3 Femoral fractures 3.11 I Proximal femoral fractures - Management with minimal resources
|
|
|
- Tabitha Flowers
- 5 years ago
- Views:
Transcription
1 1 Executive Editor: Chris Colton Author: Paul Demmer 3.11 I Proximal femoral fractures - Management with minimal resources Indication All proximal femoral fractures 1 Introduction Fractures of the upper end of the femur should be treated operatively. They should only be considered for nonoperative fracture treatment if there are neither facilities, nor skills, for surgical treatment. 2 First Aid The ABC of primary care for the injured always takes precedence over the fracture treatment. Once the safety of the patient has been established, attention is directed to the fracture. It is important in treating any femoral fracture to splint the whole leg as soon as possible, and before transport of the patient. For that purpose you need two firm boards or sticks along the leg, suitably padded, one on the inside and one along the leg and the body on the outside. 1 of 10
2 Any soft material such as clothing, blankets, etc. can be used as emergency padding. The splints should then be kept in place by bandages around both splints and the leg as well as the body. Suitably splinted, the patient can be transported to the chosen hospital facility. If no boards are available some stabilization can be achieved by splinting the fractured leg to the uninjured leg, with padding in between. 3 Principles Once a radiological diagnosis has been made, decisions about non-operative management can be taken. For non-impacted intracapsular fractures, the best nonsurgical care is to relieve pain and mobilize the patient despite the fracture. These fractures will not unite with non-surgical treatment and mobilization of the patient as a whole is of paramount importance. If a radiological diagnosis is not available, the possibility of a displaced intracapsular fracture of the proximal femur may be suggested by external rotation with slight to moderate shortening (2.5 5 cm), which increases only slightly with proximally directed pressure on the leg. Non-operative treatment of such patients is not based upon bone healing, which, as noted, does not occur without surgical treatment. Traction can be omitted, or discontinued and the patient mobilized as soon as comfort permits. 2 of 10
3 If there is marked thigh shortening which increases progressively, or is associated with palpable bone deformity, the patient is more likely to have an extracapsular fracture with potential for healing. Patients with these injuries are reasonable candidates for 6-8 weeks of traction, as described below, followed by progressive ambulation, with delayed weightbearing, in hopes of avoiding excessive deformity. For proximal femur fractures that are likely to be extracapsular (pertrochanteric or subtrochanteric), the non-operative regimen is as follows. 3.1 Straight skin traction Nonoperative treatment means that the patient will be in some form of traction for at least 6-8 weeks, often weeks. The preliminary treatment usually is straight skin traction, later converted to skeletal traction. Note the padding under the patient s calf, to keep the heel from pressing on the bed beneath it. Disadvantages of prolonged skin traction are: Loosening Constriction Friction with skin irritation Allergy 3.2 Hamilton-Russell (balanced) skin traction If skin traction is likely to be used for more than 24 hours, greater patient comfort and better control of the fracture can be achieved by using Hamilton-Russell skin traction. To apply Hamilton-Russell traction, a dedicated orthopedic bed, or a standard bed in combination with a mobile Balkan beam frame, is needed. A padded sling is placed behind the slightly flexed knee and skin traction applied to the lower leg. The traction cord and pulley system are shown here. The principle of the parallelogram of forces determines that the upward pull of the sling and the longitudinal pull of the skin traction create a resolution of force in the line of the femur, as illustrated. This configuration of traction and leg support also can be adjusted to control femoral rotation, by directing the upward support medially or laterally. Generally, to minimize external rotation at the fracture, the patella should be pointing upward, nearly perpendicular to the bed surface. 3 of 10
