CHRONIC PATELLOFEMORAL INSTABILITY
|
|
|
- Alison Wilson
- 5 years ago
- Views:
Transcription
1 INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation procedure may be selected. The emphasis is on a selective approach, rather than the use of one operation for all unstable patellae regardless of cause. DYNAMICS OF THE PATELLOFEMORAL JOINT The patellofemoral joint is intrinsically unstable because the tibial tubercle lies lateral to the long axis of the femur and the quadriceps muscle, and the patella is therefore subject to a laterally directed force. This apparent design fault is minimised by the resistance of the lateral lip of the trochlea to lateral movement of the patella during flexion (Brattström 1964). In full extension the patella lies at the upper end of the trochlea and enters its groove as flexion begins. It is important for stability that it should engage the trochlea correctly. Once engaged, the patella is held in place by two mechanisms. The first is its contact with the lateral edge of the trochlea, which acts as a lateral buffer, and the second is the soft-tissue tension which prevents it slipping laterally. In the normal knee, from 0 to 30 of flexion, the median ridge of the patella lies lateral to the centre of the trochlea; it moves medially to become centred in the trochlear groove at between 30 and 60 of flexion. As flexion proceeds the patella is more deeply engaged in the trochlea and is held firmly by soft-tissue tension. When the knee is flexed beyond 90, it tilts so that its medial facet articulates with the medial femoral condyle. Failure to stay in the trochlea. Sometimes the patella engages correctly at the start of the flexion but subluxes or dislocates as flexion proceeds. This may be due to a defective lateral trochlear margin or an unusually shallow trochlear groove. The laterally directed force applied to the patella is greater if the knee is in excessive valgus. Soft-tissue imbalance from excessively tight lateral structures or deficient medial structures can also increase the laterally directed force. The lateral structures may be tight from fibrosis of the vastus lateralis (Lloyd-Roberts and Thomas 1964) or for no obvious reason. The medial structures may be loose after injury to the medial retinaculum, from stretching after repeated dislocations or from severe wasting of the vastus medialis. ASSESSMENT The purpose of assessment is to identify the factors causing instability so that appropriate treatment may be selected. FACTORS LEADING TO PATELLAR INSTABILITY Poor engagement. If the patella fails to engage securely in the trochlea at the start of flexion it will slip laterally and as flexion continues will either dislocate completely or slip back medially to its correct position. Failure to engage may be due to an abnormally high patella, patellar dysplasia (Fig. 1) or a poorly developed trochlea. The consequences of a high patella and a proximally deficient trochlea are the same; the patella is not securely engaged at the start of flexion. D. J. Dandy, MD, MChir, FRCS, Consultant Orthopaedic Surgery Addenbrooke's Hospital, Hills Road, Cambridge CB2 2QQ, UK. Printed with the permission of EFORT. The article appears in European Instructional Course Lectures Vol. 2, Fig. 1 A dysplastic patella. 328 THE JOURNAL OF BONE AND JOINT SURGERY
2 329 Assessment follows the usual procedure of a clinical history, clinical examination and investigation. History. The history will reveal whether the symptoms began with a sudden traumatic event. The circumstances of the dislocation are also important. Does it occur with every flexion of the knee or only with twisting movements? Is there a particular movement which causes dislocation? It is also important to know the effect of the symptoms on the patient s way of life. There is little point in advising a major operation, with a prolonged period of rehabilitation, if the dislocations cause only minor inconvenience. Clinical examination. The patella is observed while the patient flexes the knee to see if it engages smoothly at the proximal end of the trochlea or more distally than normal. Does the knee flex fully or is flexion restricted by tight structures? Tests are required for generalised ligament laxity and for abnormally loose patellar retinacula. Patellar stability is assessed by gently pushing the patella laterally while flexing the knee. If the patient is apprehensive when this is done, the problem is poor patellar engagement. Sideways movement of the patella also allows the lateral and medial structures to be assessed. The Q-angle between the long axes of the quadriceps and the patellar tendon (Fig. 2) is a poor indication of the lateral forces on the patella. It is better to measure the position of the tibial tubercle with respect to the mid-line of the trochlea. With the knee flexed to 90 the tibial tubercle should lie less than 20 mm lateral to the mid-line of the femur at the upper edge of the femoral condyles; more than 20 mm indicates an abnormally lateral tubercle. Fig. 2 The Q-angle. Fig. 3a Fig. 3b Indices of patellar height: (a) the Insall-Salvati index and (b) the Blackburne-Peel index. Patellar height can be measured most accurately on radiographs. The patella is usually a little shorter than the patellar tendon and a rough estimate can be made clinically. Radiological measurements of patellar height. There are many methods of measuring the height of the patella on radiographs. The Insall-Salvati index (1971) (Fig. 3a), which compares the length of the patella with the length of the patellar