Understanding Learning is the first step to getting help.
|
|
|
- Joshua George
- 5 years ago
- Views:
Transcription
1 Understanding Inflammatory Bowel Disease (IBD) Learning is the first step to getting help. This booklet has been created through an educational grant provided by Fulford India Ltd., A subsidiary of Schering-Plough Corporation. Issued in the public interest by: I can work from 9 to 5 again Colitis and Crohn s Foundation, 6-E, Tagore Nagar, Ludhiana , Punjab, India. ccfi2007@gmail.com Inflammatory Bowel Disease (IBD) Ulcerative colitis (UC) Crohn s disease (CD) Back Cover
2 INFLAMMATORY BOWEL DISEASE (IBD) is a group of inflammatory conditions of the large intestine and, in some cases, the small intestine. It should not be confused with irritable bowel syndrome. The main forms of IBD are Crohn's disease (CD) and ulcerative colitis (UC). Inside Cover 1
3 ULCERATIVE COLITIS ULCERATIVE COLITIS Learning about UC gave me the head start I needed in my recovery. Know the facts Ulcerative Colitis (UC), an inflammatory bowel disease, can have serious effects on every aspect of your life. The first step to controlling your disease is gaining knowledge. Take the time to read this brochure so that you can have an informed discussion with your doctor. By educating yourself about UC, you can work with your doctor to make sure you're doing all you can to help manage your disease, and live the life you want. WHAT IS ULCERATIVE COLITIS? Ulcerative colitis (UC) is a disease that causes inflammation and sores, called ulcers, in the top layer of the lining of the large intestine. The inflammation usually occurs in the rectum and the lower part of the colon, but it may affect the entire colon. Ulcerative colitis does not affect the small intestine except for the lower section, called ileum. WHAT CAUSES ULCERATIVE COLITIS? The development of ulcerative colitis appears to be influenced by two factors: genetic susceptibility and environmental triggers. These two factors eventually cause the immune system to damage the lining of the colon. Genetics Ulcerative colitis tends to run in families, suggesting that genetics have a role in the disease. About 10 to 25 percent of affected people have a first-degree relative (either a sibling or parent) with either ulcerative colitis or Crohn's disease. Environment Several environmental factors, such as infections, are suspected of triggering UC in people who have a genetic susceptibility. It is not caused by emotional distress or sensitivity to certain foods or food products but these factors may trigger symptoms in some people. However, no single factor has been consistently proven to be the main trigger. COMMON VOCABULARY Doctors often use specific terms to reflect the extent of the colonic involvement. The extent of involvement is often related to the severity of symptoms and the course of the disease over time. Furthermore, treatments vary depending upon which parts of the colon are involved. Ulcerative proctitis refers to disease limited to the rectum. Distal colitis or proctosigmoiditis is used when the inflammatory process extends up to the sigmoid colon. Left sided colitis refers to the disease extending to but not beyond the splenic flexure (the sharp bend in the large intestine where the transverse colon joins the descending colon, located under the spleen). Pancolitis is used when the inflammatory process extends beyond the transverse colon. The symptoms of ulcerative colitis can be mild, moderate or severe and can fluctuate over time. Doctors use the term flare to describe the periods in which the disease becomes more active.the term remission is used to describe periods of quiescence or inactivity. 2 3
4 Everyone has different symptoms; it's vital to identify yours. I always talk to my doctor, since he understands my needs and condition. Colonic Pseudopolyps WHAT ARE THE SYMPTOMS OF ULCERATIVE COLITIS? Ulcerative colitis occurs most often in people aged between 15 and 40 years, although children and older people can also develop the disease. Ulcerative colitis affects men and women equally. The most common symptoms of ulcerative colitis are abdominal pain and bloody diarrhoea. Patients also may experience any of the following: Fatigue Weight loss Loss of appetite Rectal bleeding Loss of body fluids and nutrients About half the patients have mild symptoms. Others suffer from frequent fever, bloody diarrhoea, nausea, and severe abdominal cramps. Ulcerative colitis may also cause problems such as arthritis, inflammation of the eye, liver disease (fatty liver, hepatitis, cirrhosis, and primary sclerosing cholangitis), osteoporosis, skin rashes, anemia, and kidney stones. No one knows for sure why problems occur outside the colon. Scientists think that these complications may occur when the immune system triggers inflammation in other part of the body. These problems are usually mild and go away when the colitis is treated. HOW IS THE DIAGNOSIS OF UC MADE? Ulcerative colitis is usually diagnosed based on signs and symptoms noted during a thorough medical history and physical examination, along with the results of certain diagnostic tests, including blood and stool tests, a sigmoidoscopy (where the doctor passes a flexible instrument into the rectum and lower colon) or colonoscopy (a similar procedure, which gives the doctor a visualization of the entire colon) and histology. These steps are also helpful for ruling out other causes of colitis, including Crohn's disease, and certain infections. Blood tests are performed to check for anaemia (a low haemoglobin level) and to give an idea of your overall profile. Stool tests are used to eliminate infectious causes of diarrhoea. WHEN SHOULD I TALK TO MY DOCTOR? Whether or not you have been diagnosed with UC, you should consult a doctor if you experience any of its symptoms, including those listed below: Severe abdominal pain Blood in your bowel movements Ongoing diarrhoea Endoscopy image Unexplained fever that lasts longer than a couple of days 4 5
5 Severe haemorrhage Perforation Extensive inflammation can lead to a tear in the intestinal wall, resulting in leakage of bowel contents outside the intestine. Categorized by sudden, severe abdominal pain, shock, and excessive abdominal tenderness, this condition usually requires emergency surgery. superficial ulceration and loss of mucosal architecture Toxic megacolon This serious complication may occur when inflammation spreads from the lining of the colon to involve the entire intestinal wall. Because this involvement temporarily stops the normal contractile movements of the intestine, the large intestine may greatly expand. The person is usually severely ill with fever, abdominal pain and distension. Immediate and aggressive measures are required to minimize the risk of death. IS COLON CANCER A COMMON CONCERN? HOW IMPORTANT IS AN EARLY DIAGNOSIS? An early diagnosis is the first step in beginning treatment. This is particularly important with chronic conditions like UC, which can progress over time. Dealing with any health problem can be emotionally and physically stressful, but the sooner you receive a proper diagnosis, the better chance you will have to control your symptoms and minimize your discomfort. In the meantime, be patient. An accurate diagnosis may take some time. You should also take the time to educate yourself. Even though your doctor has the clinical expertise needed to make a diagnosis, your involvement is important in understanding what may be happening in your body and what you can do to promote your own good health. WHAT ARE THE COMPLICATIONS OF UC? Complications are less likely to occur in appropriately treated patients. Longstanding and/or severe ulcerative colitis can be associated with serious and sometimes life-threatening complications. T h e s e i n c l u d e s e v e r e h a e m o r r h a g e, t o x i c megacolon, perforation and colorectal cancer. Radiography images Colorectal cancer usually arises from premalignant changes (dysplasia) of the colonic lining which can be detected by regular screening. Although some of these changes do not progress to cancer, there is currently no way of knowing which changes will take a more serious course. Because of the risk of developing cancer, surveillance for cancer is recommended. Surveillance entails a colonoscopy at specified time intervals. This procedure can often detect premalignant changes and early colorectal cancer, and studies suggest that those detected early during surveillance should undergo a colectomy. WHAT ARE THE EXTRAINTESTINAL MANIFESTATIONS OF UC? UC may be associated with a number of complications outside the intestine. These include: Inflammation of the eye, which can cause redness and pain and, rarely, lead to vision loss. Skin disorders, where painful nodules or deep ulcers may develop on the skin. Arthritis, which may involve the large joints (e.g., knee), or the spine. Spinal involvement may include a disease called ankylosing spondylitis, which is an important cause of disability. Increased risk for certain liver disorders, such as scarring of the bile ducts, which can lead to liver failure and liver transplantation. 6 7
