The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
|
|
|
- Cameron Peters
- 5 years ago
- Views:
Transcription
1 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
2 Objectives Understand risk factors and treatment of post- partum urinary retention ti Explore urogynecologic problems immediately post-partum; partum; including urogenital atrophy, breakdown of episiotomies, rectovaginal fistulas, and sexual function Contrast treatments of urinary incontinence while a patient is still pregnant or immediately post-partum to that of a patient remote from delivery Compare and contrast the effect of mode of delivery on pelvic floor disorders
3 Acute Changes Bladder Management Effects of breastfeeding Lacerations/episiotomies i i t i Rectovaginal fistulas Sexual function Incontinence
4 Bladder Function Third month of pregnancy, bladder capacity increases 1 st sensation often , Max urge ml in supine position Standing position, the pregnant uterus exerts pressure on the bladder Doubling of bladder pressure by 38wks Once delivery occurs, without weight of pregnant uterus, postpartum bladder can be hypotonic
5 Bladder Function What is normal PVR in obstetric population? Third trimester 152+/-44mL Postpartum t 110+/-130mL 130 Non-obstetric obstetric population Agency for Health Care Policy and Research <50mL normal >200mL abnormal PVR Driggers RW, Miller CR, Zahn CM. Postpartum Urinary Retention, Letters to the Editor. Obstet & Gyn. Dec 2005:106(6)
6 Postpartum Urinary Retention Single episode of postpartum bladder overdistension May cause persistent urinary retention Irreversible damage to the detrusor muscle Recurrent UTIs Permanent voiding difficulties Early detection decreases proportion of women who require long-term catheterization At 4 years, those with postpartum urinary retention did not have higher prevalence of urinary stress incontinence Rizvi RM et al. Diagnosis and management of postpartum urinary retention. Int Journal of Gyn and Obstet (2005)91,71-71.
7 Postpartum Urinary Retention Definition of abnormal postpartum post-void residual is controversial Functional definition Absence of spontaneous micturition in the first 6 hours following vaginal delivery 6 hours after removal of indwelling catheter in cases of Cesarean delivery Incidence: % (both vaginal and Cesarean deliveries)
8 Postpartum Urinary Retention Risk factors: Instrumented delivery Pi Primiparityi it Episiotomy Sphincter disruption Larger lacerations Protracted labor- Increased 1 st or 2 nd stage, >/= 800 minutes Regional anesthesia- Epidural increases risk up to 3x Musselwhite KL, Faris P, Moore K, et al. Use of epidural anesthesia and the risk of acute postpartum urinary retention. Am J Obstet Gynecol 2007;196:472.e1-472.e5. Morphine related postoperative anesthesia (in those with cesarean section) (Liang CC, Chang SD, Chang YL, et al. Postpartum urinary retention after cesarean delivery. Int J of Gyn and Obstet (2007) 99, ) Glavind K,Bjork J. Incidence and treatment of urinary retention postpartum. Int Urogynecol J(2003) 14:
9 Postpartum Urinary Retention: The Silent Type 100 patients within 48 hours from delivery or removal of indwelling catheter Residual urine was estimated using a portable bladder scanner 37 had PVR>150mL 26 had PVR between mL 11 had PVR>200mL Clinical significance? Silent retention affects a significant proportion of patients after delivery- needs further investigation Ismail SIM and Emery SJ. The prevalence of silent postpartum retention of urine in a heterogenous cohort. Journal of Obstet & Gyn. 2008;28(5):
10 Postpartum Urinary Retention How do we prevent it? Timing and measuring the first postpartum voided volume and potentially checking the first PVR(1) Ultrasonographic volume estimation gives reasonable bladder volume assessment- transabdominal as good as transvaginal(2) Measurement by ultrasound found to be fairly accurate when compared to volume from catheterization (within 10%) 1. Zaki mm. Nvoational survey for intrapartum and postpartum bladder care:assessing the need for guidelines. BJOG: An Inter Jour of Obstet & Gyn. (2004)111(8): Yip SK et al. Ultrasonographic Estimation of Postpartum Residual Bladder Volume. Int U
11 Postpartum Urinary Retention How do we treat it? Oral analgesics, patient mobilization, providing privacy How do we ask the right questions? How are they voiding? Specifically do they have a slow stream, intermittency, hesitancy, straining, or a feeling of incomplete emptying of the bladder? Humburg J. et al. Prolonged Postpartum Urinary Retention: The Importance of Asking the Right Questions at the Right Time. Gynecol Obstet Invest. 2007;64:69-71.
