A Test of AmON2v s Evidence-
|
|
|
- Stephen Cannon
- 5 years ago
- Views:
Transcription
1 Continence for Women: A Test of AmON2v s Evidence- Based Protocol in Clinical Practice Carolyn M. Sampselle, RNC, PhD, FAAN, Jean E Wyman, RN, PhD, FAAN, Karen Kelly Thomas, RNC, PhD, Diane K. Newman, RNC, MSN, CRNP, FAAN, Mike1 Gray, CUNP, CCCN, PhD, FAAN, Molly Dougberty, RN, PhD, FAAN, Patricia A. Burns, NP, PhD, FAAN =Objective: To test the effectiveness of an evidence-based protocol for urinary incontinence in increasing identification of women with the condition and improving their outcomes. Design: Prospective formative evaluation study. Setting: Twenty-one public, private, and other women s health care sites. Participants: Women in ambulatory care settings (N = 1,474) provided descriptive statistics. Clinical outcomes were tested in 132 cases for whom pre- and posttreatment data were available. Interventions: Standardized screening and baseline follow-up forms were used to minimize time burden on clinicians; bladder and pelvic floor muscle training materials were provided to clinicians for distribution. Main Outcome Measures: Self-reported frequency, volume, and quality of life related to incontinence and cost of self-management were used to assess protocol effectiveness. Results: Frequency of incontinence episodes, estimated volume lost per episode, and the cost of self-management decreased. Quality of life improved, as reflected in decreased bother attributed to incontinence and in the number of women avoiding activities such as shopping, exercising, or travel because of incontinence. Conclusions: This simple program of pelvic floor muscle and bladder training, as it has been systematically implemented in a variety of ambulatory women s health care settings, has benefited women s continence status. The results of this project strongly support widespread application. JOGNN 29, 18-26; Keywords: Bladder training-continence- Pelvic floor-pelvic muscle-urinary incontinence Accepted: September 1999 Involuntary leakage of urine or urinary incontinence affects, on average, 2.534% of women living at home (Thorn, 1998). Such women comprise the population from which the caseloads of most ambulatory care centers are drawn. The proportion of women affected with urinary incontinence is increased by age and parity. In the perimenopausal years symptoms increase, with 31% of women reporting at least one incontinence episode per month (Burgio, Matthews, & Engel, 1991). Lagace, Hanson, and Hickner (1993) documented increases in overall incontinence and in more severe or bothersome levels of involuntary leakage among women in their 40s and 50s. In a respected study of carefully sampled women, 38% age 60 years and older who were living at home reported symptoms of urinary incontinence (Diokno, Brock, Brown, & Herzog, 1986). Vaginal birth also is associated with greater prevalence of incontinence. Women who have had even one vaginal birth are more than 2.5 times as likely to report incontinence than are their nulliparous counterparts (Jolleys, 1988; Sommer et al., 1990), and the rate of incon- 18 JOGNN Volume 29, Number 1
2 tinence increases with parity (Nygaard, DeLancey, Arnsdorf, & Murphy, 1990). Urinary incontinence is clearly a condition that affects the lives of many women and thus is of concern to the nurses who provide their health care. Recognizing the widespread impact of urinary incontinence on the health and well-being of women, the Association of Women s Health, Obstetric and Neonatal Nurses (AWHONN) designated its third organizationally supported research utilization project to focus on this condition. That 3-year project, begun in 1995, consisted of three phases: Phase I, Planning, included the development of an evidence-based protocol which has been presented in detail in a previous publication (Sampselle et al., 1997), as well as the development of data management forms and the plan for implementation of the project; Phase 11, Implementation, entailed site recruitment, training of nurses to use the evidence-based protocol, and data collection; and Phase 111, Evaluation, involved assessment of the success of the process that enabled clinicians to use the protocol. These phases are discussed A n evidence-based protocol for urinary incontinence was successfully implemented by clinicians in ordinary women s hea I th am bula tory-ca re settings. in detail in the article immediately preceding this report (Sampselle et al., 2000, pp. 9-17). The information presented here is a report of the impact of the evidencebased protocol on nursing practice and on patient outcomes. The aim of the current study was to test the effectiveness of an evidence-based protocol for urinary incontinence in increasing identification of women with the condition and improving their outcomes. Hypotheses The project investigated two broad research questions: (a) Will change occur in clinical practice after clinicians are trained to identify urinary incontinence and to intervene using an evidence-based protocol? and (b) Will patient outcomes be positively affected after the protocol is instituted in the clinical setting? Six hypotheses based on these questions were tested. The following hypothesis related to practice change: 1. More women will screen positive for urinary incontinence when routine screening is imple- mented as compared to the proportion who disclose the condition as reported in the literature. The following hypotheses related to patient outcomes: 2. Urinary incontinence episodes will decrease in frequency. 3. Urine loss per episode will decrease in volume. 4. The cost of self-management of urinary incontinence will decrease. 5. The amount of bother associated with incontinence will decrease. 6. The number of activities avoided because of incontinence will decrease. Methods The initial sample consisted of 1,474 women screened for incontinence as a part of the routine history collected in their respective ambulatory settings. The screening questions were the following: Do you ever leak urine/water when you don t want to? Do you ever leak urine/water when you cough, laugh, or exercise? Do you ever leak urine/water on the way to use the bathroom? Do you ever use pads, tissue, or cloth in your underwear to catch urine? Of the total sample screened, 57% (842) responded always or sometimes on at least one of the four screening items. Because the screening and the behavioral interventions of the evidence-based protocol are considered to be standard of care practice (Fantl et al., 1996) institutional review board approval was not required, although some participating sites obtained it. The women s willingness to complete the initial forms and to engage in the behavioral interventions presented by the clinicians constituted implied consent. The number of women who provided feedback at the 4-month follow-up (n = 132) was markedly reduced from the original number who screened positive (n= 842). Comparisons of selected baseline characteristics of the original and enduring longitudinal sample are presented in Table 1. Differences between the two groups were apparent. Older women were more likely to persist with therapy; the mean age for those retained to the 4-month follow-up was 51 years as compared to 40 for the group who originally screened positive. White women were more likely to continue to the 4-month follow-up than were black or Latina women. Women who reported a lower duration of incontinence (25 months) were less likely to persist with treatment than those who reported a longer duration (39 months). Those who were experiencing a greater number of incontinence episodes per week were more likely to continue to the 4-month point. Thus, greater severity was associated with persistence in treatment. JanuarylFebruary 2000 JOG 19
