BLADDER CANCER PATIENT GUIDEBOOK FOR PATIENTS FACING RADICAL CYSTECTOMY
|
|
|
- Oswald Vincent Hart
- 6 years ago
- Views:
Transcription
1 BLADDER CANCER PATIENT GUIDEBOOK FOR PATIENTS FACING RADICAL CYSTECTOMY
2 WHAT S IN THIS GUIDEBOOK? YOU ARE NOT ALONE What causes bladder cancer?....3 Muscle-invasive bladder cancer...3 Understanding how the body works..3 The urinary system... 3 The intestinal system... 4 Staging and grading your bladder cancer How will my cancer be treated?...5 Questions to ask your surgeon The bladder is gone now what?....6 Ileal Conduit (Ostomy) Orthotopic Neobladder... 6 Indiana Pouch... 7 Common issues following radical cystectomy surgery...7 Chemotherapy...7 Preparing for the surgery...8 What to expect after your surgery...8 Returning home Eating and nutrition... 8 Bowel care... 9 Exercise Emotions At home with your Ileal Conduit...9 At home with your Neobladder At home with your Indiana Pouch.. 10 A lifetime of checkups Where else can I get information?.. 11 How can I help others? This Patient Guidebook was created by people just like you bladder cancer patients and their caregivers. It s designed to offer you support, encouragement and tips on how to deal with the procedures and treatments for your bladder cancer. It can help you understand your disease and what to expect, the treatments you may be offered and how to manage your disease in the years ahead. We are not medical professionals and you should always turn to your medical team for advice first. But we have been where you are now and have experienced what you are feeling. To ensure accuracy, this Guidebook has been reviewed by a team of medical professionals. This Guidebook will talk about common approaches to treating muscle-invasive bladder cancer (MIBC). Keep in mind that there can be some differences, depending on the practices of your medical team and on your specific situation. We will not be using a lot of medical language, except where it might help you better communicate with your medical team and understand your disease. You ll find a handy glossary of terms on Bladder Cancer Canada s website at Remember, you re not alone. All of us at Bladder Cancer Canada are passionate about helping you to live a full and satisfying life even after a diagnosis of bladder cancer. We re doing it and so can you. The birth of this guidebook What you are about to read is the result of the creative vision of the late Greg Neely, who was Vice-President of Bladder Cancer Canada and a bladder cancer patient himself. Greg saw the need for a single source of information written from the viewpoint of Canadian bladder cancer patients and their caregivers. He wanted it clear, simple, and easy to understand that s Greg s style.
3 WHAT CAUSES BLADDER CANCER? As with many types of cancer, one of the leading risk factors of the disease is smoking. Those who smoke may be up to four times more likely to get bladder cancer. People who work with certain chemicals may also be at risk leather workers, hairdressers, mechanics and painters, among other occupations. Exposure to radiation has also been linked to bladder cancer. Caucasian men may also be at greater risk. THE URINARY SYSTEM The body takes nutrients from food and changes the nutrients to energy. After the body takes the nutrition that it needs, waste products are left behind in the blood and in the bowel. The urinary system removes the waste product called urea from the blood. Urea is made when foods containing protein (meats and some vegetables) are broken down in the body and carried in the blood to the kidneys. But the simple truth is that many will develop bladder cancer for no known reason. You may be one of those people. At this point, asking why is not nearly as helpful as focusing on what now. Many of us never knew bladder cancer existed before our diagnosis. But, it s more common than you might think, as it s the 5th most common cancer in Canada. MUSCLE-INVASIVE BLADDER CANCER Approximately 25% of bladder cancers are muscleinvasive. It means that cancer tumours have grown through the lining of the bladder into or through the bladder muscle. In most cases, this type of cancer is treated through surgery to remove the bladder (called a radical cystectomy ) and to create a new path for urine to leave the body. We ll explore the treatments in more depth as we go along. UNDERSTANDING HOW THE BODY WORKS Radical cystectomy is a big operation involving two body systems the urinary and the intestinal systems. The more we understand about how the two systems work, the better our recovery will be. Here s a brief description of these two vital systems. Our two kidneys: Remove liquid waste from the blood in the form of urine Balance salts and other substances in the blood Help regulate blood pressure Make erythropoietin, a hormone that helps make red blood cells Parts of the urinary system: The kidneys remove urea from the blood through tiny filtering units called nephrons. Urea, water and other waste substances make the urine as they pass through the nephrons and down the renal tubules of the kidney. The two ureters are narrow tubes that carry urine from the kidneys to the bladder. Muscles in the ureter walls continually tighten and relax forcing urine downward, away from the kidneys. If urine backs up, or is allowed to stand still, it can lead to kidney infection, damage, or failure. About every 10 to 15 seconds, small amounts of urine are emptied into the bladder from the ureters. 3
4 The bladder is a triangle-shaped, hollow organ located in the lower abdomen. It is held in place by ligaments that are attached to other organs and the pelvic bones. The bladder s muscle walls relax and expand to store urine, and contract and flatten to empty urine through the urethra. Two, circular sphincter muscles help keep urine from leaking out of the body by closing tightly like a rubber band around the opening of the bladder. Nerves in the bladder alert a person when it is time to urinate, or empty the bladder. The urethra is the tube that allows urine to pass outside the body. The brain signals the bladder muscles to tighten, which squeeze urine out of the bladder. At the same time, the brain signals the sphincter muscles to relax to let urine exit the bladder through the urethra. When all the signals occur in the correct order, normal urination occurs. THE INTESTINAL SYSTEM The intestines are a long, continuous tube running from the stomach to the opening where the stool leaves the body (anus). Most absorption of nutrients and water happen in the intestines, which include the small intestine, large intestine, and rectum. The small intestine (small bowel) is about 20 feet long and about an inch in diameter. Its job is to absorb most of the nutrients from what we eat and drink. Velvety tissue lines the small intestine, which is divided into the duodenum, jejunum, and ileum. The large intestine (colon or large bowel) is about 5 feet long and about 3 inches in diameter, and creates formed stool, once the nutrients are absorbed. As stool enters the rectum, nerves there create the urge to have a bowel movement. STAGING AND GRADING YOUR BLADDER CANCER Laboratory analysis of the material taken out during your Transurethral Resection of Bladder Tumour (TURBT) is used to determine the type and stage of the cancer. According to the Canadian Cancer Society, staging classifies a cancer based on its extent in the body. STAGING Tis Carcinoma in situ (flat tumour), sometimes called Cis. Ta Non-invasive papillary carcinoma. T1 The tumour is in the first layer of the bladder lining, but not the surrounding muscle. T2 The tumour has grown into the muscle. In stage T2a, the tumour is in the inner half of the muscle layer and in stage T2b, the outer half. T3 The tumour has spread to the fatty layer around the bladder muscle. T3a describes a microscopic tumour and T3b a large tumour that can be seen or felt. T4 The tumour has spread to organs outside the bladder (T4a) or to the wall of the abdomen or pelvis (T4b). Bear in mind that it can be somewhat difficult for your medical team to know the true extent of your tumour without surgery. That s because there may be a difference between clinical staging and pathological staging. The TURBT is part of the clinical staging process, which is done before treatment. Clinical staging also includes a physical exam, imaging tests (such as a CAT scan), laboratory tests (such as blood tests), and biopsies (such as those done following the TURBT). A cancer can be further staged by examining the material removed during a radical cystectomy. This process is called pathologic staging. Complete staging combines the results of the clinical staging with the surgical results. 4
