Osteoporosis is responsible for significant morbidity. Osteoporosis Therapy After Fracture in Elderly Men. Original Research
|
|
|
- Jared Snow
- 6 years ago
- Views:
Transcription
1 Original Research Osteoporosis Therapy After Fracture in Elderly Men Angela J. Shepherd, MD, Bret T. Howrey, PhD, Alvah R. Cass, MD, SM, and Gregg S. Wilkinson, PhD, MA Abstract Objective: To report the effect of osteoporosis treatment on the rate of subsequent fractures among older men after fragility fracture. Methods: Analysis of claims data of 10,608 men 65 years of age who had a fracture that occurred during Subsequent fractures, prescription drugs dispensed, procedures, therapies, and comorbidities were compared for men who received osteoporosis treatment and those who did not. Results: 4.5% of men (n = 478) received treatment. The rate of subsequent fracture was 13.5% in the treated men and 10.8% in the untreated men. Stratification by site of fracture or age at fracture did not affect results. There was no difference in number of days to subsequent fracture in the treated and untreated men. Conclusions: Few men receive treatment after an osteoporotic fracture and adherence to treatment was poor. There was no reduction in subsequent fracture with osteoporosis pharmacotherapy. The low treatment rate precludes definitive conclusions about efficacy in the clinical setting but may suggest a lack of consensus among practicing physicians about the utility of treatment in elderly men with fragility fractures. Osteoporosis is responsible for significant morbidity and mortality in men [1]. Men who have experienced a vertebral fracture have a fourfold increase in risk for subsequent fractures, and men with other fractures have a twofold increased risk for future fractures [2 5]. Antiresorptive agents are consistently associated with a 25% to 30% reduction in primary and subsequent fractures in postmenopausal women [6 11]. However, the literature is limited regarding the efficacy of antiresorptive agents for secondary prevention in men with prevalent fractures. Two studies reported good efficacy of antiresorptives for primary prevention of vertebral fractures in men with osteoporosis [12,13]. In both studies, men with pre-existing osteoporotic fractures made up approximately 50% of both treatment and control groups, with reductions of about 60% for new vertebral fractures in the treatment groups reported. More recently, a 24-month double-blind, placebo-controlled study of men with primary or hypogonadism-associated osteoporosis reported a 67% reduced risk of new morphometric vertebral fracture among men receiving the intervention (zoledronic acid once yearly). Because of the small number of fractures, neither clinical vertebral fractures nor nonvertebral fractures were reduced to a statistically significant degree [14]. In a randomized controlled trial of secondary fracture prevention after hip fracture in a population that included 75% women and 25% men, an overall 35% risk reduction was reported in patients treated with zoledronic acid. The rates of secondary vertebral and nonvertebral fractures were reduced significantly [8]. Despite the availability and likely efficacy of antiresorptive agents in the treatment of osteoporotic-related fractures, few men receive treatment after a low-impact fracture [15 17]. The objective of our study was to measure treatment rates and the effect of osteoporotic therapy on the rate of subsequent fracture among men after low-impact fracture. METHODS Data Source We conducted our study using a large US claims and integrated laboratory database that included commercially insured patients from all 50 states (Clinformatics Data Mart, OptumInsight Life Sciences). These data include de-identified patients and physicians and include claims for inpatient and outpatient care, pharmaceuticals, and durable medical equipment for 13 million annual lives. Study Population First we identified men aged 65 years and older who were enrolled between 1 January 2001 and 31 Decem- From the Department of Family Medicine, The University of Texas Medical Branch, Galveston, TX. Vol. 20, No. 7 July 2013 JCOM 303
2 Osteoporosis Therapy ber Because we examined men 65 and older, our sample included men with primary health insurance coverage through commercial insurance and those on Medicare who participated in supplemental plans. Next, we identified men who had an index fracture during the study period (n = 28,662) who were also continuously enrolled for at least 6 months prior to and 6 months following the index fracture. Fractures were determined based on the reported International Classification of Diseases, 9th Revision (ICD-9-CM) codes on the inpatient or outpatient claim. (See Appendix for a complete listing of IDC-9-CM codes used.) For the purposes of this study, fracture was defined as any closed fracture, except of the skull, face, finger, ankle, or toe, that appeared as a billed diagnosis during the study period with no claim for a fracture in the preceding 6 months. In