Comparison of the 2-Incision and Mini-Incision Posterior Total Hip Arthroplasty Technique
|
|
|
- Harold Gordon Walton
- 6 years ago
- Views:
Transcription
1 The Journal of Arthroplasty Vol. 22 No Comparison of the 2-Incision and Mini-Incision Posterior Total Hip Arthroplasty Technique A Retrospective Match-Pair Controlled Study Paul J. Duwelius, MD, Robert L. Burkhart, PA, OPA-C, John O. Hayhurst, MD, Hans Moller, MD, and Jay B.V. Butler, MD Abstract: We compared the outcomes of the mini-posterior and 2-incision total hip arthroplasty approaches by analyzing 43 matched pairs of patients. The following outcomes were evaluated: (1) Harris Hip Score, (2) Medical Outcomes Study 36-Item Short-Form Health Survey, (3) the Medical Outcomes Study Sleep Scale, and (4) the Western Ontario and McMaster Osteoarthritis Index. Function was regained earlier by patients having the 2-incision total hip arthroplasty as determined by length of hospitalization ( P =.002) and multiple return to function parameters, although this may be the result of hip precautions placed on the posterior group. Posterior miniincision patients had less operating time ( P b.0001) and blood loss ( P =.001). Complications did not differ between surgical techniques. No patients were revised. The 2-incision operation was better for function and length of stay, and the posterior mini-incision was easier to perform, although these groups used different selection criteria. Key words: minimally invasive total hip arthroplasty, match-pair outcome study, total hip arthroplasty functional outcome. n 2007 Elsevier Inc. All rights reserved. We began the performance of small-incision operations for total hip arthroplasty in February 2002 because we were attracted to the potential benefits of reduced hospitalization, improved function, and reduced pain. Since that time, there have been several publications that have questioned the use From the St. Vincent Hospital and Medical Center, Orthopaedic and Fracture Clinic, Portland, Oregon. Submitted February 14, 2006; accepted September 26, Level of evidence: level II-1 (retrospective matchedpair study). Benefits or funds were received in partial or total support of the research material described in this article from Zimmer Clinical Research Support and Royalties. Reprint requests: Paul R. Duwelius, MD, St. Vincent Hospital and Medical Center, Orthopaedic and Fracture Clinic, SW Barnes Rd. #300, Portland, OR. n 2007 Elsevier Inc. All rights reserved /07/ $32.00/0 and even the safety of small-incision surgery [1-4]. Other mini single-incision series have reported safety and reproducibility in component positioning with short-term patient follow-up [5-10]. Two-incision operations were fraught with more complications but seemed to provide superior functional results [1,3,11-13]. The literature reflects high-volume surgeons having a lower complication rate [14], and adequate training and instrumentation are important for improved results [1,3-6,15]. Because we had experience with both single posterior mini-incision and 2-incision minimally invasive surgery total hip arthroplasties, we were interested in comparing the outcomes of the patients with these 2 different operations. Our study hypothesis was that the 2-incision technique would provide earlier postoperative gains in patient function, better pain relief, and no greater prevalence of complications. 48
2 Comparison of the 2-Incision and Mini-Incision Posterior THA Technique! Duwelius et al 49 Materials and Methods Procedures Patients aged 18 years or older at the time of total hip arthroplasty, and who were operated on between December 2002 and June 2004, had either a 2-incision or posterior mini-incision operation. Two hundred eighty-four operations were performed on patients between 18 and 75 years of age who were eligible for the matched-pair analysis. Patients had the diagnosis of osteoarthritis, rheumatoid arthritis, posttraumatic arthritis, or a displaced femoral neck fracture. More than 90% of the patients in this initial cohort had the diagnosis of osteoarthritis. All patients who were operated were candidates for total hip arthroplasty and had obtained medical clearance for the operation. The first minimally invasive surgery (MIS) 2-incision technique was performed at our center on April 10, The miniposterior and 2-incision techniques have been used for approximately 5 years at our center. Approximately 200 two-incision cases and 300 mini-posterior cases had been performed before this match-pair cohort. These cohorts of patients were not considered part of the initial blearning curve.q All patients in the match-pair cohort had the diagnosis of osteoarthritis. The only patients who had a more traditional total hip arthroplasty during this time had hardware inserted from prior hip surgery (3 cases) or had morbid obesity (4 cases). The pairs were matched by the criteria listed in Table 1. All operations were performed by a single surgeon. Our 43 match-pair series was selected from a pool of 284 patients. This group was the cohort selected because they had completed the weekly patient diaries, which was so important for evaluating early postoperative follow-up and rehabilitation. The mini-posterior and 2-incision techniques have been used for approximately 5 years at our center. Clearly, some patients came to the author for the 2-incision technique and therefore were somewhat self-selected because they wanted this procedure. However, patients who did not meet the author s criteria, which has been well defined, did not receive the 2-incision procedure. There were no selection criteria for the mini-posterior incision; thus, any patient who did not fit the criteria for the 2-incision procedure, whether those patients wanted the 2-incision or not, were included in the mini-posterior group. Patients who were in the 2-incision group had selected criteria of age less than 70 years and body mass index less than 40, do not have a Crowe dysplasia classification of class III or IV, and do not have an excessive anteriorposterior bow of the femur, which would not allow Variable Table 1. Baseline and Operative Information Two-Incision Matched Patients Mini-Incision Matched Patients Age Mean SD (Min, Max) (40, 68) (43, 74) Gender, n (%) Male 24 (54) 24 (54) Female 19 (44) 19 (44) Body mass index category, n (%) Normal (b25 kg/m^2) 21 (48%) 21 (48%) Overweight 15 (35%) 15 (35%) (25-30 kg/m 2 ) Obese (N30 kg/m 2 ) 7 (16%) 7 (16%) Preoperative diagnosis, n (%) Osteoarthritis 43 (100) 43 (100) Other 0 (0) 0 (0) Length of follow-up Mean SD (Min, Max) (0.5, 2.0) (0.5, 2.0) WOMAC pain Mean SD (Min, Max) (4, 15) (2, 14) WOMAC physical function Mean SD (Min, Max) (5, 45) (8, 50) WOMAC stiffness Mean SD (Min, Max) (1, 8) (2, 8)\ safe use of a straight fully coated femoral stem. In addition, the diameter of the intramedullary canal of the femur could not exceed 18 mm, and the size of the acetabular cup could not exceed 64 mm. There were no restrictive criteria for the posterior mini-incision patients. Preoperatively, there was only one difference in the preoperative education class that patients attended. In the class for the posterior mini-incision patients, the only difference was instruction in dislocation precautions, whereas the 2-incision patients were not restricted by dislocation precautions. No patient in either group had an abduction pillow. The posterior group was instructed in avoidance of extreme flexion and internal rotation. This is the only difference in hip precautions between the 2 groups. Patients were educated on the benefits of early mobility in preventing deep venous thrombosis and the benefits of early discharge in preventing nosocomial infection. Of the 43 patients with the posterior miniincision and of the 43 patients with the 2-incision
