SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
|
|
|
- Rosalyn Stephens
- 5 years ago
- Views:
Transcription
1 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist North Cumbria University Hospital ** Consultant Obstetrician and Gynecologist North Cumbria University Hospital ABSTRACT: OBJECTIVE: The purpose of this study was to determine the functional outcomes, and to link the success of sacrospinous fixation with the age of patients, time interval between surgery and recurrence of prolapse. Also, to see if concomitant surgeries affect the outcome. STUDY DESIGN: An original observational study. METHODS AND MATERIALS: Between 2006 and 2015, 109 women underwent sacrospinous fixation for the management of symptomatic vaginal vault prolapse in North Cumbria University Hospital. Follow-up data was available for 107 patients. Inclusion criteria were women with symptomatic vaginal or vault prolapse with Baden-Walker system grade 2 which needs surgical treatment, surgically fit for surgery and have the capacity to consent to surgery. Exclusion criteria were the previous surgical treatment of vault prolapse, contraindication for a surgical intervention and have no capacity to consent to surgery. RESULTS: Out of 107 patients, 45 underwent SSLF with anterior and posterior colporrhaphy, 18 had vaginal hysterectomy, anterior and posterior colporrhaphy and sacrospinous fixation. SSLF was combined with anterior colporrhaphy in 4 and with posterior colporrhaphy in 38 women. Recurrence of prolapse was seen in only 14 patients. Advanced age showed the slightly increased risk of recurrence as of those who had the recurrence, 8 were over the age of 70. The successful surgical outcome was seen in 82%, 89%, 75% and 100% of patients when SSF was performed in combination with anterior and posterior repair, with posterior repair, with anterior repair, and with vaginal hysterectomy respectively. Among recurrence group, 57% noticed it within a year of surgery. 57% of women with the recurrence of vault prolapse successfully underwent repeated surgeries in the form of repeat sacrospinous ligament fixation, 3 women were operated with anterior and posterior colporrhaphy with synthetic mesh and 4 had anterior and posterior vaginal wall repair. CONCLUSION: Sacrospinous ligament fixation is an effective procedure with a low recurrence rate. Recurrence is slightly higher with advanced age. Concomitant surgeries do not increase the risk of recurrence. In cases of recurrence, the majority of cases showed it within 12 months of surgery. KEYWORDS: Sacrospinous ligament fixation, prolapse, concomitant surgeries, age INTRODUCTION: Apical prolapse is the descent of uterus, cervix, or vaginal vault. Various reconstructive procedures for prolapse of the vaginal apex are being done for its management. Operations for 44 Corresponding Author: Fauzia Rasool Memon, Consultant Obstetrician and Gynecologist North Cumbria University Hospital. fauziarasoolbux@yahoo.com
2 apical prolapse include transvaginal, open, and laparoscopic or robotic options. Vaginal procedures used for restoring the vaginal apex support include sacrospinous ligament fixation (SSF), iliococcygeal fascial fixation (ICFF), uterosacral ligament suspension (USLS), and u s e o f s y n t h e t i c m e s h e s. A b d o m i n a l Sacrocolopexy (ASC) is an intra-abdominal procedure for vaginal apical support. In spite of various available operations, an ideal procedure for the reconstruction of vaginal apical support has yet to be found. Sacrospinous colpopexy, 1 presented by Randall and Nichols in 1971, has turned into a favoured strategy for reestablishing vaginal support in women with vault prolapse, major prolapse of the vagina and procidentia. The age-particular incidence increased with progressing age and along these lines, better surgical techniques are required. Long term follow-up results of SSF have been published and have indicated cure rates of more than 80%. In the present study, transvaginal sacrospinous ligament fixation strategy was utilized as a component of the vaginal repair technique for marked uterovaginal prolapse and vault prolapse. The reason for this study was to assess straightforward sacrospinous fixation if performed for major vaginal and vault prolapse, helps in reducing the risk of future vault recurrence and to assess the connection between successful surgery and age of the patient, related operations and time interim between surgery and recurrence of prolapse. METHODS: One hundred and nine patients with severe prolapse of pelvic