the multicenter Study of Osteoporotic Fractures of 9704 nonblack women 65 years of age and older, these types of fractures (wrist, foot, humerus, intertrochanteric region of the hip, rib, toe, leg, pelvis, hand, clavicle and vertebral body) were found to be significantly related to reduced appendicular bone mass [18]. We excluded men who received care in hospice, skilled nursing, or rehabilitation facilities because pharmaceutical claims information was not available during those periods. In addition, we excluded any men diagnosed with co-existing cancer codes associated with bony metastasis in the 6 months prior to the index fracture [19] and those whose index fracture was associated with an ICD-9-CM E-code suggesting high-impact trauma (eg, transportation accidents and falls from more than a standing height). The E-code list is available upon request. We also excluded men who had multiple fractures in different body parts or in the same area within 1 week of the index fracture, as these diagnoses are suggestive of high-impact trauma. Finally, we excluded men who had a claim for osteoporosis treatment in the 6 months preceding the index fracture. The final cohort was 10,608 men: 478 treated and 10,130 untreated. We followed treated and untreated men from the date of the index fracture. Follow-up ended on the date of diagnosis of a subsequent fracture, disenrollment, or the end of the study (31 December 2005). Dependent Variable Our main outcome was a subsequent fracture following the index fracture. Subsequent fractures were determined using the same criteria as those used for index fractures. Subsequent fractures whose ICD-9-CM codes (first 4 digits) did not match the index fracture were considered true second fractures. In cases of vertebral fractures, if the index fracture was not otherwise classifiable by location as lumbar, thoracic, or cervical, then all subsequent claims for vertebral fractures were excluded due to inability to definitively adjucate new fractures versus claims relating to the index vertebral fracture. To verify claims associated with second fractures as unique and not follow up claims relating to the index fracture, fracture claims at the same site were required to have an associated Current Procedural Terminology (CPT) code describing treatment of the fracture in order to be considered subsequent fracture. Physician adjudication of subsequent fracture claims was done at 4 key points in the algorithm (Figure 1). Two family physicians (Cass and Shepherd) independently reviewed claims to determine accuracy of allocation into True subsequent fracture or Not subsequent fracture groups: (1) 100 cases of subsequent fracture claims within 90 days of index fracture were reviewed, (2) all 21 claims of subsequent fractures more than 90 days from the index fracture with the same diagnostic codes as index fracture and CPT codes were reviewed, (3) 100 claims of subsequent fractures more than 90 days with the same diagnostic codes as index fracture without CPT codes were reviewed, and (4) all 71 claims with nonspecific vertebral codes either as index or subsequent fracture. Each adjucation confirmed the likelihood that the fractures were correctly identified. The sensitivity of medical service claims to correctly classify fracture has been reported as 85%, with a range of 25% for thorax (rib or sternum) fractures to 97% for hip fractures. Underreporting is not common as claims are linked to physician payment and false-positive reporting is also unlikely due to the high penalty for fraudulent claims [20]. Covariates Our main independent variable was a filled prescription for an osteoporosis treatment, as determined by the presence of a prescription in the pharmacy claims. We considered treatment to be any bisphosphonate (alendronate, etidronate, ibandronate, risedronate, or zoledronic acid), calcitonin, or teriparatide. Using an intention-to-treat model, men were considered treated if the pharmacy claims indicated that a prescription for osteoporosis treatment was filled at least once in the 6 months following the index fracture. Men whose treatment was initiated 304 JCOM July 2013 Vol. 20, No. 7
3 Original Research 4 digits Dx codes match n = 1441 CPT codes n = 21* No CPT codes n = 1420* Subsequent Fx No Fx > 90 days n = 2645 Specific Fx Codes n = 1133 Subsequent Fx With subsequent Fx codes n = 5936 No match N = 1204 Nonspecific vertebral codes n = 71* Unconfirmed Fx n = 66 No Fx Men 65+ cohort (n = 10,608) 90 days n = 3291* No Fx Confirmed Fx n = 5 Subsequent Fx No Fx codes n = 4672 No Fx Figure 1. Steps of data extraction for subsequent fracture. Dx = diagnosis; Fx = fracture.