Prognosis of Aortic Intramural Hematoma With and Without Penetrating Atherosclerotic Ulcer. A Clinical and Radiological Analysis
|
|
|
- Lawrence Pierce
- 5 years ago
- Views:
Transcription
1 rognosis of Aortic Intramural Hematoma With and Without enetrating Atherosclerotic Ulcer A Clinical and Radiological Analysis Fumikiyo Ganaha, MD; D. Craig Miller, MD; Koji Sugimoto, MD; Young Soo Do, MD; Hiroki Minamiguchi, MD; Haruo Saito, MD; R. Scott Mitchell, MD; Michael D. Dake, MD Background Advances in imaging techniques have increased the recognition of aortic intramural hematomas (IMHs) and penetrating atherosclerotic ulcers (AUs); however, distinction between IMH and AU remains unclear. We intended to clarify differences between IMH coexisting with AU and IMH not associated with AU by comparisons of clinical features, imaging findings, and patient outcome to derive the optimal therapeutic approach. Methods and Results We performed a retrospective analysis of 65 symptomatic patients with aortic IMH. There were 34 patients with IMH associated with AU (group 1) and 31 patients with IMH unaccompanied by AU (group 2). Involvement of the ascending aorta (type A) was more frequent in group 2 (8 of 31, 26%), whereas most of the patients in group 1 had exclusive involvement of the descending aorta (type B) (31of 34, 91%). atients were subdivided into 2 categories, those with clinical progression and those with stable disease. Forty-eight percent of patients in group 1 and 8% in group 2 were in the progressive category ( 0.002). Clinical and radiological findings were compared between those group 1 patients who had a progressive disease course (n 12) and those who were stable (n 13). Sustained or recurrent pain ( ), increasing pleural effusion ( ), and both the maximum diameter ( 0.004) and maximum depth ( 0.003) of the AU were reliable predictors of disease progression. Conclusions This study suggests a difference in disease behavior that argues for the prognostic importance of making a clear distinction between IMH caused by AU and IMH not associated with AU. IMH with AU was significantly associated with a progressive disease course, whereas IMH without AU typically had a stable course, especially when limited to the descending thoracic aorta. (Circulation. 2002;106: ) Key Words: aorta prognosis imaging atherosclerosis Over the past decade, advances in vascular imaging technology have led to increasing recognition of aortic intramural hematomas (IMHs) in patients with acute aortic syndromes. Considered by many to be a variant of aortic dissection, the pathogenesis of IMH still remains unclear. Two different pathophysiological processes can lead to intramural hematoma formation. One is IMH without intimal disruption; in this entity, it is believed that spontaneous rupture of aortic vasa vasorum is responsible for hematoma formation within the aortic wall. 1 The other type of IMH is associated with an atherosclerotic ulcer that penetrates into the internal elastic lamina and allows hematoma formation within the media of the aortic wall. 2 4 See p 284 In previous reports, these 2 types of IMH are rarely distinguished in discussing prognoses and optimal treatment methods. 3,5,6 The concept of the Stanford classification scheme for aortic dissection has been applied to IMH because the prognostic impact of the location of IMH and its standard treatment have been considered similar to those for classic aortic dissection. 5 It is generally accepted that patients with type B (exclusive involvement of the descending aorta) IMH can be managed conservatively in the absence of disease progression, whereas early surgical interventions are recommended for type A (involvement of the ascending aorta) IMH. 5,6 On the other hand, Coady et al 7 recently reported that the prognoses of acutely symptomatic hospitalized patients with penetrating atherosclerotic ulcers (AUs) was worse than those with classic aortic dissection due to a higher incidence of aortic rupture. We reviewed 65 symptomatic patients with aortic IMH. Thirty-four patients had a AU that was considered to be the cause of IMH, whereas 31 had no evidence of a AU. The objective of this study was to clarify the differences between IMH associated with AU and IMH without AU in terms of Received February 6, 2002; revision received May 1, 2002; accepted May 1, From the Division of Cardiovascular and Interventional Radiology (F.G., K.S., Y.S.D., H.M., H.S., M.D.D.), and the Department of Cardiovascular and Thoracic Surgery (D.C.M., R.S.M.), Stanford University School of Medicine, Stanford, Calif. Correspondence to Michael D. Dake, MD, Division of Cardiovascular and Interventional Radiology, Room H-3647, Stanford University Medical Center, Stanford, CA mddake@stanford.edu 2002 American Heart Association, Inc. Circulation is available at DOI: /01.CIR A 342
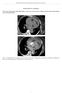
2 Ganaha et al Aortic Intramural Hematoma 343 T 1 -weighted MRI, 5,9 and displacement of intimal calcifications for transesophageal echocardiography. 4 The Stanford classification of aortic dissection was used to categorize IMH according to the location of disease. Type A indicates involvement of the ascending aorta, and type B indicates exclusive involvement of the descending aorta. 5 In addition, the aorta was subdivided into 7 segments for a detailed evaluation of the longitudinal extent of IMH and the location of any AU. These 7 segments were the ascending aorta, transverse arch, and proximal descending, mid-descending, distal descending, suprarenal abdominal, and infrarenal aorta. Top panels, Images from a group 1 patient with an IMH and no associated AU. Bottom panels, Images from a group 2 IMH patient with an accompanying AU. A, Crescentic high attenuation in the ascending and descending aortic wall (arrowheads) on noncontrast CT indicates acute IMH formation. B, A postcontrast image shows no opacification of the thickened aortic wall. The arrow indicates internal deviation of the intimal calcification. C, Contrast CT shows AU and associated IMH (arrowheads) in aortic arch. D, 2 small ulcers (arrows) apart from the AU represent intimal atheromatous ulcers and irregularity. clinical features and prognosis to establish the optimal therapeutic approach for each. Methods We treated 725 symptomatic patients with a working diagnosis of aortic dissection at Stanford University Medical Center between January 1990 and June Of those 725 patients, 663 (91%) had a classic double-barreled dissection and 66 (9%) had an aortic IMH. Diagnosis was confirmed from surgical, radiological, and/or autopsy records. One patient s hospital records were incomplete, leaving 65 cases of aortic IMH for analysis. The diagnosis of IMH was confirmed by review of the imaging studies, including CT, MRI, transesophageal echocardiography, and angiography. The images were reviewed by 3 radiologists with specialized cardiovascular training and experience. The presence of a hematoma within the aortic wall, recognizable as a crescentic or circular local aortic wall thickening (Figure, A and B), and the absence of a visible intimal flap or tear were prerequisites for the diagnosis of IMH by any imaging modality. Other modality-specific diagnostic criteria for IMH included displacement of intimal calcifications and higher attenuation of the thickened wall than blood for precontrast CT, no contrast enhancement of the thickened aortic wall for contrast CT, 8 no flow within the locally thickened aortic wall for MRI and angiography, increased signal intensity of thickened aortic wall for IMH With AU Versus IMH Without AU The 65 cases that were able to be evaluated were divided into patients with an IMH caused by a AU (group 1) and those with an IMH without evidence of a AU (group 2). In the review of imaging studies, a AU was defined as a deep ulcerated lesion in the thickest part of the IMH within the involved aorta (Figure, C). In the patients who had prominent atherosclerotic disease, tiny ulcerated lesions of a few millimeters in size were observed occasionally. These lesions often were accompanied by atheromatous plaques and intimal calcification and were typically recognized as an irregularity along the luminal surface of the aortic wall in contrast-enhanced CT images (Figure, D). These tiny ulcers were seen irrespective of the IMH extent and represented intimal atheromatous plaque ulcerations (11 cases in group 1 and 4 cases in group 2). They were easily distinguished from the typical appearance of a deeper AU. To evaluate any difference in the natural history of the disease between the 2 IMH groups, 49 of 65 patients were divided into 2 categories, those with a progressive disease process and those with stable disease. The other 16 patients (9 in group 1 and 7 in group 2) were excluded from this analysis because the observation of these patients was interrupted by an operation. A progressive disease course was defined as an increase in IMH size (longitudinal or radial) over the interval between imaging studies, evolution of the IMH to double-barreled dissection, or aortic rupture. A stable disease course was defined as an IMH that regressed spontaneously or had no interval change between imaging studies in an otherwise hemodynamically stable patient. The observation period was usually the extent of the index hospitalization; however, when pertinent follow-up information was available, it was included in the analysis. Indicators and redictors of Disease rogression in atients With IMH and AU To identify the predictors of disease progression in patients with IMH associated with AU, clinical and radiological findings were compared between those who had a progressive disease course (n 12) and those with stable disease (n 13). The clinical findings of age, sex, history of hypertension, extent of disease (Stanford classification), and presence of concomitant aortic aneurysm were evaluated. Each patient s pain response to antihypertensive therapy was also analyzed. The imaging characteristics evaluated included the presence of pleural effusion at time of hospital admission and any interval radiological changes, including number, location, maximum diameter, and maximum depth of AU, maximum diameter and maximum wall thickness of the aorta involved with IMH, and extent of IMH defined by aortic segments involved. In patients with multiple AUs (n 7), the maximum diameter, depth, and location of the largest AU were assessed. Statistical Analysis Data are expressed as mean SD or as proportions. Comparisons between patients in group 1 and 2 and patients with progressive versus stable disease course were made with the 2 test for categorical variables and unpaired Student s t test for continuous variables. A probability value 0.05 was considered statistically significant.