12 Postpartum Urinary Retention Treatment: Investigate those you suspect Abdominal ultrasound reliable Indwelling catheter hours, based on post-void residual volume Intermittent bladder catheterization Every 4-6 hours until PVR<150cc Suprapubic catheter Prophylactic antibiotics
13
14 Breastfeeding Link of urogenital atrophy and breastfeeding Hypoestrogenic state following delivery and lasting until ovulation resumes Patient presents with dyspareunia, pelvic pressure, and stress incontinence Treatment: small amounts of topical estrogen applied daily for several weeks and vaginal lubricants with coitus(olive oil and vegetable shortening)
15 Lacerations/Episiotomies More common with operative vaginal deliveries Up to 13% rate of 3 rd and 4 th degree episiotomy extensions and vaginal lacerations with outlet forceps Station and degree of instrument rotation g correlate with morbidity
16 Episiotomy Dehiscence Infection concern 0.5% of episiotomy wounds dehisce and 80% of these are due to infection Other risk factors: smoking, HPV infection, and coagulation disorders Symptoms Pain(65%), purulent discharge(65%) and fever(44%)
17 Episiotomy Treatment of infection Establish drainage, cut and remove sutures, treat with appropriate antibiotics Dehiscence Timing of repair Surgical wound must be properly cleaned and free of infection Early versus late repair: Repair may take place as long as patient is afebrile and pink, healthy granulation tissue is present Williams Gyn. Puerperium, p
18 Fistulas Rectovaginal Mainly in undeveloped d countries 90% of those in developed countries due to childbirth Tissues of birth canal lying between the leading part and the pelvic wall may be subjected to excessive pressure necrosis fistula formation Risk factors: Operative vaginal delivery Episiotomy Prolonged second stage Dystocia
19 Rectovaginal Fistula Present with uncontrollable passage of gas or feces from the vagina, malodorous vaginal discharge, or fecal soiling of undergarment
20 Rectovaginal Fistula Most are located in the distal third of the vagina just above the hymen. Delay repair until inflammation and induration have resolved. Transvaginal approach: excise fistulous track, mobilize the planes, and perform layered closure
21 Repaired Rectovaginal Fistula
22 Cloaca
23 Sexual Function Cross-sectional study using obstetric records and a postnatal survey 6 months after delivery Main outcome measures: self-reported sexual behaviors and sexual problems including vaginal dryness, painful penetration, pain during sexual intercourse, pain on orgasm, vaginal tightness, vaginal looseness, bleeding/irritation after sex, and loss of sexual desire
24 Sexual Function 484 respondents (61% response rate) 89% resumed sexual activity within six months of the birth Sexual morbidity increased after the birth: 38% report pre-pregnancy p sexual problems 83% of women reported sexual problems within the first 3 months after delivery Declined to 64% at six months Barrett,G et al. Women's Sexual Health After Childbirth. BJOG 2005;107(2):
25 Sexual Function Dyspareunia in the first 3 months was associated with vaginal delivery(p=0.01) and previous experience of dyspareunia(p=0.03) 03) At 6 months, delivery route was not significant. Only experience of dyspareunia prior to pregnancy(p<0.0001) and current breastfeeding(p=0.0006) 0006) were significant ifi Only 15% of patients with a postnatal sexual Only 15% of patients with a postnatal sexual problem discussed it with a health professional
26 Sexual Function Sphincter laceration: 270% increase in sexual pain postpartum when compared to women without perineal laceration Spontaneous lacerations versus Episiotomy It is better to tear than be cut Those with spontaneous lacerations report less pain with intercourse than do women who undergo episiotomy Rogers RG and Leeman LL. Postpartum Genitourinary Changes. Urol Clin N Am 34(2007)13-21.
