The Taipan snake venom time: a new test for lupus anticoagulant
|
|
|
- Logan Davis
- 5 years ago
- Views:
Transcription
1 J Clin Pathol 1994;47: The Taipan snake venom time: a new test for lupus anticoagulant 497 Department of Haematology, University College London Medical School, London WClE 6HX M Rooney T McNally I J Mackie S J Machin Correspondence to: T McNally ccepted for publication 25 November 1993 M Rooney, T McNally, I J Mackie, S J Machin bstract ims-to develop a specific test for lupus anticoagulant activity with reduced sensitivity to coagulation factor deficiency that would be suitable for analysis of plasmas from patients receiving oral anticoagulants. Methods- coagulation test based on the Taipan snake venom time (TSVT) with a platelet neutralisation procedure (PNP) was developed and compared with dilute Russell's viper venom time (DRWT). The TSVT was used to test plasmas from patients receiving oral anticoagulant or heparin with mild liver dysfunction and with documented lupus anticoagulant. Results-The optimised conditions for the TSVT were established and a reference range was determined in normal healthy subjects. Results were considered positive for lupus anticoagulant if the ratio was.1-1 and was reduced by.1% or to <II in the PNP. In 43 samples from patients receiving oral anticoagulants there was no correlation between level of anticoagulation and TSVT, and only seven samples had increased TSVTs. Of these, five corrected on mixing with normal plasma and two gave equivocal results. The patients with mild liver dysfunction all had normal TSVTs. The TSVT in plasmas from patients receiving heparin correlated with the heparin concentrations (as measured by the PTT, r2 =.81). Some anticoagulated plasmas showed correction in the PNP and were regarded as false positive. Fourteen of 17 patients known to have lupus anticoagulant (on the basis ofdrwt results) were also positive by the TSVT; two of the remaining three were borderline and one was negative. Conclusions-The TSVT showed satisfactory intra-assay precision and reasonable sensitivity to lupus anticoagulant, compared with the DRVVT. The TSVT was influenced by the presence of heparin but was not sensitive to the effects of oral anticoagulant. Like other lupus anticoagulant tests, it does not seem to havea 1% detection rate, but this may be due to the presence of lupus anticoagulant subtypes with distinct activities or the requirement of cofactors other than prothrombin or 112 glycoprotein-i. (7 Clin Pathol 1994;47:497-51) The lupus anticoagulant prolongs the clotting times of phospholipid dependent in vitro coagulation tests.' This is due to the presence of plasma immunoglobulins (usually IgG, IgM, or a mixture of both) which bind to the anionic phospholipids that normally support haemostatic reactions. Lupus anticoagulant was first described in patients with systemic lupus erythematosus (SLE),2 but lupus anticoagulants have since been demonstrated in a variety of clinical conditions. The presence of lupus anticoagulant has been associated with thrombosis and recurrent fetal loss,34 and these associations have established the importance of laboratory diagnosis of lupus anticoagulant. There is still considerable controversy about the most appropriate method for detecting lupus anticoagulant. Current recommendations in the United Kingdom suggest that laboratories should screen plasma and then use at least one more specific confirmatory test.5 The activated partial thromboplastin time (PIF) is the most frequently used screening test for lupus anticoagulant and confirmatory tests include the dilute Russell's viper venom time (DRVVT) and the kaolin clotting time (KCT).5 The use of mixing studies with normal plasma and correction procedures with lysed washed platelets7 or high concentrations of phospholipid8 have been a further development in laboratory diagnosis of lupus anticoagulant. Regardless of which method is used, care must be taken to ensure that laboratory procedures are standardised.5 Most patients referred for investigation of lupus anticoagulant have had previous thrombotic episodes and are consequently receiving anticoagulants. However, all of the standard tests used for lupus anti-coagulant are affected by oral anticoagulant therapy. Mixtures of normal plasma and test plasma may correct a factor deficiency without neutralising the lupus anti-coagulant effect, but the sensitivity of the testis reduced and the current recommenda-tions advise repeat testing after discontinuing oral anticoagulants.5 In many cases this cannot be considered because of the increased risk of thrombosis. We have explored the used of a reagent prepared from the venom of the Taipan snake (Oxyuranus scutellatus) that directly activates prothrombin in the presence of phospholipid and calcium ions,9 for the identification of lupus anticoagulant in patients receiving oral anticoagulants. Methods Venous blood was collected into a one-tenth J Clin Pathol: first published as /jcp on 1 June Downloaded from on 24 July 218 by guest. Protected by copyright.
2 498 Rooney, McNally, Mackie, Machin - C~ ) CO) E C1 ) S: C.) a1) a) E CD H 7 F S S volume of d16 M tri-sodium citrate and centrifuged at 2 x g for 15 minutes to prepare plasma. Platelet poor plasma (PPP) was prepared by recentrifuging the plasma at 2 x g for a further 15 minutes. ll samples were stored in aliquots at -7 C. Patients were considered positive for lupus anticoagulant according to the British Society for Haematology guidelines on testing for the lupus anticoagulant5-that is, on the basis of the results of the PTT and DRVVT-with appropriate mixing and correction tests. PTT was measured using a micronised silica reagent (Instrumentation Laboratories Ltd, Warrington, Cheshire). Thrombin time (TT) was measured using bovine thrombin and prothrombin time (PT) using phenolised rabbit brain thromboplastin (Diagnostic Reagents Ltd, Thame, Oxford). The DRVVT was measured using "Bell and lton" phospholipid reagent and Russell's viper venom (RVV) (Diagnostic Reagents Ltd). Freeze-thawed, washed platelets for the platelet neutralisation procedure (PNP) of the DRVVT and Taipan snake venom test (TSVT) were prepared from normal citrated platelet rich plasma (PRP) using a washing buffer containing inhibitors of platelet activation.' The washed platelets Reciprocal Taipan venom dilution,,-i /',/t' Reciprocal phospholipid dilution // b were finally suspended in buffer without inhibitors at a count of 4 x 19/1 and frozen at -7 C before thawing and freezing in aliquots at -7 C. The following conditions for the TSVT were defined on the basis of results of preliminary optimisation experiments performed using normal PPP and a well characterised strong lupus anticoagulant PPP. "Bell and lton" phospholipid was diluted 1 in 4 in.5 M imidazole, -1 M NaCl, ph 7-3. Taipan snake venom (TSV) (Diagnostic reagents Ltd) was reconstituted according to manufacturer's instructions and then diluted with an equal volume of -25M calcium chloride. (1 p1) phospholipid and 1,ul normal control or test PPP were mixed and incubated in a 75 x 1 mm glass tube at 37 C for 3 seconds. TSV (1 pl) were added and the clotting time measured. The test was then repeated with the platelet neutralisation procedure (PNP), substituting washed lysed platelets for phospholipid. ratio of test and control clotting times was calculated and if the test:control ratio with phospholipid was 21 1 the test was repeated using a 1:1 mixture of normal control and test plasma (NP mix). positive result for lupus anticoagulant in the TSVT was defined as a ratio of.1 1 with correction to < 1 1 or by 1% or more with the PNP. Two commercial lyophilised washed platelet preparations, Platelet Extract Reagent (lpha Laboratories, Eastleigh, Hampshire, England) and Platelet Neutralisation Reagent (Quatro Biosystems, Manchester, Lancashire England), were also tested in the TSVT. The optimised TSVT was used to study healthy normal subjects, patients receiving anticoagulants, patients with liver dysfunction, and patients referred for investigation for thrombophilia. Results When the Taipan venom concentration was *15-8 decreased at a constant phospholipid concentration, there was a progressive increase in the clotting time of normal plasma (fig 1). 1 in 2 dilution of Taipan venom was selected for further experiments to confer sensitivity while maintaining convenient clotting times. Decreasing the phospholipid concentration at a constant venom concentration produced progressively increasing clotting times with both normal plasma and a well characterised lupus anticoagulant plasma (fig 1B). 1 in 4 dilution of phospholipid in imidazole buffer was selected for use as this produced minimal prolongation of the clotting time of normal plasma, while permitting clear distinction between normal and lupus anticoagulant positive clotting times. Dilution of the washed platelets from a suspension of -4 x 19/1 resulted in increased clotting times with both normal and lupus anticoagulant plasmas (not shown). 1 in 4 dilution of this reagent was T (B) The selected for further experiments to maintain Figure 1 () The effect of Taipan snake venom concentration on the TSV'j effect ofphospholipid concentration on the TSVT of a normal ( ) and well convenient clotting times. Two commercial characterised L plasma (O---). PNP reagents were also tested and had J Clin Pathol: first published as /jcp on 1 June Downloaded from on 24 July 218 by guest. Protected by copyright.
