Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator.
|
|
|
- Alexander Moore
- 5 years ago
- Views:
Transcription
1 Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS GUIDELINE... 2 DEROGATION FROM NICE GUIDANCE OR ROYAL MARSDEN MANUAL... 2 KEY PRIORITIES FOR IMPLEMENTATION... 2 IDENTIFICATION... 2 TREATMENT AND MANAGEMENT... 2 COMMON C OMPLICATIONS... 5 INDICATIONS & C ONTRA-INDICATIONS... 6 MONITORING & CLINICAL AUDIT... 6 PATIENT INFORMATION... 6 REFERENCES... 6 CONTACT D ETAILS... 6 Page 1 of 7
2 Introduction This guidance is for use for patients undergoing complex limb reconstruction treatment involving the application of a circular frame external fixator more commonly referred to as an Ilizarov frame or Taylor Spatial Frame (TSF). It is normally indicated for patients who have the following injuries/conditions: Complex fractures - comminuted/open/peri-articular, often with associated loss of bone and soft tissue. Acute fracture stabilisation without deformity correction Fracture non-union Fracture mal-union Limb length discrepancy (congenital or acquired) Charcot foot Soft tissue contractures Osteomyelitis Paediatric growth deformities e.g. Blount s Disease Target Audience This guidance is to be used by in-patient and out-patient Physiotherapists treating patients who have a circular frame external fixator in situ. Key changes from previous guideline The general content remains the same, however the previous guideline has been updated to reflect changes in current practice concentrating on tibial and femoral circular frame external fixators. Derogation from NICE Guidance or Royal Marsden Manual No NICE guidance available. Key Priorities for Implementation To standardise post-operative management of patients undergoing limb reconstruction treatment with a circular frame external fixator. Identification Rehabilitation. Treatment and Management Limb Reconstruction is a lengthy and difficult process for patients to experience. It is ESSENTIAL that Physiotherapy supports and rehabilitates patients throughout their external fixator wearing period, and remains ongoing following external fixator removal. Improvements in muscle strength, Page 2 of 7
3 power, function and ability to complete timed functional tests such as sit-to-stand and climbing stairs have been reported up to 2 years post external fixator removal (Barker et al, 2010). The majority of patients have external fixators applied to the lower limb(s) to stabilise fractures or treat bony deformities. In deformity correction, the external fixator is attached to the bone, with circular ring(s) above and below the deformity/fracture. Correction then occurs either at the site of the acute fracture or at an osteotomy site made at the point of bony deformity. The external fixator is then adjusted daily by the patient over a period of time to restore alignment. The patient follows a specific external fixator adjustment prescription, with movement occurring at the bony gap (fracture/osteotomy site). If the external fixator is applied to stabilise a fracture (where bony alignment is acceptable), then there may not be an adjustment phase. The external fixator in this instance is there to stabilise the fracture to allow healing to occur. Bone lengthening can also be performed using the external fixator. An osteotomy is performed and the external fixator is slowly lengthened under tension to form new bone or tissue. This process is known as distraction histiogenesis. Stages of Limb Reconstruction Throughout the limb reconstruction process patients are monitored radiologically and clinically by their Consultant, Clinical Nurse Specialist and Limb Reconstruction Physiotherapist. The limb reconstruction process can be split into five stages: 1: Pre-operative: Where possible every patient will undergo physical, medical and psychological assessment and screening. 2: Post-operative latency period: The latency period refers to the length of time (usually seven to ten days) following application of the external fixator. During this time, the healing process starts (callus formation) and no adjustments are made to the external fixator. Patients should be introduced to range of movement exercises for all joints particularly the ones above and below the external fixator at this stage, and should focus on completing them as part of their daily routine. 3: The correction period Where indicated, the external fixator is adjusted (usually by the patient or carer) a small amount daily. Constant tension is applied to the area of newly forming, soft callus. The new bone that forms is called the regenerate and is only visible on x-ray once it has sufficiently calcified; this can be several weeks/months after the correction period has ended. The tension applied will also stimulate new tissue formation; this is known as distraction histiogenesis. It is during this correction phase, as bone and soft tissue becomes stretched that the patient becomes most vulnerable to losing range of movement and becoming stiff. It is imperative that patients are closely monitored during this period and may require additional physiotherapy input to help them maintain their range of movement and reduce the risk of contractures developing. Patients are provided with a full contact resting splint to maintain ankle plantigrade when sleeping/resting and should use this splint whilst their external fixator is in situ. Page 3 of 7
