Michael Y. Wang, MD, 1 and Gerd Bordon, MD 2
|
|
|
- Kristina Collins
- 5 years ago
- Views:
Transcription
1 clinical article J Neurosurg Spine 24: , 2016 Mini-open pedicle subtraction osteotomy as a treatment for severe adult spinal deformities: case series with initial clinical and radiographic outcomes Michael Y. Wang, MD, 1 and Gerd Bordon, MD 2 1 Department of Neurological Surgery, University of Miami Miller School of Medicine, Miami, Florida; and 2 Department of Orthopedic Surgery, Hospital Manises, Valencia, Spain Objective Pedicle subtraction osteotomy (PSO) is a powerful but high-risk surgical technique for destabilizing the spine for deformity correction in both the sagittal and coronal planes. Numerous reports have demonstrated the benefits of this technique for realigning the spine in a physiological posture; however, the open surgical technique is associated with a high complication rate. In this report the authors review data obtained in a series of patients who underwent PSO through a less invasive approach. Methods Sixteen patients with severe coronal- and/or sagittal-plane deformities were treated in this series. Conservative measures had failed in all cases and patients had undergone a single-level PSO or extended PSO at L-2 or L-3. Fixation was accomplished using percutaneous instrumentation and interbody or facet joint fusions were used at the remaining levels. None of the procedures were aborted or converted to a traditional open procedure. Standard clinical and radiographic measures were used to assess patient outcomes. Results Mean age was 68.8 years and mean follow-up duration was 17.7 months. An average of 7.6 levels were fused, and 50% of the patients had bilateral iliac screw fixation, with all constructs crossing both the thoracolumbar and lumbosacral junctions. Operative time averaged 356 ± 50 minutes and there was a mean blood loss of 843 ± 339 ml. The leg visual analog scale score improved from a mean of 5.7 ± 2.7 to one of 1.3 ± 1.6, and the back visual analog scale score improved from a mean of 8.6 ± 1.3 to one of 2.4 ± 2.1. The Oswestry Disability Index score improved from a mean of 50.1 ± 14.4 to 16.4 ± 12.7, representing a mean reduction of 36.0 ± 16.9 points. The SF-36 physical component summary score changed from a mean of 43.4 ± 2.6 to one of 47.0 ± 4.3, and the SF-36 mental component summary score changed from a mean of 46.7 ± 3.6 to ± 3.0. Coronal alignment improved from a mean of 27.9 ± 43.6 mm to 16.0 ± 17.2 mm. The lumbar Cobb angle improved from a mean of 41.2 ± 18.4 to 15.4 ± 9.6, and lumbar lordosis improved from 23.1 ± 15.9 to 48.6 ± Pelvic tilt improved from a mean of 33.7 ± 8.6 to 24.4 ± 6.5, and the sagittal vertical axis improved from ± 73.4 mm to 42.2 ± 39.9 mm. The final lumbar lordosis pelvic incidence difference averaged 8.4 ± There were 4 patients who failed to achieve less than or equal to a 10 mismatch on this parameter. Ten of the 16 patients underwent delayed postoperative CT, and 8 of these had developed a solid arthrodesis at all levels treated. A total of 6 complications occurred in this series. There were no cases of symptomatic proximal junction kyphosis. Conclusions Advancements in minimally invasive technique have resulted in the ability to manage increasingly complex deformities with hybrid approaches. In this limited series, the authors describe the results of utilizing a tissuesparing mini-open PSO to correct severe spinal deformities. This method was technically feasible in all cases with acceptable radiographic outcomes similar to open surgery. However, high complication rates associated with these deformity corrections remain problematic. Key Words minimally invasive; spinal deformity; interbody fusion; BMP; osteotomy; scoliosis; kyphosis; pedicle screw; percutaneous Abbreviations ASD = adult spinal deformity; MCS = mental component summary; MIS = minimally invasive surgical; ODI = Oswestry Disability Index; PCS = physical component summary; PSO = pedicle subtraction osteotomy; QOL = quality of life; SVA = sagittal vertical axis; TLIF = transforaminal lumbar interbody fusion; VAS = visual analog scale. submitted February 10, accepted July 29, include when citing Published online January 8, 2016; DOI: / SPINE AANS,
2 M. Y. Wang and G. Bordon Loss of spinal balance due to a deformity has been associated with significant negative effects on patient-reported quality of life (QOL) measures. The appropriate surgical treatment of these disorders can lead to significant and reliable improvements in a patient s pain, function, and satisfaction. As such, the treatment of adult spinal deformity (ASD) remains a major focus of spinal surgeons, and many contemporary surgical techniques have been developed to treat symptomatic kyphosis and scoliosis. The majority of these rely on some form of anterior column height restoration or osteotomy to improve spinal alignment, particularly if the deformity is severe. 5,11,14,19,20,25,27 However, these techniques often require multilevel, staged operations and involve trauma to the soft-tissue envelope and significant blood loss. In this aged ASD population of individuals, in whom multiple medical comorbidities are frequent, such surgeries pose challenges associated with high rates of intraoperative and postoperative complications. 23 Over the past decade, various minimally invasive surgical (MIS) techniques have been developed to improve the clinical outcomes of spinal deformity surgery. 22 The potential for MIS techniques to reduce the morbidity of these operations has been a major impetus in the search for improved surgical solutions. Indeed, correction of coronal deformities measuring less than 30 with minimal sagittal imbalance has become increasingly popular. 2,8,12,29 However, the limitations of these MIS methods have been highlighted in several recent publications from the International Spine Study Group (ISSG), which compared various MIS deformity operations performed at US centers with special expertise in this area. In those studies, a ceiling effect of 34 for coronal curve correction was observed unless the dorsal spine was exposed to allow for multilevel osteotomies. 10 Furthermore, significant limitations for enhancing lumbar lordosis and improving sagittal balance have been a major impediment to the utility of MIS ASD correction. These findings were corroborated in a report by Acosta et al. 1 Recognizing that a more powerful MIS method for correcting severe scoliosis and improving sagittal alignment was necessary, we sought to develop a mini-open approach to perform three-column osteotomy. This would allow for correction of more significant deformities but potentially reduce the magnitude of soft-tissue trauma seen with traditional open procedures. This technique was initially explored in a cadaveric model by Voyadzis et al. 26 and then extended to clinical application. This report expands upon the initial description of the mini-open pedicle subtraction osteotomy (PSO) in the clinical setting. 28 Methods Patient Population A consecutive series of 16 patients included in this series underwent surgical treatment over a 33 month period. All patients underwent surgery where the soft-tissue envelope was opened through a subperiosteal dissection primarily at the PSO site. The remainder of the surgery was performed through a minimally invasive approach using MIS transforaminal lumbar interbody fusion (TLIF) and percutaneous screws. Patients underwent surgery in one of two academic institutions with institutional review board approval. Clinical Outcome Measures Surgical data were obtained and analyzed retrospectively with regard to the parameters of operative time, surgical blood loss, units of allogeneic blood transfused, hospital length of stay, and discharge status. Patient-reported outcome measures included visual analog scale (VAS) (leg), VAS (back), SF-36 physical component summary (PCS), SF-36 mental component summary (MCS), and Oswestry Disability Index (ODI) scores obtained preoperatively and postoperatively at last follow-up. All clinical outcome measures were performed by the patients themselves either at home or in the clinic waiting rooms. Complications were identified through a chart review process. Radiographic Outcome Measures All patients underwent preoperative CT scanning and 36-inch standing radiography to assess spinal alignment. Cobb angles were measured to establish the degree of scoliosis. This was determined by measuring the maximal coronal angulation between the two most angulated upper vertebral endplates on 36-inch standing radiographs. Global lumbar lordosis was determined by measuring the sagittal angulation between lines drawn