Focal Anatomic Patellofemoral Inlay Resurfacing: Theoretic Basis, Surgical Technique, and Case Reports
|
|
|
- Franklin Fisher
- 5 years ago
- Views:
Transcription
1 Orthop Clin N Am 39 (2008) Focal Anatomic Patellofemoral Inlay Resurfacing: Theoretic Basis, Surgical Technique, and Case Reports Philip A. Davidson, MD a,b, *, Dennis Rivenburgh, MS, ATC, PA-C b a Department of Orthopaedic Surgery, University of South Florida, th St. N, Pinellas Park, FL 33781, USA b Tampa Bay Orthopaedic Specialists, Pinellas Park, FL 33781, USA Isolated patellofemoral degenerative changes range from 11% in men to 24% in women over the age of 55 years with symptomatic osteoarthritis of the knee [1]. Reports show an incidence of isolated patellofemoral arthritis in 9.2% of patients over 40 years [2]. The review of patients undergoing patellofemoral arthroplasty shows that the majority are women [3 8]. This may well be attributed to a higher incidence of congenital malalignment and dysplasia in women [9]. In their study of 31,516 knee arthroscopies, Curl and colleagues [10] reported approximately 20% of cases with patellar articular defects and 15% with trochlear articular pathology. Although these findings may have variable clinical significance at the time of index arthroscopy, the biomechanical alteration of the articulation may indicate a tendency for progressive degeneration. Anterior knee pain associated with patellofemoral degeneration is a very common presenting complaint to musculoskeletal health care providers, especially in active or elderly women. A multitude of factors guide treatment of patellofemoral pathology, including patient age, presenting symptoms, body type, articular morphology, static and dynamic alignment, and imaging studies. When conservative measures fail, the most common surgical procedures include debridement, chondroplasty, soft tissue or bony realignment, biologic cartilage restoration, patellectomy, total knee arthroplasty, and patellofemoral arthroplasty [8,11 18]. * Corresponding author. Department of Orthopaedic Surgery, University of South Florida, th St. N, Pinellas Park, FL address: pdavidson@tampabayortho.com (P.A. Davidson). In patients with normal patellar alignment and traumatic localized defects, standard biologic treatment options have been the mainstay of first-round surgical interventions. Biologic resurfacing described for the patellofemoral joint includes marrow stimulation techniques or biologic reconstruction. Marrow stimulation techniques include microfracture, abrasion, picking, and drilling. Biologic restoration methods include osteochondral autografts, osteochondral allografts, chondrocyte implantation, and scaffold resurfacing. Results from the biologic spectrum of treatment options have been reported with variable success rates [19 22]. Patients with chronic malalignment or dysplasia typically show degenerative, rather than focal, patellofemoral articular disease. These patients often require concomitant soft tissue and bony procedures to address the entire realm of pathologies related to the extensor mechanism and anterior knee. Prosthetic patellofemoral inlay resurfacing is a novel treatment concept introduced to the orthopedic community in The theoretic basis of this type of arthroplasty entails recreating ambient anatomy based on intraoperative topographic mapping. The implant is intrinsically stable by virtue of the inset position relative to the surrounding joint surface. Furthermore, using this strategy, concurrent soft tissue and bony surgery is facilitated, because volume is not extrinsically added to the joint. This type of surgery, in contradistinction to some procedures labeled as minimally invasive is in fact microinvasive. This is accomplished with smaller exposures, shorter operating times, simple and cannulated implantation technique, minimal bone resection, and typically less peri-operative blood loss. Resurfacing, per se, has been widely accepted for shoulder and hip /08/$ - see front matter Ó 2008 Elsevier Inc. All rights reserved. doi: /j.ocl orthopedic.theclinics.com
2 338 DAVIDSON & RIVENBURGH indications with typically near-complete unipolar articular coverage. The HemiCAP resurfacing platform technology (Arthrosurface, Inc. Franklin, MA, USA) reflects a new paradigm in joint resurfacing, based on intraoperative joint surface mapping, making use of a corresponding patientspecific implant. This system allows for restoration of complex geometric surfaces in a variety of morphologic and pathologic states. Various diameter sizes are available across a multitude of joints, using the same platform technologic principles [23 28]. The current patellofemoral HemiCAP resurfacing prosthesis is available in 20-mm diameter and focuses on relatively localized defects of the distal trochlear surface and patellar defects. The prosthesis incorporates a trochlear articular component that is connected to a fixation stud via a taper interlock and a modular polyethylene patella component (Fig. 1). A choice of 13 different offset dimensions allows for a patient-specific geometry match in the distal trochlear. Larger diameter implants are pending, to address more diffuse patellofemoral disease. Patient assessment It is important to determine the source of anterior knee pain. Physical examination includes assessment of the kinematic chain during normal gait and deep knee flexion from hip to ankle. Particular attention is directed to patellar alignment with signs of tilt and subluxation. In addition, the examination assesses the medial and lateral facets, articular crepitus, particular local pain foci, and quadriceps strength. Patients suffering from patellofemoral disease typically exhibit anterior knee pain with the extensor