4 A simpler alternative to this technique involves two separate systems. a sling suspended from the overhead frame, or supported with a rope and pulley counterweight, to provide an upward force, which lifts the leg off the bed longitudinal (distal) traction applied with skin or skeletal technique. The resulting vector force, as illustrated, is oblique, the vector sum of the upward and distal forces applied by the two weights. Note: With any longitudinal traction, the foot of the bed must be raised, tilting the bed, to avoid the traction weight s pulling the patient down the bed. With the tilted bed the weight of the patient acts as countertraction. 4 Skin traction 4.1 Application This photograph shows a commercially available skin traction kit. A simple skin traction kit can be made easily, from a roll of non-elastic adhesive strapping (approximately 3 inches, 8 cms, wide), some foam padding for the malleolar region and a wooden spacer block (suitably drilled for cord attachment). Tinct. benz. co. Non-elastic adhesive strapping Wooden spacer with hole 2 strips of foam Cotton bandage 4 of 10
5 Prior to the application of the adhesive traction strip, the skin is painted with friar s balsam (Tinct. benz.co.), or equivalent. The strip is then applied to the lower leg, from the level of the knee. The strapping is applied to the inner side of the leg, then unrolled a little further, to allow placement of the spacer and of the foam; it can then be applied to the outer side of the leg. It is important to ensure that the wooden spacer lies transversely, i.e. parallel to the sole of the foot. To prevent the development of blisters, the skin traction needs to be applied without folds or creases in the adhesive material and the covering bandage should be non-elastic. Should a crease be inevitable, due to the contour of the limb, the creased area should be lifted, partially slit transversally and the edges overlapped. 5 of 10
6 Once the adhesive strip is satisfactorily in place, ensuring that the padded lower section overlies the malleoli, an inelastic bandage is carefully wrapped around the limb from just above the malleoli to the top of the strip. Apply the overlying bandages spirally, overlapping by half. 5 Skeletal traction The initial skin traction should soon be converted to skeletal traction via a tibial pin. 6 of 10
7 5.1 Preparation for applying skeletal traction This is greatly aided by the use of a pre-assembled, sterile pack, containing the following items: Sterile towels Disinfectant Syringe Needles Local anaesthetic Scalpel with pointed blade Sharp pointed Steinmann pin, or Denham pin Jacobs chuck with T-handle Stirrup 5.2 Local anesthesia After painting the skin with antiseptic and draping with sterile towels, inject a bolus of local anesthesia (5 ml of 2% lignocaine) on each side of the tibial tuberosity, into the lateral skin at the proposed site of pin insertion and medially at the anticipated exit point, infiltrating down to the periosteum. 25 ml 20 ml 15 ml 10 ml 5 ml 5 ml 10 ml 15 ml 20 ml 25 ml 5 ml each side 5.3 Insertion of traction pin At the entry point, a stab incision is made through the skin with a pointed scalpel. A Steinmann, or preferably a Denham pin (a Denham pin has a short threaded section in the centre to prevent side-to-side motion of the pin in the bone), mounted in the T-handle, is inserted manually at a point about 2 cm dorsal to the tibial tuberosity. 2 cm As the pin is felt to penetrate the far cortex, check that the exit will coincide with the area of local anaesthetic infiltration. If not, inject additional local anaesthetic. Once the point of the pin clearly declares its exit site, make a small stab incision in the overlying skin. Once the pin is in place, ensure that there is no tension on the skin at the entry and exit points. If there is, then a small relieving incision may be necessary. 7 of 10
8 5.4 Traction setup It is important that the stirrup be freely mobile around the traction pin, to prevent rotation of the pin within the bone. Rotating pins loosen quickly and significantly increase the risk of pin track infection. Mobile stirrup Fixing screw Traction pin Application of upward and distal forces to the skeletal traction pin. A rope tied to the traction pin stirrup can apply the upward force. Distal force can then be applied separately via a loop of rope tied to each end of the pin and running distally along the medial and lateral surfaces of the calf. This must be padded to protect the skin, and a spreader (usually wood) distal to the foot is essential to avoid pressure on the malleoli. Another alternative is to make a Nissen-type traction loop, as illustrated. These were previously available commercially, but now probably will require local fabrication, if desired. 8 of 10