27 Sexual Function Retrospective cohort study Six months postpartum 35% primiparous women complain of decreased sexual sensation 24% express decreased sexual satisfaction 22% complain of dyspareunia
28 Sexual Function Intercourse related problems can persist months following delivery Best thing we can do is ask!
29 Urinary Incontinence Operative deliveries are risks for bladder dysfunction, including incontinence (Carly ME, Carley JM, Vasdev G, et al. Factors that are associated with clinically overt postpartum urinary retention after vaginal delivery. Am J Obstet Gynecol 187:430,2002) Urinary incontinence after forceps delivery was more likely to persist than that associated with vacuum or SVD (Arya LA, Jackson ND, Myers DL, et al. Risk of new-onset urinary incontinence after forceps and vacuum delivery in primiparous women. Am J Obstet Gynecol 185:1318,2001)
30 Urinary Incontinence Post-partum Treatment Options: Timed Voids Avoid Bladder Irritants Pelvic Floor Exercises Pessaries
31 Urge Urinary Incontinence May occur as commonly as stress incontinence after childbirth Up to 30% Increased association with forceps delivery and episiotomy *Mainstay of treatment: anticholinergics Casey BM et al. Obstetric antecedents for postpartum pelvic floor dysfunction. Am J Obstet Gynecol 2005;192:
32 Urinary Incontinence Women with persistent stress incontinence at 3 months postpartum t have a 92% chance of having stress urinary incontinence at 5 years Viktrup L,Lose G. The risk of stress incontinence 5 years after first delivery. Am J Obstet Gynecol 2001;185:82-7.
33 Chronic or Long Term Changes Incontinence Prolapse C d li SVD O ti Cesarean delivery vs. SVD vs. Operative Vaginal Delivery
34 Pelvic Floor Dysfunction; What have we been trained to prevent? Anal sphincter injury? Anterior damage and stress incontinence? Levator ani damage and pelvic organ prolapse? What should we worry about?
35 What latent injuries occur during birth that lay dormant leading to prolapse later in life? What is the disease process? Muscle Rupture? Connective tissue detachment? Nerve injury?
36 Distribution of Pelvic Floor Disorders % Affected Age Range (years) DI GSI POP Luber. Am J Obstetrics Gynecol 2001;184:1494
37 Urinary Incontinence Effect of one vaginal delivery on the prevalence of stress urinary incontinence Prospective trial Showing one interval vaginal delivery did not increase risk of stress urinary incontinence up to 4 years after the delivery(28.6% in controls, 21.1% 1% in vaginal delivery patients) Yip et al. Effect of one vaginal delivery on the prevalence of stress urinary incontinence: A prospective study. Neurology and Urodynamics. 22(6) Aug 2003.