3 344 Circulation July 16, 2002 TABLE 1. Characteristics of Group 1 and 2 atients Group 1 (n 34) Group 2 (n 31) Demographics Age, mean SD Male/female 15/19 19/ Stanford type A/B, n (%) 3 (8.8)/31 (91.2) 8 (25.8)/23 (74.2) 0.07 Acute/chronic 30 (88.2)/4 (11.8) 30 (96.8)/1 (3.2) 0.20 Backgrounds Hypertension, n (%) 26/31 (83.9) 25/29 (86.2) 0.80 Concomitant aortic disease, n (%) TAA 6 (17.6) 4 (12.9) 0.76 AAA 3 (8.8) 13 (38.2) 5 (16.1) 13 (41.9) TAA AAA 4 (11.8) 4 (12.9) Symptoms Associated pain, n (%) 34 (100) 29 (93.5) 0.13 Others, symptom (n) hemoptysis (1) paraplegia (1) TAA indicates thoracic aortic aneurysm; AAA, abdominal aortic aneurysm. Results Overall atient Characteristics The study population consisted of 34 men and 31 women with a mean age of years. Of the 65 patients, 60 (92%) had an acute IMH (admitted within 2 weeks of the onset of symptoms), and 5 (8%) had a chronic IMH (admitted 2 weeks after the onset of symptoms). Forty-six (71%) of the patients were transferred from other hospitals with a diagnosis of aortic IMH or suspected aortic dissection. No patient had a previous history of major trauma or the Marfan syndrome. IMH With AU Versus IMH Without AU atient Characteristics The clinical features of the patients in groups 1 and 2 are summarized in Table 1. Although not statistically significant ( 0.08), the patients in group 1 were slightly older. Involvement of the ascending aorta (type A) was more frequent in group 2, whereas most of the patients in group 1 had type B morphology ( 0.07). In terms of clinical history, there was no significant difference between the groups. Morphological Features of IMH The morphological features of IMH in group 1 and 2 patients are detailed in Table 2. Type A IMH was more frequent in group 2. There was no difference in the longitudinal extent of the IMH as represented by the numbers of involved aortic segments ( 0.88). Treatment and rognosis The treatment and clinical course of the patients in group 1 and 2 are summarized in Table 3. Type A IMH in Group 1 Three patients underwent graft replacement of the ascending aorta within 4 days of the onset of symptoms, with 2 survivors. Type A IMH in Group 2 Five patients underwent surgery within 4 days of their first symptoms. Four were successfully treated by ascending aortic graft replacement, and 1 patient died from septic complication 11 days after surgery. TABLE 2. Morphological Features of IMH in Group 1 and 2 atients Group 1 (n 34) Group 2 (n 31) Maximum diameter of aorta, mm mm mm 0.29 Maximum thickness of aortic mm mm 0.07 wall, mm Location of IMH Asc-SRA (1) Asc-SRA (1) Asc-D (1) Asc-DD (1) Asc-Arch (1) Asc-MD (1) Arch-SRA (5) Asc-D (2) Arch-DD (5) Asc-Arch (2) Arch-MD (1) Asc (1) Arch-D (1) Arch-IRA (1) D-SRA (8) Arch-SRA (4) D-DD (5) Arch-DD (2) D-MD (2) D-IRA (1) MD-SRA (1) D-SRA (3) MD-DD (2) D-DD (8) MD (1) D-MD (1) D (1) MD-DD (2) Segment numbers of IMH involvement Values are mean SD or n. Asc indicates ascending aorta; D, proximal descending thoracic aorta; MD, middle descending thoracic aorta; DD, distal descending thoracic aorta; SRA, suprarenal abdominal aorta; and IRA, infrarenal abdominal aorta.