5 GRADING In addition to showing what stage your cancer is, the pathology report following your TURBT will also generally show whether your tumour is high grade or low grade. A higher-grade cancer may grow and spread more quickly and may require immediate or more aggressive treatment. Your diagnosis of muscle-invasive bladder cancer may be based on the finding of high-grade tumours. IMPORTANT Keep a copy of the pathology report which will tell you the stage and grade of your tumour. HOW WILL MY CANCER BE TREATED? Although in selected patients, treatments to preserve the bladder (such as combined chemotherapy plus radiation and complete TURBT) may be an option, the majority of patients with muscle-invasive bladder cancer will be treated with radical cystectomy major surgery to remove the diseased bladder and to construct a new urinary diversion. (Refer to the Guidebook on Bladder Preservation for more information). In men, the surgeon will remove the bladder, prostate, seminal vesicles and pelvic lymph nodes, usually a dozen or more. In women, the surgeon may remove not only the bladder, but also the uterus, ovaries, fallopian tubes, cervix, front wall of the vagina and pelvic lymph nodes. For both men and women, the surgeon may also remove the urethra, depending on which diversion is to be created. QUESTIONS TO ASK YOUR SURGEON BEFORE SURGERY Can you explain the stage and grade of my cancer and what that means for my treatment? What are all the guideline-recommended treatment options for bladder cancer? Do you construct neobladders and Indiana Pouches as well as ileal conduits? (You ll find more information about these surgeries on the following pages.) Will I need chemotherapy? What kind of follow-up will I require from you? What limitations will this surgery impose on my life (physical, emotional, sexual)? What are the common complications of surgery and long- term effects of the disease? Are there any patients of yours with whom I can speak who have had this surgery? Am I able to obtain a second opinion from a major cancer/ teaching centre? Am I able to obtain a second opinion from a major cancer/teaching centre? When you meet with your surgeon, take a family member or close friend with you to take notes and to be a listening ear. You ll miss some of the information if you are by yourself. Write down questions you want the surgeon to answer before you get there so that you don t forget them. You could even ask permission to record the interview so that you can replay the questions and answers when you get home. 5
6 THE BLADDER IS GONE NOW WHAT? Once the bladder is removed, your surgeon needs to create a new way for the urine to drain from the kidneys to outside the body. The options are called diversions. In Canada, three diversions are common ileal conduit, orthotopic neobladder and Indiana Pouch. You will want to discuss these with your surgeon to understand which is appropriate for you and why. ILEAL CONDUIT (OSTOMY) The surgeon will take a short segment of the ileum (part of the small intestine) to create a channel for the urine to pass out of the body. The remaining bowel is sewn back together. The two ureters from the kidneys which drain the urine are attached to this segment and an opening in the right side of the abdomen is created, called a stoma. A removable bag, called a urostomy pouch, is affixed to the skin surrounding the stoma to catch the continuous flow of urine. Advantages: Shorter and relatively simple surgery, fewer potential complications, shorter segment of bowel re-purposed. Disadvantages: Must always wear an external pouch to collect urine, possible skin irritation/breakdown around stoma, infections, body image issues, potential for odour, potential for leaks. ORTHOTOPIC NEOBLADDER The surgeon will create a new bladder out of a longer segment of small intestine in the same place as the old, diseased bladder was. This neobladder will be attached to the ureters from the kidneys and also attached to the urethra so that voiding urine is done as before. The neobladder is not a muscle like your original bladder was, and does not have the same fullness sensations as does a bladder, so you must learn how to hold your urine (become continent) and how to effectively empty it using the pelvic muscles. Advantages: Near normal function, no body image issues, no external pouches, no odours. Disadvantages: Incontinence (as some may never regain full control), the inability to empty the neobladder (some may need to use a catheter daily to empty the neobladder), longer surgery time, potential for restricted flow. 6
7 INDIANA POUCH The surgeon will take a segment of large intestine and a small portion of the ileum to make an internal pouch into which the ureters flow. The short piece of small intestine is brought to the surface of the abdomen (the stoma). There is no external pouch and the stoma is very small, and can be covered with a bandage. A catheter inserted into the stoma is used several times per day to empty the pouch. 6. Erectile dysfunction in men (you need to discuss potential treatments for this with your surgeon) 7. Painful intimacy in women 8. Body image issues 9. Anxiety 10. Feeling different 11. Mucus in urine (which is continually produced by the intestinal section used to make the diversion) is unsightly and can potentially cause blockage and the need for catheterization CHEMOTHERAPY Before removing the bladder, chemotherapy (or chemo ) is often recommended (called neoadjuvant chemotherapy ). The purpose of the treatment prior to surgery is to stop the disease from spreading through the blood or lymph system to other parts of the body and to reduce the tumours. In addition, chemotherapy is usually better tolerated prior to major surgery. Advantages: No external pouch, no odours, no body image issues. Disadvantages: Longer surgery time, the need for catheterization, possible risk of leakage from the stoma, scarring of the stoma making catherization difficult, stones in the pouch. COMMON ISSUES FOLLOWING RADICAL CYSTECTOMY SURGERY Radical cystectomy and creating a urinary diversion is major abdominal surgery. As with all major surgeries, some issues are bound to arise. Some of them gradually disappear and others you adapt to over time. 1. Temporary loss of appetite 2. Reduced energy 3. Fatigue 4. Loss of weight 5. Infections Not everyone is a candidate for pre-operative chemotherapy, however, and in such cases, it may be advisable to have postsurgery chemotherapy (called adjuvant chemotherapy ). If lymph nodes are affected by the cancer, the oncologist may recommend adjuvant chemotherapy to combat further spread. The risk is that patients may decline post-surgery chemotherapy. This can happen for a number of reasons, including the fear of side effects, weakness and fatigue from the surgery itself, or thinking that the cancer is gone so chemotherapy is not necessary. Chemotherapy has side effects which can be unpleasant and these must be taken into account by both you and your doctor. However, since the goal is to extend life with good quality, you should make an informed decision, based on the recommendation of your doctor. SIDE EFFECTS OF CHEMOTHERAPY Side effects of chemotherapy will depend on the type of drug used and the dose, how the drug is given and your overall health. They can happen any time during or after chemotherapy. Most side effects go away when chemotherapy is over, although some side effects may be longer-lasting or even be permanent. Some of the most common side effects of chemotherapy drugs are fatigue, nausea, changes to blood cell counts (increasing the risk of infection), loss of appetite, effects on bowel movements and urination, and hair loss. It s important to let your medical team know of any side effects that you experience, because many of them can be treated. And, hair usually grows back after treatments have stopped. 7
