排尿障礙治療中心版權所有. Physiotherapy of Lower Urinary Tract Dysfunction.
|
|
|
- Horace Mills
- 6 years ago
- Views:
Transcription
1 Physiotherapy of Lower Urinary Tract Dysfunction
2 Lower Urinary Tract Dysfunction Urinary Incontinence Stress, urge, or mixed incontinence Frequency urgency syndrome Spastic urethral sphincter syndrome Poor relaxation of urethral sphincter Pelvic pain syndrome Chronic eliminative syndrome
3 Therapeutic modalities Medical treatment Surgical treatment Behavioral therapy Physiotherapy Electrical stimulation Biofeedback PFMT Neuromodulation Neurostimulation
4 Functional Electrical Stimulation Restoration of normal physiological reflex mechanisms in abnormal nerves and muscles Black torpedo fish in 46 AD Bors (1952) electrostimulation of pelvic floor Caldwell (1965) anal and urinary incontinence by electrical stimulator Alexander & Rowan (1968) electrodes on vaginal pessary Suhel (1975) integrated automatic vaginal stimulator
5 Neuromuscular Electrical stimulation Excitation of peripheral nerves using short pulses, adequate intensity and duration Current amplitude (intensity) Pulse width (duration) Pulse rise time Pulse repetition rate (frequency)
6 Types of Waveform
7 Muscle Fatigue Skeletal muscle is composed of aerobic slow contracting motor units and anaerobic fast contracting units Resistance to fatigue is inversely correlated to aerobic oxidative capacity At high frequency electrical stimulation the muscle fatigues rapidly due to impaired neuromuscular transmission and sarcolemmal excitation
8 Skeletal muscles Motor striated muscles are composed of slow, intermediate, and fast contracting muscles, fast muscle has times more contraction force than slow fibers Intramural urethral sphincter small slow muscle fibers Periurethral pelvic floor muscles all types of muscles Provocative situation fast fibers of PFM action to close urethra
9 Muscle Activity Plasticity of metabolic and functional properties of muscles Following denervation, muscles lose enzymatic difference Immobilization induced muscle atrophy Disuse atrophy the muscle response is weak and rapid fatigue
10 Chronic nerve stimulation To modify physiologic and metabolic characteristics of normal & atrophied muscles Transform fast to slow myosin subunits that are more fatigue resistance Anaerobic fast muscle turns into slow muscle with a high capacity for energy supply by aerobic oxidative process Increase myoglobin and mitochondria content Increase in capillary density
11 Muscle Transformation after Nerve Stimulation Transformation of fast to slow twitch muscles is progressive with the duration of stimulation The most extensive changes occur between 60 and 90 days The total number of fibers remains constant Intermittent phasic high frequency stimulation (40 to 60 Hz) induces transformation similar to that after low-frequency (10Hz) stimulation The reverse process occurs by inactivity and chronic immobilization
12 Pelvic Floor Muscle Stimulation Induces a reflex contraction of striated para- and periurethral muscles and a simultaneous reflex inhibition of detrusor contraction A sacral reflex arc and peripheral innervation must be intact No effect can be expected in complete lower motor neuron lesions
13 Nerve Stimulation for Urethral Closure Direct stimulation of efferent pudendal nerves Activation of efferent hypogastric fibers can contract smooth urethral muscles Efferent stimulation of pelvic nerves can increase intraluminal urethral pressure and increase urethral length Stimulation of pelvic floor afferents from anogenital muscles and mucosa may activate pelvic floor muscles through reflex connection
14 Nerve Stimulation for Bladder Inhibition A feedback system is present in micturition process Detrusor instability may be caused by ineffective inhibition by sphincter Intravaginal or pudendal nerve stimulation of sufficient intensity causes a complete bladder relaxation The higher intensity the more efficient bladder is inhibited via spinal reflex mechanism
15 Nerve Stimulation for Bladder Relaxation Maximal bladder inhibition is obtained at 2x to 3x of threshold intensity Relaxation of detrusor is accompanied by tightening of bladder neck fibers Detrusor inhibition after nerve stimulation may be caused by balance between cholinergic (M2,3-receptors) and beta-adrenergic adrenergic (B3- receptors) neurotransmission After maximal stimulation, high beta-adrenergic adrenergic activity and decreased cholinergic activity in rabbit detrusor strips