3 50 The Journal of Arthroplasty Vol. 22 No. 1 January 2007 operations, 40 and 25 patients, respectively, attended preoperative class. Most patients attended the preoperative class. The only patients who did not attend the preoperative class were nonlocal patients, and they were seen immediately after my preoperative visit, which was usually the day before the procedure. All patients in this category received the same education from our orthopedic nurse practitioner. All patients were instructed to maintain a postoperative diary of their recovery. In the hospital, all patients were treated with the same clinical hip pathway. Anesthesia was a shortacting spinal anesthetic using hyperbaric 0.75% Bupivacaine (Abbott) adjusted for the height and weight of the patient. The pain management included administration of valdecoxib, 40 mg (Pharmacia and Upjohn); oxycodone SR, 10 to 20 mg (Roxane); and ondansetron, 4 mg (GlaxoSmithKline). In the recovery room, 25 to 50 lg of fentanyl (Abbott) every 5 to 10 minutes was given as needed. Once the patients had returned to their room, only oral medication was used. Deep venous thrombosis prevention included the short-acting spinal anesthetic, rapid mobilization of the patient, calf high compression stockings, calf pneumatic compression, and 325 mg of aspirin each day in the hospital and for 3 months postoperatively. Patients were discharged home as soon as they were judged safe by physical therapy and internal medicine, and this could be as early as the day of the surgery. Following discharge, patients were encouraged to use aspirin and plain Tylenol for pain medications and to avoid oral narcotics. All patients were instructed to use a regular pillow between their legs while sleeping for 6 weeks for comfort. Neither group used an abduction pillow. They were told they were allowed to drive their car when they were off narcotic pain medication and had appropriate muscle control of their leg. All patients were allowed to achieve weight-bearing as tolerated. Both patient groups were treated equally with respect to weight-bearing as tolerated without regard to stem type. The type of femoral stem did not inhibit or prevent patients from being able to ambulate immediately. A tight press fit was achieved at the time of surgery with either stem to allow full immediate weight-bearing. Surgical Technique The surgical technique for the 2-incision operation has been described, [1,11-13] as has the technique for the posterior mini-incision [1,6,8, 16,17]. The implants used were a Trilogy acetabular component for all patients (Zimmer, Warsaw, Ind). We used 1 or 2 screws to augment the fixation of all acetabular components. All patients with the 2-incision total hip arthroplasty had a fully coated VerSys femoral stem (Zimmer). All surgeons reporting cases in the initial Journal for Bone and Joint Surgery (JBJS) American Orthopaedic Association (AOA) symposium used the full coat stem [11]. This implant is straight and acts more like a femoral nail, allowing easier insertion and better fit through the small posterior incision. The VerSys FullCoat stem was implanted in 11 (26%) of 43 patients with the posterior mini-incision technique, whereas 32 (74%) of 43 had a VerSys Fiber Metal MidCoat stem (Zimmer). The full coat stem was used in these cases in a Dorr C type femur or when proximal fill or bone quality was thought to be an issue. Clinical Assessment Demographics included sex, primary diagnosis, prior operations to the hip, height, weight, range of motion of the hip to be operated, leg length discrepancy, and the presence or absence of a Trendelenburg gait pattern. Clinical assessments were collected preoperatively, and postoperatively at 3 months, 6 months, and 1 year. The data for this study were extracted and summarized on May 25, At that time, there were 15 of 43 cases in each group with 1-year follow-up data available. This data included 1-year radiographs. The instruments used were the (1) Harris Hip Score, (2) the Medical Outcomes Study 36-Item Short-Form Health Survey (MOS SF-36), (3) the Medical Outcomes Study 6-Item Sleep Scale, and (4) the Western Ontario and McMaster (WOMAC) Osteoarthritis Index. Before surgery, the hospital admission date (and time) was recorded. Data recorded during surgery included the surgical technique, operating room time, fluoroscopy time, blood loss measured from the cell saver, transfusion of blood and blood products, and intraoperative complications. The MOS SF-36 is a 36-item generic survey that collects information on 8 health concepts: physical functioning, role-physical, bodily pain, general health, vitality, social functioning, role-emotional, mental health, and reported health transition. Individual items were scored on an integer scale, and concept scores were generated from composites of the item scores. Composite scores ranged from 0 to 100, with a score of 100 being the best. In addition, composite mental and physical health scores ranging from 0 to 100 were constructed using population norms. The WOMAC Osteoarthritis Index is a 24-item disease-specific survey that collects information on
4 Comparison of the 2-Incision and Mini-Incision Posterior THA Technique! Duwelius et al 51 3 areas of patient symptoms: pain, stiffness, and physical function. Individual items were scored on an integer scale, and item scores were combined to generate each area. In addition, a total WOMAC score based on all 24 items was generated. The MOS Sleep Scale is a 6-item quality of life survey, which assesses patient sleep patterns. The Harris Hip Scale is a preoperative and postoperative assessment of pain, function, range of motion, and absence of deformity designed to be equally applicable to different hip problems and different methods of treatment [18]. After discharge, for the first 6 weeks, all patients completed a patient diary recording the time they returned to activities of daily living without assistance (bathing, dressing, getting in and out of bed and chair), driving, work, and the discard of an assistive device for ambulation. Complication Assessment Complications evaluated in this study included leg length discrepancy, component malposition, subsidence, periprosthetic fracture, sciatic or femoral nerve injury, lateral femoral cutaneous nerve injury, infection, and wound problems. Radiographic Assessment Radiographs were performed immediately postoperative, at 6 weeks, 3 months, 6 months, and annual visits. These were an anterior-posterior pelvic radiograph that included the acetabulum and femoral stem as well as a lateral (cross-table) of the femur and acetabulum. For this study, the acetabular inclination and anteversion were measured from the 6-week or 3-month radiograph. From the radiograph with the longest follow-up, any evidence of component position change (migration) or radiolucent line formation, osteolysis, and heterotopic ossification was measured. The radiographic measurements were performed on the mini-posterior and 2-incision patients at the longest follow-up period. There were 15 of 43 patients with 1-year follow-up in each group. All patients in the 2-incision group had intraoperative fluoroscopy to confirm cup and stem insertion. Statistical Methods Forty-three matched pairs provided at least 80% power at a 2-sided a level of.05 to detect clinically meaningful differences in study variables Type I error rates (a level,.05) were adjusted for multiplicity using a Bonferroni correction [19]. For comparisons made only once (eg, comparisons of preoperative, operative, immediate postoperative variables, return to function, and complication rates), statistical significance was inferred at the.05 level. Unmatched analyses were performed on the matched data using SAS (v 9.13) for the Microsoft Windows 2000 platform. Clinical Assessment Results Fig. 1 presents mean scores by surgical technique at each time of assessment. Benefits in both techniques are confirmed by the large positive Fig. 1. Average Harris Hip Score and selected SF-36 and WOMAC scores at each time of assessment.