6 Choosing the right therapy for you is essential WHAT IS THE TREATMENT FOR ULCERATIVE COLITIS? Treatment of UC is tailored to the region of the colon that is involved, the severity of the inflammation and symptoms, and individual factors. For most patients, ulcerative colitis is characterized by a frustrating pattern of flares and remissions. As a result, the two main goals of treatment are to achieve and maintain remission. This usually requires long term medications. The most common drugs used to treat UC include aminosalicylates and immunosuppressive drugs. All drugs can cause side-effects; however, it is important to remember that many people take these drugs without developing serious sideeffects, and that these drugs are used only when their benefit outweighs the potential risks. Steroids are used in acute cases and should be tapered off gradually. Continuous use of steroids is associated with many side effects. Although drugs and medical therapy are central in the treatment of ulcerative colitis, surgery also has an important role in relieving symptoms, addressing serious complications, and improving quality of life. It can even be lifesaving. Specific circumstances that may require surgery include: the persistence of symptoms despite high doses of steroids; dependency upon steroids to maintain remission; worsening or new complications despite maximal drug therapy; the occurrence of serious side effects of drugs; and occurrence of premalignant or malignant changes in the colon. The most common surgery is a proctocolectomy with ileostomy i.e. removal of the colon along with the rectum, which is followed by ileal pouch anal anastamosis (IPAA). WHAT ARE THE VARIOUS DRUGS USED IN UC? Aminosalicylates (5-ASA agents). Drugs such as sulfasalazine, mesalamine and balsalazide are used to reduce the inflammation of UC and to prevent flare-ups. These drugs are usually taken orally, although they may also be given rectally as enemas. They are usually well-tolerated, but possible side effects of mesalamine preparations include nausea, vomiting, heartburn, diarrhoea, and headache. These drugs are effective in treating mild to moderate UC, and are also useful in preventing disease relapse. Immunomodulators. Drugs such as azathioprine and 6-MP have been used to maintain remission and decrease the need for steroids. However, this class of drugs may take up to 2-4 months to produce their maximal effect. You may experience side effects such as nausea, vomiting, and diarrhoea, as well as low white blood count, liver problems, pancreatitis and reduced resistance to infection. If you take these drugs you may need to have your blood count monitored on a regular basis. Cyclosporine has been given to some people who are suffering from severe flare-ups and have not responded to corticosteroid therapy. Steroids. Corticosteroids are usually given to patients with moderate to severe disease. Prednisolone is often used to control the inflammation of UC, followed by sulfasalazine or mesalamine to maintain remission. Because of the many side effects that may occur with steroid treatment, your doctor will try to wean you off this therapy as quickly as possible. Antidiarrhoeal medications. Antidiarrhoeal agents may be prescribed by your doctor. In severe cases, your doctor will closely monitor you if you are taking these drugs to avoid triggering toxic megacolon. If you are dehydrated because of diarrhoea, you will be treated with fluids and electrolytes. Biologicals. Biologicals are the latest form of therapy being used to treat ulcerative colitis. These treatments work by targeting an underlying cause of inflammation that leads to the painful and unpredictable symptoms characteristic of ulcerative colitis. 8 9
7 intestine, called the ileum, to it. The stoma is about the size of a coin and is covered by a pouch. Waste travels through the small intestine and exits the body through the stoma and into the pouch. The patient empties the pouch as needed. Ileoanal anastomosis This is a fairly new procedure that allows the patient to have bowel movements via the normal route because the small intestine is connected to the anus. The colon is still removed but the doctor creates an internal pouch from the small bowel and attaches it to the anus. Waste is stored in the pouch and passed through the anus in the usual manner. Complications of surgery As with any surgical procedure, complications may arise. Common long-term complications include: Small bowel obstruction A blockage in the small bowel can cause nausea, vomiting, cramps and abdominal pain. Approximately one-third of those who experience this complication require surgery to release the bowel from the source of obstruction. The obstruction is usually caused by scar tissue that forms in the abdominal cavity after surgery, called an adhesion. WHAT IS THE ROLE OF SURGERY? Surgery may be required to provide relief for patients who have not responded to medical treatment or whose health has been threatened by bleeding, severe illness, rupture of the colon or other complications of treatment. In addition, surgery is required when colon cancer or dysplasia, a condition that precedes it, develops. Removing the colon is called a colectomy and may be performed in 25-40% of patients. Pouchitis At least 30% of people who have received the ileoanal pouch develop inflammation, called pouchitis. The symptoms of pouchitis include frequent bowel movements and/or diarrhoea. These symptoms can be mild or severe, acute or chronic. Some patients require long-term antibiotics to manage this condition. Pouch failure Approximately 8-10% of patients develop pouch failure. Unlike pouchitis, failure requires that the pouch be removed and necessitates a switch to a permanent ileostomy. Two common surgical procedures are. Ileostomy During this procedure, the surgeon creates a small opening in the abdomen, called a stoma, and attaches the end of the small 10 11
8 You may want to consider creating a file on your computer with all this information. You can print it out and give it to your doctor on the first visit and then update it for future visits. Subsequent visits In addition to the information listed above, you can help your doctor assess how well your treatment is working by letting him or her know the following: How your symptoms have changed or improved How you feel after taking your medication What concerns you may have about the medications you are taking How your symptoms are affecting your quality of life. Remember, communication is the key to getting the best possible treatment. TALKING ABOUT UC WITH YOUR DOCTOR Let's face it, there are some aspects of UC that are embarrassing to talk about. But it is important for you to be able to discuss your illness. UC is a chronic disease and the people around you need to know what is happening to you and how they can help. It is important that you take an active role in the treatment of your UC. You must be able to talk to your doctor about your symptoms and how they are affecting your life. The first visit If you are visiting a doctor for the first time, you may want to make sure that all your medical records have been transferred. Also, you may want to consider writing down some points to discuss and questions to ask. Include the following: A description of your symptoms Foods that you think aggravate your symptoms Any other medical conditions you may have A list of all medications, vitamins, and herbal remedies you may be taking Any concerns you have about the medications you are taking Any drug allergies Any questions or concerns you may have 12 13