* = adjudication points. after the subsequent fracture were not considered treated. The duration of therapy was calculated by counting the number of prescriptions dispensed from the start of therapy to the subsequent fracture date, date of disenrollment, or end of study date. Duration of treatment was modeled as a continuous variable. Changes from one prescription for osteoporosis treatment to another were considered as continuous for analysis of treatment duration. We adjusted for potential confounders: age, year of index fracture, index fracture site, osteoporosis diagnosis, risk of secondary osteoporosis, tertiary tricyclic antidepressants, benzodiazepines, selective serotonin reuptake inhibitors, type 2 diabetes, COPD/asthma, and depressive disorders. Additional adjustments were made for indicators of frailty or fall risk: procedure claims for physical therapy and mobility procedures, durable medical equipment, diagnoses of abnormal gait, syncope and debility. Finally, we adjusted for medications associated with falling or decreased bone density: hydrocodone/ codeine containing analgesics, prednisone and proton pump inhibitors. Statistical Analysis We first generated nonparametric Kaplan-Meier curves to examine the differences between the treated and untreated groups in probability of subsequent fracture over time. We then performed semiparametric Cox proportional hazards models to estimate the difference in the hazard of a subsequent fracture for the treated and untreated groups. The number of days from index fracture to subsequent fracture was considered the primary endpoint. Men were censored at the end of the study period or end of their enrollment in the insurance plan. Models were first run for the whole sample and then stratified by index fracture site: hip, spine, and other. Initial models included only the treatment variable. The next set of Vol. 20, No. 7 July 2013 JCOM 305
4 Osteoporosis Therapy models added age, and the third set of models added the remaining covariates. The proportionality assumption was tested through examination of scaled Schoenfeld residuals and was found not to be violated [21]. RESULTS A total of 28,662 men had a study-defined fracture between 2001 and After exclusions of concurrent users of osteoporosis treatment, removal of men who did not have adequate time in the study, removal of men involved in accidents, with cancer diagnoses that can metastasize to bone and multiple concurrent fractures suggestive of high trauma, the final sample included 10,608 men. Of that group, 478 men received treatment within the first 6 months after fracture and 10,130 men did not receive treatment. Table 1 shows the characteristics of the study population in the 6 months prior to index fracture. Overall, the average age of the men at index fracture was 75 years. The proportion of men who received treatment was 4.51%. Mean number of years of continuous enrollment for treated and untreated men was 4.4 years, with a standard deviation of 1.6 years. The diagnosis of osteoporosis was higher in the treated group (11%) compared with the untreated group (2.5%). Treated men were more likely to have filled prescriptions for antidepressants (tricyclics and selective serotonin reuptake inhibitors), narcotic analgesics, proton pump ihibitors and oral prednisone. No differences were found between the treated and untreated men for most of the chronic conditions examined. COPD was the most notable exception. 28% of the treated men had COPD compared to 16% of the untreated men. Arthropathies, syncope, debility and depression were also slightly more prevalent in the treated men. A total of 1159 men (10.92%) were determined to have a subsequent fracture. The average time from index to second fracture was 435 days for the treated group and 403 days for the untreated group. Treated men filled the initial prescription 55 to 59 days post-fracture; mean length of treatment during follow-up was 478 days (16 months): 491 days (16.3 months) in the treated men with subsequent fracture and 380 days (12.7 months) in the treated men without subsequent fracture. 24% of the men who had a claim for the initial prescription had no more osteoporosis treatment prescription claims after the first prescription filling. Ad hoc analyses of the men who sustained a subsequent fracture (not included in tabled results) revealed that in the 6 months preceeding the subsequent fracture, these men were three times more likely to have received benzodiazepines (9.3% vs 3.4%) and twice as likely to have received narcotic analgesics (23% vs 13%) or prednisone prescriptions (6% vs 2.7%). Cox proportional hazard ratios of subsequent fracture by index fracture site are presented in Table 2. Hazard ratios for subsequent fractures tended to be greater for men with vertebral index fractures, but there was no difference in hazard ratios between treated and untreated men in crude, age-adjusted or fully adjusted models. Stratification of subsequent fracture by age (5-year intervals) resulted in hazard ratios for men 65 to 69 years of age of 0.80, (95% CI, ), for men 70 to 74 years of age of 1.15, (95% CI, ), for men 75 to 79 years of age of 1.18, (95% CI, ), and for men 80 years of age or older of 0.96 (95% CI, ). Figure 2 shows the time to subsequent fracture for treated vs. untreated men. There was no difference in the number of days to subsequent fracture