9 Often the simplest alternative is to use a single rope from the traction pin stirrup, directed overhead and distally through a pulley (and then through a second pulley at the foot of the bed). The position of the first pulley determines the force vector (direction) of the traction, presuming the patient remains in the selected location. Weight and direction of the traction should be adjusted to lift the knee approximately one fist-width off the bed. Pillows under the calf support the lower leg, prevent excessive knee flexion, and keep the heel off the bed, as shown. 5.5 Pin care In order to prevent pin track infection, apply a slit gauze swab (sponge) as a dressing around the pin and do not remove the crust that develops around the pin on the skin. The gauze swab should only be changed infrequently. Gauze swap 6 Mobilization in bed Assisted active mobilization and chest physiotherapy should start from day one. With the aid of a monkey chain as shown, the patient can lift himself up and the traction system allows mobilization of the knee. 9 of 10
10 7 Aftercare General guidelines Intertrochanteric fractures usually stabilize within 6-8 weeks and changing to touch weight bearing on crutches should then be considered. At this stage an x-ray is highly desirable to give further information on healing. Visible bridging callus suggests that progressive weightbearing can begin. If radiography is not available, mobilization in bed can typically be started 6-8 weeks after injury, and progressed as tolerated, encouraging the patient to use walking aids for support, to minimize pain at the fracture site. The ability to bear full weight without pain is a good sign of fracture healing. Discharge to home care should be delayed until the patient can get in and out of bed independently, and is mobile on crutches. The patient in homecare should not sit for prolonged periods in a chair, if avoidable, as this will lead to a flexion contracture at the hip joint. Note: Non-weight bearing involves flexion of the hip which can greatly increase the angular load on the healing fracture. Many surgeons believe that touch weight bearing, which allows the healing femur to be more vertical, is safer at this stage. From about 10 weeks onwards partial weight bearing should be started and increased to full weight bearing at +/ weeks. 10 of 10
3 Femoral fractures 3.12 II Femoral shaft fractures - Temporary Thomas splint
 1 Executive Editor: Chris Colton Authors: Peter V Giannoudis, Hans Christoph Pape, Michael Schütz 3 Femoral fractures Indication All femoral shaft fractures 1 General considerations 1.1 Thomas splint Temporary
1 Executive Editor: Chris Colton Authors: Peter V Giannoudis, Hans Christoph Pape, Michael Schütz 3 Femoral fractures Indication All femoral shaft fractures 1 General considerations 1.1 Thomas splint Temporary
LESSON ASSIGNMENT. After completing this lesson, you should be able to: be able to:
 LESSON ASSIGNMENT LESSON 4 Fractures of the Lower Extremities. LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: be able to: 4-1. Identify
LESSON ASSIGNMENT LESSON 4 Fractures of the Lower Extremities. LESSON ASSIGNMENT Paragraphs 4-1 through 4-8. LESSON OBJECTIVES After completing this lesson, you should be able to: be able to: 4-1. Identify
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Traction Splints. LESSON ASSIGNMENT Paragraphs 3-1 through 3-5. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify the purpose of a traction
LESSON ASSIGNMENT LESSON 3 Traction Splints. LESSON ASSIGNMENT Paragraphs 3-1 through 3-5. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify the purpose of a traction
Case Study: Christopher
 Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Case Study: Christopher Conditions Treated Anterior Knee Pain, Severe Crouch Gait, & Hip Flexion Contracture Age Range During Treatment 23 Years to 24 Years David S. Feldman, MD Chief of Pediatric Orthopedic
Are you suffering from heel pain? We can help you!
 Are you suffering from heel pain? We can help you! STOP THE PAIN! Heel pain can be effectively combated with the proven Body Armor Night Splint. Heel spurs and heel pain Why? Heel pain is among the most
Are you suffering from heel pain? We can help you! STOP THE PAIN! Heel pain can be effectively combated with the proven Body Armor Night Splint. Heel spurs and heel pain Why? Heel pain is among the most
The DM Systems Family of Wound Care Products. Wound Care
 The DM Systems Family of Wound Care Products Wound Care Wound Care The Heelift Family After the sacrum, the heel is the second most common site where pressure ulcers develop. Now that the Centers for Medicare
