Left ventricular pseudoaneurysm is a rare but serious
|
|
|
- Byron Waters
- 5 years ago
- Views:
Transcription
1 Percutaneous Closure of Left Ventricular Pseudoaneurysm Yuriy Dudiy, MD; Vladimir Jelnin, MD; Bryce N. Einhorn; Itzhak Kronzon, MD; Howard A. Cohen, MD; Carlos E. Ruiz, MD, PhD Background Left ventricular pseudoaneurysm is a rare but serious complication from myocardial infarction and cardiac surgery. Although standard treatment is surgical intervention, percutaneous closure of left ventricular pseudoaneurysm has become an option for high-risk surgical candidates. Experience with percutaneous treatment is limited to a few single case reports. This is the first series of percutaneous treatment of the left ventricular pseudoaneurysms. Methods and Results This is a retrospective analysis of 9 procedures of percutaneous repair of left ventricular pseudoaneurysm in 7 consecutive patients (ages 51 to 83 years, 6 men) completed in our Structural Heart Disease center from June 2008 to December All patients were considered as a high risk for surgery because of multiple comorbidities. Multiple imaging modalities were used before, during, and after the procedures to improve success and efficacy. The left ventricular pseudoaneurysms of all 7 patients were successfully repaired. Fluoroscopy time on average was minutes (range, 12.4 to 75.7 minutes). All patients were followed up for a period ranging from 3 to 32 months after the procedure. Each patient improved by at least 1 New York Heart Association functional class, and 4 patients improved by 2 classes. Conclusions Transcatheter closure of the left ventricular pseudoaneurysm is a feasible alternative for high-risk surgical candidates. The use of multiple imaging modalities is required for a detail planning and execution of the procedure. (Circ Cardiovasc Interv. 2011;4: ) Key Words: myocardial infarction aneurysm cardiac tamponade left ventricular pseudoaneurysm Left ventricular pseudoaneurysm is a rare but serious complication that may occur after acute myocardial infarction or cardiac surgery. Left ventricular pseudoaneurysm is a rupture of the left ventricular wall that is contained by the pericardium. In many cases, cardiac rupture results in cardiac tamponade and death. 1 In left ventricular pseudoaneurysm, however, this rupture is contained by pericardial adhesions or a new thrombus, preventing exsanguination. 1 6 The true incidence of left ventricular pseudoaneurysms is unknown. In few reports, however, myocardial infarction and previous cardiac surgery accounted for 55% and 33%, respectively, of all causes of left ventricular pseudoaneurysm. 7 Mitral valve replacements, in particular, have been associated with causing left ventricular pseudoaneurysms. 8 Although the general consensus for initial treatment is surgical intervention, 7,9 percutaneous left ventricular pseudoaneurysm closure is a new alternative for high-risk surgical candidates. Editorial see p 308 Clinical Perspective on p 326 Percutaneous closure of the left ventricular pseudoaneurysm was first described by Clift et al 10 in 2004, but experience is still limited to a few single-case reports. The purpose of this article is to report our single-center experience with percutaneous treatment of left ventricular pseudoaneurysms. Methods This retrospective study encompasses 7 consecutive patients who underwent 9 procedures of percutaneous repair of left ventricular pseudoaneurysm at the Lenox Hill Hospital Structural Heart Disease center from June 2008 to December The patients demographics are summarized in Table 1. Overall mean age was years, ranging from 51 to 83 years; 6 patients were men. All patients were considered as a high risk for surgery because of multiple comorbidities: All patients had congestive heart failure and systemic hypertension, 5 patients had atrial fibrillation, 3 patients had a permanent pacemaker, 2 patients had prior coronary bypass surgery, and 1 patient had 4 previous mitral valve replacements. Five patients had development of left ventricular pseudoaneurysm as a result of previous mitral valve replacement surgery, and 2 patients had development of left ventricular pseudoaneurysm as a result of myocardial infarction. Patients were informed about procedural risks, therapeutic alternatives, and off-label use of closure devices. Written informed consent was obtained from all patients before the procedure. The study was approved by Lenox Hill Hospital s Institutional Review Board. Procedural success was defined as the successful implantation of the closure device, without embolization or migration, at the left ventricular pseudoaneurysm orifice with no flow into the pseudoaneurysm cavity as determined by color-flow Doppler. Imaging Computed Tomographic Angiography All patients underwent computed tomographic angiography (CTA) before the procedure. We used helical acquisition with retrospective Received March 22, 2011; accepted June 6, From the Lenox Hill Heart and Vascular Institute of New York, NY. Correspondence to Carlos E. Ruiz, MD, PhD, 130 East 77th St, 9th Floor, Black Hall, New York, NY cruiz@lenoxhill.net 2011 American Heart Association, Inc. Circ Cardiovasc Interv is available at DOI: /CIRCINTERVENTIONS
2 Dudiy et al Closure of Left Ventricular Pseudoaneurysm 323 Table 1. Patient Demographics Patient Age, y Sex NYHA-FC Etiology Location LVPA Size, mm 1 59 Female III MVR Paravalvular Male II MVR Paravalvular Male III MVR Paravalvular Male III MVR Paravalvular Male III Post-MI Anteroapical a b c Male III Post-MI Anterolateral Male III MVR Paravalvular NYHA-FC indicates New York Heart Association functional classification; MI, myocardial infarction; MVR, mitral valve replacement; LVPA, left ventricular pseudoaneurysm. ECG-gated reconstruction of 16 phases at equally spaced intervals increments. Four-dimensional (4D) (time-factor) volume rendering (using Aquarius v , workstation, TeraRecon Inc, San Mateo, CA), which simulates actual heart movements, was used to evaluate the dynamic changes of the left ventricular pseudoaneurysm. Size and type of the device, as well as the approach, was selected on the basis of information obtained from the volume rendered CTA (Figure 1). The volume-rendered CTA images were also used for planning of the transapical and left ventricular pseudoaneurysm punctures, as previously described. 