mechanism under load. Weight-bearing radiographs allow for improved patellofemoral assessment and include standard anteroposterior, notch view at 30 of flexion, lateral, and an axial weight-bearing Merchant view at 45 of knee flexion [23]. Chondral damage, soft tissues including patellar and quadriceps tendons, and patellofemoral joint symmetry or dysplasia can be assessed further and quantified on magnetic resonance imaging. Focal patellofemoral resurfacing alone cannot be effective in global degenerative joint disease. Therefore, relatively monocompartmental pathology has to be verified. Patellofemoral pathology must be confirmed at the time of surgery to consider patients for patellofemoral resurfacing. Indications and contraindications The HemiCAP patellofemoral resurfacing prosthesis is intended for patients with pain and functional limitations who have not responded to conservative treatment measures or previous surgical procedures and have cartilage defects or degeneration limited to the patellofemoral joint. Both medial and lateral tibiofemoral compartments should be substantially normal or surgically addressed to render them such. Patients should show normal patellofemoral alignment, or as an alternative, improved patellar tracking can be addressed intraoperatively with concurrent procedures. Normal joint stability, both tibiofemoral and patellofemoral, and relatively good range of motion should be demonstrated before surgery. Contraindications include diffuse full-thickness articular cartilage loss extending beyond the implant, extensive bone loss, infection, advanced osteoporosis, and other metabolic or inflammatory disorders that may negatively affect implant fixation or render the joint prone to continued degeneration. Surgical technique Patellofemoral HemiCAP implantation is performed with a combination of arthroscopic and Fig. 1. (A) Trochlear resurfacing component (example with shallow trochlear offsets): cobalt-chromium alloy (Co-Cr- Mo). (B) Trochlear component. Undersurface coating: titanium (CP Ti); fixation stud: titanium alloy (Ti-6Al-4V). (C) Trochlear component (example with deep offsets) and connected fixation stud. (D) Patellar component (example with anatomic ridge): ultra-high-molecular weight polyethylene (UHMWPE).
3 ANATOMIC PATELLOFEMORAL INLAY RESURFACING 339 open surgery. The patient is positioned in the supine position, standard arthroscopic portals are placed, and the joint is inspected. Arthroscopic treatment is performed for concurrent pathologies and to confirm proper indication for prosthetic implantation. At the conclusion of the arthroscopic procedure, an arthroscopic lateral release may be performed. This may be indicated for patellofemoral realignment purposes and may also be used to facilitate exposure subsequently. The procedure is now converted into an open surgery by extending the medial portal between 4 and 7 cm, depending on the size of the patient. Alternatively a midline incision may be used. Electrocautery is used to incise the medial capsule and patellofemoral retinaculum with care to prevent damage to the underlying articular cartilage. The capsular incision can be extended either proximally or distally, depending on the patient morphology. A soft tissue sleeve of approximately 1 cm is left attached to the patella for subsequent closure and medial plication, if necessary. Bony realignment, when indicated, can be performed at this point in the procedure. The medial tissues are tagged and reflected, and the patella can be inverted to either 90 or 180, depending on surgeon preference. A retractor is placed over the lateral condyle, reflecting the patella in the lateral direction, providing access to the trochlear groove. With the knee in 90 of flexion, the HemiCAP drill guide is seated with four points of contact. The footed guide is placed in an anterior position to develop a working axis normal to the distal trochlear articular surface (Fig. 2). The fully cannulated instrumentation initiates prosthetic alignment by placing a guide pin into the center of the trochlear defect. A step drill is advanced over the guide pin until the proximal shoulder is flush to the articular surface. Care is taken to avoid overdrilling, so as not to compromise subsequent screw fixation in subchondral bone. Standard tapping technique is used before the fixation screw is placed into the center of the defect. Etched depth markings provide external reference points while advancing instruments to ultimately achieve flush prosthetic implantation. Once peak height placement of the fixation screw is verified with a trial cap, a centering shaft is seated into the taper head of the fixation component to enable its navigational properties. A contact probe is placed over the centering shaft and rotated to obtain superior/inferior and medial/lateral offsets (Fig. 3). A corresponding reamer prepares the implant bed (Fig. 4). A sizing trial with matching offsets is used to confirm a congruent fit of the trochlear component to the edge of the surrounding articular surface. Before placement of the final trochlear component, the procedure is directed toward preparation of the patellar implant. The patella s anterior-to-posterior thickness is verified to accommodate the patella component with a reaming depth of typically 6.5 mm. With the knee at 90 flexion, an alignment guide facilitates target placement of the patella component while observing range of motion. A guide pin is placed into the previously identified locationda drill guide again provides placement Fig. 2. Drill guide placement in the center of the trochlear defect, perpendicular to the joint surface. Fig. 3. Contact probe inserted over centering shaft, which is placed in the fixation component.
