A cute idiopathic autonomic neuropathy (AIAN),1 2
|
|
|
- Eustace Chambers
- 6 years ago
- Views:
Transcription
1 PAPER Micturition disturbance in acute idiopathic autonomic neuropathy R Sakakibara, T Uchiyama, M Asahina, A Suzuki, T Yamanishi, T Hattori... See end of article for authors affiliations... Correspondence to: Dr Ryuji Sakakibara, Department of Neurology, Chiba University, Inohana Chuo-Ku, Chiba , Japan; sakaki@med.m. chiba-u.ac.jp Received 26 March 2003 In revised form 6 May 2003 Accepted 7 May J Neurol Neurosurg Psychiatry 2004;75: Objective: To define the nature of micturition disturbance in patients with acute idiopathic autonomic neuropathy (AIAN). Methods: Micturitional symptoms were observed during hospital admissions and the in outpatient clinics in six patients with clinically definite AIAN (typical form in four, cholinergic in one, autonomicsensory in one). included medium-fill water cystometry, external sphincter electromyography, and a bethanechol test. Results: Four patients had and two had as the initial presentation. Patients with retention became able to urinate within a week (two to seven days). The major symptoms at the time of urodynamic studies (three weeks to four months after disease onset in most cases) were voiding difficulty and nocturnal frequency. None had urinary incontinence. Complete recovery from the micturition disturbance took from three months to.18 years. The recovery period was shorter in a patient with cholinergic, and it was longer in two patients who had a longer duration of initial. Micturition disturbance tended to improve earlier than orthostatic hypotension. The major urodynamic abnormalities were detrusor areflexia on voiding (5), denervation supersensitivity to bethanechol (3); low compliance detrusor (1); and impaired bladder sensation (2). None had neurogenic motor unit potentials of the external sphincter muscles. Conclusions: In patients with AIAN, and are common initial presentations. The underlying mechanisms seem to be pre- and postganglionic cholinergic dysfunction with preservation of somatic sphincter function. The bladder problems tend to improve earlier than orthostatic hypotension. A cute idiopathic autonomic neuropathy (AIAN),1 2 or pure pandysautonomia, is a rare but distinct clinical entity first described by Young et al in The disorder involves both sympathetic and parasympathetic nervous systems, with an acute onset, a monophasic course, and partial recovery with relative preservation of sensory function. 5 Somatic motor function is almost completely preserved. The site of lesions is the pre- and postganglionic autonomic fibres, 1 5 and the disorder is thought to have an autoimmune aetiology similar to the Guillain-Barré syndrome. 6 7 Variant forms may also occur, 5 in which sensory fibres are involved 8 9 or cholinergic autonomic fibres alone are affected. 10 The most common presenting symptoms of AIAN are orthostatic hypotension (postural dizziness, syncope), gastrointestinal (nausea, vomiting, diarrhoea, constipation, intestinal pseudo-obstruction), and sudomotor (failure to sweat, causing heat intolerance and flushing). 5 Disturbances of micturition are known to occur in this disorder, and most patients suffer from and retention, which often requires an indwelling urinary catheter. However, few studies have attempted to follow up the bladder symptoms and investigate the underlying mechanism, though Kirby et al investigated two patients with this condition. 11 In this paper we outline our findings relating to the micturition histories in six patients with AIAN, and describe the urodynamic studies that were done. METHODS Patients This was a retrospective study in which we reviewed the records of six patients with AIAN, all of whom satisfied the inclusion and exclusion diagnostic criteria Two were male 287 and four were female, median age of onset 30 years (range 9 to 46). All the patients experienced acute exacerbations of autonomic abnormalities during the first two to four weeks, but motor function was almost completely preserved. On the basis of the neurological and neurophysiological findings and the autonomic function tests (done within a month of onset except in two cases) (table 1), four patients (cases 2, 3, 4, and 5) were considered to have the typical form of the disease and the other two to have forms (case 1, acute cholinergic autonomic neuropathy; case 6, acute autonomicsensory neuropathy). Procedures Micturitional and other autonomic symptoms were observed during hospital admission and in the follow up outpatient clinic. The follow up period was six months in one patient and more than four years (4 to 18) in five. Micturition status of the patients with an indwelling urinary catheter was evaluated at least one week after removal of the catheter. Patients with urinary symptoms did not have urinary tract infection. One patient under 10 years of age (case 2) did not have a recent history of enuresis. In four patients, urodynamic studies were done three weeks to four months after the onset of disease, while in the remaining two patients, urodynamic and autonomic function tests were done four and 18 years after the onset of disease. In one patient (case 3) the urodynamic studies were repeated. None of the male patients studied had prostatic hypertrophy on abdominal ultrasonography. Informed consent was obtained from all the patients before the urodynamic studies were done. In the patients, we also undertook peripheral nerve examinations including nerve conduction studies and sural nerve biopsy.
