--Scrotum *sac of loose skin, fascia, and smooth muscle divided into 2 pouches by a septum *skin contains dartos muscle causing wrinkling
|
|
|
- Vincent Lyons
- 6 years ago
- Views:
Transcription
1 Chapter 28: Reproductive Systems Reproductive System --gametes: germ cells (sperm and secondary oocyte) --fertilization: produces one cell with one set of chromosomes from each parent --gonads: produce gametes and secrete sex hormones --Chromosomes in Somatic Cells and Gametes: a. Somatic cells (diploid): 23 pairs of chromos for a total of 46 chromosomes *each pair is homologous *22 pairs of autosomes and 1 pair of sex chromosomes (female all homologous with 2 x s, male 22 homologous with 1 sex 1X, 1Y) *produced by mitosis (4 stages prophase, metaphase, anaphase, telophase) b. Gametes (haploid): single set of chromosomes for a total of 23 *produced by meiosis (4 stages prophase, metaphase, anaphase, telophase) i. Meiosis I: results in 2 haploid daughter cells each having duplicated chromosomes, known as reduction division b/c goes from 2n to 1n ii. Meiosis II: results in division of the replicated chromosome to yield total of 4 haploid and different daughter cells --2 Major contributions to the reassortment of genetic material a. Independent assortment: of maternal and paternal homologues during meiosis I (produces 2 n combos) b. Crossing over: during prophase I of meiosis I portions of chromatids of homologous chromosomes are exchanged --Meiosis I *chromosomes become visible (already duplicated), mitotic spindle appears, nuclear mem. and nucleoli disappear *events only seen in meiosis I a. synapsis: all copies of homologous chromosomes pair off forming a tetrad b. crossing over: portions of chromatids are exchanged b/w any members of the tetrad (genetic recombination produces sister gametes that are unlike each other and unlike either parent) *Metaphase I: homolgous pairs of chromosomes line up along the equatorial plane with attached microtubules *Anaphase I: each chromosome of tetrad is pulled to opposite ends chromosomes are separated during meiosis I, not chromatids *Telophase I: result is 2 cells with haploid number of chromosomes --Meiosis II *Similar steps in cellular process as in mitosis a. centromeres split b. sister chromatids (not chromosomes) separate * net result is 4 genetically unique haploid cells/gametes Male Reproductive system --Scrotum *sac of loose skin, fascia, and smooth muscle divided into 2 pouches by a septum *skin contains dartos muscle causing wrinkling
2 *temperature regulation of testes a. sperm survival requires 3 0 C lower temp than core body temp b. cremaster muscle in spermatic cord (elevates testes on exposure to cold and during arousal, warmth reverse the process) --Testes *paired oval glands *surrounded by dense white capsule (tunica albuginea) septa form compartments called lobules *each is filled with 2-3 seminiferous tubules where sperm are formed *develop near kidney on posterior abdominal wall descend into scrotum by passing through inguinal canal during 7 th month of fetal development *Cryptochidism: testes d/n descend into the scrotum sterility and greater risk of testicular cancer *Tunica Vaginalis: piece of peritoneum that descended with testes into scrotal sac allows for easier movement of testes within scrotum --Formation of Sperm (spermatogenesis) *Location of Stages of Sperm Formation: a. seminiferous tubules contain: all stages of sperm development (spermatogonia, primary spermatocyte, secondary spermatocyte, spermatid, spermatozoa) and sertoli cells b. Leydig cells: in between tubules, secrete testosterone, LH promote production of testosterone *Supporting Cells of Sperm Formation a. Sertoli Cells: extend from basement membrane to lumen -support developing sperm cells -form blood-testis barrier (need to protect from immune system) -produce fluid and control release of sperm into lumen -secrete inhibin which slows sperm production by inhibiting FSH -synthesize ABP (androgen binding protein): binds testosterone -FSH stimulates an increase in sperm production *Spermatogenesis a. Spermatogonium (stem cells): give rise to 2 daughter cells by mitosis b. one daughter cell kept in reserve other DIFERENTIATES into primary spermatocyte c. primary spermatocyte goes through meiosis I (DNA replication, tetrad formation, crossing over) d. Secondary spermatocytes are formed (23 chromosomes each haploid, goes through meiosis II) e. 4 spermatids are formed: each haploid, all remain in contact with a cytoplasmic bridge, accounts for synchronized release of sperm that are 50% X and 50% Y --Developing spermatids remain attached to one another by a cytoplasmic bridge for 2 reasons: 1. haploid cells with 1+ defective genes will die if they d/n get the normal product of those genes; bridges allow for normal complement gene products from any of the haploid cells to defective cell 2. it is impossible for the Y carrying cells to mature w/o