4 Ganaha et al Aortic Intramural Hematoma 345 TABLE 3. Treatment and rognosis of Group 1 and 2 atients Type A (n 3) Group 1 Group 2 Type B (n 31) Type A (n 8) Type B (n 23) Conservative treatment (n 40) Alive Death from disease progression 3 (3*) 1 (1*) Death from other cause Open surgery (n 19) Alive 2 8 (3*) 4 1 Death from disease progression Death from other cause Endovascular stent-graft placement (n 6) Alive 5 (1*) Death from disease progression 0 Death from other cause 1 Hospital mortality Death from disease progression 1 3 (3*) 1 (1*) Death from other cause *atients who developed aortic rupture. Type B IMH in Group 1 Of the 31 patients with type B IMH in group 1, 17 (55%) were treated medically. In this subset, 3 deaths from progression of disease were observed at a mean of 9.3 days (range: 4 to 17 days) after the onset of symptoms. All 3 patients died from aortic rupture caused by a AU. Eight of 31 patients (26%) underwent graft replacement between 3 and 37 days (mean 9.6 days) after the onset of symptoms. Three had a ruptured AU and 4 others had signs of impending rupture, eg, poorly controlled pain (n 4), increased mediastinal or pleural effusion (n 4), or increased AU size (n 2). Endovascular repair of AU with stent-graft placement was performed in 6 (19%) of the 31 type B patients in group 1, between 1 and 49 days (mean: 17.5days) after symptom onset. Stent-graft deployment was successful in all. One patient underwent emergency stent-graft placement for a ruptured AU in the proximal descending aorta. Five patients showed signs of impending rupture, including persistent pain (n 5), increased pleural effusion (n 4), increased AU size (n 1), and pseudoaneurysm formation (n 3). In all cases, the full extent of the AU and pseudoaneurysm, but not the entire length of the IMH, were covered by the stent-graft. ain and pleural effusion lessened in 5 patients. One patient died from a massive cerebral hemorrhage 3 days after the stent-grafting. Type B IMH in Group 2 In contrast to group 1, 20 (87%) of 23 patients in group 2 were treated by antihypertensive therapy only. Three patients with a coexisting thoracic aortic aneurysm had worsening pain and increasing pleural effusion that were considered harbingers of impending rupture. All 3 underwent surgical repair with 2 postoperative deaths: 1 from aspiration pneumonia and 1 from renal failure. In-Hospital Mortality Overall, the in-hospital mortality rate was 16% in group 1 and 19% in group 2. Disease progression was the cause of death in 4 patients (12%) in group 1 and 1 patient (3%) in group 2 ( 0.20). IMH Disease Course in Groups 1 and 2 The natural history of IMH in both groups is shown in Table 4. An interval increase in IMH was observed in 5 patients with type B IMH in group 1, between 4 and 35 days (mean: 13.8 days) after initial symptom onset. This was related to progression of the AU in all cases. There were no patients in group 2 who had an increase in IMH size. Evolution to a classic double-barreled dissection occurred in 4 patients, including 1 with type A and 2 with type B IMH in group 1, and 1 patient with a type A IMH in group 2. This pathological evolution occurred between 2 and 7 days (mean 4.5) after the onset of symptoms. All 4 patients died: 3 from aortic rupture and 1 from an acute myocardial infarction related to the ascending aortic dissection. Compared with group 2, patients in group 1 with IMH had a more progressive disease course ( 0.002). This was most TABLE 4. Disease Course of IMH in Group 1 and 2 atients Group 1 (n 25) Group 2 (n 24) Stable course No change Regression 2 2 rogressive course 12 2 Aortic rupture 4 1 IMH expansion 5 0 ropagation to double-barreled dissection
5 346 Circulation July 16, 2002 TABLE 5. Comparison of Clinical and Radiological Features Between atients With rogressive and Stable Disease Courses evident in those with a type B IMH (24 in group 1; 21 in group 2), where patients with an associated AU clearly had more clinical progression ( 0.002). Indicators and redictors of Disease rogression in IMH atients With AU A comparison of clinical and radiological findings between AU patients with progressive and stable disease is shown in Table 5. Clinical Factors Uncontrollable pain was a significant indicator of disease progression ( ). Slightly more women than men had a stable disease course ( 0.07). There were no significant differences in age, Stanford disease classification, or presence of hypertension or associated aortic aneurysm between the patients with a progressive disease course and those with a stable process. rogressive Course (n 12) Stable Course (n 13) Clinical findings Age, y Sex, male/female 7/5 3/ Type A/B 1/11 0/ Hypertension, yes/no 10/2 9/ Aortic aneurysm, yes/no 3/9 6/ Uncontrollable pain, yes/no 9/1 1/ Radiological findings leural effusion At initial diagnosis, yes/no 10/2 10/ Interval change (increased/no 9/1/0 0/8/ change/decreased) Initial evaluation of AU Maximum diameter of AU, mm Maximum depth of AU, mm Numbers of AU Location of AU Asc 1 0 Arch 3 1 D 5 2 MD DD 2 6 SRA 0 1 Initial evaluation of aorta Maximum diameter of aorta, mm Maximum thickness of aorta wall, mm IMH involved segment numbers Values are mean SD or n. AU indicates penetrating atherosclerotic ulcer; Asc, ascending aorta; D, proximal descending thoracic aorta; MD, middle descending thoracic aorta; DD, distal descending thoracic aorta; and SRA, suprarenal abdominal aorta. Radiological Factors Although pleural effusion was commonly seen in patients with either a progressive or stable IMH, an interval increase in the pleural effusion was a significant indicator ( ) of progressive disease in those with a AU. In terms of the initial size of the AU, the maximum diameter and maximum depth in patients with progressive disease were mm and mm, respectively. Both values were significantly greater than those measured in patients with stable disease ( and 0.003, respectively). If a threshold of 20 mm is used for maximum AU diameter, the positive and negative predictive values for disease progression are 100% and 71%, respectively. If a value for maximum AU depth is set arbitrarily at 10 mm or greater, the positive and negative predictive values are 80% and 88%, respectively. AUs in patients with progressive disease were usually proximal ( 0.01), with the proximal descending thoracic aorta being the most common site.
6 Ganaha et al Aortic Intramural Hematoma 347 There were no significant differences in maximum aortic diameter and maximum aortic wall thickness over the extent of IMH, or in the number of involved aortic segments between those IMH patients with and without progressive disease ( 0.61, 0.16, and 0.08, respectively). Discussion History and Incidence of IMH Aortic IMH was first described in 1920 by Krukenberg 10 as dissection without intimal tear and was considered a distinct entity at autopsy. In 1988, Yamada et al 9 reported the CT and MRI findings of this condition. They predicted that the frequency of detection of this variant of aortic dissection would increase in the future as CT and MRI became more widely employed. Indeed, aortic IMH has been recognized increasingly more frequently in patients with acute aortic syndromes. In large autopsy series, the incidence of IMH in patients with aortic dissection is reported to range from 4% 11 to 13%. 12 In this series, 66 (9%) of 725 patients had an IMH, a frequency that is consistent with that reported from autopsy series. Comparison Between IMH With AU and IMH Without AU Clinical Features revious reports indicate that both IMHs and AUs commonly affect elderly patients with a history of hypertension. 2,3,6,13 Although the mean age of both groups of IMH patients is older than that for patients with classic dissection, 13 the patients in group 1 were slightly older than those in group 2 (mean age: 71.0 and 66.9 years, respectively). Hypertension and concomitant thoracic and abdominal aortic aneurysm were commonly seen in both groups, with no apparent difference in incidence between groups 1 and 2. There was a significant difference in the Stanford type of IMH between groups 1 and 2. Most of the patients in group 1 had a type B IMH (31of 34, 91%). Type A IMH was slightly more common (8 of 31, 26%) in group 2 than in group 1 ( 0.07). These results are consistent with previous reports 2,14 that showed that a AU is typically located in the descending thoracic aorta. In terms of the frequency of type A IMH without associated AU, Coady et al 13 reported that 5 (29%) of 17 patients had this finding, similar to the prevalence found in this study. Of note, there was no difference in the extent of IMH between groups 1 and 2. Treatment and rognosis In many institutions, the standard therapy over the past decade for patients with type A IMH has been early surgical graft replacement. 15 Therefore, most of the patients with a type A IMH in this study were treated surgically. As a result, the prognosis of patients with a type A IMH in both groups 1 and 2 was more favorable than that reported in other series where early operative repair was not performed. 