16 Chronic Pelvic Floor Stimulation Chronic long-term stimulation of anal and urethral sphincters applies relatively weak electrical impulses for 3 to 12 months Fast motor units are recruited first Increase frequency of slow-twitch fibers Accelerated sprouting of surviving motor units of partially denervated pelvic floor muscles High frequency ( Hz) is advised in treating stress incontinence
17 Selection of Electrical Parameters Patient adapt to current intensity within a few minutes The stimulation is constructed to increase current intensity from 0 to maximum within a few minutes A pulse length of 0.5 to 1.0 minutes is optimal to muscle contraction Biphasic pulses give 30% to 40% better therapeutic response than monophasic pulses
18 Selection of Frequency of Electrical Stimulation Maximal detrusor inhibition is obtained with a frequency of 5 Hz No difference in MUCP change in the range of Hz Good therapeutic results in stress and urge incontinence with a fixed frequency of 25 Hz Intermittent ES is superior to continuous ES to avoid muscle fatigue during long-term stimulation The most effective rest period is 3 times longer than active period
19 Functional ES for Stress urinary incontinence Successful pelvic floor stimulation was reported in % women with incontinence Patients without previous incontinence surgery have the best result Urodynamic parameters change little after functional ES for SUI Patients with SUI may have a better pelvic floor muscle contractility after ES that results in increased urethral resistance during stress
20 Long-term electrostimulation At least 6 to 8 hours daily ES is needed either anally or vaginally A treatment period of 3 to 6 months is necessary to achieve success Kegel exercises should be followed after discontinuing FES to keep pelvic floor muscles in optimal condition Treatment combined with estrogen is recommended in menopause women Mechanical vaginal mucosal irritation may occur in atrophic vaginitis
21 Short-term term Maximal stimulation Intact reflex arc must be present Maximal ES can inhibit overactive detrusor muscle, can be an alternative in treating detrusor overactivity and urge incontinence 5 to10 Hz can give optimal inhibitory effect The current intensity is successively increased below pain level of patient Duration of maximal ES is 15 to25 minutes, 4 to 10 repetitions daily for 2 to 3 days
22 Therapeutic Results after Short- term electrostimulation Successful maximal ES for pelvic floor in female urge incontinence was reported to be 52 to 92% A recurrence rate of 25% after discontinuing maximal ES in urge UI Recurrence rate of 15% within 1 year Success rate of 75% in recurrent urge urinary incontinence Repeat stimulation is needed for recurrence
23 Electrical Stimulation for SUI Transvaginal ES has been used for genuine SUI, urge and mixed urinary incontinence Reported efficacy ranges 35 to70% A placebo-controlled controlled study revealed after 15- week treatment course, pad usage diminished by >50% in 62% women compared to 19% in sham device, incontinence episode reduced >50% in 48% women compared to 13% in sham device
24 Transvaginal electrical stimulation Low frequency (20 Hz) was applied Contrasting data of effects on genuine SUI Transvaginal ES is effective in urge UI First line treatment for women with pure urge incontinence For the women with mixed type UI who does not wish to undergo PME or surgery
25 Transvaginal electrical simulator
26 Transvaginal electrical stimulation for Urge incontinence Leach reported 6% after long period of stimulation McGuire observed improvement in 93% women with urge incontinence Plevnik found 52% improved (30% cured) in pure urge incontinence Brubaker used 20 Hz frequency current and cured 49% with urodynamic DI Smith found ES reduced urine loss by 50% in 20women Sand reported 38% success rate in 20 women with DI
27 Contraindication of ES Heart pacemakers Pregnancy women Urethral obstruction and overflow incontinence Complete peripheral denervation Urinary tract infection Uterine prolapse or high grade cystocele Low compliance and cooperation of patient
28 Biofeedback Detectable or measurable response: bladder pressure or pelvic floor muscle activity A detectable response A perceptible cue : sensation of urge or tightness Active involvement of a motivated patient
29 Biofeedback for LUTD Fail to inhibit detrusor contraction Fail to adequately contract striated urethral sphincter of the pelvic floor Failed to relax the urethral sphincter or pelvic floor muscles during micturition Chronic pelvic pain due to hypertonicity of pelvic floor muscles
