Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
|
|
|
- Nicholas Haynes
- 6 years ago
- Views:
Transcription
1 Int Urogynecol J (2008) 19: DOI /s ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy Gautier Chene & Anne-Sylvie Tardieu & Denis Savary & Mikael Krief & Carole Boda & Marie-Claude Anton-Bousquet & Aslam Mansoor Received: 28 June 2007 / Accepted: 14 December 2007 / Published online: 15 January 2008 # International Urogynecology Journal 2007 Abstract The objective of the study is to evaluate the anatomical and functional results of the McCall culdoplasty in the treatment of moderate hysterocele and the prevention of enterocele and vaginal vault prolapse after vaginal hysterectomy. Using a modified McCall procedure, 185 patients underwent vaginal hysterectomy for mild or moderate uterine prolapse. Pre- and post-operative assessments were carried out using the International Continence Society staging system. The 24-month follow-up showed stable 89.2% incidence of stage 0 vaginal vault prolapse (point C) and a 10% incidence of stage 1 vaginal vault prolapse that was well tolerated and did not require revision surgery. Functional analysis showed satisfactory sexual function at 24 months post-surgery for 81.2% of patients. The McCall culdoplasty did not lead to a disruption of the vaginal axis and gave excellent anatomical and functional results in maintaining support after vaginal hysterectomy, especially in sexually active patients. Keywords McCall culdoplasty. Enterocele. Vaginal hysterectomy. Uterovaginal prolapse. Vaginal vault prolapse. Cystocele G. Chene (*) Obstetrics & Gynecology, North Hospital, CHU, St Etienne, France chenegautier@yahoo.fr A.-S. Tardieu : D. Savary : M. Krief : C. Boda : M.-C. Anton-Bousquet : A. Mansoor Obstetrics & Gynecology, Issoire Hospital, Issoire, France Introduction Enterocele and vaginal vault prolapse account for up to 16% of the mid-term and long-term complications associated with curative surgery for urogenital prolapse in vaginal hysterectomy [1]. Both these complications carry the risk of modifying the normal vaginal axis and thereby decompensating the superior and posterior vaginal wall, which in turn will cause a recurrence of the original urogenital prolapse. Furthermore, with the hernia represented by the enterocele, there is a risk of obstruction or incarceration of the bowel loops [2]. An enterocele is a peritoneal pouch that normally contains loops of small intestine or omentum and progressively disrupts the recto-vaginal Denonvilliers fascia (level II). Vaginal vault prolapse is not necessarily associated with enterocele but is rather the consequence of weak floor muscles allowing the uterosacral and cardinal ligaments to slip into the paracolpium (level I) [3]. In both cases, the predisposing causes include perineal obstetrical and surgical trauma (tears in the upper vaginal fascia) and abdominal hyperpressure (obesity, persistent constipation, and chronic cough). There are several surgical procedures that have been described as preventing vaginal vault prolapse and enterocele. This retrospective study reports the mid-term anatomical and functional results of a modified McCall culdoplasty technique. Materials and methods Our data were taken from a computer database containing the case files of 690 patients who underwent curative vaginal hysterectomy for mild or moderate hysterocele with