5 52 The Journal of Arthroplasty Vol. 22 No. 1 January 2007 Fig. 2. Statistically significant patient outcomes at each time of assessment. gains (improvement) in Harris Hip Scores, MOS SF-36 Physical Health and Physical Function scores, as well as large negative gains (improvement) in WOMAC pain, stiffness, and physical function seen with increasing time since total hip arthroplasty. Patients were considered compliant if they completed the patient diary entries during postoperative weeks 1 through 6 or if a scheduled clinical examination was attended at postoperative weeks 2 and 6, months 3 and 6, and at 1 year. Two-incision patients had a mean compliance of 91% (range, 86%-95%) during the first 6 postoperative weeks, whereas posterior mini-incision patients had a mean of 88% (range, 77%-95%) ( P =.68). At 6 weeks postoperatively, the compliance was 41 (95.3%) of 43 patients in both groups; at 6 months, 33 (76.7%) of 43 two-incision patients and 28 (65.1%) of 43 posterior mini-incision patients ( P =.23); and at 12 months, 26 (70.3%) of 37 twoincision patients and 26 (86.7%) of 30 posterior mini-incision patients ( P =.09). At 12 months, not all patients had attained their 1-year postoperative check-up. The postoperative clinical outcomes, which had statistically significant differences, are displayed in Fig. 2. There were 2 items in the Harris Hip Score that favored the 2-incision patients, and these were no assistive device needed at 2 weeks postoperatively ( P =.001) and negotiating stairs without a railing at 5 weeks postoperatively ( P =.004). There were 2 WOMAC pain subscale items that favored the posterior mini-incision, and these were no pain at night at 6 weeks ( P =.0028) and pain at night in bed at 6 weeks ( P =.004). At 6 weeks postoperatively, the total WOMAC pain subscale score for the posterior mini-incision patients was a mean of 1.22 (range, 0-10), and for the 2-incision group was a mean of 3.31 (range, 0-11) ( P =.003). Prescription antiinflammatory use had significantly greater prevalence in 2-incision patients (47%) versus mini-incision (23%) ( P =.04). At 6 weeks postoperatively, there were 2 MOS Sleep Scale items that favored the posterior mini-incision patients, which were no trouble falling asleep ( P =.0004), and if awakened, no trouble falling back to sleep ( P =.003). We have looked closely at the pain scores and graphs, and we cannot say with certainty that there is a difference in looking at our aggregate data. The numerous pain graphs at different points give data to support either group being beneficial in regards to pain relief but at different times. Results, which measured return to function, favored the 2-incision patients for 8 of the 9 items. Two of these items had statistical difference: the time to resume driving, which was 13 days (range, 2-31) for 2-incision patients and a mean of 24 days (range, 6-32) for posterior mini-incision patients ( P=.04); and the time to resume shopping, which had a mean
6 Comparison of the 2-Incision and Mini-Incision Posterior THA Technique! Duwelius et al 53 of 14 days (range, 3-24) for 2-incision patients and a mean of 26 days (range, 6-37) for mini-incision patients ( P =.01). Length of hospital stay was significantly shorter (b0.0001) for 2-incision patients with a mean of 30.7 hours (range, ) versus mini-incision patients with a mean of 44.6 hours (range, ). There were only 3 patients in the mini-posterior group who stayed longer than day 2. Two patients were discharged on postoperative day 3. None of these outliers in the mini-posterior group were related to any orthopedic problems. One patient aged 58 had dizziness and had difficulties being cleared by physical therapy. Another 68-year-old female patient had diabetes that was difficult to manage postoperatively and experienced lightheadedness and extreme calf spasms that significantly delayed mobilization. One patient was discharged on postoperative day 4. A 73-year-old woman was unable to rehabilitate quickly secondary to multiple medical problems and required 2 units of packed red blood cells (PRBCs). She also had a nutritional consult. None of these outliers in the mini-posterior group were related to any orthopedic problems. Data from the operation that has statistical difference was blood loss (as collected in a cell saver), which had a mean of 366 F 215 ml (range, ml) for the 2-incision group and a mean of 247 F 90 ml (range, ml) for the posterior mini-incision patients ( P =.001). Three 2-incision patients and one posterior mini-incision patient received allogenic blood transfusions. Although we had 1 outlier for blood loss in the 2-incision total hip arthroplasty group, there were no adverse encounters with early discharge in either group. In fact, the patient with an estimated blood loss (EBL) of 1400 ml was discharged the next day after receiving 1 unit of blood. This 65- year-old woman completed all of our discharge requirements and was discharged on the following day. Operative time for the 2-incision patients was a mean 93.7 F 90 minutes (range, minutes) as compared to a mean 61.7 F 60 minutes (range, minutes) for posterior mini-incision patients ( P =.002). There were no complaints of leg length discrepancy, and only 3 patients had a measured length difference (b5 mm) from the preoperative evaluation. Radiographic Results The mean cup abduction angle for the 2-incision hips was F 4.28 (range, ), and for the posterior mini-incision hips was F 5.38 ( ) (P =.0003). Our target number was 458 for both approaches. We had 4 outliers in the 2-incision group that were greater than 508 and 2 in the mini-posterior group. Most of the 2-incision cup abduction angles were between 458 and 508. The cup anteversion for the 2-incision hips had a mean F 5.38 (range, ), and for the posterior mini-incision hips was F 7.98 (range, ) ( P =.2624). The stem was implanted in 58 varus in 1 hip in the posterior mini-incision group, and in one 2-incision patient, the stem was in 38 varus. All other stems were in neutral alignment. Complications There were 2 (4.6%) of 43 hips with complications in the 2-incision group and none in the posterior mini-incision group. The 2 complications were 1 intraoperative femoral neck fracture, which was treated with a cerclage wire, and 1 suture abscess, which was treated with irrigation and debridement and antibiotics. For the 2-incision patients, 6 of 43 complained of some numbness in the anterolateral thigh, but none had frank myalgia paresthetica symptoms. Of 43 patients, 3 have permanent numbness in the distribution of the lateral femoral cutaneous nerve, the other 3 resolved completely. No patients complained of nerve pain. All patients selected for the 2-incision surgical technique are told of this possibility preoperatively because this is not a complication with the miniposterior approach. Leg length assessment at 6 weeks revealed that 33 (85%) 2-incision and 32 (84%) mini-posterior incision patients had equal leg lengths. There were 6 (15%) patients in the 2-incision group with leg length discrepancy at 6 weeks. There were 6 (16%) patients in the miniposterior group at 6 weeks with leg length discrepancy. Of the 20 cases per group with leg length assessment available at 6 months, both groups were 100% equal. No patient had a leg length discrepancy greater than one fourth of an inch. There were no sciatic, peroneal, or common femoral nerve injuries. There were no components that subsided. No patient in this series required revision. Discussion The hypothesis of this study was not proven. Although the patients with the 2-incision operation had overall better function and there were no statistically greater number of complications for the 2-incision than the posterior mini-incision operation, the posterior mini-incision patients had similar pain relief. Neither procedure clearly benefitted consistently in regard to decreased pain. Both
7 54 The Journal of Arthroplasty Vol. 22 No. 1 January 2007 operations were effective in improving pain and function, and both were safe. We were closer to our target cup abduction angle more consistently with the mini-posterior than with the 2-incision despite the ancillary use of fluoroscopy. Outliers continue to exist with cup position despite the use of fluoroscopy and navigation. Both operations successfully decreased the hospital stay with the mean discharge for 2-incision patients being 30 hours and for the posterior mini-incision patients being 45 hours. All 2-incision patients were the first or second case of the day, which allowed for a faster recovery time on the day of surgery. The 2-incision hospital stay was probably shorter because of patient expectations and preoperative education. This average hospital length of stay is lower than reported for traditional total hip arthroplasty operations in the National Data Base (4 days) [20]. This average is also lower than our average hospital stay of between 4 and 5 days with the traditional total hip arthroplasty and before the newer clinical hip pathway. We believe one of the reasons for the decreased hospital stay was the preoperative education and the total hip arthroplasty clinical pathway used for all patients. Shorter hospital stays are beneficial to health care costs and for reduction of nosocomial infections. Considering the longer operating time for the 2-incision technique and an average hospital stay for the mini-posterior incision, there is not much difference in the hospital costs between the two; however, both showed the advantage of shorter hospital stay and reductions in rehabilitation center costs. This study was not designed to compare small-incision operations to the traditional length operations. In this study, 2 small-incision operations were compared, and both could be completed successfully with advantages differing for the two. The matched-pair analysis allowed us to identify outcomes that differed between the techniques with statistical accounting for the multiple tests performed. We believe that the match-pair analysis method has inherent benefits, which are much greater than the 2 large series of patients, which could be disparate in their characteristics [21-26]. In the comparison of these 2 small-incision operations, there were 3 advantages for the 2-incision operation. First, the average stay was 1 day less; second, these patients had no