tendon (men 0.9 to 1.1, women 0.94 to 1.18), is popular but it has a number of practical disadvantages. The point of attachment of the tendon to the tibia is indistinct, and measurements are difficult to make after transposition of the tibial tubercle. Furthermore, the length of the patella is not always an indication of the length of its articular surface. The Blackburne and Peel index (1977) (Fig. 3b) relates the length of the articular surface of the patella to the distance of its inferior margin from the tibial plateau (men 0.85 to 1.09, women 0.79 to 1.09). It provides a more useful measure of the relationship of the patella to the trochlea than the Insall-Salvati index. Observations on a true lateral radiograph. Déjour et al (1994) have shown that a true lateral radiograph can provide much information about the anatomy of the femoral trochlea. The base of the trochlea can be seen as a radiodense line which is in direct continuity with the anterior cortex of the femur (Fig. 4). Several abnormal variants are seen. The crossing sign. If the line indicating the floor of the trochlea crosses the lateral lip of the trochlea (Figs 5b and 6), the trochlea is deficient proximally and the patella may not engage correctly. The bump sign. If the radiological line linking the anterior cortex of the femur and the floor of the trochlea is convex and has a bump, engagement of the patella will also be incorrect. A bump of more than 3 mm is abnormal (Déjour et al 1994). Dysplastic condyles. These may be indicated by an abnor- VOL. 78-B, NO. 2, MARCH 1996
3 330 D. J. DANDY Fig. 5a Fig. 5b Fig. 5c Outlines of true lateral radiographs to show (a) normal appearance (b) a crossing sign with a bump and (c) a shallow trochlea. Fig. 4 A normal true lateral radiograph. Fig. 6 True lateral radiograph showing a crossing sign. Fig. 7 True lateral radiograph showing a dysplastic trochlea. mal appearance of the lateral lip of the trochlea; there is often a small beak or spike at its upper end (see Fig. 7). Trochlear depth. The depth of the trochlea can be measured; the normal mean depth is 7.8 mm (Déjour et al 1994). A shallow trochlea (Fig. 5c) may be insufficient to prevent the patella dislocating laterally even if it engages correctly at the start of flexion. Relationship of the tibial tubercle to the trochlea. Goutallier, Bernageau and Lecudonnec (1978) described the relationship between the centre of the trochlea and the tibial tubercle on axial radiographs. These measurements can be made more accurately by CT. In normal subjects, the distance between the centre of the trochlea and the tibial tubercle is 10 to 15 mm (Fig. 8). Patellar angle. MRI or CT gives more reliable information about the condition of the trochlea and the angle of the patella than tangential radiographs (Merchant et al 1974). Lateral tilting of the patella indicates tight lateral structures. Q-angle. The Q-angle is a useful dynamic concept but an unreliable measurement, because an unstable patella lies more laterally than normal in full extension thereby decreasing the angle. CT has shown that the Q-angle measured from the centre of the patella is actually less in patients with unstable patellae than in normal subjects; if it is measured from the centre of the trochlea, it is greater in patients with unstable patellae, as would be expected. Arthroscopy. This is not needed to diagnose patellar THE JOURNAL OF BONE AND JOINT SURGERY
4 331 osteoarthritis. The presence of the latter indicates a poor prognosis. Fig. 8 A tracing of superimposed CT scans showing the relationship of the tibial crest and the femoral trochlea. The section of the tibia is stippled. instability but it is a valuable preliminary to surgical stabilisation. From the medial or suprapatellar approach the patella can be seen engaging in the trochlea. A normal patella centres at between 30 and 60 of flexion. Failure to centre in a normal trochlea suggests tight lateral structures. The contours of the trochlea and of the patella can be seen directly. A dysplastic or flattened trochlea can be seen clearly and the problems of achieving stability assessed. Lastly, the joint surfaces can be examined. Vertical fissures resembling the side of a clinker-built boat (Dandy 1984; Dandy and Griffiths 1989) are almost diagnostic of patellar instability and may be the first signs of progressive SELECTING THE OPERATION Many procedures have been described for stabilising the patella. Broadly speaking, they can be classed as distal realignments to transpose the tibial tubercle, or proximal realignments to alter the tension of the tissues attached to the patella. When selecting an operation it is important to choose the procedure which will correct the underlying problem in the individual patient; the precise technique is less important. It is wrong to use one procedure on all patients regardless of the underlying cause of dislocation. Distal realignment. This is required if the patella is abnormally high and the trochlea normal. It is achieved by transferring the tibial tubercle far enough distally to allow the patella to engage correctly in the trochlea and to bring the Blackburne-Peel index to the lower end of its normal range (Fig. 9). The amount of transposition required is variable but is usually between 10 and 20 mm. Distal transposition may also be needed if the trochlea is deficient at its upper end even although this may bring the index of patellar height below the lower limit of its normal range. Techniques for lifting the tibial tubercle anteriorly at the time of transposition, based on the work of Maquet (1976) in patients with patellofemoral osteoarthritis, are not applicable to patellofemoral instability. Moving the tibial tubercle anteriorly must reduce patellar stability (Fig. 10). Medial transposition. This is indicated if the tubercle lies too far laterally and is usually done as part of a distal Lateral radiographs before (a) and after (b) distal tibial tubercle transposition in a patient with a high patella and a shallow trochlea. Fig. 9a Fig. 9b VOL. 78-B, NO. 2, MARCH 1996