2 1008 Int Urogynecol J (2008) 19: Table 1 Pre-operative demographic characteristics of patients; the values are means, with extremes given in brackets (n=185) Means Age 60 (33 92) BMI (kg/m 2 ) ( ) Parity 2 (0 11) Birth weight of baby >4,000 g 20 (10.8%) Persistent constipation 4 (2%) Chronic cough 6 (3%) curative treatment for associated urogenital prolapse between 1998 and 2005 by two physicians. Cystocele and rectocele repair were done either with autologous tissue or Prolene mesh (Ethicon, Johnson & Johnson, USA). All the patients who had undergone vaginal hysterectomy for uterine prolapse with shortening of uterosacral, cardinal ligaments, and uterosacral ligament fixation of the posterior vaginal fornix using a modified McCall technique during this period were enrolled. All pre- and post-operative examinations systematically included a standardized medical interview primarily focused on screening for urogynecological and (or) digestive disorders and dyspareunia, together with a quality-of-life assessment based on the conti-life scale [4]. A full clinical urogenital examination was performed, assessing pelvic disorders under effort with Valsalva's maneuver and at rest. A pre-operative clinical urogynecological examination was systematically carried out to collect the preoperative clinical data. The clinical assessments complied with the International Continence Society (ICS) pelvic organ prolapse quantification staging systems. For greater accuracy, the measurements were carried out using a flexible graduated hysterometer (Flexible Hysterometer CH 10 ref 1502S10, CCD international, France). Each patient was seen and examined at 2, 12 15, and 24 months post-operatively. In addition to an interview and the quality-of-life questionnaire, a complete urogynecological examination was carried out to assess pelvic static, with special emphasis on the posterior superior vaginal segment and all other secondary decompensation. Vaginal length was measured from the introitus to the vaginal vault using a flexible graduated hysterometer. The quality of sexual activity was assessed using specific questioning to estimate the severity of any dyspareunia and whether sexual activity had stopped. Since the description of the McCall culdoplasty technique [5], many modifications of McCall original technique have been described ( external and internal McCall) [6]. This modified McCall culdoplasty technique was used during hysterectomy (peritonization was performed by closure of the pouch of Douglas by means of a pouch string suture (Prolene 0)), with intraperitoneal hitching of only uterosacral ligaments without taking the cardinal ligaments in the suture, thus keeping the ureters distant from the peritoneal suture. In contrast to the original McCall technique, a suture was placed on each side, incorporating the vagina and the uterosacral pedicles in a semipouch string fashion. The effect of this suture was to suspend the posterior vagina to the uterosacral ligaments on each side, while at the same time maintaining sufficient vaginal length. Success criteria The criteria used to compare results were the same as those of Montella and Morrill [7]. After the McCall culdoplasty, we considered a vaginal vault at point C (< 2 cm) or stage 0 as a successful outcome. The other cases were classified as failures, even when there was an improvement over the pre-operative situation. Results A total of 185 patients underwent vaginal hysterectomy for mild or moderate uterine prolapse. McCall culdoplasty was systematically carried out. Associated with this surgery were 122 curative treatments for cystocele, 140 for urinary incontinence, and 117 for rectocele. Sixty-three patients presented no cystocele, 68 no rectocele, and underwent vaginal hysterectomy with or Table 2 Associated surgical procedures performed with vaginal hysterectomy and McCall culdoplasty, intra-operative complications, and post-operative data Post-operative data Treatment for cystocele 122 Halban fascioplasty 74 (60.6%) Intervesico-vaginal mesh 48 (39.3%) Suburethral sling (TVT or TOT) 140 Treatment for rectocele 117 Levator ani myorrhaphy + denonvilliers 73 (62.3%) prerectal plication Denonvilliers prerectal plication alone 44 (37.6%) Intra-operative complications Bladder injury 2 (1.1%; 1 TVT; 1 cystocele repair) Rectal injury 1 (0.5%; posterior repair) Blood loss >500 ml 2 (1.1%; without any transfusion) Post-operative data Length of hospital stay 6.1 days (2 21) Urinary infection 14 (7.5%) Perineal abscess 1 (0.5%)