4 4: The consolidation period Once the correction is complete, the external fixator is locked and left in situ whilst the new regenerate bone consolidates. The length of time patients remain in the external fixator varies, depending on the type and extent of limb reconstruction being done. During the consolidation period, patients are often allowed to progress towards full weight bearing mobilisation. This will be guided by the Consultant following clinical review. Weight-bearing for lower extremity applications is essential for the proper maturation and ossification of either a fracture callus or a lengthening distraction gap (Green, 1990). A low impact, gym based exercise routine that avoids a patient twisting on the affected limb can be considered during this phase to increase the patient s movement, fitness and strength where appropriate. 5: External fixator removal and ongoing rehabilitation Prior to its removal, the external fixator is unlocked (dynamised).this involves loosening the external fixator struts to allow normal weight bearing through the regenerate bone. Once adequate consolidation has taken place the external fixator is removed. Patients are advised to use crutches at this time and a cast or a walking splint may be applied to protect the regenerate and allow it to consolidate further. Patients should avoid twisting on the operated limb in a weight bearing position at this stage so as not to torsion (and potentially bend or fracture through) the regenerate bone. After further review they will then have the cast or splint removed and should be allowed to increase weight bearing and activity as per their Consultant s advice. The Role of Physiotherapy during Limb Reconstruction Physiotherapy is vital throughout all the stages of limb reconstruction. The post-operative physiotherapy should start from Day 1 and continue until phase 5 rehabilitation is complete and the patient has reached their optimum physical and functional potential. Every limb reconstruction case is different so each patient requires an individualised treatment approach. The aims of physiotherapy for limb reconstruction patients are to improve movement, function and reduce pain. A prophylactic approach should also be considered to prevent musculoskeletal complications arising. Restrictions to Rehabilitation Each patient should be assessed and treated according to general principles of rehabilitation and incorporating any post-operative restrictions. Rehabilitation should be aimed at maximising function, considering the physiological principles of healing so as not to compromise the surgery or outcome. There are no absolute restrictions to rehabilitation for limb reconstruction patients. Weight bearing status varies and is patient specific. Page 4 of 7
5 Common Complications and Therapy Considerations An awareness of possible complications will enable the Physiotherapist to treat prophylactically and in a timely manner; liaising with the limb reconstruction team should a complication arise. Loss of muscle length and the development of contractures Loss of joint movement due to poor adaptation of the muscle is a major problem during limb lengthening (Barker et al, 2001). This particularly affects bi-articular muscles, those of greater size and strength, and those that have wires/pins through them (Paley, 1990). Commonly observed contracture patterns: Tibial External fixator Femoral External fixator Knee flexion, ankle plantarflexion, toe clawing Hip flexion, hip adduction, knee flexion Other complications include: Oedema Joint stiffness and decreased ROM Poor gait pattern (poor stance phase hip extension and adduction) Poor ankle/foot posture Poor weight transference Decreased proprioception Loss of muscle strength Neurovascular compromise Poor posture Loss of cardiovascular fitness General deconditioning Pain (Neurogenic / Myogenic / Osteogenic / Autonomic) Psychological problems Poor motivation/compliance Pin site/skin graft/wound infection Joint subluxation and dislocation Loss of wire tension/hardware failure Premature/delayed consolidation Fracture/deformity of regenerate bone Additional therapy considerations: Hydrotherapy Education of colleagues, friends and family Referral to other services (e.g. OT, orthotics) Midline orientation Provision of equipment / splints Smoking cessation support Page 5 of 7