2 288 Sakakibara, Uchiyama, Asahina, et al Table 1 Patient details and results of the autonomic function tests Patient Variable 1 (KA) 2 (TO) 3 (TO) 4 (MM) 5 (CK) 6 (ET) Age of onset (years)/sex 46/M 9/M 23/M 34/M 37/F 28/F Initial symptoms Anhidrosis, Diarrhoea, vomiting, Abdominal distension, vomiting Syncope Vomiting, Abdominal pain, diarrhoea Clinical form Cholinergic The urodynamic studies consisted of uroflowmetry, measurement of residual urine, urethral pressure profilometry, medium-fill (50 ml/min) water cystometry, and external sphincter electromyography (EMG) with a urodynamic computer (Urovision; Lifetech, Houston, Texas, USA) and an EMG computer (Neuropack S; Nihon Kohden, Tokyo, Japan). Uroflow curves were evaluated according to Siroky s nomogram. 16 The normal ranges of urodynamic variables were: residual urine volume under 30 ml; maximum urethral closure pressure more than 41 cm H 2 O and less than 82 cm H 2 O; first sensation at the bladder volume more than 100 ml but less than 300 ml; and bladder capacity more than 200 ml but less than 600 ml. Increased first sensation and/or bladder capacity indicates impaired bladder sensation. Analysis of sphincter motor unit potentials was done in four patients using a concentric needle electrode. According Typical form Typical form Typical form Typical form Autonomic-sensory Autonomic signs and symptoms Orthostatic syncope Pupillary abnormality Tonic pupil Tonic pupil Tonic pupil Anhidrosis Paroxysmal coughing Constipation/intestinal pseudo-obstruction Erectile dysfunction + + (afterwards) + + Urinary dysfunction Retention (3 days), Retention (7days), Voiding difficulty, nocturia Voiding difficulty Retention (2 days), Deep tendon reflexes Normal Absent Absent Absent Decreased Absent Retention (7 days), Sensory signs and symptoms Tingling sensation/numbness + (hands, feet) + (hands) + (generalised) + (generalised) Decrease in pain, touch + (hands) + (hands) + (generalised) Decrease in position, vibration/sensory ataxia, Romberg sign + (generalised) Autonomic function tests,18 years later.,4 years later. Cardiovascular function Systolic pressure fall (mm Hg) in head up tilt (70, 10 min) (normal,20) Normal Normal* 50 (30 ) (30 ) 58 Supine plasma noradrenaline (NA) (pg/ml) (normal.100) 291 np Supersensitivity to NA infusion (0.1 mg/kg, 5 min) Np np Sudomotor function Thermal/sympathetic sweat response Absent Absent Absent np Absent Absent Pupillary responses Supersensitivity to 1.25% NA instillation (60 min) Normal + + Normal + + Supersensitivity to 0.125% pilocarpine instillation (30 min) Normal np Peripheral nerve examination Nerve conduction studies Median, ulnar, tibial, sural nerves Normal Normal Normal Normal Normal Decreased SNAP Sural nerve biopsy Light microscopy: decreased fibre density + np np Electron microscopy (compared with control) Np np Small myelinated 7%, unmyelinated 3% *With heart rate increase of 60 beats/min (postural tachycardia syndrome). F, female; M, male; np, not performed; SNAP: sensory nerve action potential. np Small myelinated 26%, unmyelinated 9% to the criteria proposed by Palace et al, 17 neurogenic sphincter EMG was diagnosed when either of the following abnormalities was present: average duration of motor unit potentials.10 ms;.20% of motor unit potentials with a duration of.10 ms. A bethanechol test was done in five patients. After an infusion of 100 ml of water, 2.5 mg of bethanechol chloride was injected subcutaneously and detrusor pressure was measured for 30 minutes. A detrusor pressure increase of.15 mm H 2 O during the test is considered high. 18 The methods and definitions used for the urodynamic studies conformed to the standards proposed by the International Continence Society. 19 RESULTS Initial presentation All the patients had urinary dysfunction at the onset of their disease (table 1). Four patients had transient urinary np
3 Micturition disturbance in acute autonomic neuropathy 289 retention which required urinary catheterisation; the other two had with or without nocturnal urinary frequency. All patients with became able to urinate within a week (two to seven days), including those who underwent steroid pulse treatment. While three patients needed midodrine or L-threoDOPS for the treatment of orthostatic hypotension, none needed drug treatment for the micturition disturbance. With respect to other autonomic disturbances, all the patients except one (case 1, cholinergic ) had frequent episodes of orthostatic dizziness and syncope. All patients had intestinal pseudo-obstruction or severe constipation, and four also had vomiting, abdominal distension, and pain. All patients had anhidrosis, four had intractable paroxysmal coughing, three had tonic pupils, and all four male patients had erectile dysfunction (which developed later in a young patient). When the urodynamic studies were done, all patients still had moderate micturition disturbance (table 2). The major symptoms were and nocturnal urinary Table 2 Results of the urodynamic studies Patient frequency. However, none of the patients developed urinary incontinence or