38 Urinary Incontinence Comparing vaginal deliveries to Cesarean deliveries Higher prevalence of stress incontinence in women who have had vaginal deliveries Differences significant only in the young In older women age and obesity outweigh the method of delivery Women having Cesarean after labor have similar incidence of stress incontinence to those having vaginal delivery-> suggests labor process not the birth itself
39 Urinary Incontinence Women who had Cesarean section reported less urinary incontinence than women who delivered vaginally at: 3 months: relative risk 0.62, 95% CI ( ) 2 years postpartum: p difference did not persist Hannah ME et al. Maternal outcomes at 2 years after planned cesarean section versus planned vaginal birth for breech presentation at term: The International Randomized Term Breech Trial. Am J Obstet Gynecol 2004;191:
40 Urinary Incontinence Levator ani injuries associated with stress urinary incontinence It is unclear if the defect is responsible or marker for global pelvic floor injury
41 Urinary Incontinence Treatments: Same options as immediately post- partum Plus suburethral slings
42 Anal Incontinence Up to 40% of women with an anal sphincter laceration (including 3 rd or 4 th degrees) complain of anal incontinence Range of 20-50% Garcia V et al. Primary repair of obstetric anal sphincter laceration: a randomized trail of two surgical techniques. Am J Obstet Gynecol 2005;192(5);
43 Anal Incontinence(chronic) Up to 2 years after delivery, >25% of women with fecal incontinence report negative quality of life Despite this, few women seek treatment or even discuss with their physician 10% at 6 months 13.5% at 1 year 16.7% at 2 years Lo, Jamie et al. Quality of Life in Women With Postparum Anal Incontinence. Obste and Gynecol (4):
44 Anal Incontinence Most common cause of anal incontinence in young women is anal sphincter injury at childbirth Muscle injury responsible for most anal dysfunction but pudendal nerve damage plays a role Vaginal birth leads to overt anal sphincter lacerations in up to 6% of women Up to 30% of sphincter injuries are covert Only detectable by ultrasound of the anal sphincter complex; not associated with perineal laceration Risk factors: Episiotomy Operative vaginal delivery-vacuum vacuum less than forceps Rogers RG and Leeman LL. Postpartum Genitourinary Changes. Urol Clin N Am. 34(2007)13-21.
45 Anal Incontinence Short-term versus Long-term effects 6 year follow up after delivery 3.6% prevalence of anal incontinence First delivery by forceps associated with double risk of anal incontinence relative to spontaneous vaginal delivery Cesarean delivery not protective (MacArthur C, Glazener C, Lancashire R,et al: Faecal incontinence and mode of first delivery: A six-year longitudinal study. Br J Obstet Gynaecol 112:1075,2005.) 34yr follow up after forceps delivery Significant fecal or urinary incontinence was no more likely after forceps than after vaginal (Bollard RC,Gardiner A,Duthie GS, et al. Anal sphincter injury,fecal and urinary incontinence: A 34 year follow up after forceps delivery. Dis Colon Rectum 46:1083,2003)
46 Anal Incontinence Treatment: Dietary Anal Sphincteroplasty
47 Pelvic Organ Prolapse 300,000 pelvic organ prolapse surgeries per year in the United States Outnumber surgeries for stress incontinence 2:1 ratio 1 in 9 women will have surgery for pelvic floor g y p disorders by age 80, 30% will require re-operation
48 Pelvic Organ Prolapse Vaginal delivery risk factor most commonly cited for development of pelvic organ prolapse 2 vaginal deliveries: 8.4 times more likely to have surgery for prolapse compared to women with no deliveries When comparing vaginal delivery to cesarean delivery, increased odds ratio for prolapse in vaginal delivery group 1.82 (95% CI ) 19)