organ undergoing SSF were retrospectively studied. In this study, all patients were staged by the value of Baden- Walker system. In the years of 2006 and 2015, 109 women underwent sacrospinous fixation for the management of symptomatic vaginal vault prolapse. Follow-up information was accessible for 107 patients. Office records were looked into to evaluate the presence of recurrence of prolapse, the age of patients, time interim between surgery and recurrence of prolapse. Data was also collected for related surgeries performed with sacrospinous fixation. Mean duration of follow-up was 12.0±6 months. RESULTS: Eighty-eight (82%) patients had an earlier hysterectomy. Mean age at the time of surgery was 68 year(table 1). Sacrospinous ligament fixation was combined with the accompanying methods; 45 patients had anterior and posterior colporrhaphy (42%), 18 had the sacrospinous fixation in combination with vaginal hysterectomy, anterior colporrhaphy and posterior colporrhaphy (17%). Four anterior colporrhaphies (4%), 38 posterior colporrhaphies (35%) and one sacrospinous fixation was done as solitary procedure (1%). In one Patient (1%) just cervix was removed b e c a u s e o f d i ffi c u l t y i n c o m p l e t i n g hysterectomy due to adhesions.(fig. 1) Ninty three (87%) indicated successful o u t c o m e s w h i l e 1 4 p a t i e n t s ( 1 3 % ) demonstrated recurrent vaginal vault prolapse. Recurrent cystocele was found in 03 cases (3%), 03 developed urinary urgency and urge incontinence (3%) and one (1%) had constant vaginal pain which settled in 6 months after the operation. The average age of failure was 70 year. The results have shown slightly increased risk of failure with advanced age. (Fig. 2) Link with concomitant surgeries. SSF when performed with concomitant surgeries, showed 82%, 89%, and 75% success when done with anterior and posterior repair, with posterior colporrhaphy and with anterior colporrhaphy respectively. 100% success was seen when SSLF was done with vaginal hysterectomy, anterior and posterior vaginal wall repair (18 patients). Of 14 women who had the recurrence of vault prolapse, 8(57%) had sacrospinous fixation combined with anterior and posterior colporrhaphy. Four (29%) had SSLF with posterior vaginal wall repair, one (7%) had SSLF with anterior colporrhaphy and in 1 women (7%) SSLF was done as sole procedure. Time interval between surgery and failure We divided the group of women whose surgery failed into 3 timescales. Three women's operation failed within 6 weeks of surgery. Eight women noticed prolapse again within a year. Two women had recurrence between 2 3 years of surgery, just a single patient noticed recurrence in 6 years' time (Table 2) Eight(57%) patients with complete recurrence 45
3 of vaginal vault prolapse successfully underwent repeated surgeries, Of those 8 women, one had repeat sacrospinous ligament fixation, 3 women were operated with anterior and posterior colporrhaphy with synthetic mesh and 4 had anterior and posterior vaginal wall repair. Two were asymptomatic therefore opted for conservative management, 3 were not suitable for repeat surgery in view of comorbidities and one used shelf pessary for symptomatic relief of prolapse. Table 1 Women s age in years Number of women Percentages (%) < % % % % > % Fig. 1 Fig. 2 Table 4 Number of women (14) Time interval between surgery and recurrence of prolapse %ages 3 6 weeks 22% 8 12 months 57% years 14% 1 6 years 7% DISCUSSION: Pelvic organ prolapse (POP) is a common condition in women and its percentage increase 2 after menopause. It occurs when the pelvic organs, for example, the bladder, uterus, and bowel, drop or slide from their distinctive position into or through the vagina. Although it is not an existence debilitating condition, women with POP frequently encounter pelvic uneasiness, urinary and bowel incontinence, sensory and emptying problems of the lower urinary tract, sexual dysfunction, and a general 46 3 reduction in their quality of life. Prolapse of the vaginal vault is a well-known complication after hysterectomy. It can happen after all types of hysterectomy vaginal, abdominal, or laparoscopic and may be associated with a cystocele, rectocele, and enterocele. Surgical treatment of vaginal vault is a feasible alternative if conservative management fails. Different surgical strategies have been proposed to correct vaginal vault with or 4 without the utilization of graft material. In literature, various operative methods are 5 described for the rectification of vault prolapse.