3 Int Urogynecol J (2008) 19: Table 3 Pre- and post-operative ICS stage of the uterus and posthysterectomy cuff (n=185). Post-operative ICS stage of cystocele (n=63) and rectocele (n=68) of patients who presented no pre-operative cystocele or rectocele Vaginal vault: point C Stage 0 10 (5.4%) 185 (100%) 167 (90.2%) 158 (89.2%) Vaginal vault: point C Stage (65.4%) 0 17 (9.2%) 18 (10%) Vaginal vault: point C Stage 2 49 (26.5%) 0 1 (0.6%) 1 (0.6%) Vaginal vault: point C Stage 3 5 (2.7%) Lost to follow-up (4.3%) Cystocele (n=63) Stage (3%) 1 (1.5%) Stage (1.5%) Stage Rectocele (n=68) Stage (1.5%) Stage (3%) 2 (3%) Stage without curative treatment for urinary incontinence using suburethral TVT or transobturator tape (Table 3). A routine cystoscopy visualizing urine flow from ureters is performed at the end of the operation. The demographic data are summarized in Table 1. Surgical details, operative complications, and post-operative data are given in Table 2. Anatomical results All the patients were seen again 2, 12 15, and 24 months post-operatively. The vaginal vault remained entirely in place in 90.2% of cases at months, and subsequently at 24 months. Stage 1 decompensation involved only 9.2% of cases at 12 months and 10% at 24 months (Table 3). However, it caused no functional symptoms. The one patient with stage 2 needed no surgical treatment. Analysis of the possible occurrence of cystocele and rectocele (secondary decompensation) involved only the patients who showed no urogenital prolapse. There were 3% of cystoceles and 4.5% rectoceles at 24 months involving the patients who presented no pre-operative cystocele or rectocele. In this group, lower digestive symptoms were infrequent and involved 1% for rectal pressure, 1.6% for terminal constipation, and 4.2% for incomplete emptying of the rectum. The results are set out in Tables 3 and 4. Functional results On the 85 sexually active patients post-operatively, only five patients (5.8%) suffered from deep dyspareunia at 2 months, but there was no vaginal stenosis. At 12 months, these cases of deep dyspareunia vanished in four patients, and persisted, without being incapacitating, in one patient (Table 5). Eight (9.4%) other patients reported intromission dyspareunia at 2 months, and 0 at 12 and 24 months. We retained intromission dyspareunia only after the correction of vulvo-vaginal dryness with local oestrogeneotherapy. Post-operative vaginal length (measured by flexible graduated hysterometer) was preserved for 177 patients (9 10 cm) and less than 7 cm only in eight patients (9.4%). Six of them were not sexually active pre-operatively. In the two remaining patients, there was no correlation between short vagina and sexual life. Functional analysis showed satisfactory sexual function at 24 months post-surgery for 81.2% of patients. Discussion Our study records excellent results at 12 months confirmed at 24 months: the McCall culdoplasty technique using nonabsorbable suture, thus, seems to be very effective in Table 4 Lower digestive symptoms for the 68 patients who received no treatment for rectocele Rectal pressure 1 (1.5%) 2 (2.9%) 2 (2.9%) 2 (2.9%) Terminal constipation 3 (4.4%) 3 (4.4%) 2 (2.9%) 3 (4.4%) Incomplete emptying of the rectum 4 (5.9%) 6 (8.8%) 6 (8.8%) 8 (11.7%)
4 1010 Int Urogynecol J (2008) 19: Table 5 Characteristics of pre- and post-operative sexual activity (n=85) Sexual activity 85 (100%) 85 (100%) 85 (100%) 77 (90.5%) Satisfactory sexual activity 80 (94%) 72 (84.7%) 74 (87%) 69 (81.2%) Intromission dyspareunia 0 8 (9.4%) 0 0 Deep dyspareunia 1 (1.2%) 5 (5.8%) 1 (1.2%) 1 (1.2%) supporting the vaginal vault. Our results are consistent with those of other reports: 90% success at 12 months for Montella and Morrill [7], 90.9% at 24 and 36 months for Cruikshank and Kovac [2], and 93.5% for Colombo and Milani [8](Table 6). These excellent results probably derive from the durable reconstruction of the vaginal vault by