4 340 DAVIDSON & RIVENBURGH implant holder and placed into the taper of the fixation screw (Fig. 7). A mallet and impactor firmly seat the trochlear component. Once implantation is complete, a trial range of motion is performed. A stable and balanced extensor mechanism should be present or achieved with concurrent procedures. Closure of the medial retinacular incision is performed using standard capsular sutures. If a proximal realignment is necessary, the medial capsule can be plicated during the capsular closure. The lateral retinacular incision is left open. Fig. 4. Final trochlear implant bed after high-speed reaming. within a normal working axis to the patellar surface (Fig. 5). A cannulated drill is advanced over the guide pin until the distal shoulder of the drill is flush to the articular surface. Using a powered drill, the patella centering shaft is placed over the guide pin until it reaches the distal laser marked depth marking. The contact probe establishes patellar offsets in two dimensions. A corresponding reamer is preparing the implant bed in the patella, and a sizing trial allows verification of congruent margin fit to the surrounding articular surface (Fig. 6A and B). An anatomic or flat patellar contour can be trialed to ensure optimized tracking. The final patellar component is aligned on the implant holder and cemented into the prepared socket (Fig. 6C). The femoral trochlear component is now aligned with the appropriate offsets on the Fig. 5. Patellar drill guide placement in the center of the defect. Case reports Case 1 A 45-year-old woman, an athletically active physical education teacher, presented with bilateral knee pain for more than 20 years not associated with any trauma or patellar dislocations. Both knees had two previous knee arthroscopic debridements and no realignment procedures. None of those surgeries gave sustained relief. At the time of presentation, the patient stated I cannot do anything because of my knees; I am extremely limited in what I can do. I can t get up and down from a chair without difficulties, I can t do athletic maneuvers, and doing my job is nearly impossible. I have a constant sensation of aching made worse with any activities, and it clearly feels like there s bone on bone. Preoperative physical examination showed symmetric findings bilaterally. Range of motion was 0 to 140. There was painful arc of motion with palpable and audible crepitance from 40 to 140. Marked pain was noted with patellofemoral compression. The Q angle was 9, and the patient had symmetric quad atrophy compared with other lower extremity muscle groups. The knee was stable, and she had no specific pain with patellar lateral apprehension testing. The medial and lateral compartments were unremarkable, and the knee was stable with a small effusion. Preoperative radiographs showed advanced isolated patellofemoral arthrosis with lateral patellar subluxation. Index procedure The patient underwent left knee diagnostic arthroscopy to confirm the appropriate indications. Intraoperative findings included a 50% full-thickness loss of articular cartilage in the distal
5 ANATOMIC PATELLOFEMORAL INLAY RESURFACING 341 Fig. 6. (A) Preparation of patellar implant bed. (B) Sizing trial to verify congruent articular margins. (C) Final patellar component implanted. trochlear. The patella had loss of cartilage on the lateral facet and the patellar ridge. The medial and lateral compartments were without pathologic change. A mini-open patellofemoral resurfacing with the bipolar Arthrosurface HemiCAP device and an arthroscopic lateral release were performed. During closure, a proximal realignment with medial retinacular plication was performed. The surgery was done as an outpatient procedure with minimal blood loss. The patient had range of motion from 0 to 65 by the first postoperative week and 105 by the third postoperative week, and she returned to work with a cane by the fourth postoperative week. She regained 140 flexion by the eighth postoperative week. Rehabilitation included immediate full weight-bearing, no imposed limitation of flexion, and use of axillary crutches for 4 weeks. After her experience with this procedure, 10 months after the first patellofemoral resurfacing, she elected to have the contralateral knee treated with a similar procedure. Her second knee underwent a nearly identical operation with similar results. At last follow-up, the patient expressed a high degree of satisfaction for both knees (Table 1). Please note that at the time of surgery, excellent articular congruity was achieved for the trochlear component. Fig. 8B shows an apparent offset relative to the subchondral bone, but this implant had circumferential congruity with the ambient surface (Figs. 7 11). Fig. 7. Final trochlear component implanted.
6 342 DAVIDSON & RIVENBURGH Table 1 Case 1: outcomes measures for left knee with 12 months of follow-up and right knee with 3 months of follow-up Outcomes score Preoperative assessment Last follow-up assessment Percent improvement SF-36 (Physical) L R IKDC L R 33/ Fulkerson knee score L R Lysholm L R Tegner L R Case 2 The patient is a 59-year-old woman with a progressive history of more than 10 years of bilateral knee pain. The patient had no previous bracing, surgery, therapy, or dislocations. She complained of bilateral grinding within the front of both knees. She described severe limitations in her ability to perform activities of daily living and recreational activities. She has a sedentary job. Preoperative physical examination showed symmetric findings bilaterally. Range of motion was 0 to 135. She had painful arc of motion with palpable and audible crepitance from 30 thru 135. Pain limited the patient from doing a one-leg step up without an assistive device. Marked pain was noted with patellofemoral compression. The Q angle was 10, and the patient had symmetric quad atrophy compared with other lower extremity muscle groups. The knee was stable, and she had no increase in pain with patellar lateral apprehension testing. The medial and lateral compartments were unremarkable, and the knee was stable without effusion. Preoperative radiographs showed advanced isolated patellofemoral arthrosis with lateral patellar subluxation. Index procedure The patient underwent right knee arthroscopy with intra-articular debridement, arthroscopic lateral release, open patellofemoral HemiCAP resurfacing, and medial retinacular plication. There was minimal blood loss, and the surgery was conducted on an outpatient basis. The patient was noted to have 110 of flexion the first postoperative week, with 135 degrees after the third postoperative week. At last follow-up, 3 months after the procedure, the patient reported great Fig. 8. (A) Case 1, Merchant preoperative x-ray. (B) Case 1, Merchant postoperative x-ray after patellar and trochlear HemiCAP resurfacing with lateral release and medial retinacular plication. (Note: improved patellofemoral tracking alignment).
