Effect of Voiding Position on Uroflowmetric Parameters in Healthy and Obstructed Male Patients
|
|
|
- Magnus Ryan
- 6 years ago
- Views:
Transcription
1 Effect of Voiding Position on Uroflowmetric Parameters in Healthy and Obstructed Male Patients MISCELLANEOUS Cenk Murat Yazici, Polat Turker, Cagri Dogan Department of Urology, Namik Kemal Univercity, Tekirdag, Turkey Purpose: Uroflowmetry is frequently used and simple urodynamic test, but it may be affected by various factors. Voiding position is one of the factors that can change the results. We tried to compare the uroflowmetric parameters in sitting and standing positions during urination. Material and Methods: A total of 198 patients were enrolled to the study. All patients underwent an uroflowmetry in standing and sitting position at late afternoon (2-4 PM) of two corresponding days with a gravimetric uroflowmeter (Uroscan, Aymed, Turkey). A transabdominal ultrasonography was used to evaluate post voiding residue (PVR). All uroflowmetric parameters and PVR were compared with paired t test or Wilcoxon signed rank test. Corresponding author: Cenk Murat Yazici, MD Department of Urology, Namik Kemal Univercity, Tekirdag, 59100, Turkey. Tel: Fax: drcenkyazici@yahoo.com Received February 2012 Accepted April 2012 Results: The median age of study population was 58.0 (36-69) years. There was no statistically significant difference at voided volume of patients in standing and sitting position as it was ± 81.8 ml and ± 82.4 ml, respectively (P =.505). Mean maximum flow rate (Qmax) during urination at standing position was 15.3 ± 6.7 ml/s while it was 15.0 ± 7.0 ml/s at sitting position (P =.29). Mean average flow rate in standing position was 8.60 ± 4.0 ml/s and 8.25 ± 3.8 ml/s in sitting position (P =.054). There was a statistically significant difference between the median post-voiding residues in standing and sitting urination which was 29.5 (0-257) ml in standing and 47.5 (2-209) ml in sitting position (P <.0001). Other uroflowmetric parameters (time to maximum flow and voiding time) was not statistically different between groups. Conclusion: There are no clinically important uroflowmetric differences between voiding in sitting and standing positions so voiding position may be left to personal preferences during uroflowmetric evaluation. Keywords: urination disorders; urodynamics; predictive value of tests; posture; male Miscellaneous
2 Voiding Parameters in Positional Changes Yazici et al INTRODUCTION Uroflowmetry is a frequently used and simple urodynamic test for both diagnosis and followup of obstructive lower urinary tract symptoms (LUTS). Although it is a non-specific test, it can give valuable objective data. On the other hand, uroflowmetry may be affected by various internal and external factors such as age, sex, ethnicity, voided volume (VV) and psychological status of patients. (1) Voiding position may be another factor affecting uroflowmetric results which is related with patients health status, social and cultural characteristics. There are some studies investigating the effect of voiding position on uroflowmetric parameters. These studies reported inconsistent results, some indicating voiding position affects uroflowmetric parameters, whereas some does not. (2-4) Authors who reported supportive data about this relation concluded that positional changes of pelvic floor and thigh muscles might be effective on their results. As sitting and squatting position is the most common way of voiding habit of eastern and Middle Eastern countries, ritual or religious causes were proposed to be another explanation for those positional differences. But these theories need to be proven with more interventions because there are also some studies opposing these results. (5-7) Daily preferred urination position may also affect uroflowmetric parameters. Positions other than patients usual habit may change results causing misdiagnosis for patients. This theory also needs verification because there are very limited studies about this subject. In our study, we tried to compare the uroflowmetric parameters in different voiding positions and to discriminate the better voiding position for elimination of misdiagnosis. As sitting and standing positions during urination was the most preferred voiding positions in the western part of our country, we designed a study evaluating the uroflowmetric differences between these two positions. Secondary objective of this study was to evaluate the uroflowmetric differences at patients voiding in a different position other than their natural voiding habit. The tertiary aim of this study was to investigate the effect of urination position on patients with low maximum flow rate values suggestive of bladder outlet obstruction (BOO). MATERIAL AND METHODS Study population A total of 250 male patients, between 35 to 70 years old, admitted to urology outpatient clinic with unilateral or bilateral flank pain, from April 2011 to November 2011, were prospectively enrolled to the study. For the homogeneity of the study population, we excluded female patients. The study was approved by institutional ethic committee. Patients with a history of neurological disease, diabetes mellitus, urinary tract infection, prostate surgery, bladder and ureter stone, prostate cancer, bladder cancer, meatal stenosis, recent prostate biopsy and patients with ongoing medical treatment interfering lower urinary system function (like anticholinergics, alpha-blockers, 5-alpha reductase inhibitors, alpha stimulants, antibiotics etc.) were excluded. All patients underwent complete medical history, physical examination, digital rectal examination, urine analysis, urine culture, serum prostate specific antigen (PSA) (in patients over 40 years) and urinary system ultrasonography. Specific blood tests and radiological examination were performed according to symptoms by the choice of the clinician. Natural voiding position and the duration was asked to the patients before uroflowmetric evaluation. Natural voiding position was defined as the voiding position of patients that was used at more than 80% of their daily life micturations for a minimum of 15 years. As we evaluated sitting and standing positions, patients who had urination habit other than these positions (like squatting) were also excluded from the survey. Study design All participants were cooperative and able to urinate in both sitting and standing position. As all patients were informed about study and given a written informed consent, an uroflowmetry in standing and sitting position was performed at late afternoon (2-4 PM) of two corresponding days with a gravimetric uroflowmeter (Uroscan, Aymed, Turkey). Patients were randomized according to voiding position for the first and second day evaluation. For the privacy and comfort of patients, uroflowmetric study was performed in a private room. The entire study group was informed to uri- UROLOGY JOURNAL Vol. 10 No. 4 Autumn