The DM Systems Family of Wound Care Products Wound Care Wound Care The Heelift Family After the sacrum, the heel is the second most common site where pressure ulcers develop. Now that the Centers for Medicare
Fractures Healing & Management. Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4
 Fractures Healing & Management Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4 Fractures Despite their strength, bones are susceptible to fractures. In young people, most fractures result from trauma
Fractures Healing & Management Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4 Fractures Despite their strength, bones are susceptible to fractures. In young people, most fractures result from trauma
4 Tibial and malleolar fractures 4.12 I Tibial shaft fractures Management with limited resources
 1 Executive Editor: Peter Trafton Authors: Paul Demmer, with Chris Colton as Editorial Consultant 4 Tibial and malleolar fractures 4.12 I Tibial shaft fractures Management with limited resources Indication
1 Executive Editor: Peter Trafton Authors: Paul Demmer, with Chris Colton as Editorial Consultant 4 Tibial and malleolar fractures 4.12 I Tibial shaft fractures Management with limited resources Indication
Application of Cast Brace for Post Acute Care of Lower Extremity Fractures
 Application of Cast Brace for Post Acute Care of Lower Extremity Fractures Roy Snelson, C.P.O.*, George Irons, C.P.O.**, and Vert Mooney, M.D.*** The fracture cast brace is designed to allow early ambulation
Application of Cast Brace for Post Acute Care of Lower Extremity Fractures Roy Snelson, C.P.O.*, George Irons, C.P.O.**, and Vert Mooney, M.D.*** The fracture cast brace is designed to allow early ambulation
A Single-Bar Above-Knee Orthosis
 A Single-Bar Above-Knee Orthosis Robert O. Nitschke,* C.P.O. I would like to present a different approach to the design of aboveknee, or "long leg", orthoses. When weight-bearing is not necessary, I have
A Single-Bar Above-Knee Orthosis Robert O. Nitschke,* C.P.O. I would like to present a different approach to the design of aboveknee, or "long leg", orthoses. When weight-bearing is not necessary, I have
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
PediLoc 3.5mm and 4.5mm Contour Femur Plate Surgical Technique Surgical Technique Contour Femur Plate The technique description herein is made available to the healthcare professional to illustrate the
Injuries to the Extremities
 Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
Orthotics Measurement Board for Tibial Torsion and Toe-Out
 Orthotics Measurement Board for Tibial Torsion and Toe-Out HANS R. LEHNEIS, C.P.O. 2 COORDINATED function of the brace-anatomical complex is dependent upon the configuration and fit of the brace with the
Orthotics Measurement Board for Tibial Torsion and Toe-Out HANS R. LEHNEIS, C.P.O. 2 COORDINATED function of the brace-anatomical complex is dependent upon the configuration and fit of the brace with the
Patient Guide. Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening
 Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Technique Manual Technique Manual Rev. A 01/11/2011
 Technique Manual Technique Manual Table of Contents Introduction 4 Indications 5 Instrumentation 6 Frame Assembly 7 Position Guide 8-9 Tips and Tricks 10-13 Cleaning 14 Sterilization 14 Storage Instructions
Technique Manual Technique Manual Table of Contents Introduction 4 Indications 5 Instrumentation 6 Frame Assembly 7 Position Guide 8-9 Tips and Tricks 10-13 Cleaning 14 Sterilization 14 Storage Instructions
Essential intervention No. 3 Oedema control KEY OBJECTIVES. Danger
 Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
ANKLE SPRAINS. Explanation. Causes. Symptoms
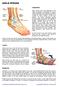 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ORTHOSCAN MOBILE DI POSITIONING GUIDE
 ORTHOSCAN MOBILE DI POSITIONING GUIDE Table of Contents SHOULDER A/P of Shoulder... 4 Tangential (Y-View) of Shoulder... 5 Lateral of Proximal Humerus... 6 ELBOW A/P of Elbow... 7 Extended Elbow... 8 Lateral
ORTHOSCAN MOBILE DI POSITIONING GUIDE Table of Contents SHOULDER A/P of Shoulder... 4 Tangential (Y-View) of Shoulder... 5 Lateral of Proximal Humerus... 6 ELBOW A/P of Elbow... 7 Extended Elbow... 8 Lateral
Extracapsular Repair Monofilament Nylon Suture
 Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Gwinnett Medical Center. Sports Medicine Program Skills Guide
 Gwinnett Medical Center Sports Medicine Program Skills Guide To find information about this event, including speakers and digital copies of this skills guide, visit: gwinnettmedicalcenter.org/sportsclinics