8 IMPORTANT Don t hesitate to call Bladder Cancer Canada and ask to speak with someone who has had the surgery you are preparing to receive. We have many peer support volunteers who will answer any questions you have, based on their own experience and acquired knowledge. It s a big help to chat with someone who has been in your shoes and is surviving and thriving. We know. We have been there! CLINICAL TRIALS In addition to the therapies approved by Health Canada, you may be able to access other bladder cancer therapies through a clinical trial. A clinical trial is a research study that tests how well a new medical approach works in people. Each study answers scientific questions and tries to find better ways to prevent, screen for, diagnose, or treat a disease such as bladder cancer. By participating in a clinical trial, you ll be helping researchers answer important questions that will further the development of new effective treatments. Clinical trials may also provide you with another option in your treatment plan. Clinical trial websites will help you find clinical trials that may be available in your area. Here s one website you can check: This site lists Canadian trials only. You can narrow your search by selecting bladder cancer under Select a Cancer Type. You may need to select Show More if bladder cancer does not display on the list you see. You can also search by province, city or trial centre. It s very important that you discuss with your medical team whether a clinical trial is right for you. PREPARING FOR THE SURGERY WHAT TO BRING TO THE HOSPITAL Slip-on shoes or slippers you ll be walking a lot Some books to read Tear-away sports pants to use when you tire of the hospital gown A list of all your medications You should not bring valuables into the hospital that may be lost or stolen WHAT TO EXPECT AFTER YOUR SURGERY As you can see, radical cystectomy is very major surgery and you ll have a lengthy recovery. Many parts of the body are affected during the surgery and need time to heal. On average, your hospital stay will be 5 to 10 days. Walking starts the day after surgery. This helps the bowels to start working again. Remember, this is bowel surgery too, not just bladder surgery! Expect to be on a liquid diet for the first few days before solid foods are gradually introduced. While in hospital, you ll have a number of IV lines and tubes, depending on your type of surgery. These will provide pain control, urine drainage and drainage of excess fluid from the surgical site. RETURNING HOME AFTER SURGERY It s not unusual for your weight to change during your hospital stay and first few weeks at home. There will be some muscle and fat weight loss, but there could be some weight gain through fluid retention. The excess fluid will gradually be cleared by the kidneys. You ve had major surgery, so your recovery will be gradual. Keep a record of your progress how many and what length of walks you ve taken (even walks in the hallways of your home count). You may also need soft, small icepacks (your groin area will be swollen for a while, which is a normal part of healing). In men, the scrotum, which contains the testicles, may swell considerably. It s important to keep the incision clean and dry until it heals, Home care is usually ordered to check on dressings and change them and to remove the stitches or staples. If you have any issues, call the surgeon s office or urologist on call. If you develop a fever, go to the nearest Emergency Room as soon as possible (it may be an indication of infection). EATING AND NUTRITION You ll need to eat small, frequent meals, which are easier on the healing bowels and shrunken stomach. You must drink at least 64 ounces of water (eight 8-ounce glasses of water or other liquids) per day. This is necessary to keep the kidneys clear, keep mucus thinner and easier to pass and not block up anywhere, and keep stools softer and easier to pass. Mucus will continue to be produced by the parts of the intestines that were used for the diversion, probably forever. So, drinking lots of water will become a lifetime commitment. Soups and stews are easy to digest, easier on the healing bowels and the easiest way to keep high nutrition for healing (try grating vegetables into soups or stews). For the first weeks, avoid fats and high-fibre foods, like popcorn and raw or undercooked vegetables. 8
9 BOWEL CARE You ll need to keep your stool soft as the bowel heals. Daily stool softeners may be recommended by your surgeon (they re available over the counter at drug stores). You ll want to limit straining while having a bowel movement to help the bowel heal, avoid putting a strain on the stitches or staples and reduce the risk of haemorrhoids. If you are constipated, some fibre intake may help, but it also means drinking plenty of water, as the fibre needs lots of water to work as a softener (the fibre can cause constipation if you don t drink enough water). There are cases where a blockage can occur in the bowel, often at the point where the sections of the bowel were re-joined during surgery. Walking a lot will help and sometimes chewing gum is recommended. EXERCISE The bowels need gentle physical activity to start working again. Walking is the best form of exercise for the first six weeks to three months the body s healing time. EMOTIONS Your emotions can best be described as a rollercoaster. That s perfectly normal after all, you ve been diagnosed with cancer, you ve had major abdominal surgery, and you re faced with a new lifestyle. It helps to have supportive family and friends around you. Don t be afraid to express your emotions by talking to others who ve gone through what you are. Contact us at Bladder Cancer Canada and we can put you in touch with someone. Our contact information is on the back of this Guidebook. Focus on your task recovery and creating a new lifestyle. Remember, your positive attitude will be a key element in your recovery. AT HOME WITH YOUR ILEAL CONDUIT (OSTOMY) The first week after your surgery your stoma may be tender and may be dark or bruised, swollen or blister-like or have spongy or yellow tissue around it. This tissue will peel off in a few days and start to look more normal. You ll also notice stitches attaching it to your skin. These will be absorbed on their own and the swelling should go down in three or four weeks. A normal healthy stoma looks soft, moist, red or pink and shiny. The skin around your stoma should look like the rest of the skin on your abdomen. It should be free of rashes, redness, scratches and bruising. If the stoma becomes irritated, get in touch with your stoma nurse, as there are products to help. Your nurses in the hospital or home care will teach you how to empty, clean and change your new urine collection pouch and how to set up a night collection system. Once your stoma size has stabilized, you ll determine the correct size for your urostomy bag, using the stoma measuring devices supplied by the ET nurse and the ostomy supply companies in their sample kits. 9