3 nate as their usual way of urination without any straining in both sitting and standing positions. Uroflowmetries with a voided volume less than 150 ml were disregarded and patients recalled for a new measurement at the same time of the corresponding day. Post voiding residue (PVR) was evaluated by transabdominal ultrasonography (Accuson X 300, Siemens AG, Munich, Germany). For this measurement, we used prolate ellipsoid method (Volume = Lenght Width Heigth 0.52) which was shown to be effective for evaluation of bladder volumes. (8) Patients were enrolled to uroflowmetry at the same time of the next day with a similar desire for urination, at a position other than the first day evaluation. Bladder capacity before voiding was the most important parameter that may change the results of uroflowmetric evaluation. We calculated the exact bladder capacity by adding PVR to voided volume during the test. The difference between the bladder capacities of corresponding days over 20% was thought to be a bias for the results. Study was repeated for the patients who had minimum 20% differences between the sum of voided volumes and PVR of corresponding days. All of the uroflowmetric parameters and PVR were compared in standing and sitting position. In order to evaluate the effect of urinary position on uroflowmetric parameters at different maximum flow rate (Qmax) values, we also subdivided the patients into three groups; as patients with Qmax < 10 ml/s, Qmax ml/s and Qmax > 15 ml/s. Statistical Analysis As we had 2 dependent groups in our study, we evaluated the normalcy of data by using one sample Kolmogorov-Smirnov test. Statistical analysis for normal data was performed by parametric test (paired t-test) and non-parametric test (Wilcoxon signed rank test) was performed for non-normal data. The statistical package for social science (SPSS Inc, Chicago, Illinois, USA) version 16.0 was used for statistical analysis. Differences were stated as statistically significant as P <.05. RESULTS After the exclusion of 52 patients, a total of 198 patients were enrolled to study (Figure). The mean age of study population was 57.1 ± 11.6 years. All patients were able to urinate in both standing and sitting positions. Only 13 patients urinate less than 150 ml during second uroflowmetric evaluation and re-evaluated in the subsequent day. There was no statistically significant difference at voided volume of patients in standing and sitting position as it was ± 81.8 ml and ± 82.4 ml, respectively (P =.505). Mean Qmax during urination at standing position was 15.3 ± 6.7 ml/s while it was 15.0 ± 7.0 ml/s at sitting position (P =.29). Mean average flow rate in standing position was 8.60 ± 4.0 ml/s and 8.25 ± 3.8 ml/s in sitting position (P =.054). There was a statistically significant difference between the median post-voiding residues in standing and sitting urination which was 29.5 (0-257) ml in standing and 47.5 (2-209) ml in sitting position (P <.0001). Other uroflowmetric parameters (time to Qmax and voiding time) was not statistically different between groups (Table 1). As Qmax values was shown to be related with the degree of bladder outlet obstruction, we sub-classified the patients as Qmax at standing position > 15 ml/s, ml/s and < 10 ml/s. (9) We evaluated the change of uroflowmetric parameters at different Qmax values of each group in standing and sitting position. There were 96 (48.5%) patients with Qmax > 15 ml/s, 64 (32.3%) patients with Qmax ml/s and 38 (19.2%) patients with Qmax < 10 ml/s. Voided volumes of all groups were similar in both sitting and standing positions and there was no statistically significant difference. Maximum flow rates in sitting and standing position were not significantly different in patients with different Qmax values (as subgroups are Qmax > 15 ml/s, Qmax ml/s and Qmax < 15 ml/s) whereas average flow rate presented a statistical difference in patients whose Qmax < 10 ml/s. The mean average flow rate increased 0.5mL/s in sitting position and this difference was found to be significant (P =.022). It was not surprising that mean time to peak flow and voiding time increased as mean maximum flow rates decreased, but there was no statistically significant difference between groups for those parameters. As it was documented in whole groups, PVR was significantly higher in sitting position of all subgroups (P <.001) (Table 2). Our study population was composed of patients who use sitting or standing position for voiding in their daily life Miscellaneous
4 Voiding Parameters in Positional Changes Yazici et al Table 1. Comparison of uroflowmetric parameters in standing and sitting position of whole study group. Standing Position Sitting Position Qmax (ml/s) 15.3 ± ± 7.0 P =.112** Time to peak flow, s 8.0 ( ) 8.3 ( ) P =.247* Average flow rate, ml/s 8.60 ± ± 3.8 P =.054** Voiding time, s 37.2 ± ± 18.9 P =.124** Voided volume, ml ± ± 82.4 P =.505** Post voiding residue, ml 29.5 (0-257) 47.5 (2-209) P <.0001* Key: Qmax, maximum flow rate. *Data were distributed non-normally according to Kolmogorov-Smirrov test so Wilcoxon signed rank test was performed for statistical analysis and P value was calculated using the median data values. **Data were distributed normally according to Kolmogorov-Smirrov test so paired t test was performed for statistical analysis and P value was calculated using the mean data values. There were 114 (57.6%) patients voiding at standing and 84 (42.4%) patients voiding in sitting position. We used patients natural voiding position as control group and evaluated the uroflowmetric parameter and PVR differences according to their natural voiding habit. The mean age of patients voiding in standing position was 56.4 ± 12.6 years. The mean age of patients voiding in sitting position was 58.2 ± 10.2 years (P =.062). Although it was not statistically significant, patients who were voiding in sitting position in their daily life had better Qmax values in sitting position. Patients who void in standing position in their daily life had significantly better uroflowmetric parameters at standing position. Nearly all uroflowmetric parameters except time to peak flow were significantly better when these patients performed uroflowmetry at their natural voiding position (standing position). On the other hand PVR was still significantly higher in sitting position unrelated to natural voiding position of patients (Table 3). DISCUSSION Uroflowmetry with PVR determination is an important and widely used urodynamic testing for evaluation of voiding dysfunction. Although it does not discriminate bladder outlet obstruction from detrusor insufficiency, it can give valuable objective data about both degree of obstruction and affectivity of the treatment. As micturition is a dynamic event, various external and internal factors may influence P this event. External factors are generally related with patients like; age, sex and psychological characteristics, whereas internal factors are mainly composed of the anatomical properties of lower urinary tract and corresponding tissues. Neurological innervations of bladder and urethra and the biomechanical properties of detrusor muscle, urethra and urethral meatus are supposed to be the main determinants of micturition in all voiding models. (10,11) At myocybernetic model defined by Bastiaanssen and colleagues, normal activity of sphincter was also supposed to be one of the factors related to micturition. According to this model, voiding position may affect striated muscle activity and geometrical properties of urethra and meatus. (10) Rad and colleagues found that, average angle between rectum and anal canal was 92 while sitting and becomes 132 when the patient gets to squatting position and concluded that this may cause relaxation of puborectalis muscles leading more easier bladder and bowel evacuation. (12) In another study, Bockus and colleagues reported that sitting position stretches the puborectalis muscle which slightly close urogenital hiatus. (13) Although there were no significant difference at Qmax and Q average values of patients in standing and sitting position, we found statistically significant higher PVR values at voiding in sitting position. This data also shows a slight obstruction at urogenital hiatus during micturition at sitting position independent to presence or absence of bladder outlet obstruction. Changes in parameters in healthy males There are some studies reporting controversial results about this subject. Yamanishi and colleagues, evaluated 21 healthy male patients in 5 different voiding positions (standing, sitting, lateral, supine and prone) and reported no difference between standing and sitting position in terms of uroflowmetric parameters. (5) In another study, Aghamir and colleagues evaluated 10 healthy males uroflowmetric parameters in standing and sitting position. They also found no difference and concluded that different voiding positions in healthy people did not influence uroflowmetric findings and PVR. (6) Confirming these findings, Unsal and colleagues found no difference in uroflowmetric parameters and PVR in standing and sitting position of 44 healthy UROLOGY JOURNAL Vol. 10 No. 4 Autumn