Gwinnett Medical Center Sports Medicine Program Skills Guide To find information about this event, including speakers and digital copies of this skills guide, visit: gwinnettmedicalcenter.org/sportsclinics
Meniscus Repair Rehabilitation Protocol
 Meniscus Repair Rehabilitation Protocol GENERAL GUIDELINES - Use the cryotherapy cuff continuously for the first 72 hours, then as needed thereafter - Ensure that the cuff never contacts the skin directly
Meniscus Repair Rehabilitation Protocol GENERAL GUIDELINES - Use the cryotherapy cuff continuously for the first 72 hours, then as needed thereafter - Ensure that the cuff never contacts the skin directly
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR
 GENERAL GUIDELINES ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR - The local anesthetic (similar to novacaine) in your knee lasts 6-12 hours - Start taking the pain medication as soon
GENERAL GUIDELINES ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR - The local anesthetic (similar to novacaine) in your knee lasts 6-12 hours - Start taking the pain medication as soon
Aesculap Targon FN. Head Preserving Solution for Medial Femoral Neck Fractures. Aesculap Orthopaedics
 Aesculap Targon FN Head Preserving Solution for Medial Femoral Neck Fractures Aesculap Orthopaedics Targon FN Operating Technique Indications for Targon FN AO 3 B. AO 3 B.2 AO 3 B.3 Undisplaced intracapsular
Aesculap Targon FN Head Preserving Solution for Medial Femoral Neck Fractures Aesculap Orthopaedics Targon FN Operating Technique Indications for Targon FN AO 3 B. AO 3 B.2 AO 3 B.3 Undisplaced intracapsular
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Instructions For Use. Surgical Technique
 Instructions For Use Surgical Technique English Instructions for use Intended use INTELLIGENT ORTHOPAEDICS instruments consist of manual surgical instruments and devices intended for use in surgical procedures.
Instructions For Use Surgical Technique English Instructions for use Intended use INTELLIGENT ORTHOPAEDICS instruments consist of manual surgical instruments and devices intended for use in surgical procedures.
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL
 ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
16 th Annual Primary Care & Sports Medicine Symposium January 29th, 2016
 To help protect your privacy, PowerPoint has blocked automatic download of this picture. 16 th Annual Primary Care & Sports Medicine Symposium January 29th, 2016 Excellence in Orthopaedics Through Education
To help protect your privacy, PowerPoint has blocked automatic download of this picture. 16 th Annual Primary Care & Sports Medicine Symposium January 29th, 2016 Excellence in Orthopaedics Through Education
Title: EZ-IO. Effective Date: January SOG Number: EMS Rescinds:
 S O G Title: EZ-IO Effective Date: January 2010 SOG Number: EMS - 25 Rescinds: Scope: Providers Authorized are AIC s in the following certifications EMT-I and EMT-P who have been trained and cleared by
S O G Title: EZ-IO Effective Date: January 2010 SOG Number: EMS - 25 Rescinds: Scope: Providers Authorized are AIC s in the following certifications EMT-I and EMT-P who have been trained and cleared by
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
THE HUMERUS 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW
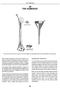 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Shoulder Dislocation. Explanation. Causes. Symptoms. Treatment. Diagnosis
 Shoulder Dislocation Explanation A dislocated shoulder occurs when the humerus separates from the scapula at the glenohumeral joint, or in simpler terms, the head of the upper arm bone (humerus) is dislodged
Shoulder Dislocation Explanation A dislocated shoulder occurs when the humerus separates from the scapula at the glenohumeral joint, or in simpler terms, the head of the upper arm bone (humerus) is dislodged
Kinesiology Tape. Table of contents:
 1 Kinesiology Tape Welcome to the Anuva application center. These application guidelines and general use instructions are intended to be used with Anuve professional quality Kinesiology tape and if followed
1 Kinesiology Tape Welcome to the Anuva application center. These application guidelines and general use instructions are intended to be used with Anuve professional quality Kinesiology tape and if followed
The nomenclature describing the orthosis is basically the same as that suggested for the molded ankle-foot orthosis (2), but the anterior shank enclos