recurrent. Post-void residual urine volume was measured in all the patients. Residual urine of more than 30 ml was noted in three (median volume, 50 ml) but none had a residual volume of more than 100 ml. Water cystometry was done in all cases. Bladder volume at first sensation, bladder capacity, or both were decreased in one patient and increased in two: one patient had increased first sensation (340 ml); another had increased bladder capacity (.750 ml; water infusion stopped to avoid overdistension). During bladder filling, one patient showed a low compliance detrusor. During voiding, five patients had detrusor areflexia. The bethanechol test was done in five patients, three of whom showed supersensitivity of the bladder. External sphincter EMG showed unrelaxing sphincter on voiding in one patient. Analysis of sphincter motor unit potentials was done in four patients, and none had neurogenic changes in the sphincter motor unit potentials. In addition to the above urodynamic abnormalities, one patient (case 2) with diurnal frequency had polyuria (.2200 ml/day) because of an excessive water intake, as he had heat intolerance caused by generalised anhidrosis. Variable 1 (KA) 2 (TO) 3 (TO) 4 (MM) 5 (CK) 6 (ET) Clinical form Cholinergic Typical form Typical form Typical form Typical form Autonomic-sensory Interval between disease onset and urodynamic studies 4 Months 18 Years 2 Months 4 Months 3 Weeks 4 Years Micturition symptoms(at the time of urodynamic studies) Nocturnal frequency Diurnal frequency +* + Urgency + + Incontinence Hesitancy/prolongation +/ + +/ + Retention Decreased urinary flow np + np np np + Post-void residual urine (ml) (normal,30) Maximum urethral closure pressure (cm H 2 O) (41,normal,82).100 np np First sensation (ml) (100,normal,300) Bladder capacity (ml) (200,normal,600) Detrusor hyperreflexia during filling Low compliance detrusor during filling + Detrusor areflexia on voiding +/ + + +/ + Supersensitivity to bethanechol injection (2.5 mg, 30 min) np Unrelaxing sphincter on voiding +/ Neurogenic motor unit potentials of the external sphincter np np Treatment Course Steroid pulse therapy, oral prednisolone Nocturia (4 months), complete recovery (6 months) Steroid pulse therapy, oral prednisolone, dihydroergotamine for OH, sildenafil for ED Diurnal frequency persisted (18 years), OH changed to POTS, Sildenafil withdrawn because of POTS (18 years) Oral prednisolone Urinary frequency, (6 months), normal UDS (2 years); OH persisted (3 years) L-threoDOPS, midodrine for OH Voiding difficulty (6 months), OH lessened but persisted (12 years) Laxative for constipation *This patient also had polyuria from heat intolerance and excessive water intake. ED, erectile dysfunction; np, not performed; OH, orthostatic hypotension; POTS, postural tachycardia syndrome; UDS, urodynamic study. Midodrine for OH Urinary Urinary frequency, frequency, OH persisted (4 years) gradually (3 months); OH lessened but persisted (17 years)
4 290 Sakakibara, Uchiyama, Asahina, et al Follow up The period for complete recovery of the micturition disturbance ranged widely, from three months to more than 18 years. There was no apparent correlation between the recovery period and the sex of the patient or the age of onset. However, the recovery period was shorter (four months) in one patient with acute cholinergic autonomic neuropathy (without orthostatic hypotension), and it was longer (more than four years) in two patients in whom the duration of initial was longer (seven days). Comparing the recovery periods for the micturition disturbance and orthostatic hypotension, the micturition disturbance tended to improve earlier than the orthostatic hypotension (three months to four years for micturition disturbance, except in one cases, where it lasted for 18 years; three years to 18 years for orthostatic hypotension). DISCUSSION Although AIAN is rare, 5 micturition disturbance is well recognised in this disorder. In the present study, all six patients showed micturition disturbance as the initial presentation, four of whom required urinary catheterisation for relief of. The other two patients had with or without nocturia. The high incidence of micturition disturbances reported here is in accordance with previous series of patients with AIAN, including the forms (acute autonomic-sensory neuropathy 8 9 and acute cholinergic neuropathy ). All of our patients with became able to urinate within a week (two to seven days). However, when the urodynamic studies were done (three weeks to four months in the majority), all patients still had moderate micturition disturbance. The major symptoms were and nocturnal urinary frequency. However, none developed urinary incontinence, post-void residuals of more than 100 ml, or recurrent. In our patients, the period for complete recovery of micturition disturbance ranged widely from three months to more than 18 years. The recovery period was shorter (four months) in one patient with acute cholinergic autonomic neuropathy (without orthostatic hypotension), and it was longer (more than four years) in the two patients who had a