5 332 D. J. DANDY Fig. 10 Maquet s operation, in which the tibial tubercle is moved 2 cm forwards, reduces the coaption of patella and trochlea. Fig. 11 Elmslie s operation for medial transposition of the tibial tubercle. Fig. 12 A technique of medial plication using lateral release and a fascial strip. Fig. 13 Albee s operation to elevate a dysplastic lateral trochlear lip. transposition (Fig. 11). Care should be taken not to move the tubercle medial to the mid-line of the trochlea; this may lead to recurrent medial dislocation. Medial transposition alone is appropriate if the trochlea is dysplastic and the patella is of normal size and height, but engages poorly in the trochlea. Adjustment of tissue tension. The tension of the soft tissues around the patella can be altered by releasing lateral structures or tightening medial structures. Lateral release. This alone is a reliable procedure for recurrent dislocation if the patella is not abnormally high and if the ligaments are not loose (Dandy and Desai 1994). For patients with normal anatomy the results of this procedure are better than those of tibial tubercle transfer or medial plication. Lateral release may be performed subcutaneously but must extend at least 4 cm above the upper pole of the patella (Dandy 1987). It is also used as an adjunct to medial plication and distal transposition; without a lateral release the patella cannot be moved to its new position. Medial tightening. The medial structures may be plicated or tightened using fascia, tendon, imbrication or advancement of the vastus medialis (Fig. 12). Medial tightening alone will correct the underlying problem only if the cause is abnormal laxity of the medial structures, which is rare. In other conditions it may be an adjunct to the main corrective procedure. Reconstruction of the lateral condyle. Procedures have been described (Albee 1919) to increase the height of a dysplastic lateral trochlear margin (Fig. 13). They are difficult to perform and often result in damage to the trochlear articular surface. The indications for increasing the height of the lateral margin of the trochlea are rare and few results have been THE JOURNAL OF BONE AND JOINT SURGERY
6 333 published. There is a suspicion that results are generally poor because of early degenerative changes on the femur. Deepening the trochlea. Procedures to deepen the trochlea by removing bone from beneath its articular surface and covering the excavated area with osteochondral flaps are an attractive intellectual solution to the problem of a defective femoral trochlea. Damage to the articular surface is, however, inevitable and there are few published results. PATTERNS OF DISLOCATION Some confusion exists over the terminology of patellofemoral instability. Recurrent dislocation. This is generally taken to mean repeated, occasional dislocation and it is the commonest form. The dislocations may occur at intervals of weeks or months. Recurrent subluxation. This implies a less drastic event than a dislocation but the distinction between the two is often unclear, particularly in patients with lax joints. The terminology has been confused by authors who have described the lateral pressure syndrome of Ficat as lateral subluxation of the patella (Metcalf 1982). Habitual dislocation. The term was probably first used to describe voluntary dislocation of the patella by children with lax ligaments. These patients may also dislocate their shoulders and temporomandibular and first carpometacarpal joints as party tricks. They should be encouraged not to do so but they may require tibial tubercle transposition and medial plication to achieve stability. The term is also applied to a patella which dislocates every time the knee flexes; in these cases it cannot be held in the reduced position throughout the full range of flexion. Common causes are a deficient or shallow trochlea combined with tight lateral structures. This type of habitual dislocation requires an extensive soft-tissue release, often extending far up the thigh, combined with tibial tubercle transfer and medial plication. Flexion may be limited because of quadriceps contracture and release of the rectus femoris is sometimes needed. Permanent dislocation. The permanently dislocated patella lies on the lateral side of the femur and cannot be reduced. Active extension of the knee is very weak and there is often a valgus deformity because the quadriceps acts as an abductor instead of an extensor of the knee. Congenital dislocation. Sometimes the patella is permanently dislocated from birth from congenital deformities or contractures of the vastus lateralis (Conn 1925). Contractures of the quadriceps muscle may also occur after intramuscular injections in the neonatal period (Green and Waugh 1968). The permanent or congenitally dislocated patella requires an extensive soft-tissue release, transfer of the tibial tubercle and medial plication. The patellofemoral joint is seldom congruent, the articular cartilage is usually deficient and the prognosis is poor. Relocation