 VACUUM-FORMED ORTHOSES FOR FRACTURE OF THE TIBIA 1 Melvin Stills, C.O. 2 The routine management of fractures of the long bones of the lower limb infers immobilization by use of plaster casts extending
VACUUM-FORMED ORTHOSES FOR FRACTURE OF THE TIBIA 1 Melvin Stills, C.O. 2 The routine management of fractures of the long bones of the lower limb infers immobilization by use of plaster casts extending
QUICK REFERENCE GUIDE. The PreFix Fixator (92000 Series) ALWAYS INNOVATING
 21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
21 The PreFix Fixator (92000 Series) ALWAYS INNOVATING INTRODUCTION The PreFix fixator is designed to provide temporary external fixation. This may be needed when local facilities or the condition of the
OPERATING MANUAL AND TECHNIQUE GUIDE FOR TITANIUM FEMORAL AND TIBIAL NAILING SYSTEMS
 OPERATING MANUAL AND TECHNIQUE GUIDE FOR TITANIUM FEMORAL AND TIBIAL NAILING SYSTEMS ORTHO-MEDICAL GMBH TITANIUM FEMORAL NAIL OPERATIVE TECHNIQUE Introduction: Why a new type of femoral nail? The latest
OPERATING MANUAL AND TECHNIQUE GUIDE FOR TITANIUM FEMORAL AND TIBIAL NAILING SYSTEMS ORTHO-MEDICAL GMBH TITANIUM FEMORAL NAIL OPERATIVE TECHNIQUE Introduction: Why a new type of femoral nail? The latest
PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique
 PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique 2957 Bow Broch_REV_B.indd 1 2/10/11 12:47 PM Surgical Technique Bowed Femur Plate The technique description herein is made available to the
PediLoc 3.5mm and 4.5mm Bowed Femur Plate Surgical Technique 2957 Bow Broch_REV_B.indd 1 2/10/11 12:47 PM Surgical Technique Bowed Femur Plate The technique description herein is made available to the
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 6 Roller Bandages. LESSON ASSIGNMENT Paragraphs 6-1 through 6-10. LESSON OBJECTIVES After completing this lesson, you should be able to: 6-1. Identify the functions of roller bandages.
LESSON ASSIGNMENT LESSON 6 Roller Bandages. LESSON ASSIGNMENT Paragraphs 6-1 through 6-10. LESSON OBJECTIVES After completing this lesson, you should be able to: 6-1. Identify the functions of roller bandages.
Ellipse Rehab Phase 2 Strengthening
 Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
Early Elbow Motion Protocol Ligament Repair of the elbow
 499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
Functional Movement Screen (Cook, 2001)
 Functional Movement Screen (Cook, 2001) TEST 1 DEEP SQUAT Purpose - The Deep Squat is used to assess bilateral, symmetrical, mobility of the hips, knees, and ankles. The dowel held overhead assesses bilateral,
Functional Movement Screen (Cook, 2001) TEST 1 DEEP SQUAT Purpose - The Deep Squat is used to assess bilateral, symmetrical, mobility of the hips, knees, and ankles. The dowel held overhead assesses bilateral,
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Correcting Joint Contractures
 559 Correcting Joint Contractures CHAPTER 59 In this chapter we discuss different aids used for gradually straightening limbs that have joint contractures. Information on contractures, their causes and
559 Correcting Joint Contractures CHAPTER 59 In this chapter we discuss different aids used for gradually straightening limbs that have joint contractures. Information on contractures, their causes and
Fig. 1. Lateral view of the patient showing stockinet in place and indelible pencil marks indicating areas where modification of the positive model wi
 Femoral Immobilizer CHARLES H. PRITHAM 1 MELVIN L. STILLS 2 During the past ten years orthotics has come to play a role in the treatment of selected patients with fractures of the femur. Fundamentally,
Femoral Immobilizer CHARLES H. PRITHAM 1 MELVIN L. STILLS 2 During the past ten years orthotics has come to play a role in the treatment of selected patients with fractures of the femur. Fundamentally,
Exercises following Copeland Surface Replacement Arthroplasty (CSRA)
 Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Provision of Rotational Stability: Prevention of Collapse: Closed Fracture Reduction: Minimally Invasive Surgery with no Exposure of the Fracture:
 INTRODUCTION Percutaneous Compression Plating was developed by considering each of the stages in the surgical procedure for pertrochanteric fractures and the ways in which these might be improved. Primary
INTRODUCTION Percutaneous Compression Plating was developed by considering each of the stages in the surgical procedure for pertrochanteric fractures and the ways in which these might be improved. Primary
Monster Walk Stand with your feet slightly closer than shoulder-width apart in an athletic stance. Loop an elastic band around your ankles.