longer duration (seven days) of initial. Thus the severity of micturition disturbance at the initial presentation may predict the duration of the subsequent disturbance. Though severe micturition disturbance appears to occur as often as orthostatic hypotension, it tended to resolve earlier in our series (within three months to four years, with one case lasting 18 years, versus three 3 years to 18 years). Although we have not done urodynamic studies during the initial retention period, atonic bladder was described in the original report by Young et al. 3 4 We carried out our urodynamic studies three weeks to four months after the onset of disease except in two cases. Our major findings included detrusor areflexia on voiding in five patients, a positive bethanechol test in three, low compliance detrusor in one, and disturbed bladder sensation in two. Our findings support the earlier study by Kirby et al, 11 who described two patients with AIAN: one cholinergic (case 1; an 11 year old girl) and one typical form (case 2; a 53 year old woman). Both initially had. In case 1, the retention resolved a month later, but she still had voiding difficulty for the following 15 years. In case 2, urinary retention persisted for four years before urodynamic studies were done, and these showed detrusor areflexia on voiding. Detrusor areflexia is a common feature in diabetic polyneuropathy, 21 and it also occurs in severely affected cases of Guillain-Barré syndrome It indicates a postganglionic type of pelvic (parasympathetic cholinergic) nerve dysfunction which is the major cause of evacuation disorders. 23 Three of our patients showed supersensitivity to a minimal amount of bethanechol. Supersensitivity to carbachol was also noted by Kirby et al in both their cases. 11 These findings most probably reflect denervation of the detrusor smooth muscles owing to the postganglionic pelvic nerve lesion, 18 which has been confirmed by a reduction of acetylcholinesterase containing nerves in biopsies of the bladder muscle. 11 One of our patients showed a low compliance detrusor, which was also noted in Kirby s case A low compliance detrusor commonly occurs in spinal conus or cauda equina lesions and indicates a preganglionic type of pelvic nerve dysfunction. 23 There was a discrepancy in that impaired bladder sensation was noted in two of our patients but in none of Kirby s cases. Impaired bladder sensation indicates disturbance of afferent fibres from the bladder wall, although it might also be a result of potential overdistension injury during the initial retention period. Analysis of the sphincter motor unit potentials showed that none had denervation potentials, which is in agreement with the earlier study. 11 The external sphincter did not relax completely during voiding in only one of the five patients who had detrusor areflexia, suggesting mild sphincter dysfunction. Nerve conduction studies and sural nerve biopsy in the present study showed severe loss of small myelinated and unmyelinated nerve fibres, with preservation of somatic motor nerves, which is consistent with previous reports. 1 5 Thus the external striated sphincter muscles (innervated by somatic pudendal nerves) tend to be preserved in this disorder. Conclusions In our patients with acute idiopathic autonomic neuropathy, and were common initial presentations. The underlying mechanisms seem to be preand postganglionic cholinergic dysfunction with preservation of somatic sphincter function. The problems tend to resolve earlier than orthostatic hypotension.... Authors affiliations R Sakakibara, T Uchiyama, M Asahina, A Suzuki, T Hattori, Department of Neurology, Chiba University School of Medicine, Chiba, Japan T Yamanishi, Department of Urology, Dokkyo Medical College, Tochigi, Japan Competing interests: none declared REFERENCES 1 Suarez GA, Fealey RD, Camillei M, et al. Idiopathic autonomic neuropathy; clinical neurophysiologic and follow-up studies on 27 patients. Neurology 1994;44: Low PA, Dyck PJ, Lambert EH, et al. Acute panautonomic neuropathy. Ann Neurol 1983;13: Young R, Asbury AK, Adams RD, et al. Pure pandysautonomia with recovery. Trans Am Neurol Assoc 1969;94: Young R, Asbury AK, Corbett JL, et al. Pure pandysautonomia with recovery; description and discussion of diagnostic criteria. Brain 1975;98: Low PA, McLeod JG. Autonomic neuropathies. In: Low PA, ed. Clinical autonomic disorders, 2nd ed. Philadelphia: Lippincott-Raven, 1997: Mericle RA, Triggs WJ. Treatment of acute pandysautonomia with intravenous immunoglobulin. J Neurol Neurosurg Psychiatry 1997;62: Sakakibara R, Hattori T, Kuwabara S, et al. Micturitional disturbance in patients with Guillain-Barré syndrome. J Neurol Neurosurg Psychiatry 1997;63: Colan RV, Snead OC, Oh SJ, et al. Acute autonomic and sensory neuropathy. Ann Neurol 1980;8: Pavesi G, Gemignani F, Macaluso GM, et al. Acute sensory and autonomic neuropathy; possible association with Coxsackie B virus infection. J Neurol Neurosurg Psychiatry 1992;55: Harik SI, Ghandour MH, Farah FS, et al. Postganglionic cholinergic dysautonomia. Ann Neurol 1977;1:393 6.