parallel to the upper endplates of L-1 and S-1. The sagittal vertical axis (SVA) was measured by dropping a plumb line from the anterior inferior aspect of the C7 vertebra. The minimum distance from this line to the posterior superior endplate of S-1 was the SVA measured in centimeters. Coronal balance was measured on anteroposterior 36-inch standing radiographs and was determined as the offset between a line drawn vertically between the pedicles of S-1 and T-1. Fusion was determined to have occurred if bridging bone had formed at all fused levels either posteriorly or in the interbody space and at the PSO site. Surgical Technique After the patient was placed in the prone position, a dorsal midline skin incision allowed access to all levels of interest. This avoided the need for multiple stab incisions, but the skin opening was only taken down to the subcutaneous fat layer so that all subsequent steps were performed through the fascia. A bilateral subperiosteal dissection was then taken laterally at the level of the intended PSO (L-2 or L-3) out laterally to the transverse processes of that level. Any interbody fusion below the level of the PSO was performed through the same incision using a unilateral subperiosteal exposure of the facet joint(s). The PSO was then performed by removing the entire posterior spinous process, lamina, and facets with a rongeur. The exiting nerve roots surrounding the pedicle to be removed were skeletonized and the right and left pedicles were removed entirely. In certain cases an extended PSO was achieved by incising the cranial intervertebral disc space. A bilateral decancellation osteotomy was then performed using a series of enlarging curettes to remove two cones of cancellous bone from the vertebral body. Cen- 770
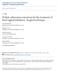
3 Mini-open pedicle subtraction osteotomy tral bone was removed with a curved curette. Cottonoids were then used to dissect and secure the lateral vertebral wall and its associated vasculature, and this was followed by removal of the posterior vertebral wall and posterior longitudinal ligament. Autologous bone removed during decompression and osteotomy was saved for later grafting purposes. Control of the spine was then achieved by placing percutaneous pedicle screws at least 3 levels above and below the PSO site. Once screw fixation was achieved, the lateral vertebral body walls were removed using a Leksell rongeur, completing the three-column osteotomy. Four rods were then bent to the appropriate degree of lordotic curvature, and 2 rods were then passed from above, 2 from below (Fig. 1). This allowed the tip of the 4 rods to meet in the open osteotomy site, protruding dorsally out of the wound. Set screws were then fashioned loosely to each screw-rod interface. In this fashion, control of the spine was achieved to allow closure of the osteotomy by manipulating the 4 rod holders (Fig. 2). A rod-to-rod connector was then used to connect the cranial and caudal rods on each side through the open site. All set screws were then final tightened. The nerve roots and thecal sac were then inspected to ensure that there was no neural compression, and any bleeding was controlled with powdered collagen matrix. Fusion above the PSO site was achieved by drilling the facet joints percutaneously and attaching 0.25 mg of recombinant human bone morphogenetic protein 2 (InFuse, Medtronic Sofamor Danek) to the screw saddle so that the osteobiological material sat between the screws and the facet joints. Mean values are presented ± SD. Fig. 2. Intraoperative photograph showing PSO reduction with the fourrod technique. Results Patient Demographics, Surgical Procedure, and Acute Hospitalization Of the 16 patients treated, half were male, and the mean age of the population was 68.8 ± 9.3 years. Follow-up time averaged 17.7 ± 10.5 months (Table 1). The average number of intervertebral disc levels fused was 7.6 ± 1.1, and 50% had bilateral iliac screw fixation. All constructs extended across the thoracolumbar and lumbosacral junctions. Six of the cases had the PSO performed at L-2, and 10 were Fig. 1. Artist s depiction of a 4-rod cantilever technique to control the spine as well as close the osteotomy to improve the deformity, as shown in the coronal (A C) and sagittal (D and E) planes. Copyright Roberto Suazo. Published with permission. 771
4 M. Y. Wang and G. Bordon TABLE 1. Demographic and acute care variables* Variable Value No. of patients 16 Male/female ratio 8:8 Mean age (yrs) 68.8 ± 9.3 Mean follow-up (mos) 17.7 ± 10.5 No. of intervertebral levels 7.6 ± 1.1 Iliac fixation 50% Extension across thoracolumbar junction 100% Extension across lumbosacral junction 100% PSO level L-2 6 L-3 10 No. of interbody fusion levels 32 Operative time (mins) 356 ± 50 Intraoperative blood loss (ml) 843 ± 339 Length of hospitalization (days) 7.2 ± 2.7 Discharge disposition Home 69% Rehabilitation 32% * Mean values are presented ± SD. done at the L-3 level. A total of 32 interbody fusion levels were performed. The operative time from skin incision to final closure averaged 356 ± 50 minutes. Intraoperative blood loss averaged 843 ± 339 ml. Half the patients received an allogeneic blood transfusion during the acute period of their hospitalization, with a mean of 1.2 units of blood given per patient. There were no conversions to fully open operations and no aborted operative attempts. The length of hospitalization averaged 7.2 ± 2.7 days with 69% of patients being discharged to home after surgery. The remaining patients were sent for inpatient rehabilitation. Clinical Outcomes Preoperative patient-reported variables were compared with postoperative outcomes established at the last followup (Table 2). Leg VAS scores improved from a mean of 5.7 ± 2.7 to one of 1.3 ± 1.6, whereas back VAS scores improved from a mean of 8.6 ± 1.3 to one of 2.4 ± 2.1. The ODI score improved from a mean of 50.1 ± 14.4 to one of 16.4 ± 12.7, representing a mean reduction of 36.0 ± 16.9 points. The SF-36 PCS score changed from a mean of 43.4 ± 2.6 to a score of 47.0 ± 4.3, whereas the SF-36 MCS score changed from a mean of 46.7 ± 3.6 to a score of ± 3.0. As a result of neural decompression, spinal stabilization, and deformity correction, the associated functional limitations were improved as expected. Maximal ambulation distance increased from a mean of 116 ± 130 feet to one of 2109 ± 3043 feet, reflecting a mean 1992 ± 2965 improvement. There were no patients for whom ambulatory function worsened. Radiographic Outcomes Preoperative radiographic measures were compared TABLE 2. Clinical and radiographic outcome measures* Measure Preoperative Postoperative Leg VAS score 5.7 ± ± 1.6 Back VAS score 8.6 ± ± 2.1 ODI score 50.1 ± ± 12.7 SF-36 PCS score 43.4 ± ± 4.3 SF-36 MCS score 46.7 ± ± 3.0 Maximal ambulation distance (ft) 116 ± ± 3043 Coronal alignment (mm) 27.9 ± ± 17.2 Lumbar Cobb angle ( ) 41.2 ± ± 9.6 Lumbar lordosis ( ) 23.1 ± ± 11.7 Pelvic tilt ( ) 33.7 ± ± 6.5 SVA (mm) ± ± 39.9 * Values are presented as the mean ± SD. with postoperative measures at last follow-up. Coronal alignment improved from a mean of 27.9 ± 43.6 mm to one of 16.0 ± 17.2 mm, representing an improvement of 29.3 ± 29.2 mm (Figs. 3 and 4). The lumbar Cobb angle improved from a mean of 41.2 ± 18.4 to one of 15.4 ± 9.6, representing an improvement of 25.9 ± The maximal preoperative Cobb angle of 75 improved to 30. The lumbar lordosis improved from a mean of 23.1 ± 15.9 to one of 48.6 ± 11.7, representing an improvement of 25.4 ± 8.4. The maximal amount of total lordosis added was 44. Pelvic tilt improved from a mean of 33.7 ± 8.6 to one of 24.4 ± 6.5, representing an improvement of 9.3 ± 8.4. The SVA improved from a mean of ± 73.4 mm to a mean of 42.2 ± 39.9 mm, representing an improvement of 60 ± 44.6 mm. In 3 patients, a final SVA of less than 60 mm was not achieved. When the final lumbar lordosis was subtracted from the pelvic incidence, the mean result was 8.4 ± There were 4 patients who failed to achieve less than or equal to a 10 mismatch on this parameter. Fusion rates were assessed based on postoperative CT scans. Of the 16 patients, 10 had undergone postoperative CT scanning and a solid arthrodesis at all levels treated had developed in 8 of these patients; CT scans were not obtained in all patients because those with no clinical or radiographic evidence of pseudarthrosis and refusing 3D imaging due to radiation dose concerns were not rescanned. CT scans were obtained at 1 year after surgery. There were no cases of symptomatic proximal junction kyphosis. Complications Complications in this series are shown in Table 3. Intraoperative complications included one unintentional durotomy. Postoperative complications included one wound infection and one watershed stroke that developed due to preexisting but undiagnosed bilateral carotid artery stenosis (degree of stenosis 99%). Implant and hardware complications included one iliac screw-rod dislodgment and one interbody graft extrusion, both of which were corrected by a return to the operating room within the first 3 months after surgery. In one patient, rod fractures developed at the 772