11 Echocardiography Each patient was examined by transthoracic (TTE) and transesophageal (TEE) echocardiography. In 5 of 7 patients, real-time, 3D TTE and TEE were also performed, using the IE33 system a with the x7-2t probe (Philips, Andover, MA). Images were obtained by using the live 3D, 3D zoom, and full-volume modalities. Images were obtained and recorded during each stage of the procedure. The operator used the information thus obtained to guide the catheters and devices throughout the procedure (Figure 2). The blood flow from the left ventricle into the left ventricular pseudoaneurysm (during LV systole) and back from the left ventricular pseudoaneurysm into the LV (during LV diastole) were evaluated by spectral and color flow Doppler. The 2D TTE was used in 1 procedure to guide and monitor percutaneous puncture of the pseudoaneurysm. Interventional Techniques All the left ventricular pseudoaneurysms were repaired by implantation of the closure device at the orifice of the pseudoaneurysm, preventing the communication between the left ventricle and pseudoaneurysm. The size and type of occlusive devices were chosen based on the dimensions of the left ventricular pseudoaneurysm orifice(s) measured using the 3D (4D) volume-rendered CTA images. In 3 procedures, left ventricular pseudoaneurysm closure were accomplished by retrograde approach to the left ventricle, using a Judkin left catheters (Cordis, Miami Lakes, FL) over a Wholey wire (Covidien Imaging, Hazelwood, MO) or a Tiger wire (St Jude Medical, St Paul, MN). In 1 patient, a 7F delivery catheter was used to deliver the Amplatzer Septal Occluder (AGA Medical Corp, Plymouth, MN); in 2 patients, the Amplatzer Vascular Plug II was delivered with guide catheters (AGA Medical Corp). A transapical approach was used in 6 procedures. It was carefully planned before the procedure with 4D volume-rendered CTA and was monitored by 3D TEE. Transapical puncture was accomplished by accessing the left ventricle percutaneously with a 21-gauge micropuncture needle (Cook Medical Inc, Bloomington, IN). A 4F or 5F radial artery sheath was then inserted into the left ventricular cavity. A Berenstein catheter was used to guide a Wholey wire (Covidien Imaging, Hazelwood, MO) or an Inoue wire (Toray International America Inc, Houston, TX) through the left ventricular pseudoaneurysm orifice, over which an appropriate-sized delivery sheath was placed. The transapical approach for procedures 5b, 5c, and 6 was accomplished by direct percutaneous puncture of the left ventricular pseudoaneurysm, followed by advancement of the wire through the orifice of the pseudoaneurysm, into the LV cavity. In procedures 5b and 6, an exchange length angled hydrophilic glide wire (Terumo Medical Corp, Somerset, NJ) was snared into the aorta and exteriorized through the right femoral artery creating a supporting arterioventricular rail. The delivery sheath was then advanced from the arterial side into the pseudoaneurysm for the retrograde delivery of the closure device. In procedure 5c, after direct left ventricular pseudoaneurysm puncture, a guide wire was ad- Figure 1. Evaluation of the anterolateral postmyocardial infarction pseudoaneurysm using 3D volume-rendered computed tomography angiogram (patient 6). A, Straight posterior view with activated cut-plane. B, Measurements of the orifice from the ventricular side. LVPA indicates left ventricular pseudoaneurysm; Ao, aorta; LV, left ventricle.
3 324 Circ Cardiovasc Interv August 2011 Figure 2. Intraprocedural transesophageal echocardiography (modified transgastric view). A, Frame demonstrates the left ventricular pseudoaneurysm with catheter (white arrow) advanced inside the pseudoaneurysm, continuous wave Doppler demonstrates blood flow to the pseudoaneurysm cavity. B, Real-time 3D transesophageal echocardiography demonstrates the pseudoaneurysm with catheter inside. C, Frame demonstrates wellpositioned closure device (black arrow) at the neck of the pseudoaneurysm, continuous wave Doppler confirms cessation of the communication between the left ventricle and left ventricular pseudoaneurysm cavity. D, Real-time 3D transesophageal echocardiography shows the en face view of the deployed closure device (black arrow). LV indicates left ventricle; LVPA, left ventricular pseudoaneurysm. vanced into the left atrium and snared by means of the transseptal approach and then exteriorized through the right femoral vein, creating an arterial-venous rail over which a 12F delivery sheath was placed from the pseudoaneurysm side for transthoracic delivery of the closure device. In 3 patients (1, 3, and 7), the transapical access was closed using a 6-mm to 4-mm Amplatzer Duct Occluder (AGA Medical Corp). In 1 patient (patient 7), after the release of the closure device and after blood flow across the device decreased, thrombin was injected into the left ventricular pseudoaneurysm cavity to expedite the clot formation. Then, Surgiflo (Ethicon Inc, Somerville, NJ) was injected into the delivery sheath to fill the track to the skin. 12 Results The left ventricular pseudoaneurysms of all 7 patients were successfully closed. One patient required 3 procedures to close the pseudoaneurysm because of the device displacement into the left ventricular pseudoaneurysm cavity (details below). Fluoroscopy time on average was minutes and ranged from 12.4 to 75.7 minutes. A total of 10 devices were used for left ventricular pseudoaneurysm closure: 5 Amplatzer Septal Occluders; 2 Amplatzer Vascular Plug II; 2 Amplatzer Muscular VSD Occluders; and 1 Amplatzer Duct Occluder (all from AGA Medical Corp). One patient, with a donut-shaped pseudoaneurysm, required 2 occluders: 1 24-mm and 1 32-mm Amplazter Septal Occluder (AGA Medical Corp). The 24-mm closure device was delivered into the anterior orifice, and the larger posterior left ventricular pseudoaneurysm orifice was then entered with 12 F delivery sheath and the second, 32-mm closure device was deployed, with the distal disc anchored with the first device (Figure 3). In the patient who required 3 procedures, initially the left ventricular pseudoaneurysm was closed by using the 12-mm Amplazter Septal Occluder (AGA Medical Corp) device, using a retrograde approach. During a CTA follow-up performed a few hours after the procedure, device migration into the left ventricular pseudoaneurysm cavity was observed. The second procedure was performed through the use of the transapical approach and the Amplatzer Muscular VSD Occluder (AGA Medical Corp) was successfully deployed into the neck of the left ventricular pseudoaneurysm. TTE and TEE confirmed the absence of flow through the device and that communication with left ventricular pseudoaneurysm was discontinued. A postprocedure CTA, however, showed a second device embolization into the left ventricular pseudoaneurysm as well. In the third procedure, a combination of transapical puncture and transseptal technique was performed. After establishing stable support of the guide wire, the 18-mm Amplazter Septal Occluder (AGA Medical Corp) was delivered in a transseptal manner. The follow-up CTA, 1 Figure 3. A donut-shaped paravalvular pseudoaneurysm (patient 1), 3D volume-rendered computed tomography angiogram (ventricular side view). A, Donut-shaped left ventricular pseudoaneurysm (LVPA) with 2 orifices (white 2-headed arrow). B, Two Amplatzer Septal Occluders (white arrows) positioned at both pseudoaneurysm orifices. MV indicates mitral valve; AO, aortic valve, LVPA, left ventricular pseudoaneurysm; RV, right ventricle; PA, pulmonary artery.