3 X- chromosome gene products bridge solves this f. Spermiogeneisis: maturation of spermatids into sperm cells (spermatozoa) --sperm morphology (adapted for reaching and penetrating a 2 0 oocyte) 1. head: contains DNA (nucleus) and acrosome (hyaluronidase and proteinase enzymes) 2. midpiece: contains mitochondria to form ATP 3. Tail: flagellum used for locomotion g. Spermiation: release of sperm cells from a Sertoli/sustenacular cell *Hormonal Control of Spermatogenesis a. puberty: hypothalamus secretes releasing hormones (GnRH) into portal system and stimulates the adenohypophysis adenohypophysis increases secretion of LH and FSH (water soluble) b. LH stimulates Leydig cells to secrete testosterone (lipid soluble) an enzyme in prostate and seminal vesicles conerts testosterone into dihydrotestosterone (DHT-more potent) c. FSH stimulates spermatogenesis: with testosterone, stimulates Sertoli cells to secrete androgen-binding protein (ABP) which keeps local hormone levels high, testosterone stimulates final steps in spermatogenesis *Effects of Inhibin Hormone (secreted by Sertoli cells) a. When sperm production is sufficient: --sertoli cells release inhibin --inhibits FSH secretion by the anterior pituitary --decreases sperm production b. When sperm production is proceeding too slowly --less inhibin is released by Sertoli cells --more FSH will be secreted --sperm production will be increased *Hormonal Effects of Testosterone a. testosterone and DHT bind to intracellular receptors and change genetic activity b. prenatal effect is male gonads and genitalia development c. at puberty, final development of secondary sexual characteristics and adult reproductive system sexual behavior and libido, male metabolism (bone and muscle mass increase), and deepening of the voice *Deficiency of 5 Alpha-Reductase a. rare genetic defect producing a deficiency of 5-alpha-reductase (enzyme that converts testosterone into DHT b. at birth, baby looks externally female due to lack of DHT during development c. at puberty: testosterone levels rise, masculine characteristics appear, breasts fail to develop, an internal exam reveals testes and other structures *Control of Testosterone Production a. negative feedback system controls blood levels of testosterone b. receptors in hypothalamus detect increase in testosterone blood level c. secretion of GnRH is inhibited d. anterior pitutiry (FSH and LH) release is slowed
4 e. Leydig cells of testes decrease testosterone secretion f. blood level returns normal --Puberty and Testosterone *Puberty: age at which individuals become capable of sexual reproduction a. Before puberty: small amounts of testosterone inhibit GnRH release b. During puberty: testosterone does not completely suppress GnRH release, resulting in increased FSH, LH, and testosterone *Testosterone a. Produced by interstitial/leydig cells, but also by adrenal cortex and sustenacular/sertoli cells b. Causes development of male sex organs in embryo, stimulates descent of testes, causes enlargement of genitals and necessary structures for sperm cell formation --Pathway of Sperm Flow through the Ducts of the Testis a. Seminiferous tubules b. Straight tubules c. Rete testis d. Efferent ducts e. Ductus epididymis: comma-shaped organ, head, body, and tail regin, multiple efferent ducts become single ductus epididymis in head region (20 ft tube if uncoiled), tail region continues as ductus deferens *Histology: lined with pseudostratified ciliated columnar epithelium, layer of smooth muscle *Function: 1. site of sperm maturation: motility increases over 2 week period 2. storage for 1-2 months 3. propels sperm onward f. Ductus (vas) deferens: pathway of 18 inch muscular tube *Histology: lined with psuedostratified columnar epithelium and covered with heavy coating of smooth muscle *Function: convey sperm along through peristaltic contractions, stored sperm remain viable for several months g. Ejaculatory Ducts: formed from duct of seminal vesicle and ampulla of vas deferens, about 1 inch long, adds fluid to prostatic urethra just before ejaculation h. Urethra: *prostatic urethra: 1 inch long *membranous urethra: passes through UG diaphragm *penile/spongy urethra: through corpus spongiosum --Accessory Sex Glands a. Seminal Vesicles: pair of pouchlike organs found posterior to the base of bladder *alkaline, viscous fluid: neutralizes acidity in vagina and male urethra, fructose for ATP production, prostaglandins stimulate sperm motility and viability, clotting proteins (different from the blood clotting factors) for coagulation of semen b. Prostate Gland: single organ inferior to bladder