postoperative hip precautions; and third, there was earlier better postoperative function with statistical difference for return to driving and return to shopping. Admittedly, two of these advantages may have been influenced by the preoperative education. Posterior mini-incision patients were instructed to follow dislocation precautions because it was felt to be safer for them. The necessity for postoperative hip precautions in patients may have influenced their return to driving and to shopping. Surgeons may no longer advocate these restrictions because of posterior capsular repair and newer implants where the neck and acetabulum do not impinge (especially with larger femoral heads). The 2-incision patients preoperatively were selfassessed to have better general health ( P =.03) versus 1 year ago ( P =.03) and have the ability to walk more than 1 mile ( P =.04) in comparison with the posterior mini-incision patients. Otherwise, preoperative activity levels did not differ between the groups following matching. There were 2 advantages between the groups for the posterior mini-incision patients. These patients had favorable differences in the technical performance of the operation with (1) less time in the operating room and (2) less blood loss. This miniposterior approach is easier to teach and has a lower learning curve. Neither group had a clear benefit in regard to pain. The numerous pain graphs at different points give data to support either group being beneficial in regards to pain relief but at different times. The strengths of this study include the match pairing that reduces the effect of several variables on the outcome, the statistical treatment, and the comparison of several clinical outcome measures [21-26]. The patient self-assessment of short-term functional weekly outcome has not been previously reported. Physicians score pain differently than patients. Surgeons may tend to perceive patients function differently, and the patients perception of their own functional improvement is what is more important [27]. The only difference in the 2 groups was that the mini-posterior group received instructions in total hip precautions whereas the 2-incision group did not. To decrease the effects of bias, the patients were matched to reduce patient selection bias and differences in preoperative quality of life measures. The matching process allowed us to control for differences in preoperative pain, function, and stiffness, reducing the confounding of patient benefits from related differences. Although additional preoperative variables could have been matched upon (eg, patient activity level), they would have certainly led to fewer matched pairs and thereby reduce the number of study patients and statistical power. Although there still may be selection bias inherent with any study and uncontrolled confounding effects, short of a randomized prospective study, this is the strongest approach for valid comparisons. The match-pair
8 Comparison of the 2-Incision and Mini-Incision Posterior THA Technique! Duwelius et al 55 criteria we used were similar to other well-established and reported series [21-26]. The limitations of this study include the fact that it is not a randomized prospective study. Twoincision patients were subselected based on age, body mass index, and femoral and acetabular anatomy. There may have been other selection bias such as the personality of patients seeking this operation and patients having higher expectations with the 2-incision operation. One of the possible causes of the differences in walking assistance postoperatively may have been the preoperative education and the potential fear instilled into patients when dislocation precautions are emphasized. These factors may influence their return to driving and their postoperative confidence. In this study, we had fewer complications with the 2-incision operation than had been reported by White and Archibeck [3]. These authors reviewed results of the 2-incision operation among several surgeons and reported a 6% incidence of fracture of the femur and 0.2% incidence of dislocation [3]. These complications were from the first 10 operations performed by the surgeons, and our results are better, most likely, because we continued to perform this operation and improve our technique. In the multicenter review of the 2-incision technique among surgeons who routinely perform the operation, the complications were 1.3% femoral fractures, 1.0% dislocation, and 0.3% revision rate [1]. Caution should be advised in performing any of these techniques with inadequate training or low volume use. Our experience reported here suggests that for surgeons who do not want to or who cannot participate in the necessary learning process for the 2-incision operation, the posterior miniincision total hip arthroplasty provided excellent patient satisfaction with minimal morbidity. Woolson et al [4] has questioned the safety of the posterior mini-incision operation based on their experience with their first 50 small-incision operations. Our experience with the posterior miniincision patients in this matched-pair series, and that of Ogonda et al [9] in a large randomized study, does not confirm the safety concerns of Woolson et al [4]. This matched-paired series of patients has adequate statistical power to detect meaningful differences between the two operative techniques studied. We conclude that these operations were safe for both groups of patients. We can also conclude that the type of outcome differed between the different types of incision. Just because we were making a conclusion that the type of outcome differed between the two approaches does not mean we were making a qualitative judgment that one was better that the other. The results of this study provides confirmation that the use of either one of these incisions, when performed safely and effectively, provides pain relief, a high level of postoperative function, decreased hospital stay, and low complication rates. What we have instead studied is two different approaches, and we reported to the orthopedic community the differences that we have found by the use of these techniques. We feel the orthopedic community needs to have information about the different techniques currently being suggested for smallincision surgery. We are simply trying to provide some information for them to make decisions. This study does not provide any information comparing the outcomes of these 2 small-incision operations with the outcomes of traditional total hip arthroplasty incisions. This study supports the use of a clinical hip pathway, the perioperative pain management protocol, and the inherent benefits of smaller incisions. References 1. Berry DJ, Berger RJ, Callaghan JJ, et al. Minimally invasive total hip arthroplasty: development, early results, and a critical analysis. J Bone Joint Surg 2003;85-A: Sculco TP. Is smaller necessarily better? Am J Orthop 2003;32: White RA, Archibech MJ. Learning curve for the minimally invasive two-incision total hip replacement. Clin Orthop Relat Res 2004;429: Woolson ST, Mow CS, Syquia JF, et al. Comparison of primary total hip replacements performed with a standard incision or a mini incision. J Bone Joint Surg 2004;86-A: Digioia AM, Plakeychuk AY, Levison TJ, et al. Miniincision technique for total hip arthroplasty with navigation. J Arthroplasty 2003;18: Hartzband MA. Posterolateral minimal incision for total hip replacement: technique and early results. Orthop Clin North Am 2004;35: Light TR, Keggi KJ. Anterior approach to hip arthroplasty. Clin Orthop 1980;152: Sculco TP, Jordan LC. The mini incision approach to total hip arthroplasty. Instr Course Lect 2004;53: Ogonda L, Wilson R, Archbold P, et al. A minimalincision technique in total hip arthroplasty does not improve early postoperative outcomes. J Bone Joint Surg 2005;87-A: Sculco TP. Minimally invasive total hip arthroplasty: in the affirmative. J Arthroplasty 2004;19(4 Supp 1): Berger RA. The technique of minimally invasive hip surgery using the two-incision approach. Instr Course Lect 2004;53:149.
9 56 The Journal of Arthroplasty Vol. 22 No. 1 January Berger RA, Duwelius PJ. Orthop Clin North Am 2004;35: Berger RA. Total hip arthroplasty using the minimally invasive two-incision approach. Clin Orthop 2003; Phillips CB, Barrett JA, Losina E, et al. Incidence rates of dislocation, pulmonary embolism, and deep infection during the first 6 months after elective total hip replacement. J Bone Joint Surg Am 2003; 85-A: Dorr LD. The mini incision hip: building a ship in a bottle. Orthopedics 2004;2: Waldman BJ. Minimally invasive total hip replacement and perioperative management: early experience. J South Orthop Assoc 2002;25: Wenz JF, Gurkan L, Jibodh SR. Mini-incision total hip arthroplasty: a comparative assessment of perioperative outcomes. Orthopaedics 2002;25: Harris WH. Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. J Bone Joint Surg 1969; S1-A: Armitage P, Berry G, Matthews JNS. Statistical methods in medical research. 4th ed. Blackwell: Malden; p Agency for Health Research and Quality. HCUPnet, Nationwide Inpatient Sample. ahrq.gov/hcupnet.asp. Accessed July 26, McPherson EJ, Dorr LD, Gruen TA, et al. Hydroxyapatite-Coated Proximal Ingrowth Femoral Stems. A Match-Pair Controlled Study. Clin Orthop Relat Res. # 135: Min B, Longjohn D, Dorr LD, et al. Radiographic comparison of diaphyseal grit blasted with smooth surface stems by matched pair analysis. Clin Orthop Relat Res 2000; Ranawat C, Beaver WB, Sharrock NE, et al. Effect of hypotensive epidural anesthesia on acetabular cement-bone fixation in total hip arthroplasty. J Bone Joint Surg 1991;73-B: Rothman RH, Hozack WJ, Ranawat A, et al. Hydroxyapatite-coated femoral stems. A matched-pair analysis of coated and uncoated implants. J Bone Joint Surg 1996;78-A: Udomkiat P, Bei-jiang M, Dorr LD, et al. Functional comparison of posterior cruciate retention and substitution knee replacement. Clin Orthop Relat Res 2000;378: Udomkiat P, Dorr LD, Long W. Matched-pair analysis of all-polyethylene versus metal-backed tibial components. J Arthroplasty 2001;16: Salmon P, Hall GM, Peerbhoy D, et al. Recovery from hip and knee arthroplasty: patients perspective on pain, function, and quality of life, and well-being up to 6 months postoperatively. Arch Phys Med Rehabil 2001;82:380.