3 The Taipan snake venom time: a new testfor lupus anticoagulant 499 C. H) 1.5 r 1*. Table Results of stability studies on TSV reagent TSVT ratio of lupus anticoagulant positive plasma Time after TSVstored on ice Freeze-thawed TSV reconstitution of TSV (hours) TSVT PNP TSVT PNP comparable performance to the "in house" reagent. The stability of the Taipan reagent was assessed by measuring the TSVT of a lupus anticoagulant plasma at varying time intervals over an eight hour period using Taipan venom reagent that was stored on ice during this period or repeatedly freeze-thawed. The Taipan venom reagent remained stable on ice and was unaffected by repeated freeze-thawing (table 1). Three different batches of TSV were tested and demonstrated a similar potency and gave a similar pattern of results with normal and lupus anticoagulant positive plasmas. Intra-assay precision of the optimised TSVT was assessed by assaying normal plasma and a well characterised lupus anticoagulant plasma 2 times. The intra-assay coefficients of variation (CV) of ratios of the TSVT and PNP of the lupus anticoagulant plasma were determined to be 4% and 3%, respectively. The interassay precision was assessed by assaying a separate aliquot of an lupus anticoagulant plasma on nine consecutive runs over a six week period and was determined to be 13% and 7-3% for the TSVT and PNP, respectively. lthough a certain degree of interassay variation was apparent in both the normal and lupus anticoagulant positive plasmas, the lupus anticoagulant plasma was correctly identified on each occasion. The optimised method was used to INR mea Figure 2 TSVT results ofplasmas from patients receiving oral anticoagulant treatment normal TSVT, increased TSVT, indicates increased TSVT results ofplasmas from one patient. Table 2 Results of correction studies performed on warfarin plasmas with abnormal TSVT results Case No INR TSVT PNP NP mix Result ?Positive ?Positive Negative ND Negative Negative Negative Negative sure the TSVT of 2 normal subjects. This group included 12 women and eight men and had a mean age of 3 years (range years). The mean (SD) of the TSVT ratios were 97 (5) and the reference range (mean 2SD) was therefore determined as ' Samples were collected from 43 patients receiving oral anticoagulants. The patient group included those starting treatment and those attending the oral anticoagulant clinic, in order to achieve a wide range of levels of anticoagulation. Some patients had international normalised ratio (INR) results below the therapeutic range <2.5) and a small number had grossly increased INRs (>4.). There was no correlation between INR and TSVT (fig 2). Thirty six of the patients receiving warfarin had normal TSVT ratios, irrespective of INR, and seven plasmas from five patients had increased TSVT ratios. Of the seven plasmas with increased TSVT ratios, two corrected by more than 1% or to < 1 1 in the PNP. These plasmas also corrected to <1 1 (case 1) and by more than 1% (case 2) in a 1:1 mix with normal plasma and so were considered as possible lupus anticoagulant positive plasmas (table 2). Five plasmas did not correct with PNP and of these, four were found to correct when a 1:1 with normal plasma was tested, indicating that prolongation of the TSVT was due to factor deficiency. The remaining plasma was not tested with a 1:1 mix with normal plasma but was from a 4 x PTT ratio Figure 3 TSVT results ofplasmas from patients receiving heparin X----- TSVT, - -PNP. J Clin Pathol: first published as /jcp on 1 June Downloaded from on 24 July 218 by guest. Protected by copyright.
4 5 Rooney, McNaly, Mackie, Machin Table 3 Median DRVVT and TSVT results of lupus anticoagulant positive patients DRVVT DRVVTPNP TSVT TSVTPNP n = Median Minimum Maximum patient found to be negative for lupus anticoagulant on two other occasions. Nine plasmas from seven patients receiving unfractionated heparin and selected at random were tested to examine the effect of heparin on the TSVT (fig 3). Heparin resulted in prolongation of the TSVT and a significant correlation was demonstrated between PTT ratio and TSVT (r' = -81, p <.1). Five patients had TSVT ratios of and in three of these the PNP corrected the TSVT ratio by more than 1%, giving an apparent positive result, while the remaining two patients corrected by <1%. Twelve patients with liver dysfunction (secondary to alcoholic liver disease, paracetamol overdose, or obstructive jaundice) with a mean INR of 1-52 (range ) and thrombin time of 15-5 (range ) were tested. ll patients had normal TSVT ratios (not shown). We also investigated 17 patients who had been diagnosed as lupus anticoagulant positive on the basis of DRVVT results. The median DRVVT and TSVT results are shown in table 3. Fourteen patients were found to be positive for lupus anticoagulant by the TSVT. Of the remaining three, one had a normal TSVT (1-6), one had a borderline TSVT (1-9) which corrected with the PNP (1 -), and one had a prolonged TSVT (1.23) but gave <1% correction with the PNP (1-14). We also tested 16 patients attending the thrombophilia clinic for investigation of previous thrombotic episodes who had abnormal DRVVTs but did not demonstrate the correction patterns typical of lupus anticoagulant. Ten of these patients had normal TSVT results. The remaining six patients all showed >1% correction with PNP but also demonstrated >1% correction in a 1:1 mix with normal plasma. Thus the TSVT allowed 1 of these patients to be classified as lupus anticoagulant negative but could not clarify the situation in the remainder. Discussion The clinical importance of antiphospholipid antibodies is becoming increasingly recognised and consequently lupus anticoagulant testing has become an essential routine procedure for haemostasis laboratories. Incidental findings of lupus anticoagulant are relatively rare and it is more usual for testing to be required after a previous unexplained thrombotic episode, often when the patient is receiving oral anticoagulants. Consequently it may be difficult to interpret results as the available tests are all dependent on adequate levels of several coagulation factors and are therefore affected by oral anticoagulants. Phospholipid dependent prothrombin activating snake venoms are suitable candidate reagents for lupus anticoagulant test systems with reduced sensitivity to oral anticoagulants, as they rely only on adequate concentrations of prothrombin and fibrinogen and are not affected by plasma concentrations of factors IX and X. The Taipan venom from Oxyuranus scutellatus contains at least one prothrombin activator of large molecular size.9 The protein apparently consists of a factor Xa-like catalytic subunit and factor Va-like cofactor unit which are potentiated by the presence of phospholipid and calcium ions. The products of venom catalysed prothrombin activation are thrombin and meizothrombin.'" ctivators such as these that have no factor Va requirement have as yet only been identified in the venoms of ustralian Elapidae."2 The action of lupus anticoagulant is universally agreed to centre on the inhibition of the role of phospholipid in haemostatic reactions. Therefore, the amount of phospholipid in a test system should be limited, as high phospholipid concentrations may mask the inhibitory effect of lupus anticoagulants. In the TSVT a 1 in 4 dilution of phospholipid resulted in good distinction between normal and lupus anticoagulant plasma clotting times, whereas higher dilutions resulted in very long clotting times, giving logistical problems for routine use and weaker clot formation, which made accurate end-point determination difficult. Confirmation of the presence of lupus anticoagulant requires correction of the clotting time on addition of lysed washed platelets or excess phospholipid, but no correction on mixing with normal plasma.' 13 1 in 4 dilution of the stock suspension of washed platelets was selected for use and gave good correction (>2%) of the TSVT ratio using a well characterised lupus anticoagulant plasma. Preparation of washed platelets is time consuming and so two commercial products designed for use in the PNP in the PIT or DRVVT were tested in the TSVT and performed well. One of the disadvantages of the DRVVT is that the RVV is unstable and activity is reduced over time, even at 4GC.'4 The results of assays performed with TSV stored on ice over an eight hour period or repeatedly freezethawed suggest that TSV is stable, even in a diluted form. This may be due to the incorporation of albumin or other stabilisers by the manufacturer in the particular TSV reagent used. This may not be the case with other products and therefore TSV stability may vary according to source. Prolongation of the TSVT was generally not related to the degree of oral anticoagulant treatment; the TSVT was normal in two patients with grossly raised INR values (8-4 and 14.2). Five anticoagulated patients did have prolonged TSVTs and of these, three corrected to <1 1 with a 5/5 mix with normal plasma, indicating that the prolongation J Clin Pathol: first published as /jcp on 1 June Downloaded from on 24 July 218 by guest. Protected by copyright.