3 - (n TABLE 1 Comparison of Baseline Cbaratmidcs Between Original and Enduring Longitudinal Sample Time 1 Retained D&I Only to Time.3 = 842) (n = 1.32) ARC' 39.9 Years.$ I. 1 Years Racial African American 18% 7 '% distribution of three La tina 10% 5 Yo major groups White 72% 88% Duration of incontinence 24.6 months 39.3 months Frequency of incontinence 2.1 /week 3.0lweek Voiding frequency while awake 5.9Iday 6.2Ida y Nocturin frequency 1.8Inight 1.3lnight p <.001 /!I <.0001 p <.002 ns FIS The specific measures identified for each variable of interest and the analyses selected to test each hypothesis are detailed below: Hypothesis 1. More women will screen positive for urinary incontinence (and will subsequently receive the recommended basic evaluation) when routine screening is implemented as compared to that proportion of women reported in the literature who disclose the condition. The proportion of women who responded positively to one or more of the four screening questions was compared to the percentage (38-41%) of women identified by survey (Burgio, Ives, Locher, & Arena, 1994; Goldstein, Hawthorne, Engeberg, McDowell, & Burgio, 1992) who indicated that they had incontinence and had discussed the problem with a health care provider. Then, using the aggregate number of women reported by participating sites who answered any of the first four screening questions positively as the denominator, the proportion who completed the basic evaluation was calculated. Hypothesis 2. Urinary incontinence episodes will decrease in frequency. Respondents indicated the frequency of urine lost during a typical week by selecting one of five categories (Item 2 on the basic evaluation, which is presented in Figure 1). Differences in the usual frequency of incontinence per week were determined by comparing the category selected on the basic evaluation with the category selected for item 2 on the ongoing evaluation (see Figure 2). Hypothesis 3. Urine loss per episode will decrease in volume. Differences in amount of urine loss per episode were assessed by comparison of baseline indications of a selected category that estimated the volume of urine lost, on average, per episode of incontinence (Item 3) on the basic evaluation with the same item on the ongoing evaluation. Hypothesis 4. The cost of self-management of urinary incontinence will decrease. A cost estimate was calculated by obtaining retail prices of all levels of protection, from panty liners to absorbent pantshper pads in two regional areas (Washington, DC, and Arizona). The mean cost of each type of protection was multiplied times the number of reported changes per day (as reported in Item 5) and then multiplied by seven to derive an estimated cost per week. These estimates were compared between the basic and the ongoing evaluations. Hypothesis 5. The amount of bother associated with incontinence will decrease. Difference in level of bother (Item 4) was compared between the basic evaluation and the ongoing evaluation. Hypothesis 6. The number of activities avoided because of incontinence will decrease. The percentage of women avoiding activities such as shopping, exercising, and traveling (Item 7) was compared between the basic evaluation and the ongoing evaluation. Analysis The statistical analyses were performed using the Statistical Package for the Social Sciences (Norusis, 1994). Chi square, t test, and repeated measures analysis of variance were used for assessment of group differences in demographic characteristics and for hypothesis testing. Descriptive statistics were generated from the 1,474 cases initially screened across the 21 participating sites. To conduct hypothesis testing of effects on 20 JOG" Volume 29, Number 1
4 ~ Date: (1-1 / / Site: I// Participant: j]/i Continence. for Women Project: Basic Evaluation On average, how often do you lose urinehvater during a typical week? How would you describe the amount of urine you usually leak? 0 Yes 0 Larger pad 0 Absorbent pant 0 Less than once a week 0 Once a week 0 More than once a week 0 Once a day 0 More than once a day 0 Damp/ a few drops 0 Weffenough to wet underpants 0 Quite weffa cupful (soaks paddother protection) 0 Verv wetlfloodslsoaks throuah outer clothes How much does this leakage bother you? Notatall VeryMuch Are you currently using pads for What type? How many times per day protection against urine leakage? do you need to change pads? 0 Sanitary pad 0 No lskid to#6 I rn How many days last week did you leak urine? I o I or fewer o or more ' 7. Are you avoiding certain activities because of a urinehater loss problem? 0 No [Skip to #8 I 0 Yes 0 Shopping 0 Dating 0 Exercising 0 Having sex 0 Traveling 0 Dancing 0 Visiting friendsbamily 0 Playing sports Do you have a history of: (check as many as apply) 0 Diabetes o Constipation o Stroke 0 Problems walking 0 Multiple Sclerosis 0 Previous treatment 0 Spinal cord injury for urine loss or surgery 11. Do you feel that your bladder is empty after you urinate/pass water? OYes ONo 12. Do you ever push down or strain to urinatelpass water? OYes ONo 13. Please list any medications that you are currently taking, either prescribed or purchased over the counter. 14. Who completed this form? 1-0 Myself 0 Nurse 0 Someone else 1 Copynght 1997 AWHONN RU3-B FIGURE 1 <:ontinence for Women Project: Basic Evaluation. The nurse will falk with you about plans for follow-up january/e'ehruary 2000 lognn 21
5 Continence for Women Project: Ongoing Evaluation during a typical week? 0 Less than once a week 0 Once a week 0 More than once a week 0 Once a day 0 More than once a day 2. How would you describe the amount of urine you usually leak? 0 Damp/ a few drops 0 Weffenough to wet underpants 0 Quite weffa cupful (soaks padslother protection) 0 Very wefffloodslsoaks through outer clothes 3. How many days last week did you leak urine? How much does this leakage bother you? 5. Are you currently using pads for protection against urine leakage? What type? How many times per day do you need to change pads? 0 No 0 Yes / Skip to #6 1 0 Panty liner 0 Sanitarv Dad I o 1 or fewer o 4 0 Larger pad 0 Absorbent pant or more 6. Are you avoiding certain activities because of a urinehater loss problem? - 0 No 1 - Skip to #7 I 0 Yes 0 Shopping 0 Dating 0 Exercising 0 Having sex 0 Traveling 0 Dancing 0 Visiting friendsfiamily 0 Playing sports 7. On average, how many times do you urinate/pass water during the day? [TI night? [Ti 8. Do you want additional treatment such as: 0 medication o surgery Copyright 1997 AWHONN 0 1 mo. O4rno. RU3-B follow-up FIGURE 2 Continence for Women Project: Ongoing Evaluation. 22 lognn Volume 29, Number 1