9 Having the support of my friends and family really helps TALKING ABOUT UC WITH FAMILY AND FRIENDS People living with a chronic illness need the support of family and friends. That's why it is important that you talk to them about UC, and how it's affecting your life. Many people don't know what UC is, and may have misconceptions about what causes it or how it is treated. Sometimes, it's hard to remember that UC can affect the people around you. For instance, a flare-up may interrupt travel or holiday plans. Encouraging those close to you to express their feelings can help alleviate misunderstandings or feelings of disappointment. Talk openly Educating your family and friends allows them to be active members of your support team. By being honest about your feelings and what you are going through, you can help family members and friends know that their support is needed and appreciated. Consider therapy UC can cause stress for the entire family. Individual or family counselling may help you talk through issues your family is facing and help you get through a particularly rough period. Discuss financial issues If you are unable to work or can't work full time, discuss financial issues together as a family and come to a mutually agreeable solution. By addressing these issues early, you and your family will be prepared if a problem arises. TALKING ABOUT UC WITH YOUR CO-WORKERS UC may make work challenging. Many people try to conceal their illness from their employer and co-workers. You know your work environment best. If you are comfortable speaking to your supervisor about your disease, initiate a conversation. Chances are, your supervisor will be glad you did. Be honest. It may be embarrassing to discuss your symptoms with your employer. But if your employer understands what you are experiencing, he or she may be able to accommodate you so you can continue to perform well at your job. Ask for what you need. Sometimes it may be something minor, such as sitting closer to the bathroom. Or you may want to avoid lunch meetings or travelling. Or maybe you want to telecommute when you are experiencing a flare-up. Don't be afraid to ask for what you need. Discuss flare-ups. You may need to leave work early or take time off during a flareup. Talk to your employer ahead of time about how your work will be handled, and if the time off will be paid or unpaid. Know your rights. Discrimination against any employee on the basis of illness is illegal. But unfortunately it does happen so you should familiarize yourself with your rights. WHERE TO GET MORE INFORMATION Your doctor is the best resource for finding out important information related to your particular case. Not all patients with ulcerative colitis are alike, and it is important that your situation is evaluated by someone who knows you as a whole person
10 CROHN'S DISEASE Crohn's disease WHAT IS CROHN S DISEASE? Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI tract, from the mouth to the anus, but it most commonly affects the lower part of the small intestine, called the ileum. The swelling extends deep into the lining of the affected organ. The swelling can cause pain and can make the intestines empty frequently, resulting in diarrhea. While ulcerative colitis causes inflammation Esophagus Small Intestine Ileum (Lower part of small intestine) Appendix Stomach Large Intestine (Cloon) Rectum and ulcers in the top layer of the large intestine lining, in Crohn s disease, all layers of the intestine may be involved, and normal healthy bowel can be found between sections of diseased bowel. What causes Crohn s disease? The cause of Crohn's is unknown. However, research suggests that Crohn's may result from an interaction among genetics, the immune system, and something in the environment. Crohn's disease most often appears when people are between the ages of 15 and 35, although children and the elderly may also be affected. Anus Who is at risk? Crohn s disease affects men and women equally and seems to run in some families. About 20 percent of people with Crohn s disease have a blood relative with some form of inflammatory bowel disease, most often a brother or sister and sometimes a parent or child. Crohn s disease can occur in people of all age groups, but it is more often diagnosed in people between the ages of 20 and 30. What are the symptoms of Crohn s disease? The most common initial symptoms of Crohn's disease include abdominal pain, cramping, and diarrhea. These symptoms show up primarily after meals, and pain is usually centered at or below the navel, often in the lower right part of the abdomen. Other symptoms of Crohn s include Loss of appetite Rectal bleeding Weight loss Conditions with similar symptoms Fever Joint pain Fatigue Sores around the anal area Some people may also develop fistulizing Crohn's, in which the intestinal wall develops fistulas or tunnels that connect the intestine to adjacent areas, including the skin, bladder, vagina, intestine, and perianal areas. Sometimes other conditions can cause abdominal symptoms that appear to be similar to those of Crohn s. These conditions include: Intestinal tuberculosis Ulcerative colitis Irritable bowel syndrome Appendicitis Diverticulitis Peptic ulcer disease
11 HOW IS CROHN S DISEASE DIAGNOSED? An accurate professional diagnosis is the first step in treating Crohn s. Proper diagnosis is particularly important with a condition like Crohn's, because its symptoms may mimic those of other conditions and its effects are chronic, progressing over time. Diagnostic tests To confirm his or her diagnosis and to rule out other conditions that can cause similar symptoms, such as other inflammatory bowel diseases, colitis, celiac disease, or irritable bowel syndrome your physician will probably perform a complete physical examination and order medical tests. These diagnostic tests may include: Blood tests Although a complete blood count cannot provide a positive diagnosis of Crohn's, physicians usually order the test in suspected cases because it may reveal intestinal bleeding, an infection, or an inflammatory condition. Radiologic examinations These exams help your physician see inside your body to determine whether you have Crohn s. Different types of tests include: Barium enema This test helps physicians visualize the colon and rectum. Upper GI and small bowel follow-through In this test, x-rays help examine the esophagus, stomach, duodenum, and small intestine after a patient drinks a barium-based liquid. Enteroclysis In this test, a tube is inserted into the nose and guided through the stomach to the duodenum, which is where the small intestine begins. A bariumbased liquid is then infused through the tube, and x- rays are used to reveal abnormalities within the small intestine. Computerized tomography (CT) scan: This extremely precise x-ray is used to detect abnormalities in the liver, kidneys, and intestines after a dye is ingested, administered intravenously, or inserted through the rectum. Ultrasound By using sound waves, this test examines organs of the pelvis and abdomen without exposure to radiation. Magnetic resonance imaging (MRI) By using radio waves and superconducting magnets, this test can help detect fistulas and abscesses within a person s body without exposure to radiation. Stool tests These noninvasive tests examine stool samples to determine whether a patient has Crohn s disease, ulcerative colitis, or a bacterial infection. Urine tests Also called urinalysis, these tests are used to detect the presence of bacteria, red blood cells, and white blood cells in your urine. When bacteria and white blood cell levels are raised, it may indicate a urinary tract infection, which can be a complication of Crohn s. Endoscopic examinations These tests use a tool called an endoscope a thin, flexible, lighted tube that is linked to a computer and video monitor. In an endoscopic exam, the endoscope is inserted into the rectum, mouth, or small abdominal incision to give gastroenterologists a detailed view of the intestinal tract. Different endoscopic exams may include Sigmoidoscopy This test is the most commonly performed endoscopic exam used to confirm a diagnosis of Crohn s. By using either a flexible or rigid instrument, a physician can evaluate the rectum and lower end of the colon for signs of inflammation