5 The Taipan snake venom time: a new testfor lupus anticoagulant was due to factor deficiency. These patients might have had more severely depressed prothrombin concentrations as a result of concomitant liver dysfunction. In the remaining two, the TSVT corrected in the PNP and so they must be considered as possible lupus anticoagulant positive patients. number of patients with mild liver dysfunction were tested by the TSVT. ll patients had normal TSVT results, suggesting that the fibrinogen and vitamin K dependent coagulation factor abnormalities induced by this condition do not adversely affect the TSVT. correlation was shown between heparin treatment (as measured by the PFT) and TSVT. lthough prolongation of the TSVT and PNP was demonstrated with increased heparin concentrations the PNP was less prolonged than the TSVT at the higher heparin values, giving a false positive effect. This is most likely attributable to the heparin neutralising activity of platelet factor 4 in the washed platelet preparation. Plasmas contaminated with heparin therefore cannot be reliably tested using the TSVT and testing should be repeated when heparin treatment has been stopped. The efficacy of the TSVT in identifying lupus anticoagulant positive plasmas was assessed by testing known lupus anticoagulant positive plasmas. The patient group comprised patients with SLE and antiphospholipid syndrome and included some patients receiving oral anticoagulant treatment. The minimum and median values of the DRVVT and TSVT were comparable but the maximum level of the TSVT was much lower than that of the DRVVT. This difference is most likely a reflection of the reduced sensitivity of the TSVT to oral anticoagulants. The TSVT correctly identified all but one of the lupus anticoagulant positive plasmas. This plasma did not fulfil the lupus anticoagulant criteria of the TSVT but was identified as lupus anticoagulant positive using the DRVVT. The reason for this discrepancy is unclear; it is possible that the lupus anticoagulant may be part of a distinct subgroup with its main mode of action directed at a site other than the prothrombinase complex which forms the basis of the TSVT. The TSVT was also used to test several plasmas which gave prolonged DRVVT results but did not give correction results typical of lupus anticoagulant. Most of these plasmas yielded normal TSVTs. Plasmas demonstrating prolonged TSVTs all showed correction with a 5/5 mix with normal plasma and correction with PNP. These results show that the TSVT is far less liable to false positive analysis than the DRVVT. 51 The TSVT can therefore be considered a suitable test for the diagnosis of lupus anticoagulant. The TSVT demonstrated satisfactory intra-assay precision and reasonable sensitivity compared with the DRVVT. It has the advantage of requiring only adequate fibrinogen and prothrombin concentrations and has reduced sensitivity to factor deficiency, an important consideration in the analysis of plasmas from patients receiving oral anticoagulants. n additional advantage is that the test is based on prothrombin, a relatively nonlabile coagulation factor, and as such may be more readily applied than the DRVVT to the assay of previously freeze-thawed plasmas. The test is easy to perform, readily adaptable for automated operation, and relatively inexpensive and is therefore suitable for use in most haemostasis laboratories. T McNally was supported by a grant from the rthritis and Rheumatism Council (No M136). 1 Shapiro SS, Thiagarajan P. Lupus anticoagulants. In: Spaet TH, ed. Progress in thrombosis and haemostasis. Vol 6. New York: Grune & Stratton, 1982: Conley CL, Hartman RC. haemorrhagic disorder caused by circulating anticoagulant in patients with disseminated lupus erythematosus. Jf Clin Invest 1952; 31: Bowie WEJ, Thompson JH, Pascuzzi C, Owen G. Thrombosis in systemic lupus erythematosus despite circulating anticoagulants. J Lab Clin Med 1963;62: Nilsson IM, sted B, Hedner U, Berezin D. Interuterine death and circulating anticoagulant, 'antithromboplastin'. cta Med Scand 1975;197: The Lupus nticoagulant Working Party of The British Society for Haematology. Guidelines on testing for the lupus anticoagulant. J Clin Pathol 1991;44: The Lupus nticoagulant Working Party of The British Society for Haematology. Detection of the lupus-like anticoagulant: current laboratory practice in The United Kingdom. J Clin Pathol 199;43: Triplett D, Brandt JT, Kaczor D, Scaeffer J. Laboratory diagnosis of lupus inhibitors: comparison of the tissue thromboplastin inhibition procedure with a new platelet neutralisation procedure. m J Clin Pathol 1983; 79: Rosove MH, Ismail M, Kozoil BJ, Runge, Kasper CK. Lupus anticoagulants: Improved diagnosis with a kaolin clotting time using rabbit brain thromboplastin in standard and high concentrations. Blood 1986;68: Speijer H, Govers-Reimslag JWP, Zwaal RF, Rosing J. Prothrombin activation by an activator from the venom of Oxyuranus scutellatus (Taipan snake). J Biol Chem 1986;261: Machin SJ, Mackie U. Platelet function tests. In: Chanarin I, ed. Laboratory haematology. n account of laboratory techniques. Edinburgh: Churchill Livingstone, 1989: Walker H., Owen WG, Esmon CT. Characterisation of the prothrombin activator from the venom of Oxyuranus scutellatus scutellatus (Taipan venom). Biochemistry 198;19: Rosing J, Tans G. Inventory of exogenous prothrombin activators for the subcommittee on nomenclature of exogenous haemostatic factors of the scientific and standardisation committee of the International Society on Thrombosis and Haemostasis. Thromb Haemostas 1991; 65: Exner T, Triplett D, Taberner D, Machin SJ. Guidelines for testing and revised criteria for lupus anticoagulants, prepared for the subcommittee for the standardization of lupus anticoagulants of the International Society on Thrombosis and Haemostasis. Thromb Haemostas 191 1; 65: Sukhu K, Mackie U. utomation of the DRVVT. Med Lab Sci 1992;49: J Clin Pathol: first published as /jcp on 1 June Downloaded from on 24 July 218 by guest. Protected by copyright.
Mohammadreza Tabatabaei IBTO COAG LAB
 Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time
 Clin. Lab. 2009;55:XXX-XXX Copyright ORIGINAL ARTICLE Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time HORATIU OLTEANU 2, KATHARINE. A. DOWNES 1, JIGAR
Clin. Lab. 2009;55:XXX-XXX Copyright ORIGINAL ARTICLE Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time HORATIU OLTEANU 2, KATHARINE. A. DOWNES 1, JIGAR
Lupus Anticoagulants (LA), Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update. Antiphospholipid. Antiphospholipid
 , Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
, Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
A Percent Correction Formula for Evaluation of Mixing Studies
 Coagulation and Transfusion Medicine / A PERCENT CORRECTION FORMULA FOR EVALUATION OF MIXING STUDIES A Percent Correction Formula for Evaluation of Mixing Studies Sheng-hsiung Chang, MD, Veronica Tillema,
Coagulation and Transfusion Medicine / A PERCENT CORRECTION FORMULA FOR EVALUATION OF MIXING STUDIES A Percent Correction Formula for Evaluation of Mixing Studies Sheng-hsiung Chang, MD, Veronica Tillema,
ACTICLOT dpt REF 824. IVD C i 2 l. Dilute Prothrombin Time Test for the Determination of Lupus Anticoagulants (LA) (CPT Code No.
 Sekisui Diagnostics, LLC 500 West Avenue, Stamford, CT 06902 M Tel. (203) 602-7777 Fax (203) 602-2221 INTENDED USE The ACTICLOT dpt is intended for the qualitative determination of Lupus Anticoagulants
Sekisui Diagnostics, LLC 500 West Avenue, Stamford, CT 06902 M Tel. (203) 602-7777 Fax (203) 602-2221 INTENDED USE The ACTICLOT dpt is intended for the qualitative determination of Lupus Anticoagulants
Determination of APTT factor sensitivity the misguiding guideline
 International Journal of Laboratory Hematology ORIGINAL ARTICLE The Official journal of the International Society for Laboratory Hematology INTERNATIONAL JOURNAL OF LABORATORY HEMATOLOGY Determination
International Journal of Laboratory Hematology ORIGINAL ARTICLE The Official journal of the International Society for Laboratory Hematology INTERNATIONAL JOURNAL OF LABORATORY HEMATOLOGY Determination
Guidelines. 704 q 2000 Blackwell Science Ltd GUIDELINES ON THE INVESTIGATION AND MANAGEMENT OF THE ANTIPHOSPHOLIPID SYNDROME
 British Journal of Haematology 2000, 109, 704±715 Guidelines GUIDELINES ON THE INVESTIGATION AND MANAGEMENT OF THE ANTIPHOSPHOLIPID SYNDROME In 1991, the Haemostasis and Thrombosis Task Force of the British
British Journal of Haematology 2000, 109, 704±715 Guidelines GUIDELINES ON THE INVESTIGATION AND MANAGEMENT OF THE ANTIPHOSPHOLIPID SYNDROME In 1991, the Haemostasis and Thrombosis Task Force of the British
TECHNICAL SERIES. Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss. ...Setting trends TULIP DIAGNOSTICS (P) LTD.