between the treated and untreated group as shown by the Kaplan-Meier curves. DISCUSSION This report examined the effect of osteoporosis treatment following an index fracture on the occurrence of subsequent fracture in insured older men in the United States. We found very low treatment rates (4.5%) and suboptimal adherence, with only 76% refilling the prescription after initiation of therapy. In the limited number of men who initiated treatment, the results of this study failed to demonstrate a reduction in subsequent fractures (all sites). There were 13.6% subsequent fractures in treated men vs 10.8% in untreated men. Limitations Our study has numerous limitations, including the small number of men who received treatment and poor compliance rate, which limits the power to detect differences between treated and untreated men. A large cohort study by Siris et al reported that a sample size of more than 30,000 compliant and noncompliant individuals was needed to detect a difference in fracture rates of 10% and 8.5% [24]. Regarding treatment biases, several characteristics of our treated group suggest that these men may have been more frail, more likely to fall, and more prone to fracture than the untreated men. Men in the treated group were 306 JCOM July 2013 Vol. 20, No. 7
5 Original Research Table 1. Characteristics of Study Population During 6 Months Prior to Index Fracture Treatment No Treatment Total n % n % n Study subjects Mean age at index fracture, yr Number of days enrolled ± SD Osteoporosis diagnosis Risk of secondary osteoporosis by diagnosis* Fall-risk diagnosis Medications associated with increased risk Tertiary tricyclic antidepressant Benzodiazepine Selective serotonin reuptake inhibitor Narcotic analgesics Proton pump inhibitors Oral prednisone Chronic medical conditions Heart disease Hypertension Hyperlipidemia COPD/asthma Arthropathies Osteoarthritis Syncope Abnormal gait Debility Depressive disorders Diabetes type Other Frailty index Durable medical equipment *Includes hyperthyroidism, hyperparathyroidism, Cushing s syndrome, cirrhosis, chronic kidney disease, and testicular hypofunction. Includes Parkinsonism, rheumatoid arthritis, osteoarthritis, dementia, alcoholism, type 1 diabetes mellitus, and stroke. Includes procedural codes for mobility issues (G0151,A0130, A0425, S0209, S5130, S9131, T1019, T1021) and physical therapy (97001, 97010, 97012, 97014, 97035, 97110, 97112, 97140, 97530, G0283). p value significant at < statistically more likely to have a pre-existing diagnosis of osteoporosis, a major risk factor for fracture. In addition, men in the treated group were more likely to be taking medications that adversely affect bone density, ie, selective serotonin reuptake inhibitors [25 29], proton pump inhibitors [30 34], and prednisone [35,36]. Treated men were also more likely to be on medications associated with falling, such as tricyclic antidepressants, benzodiazepines, and narcotic analgesics [26,28,29,37]. Finally, men in the treated group were more likely to be diagnosed with debility, which is synonymous with at least a temporary state of frailty. However, after accounting for these observed differences in the final adjusted model, we detected no apparent benefit of treatment fol- Vol. 20, No. 7 July 2013 JCOM 307
6 Osteoporosis Therapy Table 2. Cox Proportional Hazard Ratios Modeling the Association of Treatment with Hazard of Subsequent Fracture Site of Index Fracture n Subsequent Fractures Person- Years Hazard Ratio (95% Confidence Interval) Treatment Only Age Adjusted Fully Adjusted* Hip ( ) 1.24 ( ) 1.18 ( ) Spine ( ) 1.48 ( ) 1.47 ( ) Other ( ) 1.06 ( ) 0.94 ( ) Overall 10, , ( ) 1.17 ( ) 1.14 ( ) *Models adjusted for osteoporosis, fall risk diagnosis, tricyclic antidepressants, benzodiazepines, SSRIs, hydrocodone, PPIs, prednisone, heart disease, hypertension, hyperlipidemia, COPD, arthropathy, osteoarthritis, syncope, abnormal gait, debility, depression, frailty, durable medical equipment. lowing an osteoporotic fracture. While the hazard ratios declined in the final adjusted model, the overall change in magnitude suggests that the impact of the factors that may have affected treatment decisions was small. Duration of treatment is also an important factor in prevention; studies in osteoporotic women have shown that about 15 months of osteoporosis treatment is required before any difference is seen in hip fracture rates between treated and untreated women [38]. The average length of treatment in our study was 16 months. Other limitations include those inherent in claims data research. Residual confounding is a potential limitation of claims data research. We took steps to minimize this by restricting the entire cohort to men who had sustained an index fragility fracture, making treated and untreated men more comparable. We also required untreated men to be in the same period of cohort entry as treated men. Administrative data also limits information on ethnicity/race, use of over-the-counter agents such as calcium