6 In typical caseloads of ambulatory women, 57% screened positive for urinary incontinence. Nearly 25% of the incontinent women experienced episodes every day. continence status, we analyzed only the 132 cases for whom baseline (pretreatment) and 4 month (posttreatment) data were available. Differences were examined between women who finished treatment and those who dropped out. The alpha level of.05 was set to judge the significance of demonstrated differences. Results Factors Associated with Incontinence The initial sample (N = 1,474) was divided into those who reported incontinence and those who did not. The two groups were compared on selected demographic characteristics (see Table 2). Age, race, vaginal birth, and history of hysterectomy were significantly different between the continent and incontinent groups. As expected, no differences were found between groups with regard to educational level. Pretreatment Continence Status The pretreatment level of incontinence severity is reflected in the distributions presented in Table 3. Nearly 2.5% of those who were incontinent reported unwanted urine loss occurring once or more a day. When asked about use of protective pads, 37% of those reporting incontinence indicated that they required this protection, with nearly 42% having to change at least twice a day. The results presented in the following paragraphs detail the outcome of the hypothesis-testing process and constitute the actual evaluation of the protocol itself. They demonstrate its effectiveness when carried out by typical providers in ordinary clinical settings as opposed to the more systematic and controlled environment in which conventional research is conducted. Nursing Practice Outcomes Hypothesis 1 tested for an increase in the percentage of incontinent women identified by routine screening in a clinical setting as compared to those who reported seeking help as documented by previous research. Population-based surveys have found that the percentage of incontinent individuals who actually report their condition to a health care provider ranges from 38% to 41% (Burgio et al., 1994; Goldstein et al., AFter the intervention women reported decreased incontinence frequency, volume, and cost of self- management] and fewer women avoided activities because of incontinence. - TABLE 2 Factm Associated With Urinary Incontinence Vmiable Race African American Latina White Age (Mean years) Ever having given birth Vaginal birth (Mean) Hysterectomy F. h X'. Contiizeizt (n = 6.32) 50.4% 49.3% 38.8% 35 f % 1.1 f % Incontinent (n = 842) F or XL 19.0b 49.6% 50.7% 63.2% 44 e " 82.0% 53.3" 1.8 e a 19.5% 32.P P.0001.ooo 1.ooo JanuarylFebruary 2000 JOGNN 23
7 - TABU 3 Pmtreatnaetat Continence Sta- (%I.. Among Women Who Reported Urinary Incontinence (n = 842) >Ilwk llday >l/day Frequency of leaking < llwk llwk Average amount lost Damp Wet Amount bothered 1 2 by leakage (Not At All) Cupful Flood (Very Much) ). By comparison, 57% (842/1,474) of patients were identified as incontinent with the routine screening used in the current project. This represents a marked increase when measured against that reported in the literature. In addition to identifying the condition, 63% (529/842) of women who answered affirmatively on one or more of the screening questions completed a basic evaluation and nearly 78% (653/842) of them provided partial information on the basic evaluation. This evidence supports Hypothesis 1, demonstrating that, among ambulatory clinic patients, routine screening and requested completion of basic evaluation information results in identification of a higher prevalence of incontinence as compared to the proportion of women who typically initiate discussion of incontinence with a health care provider. Patient Outcomes The outcome measures of frequency of incontinence episodes, volume of leakage per episode, cost of self-management, and quality of life showed improve- ment from baseline (Time 1) to the 4-month posttreatment point (Time 3) (see Table 4). Hypothesis 2, decreased frequency of episodes of incontinence, was supported by change in the predicted direction. Women experienced significantly fewer episodes in a typical week and in the number of days of leaking in the past week. Hypothesis 3, decreased volume of leakage per incontinent episode, was supported. Women selected lower categories to reflect the extent of leakage per incontinence episode over the time of treatment. Hypothesis 4, decreased cost of self-management, Hypothesis 5, decreased amount of bother associated with incontinence, and Hypothesis 6, decreased activities avoided due to incontinence, also were supported. All indices specified by the hypotheses significantly declined from baseline to posttreatment. Discussion These results demonstrate the effectiveness of the evidence-based protocol in actual clinical settings. The TABLE 4 Changes in Continence Status Pre- and Posttreatment Among Wmm Who Reported Urinary Incontinence m I'retreatmerzt Posttrerr tmerr t,mc'lsl~rl~ (11 = 132) (n = 1.32) F Leakage in a typical week Number of days of leakage past week Average volume of urine lost" Micturition frequency during the day Frequency during the night Cost of self-management $ Bother score Percentage avoiding activities 14.0% 3.5% 7.96 "Actiial volume was not measured. Respondents indicated 1 of 4 categories ranging from a few drops to soaking outer clothes. P.002.ooo I.03 ns oo 1 24 JOG" Volume 29, Number 1
8 participating sites represented a wide range of practice settings, and the overall sample was reasonably diverse as reported in the immediately preceeding article (Sampselle et al., 2000). This supports an acceptable level of generalizability and warrants the implementation of the protocol in general ambulatory women s health care settings. Nursing Practice Outcomes It should be noted that the reported proportion of women who screened positive for urinary incontinence and subsequently underwent a complete basic evaluation (63%) is artificially low. At least 124 additional basic evaluations were completed, but were inadequately identified. That is, the basic evaluation had been completed, but it was not possible to link them accurately to a specific set of screening questions. Because a woman was to complete the basic evaluation only if her responses to screening questions indicated an incontinence problem, a less conservative estimate of follow-up would be 78% ( ). Either proportion is substantially greater than that reflected in previous surveys. This finding suggests that routine screening, coupled with a system that facilitates follow-up for basic evaluation, is effective in identifying symptomatic individuals. Thus, even more important than the systematic data management framework that was introduced by the use of the teleform technology was the ease with which the screening and basic evaluation could be conducted. Whether or not computerized scanning is used, the standardized forms address the problem of how to carve out the time needed to conduct systematic routine screening and the recommended basic evaluation of those who screened positive for incontinence. The simple educational materials described in the earlier publication (Sampselle et al., 1997) could then be used to provide information about bladder and pelvic floor muscle training. Patient Outcomes The frequency, volume, and life impact of urinary incontinence decreased following treatment. Given that 57% of the baseline (Time 1) sample of women screened reported some problem with unwanted leakage, replication of this protocol in a wide range of ambulatory sites is likely to benefit diverse types of women across the lifespan. It is noteworthy that those who were retained to the posttreatment point initially had more severe levels of incontinence as reflected in longer duration and greater frequency of involuntary loss prior to treatment. Others have reported that only 25% of incontinent women start treatment when it is offered (Samuelsson, Victor, & Tibblin, 1997). Perhaps the severity of the condition motivates women to accept and persist with behavioral therapy. Though it was not originally hypothesized, an additional benefit to women s overall well-being was noted. There