7 ANATOMIC PATELLOFEMORAL INLAY RESURFACING 343 Fig. 9. Case 1; mini open view, trochlear pathology. pain relief and near-normal range of motion (Table 2). Currently the patient is pending contralateral surgery as she waits to accumulate time off from work to accommodate the procedure and postoperative recovery (Fig. 12). Discussion Many investigators have stressed the importance of prosthetic design factors to improve outcomes of isolated patellofemoral arthroplasty [3,14,15,29 31]. A wider selection available on the market today and improved prosthetic geometry have led to increased interest in unicompartmental arthroplasty of the patellofemoral joint. In conventional onlay patellofemoral arthroplasty, the implant geometry typically dictates the new joint surface, imparting nonnative geometry. Therefore, HemiCAP inlay resurfacing may have Fig. 11. Case 1; postoperative lateral radiograph after patellar and trochlear HemiCAP resurfacing. significant intrinsic advantages in patients with patellofemoral defects surrounded by relatively healthy articular cartilage margins and proper, or improved, extensor mechanism alignment. Three-dimensional intraoperative mapping of the joint curvatures, preparation of a shallow implant bed, and placement of matching contoured articular inlay components provide preservation of healthy articular cartilage and valuable bone stock, avoid the risk of overstuffing the joint, and may keep the biomechanics of the patellofemoral joint unaltered. Soft tissues and extensor mechanism maintain their original tension, which may aid in postoperative recovery and strengthening. Prosthetic stability and fixation are embedded into the overall joint surface, providing a theoretic advantage for implant stability in comparison with exposed onlay prosthetic devices. Bone cuts, as typically performed during conventional patellofemoral arthroplasty, are avoided using the described technique. This is Fig. 10. Case 1; preoperative lateral radiograph. Table 2 Case 2: outcomes measures for right knee with 3 months of follow-up Outcomes score SF-36 Preoperative assessment Last follow-up assessment (Physical) IKDC Fulkerson knee score Lysholm Tegner Percent improvement
8 344 DAVIDSON & RIVENBURGH Fig. 12. Case 2; trochlear resurfacing component in place. not only important in the context of minimal impact on joint biomechanics but also in the background of future revision surgery, should the need arise. In particular, younger and active patients with isolated patellofemoral degeneration may benefit the most from a cartilage and bone stock preserving procedure. At the same time, older patients with more compromised or fragile health may derive a medical advantage from focal resurfacing through minimized surgical dissection, shorter procedure time, and a reduction in potential blood loss. Primary implant stability is provided through the fixation stud anchored into the distal trochlea, connected with an articular component via taper interlock, which is seated in a precisionreamed shallow implant bed. Because of the similarities in implant design and material with undersurface titanium coverage and titanium fixation component, a comparison to the goat study of Kirker-Head and colleagues [23] for focal femoral resurfacing may be suitable. The investigators have shown secondary stability with new trabecular bone abutted to the underside of the articular component and around the fixation stud without any evidence of a residual adverse inflammatory reaction to the implant or any indication of subchondral cyst formation in the medullary tissue surrounding the prosthesis. High loads and complex patellofemoral joint surface geometry are challenging for biologic resurfacing methods. Therefore, patients who have not responded to such treatment options, or are not amenable because of advanced age or postimplantation requirements with prolonged protected physical therapy, may benefit from a stable prosthetic inlay construct with immediate primary fixation that allows for accelerated rehabilitation. Patellofemoral malalignment reduces the contact area between patella and trochlea, thus, reducing the load-bearing surface over which forces from the extensor mechanism are transmitted to the femur [32]. Although overall patellofemoral joint reactive forces remain the same, the reduced contact area leads to focally elevated joint stresses [33 37]. Correction of malalignment in combination with a load-sharing congruent inlay resurfacing may help in normalizing patellofemoral joint kinematics and will have advantages for implant survivorship. Becher and colleagues [27] found no significant differences in peak contact pressure for flush HemiCAP implantation in the femoral condyle when compared with the normal, untreated joint. Future basic science investigations will need to establish scientific evidence for patellofemoral joint kinematics after HemiCAP resurfacing. The HemiCAP patellofemoral resurfacing procedure is highly reproducible and therefore has a short learning curve. Nevertheless, poor patient selection, technical errors, residual soft tissue imbalance, and continuation of patellofemoral or tibiofemoral degeneration may have a negative impact on clinical outcomes. Intermediate and long-term clinical outcomes are required to show the benefits of this technology and allow for comparison with other patellofemoral treatment options including conventional arthroplasty. Future increase in prosthetic surface coverage will make the HemiCAP patellofemoral resurfacing technology accessible to a wider range of patients with more diffuse and degenerative cartilage defects of the patellofemoral joint. Summary Distal patellofemoral inlay resurfacing with the HemiCAP technology is a novel treatment option. It is indicated for patients with relatively localized defects or degeneration limited to the distal femoral trochlear and patellar. The native joint surface geometry is intraoperatively mapped for