or vitamin D, family history, smoking, prior fractures not contained in the record, weight, results of bone mineral density measurements or radiographs, height, and body mass index, and frailty. Again, we attempted to manage many of these limitations by requiring all men to have had already sustained a fragility fracture; however, it is not possible to estimate how comparable the 2 groups were on unreported variables. Finally, we attempted to minimize the lack of ability to quantify frailty directly by examining CPT codes for physical therapy, durable medical equipment for walkers and canes, and diagnosis codes for abnormal gait, syncope and debility as indirect measures of frailty. Our study population was limited to insured men 65 years of age and older. In addition, men who received care in an inpatient skilled nursing facility or nursing home were necessarily excluded due to lack of prescriptive information needed to determine treatment status. Because Medicare is available at age 65, our study findings are most relevant to men 65 years of age with Medicare and supplementary commercial health insurance. Claims data may contain coding errors, resulting in misclassification of fractures. We attempted to minimize this type of error by having 2 physicians adjudicate approximately 300 cases of subsequent fracture claims. Claims with codes that were nonspecific (for either index or subsequent vertebral fracture) were excluded because it was not possible to ascertain whether the later claims were related to the index vertebral fracture or a second vertebral fracture. This requirement may have resulted in underestimating subsequent vertebral fractures. Finally, a limitation in our study is the lack of ability to control disenrollment or dropout from the database. One of the challenges encountered in working with private insurance data for men over the age of 65 is disenrollment due to Medicare eligibility. It is unclear to what extent such disenrollment impacts both the numerator and denominator. However, assuming the rate of dropout is relatively uniform among the treated and untreated men, calculations based on such data are stable. In addition, because this study utilized prescription fills that were not limited to the Medicare spending limit (AKA donut hole ), the results maintain high specificity. Comparison with Other Studies Our findings are similar to a report by Cree in a cohort of hip fracture patients made up of 26% men. In their report of 356 treated patients during , treatment did not change the rate of subsequent hip fracture rates 308 JCOM July 2013 Vol. 20, No. 7
7 Original Research Probability 0.50 Not Treated Treated p = No. of Days Figure 2. Kaplan-Meier plot of second fracture-free survival. Survival time starts (0) at day 90 following the index fracture. (6% vs. 4%) with a reported adherence rate of 62% at 1.5 years [39]. All men who received treatment in the study received bisphosphonates. Like ours, their study took place in a real-world setting and had low use of osteoporosis treatment. The fact that neither study was able to show differences when studying small numbers (< 500) patients may likely reflect power issues. Our findings did not concur with those from 3 randomized controlled trials looking at primary prevention of fractures in men. In these studies (which included approximately 50% of men with prior osteoporotic fractures), alendronate treatment resulted in a 60% reduction for new vertebral fractures. New nonvertebral fractures were not reduced significantly [12,13]. The men in both controlled trials were considerably younger (57 years [12] and 63 years [13]) than those in our study (75 years). In these controlled trials, compliance was not an issue, nor was length of follow-up time, as all men were required to have at least 2 years of follow-up with monitored treatment. Our study was done at a time when zoledronic acid was rarely used for men, but in the 2007 report of the HORIZON Recurrent Fracture Trial involving 2127 persons (508 men) with hip fracture, Lyles et al reported a significant (35%) risk reduction for any new clinical fracture with zoledronic acid [8]. In a 2013 report on primary prevention of fracture by Boonen et al involving 1199 men (574 in the intention to treat group), zolendronic acid was associated with a 67% risk reduction in morphometric vertebral fractures after 2 years; reductions were also reported in men with clinical vertebral or nonvertebral fractures, but these reductions did not reach significance due to the small overall number of fractures [14]. These studies suggests that treatment with intravenous zoledronic acid and 100% compliance, we can expect to see some reduction in subsequent fractures. Conclusions The current claims data study of 10,608 elderly men diagnosed with a fragility fracture failed to show significant reductions in fractures after treatment with (mostly) oral bisphosphonates; this lack of significance may be due to insufficient power to detect differences due to small numbers of treated men (4.5%) and a relatively rare event as the endpoint (subsequent fracture). The lack of treatment benefit observed in our study may have been influenced by the advanced age and cormorbidity burden; the low treatment rates, suboptimal compliance, and length of duration of treatment prior to a subsequent fracture likely influenced results. To illustrate this point, the mean time to treatment was about 60 days; the mean time to a Vol. 20, No. 7 July 2013 JCOM 309