4 Dudiy et al Closure of Left Ventricular Pseudoaneurysm 325 Follow-Up All patients were followed up for a period ranging from 3 to 32 months (mean, months) after the procedure. Although prevention of left ventricular pseudoaneurysm rupture was the primary goal of repair, 3 patients improved by 1 New York Heart Association functional class, and 4 improved by 2 classes. There were no complications observed during the follow-up period. Figure 4. Three-dimensional volume-rendered computed tomography angiogram demonstrates diverse shapes, sizes, and locations of the left ventricular pseudoaneurysms. Frames A and B demonstrate paravalvular pseudoaneurysms. Frames C and D demonstrate post myocardial infarction left ventricular pseudoaneurysms. week after the procedure, confirmed device position at the left ventricular pseudoaneurysm neck without any evidence of blood extravasation. Previously embolized devices were left inside the left ventricular pseudoaneurysm cavity. There were no complications observed in any of the patients. Table 2. Closure Details Discussion The left ventricular pseudoaneurysm is a rare but potentially lethal complication of myocardial infarction, cardiac surgery, trauma, and infections. Untreated, pseudoaneurysms have a 30% to 45% risk of rupture within the first year. Surgical repair of the left ventricular pseudoaneurysm carries a high risk of morbidity and mortality, mortality rate of 20% to 36% 3 5,7,9,13,14 ; however, is better than medical treatment, which carries an even higher mortality rate of 48%. 7 This study is the first reported series of percutaneous closure of the left ventricular pseudoaneurysm to date. Despite the small number of patients, successful closure with no complication in 7 consecutive patients demonstrates feasibility and safety of the percutaneous repair of the left ventricular pseudoaneurysms. This study was limited by the small number of patients. We cannot, therefore, recommend any particular type of device or judge if there is any advantages of one device over another. Moreover, we believe that an individualized approach should be used for every case because of the unique anatomic characteristics of pseudoaneurysms (size and location of the pseudoaneurysm orifice, length of the neck, shape of the pseudoaneurysm cavity, etc) (Figure 4). All these parameters should be accounted when selecting the closure device. For example, for a pseudoaneurysm with a long neck, devices that have a lengthier waist, such as Amplatzer Duct Occluder or muscular VSD Occluder (both from AGA Medical Corp, Plymouth, MN), are warranted. Closure devices used in our study along with orifices size and oversize ratio are presented in Table 2. We think that the 2 device dislodgments in patient 5 were, most likely, caused by the friability of the myocardium after the recent myocardial infarction (10 days) rather than device size mismatch. Use of the 3D/4D volume-rendered CTA images and, to a lesser extent, 3D echocardiography, allows appreciation of the 3D anatomy of the pseudoaneurysm and neighboring Patient Approach Fluoroscopy Time, min Orifice Size, mm Device Oversize Ratio 1 Transapical* mm ASO mm ASO Retrograde mm AVP II Transapical* mm AmVSD Retrograde mm AVP II 1.0 5a Retrograde mm ASO 1.2 B Retrograde/Transapical mm AmVSD 1.1 C Transseptal/Transapical mm ASO Retrograde/Transapical mm ASO Transapical* mm ADO 1.4 ASO indicates Amplatzer Septal Occluder; AVP, Amplatzer Vascular Plug; AmVSD, Amplatzer Muscular VSD Occluder; and ADO, Amplatzer Duct Occluder (all from AGA Medical Corp, Plymouth, MN). *Transapical access site closure; direct puncture of LVPA; ratio between maximal orifice diameter and body of the device.
5 326 Circ Cardiovasc Interv August 2011 structures helping to select the appropriate closure device. The TTE, which was used in 1 case of anterolateral left ventricular pseudoaneurysm, was very useful during the transthoracic puncture of the pseudoaneurysm. Pseudoaneurysm wall tenting was clearly seen on the 2D image, confirming the position of the puncture needle. The intraprocedure TEE guidance was also very useful for confirmation of the position of the catheters and closure device. There is no standardized approach for left ventricular pseudoaneurysm closure, and no standard fluoroscopy views have been defined. Fluoroscopic imaging for left ventricular pseudoaneurysm percutaneous closure, therefore, can be challenging. The 3D echocardiography and 3D volumerendered CTA can help to quickly interpolate the 2D fluoroscopic view into 3D structures. Conclusion Transcatheter closure of the left ventricular pseudoaneurysm is a feasible alternative for high-risk surgical candidates. The use of multiple imaging modalities is required for detailed planning and execution of the procedure. Disclosures Dr Ruiz is a consultant and educational grant recipient from Philips Healthcare and is a proctor for AGA Medical Corp. Dr Kronzon has received speaking honoraria from Philips Healthcare and is a research grant recipient from GE. References 1. Van Tassel RA, Edwards JE. Rupture of heart complicating myocardial infarction: analysis of 40 cases including nine examples of left ventricular false aneurysm. Chest. 1972;61: Vlodaver Z, Coe JI, Edwards JE. True and false left ventricular aneurysms: propensity for the alter to rupture. Circulation. 1975;51: Yeo TC, Malouf JF, Oh JK, Seward JB. Clinical profile and outcome in 52 patients with cardiac pseudoaneurysm. Ann Intern Med. 1998;128: Pretre R, Linka A, Jenni R, Turina MI. Surgical treatment of acquired left ventricular pseudoaneurysms. Ann Thorac Surg. 2000;70: Eren E, Bozbuga N, Toker ME, Keles C, Rabus MB, Yildirim O, Guler M, Balkanay M, Isik O, Yakut C. Surgical treatment of post-infarction left ventricular pseudoaneurysm: a two-decade experience. Tex Heart Inst J. 2007;34: Figueras J, Alcalde O, Barrabes JA, Serra V, Alguersuari J, Cortadellas J, Lidon RM. Changes in hospital mortality rates in 425 patients with acute ST-elevation myocardial infarction and cardiac rupture over a 30-year period. Circulation. 2008;118: Frances C, Romero A, Grady D. Left ventricular pseudoaneurysm. JAm Coll Cardiol. 1998;32: Sakai K, Nakamura K, Ishizuka N, Nakagawa M, Hosoda S. Echocardiographic findings and clinical features of left ventricular pseudoaneurysm after mitral valve replacement. Am Heart J. 1992;124: Atik FA, Navia JL, Vega PR, Gonzalez-Stawinski GV, Alster JM, Gillinov AM, Svensson LG, Pettersson BG, Lytle BW, Blackstone EH. Surgical treatment of postinfarction left ventricular pseudoaneurysm. Ann Thorac Surg. 2007;83: Clift P, Thorne S, de Giovanni J. Percutaneous device closure of a pseudoaneurysm of the left ventricular wall. Heart. 