4 Sacrospinous ligament fixation technique has been applied for apical support procedures for many decades. Fixation of the vaginal apex to the sacrospinous ligament has many advantages. It keeps the vaginal axis in the midline and empowers change of the vaginal length. As a vaginal system, it allows simultaneous management of anterior and posterior vaginal wall prolapse, which is presented in no fewer than two third of cases 4 with total prolapse. By utilizing a transvaginal approach, the potential complications of laparotomy are avoided and have the added benefit of reduced hospital stay and quick 6,7,8 recovery, also sexual potency is maintained. We assessed our experience of SSF with pelvic reconstruction over a 10 year time span. Our surgery success rate (87%) was practically identical with those reported already (67-97%) in a literature review which showed that cure rates of prolapse-related symptoms ranged from 70 to 98 percent (only four studies reported subjective results) and the range of 9 objective cure rates was 67 to 97 percent. Recurrence of apical prolapse after SSF has been reported in 2 to 19 percent of women and of anterior vaginal wall prolapse in 6 to 29 1,10-19 percent. This study also showed apical prolapse in 13% of cases which is not more than already described in other studies. Our study demonstrated most recurrences within 12 months and it is seen in 13% of all surgeries performed. A few reviews have demonstrated a repeat of prolapse in roughly 25% within 5 years, the requirement for repeat 1 surgery is 17%. Recurrence cases in this study were managed with successful repeat surgeries in 57% of cases while others had conservative management. Type of associated surgery with SSLF have no influence on the failure of the procedure as more than 75% success was seen when sacrospinous ligament fixation was done with anterior and posterior repair, with posterior colporrhaphy and with anterior colporrhaphy. More randomized control trials are expected to assess the best treatment for vaginal apical prolapse. Sacrospinous ligament fixation gives great long-term objective and subjective results and enhances personal satisfaction in women treated with the surgery. CONCLUSION: Sacrospinous ligament fixation is an effective and safe procedure with a low recurrence rate. Recurrence risk is slightly higher with advanced age. A concomitant surgery does not increase the risk of recurrence or failure of the procedure. In cases of recurrences, the majority of cases showed it within 12 months of surgery. Repeat procedures performed were also through vaginal route with good success rate. REFERENCES: 1. Randall CL, Nichols DH. Surgical treatment o f v a g i n a l i n v e r s i o n. O b s t e t Gynecol.1971;38: Brown DN. Pelvic organ prolapse: a consequence of nature or nurture? Menopause 2015;22: Lowder JL, Ghetti C, Nikolajski C, et al. Body image perceptions in women with pelvic organ prolapse: a qualitative study. Am J Obstet Gynecol 2011; 204:441.e1 4. Cvach K, Dwyer P. Surgical management of pelvic organ prolapse: abdominal and vaginal approaches. World J Urol 2012;30: Ramalingam K, Monga A. Management of vault prolapsed. The Obstetrician & Gynaecologist 2013;15: Maher C, Feiner B, Baessler K, Schmid C. Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev Siddiqui NY, Grimes CL, Casiano ER, et al. Mesh sacrocolpopexy compared with native tissue vaginal repair: a systematic review and meta-analysis. Obstet Gynecol 2015; 125: Anand M, Weaver AL, Fruth KM, et al. Perioperative Complications and Cost of Vaginal, Open Abdominal, and Robotic Surgery for Apical Vaginal Vault Prolapse. Female Pelvic Med ReconstrSurg 2017; 23:27) 9. Beer M, Kuhn A. Surgical techniques for vault prolapse: a review of the literature. Eur J Obstet Gynecol ReprodBiol 2005; 119:
5 10. Maher CF, Murray CJ, Carey MP, Dwyer PL, Ugoni AM. Iliococcygeus or sacrospinous fixation for vaginal vault prolapse. Am J Obstet Gynecol 2001; 98: Lin TY, Su TH, Wang YL, Lee MY, Hsieh CH, Wang KG, Chen GD. Risk factors for failure of transvaginal sacrospinous uterine suspension in the treatment of uterovaginal prolapse. J Formos Med Assoc (4): Maher CF, Qatawneh AM, Dwyer PL, et al. Abdominal sacral colpopexy or vaginal sacrospinous colpopexy for vaginal vault prolapse: a prospective randomized study. Am J Obstet Gynecol 2004; 190: Lantzsch T, Goepel C, Wolters M, et al. Sacrospinous ligament fixation for vaginal vault prolapse. Arch Gynecol Obstet 2001; 265: Nieminen K, Huhtala H, Heinonen P. Anatomic and functional assessment and risk factors of recurrent prolapse after vaginal sacrospinous fixation. Acta Obstet Gynecol Scand : Bracken JN, Tran DH, Kuehl TJ, Larsen W, Yandell PM, Shull BL. A novel transvaginal approach to correct recurrent apical prolapse after failed sacral colpopexy: case series. IntUrogynecol J 2012;23: Toh VV, Bogne V, Bako A. Management of recurrent vault prolapse. IntUrogynecol J 2012;23: Maher C, Baessler K, Glazener C, Adams E, Hagen S. Surgical management of pelvic organ prolapse in women: A short version Cochrane review. NeurolUrodyn 2008; 27: Chmielewski L, Walters MD, Weber AM, et al. Reanalysis of a randomized trial of 3 techniques of anterior colporrhaphy using clinically relevant definitions of success. Am J Obstet Gynecol 2011;205:69. e Jessica N. Bracken, Diana H. Tran, Thomas J. Kuehl. A novel transvaginal approach to correct recurrent apical prolapse after failed sacral colpopexy: case series IntUrogynecol J 2012; 23: Submitted for publication: Accepted for publication: After Revision When Imam Ali was asked about Faith in Religion, he replied that the structure of faith is supported by four pillars endurance, conviction, justice and jihad. Hazrat Ali (Karmulha Wajhay) 48
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
The UK National Prolapse Survey: 10 years on
 Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
University College Hospital
 University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Surgery for women with apical vaginal prolapse(review)
 Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
Safety and short term outcomes of a new truly minimallyinvasive mesh-less and dissection-less anchoring system for pelvic organ prolapse apical repair
 ORIGINAL ARTICLE Vol. 43 (3): 533-539, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0356 Safety and short term outcomes of a new truly minimallyinvasive mesh-less and dissection-less anchoring system
ORIGINAL ARTICLE Vol. 43 (3): 533-539, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0356 Safety and short term outcomes of a new truly minimallyinvasive mesh-less and dissection-less anchoring system
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse
 SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Polypropylene vaginal mesh implants for vaginal prolapse
 Polypropylene vaginal mesh implants for vaginal prolapse This statement has been developed and reviewed by the Women s Health Committee and approved by the RANZCOG Board and Council. A list of Women s
Polypropylene vaginal mesh implants for vaginal prolapse This statement has been developed and reviewed by the Women s Health Committee and approved by the RANZCOG Board and Council. A list of Women s
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Recent advances in POP. Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany
 Recent advances in POP Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany Level of pelvic floor support Level I apical Level II transverse/ horizontal Level
Recent advances in POP Dr. Bernhard Uhl Department for Obstetrics and Gynecology St. Vinzenz-Hospital Dinslaken Germany Level of pelvic floor support Level I apical Level II transverse/ horizontal Level
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
Scottish Clinical Coding Standards
 Scottish Clinical Coding Standards Number 16 October 2017 Scottish Clinical Coding Standards ICD-10 Sepsis Sepsis is a serious condition which must always be coded when documented in the medical record.