5 Mini-open pedicle subtraction osteotomy Fig. 3. Illustrative case showing anteroposterior (A and B) and lateral (C and D) 36-inch standing radiographs before and after the mini-open PSO was performed for deformity correction. PSO site 12 months after surgery (Fig. 4). There were no deaths or cases of paralysis. Discussion The search for a less morbid method for surgically correcting kyphoscoliosis has remained elusive despite the development of numerous MIS procedures. To date, few MIS publications have reported or focused on the patient s sagittal balance, a metric that may be the most reliable predictor of surgical success as determined by QOL measures. 6,13,15,21 A recent meta-analysis by Costanzo et al. reviewed lateral interbody MIS fusion results as reported in 14 peer-reviewed papers. 7 The study encompassed a total of 1266 levels in 476 patients and found that obtaining additional lordosis of greater than 10 or improvements in SVA of more than 5 cm was difficult to achieve. The development of anterior column release techniques has led to improvement in these two factors; Manwaring et al. reported on their first 9 cases managed with this technique, indicating that lumbar lordosis improved by 16.5 and the SVA was on average reduced by 4.8 cm. 18 However, the rate of complications associated with this approach has not been fully evaluated and is likely to be high given the proximity of large retroperitoneal vessels that may not be adequately visualized or controlled. 4,16 Furthermore, this technique is technically challenging and may not be easily learned or applied. Currently, lateral approaches are used very effectively for coronal realignment, 3 but sagittal realignment has remained challenging. Thus, many series of MIS approaches involve open posterior exposures that include open multilevel osteotomies. 24 In the current report we describe our initial experience with a mini-open PSO technique. This method was originally described in 2012 as an attempt to minimize the high morbidity rate seen with open PSO surgeries. 28 While the procedure requires opening the PSO site, this opening is roughly what is needed for a two-level posterior instrumented fusion. Opening this area accomplishes 4 very important goals: 1) it allows for efficient decompression of neural elements at a level that is frequently stenotic; 2) it allows for the application of well-accepted and widely used standard PSO methods used in open surgery; 3) it allows for direct visualization of the thecal sac during osteotomy closure, which is a potential source of catastrophic complications with PSO surgery; and 4) it allows for connection of the 4 rods passed from above and below the surgery site. The 4-rod technique is borrowed from traditional open ASD surgery and is known as a rod-cantilever technique. This approach allows for creation of a lordotic construct passed subfascially through a kyphotic spinal column, which is a major challenge in MIS procedures. These 4 rods allow for control of the spine during osteotomy clo- 773
6 M. Y. Wang and G. Bordon Fig. 4. Illustrative case showing rod fracture following mini-open PSO due to a nonunion at the osteotomy level: before rod fracture (left) and after fracture (right). sure, which is challenging in the absence of a complete opening of the soft-tissue envelope. A final benefit of the rod-cantilever method is that it helps reduce hardware pullout during the deformity reduction by separating the spine into two biomechanically discrete units (cranial and caudal constructs). Thus, all 6 8 screws in the upper part of the construct work in unison rather than independently. Using these methods, we were able to achieve a mean improvement of the lumbar Cobb angle of 25.9 ± Lumbar lordosis was improved from by a mean of 25.4 ± 8.4, and the maximal amount of total lordosis added was 44. This was accompanied by a mean SVA reduction of 60 ± 44.6 mm. With these changes in spinal alignment, we saw the expected changes in patient QOL and function one expects with standard, open deformity surgery. In this study, the ODI was reduced an average of 36 points, well above the minimal clinically important difference threshold. All surgeries were conducted in a single setting on 1 day, which is important given the recent trend for MIS ASD surgery to be performed over multiple days with different anesthetic administrations and multiple approaches. While the advantages of limiting the scope of any single surgical event are obvious, comparisons to open surgery require that MIS procedures be comparable in terms of cost and scope. Complications As with any new technique, a critical scientific appraisal of its drawbacks is vital to allow for sustainable advancements. Since this technique involves a PSO, all of the attendant risks and complications of that component of the technique are to be expected in both MIS and open TABLE 3. Complications Complication versions of the surgery. This is evidenced by the significant average blood loss of 843 ml. While advancements in surgical hemostasis would offer the opportunity for reductions in blood loss, we would not expect the blood loss from the osteotomy to be any less than that seen in an open surgery. Similarly, one would expect to see hardware failures in this series. Due to the destabilizing effects of a threecolumn osteotomy, a nonunion at the PSO site, combined with the acute rod bends necessary, lends a high rate of rod fracture to the construct. 17 In a recent series by Lenke s group, the rate of pseudarthrosis with rod fracture could be expected to be as high as 10%. 9 The reports on open ASD surgery underscore the need for long-term outcome studies in the range of 5 to 10 years so that the full effects and long-term outcome of these complex procedures can be fully and adequately assessed. 30 Limitations of This Study This study has numerous limitations. The short-term follow-up does not adequately capture the true rates of pseudarthrosis and hardware failure that can only be detected with long-term monitoring of these patients. Follow-up CT scanning is not performed in all patients and currently serves as the gold standard for identifying nonunions in the absence of clinical symptoms. The application of the mini-pso also relies heavily on off-label use of cages and osteobiologics to promote a successful fusion. With regard to meeting the spinal deformity correction, this series demonstrates a significant improvement over previous techniques. However, in 3 of our patients a final SVA of less than 60 mm was not achieved, and in 4 patients mismatch remained between lumbar lordosis and pelvic incidence by more than 10. The mean final pelvic tilt was 24.4, and 8 patients fell short of a final pelvic No. Conversion to open surgery 0 Wound infection 1 Unintentional durotomy 1 Nerve root injury 0 Pneumonia 0 Deep vein thrombosis 0 Pulmonary embolism 0 Urinary tract infection 0 Rod-screw dislodgment 1 Rod fracture 1 Interbody cage displacement 1 Proximal junctional kyphosis 0 Renal failure 0 Myocardial infarction 0 Paralysis 0 Stroke 1 Blindness 0 Death 0 774