2004;90:e Jelnin V, Einhorn BN, Dudiy Y, Kronzon I, Cohen HA, Ruiz CE. Percutaneous trans-apical access and closure. J Am Coll Cardiol. In press. 12. Martinez CA, Rosen R, Cohen H, Ruiz CE. A novel method for closing the percutaneous transapical access tract using coils and gelatin matrix. J Invasive Cardiol. 2010;22:E107 E Komeda M, David TE. Surgical treatment of postinfarction false aneurysm of the left ventricle. J Thorac Cardiovasc Surg. 1993;106: Mackenzie JW, Lemole GM. Pseudoaneurysm of the left ventricle. Tex Heart Inst J. 1994;21: CLINICAL PERSPECTIVE Left ventricular pseudoaneurysm is a serious complication of cardiac surgery and of acute myocardial infarction. If left untreated, it may be complicated by rupture, bleeding, infection, and death. Until recently, the only effective method to repair pseudoaneurysms has been surgery. Using combined imaging modalities and transcatheter techniques, we were able to close left ventricular pseudoaneurysms percutaneously, by occluding its communication with the ventricular chamber, without major complications. This approach represents a potential alternative to surgical closure, especially in patients at excessive risk for cardiac surgery.
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis
 JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device
 273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
Hybrid Muscular VSD Closure in Small Weight Children
 Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Type Size AP/PS RP/RS Qp/Qs. Ia Resistive <0.3 < Ib Resistive <0.3 < IIa Resistive <0.5 >2
 Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Para-valvular Leak Closure
 Para-valvular Leak Closure Antonios Halapas, MD, PhD, FESC THV & Hygeia Hospital Heart Team Athens, Greece Disclosures I and the HYGEIA Hospital «Heart Team» have received research and travel grants from
Para-valvular Leak Closure Antonios Halapas, MD, PhD, FESC THV & Hygeia Hospital Heart Team Athens, Greece Disclosures I and the HYGEIA Hospital «Heart Team» have received research and travel grants from
Transcatheter Closure of Acute Myocardial Infarction VSD
 The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
We present the case of an asymptomatic, 75-year-old
 Images in Cardiovascular Medicine Asymptomatic Rupture of the Left Ventricle Lech Paluszkiewicz, MD; Stefan Ożegowski, MD; Mohammad Amin Parsa, MD; Jan Gummert, PhD, MD We present the case of an asymptomatic,
Images in Cardiovascular Medicine Asymptomatic Rupture of the Left Ventricle Lech Paluszkiewicz, MD; Stefan Ożegowski, MD; Mohammad Amin Parsa, MD; Jan Gummert, PhD, MD We present the case of an asymptomatic,
Transcatheter closure of patent foramen ovale using the internal jugular venous approach
 New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
Cite this article as:
 doi: 10.21037/acs.2018.09.05 Cite this article as: Cheung A. Early experience of TIARA transcatheter mitral valve replacement system.. doi: 10.21037/acs.2018.09.05 This is a PDF file of an edited manuscript
doi: 10.21037/acs.2018.09.05 Cite this article as: Cheung A. Early experience of TIARA transcatheter mitral valve replacement system.. doi: 10.21037/acs.2018.09.05 This is a PDF file of an edited manuscript
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE ECHOCARDIOGRAPHY IN INTERVENTIONAL CARDIOLOGY
 ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE Aristides G. Panlilio, MD, FPCP, FPCC,FPSE, FASE Philippine Heart Center Chinese General Hospital and Medical Center
ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE Aristides G. Panlilio, MD, FPCP, FPCC,FPSE, FASE Philippine Heart Center Chinese General Hospital and Medical Center
Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device
 Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
TCTAP C-217 Bilateral Pulmonary Arterio Venus Fistula Managed by Vascular Plugs and Coil Manotosh Panja 1 1 BelleVue Clinic, India
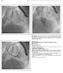 S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών Σ.Ράμμος
 ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
Percutaneous VSD closure
 Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
TEE Essential in Paravalvular Leak Closure and Pseudoaneurysm Repair. Gerard T Wilkins
 TEE Essential in Paravalvular Leak Closure and Pseudoaneurysm Repair. Gerard T Wilkins Assoc Prof Medicine Consultant Cardiologist Dunedin Hospital Structural Heart Disease: short history Rubio-Alvares
TEE Essential in Paravalvular Leak Closure and Pseudoaneurysm Repair. Gerard T Wilkins Assoc Prof Medicine Consultant Cardiologist Dunedin Hospital Structural Heart Disease: short history Rubio-Alvares
Cigna - Prior Authorization Procedure List Cardiology
 Cigna - Prior Authorization Procedure List Cardiology Category CPT Code CPT Code Description 33206 Insertion of new or replacement of permanent pacemaker with transvenous electrode(s); atrial 33207 Insertion
Cigna - Prior Authorization Procedure List Cardiology Category CPT Code CPT Code Description 33206 Insertion of new or replacement of permanent pacemaker with transvenous electrode(s); atrial 33207 Insertion
evicore cardiology procedures and services requiring prior authorization
 evicore cardiology procedures and services requiring prior authorization Moda Health Commercial Group and Individual Members* *Check EBT to verify member enrollment in evicore program Radiology Advanced
evicore cardiology procedures and services requiring prior authorization Moda Health Commercial Group and Individual Members* *Check EBT to verify member enrollment in evicore program Radiology Advanced
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE. Krishna Kumar SevenHills Hospital, Mumbai, India
 INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
Conflict of Interests
 Introduction to Interventional Echocardiography Roberto M Lang, MD Tomtec Conflict of Interests Research Grants Philips Medical Imaging Research Grants Speakers bureau Advisory bureau 1 Structural Heart
Introduction to Interventional Echocardiography Roberto M Lang, MD Tomtec Conflict of Interests Research Grants Philips Medical Imaging Research Grants Speakers bureau Advisory bureau 1 Structural Heart
Copyright 2017 American College of Emergency Physicians. All rights reserved.