49 Pelvic Organ Prolapse Treatment: Pelvic Floor Physical Therapy Pessaries Surgical Correction
50 What about birth?
51 Which Route? Does elective cesarean delivery prevent the development of pelvic floor disorders? National Institute of Health s conference Cesarean Delivery on Maternal Request -quality of evidence in support of this is weak When comparing women with 3 SVDs to 3 Cesarean sections: comparable rates of stress urinary incontinence (how many years later?) Impact seems more significant in the short term. As patients age, impact of delivery route becomes less significant Rogers RG and Leeman LL. Postpartum Genitourinary Changes. Urol Clin N Am. 34(2007)
52 Not all vaginal deliveries are created equal! Incidence of pelvic floor dysfunction symptoms are increased with: Birthweight >4000gms Episiotomy
53 Cesarean Delivery for Maternal Request 2.5% of all births in the United States in 2003 Poll of English female obstetricians (Wagner M: Choosing caesarean section. Lancet 356:1677,2000.) 30% expressed preference for an elective cesarean delivery rather than vaginal delivery Sited avoidance of pelvic floor injury as explanation for their choice
54
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
INTRAPARTUM AND POSTNATAL BLADDER CARE
 INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence
 A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
A PATIENT GUIDE TO Understanding Stress Urinary Incontinence Q: What is SUI? A: Stress urinary incontinence is defined as the involuntary leakage of urine. The problem afflicts approximately 18 million
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Provenance Rehabilitation Pelvic Intake Form
 Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Urogynecology ICD-9 to ICD-10 Crosswalks
 1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
1100 Wayne Ave, Suite 825 Silver Spring, MD 20910 301.273.0570 Fax 301.273.0778 info@augs.org www.augs.org Urogynecology ICD-9 to ICD-10 Crosswalks ICD 9 ICD 9 Description ICD 10 Code ICD 10 Description
Management of Urinary Incontinence in Older Women. Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital
 Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Management of Urinary Incontinence in Older Women Dr. Cecilia Cheon Department of Obs. & Gyn. Queen Elizabeth Hospital Epidemiology Causes Investigation Treatment Conclusion Elderly Women High prevalence
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Guidelines on the Management of Complications related to Female Genital Mutilation
 Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Among parous women, cesarean birth reduces the
 Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Bladder care postpartum including bladder care for women with epidural analgesia (GL792)
 Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Original article. Mst. Hosna Ara Khatun, 1 Jahanara Arzu 2. Prof. Zulfe Ara Haider 3.
 Original article Short term catheterization versus long term catheterization after vaginal prolapsed surgery: A randomized control trial in Dhaka National Medical College & Hospital Mst. Hosna Ara Khatun,
Original article Short term catheterization versus long term catheterization after vaginal prolapsed surgery: A randomized control trial in Dhaka National Medical College & Hospital Mst. Hosna Ara Khatun,
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Female Symptom Monitor
 Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Purpose. Policy Statement. Principles. Applicability. Responsibility
 Grey Nuns Community Hospital Postpartum Bladder Management Policy Approved by: Senior Director of Operations, Women s & Child Health, GNCH/MCH Facility Chief, Obstetrics/Gynecology, GNCH Facility Chief,
Grey Nuns Community Hospital Postpartum Bladder Management Policy Approved by: Senior Director of Operations, Women s & Child Health, GNCH/MCH Facility Chief, Obstetrics/Gynecology, GNCH Facility Chief,
Female Symptom Monitor
 Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Operative Vaginal Delivery and Pelvic Floor Trauma. Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center
 + Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
+ Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
Uterine prolapse & Fistulas. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
A Clinical Guideline for Bladder Care in Labour and Postnatally
 For Use in: Maternity department By: Clinical staff caring for women during pregnancy, labour and postnatally For: Obstetric patients Division responsible for document: Division 3- Women and Children s
For Use in: Maternity department By: Clinical staff caring for women during pregnancy, labour and postnatally For: Obstetric patients Division responsible for document: Division 3- Women and Children s
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
The circumferential obstetric fistula: characteristics, management and outcomes
 DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
DOI: 10.1111/j.1471-0528.2007.01329.x www.blackwellpublishing.com/bjog Short communication The circumferential obstetric fistula: characteristics, management and outcomes A Browning Barhirdar Hamlin Fistula
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD
 PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Maternity Services. Comment / Changes / Approval. First draft of new guidelines. Comments included after consultation.
 Bladder Care v4.0 Nov 2016 for public website FINAL NOV16 Document Control Title Bladder Care Guideline Author Directorate Women and Children s Version Date Issued Status 0.1 Jun Draft 2009 0.2 July 2009
Bladder Care v4.0 Nov 2016 for public website FINAL NOV16 Document Control Title Bladder Care Guideline Author Directorate Women and Children s Version Date Issued Status 0.1 Jun Draft 2009 0.2 July 2009
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
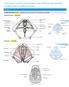 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
FEMALE SYMPTOM MONITOR
 FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
FEMALE SYMPTOM MONITOR Name: Occupation: Date: Age: Complaints: 1. 2. 3. GYNECOLOGICAL HISTORY: # pregnancies: # live births: Wt. heaviest baby: lbs oz Length pushing stage: hours Forceps? Yes No Episiotomies?