5 Table 2. Changes in uroflowmetric parameters in standing and sitting position according to maximum flow rates (Qmax). Qmax > 15 ml/s (n = 96) Qmax < 15 ml/s (n = 102) Standing Sitting P Standing Sitting P Qmax (ml/s) 20.7 ± ± ** 10.3 ± ± ** Time to peak flow, s 7.4 ( ) 7.4 ( ).944* 8.5 ( ) 9.6 (3-50.8).149* Average flow rate, ml/s 11.5 ± ± ** 5.7 ± ± ** Voiding time, s 28.5 ± ± ** 47.3 ± ± ** Voided volume, ml ± ± ** 254 ± ± ** Post voiding residue, ml 19 ( ) 35.5 (0-128) <.001* 44.0 (0-257) 66.5 (4-209) <.001* Qmax ml/s (n = 64) Qmax < 10 ml/s (n = 38) Standing Sitting P Standing Sitting P Qmax, ml/s 12.0 ± ± ** 7.4 ± ± ** Time to peak flow, s 8.1 ( ) 9.4 ( ).120* 14.7 ± ± ** Average flow rate, ml/s 6.7 ± ± ** 4.2 ± ± ** Voiding time, s 41.7 ± ± ** 55.5 ( ) 47.3 ( ).231** Voided volume, ml ± ± ** 247 ± ± ** Post voiding residue, ml 49.1 ± ± 47.9 < ± ± 38.9 <.001 Key: Qmax, maximum flow rate. *Data were distributed non-normally according to Kolmogorov-Smirrov test so Wilcoxon signed rank test was performed for statistical analysis and P value was calculated using the median data values. **Data were distributed normally according to Kolmogorov-Smirrov test so paired t test was performed for statistical analysis and P value was calculated using the mean data values. Table 3. Comparison of uroflowmetric parameters in standing and sitting position according to preferred voiding position in daily life. Patients preferring standing position for micturition Patients preferring sitting position for micturition Standing Sitting P Sitting Standing P Qmax, ml/sec 15.0 ± ± ** ± ± ** Time to peak flow, s 8.4 ( ) 9.2 ( ).257* 7.4 ( ) 7.5 ( ).653* Average flow rate, ml/s 8.4 ± ± ** 8.7 ± ± ** Voiding time, s 37.5 ± ± ** 37.0 ± ± ** Voided volume, ml 270 ± ± ** ± ± ** Post voiding residue, ml 32.0 (0-257) 48 (2-209) <.001* 45.5 (2.198) 25.0 (0-166) <.001* Key: Qmax, maximum flow rate. *Data were distributed non-normally according to Kolmogorov-Smirrov test so Wilcoxon signed rank test was performed for statistical analysis and P value was calculated using the median data values. **Data were distributed normally according to Kolmogorov-Smirrov test so paired t test was performed for statistical analysis and P value was calculated using the mean data values. males and concluded that patients might be asked for their preference voiding position during uroflowmetric evaluation. (7) In contrast, Eryildirim and colleagues reported that maximum and average flow rates were significantly higher in sitting position at their 30 healthy males series, but there was no difference in PVR values between these positions. (1) In another study with 61 young male participants, Choudhury and colleagues found significant lower flow rates at sitting position than standing position, but PVR was still not different between the groups. (2) We also did not find any significant difference in uroflowmetric parameters at standing and sitting position. Although it was not statistically significant, patients who had Qmax > 10 ml/s was able to void with higher flow rates and lower voiding time at standing position. It was not surprising that PVR increased as Qmax decreased. According to statistical analysis PVR was significantly higher in sitting position in all groups, but this difference was not over 25 ml and had no clinical im Miscellaneous
6 Voiding Parameters in Positional Changes Yazici et al portance in terms of treatment opportunities. According to our results patients who had high Qmax values were able to void better at standing position with significant lower PVR values. Changes of parameters in patients with lower Qmax values There are also limited numbers of studies evaluating the effect of voiding position on uroflowmetric parameters in patients with obstructive LUTS. Unsal and colleagues, reported the results of uroflowmetric parameters of 44 BPH and 44 healthy patients in both sitting and standing positions. They used maximum flow rate of 15 ml/s as cut-off point and did not find any difference in uroflowmetric parameters and PVR between the groups. (7) In another study with 10 BPH patients, authors found no difference in uroflowmetric parameters in standing and sitting position while PVR was significantly lower in sitting position. (6) We evaluated 102 patients with Qmax < 15 ml/s and did not find any difference in uroflowmetric parameters including Qmax, Q average and voided volume, but there was a significant difference in PVR. Same relation was also observed in patients with Qmax > 15 ml/s that PVR was significantly higher in sitting position while Qmax, Q average and voided volume was not statistically different in those patients. Opposing to Unsal and colleagues results, our study did not show any significant difference that Qmax value of 15 ml/s was a cut-off point for uroflowmetric parameters in standing and sitting position. We also did not find any difference at uroflowmetric parameters of patients who had borderline obstruction with Qmax ml/s. But, as obstruction became severe (Qmax < 10 ml/s), sitting position was seem to be more advantageous for flow rates that average flow rate was significantly higher in sitting position. This was the only significant difference of uroflowmetric parameters in our study. So the patients with Qmax values < 10 ml/s may be advised to urinate in sitting position to have higher Qmax values. Post voiding residue of patients with lower Qmax values was also significantly higher in sitting position, but like patients with high Qmax values, the difference was not over 25 ml and did not change treatment protocol for those patients. Figure. The study flow chart. Changes in parameters according to natural voiding position There are very limited studies evaluating the changes of uroflowmetric parameters related to voiding position other than patients daily life habit. In a study designed in Saudi Arabia, where participants void in sitting position because of religious traditions, authors found no difference in uroflowmetric parameters, whereas patients had significantly higher PVR values at standing position. But this difference between the mean PVR was not over 15 ml (73 ± 80.2 in sitting and 86.1 ± 77 in standing position). Although authors did not find any statistically significant difference at their series, they concluded that obliging the patients to void in a position to which they are not familiar may alter micturition act and might produce higher cerebellar inhibitory effect during voiding. (3) In our study, we had nearly equal number of patients who use standing or sitting position in their daily life (57.4% vs. 42.6%, respectively). In both group, patients had higher Qmax values when they performed uroflowmetric evaluation in their natural position and this relation was significant in patients who use standing position in their daily life. Patients, who were voiding in standing position, had 6% decrease in Qmax and 7% decrease in Q average values when they performed uroflowmetry at sitting posi- UROLOGY JOURNAL Vol. 10 No. 4 Autumn