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6
 Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
Total Hip Arthroplasty Performed Using Conventional and Computer-Assisted, Tissue- Preserving Techniques 6 Stephen B. Murphy, MD, Timo M. Ecker, MD and Moritz Tannast, MD Introduction Less invasive techniques
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of minimally invasive two-incision surgery for total hip replacement Introduction This
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of minimally invasive two-incision surgery for total hip replacement Introduction This
Original Article-Surgery. Masjudin Tumin, Kyung Soon Park, Azlina Amir Abbas and Taek Rim Yoon* INTRODUCTION
 Original Article-Surgery www.cmj.ac.kr Comparison of the Outcome in Bilateral Staged Total Hip Arthroplasty: Modified Two-Incision Minimally Invasive Technique versus the Conventional Posterolateral Approach
Original Article-Surgery www.cmj.ac.kr Comparison of the Outcome in Bilateral Staged Total Hip Arthroplasty: Modified Two-Incision Minimally Invasive Technique versus the Conventional Posterolateral Approach
Burwood Road, Concord 160 Belmore Road, Randwick
 www.orthosports.com.au 47 49 Burwood Road, Concord 160 Belmore Road, Randwick Anterior Approach to the Hip Orthopaedic surgeon What s the fuss all about this NEW surgery? Not a new approach or surgery
www.orthosports.com.au 47 49 Burwood Road, Concord 160 Belmore Road, Randwick Anterior Approach to the Hip Orthopaedic surgeon What s the fuss all about this NEW surgery? Not a new approach or surgery
Anterior Approach to Hip Replacement Surgery
 Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Bone Bangalore
 Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
Hip Arthroplasty with Minimally Invasive Surgery
 The Journal of Arthroplasty Vol. 21 No. 6 Suppl. 2 2006 Hip Arthroplasty with Minimally Invasive Surgery A Survey Comparing the Opinion of Highly Qualified Experts vs Patients Javad Parvizi, MD, FRCS,
The Journal of Arthroplasty Vol. 21 No. 6 Suppl. 2 2006 Hip Arthroplasty with Minimally Invasive Surgery A Survey Comparing the Opinion of Highly Qualified Experts vs Patients Javad Parvizi, MD, FRCS,
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
Credentials: Advances in Hip Arthritis Treatment. About My Former Practice: What is Arthritis?
 Advances in Hip Arthritis Treatment C. Brian Blackwood, MD www.boulderhipandknee.com (303) 974-4705 Credentials: University Of Washington- SOM University of New Mexico- Residency Coon Joint Replacement
Advances in Hip Arthritis Treatment C. Brian Blackwood, MD www.boulderhipandknee.com (303) 974-4705 Credentials: University Of Washington- SOM University of New Mexico- Residency Coon Joint Replacement
CLINICAL PAPER / ORTHOPEDIC
 HIP LEG LENGTH AND OFFSET Kelley T.C. and Swank M.L. (2009) Using CAS leads to more accurate positioning within the safe zone (inclination between 30 and 50, anteversion between 5 and 25 ) CAS improves
HIP LEG LENGTH AND OFFSET Kelley T.C. and Swank M.L. (2009) Using CAS leads to more accurate positioning within the safe zone (inclination between 30 and 50, anteversion between 5 and 25 ) CAS improves
Case Report Anterior Subluxation after Total Hip Replacement Confirmed by Radiographs: Report of Two Cases
 SAGE-Hindawi Access to Research Advances in Orthopedics Volume 2011, Article ID 519254, 4 pages doi:10.4061/2011/519254 Case Report Anterior Subluxation after Total Hip Replacement Confirmed by Radiographs:
SAGE-Hindawi Access to Research Advances in Orthopedics Volume 2011, Article ID 519254, 4 pages doi:10.4061/2011/519254 Case Report Anterior Subluxation after Total Hip Replacement Confirmed by Radiographs:
Total Hip Replacement. Find out why the Anterior Approach may be right for you.
 Total Hip Replacement Find out why the Anterior Approach may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of the Direct Anterior Approach to total hip arthroplasty.
Total Hip Replacement Find out why the Anterior Approach may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of the Direct Anterior Approach to total hip arthroplasty.
Total Knee Replacement
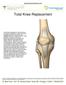 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Clinical Practice Guideline for Patients Requiring Total Hip Replacement
 Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Clinical Practice Guideline for Patients Requiring Total Hip Replacement Inclusions Patients undergoing elective total hip replacement Exclusions Patients with active local or systemic infection or medical
Two Years Outcomes Of Total Hip Replacement Using A Short Stem With Femoral Neck Anchoring
 Two Years Outcomes Of Total Hip Replacement Using A Short Stem With Femoral Neck Anchoring Elias I. 1, Krieger M 1, Rinaldi G. 2, Christian L. 1, Mancini N. 2 1 Klinik Rotes Kreutz, Frankfurt Am Main,
Two Years Outcomes Of Total Hip Replacement Using A Short Stem With Femoral Neck Anchoring Elias I. 1, Krieger M 1, Rinaldi G. 2, Christian L. 1, Mancini N. 2 1 Klinik Rotes Kreutz, Frankfurt Am Main,
Hip Resurfacing.
 Hip Resurfacing http://www.birminghamhipresurfacing.com/hipresurfacing/technology.cfm The end of the femur is capped somewhat like a tooth cap The hip socket receives a cupped implant to move together
Hip Resurfacing http://www.birminghamhipresurfacing.com/hipresurfacing/technology.cfm The end of the femur is capped somewhat like a tooth cap The hip socket receives a cupped implant to move together
DIRECT SUPERIOR HIP APPROACH IN TOTAL HIP ARTHROPLASTY. Anil Thomas, MD Adult Reconstruction Peachtree Orthopedics Atlanta, GA
 DIRECT SUPERIOR HIP APPROACH IN TOTAL HIP ARTHROPLASTY Anil Thomas, MD Adult Reconstruction Peachtree Orthopedics Atlanta, GA Disclosures None Direct Superior Approach History and development of the approach
DIRECT SUPERIOR HIP APPROACH IN TOTAL HIP ARTHROPLASTY Anil Thomas, MD Adult Reconstruction Peachtree Orthopedics Atlanta, GA Disclosures None Direct Superior Approach History and development of the approach
Hip Surgery and Mobility
 Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers
 CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
Total Hip Replacement
 PATIENT EDUCATION Total Hip Replacement A guide to understanding total hip replacement surgery, featuring The George Archer Story. BACK TO MOBILITY George Archer s Personal Adventure On April16, 1996,
PATIENT EDUCATION Total Hip Replacement A guide to understanding total hip replacement surgery, featuring The George Archer Story. BACK TO MOBILITY George Archer s Personal Adventure On April16, 1996,
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing
 Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Robotic-Arm Assisted Surgery
 Mako TM Robotic-Arm Assisted Surgery for Total Hip Replacement A Patient s Guide Causes of Your Hip Pain Your joints are involved in almost every activity you do. Movements such as walking, bending and
Mako TM Robotic-Arm Assisted Surgery for Total Hip Replacement A Patient s Guide Causes of Your Hip Pain Your joints are involved in almost every activity you do. Movements such as walking, bending and
TOTAL KNEE ARTHROPLASTY (Total Knee Replacement) The Knee Joint
 (Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
(Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
Preventing complications in THR
 Preventing complications in THR Dr. (Prof.) Anil Arora MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic
Preventing complications in THR Dr. (Prof.) Anil Arora MS (Ortho) DNB (Ortho) Dip SIROT (USA) FAPOA (Korea), FIGOF (Germany), FJOA (Japan) Commonwealth Fellow Joint Replacement (Royal National Orthopaedic
Anesthesia for Total Hip and Knee Arthroplasty
 Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
Anesthesia for Total Hip and Knee Arthroplasty Typical approach Describe anesthesia technique Rather Describe issues with THA and TKA How anesthesia can modify Issues Total Hip Total Knee Blood Loss ++
ACETABULAR CUP SURGICAL TECHNIQUE
 ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
ACETABULAR CUP SURGICAL TECHNIQUE ACETABULAR CUP DEVICE INDICATIONS FOR USE The ICONACY I-Hip total hip replacement is indicated for the following conditions: 1. A severely painful and/or disabled hip
Periacetabular Osteotomy (PAO)
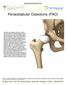 Periacetabular Osteotomy (PAO) At the top of your thigh bone, the femur, is a ball shaped structure called the femoral head, which fits in a socket in the pelvis, called the acetabulum. Both of these structures