5,13 In patients with a type B IMH, there was a significant difference in treatment and prognosis between groups 1 and 2. Twenty (87%) of the 23 type B patients in group 2 were treated exclusively by antihypertensive therapy without complications. In contrast, among the 17 patients in group 1 who were treated medically, there were 3 deaths from aortic rupture. Among the 31 patients with a type B IMH in group 1, 8 underwent surgical intervention and 6 were treated with endovascular methods. Endovascular treatment with a stentgraft successfully covered the AU in all 6 patients without early pseudoaneurysm formation. Given that AUs tend to occur in elderly patients with severe atherosclerosis and other comorbidities that put them at high surgical risk, in our limited experience, this minimally invasive endovascular approach may have considerable advantages in this disease compared with conventional open surgical repair. Natural History of AU There exists widespread confusion in the literature about disease behavior of the AU. Stanson et al 2 and Coady et al 7 found AUs to be malignant, but most of these patients had acute symptoms. In contrast, Harris et al 16 and Quint et al 17 reported a lower incidence of life-threatening complications in a patient sample where asymptomatic patients were enrolled. The considerable difference in prognosis probably can be explained by the differences in patient substrate (symptomatic versus asymptomatic). In our series, all patients (group 1) were symptomatic, and this may explain a higher incidence of disease progression. A more aggressive approach should be considered for acutely symptomatic patients. Relationship Between IMH and AU In previous reports of IMHs, many investigators have identified AUs as a cause of IMHs, 3,4,6 whereas others have considered AUs and IMHs to be distinct, unrelated entities. 13 Indeed, a lack of agreement in the terminology used in the literature to describe IMH and AU is clearly evident. Because our results suggest a major difference in prognosis according to whether the IMH coexists with AU or without a AU, it is important to distinguish these 2 types of IMH. ractically speaking, this differentiation must be made by imaging techniques because clinical separation is not possible. Indicators and redictors of Disease rogression in atients With AU We are not aware of reports in which predictive factors of disease progression were investigated in patients with IMHs associated with a AU. ersistent or recurrent pain despite aggressive treatment and an interval increase of pleural effusion were significant and important indicators of disease progression. As for the implications of initial AU size, maximum diameter and depth both correlated significantly with disease progression. atients with a AU that initially measured 20 mm or more in maximum diameter or 10 mm or greater in maximum depth have a high risk of disease progression and thus should be considered candidates for early surgical or endovascular repair. In addition, it is apparent that not only AUs in the ascending or arch but also those in the proximal descending aorta had a more malignant course ( 0.01) compared with
7 348 Circulation July 16, 2002 that observed for AUs in the middle and distal descending aorta. ossible explanations for this tendency include greater hemodynamic stress within the proximal aortic wall or a greater preponderance of elastin over collagen in the media of the proximal aorta compared with the descending thoracic aorta. 18 Regardless of the exact pathophysiological mechanism, early aggressive treatment with either open surgical or endovascular stent-graft repair is prudent for patients with IMH and a proximal AU, especially in those with uncontrollable pain and/or increasing pleural effusion. Limitations of This Study A weakness of this study is the lack of strict diagnostic uniformity in the patient selection. We defined a diagnostic criterion as absence of a visible intimal flap or tear identified by any imaging technique, however, because of differences in the relative abilities of each imaging modality to detect intimal disruption and the evolution in technology that has improved image resolution over the 10-year study period, the diagnostic data used to select patients in this study were not absolutely comparable. Thus, the validity of inferences made from results of this study is questionable. Another limitation is related to the end points. We defined an IMH expansion as an increase in IMH size over the interval between imaging studies, and a stable disease course as one that regressed spontaneously or had no interval change between imaging studies. To reliably compare individual courses of disease, it is ideally necessary to predetermine the timing of imaging studies for the evaluation of interval changes. For example, it would be optimal if baseline studies were obtained at clinically equivalent starting points (eg, at the onset of symptoms), and then follow-up examinations performed at regular prescribed intervals. Because of the constraints imposed by the retrospective nature of this study, however, it is only possible to review studies performed at clinically required intervals. Conclusions This study suggests substantial differences in the clinical features and the patients prognoses in patients with an IMH caused by AU and those with an IMH not associated with a AU. atients with IMH due to a AU commonly had a progressive downhill clinical course, particularly when symptomatic, even when the IMH was limited to the descending thoracic aorta. In comparison, patients with an IMH without an ulcer were typically fairly stable, particularly when the IMH was limited to the descending aorta. Thus, these 2 types of IMH should be distinguished clinically and, more importantly, be managed differently. In terms of treatment for patients with an IMH without a AU, most with a type B IMH can be treated conservatively with aggressive blood pressure control. On the other hand, those with a type A IMH should be treated with early surgical repair. 5,6,15 When the IMH is associated with a AU, urgent surgical aortic graft replacement should be considered not only for patients with a type A IMH, but also for those with a type B IMH, especially if persistent pain and/or interval increase in pleural effusion are present. Acknowledgment The authors thank Eric Huffman for help with the preparation of the manuscript. References 1. Gore I. athogenesis of dissecting aneurysm of the aorta. Arch athol Lab Med. 1952;53: Stanson AW, Kazmier FJ, Hollier LH, et al. enetrating atherosclerotic ulcers of the thoracic aorta: natural history and clinicopathologic correlations. Ann Vasc Surg. 1986;1: Harris KM, Braverman AC, Gutierrez FR, et al. Transesophageal echocardiographic and clinical features of aortic intramural hematoma. J Thorac Cardiovasc Surg. 1997;114: Mohr-Kahaly S, Erbel R, Kearney F, et al. Aortic intramural hemorrhage visualized by transesophageal echocardiography: findings and prognostic implications. J Am Coll Cardiol. 1994;23: Nienaber CA, von Kodolitsch Y, etersen B, et al. Intramural hemorrhage of the thoracic aorta: diagnostic and therapeutic implications. Circulation. 1995;92: Muluk SC, Kaufman JA, Torchiana DF, et al. Diagnosis and treatment of thoracic aortic intramural hematoma. J Vasc Surg. 1996;24: Coady MA, Rizzo JA, Hammond GL, et al. enetrating ulcer of the thoracic aorta: what is it? How do we recognize it? How do we manage it? J Vasc Surg. 1998;27: Sueyoshi E, Matsuoka Y, Sakamoto I, et al. Fate of intramural hematoma of the aorta: CT evaluation. J Comput Assist Tomogr. 1997;21: Yamada T, Tada S, Harada J. Aortic dissection without intimal rupture: diagnosis with MR imaging and CT. Radiology. 1988;168: Krukenberg E. Beiträge zur Frage des Aneurysma dissecans. Beitr athol Anat Allg athol. 1920;67: Hirst AE, Johns VJ, Kime SW. Dissecting aneurysm of the aorta: a review of 505 cases. Medicine. 1958;37: Wilson SK, Hutchins GM. Aortic dissecting aneurysms: causative factors in 204 subjects. Arch athol Lab Med. 1982;106: Coady MA, Rizzo JA, Elefteriades JA. athologic variants of thoracic aortic dissections: penetrating atherosclerotic ulcers and intramural hematomas. Cardiol Clin. 1999;17: Kazerooni EA, Bree RL, Williams DM. enetrating atherosclerotic ulcers of the descending thoracic aorta: evaluation with CT and distinction from aortic dissection. Radiology. 1992;183: Robbins RC, MacManus R, Mitchell RS, et al. Management of patients with intramural hematoma of the thoracic aorta. Circulation. 1993;88(5 pt 2):II1 II Harris JA, Bis KG, Glover JL, et al. enetrating atherosclerotic ulcers of the aorta. J Vasc Surg. 1994;19: Quint LE, Williams DM, Francis IR, et al. Ulcer like lesions of the aorta: imaging features and natural history. Radiology. 2000;218: Borst HG, Heinemann MK, Stone CD. athogenesis. In: Surgical Treatment of Aortic Dissection. New York, NY: Churchill Livingstone Inc; 1996:47 54.