the hitching of the uterosacral and cardinal ligaments, which ensures an efficient suspension of the posterior superior vagina and maintenance of the physiological length and axis of the vagina. But, if the McCall culdoplasty is an efficient technique for moderate prolapse, the number of severe prolapse in our series (n=54) seems to be too small to give definitive conclusions for all stages. However, like Montella and Morrill [7], we recorded only those patients who presented no prolapse of the vaginal vault or prior enterocele and who had undergone preventive culdoplasty and vaginal vault fixation. The other studies recorded different populations presenting complex urogynecological prolapses with associated prolapse of the vaginal vault (but with no clear indication of the pre-operative staging), in which case McCall culdoplasty is then considered to be curative, and consequently the results need to be moderated. In another unpublished series distinct from the one we present here, there were three cases of ureteral complications that required surgery, with ureteral reimplantation in one case. In addition, a fourth patient presented dyspareunia linked to a constriction of the vaginal vault that had to be dealt with surgically. These four cases lie outside the scope of our study, as these patients presented a prior prolapse of the vaginal vault. Concerning the risk of enterocele, the diagnosis is usually made from a clinical picture of lower digestive symptoms with rectal pressure, terminal constipation, and incomplete emptying of the rectum [9]. However, (a) the rates are practically identical to the pre-operative rates in our subgroup without rectocele, and (b) some authors consider that these lower digestive symptoms are in no way specific to an enterocele [10]. The absence of a direct connection between digestive symptoms and McCall culdoplasty could therefore be expected. Other techniques have also been described: Richter sacrospinous ligament fixation [11], which is very effective for the treatment of vaginal vault prolapse, remains controversial for prevention, as it shifts the vaginal axis and can lead to up to 22% decompensation of the anterior level [8, 12]. Considering the subgroup of 63 and 68 patients in our series, we observed no decompensation of anterior (only 3%) and (or) posterior levels (only 4.5%), probably because of the preservation of the vaginal length and axis, which is consistent with the scant data reported in the literature on this subject. In addition, sacrospinous ligament fixation is a more delicate technique that carries a risk of vascular and nervous system complications (sciatic and pudendal lesion and damage to perirectal vessels) [11, 13]. The few studies Table 6 Post-operative ICS stage of the posthysterectomy cuff (review of the literature) 2 months 12 months 24 months 36 months months Our study Stage 0 100% (185/185) 90.2% (167/185) 89.2% (158/177) Stage I 9.2% (17/185) 10% (18/177) Stage II 0.6% (1/185) 0.6% (1/177; 8 drop out Montella and Morrill [5] Stage 0 100% (43/43) 90% (39/43) Stage I 7% (3/43) Stage II 3% (1/43) Cruikshank and Kovac [2] Stage I 100% (33/33) 91% (30/33) 91% (30/33) Stage II 6% (2/33; 1 dropout) 6% (2/33; 1 dropout) Colombo and Milani [6] Stage % (58/62) Stage II 5% (3/62; 1 dropout)
5 Int Urogynecol J (2008) 19: that have compared the McCall and Richter techniques have concluded that the McCall technique is to be preferred [8]. Likewise, McCall culdoplasty also proves more efficacious than a simple peritoneal suture of the vaginal vault or a Moschcowitz type culdoplasty [2]. In addition to these very good anatomical results, the McCall technique gives equally good functional results with a satisfactory sexual function at 24 months postsurgery for 81.2% of patients. Our results are consistent with those of Colombo and Milani who found a sexual activity maintained with no dyspareunia in 75% [8]. Instances of intromission dyspareunia were