 POLICY Approved April 2017 Guidelines for the Use of Transesophageal Echocardiography (TEE) in the ED for Cardiac Arrest Approved by the ACEP Board of Directors April 2017 1. Introduction The American
POLICY Approved April 2017 Guidelines for the Use of Transesophageal Echocardiography (TEE) in the ED for Cardiac Arrest Approved by the ACEP Board of Directors April 2017 1. Introduction The American
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
Originally Posted: November 15, 2014 BRUIT IN THE GROIN
 Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
The earliest application of intracardiac imaging
 Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
Perventricular Closure of Muscular VSD
 Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Percutaneous Transapical Access for Thoracic Endovascular Repair
 Percutaneous Transapical Access for Thoracic Endovascular Repair Atman P. Shah MD FACC FSCAI Co-Director, Hans Hecht Cardiac Catheterization Laboratory Clinical Director, Section of Cardiology Associate
Percutaneous Transapical Access for Thoracic Endovascular Repair Atman P. Shah MD FACC FSCAI Co-Director, Hans Hecht Cardiac Catheterization Laboratory Clinical Director, Section of Cardiology Associate
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter
 Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter Nirat Beohar, MD Associate Professor of Medicine Director Cardiac Catheterization Laboratory, Medical Director Structural
Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter Nirat Beohar, MD Associate Professor of Medicine Director Cardiac Catheterization Laboratory, Medical Director Structural
Diagnostic & Therapeutic Cardiac Catheterization Coder 2017
 Diagnostic & Therapeutic Cardiac Catheterization Coder 2017 Including peripheral and cardiovascular services and procedures Prepared and Published By: MedLearn Publishing A Division of Panacea Healthcare
Diagnostic & Therapeutic Cardiac Catheterization Coder 2017 Including peripheral and cardiovascular services and procedures Prepared and Published By: MedLearn Publishing A Division of Panacea Healthcare
Percutaneous Mitral Valve Repair
 Percutaneous Mitral Valve Repair MitraClip: Procedure, Data, Patient Selection Chad Rammohan, MD FACC Director, Cardiac Cath Lab El Camino Hospital Mountain View, California Mitral Regurgitation MitraClip
Percutaneous Mitral Valve Repair MitraClip: Procedure, Data, Patient Selection Chad Rammohan, MD FACC Director, Cardiac Cath Lab El Camino Hospital Mountain View, California Mitral Regurgitation MitraClip
Subacute left ventricular outflow tract obstruction after transapical closure of a mitral paravalvular leak in the region of the aortomitral curtain
 DOI: 10.1111/echo.13357 CASE REPORT Subacute left ventricular outflow tract obstruction after transapical closure of a mitral paravalvular leak in the region of the aortomitral curtain Sathish Chikkabyrappa
DOI: 10.1111/echo.13357 CASE REPORT Subacute left ventricular outflow tract obstruction after transapical closure of a mitral paravalvular leak in the region of the aortomitral curtain Sathish Chikkabyrappa
Congenital Absence of the Left Atrial Appendage Visualized by 3D Echocardiography in Two Adult Patients
 DOI: 10.1111/echo.12882 2015, Wiley Periodicals, Inc. Echocardiography CASE REPORT Congenital Absence of the Left Atrial Appendage Visualized by 3D Echocardiography in Two Adult Patients Mona Saleh, B.A.,*
DOI: 10.1111/echo.12882 2015, Wiley Periodicals, Inc. Echocardiography CASE REPORT Congenital Absence of the Left Atrial Appendage Visualized by 3D Echocardiography in Two Adult Patients Mona Saleh, B.A.,*
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
 Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
TAVR: Echo Measurements Pre, Post And Intra Procedure
 2017 ASE Florida, Orlando, FL October 10, 2017 8:00 8:25 AM 25 min TAVR: Echo Measurements Pre, Post And Intra Procedure Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
2017 ASE Florida, Orlando, FL October 10, 2017 8:00 8:25 AM 25 min TAVR: Echo Measurements Pre, Post And Intra Procedure Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
Peripheral and Cardiology Coder 2018
 Peripheral and Cardiology Coder 2018 Cardiovascular Services and Procedures Prepared and Published By: MedLearn Publishing A Division of MedLearn Media, Inc. 445 Minnesota Street, Suite 514 St. Paul, MN
Peripheral and Cardiology Coder 2018 Cardiovascular Services and Procedures Prepared and Published By: MedLearn Publishing A Division of MedLearn Media, Inc. 445 Minnesota Street, Suite 514 St. Paul, MN
Cardioband: una chance per l insufficienza mitralica funzionale
 HEARTLINE Genova 10-11 novembre 2017 Cardioband: una chance per l insufficienza mitralica funzionale Sergio Berti Ospedale del Cuore Fondazione C.N.R. Reg Toscana Massa/Pisa Reduction of Septo Lateral
HEARTLINE Genova 10-11 novembre 2017 Cardioband: una chance per l insufficienza mitralica funzionale Sergio Berti Ospedale del Cuore Fondazione C.N.R. Reg Toscana Massa/Pisa Reduction of Septo Lateral
Devices to Protect Against Stroke in Atrial Fibrillation
 Devices to Protect Against Stroke in Atrial Fibrillation Jonathan C. Hsu, MD, MAS Associate Clinical Professor Division of Cardiology, Section of Cardiac Electrophysiology June 2, 2018 Disclosures Honoraria
Devices to Protect Against Stroke in Atrial Fibrillation Jonathan C. Hsu, MD, MAS Associate Clinical Professor Division of Cardiology, Section of Cardiac Electrophysiology June 2, 2018 Disclosures Honoraria
Organic mitral regurgitation
 The best in heart valve disease Organic mitral regurgitation Ewa Szymczyk Department of Cardiology Medical University of Lodz, Poland I have nothing to declare Organic mitral regurgitation leaflet abnormality
The best in heart valve disease Organic mitral regurgitation Ewa Szymczyk Department of Cardiology Medical University of Lodz, Poland I have nothing to declare Organic mitral regurgitation leaflet abnormality
Percutaneous Intervention for totally Occluded Coarctation Of Aorta. John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology
 Percutaneous Intervention for totally Occluded Coarctation Of Aorta John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology Background Coarctation of aorta (CoA) forms 5-7% of congenital heart diseases
Percutaneous Intervention for totally Occluded Coarctation Of Aorta John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology Background Coarctation of aorta (CoA) forms 5-7% of congenital heart diseases
CIPG Transcatheter Aortic Valve Replacement- When Is Less, More?
 CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
Professor and Chief, Division of Cardiac Surgery Chief Medical Officer, Harpoon Medical. The Houston Aortic Symposium February 23-25, 2017
 James S. Gammie, MD Professor and Chief, Division of Cardiac Surgery Chief Medical Officer, Harpoon Medical The Houston Aortic Symposium February 2-25, 2017 Disclosure Statement of Financial Interest Within
James S. Gammie, MD Professor and Chief, Division of Cardiac Surgery Chief Medical Officer, Harpoon Medical The Houston Aortic Symposium February 2-25, 2017 Disclosure Statement of Financial Interest Within
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Para-valvular Leak Closure
 Para-valvular Leak Closure Antonios Chalapas, MD, PhD, FESC THV & Hygeia Hospital Heart Team Athens, Greece HYGEIA Hospital Heart Team Cardiologists: M Chrissoheris, Κ Papadopoulos, A Tzifa, A Chalapas,
Para-valvular Leak Closure Antonios Chalapas, MD, PhD, FESC THV & Hygeia Hospital Heart Team Athens, Greece HYGEIA Hospital Heart Team Cardiologists: M Chrissoheris, Κ Papadopoulos, A Tzifa, A Chalapas,
Atrial Septal Defect Closure. Stephen Brecker Director, Cardiac Catheterisation Labs
 Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Fabien Praz, Andreas Wahl, Sophie Beney, Stephan Windecker, Heinrich P. Mattle*, Bernhard Meier
 Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
2D/3D in Evaluation of Atrial Septum
 2D/3D in Evaluation of Atrial Septum Roberto M Lang, MD OSTIUM SECUNDUM ASD: 2D AND 3D TNSESOPHAGEAL ECHO 1 Biplane views 90 0 3D Acquisi on Acquire 3D volume Lang RM et al. JASE 2012;25:3 46. Right atrial
2D/3D in Evaluation of Atrial Septum Roberto M Lang, MD OSTIUM SECUNDUM ASD: 2D AND 3D TNSESOPHAGEAL ECHO 1 Biplane views 90 0 3D Acquisi on Acquire 3D volume Lang RM et al. JASE 2012;25:3 46. Right atrial
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
5 th Asia Pacific Congenital and Structural Heart (APCASH) Intervention Symposium 2014
 5 th Asia Pacific Congenital and Structural Heart (APCASH) Intervention Symposium 2014 Allied Health Session What You Need to Know for Complication Management in Structural Heart Intervention (From Instrument
5 th Asia Pacific Congenital and Structural Heart (APCASH) Intervention Symposium 2014 Allied Health Session What You Need to Know for Complication Management in Structural Heart Intervention (From Instrument
Paravalvular leak (PVL) is a rare but important
 Paravalvular Leak losure: The pical pproach Imaging and procedural considerations for PVL closure via surgical and percutaneous transapical approaches. y Sonnit Sharma, M, S; had Kliger, M; Vladimir Jelnin,
Paravalvular Leak losure: The pical pproach Imaging and procedural considerations for PVL closure via surgical and percutaneous transapical approaches. y Sonnit Sharma, M, S; had Kliger, M; Vladimir Jelnin,
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ
 ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
Percutaneous mitral valve repair/replacement. Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein
 Percutaneous mitral valve repair/replacement Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein Mitral Valve anatomy Difference between AoV and MV Aortic Valve Mitral Valve Transcatheter Mitral
Percutaneous mitral valve repair/replacement Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein Mitral Valve anatomy Difference between AoV and MV Aortic Valve Mitral Valve Transcatheter Mitral
Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid Annuloplasty
 Case Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid nnuloplasty
Case Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid nnuloplasty
Results of Transapical Valves. A.P. Kappetein Dept Cardio-thoracic surgery
 Results of Transapical Valves A.P. Kappetein Dept Cardio-thoracic surgery Rotterda am, The Netherlands 2002 FIM 2003 2005 2006 2010 THV THV Cribier-Edwards Edwards Edwards Sapien Sapien XT Bovine pericardium
Results of Transapical Valves A.P. Kappetein Dept Cardio-thoracic surgery Rotterda am, The Netherlands 2002 FIM 2003 2005 2006 2010 THV THV Cribier-Edwards Edwards Edwards Sapien Sapien XT Bovine pericardium
Bioprosthetic Mitral Valve Dysfunction: Innovation and Evolution of a New Therapeutic Technique
 Bioprosthetic Mitral Valve Dysfunction: Innovation and Evolution of a New Therapeutic Technique Charanjit S. Rihal MD MBA Professor and Chair Division of Cardiovascular Diseases Mayo Clinic DISCLOSURES
Bioprosthetic Mitral Valve Dysfunction: Innovation and Evolution of a New Therapeutic Technique Charanjit S. Rihal MD MBA Professor and Chair Division of Cardiovascular Diseases Mayo Clinic DISCLOSURES
2. Case Report. 1. Introduction
 Case Reports in Cardiology Volume 2016, Article ID 3251032, 5 pages http://dx.doi.org/10.1155/2016/3251032 Case Report Ventricular Septal Perforation after Biventricular Takotsubo Cardiomyopathy Successfully
Case Reports in Cardiology Volume 2016, Article ID 3251032, 5 pages http://dx.doi.org/10.1155/2016/3251032 Case Report Ventricular Septal Perforation after Biventricular Takotsubo Cardiomyopathy Successfully
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children
 Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Transcatheter Aortic Valve Implantation Management of risks and complications
 Transcatheter Aortic Valve Implantation Management of risks and complications TAVI Summit, Seoul, Korea, Spetember 3rd, 2011 Alain Cribier University of Rouen, France Complications of TAVI Depending on
Transcatheter Aortic Valve Implantation Management of risks and complications TAVI Summit, Seoul, Korea, Spetember 3rd, 2011 Alain Cribier University of Rouen, France Complications of TAVI Depending on
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor. Cardiothoracic Radiology
 New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION. Original Date: October 2015 Page 1 of 5
 National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION CPT Codes: 93451, 93452, 93453, 93454, 93455, 93456, 93457, 93458, 93459, 93460, 93461 LCD ID Number:
National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION CPT Codes: 93451, 93452, 93453, 93454, 93455, 93456, 93457, 93458, 93459, 93460, 93461 LCD ID Number:
When Does 3D Echo Make A Difference?