was a decrease in the frequency of nocturia experienced by women posttreatment. While nocturia is clearly not incontinence, it disrupts sleep and can affect overall well-being. As can be seen in Table 4, the frequency of nocturia declined from a pretreatment level of 1.7 to a posttreatment frequency of.9 (F = 5.9, p =.012). This phenomenon has not been reported previously and deserves further investigation. The statistics and the hypothesis testing tell only part of the story. Anecdotal evidence contributed by site coordinators provides powerful insights into the impact of the protocol on the lives of individual women. One nurse told of a patient who offered to pay her own way to the AWHONN Convention so that she could explain to other women s health nurses how important the program was. You changed my life! she told the nurse who had implemented the protocol, I want other nurses to know about this. Another woman whose voiding frequency decreased from about 15 to 8 times in the course of a 24-hour period, asked of the nurse who helped her, Why haven t I heard about this before now? Implications for Nursing Practice The results of this study demonstrate clear benefits to the health of women when this protocol is incorporated into standard ambulatory patient care. The four recommended screening questions will identify higher numbers of women at risk than will a less systematic approach. Given the significantly greater risk of women who have had a hysterectomy, nurses should be particularly vigilant when assessing this group. The basic evaluation questions allow determination of which candidates will benefit more from referral, such as for treatment of neurologic disease, and those who should receive information about the value of bladder and pelvic floor muscle training. Information about available patient education materials and their incorporation into typical practice settings is discussed in detail (Sampselle et al., 1997), and updates are available at the AHCPR web-site htm. Further research is in progress at the University of Michigan to assess the potential of the recommended behavioral intervention for the prevention of urinary incontinence. Given the very high attrition rates for African American and Latina women, further research is warranted to identify more effective implementation of the protocol for these groups. This will require the development and testing of culturally appropriate materials as well as translation into Spanish. JanuarylFebruary 2000 JOGNN 25
9 In summary, this evidence-based protocol, as it has been systematically implemented in a variety of ambulatory women s health care settings, facilitated systematic screening and obtaining of baseline evaluation data. The simple program of pelvic floor muscle and bladder training yielded significant improvements in women s continence status. The results of this project support widespread incorporation of the protocol into clinical practice in ambulatory care sites. REFERENCES Burgio, K. L., Ives, D. G., Locher, J. L., & Arena, V.C. (1994). Treatment seeking for urinary incontinence in adults. Journal of the American Geriatric Society, 42(2), Burgio, K. L., Matthews, K. A., & Engel, B T. (1991). Prevalence, incidence and correlates of urinary incontinence in healthy, middle-aged women. Journal of Urology, 146, Diokno, A. C., Brock, B. M., Brown, H. B., & Herzog, A. R. (1986). Prevalence of urinary incontinence and other urologic symptoms in the non-institutionalized elderly. Journal of Urology, 136, Fantl, J. A., Newman, D. K., Colling, J., DeLancey, J. 0. L., Keeys, C., Loughery, R., McDowell, B. J., Norton, P., Ouslander, J., Schnelle, J., Staskin, D., Tries, J., Urich, V., Vitousek, S. H., Weiss, B. D., & Whitmore, K. (1996). Urinary incontinence in adults: Acute & chronic management. (Clinical Practice Guideline, No. 2, 1996 Update, AHCPR Publication No ). Rockville, MD: U.S. Department of Health and Human Services. Goldstein, M., Hawthorne, M. E., Engeberg, S., McDowell, B. J., & Burgio, K. L. (1992). Urinary incontinence: Why people do not seek help. Journal of Gerontologic Nursing, 18(4), Jolleys, J. V. (1988). Reported prevalence of urinary incontinence in women in a general practice. British Medical Journal, 296, Lagace, E. A., Hansen, W., & FIickner, J. M. (1993). Prevalence and severity of urinary incontinence in ambulatory adults: An UPRNet study. Journal of Family Practice, 36(6), Norusis, Marija. (1994). SPSS Advanced Statistics 6.1. Chicago: SPSS Inc. Nygaard, I., DeLancey, J., Arnsdorf, L., & Murphy, E. (1990). Exercise and incontinence. Obstetrics & Gynecology, 75(5), Sampselle, C. M., Burns, P., Dougherty, M., Thomas, K. K., Newman, D. K., & Wyman, J. (1997). Continence for women: Evidence-based practice. Journal of Obstetric, Gynecologic, and Neonatal Nursing, 26, Sampselle, C. M., Wyman, J. F., Thomas, K. K., Newman, D. K., Gray, M., Dougherty, M., & Burns, P.A. (2000). Continence for women: Evaluation of AWHONN s third research utilization project. Journal of Obstetric, Gynecologic, and Neonatal Nursing, 29, Samuelsson, E., Victor, A., & Tibblin, G. (1997). A population study of urinary incontinence and nocturia among women aged years. Prevalence, well-being and wish for treatment. Acta Obstetrica et Gynecologica Scandinauica, 76( l), Sommer, P., Bauer, T., Nielsen, K. K., Kristensen, G. G., Hermann, K. s., & Nordling, J. (1990). Voiding patterns and prevalence of incontinence in women. A questionnaire survey. British Journal of Urology, 66(1), Thom, D. (1998). Variation in estimates of urinary incontinence prevalence in the community: Effects of differences in definition, population characteristics, and study type. Journal of the American Geriatric Society, 46(4), Carolyn M. Sampselle is a professor of nursing and women s studies and associate professor of obstetrics and gynecology, University of Michigan, School of Nursing in Ann Arbor. Jean E Wyman is a professor, Cora Meidl Siehl Chair in Nursing Research, at the University of Minnesota, School of Nursing in Minneapolis. Karen Kelly Thomas is director of research, programs, and publications, Association of Women s Health, Obstetric and Neonatal Nurses, Washington, DC. Diane K. Newman is an adult nurse practitioner, DKN & Associates, Inc., Philadelphia, PA. Mike1 Gray is a nurse practitioner and associate professou, Department of Urology and School of Nursing, University of Virginia, Charlottesville. Molly Dougherty is Frances Hill Fox Professor, Department of Community and Mental Health, University of North Carolina at Chapel Hill. Patricia A. Burns is dean and professor, University of South Florida College of Nursing, Tampa. Address for correspondence: Carolyn M. Sampselle, RNC, PhD, F M, University of Michigan, School of Nursing, 400 North Ingalls, Ann Arbor, MI csampsll@umich.edu. 26 JOGNN Volume 29, Number 1
The UNIVERSITY of NEWCASTLE
 The UNIVERSITY of NEWCASTLE R esearch C entre for G ender and H ealth Characteristics of Australian women with incontinence according to incontinence severity and treatment-seeking behaviour Results from
The UNIVERSITY of NEWCASTLE R esearch C entre for G ender and H ealth Characteristics of Australian women with incontinence according to incontinence severity and treatment-seeking behaviour Results from
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania VOIDING DIARY. Column #3 LEAK
 743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 VOIDING DIARY This paperwork MUST be completed prior to your appointment. If not, your appointment will need to be rescheduled.
