11/15/2017. Reproductive System. Anatomy of Male Reproductive System. Reproductive Organs of the Male, Sagittal View
|
|
|
- Reynard Mathews
- 5 years ago
- Views:
Transcription
1 Reproductive System What is sex? Biological science perspective Primary sex organs (gonads): testes and ovaries Produce gametes (sex cells): sperm and ova Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive organs: Internal ducts and glands external genitalia including copulatory organs Anatomy of Male Reproductive System Testes: sperm-producing male gonads that lie within the scrotum Sperm is delivered to body through system of ducts: epididymis, ductus (vas) deferens, ejaculatory duct, and urethra Accessory sex glands: seminal glands, prostate, and bulbo-urethral glands Reproductive Organs of the Male, Sagittal View Scrotum Sac of skin and superficial fascia outside abdominopelvic cavity Contains paired testes 3 C lower than core body temperature necessary for sperm production Midline septum divides scrotum into two compartments, one for each testis 1
2 Testis, Scrotum and Spermatic Cord Spermatic cord encloses nerve fibers, blood vessels, and lymphatics that supply testes The Testes Each testis is surrounded by tunica vaginalis and tunica albuginea Septa divide testis into ~250 lobules, each containing one to four seminiferous tubules Interstitial endocrine cells: located in soft tissue surrounding seminiferous tubules Produce androgens, such as testosterone Secrete it into interstitial fluid Myoid cells surround each seminiferous tubule Smooth muscle like cells that may squeeze sperm and testicular fluids out of testes Structure of the Testis Sperm is conveyed from seminiferous tubules to straight tubule to rete testis to efferent ductules to epididymis Sperm are stored in tail of epididymis until ejaculation 2
3 Structure of the Testis Male Reproductive Structures Male Duct System Ducts carry sperm from testes to body exterior Epididymis Ductus deferens formerly known as vas deferens Ejaculatory duct Urethra 3
4 Epididymis Duct of the epididymis is ~ 6 m in length Microvilli (stereocilia) absorb testicular fluid and pass nutrients to stored sperm Nonmotile sperm enter, pass slowly through (~ 20 days), become motile Can be stored several months During ejaculation, epididymis contracts, expelling sperm into ductus deferens Ductus Deferens and Ejaculatory Duct Ductus deferens (vas deferens) ~ 45 cm long Passes through inguinal canal to pelvic cavity Expands to form ampulla Joins duct of seminal vesicle to form ejaculatory duct Smooth muscle in walls propels sperm from epididymis to urethra Vasectomy: cutting and ligating ductus deferens Nearly 100% effective form of birth control Urethra Conveys both urine and semen (at different times) Has three regions Prostatic urethra: surrounded by prostate Intermediate part of the urethra (membranous urethra): in urogenital diaphragm Spongy urethra: runs through penis; opens at external urethral orifice 4
5 Male Accessory Glands Seminal glands or seminal vesicles On posterior bladder surface Contains smooth muscle that contracts during ejaculation Produces viscous alkaline seminal fluid Fructose, citric acid, coagulating enzyme (vesiculase), and prostaglandins Comprises 70% volume of semen Duct of seminal gland joins ductus deferens to form ejaculatory duct Bulbo-urethral glands Pea-sized glands inferior to prostate Produce thick, clear mucus during sexual arousal Lubricate urethra and glans penis Neutralize traces of acidic urine in urethra Male Accessory Glands Prostate Encircles urethra inferior to bladder Size of peach pit Consists of smooth muscle that contracts during ejaculation Secretes milky, slightly acid fluid Contains citrate, enzymes, and prostate-specific antigen (PSA) Plays a role in sperm activation Enters prostatic urethra during ejaculation Makes up one-third of semen volume Semen (1 of 2) Milky-white mixture of sperm and accessory gland secretions 2 5 ml semen are ejaculated containing million sperm/ml Contains fructose for ATP production, protects and activates sperm, and facilitates sperm movement Alkaline fluid neutralizes acidity of male urethra and female vagina and enhances motility 5