 For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
A Novel Clotting Assay for Quantitation of Plasma Prothrombin (Factor II) Using Echis multisquamatus Venom
 Coagulation and Transfusion Medicine VENOM-BSED PROTHROMBN SSY Novel Clotting ssay for Quantitation of Plasma Prothrombin (Factor ) Using Echis multisquamatus Venom Ramona]. Petrovan, PhD, Samuel. Rapaport,
Coagulation and Transfusion Medicine VENOM-BSED PROTHROMBN SSY Novel Clotting ssay for Quantitation of Plasma Prothrombin (Factor ) Using Echis multisquamatus Venom Ramona]. Petrovan, PhD, Samuel. Rapaport,
HEMOSTASIS Quality Time saving Economy Practicability Quality assurance Precision
 Quality Time saving Economy Practicability Quality assurance Precision exclusive distributor of for France, Netherlands, Belgium and Luxembourg List of frozen reagents In 1992, Precision BioLogic began
Quality Time saving Economy Practicability Quality assurance Precision exclusive distributor of for France, Netherlands, Belgium and Luxembourg List of frozen reagents In 1992, Precision BioLogic began
Antiphospholipid antibodies in patients with venous thrombosis at Kenyatta National Hospital
 Research article Department of Human Pathology, School of Medicine, University of Nairobi, P. O. Box 19676 00202, Nairobi, Kenya Corresponding author: Dr KA Barasa, Department of Human Pathology, School
Research article Department of Human Pathology, School of Medicine, University of Nairobi, P. O. Box 19676 00202, Nairobi, Kenya Corresponding author: Dr KA Barasa, Department of Human Pathology, School
Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome
 Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Comparison of Three Methods for Measuring Factor VIII Levels in Plasma
 Coagulation and Transfusion Medicine / THREE FACTOR VIII ASSAYS Comparison of Three Methods for Measuring Factor VIII Levels in Plasma Wayne L. Chandler, MD, Chris Ferrell, MT(ASCP), Joo Lee, MT(ASCP),
Coagulation and Transfusion Medicine / THREE FACTOR VIII ASSAYS Comparison of Three Methods for Measuring Factor VIII Levels in Plasma Wayne L. Chandler, MD, Chris Ferrell, MT(ASCP), Joo Lee, MT(ASCP),
Laboratory Diagnosis of Lupus Inhibitors: A Comparison of the Tissue Thromboplastin Inhibition Procedure with a New Platelet Neutralization Procedure
 Laboratory Diagnosis of Lupus Inhibitors: A Comparison of the Tissue Thromboplastin Inhibition Procedure with a New Platelet Neutralization Procedure DOUGLAS A. TRIPLETT, M.D., JOHN T. BRANDT, M.D. JANIS
Laboratory Diagnosis of Lupus Inhibitors: A Comparison of the Tissue Thromboplastin Inhibition Procedure with a New Platelet Neutralization Procedure DOUGLAS A. TRIPLETT, M.D., JOHN T. BRANDT, M.D. JANIS
Introduction to coagulation and laboratory tests
 Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
Oral Factor Xa Inhibitors and Clinical Laboratory Monitoring
 Oral Factor Xa Inhibitors and Clinical Laboratory Monitoring MELISSA L. WHITE ABSTRACT Oral anticoagulation therapy is currently undergoing great changes with the development and use of several new medications.
Oral Factor Xa Inhibitors and Clinical Laboratory Monitoring MELISSA L. WHITE ABSTRACT Oral anticoagulation therapy is currently undergoing great changes with the development and use of several new medications.
T he antiphospholipid syndrome (APS) is a thrombophilic
 1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
Testing strategies for diagnosing lupus anticoagulant: decision analysis Segal J B, Lehmann H P, Petri M, Mueller L, Kickler T S
 Testing strategies for diagnosing lupus anticoagulant: decision analysis Segal J B, Lehmann H P, Petri M, Mueller L, Kickler T S Record Status This is a critical abstract of an economic evaluation that
Testing strategies for diagnosing lupus anticoagulant: decision analysis Segal J B, Lehmann H P, Petri M, Mueller L, Kickler T S Record Status This is a critical abstract of an economic evaluation that
Internal Quality Control in the Haemostasis laboratory. Dr Steve Kitchen Sheffield Haemophilia and Thrombosis centre & UK NEQAS Blood Coagulation
 Internal Quality Control in the Haemostasis laboratory Dr Steve Kitchen Sheffield Haemophilia and Thrombosis centre & UK NEQAS Blood Coagulation Why do we need Quality control? Philadelphia Enquirer Aug
Internal Quality Control in the Haemostasis laboratory Dr Steve Kitchen Sheffield Haemophilia and Thrombosis centre & UK NEQAS Blood Coagulation Why do we need Quality control? Philadelphia Enquirer Aug
Lupus Anticoagulant Testing Performance and Practices by North American Clinical Laboratories
 Coagulation and Transfusion Medicine / Lupus Anticoagulant Testing Lupus Anticoagulant Testing Performance and Practices by North American Clinical Laboratories Francine R. Dembitzer, MD, 1 Marlies R.
Coagulation and Transfusion Medicine / Lupus Anticoagulant Testing Lupus Anticoagulant Testing Performance and Practices by North American Clinical Laboratories Francine R. Dembitzer, MD, 1 Marlies R.
Stability of prothrombin time and activated partial thromboplastin time tests under different storage conditions
 Clinica Chimica Acta 300 (2000) 13 21 www.elsevier.com/ locate/ clinchim Stability of prothrombin time and activated partial thromboplastin time tests under different storage conditions L.V. Rao *, A.O.
Clinica Chimica Acta 300 (2000) 13 21 www.elsevier.com/ locate/ clinchim Stability of prothrombin time and activated partial thromboplastin time tests under different storage conditions L.V. Rao *, A.O.