7 tion. This decrease was lower and statistically insignificant in patients who use sitting position in their daily life as; 2.5% worsening in Qmax and no change on Q average. On the other hand, post voiding residue was significantly higher in sitting position in both groups, unrelated to natural voiding position. So, the uroflowmetric parameters were not affected by the natural voiding habit of patients in our study. Different voiding positions other than sitting and standing were also evaluated by some authors. Aghamir and colleagues, also evaluated crouching position and report no difference in uroflowmetric parameters. (6) Similar conclusion was also reported by Unsal and colleagues that crouching position did not alter uroflowmetric parameters in healthy males. (7) Although sitting position was seem to be advantageous than standing position, Eryildirim and colleagues reported no difference between sitting and squatting position. (1) On the other hand, Amjadi and colleagues reported a significant improvement of uroflowmetric parameters of obstructed patients as they micturate in crouching position. (4) In our study we were not able to analyze uroflowmetric differences in other voiding positions like crouching, squatting, recombinant or supine. But our entire study group was using standing or sitting position in their daily life. Different theories had been proposed to define the effect of voiding position on uroflowmetric parameters. According to their results, El-Bahnasawy and colleagues proposed that patients who void in the sitting position throughout their life will have micturitional reflexes modified and conditioned to this position. (3) But in our study we were able to observe that patients who void at sitting position in their whole life was able to void in standing position without any change in uroflowmetric parameters. Amjadi and colleagues, propose another theory according to their results and proposed that relaxation of pelvic floor musculature may be a reason for decrease in bladder outlet resistance and abdominal musculature may help to increase intra-abdominal pressure helping micturition in crouching position. (4) This may be true for crouching position but it does not seem to work in sitting position according to our results. Although we did not find significant uroflowmetric differences among voiding positions, we have similar results with Choudhury and colleagues and Uluocak and colleagues who demonstrated a decrease in uroflowmetric parameters in sitting position. (2,14) As it was shown at Uluocak s study, patients may have lower voiding detrusor pressure in sitting position. On the other hand gravity, slower detrusor contractions and altered geometry of bladder may be an advantage for voiding in standing position. Uroflowmetric evaluation is a popular and frequently used test that has been performed by many centers in all around the world. Although we had large number of patients in our study, this may not be enough to make a direct conclusion for general population. In order to understand the exact effect of voiding position on uroflowmetric parameters, more well-organized, prospective studies with higher number of participants are needed. CONCLUSION As a conclusion, the preferred voiding positions may differ among people because of several factors like social, cultural and medical reasons. As there are no clinically important uroflowmetric differences between voiding in sitting and standing positions, voiding position may be left to personal preferences during uroflowmetric evaluation. According to our results it seems that the best voiding position is the position in which patient feels most comfortable. CONFLICT OF INTEREST None declared. REFERENCES 1. Eryildirim B, Tarhan F, Kuyumcuoğlu U, Erbay E, Pembegül N. Position-related changes in uroflowmetric parameters in healthy young men. Neurourol Urodyn. 2006;25: Choudhury S, Agarwal MM, Mandal AK et al. Which voiding position is associated with lowest flow rates in healthy adult men? Role of natural voiding position. Neurourol Urodyn. 2010;29: El-Bahnasawy MS, Fadl FA. Uroflowmetric differences between standing and sitting positions for men used to void in the sitting position. Urology. 2008;71: Amjadi M, Madaen SK, Pour-Moazen H. Uroflowmetry findings in patients with bladder outlet obstruction symptoms in standing and crouching positions. Urol J. 2006;3: Miscellaneous
8 Voiding Parameters in Positional Changes Yazici et al 5. Yamanishi T, Yasuda K, Sakakibara R et al. Variation in urinary flow according to voiding position in normal males. Neurourol Urodyn. 1999;18: Aghamir SM, Mohseni M, Arasteh S. The effect of voiding position on uroflowmetry findings of healthy men and patients with benign prostatic hyperplasia. Urol J. 2005;2: Unsal A, Cimentepe E. Effect of voiding position on uroflowmetric parameters and post-void residual urine volume in patients with benign prostatic hyperplasia. Scand J Urol Nephrol. 2004;38: Dicuio M, Pomara G, Menchini Fabris F, Ales V, Dahlstrand C, Morelli G. Measurements of urinary bladder volume: comparison of five ultrasound calculation methods in volunteers. Arch Ital Urol Androl. 2005;77: J. de la Rosette, G. Alivizatos, S. Madersbacher et al. EAU Guidelines Benign prostatic hyperplasia; p Bastiaanssen EH, van Leeuwen JL, Vanderschoot J, Redert PA. A myocybernetic model of the lower urinary tract. J Theor Biol. 1996;178: Valentini FA, Besson GR, Nelson PP, Zimmern PE. A mathematical micturition model to restore simple flow recordings in healthy and symptomatic individuals and enhance uroflow interpretation. Neurourol Urodyn. 2000;19: Rad S. Impact of ethnic habits on defecographic measurements. Arch Iranian Med 2002;5: Bockus HL. Gastroenterology. Philadelphia: Saunders Co; vol 2, P Uluocak N, Oktar T, Acar O, Incesu O, Ziylan O, Erkorkmaz U. Positional changes in voiding dynamics of children with non-neurogenic bladder dysfunction. Urology. 2008;72: UROLOGY JOURNAL Vol. 10 No. 4 Autumn
Impact of urethral catheterization on uroflow during pressure-flow study
 Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
CHAPTER 6. M.D. Eckhardt, G.E.P.M. van Venrooij, T.A. Boon. hoofdstuk :49 Pagina 89
 hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
hoofdstuk 06 19-12-2001 09:49 Pagina 89 Urethral Resistance Factor (URA) Versus Schäfer s Obstruction Grade and Abrams-Griffiths (AG) Number in the Diagnosis of Obstructive Benign Prostatic Hyperplasia
Role of herbal drugs in the management of benign prostatic hyperplasia: Clinical trial to evaluate the efficacy and safety of Himplasia
 [Medicine Update (2003): 11(2), 55-58] Role of herbal drugs in the management of benign prostatic hyperplasia: Clinical trial to evaluate the efficacy and safety of Himplasia Arora, R.P., CMO, Rajiba L.
[Medicine Update (2003): 11(2), 55-58] Role of herbal drugs in the management of benign prostatic hyperplasia: Clinical trial to evaluate the efficacy and safety of Himplasia Arora, R.P., CMO, Rajiba L.