6 Semen (2 of 2) Characteristics of semen Contain prostaglandins that decrease viscosity of mucus in cervix and stimulate reverse peristalsis in uterus Contains the hormone relaxin and other enzymes that enhance sperm motility Contains ATP for energy Can suppress female immune response Antibiotic chemicals destroy some bacteria Clotting factors coagulate semen initially to prevent draining out, then liquefy it by fibrinolysin so sperm can finish journey Cell Division in Body Cells: Mitosis Chromosome number 23 HOMOLOGOUS pairs for total of 46 diploid condition Chromosome number unaffected by cell division mother and daughter cells have the same number Increases number of body cells (development) or regenerates tissues (throughout life) Cell Division and the Production of Gametes: Meiosis Gamete formation involves meiosis, which differs from mitosis Involves two consecutive cell divisions (meiosis I and II), but only one round of DNA replication Produces four daughter cells Functions of meiosis Number of chromosomes are cut in half (2n to n) Diploid mother cells to haploid sex cells Prepare for union of two haploid gametes into one diploid zygote Introduces genetic diversity 6
7 Followed by growth and development of daughter cells into mature cells Independent Assortment of Homologous Chromosomes in Meiosis Supporting Genetic Diversity Introduces genetic variability Random alignment of homologous pairs in meiosis I leads to variability of gametes Crossover variability of gametes (not shown) Results in no two gametes being exactly alike All are different from original mother cells 7
8 Spermatogenesis Reminder: most body cells have 46 chromosomes: Two sets (23 pairs) of chromosomes One maternal, one paternal: homologous chromosomes Referred to as diploid chromosomal number (2n) Gametes have only 23 chromosomes: haploid chromosomal number (n) Only one member of homologous pair Occurs in seminiferous tubules of testis beginning at puberty Spermatogenic cells give rise to sperm Spermatogenesis Spermiogenesis: Transformation of a Spermatid into a Functional Sperm Major regions of sperm: Head: genetic region that includes nucleus and helmetlike acrosome containing hydrolytic enzymes that enable sperm to penetrate egg Midpiece: metabolic region containing mitochondria that produce ATP to move tail Tail: locomotor region that includes flagellum 8
9 Spermatogenesis: Summary of Events in the Seminiferous Tubules Role of sustentocytes (also called Sertoli cells) Extend through wall of tubule and surround developing cells Provide nutrients and signals to dividing cells Move cells along to lumen Secrete testicular fluid into lumen for sperm transport Phagocytize faulty germ cells and excess cytoplasm Produce chemical mediators to regulate spermatogenesis Tight junctions that divide tubule into two compartments and form blood testis barrier Basal compartment: area where spermatogonia and primary spermatocytes are located Adluminal compartment: area where meiotically active cells and tubule lumen are located Hormonal Regulation of Testicular Function, the Hypothalamic-Pituitary- Gonadal (HPG) Axis 1. Hypothalamus releases GnRH 2. GnRH binds to anterior pituitary gonadotropic cells stimulating FSH and LH release 3. FSH stimulates sustentocytes to release androgen-binding protein (ABP) ABP keeps concentration of testosterone high near spermatogenic cells, promoting spermatogenesis 4. LH binds to interstitial endocrine cells, prodding them to secrete testosterone 5. Testosterone entering blood stimulates sex organ maturation, secondary sex characteristics, and libido 6. Rising testosterone levels negative feed back on GnRH and on pituitary 7. Inhibin: released by sustenocytes when sperm count high; inhibits GnRH and FSH release The Hypothalamic-Pituitary-Gonadal (HPG) Axis Amount of testosterone and sperm produced by testes reflects balance among three interacting sets of hormones Balance takes 3 years to achieve, after which testosterone and sperm production are fairly stable throughout life Without GnRH and gonadotropins, testes atrophy, and sperm and testosterone production ceases 9
10 Plasma Testosterone and Sperm Production Levels Versus Age in Male Humans Mechanism and Effects of Testosterone Activity (1 of 3) Testosterone, synthesized from cholesterol, is transformed at some target cells Converted to dihydrotestosterone (DHT) in prostate and estradiol in some brain neurons Prompts spermatogenesis and targets all accessory organs Has multiple anabolic effects throughout body Deficiency leads to atrophy of accessory organs, semen volume declines, and erection/ejaculation are impaired; treatment: testosterone replacement Mechanism and Effects of Testosterone Activity (2 of 3) Male secondary sex characteristics: features induced in nonreproductive organs by male sex hormones (mainly testosterone) Appearance of pubic, axillary, and facial hair Enhanced growth of chest hair; deepening of voice Skin thickens and becomes oily Bones grow, increase in density Skeletal muscles increase in size and mass Boosts basal metabolic rate Basis of sex drive (libido) in males 10