Periacetabular Osteotomy (PAO) At the top of your thigh bone, the femur, is a ball shaped structure called the femoral head, which fits in a socket in the pelvis, called the acetabulum. Both of these structures
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Presented by : Frank Filice (PT) London Health Sciences Centre
 Total Hip Arthroplasty Presented by : Frank Filice (PT) London Health Sciences Centre June 20, 2008 Purpose Provide information that explains the rationale for the post-op precautions. Provide some general
Total Hip Arthroplasty Presented by : Frank Filice (PT) London Health Sciences Centre June 20, 2008 Purpose Provide information that explains the rationale for the post-op precautions. Provide some general
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Day of Surgery Discharge after Unicompartmental Knee Arthroplasty (UKA): An Effective Perioperative Pathway. Jay Patel, MD Hoag Orthopedic Institute
 Day of Surgery Discharge after Unicompartmental Knee Arthroplasty (UKA): An Effective Perioperative Pathway Jay Patel, MD Hoag Orthopedic Institute UKA Rapid Recovery Protocol Purpose of Study Describe
Day of Surgery Discharge after Unicompartmental Knee Arthroplasty (UKA): An Effective Perioperative Pathway Jay Patel, MD Hoag Orthopedic Institute UKA Rapid Recovery Protocol Purpose of Study Describe
ADVANCES IN JOINT REPLACEMENT AND REHABILITATION IMPLICATIONS
 ADVANCES IN JOINT REPLACEMENT AND REHABILITATION IMPLICATIONS VALENTIN ANTOCI JR. MD PHD Hip and Knee Surgeon Assistant Professor of Orthopedic Surgery Alpert Medical School with Brown University University
ADVANCES IN JOINT REPLACEMENT AND REHABILITATION IMPLICATIONS VALENTIN ANTOCI JR. MD PHD Hip and Knee Surgeon Assistant Professor of Orthopedic Surgery Alpert Medical School with Brown University University
Differences in Functional and Pain-related Outcomes for Patients Following Total Hip Arthroplasty Performed Using a Posterior versus Anterior Approach
 Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2014 Differences in Functional and Pain-related Outcomes for Patients Following Total Hip Arthroplasty Performed
Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2014 Differences in Functional and Pain-related Outcomes for Patients Following Total Hip Arthroplasty Performed
SURGICAL TECHNIQUE. Alpine Cementless Hip Stem
 SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
Management of Hip Fractures
 Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
Management of Hip Fractures in the Elderly Patient David A. Brown MD COL U.S. Army Ret. The Center for Orthopedics and Neurosurgery Optimizing Management of Hip Fractures in the Elderly Patient Optimizing
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Hip Replacement - Anterior
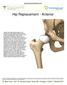 Hip Replacement - Anterior Anterior hip replacement surgery is an alternative to hip replacements where the surgeon accesses the hip joint from the side or through the buttocks. The anterior procedure
Hip Replacement - Anterior Anterior hip replacement surgery is an alternative to hip replacements where the surgeon accesses the hip joint from the side or through the buttocks. The anterior procedure
Benefits of Posterior Single-Incision Less-Invasive THA using the SL-Plus Cementless Stem
 Benefits of Posterior Single-Incision Less-Invasive THA using the SL-Plus Cementless Stem Todd V. Swanson, MD Desert Orthopaedic Center Las Vegas, Nevada, USA Abstract Four hundred six consecutive cementless
Benefits of Posterior Single-Incision Less-Invasive THA using the SL-Plus Cementless Stem Todd V. Swanson, MD Desert Orthopaedic Center Las Vegas, Nevada, USA Abstract Four hundred six consecutive cementless
Hemiarthroplasty (half hip replacement)
 Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty
 texas orthopaedic journal CASE REPORT Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty Gaurav S. Sharma, BA; Ronald W. Lindsey, MD Department of Orthopaedic Surgery
texas orthopaedic journal CASE REPORT Leg Length Discrepancy in a Patient with Ipsilateral Total Knee and Total Hip Arthroplasty Gaurav S. Sharma, BA; Ronald W. Lindsey, MD Department of Orthopaedic Surgery
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
Approach Patients with CONFIDENCE
 Design Rationale Approach Patients with CONFIDENCE The ACTIS Total Hip System is the first DePuy Synthes stem specifically designed to be utilized with tissue sparing approaches, such as the anterior
Design Rationale Approach Patients with CONFIDENCE The ACTIS Total Hip System is the first DePuy Synthes stem specifically designed to be utilized with tissue sparing approaches, such as the anterior
ACTIS. TOTAL HIP SYSTEM Approach Active Patients with Confidence DESIGN RATIONALE
 ACTIS TOTAL HIP SYSTEM Approach Active Patients with Confidence DESIGN RATIONALE APPROACH ACTIVE PATIENTS WITH CONFIDENCE The ACTIS Total Hip System is the first DePuy Synthes Companies of Johnson & Johnson
ACTIS TOTAL HIP SYSTEM Approach Active Patients with Confidence DESIGN RATIONALE APPROACH ACTIVE PATIENTS WITH CONFIDENCE The ACTIS Total Hip System is the first DePuy Synthes Companies of Johnson & Johnson
Early Complications of Anterior Supine Intermuscular Total Hip Arthroplasty
 n Feature Article Early Complications of Anterior Supine Intermuscular Total Hip Arthroplasty Chengla Yi, MD, PhD; Juan F. Agudelo, MD; Michael R. Dayton, MD; Steven J. Morgan, MD abstract Full article
n Feature Article Early Complications of Anterior Supine Intermuscular Total Hip Arthroplasty Chengla Yi, MD, PhD; Juan F. Agudelo, MD; Michael R. Dayton, MD; Steven J. Morgan, MD abstract Full article
Chronic Lymphedema of the Lower Limb: A Rare Cause of Dislocation of Total Hip Arthroplasty
 Open Access Case Report DOI: 10.7759/cureus.579 Chronic Lymphedema of the Lower Limb: A Rare Cause of Dislocation of Total Hip Arthroplasty Raju Vaishya 1, Amit Kumar Agarwal 1, Nishint Gupta 2, Vipul
Open Access Case Report DOI: 10.7759/cureus.579 Chronic Lymphedema of the Lower Limb: A Rare Cause of Dislocation of Total Hip Arthroplasty Raju Vaishya 1, Amit Kumar Agarwal 1, Nishint Gupta 2, Vipul
TOTAL HIP REPLACEMENT:
 THR Prosthesis Design TOTAL HIP REPLACEMENT: PROSTHESIS DESIGN FEATURES JESS JOHNSTON & MELINDA ZIETH History of Hip Prosthesis Joint Replacement Registry Implant Design Technology & Future History and
THR Prosthesis Design TOTAL HIP REPLACEMENT: PROSTHESIS DESIGN FEATURES JESS JOHNSTON & MELINDA ZIETH History of Hip Prosthesis Joint Replacement Registry Implant Design Technology & Future History and
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
Advances in Joint Replacement
 Advances in Joint Replacement Seth Greenky, MD Chairman, Musculoskeletal Services, St. Joseph s Hospital Partner, Syracuse Orthopedic Specialists Associate Clinical Professor, Upstate Medical Center CoMedical
Advances in Joint Replacement Seth Greenky, MD Chairman, Musculoskeletal Services, St. Joseph s Hospital Partner, Syracuse Orthopedic Specialists Associate Clinical Professor, Upstate Medical Center CoMedical
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Metha Short Hip Stem System
 Metha Short Hip Stem System Accuracy That Stands Alone Aesculap Orthopaedics Metha Short Hip Stem System Designed For Anatomic Accuracy The Metha Short Hip Stem is designed for anatomic accuracy to restore
Metha Short Hip Stem System Accuracy That Stands Alone Aesculap Orthopaedics Metha Short Hip Stem System Designed For Anatomic Accuracy The Metha Short Hip Stem is designed for anatomic accuracy to restore
Total hip replacement
 Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Hip Fractures. Anatomy. Causes. Symptoms
 Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Tradition Hip Primary Surgical Technique
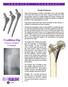 Design Rationale Many total hip designs in today s marketplace do not take advantage of the known forces present in the femur. Long term stability of a total hip prosthesis requires an implant design and
Design Rationale Many total hip designs in today s marketplace do not take advantage of the known forces present in the femur. Long term stability of a total hip prosthesis requires an implant design and
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication?
 CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
Navigation for total hip arthroplasty
 Interact Surg (2008) 3: 128 134 Springer 2008 DOI 10.1007/s11610-008-0084-4 ORIGINAL ARTICLE Navigation for total hip arthroplasty O. Guyen 1,V.Pibarot 1, J. Bejui-Hugues 2,SCORGroup 1 Service de chirurgie
Interact Surg (2008) 3: 128 134 Springer 2008 DOI 10.1007/s11610-008-0084-4 ORIGINAL ARTICLE Navigation for total hip arthroplasty O. Guyen 1,V.Pibarot 1, J. Bejui-Hugues 2,SCORGroup 1 Service de chirurgie
Effect of Superior Placement of the Hip Center on Abductor Muscle Strength in Total Hip Arthroplasty
 The Journal of Arthroplasty Vol. 24 No. 2 2009 Effect of Superior Placement of the Hip Center on Abductor Muscle Strength in Total Hip Arthroplasty Takahiko Kiyama, MD, Masatoshi Naito, MD, PhD, Hiroshi
The Journal of Arthroplasty Vol. 24 No. 2 2009 Effect of Superior Placement of the Hip Center on Abductor Muscle Strength in Total Hip Arthroplasty Takahiko Kiyama, MD, Masatoshi Naito, MD, PhD, Hiroshi
A Patient s Guide to Artificial Joint Replacement of the Hip, Anterior Approach
 A Patient s Guide to Artificial Joint Replacement of the Hip, Anterior Approach 2321 Coronado Idaho Falls, ID 83404 Phone: 208-227-1100 jpond@summitortho.net DISCLAIMER: The information in this booklet
A Patient s Guide to Artificial Joint Replacement of the Hip, Anterior Approach 2321 Coronado Idaho Falls, ID 83404 Phone: 208-227-1100 jpond@summitortho.net DISCLAIMER: The information in this booklet
ORIGINAL PAPER. Department of Orthopedic Surgery, Hamamatsu Medical Center ABSTRACT
 Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
Nagoya J. Med. Sci. 71. 145 ~ 150, 2009 ORIGINAL PAPER AUTOGENOUS BULK STRUCTURAL BONE GRAFTING FOR RECONSTRUCTION OF THE ACETABLUM IN PRIMARY TOTAL HIP ARTHROPLASTY: AVERAGE 12-YEAR FOLLOW-UP TETSUO MASUI,
76 F: Plays tennis, lives independently, told she has weak bone
 Femoral Neck Fractures In the ELDERLY What to do, when and why Frank Liporace, MD Chairman & VP, Dept of Orthopaedics Chief of Trauma & Adult Reconstruction Jersey City Medical Center / RWJ Barnabas Health
Femoral Neck Fractures In the ELDERLY What to do, when and why Frank Liporace, MD Chairman & VP, Dept of Orthopaedics Chief of Trauma & Adult Reconstruction Jersey City Medical Center / RWJ Barnabas Health
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
ANTERIOR TOTAL HIP ARTHOPLASTY
 ANTERIOR TOTAL HIP ARTHOPLASTY And Other Approaches Bill Rhodes PTA 236 Total Hip Arthoplasty (THA) Background THA, also know as Total Hip Replacement Regarded as the most valued development in orthopedics
ANTERIOR TOTAL HIP ARTHOPLASTY And Other Approaches Bill Rhodes PTA 236 Total Hip Arthoplasty (THA) Background THA, also know as Total Hip Replacement Regarded as the most valued development in orthopedics
Mini-Incision THA. What Qualifies? A Rose by Any Other Name? Todd V. Swanson, MD Las Vegas, Nevada, USA
 2 nd nd Annual Impact of Emerging Technology on Hip and Knee Reconstruction November 16, 2003 Mini-Incision THA Todd V. Swanson, MD Las Vegas, Nevada, USA A Rose by Any Other Name? Mini-Incision Surgery?
2 nd nd Annual Impact of Emerging Technology on Hip and Knee Reconstruction November 16, 2003 Mini-Incision THA Todd V. Swanson, MD Las Vegas, Nevada, USA A Rose by Any Other Name? Mini-Incision Surgery?
Patient Information for Consent
 Patient Information for Consent ER OS01 Total Hip Replacement Enhanced Recovery Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI
Patient Information for Consent ER OS01 Total Hip Replacement Enhanced Recovery Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI
Partial Knee Replacement
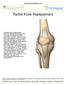 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Use Of A Long Femoral Stem In The Treatment Of Proximal Femoral Fractures: A Report Of Four Cases
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 5 Number 1 Use Of A Long Femoral Stem In The Treatment Of Proximal Femoral Fractures: A Report Of Four Cases C Yu, V Singh Citation C Yu, V Singh..
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 5 Number 1 Use Of A Long Femoral Stem In The Treatment Of Proximal Femoral Fractures: A Report Of Four Cases C Yu, V Singh Citation C Yu, V Singh..
Total Hip Replacement. Find out why Total Hip Replacement may be right for you.
 Total Hip Replacement Find out why Total Hip Replacement may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of hip anatomy, arthritis and total hip arthroplasty.
Total Hip Replacement Find out why Total Hip Replacement may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of hip anatomy, arthritis and total hip arthroplasty.
PARTIAL KNEE REPLACEMENT
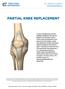 PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Total Hip Replacement in Diaphyseal Aclasis: A Case Report
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 6 Number 1 Total Hip Replacement in Diaphyseal Aclasis: A Case Report V Singh, S Carter Citation V Singh, S Carter.. The Internet Journal of
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 6 Number 1 Total Hip Replacement in Diaphyseal Aclasis: A Case Report V Singh, S Carter Citation V Singh, S Carter.. The Internet Journal of
THE RECOVERY PROCESS
 THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
Advantage Orthopaedics, P.C.
 TOTAL HIP REPLACEMENT Whether you have just begun exploring treatment options or have already decided with your orthopaedic surgeon to undergo hip replacement surgery, this booklet will help you understand
TOTAL HIP REPLACEMENT Whether you have just begun exploring treatment options or have already decided with your orthopaedic surgeon to undergo hip replacement surgery, this booklet will help you understand
Reverse Total Shoulder Replacement
 Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Reverse Total Shoulder Replacement Every year, thousands of conventional total shoulder replacements are successfully done in the United States for patients with shoulder arthritis. This type of surgery,
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up
 Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components.