5 Micturition disturbance in acute autonomic neuropathy Kirby R, Fowler CJ, Gosling JA, et al. Bladder dysfunction in distal autonomic neuropathy of acute onset. J Neurol Neurosurg Psychiatry 1985;48: Kita K, Hirayama K, Ito N. Acute idiopathic pandysautonomia; report of four cases. Auton Nerv Syst 1983;20: Kita K, Hirayama K. A morphological approach to autonomic function; quantitative electronmicroscopic studies on unmyelinated fibers from sural nerve biopsies in patients with systemic dysautonomia. Auton Nerv Syst 1986;23: Asahina M, Kuwabara S, Suzuki A, et al. Autonomic function in demyelinating and axonal subtypes of Guillain-Barré syndrome. Acta Neurol Scand 2002;105: Cross SA. Autonomic disorders of the pupil, ciliary body, and lachrymal apparatus. In: Low PA, ed. Clinical autonomic disorders, 2nd ed. Philadelphia: Lippincott-Raven, 1997: Siroky MB, Olsson CA, Krane RJ. The flow rate nomogram, 2. Clinical correlation. J Urol 1980;123: Palace J, Chandiramani VA, Fowler CJ. Value of sphincter electromyography in the diagnosis of multiple system atrophy. Muscle Nerve 1997;20: Lapides J, Friend CR, Ajemian EP, et al. Denervation supersensibility as a test for neurogenic bladder. Surg Gyn Obst 1962;114: Abrams P, Blaivas JG, Stanton SL, et al. The standardization of terminology of lower urinary tract function; produced by the International Continence Society Committee on Standardization of Terminology. Neurourol Urodynam 1988;7: Takayama H, Kazahaya Y, Kashihara N, et al. A case of post-ganglionic cholinergic dysautonomia. J Neurol Neurosurg Psychiatry 1987;50: Kaplan SA, Te AE, Blaivas JG. Urodynamic findings in patients with diabetic cystopathy. J Urol 1995;153: Wheeler JS, Siroky MB, Pavlakis A, et al. The urological aspects of the Guillain-Barré syndrome. J Urol 1984;131: Blaivas JG. The neurophysiology of micturition; a clinical study of 550 patients. J Urol 1982;127: Skehan AM, Downie JW, Awad SA. The pathophysiology of contractile activity in the chronic decentralized feline bladder. J Urol 1993;149: Snape J, Duffin HM, Castleden CM. Urodynamic findings in sacrococcygeal chordoma. Br J Urol 1987;59:50 2. ECHO... Bladder dysfunction in Duchenne muscular dystrophy can be treated M en and boys with Duchenne muscular dystrophy may be suffering with bladder problems unnecessarily, a UK study has found. Symptoms of detrusor hyperreflexia, at least, can be treated successfully. A chance finding of reported urinary problems in the condition alerted doctors at a paediatric neurology unit to a need to investigate further. Please visit the Journal of More than half (46/74) of 88 males aged 3 31 years with Duchenne muscular dystrophy at Neurology, one neuromuscular clinic had urinary problems not previously raised with their doctors. Neurosurgery, These included daytime and night time incontinence, frequency, urgency, hesitancy, and and Psychiatry stress incontinence and covered young boys able to walk and older males using wheelchairs. website Twenty one males with symptoms were offered kidney and bladder ultrasonography before [ com] for a link and after bladder emptying and videourodynamic tests to isolate the nature of the problem. to the full text Of the 10 who opted for both investigations, nine had results suggesting detrusor of this article. hyperreflexia; seven of them had a small bladder. Five with similar symptoms opted just for ultrasonography. The ultrasonographic studies confirmed complete emptying of the bladder in all patients. All reported symptoms improved significantly and night time incontinence resolved with oxybutinin treatment in 10 males (seven and three, respectively, from each group). The neurological reasons for the urinary symptoms were unclear. Urinary problems are not generally recognised with Duchenne muscular dystrophy among doctors, and parents assume they are part and parcel of the condition. m Archives of Disease in Childhood 2003;88:
Urinary dysfunction and orthostatic hypotension in multiple system atrophy: which is the more common and earlier manifestation?
 J Neurol Neurosurg Psychiatry 2;68:65 69 65 Uro-Neurology Group R Sakakibara T Hattori T Uchiyama Autonomic Group, Department of Neurology K Kita M Asahina A Suzuki Department of Urology, Chiba University,
J Neurol Neurosurg Psychiatry 2;68:65 69 65 Uro-Neurology Group R Sakakibara T Hattori T Uchiyama Autonomic Group, Department of Neurology K Kita M Asahina A Suzuki Department of Urology, Chiba University,
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
We have heard a great deal about "overactive" bladder recently. But what
 BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine,
BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY IN CHILDREN
 0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
0022-5347/00/1645-1686/0 THE JOURNAL OF UROLOGY Vol. 164, 1686 1690, November 2000 Copyright 2000 by AMERICAN UROLOGICAL ASSOCIATION, INC. Printed in U.S.A. BIOFEEDBACK TRAINING FOR DETRUSOR OVERACTIVITY
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Videourodynamic and sphincter motor unit potential analyses in Parkinson s disease and multiple system atrophy
 6 Department of Neurology, Chiba University, 1 8 1 Inohana, Chuo-ku, Chiba 26 867 Japan R Sakakibara T Hattori T Uchiyama Department of Urology T Yamanishi Correspondence to: Dr R Sakakibara sakaki@med.m.chiba-u.ac.jp
6 Department of Neurology, Chiba University, 1 8 1 Inohana, Chuo-ku, Chiba 26 867 Japan R Sakakibara T Hattori T Uchiyama Department of Urology T Yamanishi Correspondence to: Dr R Sakakibara sakaki@med.m.chiba-u.ac.jp
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction?