7 Mini-open pedicle subtraction osteotomy tilt of less than 25. The inability to add posterior column osteotomies due to the limited opening of the soft-tissue envelope is likely responsible for these effects, as currently there is no method for performing posterior column osteotomies in an efficient MIS manner. While the clinical outcome measures in these patients demonstrated significant improvements, this was in part due to the severity of their preoperative disability. It is likely that closer approximation to the ideal sacral-pelvic parameters would have resulted in even better clinical outcomes. Conclusions Ultimately, the feasibility of this mini-open PSO technique will need to be validated with large clinical series at multiple institutions and with longer follow-up periods, preferably over 5 years. Given the propensity for delayed hardware pullout, rod breakage, pseudarthrosis, and proximal junctional kyphosis, this technique must be fully validated before widespread acceptance can be expected. However, by respecting traditional deformity principles, we were able to achieve excellent deformity correction in two planes without the extensive soft-tissue envelope disruption seen in the open procedures. References 1. Acosta FL, Liu J, Slimack N, Moller D, Fessler R, Koski T: Changes in coronal and sagittal plane alignment following minimally invasive direct lateral interbody fusion for the treatment of degenerative lumbar disease in adults: a radiographic study. J Neurosurg Spine 15:92 96, Anand N, Rosemann R, Khalsa B, Baron EM: Mid-term to long-term clinical and functional outcomes of minimally invasive correction and fusion for adults with scoliosis. Neurosurg Focus 28(3):E6, Arnold PM, Anderson KK, McGuire RA Jr: The lateral transpsoas approach to the lumbar and thoracic spine: A review. Surg Neurol Int 3 (Suppl 3):S198 S215, Assina R, Majmundar NJ, Herschman Y, Heary RF: First report of major vascular injury due to lateral transpsoas approach leading to fatality. J Neurosurg Spine 21: , Bridwell KH, Lewis SJ, Lenke LG, Baldus C, Blanke K: Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance. J Bone Joint Surg Am 85-A: , Clark AJ, Garcia RM, Keefe MK, Koski TR, Rosner MK, Smith JS, et al: Results of the AANS membership survey of adult spinal deformity knowledge: impact of training, practice experience, and assessment of potential areas for improved education: Clinical article. J Neurosurg Spine 21: , Costanzo G, Zoccali C, Maykowski P, Walter CM, Skoch J, Baaj AA: The role of minimally invasive lateral lumbar interbody fusion in sagittal balance correction and spinal deformity. Eur Spine J 23 (Suppl 6): , Dakwar E, Cardona RF, Smith DA, Uribe JS: Early outcomes and safety of the minimally invasive, lateral retroperitoneal transpsoas approach for adult degenerative scoliosis. Neurosurg Focus 28(3):E8, Dickson DD, Lenke LG, Bridwell KH, Koester LA: Risk factors for and assessment of symptomatic pseudarthrosis after lumbar pedicle subtraction osteotomy in adult spinal deformity. Spine (Phila Pa 1976) 39: , Haque RM, Mundis GM Jr, Ahmed Y, El Ahmadieh TY, Wang MY, Mummaneni PV, et al: Comparison of radiographic results after minimally invasive, hybrid, and open surgery for adult spinal deformity: a multicenter study of 184 patients. Neurosurg Focus 36(5):E13, Heary RF, Bono CM: Pedicle subtraction osteotomy in the treatment of chronic, posttraumatic kyphotic deformity. J Neurosurg Spine 5:1 8, Hsieh PC, Koski TR, Sciubba DM, Moller DJ, O Shaughnessy BA, Li KW, et al: Maximizing the potential of minimally invasive spine surgery in complex spinal disorders. Neurosurg Focus 25(2):E19, Johnson RD, Valore A, Villaminar A, Comisso M, Balsano M: Pelvic parameters of sagittal balance in extreme lateral interbody fusion for degenerative lumbar disc disease. J Clin Neurosci 20: , Kim YJ, Bridwell KH, Lenke LG, Cheh G, Baldus C: Results of lumbar pedicle subtraction osteotomies for fixed sagittal imbalance: a minimum 5-year follow-up study. Spine (Phila Pa 1976) 32: , Le Huec JC, Faundez A, Dominguez D, Hoffmeyer P, Aunoble S: Evidence showing the relationship between sagittal balance and clinical outcomes in surgical treatment of degenerative spinal diseases: a literature review. Int Orthop 39:87 95, Lenke LG: Editorial. Sagittal balance. J Neurosurg Spine 20: , Luca A, Lovi A, Galbusera F, Brayda-Bruno M: Revision surgery after PSO failure with rod breakage: a comparison of different techniques. Eur Spine J 23 (Suppl 6): , Manwaring JC, Bach K, Ahmadian AA, Deukmedjian AR, Smith DA, Uribe JS: Management of sagittal balance in adult spinal deformity with minimally invasive anterolateral lumbar interbody fusion: a preliminary radiographic study. J Neurosurg Spine 20: , Mummaneni PV, Dhall SS, Ondra SL, Mummaneni VP, Berven S: Pedicle subtraction osteotomy. Neurosurgery 63 (3 Suppl): , Ondra SL, Marzouk S, Koski T, Silva F, Salehi S: Mathematical calculation of pedicle subtraction osteotomy size to allow precision correction of fixed sagittal deformity. Spine (Phila Pa 1976) 31:E973 E979, Scheer JK, Lafage V, Smith JS, Deviren V, Hostin R, Mc- Carthy IM, et al: Impact of age on the likelihood of reaching a minimum clinically important difference in 374 three-column spinal osteotomies: clinical article. J Neurosurg Spine 20: , Schwender JD, Holly LT, Rouben DP, Foley KT: Minimally invasive transforaminal lumbar interbody fusion (TLIF): technical feasibility and initial results. J Spinal Disord Tech 18 (Suppl):S1 S6, Smith JS, Shaffrey CI, Glassman SD, Berven SH, Schwab FJ, Hamill CL, et al: Risk-benefit assessment of surgery for adult scoliosis: an analysis based on patient age. Spine (Phila Pa 1976) 36: , Tormenti MJ, Maserati MB, Bonfield CM, Okonkwo DO, Kanter AS: Complications and radiographic correction in adult scoliosis following combined transpsoas extreme lateral interbody fusion and posterior pedicle screw instrumentation. Neurosurg Focus 28(3):E7, van Loon PJ, van Stralen G, van Loon CJ, van Susante JL: A pedicle subtraction osteotomy as an adjunctive tool in the surgical treatment of a rigid thoracolumbar hyperkyphosis; a preliminary report. Spine J 6: , Voyadzis J, Gala V, O Toole J, Eicholz K, Fessler R: Minimally invasive posterior osteotomies. Neurosurgery 63:A204 A210, Wang MY, Berven SH: Lumbar pedicle subtraction osteotomy. Neurosurgery 60:ONS140 ONS146, Wang MY, Madhavan K: Mini-open pedicle subtraction 775
8 M. Y. Wang and G. Bordon osteotomy: surgical technique. World Neurosurg 81:843. e e14, Wang MY, Mummaneni PV: Minimally invasive surgery for thoracolumbar spinal deformity: initial clinical experience with clinical and radiographic outcomes. Neurosurg Focus 28(3):E9, Yadla S, Maltenfort MG, Ratliff JK, Harrop JS: Adult scoliosis surgery outcomes: a systematic review. Neurosurg Focus 28(3):E3, 2010 Disclosures Dr. Wang serves as a consultant for and receives royalty payments from DePuy-Synthes Spine, Inc., is a consultant for Aesculap Spine, owns stock in Spinicity, and has received grants from the Department of Defense. Dr. Bordon is a consultant for DePuy and Medtronic. Author Contributions Conception and design: Wang. Acquisition of data: Wang. Drafting the article: Wang. Critically revising the article: both authors. Correspondence Michael Y. Wang, Department of Neurological Surgery, Lois Pope Life Center, 1095 NW 14th Terrace, Miami, FL mwang2@med.miami.edu. 776
Maintenance of sagittal and coronal balance has
 Neurosurg Focus 36 (5):E14, 2014 AANS, 2014 Limitations and ceiling effects with circumferential minimally invasive correction techniques for adult scoliosis: analysis of radiological outcomes over a 7-year
Neurosurg Focus 36 (5):E14, 2014 AANS, 2014 Limitations and ceiling effects with circumferential minimally invasive correction techniques for adult scoliosis: analysis of radiological outcomes over a 7-year
Minimally invasive surgical technologies for the
 J Neurosurg Spine 15:92 96, 2011 Changes in coronal and sagittal plane alignment following minimally invasive direct lateral interbody fusion for the treatment of degenerative lumbar disease in adults:
J Neurosurg Spine 15:92 96, 2011 Changes in coronal and sagittal plane alignment following minimally invasive direct lateral interbody fusion for the treatment of degenerative lumbar disease in adults:
Surgery for adult spinal deformity (ASD) remains
 Neurosurg Focus 36 (5):E12, 2014 AANS, 2014 Less invasive surgery for treating adult spinal deformities: ceiling effects for deformity correction with 3 different techniques Michael Y. Wang, M.D., 1 Praveen
Neurosurg Focus 36 (5):E12, 2014 AANS, 2014 Less invasive surgery for treating adult spinal deformities: ceiling effects for deformity correction with 3 different techniques Michael Y. Wang, M.D., 1 Praveen
Clinical and radiographic parameters associated with best versus worst clinical outcomes in minimally invasive spinal deformity surgery
 clinical article J Neurosurg Spine 25:21 25, 2016 Clinical and radiographic parameters associated with best versus worst clinical outcomes in minimally invasive spinal deformity surgery Khoi D. Than, MD,
clinical article J Neurosurg Spine 25:21 25, 2016 Clinical and radiographic parameters associated with best versus worst clinical outcomes in minimally invasive spinal deformity surgery Khoi D. Than, MD,
Perioperative Complications of Pedicle Subtraction Osteotomy
 630 Original Article GLOBAL SPINE JOURNAL THIEME Perioperative Complications of Pedicle Subtraction Osteotomy Michael D. Daubs 1 Darrel S. Brodke 2 Prokopis Annis 2 Brandon D. Lawrence 2 1 Division of
630 Original Article GLOBAL SPINE JOURNAL THIEME Perioperative Complications of Pedicle Subtraction Osteotomy Michael D. Daubs 1 Darrel S. Brodke 2 Prokopis Annis 2 Brandon D. Lawrence 2 1 Division of
Surgery for ASD remains a challenging proposition.