Case Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer
 Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
A Case of Type A Aortic Intramural Hematoma Successfully Managed with Medical Therapy. ( aortic intramural hematoma; IMH ) A ( type A IMH ) type A IMH
 A Case of Type A Aortic Intramural Hematoma Successfully Managed with Medical Therapy 21 A ( aortic intramural hematoma; IMH ) A ( type A IMH ) 67 20 type A IMH 20 W. H. Lin, C. Y. Chen, H. I. Yeh, and
A Case of Type A Aortic Intramural Hematoma Successfully Managed with Medical Therapy 21 A ( aortic intramural hematoma; IMH ) A ( type A IMH ) 67 20 type A IMH 20 W. H. Lin, C. Y. Chen, H. I. Yeh, and
Clinical management and treatment of thoracic aortic diseases. Evolution of IMH. Luigi Lovato
 Clinical management and treatment of thoracic aortic diseases Evolution of IMH Luigi Lovato Cardio-Thoracic and Vascular Department Cardio-Thoracic Radiology-University Hospital S. Orsola-Malpighi Bologna-Italy
Clinical management and treatment of thoracic aortic diseases Evolution of IMH Luigi Lovato Cardio-Thoracic and Vascular Department Cardio-Thoracic Radiology-University Hospital S. Orsola-Malpighi Bologna-Italy
Animesh Rathore, MD 4/21/17. Penetrating atherosclerotic ulcers of aorta
 Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
ACUTE AORTIC SYNDROMES
 ACUTE AORTIC SYNDROMES AGNETA FLINCK MD, PhD Dept. of Thoracic Radiology Sahlgrenska University Hospital ACUTE AORTIC SYNDROMES Aortic dissection Intramural hematoma (IMH) 5-20% Penetrating atherosclerotic
ACUTE AORTIC SYNDROMES AGNETA FLINCK MD, PhD Dept. of Thoracic Radiology Sahlgrenska University Hospital ACUTE AORTIC SYNDROMES Aortic dissection Intramural hematoma (IMH) 5-20% Penetrating atherosclerotic
Aortic intramural hematoma (IMH) has been recognized
 Long-Term Prognosis of Patients With Type A Aortic Intramural Hematoma Shuichiro Kaji, MD; Takashi Akasaka, MD; Yoko Horibata, MD; Kazuhiro Nishigami, MD; Hiroyuki Shono, MD; Minako Katayama, MD; Atsushi
Long-Term Prognosis of Patients With Type A Aortic Intramural Hematoma Shuichiro Kaji, MD; Takashi Akasaka, MD; Yoko Horibata, MD; Kazuhiro Nishigami, MD; Hiroyuki Shono, MD; Minako Katayama, MD; Atsushi
Diseases of Aorta: Marfan, Dissection, Atheroma
 31 st Annual State of the Art Echocardiography San Diego, CA February 20, 2018 9:00 9:20 AM 20 min Diseases of Aorta: Marfan, Dissection, Atheroma Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology
31 st Annual State of the Art Echocardiography San Diego, CA February 20, 2018 9:00 9:20 AM 20 min Diseases of Aorta: Marfan, Dissection, Atheroma Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology
Aortic CT: Intramural Hematoma. Leslie E. Quint, M.D.
 Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Update on Acute Aortic Syndrome
 SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias. UCSF Vascular Symposium April 7-9, Acute Aortic Dissection
 Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Stent-Graft Repair of Penetrating Atherosclerotic Ulcers in the Descending Thoracic Aorta: Mid-Term Results
 Stent-Graft Repair of Penetrating Atherosclerotic Ulcers in the Descending Thoracic Aorta: Mid-Term Results Philippe Demers, MD, MS, D. Craig Miller, MD, R. Scott Mitchell, MD, Stephen T. Kee, MD, Lynn
Stent-Graft Repair of Penetrating Atherosclerotic Ulcers in the Descending Thoracic Aorta: Mid-Term Results Philippe Demers, MD, MS, D. Craig Miller, MD, R. Scott Mitchell, MD, Stephen T. Kee, MD, Lynn
The potential value of intravascular ultrasound imaging in diagnosis of aortic intramural hematoma
 Journal of Geriatric Cardiology (2011) 8: 224 229 2011 IGC All rights reserved; www.jgc301.com Research Articles Open Access The potential value of intravascular ultrasound imaging in diagnosis of aortic
Journal of Geriatric Cardiology (2011) 8: 224 229 2011 IGC All rights reserved; www.jgc301.com Research Articles Open Access The potential value of intravascular ultrasound imaging in diagnosis of aortic
Study of aortic ulcer by using MDCTA
 Study of aortic ulcer by using MDCTA Poster No.: C-3085 Congress: ECR 2010 Type: Topic: Educational Exhibit Vascular Authors: L. Saba, R. Sanfilippo, M. Atzeni, D. Ribuffo, R. Montisci, G. Mallarini; Cagliari/IT
Study of aortic ulcer by using MDCTA Poster No.: C-3085 Congress: ECR 2010 Type: Topic: Educational Exhibit Vascular Authors: L. Saba, R. Sanfilippo, M. Atzeni, D. Ribuffo, R. Montisci, G. Mallarini; Cagliari/IT
Diseases of the Aorta
 Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
Penetrating Atherosclerotic Ulcer
 April 2016 Penetrating Atherosclerotic Ulcer Michael Nguyen, Harvard Medical School Year III Outline Introduction to Penetrating Atherosclerotic Ulcers Radiographic Features Treatment and Prognosis Patient
April 2016 Penetrating Atherosclerotic Ulcer Michael Nguyen, Harvard Medical School Year III Outline Introduction to Penetrating Atherosclerotic Ulcers Radiographic Features Treatment and Prognosis Patient
Endovascular stent-graft repair for penetrating atherosclerotic ulcer in the infrarenal abdominal aorta
 Endovascular stent-graft repair for penetrating atherosclerotic ulcer in the infrarenal abdominal aorta Yoshihiko Tsuji, MD, a Yosuke Tanaka, MD, a Atsushi Kitagawa, MD, a Yutaka Hino, MD, a Takanori Taniguchi,
Endovascular stent-graft repair for penetrating atherosclerotic ulcer in the infrarenal abdominal aorta Yoshihiko Tsuji, MD, a Yosuke Tanaka, MD, a Atsushi Kitagawa, MD, a Yutaka Hino, MD, a Takanori Taniguchi,
Midterm follow-up of penetrating ulcer and intramural hematoma of the aorta
 Midterm follow-up of penetrating ulcer and intramural hematoma of the aorta Shawn L. Tittle, MD a Raymond J. Lynch, BS a Patricia E. Cole, MD b Harsimran S. Singh, BS a John A. Rizzo, PhD c Gary S. Kopf,
Midterm follow-up of penetrating ulcer and intramural hematoma of the aorta Shawn L. Tittle, MD a Raymond J. Lynch, BS a Patricia E. Cole, MD b Harsimran S. Singh, BS a John A. Rizzo, PhD c Gary S. Kopf,
Long-term Follow-up of Aortic Intramural Hematomas and Penetrating Ulcers
 Long-term Follow-up of Aortic Intramural Hematomas and Penetrating Ulcers Alan S. Chou, BA, Bulat A. Ziganshin, MD, Paris Charilaou, MD, Maryann Tranquilli, RN, John A. Rizzo, PhD, John A. Elefteriades,
Long-term Follow-up of Aortic Intramural Hematomas and Penetrating Ulcers Alan S. Chou, BA, Bulat A. Ziganshin, MD, Paris Charilaou, MD, Maryann Tranquilli, RN, John A. Rizzo, PhD, John A. Elefteriades,
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D.
 CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
Detection of Intimal Defect by 64-Row Multidetector Computed Tomography in Patients With Acute Aortic Intramural Hematoma
 Detection of Intimal Defect by 64-Row Multidetector Computed Tomography in Patients With Acute Aortic Intramural Hematoma Takeshi Kitai, MD; Shuichiro Kaji, MD; Atsushi Yamamuro, MD; Tomoko Tani, MD; Makoto
Detection of Intimal Defect by 64-Row Multidetector Computed Tomography in Patients With Acute Aortic Intramural Hematoma Takeshi Kitai, MD; Shuichiro Kaji, MD; Atsushi Yamamuro, MD; Tomoko Tani, MD; Makoto
Case 8036 Multiple penetrating atherosclerotic ulcers
 Case 8036 Multiple penetrating atherosclerotic ulcers Santiago I, Seco M, Curvo-Semedo L Section: Cardiovascular Published: 2010, Feb. 22 Patient: 78 year(s), male Clinical History A 78-year-old hypertensive
Case 8036 Multiple penetrating atherosclerotic ulcers Santiago I, Seco M, Curvo-Semedo L Section: Cardiovascular Published: 2010, Feb. 22 Patient: 78 year(s), male Clinical History A 78-year-old hypertensive
Disclosures: Acute Aortic Syndrome. A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO
 Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Management of intramural hematoma and penetrating ulcers - what is different? D.Böckler University Hospital Heidelberg, Germany
 Management of intramural hematoma and penetrating ulcers - what is different? D.Böckler University Hospital Heidelberg, Germany Disclosure Speaker name: Dittmar Böckler I have the following potential conflicts
Management of intramural hematoma and penetrating ulcers - what is different? D.Böckler University Hospital Heidelberg, Germany Disclosure Speaker name: Dittmar Böckler I have the following potential conflicts
Vascular Intervention
 10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
Penetrating Atherosclerotic Aortic Ulcer: Documentation by Transesophageal Echocardiography
 JACC Vol. 32, No. 1 July 1998:83 9 83 ATHEROSCLEROSIS Penetrating Atherosclerotic rtic Ulcer: Documentation by Transesophageal Echocardiography ISIDRE VILACOSTA, MD, JOSÉ ALBERTO SAN ROMÁN, MD,* PALOMA
JACC Vol. 32, No. 1 July 1998:83 9 83 ATHEROSCLEROSIS Penetrating Atherosclerotic rtic Ulcer: Documentation by Transesophageal Echocardiography ISIDRE VILACOSTA, MD, JOSÉ ALBERTO SAN ROMÁN, MD,* PALOMA
Acute Aortic Syndromes
 Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Superior vena cava obstruction caused by ascending aortic pseudoaneurysm as assessed by multi-detector row computed tomography
 Journal of Cardiology Cases (2011) 3, e98 e102 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/jccase Case Report Superior vena cava obstruction caused by ascending aortic
Journal of Cardiology Cases (2011) 3, e98 e102 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/jccase Case Report Superior vena cava obstruction caused by ascending aortic
IMH/Penetrating Aortic Ulcers/ Saccular Aneurysms: How to manage and when to intervene
 IMH/Penetrating Aortic Ulcers/ Saccular Aneurysms: How to manage and when to intervene UCSF Vascular Surgery Symposium 2018 Sukgu M Han, MD, MS Assistant Professor of Clinical Surgery Co-director, Comprehensive
IMH/Penetrating Aortic Ulcers/ Saccular Aneurysms: How to manage and when to intervene UCSF Vascular Surgery Symposium 2018 Sukgu M Han, MD, MS Assistant Professor of Clinical Surgery Co-director, Comprehensive
Acute Aortic Syndromes
 Acute Aortic Syndromes None Disclosures Smita Patel, M.B.B.S., M.R.C.P., F.R.C.R. Associate Professor, University of Michigan Ann Arbor, MI Objectives To review common CTA findings of acute aortic syndromes
Acute Aortic Syndromes None Disclosures Smita Patel, M.B.B.S., M.R.C.P., F.R.C.R. Associate Professor, University of Michigan Ann Arbor, MI Objectives To review common CTA findings of acute aortic syndromes
Χρόνιος διαχωρισμός. υπερηχοκαρδιογραφική. αορτής. παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ
 Χρόνιος διαχωρισμός αορτής υπερηχοκαρδιογραφική παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ 8-2-2018 The Normal Aorta (conduit function + control ) *Aortic expansion is about
Χρόνιος διαχωρισμός αορτής υπερηχοκαρδιογραφική παρακολούθηση ή άλλη; Α. Παπασπυρόπουλος ΕΠΙΜΕΛΗΤΗΣ ΓΝ.ΝΙΚΑΙΑΣ ΠΕΜΠΤΗ 8-2-2018 The Normal Aorta (conduit function + control ) *Aortic expansion is about
Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE
 Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE Disclosures related to this talk : NONE 2 Clinical case A 40 year-old
Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE Disclosures related to this talk : NONE 2 Clinical case A 40 year-old
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD
 Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
No Disclosure. Aortic Dissection in Japan. This. The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair
 No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
IMAGING the AORTA. Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011
 IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D.
 Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Journal of Cardiovascular Magnetic Resonance 2010, 12:27
 Journal of Cardiovascular Magnetic Resonance This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon.
Journal of Cardiovascular Magnetic Resonance This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon.
Acute aortic syndrome
 Keynote Lecture Series Acute aortic syndrome Joel S. Corvera Division of Cardiothoracic Surgery, Indiana University School of Medicine and Indiana University Health, Indianapolis, IN, USA Correspondence
Keynote Lecture Series Acute aortic syndrome Joel S. Corvera Division of Cardiothoracic Surgery, Indiana University School of Medicine and Indiana University Health, Indianapolis, IN, USA Correspondence
SUPPLEMENTAL MATERIAL
 SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
Multimodality Imaging of the Thoracic Aorta
 Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Peter I. Kalmar, 1 Peter Oberwalder, 2 Peter Schedlbauer, 1 Jürgen Steiner, 1 and Rupert H. Portugaller Introduction. 2.
 Case Reports in Medicine Volume 2013, Article ID 714914, 4 pages http://dx.doi.org/10.1155/2013/714914 Case Report Secondary Aortic Dissection after Endoluminal Treatment of an Intramural Hematoma of the
Case Reports in Medicine Volume 2013, Article ID 714914, 4 pages http://dx.doi.org/10.1155/2013/714914 Case Report Secondary Aortic Dissection after Endoluminal Treatment of an Intramural Hematoma of the
Katarzyna J. Macura 1, Frank M. Corl, Elliot K. Fishman, David A. Bluemke
 Downloaded from www.ajronline.org by 174.110.46.171 on 02/10/18 from IP address 174.110.46.171. opyright RRS. For personal use only; all rights reserved cute aortic syndromes refer to the spectrum of aortic
Downloaded from www.ajronline.org by 174.110.46.171 on 02/10/18 from IP address 174.110.46.171. opyright RRS. For personal use only; all rights reserved cute aortic syndromes refer to the spectrum of aortic
Remarkable progress has been made in recent years
 Intramural Hematoma and Penetrating Atherosclerotic Ulcer of the Aorta Thoralf M. Sundt, MD Division of Cardiovascular Surgery, Mayo Clinic, Rochester, Minnesota Intramural hematoma and penetrating aortic
Intramural Hematoma and Penetrating Atherosclerotic Ulcer of the Aorta Thoralf M. Sundt, MD Division of Cardiovascular Surgery, Mayo Clinic, Rochester, Minnesota Intramural hematoma and penetrating aortic
2014 ESC Guidelines on the Diagnosis & Treatment of AORTIC DISEASES
 2014 ESC Guidelines on the Diagnosis & Treatment of AORTIC DISEASES Prof. Fausto J. Pinto, FESC, FACC, FASE President, ESC University Hospital Sta Maria University of Lisbon, Portugal Professor Fausto