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 VOIDING DIARY This paperwork MUST be completed prior to your appointment. If not, your appointment will need to be rescheduled.
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
The development of a questionnaire to measure the severity of symptoms and the quality of life before and after surgery for stress incontinence
 BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
Management of Incontinence and Pelvic Floor Disorders
 Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Information on Physical Therapy For Urogynecologic Problems
 Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
UNC Urogynecology and Reconstructive Pelvic Surgery Division of Female Pelvic Medicine and Reconstructive Surgery (FPMRS)
 UNC Urogynecology and Reconstructive Pelvic Surgery Division of Female Pelvic Medicine and Reconstructive Surgery (FPMRS) We look forward to your upcoming visit with us. Our goal is to provide you with
UNC Urogynecology and Reconstructive Pelvic Surgery Division of Female Pelvic Medicine and Reconstructive Surgery (FPMRS) We look forward to your upcoming visit with us. Our goal is to provide you with
Entered: / / 20 Initials: Verified: / /20 Initials: mm dd yy mm dd yy. Patient ID - - Visit: 1 For office use only.
 Entered: / / 20 Initials: Verified: / /20 Initials: mm dd yy mm dd yy Patient ID - - Visit: 1 For office use only. UIB Version: 08/28/2006 Form Completion Date / / 20 mm dd yy Directions: For the following
Entered: / / 20 Initials: Verified: / /20 Initials: mm dd yy mm dd yy Patient ID - - Visit: 1 For office use only. UIB Version: 08/28/2006 Form Completion Date / / 20 mm dd yy Directions: For the following
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Todd Martin, PT Jared Bailey, PT Samantha Stollberg, PT, PRPC Karen Bailey, PT John Hollinshead, PT Sarada Bird, DPT Adrian Asencio, OTR/L, CHT
 Adrian Asencio, OTR/L, CHT Please fill out the enclosed forms and bring them with you to your first appointment. At that time, we will do a brief examination of your pelvic floor muscles, and you are welcome
Adrian Asencio, OTR/L, CHT Please fill out the enclosed forms and bring them with you to your first appointment. At that time, we will do a brief examination of your pelvic floor muscles, and you are welcome
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Urinary dysfunction assessment tool (care home)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
CommonKnowledge. Pacific University. Gina Clark Pacific University. Lauren Murphy Pacific University. Recommended Citation.
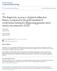 Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2012 The diagnostic accuracy of patient subjective history compared to the gold standard of urodynamic testing
Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2012 The diagnostic accuracy of patient subjective history compared to the gold standard of urodynamic testing
Incontinence: The silent scourge of the young and old. The International Continence Society has. In this article:
 Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Focus on CME at the University of Toronto Incontinence: The silent scourge of the young and old By Sender Herschorn, BSc, MDCM, FRCSC In this article: 1. What is the workup for urinary incontinence? 2.
Incontinence Patient Information Form
 Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Questionnaire for Incontinent Patients
 Questionnaire for Incontinent Patients Name Date: Date of birth: weight: height: Vaginal deliveries: Caesarean Sections: profession: No Yes Sometimes Yes 50% or more Do you lose urine during sneezing or
Questionnaire for Incontinent Patients Name Date: Date of birth: weight: height: Vaginal deliveries: Caesarean Sections: profession: No Yes Sometimes Yes 50% or more Do you lose urine during sneezing or
Patient History. 6. Rate the severity of this problem from 0-10 /10 7. Describe previous treatment/exercises
 Patient History OUTPATIENT PHYSICAL THERAPY Name Age Date Best phone number to reach you: Email: check if you prefer to be reached by email 1. Describe the current problem that brought you here 2. When
Patient History OUTPATIENT PHYSICAL THERAPY Name Age Date Best phone number to reach you: Email: check if you prefer to be reached by email 1. Describe the current problem that brought you here 2. When
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
PREVALENCE OF URINARY INCONTINENCE AND INTENTION TO SEEK TREATMENT IN THE ELDERLY
 Prevalence of Urinary Incontinence in the Elderly PREVALENCE OF URINARY INCONTINENCE AND INTENTION TO SEEK TREATMENT IN THE ELDERLY I-Jen Tseng, Yen-Ta Chen, Ming-Tan Chen, Hsin-Yi Kou, 1 and Shu-Fen Tseng
Prevalence of Urinary Incontinence in the Elderly PREVALENCE OF URINARY INCONTINENCE AND INTENTION TO SEEK TREATMENT IN THE ELDERLY I-Jen Tseng, Yen-Ta Chen, Ming-Tan Chen, Hsin-Yi Kou, 1 and Shu-Fen Tseng
AgePage. Urinary Incontinence
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
AgePage. Urinary Incontinence
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about grandchildren and visiting with neighbors. But lately she s been having a big problem that
Trainee Assessment. Incontinence. Unit standard Version Level Credits
 Trainee Assessment Incontinence Unit standard Version Level Credits 28546 Describe incontinence and interventions to assist a person in a health or wellbeing setting 1 3 5 Your name: Your workplace: Your
Trainee Assessment Incontinence Unit standard Version Level Credits 28546 Describe incontinence and interventions to assist a person in a health or wellbeing setting 1 3 5 Your name: Your workplace: Your
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
A word about incontinence
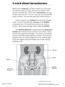 A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women
 When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women Grace Umejei, BSN, RN, CWOC. Texas Health Presbyterian Hospital Dallas NICHE Online Connect Webinars
When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women Grace Umejei, BSN, RN, CWOC. Texas Health Presbyterian Hospital Dallas NICHE Online Connect Webinars
FEMALE SYMPTOM MONITOR
 FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
Training a Wayward Bladder
 D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
D. James Ballard, PT, DPT, GCS The University of Utah, Dept. of Physical Therapy Training a Wayward Bladder Agenda 1. Discuss urinary incontinence 2. Review pelvic floor and lower urinary tract functional
Urinary Incontinence? - gør dig ikke skakmat...
 Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Urogynecology History Questionnaire. Name: Date: Date of Birth: Age:
 Urogynecology History Questionnaire Name: Date: Date of Birth: Age: 1. Have you had treatment for urinary tract diseases such as (please check): stones, kidney disease, infections, tumors, injuries? 2.
Urogynecology History Questionnaire Name: Date: Date of Birth: Age: 1. Have you had treatment for urinary tract diseases such as (please check): stones, kidney disease, infections, tumors, injuries? 2.
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania
 743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 Name: DOB: / / Age: Address: City: State: Zip: Home Phone: Work Phone: Cell Phone: Reason for your visit today: Who referred you
743 Jefferson Avenue Suite 203 Scranton, Pennsylvania 18510 570.344.9997 Name: DOB: / / Age: Address: City: State: Zip: Home Phone: Work Phone: Cell Phone: Reason for your visit today: Who referred you
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
WHAT TYPES OF CONTINENCE PRODUCTS ARE THERE?
 15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
History of Present Illness Please answer the following questions
 Last Name First Name Date of Birth: / / What is the main reason for your visit today? Social Security Number: History of Present Illness Please answer the following questions Bladder Cancer Urinary Tract
Last Name First Name Date of Birth: / / What is the main reason for your visit today? Social Security Number: History of Present Illness Please answer the following questions Bladder Cancer Urinary Tract
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment
 Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Coping with urges and leaks?
 OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
OAB AND YOU Coping with urges and leaks? Let me help you learn more about overactive bladder (OAB) symptoms and ways to help manage them 1 HOW DOES THE BLADDER WORK? Within the urinary tract, the kidneys
URINARY INCONTINENCE FOR FALLS PREVENTION. by Susan Elms P.T. Elms Physiotherapy
 URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urogyn Initial Visit Packet
 Urogyn Initial Visit Packet Please complete the questions. If they do not apply you can skip to the next question or the next section whichever is appropriate. Thanks so much for your time. This will help
Urogyn Initial Visit Packet Please complete the questions. If they do not apply you can skip to the next question or the next section whichever is appropriate. Thanks so much for your time. This will help
Y0028_2726_0 File&Use Bladder Control Does Matter
 Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
UNC Urogynecology and Reconstructive Pelvic Surgery Division of Female Pelvic Medicine and Reconstructive Surgery (FPMRS)
 UNC Urogynecology and Reconstructive Pelvic Surgery Division of Female Pelvic Medicine and Reconstructive Surgery (FPMRS) We are looking forward to your upcoming visit with us. Our goal is to provide you
UNC Urogynecology and Reconstructive Pelvic Surgery Division of Female Pelvic Medicine and Reconstructive Surgery (FPMRS) We are looking forward to your upcoming visit with us. Our goal is to provide you
Information for Patients. Overactive bladder syndrome (OAB) English
 Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
Information for Patients Overactive bladder syndrome (OAB) English Table of contents What is the bladder?... 3 What are overactive bladder symptoms?... 3 What causes overactive bladder symptoms?... 3 Diagnosis
The Development of the Revised Urinary Incontinence Scale (RUIS) Jan Sansoni, Nick Marosszeky, Emily Sansoni, Graeme Hawthorne.
 Study funded by the Australian Government Department of Health and Ageing as part of the National Continence Management Strategy The Development of the Revised Urinary Incontinence Scale (RUIS) Jan Sansoni,
Study funded by the Australian Government Department of Health and Ageing as part of the National Continence Management Strategy The Development of the Revised Urinary Incontinence Scale (RUIS) Jan Sansoni,
Information to Help You Live Life to the Fullest
 Information to Help You Live Life to the Fullest For more information and to join the conversation visit: Prevail.com/LOBC 800-227-3551 CONSUMER EDUCATION 2015 First Quality Products, Inc. All rights reserved.
Information to Help You Live Life to the Fullest For more information and to join the conversation visit: Prevail.com/LOBC 800-227-3551 CONSUMER EDUCATION 2015 First Quality Products, Inc. All rights reserved.
Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC)
 Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC) Name: Age: Reason for visit/referral: Are you referred for or interested in surgery? Yes No Maybe Referring
Female Pelvic Medicine & Reconstructive Surgery Beth Israel Deaconess Medical Center (BIDMC) Name: Age: Reason for visit/referral: Are you referred for or interested in surgery? Yes No Maybe Referring
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Differences in Prevalence of Urinary Incontinence by Race /Ethnicity
 Differences in Prevalence of Urinary Incontinence by Race /Ethnicity David H. Thom, MD, PhD, 1 Stephen K. Van Den Eeden, PhD, 2 Arona I. Ragins, MA, 2 Christina Wassel-Fyr, MS, 1 Eric Vittinghof, PhD,
Differences in Prevalence of Urinary Incontinence by Race /Ethnicity David H. Thom, MD, PhD, 1 Stephen K. Van Den Eeden, PhD, 2 Arona I. Ragins, MA, 2 Christina Wassel-Fyr, MS, 1 Eric Vittinghof, PhD,
Name: Date: Referring Provider: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary).
 Name: Date: Referring Provider: Age: D.O.B. Race/ ethnicity: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary). We are interested in learning
Name: Date: Referring Provider: Age: D.O.B. Race/ ethnicity: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary). We are interested in learning
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Patient History Form
 Outpatient Rehabilitation 1000 Fowler Way, Suite 6 Placerville, CA 95667 T: 530-344-5430; F: 530-344-5431 Patient History Form Please fill in the following questionnaire to the best of your ability. The
Outpatient Rehabilitation 1000 Fowler Way, Suite 6 Placerville, CA 95667 T: 530-344-5430; F: 530-344-5431 Patient History Form Please fill in the following questionnaire to the best of your ability. The
Female Symptom Monitor
 Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
Featured Topic: Bladder Health
 Featured Topic: Bladder Health 3 signs of an overactive bladder (from heathline.com) Gotta go, NOW Sudden, overwhelming need to urinate; you may not make it to the bathroom on time Can happen even if you
Featured Topic: Bladder Health 3 signs of an overactive bladder (from heathline.com) Gotta go, NOW Sudden, overwhelming need to urinate; you may not make it to the bathroom on time Can happen even if you
UROGYNECOLOGY. In your own words, please write the nature of your medical problem for which you are being seen today.