12 Colonoscopy This test examines the full length of the colon, as well as the lower part of the small intestine. Upper endoscopy In this exam, an endoscope is placed into a patient s mouth and guided through the stomach to the upper intestine. Although there is no cure for Crohn's, the sooner Crohn s is diagnosed, the better chance you have of managing its symptoms and avoiding potentially serious complications of the disease. HOW IS CROHN S DISEASE DIAGNOSED? In most cases, people with Crohn's disease are treated by a gastroenterologist. Sometimes your gastroenterologist may be an internist or family practitioner. WHAT ARE THE COMPLICATIONS OF CROHN S DISEASE? The complications that Crohn s patients experience depend on the location and severity of the disease. Some complications can be life threatening, while others are manageable with the help of treatment plans prescribed by a gastroenterologist. SERIOUS COMPLICATIONS CROHN S MAY CAUSE SERIOUS COMPLICATIONS, WHICH CAN HAPPEN OVER THE COURSE OF THE ILLNESS: Obstruction Obstructions can occur when the intestinal wall swells inward, reducing the capacity for fluids to flow through the intestine. A patient may experience painful cramps or vomiting due to food that is not able to bypass the obstruction. Patients who experience an obstructive episode are usually hospitalized and given intravenous fluids and salts to compensate for fluid losses. Fistula Sometimes ulcers caused by Crohn's will channel through the gut wall to adjacent areas, including the skin, bladder, vagina, intestine, and perianal areas. These occurrences are known as fistulas and may require medical or surgical therapy. Abscess An abscess is a localized collection of bacteria that eventually accumulates pus and places painful pressure on adjacent tissues. A fistula that tracks into the abdominal cavity may produce infection and form an abscess. Abscesses may also occur in the pelvic tissues or the perineum, if a fistula fails to drain. Abscesses can be difficult for gastroenterologists to diagnose; however, after they are located, they should be drained. This may require surgery. Patients are usually given a course of antibiotics to reduce the risk of further infection. Free perforation A free perforation is the formation of a hole in the bowel wall that allows intestinal contents to enter the abdominal cavity. Signs of free perforation include sudden, severe abdominal pain, shock, and excessive abdominal tenderness. The infection that results is called peritonitis and requires emergency surgery in which the leak is sealed and the abdominal cavity is cleansed to stop infection. Hemorrhage In rare cases, a bleeding ulcer may burrow through the gut wall and shear an artery. This produces a life-threatening hemorrhage that may require blood transfusions and special measures to promote blood clotting. Sometimes emergency surgery is required. People with Crohn s may experience chronic or long-lasting complications that require ongoing management: Anemia Anemia is a condition that results from lack of red blood cells. Anemia in Crohn's may be the result of chronic blood loss; bone marrow depression; or failure to absorb iron and folic acid, which are important in stimulating the production of red blood cells. Certain medications, such as sulfasalazine, may also exacerbate anemia. To combat most cases of anemia, gastroenterologists often prescribe supplements, and recommend a diet rich in iron
13 Malnutrition Malnutrition occurs when the body does not receive enough nutrients to grow and develop properly. Loss of protein, tissue breakdown due to steroid use, poor diet and, in some cases, failure to absorb nutrients result in weight loss and nutritional deficiencies. Gastroenterologists often prescribe nutritional supplements to avoid the complications that result from deficiencies in vitamins A, D, E, and K. WHAT ARE THE CURRENT TREATMENT OPTIONS? Currently, there is no cure for Crohn s. In the meantime, the goals of treating Crohn s are to suppress inflammation, enable healing of the intestinal lining, and relieve the symptoms of fever, diarrhea, and abdominal pain. Currently available treatments for Crohn s include: Anti-inflammatory medication Most people who have Crohn s receive one or more different types of drugs designed to control inflammation. These may include sulfasalazine, other medications containing mesalamine (known as 5-ASA agents), and corticosteroids. Immunosuppressive medication These drugs block the body s immune response, which leads to inflammation. Immunosuppressive medications used to treat Crohn s include azathioprine, 6-mercaptopurine, methotrexate, and cyclosporine. Biologics Infliximab is the first agent approved for moderate to severe Crohn's disease in adults and children who haven't responded well to other therapies. This is useful for both inducing remission as well as maintenance of remission. Antibiotics Antibiotics, such as metronidazole and ciprofloxacin, may help heal abscesses and fistulas. Other antibiotics may be prescribed to treat bacterial growth in the intestine caused by obstruction or abscesses. Antidiarrheal medication Antidiarrheal medication offers some relief for the diarrhea that many people with Crohn s experience. Loperamide, codeine, and even fiber powders can help alleviate symptoms. Nutritional supplements: Nutritional supplements are helpful for people who lose calories and nutrients from diarrhea or decreased appetite. Supplements can help fuel the body and replenish iron, calcium, other minerals, and vitamins. Surgery: If other treatments do not effectively control symptoms, your doctor may recommend surgery to close fistulas or remove the part of the intestine where the inflammation is most severe. Unfortunately, this procedure usually leads to only temporary remission of symptoms. The inflammation often returns near the area where the tissue was removed. Some people may experience long periods of remission when they are free of symptoms. However, symptoms usually recur at various times over a person's lifetime. It is not possible to predict when a remission may occur or when symptoms will return. Because of the unpredictability of Crohn's, you may need medical care for some time
14 The sooner you understand your condition, the better. FREQUENTLY ASKED QUESTIONS How does IBD affect daily life? IBD affects every patient differently, depending on the severity of each individual case. IBD is often cyclical in nature. You may experience periods of remission from your symptoms between flare-up periods. Although IBD is a serious, chronic disease, many patients respond well to treatment and live productive, active lives. What if my symptoms seem to be in remission? Some people may experience long periods of remission when they are free of symptoms. These periods can last for years. However, the symptoms usually recur at various times over a person's lifetime. It is not possible to predict when a remission may occur, or when symptoms will return. Because of the unpredictability of UC, your doctor may recommend ongoing medical treatment and regular office visits to monitor your condition. The treatment plan that's right for you may include drugs, nutritional supplements, surgery, or a combination of these options. What if I choose to postpone treatment? Not dealing with IBD properly can lead to more serious problems, including bowel obstructions or strictures (narrowing of the intestine). And if problems remain untreated, invasive surgery may be your only option. To avoid these potential problems, it's best to seek out a proper diagnosis as early as possible. Why me? While the true cause of IBD is unknown, it is believed that a number of factors play a role. For instance, genetics and heredity play a role - individuals whose family members have UC are more likely to develop it themselves. Environmental factors may play a role, but specific factors have not been identified. It's important to remember that you did not do anything to cause your illness, and that you are not alone. What is the role of diet in IBD? Major dietary considerations are not required. Milk products are to be avoided in those with symptoms of lactose intolerance. During active disease, low roughage diet is generally advised. When disease is in remission, a normal diet is advised but very spicy, greasy foods should be avoided. In addition, any particular food known to precipitate symptoms should be brought to the knowledge of the treating doctor. How does stress relate to IBD? Stress does not cause IBD. However, some people who already have UC report that stressful events precede a flare-up. Although living with IBD is not easy, it is important to try to control your stress whenever possible and maintain a positive outlook. There are many ways to manage stress - while some people seek support or meditate, others like vigorous activity. Still others like to talk about their feelings. Find the way that works best for you. Does IBD affect a woman's ability to conceive? Generally speaking, a woman with IBD whose disease is inactive has the same ability to conceive as women who are unaffected. She can experience a normal, full-term delivery. Flare-ups during pregnancy can usually be effectively treated with medical therapy. On the other hand, women with active disease may be more likely to have a miscarriage or premature delivery. Can it lead to cancer? Yes, IBD patients can develop cancer though the risk is very low in patients with well controlled disease. However, after years of disease regular follow-ups is recommended. What about alternative therapies? I am told indigenous medicines can cure the disease? As yet there is no scientific evidence that any of the available alternative therapies are effective for IBD 24 Inside back 25
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
What is ulcerative colitis?