PICT ANTICOAGULANT MONITORING 1. PEFAKIT PICT. Clotting Assay. PEFAKIT PiCT. PEFAKIT PICT Calibrators UFH. PEFAKIT PICT Controls UFH
 1 2 3 4 PEFAKIT PiCT PEFAKIT PICT Calibrators UFH PEFAKIT PICT Controls UFH PEFAKIT PICT Calibrators LMWH Clotting Assay PICT 1. PEFAKIT PICT Package size 8-505-01 kit 80 3 vials of PiCT Activator (2mL)
1 2 3 4 PEFAKIT PiCT PEFAKIT PICT Calibrators UFH PEFAKIT PICT Controls UFH PEFAKIT PICT Calibrators LMWH Clotting Assay PICT 1. PEFAKIT PICT Package size 8-505-01 kit 80 3 vials of PiCT Activator (2mL)
Instruments smart solutions & service IGZ Instruments AG Räffelstrasse 32 CH 8045 Zürich
 ADP (Adenosine-5 -Diphosphate) 101312 3 x 0.5mL ADP is a lyophilized preparation of adenosine-5 -diphosphate. The working concentration of the reconstituted reagent is 2 x 10-4 M. ADP is for use in routine
ADP (Adenosine-5 -Diphosphate) 101312 3 x 0.5mL ADP is a lyophilized preparation of adenosine-5 -diphosphate. The working concentration of the reconstituted reagent is 2 x 10-4 M. ADP is for use in routine
Interactive Case Vignette: DOACs (Direct Oral Anti-Coagulants) vs. Warfarin for APLA (Anti-Phospholipid Antibody Syndrome)
 Interactive Case Vignette: DOACs (Direct Oral Anti-Coagulants) vs. Warfarin for APLA (Anti-Phospholipid Antibody Syndrome) Ara Metjian, MD Duke Debates Benign Hematologic Highlights April 22, 2017 Disclaimer
Interactive Case Vignette: DOACs (Direct Oral Anti-Coagulants) vs. Warfarin for APLA (Anti-Phospholipid Antibody Syndrome) Ara Metjian, MD Duke Debates Benign Hematologic Highlights April 22, 2017 Disclaimer
Coagulation, Haemostasis and interpretation of Coagulation tests
 Coagulation, Haemostasis and interpretation of Coagulation tests Learning Outcomes Indicate the normal ranges for routine clotting screen and explain what each measurement means Recognise how to detect
Coagulation, Haemostasis and interpretation of Coagulation tests Learning Outcomes Indicate the normal ranges for routine clotting screen and explain what each measurement means Recognise how to detect
Antiphospholipid Syndrome ( APS)
 Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche
 L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
Comparison of Samples Obtained From 3.2% Sodium Citrate Glass and Two 3.2% Sodium Citrate Plastic Blood Collection Tubes Used in Coagulation Testing
 Coagulation and Transfusion Medicine / GLASS VS PLASTIC IN HEMOSTASIS TESTING Comparison of Samples Obtained From 3.2% Sodium Citrate Glass and Two 3.2% Sodium Citrate Plastic Blood Collection Tubes Used
Coagulation and Transfusion Medicine / GLASS VS PLASTIC IN HEMOSTASIS TESTING Comparison of Samples Obtained From 3.2% Sodium Citrate Glass and Two 3.2% Sodium Citrate Plastic Blood Collection Tubes Used
Anticoagulants. Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT
 Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Haemostasis Thrombosis Phases Endogenous anticoagulants Stopping blood loss Pathological formation of a haemostatic plug Arterial associated with atherosclerosis Venous blood stasis e.g. DVT Vascular Platelet
Optimal Utilization of Thrombophilia Testing
 Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
8. The use of calibrated thromboplastins in clinical practice 297 Authors 297 Acknowledgements 298 References 298 Appendix 1
 Annex 6 Guidelines for thromboplastins and plasma used to control oral anticoagulant therapy with vitamin K antagonists Replacement of Annex 3 of WHO Technical Report Series, No. 889 1. Introduction 273
Annex 6 Guidelines for thromboplastins and plasma used to control oral anticoagulant therapy with vitamin K antagonists Replacement of Annex 3 of WHO Technical Report Series, No. 889 1. Introduction 273
Primary Exam Physiology lecture 5. Haemostasis
 Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
AN INTERESTING CASE OF RESPIRATORY DISTRESS. Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai
 AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
Antiphospholipid Syndrome
 Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
Inherited Thrombophilia Testing. George Rodgers, MD, PhD Kristi Smock MD
 Inherited Thrombophilia Testing George Rodgers, MD, PhD Kristi Smock MD Prevalence and risk associated with inherited thrombotic disorders Inherited Risk Factor % General Population % Patients w/ Thrombosis
Inherited Thrombophilia Testing George Rodgers, MD, PhD Kristi Smock MD Prevalence and risk associated with inherited thrombotic disorders Inherited Risk Factor % General Population % Patients w/ Thrombosis
Appendix 3 PCC Warfarin Reversal
 Appendix 3 PCC Warfarin Reversal Reversal of Warfarin and Analogues 1. Principle of Procedure Guidelines for the Reversal of Oral-anticoagulation in the Event of Life Threatening Haemorrhage Prothrombin
Appendix 3 PCC Warfarin Reversal Reversal of Warfarin and Analogues 1. Principle of Procedure Guidelines for the Reversal of Oral-anticoagulation in the Event of Life Threatening Haemorrhage Prothrombin
Please note that the uses described in the following page(s) have not been approved or cleared by FDA, with respect to the described assay or test.
 Please note that the uses described in the following page(s) have not been approved or cleared by FDA, with respect to the described assay or test. In the US, the product is intended For Research Use Only.
Please note that the uses described in the following page(s) have not been approved or cleared by FDA, with respect to the described assay or test. In the US, the product is intended For Research Use Only.
Generate Knowledge Lupus Anticoagulant Testing Made Simple
 Generate Knowledge Lupus Anticoagulant Testing Made Simple Paul Riley, PhD, MBA Learning objectives Describe antiphospholipid syndrome (aps) and role of the lupus anticoagulant (LA) in thrombosis Present
Generate Knowledge Lupus Anticoagulant Testing Made Simple Paul Riley, PhD, MBA Learning objectives Describe antiphospholipid syndrome (aps) and role of the lupus anticoagulant (LA) in thrombosis Present
Laboratory monitoring of oral anticoagulants. A/Prof. Lee Lai Heng Haematology Singapore General Hospital
 Laboratory monitoring of oral anticoagulants A/Prof. Lee Lai Heng Haematology Singapore General Hospital Relevant Disclosures Educational and Travel Grants Bayer, Leo, Bristol Meyer Squib Advisory Boards
Laboratory monitoring of oral anticoagulants A/Prof. Lee Lai Heng Haematology Singapore General Hospital Relevant Disclosures Educational and Travel Grants Bayer, Leo, Bristol Meyer Squib Advisory Boards
Autoantibodies have been implicated in a variety of diseases.
 Antiphospholipid Antibodies Douglas A. Triplett, MD Objective. To review the role of lupus anticoagulants in the pathogenesis of both venous and arterial thromboembolic events, as well as in recurrent
Antiphospholipid Antibodies Douglas A. Triplett, MD Objective. To review the role of lupus anticoagulants in the pathogenesis of both venous and arterial thromboembolic events, as well as in recurrent
NEW ONE-STAGE PROCEDURES FOR THE QUANTITATIVE DETERMINATION OF PROTHROMBIN AND LABILE FACTOR*
 NEW ONE-STAGE PROCEDURES FOR THE QUANTITATIVE DETERMINATION OF PROTHROMBIN AND LABILE FACTOR* MARIO STEFANINI, M.D.f From the Department ofbiochemistry, Marquette University School of Medicine, Milwaukee,
NEW ONE-STAGE PROCEDURES FOR THE QUANTITATIVE DETERMINATION OF PROTHROMBIN AND LABILE FACTOR* MARIO STEFANINI, M.D.f From the Department ofbiochemistry, Marquette University School of Medicine, Milwaukee,
SYNOPSIS Prothrombin, both by a one- and a two-stage method, and progressive
 J. clin. Path., 197, 23, 291-295 Estimation of prothrombin in liver disease P. M. MANNUCCI From the University Institute of Medical Pathology, Ospedale Policlinico, Milan, Italy SYNOPSIS Prothrombin, both
J. clin. Path., 197, 23, 291-295 Estimation of prothrombin in liver disease P. M. MANNUCCI From the University Institute of Medical Pathology, Ospedale Policlinico, Milan, Italy SYNOPSIS Prothrombin, both
The LaboratoryMatters
 Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
SENSITIVITY OF DIFFERENT THROMBOPLASTIN REAGENTS TO FACTOR VII DEFICIENCY IN THE BLOOD OF BEAGLE DOGS
 Laboratory Animals (1970) 4, 55-59. 55 SENSITIVITY OF DIFFERENT THROMBOPLASTIN REAGENTS TO FACTOR VII DEFICIENCY IN THE BLOOD OF BEAGLE DOGS by D. E. HALL Biological Research Department, BDH (Research)
Laboratory Animals (1970) 4, 55-59. 55 SENSITIVITY OF DIFFERENT THROMBOPLASTIN REAGENTS TO FACTOR VII DEFICIENCY IN THE BLOOD OF BEAGLE DOGS by D. E. HALL Biological Research Department, BDH (Research)
Guidance for management of bleeding in patients taking the new oral anticoagulant drugs: rivaroxaban, dabigatran or apixaban
 Guidance for management of bleeding in patients taking the new oral anticoagulant drugs: rivaroxaban, dabigatran or apixaban Purpose The aim of this guidance is to outline the management of patients presenting