resolved at 12 months and can probably be explained by complications arising from perineorrhaphy (scarring tissue of the perinal body, narrowing of the introitus during posterior colporrhaphy, or perineorrhaphy). Cases of deep dyspareunia practically disappeared at 12 months post-operatively and can probably be explained by the healing process or vulvovaginal dryness corrected by the application of vaginal suppositories and a topical estrogen-based moisturizer (local estrogenotherapy) [14]. We found no correlation between post-operative vaginal length and deep dyspareunia: Of the eight patients with a vaginal length of less than 7 cm, none complained of deep dyspareunia. By contrast, two patients with deep dyspareunia had a measured vaginal length of 10 cm. No immediate, early, or late complications arising from narrowing of the vaginal vault were recorded. So, vaginal anatomy measured by length does not seem to be correlated well with sexual function, particularly symptoms of deep dyspareunia and vaginal dryness [15]. Conclusion The McCall technique ensures a secure hold for the vaginal vault during vaginal hysterectomy for the treatment of mild and moderate uterine prolapse. It rebuilds a support for the vaginal vault by tying up the complex formed by the uterosacral-cardinal ligaments. The McCall culdoplasty proved both anatomically and functionally efficient for the prevention of vaginal vault prolapse and enterocele after vaginal hysterectomy. Conflicts of interest References None. 1. Ranney B (1981) Enterocele, vaginal prolapse, pelvic hernia: recognition and treatment. Am J Obstet Gynecol 140: Cruikshank SH, Kovac R (1999) Randomized comparison of three surgical methods used at the time of vaginal hysterectomy to prevent posterior enterocele. Am J Obstet Gynecol 180: DeLancey JOL (1992) Anatomic aspects of vaginal eversion after hysterectomy. Am J Obstet Gynecol 166: Amarenco G, Arnould B, Carita P, Haab F, Labat JJ, Richard F (2003) European psychometric validation of the CONTILIFE : a quality of life questionnaire for urinary incontinence. Eur Urol 43 (3): McCall ML (1957) Posterior culdeplasty: surgical correction of enterocele during vaginal hysterectomy; a preliminary report. Obstet Gynecol 10: Lee Ra (1992) Atlas of gynecologic surgery. WB Saunders, Philadelphia 7. Montella JM, Morrill MY (2005) Effectiveness of the McCall culdeplasty in maintaining support after vaginal hysterectomy. Int Urogynecol J 16: Colombo M, Milani R (1998) Sacrospinous ligament fixation and modified McCall culdoplasty during vaginal hysterectomy for advanced uterovaginal prolapse. Am J Obstet Gynecol 179: Holley RL (1994) Enterocele: a review. Obstet Gynecol Surv 49: Chou Q, Weber AW, Piedmonte MR (2000) Clinical presentation of enterocele. Obstetv Gynecol 96: Richter K (1982) Massive eversion of the vagina: pathogenesis, diagnosis, and therapy of the true prolapse of the vaginal stump. Clin Obstet Gynecol 25: Carey MP, Slack MC (1994) Transvaginal sacrospinous colpopexy for vault and marked uterovaginal prolapse. Br J Obstet Gynaecol 101: Alevizon SJ, Finan MA (1996) Sacrospinous colpopexy: management of postoperative pudendal nerve entrapment. Obstet Gynecol 88: Given FT, Muhlendorf IK, Brownong GM (1993) Vaginal length and sexual function after colpopexy for complete uterovaginal eversion. Am J Obstet Gynecol 169: Weber AM, Walters MD, Shover LR, Mitchinson A (1995) Vaginal anatomy and sexual function. Obstet Gynecol 86:
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
ISSN (o): Sacrospinous fixation: an efficient technique for prevention and treatment of vault prolapse
 Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Original article www.ijrhs.com ISSN (o):2321 7251 Sacrospinous fixation: an efficient technique for prevention and treatment of vault Rajshree dayanand katke 1, Usha kiran. 2 1M.D.(Obstetrics & Gynecology),
Posterior vaginal compartment repairs: Where are the main anatomical defects?