 London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE
 POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE POTS Irritable heart syndrome. Soldier s heart. Effort syndrome. Vasoregulatory asthenia. Neurocirculatory asthenia. Anxiety neurosis.
POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE POTS Irritable heart syndrome. Soldier s heart. Effort syndrome. Vasoregulatory asthenia. Neurocirculatory asthenia. Anxiety neurosis.
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
P ure autonomic failure (PAF) is a sporadic idiopathic
 PAPER Progression and prognosis in pure autonomic failure (): comparison with multiple system atrophy N Mabuchi, M Hirayama, Y Koike, H Watanabe, H Ito, R Kobayashi, K Hamada, G Sobue... See end of article
PAPER Progression and prognosis in pure autonomic failure (): comparison with multiple system atrophy N Mabuchi, M Hirayama, Y Koike, H Watanabe, H Ito, R Kobayashi, K Hamada, G Sobue... See end of article
The new International Continence Society
 ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
NEUROUROLOGY BACKGROUND
 NEUROUROLOGY BACKGROUND Lower urinary tract dysfunction is common among patients with underlying neurologic conditions. Also known as neurogenic bladder, this occurs as a result of the disruption of the
NEUROUROLOGY BACKGROUND Lower urinary tract dysfunction is common among patients with underlying neurologic conditions. Also known as neurogenic bladder, this occurs as a result of the disruption of the
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
What neurologists need to understa
 98 PRACTICAL NEUROLOGY INTRODUCTION Urodynamics has been used in the investigation of bladder dysfunction since the 1950s, although the first report describing bladder pressure measurement dates from 1882
98 PRACTICAL NEUROLOGY INTRODUCTION Urodynamics has been used in the investigation of bladder dysfunction since the 1950s, although the first report describing bladder pressure measurement dates from 1882
Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder
 European Urology European Urology 45 (2004) 240 244 Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder A. Raes a,, P. Hoebeke b, I. Segaert a, E. Van
European Urology European Urology 45 (2004) 240 244 Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder A. Raes a,, P. Hoebeke b, I. Segaert a, E. Van
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Male LUTS. Dr. Brian Ho. Division of Urology Department of Surgery Queen Mary Hospital
 Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction
 Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
Do Now pg What is the fight or flight response? 2. Give an example of when this response would kick in.
 Do Now pg 81 1. What is the fight or flight response? 2. Give an example of when this response would kick in. Autonomic Nervous System The portion of the PNS that functions independently (autonomously)
Do Now pg 81 1. What is the fight or flight response? 2. Give an example of when this response would kick in. Autonomic Nervous System The portion of the PNS that functions independently (autonomously)
Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies
 138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
138 Original Article Comparison of Sudomotor and Sensory Nerve Testing in Painful Sensory Neuropathies James M. Killian, MD,* Shane Smyth, MD,* Rudy Guerra, PhD, Ishan Adhikari, MD,* and Yadollah Harati,
VOIDING DYSFUNCTION IN MULTIPLE SCLEROSIS
 Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (3): 315-320, May - June, 2000 VOIDING DYSFUNCTION IN MULTIPLE SCLEROSIS CEYHUN OZYURT, ÇAG
Urological Neurology Brazilian Journal of Urology Official Journal of the Brazilian Society of Urology Vol. 26 (3): 315-320, May - June, 2000 VOIDING DYSFUNCTION IN MULTIPLE SCLEROSIS CEYHUN OZYURT, ÇAG
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Physiologic Anatomy and Nervous Connections of the Bladder
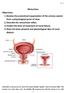 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Neurological control of the bladder in health and disease
 Section 1 Chapter 1 Neurological control of pelvic organ functions Neurological control of the bladder in health and disease Derek J. Griffiths and Apostolos Apostolidis Peripheral control of micturition
Section 1 Chapter 1 Neurological control of pelvic organ functions Neurological control of the bladder in health and disease Derek J. Griffiths and Apostolos Apostolidis Peripheral control of micturition
Neural Control of Lower Urinary Tract Function. William C. de Groat University of Pittsburgh Medical School
 Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories
 Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
Neurourology and Urodynamics 20:249±257 (2001) Involuntary Detrusor Contractions: Correlation of Urodynamic Data to Clinical Categories Lauri J. Romanzi, Asnat Groutz, Dianne M. Heritz, and Jerry G. Blaivas*
URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW Author : Ian Battersby Categories : Vets Date : August 3, 2009
Vet Times The website for the veterinary profession https://www.vettimes.co.uk URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW Author : Ian Battersby Categories : Vets Date : August 3, 2009
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Premotor PD: autonomic failure
 Premotor PD: autonomic failure Division of Neurobiology Department of Neurology Medical University of Innsbruck Non-motor symptoms in PD Autonomic OH, constipation, impotence, urinary incontinence or retention,