11 Mechanism and Effects of Testosterone Activity (3 of 3) Testosterone Masculinizes embryonic brain Continues to exert effect well into adulthood Although adrenal glands also produce androgens in small amounts, production is insufficient to maintain normal testosterone-mediated functions Organs of the Female Reproductive System, Midsagittal Section Internal Female Reproductive Organs 11
12 Ovaries Each ovary is held in place by several ligaments Two poorly defined regions Outer cortex: houses forming gametes Inner medulla: contains large blood vessels and nerves Ovarian follicles: Contain immature egg (oocyte) surrounded by cells Follicles go through several stages of development Primordial follicle: single layer of follicle cells plus oocyte More mature follicles: several layers of granulosa cells plus oocyte Ovulation and Corpus Luteum Follicles in Different Developmental Phases Female Duct System Tube system includes: Uterine tubes Each tube ~10 cm (4 in) long receives ovulated oocyte and are usual site of fertilization Oocyte is carried along toward uterus by smooth muscle peristalsis and ciliary action Nonciliated cells of tube function to nourish oocyte and sperm Uterus Vagina 12
13 The Uterus Hollow, thick-walled, muscular organ Function is to receive, retain, and nourish fertilized ovum Regions of uterus Body: major portion Fundus: rounded superior region Isthmus: narrowed inferior region Cervix: narrow neck, or outlet; projects into vagina Cervical glands secrete mucus that blocks sperm entry except during midcycle The Uterus Uterine wall Three layers of wall Perimetrium Myometrium interlacing layers of smooth muscle Contracts rhythmically during childbirth Endometrium: mucosal lining Fertilized egg burrows into endometrium and resides there during development Stratum functionalis (functional layer) Changes in response to ovarian hormone cycles Shed during menstruation Stratum basalis (basal layer) Forms new stratum functionalis after menstruation Unresponsive to ovarian hormones Endometrium 13
14 The Vagina Thin-walled tube 8 10 cm (3 4 inches) in length Functions as birth canal, passageway for menstrual flow, and organ of copulation Layers of wall Fibroelastic adventitia Smooth muscle muscularis Stratified squamous mucosa with rugae Vaginal secretions are acidic in adult females, but alkaline in adolescents Mucosa near vaginal orifice forms incomplete partition called hymen that ruptures with intercourse External Genitalia Female external genitalia, also called vulva or pudendum, include: Mons pubis: fatty area overlying pubic symphysis Labia majora: hair-covered, fatty skin folds Labia minora: skin folds lying within labia majora Vestibule: recess within labia minora Greater vestibular glands Flank vaginal opening Release mucus into vestibule for lubrication Clitoris: anterior to vestibule Glans of the clitoris: exposed portion Prepuce of the clitoris: hoods glans Perineum External Genitalia 14
15 Oogenesis Oogenesis: production of female gametes takes years to complete Begins in fetal period Oogonia (2n ovarian stem cells) multiply by mitosis and store nutrients Primary oocytes develop in primordial follicles that become surrounded by follicle cells Primary oocytes begin meiosis but stall in prophase I At birth, female presumed to have lifetime supply of primary oocytes Each month after puberty, a few primary oocytes are activated One from this group is selected each month to become dominant follicle that resumes meiosis I Events of Oogenesis Oogenesis produces one viable ovum with three polar bodies Unequal divisions ensure oocyte has ample nutrients for 6- to 7-day journey to uterus Polar bodies degenerate and die The Ovarian Cycle Ovarian cycle: monthly (~28 day) series of events associated with maturation of egg Two consecutive phases, with ovulation occurring midcycle between phases Follicular phase: period of vesicular follicle growth (days 1 14) Luteal phase: period of corpus luteum activity (days 14 28) Only 10 15% women have 28-day cycle Follicular phase varies, but luteal phase is always 14 days from ovulation to end of cycle 15