 Thank you for taking the time to fill out this questionnaire. A detailed and accurate health history will enable us to give you the best care and treatment. NAME AGE DATE In your own words, please write
Thank you for taking the time to fill out this questionnaire. A detailed and accurate health history will enable us to give you the best care and treatment. NAME AGE DATE In your own words, please write
Northeast Ohio Urogynecology Patient History Intake Form. Last Name First Name Age. Date of Birth Race Referring Physician.
 Northeast Ohio Urogynecology Patient History Intake Form Last Name _First Name Age_ Date of Birth Race Referring Physician Reason for Visit: _ Allergies: Preferred Lab (circle): QUEST LABCARE PLUS LABCORP
Northeast Ohio Urogynecology Patient History Intake Form Last Name _First Name Age_ Date of Birth Race Referring Physician Reason for Visit: _ Allergies: Preferred Lab (circle): QUEST LABCARE PLUS LABCORP
Patient Registration (Please complete all pages. Thank you.) PATIENT INFORMATION
 Patient Registration (Please complete all pages. Thank you.) PATIENT INFORMATION PATIENT NAME (Last, First, Middle Initial) EMAIL ADDRESS ADDRESS SOCIAL SECURITY NUMBER DATE OF BIRTH CITY STATE ZIP HOME
Patient Registration (Please complete all pages. Thank you.) PATIENT INFORMATION PATIENT NAME (Last, First, Middle Initial) EMAIL ADDRESS ADDRESS SOCIAL SECURITY NUMBER DATE OF BIRTH CITY STATE ZIP HOME
Female Symptom Monitor
 Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Compassionate and effective management
 IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Mary South, MD 3647 Medina Road Medina, OH Phone: Fax: has an appointment. on at AM/PM.
 Mary South, MD 3647 Medina Road Medina, OH 44256 Phone: 234-205-2040 Fax: 234-205-2040 has an appointment on at AM/PM. To make sure your first visit goes smoothly, we ask that you complete the enclosed
Mary South, MD 3647 Medina Road Medina, OH 44256 Phone: 234-205-2040 Fax: 234-205-2040 has an appointment on at AM/PM. To make sure your first visit goes smoothly, we ask that you complete the enclosed
MICHELLEFEDEWA _. mum AND RESEARCH eumamas 0N URINARY. INCONTINENCE IN AMBULATORY CARES j - Schaiaréy ngect 15mm Degree 0% as.
 ms osvaomam or A PHYSICAL assassmzwnom FOR, ' UTILIZATION OF THE AGENCY FOR HEALTH. CARE mum AND RESEARCH eumamas 0N URINARY INCONTINENCE IN AMBULATORY CARES j - Schaiaréy ngect 15mm Degree 0% as. 3-,
ms osvaomam or A PHYSICAL assassmzwnom FOR, ' UTILIZATION OF THE AGENCY FOR HEALTH. CARE mum AND RESEARCH eumamas 0N URINARY INCONTINENCE IN AMBULATORY CARES j - Schaiaréy ngect 15mm Degree 0% as. 3-,
Urinary Incontinence. a problem for many
 Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Name DOB Age Date Address Phone
 Patient History Name DOB Age Date Address Phone E-mail 1. Describe the current problem that brought you here: 2. When did your problem first begin? 3. Was your first episode of the problem related to a
Patient History Name DOB Age Date Address Phone E-mail 1. Describe the current problem that brought you here: 2. When did your problem first begin? 3. Was your first episode of the problem related to a
Help-seeking and associated factors in female urinary incontinence The Norwegian EPINCONT Study
 ORIGINAL PAPER Help-seeking and associated factors in female urinary incontinence The Norwegian EPINCONT Study Yngvild S. Hannestad, Guri Rortveit and Steinar Hunskaar Section for General Practice, Department
ORIGINAL PAPER Help-seeking and associated factors in female urinary incontinence The Norwegian EPINCONT Study Yngvild S. Hannestad, Guri Rortveit and Steinar Hunskaar Section for General Practice, Department
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS.
 IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
Dear. Kind regards and thanks in advance
 Dear Kind regards and thanks in advance 1 Questionnaire prior to surgery Personal identity number: Name Address Postal code Phone Email City If the above information is missing or incorrect, please fill
Dear Kind regards and thanks in advance 1 Questionnaire prior to surgery Personal identity number: Name Address Postal code Phone Email City If the above information is missing or incorrect, please fill
PELVIC FLOOR QUESTIONNAIRE. Occupation Employer Hours worked per week. What are your symptoms?
 PELVIC FLOOR QUESTIONNAIRE Name Age: Weight: Occupation Employer Hours worked per week What are your symptoms? When did symptoms start? (Onset Date) Surgery Date Where did you have surgery? Cause of symptoms?
PELVIC FLOOR QUESTIONNAIRE Name Age: Weight: Occupation Employer Hours worked per week What are your symptoms? When did symptoms start? (Onset Date) Surgery Date Where did you have surgery? Cause of symptoms?