 When Does 3D Echo Make A Difference? Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network 1 Practical Applications of 3D Echocardiography Recommended
When Does 3D Echo Make A Difference? Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network 1 Practical Applications of 3D Echocardiography Recommended
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome
 A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
Mitral Regurgitation
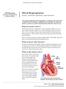 UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm
 CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
Cardiac ultrasound protocols
 Cardiac ultrasound protocols IDEXX Telemedicine Consultants Two-dimensional and M-mode imaging planes Right parasternal long axis four chamber Obtained from the right side Displays the relative proportions
Cardiac ultrasound protocols IDEXX Telemedicine Consultants Two-dimensional and M-mode imaging planes Right parasternal long axis four chamber Obtained from the right side Displays the relative proportions
Edwards Sapien. Medtronic CoreValve. Inoperable FDA approved High risk: in trials. FDA approved
 Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Imaging Evaluation of the Ventricular Septum
 Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Rotation: Echocardiography: Transthoracic Echocardiography (TTE)
 Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Transcatheter closure of right coronary artery fistula to the right ventricle
 Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments
 CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency
 Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency Rahul R. Jhaveri, MD, Muhamed Saric, MD, PhD, FASE, and Itzhak Kronzon, MD, FASE, New York, New York Background: Two-dimensional
Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency Rahul R. Jhaveri, MD, Muhamed Saric, MD, PhD, FASE, and Itzhak Kronzon, MD, FASE, New York, New York Background: Two-dimensional
Jian Fang 1, Shaobo Xie 2, Lunchao Ma 2, Chao Yang 2. Original Article
 Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure
 Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Occlusion de l'auricule gauche: Niche ou réel avenir? D Gras, MD, Nantes, France
 Occlusion de l'auricule gauche: Niche ou réel avenir? D Gras, MD, Nantes, France LAA Occlusion Is there a real future? Background Protect AF Trial Other Studies CAP, ASAP, Prevail Left Atrial Appendage
Occlusion de l'auricule gauche: Niche ou réel avenir? D Gras, MD, Nantes, France LAA Occlusion Is there a real future? Background Protect AF Trial Other Studies CAP, ASAP, Prevail Left Atrial Appendage
Image Assistance in TAVI Why CT? Won-Jang Kim, MD, PhD Clinical Assistant Professor of Medicine, Heart Institute, Asan Medical Center, Seoul, Korea
 Image Assistance in TAVI Why CT? Won-Jang Kim, MD, PhD Clinical Assistant Professor of Medicine, Heart Institute, Asan Medical Center, Seoul, Korea Major Uses of CT in TAVI Ileofemoral Patient Arterial
Image Assistance in TAVI Why CT? Won-Jang Kim, MD, PhD Clinical Assistant Professor of Medicine, Heart Institute, Asan Medical Center, Seoul, Korea Major Uses of CT in TAVI Ileofemoral Patient Arterial
Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504
 Transcatheter valve-in-valve e implantation for aortic bioprosthetic valve dysfunction Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504 Your responsibility This
Transcatheter valve-in-valve e implantation for aortic bioprosthetic valve dysfunction Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504 Your responsibility This
Cardiac Masses. Cardiac Masses: Considerations. Dennis A. Tighe, MD, FASE. University of Massachusetts Medical School Worcester, MA 4/16/2018
 Cardiac Masses Dennis A. Tighe, MD, FASE University of Massachusetts Medical School Worcester, MA Cardiac Masses: Considerations Definition of the mass Nature Location Benign or malignant Presentation
Cardiac Masses Dennis A. Tighe, MD, FASE University of Massachusetts Medical School Worcester, MA Cardiac Masses: Considerations Definition of the mass Nature Location Benign or malignant Presentation
Atrial fibrillation (AF), one of the
 Hellenic J Cardiol 2013; 54: 408-412 Case Report Left Atrial Appendage Occlusion with the Amplatzer Amulet for Stroke Prevention in Atrial Fibrillation: The First Case in Greece Apostolos Tzikas, Lambros
Hellenic J Cardiol 2013; 54: 408-412 Case Report Left Atrial Appendage Occlusion with the Amplatzer Amulet for Stroke Prevention in Atrial Fibrillation: The First Case in Greece Apostolos Tzikas, Lambros
2/14/2018 CASE STUDIES: COMPLICATIONS OF MYOCARDIAL INFARCTION. Judy Hung, MD Cardiology Division Massachusetts General Hospital Boston, MA CASE 1
 CASE STUDIES: COMPLICATIONS OF MYOCARDIAL INFARCTION Judy Hung, MD Cardiology Division Massachusetts General Hospital Boston, MA CASE 1 1 PRESENTATION 57 yo male with a past medical history of hypertension
CASE STUDIES: COMPLICATIONS OF MYOCARDIAL INFARCTION Judy Hung, MD Cardiology Division Massachusetts General Hospital Boston, MA CASE 1 1 PRESENTATION 57 yo male with a past medical history of hypertension
Radiology of the respiratory/cardiac diseases (part 2)
 Cardiology Cycle - Lecture 6 436 Teams Radiology of the respiratory/cardiac diseases (part 2) Objectives Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Leena Alwakeel Aroob Alhuthail
Cardiology Cycle - Lecture 6 436 Teams Radiology of the respiratory/cardiac diseases (part 2) Objectives Done By Team Leaders: Khalid Alshehri Hanin Bashaikh Team Members: Leena Alwakeel Aroob Alhuthail
2/28/2010. Speakers s name: Paul Chiam. I have the following potential conflicts of interest to report: NONE. Antegrade transvenous transseptal route
 Transcatheter Aortic Valve Implantation Asian perspective Speakers s name: Paul Chiam Paul TL Chiam MBBS, MRCP, FACC I have the following potential conflicts of interest to report: NONE Consultant National
Transcatheter Aortic Valve Implantation Asian perspective Speakers s name: Paul Chiam Paul TL Chiam MBBS, MRCP, FACC I have the following potential conflicts of interest to report: NONE Consultant National
Atrial Septal Defects
 Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
The Role of Imaging in Transcatheter Aortic Valve Implantation
 The Role of Imaging in Transcatheter Aortic Valve Implantation Helmut Baumgartner Westfälische Wilhelms-Universität Münster Division of Adult Congenital and Valvular Heart Disease Department of Cardiovascular
The Role of Imaging in Transcatheter Aortic Valve Implantation Helmut Baumgartner Westfälische Wilhelms-Universität Münster Division of Adult Congenital and Valvular Heart Disease Department of Cardiovascular
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CY2015 Hospital Outpatient: Endovascular Procedure APCs and Complexity Adjustments
 CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
My Choice For Percutaneous Mitral Valve Replacement. Jose Luis Navia, MD.