16 Ovarian Cycle: Development and Fate of Ovarian Granulosa cells Follicles Follicular cells Stages of Follicle Development Secondary follicle becomes vesicular follicle Connective tissue and granulosa cells condense to form theca folliculi Zona pellucida: thick, glycoprotein-rich membrane secreted by oocyte, encapsulating it Early vesicular follicle formed when clear fluid begins to accumulate between granulosa cells Antrum continues to expand with fluid isolating oocyte Isolated oocyte with its surrounding granulosa cells called corona radiata When follicle is full size (2.5 cm or 1 inch), it bulges from external ovary surface It is ready to be ovulated Follicular Phase of the Ovarian Cycle During follicular phase, several vesicular (antral) follicles are stimulated to grow Triggered by rising levels of anterior pituitary hormone FSH follicle stimulating hormone FSH levels drop around middle of follicular phase Causes only one antral follicle, dominant follicle, to be selected to continue on How dominant follicle is chosen is still uncertain Primary oocyte of dominant follicle completes meiosis I to form 2 oocyte and polar body Granulosa cells then send signal to oocyte, causing it to stop at metaphase II 16
17 Ovulation Rising levels of LH cause ovary wall to rupture, expelling secondary oocyte with its corona radiata to peritoneal cavity some women experience a twinge of pain at ovulation 1 2% of ovulations release more than one secondary oocyte, which, if fertilized, result in fraternal twins Luteal Phase of the Ovarian Cycle After ovulation, ruptured follicle collapses, and antrum fills with clotted blood Remaining granulosa cells and internal thecal cells enlarge to form corpus luteum Corpus luteum secretes progesterone and some estrogen If no pregnancy occurs, corpus luteum degenerates into corpus albicans (scar) in 10 days If pregnancy occurs, corpus luteum produces hormones that sustain pregnancy until placenta takes over, at about 3 months Regulation of Female Reproductive System Hormonal Regulation of Ovarian Cycle Establishing the ovarian cycle Before puberty, ovaries secrete small amounts of estrogen, inhibiting hypothalamic release of GnRH As puberty nears, if leptin levels are adequate, hypothalamus becomes less estrogen-sensitive, so GnRH is released, stimulating FSH and LH release by pituitary FSH and LH stimulate follicles to grow, mature, and secrete sex hormones FSH stimulates granulosa cells to release estrogen LH stimulates thecal cells to produce androgens, which granulosa converts to estrogens Events continue until an adult cyclic pattern is achieved and menarche occurs 17
18 Regulation of the Ovarian Cycle Hormonal Regulation of Ovarian Cycle Negative feedback inhibits gonadotropin release Increasing levels of plasma estrogen levels exert negative feedback inhibition on FSH and LH release Inhibin from granulosa cells also inhibits FSH release Only dominant follicle can withstand this dip in FSH Other developing follicles deteriorate Positive feedback stimulates gonadotropin release Estrogen levels continue to rise as a result of continued release by dominant follicle When levels reach a critical high value, a brief positive feedback occurs on brain and anterior pituitary Triggers LH surge Hormonal Regulation of Ovarian Cycle LH surge triggers ovulation and formation of the corpus luteum High estrogen levels trigger release of stored LH, and some FSH, by anterior pituitary at midcycle Surge triggers ovulation Shortly after ovulation: Estrogen levels decline LH transforms ruptured follicle into corpus luteum LH stimulates corpus luteum to secrete progesterone and some estrogen almost immediately Progesterone helps maintain stratum functionalis Maintains pregnancy, if it occurs 18
19 Hormonal Regulation of Ovarian Cycle Negative feedback inhibits LH and FSH release Negative feedback from rising plasma progesterone and estrogen levels inhibits LH and FSH release If no fertilization occurs: Corpus luteum degenerates when LH levels start to fall Causes a sharp decrease in estrogen and progesterone, which in turn ends blockage of FSH and LH secretion, causing cycle to start all over again The Uterine (Menstrual) Cycle Uterine (menstrual) cycle: cyclic series of changes in endometrium that occur in response to fluctuating ovarian hormone levels 1. Days 1 5: menstrual phase Ovarian hormones are at lowest levels Gonadotropin levels are beginning to rise Stratum functionalis detaches from uterine wall and is shed Menstrual flow of blood and tissue lasts 3 5 days By day 5, growing ovarian follicles start to produce more estrogen The Uterine (Menstrual) Cycle 2. Days 6 14: proliferative (preovulatory) phase Rising estrogen levels prompt generation of new stratum functionalis layer As layer thickens, glands enlarge, and spiral arteries increase in number Estrogen also increases synthesis of progesterone receptors in endometrium Thins out normally thick, sticky cervical mucus to facilitate sperm passage Ovulation occurs at end of proliferative phase on day 14 19