Downloaded from armaghanj.yums.ac.ir at 19: on Friday March 22nd 2019 SPSS IQOL : IRCT N1. : *** **** *****
 : :.. :.. SPSS.. : /±/.( p
: :.. :.. SPSS.. : /±/.( p
Research. Estrogen receptors have been identified
 Research UROGYNECOLOGY Postmenopausal hormone therapy and incident urinary incontinence in middle-aged women Mary K. Townsend, ScD; Gary C. Curhan, MD, ScD; Neil M. Resnick, MD; Francine Grodstein, ScD
Research UROGYNECOLOGY Postmenopausal hormone therapy and incident urinary incontinence in middle-aged women Mary K. Townsend, ScD; Gary C. Curhan, MD, ScD; Neil M. Resnick, MD; Francine Grodstein, ScD
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Date: Initial Visit: am/pm 1st Return: am/pm
 DEMOGRAPHICS RECORDS Patient Code: MDK / LK / KH / KC-H / JS Date: Initial Visit: am/pm 1st Return: am/pm Patient Aware: Yes No FAX WALK-IN PATIENT CALLED Rx Date: DTA: PATIENT INFORMATION: Injury/Diagnosis:
DEMOGRAPHICS RECORDS Patient Code: MDK / LK / KH / KC-H / JS Date: Initial Visit: am/pm 1st Return: am/pm Patient Aware: Yes No FAX WALK-IN PATIENT CALLED Rx Date: DTA: PATIENT INFORMATION: Injury/Diagnosis:
NEW PATIENT APPOINTMENT UROLOGY
 Urology 2119 East South Blvd. 2 nd Floor Phone: 334-613-7070 NEW PATIENT APPOINTMENT UROLOGY, you have an appointment with Dr. Geoffrey Habermacher Dr. Joseph Pazona Larry Thomas CRNP Sherry Henning CRNP
Urology 2119 East South Blvd. 2 nd Floor Phone: 334-613-7070 NEW PATIENT APPOINTMENT UROLOGY, you have an appointment with Dr. Geoffrey Habermacher Dr. Joseph Pazona Larry Thomas CRNP Sherry Henning CRNP
Tips & Tricks for Usage
 Life. Not leaks. BLADDER SUPPORT FOR WOMEN Tips & Tricks for Usage Based on feedback from users and clinicians, here are some questions and answers that might help with using your uresta bladder support
Life. Not leaks. BLADDER SUPPORT FOR WOMEN Tips & Tricks for Usage Based on feedback from users and clinicians, here are some questions and answers that might help with using your uresta bladder support
Patient History. Name Age Date. 2. When did your problem first begin?
 Patient History Name Age Date 1. Describe the problem that brought you here? 2. When did your problem first begin? 3. Was your first episode of the problem related to a specific incident/injury? Yes/No
Patient History Name Age Date 1. Describe the problem that brought you here? 2. When did your problem first begin? 3. Was your first episode of the problem related to a specific incident/injury? Yes/No
NZQA registered unit standard version 1 Page 1 of 5
 Page 1 of 5 Title Describe continence, incontinence, interventions, and required reporting in an aged care, health, or disability context Level 2 Credits 8 Purpose People credited with this unit standard
Page 1 of 5 Title Describe continence, incontinence, interventions, and required reporting in an aged care, health, or disability context Level 2 Credits 8 Purpose People credited with this unit standard
Glossary of terms Urinary Incontinence
 Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
Patient Information English Glossary of terms Urinary Incontinence Anaesthesia (general, spinal, or local) Before a procedure you will get medication to make sure that you don t feel pain. Under general
UW MEDICINE PATIENT EDUCATION. About Your Surgery DRAFT
 UW MEDICINE PATIENT EDUCATION About Your Surgery Transurethral resection of the prostate (TURP) This handout describes a transurethral resection of the prostate. It also gives instructions to follow before
UW MEDICINE PATIENT EDUCATION About Your Surgery Transurethral resection of the prostate (TURP) This handout describes a transurethral resection of the prostate. It also gives instructions to follow before
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
Unintended urine loss is a common symptom among
 Informal Caregiving Time and Costs for Urinary Incontinence in Older Individuals in the United States Kenneth M. Langa, MD, PhD,* # Nancy H. Fultz, PhD, Sanjay Saint, MD, MPH,* # Mohammed U. Kabeto, MS,
Informal Caregiving Time and Costs for Urinary Incontinence in Older Individuals in the United States Kenneth M. Langa, MD, PhD,* # Nancy H. Fultz, PhD, Sanjay Saint, MD, MPH,* # Mohammed U. Kabeto, MS,
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Urogynecology Associates of Philadelphia URODYNAMIC TESTING
 URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
URODYNAMIC TESTING Urogynecology Associates of Philadelphia Most women with urinary incontinence will need to complete a few simple tests, performed in the office, to help your doctor assess your symptoms
Welcome to the Centre for Aging and Wellness at Florida Hospital!
 133 Benmore Dr. Winter Park, FL 32789 PH: 407-599-6060 FAX: 407-646-7747 Welcome to the Centre for Aging and Wellness at Florida Hospital! We are pleased you have chosen us as part of your health care
133 Benmore Dr. Winter Park, FL 32789 PH: 407-599-6060 FAX: 407-646-7747 Welcome to the Centre for Aging and Wellness at Florida Hospital! We are pleased you have chosen us as part of your health care
encathopedia Volume 7 PARKINSON S AND THE BLADDER
 encathopedia Volume 7 PARKINSON S AND THE BLADDER Parkinson s disease Parkinson s is a progressive neurological condition. In people with Parkinson s, some of the brain cells that create the chemical dopamine
encathopedia Volume 7 PARKINSON S AND THE BLADDER Parkinson s disease Parkinson s is a progressive neurological condition. In people with Parkinson s, some of the brain cells that create the chemical dopamine
case Prof. Dr.J.Vande Walle Feb Universitair Ziekenhuis Gent 1
 case Prof. Dr.J.Vande Walle Feb 2012 1 A boy, 10 years old! Bedwetting 5/7days! nocturia! wet pants! Frequency 5 x/day! constipation! adhd! URI/ uropathie 2 Urological symptoms* /ALARMSYMPTOMS Yes Leakages
case Prof. Dr.J.Vande Walle Feb 2012 1 A boy, 10 years old! Bedwetting 5/7days! nocturia! wet pants! Frequency 5 x/day! constipation! adhd! URI/ uropathie 2 Urological symptoms* /ALARMSYMPTOMS Yes Leakages
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Diagnosis and Treatment of Urinary Incontinence. Urinary Incontinence
 Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Diagnosis and Treatment of Urinary Incontinence Leslee L. Subak, MD Professor Obstetrics, Gynecology & RS Epidemiology, Urology University of California, San Francisco Urinary Incontinence Common - 25%
Numerous articles about urinary incontinence (UI) begin
 Self-Reported Social and Emotional Impact of Urinary Incontinence Nancy H. Fultz, PhD,* and A. Regula Herzog, PhD* From the *Institute for Social Research and Institute of Gerontology, and Department of
Self-Reported Social and Emotional Impact of Urinary Incontinence Nancy H. Fultz, PhD,* and A. Regula Herzog, PhD* From the *Institute for Social Research and Institute of Gerontology, and Department of