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Example Clinical Guideline for Immediate Postpartum LARC Insertion
 Example Clinical Guideline for Immediate Postpartum LARC Insertion RATIONALE Delay in contraceptive provision until the six week postpartum appointment can leave some women at risk for rapid repeat pregnancy.
Example Clinical Guideline for Immediate Postpartum LARC Insertion RATIONALE Delay in contraceptive provision until the six week postpartum appointment can leave some women at risk for rapid repeat pregnancy.
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Latest Treatments for a Leaky Bladder None
 Latest Treatments for a Leaky Bladder None Financial Disclosures Jeremiah McNamara, MD, OBGYN Boulder Women s Care 303-500-1947 Boulder Women s Care Agenda: Prolapse & Urinary Incontinence The Pelvic Floor
Latest Treatments for a Leaky Bladder None Financial Disclosures Jeremiah McNamara, MD, OBGYN Boulder Women s Care 303-500-1947 Boulder Women s Care Agenda: Prolapse & Urinary Incontinence The Pelvic Floor
Does delayed child-bearing increase the risk of levator injury in labour?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
* 梁景忠醫師 所有發表期刊論文 Bibliography
 * 梁景忠醫師 所有發表期刊論文 Bibliography A. First author and Corresponding author (2000- ) 1. Liang CC, Tseng CJ, Soong YK: The usefulness of cystoscopy in the staging of cervical cancer. Gynecol Oncol 76: 200-3,
* 梁景忠醫師 所有發表期刊論文 Bibliography A. First author and Corresponding author (2000- ) 1. Liang CC, Tseng CJ, Soong YK: The usefulness of cystoscopy in the staging of cervical cancer. Gynecol Oncol 76: 200-3,
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
Patient Advice for Third & Fourth Degree Tears
 Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
NEW POSTNATAL URINARY INCONTINENCE : OBSTETRIC AND OTHER RISK FACTORS IN PRIMIPARAE. New postnatal urinary incontinence in primiparae
 Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Birth Trauma. H. P. Dietz. University of Sydney, Nepean Campus. Penrith, Australia
 Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Introduction/Learning Objectives. Incontinence: Natural History. Course Outline 10/14/2016. Urinary Incontinence: Conservative Measures
 Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Management of Urinary Complications after Prostatectomy Course Faculty: Introduction/Learning Objectives Jaspreet S. Sandhu, MD Associate Attending Urologist Department of Surgery/Urology Memorial Sloan
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Urogynaecology & Prolapse. Alexander Denning and Leifa Jennings
 + Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
+ Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Questionnaire for Incontinent Patients
 Questionnaire for Incontinent Patients Name Date: Date of birth: weight: height: Vaginal deliveries: Caesarean Sections: profession: No Yes Sometimes Yes 50% or more Do you lose urine during sneezing or
Questionnaire for Incontinent Patients Name Date: Date of birth: weight: height: Vaginal deliveries: Caesarean Sections: profession: No Yes Sometimes Yes 50% or more Do you lose urine during sneezing or
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE
 493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
493495.q7:480499_P0 6/5/09 10:23 AM Page 1 WHAT YOU SHOULD KNOW ABOUT YOUR DIAGNOSIS OF STRESS URINARY INCONTINENCE 493495.q7:480499_P0 6/5/09 10:23 AM Page 2 What is Stress Urinary Incontinence? Urinary
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Marietta Mahendeka, M.D. Obstetrician and Gynaecologist Bugando Medical Centre Tanzania. Tutor: Dr Luc de Bernis, WHO
 A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
A COMPARATIVE STUDY OF THE MANAGEMENT OF VESICO AND/OR RECTO-VAGINAL FISTULAE AT BUGANDO MEDICAL CENTRE, MWANZA, TANZANIA, EAST AFRICA: A RETROSPECTIVE STUDY Marietta Mahendeka, M.D. Obstetrician and Gynaecologist