30 Cystometry biofeedback for urge incontinence For women who failed electrical stimulation, were intolerant to anticholinergics, Urodynamic detrusor overactivity was proven Performed several voluntary PFMC at episodes of DI while watching CMG tracing and EMG activity Try to inhibit urge incontinence as longer duration as possible at home
31 Bladder biofeedback Train patients to inhibit detrusor contraction voluntarily and to contract periurethral muscles selectively Bladder pressure biofeedback to treat urge incontinence by watching intravesical pressure rise during CMG 81% improvement rate was reported and 36% success rate at 5 year follow-up
32 Detrusor overactivity and CMG biofeedback
33 Biofeedback to inhibit detrusor instability
34 Pelvic Floor Muscle Biofeedback Vaginal manometry by perineometry Kegel reported a 90% improvement rate Vaginal electromyography in 8 week program 80% younger and 67% older group reported no more incontinence Anal sphincter biofeedback by perineal surface EMG or rectal probe
35 陰道壓力儀
36 Pelvic floor hypertonicity & overactivity Etiology Persistence of a reaction phase to noxious stimulus of LUTS (e.g. inflammation, infection, irritation, post-surgery) surgery) learned dysfunctional voiding behavior Persistent transitional phase in the development of micturition control Sexual abuse
37 Clinical presentation Dysfunctional voiding Increased pelvic floor activity during voiding Urgency frequency, poor stream, intermittency, hesitancy Urinary retention Constipation Pelvic or perianal pain Certain pelvic pain (e.g. interstitial cystitis, prostatodynia, urethral syndrome) is associated with pelvic floor hypertonicity
38 -diet regulation -drinking and voiding chart -pharmacotherapy Bladder dysfunction -incontinence -reflux -mucosal ischaemia Pelvic floor dysfunction Overtraining of the pelvic floor muscles Biofeedback electrical stimulation manual technique -milk-back of urine -residual urine -pelvic pain
39 Aims of physical therapy To improve dietary and micturition routine To improve proprioception and body awareness of PF: focus on relaxing the PF and voluntary sphincter control To decrease any associated hypertonicity or pain in the PF To optimize functional use of PF
40 Evaluation A complete history Frequency /volume chart for 3 days Neurological examination (lower quarter) proprioception,, sensation Peripheral reflexes Physical examination PF function: Rectal /vaginal tone, contractility, endurance, ability to contract and relax PF voluntarily,, relation between PF & adjacent pelvic viscera pelvic pain: trigger point, tenderness Sacroiliac & coccygeal position /mobility
41 Behavioral modification Instruction on urinary system and PF dysfunction Diet: avoid bladder stimulants, high fiber adequate daily intake of water General recommendations for changing wrong voiding behavior take time for micturition, do not push Instruct a proper toilet posture: sit for voiding every time (men also) no straining timed voiding (3 ½~4 hours)
42 Manual technique To restore sacroiliac & sacrococcygeal alignment To improve proprioceptive awareness Muscle energy technique Proprioceptive technique: direct pressure, tapping, use of stretch reflex To decrease tension and promote relaxation of the musculature Massage Trigger point pressure Myofascial release
43
44 Clinical effectiveness Standford CA internal myofascial release, 18 sessions hypertonus & pain in type III chronic prostatitis Jerome MW myofascial release, weeks 83% urgency-frequency syndrome symptom relief & hypertonus 70% interstitial cystitis
45 Pelvic floor exercise (PME) with EMG biofeedback Convert pelvic floor/urethral sphincter activity into visual or auditory signal Goal: to help identify pelvic floor musculature to perceive difference between contraction, relaxation, and straining to voluntary relax & control pelvic floor
46 EMG biofeedback: children with dysfunctional voiding Anal plug or surface electrode on perineal skin Protocol: a short submaximal contraction (3 sec) a prolonged relaxation (30 sec) for 30 times with diaphragmatic breathing progress: increase holding time (10 s) followed by prolonged relaxation (30 s)
47 PME with EMG biofeedback Intravaginal/ / intra-anal anal EMG sensor Glazer Protocol 1. One minute rest, pre baseline 2. Five rapid contraction (flicks) with 10-s s rest between each 3. Five 10-s s contractions with 10-s s rest between each (tonic) 4. A single endurance contraction of 60-s 5. One minute rest, post baseline
48
49 劉 xx,40y/o for PME training first time
50 劉 xx,40y/o for PME training 3month
51 Home program: 5-s s contraction/10-s s relaxation 60 repetitions twice daily progress to 10-s s contraction/10-s s relaxation Functional application in corresponding situation during daily life practice in different posture practice relaxation during voiding anticipate urge situation by submaximal PF contraction EMG + uroflowmetry Cystometric biofeedback : cyclic filling
52 Clinical effect For dyfunctional voiding 51-83% improve for the long term follow up normal flow curve & good pelvic floor relaxation no significant residual urine improve constipation decrease occurrences of UTI For pelvic pain % pain relief in levator syndrome - 83% pain relief in vulvovaginal pain
53 Additional treatment for other urological symptoms Detrusor instability: anticholinergic drugs Recurrent UTI: antibiotics Chronic constipation regulation of diet bowel training drug therapy * Neuman et al: UTIs were largely resolved after treating obstipation
54 Important factors for success Motivation and cooperation Appropriate selection of patients intact nervous system Biofeedback training (Deindal( et al): Improvement in women with inappropriate pubococcygeal activity Not in those with urethral sphincter repetitive discharge
55 Other Non-surgical Therapies for Incontinence Vaginal cones are a method of biofeedback 70% (19/27) with mild SUI had complete or >50% improvement after vaginal cone therapy, 7/50 with severe SUI had similar success rate Electrostimulation of pudendal nerve (prolonged pudendal nerve conduction velocity in 97% SUI) is effective in 62% with SUI and 20% were dry Electromagnetic stimulation
56 Multiple purposes Electrostimulator and Biofeedback
57 Patient visualization & biofeedback
58 Clinical effect Magnus et al: interstitial cystitis, 54% benefit from suprapubic TENS Park et al: Prostatodynia,, 20Hz, anal plug, pain and muscle spasm in 18 sessions Walsh et al: irritative voiding syndrome, 1 week urinary symptom temporally 100% relapse within 6 months Effectiveness depend on frequent, ongoing treatment
59 Electrogalvanic stimulation for levator ani spasm A high voltage direct current (80-120Hz) Possible mechanism high frequency nerve stimulation induce tentanic and fatique of levator ani break the spasm-pain pain Clinical result: Rectal probe, high voltage galvanic stimulation, 80 or 120 cps, 1 h 90% relieve symptoms high relapse rate in 6 months
60 Combination therapy Behavioral modification Manual technique Biofeedback Electrical stimulation Pharmacotherapy
61 Electrostimulation and electromodulation for NVD Detrusor contractility reduces during electrostimulation of pelvic floor Detrusor overactivity Sacral neuromodulation, Surface sacral electromagnetic current stimulation Detrusor underactivity Sacral nerve or Intravesical neurostimulation
62 Electrical stimulation 5-20Hz, 210μs, low level intensity Intravaginal/ intranal electrode transcutaneous electrodes: sacral dermatome: - sacral, suprapubic,, common peroneal, posterior tibial nerves mechanism of action Large skin afferents suppress spontaneous reflex activity within the dermatome
63 Implantation of Sacral Stimulator
64 Correct placement of electrode on Sacral nerves
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Technologies and architectures" Stimulator, electrodes, system flexibility, reliability, security, etc."
 March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
Electrostimulation Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents. Electrostimulation. Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Updates in the nonpharmacological. treatment on overactive bladder
 Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Physiologic Anatomy and Nervous Connections of the Bladder
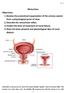 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Posterior Tibial Nerve Stimulation
 Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY
 PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
PREVENTING URINARY INCONTINENCE through PELVIC FLOOR REHABILITATION in DISABLED ELDERLY Paolo DI BENEDETTO Lecturer, Tor Vergata University, Rome, Italy Former Director of Rehabilitation Department Institute
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain
 Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN. Riette Vosloo Physiotherapist in Women s s Health
 CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
03/13/18. A. Symptoms lasting for greater than or equal to 12 months that have resulted to significant impairment in activities of daily living; and
 Reference #: MC/I008 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Reference #: MC/I008 Page: 1 of 5 PRODUCT APPLICATION: PreferredOne Administrative Services, Inc. (PAS) ERISA PreferredOne Administrative Services, Inc. (PAS) Non-ERISA PreferredOne Community Health Plan
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Urinary Continence & Management Post Stroke
 Urinary Continence & Management Post Stroke Incontinence and Stroke occurs in greater than 50% of acute stroke patients despite the personal, economic and psychosocial impact treatment evidence specific
Urinary Continence & Management Post Stroke Incontinence and Stroke occurs in greater than 50% of acute stroke patients despite the personal, economic and psychosocial impact treatment evidence specific
Training a Wayward Bladder
 D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
Pelvic Floor and More.. Urinary Continence. Urinary Incontinence. Normal Bladder Function
 Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
Pelvic Floor and More.. Jo Pitts Women s and Men s Health Physiotherapist Milton Keynes University Hospital Women s and Men s Health Physiotherapy at MKUH Pregnancy-related back and pelvic girdle pain
EE 791 Lecture 10. FES April 1, EE 791 Lecture 10 1
 EE 791 Lecture 10 FES April 1, 2013 EE 791 Lecture 10 1 Normal Functional Control EE 791 Lecture 10 2 Current uses of FES Cardiovascular Exercise Breathing assist Grasping and Reaching Transfer and Standing
EE 791 Lecture 10 FES April 1, 2013 EE 791 Lecture 10 1 Normal Functional Control EE 791 Lecture 10 2 Current uses of FES Cardiovascular Exercise Breathing assist Grasping and Reaching Transfer and Standing
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
17 th European congress of Physical Rehabilitation Medicine. 38th SIMFER congress
 17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE
 PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Objectives. Key Outlines:
 Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
NEUROPATHIC BLADDER DISORDERS
 NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Dr Hannah Blakely. Dr Ben Sharp. Ms Julee Binns. Sara Widdowson. 7:15-8:15 Breakfast Session: Oxford Women's Health
 Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Urodynamics in women. Aims of Urodynamics in women. Why do Urodynamics?
 Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Urodynamics in women Chendrimada Madhu MD, MA, MRCOG Subspecialty Trainee in Urogynaecology Southmead Hospital 2013 Aims of Urodynamics in women n Confirmation of incontinence and its cause n Definition
Female Pelvic Medicine & Reconstructive Surgery
 Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
Female Pelvic Medicine & Reconstructive Surgery APPLICATION FOR NEW FELLOWSHIP Name of Institution: McGill University Location: Royal Victoria Hospital (Glen Site), St Mary s Hospital Centre Type of Fellowship:
072 Posted: 10/17/06 Page 1 of 25
 072 Posted: 10/17/06 Page 1 of 25 Incontinence Therapy Selected Treatments and Devices Medical Policy When services are covered We cover the following treatments for urinary incontinence: 1 Behavioral
072 Posted: 10/17/06 Page 1 of 25 Incontinence Therapy Selected Treatments and Devices Medical Policy When services are covered We cover the following treatments for urinary incontinence: 1 Behavioral
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors
 DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
Video-urodynamics. P J R Shah Institute of Urology and UCH
 Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Video-urodynamics P J R Shah Institute of Urology and UCH Bladder Function Storage Capacity and Pressure Emptying Pressure/flow/emptying URODYNAMIC INVESTIGATIONS Free urine flow rate Urethral pressure
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Pelvic Floor Therapy for the Oncology Patient
 Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
URGE MOTOR INCONTINENCE
 URGE MOTOR INCONTINENCE URGE INCONTINENCE COMMONEST TYPE IN ELDERLY WOMEN Causes: 1 - Defects in CNS regulation Stroke Parkinson s disease Dementia (Alzheimer s and other types) Normopressure hydrocephalus
URGE MOTOR INCONTINENCE URGE INCONTINENCE COMMONEST TYPE IN ELDERLY WOMEN Causes: 1 - Defects in CNS regulation Stroke Parkinson s disease Dementia (Alzheimer s and other types) Normopressure hydrocephalus
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Case Study: Abdominal & Pelvic Pain
 WRHA: Less Pain, More Gain! Case Study: Abdominal & Pelvic Pain Presented November 4, 2013 Dr. Kelli Berzuk Pelvic Floor Physiotherapist WRHA: Less Pain, More Gain! Case Study To respect patient privacy
WRHA: Less Pain, More Gain! Case Study: Abdominal & Pelvic Pain Presented November 4, 2013 Dr. Kelli Berzuk Pelvic Floor Physiotherapist WRHA: Less Pain, More Gain! Case Study To respect patient privacy