2014 ESC Guidelines on the Diagnosis & Treatment of AORTIC DISEASES Prof. Fausto J. Pinto, FESC, FACC, FASE President, ESC University Hospital Sta Maria University of Lisbon, Portugal Professor Fausto
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Chronic type A dissection: when to operate? Francois Dagenais, MD PII: S0022-5223(18)33131-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.032 Reference: YMTC 13781 To appear in: The
Accepted Manuscript Chronic type A dissection: when to operate? Francois Dagenais, MD PII: S0022-5223(18)33131-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.032 Reference: YMTC 13781 To appear in: The
Echocardiographic Evaluation of the Aorta
 Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Role of Gender in TEVAR and EVAR results from the GREAT registry
 Role of Gender in TEVAR and EVAR results from the GREAT registry Mauro Gargiulo Vascular Surgery University of Bologna - DIMES Policlinico S.Orsola-Malpighi Bologna, Italy mauro.gargiulo2@unibo.it Disclosure
Role of Gender in TEVAR and EVAR results from the GREAT registry Mauro Gargiulo Vascular Surgery University of Bologna - DIMES Policlinico S.Orsola-Malpighi Bologna, Italy mauro.gargiulo2@unibo.it Disclosure
Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta
 02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
Total Endovascular Repair Type A Dissection. Eric Herget Interventional Radiology
 Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure
 Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
Thoracic Endovascular Aortic Repair (TEVAR) Indications and Basic Procedure Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosure Speaker name: Tilo Kölbel, MD I
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial
 An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry
 University of Milan Thoracic Aortic Research Center Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry Santi Trimarchi, MD, PhD Associate
University of Milan Thoracic Aortic Research Center Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry Santi Trimarchi, MD, PhD Associate
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
Penetrating atherosclerotic ulcers of the aorta
 Penetrating atherosclerotic ulcers of the aorta James A. Harris, MD, Kostaki G. Bis, MD, John L. Glover, MD, Phillip J. Bendick, PhD, Anil Shetty, PhD, and O. William Brown, MD, RDyal Oak, Mich. Purpose:
Penetrating atherosclerotic ulcers of the aorta James A. Harris, MD, Kostaki G. Bis, MD, John L. Glover, MD, Phillip J. Bendick, PhD, Anil Shetty, PhD, and O. William Brown, MD, RDyal Oak, Mich. Purpose:
TEVAR FOR! THORACIC AORTIC TRAUMA"
 10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
Endovascular Repair of Infrarenal Abdominal Aorta Penetrating Atherosclerotic Ulcers: Review of Our Experience
 EJVES Extra (2008) 16, 4e9 SHORT REPORT Endovascular Repair of Infrarenal Abdominal Aorta Penetrating Atherosclerotic Ulcers: Review of Our Experience B. Fyntanidou a, *, E. Massa b, A. Papachristodoulou
EJVES Extra (2008) 16, 4e9 SHORT REPORT Endovascular Repair of Infrarenal Abdominal Aorta Penetrating Atherosclerotic Ulcers: Review of Our Experience B. Fyntanidou a, *, E. Massa b, A. Papachristodoulou
Percutaneous Approaches to Aortic Disease in 2018
 Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Importance of false lumen thrombosis in type B aortic dissection prognosis
 Importance of false lumen thrombosis in type B aortic dissection prognosis Santi Trimarchi, MD, PhD, a Jip L. Tolenaar, MD, a Frederik H. W. Jonker, MD, PhD, b Brian Murray, MD, c Thomas T. Tsai, MD, d
Importance of false lumen thrombosis in type B aortic dissection prognosis Santi Trimarchi, MD, PhD, a Jip L. Tolenaar, MD, a Frederik H. W. Jonker, MD, PhD, b Brian Murray, MD, c Thomas T. Tsai, MD, d
La sindrome aortica acuta oggi
 University of Milan Thoracic Aortic Research Center La sindrome aortica acuta oggi Santi Trimarchi, MD, PhD Professore Associato di Chirurgia Vascolare, Università degli Studi di Milano Direttore, Divisione
University of Milan Thoracic Aortic Research Center La sindrome aortica acuta oggi Santi Trimarchi, MD, PhD Professore Associato di Chirurgia Vascolare, Università degli Studi di Milano Direttore, Divisione
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
2 nd International Meeting on Aortic Diseases Liege, Belgium September, 2010
 Bovine Aortic Arch Not a Benign Variant 2 nd International Meeting on Aortic Diseases Liege, Belgium September, 2010 John A. Elefteriades, MD William W.L. Glenn Professor and Chief, Section of Cardiac
Bovine Aortic Arch Not a Benign Variant 2 nd International Meeting on Aortic Diseases Liege, Belgium September, 2010 John A. Elefteriades, MD William W.L. Glenn Professor and Chief, Section of Cardiac
Current Trends in. Torin P. Fitton, MD Division of Cardiothoracic Surgery Lahey Clinic NO DISCLOSURES. Aortic Syndromes
 Current Trends in Aortic Syndromes Torin P. Fitton, MD Division of Cardiothoracic Surgery Lahey Clinic NO DISCLOSURES Aortic Syndromes Aortic Aneurysm Aortic Dissection Intramural Hematoma (IMH) Penetrating
Current Trends in Aortic Syndromes Torin P. Fitton, MD Division of Cardiothoracic Surgery Lahey Clinic NO DISCLOSURES Aortic Syndromes Aortic Aneurysm Aortic Dissection Intramural Hematoma (IMH) Penetrating
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA)
 The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations
 The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
TEVAR for Chronic dissections: indications for TEVAR, long term results
 TEVAR for Chronic dissections: indications for TEVAR, long term results J Sobocinski, R Azzaoui, B Maurel, R Spear, T Martin-Gonzalez, A Hertault, S Haulon Centre de l Aorte, Chirurgie vasculaire, Hôpital
TEVAR for Chronic dissections: indications for TEVAR, long term results J Sobocinski, R Azzaoui, B Maurel, R Spear, T Martin-Gonzalez, A Hertault, S Haulon Centre de l Aorte, Chirurgie vasculaire, Hôpital
Development of a Branched LSA Endograft & Ascending Aorta Endograft
 Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
Diseases of the aorta
 Diseases of the aorta Aneurysm, dissection and aortitis are the main pathologies (Fig. 18.79 ). data:text/html;charset=utf-8,%3ch2%20id%3d%22cc5a0836d6aa490ca26dd7c15632b559%22%20style%3d%22margin%3a%201.3em%200px%200.5em%3b%20padding%3a%200px%3b%20border%3a%200px%3b%20font-fa
Diseases of the aorta Aneurysm, dissection and aortitis are the main pathologies (Fig. 18.79 ). data:text/html;charset=utf-8,%3ch2%20id%3d%22cc5a0836d6aa490ca26dd7c15632b559%22%20style%3d%22margin%3a%201.3em%200px%200.5em%3b%20padding%3a%200px%3b%20border%3a%200px%3b%20font-fa
Long-Term Predictors of Descending Aorta Aneurysmal Change in Patients With Aortic Dissection
 Journal of the American College of Cardiology Vol. 50, No. 8, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.03.064
Journal of the American College of Cardiology Vol. 50, No. 8, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.03.064
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
The natural history of uncomplicated type B dissection, PAU and IMH: the IRAD knowledge. Santi Trimarchi, MD, PhD
 IRCCS Policlinico San Donato University of Milan Thoracic Aortic Research Center The natural history of uncomplicated type B dissection, PAU and IMH: the IRAD knowledge Santi Trimarchi, MD, PhD No COI
IRCCS Policlinico San Donato University of Milan Thoracic Aortic Research Center The natural history of uncomplicated type B dissection, PAU and IMH: the IRAD knowledge Santi Trimarchi, MD, PhD No COI