of the patella on the front of the femur may restore extension in these patients but flexion is usually severely restricted and release of the rectus femoris from its attachment to the pelvis may be required. SPECIAL SITUATIONS There are a few special disorders which require different methods from those outlined above. Dislocation in the immature skeleton. It is not safe to perform relocation of the tibial tubercle until growth is complete because of the risk of premature fusion at the front of the tibial physis and genu recurvatum deformity (Pappas, Anas and Toczylowski 1984). Stabilising procedures in children must use soft tissue only. Many of these fail and must be considered as the first steps in a two-stage procedure, the second being performed when growth is complete. Stabilisation is important in children for two reasons. First, it is necessary to replace the patella in the trochlea to encourage normal development of the patellofemoral joint. Secondly, articular surface lesions from recurrent dislocation in childhood lead to early osteoarthritis. Of the many soft-tissue operations described, medial plication and lateral release are probably the procedures of choice. If they do not control the stability, a semitendinosus tenodesis (Baker et al 1972) (Fig. 14) is effective but it may need to be reversed later to avoid osteoarthritis of the medial facet. Pathological ligament laxity. Ligamentous laxity of the knee may be part of a generalised joint laxity or, less commonly, be confined to the knee (Carter and Sweetnam 1958). The patella can be very difficult to stabilise if there is abnormal laxity because the soft tissues neither guide it into the trochlea at the start of flexion nor hold it there once engaged. Lateral release alone is ineffective and must be combined with medial tightening and transfer of the tibial tubercle. Care must be taken not to produce medial dislocation of the patella in these cases. Fig. 14 A semitendinosus tenodesis with lateral release. VOL. 78-B, NO. 2, MARCH 1996
7 334 D. J. DANDY osteoarthritis but patellectomy will not stabilise the patella. Both patellectomy and stabilisation may be required, either combined or as staged procedures, and the complexity of the problem should be explained to the patient. Fig. 15a Fig. 15b Techniques for stabilisation after patellectomy: (a) the lateral margin of the tendon is lengthened by transverse incisions; and (b) the tendon is rolled into a tube to create a convex undersurface. Subluxation on extension. In some knees the patella subluxes laterally on full extension and reduces on flexion as it engages in the trochlea (Dandy 1971). In these patients there is usually a high patella, ligament laxity and often a deficient lateral condyle. Many such patients have other congenital anomalies such as talipes or congenital dislocation of the hip in the same limb. Lateral release alone is never sufficient and an extensive reconstructive procedure is required for stabilisation. Dislocation after patellectomy. Patellectomy enjoyed a brief period of popularity for patellofemoral instability but it has proved ineffective. Dislocation of the patellar tendon ensues and this may be more difficult to stabilise than dislocation of the patella itself. It may also follow patellectomy for fractures of the patella. The patellar tendon can be stabilised by a wide lateral release combined with transfer of the tibial tubercle. Medial transposition alone may be adequate but distal transposition is helpful if there is an extensor lag. These procedures alone are insufficient because the undersurface of the tendon becomes concave to conform with the convexity of the lateral edge of the trochlea. This concavity must be reversed by a series of transverse cuts along its lateral edge so that the tendon lies comfortably in the trochlea. A convenient technique is to split the lateral half of the tendon in the coronal plane and make the transverse cuts in such a way that they coincide with an intact leaf of tendon above and below (Fig. 15). For additional security the flaps can be rolled anteriorly and stitched to the medial half of the tendon to form a tube. Instability in the presence of patellofemoral osteoarthritis. Severe osteoarthritis combined with patellar instability presents a difficult problem. Stabilisation may aggravate the COMPLICATIONS Patellofemoral osteoarthritis. This is common in the presence of patellar instability, whether treated or untreated. Inappropriate transfer of the tubercle is said to aggravate the condition by exposing the patellar articular surface to increased loads but there is no evidence that judicious transposition to correct a high patella carries the same risk. There is no evidence, either, that anterior advancement of the tibial tubercle at the time of transposition reduces the incidence of later osteoarthritis. Medial dislocation of the patella. This may follow excessive medial transposition of the tubercle particularly if there is ligament laxity, a defective trochlea or excessive medial plication. The tubercle should never be moved medial to the centre of the trochlea. The movement of the patella along the trochlea should be observed at the end of the operation to exclude medial subluxation. Loss of flexion. Distal transposition or relocation of a permanently dislocated patella may be followed by loss of flexion. Persistent gentle physiotherapy will eventually restore flexion but this may take as long as a year. Release of the rectus femoris from the pelvis is said to relieve this problem but I have