10 If your stoma is round, experienced patients recommend using an external bag with an opening pre-cut to size. This avoids trying to precision cut a round hole not easy and certainly not fun! Many of us find that a onepiece appliance (another name for the urostomy bag, also called a pouch) is easier to handle than a two-piece unit with a flange and then adding the bag, which is much bulkier. But try them both. Another tip for men, suspenders are a lot easier on the appliance and the area around the stoma than a belt. Again, this is something that you will try and work with and find what combination best works for you. Supplies are available at home healthcare or other medical supply stores. Experiment with different ostomy products and contact the providers as they have patient support personnel who can help. Major suppliers include Hollister ( and Coloplast ( Both companies offer free samples of their products. AT HOME WITH YOUR NEOBLADDER Neobladder patients are typically sent home with two tubes a catheter in the urethra and a suprapubic catheter in the abdomen, both helping drain the new neobladder. Your nurses in the hospital or home care will teach you how to flush the tubes to clear mucus. This flush needs to be done at regular intervals, as recommended by your medical team, usually about every four hours day and night. It doesn t hurt to flush more frequently. You should seek immediate medical attention if you are unable to flush the mucus and urine through the tubes there may be a blockage. Since you will be sleeping with urine collection bags attached to tubes, experiment until you find a comfortable sleeping position. You may need something to sleep in other than pyjamas, because of the restrictions of the tubes. AT HOME WITH YOUR INDIANA POUCH The first week after your surgery your stoma may look dark or bruised, look swollen or blister-like or have spongy or yellow tissue around it. This tissue will peel off in a few days and start to look more normal. A normal healthy stoma looks soft, moist, red or pink and shiny and should be flush with the skin. The skin around your stoma should look like the rest of the skin on your abdomen. It should be free of rashes, redness, scratches and bruising. Typically, patients are sent home with a suprapubic catheter in the abdomen and possibly a small tube in the new stoma, both helping drain the pouch of urine and mucus for several weeks. Your nurses in the hospital or homecare will also teach you how to take care of your stoma and catheterize your new Indiana Pouch, once the tubes are taken out. Usually, you will begin by catheterizing every two hours for the fi t week or so, gradually increasing the time between catheterizations as the pouch begins to stretch. Catheters are available at home healthcare or other medical supply stores. A LIFETIME OF CHECKUPS Of course, it s a great relief to hear your doctor say the words all clear after your first checkup. However, that s not the end of this chapter of your life. You ll need regular checkups, usually including CT scans and blood work. These checkups will be more frequent at first and gradually reduced to one or two a year for the rest of your life to ensure early detection should the cancer come back. With careful attention to your lifestyle, you can live a healthy life. Be encouraged. Be diligent. And choose to help someone else who faces this diagnosis to look ahead with a positive attitude. After the tubes are removed in a few weeks, it s normal to have incontinence and you may need to wear disposable underwear or pads. Daytime continence usually returns, but night time incontinence can be a lifetime issue. Lots of patience is essential. Washable bed protectors (available at home healthcare or medical supply stores) and incontinence pants are often necessary. 10
11 WHERE ELSE CAN I GET INFORMATION? The Bladder Cancer Canada website ( has a wealth of information, including links to other reliable websites. The Internet provides lots of information, some of it is accurate and helpful and some inaccurate and anything but helpful. However, many world-class cancer centres provide information on line that may help you. But the best source of information in your specific case is your own medical team. If you are uncertain about your doctor s advice, you are entitled to a second opinion. Please speak to your family doctor or Bladder Cancer Canada about who you can be referred to. HOW CAN I HELP OTHERS? WALK WITH US Each September, in many cities across Canada, Bladder Cancer Canada organizes Awareness Walks. The walks allow us to tell Canadians about this common cancer. Walk participants can also collect sponsors, to raise much-needed funds to provide support, spread awareness and aid in research. You can walk, raise money among your family and friends, or volunteer to help coordinate the day s activities at your local walk. SPREAD THE WORD Tell your friends, family and healthcare providers about bladder cancer and Bladder Cancer Canada. You can also speak with others who are on this journey with bladder cancer and prove to be an encouragement and a lifeline to them. To find out how you can help or to get help yourself go to the Bladder Cancer Canada website at Our website has excellent and reliable discussion forums where you can ask questions or share. You can also sign up for our e-newsletter to stay up-to-date on upcoming events or research news. We wish you every success in your journey with bladder cancer. Let us know how we can help you. That s why we re here. HELPFUL WEBSITES: Bladder Cancer Canada Mayo Clinic - diseases-conditions/bladder-cancer/ basics/definition/con Cleveland Clinic - org/urology-kidney/diseases-conditions/ bladder-cancer.aspx Johns Hopkins Bladder Cancer Advocacy Network (BCAN US) - Canadian Cancer Society - cancer.ca/en/cancer-information/ cancer-type/bladder/bladder-cancer/ Canadian Urological Association National Cancer Institute (US) types/bladder Cornell Urology clinical-conditions/bladder-cancer/ 11
12 ABOUT BLADDER CANCER CANADA Bladder Cancer Canada was formed in 2009 by bladder cancer survivors. We are a national charity with a mission to: Help bladder cancer patients and their support teams address the day-to-day issues of this disease Increase awareness of bladder cancer among the general public and medical community Fund research which pursues the diagnosis, treatment and elimination of bladder cancer. Bladder cancer awareness among Canadians is at a relatively early stage. There is little public awareness of the symptoms of the disease and, unless diagnosed with this cancer, most people are not well educated about it. Bladder Cancer Canada creates awareness about this cancer since an early diagnosis usually results in a better outcome. For more information, visit Contact us: Bladder Cancer Canada 4936 Yonge St, Suite 1000 Toronto, ON M2N 6S3 info@bladdercancercanada.org or call us at You can also follow us on /BladderCancerCanada /BladderCancerCA /BladderCancerCanada SPECIAL THANK YOU NOTES We d like to thank those who took part in the production and review of this guidebook: Greg Neely, Jack Moon, Ieva Fraser, Ed Moffat, Valerie MacLeod, Elixir Marketing Inc., Tarik Alam RN, Dr. Bobby Shayegan, Tammy Northam and David Guttman. The project manager and editor of the Patient Guidebook series is Stephen Wilson. We are grateful to AstraZeneca, Merck and Roche, whose generous financial support has made this guidebook possible. bladdercancercanada.org P03E Revised November 2017
BLADDER CANCER PATIENT GUIDEBOOKOK
 BLADDER CANCER PATIENT GUIDEBOOKOK BLADDER PRESERVATION STRATEGIES FOR MUSCLE-INVASIVE BLADDER CANCER WHAT S IN THIS GUIDEBOOK? What causes bladder cancer?.... 3 Muscle-invasive bladder cancer.............