20 The Uterine (Menstrual) Cycle 3. Days 15 28: secretory (postovulatory) phase Phase that is most consistent in duration Endometrium prepares for embryo to implant Rising progesterone levels from corpus luteum prompt: Functional layer to become a secretory mucosa Endometrial glands to enlarge and secrete nutrients into uterine cavity Thickened mucus to form cervical mucus plug that blocks entry of more sperm, pathogens, or debris The Uterine (Menstrual) Cycle 3. Days 15 28: secretory (postovulatory) phase If fertilization does not occur: Corpus luteum degenerates toward end of secretory phase; progesterone levels fall Causes spiral arteries to kink and spasm Endometrial cells die, and glands regress Spiral arteries constrict again, then relax and open wide, causing a rush of blood into weakened capillary beds Blood vessels fragment, and functional layer sloughs off Uterine cycle starts all over again on first day of menstruation 20
21 Effects of Estrogens and Progesterones Estrogens: Promote oogenesis and follicle growth in ovary Exert anabolic effect on female reproductive tract Support rapid short-lived growth spurts at puberty Induce secondary sex characteristics Growth of breasts Increased deposit of subcutaneous fat (hips and breasts) Widening and lightening of pelvis Progesterone works with estrogen to establish and regulate uterine cycle Promotes changes in cervical mucus Effects of placental progesterone during pregnancy Inhibits uterine motility Helps prepare breasts for lactation Developmental Aspects of Reproductive System Embryological and Fetal Events Determination of genetic sex Of 46 chromosomes in fertilized egg, two are sex chromosomes (other 44 are autosomes) X chromosome (large) Y chromosome (quite small) If fertilizing sperm delivers an X chromosome, fertilized egg will contain XX, and embryo will develop ovaries X egg + X sperm XX (female offspring) If fertilizing sperm delivers a Y chromosome, fertilized egg will contain XY, and embryo will develop testes X egg + Y sperm XY (male offspring) Males are XY: so ~50% of sperm contain X chromosome, and ~50% contain Y chromosome 21
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
The Reproductive System
 The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Male Reproductive System Dr. Gary Mumaugh
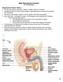 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Chapter 27 The Reproductive System. MDufilho
 Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
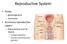 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
The Reproductive System
 Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
Female Reproductive System
 Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
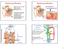 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Aniko Szabo Hill 1 of 12
 Common Function: produce offsprings endocrine glands: sex hormone production Primary organs or gonads: sex cell or gametes production Secondary or accessory organs: glands nourish gametes ducts transport
Common Function: produce offsprings endocrine glands: sex hormone production Primary organs or gonads: sex cell or gametes production Secondary or accessory organs: glands nourish gametes ducts transport
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
Chapter 46 ~ Animal Reproduction
 Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Lecture 28, The Reproductive System
 Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Physiology of Male Reproductive System
 Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Chapter 2. Reproductive system matures and becomes capable of reproduction
 Chapter 2 Human Reproductive Anatomy and Physiology Key Terms Embryo Menarche Menopause Oxytocin Ovum Prostate gland Puberty Smegma zygote Puberty Involves changes in the whole body and psyche Reproductive
Chapter 2 Human Reproductive Anatomy and Physiology Key Terms Embryo Menarche Menopause Oxytocin Ovum Prostate gland Puberty Smegma zygote Puberty Involves changes in the whole body and psyche Reproductive
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Anatomy Lecture Notes Chapter 24
 primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
Lab Activity 33. Anatomy of the Reproductive System. Portland Community College BI 233
 Lab Activity 33 Anatomy of the Reproductive System Portland Community College BI 233 Scrotum Sac of skin and superficial fascia that hangs outside the abdominopelvic cavity at the root of the penis Contains
Lab Activity 33 Anatomy of the Reproductive System Portland Community College BI 233 Scrotum Sac of skin and superficial fascia that hangs outside the abdominopelvic cavity at the root of the penis Contains
Biology of Reproduction- Zool 346 Exam 2
 Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Special Parts: Gender. Why Have Sex?
 Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
BIOL 2402 Reproductive Systems!
 Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Health Science: the structures & functions of the reproductive system
 Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O.
 UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O. OBJECTIVES Introduction Functional anatomy of male sex organ Functional anatomy of female sex organ
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O. OBJECTIVES Introduction Functional anatomy of male sex organ Functional anatomy of female sex organ
Chapter 22 Reproductive Systems. Male Reproductive Organs. Male Reproductive Organs. Specialized to produce, maintain the male sex cells (sperm)
 Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23
 AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
Reproductive Systems. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal
 What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
Reproductive System. Where it all begins
 Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
The Reproductive System
 A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
 MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
The Male Reproductive System
 The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport
 Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport (epididymis, ductus deferens(vas deferens), ejaculatory
Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport (epididymis, ductus deferens(vas deferens), ejaculatory
Male Reproductive Physiology
 Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5)
 IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System
 Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
9.4 Regulating the Reproductive System
 9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
AP Biology Ch ANIMAL REPRODUCTION. Using only what you already know (you cannot look up anything) complete the chart below.
 AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
Human Reproductive Anatomy The female anatomy first just the reproductive parts:
 Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
The Reproductive System Outline PART 1: ANATOMY OF THE MALE REPRODUCTIVE SYSTEM (pp ; Figs ) 27.1 The testes are enclosed and
 The Reproductive System Outline PART 1: ANATOMY OF THE MALE REPRODUCTIVE SYSTEM (pp. 1027 1034; Figs. 27.1 27.5) 27.1 The testes are enclosed and protected by the scrotum (pp. 1028 1030; Figs. 27.1 27.3)
The Reproductive System Outline PART 1: ANATOMY OF THE MALE REPRODUCTIVE SYSTEM (pp. 1027 1034; Figs. 27.1 27.5) 27.1 The testes are enclosed and protected by the scrotum (pp. 1028 1030; Figs. 27.1 27.3)
Ch 28 Lecture Study Guide
 Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Lab #9: Kidney: Gross Anatomy & Histology
 Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Chapter 36 Active Reading Guide Reproduction and Development
 Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Bio 104 Reproductive System
 63 Lecture Outline: Reproductive System Hole s HAP [Chapters 22, 23] I. Introduction A. Primary sex characteristics Male Female B. Secondary sex characteristics Male: 9 14 yrs. Reproductive development
63 Lecture Outline: Reproductive System Hole s HAP [Chapters 22, 23] I. Introduction A. Primary sex characteristics Male Female B. Secondary sex characteristics Male: 9 14 yrs. Reproductive development
The reproductive lifespan
 The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception
 PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 28 The Reproductive System Organs include: testes, ductus deferens, epididymis, ejaculatory ducts, urethra, seminal vesicles, prostate, bulbourethral
Principles of Anatomy and Physiology 14 th Edition CHAPTER 28 The Reproductive System Organs include: testes, ductus deferens, epididymis, ejaculatory ducts, urethra, seminal vesicles, prostate, bulbourethral
4.05 Remember the structures of the reproductive system
 4.05 Remember the structures of the reproductive system 4.05 Remember the structures of the reproductive system Essential question What are the structures of the reproductive system? 2 Structures of the
4.05 Remember the structures of the reproductive system 4.05 Remember the structures of the reproductive system Essential question What are the structures of the reproductive system? 2 Structures of the
Endocrine and Reproductive Systems. Chapter 39: Biology II
 Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Web Activity: Simulation Structures of the Female Reproductive System
 differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
Reproductive Hormones
 Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Reproduction. Human Reproductive System. Scrotum. Male Reproductive System
 Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