6 Advice on community exercise schemes and classes (e.g. local gym, walking groups) For external fixators on the upper limb the above complications and therapy considerations also apply; please contact the Limb Reconstruction Physiotherapist for further guidance. Discharge from Out Patient Physiotherapy Once the external fixator is removed, emphasis should be placed on functional rehabilitation with well-defined goals. It is also important to continue to address any specific problems/complications related to muscle length and strength, joint range of movement, posture, swelling, gait, cardiovascular fitness and endurance to optimise outcome and maximise normal function. The patient will be guided by their Consultant as to when it is appropriate to return to work/specific activities. If you are unsure of the limb reconstruction process that your patient is undergoing and would like to discuss their Physiotherapy intervention, or have any concerns about progress please contact the Senior Physiotherapist in Limb Reconstruction who will be happy to discuss and advise as needed. Indications & Contra-indications These guidelines should be used by Physiotherapists for those patients undergoing limb reconstruction treatment with a circular frame external fixator. Monitoring & Clinical Audit These guidelines are included in the induction document for new team members. Use of this guidance is documented in post-operative clinical notes. Copy of this guidance is sent with all referrals for ongoing Physiotherapy (outpatients). Guidance document reviewed and amended as indicated very 2 years. Patient Information This guideline has been updated in association with the patient information leaflet; Patient information for patients undergoing limb reconstruction treatment, which was approved for use at the Physiotherapy Clinical Governance Panel meeting (27 th January 2015). References Barker K.L, Simpson H.R, Lamb S.E (2001) Loss of knee range of motion in leg lengthening. Journal of Orthopaedic Sports Physical Therapy. Vol:31(5) pp Barker K.L, Lamb S.E, Simpson H.R, (2010). Recovery of muscle strength and power after limblengthening surgery. Archives of Physical Medicine and Rehabilitation. Vol:91(3) pp Green S.A. (1990), Physiotherapy during Ilizarov fixation. Techniques in Orthopaedics, Vol:5(4) pp61-65 Page 6 of 7
7 Paley D. (1990) Problems, obstacles, and complications of limb lengthening by the Ilizarov technique. Clinical Orthopedics Vol. 250: pp81-104, Contact Details Suzanne Swaine Senior Physiotherapist in Limb Reconstruction and Orthopaedics Tel: extension Pager 737* KH Debbie Bond Clinical Nurse Specialist, Limb Reconstruction Tel: extension Pager 737* KH Mr Graeme Groom MA FRCS Consultant Orthopaedic Surgeon Mr Om Lahoti MS (Orth) FRCS (Orth) Consultant Orthopaedic Surgeon (adult patients) (paediatric patients) Miss Sarah Phillips TD BSc FRCS (Orth) Consultant Orthopaedic Surgeon Page 7 of 7
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Limb lengthening and reconstruction. Children s Hospital Information for Patients, Parents and Carers
 Limb lengthening and reconstruction Children s Hospital Information for Patients, Parents and Carers Advice for leg lengthening and reconstruction Introduction This booklet has been designed to provide
Limb lengthening and reconstruction Children s Hospital Information for Patients, Parents and Carers Advice for leg lengthening and reconstruction Introduction This booklet has been designed to provide
Total ankle replacement
 Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
Patient Guide. Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening
 Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes
 Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes Irving Building Occupational Therapy, Rehabilitation Services 0161 206 519 G1809190W. Design Services, Salford Royal NHS Foundation
Instructions for Ilizarov and Taylor Spatial Frame Foot Drop Splints and Shoes Irving Building Occupational Therapy, Rehabilitation Services 0161 206 519 G1809190W. Design Services, Salford Royal NHS Foundation
Stress Fracture Of The Supracondylar Region Of The Femur Induced By The Weight Of The Tibial Ring Fixator
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 4 Number 1 Stress Fracture Of The Supracondylar Region Of The Femur Induced By The Weight Of The Tibial Ring S Dhar, M Mir Citation S Dhar, M
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 4 Number 1 Stress Fracture Of The Supracondylar Region Of The Femur Induced By The Weight Of The Tibial Ring S Dhar, M Mir Citation S Dhar, M
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
Triple Pelvic Osteotomy(TPO)
 Produced: April 2015 Ref: 251/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Osteotomy(TPO) Welcome to the Royal Orthopaedic Hospital (ROH).
Produced: April 2015 Ref: 251/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Osteotomy(TPO) Welcome to the Royal Orthopaedic Hospital (ROH).
