Ch 28 Lecture Study Guide
|
|
|
- Miranda Blair
- 5 years ago
- Views:
Transcription
1 Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports male and female reproductive cells (gametes) Produces reproductive hormones 2. In what way are the male and female reproductive systems very different? Female produces 1 gamete/month Retains and nurtures zygote Male produces large quantities of gametes 500M/day! Begins at puberty and continues past age What do the male gonads (testes) produce? Produce male gametes (spermatozoa, sperm) Produce hormones Male sex hormones (androgens, primarily testosterone) Inhibin 4. What is emission? Movement of mature spermatozoa move through male duct system, are mixed with secretions of accessory glands 5. What is semen? Sperm mixed with accessory gland secretions 6. What are the female gonads (ovaries) responsible for? Release 1 immature gamete (oocyte) each month Produce hormones Female sex hormones (estrogens, progestins) Inhibin 7. The uterine tube carries the oocyte to the uterus.
2 8. What happens if sperm reaches the oocyte in the uterine tube? Fertilization is initiated Oocyte matures into ovum 9. During sexual intercourse, ejaculation introduces ejaculation into the vagina. 10. What are the general course of events that occur in human reproduction once semen is introduced into the vagina? 1. Spermatozoa ascend female reproductive tract Seek out oocyte (generates heat, attracts sperm like heat seeking missile) 2. If fertilization occurs in uterine tube: sperm + ovum zygote 3. Zygote travels to uterus 4. Uterus encloses/supports developing embryo 5. Embryo grows into fetus and prepares for birth 11. Define gamete. Reproductive cells (spermatozoa or oocyte) that contain half the normal chromosome complement 12. Define gametogenesis. Formation of gametes 13. A female gamete is called an oocyte and is produced during development (before birth). 14. A male gamete is called a spermatozoa (sperm) and is produced during lifetime (begins at puberty and continues past age In males and females, gametogenesis involves mitosis and meiosis. 16. What is mitosis? What does it produce? Process of somatic cell division Produces 2 diploid daughter cells Have same number of (paired) chromosomes as parent cell, i.e., 46 (23 x 2)
3 17. What is meiosis? What does it produce? reduction division Special cell division involved in gamete production Produces 2 haploid daughter cells Have one half (unpaired) the number of chromosomes in the parent cell, i.e., When does mitosis occur? What is mitosis not limited to? Mitosis occurs during division of somatic (body) cells and is not limited to gametogenesis 19. Meiosis is only involved in the production of sex cells. 20. What does meiosis involve? Involves two cycles of cell division Chromosomes (each with two chromatids) pair up = tetrad During first division, tetrads split During second division, chromatids split 21. What does meiosis produce? Produces gametes with one half the number of chromosomes, i.e., Why is it okay that meiosis produces gametes with one half the normal number of chromosomes? Fusion of male gamete (sperm) and female gamete (oocyte) produces cell with correct number of chromosomes (diploid), i.e., 46 (23 from each parent) 23. What does each process of gametogenesis in males produce? (Gametogenesis begins with stem cells called spermatogonium). Mitotic division produces Primary spermatocyte + stem cell Meiosis I produces Secondary spermatocyte Meiosis II produces Spermatid (undifferentiated male gametes Spermiogenesis produces Spermatozoa (sperm)
4 24. What does each process of gametogenesis in females produce? (Gametogenesis begins with stem cells called oogonium). Mitotic division produces Primary oocyte Meiosis I produces Secondary oocyte + polar body Meiosis II produces Ovum + polar body (after fertilization) Spermiogenesis produces N/A females do not produce sperm 25. Define spermatogenesis. Process of spermatozoa (sperm) development 26. What 3 integrated processes are involved in spermatogenesis? 1. Mitosis 2. Meiosis 3. Spermiogenesis 27. Where does spermatogenesis occur? Occurs in seminiferous tubules (ST) in testes 28. Briefly describe what occurs during mitosis in spermatogenesis. Spermatogonium (stem cell) spermatogonium + primary spermatocyte Primary spermatocyte pushed toward lumen of ST On going throughout lifetime 29. Briefly describe what occurs during meiosis in spermatogenesis. Primary spermatocyte first division secondary spermatocytes second division spermatids = undifferentiated male gametes Each primary spermatocyte 4 spermatids 30. Define spermiogenesis. Last stage of spermatogenesis Begins with spermatids small, relatively unspecialized cells Physical maturation of spermatids Involves major structural changes Differentiate into mature spermatozoa Highly specialized cells