9 ANATOMIC PATELLOFEMORAL INLAY RESURFACING 345 inset surface components with matching offsets. The trochlear and patellar prostheses are implanted congruent to the surrounding articular surface, conveying intrinsic stability. Proper patellofemoral tracking must be present or should be addressed in concurrent procedures. This patellofemoral resurfacing system may provide advantages for joint preservation, biomechanics, and component fixation when compared with traditional onlay arthroplasty. This initial report outlines theoretic concepts and surgical technique and provides case reports. References [1] McAlindon TE, Snow S, Cooper C, et al. Radiographic pattern of osteo-arthritis of the knee joint in the community: the importance of the patellofemoral joint. Ann Rheum Dis 1992;51: [2] Davis AP, Vince AS, Shepstone L, et al. The Radiologic prevalence of patellofemoral osteoarthritis. Clin Orthop 2002;402: [3] Blazina ME, Fox JM, Del Pizzo W, et al. Patellofemoral replacement. Clin Orthop Relat Res 1979;144: [4] Arciero RA, Toomey HE. Patellofemoral arthroplasty: a three- to nine-year follow-up study. Clin Orthop Relat Res 1988;236: [5] Cartier P, Sanouiller JL, Grelsamer R. Patellofemoral arthroplasty: year follow-up study. J Arthroplasty 1990;5: [6] De Winter WE, Feith R, van Loon CJ. The Richards type II patellofemoral arthroplasty: 26 cases followed for 1 20 years. Acta Orthop Scand 2001;72: [7] Krajca-Radcliffe JB, Coker TP. Patellofemoral arthroplasty: A2- to 18-year follow up study. Clin Orthop Relat Res 1996;330: [8] Argenson JN, Flecher X, Parratte S, et al. Patellofemoral arthroplasty: an update. Clin Orthop Relat Res 2005;440:50 3. [9] Lonner JH. Patellofemoral arthroplasty. J Am Acad Orthop Surg 2007;15(8): [10] Curl WW, Krome J, Gordon ES, et al. Cartilage injuries: a review of 31,516 knee arthroscopies. Arthroscopy 1997;13(4): [11] Fulkerson JP. Alternatives to patellofemoral arthroplasty. Clin Orthop Relat Res 2005;436: [12] Gomoll AH, Minas T, Farr J, et al. Treatment of chondral defects in the patellofemoral joint. J Knee Surg 2006;19(4): [13] Mandelbaum B, Browne JE, Fu F, et al. Treatment outcomes of autologous chondrocyte implantation for full-thickness articular cartilage defects of the trochlea. Am J Sports Med 2007;35(6): [14] Leadbetter WB, Ragland PS, Mont MA. The appropriate use of patellofemoral arthroplasty: an analysis of reported indications, contraindications, and failures. Clin Orthop Relat Res 2005;436:91 9. [15] Leadbetter WB, Seyler TM, Ragland PS, et al. Indications, contraindications, and pitfalls of patellofemoral arthroplasty. J Bone Joint Surg Am 2006; 88(Suppl 4): [16] Mont MA, Haas S, Mullick T, et al. Total knee arthroplasty for patellofemoral arthritis. J Bone Joint Surg Am 2002;84(11): [17] Parvizi J, Stuart MJ, Pagnano MW, et al. Total knee arthroplasty in patients with isolated patellofemoral arthritis. Clin Orthop Relat Res 2001;392: [18] Grelsamer RP, Stein DA. Patellofemoral arthritis. J Bone Joint Surg Am 2006;88(8): [19] Federico DJ, Reider B. Results of isolated patellar debridement for patellofemoral pain in patients with normal patellar alignment. Am J Sports Med 1997;25: [20] Hangody L, Fules P. Autologous osteochondral mosaicplasty for the treatment of full-thickness defects of weight-bearing joints: ten years of experimental and clinical research. J Bone Joint Surg Am 2003;85(Suppl 2): [21] Minas T, Bryant T. The role of autologous chondrocyte implantation in the patellofemoral joint. Clin Orthop Relat Res 2005;436:30 9. [22] Nakagawa K, Wada Y, Minamide M, et al. Deterioration of longterm clinical results after the Elmslie-Trillat procedure for islocation of the patella. J Bone Joint Surg [Br] 2002;84: [23] Kirker-Head CA, Van Sickle DC, Ek SW, et al. Safety of, and biological and functional response to, a novel metallic implant for the management of focal full-thickness cartilage defects: preliminary assessment in an animal model out to 1 year. J Orthop Res 2006;24(5): [24] Burks JB. Implant arthroplasty of the first metatarsalphalangeal joint. Clin Podiatr Med Surg 2006; 23(4): [25] Jäger M, Begg MJ, Krauspe R. Partial hemi-resurfacing of the hip joint a new approach to treat local osteochondral defects? [review]. Biomed Tech (Berl) 2006;51(5 6): [26] Scalise JJ, Miniaci A, Iannotti JP. Resurfacing arthroplasty of the humerus: indications, surgical technique, and clinical results. Techniques in Shoulder and Elbow Surgery 2007;8(3): [27] Becher C, Huber R, Thermann H, et al. Effects of a contoured articular prosthetic device on tibiofemoral peak contact pressure: a biomechanical study. Knee Surg Sports Traumatol Arthrosc 2008;16(1): [28] Baldini A, Anderson JA, Cerulli-Mariani P, et al. Patellofemoral evaluation after total knee arthroplasty. Validation of a new weight-bearing axial radiographic view. J Bone Joint Surg Am 2007;89(8): [29] Lonner JH. Patellofemoral arthroplasty. Pros, cons, and design considerations. Clin Orthop Relat Res 2004;428:
10 346 DAVIDSON & RIVENBURGH [30] Sisto DJ, Sarin VK. Custom patellofemoral arthroplasty of the knee. J Bone Joint Surg Am 2006;88: [31] Argenson JN, Guillaume JM, Aubaniac JM. Is there a place for patellofemoral arthroplasty? Clin Orthop Relat Res 1995;321: [32] Huberti HH, Hayes WC. Patellofemoral contact pressures. The influence of q-angle and tendofemoral contact. J Bone Joint Surg Am 1984;66: [33] Goodfellow J, Hungerford DS, Woods C. Patellofemoral joint mechanics and pathology. 2. Chondromalacia patellae. J Bone Joint Surg Br 1976;58: [34] Heino Brechter J, Powers CM. Patellofemoral stress during walking in persons with and without patellofemoral pain. Med Sci Sports Exerc 2002;34: [35] Ward SR, Powers CM. The influence of patella alta on patellofemoral joint stress during normal and fast walking. Clin Biomech (Bristol, Avon) 2004;19: [36] Ward SR, Terk MR, Powers CM. Influence of patella alta on knee extensor mechanics. J Biomech 2005;38: [37] Ward SR, Terk MR, Powers CM. Patella alta: association with patellofemoral alignment and changes in contact area during weight-bearing. J Bone Joint Surg Am 2007;89(8):