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Advice following Anterior Cruciate Ligament (ACL) reconstruction
 Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway
 Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Tibial deformity correction by Ilizarov method
 International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
Physiotherapy information for Achilles Tendinopathy
 Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Rehabilitation programme after hemiarthroplasty surgery
 Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
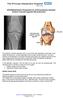 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Multiple Exostoses / Multiple Osteochondroma of the Lower Limb Guide By Dror Paley M.D.,
 Multiple Exostoses / Multiple Osteochondroma of the Lower Limb Guide By Dror Paley M.D., Director of the Paley Advanced Limb Lengthening Institute at St. Mary s Hospital in West Palm Beach, Florida. Located
Multiple Exostoses / Multiple Osteochondroma of the Lower Limb Guide By Dror Paley M.D., Director of the Paley Advanced Limb Lengthening Institute at St. Mary s Hospital in West Palm Beach, Florida. Located
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
TPO (Triple Pelvic Osteotomy) Information for young people
 Produced: Oct 2014 Ref: 201/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Information for young people Welcome to the Royal Orthopaedic
Produced: Oct 2014 Ref: 201/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Information for young people Welcome to the Royal Orthopaedic
Dislocation of the Patella Knee 1
 Dislocation of the Patella Knee 1 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Dislocation of the Patella Knee 1 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
A patient s guide to the. physiotherapy exercises and advice following excision of ilium with fibula strut
 A patient s guide to the physiotherapy exercises and advice following excision of ilium with fibula strut This booklet outlines the likely physiotherapy treatment you will receive while in hospital. Although
A patient s guide to the physiotherapy exercises and advice following excision of ilium with fibula strut This booklet outlines the likely physiotherapy treatment you will receive while in hospital. Although
Physiotherapy following peri acetabular osteotomy (PAO) surgery
 Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Post-operative information ACL reconstruction
 Post-operative information ACL reconstruction On discharge: Ensure you are steady on your crutches at the time of hospital discharge. Feel free to put your full weight on your operated knee, and bend the
Post-operative information ACL reconstruction On discharge: Ensure you are steady on your crutches at the time of hospital discharge. Feel free to put your full weight on your operated knee, and bend the
Protocol for the Management of Hip Arthroscopy Surgery
 Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
A Patient s Guide to Rotational Deformities in Children
 A Patient s Guide to Rotational Deformities in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Rotational Deformities in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
Rehabilitation programme after internal fixation surgery
 Rehabilitation programme after internal fixation surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after internal fixation surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Anterior Cruciate Ligament (ACL) Reconstruction: Rehabilitation
 Anterior Cruciate Ligament (ACL) Reconstruction: Rehabilitation Andy Phillipson MB ChB FRCS (Orth) Consultant Orthopaedic Surgeon Introduction The ACL is one of the most important ligaments in the knee.
Anterior Cruciate Ligament (ACL) Reconstruction: Rehabilitation Andy Phillipson MB ChB FRCS (Orth) Consultant Orthopaedic Surgeon Introduction The ACL is one of the most important ligaments in the knee.
Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions?
 Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions? James J Hutson Jr MD Professor Orthopedic Trauma Ryder
Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions? James J Hutson Jr MD Professor Orthopedic Trauma Ryder
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Miami combined ILLRS LLRS and ASAMI-BR Conference Presentations by Dr. M M Bari
 Orthopedics and Rheumatology Open Access Journal Conference Proceedings Volume 1 Issue 5 - December 2015 Ortho & Rheum Open Access J Copyright All rights are reserved by Ashraf Elazab Miami combined ILLRS
Orthopedics and Rheumatology Open Access Journal Conference Proceedings Volume 1 Issue 5 - December 2015 Ortho & Rheum Open Access J Copyright All rights are reserved by Ashraf Elazab Miami combined ILLRS
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
YOUR TOTAL KNEE REPLACEMENT
 YOUR TOTAL KNEE REPLACEMENT Dr. M.S. Barrow Barrow Physiotherapy MBBch (Wits), FCS (SA) Orth. Waterfall City Hospital Orthopaedic Surgeon Tel: 011 304 7829 Suite 5, East Wing, Sunninghill Hospital www.barrowphysiotherapy.co.za
YOUR TOTAL KNEE REPLACEMENT Dr. M.S. Barrow Barrow Physiotherapy MBBch (Wits), FCS (SA) Orth. Waterfall City Hospital Orthopaedic Surgeon Tel: 011 304 7829 Suite 5, East Wing, Sunninghill Hospital www.barrowphysiotherapy.co.za
Post-operative information Total knee replacement
 Post-operative information Total knee replacement Day of operation You will arrive on the ward following your surgery. You may have had a spinal anaesthetic which will wear off after a couple of hours.
Post-operative information Total knee replacement Day of operation You will arrive on the ward following your surgery. You may have had a spinal anaesthetic which will wear off after a couple of hours.