 What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
WHAT IS ULCERATIVE COLITIS?
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
Ulcerative Colitis. ulcerative colitis usually only affects the colon.
 Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Crohn's disease CAUSES COURSE OF CROHN'S DISEASE TREATMENT. Sulfasalazine
 Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
ULCERATIVE COLITIS. Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC
 ULCERATIVE COLITIS Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC What is Ulcerative Colitis? Ulcerative colitis (UC) is a disease marked by inflammation
ULCERATIVE COLITIS Sean Lynch, MD and Richard Bloomfeld, MD Wake Forest University School of Medicine Winston-Salem, NC What is Ulcerative Colitis? Ulcerative colitis (UC) is a disease marked by inflammation
Certain genes passed on from parent to child increase the risk of developing Crohn's disease, if the right trigger occurs.
 Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Inflammatory Bowel Disease. Your Illness and Its Treatment
 Inflammatory Bowel Disease Your Illness and Its Treatment What Is Inflammatory Bowel Disease? Inflammatory bowel disease (IBD) is inflammation (irritation and swelling) of the digestive tract. Your digestive
Inflammatory Bowel Disease Your Illness and Its Treatment What Is Inflammatory Bowel Disease? Inflammatory bowel disease (IBD) is inflammation (irritation and swelling) of the digestive tract. Your digestive
What is Crohn's disease?
 What is Crohn's disease? Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area
What is Crohn's disease? Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area
Welcome to Week 2 of the Crohn s & Colitis Foundation of America (CCFA) Online Support Group.
 Welcome to Week 2 of the Crohn s & Colitis Foundation of America (CCFA) Online. Last week s material consisted of an overview of inflammatory bowel diseases (IBD), specifically Crohn s disease and ulcerative
Welcome to Week 2 of the Crohn s & Colitis Foundation of America (CCFA) Online. Last week s material consisted of an overview of inflammatory bowel diseases (IBD), specifically Crohn s disease and ulcerative
The London Gastroenterology Partnership CROHN S DISEASE
 CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
INFLAMMATORY BOWEL DISEASE (IBD): CROHN S DISEASE
 INFLAMMATORY BOWEL DISEASE (IBD): CROHN S DISEASE Symptoms The symptoms of Crohn s disease can vary from person to person, based on where the disease is in the body and how bad the inflammation is. The
INFLAMMATORY BOWEL DISEASE (IBD): CROHN S DISEASE Symptoms The symptoms of Crohn s disease can vary from person to person, based on where the disease is in the body and how bad the inflammation is. The
Small Bowel and Colon Surgery
 Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
The National Association of Crohn s and Colitis of Trinidad and Tobago CROHN S DISEASE AND ULCERATIVE COLITIS GENERAL PATIENT INFORMATION
 The National Association of Crohn s and Colitis of Trinidad and Tobago CROHN S DISEASE AND ULCERATIVE COLITIS GENERAL PATIENT INFORMATION You are reading this pamphlet because you or someone you known
The National Association of Crohn s and Colitis of Trinidad and Tobago CROHN S DISEASE AND ULCERATIVE COLITIS GENERAL PATIENT INFORMATION You are reading this pamphlet because you or someone you known
UNDERSTANDING CROHN S DISEASE
 UNDERSTANDING CROHN S DISEASE START YOUR JOURNEY TOWARD UNDERSTANDING INFLAMMATORY BOWEL DISEASE CONTENTS INTRODUCTION 4 WHAT IS CROHN S DISEASE? 6 Symptoms of Crohn s disease 6 WHAT CAUSES CROHN S DISEASE?
UNDERSTANDING CROHN S DISEASE START YOUR JOURNEY TOWARD UNDERSTANDING INFLAMMATORY BOWEL DISEASE CONTENTS INTRODUCTION 4 WHAT IS CROHN S DISEASE? 6 Symptoms of Crohn s disease 6 WHAT CAUSES CROHN S DISEASE?
Colon Cancer Surgery
 Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
What is Inflammatory Bowel Disease (IBD)?
 INFLAMMATORY BOWEL DISEASE (IBD) What is Inflammatory Bowel Disease (IBD)? Inflammatory bowel disease, or IBD, is when there is inflammation, or swelling, in the gastrointestinal (GI) tract and a lifelong
INFLAMMATORY BOWEL DISEASE (IBD) What is Inflammatory Bowel Disease (IBD)? Inflammatory bowel disease, or IBD, is when there is inflammation, or swelling, in the gastrointestinal (GI) tract and a lifelong
SURVIVING & THRIVING. A Guide to Living with Crohn s Disease or Ulcerative Colitis.
 SURVIVING & THRIVING A Guide to Living with Crohn s Disease or Ulcerative Colitis www.crohnsandcolitis.ca You or someone you care about has been diagnosed with Crohn s disease or ulcerative colitis (the
SURVIVING & THRIVING A Guide to Living with Crohn s Disease or Ulcerative Colitis www.crohnsandcolitis.ca You or someone you care about has been diagnosed with Crohn s disease or ulcerative colitis (the
Colectomy. Surgical treatment for Ulcerative Colitis (UC) and Familial Adenomatous Polyposis (FAP) Patient and Family Education
 Patient and Family Education Colectomy Surgical treatment for Ulcerative Colitis (UC) and Familial Adenomatous Polyposis (FAP) A colectomy is a surgery that removes the colon, or large intestine. The colectomy
Patient and Family Education Colectomy Surgical treatment for Ulcerative Colitis (UC) and Familial Adenomatous Polyposis (FAP) A colectomy is a surgery that removes the colon, or large intestine. The colectomy
Colon Cancer , The Patient Education Institute, Inc. oc Last reviewed: 05/17/2017 1
 Colon Cancer Introduction Colon cancer is fairly common. About 1 in 15 people develop colon cancer. Colon cancer can be a life threatening condition that affects the large intestine. However, if it is
Colon Cancer Introduction Colon cancer is fairly common. About 1 in 15 people develop colon cancer. Colon cancer can be a life threatening condition that affects the large intestine. However, if it is
INFLAMMATORY BOWEL DISEASE. Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic
 INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
The Role of Surgery in Inflammatory Bowel Disease. Cory D Barrat, MD Colon and Rectal Surgeon Mercy Health
 The Role of Surgery in Inflammatory Bowel Disease Cory D Barrat, MD Colon and Rectal Surgeon Mercy Health THANKS FOR INVITING ME! I have no financial disclosures Outline - Who am I and what do I do? -
The Role of Surgery in Inflammatory Bowel Disease Cory D Barrat, MD Colon and Rectal Surgeon Mercy Health THANKS FOR INVITING ME! I have no financial disclosures Outline - Who am I and what do I do? -
LAPAROSCOPIC APPENDICECTOMY
 LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
PATIENT INFORMATION FROM YOUR SURGEON & SAGES. Laparoscopic Colon Resection
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Colon Resection About Conventional
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Colon Resection About Conventional
more intense treatments are needed to get rid of the infection.