Scottish Clinical Coding Standards Number 16 October 2017 Scottish Clinical Coding Standards ICD-10 Sepsis Sepsis is a serious condition which must always be coded when documented in the medical record.
Surgical management of pelvic organ prolapse in women(review)
 Cochrane Database of Systematic Reviews Surgical management of pelvic organ prolapse in women (Review) MaherC,FeinerB,BaesslerK,SchmidC MaherC,FeinerB,BaesslerK,SchmidC. Surgical management of pelvic organ
Cochrane Database of Systematic Reviews Surgical management of pelvic organ prolapse in women (Review) MaherC,FeinerB,BaesslerK,SchmidC MaherC,FeinerB,BaesslerK,SchmidC. Surgical management of pelvic organ
Index. Cyclical pelvic pain, 37 Cystocele, 22, 23, 25, 48, 51, 52, 54, 56, 124, 148, 160
 A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO
 AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
AN AMERICAN UROGYNECOLOGIC SOCIETY (AUGS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR SURGICAL PROCEDURES TO TREAT PELVIC ORGAN PROLAPSE NEED FOR A WORKING
HYSTERECTOMY FOR BENIGN CONDITIONS
 UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
PROLAPSE. By Charlotte Robinson Women s Health Speciality Attachment
 PROLAPSE. By Charlotte Robinson Women s Health Speciality Attachment Introduction Case example Pelvic organ prolapse - Epidemiology - Aetiology - Anatomy - Types of prolapse/ severity - Examination/Investigation
PROLAPSE. By Charlotte Robinson Women s Health Speciality Attachment Introduction Case example Pelvic organ prolapse - Epidemiology - Aetiology - Anatomy - Types of prolapse/ severity - Examination/Investigation
Bilateral sacrospinous fixation after second recurrence of vaginal vault prolapse:
 Bilateral sacrospinous fixation after second recurrence of vaginal vault prolapse: efficacy and impact on quality of life and sexuality. Salvatore Giovanni Vitale 1, Diego Rossetti 2, Marco Noventa 3,
Bilateral sacrospinous fixation after second recurrence of vaginal vault prolapse: efficacy and impact on quality of life and sexuality. Salvatore Giovanni Vitale 1, Diego Rossetti 2, Marco Noventa 3,
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Surgical management of pelvic organ prolapse in women (Review)
 Surgical management of pelvic organ prolapse in women (Review) Maher C, Feiner B, Baessler K, Glazener CMA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Surgical management of pelvic organ prolapse in women (Review) Maher C, Feiner B, Baessler K, Glazener CMA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Are effective nonsurgical treatments available for women with pelvic organ prolapse?
 Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
Are effective nonsurgical treatments available for women with pelvic organ prolapse? For women with asymptomatic prolapse, education and reassurance are appropriate. Women may not realize that symptoms
HYSTERECTOMY FOR BENIGN CONDITIONS
 HYSTERECTOMY FOR BENIGN CONDITIONS UnitedHealthcare Oxford Clinical Policy Policy Number: SURGERY 104.7 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
HYSTERECTOMY FOR BENIGN CONDITIONS UnitedHealthcare Oxford Clinical Policy Policy Number: SURGERY 104.7 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Options for Vaginal Prolapse. What is prolapse? What is prolapse? Disclosures 10/23/2013. Michelle Y. Morrill, M.D. None
 Options for Vaginal Prolapse Disclosures None Michelle Y. Morrill, M.D. Director of Urogynecology Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department of Ob/Gyn, UCSF What is prolapse?