INITIAL REHABILITATION PHASE 0-4 weeks. Posterolateral Corner Injury
 Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Knee arthroscopy surgery
 Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information. Forefoot surgery. Barts Health Physiotherapy Website:
 Patient information Forefoot surgery Barts Health Physiotherapy Website: www.bartshealth.nhs.uk/physiotherapy This booklet is for patients following surgery to the front of their foot. This may include
Patient information Forefoot surgery Barts Health Physiotherapy Website: www.bartshealth.nhs.uk/physiotherapy This booklet is for patients following surgery to the front of their foot. This may include
Patellar Instability. OrthoInfo Patella Instability Page 1 of 5
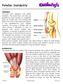 Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Phone: Phase 1. Inpatient. op day 5. Goals of. 1) Independent weight bearing. Partial. supports. 4) Instruct and. Treatment: 1) Ambulation
 North Jersey Orthopaedic Institute Rutgers, The Statee University of New Jersey 140 Bergen Street, D1610 Newark, NJ 07101 973-972-2150 South Orange Ambulatory Center Hackensack Medical Plaza Overlook Medical
North Jersey Orthopaedic Institute Rutgers, The Statee University of New Jersey 140 Bergen Street, D1610 Newark, NJ 07101 973-972-2150 South Orange Ambulatory Center Hackensack Medical Plaza Overlook Medical
ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS
 Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
Bahrain Medical Bulletin, Volume 17, Number 2, June 1995 Original ILIZAROV TECHNIQUE IN CORRECTING LIMBS DEFORMITIES: PRELIMINARY RESULTS Saleh W. Al-Harby, FRCS(Glasg)* This is a prospective study of
Deformity correction. A patient's guide. Information for patients Sheffield Teaching Hospitals
 Deformity correction A patient's guide Information for patients Sheffield Teaching Hospitals This leaflet applies to any deformity correction and it will set out the general principles and complications.
Deformity correction A patient's guide Information for patients Sheffield Teaching Hospitals This leaflet applies to any deformity correction and it will set out the general principles and complications.
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Mr Paul Y F Lee All in side - ACL Reconstruction Version 2.2. Sports Knee Surgery. Rehabilitation protocol. ACL Reconstruction.
 Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
Soft tissue Injury of the Knee (self-management) Knee 3
 Soft tissue Injury of the Knee (self-management) Knee 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows
Soft tissue Injury of the Knee (self-management) Knee 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows
Avulsion Fracture of the Foot Foot 1
 Avulsion Fracture of the Foot Foot 1 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Avulsion Fracture of the Foot Foot 1 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital
 Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital Hand Fractures (distal to carpus) Soft tissue injury with an underlying
Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital Hand Fractures (distal to carpus) Soft tissue injury with an underlying
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY
 MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
MEDIAL PATELLOFEMORAL LIGAMENT REPAIR & TIBIAL TUBERCLE OSTEOTOMY Revised SEP 2013 SPECIAL PRECAUTIONS/ LIMITATIONS: 1) CRUTCHES/ WEIGHT BEARING: Partial weight bearing at day 1 in brace locked at 0 extension
Modern Rx of Polio. with Ilizarov & new techniques
 Modern Rx of Polio with Ilizarov & new techniques Poliomyelitis Best Teacher of Orthopaedics Teaches Thorough clinical examination Muscle charting Gait Analysis Analysis of Joint Instability Precision
Modern Rx of Polio with Ilizarov & new techniques Poliomyelitis Best Teacher of Orthopaedics Teaches Thorough clinical examination Muscle charting Gait Analysis Analysis of Joint Instability Precision
Lapidus procedure and Akin osteotomy
 Lapidus procedure and Akin osteotomy Bunion surgery Information for patients Department of Podiatric Surgery What is a bunion? A bunion is a bony deformity of the joint at the base of the big toe (hallux).
Lapidus procedure and Akin osteotomy Bunion surgery Information for patients Department of Podiatric Surgery What is a bunion? A bunion is a bony deformity of the joint at the base of the big toe (hallux).