5 *secretes milky, ph 6.5 fluid that increases sperm motility and viability --citric acid for ATP production --enzymes for liquefaction (lysozyme, hyaluronidase, amylase, fibrinolysin) --PSA --seminalplasmin (antibiotic) prevents UTI in males c. Bulbourethral or Cowper s Glands *during sexual arousal secrete alkaline mucus neutralizes acids and lubricates --Vasectomy: male sterilization, vas deferens cut and tied off, sperm production continues, sperm degenerate, 100% effective, 40% reversible --Spermatic Cord: all structures passing to and from the testes *testicular artery, pampiniform plexus of veins, autonomic nerves, lymphatic vessels, ductus/vas deferens, cremaster muscle --Inguinal Canal and Inguinal Hernias *Indirect hernia: loop of intestine protruding through deep ring *Direct hernia: loop of intestine pushes through posterior wall of inguinal canal *more common in males --Semen *mixture of sperm and seminal fluid: glandular secretions and fluid of seminiferous tubules, slightly alkaline, milky appearance, sticky, contains nutrients, clotting proteins and antibiotic seminal plasmin (antibiotic) *typical ejaculate is ml in volume *normal sperm count is million/ml *coagulate within 5 minutes reliquefies in 15 min due to enzymes produced by the prostate gland *semen analysis: bad news if it reveals lack of forward motility, low count or abnormal shapes --Penis *passageway for semen and urine *body composed of three erectile tissue masses filled with blood sinuses *composed of bulb, crura, body, and glans penis *Cross section of penis a. corpora cavernosa: upper paired erectile tissue masses, begins as crura of the penis attached to the ischial and pubic rami and covered by ischiocavernosus muscle b. Corpus spongiosum: lower erectile tissue mass, surrounds urethra, begins as bulb of penis covered by bulbospongiosus muscle, ends as glans penis *Glans Penis: enlarged distal end of corpus spongiosum, external urethral orifice is small slit, covered by loosely fitting prepuce or foreskin --Erection and Ejaculation a. Erection *sexual stimulation dilates the arteries supplying the penis *blood enters the penis compressing the veins so that the blood is trapped *parasympathetic reflex causes erection
6 *Neural Control of Erection: -Stimulation: tactile or psychological -Parasympathetic: erection due to vasodilation of blood vessels -Sympathetic: causes ejaculation, erection, emission b. Ejaculation *muscle contractions close sphincter at base of bladder and move fluids through ductus deferens, seminal vesicles, and ejaculatory ducts *ischiocavernous and bulbospongiosus complete the job --Male Reproductive dysfunctions or Disorders *Hypogonadism: a. results from defects in spermatogenesis and/or steroidogenesis b. may be primary defect of testis function or hypothalamic-pituitary dysfunction c. can distinguish between pre-pubertal and post-pubertal dysfunction from presence or absence of secondary sexual characteristics (eunuchoidism) d. resistance to androgens (testicular feminization) receptor for testosterone is defective, testis fail to descent and no male secondary characteristics form Female Reproductive System --Female Reproductive System *ovaries produce 2 nd oocytes and hormones *uterine tubes transport fertilized ova *uterus where fetal development occurs *vagina and external genitalia constitute the vulva *mammary glands produce milk --The Ovary *Regional histology a. tunica albuginea: capsule of dense CT b. cortex: region just deep to the tunica, contain follicles c. medulla: deeper region composed of CT, blood vessels, and lymphatics d. germinal epithelium: simple epithelial covering over the ovary --Follicular Stages a. Primordial follicle: single cell layer surrounds oocyte, squamous granulosa b. Primary follicle: 6-7 layers granulose cells surround oocyte, cuboidal granulosa c. Secondary follicle: antrum forms d. Graafian follicle: mature follicle e. ovulation f. Corpus luteum: ovulation wound, fills in with hormone secreting cells g. Corpus albicans: white scar left after corpus luteum is not needed --Layers a. Germinal epithelium: outside most layer of ovary (does not have germ cells) b. Tunica albuginea: CT under germinal epithelium c. Theca folliculi: vascular tissue; differentiates into theca externa and interna *Theca externa: CT with smooth m. and collagen *Theca interna: vascular, surrounds granulose cells of follicle d. Primary follicle: with granulose cells
7 e. Zona pellucida: glycoprotein layer b/w follicle and granulose f. corona radiata: innermost granulose layer, firmly attached to the zona pellucida; is released with follicle during ovulation g. antrum: space filled with fluid secreted by granulose cells, generates hydrostatic pressure to expel the oocyte during ovulation h. granulose cells: also nourish the maturing oocyte i. Graafian follicle: mature follicle, oocyte within is arrested at metaphase of meioss II at ovulation time --Life History of Oogonia *during fetal development, germ cells from yolk sac migrate to ovary and become oogonia *In the fetus, oogonia divide by mitosis to produce millions of oogonia but most degenerate (atresia) *some develop (differentiate) into primary oocytes and stop in prophase stage of meiosis I (still in utero) -200,000 to 2 million present at birth, atresia continues -40,000 remain at puberty but only 400 mature during a woman s life *starting at puberty, each month, hormones cause meiosis I to resume in several follicles so that metaphase of meiosis II is reached by ovulation, usually only one reaches maturity and is ovulated *meiosis II is completed only if the oocyte is fertilized by the sperm *Polar bodies: packets of discarded DNA, the secondary oocyte receives most of the cytoplasm --Uterine/Fallopian Tubes *infundibulum: open funnel-shaped portion near the ovary -fimbriae are moving finger-like processes, one is attached to ovary *ampulla: central, longest region of tube *isthmus: narrowest portion joins uterus *Histology a. mucosa: ciliated columnar epithelium with secretory cells provide nutrients and cilia move along ovum b. muscularis: circular and longitudinal smooth muscle, peristalsis helps move ovum down to the uterus c. serosa: outer serous membrane *Function: a. fimbriae sweep oocyte into tube, cilia and peristalsis move it along, sperm reaches oocyte in ampulla b. fertilization occurs within 24 hours after ovulation c. zygote reaches uterus about 7 days after ovulation --Uterus *endometrium: simple columnar epithelium, stroma of CT and endometrial glands a. stratum functionalis: shed during menstruation b. stratum basalis: replaces stratum functionalis each month *myometrium: 3 layers of smooth muscle *perimetrium: visceral peritoneum *Blood supply to uterus: uterine arteries branch as arcuate arteries and radial arteries that supply the myometrium, straight and spiral branches penetrate to the endometrium (spiral arterioles supply the stratum functionalis, their constriction
8 due to hormonal changes starts menstrual cycle) --Vagina *4 inch fibromuscular organ ending at cervix -mucosal layer: stratified squamous epithelium and areolar CT, large stores of glycogen breakdown to produce acidic ph -muscularis layer: smooth m. allows considerable stretch -adventitia: loose CT that binds it to other organs --Mammary Glands *modified sweat/sudoriferous glands: produce milk -milk secreting glands open by lactiferous ducts at the nipple, areola is pigmented area around nipple -suspensory ligaments suspend breast from deep fascia of pectoral muscles --Female Reproductive Cycle *controlled by monthly hormone cycle of anterior pituitary, hypothalamus, and ovary *Ovarian cycle: changes In ovary during and after maturation of oocyte *Uterine cycle: preparation of uterus to receive fertilized ovum, if implantation does not occur, the stratum functionalis is shed during menstruation *hormonal regulation of reproductive cycle a. GnRH secreted by the hypothalamus controls the female reproductive cycle -stimulates anterior pituitary to secrete FSH and LH -FSH initiates growth of follicles that secrete estrogen (estrogen maintains reproductive organs) -LH stimulates ovulation and promotes formation of the corpus luteum which secretes estrogens, progesterone, relaxin and inhibin b. Progesterone: prepares uterus for implantation and the mammary glands for milk secretion c. Relaxin: facilitates implantation in the relaxed uterus d. Inhibin: inhibits the secretion of FSH --Overview of Hormonal Regulation a. Estrogens: *promote development and maintenance of female reproductive structures, feminine secondary sex characteristics, and breasts *increase protein anabolism *lower blood cholesterol *moderate levels inhibit release of GnRH, FSH, and LH b. Progesterone *works with estrogens to prepare endometrium for implantation *prepares breasts to secrete milk *inhibits release of GnRH and LH c. Relaxin *inhibits contractions of uterine smooth m. *during labor, relaxes pubic symphysis and dilates uterine cervix d. Inhibin *inhibits release of FSH and to a lesser extent LH
9 --Menstrual Phase *In ovary: -20 follices that began to develop 6 days before are now beginning to secrete estrogen -fluid is filling the antrum from granulose cells (secondary follicles) *In uterus: -declining levels of progesterone caused spiral arteries to constrict-ischemia causes glandular tissue dies -stratum functionalis layer is sloughed off along with 50 to 150 ml of blood --Preovulatory Phase *most variable timeline (lasts from day 6 to 13) *In ovary: (follicular phase) -follicular secretion of estrogen and inhibin has slowed the secretion of FSH -dominant follicle survives to day 6 -by day 14, graafian follicle has enlarged and bulges at surface -increasing estrogen levels trigger the secretion of LH *In uterus (proliferative phase) -increasing estrogen levels have repaired and thickened the stratum functionalis to 4-10 mm in thickness --Ovulation *rupture of follicle and release of secondary oocyte on day 14 *cause: increasing levels of estrogen stimulate release of GnRH which stimulates anterior pituitary to release more LH *Corpus hemorrhagicum results *Signs of ovulation a. increase in basal body temp b. changes in cervical mucus c. cervix softens d. mittelschmerz pain --Postovulatory Phase *most constant timeline (lasts 14 days) *In Ovary: (luteal phase) -If fertilization d/n occur, corpus albicans is formed: as ovarian hormone levels drop (hear end of cycle), secretion of GnRH, FSH, LH begins to rise -If fertilization occurs: developing embryo secretes human chorionic gonadotropin (hcg) which maintains corpus luteum and its hormone secretions *In uterus (secretory phase) -hormones from corpus luteum promote thickening of endometrium to mm (formation of more endometrial glands and vascularization) -if no fertilization occurs, menstrual phase will begin --What cells convert androgens into estrogens? granulose cells --What hormone acts on these cells? FSH --What hormone stimulates theca cells? LH (stimulates smooth m. contraction in theca helping with ovulation)
10
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
The Reproductive System
 Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Aniko Szabo Hill 1 of 12
 Common Function: produce offsprings endocrine glands: sex hormone production Primary organs or gonads: sex cell or gametes production Secondary or accessory organs: glands nourish gametes ducts transport
Common Function: produce offsprings endocrine glands: sex hormone production Primary organs or gonads: sex cell or gametes production Secondary or accessory organs: glands nourish gametes ducts transport
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
Male Reproductive System Dr. Gary Mumaugh
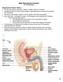 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Anatomy Lecture Notes Chapter 24
 primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
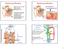 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Lab Activity 33. Anatomy of the Reproductive System. Portland Community College BI 233
 Lab Activity 33 Anatomy of the Reproductive System Portland Community College BI 233 Scrotum Sac of skin and superficial fascia that hangs outside the abdominopelvic cavity at the root of the penis Contains
Lab Activity 33 Anatomy of the Reproductive System Portland Community College BI 233 Scrotum Sac of skin and superficial fascia that hangs outside the abdominopelvic cavity at the root of the penis Contains
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 28 The Reproductive System Organs include: testes, ductus deferens, epididymis, ejaculatory ducts, urethra, seminal vesicles, prostate, bulbourethral
Principles of Anatomy and Physiology 14 th Edition CHAPTER 28 The Reproductive System Organs include: testes, ductus deferens, epididymis, ejaculatory ducts, urethra, seminal vesicles, prostate, bulbourethral
Lecture 28, The Reproductive System
 Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Reproductive System
 The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O.
 UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O. OBJECTIVES Introduction Functional anatomy of male sex organ Functional anatomy of female sex organ
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O. OBJECTIVES Introduction Functional anatomy of male sex organ Functional anatomy of female sex organ
Bio 104 Reproductive System
 63 Lecture Outline: Reproductive System Hole s HAP [Chapters 22, 23] I. Introduction A. Primary sex characteristics Male Female B. Secondary sex characteristics Male: 9 14 yrs. Reproductive development
63 Lecture Outline: Reproductive System Hole s HAP [Chapters 22, 23] I. Introduction A. Primary sex characteristics Male Female B. Secondary sex characteristics Male: 9 14 yrs. Reproductive development
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Ch 28 Lecture Study Guide
 Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
 MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
Biology of Reproduction- Zool 346 Exam 2
 Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
11/15/2017. Reproductive System. Anatomy of Male Reproductive System. Reproductive Organs of the Male, Sagittal View
 Reproductive System What is sex? Biological science perspective Primary sex organs (gonads): testes and ovaries Produce gametes (sex cells): sperm and ova Secrete steroid sex hormones Androgens (males)
Reproductive System What is sex? Biological science perspective Primary sex organs (gonads): testes and ovaries Produce gametes (sex cells): sperm and ova Secrete steroid sex hormones Androgens (males)
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport
 Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport (epididymis, ductus deferens(vas deferens), ejaculatory
Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport (epididymis, ductus deferens(vas deferens), ejaculatory
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23
 AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Reproductive System. Where it all begins
 Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
FIGURE The tunica albuginea is a connective tissue capsule forming the outer part of each testis.
 Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
18 Urinary system. 19 Male reproductive system. Female reproductive system. Blok 11: Genital and Urinary Tract Diseases
 Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
Physiology of Male Reproductive System
 Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Chapter 28 The Reproductive Systems
 Chapter 28 The Reproductive Systems Sexual reproduction produces new individuals germ cells called gametes (sperm & 2nd oocyte) fertilization produces one cell with one set of chromosomes from each parent
Chapter 28 The Reproductive Systems Sexual reproduction produces new individuals germ cells called gametes (sperm & 2nd oocyte) fertilization produces one cell with one set of chromosomes from each parent
Chapter 27 The Reproductive System. MDufilho
 Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Chapter 22 Reproductive Systems. Male Reproductive Organs. Male Reproductive Organs. Specialized to produce, maintain the male sex cells (sperm)
 Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
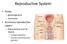 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
10 Reproductive System
 Chapter 10 Reproductive System Male Reproductive System -The male reproductive system consists of the penis, testes, scrotum, a series of ducts (epididymis, vas deferens, ejaculatory ducts, and urethra),
Chapter 10 Reproductive System Male Reproductive System -The male reproductive system consists of the penis, testes, scrotum, a series of ducts (epididymis, vas deferens, ejaculatory ducts, and urethra),
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
Special Parts: Gender. Why Have Sex?
 Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
The Reproductive System
 A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
BIOL 2402 Reproductive Systems
 Collin College Dr. Chris Doumen BIOL 2402 Reproductive Systems 1 Reproductive System Most systems between males and females in the human body are similar in structure. The exception of course are the organs
Collin College Dr. Chris Doumen BIOL 2402 Reproductive Systems 1 Reproductive System Most systems between males and females in the human body are similar in structure. The exception of course are the organs
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception
 PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Health Science: the structures & functions of the reproductive system
 Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Cell Divisions. The autosomes represent the whole body. * Male Sex Chromosomes: XY * Female Sex Chromosomes: XX
 Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Male Reproductive Physiology
 Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Bio 182- Ecology Unit Outline 1
 Bio 182- Ecology Unit Outline 1 Reproductive System Introduction 1. Functions: a. Procreation b. Bonding between sexes 2. Gonads: a. Male-testes b. Female-ovaries Male Reproductive System Male Reproductive
Bio 182- Ecology Unit Outline 1 Reproductive System Introduction 1. Functions: a. Procreation b. Bonding between sexes 2. Gonads: a. Male-testes b. Female-ovaries Male Reproductive System Male Reproductive
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM
 Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
The Sex Hormones & Reproductive Systems (6)
 The Sex Hormones & Reproductive Systems (6) The Male Reproductive System The male reproductive system Lumen) Sperm Scrotum ~300 lobules Sertoli cell Leydig cell Testosterone Testes : - produce sperm cells
The Sex Hormones & Reproductive Systems (6) The Male Reproductive System The male reproductive system Lumen) Sperm Scrotum ~300 lobules Sertoli cell Leydig cell Testosterone Testes : - produce sperm cells
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 21 Female Reproductive System 1 Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of female reproductive system
BIOH122 Human Biological Science 2 Session 21 Female Reproductive System 1 Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of female reproductive system
Reproductive Systems. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
describe the parts and function of semen and the glands that contribute to it
 You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
MALE REPRODUCTIVE SYSTEM
 1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
Histology of Male Reproductive System
 Histology of Male Reproductive System Lecture Objectives Describe the histological features of the male reproductive system Male Reproductive System The male structures of reproduction include the: testes,
Histology of Male Reproductive System Lecture Objectives Describe the histological features of the male reproductive system Male Reproductive System The male structures of reproduction include the: testes,
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5)
 IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System
 Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Human Reproductive Anatomy The female anatomy first just the reproductive parts:
 Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Male reproductive system The physiology of sexual act
 Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
The Reproductive System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska
 27 The Reproductive System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The reproductive system is designed to perpetuate the species
27 The Reproductive System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The reproductive system is designed to perpetuate the species
9.4 Regulating the Reproductive System
 9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