BLADDER CANCER PATIENT GUIDEBOOKOK BLADDER PRESERVATION STRATEGIES FOR MUSCLE-INVASIVE BLADDER CANCER WHAT S IN THIS GUIDEBOOK? What causes bladder cancer?.... 3 Muscle-invasive bladder cancer.............
PATIENT GUIDEBOOK FOR PATIENTS WITH NONMUSCLE-INVASIVE BLADDER CANCER
 BLADDER CANCER PATIENT GUIDEBOOK FOR PATIENTS WITH NONMUSCLE-INVASIVE BLADDER CANCER YOU ARE NOT ALONE WHAT S IN THIS GUIDEBOOK? Nonmuscle-invasive Bladder Cancer...3 What causes bladder cancer?.... 3
BLADDER CANCER PATIENT GUIDEBOOK FOR PATIENTS WITH NONMUSCLE-INVASIVE BLADDER CANCER YOU ARE NOT ALONE WHAT S IN THIS GUIDEBOOK? Nonmuscle-invasive Bladder Cancer...3 What causes bladder cancer?.... 3
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Cystectomies and bladder preservation: What you need to know
 Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
Cystectomies and bladder preservation: What you need to know Robin Morash RN, BNSc, MHS Bladder Cancer Canada November 21, 2018 Presentation goals Review the options for treatment of muscle-invasive bladder
UNDERSTANDING BLADDER CANCER
 UNDERSTANDING BLADDER CANCER Learn About Your Treatment Options After Your Diagnosis If your doctor has told you that you have bladder cancer, you likely have many questions and concerns. Learning about
UNDERSTANDING BLADDER CANCER Learn About Your Treatment Options After Your Diagnosis If your doctor has told you that you have bladder cancer, you likely have many questions and concerns. Learning about
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
BCAN Fall Series: Survivorship
 BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
BCAN Fall Series: Survivorship The New Normal after Bladder Removal and Urinary Diversion Vashti Livingston RN, MS, CNS, CWOCN Ambulatory Urology MSKCC NYC livingsv@mskcc.org Disclosure None BCAN Volunteer
Radical Prostatectomy
 2014 Radical Prostatectomy Radical Prostatectomy What is a radical prostatectomy? During a radical prostatectomy, the entire prostate gland, the part of the urethra that it surrounds, and the seminal vesicles
2014 Radical Prostatectomy Radical Prostatectomy What is a radical prostatectomy? During a radical prostatectomy, the entire prostate gland, the part of the urethra that it surrounds, and the seminal vesicles
SAMPLE. What Is a Urostomy? Your Child s Urostomy
 What Is a Urostomy? An ostomy is a surgically created opening in the abdomen for the discharge of body waste. Ostomies that discharge urine are urostomies. After the ostomy is created, your child will
What Is a Urostomy? An ostomy is a surgically created opening in the abdomen for the discharge of body waste. Ostomies that discharge urine are urostomies. After the ostomy is created, your child will
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients
 Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Cystectomy and Bladder Reconstruction (Continent Urinary Diversion) Department of Urology Information for patients i Introduction You and your consultant have decided that you need a cystectomy (removal
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~
 Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Understanding Women's Sexuality after Bladder Cancer webinar. Part I: The Physical Impact
 Understanding Women's Sexuality after Bladder Cancer webinar Tuesday, December 1, 2015 Part I: The Physical Impact Presented by LaShon Day received her Masters of Science as a Physician s Assistant at
Understanding Women's Sexuality after Bladder Cancer webinar Tuesday, December 1, 2015 Part I: The Physical Impact Presented by LaShon Day received her Masters of Science as a Physician s Assistant at
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Urinary stoma. This is the simplest and most straightforward form of
 This is the simplest and most straightforward form of urinary drainage following surgery to remove the bladder (cystectomy). You may see it referred to as a urostomy, an ileal conduit or urinary diversion.
This is the simplest and most straightforward form of urinary drainage following surgery to remove the bladder (cystectomy). You may see it referred to as a urostomy, an ileal conduit or urinary diversion.
Patient & Family Guide. Bowel Surgery.
 Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Robotic Prostatectomy - After Surgery
 PATIENT EDUCATION patienteducation.osumc.edu Robotic Prostatectomy - After Surgery Here are general guidelines for home after your surgery. Your doctor may give you other instructions based on your needs
PATIENT EDUCATION patienteducation.osumc.edu Robotic Prostatectomy - After Surgery Here are general guidelines for home after your surgery. Your doctor may give you other instructions based on your needs
preparing for surgery
 preparing for surgery Facing the news that you need to have a stoma is very difficult but with thousands of people having stoma surgery each year, it is important to remember that you are not alone and
preparing for surgery Facing the news that you need to have a stoma is very difficult but with thousands of people having stoma surgery each year, it is important to remember that you are not alone and
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
Surgery. In this fact sheet. Surgery: English
 Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
RADICAL PROSTATECTOMY
 Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Tennyson Centre Suite 19 520 South Road Kurralta Park SA 5037 P 08 8292 2399 F 08 8292 2388 admin@urologicalsolutions.com.au www.urologicalsolutions.com.au Darwin Private Hospital Suite 5 Rocklands Drive
Retropubic Prostatectomy
 2014 Retropubic Prostatectomy Retropubic Prostatectomy What is the prostate? The prostate is a gland that makes a fluid that helps sperm move. It also gives nourishment for the sperm. It is about the size
2014 Retropubic Prostatectomy Retropubic Prostatectomy What is the prostate? The prostate is a gland that makes a fluid that helps sperm move. It also gives nourishment for the sperm. It is about the size
LAPAROSCOPIC HERNIA REPAIR
 LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
Your Bowel Operation Hartmanns Procedure
 Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment
 Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Expectations and Post Op Instructions: Robotic Cystectomy / Ileal Conduit.