Hip Resurfacing System
 Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
Hip Resurfacing System The Arthrosurface HemiCAP Hip Hemiarthroplasty System restores the articular surface geometry of the femoral head and preserves functional structures using an innovative 3 dimensional
Description Materials Indications Patient selection factors to be considered include: Contraindications Absolute contraindications include:
 Description The Patello-Femoral Wave Arthroplasty Systems incorporate a distal femoral trochlear surface articular component that mates to a taper post via a taper interlock, and an all-polyethylene patella
Description The Patello-Femoral Wave Arthroplasty Systems incorporate a distal femoral trochlear surface articular component that mates to a taper post via a taper interlock, and an all-polyethylene patella
Custom Patellofemoral Arthroplasty of the Knee. Surgical Technique
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Custom Patellofemoral Arthroplasty of the Knee. Surgical Technique Domenick
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Custom Patellofemoral Arthroplasty of the Knee. Surgical Technique Domenick
Technique Guide Hip Resurfacing System
 Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
Technique Guide Hip Resurfacing System Approximately 5%-18% of all hip arthroplasties are completed on patients with a primary diagnosis of osteonecrosis. Patients are generally younger adults age 35 years
Talar Dome System Surgical Technique
 Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Talar Dome System Surgical Technique CAP TALAR DOME RESURFACING HEMIARTHROPLASTY IMPLANT Surgical Technique Guide Description The HemiCAP Contoured Articular Prosthetic incorporates an articular resurfacing
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Technique Guide Wrist Hemiarthroplasty System
 Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
Technique Guide Wrist Hemiarthroplasty System The WristMotion TM Wrist Hemiarthroplasty System restores mobility and maintains native biomechanics using a dual curvature HemiCAPITATE implant that locks
Unicompartmental Knee Replacement
 Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
WristMotion Wrist Hemiarthroplasty System Instructions for Use
 WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
WristMotion Wrist Hemiarthroplasty System Instructions for Use Description The Arthrosurface WristMotion Wrist Hemiarthroplasty System consists of a contoured capitate articular implant designed to articulate
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
CAUTION: Ceramic liners are not approved for use in the United States.
 Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
Total Hip Prostheses, Self-Centering Hip Prostheses and Hemi-Hip Prostheses IMPORTANT: This essential product information sheet does not include all of the information necessary for selection and use of
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS
 SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
SURGICAL TECHNIQUE CEMENTED & PRESS-FIT UNIFIED INSTRUMENTATION INTRAOPERATIVE FLEXIBILITY PROVEN BIOMECHANICS INTRODUCTION The Summit Tapered Hip System s comprehensive set of implants and instruments
Glenoid Resurfacing Technique Guide
 Glenoid Resurfacing Technique Guide Restoring the Freedom of Motion 2 Description The HemiCAP Contoured Articular Prosthetic humeral component incorporates an articular resurfacing component and a taper
Glenoid Resurfacing Technique Guide Restoring the Freedom of Motion 2 Description The HemiCAP Contoured Articular Prosthetic humeral component incorporates an articular resurfacing component and a taper
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Bone Preservation Stem
 TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK Bone Preservation Stem Featuring GRIPTION Coating Surgical Technique Implant Geometry Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Case report. Open Access. Abstract
 Open Access Case report Dissociation of mobile-bearing patellar component in low contact stress patellofemoral arthroplasty, its mechanism and management: two case reports Hans-Peter W van Jonbergen*,
Open Access Case report Dissociation of mobile-bearing patellar component in low contact stress patellofemoral arthroplasty, its mechanism and management: two case reports Hans-Peter W van Jonbergen*,
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical Assessment 1. Proper implant diameter is determined by placing the appropriately sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical Assessment 1. Proper implant diameter is determined by placing the appropriately sized trial over the
Technique Guide Patello-Femoral Arthroplasty
 Technique Guide Patello-Femoral Arthroplasty The HemiCAP Patello-Femoral Kahuna Arthroplasty System restores the unique articular surface geometry of the Patella and the Femoral Trochlear groove. The HemiCAP
Technique Guide Patello-Femoral Arthroplasty The HemiCAP Patello-Femoral Kahuna Arthroplasty System restores the unique articular surface geometry of the Patella and the Femoral Trochlear groove. The HemiCAP
Medial Patellofemoral Ligament (MPFL) Surgical Technique
 Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Medial Patellofemoral Ligament (MPFL) Surgical Technique Medial Patellofemoral Ligament The medial patellofemoral complex, consisting of the medial patellofemoral ligament (MPFL) and the medial patellotibial
Integra Cadence Total Ankle System PATIENT INFORMATION
 Integra Cadence Total Ankle System PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal Fibular
Integra Cadence Total Ankle System PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal Fibular
Why precision is powerful
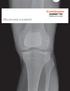 Why precision is powerful A new answer for isolated patellofemoral OA First generation PFJ implants had sharp, constraining trochlear grooves and were prone to complications such as maltracking and catching
Why precision is powerful A new answer for isolated patellofemoral OA First generation PFJ implants had sharp, constraining trochlear grooves and were prone to complications such as maltracking and catching
Arthroscopically assisted Knee Resurfacing (AKR)
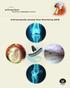 Arthroscopically assisted Knee Resurfacing (AKR) U The First Meniscal Sparing Knee Resurfacing Preserves meniscus & articular cartilage Maintains soft tissue envelope Inlay components match patient anatomy
Arthroscopically assisted Knee Resurfacing (AKR) U The First Meniscal Sparing Knee Resurfacing Preserves meniscus & articular cartilage Maintains soft tissue envelope Inlay components match patient anatomy
Surgical Technique Final Trial Reduction and Component Implantation of
 Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Surgical Technique Final Trial Reduction and Component Implantation of TC *smith&nephew TC-PLUS PRIMARY Mobile Bearing TC-PLUS PRIMARY Mobile Bearing Final Trial Reduction and Component Implantation of
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patella Planing System
 REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
REFERENCE GUIDE AND SURGICAL TECHNIQUE Patella Planing System SPECIALIST INSTRUMENTS AN ONLAY PATELLA PREPARATION SYSTEM TECHNIQUE FOR PRIMARY PATELLAR RESURFACING The Specialist 2 Patellar Planer System
TaperFill. Surgical Technique
 TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
TaperFill Surgical Technique Table of Contents Indications and Contraindications 3 TaperFill Hip Size Charts 4-5 DJO Surgical 9800 Metric Boulevard Austin, TX (800) 456-8696 www.djosurgical.com Preoperative
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Bipolar Radial Head System
 Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
Bipolar Radial Head System Katalyst Surgical Technique DESCRIPTION The Katalyst Telescoping Bipolar Radial Head implant restores the support and bearing surface of the radial head in the face of fracture,
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
PLR. Proximal Loading Revision Hip System
 PLR Proximal Loading Revision Hip System The PLR splined revision stem is designed to recreate the natural stresses in the revised femur, where proximal bone may be compromised. PLR Hip System Design Considerations
PLR Proximal Loading Revision Hip System The PLR splined revision stem is designed to recreate the natural stresses in the revised femur, where proximal bone may be compromised. PLR Hip System Design Considerations
Integra. Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE
 Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
Integra Katalyst Bipolar Radial Head System SURGICAL TECHNIQUE Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical
Total Knee Replacement
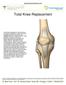 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
The Problem of Patellofemoral Pain. The Low Back Pain of the Lower Extremity. Objectives. Christopher M. Powers, PhD, PT, FACSM, FAPTA
 Mechanisms Underlying Patellofemoral Joint Pain: What have we learned over the last 20 years? Professor Co Director, Musculoskeletal Biomechanics Research Laboratory Objectives 1. Highlight recent research
Mechanisms Underlying Patellofemoral Joint Pain: What have we learned over the last 20 years? Professor Co Director, Musculoskeletal Biomechanics Research Laboratory Objectives 1. Highlight recent research
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Technique Guide Toe Hemiarthroplasty
 Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty
 Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Technique Guide Toe Hemiarthroplasty The HemiCAP Toe Resurfacing Systems restore the surface geometry of the metatarsal head and preserve functional structures using an innovative 3 dimensional mapping
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Biomechanics of. Knee Replacement. Mujda Hakime, Paul Malcolm
 Biomechanics of Knee Replacement Mujda Hakime, Paul Malcolm 1 Table of contents Knee Anatomy Movements of the Knee Knee conditions leading to knee replacement Materials Alignment and Joint Loading Knee
Biomechanics of Knee Replacement Mujda Hakime, Paul Malcolm 1 Table of contents Knee Anatomy Movements of the Knee Knee conditions leading to knee replacement Materials Alignment and Joint Loading Knee
Mako Partial Knee Patellofemoral
 Mako Partial Knee Patellofemoral Mako Robotic-Arm Assisted Surgery Surgical reference guide Table of contents Implant compatibility.... 3 Pre-operative implant planning... 4 Intra-operative planning....
Mako Partial Knee Patellofemoral Mako Robotic-Arm Assisted Surgery Surgical reference guide Table of contents Implant compatibility.... 3 Pre-operative implant planning... 4 Intra-operative planning....
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Surgical Technique. *smith&nephew JOURNEY PFJ OXINIUM Patellofemoral Joint with Oxidized Zirconium
 Surgical Technique *smith&nephew JOURNEY PFJ OXINIUM Patellofemoral Joint with Oxidized Zirconium Surgical Technique JOURNEY PFJ Patellofemoral Joint with OXINIUM Oxidized Zirconium Contents Product Overview...2
Surgical Technique *smith&nephew JOURNEY PFJ OXINIUM Patellofemoral Joint with Oxidized Zirconium Surgical Technique JOURNEY PFJ Patellofemoral Joint with OXINIUM Oxidized Zirconium Contents Product Overview...2
Surgical Technique. Hip System
 Surgical Technique Hip System INDICATIONS FOR USE The TaperSet Hip System is designed for total or partial hip arthroplasty and is intended to be used with compatible components of the Consensus Hip System.