 My Choice For Percutaneous Mitral Valve Replacement Jose Luis Navia, MD. Disclosure Edwards Lifescienses St. Jude Medical MAQUET NaviGate Consultant, Investigator Consultant, Investigator Consultant, Investigator
My Choice For Percutaneous Mitral Valve Replacement Jose Luis Navia, MD. Disclosure Edwards Lifescienses St. Jude Medical MAQUET NaviGate Consultant, Investigator Consultant, Investigator Consultant, Investigator
Interventional procedures guidance Published: 26 July 2017 nice.org.uk/guidance/ipg586
 Transcatheter aortic valve implantation for aortic stenosis Interventional procedures guidance Published: 26 July 17 nice.org.uk/guidance/ipg586 Your responsibility This guidance represents the view of
Transcatheter aortic valve implantation for aortic stenosis Interventional procedures guidance Published: 26 July 17 nice.org.uk/guidance/ipg586 Your responsibility This guidance represents the view of
First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not Always
 ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
Portico (St. Jude Medical Inc, St.
 Review Article Portico Transcatheter Heart Valve Apostolos Tzikas 1,2, Michael Chrissoheris 2, Antonios Halapas 2, Konstantinos Spargias 2 1 Interbalkan European Medical Centre, Thessaloniki, 2 Hygeia
Review Article Portico Transcatheter Heart Valve Apostolos Tzikas 1,2, Michael Chrissoheris 2, Antonios Halapas 2, Konstantinos Spargias 2 1 Interbalkan European Medical Centre, Thessaloniki, 2 Hygeia
Prior Authorization for Non-emergency Cardiac Imaging Procedures
 Attention: All Providers Prior Authorization for Non-emergency Cardiac Imaging Procedures The N.C. Medicaid Program is considering implementation of a prior authorization (PA) program for non-emergency
Attention: All Providers Prior Authorization for Non-emergency Cardiac Imaging Procedures The N.C. Medicaid Program is considering implementation of a prior authorization (PA) program for non-emergency
Left atrial appendage (LAA) closure is now a commercially
 Assessing Anatomy for Left Atrial Appendage Closure The roles of TEE and CTA in anatomic assessment and device selection for LAA closure. BY DEE DEE WANG, MD, AND MARVIN H. ENG, MD Left atrial appendage
Assessing Anatomy for Left Atrial Appendage Closure The roles of TEE and CTA in anatomic assessment and device selection for LAA closure. BY DEE DEE WANG, MD, AND MARVIN H. ENG, MD Left atrial appendage
Real-Time Three-Dimensional Transesophageal Echocardiography in Transcutaneous, Catheter-Based Procedures for Repair of Structural Heart Diseases
 Real-Time Three-Dimensional Transesophageal Echocardiography in Transcutaneous, Catheter-Based Procedures for Repair of Structural Heart Diseases Gila Perk, MD, Carlos Ruiz, MD, PhD, Muhamed Saric, MD,
Real-Time Three-Dimensional Transesophageal Echocardiography in Transcutaneous, Catheter-Based Procedures for Repair of Structural Heart Diseases Gila Perk, MD, Carlos Ruiz, MD, PhD, Muhamed Saric, MD,
Complicated Percutaneous Repair of a Paravalvular Mitral Leak. Dr. K Kam Resident Specialist Division of Cardiology, PWH M&T (Courtesy: Prof.
 Complicated Percutaneous Repair of a Paravalvular Mitral Leak Dr. K Kam Resident Specialist Division of Cardiology, PWH M&T (Courtesy: Prof. PW Lee) A new job for echo guy Interventional echocardiologist!
Complicated Percutaneous Repair of a Paravalvular Mitral Leak Dr. K Kam Resident Specialist Division of Cardiology, PWH M&T (Courtesy: Prof. PW Lee) A new job for echo guy Interventional echocardiologist!
Percutaneous Therapy for Calcific Mitral Valve Disease
 31 st Annual State of the Art Echocardiography San Diego, CA February 18, 2018 5:00 5:15 PM 15 min Percutaneous Therapy for Calcific Mitral Valve Disease Muhamed Sarić MD, PhD, MPA Director of Noninvasive
31 st Annual State of the Art Echocardiography San Diego, CA February 18, 2018 5:00 5:15 PM 15 min Percutaneous Therapy for Calcific Mitral Valve Disease Muhamed Sarić MD, PhD, MPA Director of Noninvasive
Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM
 The Patient with Aortic Stenosis and Mitral Regurgitation Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM Aortic Stenosis + Mitral Regurgitation?
The Patient with Aortic Stenosis and Mitral Regurgitation Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM Aortic Stenosis + Mitral Regurgitation?
AMPLATZER Septal Occluder
 AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