 Total Hip Replacement In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components. The damaged femoral head is removed
Total Hip Replacement In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components. The damaged femoral head is removed
Fracture Surgery. Post-Operative Care. And. Rehabilitation Protocol
 PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
WHAT DO YOU THINK? 1. How many people in the United States undergo hip replacement surgery each year? a) 80,000. b) 330,000.
 1 WHAT DO YOU THINK? 1. How many people in the United States undergo hip replacement surgery each year? a) 80,000 b) 330,000 c) 650,000 2. What disease is the leading cause of disability in the U.S.? a)
1 WHAT DO YOU THINK? 1. How many people in the United States undergo hip replacement surgery each year? a) 80,000 b) 330,000 c) 650,000 2. What disease is the leading cause of disability in the U.S.? a)
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes
 The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
The Birmingham Interlocking Pelvic Osteotomy (BIPO) for Acetabular Dysplasia: 13 to 21 Year Survival Outcomes Omer Mei-Dan, MD Dylan Jewell, BSc, MSc, FRCS Tigran Garabekyan, MD Jason Brockwell, FRCSEdOrth
Strive to improve your quality of life with AMIS
 Strive to improve your quality of life with AMIS STRIVE TO IMPROVE YOUR Q The AMIS (Anterior Minimally Invasive Surgery) approach is a true intermuscular and internervous minimally invasive surgical technique.
Strive to improve your quality of life with AMIS STRIVE TO IMPROVE YOUR Q The AMIS (Anterior Minimally Invasive Surgery) approach is a true intermuscular and internervous minimally invasive surgical technique.
Total Hip Replacement Surgery
 Total Hip Replacement Surgery On this page: Overview What is Total hip replacement (THA)? Anatomy Preparing for surgery The Operation Post-Operative Possible Complications Exercise Restrictions Overview
Total Hip Replacement Surgery On this page: Overview What is Total hip replacement (THA)? Anatomy Preparing for surgery The Operation Post-Operative Possible Complications Exercise Restrictions Overview
Are You Living with. Hip Pain? MAKOplasty may be the right treatment option for you.
 Are You Living with Hip Pain? MAKOplasty may be the right treatment option for you. Hip pain shouldn t keep you from doing the things you love. Understanding Common Causes of Hip Pain If you are one of
Are You Living with Hip Pain? MAKOplasty may be the right treatment option for you. Hip pain shouldn t keep you from doing the things you love. Understanding Common Causes of Hip Pain If you are one of
The arc of pelvic motion has been shown to be as great as 70 through sit to stand activities 1 DiGioia CORR 2006
 The arc of pelvic motion has been shown to be as great as 70 through sit to stand activities 1 DiGioia CORR 2006 Overview Every patient moves differently 1 and their total hip replacement should be optimised
The arc of pelvic motion has been shown to be as great as 70 through sit to stand activities 1 DiGioia CORR 2006 Overview Every patient moves differently 1 and their total hip replacement should be optimised
Fracture involving the femoral neck is a common
 . 234. Chinese Journal of Traumatology 2010; 13(4):234-239 Comparative study of anterolateral approach versus posterior approach for total hip replacement in the treatment of femoral neck fractures in
. 234. Chinese Journal of Traumatology 2010; 13(4):234-239 Comparative study of anterolateral approach versus posterior approach for total hip replacement in the treatment of femoral neck fractures in
introduction jointunderstanding benefits of knee-replacement surgery
 introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis?
![Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis? Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis?](/thumbs/78/78456133.jpg) Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis? Diagnosis: Ceramic head fracture In the 1970 s, Boutin implemented ceramic in modern total hip arthroplasty (THA).
Case report: Pain L THR [ post THR 2 years; with history of trivial fall] Your Diagnosis? Diagnosis: Ceramic head fracture In the 1970 s, Boutin implemented ceramic in modern total hip arthroplasty (THA).
Non-Arthroplasty Hip Surgery. Javad Parvizi MD FRCS Professor of Orthopaedic Surgery
 Non-Arthroplasty Hip Surgery Javad Parvizi MD FRCS Professor of Orthopaedic Surgery Subcapital reduction osteotomy Relative lengthening of femoral neck (Perthes) AVN surgery Femoral osteotomy Trap door
Non-Arthroplasty Hip Surgery Javad Parvizi MD FRCS Professor of Orthopaedic Surgery Subcapital reduction osteotomy Relative lengthening of femoral neck (Perthes) AVN surgery Femoral osteotomy Trap door
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
Survey of Postoperative Satisfaction and Pain Following Femoral Nerve Block and On-Q Pain Pump Catheter in Total Knee Replacement.
 1 Survey of Postoperative Satisfaction and Pain Following Femoral Nerve Block and On-Q Pain Pump Catheter in Total Knee Replacement Megan Kozar Mentored by Nanette Schwann, MD 2 Abstract Total knee replacement
1 Survey of Postoperative Satisfaction and Pain Following Femoral Nerve Block and On-Q Pain Pump Catheter in Total Knee Replacement Megan Kozar Mentored by Nanette Schwann, MD 2 Abstract Total knee replacement
Patellofemoral Replacement
 Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
Patellofemoral Replacement During knee replacement surgery, damaged bone and cartilage is resurfaced with metal and plastic components. Patellofemoral replacement is a type of "partial" knee replacement
TECHNIQUE OF TISSUE-PRESERVING, MINIMALLY-INVASIVE TOTAL HIP ARTHROPLASTY USING A SUPERIOR CAPSULOTOMY
 TECHNIQUE OF TISSUE-PRESERVING, MINIMALLY-INVASIVE TOTAL HIP ARTHROPLASTY USING A SUPERIOR CAPSULOTOMY STEPHEN B. MURPHY, MD Preservation of the tissues surrounding the hip may improve hip joint stability
TECHNIQUE OF TISSUE-PRESERVING, MINIMALLY-INVASIVE TOTAL HIP ARTHROPLASTY USING A SUPERIOR CAPSULOTOMY STEPHEN B. MURPHY, MD Preservation of the tissues surrounding the hip may improve hip joint stability
Comparison of navigation accuracy in THA between the mini-anterior and -posterior approaches
 THE INTERNATIONAL JOURNAL OF MEDICAL ROBOTICS AND COMPUTER ASSISTED SURGERY Int J Med Robotics Comput Assist Surg 2009; 5: 20 25. Published online 23 December 2008 in Wiley InterScience (www.interscience.wiley.com)..226
THE INTERNATIONAL JOURNAL OF MEDICAL ROBOTICS AND COMPUTER ASSISTED SURGERY Int J Med Robotics Comput Assist Surg 2009; 5: 20 25. Published online 23 December 2008 in Wiley InterScience (www.interscience.wiley.com)..226
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training.
 Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
Optimum implant geometry
 Design Rationale Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Design Rationale Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
One- or two-stage bilateral total hip arthroplasty
 Hip One- or two-stage bilateral total hip arthroplasty A PROSPECTIVE, RANDOMISED, CONTROLLED STUDY IN AN ASIAN POPULATION S. Bhan, A. Pankaj, R. Malhotra From the All India Institute of Medical Sciences,
Hip One- or two-stage bilateral total hip arthroplasty A PROSPECTIVE, RANDOMISED, CONTROLLED STUDY IN AN ASIAN POPULATION S. Bhan, A. Pankaj, R. Malhotra From the All India Institute of Medical Sciences,
FAQ s: Hip Arthroscopy with Dr. Boyle
 AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
Total Knee Replacement
 Total Knee Replacement Learn About: How Your Knee Works Knee Related Problems Candidates for Knee Replacement Surgery What to Expect From Your Artificial Knee Preparing for Knee Replacement Your Surgery
Total Knee Replacement Learn About: How Your Knee Works Knee Related Problems Candidates for Knee Replacement Surgery What to Expect From Your Artificial Knee Preparing for Knee Replacement Your Surgery
Total Hip Replacement
 AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