 Int Urogynecol J (2016) 27:741 745 DOI 10.1007/s00192-015-2874-7 ORIGINAL ARTICLE Posterior vaginal compartment repairs: Where are the main anatomical defects? Bernard T. Haylen 1 & Sushen Naidoo 2 & Stephen
Int Urogynecol J (2016) 27:741 745 DOI 10.1007/s00192-015-2874-7 ORIGINAL ARTICLE Posterior vaginal compartment repairs: Where are the main anatomical defects? Bernard T. Haylen 1 & Sushen Naidoo 2 & Stephen
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
JMSCR Volume 03 Issue 03 Page March 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Quality of Life among Patients after Vaginal Hysterectomy and Pelvic Floor Repair Operation ABSTRACT Authors S Lovereen 1, F A Suchi 2,
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy
 Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair vaginal vault prolapse The vaginal
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
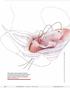 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
High success rate and considerable adverse events of pelvic prolapse surgery with Prolift: A single center experience
 Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Available online at www.sciencedirect.com ScienceDirect Taiwanese Journal of Obstetrics & Gynecology 52 (2013) 389e394 Short Communication High success rate and considerable adverse events of pelvic prolapse
Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy
 Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
Int Urogynecol J (2011) 22:577 584 DOI 10.1007/s00192-010-1325-8 ORIGINAL ARTICLE Long-term outcomes of modified high uterosacral ligament vault suspension (HUSLS) at vaginal hysterectomy Stergios K. Doumouchtsis
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay
 High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
High-field (3T) magnetic resonance defecography with functional assessment of the evacuation phase: A pictorial essay Poster No.: C-430 Congress: ECR 2009 Type: Educational Exhibit Topic: Abdominal and
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
ig. 2. The organs and their outlet tubes.
 Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Fig. 1. Birth-related laxity. The diagram shows the baby s head severely stretching ligaments and other tissues in and outside the vagina. This may cause various degrees of looseness, prolapse of the bladder
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy
 Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Ina S. Irabon, MD, FPOGS, FPSRM, FPSGE Obstetrics and Gynecology Reproductive Endocrinology and Infertility Laparoscopy and Hysteroscopy Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology
 Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Functional anatomy of the female pelvic floor and lower urinary tract Stefano Floris, MD, PhD Department of Obstetrics and Gynaecology Ospedale San Giovanni di Dio, Gorizia, Italy ANATOMY URINARY CONTINENCE
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of infracoccygeal sacropexy using mesh to repair uterine prolapse Uterine prolapse
High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
 Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
Int Urogynecol J (2010) 21:515 522 DOI 10.1007/s00192-009-1064-x ORIGINAL ARTICLE High levator myorraphy versus uterosacral ligament suspension for vaginal vault fixation: a prospective, randomized study
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Index. Cyclical pelvic pain, 37 Cystocele, 22, 23, 25, 48, 51, 52, 54, 56, 124, 148, 160
 A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
A Abdominal approach, 141 Abdominal hernia s surgery, 123, 124 Abdominal sacrocolpopexy (ASC), 116, 117 Abnormal uterine bleeding, 96 Anterior compartment repair, 101, 102 Apical compartment repair, 96
Degree of uterine prola pse
 by R. MITRA,* M.S., D.G.O. J Before the middle of the nineteenth century very little attention was directed towards the advancement of knowledge about the anatomical supports of the genital organs or towards
by R. MITRA,* M.S., D.G.O. J Before the middle of the nineteenth century very little attention was directed towards the advancement of knowledge about the anatomical supports of the genital organs or towards
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Female Urology. Young-Suk Lee, Deok Hyun Han, Ji Youl Lee 1, Joon Chul Kim 2, Myung-Soo Choo 3, Kyu-Sung Lee
 www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
www.kjurology.org DOI:1.4111/kju.21.51.3.187 Female Urology Anatomical and Functional Outcomes of Posterior Intravaginal Slingplasty for the Treatment of Vaginal Vault or Uterine Prolapse: A Prospective,
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
Management of Urogenital Prolapse of Women in Primary Care. Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner
 Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
Management of Urogenital Prolapse of Women in Primary Care Lizzie McManus MBE RGN RMN Practice nurse Womens health practitioner Primary Care Womens Health Forum www.pcwhf.org.uk Useful websites RCN genital
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolaps: Anteriore Rektopexie nach D Hoore. Prof. Dr. med. F. Hetzer
 Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent braided suture
 Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Urogynaecology & Prolapse. Alexander Denning and Leifa Jennings
 + Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
+ Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY)
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
Sexual function after sacrospinous fixation for vaginal vault prolapse: bad or mad?