Premotor PD: autonomic failure Division of Neurobiology Department of Neurology Medical University of Innsbruck Non-motor symptoms in PD Autonomic OH, constipation, impotence, urinary incontinence or retention,
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
Perineal Electrophysiologic Tests
 Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
TEXT-BASED MULTIPLE CHOICE QUESTIONS
 TEXT-BASED MULTIPLE CHOICE QUESTIONS 1. Which is true regarding the normal control of urine storage? A. The intravesical pressure increases to a threshold pressure (approximately 25 cm H 2 O) as the bladder
TEXT-BASED MULTIPLE CHOICE QUESTIONS 1. Which is true regarding the normal control of urine storage? A. The intravesical pressure increases to a threshold pressure (approximately 25 cm H 2 O) as the bladder
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Neuropathic bladder and spinal dysraphism
 Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
THE vesical dysfunction which follows injury or disease of the spinal cord
 VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
김준철 가톨릭대학교의과대학비뇨기과학교실
 비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
EXPERIMENTAL AND THERAPEUTIC MEDICINE 4: , 2012
 1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
1112 Usefulness of total bladder capacity and post void residual urine volume as a predictor of detrusor overactivity with impaired contractility in stroke patients SANG HYUB LEE, JOONG GEUN LEE, GYEONG
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
URINARY INCONTINENCE IN THE. Summary
 Age and Ageing (984) 3, 23-234 H. D. H. EASTWOOD Consultant in Geriatric Medicine R WARRELL' Senior Registrar in Geriatric Medicine URNARY NCONTNENCE N THE ELDERLY FEMALE: PREDCTON, N D AG NOSS AND OUTCOME
Age and Ageing (984) 3, 23-234 H. D. H. EASTWOOD Consultant in Geriatric Medicine R WARRELL' Senior Registrar in Geriatric Medicine URNARY NCONTNENCE N THE ELDERLY FEMALE: PREDCTON, N D AG NOSS AND OUTCOME
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
PARKINSONIAN DISORDERS AND PURE AUTONOMIC FAILURE
 CHAPTER 8 KEYPOINTS: PARKINSONIAN DISORDERS AND PURE AUTONOMIC FAILURE INTRODUCTION Disorders of bladder, bowel and sexual function are common problems in Parkinson s disease (PD), multiple system atrophy
CHAPTER 8 KEYPOINTS: PARKINSONIAN DISORDERS AND PURE AUTONOMIC FAILURE INTRODUCTION Disorders of bladder, bowel and sexual function are common problems in Parkinson s disease (PD), multiple system atrophy
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome
 Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Mechanisms of Disease: central nervous system involvement in overactive bladder syndrome Karl-Erik Andersson SUMMARY The pathophysiology of overactive bladder syndrome (OABS) and detrusor overactivity
Re-evaluation of differential sacral rhizotomy for neurological bladder disease
 J Neurosurg 48:773-778, 1978 Re-evaluation of differential sacral rhizotomy for neurological bladder disease GAYLAN L. ROCKSWOLD, M.D., PH.D., SHELLEY N. CHOU, M.D., PH.D., AND WILLIAM E. BRADLEY, M.D.
J Neurosurg 48:773-778, 1978 Re-evaluation of differential sacral rhizotomy for neurological bladder disease GAYLAN L. ROCKSWOLD, M.D., PH.D., SHELLEY N. CHOU, M.D., PH.D., AND WILLIAM E. BRADLEY, M.D.
Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity
 ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
ORIGINAL ARTICLE Vol. 41 (3): 521-526, May - June, 2015 doi: 10.1590/S1677-5538.IBJU.2014.0204 Flowmetry/ pelvic floor electromyographic findings in patients with detrusor overactivity Farshid Alizadeh
NIH Public Access Author Manuscript Neurology. Author manuscript; available in PMC 2009 February 10.
 NIH Public Access Author Manuscript Published in final edited form as: Neurology. 2008 May 13; 70(20): 1926 1932. doi:10.1212/01.wnl.0000312280.44805.5d. Autonomic Ganglia: Target and Novel Therapeutic
NIH Public Access Author Manuscript Published in final edited form as: Neurology. 2008 May 13; 70(20): 1926 1932. doi:10.1212/01.wnl.0000312280.44805.5d. Autonomic Ganglia: Target and Novel Therapeutic
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes
 Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Neurourology and Urodynamics 19:127 135 (2000) A Simplified Urinary Incontinence Score for the Evaluation of Treatment Outcomes Asnat Groutz, Jerry G. Blaivas,* and Jarrod E. Rosenthal Weill Medical College,
Management of LUTS after TURP and MIT
 Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
Management of LUTS after TURP and MIT Hong Sup Kim Konkuk University TURP & MIT TURP : Gold standard MIT TUIP TUNA TUMT HIFU LASER Nd:YAG, ILC, HoLRP, KTP LUTS after TURP and MIT Improved : about 70% Persistent
What is Nocturia? What are the Consequences of Nocturia? 23/10/12. Dr. Tam Cheuk Kwan Consultant, Dept. of M&G Tuen Mun Hospital
 Survival 23/10/12 Dr. Tam Cheuk Kwan Consultant, Dept. of M&G Tuen Mun Hospital What is Nocturia? Nocturia is the complaint that the individual has to wake at night one or more times to void. (ICS definition
Survival 23/10/12 Dr. Tam Cheuk Kwan Consultant, Dept. of M&G Tuen Mun Hospital What is Nocturia? Nocturia is the complaint that the individual has to wake at night one or more times to void. (ICS definition
The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery
 The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery SPINE Volume 35, Number 17, pp E849 E854 2010, Lippincott Williams & Wilkins Chun-Hao
The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery SPINE Volume 35, Number 17, pp E849 E854 2010, Lippincott Williams & Wilkins Chun-Hao