Options for Vaginal Prolapse Disclosures None Michelle Y. Morrill, M.D. Director of Urogynecology Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department of Ob/Gyn, UCSF What is prolapse?
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
American Journal of Obstetrics and Gynecology
 American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Pelvic Health Coding & Payment Quick Reference
 Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
Payer policies will vary and should be verified prior to treatment for limitations on diagnosis, coding or site of service requirements. The coding options listed within this guide are commonly used codes
Total vs Subtotal Hysterectomy
 Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
ISSN (o): Sacrospinous fixation: an efficient technique for prevention and treatment of vault prolapse
 Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Management of Urogenital Prolapse of Women in Primary Care. Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner
 Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases.
 Research Article http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases. Hasan Çılgın*
Research Article http://www.alliedacademies.org/research-and-reports-in-gynecology-and-obstetrics Effects of uterus-preserving surgical modalities on sexual functions in total prolapsus cases. Hasan Çılgın*
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Imaging of Pelvic Floor Weakness. Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne
 Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Imaging of Pelvic Floor Weakness Dr Susan Kouloyan-Ilic Radiologist Epworth Medical Imaging The Women s, Melbourne Outline Overview and Epidemiology Risk Factors, Causes and Results Review of Relevant
Female Urology. Young-Suk Lee, Deok Hyun Han, Ji Youl Lee 1, Joon Chul Kim 2, Myung-Soo Choo 3, Kyu-Sung Lee
 www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October :00-18:00
 Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October 2012 14:00-18:00 Start End Topic Speakers 14:00 14:30 Introduction, Evidence and Applied Anatomy Salma Kayani 14:30 14:50 Applied Anatomy
Reconstructive Pelvic Floor Surgery: Sacrocolpopexy W43, 16 October 2012 14:00-18:00 Start End Topic Speakers 14:00 14:30 Introduction, Evidence and Applied Anatomy Salma Kayani 14:30 14:50 Applied Anatomy
Surgery for vaginal vault prolapse. Patient decision aid
 Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Advances in Bioscience and Clinical Medicine ISSN:
 Advances in Bioscience and Clinical Medicine ISSN: 2203-1413 www.abcmed.aiac.org.au Review Paper Adaptation of Pelvic Organ Prolapse Guideline in Iranian Adult Women Parvin Bastani, Fateme Mallah, Leili
Advances in Bioscience and Clinical Medicine ISSN: 2203-1413 www.abcmed.aiac.org.au Review Paper Adaptation of Pelvic Organ Prolapse Guideline in Iranian Adult Women Parvin Bastani, Fateme Mallah, Leili
Bilateral iliococcygeal fixation for vaginal vault prolapse and enterocele repair using a new suturing device the digital needle driver
 BJOG: an International Journal of Obstetrics and Gynaecology August 2005, Vol. 112, pp. 1145 1149 DOI: 10.1111/j.1471-0528.2005.00616.x SURGICAL TECHNIQUE Bilateral iliococcygeal fixation for vaginal vault
BJOG: an International Journal of Obstetrics and Gynaecology August 2005, Vol. 112, pp. 1145 1149 DOI: 10.1111/j.1471-0528.2005.00616.x SURGICAL TECHNIQUE Bilateral iliococcygeal fixation for vaginal vault
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
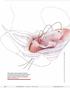 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
Thesis. Reference. To mesh or not to mesh: a review of pelvic organ reconstructive surgery. DAELLENBACH, Patrick Peter
 Thesis To mesh or not to mesh: a review of pelvic organ reconstructive surgery DAELLENBACH, Patrick Peter Abstract Pelvic organ prolapse (POP) is a major health issue with a lifetime risk of undergoing