 What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
Chapter 34. Nursing Care of Patients with Lower Gastrointestinal Disorders
 Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
X-Plain Sigmoidoscopy Reference Summary
 X-Plain Sigmoidoscopy Reference Summary Introduction Colon diseases are common. A sigmoidoscopy is a test that can help detect colon diseases. If your doctor recommends that you have a sigmoidoscopy, the
X-Plain Sigmoidoscopy Reference Summary Introduction Colon diseases are common. A sigmoidoscopy is a test that can help detect colon diseases. If your doctor recommends that you have a sigmoidoscopy, the
Inflectra for Crohn s disease
 Inflectra for Crohn s disease Some important information to get you started with your treatment This booklet is intended only for use by patients who have been prescribed Inflectra. Introduction When you
Inflectra for Crohn s disease Some important information to get you started with your treatment This booklet is intended only for use by patients who have been prescribed Inflectra. Introduction When you
Appendicitis. Diagnosis and Surgery
 Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
3/22/2011. Inflammatory Bowel Disease. Inflammatory Bowel Disease Objectives: Appendicitis. Lemone and Burke Chapter 26
 Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
Top 10 Things you need to know about IBD. Suresh Pola, MD Kaiser San Diego
 Top 10 Things you need to know about IBD Suresh Pola, MD Kaiser San Diego Top 10 Things to Know: IBD What you can eat How to treat the pain Not all diarrhea is a flare Ways to reduce your risk of getting
Top 10 Things you need to know about IBD Suresh Pola, MD Kaiser San Diego Top 10 Things to Know: IBD What you can eat How to treat the pain Not all diarrhea is a flare Ways to reduce your risk of getting
Ulcerative Colitis. National Digestive Diseases Information Clearinghouse. What is ulcerative colitis (UC)?
 Ulcerative Colitis National Digestive Diseases Information Clearinghouse What is ulcerative colitis (UC)? Ulcerative colitis is a chronic, or long-lasting, disease that causes inflammation and sores, called
Ulcerative Colitis National Digestive Diseases Information Clearinghouse What is ulcerative colitis (UC)? Ulcerative colitis is a chronic, or long-lasting, disease that causes inflammation and sores, called
Limited Bowel Resection. Surgery for Crohn s Disease
 Limited Bowel Resection Surgery for Crohn s Disease What Is Crohn s Disease? Crohn s disease is inflammation (irritation and swelling) of the digestive tract. Crohn s disease occurs anywhere from the mouth
Limited Bowel Resection Surgery for Crohn s Disease What Is Crohn s Disease? Crohn s disease is inflammation (irritation and swelling) of the digestive tract. Crohn s disease occurs anywhere from the mouth
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
Inflammatory Bowel Disease
 page 1 Inflammatory Bowel Disease stay healthy. Food moves from the esophagus down to the small intestine, where the nutrients are absorbed into the blood. Leftover water and solid waste then move down
page 1 Inflammatory Bowel Disease stay healthy. Food moves from the esophagus down to the small intestine, where the nutrients are absorbed into the blood. Leftover water and solid waste then move down
Garrick Brown, MD. Digestive Health Specialists Tacoma Gig Harbor
 Garrick Brown, MD Digestive Health Specialists Tacoma Gig Harbor Today s Objectives Define IBD, its potential causes and diagnosis Discuss management and treatment Discuss complementary and alternative
Garrick Brown, MD Digestive Health Specialists Tacoma Gig Harbor Today s Objectives Define IBD, its potential causes and diagnosis Discuss management and treatment Discuss complementary and alternative
This information explains the advice about Crohn's disease that is set out in NICE guideline CG152.
 Information for the public Published: 1 October 2012 nice.org.uk About this information NICE guidelines provide advice on the care and support that should be offered to people who use health and care services.
Information for the public Published: 1 October 2012 nice.org.uk About this information NICE guidelines provide advice on the care and support that should be offered to people who use health and care services.
UNDERSTANDING ULCERATIVE COLITIS
 UNDERSTANDING ULCERATIVE COLITIS START YOUR JOURNEY TOWARD UNDERSTANDING INFLAMMATORY BOWEL DISEASE CONTENTS INTRODUCTION 4 WHAT IS ULCERATIVE COLITIS? 6 Symptoms of ulcerative colitis 6 WHAT CAUSES ULCERATIVE
UNDERSTANDING ULCERATIVE COLITIS START YOUR JOURNEY TOWARD UNDERSTANDING INFLAMMATORY BOWEL DISEASE CONTENTS INTRODUCTION 4 WHAT IS ULCERATIVE COLITIS? 6 Symptoms of ulcerative colitis 6 WHAT CAUSES ULCERATIVE
Surgery and Crohn s. Crohn s Disease 70 % Why Operate? Complications of Disease. The Gastrointestinal Tract. Surgery for Inflammatory Bowel Disease
 The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
Inflammatory Bowel Disease
 Inflammatory Bowel Disease Inflammatory bowel disease (IBD) is a group of inflammatory conditions of the colon and small intestine. Crohn's disease andulcerative colitis are the principal types of inflammatory
Inflammatory Bowel Disease Inflammatory bowel disease (IBD) is a group of inflammatory conditions of the colon and small intestine. Crohn's disease andulcerative colitis are the principal types of inflammatory
Diverticular Disease Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Diverticular Disease Diverticulum refers to a side-branch or pouch which sticks outwards from the wall
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Diverticular Disease Diverticulum refers to a side-branch or pouch which sticks outwards from the wall
Medical therapies and IBD
 Medical therapies and IBD Although there is no cure for IBD, there are many treatment options available. There is no standard treatment for IBD that is effective in all situations or for all patients,
Medical therapies and IBD Although there is no cure for IBD, there are many treatment options available. There is no standard treatment for IBD that is effective in all situations or for all patients,
What Is an Endoscopic Ultrasound (EUS)?
 ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
ENDOSCOPIC ULTRASOUND (EUS) What Is an Endoscopic Ultrasound (EUS)? An endoscopic ultrasound (EUS) is a specialized procedure that blends: Endoscopy use of a scope to look at the inside lining of the gastrointestinal
Abdominal surgery for Crohn's disease. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Abdominal surgery for Crohn's disease Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Abdominal surgery for Crohn's disease Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Understanding Inflammatory Bowel Diseases (IBD):
 Understanding Inflammatory Bowel Diseases (IBD): What Every Patient Needs to Know William H Holderman, MD Digestive Health Specialists Tacoma, WA Today s Objectives Define IBD, its potential causes and
Understanding Inflammatory Bowel Diseases (IBD): What Every Patient Needs to Know William H Holderman, MD Digestive Health Specialists Tacoma, WA Today s Objectives Define IBD, its potential causes and
Surgery for Inflammatory Bowel Disease
 Surgery for Inflammatory Bowel Disease Emily Steinhagen, MD Assistant Professor Department of Surgery, Division of Colorectal Surgery University Hospitals Cleveland Medical Center Common Questions Why
Surgery for Inflammatory Bowel Disease Emily Steinhagen, MD Assistant Professor Department of Surgery, Division of Colorectal Surgery University Hospitals Cleveland Medical Center Common Questions Why
I B D. etter than this. isease UNDERSTANDING INFLAMMATORY BOWEL DISEASES
 I B D m etter than this isease UNDERSTANDING INFLAMMATORY BOWEL DISEASES What types of people have learned how to manage their IBD? Athletes Musicians Firefighters DOCTORS HEROES Artists Presidents Actors
I B D m etter than this isease UNDERSTANDING INFLAMMATORY BOWEL DISEASES What types of people have learned how to manage their IBD? Athletes Musicians Firefighters DOCTORS HEROES Artists Presidents Actors
CROHN S DISEASE. The term "inflammatory bowel disease" includes Crohn's disease and the other related condition called ulcerative colitis.
 CROHN S DISEASE What does it consist of? Crohn s disease is an inflammatory process that affects mostly to the intestinal tract, although it can affect any other part of the digestive apparatus from the
CROHN S DISEASE What does it consist of? Crohn s disease is an inflammatory process that affects mostly to the intestinal tract, although it can affect any other part of the digestive apparatus from the
There is no single IBD diet
 Nutrition and IBD There is no single IBD diet Nutrition plays an important role in health, during times of IBD disease activity as well as during remission. Although diet does not cause or cure IBD, the
Nutrition and IBD There is no single IBD diet Nutrition plays an important role in health, during times of IBD disease activity as well as during remission. Although diet does not cause or cure IBD, the
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Contrast Materials Patient Safety: What are contrast materials and how do they work?
 Contrast Materials Patient Safety: What are contrast materials and how do they work? Which imaging exams use contrast materials? How safe are contrast materials? How should I prepare for my imaging procedure
Contrast Materials Patient Safety: What are contrast materials and how do they work? Which imaging exams use contrast materials? How safe are contrast materials? How should I prepare for my imaging procedure
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Understanding Your Benefits and Risks
 IBD Treatment Options Understanding Your Benefits and Risks benefit risk assessment tool Understand your options. Improve your health... and life. Inflammatory bowel disease (IBD) is two, separate disorders
IBD Treatment Options Understanding Your Benefits and Risks benefit risk assessment tool Understand your options. Improve your health... and life. Inflammatory bowel disease (IBD) is two, separate disorders
Inflammatory Bowel Disease and Surgery: What You Should Know
 Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
The appendix is a small, tube-like structure attached to the first part of the large intestine, also called the colon. The appendix.
 The appendix is a small, tube-like structure attached to the first part of the large intestine, also called the colon. The appendix is located in the lower right portion of the abdomen. It has no known
The appendix is a small, tube-like structure attached to the first part of the large intestine, also called the colon. The appendix is located in the lower right portion of the abdomen. It has no known
Crohn s Disease. Questions & Answers
 Crohn s Disease Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard - 0141 810 3151 Ph.
Crohn s Disease Questions & Answers GLASGOW COLORECTAL CENTRE Ross Hall Hospital 221 Crookston Road Glasgow G52 3NQ e-mail: info@colorectalcentre.co.uk Ph: Main hospital switchboard - 0141 810 3151 Ph.
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
What Is Peptic Ulcer Disease?
 What Is Peptic Ulcer Disease? Peptic ulcer disease is when painful sores form in the lining of the stomach, duodenum (start of the small intestine) or bowels. An ulcer can cause belly pain and, in some
What Is Peptic Ulcer Disease? Peptic ulcer disease is when painful sores form in the lining of the stomach, duodenum (start of the small intestine) or bowels. An ulcer can cause belly pain and, in some
X-Plain Colostomy Reference Summary
 X-Plain Colostomy Reference Summary Introduction Diseases of the colon and intestines are common. When diseases of the intestines are treated with surgery, it sometimes results in a colostomy or an ileostomy.
X-Plain Colostomy Reference Summary Introduction Diseases of the colon and intestines are common. When diseases of the intestines are treated with surgery, it sometimes results in a colostomy or an ileostomy.
Tapeworm Infection. Tapeworm
 Tapeworm Infection Introduction Tapeworm infection is caused by ingesting food or water that is contaminated with tapeworm eggs or larvae. Larvae are newly hatched tapeworms. A tapeworm may attach itself
Tapeworm Infection Introduction Tapeworm infection is caused by ingesting food or water that is contaminated with tapeworm eggs or larvae. Larvae are newly hatched tapeworms. A tapeworm may attach itself
THE CUTTING EDGE SURGERY FOR CROHN S DISEASE & ULCERATIVE COLITIS. crohnsandcolitis.ca
 THE CUTTING EDGE SURGERY FOR CROHN S DISEASE & ULCERATIVE COLITIS crohnsandcolitis.ca There are many treatments that help manage Crohn s and colitis. Crohn s and Colitis Canada urges you to become knowledgeable
THE CUTTING EDGE SURGERY FOR CROHN S DISEASE & ULCERATIVE COLITIS crohnsandcolitis.ca There are many treatments that help manage Crohn s and colitis. Crohn s and Colitis Canada urges you to become knowledgeable
Inflammatory Bowel Disease Medical Exam Questionnaire
 Patient Name: MR: Date: Name DOB / / Age Marital Status Race Gender M / F Height Present Weight Usual Weight Insurance Managed Care Self referral Yes No Yes No Yes No Primary Care Physician Referring Physician
Patient Name: MR: Date: Name DOB / / Age Marital Status Race Gender M / F Height Present Weight Usual Weight Insurance Managed Care Self referral Yes No Yes No Yes No Primary Care Physician Referring Physician
How do I choose amongst medicines for inflammatory bowel disease. Maria T. Abreu, MD
 How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
Glencoe Health. Lesson 3 The Digestive System
 Glencoe Health Lesson 3 The Digestive System Health espotlight Video BIG IDEA The digestive system provides nutrients and energy for your body through the digestion of food. New Vocabulary mastication
Glencoe Health Lesson 3 The Digestive System Health espotlight Video BIG IDEA The digestive system provides nutrients and energy for your body through the digestion of food. New Vocabulary mastication
Speaker Introduction
 Speaker Introduction Stephen B. Hanauer, MD Professor of Medicine and Clinical Pharmacology University of Chicago Pritzker School of Medicine Chief of Gastroenterology, Hepatology, and Nutrition University
Speaker Introduction Stephen B. Hanauer, MD Professor of Medicine and Clinical Pharmacology University of Chicago Pritzker School of Medicine Chief of Gastroenterology, Hepatology, and Nutrition University
What Is Pancreatitis?