 Off-season Lower-Body Tennis Exercises Research conducted on elite tennis players shows that lower-body strength is the same on both the left and right sides. Therefore, lower-body training for tennis
Off-season Lower-Body Tennis Exercises Research conducted on elite tennis players shows that lower-body strength is the same on both the left and right sides. Therefore, lower-body training for tennis
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
The Transtibial Amputation
 The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
Anterior Approach. Skills Stations
 Anterior Approach Skills Stations Anterior Approach Draping Option One Extra large drape Clear drape Step 1 Use a clear U drape (non sterile) around operative area and towards the foot. Tip: A towel wrapped
Anterior Approach Skills Stations Anterior Approach Draping Option One Extra large drape Clear drape Step 1 Use a clear U drape (non sterile) around operative area and towards the foot. Tip: A towel wrapped
Speed Your Recovery. After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint.
 FO R THE TO TAL KNEE REPLACEMENT PATIENT Speed Your Recovery After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint. The exercises may
FO R THE TO TAL KNEE REPLACEMENT PATIENT Speed Your Recovery After your knee surgery, you will need to perform exercises to strengthen the muscles that affect the replacement joint. The exercises may
A3.1 Simple, oblique A3.2 Simple, transverse A3.3 Comminuted
 Dynamic hip screw (DHS) - Indications A1 Fractures in the trochanter region, simple pertrochanteric A1.1 Along the intertrochanteric line A1.2 Through the greater trochanter A1.3 Extending distal to the
Dynamic hip screw (DHS) - Indications A1 Fractures in the trochanter region, simple pertrochanteric A1.1 Along the intertrochanteric line A1.2 Through the greater trochanter A1.3 Extending distal to the
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
Guide to Knee Surgery
 Guide to Knee Surgery Jeffrey B. Witty, M.D. North Oaks Orthopaedic Specialty Center Hammond, LA 70403 Day phone: (985) 230 2663 After hours number: (985) 345-2700 Fax: (985) 230 2665 Website: drjeffreywitty.com
Guide to Knee Surgery Jeffrey B. Witty, M.D. North Oaks Orthopaedic Specialty Center Hammond, LA 70403 Day phone: (985) 230 2663 After hours number: (985) 345-2700 Fax: (985) 230 2665 Website: drjeffreywitty.com
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Functional Movement Test. Deep Squat
 Functional Movement Test Put simply, the FMS is a ranking and grading system that documents movement patterns that are key to normal function. By screening these patterns, the FMS readily identifies functional
Functional Movement Test Put simply, the FMS is a ranking and grading system that documents movement patterns that are key to normal function. By screening these patterns, the FMS readily identifies functional
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Surgical Technique.
 Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
Developed by: Physiotherapy Department Surrey Memorial Hospital. Printshop #
 Developed by: Physiotherapy Department Surrey Memorial Hospital Printshop # 255171 The following exercises are intended for you to continue at home. Your physiotherapist will teach and mark the exercises
Developed by: Physiotherapy Department Surrey Memorial Hospital Printshop # 255171 The following exercises are intended for you to continue at home. Your physiotherapist will teach and mark the exercises
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
Novelties BORT. Benefit on your side. Support for better mobility for the aged. We constantly develop new care solutions for you.