Dissection de type B: l étude Instead et corollaire stratégique
 Dissection de type B: l étude Instead et corollaire stratégique Christoph A. Nienaber, MD, FACC University Rostock Heartcenter Med. Clinic I Cardiology christoph.nienaber@med.uni-rostock.de Type B aortic
Dissection de type B: l étude Instead et corollaire stratégique Christoph A. Nienaber, MD, FACC University Rostock Heartcenter Med. Clinic I Cardiology christoph.nienaber@med.uni-rostock.de Type B aortic
Introducing the GORE TAG Conformable Thoracic Stent Graft with ACTIVE CONTROL System
 Introducing the GORE TAG Conformable Thoracic Stent Graft with ACTIVE CONTROL System K. Oikonomou Department of Vascular Surgery Regensburg University Disclosures W.L. Gore & Associates Sponsored Presentation
Introducing the GORE TAG Conformable Thoracic Stent Graft with ACTIVE CONTROL System K. Oikonomou Department of Vascular Surgery Regensburg University Disclosures W.L. Gore & Associates Sponsored Presentation
I have the following financial relationships to disclose:
 Novel Approaches to Endovascular Management of Aortic Aneurysms Rodney A White, MD Medical Director, Vascular Services MemorialCare Heart & Vascular Institute Long Beach Memorial Hospital Long Beach, California
Novel Approaches to Endovascular Management of Aortic Aneurysms Rodney A White, MD Medical Director, Vascular Services MemorialCare Heart & Vascular Institute Long Beach Memorial Hospital Long Beach, California
Optimal Treatment of Chronic Dissection
 Optimal Treatment of Chronic Dissection Chun-Che Shih 施俊哲 MD, Ph.D. Chief, Professor Institute of Clinical Medicine National Yang Ming University Division of Cardiovascular Surgery Taipei Veterans General
Optimal Treatment of Chronic Dissection Chun-Che Shih 施俊哲 MD, Ph.D. Chief, Professor Institute of Clinical Medicine National Yang Ming University Division of Cardiovascular Surgery Taipei Veterans General
Aortic Dissection Without Intimal Tear: Case Report and Findings on Transesophageal Echocardiography
 Aortic Dissection Without Intimal Tear: Case Report and Findings on Transesophageal Echocardiography James P. Eichelberger, MD, Rochester, New York Transesophageal echocardiography (TEE) relies on the
Aortic Dissection Without Intimal Tear: Case Report and Findings on Transesophageal Echocardiography James P. Eichelberger, MD, Rochester, New York Transesophageal echocardiography (TEE) relies on the
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Experience of endovascular procedures on abdominal and thoracic aorta in CA region
 Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Penetrating atherosclerotic ulcer (PAU) is defined as
 Ann Vasc Dis Vol.5, No.1; 2012; pp8 14 2012 Annals of Vascular Diseases doi: 10.34000/avd.oa.11.00916 Original Article Abdominal Aortic Disease Caused by Penetrating Atherosclerotic Ulcers Masataka Sato,
Ann Vasc Dis Vol.5, No.1; 2012; pp8 14 2012 Annals of Vascular Diseases doi: 10.34000/avd.oa.11.00916 Original Article Abdominal Aortic Disease Caused by Penetrating Atherosclerotic Ulcers Masataka Sato,
Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta
 Brief Reports Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta Mikolaj Wojtaszek, MD, PhD, Krzysztof Milczarek, MD, PhD, Jacek Szmidt, MD, PhD, and Olgierd Rowinski,
Brief Reports Emergency Endovascular Treatment for Ruptured Type B Dissection in the Abdominal Aorta Mikolaj Wojtaszek, MD, PhD, Krzysztof Milczarek, MD, PhD, Jacek Szmidt, MD, PhD, and Olgierd Rowinski,
Transluminal placement of endovascular stentgrafts for the treatment of type A aortic dissection with an entry tear in the descending thoracic aorta
 CLINICAL RESEARCH STUDIES Transluminal placement of endovascular stentgrafts for the treatment of type A aortic dissection with an entry tear in the descending thoracic aorta Noriyuki Kato, MD, a Takatsugu
CLINICAL RESEARCH STUDIES Transluminal placement of endovascular stentgrafts for the treatment of type A aortic dissection with an entry tear in the descending thoracic aorta Noriyuki Kato, MD, a Takatsugu
I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical Department National Taiwan University Hospital
 Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Multimodality Imaging in Aortic Diseases:
 Multimodality Imaging in Aortic Diseases: Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee MedStar Washington Hospital Center MedStar Health Research Institute Georgetown University
Multimodality Imaging in Aortic Diseases: Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee MedStar Washington Hospital Center MedStar Health Research Institute Georgetown University
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns
 CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
Aortic dissection is one of the most catastrophic events that affects
 Surgery for Acquired Cardiovascular Disease Midterm results of stent-graft repair of acute and chronic aortic dissection with descending tear: The complicationspecific approach Noriyuki Kato, MD a Takatsugu
Surgery for Acquired Cardiovascular Disease Midterm results of stent-graft repair of acute and chronic aortic dissection with descending tear: The complicationspecific approach Noriyuki Kato, MD a Takatsugu
, David Stultz, MD. Aortic Dissection. David Stultz, MD October 7, 2003
 Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
New ASE Guidelines: What you must know
 New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
Acute aortic syndrome : Comprehensive MDCT evaluation
 Acute aortic syndrome : Comprehensive MDCT evaluation Poster No.: C-2290 Congress: ECR 2018 Type: Educational Exhibit Authors: S. Ilic, Z. Badnjar, D. Raceta Masic, D. Raicevic, V. Vujovic ; 1 1 2 2 2
Acute aortic syndrome : Comprehensive MDCT evaluation Poster No.: C-2290 Congress: ECR 2018 Type: Educational Exhibit Authors: S. Ilic, Z. Badnjar, D. Raceta Masic, D. Raicevic, V. Vujovic ; 1 1 2 2 2
Aneurysms & a Brief Discussion on Embolism
 Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques
 Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Delayed Surgical Management of Traumatic Pseudoaneurysm of the Ascending Aorta in Multiple Trauma
 CASE REPORT J Trauma Inj 2018;31(1):29-33 http://doi.org/10.20408/jti.2018.31.1.29 JOURNAL OF TRAUMA AND INJURY Delayed Surgical Management of Traumatic Pseudoaneurysm of the Ascending Aorta in Multiple
CASE REPORT J Trauma Inj 2018;31(1):29-33 http://doi.org/10.20408/jti.2018.31.1.29 JOURNAL OF TRAUMA AND INJURY Delayed Surgical Management of Traumatic Pseudoaneurysm of the Ascending Aorta in Multiple
High Risk Uncomplicated Type B Dissection
 High Risk Uncomplicated Type B Dissection Ali Azizzadeh, MD, FACS Director, Vascular Surgery Vice Chair, Department of Surgery Associate Director, Heart Institute Cedars-Sinai Medical Center Los Angeles,
High Risk Uncomplicated Type B Dissection Ali Azizzadeh, MD, FACS Director, Vascular Surgery Vice Chair, Department of Surgery Associate Director, Heart Institute Cedars-Sinai Medical Center Los Angeles,
Jean Jeudy, MD. Disease is very old, and nothing about it has changed. It is we who change as we learn to recognize what was formerly imperceptible.
 Armed Forces Institute of Pathology D e p a r t m e n t o f D i a g n o s t i c R a d i o l o g y T h e A c u t e A o r t i c S y n d r o m e s Jean Jeudy, MD BB aa lltt iimm oo rr e e,, MM aa rr yy llaa
Armed Forces Institute of Pathology D e p a r t m e n t o f D i a g n o s t i c R a d i o l o g y T h e A c u t e A o r t i c S y n d r o m e s Jean Jeudy, MD BB aa lltt iimm oo rr e e,, MM aa rr yy llaa