5 31. Define spermiation. When spermatozoa: Detach from Sertoli cells Enter lumen of ST 32. How long does it take from spermatogonium to spermiation? From spermatogonium to spermiation in 9 weeks 33. Matching: YOU WILL USE THE SOME CHOICES BELOW MORE THAN ONCE. B Flagellum; provides motility A. Testosterone D Nurse cells B. Tail of spermatozoon A Maintains accessory glands and organs C. Middle piece of spermatozoon G Contains enzymes to dissolve oocyte wall D. Sustentacular cells F Large cells in interstitial spaces between ST E. Head of spermatozoon A Stimulates metabolism, esp. protein synthesis (m. growth) F. Interstitial (Leydig) cells A Stimulates spermatogenesis and spermatozoa maturation G. Acrosomal cap of spermatozoon D Extend between other cells from ST capsule to lumen H. Spermatozoon C Contains mitochondria for energy to move tail A Secreted by Interstitial (Leydig) cells F Stimulated by LH to produce androgens H Has no energy reserves; uses nutrients from surrounding fluids A Affects CNS, including libido (sex drive) F Responsible for production of androgens E Nucleus with chromosomes (DNA) D Sertoli cells A Establishes/maintains secondary sex characteristics D Surround developing spermatocytes & spermatids in ST H Loses all other organelles to make light weight 34. What are the interstitial (Leydig) cells? Large cells in interstitial spaces between ST responsible for the production of the androgen, testosterone. 35. List the functions of testosterone. 1. Stimulates spermatogenesis and spermatozoa maturation 2. Affects CNS, including libido (sexual drive) 3. Stimulates metabolism, especially protein synthesis, muscle growth 4. Establishes/maintains secondary sex characteristics, e.g., facial hair 5. Maintains male accessory glands and organs
6 36. What are the sustentacular cells? List AKAs. Nurse cells /Sertoli cells Extend between other cells from ST capsule to lumen Surround developing spermatocytes and spermatids in ST 37. List the 6 major functions of the sustentacular cells and briefly describe each. 1. Maintain blood testis barrier Cells joined by tight junctions Isolates STs 2. Support mitosis and meiosis Cells stimulated by FSH (and presence of T) Promote spermatogenesis 3. Support spermiogenesis Provide nutrients for development Phagocytize cytoplasm shed by spermatids 4. Produce inhibin Stimulated by factors released by developing spermatozoa Provides feedback control of spermatogenesis Inhibits (decreases) production of FSH by AP 5. Produce androgen binding protein (ABP) Stimulated by FSH Binds T in ST fluid, elevates levels 6. Secrete Mullerian inhibiting factor (MIF) Causes regression of fetal ducts that form uterine tubes and uterus 38. What are the functions of the epididymis? Monitors and adjusts composition of ST fluid Recycles damaged spermatozoa Stores/protects spermatozoa and facilitates functional maturation 39. Why is the epididymis important to the survival of spermatozoa? Spermatozoa in ST functionally immature Incapable of fertilization or locomotion Become mature in epididymis (but not motile)
7 40. What must a spermatozoa undergo to become motile? Explain. To become motile, spermatozoa must undergo capacitation Become motile when mixed with seminal vesicle fluid Capable of successful fertilization when exposed to female reproductive tract 41. What does capacitation mean? Sperm maturation 42. What are the functions of the ductus deferens? List any AKAs. Transport spermatozoa from epididymis to urethra Store spermatozoa (several months) In state of suspended animation Low metabolic rates 43. What is seminal fluid? Which accessory glands contribute to the production of seminal fluid? How much does each accessory gland contribute? A mixture of secretions from several glands including: Seminal vesicles (60%) Prostate gland (20 30%) Bulbourethral glands (10 20%) 44. List the accessory glands of the male reproductive system. 1. Seminal vesicles 2. Prostate gland 3. Bulbourethral glands 45. What do the secretions of the seminal vesicles contain? 1. High concentrations of fructose (easily metabolized by spermatozoa) 2. Prostaglandins stimulate smooth muscle contractions in male and female reproductive tracts 3. Fibrinogen forms temporary clot in vagina after ejaculation (seminal plug) 46. What is the primary source of energy for spermatozoa? Fructose
8 47. What effect do secretions from the seminal vesicles have on functional spermatozoa? Secretions make functional spermatozoa motile (flagella begins beating) 48. When are secretions from the seminal vesicles discharged into the ejaculatory duct? Secretions discharged into ejaculatory duct at emission (due to contractions in ductus deferens, SVs, and prostate gland) 49. What does the prostate gland produce? Into what is it ejected? Produces prostatic fluid, which contains seminalplasmin = antibiotic that may help prevent urinary tract infections Ejected into prostatic urethra 50. What are the bulbourethral glands? List any AKAs. What functions do their secretions perform? Mucous glands Secretions Help neutralize urinary acids remaining in urethra Lubricate glans (tip of) penis 51. Define ejaculate. The volume of fluid released at ejaculation (usually 2 5 ml of semen) 52. What does the fluid, semen contain/what are the components of semen? 1. Spermatozoa Sperm count = million/ml semen (ideally > 60 million/ejaculate) 2. Seminal fluid = mixture of glandular secretions from: SV (60%) Prostate (30%) Bulbourethral glands (5%) Sustentacular cells and epididymis (5%) 3. Enzymes Protease helps dissolve vaginal mucous secretions Seminalplasmin (from prostate) Prostatic enzyme converts fibrinogen to fibrin after ejaculation Fibrinolysin liquefies clotted semen
9 53. Explain the role that the hypothalamus plays in the male reproductive system. Hypothalamus GnRH ant pit Ant pit LH (ICSH) interstitial (Leydig) Cells testosterone (T) FSH Testosterone + FSH sustentacular cells Synthesis of ABP (Androgen binding protein binds androgens, primarily testosterone, in the fluid contents of the STs. Thought to be important in elevating concentration of androgens within the STs and stimulating spermatogenesis) Stimulation of spermatogenesis and spermiogenesis 54. How do the sustentacular cells (the target cells of FSH) regulate the production of FSH? Factors released by developing spermatozoa sustentacular cells inhibin inhibits (decreases) FSH production by AP 55. List the physiological effects of testosterone. 1. Stimulates spermatogenesis (with FSH) 2. Maintains male accessory glands and organs 3. Establishes/maintains secondary sex characteristics 4. Stimulates anabolic metabolism, especially bone and muscle growth, RBC formation 5. On CNS, including libido (sexual drive) 56. In males, why is there an narrow range of plasma FSH, LH and testosterone? In males, GnRH pulse frequency relatively steady narrow range of plasma FSH, LH, T 57. As testosterone secretion accelerates at puberty, what happens? T secretion accelerates at puberty Sexual maturation Appearance of secondary sex characteristics 58. How is testosterone production controlled? Negative feedback controls T production Inc T inhibits release of GnRH dec LH dec T 59. List the functions of the female reproductive system. 1. Produces gametes and reproductive hormones 2. Protects and supports developing embryo 3. Nourishes newborn infant
10 60. Define and describe oogenesis. Ovum production 61. Compare oogenesis to spermatogenesis. Before birth Mitotic divisions complete Oogonia (stem cells) primary oocytes (vs. ongoing throughout lifetime in males) Primary oocytes begin meiosis I Cytoplasm of oocyte unevenly distributed during 2 meiotic divisions; produces: One functional ovum (with most of original cytoplasm) 2 3 polar bodies = nonfunctional cells that later disintegrate (vs. primary spermatocyte 4 spermatozoa) Ovary releases secondary oocyte instead of mature ovum Meiosis not completed unless/until fertilization 62. List the characteristics of primary oocytes. Are daughter cells of oogonia (stem cells) Located in ovarian cortex in clusters (egg nests) Surrounded by follicle cells = primordial follicle 2 M primary oocytes at birth Meiosis I (primary oocyte secondary oocyte) Begins during fetal development Stops early in meiosis I (suspended development) Doesn t continue until after puberty (numbers reduced to 400,000 due to atresia) 63. What generally occurs during the ovarian cycle? 1. Formation of primary follicles 2. Formation of secondary follicles 3. Formation of tertiary follicle 4. Ovulation 5. Formation of corpus luteum 6. Formation of corpus albicans 64. When does the ovarian cycle begin? Why? Begins after puberty when groups of primordial follicles develop into primary follicles each month Process begins due to increased FSH at puberty
11 65. What are the 2 phases of the ovarian cycle? Involves 2 phases Follicular (preovulatory) phase Luteal (postovulatory) phase 66. What generally occurs during the follicular phase of the ovarian cycle? List aka for follicular phase. Aka: preovulatory phase Formation of primary follicles Formation of secondary follicles Formation of tertiary follicle primary oocyte completes meiosis I (just before ovulation) Primary oocyte undergoes (meiotic division) producing secondary oocyte and polar body Secondary oocyte enters meiosis II Secondary oocyte and surrounding granulosa cells lose connections with follicular wall 67. What occurs in the formation of primary follicles in the follicular phase? Every month AP FSH some primordial follicles (with primary oocyte) primary follicles (with primary oocyte) 68. What is the zona pellucida? Glycoprotein layer around primary oocyte 69. What are granulosa cells? Rounded, larger follicle cells outside zona pellucida 70. What are thecal cells? Layer of follicle cells adjacent to ovarian stroma 71. What do the granulosa and thecal cells work together to produce? Estrogen (continues in all follicles) 72. What happens during the formation of secondary follicles during the follicular phase? Each month, only a few (1 3) primary follicles become secondary follicles Primary oocyte increases in size Follicle wall thickens Granulosa cells secrete follicular fluid Follicle enlarges rapidly as follicular fluid accumulates
12 73. What happens during the formation of tertiary follicles during the follicular phase? 8 10 th day after start of ovarian cycle, ovaries usually contain 1 secondary follicle On th day, forms large tertiary (Graafian) follicle Tertiary follicle spans cortex bulge on surface of ovary Oocyte projects into antrum (central chamber of follicle) 74. What happens at the end of tertiary follicle development? Increasing LH causes the primary oocyte to Complete meiosis I (just before ovulation) Primary oocyte (meiotic division) secondary oocyte and polar body 75. What happens when a secondary oocyte enters meiosis II? Meiosis stops and is not completed unless fertilization occurs 76. What happens on day 14 of a 28 day cycle? Day 14 (of 28 day cycle), secondary oocyte and surrounding granulosa cells (corona radiata) lose connections with follicular wall (in preparation for ovulation) 77. What occurs during ovulation? 1. Tertiary follicle (ovarian) wall ruptures 2. Secondary oocyte released into pelvic cavity 3. Sticky follicular fluid keeps corona radiata attached to ovary surface Comes in contact with fimbriae, or Fluid currents transfer secondary oocyte to uterine tube 4. Marks end of ovarian follicular phase and start of luteal phase 78. What generally occurs during the luteal phase of the ovarian cycle? List aka for luteal phase. Aka: Postovulatory phase Formation and degeneration of corpus luteum (CL) 79. What does the luteal phase involve? Involves formation and degeneration of corpus luteum (CL) Empty tertiary follicle collapses, ruptured blood vessels leak into antrum corpus hemorrhagicum (bloody body) LH stimulates remaining granulosa cells proliferate corpus luteum (CL, yellow body)
13 80. What does the corpus luteum (CL) produce? Progesterone = principle ovarian hormone after ovulation Small amount of estrogen (principle hormone before ovulation) 81. What is the primary function of progesterone? What does progesterone stimulate? Primary function is to prepare uterus for pregnancy Stimulates: Development of uterine lining (endometrium) Secretions of uterine glands 82. Describe what happens in the absence of fertilization. CL begins to degenerate 12 days after ovulation Estrogen and progesterone levels fall Fibroblasts invade corpus luteum corpus albicans (white body) Disintegration (involution) of corpus luteum marks end of ovarian cycle FSH new cycle and new follicular phase Another group of primordial follicles form primary follicles 83. Describe the uterine tube. A hollw muscular tube lined with mucosal membrane that produces mucus. The mucosa is surrounded by layers of smooth muscle 84. The oocyte is transported from the infundibulum to the uterine cavity, which normally takes 3 4 days. 85. Secondary oocyte transport involves ciliary movements and peristaltic contractions. 86. Where does fertilization occur and when must it happen? Occurs near boundary between ampulla and isthmus Must happen during first hours 87. What is the nutrient supply for the spermatozoa and developing oocyte? Lipids and glycogen
14 88. What is the function of the uterine wall? Provides for developing embryo (weeks 1 8) and fetus (week 9 through delivery) with: Protection Nutritional support Waste removal 89. List the 3 layers of the uterine wall. 1. Perimetrium 2. Myometrium 3. Endometrium 90. Describe the Perimetrium. Serous membrane that covers outer surface of uterus Continuous with peritoneal lining of abdominopelvic cavity 91. Describe the Myometrium. Thick layers of smooth muscle Longitudinal, circular, oblique layers Provides force needed to move fetus out of uterus and into vagina Arteries Arcuate radial arteries (in myometrium) straight spiral (endometrium) 92. Describe the Endometrium. Thin glandular, vascular layer Lines surface of uterine cavity Supports physiological demands of (potential) fetus Under influence of estrogen Uterine glands, blood vessels, and epithelium change with phases of monthly uterine cycle Has 2 zones 93. What are the 2 zones of the endometrium? 1. Basilar 2. Functional
15 94. Describe the basilar zone of the uterine wall. Outer zone, adjacent to myometrium Attaches endometrium to myometrium Contains Terminal branches of uterine glands Straight arteries Structure remains constant over time 95. Describe the functional zone of the uterine wall. Closest to uterine cavity; thickest Contains most of uterine glands Blood supply provided by spiral arteries Undergoes cyclical changes in response to sex hormones Degeneration, sloughing menses 96. What is the uterine/endometrial (menstrual) cycle? Repeating series of changes in structure of endometrium that occur in response to the ovarian hormones (E and P) and whose average length is 28 days (range 21 35) 97. What are the 3 phases of the uterine/endometrial cycle and when does each occur? 1. Menses occurs during early follicular phase of ovarian cycle 2. Proliferative phase occurs during later follicular phase of ovarian cycle 3. Secretory phase corresponds to luteal phase of ovarian cycle 98. What does menses mark the beginning of? Marks beginning of uterine cycle (Day 1) 99. Define menses. Degeneration and loss of entire functional zone of endometrium where blood cells and degenerated tissues break away and enter uterine lumen, vagina 100. What causes the degeneration and loss of the entire functional zone of the Endometrium? Caused by constriction of spiral arteries reduced blood flow to endometrium no O2 or nutrients Secretory glands deteriorate Arterial walls rupture
16 101. What is menstruation? How long does it last? How much blood is lost during menstruation? endometrial sloughing Lasts 1 7 days Lose small amount of blood (35 50 ml) 102. What is dysmenorrheal? What is its cause(s)? Painful menstruation Due to uterine inflammation and contraction (due to prostaglandins) Other conditions of pelvic structures 103. Describe the proliferative phase of the uterine (menstrual) cycle. After menses (Days 8 14) Increase in basilar uterine gland cells Further growth and vascularization restoration of functional zone Occurs at same time as enlargement of primary and secondary follicles in ovary (follicular phase) Phase stimulated and sustained by E from ovarian follicles 104. Describe the secretory phase of the uterine (menstrual) cycle. Begins at ovulation (Day 14) Lasts as long as CL (14 days) Occurs in response to CL P and E Endometrial glands enlarge Arteries elongate and spiral through functional zone Secretory activities peak 12 days after ovulation CL stops producing P and E Glandular activity declines over next 1 2 days Uterine cycle ends (Day 28, 14 days after ovulation) 105. A new menses cycle (day 1) begins with the disintegration of the functional zone followed by menses When does ovulation occur? Day What is menarche? First uterine cycle at puberty (approx age 11 12)
17 108. What does amenorrhea mean? List the 2 types. Amenorrhea = no menses 2 types: Primary amenorrhea Secondary amenorrhea 109. What is primary amenorrhea? What is it caused by? Failure to initiate menses; no menarche Caused by: Developmental abnormalities (e.g. nonfunctional ovaries, absence of uterus) Endocrine or genetic disorder Malnutrition 110. What is secondary amenorrhea? What is it caused by? Menses interrupted for > 6 months Caused by: Physical stresses (e.g., drastic weight loss, anorexia nervosa, intensive physical training (marathon runners)) Emotional stresses (e.g., severe depression, grief) 111. The female reproductive tract is under the control of the pituitary and the ovaries The female reproductive tract is more complicated than in males because both ovarian and uterine cycles have to be coordinated. If they are not coordinated, what happens and why? If not coordinated, infertility results: Uterus normal but do not ovulate Ovulate but uterus abnormal 113. Explain the role that the hypothalamus plays in the female reproductive system. GnRH from Hth regulates reproductive function in females (like males) But, GnRH amount and release frequency changes throughout ovarian cycle (constant in males) GnRH FSH and/or LH depending on pulse frequency and amount secreted Change in GnRH controlled by estrogen and progesterone
18 114. In the female reproductive system, how is the role of GnRH similar to and different than its role in the male reproductive tract? 1. GnRh amount and release frequency varies during ovarian cycle in females, it is constant in males 2. GnRh pulse frequency variable in women, so FSH and LH secretion varies, it is constant in males 3. Similarity: GnRH stimulates FSH secretion and LH synthesis in males and females 115. FSH stimulates the monthly development of monthly development of some primordial follicles into primary follicles What is the function of FSH females and males? Females promotes egg and follicle development in ovaries Males promotes sperm development in testes (STs) 117. What happens to FSH levels as secondary follicles develop? As secondary follicles develop, FSH decreases due to negative feedback effects of inhibin (produced by granulosa cells) 118. As follicular development /maturation continues it is supported by FSH, estrogen and LH What two types of cells work together to produce estrogens? Follicle and thecal cells 120. What are the follicle cells around the oocyte in the ovary responsible for? The production of estrogen and inhibin 121. What is the dominant hormone prior to ovulation? Estrogens (E) 122. What happens to the estrogen levels as the tertiary follicle begins forming? Estrogens rise sharply as tertiary follicle begins forming
19 123. List the physiological effects of estrogen. 1. Stimulates endometrial growth and secretion 2. Maintains accessory glands and organs 3. Establishes/maintains female secondary sex characteristics Body hair distribution, fat deposits 4. Stimulates bone and muscle growth 5. Affects CNS (esp. Hth E inc sex drive) 124. A sudden surge of LH is released in response to high estrogen levels What does a sudden surge in LH trigger? Sudden surge triggers: Completion of meiosis I by primary oocyte (in tertiary follicle) secondary oocyte Rupture of follicular wall Ovulation (9 hours after LH peak) 126. What does LH promote in females? Ovarian secretion of progesterone 127. What does LH promote in males? Testicular secretion of testosterone 128. By what ovarian structure is progesterone secreted and what is it secreted in response to? Secreted by CL in response to LH peak 129. What is the dominant hormone after ovulation? Progesterone is the dominant hormone after ovulation (as P inc, E dec) 130. What is the primary function of progesterone in female reproduction? To prepare uterus for possible pregnancy
20 131. What happens to the progesterone levels at and after LH reaches its peak? Increases endometrium functional zone Growth Secretion Blood supply Remains high for 7 days Declines as CL degenerates (when pregnancy doesn t occur) Decreased P and E initiates menses and increasing GnRH stimulates FSH, etc Inhibin is secreted by follicular cells and inhibits FSH production and secretion (causes a of FSH and possible GnRH in both males and females) What is the relationship between hormones and body temperature? Monthly hormonal fluctuations affect core body temperature Basal body temp lower during follicular phase, when E dominant hormone Decreases basal body temperature (BBT) at ovulation Large increase during luteal phase, when P dominates Use to plan/avoid fertilization 134. What coordinates sexual function? Coordinated by complex neural reflexes 135. In order for the male reproductive system to function successfully, what must occur? Sperm count must be adequate Semen must have correct ph and nutrients Erection and ejaculation must function properly 136. What is impotence? The inability to achieve or maintain an erection 137. In order for the female reproductive system to function successfully, what must occur? Ovarian and uterine cycles must coordinate properly Ovulation and oocyte transport must occur normally Environment of reproductive tract must support: Survival and movement of sperm Fertilization of oocyte Maintenance of pregnancy Embryonic and fetal development
21 138. What must the environment of the reproductive tract support so that the function of the female reproductive tract is successful? 1. Survival and movement of sperm 2. Fertilization of oocyte 3. Maintenance of pregnancy 4. Embryonic and fetal development 139. List characteristics of menopause. Occurs at age Time when ovulation and menstruation cease No primordial follicles left to respond to FSH E and P decrease GnRH, FSH, LH increase Accompanied by variety of physiological effects (p ) 140. List characteristics of male climacteric (andropause) Occurs at age Period of declining reproductive function T decreases FSH and LH increase Sperm production continues (into 80s) but sex drive reduced
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
The Reproductive System
 Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Physiology of Male Reproductive System
 Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
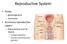 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Lecture 28, The Reproductive System
 Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
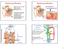 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
9.4 Regulating the Reproductive System
 9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Chapter 27 The Reproductive System. MDufilho
 Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
The reproductive lifespan
 The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
Chapter 46 ~ Animal Reproduction
 Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Reproductive Hormones
 Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Chapter 36 Active Reading Guide Reproduction and Development
 Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
 MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
The Male Reproductive System
 The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
Biology of Reproduction- Zool 346 Exam 2
 Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY
 Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
10.7 The Reproductive Hormones
 10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
FIGURE The tunica albuginea is a connective tissue capsule forming the outer part of each testis.
 Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
CASE 41. What is the pathophysiologic cause of her amenorrhea? Which cells in the ovary secrete estrogen?
 CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
Web Activity: Simulation Structures of the Female Reproductive System
 differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
Embryology Lecture # 4
 1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal
 What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
to ensure the. Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion of.
 The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
Reproduction and Development. Female Reproductive System
 Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
Human Reproductive Anatomy The female anatomy first just the reproductive parts:
 Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Reproductive Systems. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
The Reproductive System
 The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System
 A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Gametogenesis. Omne vivum ex ovo All living things come from eggs.
 Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Omne vivum ex ovo All living things come from eggs. William Harvery, 1651 Gametogenesis This lecture is the preface, so to speak, to embryology; that is, it introduces the development of the specialized
Male Reproductive System
 Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
AP Biology Ch ANIMAL REPRODUCTION. Using only what you already know (you cannot look up anything) complete the chart below.
 AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
11/15/2017. Reproductive System. Anatomy of Male Reproductive System. Reproductive Organs of the Male, Sagittal View
 Reproductive System What is sex? Biological science perspective Primary sex organs (gonads): testes and ovaries Produce gametes (sex cells): sperm and ova Secrete steroid sex hormones Androgens (males)
Reproductive System What is sex? Biological science perspective Primary sex organs (gonads): testes and ovaries Produce gametes (sex cells): sperm and ova Secrete steroid sex hormones Androgens (males)
Special Parts: Gender. Why Have Sex?
 Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
2 - male hormones/ female system
 2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23
 AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
BIOL 2402 Reproductive Systems!
 Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Endocrine and Reproductive Systems. Chapter 39: Biology II
 Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Health Science: the structures & functions of the reproductive system
 Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM
 Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
Female Reproductive System. Lesson 10
 Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
Female Reproductive System
 Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5)
 IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
Human Reproduction. Human Reproductive System. Scrotum. Male Reproductive System
 Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Mohammad Sha ban. Basheq Jehad. Hamzah Nakhleh
 11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
Animal Reproduction Chapter 46. Fission. Budding. Parthenogenesis. Fragmentation 11/27/2017
 Animal Reproduction Chapter 46 Both asexual and sexual reproduction occur in the animal kingdom Sexual reproduction is the creation of an offspring by fusion of a male gamete (sperm) and female gamete
Animal Reproduction Chapter 46 Both asexual and sexual reproduction occur in the animal kingdom Sexual reproduction is the creation of an offspring by fusion of a male gamete (sperm) and female gamete
Hormonal Control of Human Reproduction
 Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara
 Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM
 Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Cell Divisions. The autosomes represent the whole body. * Male Sex Chromosomes: XY * Female Sex Chromosomes: XX
 Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Chapter 2. Reproductive system matures and becomes capable of reproduction
 Chapter 2 Human Reproductive Anatomy and Physiology Key Terms Embryo Menarche Menopause Oxytocin Ovum Prostate gland Puberty Smegma zygote Puberty Involves changes in the whole body and psyche Reproductive
Chapter 2 Human Reproductive Anatomy and Physiology Key Terms Embryo Menarche Menopause Oxytocin Ovum Prostate gland Puberty Smegma zygote Puberty Involves changes in the whole body and psyche Reproductive
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