 Expectations and Post Op Instructions: Robotic Cystectomy / Ileal Conduit. You are about to undergo a major operation. The healing process takes time and we would like for you to observe the following
Expectations and Post Op Instructions: Robotic Cystectomy / Ileal Conduit. You are about to undergo a major operation. The healing process takes time and we would like for you to observe the following
Robotic Prostatectomy - After Surgery
 PATIENT EDUCATION patienteducation.osumc.edu Robotic Prostatectomy - After Surgery Here are general guidelines for home after your surgery. Your doctor may give you other instructions based on your needs
PATIENT EDUCATION patienteducation.osumc.edu Robotic Prostatectomy - After Surgery Here are general guidelines for home after your surgery. Your doctor may give you other instructions based on your needs
A word about incontinence
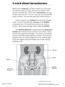 A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
BLADDER CANCER CONTENT CREATED BY. Learn more at
 BLADDER CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK TO YOUR DOCTOR Table of Contents WHAT IS BLADDER CANCER? 4 TYPES OF BLADDER CANCER 5 GRADING AND STAGING 8 TREATMENT OVERVIEW
BLADDER CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK TO YOUR DOCTOR Table of Contents WHAT IS BLADDER CANCER? 4 TYPES OF BLADDER CANCER 5 GRADING AND STAGING 8 TREATMENT OVERVIEW
Lee Jackson, M.D. Post-Operation Information and Instructions
 Post-Operation Information and Instructions While a robotic prostatectomy is performed routinely, it is still a relatively major surgery that will take some time and effort to recover from. The following
Post-Operation Information and Instructions While a robotic prostatectomy is performed routinely, it is still a relatively major surgery that will take some time and effort to recover from. The following
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Bladder Cancer Canada November 21st, Bladder Cancer 2018: A brighter light at the end of the cystoscope
 Bladder Cancer Canada November 21st, 2018 Bladder Cancer 2018: A brighter light at the end of the cystoscope Chris Morash MD FRCSC Associate Professor, University of Ottawa Head, Urological Oncology Bladder
Bladder Cancer Canada November 21st, 2018 Bladder Cancer 2018: A brighter light at the end of the cystoscope Chris Morash MD FRCSC Associate Professor, University of Ottawa Head, Urological Oncology Bladder
Neurogenic Bladder: What You Should Know. A Guide for People with Spinal Cord Injury
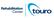 Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
SPECIAL EDITION: Men s Health
 SPECIAL EDITION: Men s Health 1 Heart Health If you re like most Americans, heart health might be something you don t think about very often. You should. The risk of heart disease increases with age and
SPECIAL EDITION: Men s Health 1 Heart Health If you re like most Americans, heart health might be something you don t think about very often. You should. The risk of heart disease increases with age and
Discussions about Mitrofanoff
 Discussions about Mitrofanoff This booklet provides general supporting information, alongside clinical information, which will be provided by your Doctor or Specialist Nurse. What is a Mitrofanoff? A Mitrofanoff,
Discussions about Mitrofanoff This booklet provides general supporting information, alongside clinical information, which will be provided by your Doctor or Specialist Nurse. What is a Mitrofanoff? A Mitrofanoff,
Sacrospinous Vault Suspension
 gynaecology program Pre- and Post-operative Instructions: Sacrospinous Vault Suspension Informed Consent As part of informed consent, your doctor will talk to you about: What will be done during the surgery
gynaecology program Pre- and Post-operative Instructions: Sacrospinous Vault Suspension Informed Consent As part of informed consent, your doctor will talk to you about: What will be done during the surgery
Appendicitis. Diagnosis and Surgery
 Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
BLADDER HEALTH. Muscle Invasive Bladder Cancer: A Patient Guide
 BLADDER HEALTH Muscle Invasive Bladder Cancer: A Patient Guide Table of Contents Bladder Cancer Expert Panel Mike's Story: A Patient Story.... Introduction.... GET THE FACTS What is bladder cancer?....
BLADDER HEALTH Muscle Invasive Bladder Cancer: A Patient Guide Table of Contents Bladder Cancer Expert Panel Mike's Story: A Patient Story.... Introduction.... GET THE FACTS What is bladder cancer?....
WHAT TYPES OF CONTINENCE PRODUCTS ARE THERE?
 15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
Inflammatory Bowel Disease. Your Illness and Its Treatment
 Inflammatory Bowel Disease Your Illness and Its Treatment What Is Inflammatory Bowel Disease? Inflammatory bowel disease (IBD) is inflammation (irritation and swelling) of the digestive tract. Your digestive
Inflammatory Bowel Disease Your Illness and Its Treatment What Is Inflammatory Bowel Disease? Inflammatory bowel disease (IBD) is inflammation (irritation and swelling) of the digestive tract. Your digestive
Limited Bowel Resection. Surgery for Crohn s Disease
 Limited Bowel Resection Surgery for Crohn s Disease What Is Crohn s Disease? Crohn s disease is inflammation (irritation and swelling) of the digestive tract. Crohn s disease occurs anywhere from the mouth
Limited Bowel Resection Surgery for Crohn s Disease What Is Crohn s Disease? Crohn s disease is inflammation (irritation and swelling) of the digestive tract. Crohn s disease occurs anywhere from the mouth
BLADDER CANCER: PATIENT INFORMATION
 BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Open Radical Prostatectomy Surgery
 To learn about radical prostatectomy surgery, you will need to know these words: The prostate is the sexual gland that makes fluid to help sperm move around. The prostate surrounds the urethra at the neck
To learn about radical prostatectomy surgery, you will need to know these words: The prostate is the sexual gland that makes fluid to help sperm move around. The prostate surrounds the urethra at the neck
Urinary Tract Infections
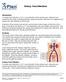 Urinary Tract Infections Introduction A urinary tract infection, or UTI, is an infection of the urinary tract. Infections are caused by microbes, including bacteria, fungi and viruses. Microbes are organisms
Urinary Tract Infections Introduction A urinary tract infection, or UTI, is an infection of the urinary tract. Infections are caused by microbes, including bacteria, fungi and viruses. Microbes are organisms
Returning Home After Prostatectomy
 Returning Home After Prostatectomy Catholic Medical Center in conjunction with Manchester Urology Associates is proud to be one of the few hospitals in the United States to offer Robotic Assisted radical
Returning Home After Prostatectomy Catholic Medical Center in conjunction with Manchester Urology Associates is proud to be one of the few hospitals in the United States to offer Robotic Assisted radical
Pathology Driving Decisions
 Pathology Driving Decisions Part I: Understanding Your Diagnosis and Your Treatment Options May 7, 2018 Presented by: Dr. Matthew Mossanen completed his college and medical school training at UCLA. He
Pathology Driving Decisions Part I: Understanding Your Diagnosis and Your Treatment Options May 7, 2018 Presented by: Dr. Matthew Mossanen completed his college and medical school training at UCLA. He
Bowel cancer. In this fact sheet: Page 1 of 13 Macmillan fact sheet 2017: Bowel cancer. Bowel Cancer: English