no personal experience of this technique. Recurrence of dislocation after stabilisation. The management after a failed stabilisation operation is no different from that of a patella which has not undergone previous surgery. Thorough assessment to discover the cause of failure is essential. Corrective surgery is usually effective but some patellae continue to dislocate even when all underlying causes appear to have been removed. ASSESSMENT OF RESULTS There is no general agreement on the best way to assess the outcome of surgery for chronic patellar instability. The scoring system of Crosby and Insall (1976) is widely used but the good and excellent grades are generous and may include patients with a recurrence of dislocation. The situation is complicated because some patients experience an occasional dislocation in the immediate postoperative period before the tissues have matured and the quadriceps has regained power. Such a patient may later achieve an excellent result. The symptoms of osteoarthritis may also interfere with the assessment of stability by the Crosby and Insall score. Few scoring systems take account of the patients frequent complaint that although the patella has never dislocated, it feels as though it might. The subjective grading of feels completely stable; feels occasionally unstable but THE JOURNAL OF BONE AND JOINT SURGERY
8 335 never dislocates; continues to dislocate is simple to apply and may yield more information than complicated knee scores. REFERENCES Albee FH. Orthopaedic and reconstruction surgery: industrial and civilian. Philadelphia, etc: WB Saunders Company, Baker RH, Carroll N, Dewar FP, Hall JE. The semitendinosus tenodesis for recurrent dislocation of the patella. J Bone Joint Surg [Br] 1972;54-B: Blackburne JS, Peel TE. A new method of measuring patellar height. J Bone Joint Surg [Br] 1977;59-B: Brattström H. Shape of the intercondylar groove normally and in recurrent dislocation of patella: a clinical and x-ray-anatomical investigation. Acta Orthop Scand 1964; Suppl 68: Carter C, Sweetnam R. Familial joint laxity and recurrent dislocation of the patella. J Bone Joint Surg [Br] 1958;40-B: Conn HR. A new method for operative reduction for congenital luxation of the patella. J Bone Joint Surg 1925;7: Crosby EB, Insall J. Recurrent dislocation of the patella: relation of treatment to osteoarthritis. J Bone Joint Surg [Am] 1976;58-A:9-13. Dandy DJ. Recurrent subluxation of the patella on extension of the knee. J Bone Joint Surg [Br] 1971;53-B: Dandy DJ. Arthroscopy of the knee: a diagnostic colour atlas. London: Butterworths, Dandy DJ. Arthroscopic management of the knee. 2nd ed. Edinburgh, etc: Churchill Livingstone, Dandy DJ, Griffiths D. Lateral release for recurrent dislocation of the patella. J Bone Joint Surg [Br] 1989;71-B: Dandy DJ, Desai SS. The results of arthroscopic lateral release of the extensor mechanism for recurrent dislocation of the patella after 8 years. Arthroscopy 1994;10: Déjour H, Walch G, Nove-Josserand L, Guier Ch. Factors of patellar instabilty: an anatomic radiologic study. Knee Surg Sports Traum Arthrosc 1994;2: Goutallier D, Bernageau J, Lecudonnec B. Measurement of the tibial tuberosity, patella groove distanced technique and results (Authors trans). Rev Chir Orthop 1978;64: Green JP, Waugh W. Congenital lateral dislocation of the patella. J Bone Joint Surg [Br] 1968;50-B: Insall J, Salvati E. Patella position in the normal knee joint. Radiology 1971;101: Lloyd-Roberts GC, Thomas TG. The etiology of quadriceps contracture in children. J Bone Joint Surg [Br] 1964;46-B: Maquet P. Advancement of the tibial tuberosity. Clin Orthop 1976; 115: Merchant AC, Mercer RL, Jacobsen RH, Cool CR. Roentgenographic analysis of patellofemoral congruence. J Bone Joint Surg [Am] 1974;56-A: Metcalf RW. An arthroscopic method for lateral release of the subluxating or dislocating patella. Clin Orthop 1982;167:9-18. Pappas AM, Anas P, Toczylowski HM Jr. Asymmetrical arrest of the proximal tibial physis and genu recurvatum deformity. J Bone Joint Surg [Am] 1984;66-A: VOL. 78-B, NO. 2, MARCH 1996
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
HABITUAL DISLOCATION OF THE PATELLA IN FLEXION
 HABITUAL DISLOCATION OF THE PATELLA IN FLEXION NEIL R. BERGMAN, PETER F. WILLIAMS From the Royal Children s Hospital, Melbourne Thirty-five patients with habitual dislocation of the patella in fiexion
HABITUAL DISLOCATION OF THE PATELLA IN FLEXION NEIL R. BERGMAN, PETER F. WILLIAMS From the Royal Children s Hospital, Melbourne Thirty-five patients with habitual dislocation of the patella in fiexion
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Muscle Testing of Knee Extensors. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Muscle Testing of Knee Extensors Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Muscle Testing of Knee Extensors othe Primary muscle Quadriceps Femoris -Rectus
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Patellar Ligament Disease.
 Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Patellar Ligament Disease. The patellar ligament disease is a condition of the stifle where the cartilage keeping the patella in place over knee joint is weakened or damaged. The patella is held in place
Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality
 International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
International Orthopaedics (SICOT) (2010) 34:305 309 DOI 10.1007/s00264-009-0929-4 ORIGINAL PAPER Tibial tubercle osteotomy in patello-femoral instability and in patellar height abnormality Jacques H.
