Module 5 Management Of Urinary Incontinence
|
|
|
- Ethan Hines
- 5 years ago
- Views:
Transcription
1 Management Of Urinary Incontinence V3: Last Reviewed September 2017
2 Learning Outcomes Outline conservative management options Discover the options available to manage the different types of incontinence Recap and summary with questions, evaluation and certificate
3 Section 1 Introduction
4 Introduction From previous modules and additional reading, you will already be familiar with the different types of incontinence and their causes and assessment Once the continence assessment has been carried out, a management plan can then be devised Treatments and correct management can relieve symptoms and improve a person s quality of life, as well as promote independence and dignity This module will cover the treatment options and management for the five main types of urinary incontinence
5 Section 2 Treatment Options
6 Types of Urinary Incontinence
7 Stress Incontinence Pressure Leakage
8 Stress Incontinence Treatments Pelvic Floor Pelvic Floor Muscle Exercises (PFME) are the first line of treatment for stress incontinence in both men and women (Thirugnanasothy, 2010) Pelvic floor exercises should be carried out for at least three months Motivation and cognition are important, and for those that cannot contract their pelvic floor muscles, biofeedback and electrical stimulation can be used (NICE, 2010) The continence nurse or specialist physiotherapist will ensure the exercises are done correctly and they will also monitor patient progress All women should be offered pelvic floor exercise treatment in their first pregnancy to prevent postnatal stress urinary incontinence (NICE, 2013)
9 Other Stress Incontinence Treatments Treat constipation if present, as this can reduce the strain on the pelvic floor muscles (Thirugnanasothy, 2010) Ensure sufficient and appropriate fluid intake Weight reduction If conservative management is not effective Urethral injections to bulk (ICS, 2013) Surgery to support the neck of the bladder and urethra Medication if previous surgery has failed or not appropriate
10 Other Stress Incontinence Treatments Artificial sphincter (ICS, 2013) if previous surgery has failed Appropriate containment aids: - Disposable pads - Washable underwear - Sheaths (Newman & Wein, 2009)
11 Urge Incontinence Nerve impulse Detrusor muscle instability Leakage
12 Urge Incontinence Treatments Bladder Retraining Bladder retraining is the first line of treatment in both men and women for urge incontinence, and must be tried for at least a six week period (NICE, 2012) The aim is to extend voiding intervals to allow the bladder to fill more, increasing the volume and also giving control over the need to void (UroGynecology Specialty Center, 2014) Once a pattern is identified, bladder retraining can be used to predict and avoid incontinence (NICE, 2012)
13 Other Urge Incontinence Treatments Botox can be suitable for those with detrusor over activity who have not improved with conservative management. They involve injections into the bladder wall/detrusor muscle. Some people may find it difficult to void post Botulinum Toxin Type A, therefore, they must be taught and be able to do intermittent selfcatheterisation for as long as necessary. Percutaneous sacral nerve stimulation involves an implant that controls the sacral nerve supply to the bladder, allowing the person to control voiding. The person can carry it out in their own home. This is suitable for those who conservative management has not helped, and cannot perform intermittent selfcatheterisation (NICE, 2013)
14 Mixed Incontinence The principle symptom is treated first. Bladder training and pelvic floor exercises should be included (Mevcha and Hashim, 2009)
15 Overflow Incontinence Possible detrusor under activity Possible obstruction Leakage The treatment will depend on the reason. It may be either caused by bladder outlet obstruction, or detrusor under activity, or both.
16 Overflow Incontinence Treatments Toileting position Allow enough time for voiding Double voiding Bowel management, treat constipation Fluids (limit caffeine intake) Intermittent catheterisation or indwelling urethral catheter Medication review Surgery: prostate surgery/prolapse/fibroids/urethral stricture (Newman, Slack and Wein, 2011)
17 Time for Myth or Fact Understand the importance of a comprehensive continence assessment Discuss in detail the key elements of the continence assessment Outline the baseline investigations carried out as part of a continence assessment List some additional investigations that may be performed by the specialist nurse or doctor Appreciate the importance of effective interpersonal and communication skills when discussing continence issues with an individual V4: V4: Last Last Reviewed V4: Last September Reviewed May This 2017 This programme This programme has has been been has accredited been accredited by by the the RCN by RCN Centre the Centre RCN for Centre for Professional for Professional Accreditation Accreditation until until 4 th 4 th until September 7 th June Accreditation applies only only to to the the educational content of of the the programme and and does does not not apply apply to to any any product.
18 Myth or Fact? Urinary incontinence will improve if left untreated Myth or Fact?
19 Myth or Fact? Myth If left untreated, symptoms will only become worse and lead to unnecessary anguish
20 Myth or Fact? Nursing staff need a knowledge of urinary incontinence and treatment options Myth or Fact?
21 Myth or Fact? Fact Nurses need to have an understanding of the types, causes, assessment and treatment options available in order to promote dignity, independence and quality of life
22 Myth or Fact? Surgery is unavoidable in treating urinary incontinence Myth or Fact?
23 Myth or Fact? Myth Pelvic floor muscle training and behavioural therapy can greatly reduce or even eliminate symptoms
24 Section 2 Treatment Options Continued
25 Functional Incontinence
26 Functional Incontinence Treatments When a person you are caring for is incontinent, always ask yourself Can they get out of their bed or chair easily? Does the person need assistance? Ensure they can summon assistance if needed. Do they communicate with body language or sounds that indicate they need to go to the toilet? Watch for non-verbal cues such as pulling clothing, agitation or wandering. Do they know where the toilet is? Is there adequate lighting and signs? Are the floor surfaces clear or hazards / slippery surfaces? Can clothing be easily removed or adjusted? Footwear should be well fitting and non slip. Is the toilet clean and private? Are there adequate hand washing facilities?
27 Section 3 Toileting Programmes
28 Toileting Programmes When choosing a behavioural management programme, take into account that prompted voiding and bladder retraining are particularly suitable for people with cognitive impairment A bladder/voiding diary can identify if the person can feel when their bladder is full and also how often voiding is indicated (Shenot, 2014) Assisted toileting takes place at set times or on request, usually when the person is dependent on help to get to the toilet and often with those that have limited mobility or who are confused
29 Toileting Programmes Scheduled / timed toileting means voiding urine according to the time, rather than waiting for the need or urge to void (Mayo, 2014) The person goes to, or is prompted or taken to the toilet at a scheduled time before they have the urge to void Scheduled toileting can be time established by evaluation of fluid charts or after meals, on waking, midmorning, mid afternoon and before settling Scheduled toileting reinforces healthy habits and can be used with those who are confused
30 Section 4 Recap
31 Recap There are multiple treatments for each type of urinary incontinence The use of pads, appliances and catheters are not a treatment for urinary incontinence. They should only be used following assessment and treatment of reversible causes (Wagg, 2007). They can also be used during the treatment/management phase, but stopped once continence has been achieved
32 Assessment Test your knowledge of this module by using the interactive quiz in step two of the elearning tool A certificate will be available on a pass rate of 80% or over Good luck!
33 Section 5 References
34 References ICS. (2013). ICS Fact Sheets: A Background to Urinary and Faecal Incontinence. Available: [Online] [Last accessed ] Mayo Clinic. (2014). Treatments and Drugs. Available: [Online] [Last accessed ] Mevcha, A. and Hashim, H. (2009). Bladder Training Urinary Incontinence - Good Clinical Care Foundation. Foundation Years Journal. 3 (5), p 36. NICE. (2010). Lower urinary tract symptoms: The management of lower urinary tract symptoms in men. Available: [Online] [Last accessed ] NICE. (2012). Urinary incontinence in neurological disease: Management of lower urinary tract dysfunction in neurological disease. Available: [Online] [Last accessed ] Newman, D, K., Wein, A, J. (2009). Managing and Treating Urinary Incontinence. 2nd Ed. Health Professions Press: Baltimore.
35 References Shenot, P, J. (2014). Urinary Incontinence in Adults. Available: [Online] [Last accessed ] Newman, D, K., Slack, A., Wein, A, J. (2011). Fast Facts: Bladder Disorders. 2nd Ed. Health Press Limited: Oxford. Thirugnanasothy, S. (2010). Managing Urinary Incontinence in Older People. BMJ. C3835, p 341. UroGynecology Specialty Center (2014). Urinary Incontinence. Available: [Online] [Last accessed ] Wagg, A. (2007). Continence. Available: [Online] [Last accessed ]
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
NZQA registered unit standard version 1 Page 1 of 5
 Page 1 of 5 Title Describe continence, incontinence, interventions, and required reporting in an aged care, health, or disability context Level 2 Credits 8 Purpose People credited with this unit standard
Page 1 of 5 Title Describe continence, incontinence, interventions, and required reporting in an aged care, health, or disability context Level 2 Credits 8 Purpose People credited with this unit standard
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd
 Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd Segment 1 What is continence? Incontinence is not a but a sign of What organs are involved? and Urine incontinence
Continence Worksheet Name: Date: Name of Trainer: Name of Company: Clinical Update (NZ) Ltd Segment 1 What is continence? Incontinence is not a but a sign of What organs are involved? and Urine incontinence
Urinary dysfunction assessment tool (community)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (community) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Urinary dysfunction assessment tool (care home)
 Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
Addressograph label CHI:... Name:... Address:...... Urinary dysfunction assessment tool (care home) Past medical history: Is the patient on medications which can affect bladder function? If, please list
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Trainee Assessment. Incontinence. Unit standard Version Level Credits
 Trainee Assessment Incontinence Unit standard Version Level Credits 28546 Describe incontinence and interventions to assist a person in a health or wellbeing setting 1 3 5 Your name: Your workplace: Your
Trainee Assessment Incontinence Unit standard Version Level Credits 28546 Describe incontinence and interventions to assist a person in a health or wellbeing setting 1 3 5 Your name: Your workplace: Your
Incontinence in neurological disease
 nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
nice bulletin Incontinence in neurological disease NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin - Incontinence in neurological disease.indd
Clean Intermittent Self-Catheterisation (CISC)
 Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Saint Mary s Hospital & Trafford General Hospital Uro-gynaecology Service Information for Patients Clean Intermittent Self-Catheterisation (CISC) What is catheterisation? Catheterisation involves passing
Information to Help You Live Life to the Fullest
 Information to Help You Live Life to the Fullest For more information and to join the conversation visit: Prevail.com/LOBC 800-227-3551 CONSUMER EDUCATION 2015 First Quality Products, Inc. All rights reserved.
Information to Help You Live Life to the Fullest For more information and to join the conversation visit: Prevail.com/LOBC 800-227-3551 CONSUMER EDUCATION 2015 First Quality Products, Inc. All rights reserved.
Module 3 Causes Of Urinary Incontinence
 Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Causes Of Urinary Incontinence V4: Last Reviewed September 2017 Learning Outcomes Appreciate the numerous requirements and skills necessary for the person to achieve and maintain urinary continence Discuss
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Urinary Incontinence. Lora Keeling and Byron Neale
 Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Urinary Incontinence Lora Keeling and Byron Neale Not life threatening. Introduction But can have a huge impact on quality of life. Two main types of urinary incontinence (UI). Stress UI leakage on effort,
Intravesical Botox Injections
 Intravesical Botox Injections Department of Urology Patient Information What What is is Botox? Botox? Botox or Botulinum Type-A is toxin produced by bacteria called Clostridium Botulinum. It is given intravesically
Intravesical Botox Injections Department of Urology Patient Information What What is is Botox? Botox? Botox or Botulinum Type-A is toxin produced by bacteria called Clostridium Botulinum. It is given intravesically
WHAT TYPES OF CONTINENCE PRODUCTS ARE THERE?
 15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
15 CAN HELP MANAGE WHAT ARE? Continence products help manage the symptoms of poor bladder and bowel control. They may be used for a short time during treatment. They can also be used long term if poor
Managing Female Urinary Incontinence Within Primary Care
 Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
Managing Female Urinary Incontinence Within Primary Care Angela Patterson Lead Clinical Nurse Specialist in Bladder and Bowel Dysfunction. South Eastern HSCT Background More than 14 million in the UK affected
Disease Management. Incontinence Care. Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09
 Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
Disease Management in Incontinence Care Chan Sau Kuen Continence Nurse Consultant United Christian Hospital 14/11/09 What is incontinence? Definition of Incontinence - Is the compliant of any involuntary
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Overactive bladder. Information for patients from Urogynaecology
 Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries
 Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
Intermittent self-catheterisation (ISC) Information for patients Spinal Injuries page 2 of 12 What is clean intermittent self-catheterisation (CISC)? Urinary catheterisation is a procedure used to drain
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Overactive Bladder Syndrome
 Page 1 of 5 Overactive Bladder Syndrome Overactive bladder syndrome is common. Symptoms include an urgent feeling to go to the toilet, going to the toilet frequently, and sometimes leaking urine before
Page 1 of 5 Overactive Bladder Syndrome Overactive bladder syndrome is common. Symptoms include an urgent feeling to go to the toilet, going to the toilet frequently, and sometimes leaking urine before
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
INCONTINENCE AND OTHER UROLOGICAL DILEMMAS DR. ANNA LAWRENCE UROLOGIST AUCKLAND HOSPITAL 161 UROLOGY
 INCONTINENCE AND OTHER UROLOGICAL DILEMMAS DR. ANNA LAWRENCE UROLOGIST AUCKLAND HOSPITAL 161 UROLOGY COVERING INCONTINENCE BE ON JUST NAPPIES CATHETERS TYPES AVAILABLE AND WHEN TO USE THEM JJ STENTS???
INCONTINENCE AND OTHER UROLOGICAL DILEMMAS DR. ANNA LAWRENCE UROLOGIST AUCKLAND HOSPITAL 161 UROLOGY COVERING INCONTINENCE BE ON JUST NAPPIES CATHETERS TYPES AVAILABLE AND WHEN TO USE THEM JJ STENTS???
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors
 DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire
 Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
Intermittent Self-Catheterisation / Catheterisation Continence Advisory Service Community & Therapy Services North Lincolnshire This leaflet has been designed to give you important information about Intermittent
Please read the following information and have the child follow the bladder retraining protocol included.
 Urology Clinic Hospital for Sick Children Please read the following information and have the child follow the bladder retraining protocol included. Information on bladder retraining, urinary tract infections
Urology Clinic Hospital for Sick Children Please read the following information and have the child follow the bladder retraining protocol included. Information on bladder retraining, urinary tract infections
Information on Physical Therapy For Urogynecologic Problems
 Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Paediatric Urotherapy Training
 Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
Paediatric Urotherapy Training Frances Shit NS, MSc (Hons), ET, Dept. of Surgery, PWH, CUHK HKSAR Urinary Incontinence in Children Urine leakage in a child from 5 years of age Leakage occurs on a regular
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS
 CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS The minimum standards required to initiate specialised conservative
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS The minimum standards required to initiate specialised conservative
Neurogenic Bladder: What You Should Know. A Guide for People with Spinal Cord Injury
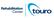 Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Overactive Bladder. When to see a doctor. Normal bladder function
 Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Appendix F: Continence Care and Bowel Management Program Training Presentation. Audience: For Front-line Staff Release Date: December 22, 2010
 Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix F: Continence Care and Bowel Management Program Training Presentation Audience: For Front-line Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
NORTHWICK PARK DEPENDENCY SCORE
 NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
Continence Promotion in
 Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Everybody s Business- Continence Promotion in Aged Care Melissa O Grady Clinical Nurse Consultant Continence Warning Some graphic images are contained in this presentation Objectives What is Old Age? What
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Implementing Clean Intermittent Catheterisation (CIC)
 Implementing Clean Intermittent Catheterisation (CIC) Julie Dicker (Spina Bifida CNC) Kids Rehab The Children s Hospital at Westmead Reasons for CIC: Neurogenic Bladder CIC is the gold standard for this
Implementing Clean Intermittent Catheterisation (CIC) Julie Dicker (Spina Bifida CNC) Kids Rehab The Children s Hospital at Westmead Reasons for CIC: Neurogenic Bladder CIC is the gold standard for this
Policy for Prostatism/Lower Urinary Tract Symptoms in men
 NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
NHS Halton Clinical Commissioning Group NHS Liverpool Clinical Commissioning Group NHS St Helens Clinical Commissioning Group NHS South Sefton Clinical Commissioning Group NHS Southport and Formby Clinical
When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women
 When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women Grace Umejei, BSN, RN, CWOC. Texas Health Presbyterian Hospital Dallas NICHE Online Connect Webinars
When Laughing is No Longer Funny Managing Transient Urinary Incontinence in Hospitalized Elderly Women Grace Umejei, BSN, RN, CWOC. Texas Health Presbyterian Hospital Dallas NICHE Online Connect Webinars
A word about incontinence
 A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Continence. Who cares and does it matter? Dr Carl Hanger Geriatrician, CDHB SI Alliance Stroke Education Day 2/11/17
 Continence. Who cares and does it matter? Dr Carl Hanger Geriatrician, CDHB SI Alliance Stroke Education Day 2/11/17 1500 pages, leading stroke experts Does it Matter? Definitely! Patient Dignity / QOL
Continence. Who cares and does it matter? Dr Carl Hanger Geriatrician, CDHB SI Alliance Stroke Education Day 2/11/17 1500 pages, leading stroke experts Does it Matter? Definitely! Patient Dignity / QOL
Stricture guide. Urology department. yeovilhospital.nhs.uk
 Stricture guide Urology department 01935 384 394 yeovilhospital.nhs.uk What is a urethral stricture? A urethral stricture is a narrowing or restriction of the urethra (the tube from your bladder through
Stricture guide Urology department 01935 384 394 yeovilhospital.nhs.uk What is a urethral stricture? A urethral stricture is a narrowing or restriction of the urethra (the tube from your bladder through
Clinical Model for IC 5
 Clinical Model for IC 5 The WHAT What is ideal clinical care for urinary incontinence? SELF-ASSESSMENT What components of ideal continence care is the hospital currently following? The HOW How can you
Clinical Model for IC 5 The WHAT What is ideal clinical care for urinary incontinence? SELF-ASSESSMENT What components of ideal continence care is the hospital currently following? The HOW How can you
Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises
 MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
Urinary Incontinence? - gør dig ikke skakmat...
 Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Urinary Incontinence? - gør dig ikke skakmat... The International Continence Society (ICS) have defined urinary incontinence as invo- luntary loss of urine to such an extent that it constitutes a social
Stress incontinence -- occurs during certain activities like coughing, sneezing, laughing, or exercise.
 Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Hydration Practices and Urinary Incontinence Care Planning
 AHRQ Safety Program for Long term Long-term Care: HAIs/CAUTI Hydration Practices and Urinary Incontinence Care Planning National Content Series for Facility Team Leads and Core Team Members September 17,
AHRQ Safety Program for Long term Long-term Care: HAIs/CAUTI Hydration Practices and Urinary Incontinence Care Planning National Content Series for Facility Team Leads and Core Team Members September 17,
December Objectives. Housekeeping Announcements
 Comprehensive Review of Regulations & Interpretive Guidance for Top F-Tags Bowel/Bladder Incontinence, Catheter, & UTI Requirements F690 Objectives 1. Identify the regulatory requirements related to Bowel/Bladder
Comprehensive Review of Regulations & Interpretive Guidance for Top F-Tags Bowel/Bladder Incontinence, Catheter, & UTI Requirements F690 Objectives 1. Identify the regulatory requirements related to Bowel/Bladder
HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY
 HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY JANE FRAHM, BS,PT,BCIA PMDB 7/7/2010 jdf,pt 1 REHABILITATION INSTITUTE OF MICHIGAN RIM PART OF COMPREHENSIVE TREATMENT PROGRAM. 7/7/2010
HOW PHYSICAL THERAPY CAN MAKE A DIFFERENCE AFTER PROSTATE SURGERY JANE FRAHM, BS,PT,BCIA PMDB 7/7/2010 jdf,pt 1 REHABILITATION INSTITUTE OF MICHIGAN RIM PART OF COMPREHENSIVE TREATMENT PROGRAM. 7/7/2010
Care Trigger Continence Management Publication code: HCR
 Care Trigger Continence Management Publication code: HCR-0312-045 Care Trigger Check list of Evidence National Care Does the care service have policies in place for: Promotion of continence that separates
Care Trigger Continence Management Publication code: HCR-0312-045 Care Trigger Check list of Evidence National Care Does the care service have policies in place for: Promotion of continence that separates
Urinary Incontinence. a problem for many
 Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
A Healthy Bladder. What to do if things go wrong.
 A Healthy Bladder What to do if things go wrong www.bladderandbowel.org Contents Introduction How the bladder works What can go wrong with the bladder? Keeping a healthy bladder What can be done to treat
A Healthy Bladder What to do if things go wrong www.bladderandbowel.org Contents Introduction How the bladder works What can go wrong with the bladder? Keeping a healthy bladder What can be done to treat
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
B l a d d e r & B o w e l C a r e. For Patients with Spinal Cord Injuries
 B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
B l a d d e r & B o w e l C a r e For Patients with Spinal Cord Injuries 1 Bladder Specific Care Intermittent Catheterization (IC) is used to empty the bladder with a catheter. A catheter is a tube that
Sacral Neuromodulation (SNM)
 47 Sacral Neuromodulation (SNM) for overactive bladder symptoms and for non-obstructive voiding dysfunction Patient Information Women and Children - Obstetrics and Gynaecology Sacro Neuromodulation Contents
47 Sacral Neuromodulation (SNM) for overactive bladder symptoms and for non-obstructive voiding dysfunction Patient Information Women and Children - Obstetrics and Gynaecology Sacro Neuromodulation Contents
Incontinence Patient Information Form
 Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Incontinence Patient Information Form (To be completed by patient) Before talking with you, the doctor would like some information about your urine leakage. These questions are important for finding out
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Appendix E: Continence Care and Bowel Management Program Training Presentation. Audience: For Registered Staff Release Date: December 22, 2010
 Appendix E: Continence Care and Bowel Management Program Training Presentation Audience: For Registered Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
Appendix E: Continence Care and Bowel Management Program Training Presentation Audience: For Registered Staff Release Date: December 22, 2010 Objectives Address individual needs and preferences with respect
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS.
 IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
IF YOU VE GOT TO GO, WE VE GOT SOLUTIONS. Get the facts about urinary incontinence and get real solutions. HENRY FORD PELVIC HEALTH & CONTINENCE CENTER HENRY FORD WOMEN S HEALTH SERVICES INCONVENIENCE?
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Urinary incontinence: the management of urinary incontinence in women
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence: the management of urinary incontinence in women 1.1 Short title Urinary incontinence 2 Background a) The National
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE BASIC ASSESSMENT & CONSERVATIVE MANAGEMENT OF BLADDER AND BOWEL SYMPTOMS
 CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE BASIC ASSESSMENT & CONSERVATIVE MANAGEMENT OF BLADDER AND BOWEL SYMPTOMS The minimum standards required to initiate a basic continence assessment of bladder
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE BASIC ASSESSMENT & CONSERVATIVE MANAGEMENT OF BLADDER AND BOWEL SYMPTOMS The minimum standards required to initiate a basic continence assessment of bladder
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN. Riette Vosloo Physiotherapist in Women s s Health
 CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider.
 Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Please complete this voiding diary and questionnaire. Bring both of them with you to your next appointment with your provider. To begin the diary, please choose two days when you will be at home. The two
Continence Management
 Dear Learner, This training guide was designed for you to complete as a selfstudy activity. Please do the following in order to ensure successful completion: First, read through EVERYTHING. There is a
Dear Learner, This training guide was designed for you to complete as a selfstudy activity. Please do the following in order to ensure successful completion: First, read through EVERYTHING. There is a
Talk about Clean Intermittent Catheterisation (CIC)
 Talk about Clean Intermittent Catheterisation (CIC) Where does urine (wee) come from? Urine (wee) is made in the kidneys. We each have two kidneys. Each kidney has a little tube that connects to the bladder.
Talk about Clean Intermittent Catheterisation (CIC) Where does urine (wee) come from? Urine (wee) is made in the kidneys. We each have two kidneys. Each kidney has a little tube that connects to the bladder.
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Updates in the nonpharmacological. treatment on overactive bladder
 Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
Oxford Pelvic Floor Services A guide to the pelvic floor muscles. Information for men
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
SECTION H: BLADDER AND BOWEL. H0100: Appliances. Item Rationale Health-related Quality of Life. Planning for Care
 SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
OHTAC Recommendation
 OHTAC Recommendation Sacral Nerve Stimulation for the Management of Urge Incontinence, Urgency-Frequency, Urinary Retention and Fecal Incontinence March 2, 2005 1 The Ontario Health Technology Advisory
OHTAC Recommendation Sacral Nerve Stimulation for the Management of Urge Incontinence, Urgency-Frequency, Urinary Retention and Fecal Incontinence March 2, 2005 1 The Ontario Health Technology Advisory
Incontinence. Urinary. In Adults. THIS PUBLICATION IS OUT OF DATE. For most current information:
 Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
Urinary Incontinence In Adults A Patient's Guide r I When you eat and drink, your body absorbs the liquid. The kidneys filter out waste products from the body fluids and make urine. Urine travels down
encathopedia Volume 7 PARKINSON S AND THE BLADDER
 encathopedia Volume 7 PARKINSON S AND THE BLADDER Parkinson s disease Parkinson s is a progressive neurological condition. In people with Parkinson s, some of the brain cells that create the chemical dopamine
encathopedia Volume 7 PARKINSON S AND THE BLADDER Parkinson s disease Parkinson s is a progressive neurological condition. In people with Parkinson s, some of the brain cells that create the chemical dopamine