 See the corresponding editorial in this issue, pp 1 3. J Neurosurg Spine 18:4 12, 2013 AANS, 2013 Improvement of sagittal balance and lumbar lordosis following less invasive adult spinal deformity surgery
See the corresponding editorial in this issue, pp 1 3. J Neurosurg Spine 18:4 12, 2013 AANS, 2013 Improvement of sagittal balance and lumbar lordosis following less invasive adult spinal deformity surgery
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Prevention of PJF: Surgical Strategies to Reduce PJF. Robert Hart, MD Professor OHSU Orthopaedics Portland OR. Conflicts
 Prevention of PJF: Surgical Strategies to Reduce PJF Robert Hart, MD Professor OHSU Orthopaedics Portland OR Conflicts Consultant Depuy Spine, Medtronic Royalties Seaspine, Depuy Research/Fellowship Support
Prevention of PJF: Surgical Strategies to Reduce PJF Robert Hart, MD Professor OHSU Orthopaedics Portland OR Conflicts Consultant Depuy Spine, Medtronic Royalties Seaspine, Depuy Research/Fellowship Support
Flatback Syndrome. Pathologic Loss of Lumbar Lordosis
 Flatback Syndrome Pathologic Loss of Lumbar Lordosis Robert P. Norton, MD Florida Spine Specialists Orthopaedic Spine Surgery Clinical Associate Professor, FAU College of Medicine Boca Raton, FL Courtesy
Flatback Syndrome Pathologic Loss of Lumbar Lordosis Robert P. Norton, MD Florida Spine Specialists Orthopaedic Spine Surgery Clinical Associate Professor, FAU College of Medicine Boca Raton, FL Courtesy
Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium
 Original Study Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium Tatsuya Yasuda, Tomohiko Hasegawa, Yu Yamato, Sho Kobayashi, Daisuke Togawa, Shin
Original Study Proximal junctional kyphosis in adult spinal deformity with long spinal fusion from T9/T10 to the ilium Tatsuya Yasuda, Tomohiko Hasegawa, Yu Yamato, Sho Kobayashi, Daisuke Togawa, Shin
The Kickstand Rod technique for correction of coronal imbalance in patients with adult spinal deformity: theory and technical considerations
 Case Report The Kickstand Rod technique for correction of coronal imbalance in patients with adult spinal deformity: theory and technical considerations Melvin C. Makhni 1, Meghan Cerpa 2, James D. Lin
Case Report The Kickstand Rod technique for correction of coronal imbalance in patients with adult spinal deformity: theory and technical considerations Melvin C. Makhni 1, Meghan Cerpa 2, James D. Lin
Spinal deformities, such as increased thoracic
 An Original Study Clinical and Radiographic Evaluation of Sagittal Imbalance: A New Radiographic Assessment Hossein Elgafy, MD, MCh, FRCS Ed, FRCSC, Rick Bransford, MD, Hassan Semaan, MD, and Theodore
An Original Study Clinical and Radiographic Evaluation of Sagittal Imbalance: A New Radiographic Assessment Hossein Elgafy, MD, MCh, FRCS Ed, FRCSC, Rick Bransford, MD, Hassan Semaan, MD, and Theodore
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique
 Case Report Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique Shaishav Bhagat 1, Alexander Z. E. Durst
Case Report Simultaneous anterior vertebral column resection-distraction and posterior rod contouring for restoration of sagittal balance: report of a technique Shaishav Bhagat 1, Alexander Z. E. Durst
Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance: Surgical technique.
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 3-1-2004 Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance: Surgical technique. Keith
Washington University School of Medicine Digital Commons@Becker Open Access Publications 3-1-2004 Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance: Surgical technique. Keith
Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity
 Eur Spine J (2013) 22:2130 2135 DOI 10.1007/s00586-013-2942-y OPEN OPERATING THEATRE (OOT) Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity Ibrahim Obeid Fethi Laouissat
Eur Spine J (2013) 22:2130 2135 DOI 10.1007/s00586-013-2942-y OPEN OPERATING THEATRE (OOT) Asymmetric T5 Pedicle Subtraction Osteotomy (PSO) for complex posttraumatic deformity Ibrahim Obeid Fethi Laouissat
Implementation of Pre-operative Planning:
 Implementation of Pre-operative Planning: 1-Year Results Using Patient-Specific UNiD Rods in Adult Deformity C.J. Kleck, MD 06/16/2017 Pre-operative Planning In the fields of observation chance favors
Implementation of Pre-operative Planning: 1-Year Results Using Patient-Specific UNiD Rods in Adult Deformity C.J. Kleck, MD 06/16/2017 Pre-operative Planning In the fields of observation chance favors
between pelvic incidence and lumbar lordosis (PI-LL), and C2 7 SVA. The operative patients with baseline C-7
 spine clinical article J Neurosurg Spine 23:153 158, 2015 How the neck affects the back: changes in regional cervical sagittal alignment correlate to HRQOL improvement in adult thoracolumbar deformity
spine clinical article J Neurosurg Spine 23:153 158, 2015 How the neck affects the back: changes in regional cervical sagittal alignment correlate to HRQOL improvement in adult thoracolumbar deformity
Surgical treatment for adult spinal deformity: Conceptual approach and surgical strategy
 REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Surgical treatment for adult spinal deformity: Conceptual approach and surgical strategy Yukihiro Matsuyama Department of Orthopedic Surgery, Hamamatsu
REVIEW ARTICLE SPINE SURGERY AND RELATED RESEARCH Surgical treatment for adult spinal deformity: Conceptual approach and surgical strategy Yukihiro Matsuyama Department of Orthopedic Surgery, Hamamatsu
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Is Circumferential Minimally Invasive Surgery Effective in the Treatment of Moderate Adult Idiopathic Scoliosis?
 Clin Orthop Relat Res (2014) 472:1762 1768 DOI 10.1007/s11999-014-3565-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: MINIMALLY INVASIVE
Clin Orthop Relat Res (2014) 472:1762 1768 DOI 10.1007/s11999-014-3565-2 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons SYMPOSIUM: MINIMALLY INVASIVE
Association between bicortical screw fixation at upper instrumented vertebra and risk for upper instrumented vertebra fracture
 CLINICAL ARTICLE J Neurosurg Spine 26:638 644, 2017 Association between bicortical screw fixation at upper instrumented vertebra and risk for upper instrumented vertebra fracture Young-Seop Park, MD, 1
CLINICAL ARTICLE J Neurosurg Spine 26:638 644, 2017 Association between bicortical screw fixation at upper instrumented vertebra and risk for upper instrumented vertebra fracture Young-Seop Park, MD, 1
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases-
 Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Thoracic or lumbar spinal surgery in patients with Parkinson s disease -A two-center experience of 32 cases- Department of Orthopedic Surgery, Graduate School of Medicine, Kyoto university Hiroaki Kimura,
Adult Spinal Deformity: Principles of Surgical Correction
 Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
Adult Spinal Deformity: Principles of Surgical Correction S. Samuel Bederman, MD PhD FRCSC Department of Orthopaedic Surgery California Orthopaedic Association, Indian Wells, CA April 25, 2015 2 3 4 Adult
Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion
 Original Study Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion Tomohide Segawa 1, Hirohiko Inanami 1, Hisashi Koga 2 1 Department of Orthopaedic Surgery, Inanami Spine and
Original Study Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion Tomohide Segawa 1, Hirohiko Inanami 1, Hisashi Koga 2 1 Department of Orthopaedic Surgery, Inanami Spine and
Adult spinal deformity is a complex disease with
 Neurosurg Focus 36 (5):E9, 2014 AANS, 2014 Long fusion from sacrum to thoracic spine for adult spinal deformity with sagittal imbalance: upper versus lower thoracic spine as site of upper instrumented
Neurosurg Focus 36 (5):E9, 2014 AANS, 2014 Long fusion from sacrum to thoracic spine for adult spinal deformity with sagittal imbalance: upper versus lower thoracic spine as site of upper instrumented
Radiographic Outcome and Complications after Single-level Lumbar Extended Pedicle Subtraction Osteotomy for Fixed Sagittal Malalignment:
 Radiographic Outcome and Complications after Single-level Lumbar Extended Pedicle Subtraction Osteotomy for Fixed Sagittal Malalignment: Traditional A PSO Retrospective Analysis of 55 Adult Spinal Deformity
Radiographic Outcome and Complications after Single-level Lumbar Extended Pedicle Subtraction Osteotomy for Fixed Sagittal Malalignment: Traditional A PSO Retrospective Analysis of 55 Adult Spinal Deformity
Analysis of instrumentation failures after three column osteotomies of the spine
 Kavadi et al. Scoliosis and Spinal Disorders (2017) 12:19 DOI 10.1186/s13013-017-0127-x RESEARCH Open Access Analysis of instrumentation failures after three column osteotomies of the spine Niranjan Kavadi