 Surg Endosc (2009) 23:1013 1017 DOI 10.1007/s00464-008-0108-5 Sexual function after sacrospinous fixation for vaginal vault prolapse: bad or mad? Marc Baumann Æ Claudia Salvisberg Æ Michel Mueller Æ Annette
Surg Endosc (2009) 23:1013 1017 DOI 10.1007/s00464-008-0108-5 Sexual function after sacrospinous fixation for vaginal vault prolapse: bad or mad? Marc Baumann Æ Claudia Salvisberg Æ Michel Mueller Æ Annette
American Journal of Obstetrics and Gynecology
 American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
The UK National Prolapse Survey: 10 years on
 Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Int Urogynecol J (2018) 29:795 801 DOI 10.1007/s00192-017-3476-3 ORIGINAL ARTICLE The UK National Prolapse Survey: 10 years on Swati Jha 1 & Alfred Cutner 2 & Paul Moran 3 Received: 28 June 2017 /Accepted:
Breast Carcinoma The Hard Way
 Women s Health Breast Carcinoma The Hard Way C50 - Malignant neoplasm of breast C50.0 Malignant neoplasm of nipple and areola C50.01 - Malignant neoplasm of nipple and areola, female C50.011 - Malignant
Women s Health Breast Carcinoma The Hard Way C50 - Malignant neoplasm of breast C50.0 Malignant neoplasm of nipple and areola C50.01 - Malignant neoplasm of nipple and areola, female C50.011 - Malignant
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Surgical management of pelvic organ prolapse in women (Review)
 Surgical management of pelvic organ prolapse in women (Review) Maher C, Feiner B, Baessler K, Glazener CMA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Surgical management of pelvic organ prolapse in women (Review) Maher C, Feiner B, Baessler K, Glazener CMA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
Infracoccygeal sacropexy using mesh for uterine prolapse repair
 Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Infracoccygeal sacropexy using mesh for uterine Issued: January 2009 www.nice.org.uk/ipg280 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study
 Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Efficacy and Adverse Effects of Monarc Versus Tension-free Vaginal Tape Obturator: a Retrospective One-year Follow-up Study Yvonne KY CHENG MBChB, MRCOG William WK TO MBBS, M Phil, FRCOG, FHKAM (O&G) HX
Urogynecology: Evidence-Based Clinical Practice
 Urogynecology: Evidence-Based Clinical Practice Kate H. Moore Urogynecology: Evidence-Based Clinical Practice Second Edition Kate H. Moore, MBBS, FRCOG, FRANZCOG, MD, CU Department Obstetrics & Gynaecology
Urogynecology: Evidence-Based Clinical Practice Kate H. Moore Urogynecology: Evidence-Based Clinical Practice Second Edition Kate H. Moore, MBBS, FRCOG, FRANZCOG, MD, CU Department Obstetrics & Gynaecology
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Urogynecology Curriculum for the PGY III and IV Resident
 Urogynecology Curriculum for the PGY III and IV Resident Sinai Hospital of Baltimore Maryland Department of Obstetrics and Gynecology I. Educational Purpose: The dedicated Urogynecology rotation is intended
Urogynecology Curriculum for the PGY III and IV Resident Sinai Hospital of Baltimore Maryland Department of Obstetrics and Gynecology I. Educational Purpose: The dedicated Urogynecology rotation is intended
Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation in Treatment of Vaginal Vault Prolapse
 ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