 What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
What Is Pancreatitis? Pancreatitis is inflammation (swelling) of the pancreas that is most often caused by gallstones or alcohol abuse. There are other causes that your gastroenterologist will look for,
X-ray (Radiography) - Lower GI Tract
 Scan for mobile link. X-ray (Radiography) - Lower GI Tract Lower gastrointestinal tract radiography or lower GI uses a form of real-time x-ray called fluoroscopy and a barium-based contrast material to
Scan for mobile link. X-ray (Radiography) - Lower GI Tract Lower gastrointestinal tract radiography or lower GI uses a form of real-time x-ray called fluoroscopy and a barium-based contrast material to
Laparoscopic Gastric Bypass Information
 1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
The Road to Remission
 The Road to Remission Understanding, Treating and Living with Inflammatory Bowel Disease IBDCenterOrlando.com As many as 1.5 million Americans currently suffer from inflammatory bowel disease (IBD), and
The Road to Remission Understanding, Treating and Living with Inflammatory Bowel Disease IBDCenterOrlando.com As many as 1.5 million Americans currently suffer from inflammatory bowel disease (IBD), and
COLORECTAL RESECTIONS
 COLORECTAL RESECTIONS What is a colorectal (bowel) resection? Surgery to remove a part of the large bowel is called a resection. Different parts of the colon require different operations and have different
COLORECTAL RESECTIONS What is a colorectal (bowel) resection? Surgery to remove a part of the large bowel is called a resection. Different parts of the colon require different operations and have different
What is Irritable Bowel Syndrome (IBS)?
 What is Irritable Bowel Syndrome (IBS)? Irritable bowel syndrome (IBS) is a health issue found in your intestines (gut). IBS can cause symptoms such as: Belly pain. Cramping. Gas. Bloating (or swelling)
What is Irritable Bowel Syndrome (IBS)? Irritable bowel syndrome (IBS) is a health issue found in your intestines (gut). IBS can cause symptoms such as: Belly pain. Cramping. Gas. Bloating (or swelling)
What is a Colonoscopy?
 What is a Colonoscopy? A colonoscopy is a test to look inside your colon. A colonoscopy is done by a gastroenterologist, a doctor trained in looking at the gastrointestinal (GI) tract. The main tool used
What is a Colonoscopy? A colonoscopy is a test to look inside your colon. A colonoscopy is done by a gastroenterologist, a doctor trained in looking at the gastrointestinal (GI) tract. The main tool used
A Trip Through the GI Tract: Common GI Diseases and Complaints. Jennifer Curtis, MD
 A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
A Trip Through the GI Tract: Common GI Diseases and Complaints Jennifer Curtis, MD Colon Cancer How does it develop? Most cancers arise from polyps Over time these can turn into cancer Combination of genetic
Bleeding in the Digestive Tract
 Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
A PARENT S GUIDE TO INFLAMMATORY BOWEL DISEASE
 A PARENT S GUIDE TO INFLAMMATORY BOWEL DISEASE START YOUR JOURNEY TOWARD UNDERSTANDING INFLAMMATORY BOWEL DISEASE CONTENTS INTRODUCTION 4 WHAT IS INFLAMMATORY BOWEL DISEASE? 6 Crohn s disease 6 Ulcerative
A PARENT S GUIDE TO INFLAMMATORY BOWEL DISEASE START YOUR JOURNEY TOWARD UNDERSTANDING INFLAMMATORY BOWEL DISEASE CONTENTS INTRODUCTION 4 WHAT IS INFLAMMATORY BOWEL DISEASE? 6 Crohn s disease 6 Ulcerative
At the outset, we want to clear up some terminology issues. IBS is COPYRIGHTED MATERIAL. What Is IBS?
 1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
Definitions. Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency)
 CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS
 SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
PEDIATRIC INFLAMMATORY BOWEL DISEASE
 PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Information on Laparoscopic Extended Right Hemicolectomy. Colon surgery. The Colon. Laparoscopic Extended Right Hemicolectomy
 Colon surgery Patients undergo colon surgery for a number of conditions including: colorectal cancer, polyps, inflammatory bowel disease (Crohn s disease and ulcerative colitis), colonic inertia, stricture
Colon surgery Patients undergo colon surgery for a number of conditions including: colorectal cancer, polyps, inflammatory bowel disease (Crohn s disease and ulcerative colitis), colonic inertia, stricture
The ABCs of Inflammatory Bowel Disease. Jennifer Choi, M.D. Associate Director March 31, 2012
 The ABCs of Inflammatory Bowel Disease Jennifer Choi, M.D. Associate Director March 31, 2012 What Will This Talk Cover? What is IBD? What causes it? What are complications of it? How do I find out if I
The ABCs of Inflammatory Bowel Disease Jennifer Choi, M.D. Associate Director March 31, 2012 What Will This Talk Cover? What is IBD? What causes it? What are complications of it? How do I find out if I
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Doncaster & Bassetlaw Medicines Formulary
 Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children
 Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
Colorectal Cancer Screening
 Scan for mobile link. Colorectal Cancer Screening What is colorectal cancer screening? Screening examinations are tests performed to identify disease in individuals who lack any signs or symptoms. The
Scan for mobile link. Colorectal Cancer Screening What is colorectal cancer screening? Screening examinations are tests performed to identify disease in individuals who lack any signs or symptoms. The
For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU)
 Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Form: D-8705 Pancreatitis For family, friends and caregivers of a patient with pancreatitis in the Medical Surgical Intensive Care Unit (MSICU) This brochure will give you more information about: The causes
Dr David Epstein Vincent Pallotti Hospital and University of Cape Town
 Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Ulcerative colitis: the management of ulcerative colitis Quality standard title: Ulcerative
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Ulcerative colitis: the management of ulcerative colitis Quality standard title: Ulcerative
F A M N O P R S ! D !
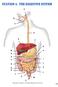 A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
PATIENT HISTORY FORM
 PATIENT HISTORY FORM Date: Page 1 of 5 Last Name: First Name: Middle Initial: Referred By: Age: Primary Care Doctor: Please provide name(s) of other physician(s) that you have visited within the last year:
PATIENT HISTORY FORM Date: Page 1 of 5 Last Name: First Name: Middle Initial: Referred By: Age: Primary Care Doctor: Please provide name(s) of other physician(s) that you have visited within the last year:
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Copyright The Food Intolerance Testing Group. All rights reserved. No part of this publication may be
 Copyright 2018 The Food Intolerance Testing Group All rights reserved. No part of this publication may be reproduced, distributed, or transmitted in any form or by any means, including photocopying, recording,
Copyright 2018 The Food Intolerance Testing Group All rights reserved. No part of this publication may be reproduced, distributed, or transmitted in any form or by any means, including photocopying, recording,
Chronic Pancreatitis (1 of 4) i
 Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Ulcerative colitis (UC) is a. The Patient with Newly Diagnosed Ulcerative Colitis: Anticipating the Questions and Individualizing the Answers
 The Patient with Newly Diagnosed Ulcerative Colitis: Anticipating the Questions and Individualizing the Answers James Gregor, MD, Division of Gastroenterology, The University of Western Ontario, London,
The Patient with Newly Diagnosed Ulcerative Colitis: Anticipating the Questions and Individualizing the Answers James Gregor, MD, Division of Gastroenterology, The University of Western Ontario, London,
Your Bowel Operation Hartmanns Procedure
 Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