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Hee Young Park, Joo Yong Lee, Sung Yul Park, Seung Wook Lee, Yong Tae Kim, Hong Yong Choi, Hong Sang Moon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.92 Voiding Dysfunction Efficacy of Alpha Blocker Treatment According to the Degree of Intravesical Prostatic Protrusion Detected by Transrectal
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.2.92 Voiding Dysfunction Efficacy of Alpha Blocker Treatment According to the Degree of Intravesical Prostatic Protrusion Detected by Transrectal
Clinical Study Treatment Strategy According to Findings on Pressure-Flow Study for Women with Decreased Urinary Flow Rate
 Advances in Urology Volume 2009, Article ID 782985, 5 pages doi:10.1155/2009/782985 Clinical Study Treatment Strategy According to Findings on Pressure-Flow Study for Women with Decreased Urinary Flow
Advances in Urology Volume 2009, Article ID 782985, 5 pages doi:10.1155/2009/782985 Clinical Study Treatment Strategy According to Findings on Pressure-Flow Study for Women with Decreased Urinary Flow
LUTS after TURP: How come and how to manage? Matthias Oelke
 LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
LUTS after TURP: How come and how to manage? Matthias Oelke Department of Urology Global Congress on LUTD, Rome, 26 th June 2015 Disclosures Consultant, speaker, trial participant and/or research grants
EXPERIMENTAL AND THERAPEUTIC MEDICINE 4: , 2012
 1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
EFFECT OF INTRAVESICAL PROSTATIC PROTRUSION (IVPP) ON LOWER URINARY TRACT FUNCTION AND MANAGEMENT
 EFFECT OF INTRAVESICAL PROSTATIC PROTRUSION (IVPP) ON LOWER URINARY TRACT FUNCTION AND MANAGEMENT Rajaraman T 1, Balaji A. R 2, Vetrichandar S 3, Shekar M. G 4, Bhat K. R. S 5, Muthurathinam R 6, Ashokkumar
EFFECT OF INTRAVESICAL PROSTATIC PROTRUSION (IVPP) ON LOWER URINARY TRACT FUNCTION AND MANAGEMENT Rajaraman T 1, Balaji A. R 2, Vetrichandar S 3, Shekar M. G 4, Bhat K. R. S 5, Muthurathinam R 6, Ashokkumar
EAU GUIDELINES POCKET EDITION 3
 EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
EAU GUIDELINES POCKET EDITION 3 CONTENTS: BENIGN PROSTATIC HYPERPLASIA URINARY INCONTINENCE UROLITHIASIS 2 3 EAU POCKET GUIDELINES POCKET EDITION 3 This is one of a series of convenient pocket size books
Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic Study
 www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.12.840 Voiding Dysfunction/Female Urology Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic
www.kjurology.org http://dx.doi.org/10.4111/kju.2013.54.12.840 Voiding Dysfunction/Female Urology Effect of Transurethral Resection of the Prostate Based on the Degree of Obstruction Seen in Urodynamic
Index. urologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Index Note: Page numbers of article titles are in boldface type. A Ablative therapies, transurethral needle ablation, Adverse events, sexual side effects of BPH Aging, and incidence of BPH associated with
Chapter 4: Research and Future Directions
 Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
Chapter 4: Research and Future Directions Introduction Many of the future research needs listed in the 1994 Agency for Health Care Policy and Research (AHCPR) clinical practice guideline Benign Prostatic
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach)
 Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
Dysfunctional Voiding Patients: When Do you Give Medication and Why (A Practical approach) Andrew Combs, PA-C Director, Pediatric Urodynamics Division of Pediatric Urology New York Presbyterian-Weill Cornell
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME?
 URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Patient Information. Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE
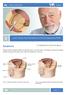 Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
Patient Information English 32 Lower Urinary Tract Symptoms (LUTS) and Diagnosis of BPE Symptoms The underlined terms are listed in the glossary. Benign prostatic enlargement (BPE) can affect the way you
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
Voiding Dysfunction Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU.
 Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Lower urinary tract symptoms (LUTS) are common, affecting approximately
 Diagn Interv Radiol 2012; 18:277 281 Turkish Society of Radiology 2012 ABDOMINAL IMAGING ORIGINAL ARTICLE Diagnostic values of detrusor wall thickness, postvoid residual urine, and prostate volume to evaluate
Diagn Interv Radiol 2012; 18:277 281 Turkish Society of Radiology 2012 ABDOMINAL IMAGING ORIGINAL ARTICLE Diagnostic values of detrusor wall thickness, postvoid residual urine, and prostate volume to evaluate
Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study
 Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study Yoshihisa Matsukawa,* Momokazu Gotoh, Tomonori Komatsu, Yasuhito Funahashi, Naoto Sassa and Ryohei Hattori
Efficacy of Silodosin for Relieving Benign Prostatic Obstruction: Prospective Pressure Flow Study Yoshihisa Matsukawa,* Momokazu Gotoh, Tomonori Komatsu, Yasuhito Funahashi, Naoto Sassa and Ryohei Hattori
PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA
 St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
St. Louis Hospital PROSTATIC EMBOLIZATION FOR BENIGN HYPERPLASIA INITIAL CLINICAL RESULTS Faculty of Medical Sciences New University of Lisbon JOÃO PISCO LUÍS CAMPOS PINHEIRO TIAGO BILHIM HUGO RIO TINTO
DOWNLOAD OR READ : TREATMENT OF BENIGN PROSTATIC HYPERPLASIA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TREATMENT OF BENIGN PROSTATIC HYPERPLASIA PDF EBOOK EPUB MOBI Page 1 Page 2 treatment of benign prostatic hyperplasia treatment of benign prostatic pdf treatment of benign prostatic
DOWNLOAD OR READ : TREATMENT OF BENIGN PROSTATIC HYPERPLASIA PDF EBOOK EPUB MOBI Page 1 Page 2 treatment of benign prostatic hyperplasia treatment of benign prostatic pdf treatment of benign prostatic
RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, PATIENTS WITH BENIGN PROSTATIC HYPERPLASIA
 American Urological Association symptom index for BPH RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, AND DISEASE-SPECIFIC QUALITY OF LIFE QUESTION IN PATIENTS WITH
American Urological Association symptom index for BPH RELATIONSHIPS BETWEEN AMERICAN UROLOGICAL ASSOCIATION SYMPTOM INDEX, PROSTATE VOLUME, AND DISEASE-SPECIFIC QUALITY OF LIFE QUESTION IN PATIENTS WITH
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Office Management of Benign Prostatic Enlargement
 Focus on CME at McGill University Office Management of Benign Prostatic Enlargement Symptomatic benign prostate enlargement is a common medical problem encountered in our aging society. Watchful waiting,