 Novelties 2016 First class quality products for every joint Extended product diversity supports your all-round care Support for better mobility for the aged. BORT Novelties We constantly develop new care
Novelties 2016 First class quality products for every joint Extended product diversity supports your all-round care Support for better mobility for the aged. BORT Novelties We constantly develop new care
Ankle Rehabilitation with Wakefield Sports Clinic
 Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Exercises following arthroscopic (or open) anterior stabilisation
 Physiotherapy patient information Exercises following arthroscopic (or open) anterior stabilisation Introduction The shoulder joint is designed to give a large amount of movement, therefore support from
Physiotherapy patient information Exercises following arthroscopic (or open) anterior stabilisation Introduction The shoulder joint is designed to give a large amount of movement, therefore support from
Hip Replacement PROGRAM. Nightingale. Home Healthcare
 Hip Replacement PROGRAM TM Nightingale Home Healthcare Why Do I Need A Hip Replacement? Hip replacements are performed for one reason; something has happened to the hip joint that has made it 1) too painful
Hip Replacement PROGRAM TM Nightingale Home Healthcare Why Do I Need A Hip Replacement? Hip replacements are performed for one reason; something has happened to the hip joint that has made it 1) too painful
Northumbria Healthcare NHS Foundation Trust. Knee Arthroscopy. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Knee Arthroscopy: Postoperative Instructions
 Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Practical Reduction Techniques: Diaphyseal Reduction. Philip Wolinsky University of California at Davis Medical Center
 OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
OTA Specialty Day 2016 Practical Reduction Techniques: Diaphyseal Reduction Philip Wolinsky University of California at Davis Medical Center 8:55 am 9:55 am Tips and Tricks: Practical Reduction Techniques
E. Guţu, V. Iacub, D. Casian, G. Cristalov DRESSINGS AND BANDAGES. Methodical recommendation for III year students of medical faculty
 Ministry of Health and Social Protection of Republic of Moldova State University of Medicine and Pharmacy N.Testemiţanu Chair of General Surgery and Semiology E. Guţu, V. Iacub, D. Casian, G. Cristalov
Ministry of Health and Social Protection of Republic of Moldova State University of Medicine and Pharmacy N.Testemiţanu Chair of General Surgery and Semiology E. Guţu, V. Iacub, D. Casian, G. Cristalov
Shoulder Exercises Phase 1 Phase 2
 Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Skill Evaluation Sheets
 Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
Musculoskeletal Injuries
 Musculoskeletal Injuries KNOWLEDGE OBJECTIVES 1. Identify the four main structures of the musculoskeletal system. 2. List five common signs or symptoms of musculoskeletal injuries. 3. List seven signs
Musculoskeletal Injuries KNOWLEDGE OBJECTIVES 1. Identify the four main structures of the musculoskeletal system. 2. List five common signs or symptoms of musculoskeletal injuries. 3. List seven signs
Rehabilitation Program Following Isolated Biceps Tenodesis
 Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
Meniscus Problems - Torn Meniscus Repair
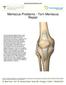 Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Amputations. Chapter 23
 Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual
 Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Zenith. Total Ankle Replacement Surgical technique
 Total Ankle Replacement Surgical technique Contents Operative summary 4 Pre-operative planning and templating 6 Patient positioning 6 Exposure 6 Saw blades 7 Joint line definition 7 Tibial alignment jig
Total Ankle Replacement Surgical technique Contents Operative summary 4 Pre-operative planning and templating 6 Patient positioning 6 Exposure 6 Saw blades 7 Joint line definition 7 Tibial alignment jig
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
High Tibial Osteotomy (HTO) Rehabilitation Protocols
 High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
Ex Fix Rehab Phase II Strengthening
 Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
MANUAL PRODUCT 3 RD EDITION. Pediatric Ankle Joint P: F: BeckerOrthopedic.com.
 PRODUCT MANUAL 3 RD EDITION P: 800-521-2192 248-588-7480 F: 800-923-2537 248-588-2960 BeckerOrthopedic.com Patent Pending 2018 Becker Orthopedic Appliance Co. All rights reserved. TRIPLE ACTION DIFFERENCE
PRODUCT MANUAL 3 RD EDITION P: 800-521-2192 248-588-7480 F: 800-923-2537 248-588-2960 BeckerOrthopedic.com Patent Pending 2018 Becker Orthopedic Appliance Co. All rights reserved. TRIPLE ACTION DIFFERENCE
Key Words. clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma. Linked Core Abilities
 Lesson 4 Treating for Shock and Immobilizing Fractures Key Words clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma What You Will Learn to Do Determine first
Lesson 4 Treating for Shock and Immobilizing Fractures Key Words clammy closed fracture dislocation fainting ligament open fracture splint sprain strain trauma What You Will Learn to Do Determine first
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
Patellofemoral Pain Syndrome
 What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
Body Bar FLEX. Exercises for the Core and Abdominals. by Gordon L. Brown, Jr. for Body Bar, Inc.
 Body Bar FLEX Exercises for the Core and Abdominals by Gordon L. Brown, Jr. for Body Bar, Inc. 1 Exercises for the Core and Abdominals This presentation features stretching and strengthening exercises
Body Bar FLEX Exercises for the Core and Abdominals by Gordon L. Brown, Jr. for Body Bar, Inc. 1 Exercises for the Core and Abdominals This presentation features stretching and strengthening exercises