 Bowel Cancer: English Bowel cancer This information is about bowel cancer and treatments for bowel cancer. Any words that are underlined are explained in the word list at the end. If you have any questions,
Bowel Cancer: English Bowel cancer This information is about bowel cancer and treatments for bowel cancer. Any words that are underlined are explained in the word list at the end. If you have any questions,
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients
 Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Trans Urethral Resection of Bladder Tumour (TURBT) Department of Urology Information for Patients i Why do I need a trans urethral resection of bladder tumour Your recent cystoscopy has shown a growth
Continence Promotion. CATHETER CARE CONTINENCE CARE CONVEENS STOMAS
 Continence Promotion. 1 CATHETER CARE CONTINENCE CARE CONVEENS STOMAS CHARACTERISTICS OF URINE 2 A liquid excrement consisting of water, salts, and urea, which is made in the kidneys then released through
Continence Promotion. 1 CATHETER CARE CONTINENCE CARE CONVEENS STOMAS CHARACTERISTICS OF URINE 2 A liquid excrement consisting of water, salts, and urea, which is made in the kidneys then released through
A VIDEO SERIES. living WELL. with kidney failure LIVING WELL
 A VIDEO SERIES living WELL with kidney failure LIVING WELL Contents 2 Introduction 3 What will I learn? 5 Who is on my healthcare team? 6 Who is affected by kidney failure? 6 How does kidney failure affect
A VIDEO SERIES living WELL with kidney failure LIVING WELL Contents 2 Introduction 3 What will I learn? 5 Who is on my healthcare team? 6 Who is affected by kidney failure? 6 How does kidney failure affect
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Regaining sexual activity after major bowel surgery. Advice for women
 Regaining sexual activity after major bowel surgery Advice for women How does major bowel surgery affect women? Bowel surgery is often major surgery and it can affect women and their partners in different
Regaining sexual activity after major bowel surgery Advice for women How does major bowel surgery affect women? Bowel surgery is often major surgery and it can affect women and their partners in different
Breast Surgery. Breast Surgery
 Words to know... The breast area has many parts: fibrous tissue glandular tissue fat lymph channels and nodes Fibrous tissue anchors the breast to the chest and provides structural support for the breast.
Words to know... The breast area has many parts: fibrous tissue glandular tissue fat lymph channels and nodes Fibrous tissue anchors the breast to the chest and provides structural support for the breast.
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
A Patient s Guide to HIVEC Treatment HIVECTM
 A Patient s Guide to HIVEC Treatment HIVECTM Contents Pages 1. Understanding Bladder Cancer 1. Understanding Bladder Cancer 2. Tumour Stages 3. What is HIVEC Treatment? 4. How Does it Work? 5. Before Your
A Patient s Guide to HIVEC Treatment HIVECTM Contents Pages 1. Understanding Bladder Cancer 1. Understanding Bladder Cancer 2. Tumour Stages 3. What is HIVEC Treatment? 4. How Does it Work? 5. Before Your
MY surgery: There are two common types of surgery for colon cancer. The one you receive depends on the stage and location of your tumour.
 MY surgery: - There are two common types of surgery for colon cancer. The one you receive depends on the stage and location of your tumour. In addition to explaining both options, this section gives you
MY surgery: - There are two common types of surgery for colon cancer. The one you receive depends on the stage and location of your tumour. In addition to explaining both options, this section gives you
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
In-patient brachytherapy for gynaecological cancer. Cancer Services Information for patients
 In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
In-patient brachytherapy for gynaecological cancer Cancer Services Information for patients i Introduction This booklet provides information about brachytherapy (a type of internal radiotherapy). We hope
Bladder Cancer. Understanding your diagnosis cancer.ca
 Bladder Cancer Understanding your diagnosis 1 888 939-3333 cancer.ca Bladder Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed
Bladder Cancer Understanding your diagnosis 1 888 939-3333 cancer.ca Bladder Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
Pelvic Floor Muscle Exercises and Advice for Men Why are my pelvic floor muscles important? Your pelvic floor muscles are important for bladder and bowel control. These muscles help to keep the bladder
After Adrenal Cancer Treatment
 After Adrenal Cancer Treatment Living as a Cancer Survivor For many people, cancer treatment often raises questions about next steps as a survivor. Lifestyle Changes After Treatment for Adrenal Cancer
After Adrenal Cancer Treatment Living as a Cancer Survivor For many people, cancer treatment often raises questions about next steps as a survivor. Lifestyle Changes After Treatment for Adrenal Cancer
TURBT (Transurethral Resection of the Bladder Tumour)
 TURBT (Transurethral Resection of the Bladder Tumour) Exceptional healthcare, personally delivered Trans Urethral Resection of Bladder Tumour (TURBT) This leaflet answers some of the questions you may
TURBT (Transurethral Resection of the Bladder Tumour) Exceptional healthcare, personally delivered Trans Urethral Resection of Bladder Tumour (TURBT) This leaflet answers some of the questions you may
My Urinary Catheter Passport Looking after my urinary catheter
 Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Managing your suprapubic catheter
 Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Managing your suprapubic catheter What you need to know The information contained in this booklet is intended to assist you in understanding your proposed surgery. Not all of the content will apply to
Laparoscopic Gastric Bypass Information
 1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
URINARY DIVERSIONS. Winter 2016 Dr P. O Malley
 URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
URINARY DIVERSIONS Winter 2016 Dr P. O Malley OVERVIEW Who gets diversions? What s involved with cystectomy? What are the different types of diversions? What are the problems with various diversions? How
Quick Facts about Ampullary Cancer
 Quick Facts about Ampullary Cancer What is the Ampulla of Vater? Princess Margaret The liver, gallbladder and pancreas produce important fluids to help you digest food. These fluids are carried through
Quick Facts about Ampullary Cancer What is the Ampulla of Vater? Princess Margaret The liver, gallbladder and pancreas produce important fluids to help you digest food. These fluids are carried through
The Infant/Child with a Bowel Ostomy
 The Infant/Child with a Bowel Ostomy Thank you for choosing the Medical College of Georgia Hospitals and Clinics for your child s health care needs. This information is to help answer some of the questions
The Infant/Child with a Bowel Ostomy Thank you for choosing the Medical College of Georgia Hospitals and Clinics for your child s health care needs. This information is to help answer some of the questions
Beyond Cancer Moving On
 Beyond Cancer Moving On Today, people with cancer have a better chance at living a normal life than ever before in history. In fact, there are more than 10 million survivors people who have, or are living
Beyond Cancer Moving On Today, people with cancer have a better chance at living a normal life than ever before in history. In fact, there are more than 10 million survivors people who have, or are living
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
What is a Colonoscopy?