Kavadi et al. Scoliosis and Spinal Disorders (2017) 12:19 DOI 10.1186/s13013-017-0127-x RESEARCH Open Access Analysis of instrumentation failures after three column osteotomies of the spine Niranjan Kavadi
Over the past several decades, surgical treatment
 See the corresponding editorial in this issue (E16). Complications in adult spinal deformity surgery: an analysis of minimally invasive, hybrid, and open surgical techniques Neurosurg Focus 36 (5):E15,
See the corresponding editorial in this issue (E16). Complications in adult spinal deformity surgery: an analysis of minimally invasive, hybrid, and open surgical techniques Neurosurg Focus 36 (5):E15,
Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis
 J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
J Child Orthop (2012) 6:137 143 DOI 10.1007/s11832-012-0400-8 ORIGINAL CLINICAL ARTICLE Screws versus hooks: implant cost and deformity correction in adolescent idiopathic scoliosis Bradley P. Jaquith
Spine: Base to Summit 2018 Beaver Creek, CO ǀ January 18-21, 2018 Program
 THURSDAY, JANUARY 18 6:30 Registration, Breakfast and Exhibits Heritage Hall Foyer/Brown Dempsey Room 4:00 Welcome C. Shaffrey, MD SESSION 1: The Best Technique Is Grouse Mountain Room Mod: R. Haid, MD
THURSDAY, JANUARY 18 6:30 Registration, Breakfast and Exhibits Heritage Hall Foyer/Brown Dempsey Room 4:00 Welcome C. Shaffrey, MD SESSION 1: The Best Technique Is Grouse Mountain Room Mod: R. Haid, MD
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Restoration of coronal imbalance in the
 INSTRUMENTATION AND TECHNIQUE Provisional Ipsilateral Expandable Rod for Disc Space Distraction in Minimally Invasive Transforaminal Lumbar Interbody Fusion: Operative Technique Luis M. Tumialán, MD* Justin
INSTRUMENTATION AND TECHNIQUE Provisional Ipsilateral Expandable Rod for Disc Space Distraction in Minimally Invasive Transforaminal Lumbar Interbody Fusion: Operative Technique Luis M. Tumialán, MD* Justin
Long lumbar instrumented fusions have been described
 SPINE Volume 37, Number 16, pp 1407 1414 2012, Lippincott Williams & Wilkins SURGERY Upper Instrumented Vertebral Fractures in Long Lumbar Fusions What Are the Associated Risk Factors? Stephen J. Lewis,
SPINE Volume 37, Number 16, pp 1407 1414 2012, Lippincott Williams & Wilkins SURGERY Upper Instrumented Vertebral Fractures in Long Lumbar Fusions What Are the Associated Risk Factors? Stephen J. Lewis,
Adult spinal deformity, including degenerative scoliosis,
 SPINE Volume 41, Number 10, pp 880 884 ß 2016 Wolters Kluwer Health, Inc. All rights reserved DEFORMITY Risk Assessment of Lumbar Segmental Artery Injury During Lateral Transpsoas Approach in the Patients
SPINE Volume 41, Number 10, pp 880 884 ß 2016 Wolters Kluwer Health, Inc. All rights reserved DEFORMITY Risk Assessment of Lumbar Segmental Artery Injury During Lateral Transpsoas Approach in the Patients
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
The normal standing posture with least energy expenditure
 CLINICAL ARTICLE J Neurosurg Spine 27:74 80, 2017 The impact of spinopelvic morphology on the short-term outcome of pedicle subtraction osteotomy in 104 patients Karin Eskilsson, MD, 1 Deep Sharma, MS,
CLINICAL ARTICLE J Neurosurg Spine 27:74 80, 2017 The impact of spinopelvic morphology on the short-term outcome of pedicle subtraction osteotomy in 104 patients Karin Eskilsson, MD, 1 Deep Sharma, MS,
Adolescent Idiopathic Scoliosis
 Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Adolescent Idiopathic Scoliosis Surgical Treatment Comparisons By: Dr. Alex Rabinovich and Dr. Devin Peterson Options 1. Pedicle Screws versus Hooks 2. Posterior versus Anterior Instrumentation 3. Open
Ning Liu, MD, 1,3 and Kirkham B. Wood, MD 1,2
 TECHNICAL NOTE J Neurosurg Spine 26:368 373, 2017 Multiple-hook fixation in revision spinal deformity surgery for patients with a previous multilevel fusion mass: technical note and preliminary outcomes
TECHNICAL NOTE J Neurosurg Spine 26:368 373, 2017 Multiple-hook fixation in revision spinal deformity surgery for patients with a previous multilevel fusion mass: technical note and preliminary outcomes
Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion
 Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
T.L.I.F. Surgical Technique. Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System.
 Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose
 Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
of thoracolumbar angular kyphosis.
 spine clinical article J Neurosurg Spine 23:42 48, 2015 Expanded eggshell procedure combined with closing-opening technique (a modified vertebral column resection) for the treatment of thoracic and thoracolumbar
spine clinical article J Neurosurg Spine 23:42 48, 2015 Expanded eggshell procedure combined with closing-opening technique (a modified vertebral column resection) for the treatment of thoracic and thoracolumbar
Pedicle Subtraction Osteotomy. Case JB. Antonio Castellvi 5/19/2017
 Pedicle Subtraction Osteotomy John M. Small MD Florida Orthopedic Institute University South Florida Department Orthopedic Surgery Castellvi Spine May 11, 2017 Case JB 66 y/o male 74 235 lbs Retired police
Pedicle Subtraction Osteotomy John M. Small MD Florida Orthopedic Institute University South Florida Department Orthopedic Surgery Castellvi Spine May 11, 2017 Case JB 66 y/o male 74 235 lbs Retired police
Original Investigation. Peng Luo 1*, Rong-Xue Shao 2*, Ai-Min Wu 1, Hua-Zi Xu 1, Yong-Long ChI 1, Yan LIn 1 ABSTRACT
 DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Clinical Study Acute Reciprocal Changes Distant from the Site of Spinal Osteotomies Affect Global Postoperative Alignment
 SAGE-Hindawi Access to Research Advances in Orthopedics Volume 2011, Article ID 415946, 7 pages doi:10.4061/2011/415946 Clinical Study Acute Reciprocal Changes Distant from the Site of Spinal Osteotomies
SAGE-Hindawi Access to Research Advances in Orthopedics Volume 2011, Article ID 415946, 7 pages doi:10.4061/2011/415946 Clinical Study Acute Reciprocal Changes Distant from the Site of Spinal Osteotomies
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Postoperative Change of Thoracic Kyphosis after Corrective Surgery for Adult Spinal Deformity
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Postoperative Change of Thoracic Kyphosis after Corrective Surgery for Adult Spinal Deformity Tatsuya Yasuda 1), Tomohiko Hasegawa 2), Yu Yamato 2),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Postoperative Change of Thoracic Kyphosis after Corrective Surgery for Adult Spinal Deformity Tatsuya Yasuda 1), Tomohiko Hasegawa 2), Yu Yamato 2),
Fixed Sagittal Plane Imbalance
 Global Spine Journal Review Article 287 Jason W. Savage 1 Alpesh A. Patel 1 1 Department of Orthopaedic Surgery, Northwestern University Feinberg School of Medicine, Chicago, Illinois, United States Global
Global Spine Journal Review Article 287 Jason W. Savage 1 Alpesh A. Patel 1 1 Department of Orthopaedic Surgery, Northwestern University Feinberg School of Medicine, Chicago, Illinois, United States Global
Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity: Technical Note Involving 13 Cases
 Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
Technical Note Clinics in Orthopedic Surgery 2013;5:225-229 http://dx.doi.org/10.4055/cios.2013.5.3.225 Lumbosacral Fixation Using the Diagonal S2 Screw for Long Fusion in Degenerative Lumbar Deformity:
5/27/2016. Sagittal Balance What is It and How Did We Get Here? Sagittal Balance. Steven J. Tresser, MD Tampa, FL. Concept:
 Sagittal Balance What is It and How Did We Get Here? Steven J. Tresser, MD Tampa, FL Number of Articles Published on Sagittal Balance/Alignment by Year 350 300 250 200 150 100 50 0 Sagittal Balance Concept:
Sagittal Balance What is It and How Did We Get Here? Steven J. Tresser, MD Tampa, FL Number of Articles Published on Sagittal Balance/Alignment by Year 350 300 250 200 150 100 50 0 Sagittal Balance Concept:
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late complications
 Int J Clin Exp Med 2015;8(4):5731-5738 www.ijcem.com /ISSN:1940-5901/IJCEM0006438 Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late
Int J Clin Exp Med 2015;8(4):5731-5738 www.ijcem.com /ISSN:1940-5901/IJCEM0006438 Original Article Selection of proximal fusion level for degenerative scoliosis and the entailing proximal-related late
Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with Thoracolumbar Fractures
 Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
Journal of Clinical and Nursing Research 2018, 2(1): 23-27 Journal of Clinical and Nursing Research Clinical Analysis of Minimally Invasive Single-segment Reduction and Internal Fixation in Patients with
ASJ. Radiologic and Clinical Courses of Degenerative Lumbar Scoliosis (10 25 ) after a Short-Segment Fusion. Asian Spine Journal.
 Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis
 Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN Disclosures
Comparison of Clinical Outcomes Following Minimally Invasive Lateral Interbody Fusion Stratified by Preoperative Diagnosis Kaveh Khajavi, MD, FACS Alessandria Y. Shen, MSPH Anthony Hutchison, MSN Disclosures
Results of Corrective Osteotomy and Treatment Strategy for Ankylosing Spondylitis with Kyphotic Deformity
 Original Article Clinics in Orthopedic Surgery 2015;7:330-336 http://dx.doi.org/10.4055/cios.2015.7.3.330 Results of Corrective Osteotomy and Treatment Strategy for Ankylosing Spondylitis with Kyphotic
Original Article Clinics in Orthopedic Surgery 2015;7:330-336 http://dx.doi.org/10.4055/cios.2015.7.3.330 Results of Corrective Osteotomy and Treatment Strategy for Ankylosing Spondylitis with Kyphotic
There is No Remarkable Difference Between Pedicle Screw and Hybrid Construct in the Correction of Lenke Type-1 Curves
 DOI: 10.5137/1019-5149.JTN.20522-17.1 Received: 11.04.2017 / Accepted: 12.07.2017 Published Online: 21.09.2017 Original Investigation There is No Remarkable Difference Between Pedicle Screw and Hybrid
DOI: 10.5137/1019-5149.JTN.20522-17.1 Received: 11.04.2017 / Accepted: 12.07.2017 Published Online: 21.09.2017 Original Investigation There is No Remarkable Difference Between Pedicle Screw and Hybrid
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Object As spinal fusions become more common and more complex, so do the sequelae of these procedures, some
 clinical article J Neurosurg Spine 24:639 643, 2016 Fracture of fusion mass after hardware removal in patients with high sagittal imbalance Cara L. Sedney, MD, MA, 1 Scott D. Daffner, MD, 2 Jared J. Stefanko,
clinical article J Neurosurg Spine 24:639 643, 2016 Fracture of fusion mass after hardware removal in patients with high sagittal imbalance Cara L. Sedney, MD, MA, 1 Scott D. Daffner, MD, 2 Jared J. Stefanko,
T.L.I.F. Transforaminal Lumbar Interbody Fusion
 T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
Disclosures. Outline. General Guideline 6/4/2011. Consultant Medtronic, Stryker, Depuy. Osteotomy Planning and the Impact of Reciprocal Changes
 Disclosures Consultant Medtronic, Stryker, Depuy Osteotomy Planning and the Impact of Reciprocal Changes Christopher Ames MD Associate Professor Director of Spine Tumor and Deformity Surgery UCSF Department
Disclosures Consultant Medtronic, Stryker, Depuy Osteotomy Planning and the Impact of Reciprocal Changes Christopher Ames MD Associate Professor Director of Spine Tumor and Deformity Surgery UCSF Department
ASJ. Surgical Treatment of Adult Degenerative Scoliosis. Asian Spine Journal. Introduction. Classification of Adult Scoliosis
 Asian Spine Journal Asian Spine Review Journal Article Asian Spine J Surgical 2014;8(3):371-381 treatment of http://dx.doi.org/10.4184/asj.2014.8.3.371 adult degenerative scoliosis 371 Surgical Treatment
Asian Spine Journal Asian Spine Review Journal Article Asian Spine J Surgical 2014;8(3):371-381 treatment of http://dx.doi.org/10.4184/asj.2014.8.3.371 adult degenerative scoliosis 371 Surgical Treatment
Clinical Study The Effect of the Retroperitoneal Transpsoas Minimally Invasive Lateral Interbody Fusion on Segmental and Regional Lumbar Lordosis
 The Scientific World Journal Volume 2012, Article ID 516706, 7 pages doi:10.1100/2012/516706 The cientificworldjournal Clinical Study The Effect of the Retroperitoneal Transpsoas Minimally Invasive Lateral
The Scientific World Journal Volume 2012, Article ID 516706, 7 pages doi:10.1100/2012/516706 The cientificworldjournal Clinical Study The Effect of the Retroperitoneal Transpsoas Minimally Invasive Lateral
Laterally positioned hemivertebrae and the resultant. Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases.
 spine case report J Neurosurg Spine 22:84 89, 2015 Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases Shaheryar F. Ansari, MD, 1 Richard B. Rodgers, MD, 2 and Daniel H. Fulkerson,
spine case report J Neurosurg Spine 22:84 89, 2015 Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases Shaheryar F. Ansari, MD, 1 Richard B. Rodgers, MD, 2 and Daniel H. Fulkerson,
Pedicle Subtraction Osteotomy
 Pedicle Subtraction Osteotomy Manish K. Singh, David M. Ibrahimi, Christopher I. Shaffrey, and Justin S. Smith 8 8.1 Introduction Pedicle subtraction osteotomy (PSO) is a surgical procedure that can be
Pedicle Subtraction Osteotomy Manish K. Singh, David M. Ibrahimi, Christopher I. Shaffrey, and Justin S. Smith 8 8.1 Introduction Pedicle subtraction osteotomy (PSO) is a surgical procedure that can be
Department of Neurosurgery, St. Elisabeth Hospital, Warsaw, Poland 3
 Signature: Pol J Radiol, 2017; 82: 287-292 DOI: 10.12659/PJR.899975 CASE REPORT Received: 2016.06.08 Accepted: 2016.09.05 Published: 2017.05.28 Authors Contribution: A Study Design B Data Collection C
Signature: Pol J Radiol, 2017; 82: 287-292 DOI: 10.12659/PJR.899975 CASE REPORT Received: 2016.06.08 Accepted: 2016.09.05 Published: 2017.05.28 Authors Contribution: A Study Design B Data Collection C
Percutaneous Posterior Fixation: A Unique Entity to minimize Further Damage to Patient with Traumatic Spine
 Kaushal R Patel et al RESEARCH ARTICLE 10.5005/jp-journals-10039-1129 Percutaneous Posterior Fixation: A Unique Entity to minimize Further Damage to Patient with Traumatic Spine 1 Kaushal R Patel, 2 Jayprakash
Kaushal R Patel et al RESEARCH ARTICLE 10.5005/jp-journals-10039-1129 Percutaneous Posterior Fixation: A Unique Entity to minimize Further Damage to Patient with Traumatic Spine 1 Kaushal R Patel, 2 Jayprakash
Idiopathic scoliosis Scoliosis Deformities I 06
 What is Idiopathic scoliosis? 80-90% of all scolioses are idiopathic, the rest are neuromuscular or congenital scolioses with manifest primary diseases responsible for the scoliotic pathogenesis. This
What is Idiopathic scoliosis? 80-90% of all scolioses are idiopathic, the rest are neuromuscular or congenital scolioses with manifest primary diseases responsible for the scoliotic pathogenesis. This
Due to advances in medical care, the life expectancy
 Neurosurg Focus 28 (3):E9, 2010 Minimally invasive surgery for thoracolumbar spinal deformity: initial clinical experience with clinical and radiographic outcomes Mi c h a e l Y. Wa n g, M.D., 1 a n d
Neurosurg Focus 28 (3):E9, 2010 Minimally invasive surgery for thoracolumbar spinal deformity: initial clinical experience with clinical and radiographic outcomes Mi c h a e l Y. Wa n g, M.D., 1 a n d
Vertebral column decancellation for the management of sharp angular spinal deformity
 Eur Spine J (2011) 20:1703 1710 DOI 10.1007/s00586-011-1771-0 ORIGINAL ARTICLE Vertebral column decancellation for the management of sharp angular spinal deformity Yan Wang Lawrence G. Lenke Received:
Eur Spine J (2011) 20:1703 1710 DOI 10.1007/s00586-011-1771-0 ORIGINAL ARTICLE Vertebral column decancellation for the management of sharp angular spinal deformity Yan Wang Lawrence G. Lenke Received:
Degenerative L4-5 SPONDYLOLISTHESIS with Stenosis: Laminectomy and Postero-Lateral Fusion. Rick C. Sasso MD
 Degenerative L4-5 SPONDYLOLISTHESIS with Stenosis: Laminectomy and Postero-Lateral Fusion Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure:
Degenerative L4-5 SPONDYLOLISTHESIS with Stenosis: Laminectomy and Postero-Lateral Fusion Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure:
RESEARCH HUMAN CLINICAL STUDIES
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Justin S. Smith, MD, PhD* Christopher I. Shaffrey, MD* Christopher P. Ames, MD Jason Demakakos, MS Kai-Ming G. Fu, MD, PhDjj Sassan