Guidance for management of bleeding in patients taking the new oral anticoagulant drugs: rivaroxaban, dabigatran or apixaban Purpose The aim of this guidance is to outline the management of patients presenting
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) CORE SPC FOR HUMAN PROTHROMBIN COMPLEX PRODUCTS (CPMP/BPWG/3735/02)
 European Medicines Agency Human Medicines Evaluation Unit London, 21 October 2004 Corrigendum, 18 November 2004 CPMP/BPWG/3735/02 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) CORE SPC FOR HUMAN
European Medicines Agency Human Medicines Evaluation Unit London, 21 October 2004 Corrigendum, 18 November 2004 CPMP/BPWG/3735/02 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) CORE SPC FOR HUMAN
Diagnosis of hypercoagulability is by. Molecular markers
 Agenda limitations of clinical laboratories to evaluate hypercoagulability and the underlying cause for thrombosis what is the INR the lupus anticoagulant and the antiphospholipid antibody syndrome hassouna
Agenda limitations of clinical laboratories to evaluate hypercoagulability and the underlying cause for thrombosis what is the INR the lupus anticoagulant and the antiphospholipid antibody syndrome hassouna
Behzad Poopak, DCLS PhD
 Behzad Poopak, DCLS PhD Test Report Name Age Critical Low HEMATOLOGY Activated Partial Thromboplastin Time, Plasma Critical High - 150 sec Units Fibrinogen 60 - mg/dl INR (International Normalizing
Behzad Poopak, DCLS PhD Test Report Name Age Critical Low HEMATOLOGY Activated Partial Thromboplastin Time, Plasma Critical High - 150 sec Units Fibrinogen 60 - mg/dl INR (International Normalizing
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
M B Garvey. University of Toronto
 Do I really need that test??? M B Garvey Professor Emeritus University of Toronto St Michael s Hospital No relevant conflicts of interest 1 HEMOSTASIS IS LIKE LOVE Everybody talks about it, nobody understands
Do I really need that test??? M B Garvey Professor Emeritus University of Toronto St Michael s Hospital No relevant conflicts of interest 1 HEMOSTASIS IS LIKE LOVE Everybody talks about it, nobody understands
Factor VIII Inhibitor Testing: Nijmegen Modifications, Experience and Recommendations
 Factor VIII Inhibitor Testing: Nijmegen Modifications, Experience and Recommendations Bert Verbruggen Radboud University Nijmegen Medical Centre The Netherlands 2-12-2008 DISCLOSURE None 2-12-2008 2 ECAT
Factor VIII Inhibitor Testing: Nijmegen Modifications, Experience and Recommendations Bert Verbruggen Radboud University Nijmegen Medical Centre The Netherlands 2-12-2008 DISCLOSURE None 2-12-2008 2 ECAT
Material and methods. Venous blood was taken from hospital patients, using. a butterfly needle (21 gauge; Abbott Laboratories,
 Evaluation of sealed vacuum extraction method (Seditainer) for measurement of erythrocyte sedimentation rate J Clin Pathol 1989;42:313-317 W N PTTON, P J MEYER, J STURT* *Department ofhaematology, Medical
Evaluation of sealed vacuum extraction method (Seditainer) for measurement of erythrocyte sedimentation rate J Clin Pathol 1989;42:313-317 W N PTTON, P J MEYER, J STURT* *Department ofhaematology, Medical
Evaluation Report. Eurolyser PT (INR) test kit (ST0180) on CUBE and smart analysers
 Evaluation Report Eurolyser PT test kit (ST0180) on CUBE and smart analysers Locations Location 1: Eurolyser Diagnostica GmbH Operator: Simone Wieser Date: 30.06.2015 Specimens The specimens used for analysis
Evaluation Report Eurolyser PT test kit (ST0180) on CUBE and smart analysers Locations Location 1: Eurolyser Diagnostica GmbH Operator: Simone Wieser Date: 30.06.2015 Specimens The specimens used for analysis
A Case of Factor XII Deficiency Which was Found in Recurrent Spontaneous Abortion. Y. S. Nam, I. H. Kim, T. K. Yoon, C. N. Lee and K. Y.
 12 1 A Case of Factor XII Deficiency Which was Found in Recurrent Spontaneous Abortion Y S Nam, I H Kim, T K Yoon, C N Lee and K Y Cha Department of Obstetrics and Gynecology, College of Medicine, Pocheon
12 1 A Case of Factor XII Deficiency Which was Found in Recurrent Spontaneous Abortion Y S Nam, I H Kim, T K Yoon, C N Lee and K Y Cha Department of Obstetrics and Gynecology, College of Medicine, Pocheon
Inhibition by Human Thrombomodulin of Factor Xa-mediated Cleavage of Prothrombin
 Inhibition by Human Thrombomodulin of Factor Xa-mediated Cleavage of Prothrombin E. Anne Thompson and Hatem H. Salem Department ofmedicine, Monash Medical School, Prahran, 3181, Victoria, Australia Abstract
Inhibition by Human Thrombomodulin of Factor Xa-mediated Cleavage of Prothrombin E. Anne Thompson and Hatem H. Salem Department ofmedicine, Monash Medical School, Prahran, 3181, Victoria, Australia Abstract
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT 500 IU powder and solvent for solution for infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION is presented as a powder and solvent
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT 500 IU powder and solvent for solution for infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION is presented as a powder and solvent
Activation of Factor IX by the reaction product of tissue factor and
 Proc. Natl. Acad. Sci. USA Vol. 74, No. 12, pp. 5260-5264, December 1977 Biochemistry Activation of Factor IX by the reaction product of tissue factor and Factor VII: Additional pathway for initiating
Proc. Natl. Acad. Sci. USA Vol. 74, No. 12, pp. 5260-5264, December 1977 Biochemistry Activation of Factor IX by the reaction product of tissue factor and Factor VII: Additional pathway for initiating
Antiphospholipid antibodies
 CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
Thrombophilia: To test or not to test
 Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Causes of isolated prolonged activated partial thromboplastin time in an acute care general hospital
 O r i g i n a l A r t i c l e Singapore Med J 2005; 46(9) : 450 Causes of isolated prolonged activated partial thromboplastin time in an acute care general hospital W J Chng, C Sum, P Kuperan Department
O r i g i n a l A r t i c l e Singapore Med J 2005; 46(9) : 450 Causes of isolated prolonged activated partial thromboplastin time in an acute care general hospital W J Chng, C Sum, P Kuperan Department
patients with systemic lupus erythematosus
 332 Institute of Clinical Medicine I, University of Rome "La Sapienza," Rome, Italy D Ferro M Saliola C Quintarelli G Valesini S Basili A M Grandilli M S Bonavita F Violi Correspondence to: Dr Francesco
332 Institute of Clinical Medicine I, University of Rome "La Sapienza," Rome, Italy D Ferro M Saliola C Quintarelli G Valesini S Basili A M Grandilli M S Bonavita F Violi Correspondence to: Dr Francesco
Insights on the Quality of Coagulation Testing
 Insights on the Quality of Coagulation Testing Piet Meijer ECAT Foundation The Netherlands No conflicts of interest HAEMOSTATIC BALANCE BLEEDING HAEMOSTATIC BALANCE THROMBOSIS HAEMOSTATIC BALANCE Thrombosis
Insights on the Quality of Coagulation Testing Piet Meijer ECAT Foundation The Netherlands No conflicts of interest HAEMOSTATIC BALANCE BLEEDING HAEMOSTATIC BALANCE THROMBOSIS HAEMOSTATIC BALANCE Thrombosis
Active date July Ratification date: Review date January 2014 Applies to: Staff managing patients on warfarin. Exclusions:
 Guideline Title: Guidelines for the management of warfarin reversal [key words : Beriplex, Octaplex, PCC, vitamin K, anticoagulant, anticoagulation] Authors: Dr Sarah Allford, Consultant Haematologist
Guideline Title: Guidelines for the management of warfarin reversal [key words : Beriplex, Octaplex, PCC, vitamin K, anticoagulant, anticoagulation] Authors: Dr Sarah Allford, Consultant Haematologist
(4-7). Such variations might be technical
 DEVELOPMENT OF INCREASED FACTOR VII ACTIVITY DURING THE SPONTANEOUS COAGULATION OF BLOOD By CHARLES L. JOHNSTON, JR.* AND PETER F. HJORT (From the Institute for Thrombosis Research, University Hospital
DEVELOPMENT OF INCREASED FACTOR VII ACTIVITY DURING THE SPONTANEOUS COAGULATION OF BLOOD By CHARLES L. JOHNSTON, JR.* AND PETER F. HJORT (From the Institute for Thrombosis Research, University Hospital
Save My Exams! The Home of Revision For more awesome GCSE and A level resources, visit us at Heart & Circulation
 Heart & Circulation Question Paper 3 Level International A Level Subject Biology Exam Board Edexcel Topic Molecules, Transport and Health Sub-Topic Heart & Circulation Booklet Question paper 3 Time Allowed:
Heart & Circulation Question Paper 3 Level International A Level Subject Biology Exam Board Edexcel Topic Molecules, Transport and Health Sub-Topic Heart & Circulation Booklet Question paper 3 Time Allowed:
Heparin neutralizing activity test in the diagnosis
 J. clin. Path., 1975, 28, 975-979 Heparin neutralizing activity test in the diagnosis of acute myocardial infarction J. R. O'BRIEN, M. ETHERINGTON, SANDRA JAMIESON, P. LAWFORD, JANET SUSSEX, AND S. V.