1 Olsson CA, Willscher MK, Austen G Jr, Siroky MB and Krane RJ. Management of prostatic fistulas. Urol Surv 1976;25:135.
 Michael B. Siroky, MD FACS 720 Harrison Avenue Suite 606 Boston, Ma 02118 TEL: 617 638-8555 FAX: 617 638-8487 CHAPTERS, MONOGRAPHS, REVIEWS (Peer reviewed journals in bold) 1 Olsson CA, Willscher MK, Austen
Michael B. Siroky, MD FACS 720 Harrison Avenue Suite 606 Boston, Ma 02118 TEL: 617 638-8555 FAX: 617 638-8487 CHAPTERS, MONOGRAPHS, REVIEWS (Peer reviewed journals in bold) 1 Olsson CA, Willscher MK, Austen
Indications and Uses of Testing. Laboratory Testing of Autonomic Function. Generalized Autonomic Failure. Benign Disorders 12/30/2012.
 Indications and Uses of Testing Laboratory Testing of Autonomic Function Conditions of generalized autonomic failure Help define the degree of autonomic dysfunction and distinguish more benign from life
Indications and Uses of Testing Laboratory Testing of Autonomic Function Conditions of generalized autonomic failure Help define the degree of autonomic dysfunction and distinguish more benign from life
Urodynamic findings in women with insensible incontinence
 bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
bs_bs_banner International Journal of Urology (2013) 20, 429 433 doi: 10.1111/j.1442-2042.2012.03146.x Original Article: Clinical Investigation Urodynamic findings in women with insensible Benjamin M Brucker,
A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging
 61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
Ganglionic Blockers. Ganglion- blocking agents competitively block the action of
 Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
November 16-18, 2017 Hotel Monteleone New Orleans, LA. Provided by
 November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Diabetic Neuropathy: A Global and Growing Problem John D. England, MD Louisiana State University Health Sciences Center School of Medicine
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Skin sympathetic nerve activity in Guillain-Barré syndrome: a microneurographic study
 Journal of Neurology, Neurosurgery, and Psychiatry 997;6:57 54 57 SHORT REPORT Fourth Department of Internal Medicine, Aichi Medical University K Yamamoto T Mitsuma Department of Neurology, School of Medicine,
Journal of Neurology, Neurosurgery, and Psychiatry 997;6:57 54 57 SHORT REPORT Fourth Department of Internal Medicine, Aichi Medical University K Yamamoto T Mitsuma Department of Neurology, School of Medicine,
Parkinson s Disease and Multiple System Atrophy
 Parkinson s Disease and Multiple System Atrophy Jalesh N. Panicker MD, FRCP Department of Uro-Neurology National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen Square, London
Parkinson s Disease and Multiple System Atrophy Jalesh N. Panicker MD, FRCP Department of Uro-Neurology National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen Square, London
Chapter 14 The Autonomic Nervous System Chapter Outline
 Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Guillain-Barré Syndrome
 Guillain-Barré Syndrome Ouch! www.philippelefevre.com Guillain-Barré Syndrome Acute post-infective polyneuropathy Heterogeneous condition with several variant forms Lipid A Neuronal Ganglioside Pathogenesis
Guillain-Barré Syndrome Ouch! www.philippelefevre.com Guillain-Barré Syndrome Acute post-infective polyneuropathy Heterogeneous condition with several variant forms Lipid A Neuronal Ganglioside Pathogenesis
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
The new ICCS terminology J Urol 176, , 2006
 The new ICCS terminology J Urol 176, 314-324, 2006 The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Report from the Standardisation Committee of the International
The new ICCS terminology J Urol 176, 314-324, 2006 The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Report from the Standardisation Committee of the International
Impact of urethral catheterization on uroflow during pressure-flow study
 Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Research Report Impact of urethral catheterization on uroflow during pressure-flow study Journal of International Medical Research 2016, Vol. 44(5) 1034 1039! The Author(s) 2016 Reprints and permissions:
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Bladder dysfunction. Dr behnaz ansari
 Bladder dysfunction Dr behnaz ansari Anatomic Considerations: in the autonomic nervous system there are always two efferent neurons serving this function, one (preganglionic) arising from its nucleus in
Bladder dysfunction Dr behnaz ansari Anatomic Considerations: in the autonomic nervous system there are always two efferent neurons serving this function, one (preganglionic) arising from its nucleus in
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
NEUROPATHIC BLADDER DISORDERS
 NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