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
A Discussion on the Etiology and Relationship to Recurrent Dislocation of the Patella
 CONTRACTURE OF THE QUADRICEPS MUSCLE A Discussion on the Etiology and Relationship to Recurrent Dislocation of the Patella D. R. GUNN, SINGAPORE The objects ofthis paper are to suggest that an important
CONTRACTURE OF THE QUADRICEPS MUSCLE A Discussion on the Etiology and Relationship to Recurrent Dislocation of the Patella D. R. GUNN, SINGAPORE The objects ofthis paper are to suggest that an important
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Musculoskeletal Applications for CT. Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine
 Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
10/30/18. Disclosures. Recurrent Patellar Instability. Management of Recurrent Patellar Instability
 Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Management of Recurrent Patellar Instability Miho J. Tanaka, MD Associate Professor Director, Women s Sports Medicine Program ORTHOPAEDIC SURGERY Disclosures None Recurrent Patellar Instability Lack of
Knee Joint Anatomy 101
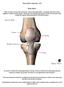 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi
 The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
Acute patellar dislocation in adults
 CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
CASE STUDY 14 Acute patellar dislocation in adults What are the reasons for the first acute dislocation? How can we document the pathoanatomy? What is our treatment concept? Table CS14 Patellofemoral joint
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Assessment of Patellar Laxity in the in vitro Native Knee
 Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
Assessment of Patellar Laxity in the in vitro Native Knee By Mark C. Komosa Submitted to the graduate degree program in Bioengineering and the Graduate Faculty of the University of Kansas in partial fulfillment
A Patient s Guide to Patellofemoral Problems
 A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Patellofemoral Problems 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
and K n e e J o i n t Is the most complicated joint in the body!!!!
 K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Imaging in patellofemoral instability is essential to the accurate
 REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
The Three-In-One Proximal and Distal Soft Tissue Patellar Realignment Procedure
 0363-5465/99/2727-0575$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 27, No. 5 1999 American Orthopaedic Society for Sports Medicine The Three-In-One Proximal and Distal Soft Tissue Patellar Realignment
0363-5465/99/2727-0575$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 27, No. 5 1999 American Orthopaedic Society for Sports Medicine The Three-In-One Proximal and Distal Soft Tissue Patellar Realignment
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
DISCLOSURES. Overview 09/24/2015. Patellofemoral Instability and Treatment Options. I do not have anything to disclose
 Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
Patellofemoral Instability and Treatment Options Gregory Purnell, MD Department of Orthpoaedic Surgery Sports Medicine and Arthroscopy Allegheny Health Network Orthopaedic Surgeon, Pittsburgh Pirates Baseball
The Knee. Clarification of Terms. Osteology of the Knee 7/28/2013. The knee consists of: The tibiofemoral joint Patellofemoral joint
 The Knee Clarification of Terms The knee consists of: The tibiofemoral joint Patellofemoral joint Mansfield, p273 Osteology of the Knee Distal Femur Proximal tibia and fibula Patella 1 Osteology of the
The Knee Clarification of Terms The knee consists of: The tibiofemoral joint Patellofemoral joint Mansfield, p273 Osteology of the Knee Distal Femur Proximal tibia and fibula Patella 1 Osteology of the
Patellar instability
 Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Page 1 of 13 Specific Injuries D Goodwin 1, W Postma 2 * Patellar instability Abstract Introduction Patellar instability is most common among adolescent female athletes, although anyone can be affected.
Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery. Restore patella stability.
 Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
Page 1 of 5 Elizabeth A. Arendt Professor & Vice Chair University of Minnesota Department of Orthopaedic Surgery Restore patella stability. Restore / improve function. I have no conflicts to declare. 1987
5/14/2013. Acute vs Chronic Mechanism of Injury:
 Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Third Annual Young Athlete Conference: The Lower Extremity February 22, 2013 Audrey Lewis, DPT Acute vs Chronic Mechanism of Injury: I. Direct: blow to the patella II. Indirect: planted foot with a valgus
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Myology of the Knee. PTA 105 Kinesiology
 Myology of the Knee PTA 105 Kinesiology Objectives Describe the planes of motion and axes of rotation of the knee joint Visualize the origins and insertions of the muscles about the knee List the innervations
Myology of the Knee PTA 105 Kinesiology Objectives Describe the planes of motion and axes of rotation of the knee joint Visualize the origins and insertions of the muscles about the knee List the innervations
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
No Disclosures. Topics. Pediatric ACL Tears
 Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Knee Injuries in Skeletally Immature Athletes No Disclosures Zachary Stinson, M.D. 2 Topics ACL Tears and Tibial Eminence Fractures Meniscus Injuries Discoid Meniscus Osteochondritis Dessicans Patellar
Jacques Menetrey, MD, PD. Uniklinik Balgrist. Unité d Orthopédie et Traumatologie du Sport (UOTS)
 Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Acute patellar dislocation: conservative or surgical treatment Jacques Menetrey, MD, PD Unité d Orthopédie et Traumatologie du Sport (UOTS) Service de chirurgie orthopédique et traumatologie de l appareil
Masterclass. Tips and tricks for a successful outcome. E. Verhaven, M. Thaeter. September 15th, 2012, Brussels
 Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
UNIT 7 JOINTS. Knee and Ankle Joints DR. ABDEL-MONEM A. HEGAZY
 UNIT 7 JOINTS Knee and Ankle Joints BY DR. ABDEL-MONEM A. HEGAZY (Degree in Bachelor of Medicine and Surgery with honor 1983, Dipl."Gynaecology and Obstetrics "1989, Master "Anatomy and Embryology "1994,
UNIT 7 JOINTS Knee and Ankle Joints BY DR. ABDEL-MONEM A. HEGAZY (Degree in Bachelor of Medicine and Surgery with honor 1983, Dipl."Gynaecology and Obstetrics "1989, Master "Anatomy and Embryology "1994,
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Plaster-Wedging Technique:
 Plaster-Wedging Technique: An Appropriate, Safe, Quick, & Economical Method To Stretch Soft Tissue Contractures Of The Knee H.M. Steenbeek General Information. In the field of physical rehabilitation of
Plaster-Wedging Technique: An Appropriate, Safe, Quick, & Economical Method To Stretch Soft Tissue Contractures Of The Knee H.M. Steenbeek General Information. In the field of physical rehabilitation of
Anterior knee pain.
 Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
Anterior knee pain What are the symptoms? Anterior knee pain is very common amongst active adolescents and athletes participating in contact sports. It is one of the most common problems/injuries seen
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Physiotherapy in Recurrent Dislocation of Patella-Wiberg Type II Farzana Alam, Subhadeep Roy Choudhury BPT,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Physiotherapy in Recurrent Dislocation of Patella-Wiberg Type II Farzana Alam, Subhadeep Roy Choudhury BPT,
The patella connects the quadriceps tendon in the thigh to the patellar tendon below the knee attaching to the tibial tuberosity of the shin bone.
 ISO 9001:2015 FS 550968 Patellofemoral Pain Anterior Knee Pain or pain at the kneecap - is a very common complaint. Most anterior knee pain is from the joint between the kneecap (patella) and the thigh
ISO 9001:2015 FS 550968 Patellofemoral Pain Anterior Knee Pain or pain at the kneecap - is a very common complaint. Most anterior knee pain is from the joint between the kneecap (patella) and the thigh
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
A lateral approach defect closure technique with deep fascia flap for valgus knee TKA
 Jiang and Fernandes Journal of Orthopaedic Surgery and Research (2015) 10:173 DOI 10.1186/s13018-015-0316-3 RESEARCH ARTICLE Open Access A lateral approach defect closure technique with deep fascia flap
Jiang and Fernandes Journal of Orthopaedic Surgery and Research (2015) 10:173 DOI 10.1186/s13018-015-0316-3 RESEARCH ARTICLE Open Access A lateral approach defect closure technique with deep fascia flap
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Medial patellofemoral ligament reconstruction using dual patella docking technique
 2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
2018; 4(3): 298-304 ISSN: 2395-1958 IJOS 2018; 4(3): 298-304 2018 IJOS www.orthopaper.com Received: 24-05-2018 Accepted: 25-06-2018 Dr. Ullas Mahesh Assistant Professor, Department of Orthopaedics, Bangalore,
As for the forelimb, treatment of condition of the hindlimb may be treated by both localised therapy, applying the laser
 MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
PART III Case Studies
 PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
ANATOMIC. Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0
 ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management
 SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
SOFT TISSUE INJURIES OF THE KNEE: Primary Care and Orthopaedic Management Gauguin Gamboa Australia has always been a nation where emphasis on health and fitness has resulted in an active population engaged
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports Medicine 15. Unit I: Anatomy. The knee, Thigh, Hip and Groin. Part 4 Anatomies of the Lower Limbs
 Sports Medicine 15 Unit I: Anatomy Part 4 Anatomies of the Lower Limbs The knee, Thigh, Hip and Groin Anatomy of the lower limbs In Part 3 of this section we focused upon 11 of the 12 extrinsic muscles
Sports Medicine 15 Unit I: Anatomy Part 4 Anatomies of the Lower Limbs The knee, Thigh, Hip and Groin Anatomy of the lower limbs In Part 3 of this section we focused upon 11 of the 12 extrinsic muscles
The Knee. Tibio-Femoral
 The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Management of ACL Elongation in the Surgical Treatment of Congenital Knee Dislocation
 Management of ACL Elongation in the Surgical Treatment of Congenital Knee Dislocation Kevin E. Klingele, MD; Scott Stephens, MD abstract Full article available online at Healio.com/Orthopedics. Search:
Management of ACL Elongation in the Surgical Treatment of Congenital Knee Dislocation Kevin E. Klingele, MD; Scott Stephens, MD abstract Full article available online at Healio.com/Orthopedics. Search:
PATELLECTOMY. The former are usually the result of a blow or. a fall to the ground onto the flexed knee;
 POSTGRAD. MED. J. (1964), 40, 531 REMOVAL of the patella for fracture began to be performed towards the end of the last century. Good reports followed the introduction of this novel procedure and everyone
POSTGRAD. MED. J. (1964), 40, 531 REMOVAL of the patella for fracture began to be performed towards the end of the last century. Good reports followed the introduction of this novel procedure and everyone
The suction cup mechanism is enhanced by the slightly negative intra articular pressure within the joint.
 SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
FACTORS AFFECTING PATELLAR TRACKING IN TOTAL KNEE ARTHROPLASTY
 FACTORS AFFECTING PATELLAR TRACKING IN TOTAL KNEE ARTHROPLASTY Essay submitted in partial fulfillment of M.Sc. Degree in Orthopaedic surgery Cairo University By Ahmed Ali Ahmed Ali Elsayed M.B.B.Ch Supervised
FACTORS AFFECTING PATELLAR TRACKING IN TOTAL KNEE ARTHROPLASTY Essay submitted in partial fulfillment of M.Sc. Degree in Orthopaedic surgery Cairo University By Ahmed Ali Ahmed Ali Elsayed M.B.B.Ch Supervised
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction
 In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
In Vivo Positioning Analysis of Medial Patellofemoral Ligament Reconstruction Elvire Servien,* y MD, PhD, Brett Fritsch, z MD, Sébastien Lustig, y MD, Guillaume Demey, y Romain Debarge, y MD, Carole Lapra,
BIOMECHANICS OF PATELLA FUNCTION. PETER G. KRAMER, EdD, PT*
 01 96-601 l/86/0806-0301$02.00/0 THE JOURNAL OF ORTHOPAED~C AND SPORTS PHYSICAL THERAPY Copyright 0 1986 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
01 96-601 l/86/0806-0301$02.00/0 THE JOURNAL OF ORTHOPAED~C AND SPORTS PHYSICAL THERAPY Copyright 0 1986 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Patellofemoral Replacement
 Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study
 Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
Prague Medical Report / Vol. 106 (2005) No. 2, p. 159 166 159) Combined Pelvic Osteotomy in the Treatment of Both Deformed and Dysplastic Acetabulum Three Years Prospective Study Al Razi Orthopedic Hospital,
PATELLA REALIGNMENT SURGERY
 PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO PATELLA REALIGNMENT SURGERY and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office Paillard 2011 YOU HAVE A PATELLA DYSFUNCTION YOU
PATIENT INFORMATION SHEET YOU ARE GOING TO UNDERGO PATELLA REALIGNMENT SURGERY and sports traumatology ORTHOPAEDIC SURGERY Doctor Philippe Paillard Office Paillard 2011 YOU HAVE A PATELLA DYSFUNCTION YOU
Patellar Instability. OrthoInfo Patella Instability Page 1 of 5
 Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
World Medical & Health Games
 Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
Management of Patellofemoral Pain Syndrome João Barroso Orthopaedic department ULS Matosinhos Portugal Introduction Anterior Knee Pain affects 1 in 4 athletes very common! (Knowles et al) Patellofemoral
DIAGNOSIS AND EARLY MANAGEMENT OF KNEE INJURIES
 DIAGNOSIS AND EARLY MANAGEMENT OF KNEE INJURIES INTRODUCTION: The knee is a common site of athletic injury. The knee injuries can be classified either into traumatic or acute and chronic, with overuse
DIAGNOSIS AND EARLY MANAGEMENT OF KNEE INJURIES INTRODUCTION: The knee is a common site of athletic injury. The knee injuries can be classified either into traumatic or acute and chronic, with overuse
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
(iv) Patellofemoral dysfunction Extensor mechanism malalignment
 Current Orthopaedics (2006) 20, 103 111 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: SOFT TISSUE KNEE PROBLEMS (iv) Patellofemoral dysfunction Extensor
Current Orthopaedics (2006) 20, 103 111 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: SOFT TISSUE KNEE PROBLEMS (iv) Patellofemoral dysfunction Extensor
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Axial Scan Orientation and the Tibial Tubercle Trochlear Groove Distance: Error Analysis and Correction
 Musculoskeletal Imaging Original Research Yao et al. MRI Measurements of the TT-TG Distance Musculoskeletal Imaging Original Research Lawrence Yao 1 Neville Gai 1 Robert D. Boutin 2 Yao L, Gai N, Boutin
Musculoskeletal Imaging Original Research Yao et al. MRI Measurements of the TT-TG Distance Musculoskeletal Imaging Original Research Lawrence Yao 1 Neville Gai 1 Robert D. Boutin 2 Yao L, Gai N, Boutin
Complications of Total Knee Arthroplasty
 Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