ISRN Obstetrics and Gynecology Volume 2013, Article ID 958670, 5 pages http://dx.doi.org/10.1155/2013/958670 Clinical Study Posterior Intravaginal Slingplasty versus Unilateral Sacrospinous Ligament Fixation
For personal use only. Injury-free vaginal surgery: Case-based protective tactics
 For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
For mass reproduction, content licensing and permissions contact Dowden Health Media. OBG MANAGEMENT Lennox Hoyte, MD Director of Female Pelvic Medicine and Reconstructive Surgery, Department of Obstetrics
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Tian-Ni Kuo 1, Ming-Ping Wu 1,2 *
 RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
RESEARCH LETTER THE USE OF A CONCOMITANT TENSION-FREE VAGINAL MESH TECHNIQUE AND A TENSION-FREE MIDURETHRAL SLING IN TREATING PELVIC ORGAN PROLAPSE AND OCCULT STRESS URINARY INCONTINENCE Tian-Ni Kuo 1,
PROLAPSE. By Charlotte Robinson Women s Health Speciality Attachment
 PROLAPSE. By Charlotte Robinson Women s Health Speciality Attachment Introduction Case example Pelvic organ prolapse - Epidemiology - Aetiology - Anatomy - Types of prolapse/ severity - Examination/Investigation
PROLAPSE. By Charlotte Robinson Women s Health Speciality Attachment Introduction Case example Pelvic organ prolapse - Epidemiology - Aetiology - Anatomy - Types of prolapse/ severity - Examination/Investigation
Aetiology 1998 Bump & Norton Theoretical model
 Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
Obliterative Procedures LeFort Colpocleisis Colpectomy (Vaginectomy) April 4, 2018
 Obliterative Procedures LeFort Colpocleisis Colpectomy (Vaginectomy) April 4, 2018 Obliterative Procedures for uterovaginal prolapse Total colpocleisis Partial colpocleisis (LeFort) Vaginectomy (colpectomy)-
Obliterative Procedures LeFort Colpocleisis Colpectomy (Vaginectomy) April 4, 2018 Obliterative Procedures for uterovaginal prolapse Total colpocleisis Partial colpocleisis (LeFort) Vaginectomy (colpectomy)-
Bilateral iliococcygeal fixation for vaginal vault prolapse and enterocele repair using a new suturing device the digital needle driver
 BJOG: an International Journal of Obstetrics and Gynaecology August 2005, Vol. 112, pp. 1145 1149 DOI: 10.1111/j.1471-0528.2005.00616.x SURGICAL TECHNIQUE Bilateral iliococcygeal fixation for vaginal vault
BJOG: an International Journal of Obstetrics and Gynaecology August 2005, Vol. 112, pp. 1145 1149 DOI: 10.1111/j.1471-0528.2005.00616.x SURGICAL TECHNIQUE Bilateral iliococcygeal fixation for vaginal vault
PROCEDURE EDUCATION LITERATURE AND CONSENT FORM SURGERY FOR UTEROVAGINAL PROLAPSE
 Premier Women s Health a division of MaternOhio Clinical Associates 3600 Olentangy River Rd, Ste 490, Columbus, OH 43215 Tel: 614-459-1000 Fax 614-459-1382 http://www.moca-obgyns.com/practice-premier/
Premier Women s Health a division of MaternOhio Clinical Associates 3600 Olentangy River Rd, Ste 490, Columbus, OH 43215 Tel: 614-459-1000 Fax 614-459-1382 http://www.moca-obgyns.com/practice-premier/
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse
 British Journal of Obstetrics and Gynaecology June 2001, Vol. 108, pp. 629±633 Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse Elad Leron a, Stuart L. Stanton b, * Objective
British Journal of Obstetrics and Gynaecology June 2001, Vol. 108, pp. 629±633 Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse Elad Leron a, Stuart L. Stanton b, * Objective