Patient Information & Exercise Folder
 MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
Ankle Fracture Weber B Ankle 3
 Ankle Fracture Weber B Ankle 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Ankle Fracture Weber B Ankle 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Rehabilitation programme after cannulated hip screw surgery
 Rehabilitation programme after cannulated hip screw surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation
Rehabilitation programme after cannulated hip screw surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Tibial Nailing for Tibial Shaft Fracture
 Tibial Nailing for Tibial Shaft Fracture Patient Information Trauma and Orthopaedics Department Author ID: KC Leaflet Number: Musc 015 Name of Leaflet: Tibial Nailing for Nail Shaft Fracture Version: 4
Tibial Nailing for Tibial Shaft Fracture Patient Information Trauma and Orthopaedics Department Author ID: KC Leaflet Number: Musc 015 Name of Leaflet: Tibial Nailing for Nail Shaft Fracture Version: 4
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron
 Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
Big toe (Hallux) corrective surgery Including Scarf, Weils, Akin/Chevron Orthopaedic Department Patient information leaflet This patient information booklet is designed to provide you with information
MATRIX-INDUCED AUTOLOGOUS CHONDROCYTE IMPLANTATION PHYSICAL THERAPY PRESCRIPTION
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
Achilles tendon rupture: management and rehabilitation
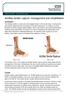 Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Total Knee Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Patient Information Physiotherapy after Total Knee Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Distal Radius Fracture (for review) Wrist 3
 Distal Radius Fracture (for review) Wrist 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent
Distal Radius Fracture (for review) Wrist 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Knee arthroscopy surgery
 Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Ankle, sub-talar or mid-foot joint fusion
 Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Orthopaedic Surgery. Elective Total Hip Replacement
 Orthopaedic Surgery Elective Total Hip Replacement The Department of Orthopaedics offers specialist medical and surgical treatments on musculoskeletal disorders, joint replacements, foot and ankle disorders,
Orthopaedic Surgery Elective Total Hip Replacement The Department of Orthopaedics offers specialist medical and surgical treatments on musculoskeletal disorders, joint replacements, foot and ankle disorders,
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan
 Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Physiotherapy after your hip arthroscopy
 Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Stabilisation of the shoulder joint
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline
 Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY
 1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment.
 24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Pilon Fractures - OrthoInfo - AAOS. Copyright 2010 American Academy of Orthopaedic Surgeons. Pilon Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Let s be Precice! the RCH Experience with the Precice Lengthening Nail. Cheryl Dingey RN / Nurse coordinator Limb Reconstruction
 Let s be Precice! the RCH Experience with the Precice Lengthening Nail Cheryl Dingey RN / Nurse coordinator Limb Reconstruction Causes of Leg length discrepancy in children Congenital born with a problem
Let s be Precice! the RCH Experience with the Precice Lengthening Nail Cheryl Dingey RN / Nurse coordinator Limb Reconstruction Causes of Leg length discrepancy in children Congenital born with a problem
SOFT TISSUE KNEE INJURIES
 SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
SOFT TISSUE KNEE INJURIES Soft tissue injuries of the knee commonly occur in all sports or in any activity that requires sudden changes in activity or movement. The knee is a complex joint and any injury
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GENERAL GUIDELINES GUIDELINES FOR REHABILITATION FOLLOWING DISTAL
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GENERAL GUIDELINES GUIDELINES FOR REHABILITATION FOLLOWING DISTAL
A Patient s Guide to Post-Operative Advice Following Pes Cavus
 A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
Intramedullary Nailing for Femur Fracture Management
 514-412-4400, ext. 23310 thechildren.com/trauma Intramedullary Nailing for Femur Fracture Management A Guide for Parents The femur is the longest bone in the body. It begins at the hip joint and ends at
514-412-4400, ext. 23310 thechildren.com/trauma Intramedullary Nailing for Femur Fracture Management A Guide for Parents The femur is the longest bone in the body. It begins at the hip joint and ends at
A Patient s Guide to Bipartite Patella
 A Patient s Guide to Bipartite Patella 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Bipartite Patella 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet is compiled from a variety
Paediatric Physiotherapy Donna-Marie Jones Paediatric Physiotherapy Chelmsley Wood Primary Care Centre Crabtree Drive Chelmsley Wood Solihull B37 5BU
 Solihull Community Children s Services Name of service Service manager Contact details Paediatric Physiotherapy Donna-Marie Jones Paediatric Physiotherapy Chelmsley Wood Primary Care Centre Crabtree Drive
Solihull Community Children s Services Name of service Service manager Contact details Paediatric Physiotherapy Donna-Marie Jones Paediatric Physiotherapy Chelmsley Wood Primary Care Centre Crabtree Drive
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Surgical repair of achilles tendon
 Surgical repair of achilles tendon Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure A tendon is a band of tissue that
Surgical repair of achilles tendon Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure A tendon is a band of tissue that
BCCH Emergency Department LOWER LIMB INJURIES Resource pack
 1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
1 BCCH Emergency Department LOWER LIMB INJURIES Resource pack Developed by: Rena Heathcote RN. 2 Knee Injuries The knee joint consists of a variety of structures including: 3 bones (excluding the patella)