Focus on CME at McGill University Office Management of Benign Prostatic Enlargement Symptomatic benign prostate enlargement is a common medical problem encountered in our aging society. Watchful waiting,
Development of mathematical model for lower urinary tract dysfunctions
 Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
Development of mathematical model for lower urinary tract dysfunctions Mohanad A.Deaf 1, Mohamed A.A.Eldosoky 1, Ahmed M. El-Garhy 2, Hesham W.Gomma 2, Ahmed S.El-Azab 3 Dept. of Biomedical Engineering,
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Effects of Isosorbide Dinitrate on the Urinary Flow Rate in Patients With Benign Prostatic Hyperplasia
 Miscellaneous Effects of Isosorbide Dinitrate on the Urinary Flow Rate in Patients With Benign Prostatic Hyperplasia Ali Roshani, 1 Iraj Khosropanah, 1 Mohammad Salehi, 1 Alireza Noshad Kamran 2 Keywords:
Miscellaneous Effects of Isosorbide Dinitrate on the Urinary Flow Rate in Patients With Benign Prostatic Hyperplasia Ali Roshani, 1 Iraj Khosropanah, 1 Mohammad Salehi, 1 Alireza Noshad Kamran 2 Keywords:
A Comparative Study of Efficacy and Safety Between Tamsulosin and Terazosin in the Treatment of Symptomatic Benign Prostatic Hyperplasia
 Chattagram Maa-O-Shishu Hospital Medical College Journal Original Article A Comparative Study of Efficacy and Safety Between Tamsulosin and Terazosin in the Treatment of Symptomatic Benign Prostatic Hyperplasia
Chattagram Maa-O-Shishu Hospital Medical College Journal Original Article A Comparative Study of Efficacy and Safety Between Tamsulosin and Terazosin in the Treatment of Symptomatic Benign Prostatic Hyperplasia
= 0.62, P <0.001) with important clinical exceptions. There was negative correlation between the PV and Qmax (r s
 Original Article 60 Relationships between Prostatic Volume and Intravesical Prostatic Protrusion on Transabdominal Ultrasound and Benign Prostatic Obstruction in Patients with Lower Urinary Tract Symptoms
Original Article 60 Relationships between Prostatic Volume and Intravesical Prostatic Protrusion on Transabdominal Ultrasound and Benign Prostatic Obstruction in Patients with Lower Urinary Tract Symptoms
Hakmin Lee, Minsoo Choo, Myong Kim, Sung Yong Cho, Seung Bae Lee, Hyeon Jeong, Hwancheoul Son
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.1.47 Original Article - Voiding Dysfunction http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.1.47&domain=pdf&date_stamp=2014-1-17 Changes
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.1.47 Original Article - Voiding Dysfunction http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.1.47&domain=pdf&date_stamp=2014-1-17 Changes
H6D-MC-LVHR Clinical Study Report Synopsis Page LVHR Synopsis (LY450190)
 H6D-MC-LVHR Clinical Study Report Synopsis Page 1 2. LVHR Synopsis H6D-MC-LVHR Clinical Study Report Synopsis Page 2 Clinical Study Report Synopsis: Study H6D-MC-LVHR Title of Study: A Randomized, Double-Blind,
H6D-MC-LVHR Clinical Study Report Synopsis Page 1 2. LVHR Synopsis H6D-MC-LVHR Clinical Study Report Synopsis Page 2 Clinical Study Report Synopsis: Study H6D-MC-LVHR Title of Study: A Randomized, Double-Blind,
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Original Article - Lasers in Urology. Min Ho Lee, Hee Jo Yang, Doo Sang Kim, Chang Ho Lee, Youn Soo Jeon
 www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
www.kjurology.org http://dx.doi.org/10.4111/kju.2014.55.11.737 Original Article - Lasers in Urology http://crossmark.crossref.org/dialog/?doi=10.4111/kju.2014.55.11.737&domain=pdf&date_stamp=2014-11-16
Prostate Gland Volume and Its Relationship to Complications of Benign Prostatic Enlargement
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 6 Ver. II (Jun. 2015), PP 33-37 www.iosrjournals.org Prostate Gland Volume and Its Relationship
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 6 Ver. II (Jun. 2015), PP 33-37 www.iosrjournals.org Prostate Gland Volume and Its Relationship
Assistant Professor, Department of General Surgery, NEIGRIHMS, Shillong, Meghalaya, India
 Original Research Article Study of the Relationship between Presence of Bilateral Inguinal Hernia and Intensity of Lower Urinary Tract Symptoms in a Tertiary Care Centre of Eastern India Partha Pratim
Original Research Article Study of the Relationship between Presence of Bilateral Inguinal Hernia and Intensity of Lower Urinary Tract Symptoms in a Tertiary Care Centre of Eastern India Partha Pratim
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Lasers in Urology. Sae Woong Choi, Yong Sun Choi, Woong Jin Bae, Su Jin Kim, Hyuk Jin Cho, Sung Hoo Hong, Ji Youl Lee, Tae Kon Hwang, Sae Woong Kim
 www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.12.824 Lasers in Urology 120 W Greenlight HPS Laser Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia in
www.kjurology.org http://dx.doi.org/10.4111/kju.2011.52.12.824 Lasers in Urology 120 W Greenlight HPS Laser Photoselective Vaporization of the Prostate for Treatment of Benign Prostatic Hyperplasia in
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Increasing Awareness, Diagnosis, and Treatment of BPH, LUTS, and EP
 Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
Introduction to Enlarged Prostate E. David Crawford, MD Professor of Surgery (Urology) and Radiation Oncology Head, Urologic Oncology E. David Crawford Endowed Chair in Urologic Oncology University of
LONG-TERM SAFETY AND EFFICACY OF TAMSULOSIN FOR THE TREATMENT OF LOWER URINARY TRACT SYMPTOMS ASSOCIATED WITH BENIGN PROSTATIC HYPERPLASIA
 0022-5347/03/1702-0498/0 Vol. 170, 498 502, August 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000076140.68657.fd LONG-TERM SAFETY
0022-5347/03/1702-0498/0 Vol. 170, 498 502, August 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000076140.68657.fd LONG-TERM SAFETY
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page
 The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page 1377-1386 Evaluation of Silodosin in Comparison to Tamuslosin in Treatment of Benign Prostatic Hyperplasia with lower Urinary
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page 1377-1386 Evaluation of Silodosin in Comparison to Tamuslosin in Treatment of Benign Prostatic Hyperplasia with lower Urinary
Adrenoceptor Antagonist Tamsulosin for the Treatment of Voiding Symptoms Improves Nocturia and Sleep Quality in Women. The α 1 FEMALE UROLOGY
 The α 1 Adrenoceptor Antagonist Tamsulosin for the Treatment of Voiding Symptoms Improves Nocturia and Sleep Quality in Women Sun-Ouck Kim, Hyang Sik Choi, Dongdeuk Kwon FEMALE UROLOGY Department of Urology,
The α 1 Adrenoceptor Antagonist Tamsulosin for the Treatment of Voiding Symptoms Improves Nocturia and Sleep Quality in Women Sun-Ouck Kim, Hyang Sik Choi, Dongdeuk Kwon FEMALE UROLOGY Department of Urology,