Surgical Technique Hip System INDICATIONS FOR USE The TaperSet Hip System is designed for total or partial hip arthroplasty and is intended to be used with compatible components of the Consensus Hip System.
Resurfacing Patellar Preparation
 Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Recurrent subluxation or dislocation after surgical
 )263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
)263( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY CASE REPORT Persistent Medial Subluxation of the Ulna with Radiotrochlear Articulation Amir R. Kachooei, MD; David Ring, MD, PhD Research
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Patellofemoral Osteoarthritis
 Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Patellofemoral Osteoarthritis Arthritis of the patellofemoral joint refers to degeneration (wearing out) of the cartilage on the underside of the patella (kneecap) and the trochlea (groove) of the femur.
Over 20 Years of Proven Clinical Success. Zimmer Natural-Knee II System
 Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Patellofemoral Replacement
 Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
Doron Sher. 160 Belmore Rd, Randwick Burwood Rd, Concord. MBBS, MBiomedE, FRACS FAOrthA
 Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Doron Sher MBBS, MBiomedE, FRACS FAOrthA 160 Belmore Rd, Randwick 47 49 Burwood Rd, Concord www.kneedoctor.com.au www.orthosports.com.au Medial PatelloFemoral (MPFL) And AnteroLateral Ligament (ALL) Reconstruction
Partial Knee Replacement
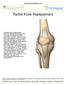 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Clinical Evaluation Surgical Technique
 Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
Clinical Evaluation Surgical Technique Table of Contents EMPERION Specifications 3 EMPERION Surgical Technique 9 EMPERION Catalog 18 Nota Bene: This technique description herein is made available to the
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
A novel cementless option. Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
 A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
Integra. Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION
 Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
PARTIAL KNEE REPLACEMENT
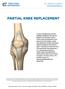 PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
TOTAL KNEE ARTHROPLASTY (TKA)
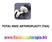 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
SURGICAL TECHNIQUE. Alpine Cementless Hip Stem
 SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
UDHT08.1.qxd:UDHT /03/08 17:14 Page 1. Surgical. Technique. Elbow Prosthesis. RHS Radial Head System.
 UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
 Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Use of a partial humeral head resurfacing system for management of an osseous mechanic... Page 1 of 12 Int J Shoulder Surg. 2011 Jan-Mar; 5(1): 17 20. doi: 10.4103/0973-6042.80465. PMCID: PMC3109768 Copyright
Modular Ulnar Head surgical technique. Transforming Extremities
 First Choice Modular Ulnar Head surgical technique Transforming Extremities instrumentation Head and Collar Trials Assembly Pad Starter Awl Trial Extractor Osteotomy Guide Stem Trials Implant Impactor
First Choice Modular Ulnar Head surgical technique Transforming Extremities instrumentation Head and Collar Trials Assembly Pad Starter Awl Trial Extractor Osteotomy Guide Stem Trials Implant Impactor
Why do I perform PFP? Fernando Fonseca, MD PhD Head of Department Orthopaedics
 Why do I perform PFP? Fernando Fonseca, MD PhD Head of Department Orthopaedics Acknowledges to António Completo Paulo Flores Susana Meireles André Castro Disclosures: None ... Knee is one of the most complex
Why do I perform PFP? Fernando Fonseca, MD PhD Head of Department Orthopaedics Acknowledges to António Completo Paulo Flores Susana Meireles André Castro Disclosures: None ... Knee is one of the most complex
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Surgical. Technique. AEQUALIS Spherical Base Glenoid. Shoulder Prosthesis.
 Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Surgical Technique Shoulder Prosthesis AEQUALIS Spherical Base Glenoid www.tornier.com CONTENTS CONTENTS 1. Subscapularis 2. Anterior capsule 3. Humeral protector 4. Inserting retractors 1. DESIGN FEATURES
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Chondral Disease of the Knee
 Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
Chondral Disease of the Knee Chondral Disease of the Knee A Case-Based Approach Brian J. Cole, MD, MBA Associate Professor, Department of Orthopedics and Department of Anatomy and Cell Biology Director,
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Fixed and Variable Geometry Total Shoulder Arthroplasty
 Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Fixed and Variable Geometry Total Shoulder Arthroplasty RECOVERY FUNCTION SURVIVORSHIP DePuy believes in an approach to total shoulder replacement that places equal importance on recovery, function and
Resurfacing Distal Femur. Orthopaedic Salvage System
 Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
THE P.F.C. SIGMA FEMORAL ADAPTER. Surgical Technique
 THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
S h o u l d e r Solutions by Tornier C o n v e r T i b l e S h o u l d e r S y S T e m
 S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
S h o u l d e r Solutions by Tornier C o n v e r t i b l e s h o u l d e r s y s t e m C o n v e r t i b l e s h o u l d e r s y s t e m A n a t o m i c Aequalis Ascend Flex - UDZF131 One System. Two Solutions.
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Tradition Hip Primary Surgical Technique
 Design Rationale Many total hip designs in today s marketplace do not take advantage of the known forces present in the femur. Long term stability of a total hip prosthesis requires an implant design and
Design Rationale Many total hip designs in today s marketplace do not take advantage of the known forces present in the femur. Long term stability of a total hip prosthesis requires an implant design and
BICEPTOR Tenodesis System
 BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