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Justin S. Smith, MD, PhD* Christopher I. Shaffrey, MD* Christopher P. Ames, MD Jason Demakakos, MS Kai-Ming G. Fu, MD, PhDjj Sassan
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Radiographic and clinical outcomes following MIS-TLIF in patients with adult lumbar degenerative scoliosis
 Zhao et al. Journal of Orthopaedic Surgery and Research (2018) 13:93 https://doi.org/10.1186/s13018-018-0764-7 RESEARCH ARTICLE Radiographic and clinical outcomes following MIS-TLIF in patients with adult
Zhao et al. Journal of Orthopaedic Surgery and Research (2018) 13:93 https://doi.org/10.1186/s13018-018-0764-7 RESEARCH ARTICLE Radiographic and clinical outcomes following MIS-TLIF in patients with adult
Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June Section: Surgery Last Reviewed Date: June 2013
 Medical Policy Manual Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June 2007 Section: Surgery Last Reviewed Date: June 2013 Policy No: 157 Effective Date: August 1, 2013 IMPORTANT REMINDER
Medical Policy Manual Topic: Percutaneous Axial Anterior Lumbar Fusion Date of Origin: June 2007 Section: Surgery Last Reviewed Date: June 2013 Policy No: 157 Effective Date: August 1, 2013 IMPORTANT REMINDER
KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients
 Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Xi an Hong Hui Hospital Xi an, Shaanxi, China KumaFix fixation for thoracolumbar burst fractures: a prospective study on selective consecutive patients Dingjun Hao, Baorong He, Liang Yan Hong Hui Hospital,
Extreme lateral lumbar interbody fusion (XLIF) in the management of degenerative scoliosis: a retrospective case series
 Original Study Extreme lateral lumbar interbody fusion (XLIF) in the management of degenerative scoliosis: a retrospective case series Konstantinos N. Paterakis 1,2, Alexandros G. Brotis 2, Athanasios
Original Study Extreme lateral lumbar interbody fusion (XLIF) in the management of degenerative scoliosis: a retrospective case series Konstantinos N. Paterakis 1,2, Alexandros G. Brotis 2, Athanasios
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Int J Clin Exp Med 2016;9(11): /ISSN: /IJCEM
 Int J Clin Exp Med 2016;9(11):21748-21755 www.ijcem.com /ISSN:1940-5901/IJCEM0034462 Original Article Revision surgery outcomes of proximal junctional failure in surgically treated patients with posterior
Int J Clin Exp Med 2016;9(11):21748-21755 www.ijcem.com /ISSN:1940-5901/IJCEM0034462 Original Article Revision surgery outcomes of proximal junctional failure in surgically treated patients with posterior
Sagittal balance analysis after pedicle subtraction osteotomy in ankylosing spondylitis
 DOI 10.1007/s00586-011-1929-9 ORIGINAL ARTICLE Sagittal balance analysis after pedicle subtraction osteotomy in ankylosing spondylitis Romain Debarge Guillaume Demey Pierre Roussouly Received: 11 July
DOI 10.1007/s00586-011-1929-9 ORIGINAL ARTICLE Sagittal balance analysis after pedicle subtraction osteotomy in ankylosing spondylitis Romain Debarge Guillaume Demey Pierre Roussouly Received: 11 July
Caudal Vertebral Body Fractures Following Lateral Interbody Fusion in Nonosteoporotic Patients
 The Ochsner Journal 14:123 130, 2014 Ó Academic Division of Ochsner Clinic Foundation Caudal Vertebral Body Fractures Following Lateral Interbody Fusion in Nonosteoporotic Patients Gabriel C. Tender, MD
The Ochsner Journal 14:123 130, 2014 Ó Academic Division of Ochsner Clinic Foundation Caudal Vertebral Body Fractures Following Lateral Interbody Fusion in Nonosteoporotic Patients Gabriel C. Tender, MD
Since its initial description in 2006, the lateral interbody. Motor nerve injuries following the minimally invasive lateral transpsoas approach
 J Neurosurg Spine 7:7 3, 0 Motor nerve injuries following the minimally invasive lateral transpsoas approach Clinical article Kevin S. Cahill, M.D., Ph.D., M.P.H., Joseph L. Martinez, M.D., Michael Y.
J Neurosurg Spine 7:7 3, 0 Motor nerve injuries following the minimally invasive lateral transpsoas approach Clinical article Kevin S. Cahill, M.D., Ph.D., M.P.H., Joseph L. Martinez, M.D., Michael Y.
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Original Policy Date
 MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
The Influence of Spinal Deformities on Acetabular Orientation in Total Hip Arthroplasty
 The Influence of Spinal Deformities on Acetabular Orientation in Total Hip Arthroplasty S. SAMUEL BEDERMAN MD PhD FRCSC Scoliosis & Spine Tumor Center S. SAMUEL BEDERMAN MD PhD FRCSC disclosures October
The Influence of Spinal Deformities on Acetabular Orientation in Total Hip Arthroplasty S. SAMUEL BEDERMAN MD PhD FRCSC Scoliosis & Spine Tumor Center S. SAMUEL BEDERMAN MD PhD FRCSC disclosures October
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Change of Sagittal Spinopelvic Parameters after Selective and Non-Selective Fusion in Lenke Type 1 Adolescent Idiopathic Scoliosis Patients
 DOI: 10.5137/1019-5149.JTN.22557-18.2 Received: 13.01.2018 / Accepted: 09.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Change of Sagittal Spinopelvic Parameters after
DOI: 10.5137/1019-5149.JTN.22557-18.2 Received: 13.01.2018 / Accepted: 09.04.2018 Published Online: 24.04.2018 Turk Neurosurg, 2018 Original Investigation Change of Sagittal Spinopelvic Parameters after
Effect of direct vertebral body derotation on the sagittal profile in adolescent idiopathic scoliosis
 Eur Spine J (2012) 21:31 39 DOI 10.1007/s00586-011-1991-3 ORIGINAL ARTICLE Effect of direct vertebral body derotation on the sagittal profile in adolescent idiopathic scoliosis Steven W. Hwang Amer F.
Eur Spine J (2012) 21:31 39 DOI 10.1007/s00586-011-1991-3 ORIGINAL ARTICLE Effect of direct vertebral body derotation on the sagittal profile in adolescent idiopathic scoliosis Steven W. Hwang Amer F.
SURGICAL TECHNIQUE MANUAL. InterFuse T
 1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
Preoperative full-length standing radiographs and revision rates in lumbar degenerative scoliosis
 CLINICAL ARTICLE J Neurosurg Spine 28:581 585, 2018 Preoperative full-length standing radiographs and revision rates in lumbar degenerative scoliosis Joshua T. Bunch, MD, 1 Steven D. Glassman, MD, 1 Howard
CLINICAL ARTICLE J Neurosurg Spine 28:581 585, 2018 Preoperative full-length standing radiographs and revision rates in lumbar degenerative scoliosis Joshua T. Bunch, MD, 1 Steven D. Glassman, MD, 1 Howard
Department of Neurosurgery, University of Virginia, Charlottesville, Virginia
 J Neurosurg Spine 9:000 000, 9:326 331, 2008 Neurological symptoms and deficits in adults with scoliosis who present to a surgical clinic: incidence and association with the choice of operative versus
J Neurosurg Spine 9:000 000, 9:326 331, 2008 Neurological symptoms and deficits in adults with scoliosis who present to a surgical clinic: incidence and association with the choice of operative versus
Congenital Spine Deformity: Surgical Treatment Options. Spine Masters. Fri May , 4:10-4:25 Paul Sponseller MD
 Congenital Spine Deformity: Surgical Treatment Options Spine Masters Fri May19 2017, 4:10-4:25 Paul Sponseller MD Disclosures Medical Education Reviews JBJS Depuy Synthes Spine: Research, royalties Globus:
Congenital Spine Deformity: Surgical Treatment Options Spine Masters Fri May19 2017, 4:10-4:25 Paul Sponseller MD Disclosures Medical Education Reviews JBJS Depuy Synthes Spine: Research, royalties Globus:
