 Medicine CLINICAL CASE REPORT Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract A Case Report Li Yue-Chun, MD, Lin Jia-Feng,
Medicine CLINICAL CASE REPORT Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract A Case Report Li Yue-Chun, MD, Lin Jia-Feng,
CATHETER ABLATION FOR TACHYCARDIAS
 190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
Ventriculoatrial Block During a Narrow-QRS Tachycardia: What Is the Tachycardia Mechanism? IV
 174 ARRHYTHMIA OF THE MONTH Section Editor: Fred Morady, M.D. Ventriculoatrial Block During a Narrow-QRS Tachycardia: What Is the Tachycardia Mechanism? IV FRED MORADY, M.D. From the Cardiology Division,
174 ARRHYTHMIA OF THE MONTH Section Editor: Fred Morady, M.D. Ventriculoatrial Block During a Narrow-QRS Tachycardia: What Is the Tachycardia Mechanism? IV FRED MORADY, M.D. From the Cardiology Division,
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ. ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C
 ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
Characteristics of Rapid Rhythms Recorded Within Pulmonary Veins During Atrial Fibrillation
 Characteristics of Rapid Rhythms Recorded Within Pulmonary Veins During Atrial Fibrillation HIROSHI TADA, MEHMET ÖZAYDIN, HAKAN ORAL, BRADLEY P. KNIGHT, AMAN CHUGH, CHRISTOPH SCHARF, FRANK PELOSI, Jr.,
Characteristics of Rapid Rhythms Recorded Within Pulmonary Veins During Atrial Fibrillation HIROSHI TADA, MEHMET ÖZAYDIN, HAKAN ORAL, BRADLEY P. KNIGHT, AMAN CHUGH, CHRISTOPH SCHARF, FRANK PELOSI, Jr.,
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation
 Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
Where are the normal pacemaker and the backup pacemakers of the heart located?
 CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
CASE 9 A 68-year-old woman presents to the emergency center with shortness of breath, light-headedness, and chest pain described as being like an elephant sitting on her chest. She is diagnosed with a
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
ELECTROCARDIOGRAPHY (ECG)
 ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
Electrophysiology and Cathether Ablation: Historical Evolution. Saverio Iacopino, MD, FACC, FESC
 Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
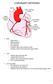 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B. Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D.
 Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Wolff-Parkinson-White Syndrome with Gradual Transition from Type A to Type B Yoshikazu SUZUKI, M.D., Hajime TERADA, M.D., and Noboru YAMAZAKI, M.D. SUMMARY This report documents a case which showed type
Electrocardiogram and Heart Sounds
 Electrocardiogram and Heart Sounds Five physiologic properties of cardiac muscle Automaticity: SA node is the primary pacemaker of the heart, but any cells in the conduction system can initiate their
Electrocardiogram and Heart Sounds Five physiologic properties of cardiac muscle Automaticity: SA node is the primary pacemaker of the heart, but any cells in the conduction system can initiate their
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring
 Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring Yu-Zhen ZHANG, M.D.,* Shi-Wen WANG, M.D.,* Da-Yi Hu, M.D.,**
Prediction of Life-Threatening Arrhythmia in Patients after Myocardial Infarction by Late Potentials, Ejection Fraction and Holter Monitoring Yu-Zhen ZHANG, M.D.,* Shi-Wen WANG, M.D.,* Da-Yi Hu, M.D.,**
480 April 2004 PACE, Vol. 27
 Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence
 www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
Premature Atrial Contractions Managed With Slow Pathway Ablation
 Maced J Med Sci electronic publication ahead of print, published on November 25, 2008 as doi:10.3889/mjms.1857-5773.2008.0018 Trajkov et al. Slow Pathway Ablation Macedonian Journal of Medical Sciences.
Maced J Med Sci electronic publication ahead of print, published on November 25, 2008 as doi:10.3889/mjms.1857-5773.2008.0018 Trajkov et al. Slow Pathway Ablation Macedonian Journal of Medical Sciences.
Lancaster Avenue, Philadelphia, Pennsylvania. to every frequency distribution has never been. as bimodal if there were two or more distinct cycle
 Postgraduate Medical Journal (February 1978) 54, 86-91. Differentiation of irregular rhythms by frequency distribution analysis S. TALBOT M.B., M.R.C.P. L. S. DREIFUS* M.D. Department of Cardiology, Hammersmith
Postgraduate Medical Journal (February 1978) 54, 86-91. Differentiation of irregular rhythms by frequency distribution analysis S. TALBOT M.B., M.R.C.P. L. S. DREIFUS* M.D. Department of Cardiology, Hammersmith
Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες. Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο
 Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο Όλες οι κοιλιακές αρρσθμίες δεν είναι ίδιες Υπάρτοσν διαθορές ζηον πληθυσμό, ηον μηχανισμό
Φαρμακεσηική αγωγή ζηις ιδιοπαθείς κοιλιακές αρρσθμίες Άννα Κωζηοπούλοσ Επιμελήηρια Α Ωνάζειο Καρδιοτειροσργικό Κένηρο Όλες οι κοιλιακές αρρσθμίες δεν είναι ίδιες Υπάρτοσν διαθορές ζηον πληθυσμό, ηον μηχανισμό
Declaration of conflict of interest NONE
 Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Monophasic action potentials of right atrium and electrophysiological properties of AV conducting
 British Heart journal, 1976, 38, 1350-1354. Monophasic action potentials of right atrium and electrophysiological properties of AV conducting system in patients with hypothyroidism S. Gavrilescu, C. Luca,
British Heart journal, 1976, 38, 1350-1354. Monophasic action potentials of right atrium and electrophysiological properties of AV conducting system in patients with hypothyroidism S. Gavrilescu, C. Luca,
December 2018 Tracings
 Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
'Dual atrioventricular nodal pathways' in patients with Wolff-Parkinson-White syndrome*
 Br Heart 7 1980; 43: 7-13 'Dual atrioventricular nodal pathways' in patients with Wolff-Parkinson-White syndrome* EDWARD L C PRITCHETT, ERIC N PRYSTOWSKY, DAVID G BENDITT, JOHN J GALLAGHER From the Division
Br Heart 7 1980; 43: 7-13 'Dual atrioventricular nodal pathways' in patients with Wolff-Parkinson-White syndrome* EDWARD L C PRITCHETT, ERIC N PRYSTOWSKY, DAVID G BENDITT, JOHN J GALLAGHER From the Division
Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation
 J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
CARDIAC PHYSIOLOGY. Amelyn U. Ramos-Rafael,M.D. Functional Anatomy of the Heart
 CARDIAC PHYSIOLOGY Amelyn U. Ramos-Rafael,M.D. Functional Anatomy of the Heart 1 Functional Anatomy of The Heart The Atria relatively thin walled The Ventricles ventricular walls thicker than atrial walls
CARDIAC PHYSIOLOGY Amelyn U. Ramos-Rafael,M.D. Functional Anatomy of the Heart 1 Functional Anatomy of The Heart The Atria relatively thin walled The Ventricles ventricular walls thicker than atrial walls
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
complicating myocardial infarction
 British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
British Heart Journal, I970, 32, 21. Bretylium tosylate in treatment of refractory ventricular arrhythmias complicating myocardial infarction G. Terry,1 C. W. Vellani, M. R. Higgins, and A. Doig From the