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National
 Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Okubo, Kazutoshi; Aoki, Katsuya; Wa. Right Research, Inc. Published by Elsevie
 Title Objective patterning of uroflowmetr daytime and nighttime wetting. Kanematsu, Akihiro; Johnin, Kazuyos Author(s) Okubo, Kazutoshi; Aoki, Katsuya; Wa Yoshino, Kaoru; Tanaka, Shiro; Tani Osamu Citation
Title Objective patterning of uroflowmetr daytime and nighttime wetting. Kanematsu, Akihiro; Johnin, Kazuyos Author(s) Okubo, Kazutoshi; Aoki, Katsuya; Wa Yoshino, Kaoru; Tanaka, Shiro; Tani Osamu Citation
Overview. Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia. Iain McAuley September 15, 2014
 Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
Urology Dine and Learn: Erectile Dysfunction & Benign Prostatic Hyperplasia Iain McAuley September 15, 2014 Overview Review of the most recent guidelines for ED and BPH ED Guidelines CUA 2006 AUA 2011
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity
 ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
Novel Natural Fill Telemetric Pressure Flow Study of Discomfort and Bladder Outlet Obstruction
 Novel Natural Fill Telemetric Pressure Flow Study of Discomfort and Bladder Outlet Obstruction Hyoun-Joong Kong, Sunmee Park, Tack Lee, Ji Youl Lee, Hee Chan Kim and Seung-June Oh* From the Interdisciplinary
Novel Natural Fill Telemetric Pressure Flow Study of Discomfort and Bladder Outlet Obstruction Hyoun-Joong Kong, Sunmee Park, Tack Lee, Ji Youl Lee, Hee Chan Kim and Seung-June Oh* From the Interdisciplinary
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
National Kidney and Urologic Diseases Information Clearinghouse
 Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
Urodynamic Testing National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the urinary tract? The urinary tract
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
Cross-sectional and longitudinal studies on interaction between bladder compliance and outflow obstruction in men with benign prostatic hyperplasia
 Asian J Androl 2007; 9 (1): 51 56 DOI: 10.1111/j.1745-7262.2007.00221.x www.asiaandro.com. Original Article. Cross-sectional and longitudinal studies on interaction between bladder compliance and outflow
Asian J Androl 2007; 9 (1): 51 56 DOI: 10.1111/j.1745-7262.2007.00221.x www.asiaandro.com. Original Article. Cross-sectional and longitudinal studies on interaction between bladder compliance and outflow
Pressure-flow nomogram for women with lower urinary
 Clinical research Pressure-flow nomogram for women with lower urinary tract symptoms Bartosz Dybowski, Ewa Bres-Niewada, Piotr Radziszewski Department of Urology, Medical University of Warsaw, Poland Submitted:
Clinical research Pressure-flow nomogram for women with lower urinary tract symptoms Bartosz Dybowski, Ewa Bres-Niewada, Piotr Radziszewski Department of Urology, Medical University of Warsaw, Poland Submitted:
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
THE EVOLUTION OF DETRUSOR OVERACTIVITY AFTER WATCHFUL WAITING, MEDICAL THERAPY AND SURGERY IN PATIENTS WITH BLADDER OUTLET OBSTRUCTION
 0022-5347/03/1692-0535/0 Vol. 169, 535 539, February 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000045600.69261.73 THE EVOLUTION
0022-5347/03/1692-0535/0 Vol. 169, 535 539, February 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000045600.69261.73 THE EVOLUTION
NON-Neurogenic Chronic Urinary Retention AUA White Paper
 NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
NON-Neurogenic Chronic Urinary Retention AUA White Paper Great Lakes SUNA Inside Urology March 16, 2018 Michelle J. Lajiness FNP-BC Nurse Practitioner DMC Urology Incidence Really unknown Lack consensus
Impact of Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Treatment with Tamsulosin and Solifenacin Combination Therapy on Erectile Function
 www.kjurology.org DOI:10.4111/kju.2011.52.1.49 Sexual Dysfunction Impact of Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Treatment with Tamsulosin and Solifenacin Combination Therapy on Erectile
www.kjurology.org DOI:10.4111/kju.2011.52.1.49 Sexual Dysfunction Impact of Lower Urinary Tract Symptoms/Benign Prostatic Hyperplasia Treatment with Tamsulosin and Solifenacin Combination Therapy on Erectile
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION
 EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
EAU GUIDELINES ON NON- NEUROGENIC MALE LUTS INCLUDING BENIGN PROSTATIC OBSTRUCTION (Text update March 2017) S. Gravas (Chair), T. Bach, M. Drake, M. Gacci, C. Gratzke, T.R.W. Herrmann, S. Madersbacher,
Alpha antagonists from initial concept to routine clinical practice
 european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
Shrestha A, Chalise PR, Sharma UK, Gyawali PR, Shrestha GK, Joshi BR. Department of Surgery, TU Teaching Hospital, Maharajgunj, Kathmandu, Nepal
 Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
Original Article Intravesical Prostatic Protrusion is better than Prostate Volume in Predicting Symptom Severity in Benign Prostatic Hyperplasia: A Prospective Clinical Study Shrestha A, Chalise PR, Sharma
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Elderly Men with Luts: The Role of Urodynamics
 Original Research Paper Medical Science Elderly Men with Luts: The Role of Urodynamics Dr. Ala a Al-Deen Al-Dabbagh Consultant urologist,al-yarmouk Teaching Hospital Department of urology/baghdad/iraq,
Original Research Paper Medical Science Elderly Men with Luts: The Role of Urodynamics Dr. Ala a Al-Deen Al-Dabbagh Consultant urologist,al-yarmouk Teaching Hospital Department of urology/baghdad/iraq,
Can men with prostates sized 80 ml or larger be managed conservatively?
 Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Original Article - Lower Urinary Tract Dysfunction Investig Clin Urol 2017;58:359-364. pissn 2466-0493 eissn 2466-054X Can men with prostates sized 80 ml or larger be managed conservatively? Alvin Lee,
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Case studies: LUTS. Case 1 history. Case 1 - questions. Case 1 - outcome. Case 2 - history. Case 1 learning point 14/07/2015 DR JON REES
 Case 1 history Case studies: LUTS DR JON REES A 49 year old male comes to see you he has had gradual deterioration of his flow over the last few years- he saw a colleague of yours 6 weeks ago who recorded
Case 1 history Case studies: LUTS DR JON REES A 49 year old male comes to see you he has had gradual deterioration of his flow over the last few years- he saw a colleague of yours 6 weeks ago who recorded
Bladder outlet obstruction number- a good indicator of infravesical obstruction in patients with benign prostatic enlargement?