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
10/15/2012. Pelvic Pain and Dysfunction
 Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
Pain and Holly Bommersbach PT, MPT Angela De La Cruz PT, MPT Pain which occurs in the perineal and/or anal areas Pain in the lower abdomen, low back and/or pelvic girdle Pain may often affect other areas,
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
21/03/2016. The urogynaecologist approach. Urinary continence management in women: a multidisciplinary approach. Dr Anna Rosamillia
 Urinary continence management in women: a multidisciplinary approach The urogynaecologist approach Dr Anna Rosamillia What is normal bladder function? Incontinence is not normal Normal voiding is 7-8 times
Urinary continence management in women: a multidisciplinary approach The urogynaecologist approach Dr Anna Rosamillia What is normal bladder function? Incontinence is not normal Normal voiding is 7-8 times
Refractory Lower Urinary Tract Symptoms
 Sacral Neuromodulation for Treatment of Refractory Lower Urinary Tract Symptoms Alex Kavanagh, PGY3 Mar 30/2011 Goals 1. Define sacral neuromodulation (SNM) and review the clinical implementation 2. Provide
Sacral Neuromodulation for Treatment of Refractory Lower Urinary Tract Symptoms Alex Kavanagh, PGY3 Mar 30/2011 Goals 1. Define sacral neuromodulation (SNM) and review the clinical implementation 2. Provide
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Pelvic Floor Exercise. Brigi0e Fung Physiotherapist
 Pelvic Floor Exercise Brigi0e Fung Physiotherapist Treatment for urinary incontinence Pelvic floor muscle exercise (Kegel, 1948) Bladder retraining Behaviour modification Treatment for urinary incontinence
Pelvic Floor Exercise Brigi0e Fung Physiotherapist Treatment for urinary incontinence Pelvic floor muscle exercise (Kegel, 1948) Bladder retraining Behaviour modification Treatment for urinary incontinence
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
EFFECT OF BIOFEEDBACK ON URINARY INCONTINENCE
 Case report: ABSTRACT: EFFECT OF BIOFEEDBACK ON URINARY INCONTINENCE Mohammed Sheeba Kauser, C.S.Ram 1 Postgraduate Trainee,Department of physiotherapy, I.T.S, U.P, India 1- Director, I.T.S,U.P.India.
Case report: ABSTRACT: EFFECT OF BIOFEEDBACK ON URINARY INCONTINENCE Mohammed Sheeba Kauser, C.S.Ram 1 Postgraduate Trainee,Department of physiotherapy, I.T.S, U.P, India 1- Director, I.T.S,U.P.India.
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY
 HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY JANE FRAHM, BS,PT,BCIA PMDB 7/7/2010 jdf,pt 1 REHABILITATION INSTITUTE OF MICHIGAN RIM PART OF COMPREHENSIVE TREATMENT PROGRAM. 7/7/2010
HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY JANE FRAHM, BS,PT,BCIA PMDB 7/7/2010 jdf,pt 1 REHABILITATION INSTITUTE OF MICHIGAN RIM PART OF COMPREHENSIVE TREATMENT PROGRAM. 7/7/2010
Neuromodulation and the pudendal nerve
 Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Pelvic Floor Stimulation as a Treatment of Urinary Incontinence
 Pelvic Floor Stimulation as a Treatment of Urinary Incontinence Policy Number: 1.01.17 Last Review: 2/2014 Origination: 2/2007 Next Review: 2/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Pelvic Floor Stimulation as a Treatment of Urinary Incontinence Policy Number: 1.01.17 Last Review: 2/2014 Origination: 2/2007 Next Review: 2/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
A over-the-counter medical device that utilizes muscle stimulation for the treatment of stress, urge and mixed urinary incontinence.
 A over-the-counter medical device that utilizes muscle stimulation for the treatment of stress, urge and mixed urinary incontinence. An over-the-counter medical device that utilizes muscle stimulation
A over-the-counter medical device that utilizes muscle stimulation for the treatment of stress, urge and mixed urinary incontinence. An over-the-counter medical device that utilizes muscle stimulation
Electrical pelvic floor stimulation: a possible alternative treatment for reflex urinary incontinence in patients with spinal cord injury
 Spinal Cord (1996)34 411-415 @ 1996 International Medical Society of Paraplegia ll rights reserved 1362-4393/96 $1200 lectrical pelvic floor stimulation a possible alternative treatment for reflex urinary
Spinal Cord (1996)34 411-415 @ 1996 International Medical Society of Paraplegia ll rights reserved 1362-4393/96 $1200 lectrical pelvic floor stimulation a possible alternative treatment for reflex urinary
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