Thesis To mesh or not to mesh: a review of pelvic organ reconstructive surgery DAELLENBACH, Patrick Peter Abstract Pelvic organ prolapse (POP) is a major health issue with a lifetime risk of undergoing
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation in Treatment of Vaginal Vault Prolapse
 ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
Dear Mrs. Burch and editors of the BMJ,
 Dear Mrs. Burch and editors of the BMJ, We are pleased that our manuscript entitled: Sacrospinous hysteropexy versus vaginal hysterectomy with uterosacral ligament suspension in women with uterine prolapse
Dear Mrs. Burch and editors of the BMJ, We are pleased that our manuscript entitled: Sacrospinous hysteropexy versus vaginal hysterectomy with uterosacral ligament suspension in women with uterine prolapse
Anterior six arms prolene mesh for high stage vaginal prolapse: five years follow-up
 ORIGINAL ARTICLE Vol. 43 (3): 525-532, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0482 Anterior six arms prolene mesh for high stage vaginal prolapse: five years follow-up Luis Gustavo M. de Toledo
ORIGINAL ARTICLE Vol. 43 (3): 525-532, May - June, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0482 Anterior six arms prolene mesh for high stage vaginal prolapse: five years follow-up Luis Gustavo M. de Toledo
SGS Annual Course in Advanced Gynecologic Surgery New Orleans, LA
 SGS Annual Course in Advanced Gynecologic Surgery New Orleans, LA Thursday, November 29 Royal Sonesta New Orleans 7:00 7:20 am Registration and Continental Breakfast 7:20 7:30 am Welcome and Opening Remarks
SGS Annual Course in Advanced Gynecologic Surgery New Orleans, LA Thursday, November 29 Royal Sonesta New Orleans 7:00 7:20 am Registration and Continental Breakfast 7:20 7:30 am Welcome and Opening Remarks
Laparoscopic Uterine Conservation in Uterovaginal Prolapse
 SMGr up Laparoscopic Uterine Conservation in Uterovaginal Prolapse Hasan Cilgin Medicine Faculty of Kafkas University, Kars, Turkey *Corresponding author: Hasan Cilgin, Medicine Faculty of Kafkas University,
SMGr up Laparoscopic Uterine Conservation in Uterovaginal Prolapse Hasan Cilgin Medicine Faculty of Kafkas University, Kars, Turkey *Corresponding author: Hasan Cilgin, Medicine Faculty of Kafkas University,
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of uterine suspension using mesh (including sacrohysteropexy) to repair uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of uterine suspension using mesh (including sacrohysteropexy) to repair uterine prolapse
Pelvic Floor. Reimbursement & Coding Guide
 Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Pelvic Floor Reimbursement & Coding Guide Pelvic Floor Reimbursement and Coding Guide ACell Pelvic Floor Matrix products are biologically-derived devices comprised of porcine Urinary Bladder Matrix (UBM),
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Le Forts partial colpocleisis: a review of one surgeons experience
 Gynecol Surg (2004) 1:15 19 DOI 10.1007/s10397-004-0006-3 ORIGINAL ARTICLE Amanda J. O Leary Sanjay K. Vyas Le Forts partial colpocleisis: a review of one surgeons experience Published online: 13 February
Gynecol Surg (2004) 1:15 19 DOI 10.1007/s10397-004-0006-3 ORIGINAL ARTICLE Amanda J. O Leary Sanjay K. Vyas Le Forts partial colpocleisis: a review of one surgeons experience Published online: 13 February
Eric R. Sokol, MD. Bio. CLINICAL OFFICES Gynecology Clinic 900 Blake Wilbur Dr. Palo Alto, CA Tel (650) Fax (650) BIO
 CLINICAL OFFICES Gynecology Clinic 900 Blake Wilbur Dr Bio Palo Alto, CA 94304 Associate Professor of Obstetrics and Gynecology (Gynecology-Urogynecology) and, by courtesy, of Urology at the Stanford University
CLINICAL OFFICES Gynecology Clinic 900 Blake Wilbur Dr Bio Palo Alto, CA 94304 Associate Professor of Obstetrics and Gynecology (Gynecology-Urogynecology) and, by courtesy, of Urology at the Stanford University