 Bladder outlet obstruction number- a good indicator of infravesical obstruction in patients with benign prostatic enlargement? Damir Aganovic*, Hajrudin Spahovic, Alden Prcic, Osman Hadziosmanovic Department
Bladder outlet obstruction number- a good indicator of infravesical obstruction in patients with benign prostatic enlargement? Damir Aganovic*, Hajrudin Spahovic, Alden Prcic, Osman Hadziosmanovic Department
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Does uroflowmetry parameter facilitate discrimination between detrusor underactivity and bladder outlet obstruction?
 Original Article - Lower Urinary Tract Dysfunction pissn 2466-0493 eissn 2466-054X Does uroflowmetry parameter facilitate discrimination between detrusor underactivity and bladder outlet obstruction? Kwon
Original Article - Lower Urinary Tract Dysfunction pissn 2466-0493 eissn 2466-054X Does uroflowmetry parameter facilitate discrimination between detrusor underactivity and bladder outlet obstruction? Kwon
An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms
 Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Case Report INJ 2010;14:125-129 An Anteriorly Positioned Midline Prostatic Cyst Resulting in Lower Urinary Tract Symptoms Joo-Yong Lee, Dong-Hyuk Kang, Hee-Young Park, Jung-Soo Park, Young-Woo Son, Hong-Sang
Clinical Studies with Speman in Cases of Benign Enlargement of Prostate
 [The Indian Practitioner (1971): 6, 281] Clinical Studies with Speman in Cases of Benign Enlargement of Prostate Agarwal, V.K., M.S., F.I.C.S., Professor of Surgery, and Gupta, R.K., M.B.,B.S., Research
[The Indian Practitioner (1971): 6, 281] Clinical Studies with Speman in Cases of Benign Enlargement of Prostate Agarwal, V.K., M.S., F.I.C.S., Professor of Surgery, and Gupta, R.K., M.B.,B.S., Research
Female Urology MANAGEMENT OF FUNCTIONAL BLADDER NECK OBSTRUCTION IN WOMEN: USE OF -BLOCKERS AND PEDIATRIC RESECTOSCOPE FOR BLADDER NECK INCISION
 0022-5347/99/1626-2061/0 THE JOURNAL OF UROLOGY Vol. 162, 2061 2065, December 1999 Copyright 1999 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. Female Urology MANAGEMENT OF FUNCTIONAL BLADDER
0022-5347/99/1626-2061/0 THE JOURNAL OF UROLOGY Vol. 162, 2061 2065, December 1999 Copyright 1999 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. Female Urology MANAGEMENT OF FUNCTIONAL BLADDER
Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy?
 Original Article Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy? Sherif Azab 1, Ayman Osama 2, Mona Rafaat 3 1 Urology Department, Faculty
Original Article Does normalizing PSA after successful treatment of chronic prostatitis with high PSA value exclude prostatic biopsy? Sherif Azab 1, Ayman Osama 2, Mona Rafaat 3 1 Urology Department, Faculty
Urodynamic Assessments of Bladder Outflow Obstruction Associated with Benign Prostatic Hyperplasia
 Original Article Urodynamic Assessments of Bladder Outflow Obstruction Associated with Benign Prostatic Hyperplasia Kun Dou, MD; QiGui Liu, MD; Xin Li, MD; QingYu Zhou, MD; XiaoLu Han, MD Kun Dou is a
Original Article Urodynamic Assessments of Bladder Outflow Obstruction Associated with Benign Prostatic Hyperplasia Kun Dou, MD; QiGui Liu, MD; Xin Li, MD; QingYu Zhou, MD; XiaoLu Han, MD Kun Dou is a
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
INVESTIGATION OF LOWER URINARY TRACT SYMPTOMS IN UROLOGICAL OUTPATIENTS USING ORIGINAL IPSS PLUS POST MICTURITION DRIBBLE QUESTIONNAIRE
 INVESTIGATION OF LOWER URINARY TRACT SYMPTOMS IN UROLOGICAL OUTPATIENTS USING ORIGINAL IPSS PLUS POST MICTURITION DRIBBLE QUESTIONNAIRE Tadashi Hanail*, Seiji Matsumotol*, Nobutaka Shimizu, Hirotsugu Uemural
INVESTIGATION OF LOWER URINARY TRACT SYMPTOMS IN UROLOGICAL OUTPATIENTS USING ORIGINAL IPSS PLUS POST MICTURITION DRIBBLE QUESTIONNAIRE Tadashi Hanail*, Seiji Matsumotol*, Nobutaka Shimizu, Hirotsugu Uemural
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Predictors of short-term overactive bladder symptom improvement after transurethral resection of prostate in men with benign prostatic obstruction
 bs_bs_banner International Journal of Urology (2014) 21, 1035 1040 doi: 10.1111/iju.12482 Original Article: Clinical Investigation Predictors of short-term overactive bladder symptom improvement after
bs_bs_banner International Journal of Urology (2014) 21, 1035 1040 doi: 10.1111/iju.12482 Original Article: Clinical Investigation Predictors of short-term overactive bladder symptom improvement after
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
Testosterone Replacement Alone for Testosterone Deficiency Syndrome Improves Moderate Lower Urinary Tract Symptoms: One Year Follow-Up
 pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 April 31(1): 47-52 http://dx.doi.org/10.5534/wjmh.2013.31.1.47 Original Article Testosterone Replacement Alone for Testosterone Deficiency Syndrome
pissn: 2287-4208 / eissn: 2287-4690 World J Mens Health 2013 April 31(1): 47-52 http://dx.doi.org/10.5534/wjmh.2013.31.1.47 Original Article Testosterone Replacement Alone for Testosterone Deficiency Syndrome
BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY IN CHILDREN
 0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
A Study of Relationship of Prostate Volume, Prostate Specific Antigen and age in Benign Prostatic Hyperplasia
 ORIGINAL RESEARCH www.ijcmr.com A Study of Relationship of Prostate Volume, Prostate Specific Antigen and age in Benign Prostatic Hyperplasia Rupam Deori 1, Bijoyananda Das 2, Mustafa Abdur Rahman 3 ABSTRACT
ORIGINAL RESEARCH www.ijcmr.com A Study of Relationship of Prostate Volume, Prostate Specific Antigen and age in Benign Prostatic Hyperplasia Rupam Deori 1, Bijoyananda Das 2, Mustafa Abdur Rahman 3 ABSTRACT
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