 What is a Colonoscopy? A colonoscopy is a test to look inside your colon. A colonoscopy is done by a gastroenterologist, a doctor trained in looking at the gastrointestinal (GI) tract. The main tool used
What is a Colonoscopy? A colonoscopy is a test to look inside your colon. A colonoscopy is done by a gastroenterologist, a doctor trained in looking at the gastrointestinal (GI) tract. The main tool used
Diverticular Disease Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
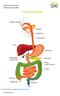 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Diverticular Disease Diverticulum refers to a side-branch or pouch which sticks outwards from the wall
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Diverticular Disease Diverticulum refers to a side-branch or pouch which sticks outwards from the wall
Managing your bladder with a Supra-pubic catheter at home
 Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Managing your bladder with a Supra-pubic catheter at home Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. Managing your bladder with a Supra-pubic catheter at home The purpose
Surgery Choices for Breast Cancer
 Surgery Choices for Breast Cancer Surgery Choices for Women with DCIS or Breast Cancer As a woman with DCIS (ductal carcinoma in situ) or breast cancer that can be removed with surgery, you may be able
Surgery Choices for Breast Cancer Surgery Choices for Women with DCIS or Breast Cancer As a woman with DCIS (ductal carcinoma in situ) or breast cancer that can be removed with surgery, you may be able
UNDERSTANDING. Permanent Birth Control for Men
 UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
UNDERSTANDING VASECTOMY Permanent Birth Control for Men Is Vasectomy for You? Vasectomy is a simple, safe procedure that makes a man sterile (unable to father a child). It s the most effective birth control
Inguinal hernias may be present from birth but may not become evident until later in life. They are usually more common in men.
 This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
1st stage neuromodulation test
 1st stage neuromodulation test Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 12 This leaflet is to give you some background information
1st stage neuromodulation test Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 12 This leaflet is to give you some background information
Part II: Treatment. A Woman-to-Woman Talk with Dr. Armine Smith. Wednesday, March 8, Presented by
 Women & Bladder Cancer A Woman-to-Woman Talk with Dr. Armine Smith Wednesday, March 8, 2017 Part II: Treatment Presented by Dr. Smith is an Assistant Professor of Urology at Johns Hopkins University and
Women & Bladder Cancer A Woman-to-Woman Talk with Dr. Armine Smith Wednesday, March 8, 2017 Part II: Treatment Presented by Dr. Smith is an Assistant Professor of Urology at Johns Hopkins University and
Robot Assisted Total Laparoscopic Hysterectomy
 Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Robot Assisted Total Laparoscopic Hysterectomy What is a robot assisted total laparoscopic hysterectomy? It is the removal of the uterus, including the cervix, through four small (1/2-1 ) abdominal incisions
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
ABDOMINAL PERINEAL RESECTION
 ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~
 Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter An organ in the body that makes urine. Most people have
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter An organ in the body that makes urine. Most people have
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
Colectomy. Surgical treatment for Ulcerative Colitis (UC) and Familial Adenomatous Polyposis (FAP) Patient and Family Education
 Patient and Family Education Colectomy Surgical treatment for Ulcerative Colitis (UC) and Familial Adenomatous Polyposis (FAP) A colectomy is a surgery that removes the colon, or large intestine. The colectomy
Patient and Family Education Colectomy Surgical treatment for Ulcerative Colitis (UC) and Familial Adenomatous Polyposis (FAP) A colectomy is a surgery that removes the colon, or large intestine. The colectomy
Complex Care Hub Manual Bowel Ostomies: Ileostomy, Jejeunostomy, Colostomy
 Complex Care Hub Manual Bowel Ostomies: Ileostomy, Jejeunostomy, Colostomy Table of Contents 1. Overview of the gastrointestinal tract... 2 2. What is a stoma/ostomy?... 2 2.1 What is a Jejeunostomy?...3
Complex Care Hub Manual Bowel Ostomies: Ileostomy, Jejeunostomy, Colostomy Table of Contents 1. Overview of the gastrointestinal tract... 2 2. What is a stoma/ostomy?... 2 2.1 What is a Jejeunostomy?...3
Lower Anterior Resection (LAR) with Ileostomy
 Lower Anterior Resection (LAR) with Ileostomy Information for patients and families UHN Read this information to learn: what an LAR with ileostomy is how to care for yourself when you get home what problems
Lower Anterior Resection (LAR) with Ileostomy Information for patients and families UHN Read this information to learn: what an LAR with ileostomy is how to care for yourself when you get home what problems
Surgery for Polyps or Colon Cancer (Updated 10.08)
 S PATIENT INFORMATION oregon surgical specialists Surgery for Polyps or Colon Cancer (Updated 10.08) Colon cancer is cancer of the large intestine, or colon. The colon is a muscular tube that forms the
S PATIENT INFORMATION oregon surgical specialists Surgery for Polyps or Colon Cancer (Updated 10.08) Colon cancer is cancer of the large intestine, or colon. The colon is a muscular tube that forms the
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
Muscle-invasive bladder cancer
 Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? The most common type of bladder cancer is non muscle-invasive,
Patient Information English 4 Muscle-invasive bladder cancer The underlined terms are listed in the glossary. What is muscle-invasive bladder cancer? The most common type of bladder cancer is non muscle-invasive,
Quick facts about gallbladder cancer
 Quick facts about gallbladder cancer What is the gallbladder? Princess Margaret The gallbladder is a small, pear-shaped organ located under right side of the liver. The gallbladder concentrates and stores
Quick facts about gallbladder cancer What is the gallbladder? Princess Margaret The gallbladder is a small, pear-shaped organ located under right side of the liver. The gallbladder concentrates and stores