J. clin. Path., 1975, 28, 975-979 Heparin neutralizing activity test in the diagnosis of acute myocardial infarction J. R. O'BRIEN, M. ETHERINGTON, SANDRA JAMIESON, P. LAWFORD, JANET SUSSEX, AND S. V.
The effect of the direct oral anticoagulants (DOACs) on haemostasis tests.
 The effect of the direct oral anticoagulants (DOACs) on haemostasis tests. Emmanuel J Favaloro, Haematology, ICPMR, Pathology West, Sydney Centres for Thrombosis and Haemostasis, Westmead Hospital (with
The effect of the direct oral anticoagulants (DOACs) on haemostasis tests. Emmanuel J Favaloro, Haematology, ICPMR, Pathology West, Sydney Centres for Thrombosis and Haemostasis, Westmead Hospital (with
Name and Intended Use
 Name and Intended Use Anti-Prothrombin IgG/IgM is an indirect solid phase enzyme immunoassay (ELISA) for the quantitative measurement of IgG and IgM class autoantibodies against Prothrombin in human serum
Name and Intended Use Anti-Prothrombin IgG/IgM is an indirect solid phase enzyme immunoassay (ELISA) for the quantitative measurement of IgG and IgM class autoantibodies against Prothrombin in human serum
Prothrombin (Human) ELISA Kit
 Prothrombin (Human) ELISA Kit Catalog Number KA0496 96 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay... 3 General
Prothrombin (Human) ELISA Kit Catalog Number KA0496 96 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay... 3 General
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Single Technology Appraisal (STA)
 Thank you for agreeing to give us a statement on your organisation s view of the technology and the way it should be used in the NHS. Healthcare professionals can provide a unique perspective on the technology
Thank you for agreeing to give us a statement on your organisation s view of the technology and the way it should be used in the NHS. Healthcare professionals can provide a unique perspective on the technology
Measuring IgG anti-a/b titres using dithiothreitol (DTT)
 Measuring IgG anti-a/b titres using dithiothreitol (DTT) R. C. KNIGHT From the Department of Haematology, St Thomas's Hospital, London SEJ Journal of Clinical Pathology, 1978, 31, 283-287 SUMMARY In comparing
Measuring IgG anti-a/b titres using dithiothreitol (DTT) R. C. KNIGHT From the Department of Haematology, St Thomas's Hospital, London SEJ Journal of Clinical Pathology, 1978, 31, 283-287 SUMMARY In comparing
NOACS/DOACS*: COAGULATION TESTS
 NOACS/DOACS*: COAGULATION TESTS OBJECTIVES: To describe the effect of the newer direct oral anticoagulants (DOACs) on laboratory coagulation tests which are widely available: prothrombin time (PT), international
NOACS/DOACS*: COAGULATION TESTS OBJECTIVES: To describe the effect of the newer direct oral anticoagulants (DOACs) on laboratory coagulation tests which are widely available: prothrombin time (PT), international
Andexanet Alfa: Reversal agent for FXa Inhibitors
 Andexanet Alfa: Reversal agent for FXa Inhibitors Grace Gilmore, Prof Ross Baker, Dr Jim Tiao, Dr Quintin Hughes, Dr Jasmine Tay, Scott McGregor WA Centre for Thrombosis and Haemostasis, Murdoch University,
Andexanet Alfa: Reversal agent for FXa Inhibitors Grace Gilmore, Prof Ross Baker, Dr Jim Tiao, Dr Quintin Hughes, Dr Jasmine Tay, Scott McGregor WA Centre for Thrombosis and Haemostasis, Murdoch University,
POM. SUMMARY OF PRODUCT CHARACTERISTICS UK Specific
 (500 IU coagulation (human factor IX prothrombin per vial, powder complex) and solvent for infusion Human Prothrombin Complex) POM SUMMARY OF PRODUCT CHARACTERISTICS UK Specific Octapharma Limited The
(500 IU coagulation (human factor IX prothrombin per vial, powder complex) and solvent for infusion Human Prothrombin Complex) POM SUMMARY OF PRODUCT CHARACTERISTICS UK Specific Octapharma Limited The
ANTICOAGULANT THERAPY
 J. cliti. Path. (1958), 11, 62. OWREN'S METHOD FOR THE CONTROL OF ANTICOAGULANT THERAPY BY M. J. ALLINGTON From the Departmenit of Haematology, Radcliffe Infirnmary, Oxford (RECEIVED FOR PUBLICATION OCTOBER
J. cliti. Path. (1958), 11, 62. OWREN'S METHOD FOR THE CONTROL OF ANTICOAGULANT THERAPY BY M. J. ALLINGTON From the Departmenit of Haematology, Radcliffe Infirnmary, Oxford (RECEIVED FOR PUBLICATION OCTOBER
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION IN ADULTS RECEIVING ANTI-COAGULANTS
 Hairmyres Hospital MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION IN ADULTS RECEIVING ANTI-COAGULANTS Bleeding in patients on anticoagulants, even in the absence of over-anticoagulation, can be life-threatening
Hairmyres Hospital MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION IN ADULTS RECEIVING ANTI-COAGULANTS Bleeding in patients on anticoagulants, even in the absence of over-anticoagulation, can be life-threatening
DISCLOSURE. Presented by: Merav Sendowski, MD Oregon Health and Science University
 Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
The Assay and Properties of Labile Factor (Factor V)
 Marquette University e-publications@marquette Biomedical Sciences Faculty Research and Publications Health Sciences, College of -1-1960 The Assay and Properties of Labile Factor (Factor V) Armand J. Quick
Marquette University e-publications@marquette Biomedical Sciences Faculty Research and Publications Health Sciences, College of -1-1960 The Assay and Properties of Labile Factor (Factor V) Armand J. Quick
Coagulation an Overview Dr.Abdolreza Abdolr Afrasiabi Thal assem a & Heamophili hilia G ene i tic R esearc C en er Shiraz Medical Medic University
 In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
Dr Shikha Chattree Haematology Consultant Sunderland Royal infirmary
 Dr Shikha Chattree Haematology Consultant Sunderland Royal infirmary Increasing use of Novel Oral Anticoagulants (NOACs) in the management of prophylaxis and management of venous thromboembolism and in
Dr Shikha Chattree Haematology Consultant Sunderland Royal infirmary Increasing use of Novel Oral Anticoagulants (NOACs) in the management of prophylaxis and management of venous thromboembolism and in
Coagulation disorders (thrombophilias) are a rare but
 Physician Knowledge and Practices in the Evaluation of Coagulopathies in Stroke Patients Cheryl D. Bushnell, MD, MHS; Larry B. Goldstein, MD Background and Purpose Coagulopathies are a rare cause of ischemic
Physician Knowledge and Practices in the Evaluation of Coagulopathies in Stroke Patients Cheryl D. Bushnell, MD, MHS; Larry B. Goldstein, MD Background and Purpose Coagulopathies are a rare cause of ischemic
COAGULANT THERAPY. of in-patients on anticoagulant treatment. As a. 24, or even more, hours earlier than did
 J. clin. Path. (1958), 11, 56. COMPARISON OF QUICK'S, OWREN'S, AND WARE'S TECHNIQUES FOR THE CONTROL OF ANTI- COAGULANT THERAPY BY M. TOOHEY From tize Aniticoagulanit Unit, New End Hospital, Lonidoni,
J. clin. Path. (1958), 11, 56. COMPARISON OF QUICK'S, OWREN'S, AND WARE'S TECHNIQUES FOR THE CONTROL OF ANTI- COAGULANT THERAPY BY M. TOOHEY From tize Aniticoagulanit Unit, New End Hospital, Lonidoni,
Blood clotting. Subsequent covalent cross-linking of fibrin by a transglutaminase (factor XIII) further stabilizes the thrombus.
 Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Blood clotting It is the conversion, catalyzed by thrombin, of the soluble plasma protein fibrinogen (factor I) into polymeric fibrin, which is deposited as a fibrous network in the primary thrombus. Thrombin
Further study has tended to confirm this interpretation.
 PROPERTIES OF AN ANTICOAGULANT FOUND IN THE BLOOD OF A HEMOPHILIAC By F. L. MUNRO (From the Charlotte Drake Cardeza Foundation, Department of Medicine, College and Hospital, Philadelphia) Jefferson Medical
PROPERTIES OF AN ANTICOAGULANT FOUND IN THE BLOOD OF A HEMOPHILIAC By F. L. MUNRO (From the Charlotte Drake Cardeza Foundation, Department of Medicine, College and Hospital, Philadelphia) Jefferson Medical
Blood transfusion. Dr. J. Potgieter Dept. of Haematology NHLS - TAD
 Blood transfusion Dr. J. Potgieter Dept. of Haematology NHLS - TAD General Blood is collected from volunteer donors >90% is separated into individual components and plasma Donors should be: healthy, have
Blood transfusion Dr. J. Potgieter Dept. of Haematology NHLS - TAD General Blood is collected from volunteer donors >90% is separated into individual components and plasma Donors should be: healthy, have
Recommendations for Celiac Disease Testing. IgA & ttg IgA
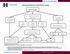 Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
THROMBOPHILIA SCREENING
 THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
G. I. C. INGRAM* AND ROSEMARY BIGGS with analyses by P. ARMITAGE (RECEIVED FOR PUBLICATION AUGUST 15, 1952)
 J. clin. Path. (1953), 6, 46. LABORATORY TESTS FOR INCIPIENT THROMBOSIS BY G. I. C. INGRAM* AND ROSEMARY BIGGS with analyses by P. ARMITAGE From the Department of Surgery, University of Edinburgh, the
J. clin. Path. (1953), 6, 46. LABORATORY TESTS FOR INCIPIENT THROMBOSIS BY G. I. C. INGRAM* AND ROSEMARY BIGGS with analyses by P. ARMITAGE From the Department of Surgery, University of Edinburgh, the
Human coagulation factor Xa, FXa ELISA Kit
 Human coagulation factor Xa, FXa ELISA Kit Catalog No: E1613h 96 Tests Operating instruction www.eiaab.com FOR RESEARCH USE ONLY; NOT FOR THERAPEUTIC OR DIAGNOSTIC APPLICATIONS! PLEASE READ THROUGH ENTIRE
Human coagulation factor Xa, FXa ELISA Kit Catalog No: E1613h 96 Tests Operating instruction www.eiaab.com FOR RESEARCH USE ONLY; NOT FOR THERAPEUTIC OR DIAGNOSTIC APPLICATIONS! PLEASE READ THROUGH ENTIRE
approach Local INR correction: justification for a simplified Results-All system groups required correction, logarithm of local prothrombin time
 3 Clin Pathol 1997;5:73-79 Thrombosis Reference Centre, Withington Hospital, Manchester, M 2LR, UK Correspondence to: Mr Craig. Accepted for publication June 1997 Local correction: justification for a
3 Clin Pathol 1997;5:73-79 Thrombosis Reference Centre, Withington Hospital, Manchester, M 2LR, UK Correspondence to: Mr Craig. Accepted for publication June 1997 Local correction: justification for a
Point of Care Testing in Coagulation
 Point of Care Testing in Coagulation Dr Steve Kitchen Scientific Director,UK NEQAS Blood Coagulation Head Scientist Coagulation Laboratory, Royal Hallamshire Hospital Sheffield UK POCT in Haemostasis Patient
Point of Care Testing in Coagulation Dr Steve Kitchen Scientific Director,UK NEQAS Blood Coagulation Head Scientist Coagulation Laboratory, Royal Hallamshire Hospital Sheffield UK POCT in Haemostasis Patient
HbA1c (Human) ELISA Kit
 HbA1c (Human) ELISA Kit Cat. No.:DEIA3509 Pkg.Size:96T Intended use GHbA1c (Human) ELISA Kit is a sandwich enzyme immunoassay for the quantitative measurement of human GHbA1c. General Description vhemoglobin,
HbA1c (Human) ELISA Kit Cat. No.:DEIA3509 Pkg.Size:96T Intended use GHbA1c (Human) ELISA Kit is a sandwich enzyme immunoassay for the quantitative measurement of human GHbA1c. General Description vhemoglobin,
Challenges in Coagulation
 Challenges in Coagulation Michael H. Rosove, MD Clinical Professor of Medicine UCLA Division of Hematology-Oncology April 30, 2016 Vitamin K Deficiency Vitamin K1 source from diet Vitamin K2 source from
Challenges in Coagulation Michael H. Rosove, MD Clinical Professor of Medicine UCLA Division of Hematology-Oncology April 30, 2016 Vitamin K Deficiency Vitamin K1 source from diet Vitamin K2 source from
have been examined. Six specimens of normal synovial membrane were also examined. SYNOVIAL MEMBRANE EXTRACTS
 J Clin Pathol 1982;35:673-680 Anticoagulant antibodies in the synovial membranes of patients suffering from haemophilia, rheumatoid arthritis and other rheumatic disorders SG RAINSFORD, A ARONSTAM, EJ
J Clin Pathol 1982;35:673-680 Anticoagulant antibodies in the synovial membranes of patients suffering from haemophilia, rheumatoid arthritis and other rheumatic disorders SG RAINSFORD, A ARONSTAM, EJ
Mouse HBsAg(Hepatitis B Virus Surface Antigen) ELISA Kit
 Mouse HBsAg(Hepatitis B Virus Surface Antigen) ELISA Kit Catalogue No.: EM0002 Size: 96T Reactivity: Mouse Application: This immunoassay kit allows for the qualitative determination of HBsAg in Mouse serum
Mouse HBsAg(Hepatitis B Virus Surface Antigen) ELISA Kit Catalogue No.: EM0002 Size: 96T Reactivity: Mouse Application: This immunoassay kit allows for the qualitative determination of HBsAg in Mouse serum
Collection of Blood Specimens by Venipuncture for Plasma-Based Coagulation Assays Necessity of a Discard Tube
 Coagulation and Transfusion Medicine / Discard Tube Unnecessary for Coagulation Assays Collection of Blood Specimens by Venipuncture for Plasma-Based Coagulation Assays Necessity of a Discard Tube Maarten
Coagulation and Transfusion Medicine / Discard Tube Unnecessary for Coagulation Assays Collection of Blood Specimens by Venipuncture for Plasma-Based Coagulation Assays Necessity of a Discard Tube Maarten
GUIDELINES FOR MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION WITH ORAL ANTICOAGULANTS
 GUIDELINES FOR MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION WITH ORAL ANTICOAGULANTS This guideline covers the management of patients being treated with Vitamin K antagonists (VKA): Warfarin Acenocoumarol
GUIDELINES FOR MANAGEMENT OF BLEEDING AND EXCESSIVE ANTICOAGULATION WITH ORAL ANTICOAGULANTS This guideline covers the management of patients being treated with Vitamin K antagonists (VKA): Warfarin Acenocoumarol
Human Prothrombin Complex (PCC) (Beriplex P/N) in the emergency reversal of anticoagulation BCSLS Congress 2012 Kamloops, BC
 Human Prothrombin Complex (PCC) (Beriplex P/N) in the emergency reversal of anticoagulation BCSLS Congress 2012 Kamloops, BC Ayman Kafal Medical Affairs, Leader CSL Behring Canada 1 Prothrombin Complex
Human Prothrombin Complex (PCC) (Beriplex P/N) in the emergency reversal of anticoagulation BCSLS Congress 2012 Kamloops, BC Ayman Kafal Medical Affairs, Leader CSL Behring Canada 1 Prothrombin Complex
Major Haemorrhage Protocol. Commentary
 Hairmyres Hospital Monklands Hospital Wishaw General Hospital Major Haemorrhage Protocol Commentary N.B. There is a separate NHSL protocol for the Management of Obstetric Haemorrhage Authors Dr Tracey
Hairmyres Hospital Monklands Hospital Wishaw General Hospital Major Haemorrhage Protocol Commentary N.B. There is a separate NHSL protocol for the Management of Obstetric Haemorrhage Authors Dr Tracey