8 Osteoporosis Therapy subsequent fracture was 435 days. The intervening time interval may have been too short to realize the benefit of treatment. Lack of treatment post-fracture may carry adverse health consequences for patients as well as increased health care costs for the health care system. If patients are to benefit from the fracture risk reductions reported in clinical trials, clinicians may want to consider yearly intravenous therapy and collaborate with researchers to discover novel ways to increase compliance with long-term oral medications. Further large scale studies are needed if we are to better understand how to achieve a reduction of subsequent nonvertebral fractures in elderly men. Acknowledgment: We would like to thank Karen Pierson, Assistant Director of Research Support Services, for her assistance with data management. Corresponding author: Angela J. Shepherd, MD, Dept. of Family Medicine, The University of Texas Medical Branch, 301 University Blvd., Galveston, TX 77555, ajshephe@ utmb.edu. Funding/support: This study was conducted with the support of the Institute for Translational Sciences at the University of Texas Medical Branch, supported in part by a Clinical and Translational Science Award (UL1TR000071) from the National Center for Advancing Translational Sciences, National Institutes of Health. Financial disclosures: None. Author contributions: conception and design, AJS, BH, ARC, GSW; analysis and interpretation of data, AJS, BH, ARC, GSW; drafting of article, AJS, BH, GSW; critical revision of the article, AJS, BH, ARC, GSW; statistical expertise, BH, ARC, GSW; obtaining of funding, GSW; collection and assembly of data, AJS, BH. References 1. Roerholt C, Eiken P, Abrahamsen B. Initiation of antiosteoporotic therapy in patients with recent fractures: a nationwide analysis of prescription rates and persistence. Osteoporos Int 2009;20: Klotzbuecher C, Ross P, Landsman P, et al. Patients with prior fractures have an increased risk of future fractures: a summary of the literature and statistical synthesis. J Bone Miner Res 2000;15: Elliot-Gibson V, Bogoch ER, Jamal SA, et al. Practice patterns in the diagnosis and treatment of osteoporosis after a fragility fracture: a systematic review. Osteoporos Int 2004;15: Haentjens P, Autier J, Collins B, et al. Colles fracture, spine fracture, and subsequent risk of hip fracture in men and women. A meta-analysis. J Bone Joint Surg Am 2003;85- A(10): Kanis J, Johnell P, De Laet C, et al. A meta-analysis of previous fracture and subsequent fracture risk. Bone 2004;35: Harris S, Watts N, Genant H, et al. Effects of risedronate treatment on vertebral and nonvertebral fractures in women with postmenopausal osteoporosis: a randomized controlled trial. JAMA 1999;282: Reginster J, Minnett H, Sorensen O, et al. Randomized trial of the effects of Risedronate on vertebral fractures in women with established postmenopausal osteoporosis. Osteoporosis Int 2000;11: Lyles K, Colon-Emeric C, Magaziner J, et al. Zoledronic acid and clinical fractures and mortality after hip fracture. N Engl J Med 2007;357: Black D, Delmas P, Eastell R, et al. Once-yearly zolendronic acid for treatment of postmenopausal osteoporosis. N Engl J Med 2007;356: Black D, Cummings S, Karpf D, et al. Randomised trial of effect of alendronate on risk of fracture in women with existing vertebral fractures. Lancet 1996;347: Morin S, Rahme E, Behlouli H, et al. Effectiveness of antiresoprtive agents in the prevention of recurrent hip fractures. Osteoporos Int 2007;18: Ringe J, Faber H, Farahmand P, et al. Efficacy of risedronate in men with primary and secondary osteoporosis: results of a 1-year study. Rheumatol Int 2006;26: Orwoll E, Ettinger M, Weiss S, et al. Alendronate for the treatment of osteoporosis in men. N Engl J Med 2000;343: Boonen S, Reginster J, Kaufman J, et al. Fracture risk and zoledronic acid therapy in men with osteoporosis. N Engl J Med 2012;367: Kiebzak G, Beinart G, Perser K, et al. Undertreatment of osteoporosis in men with hip fracture. Arch Intern Med 2002;162: Feldstein A, Nicholson G, Orwoll E, et al. The near absence of osteoporosis treatment in older men with fractures. Osteoporosis Int 2005;16: Shepherd A, Wilkinson G, Ray L, et al. Treatment for older men with fractures. Osteoporos Int 2012;23: Seeley D, Browner W, Nevitt M, et al. Which fractures are associated with low appendicular bone mass in elderly women? The Study of Osteoporotic Fractures Research Group. Ann Intern Med 1991;115: Buck C ICD-9 CM for physicians. 1st ed. Saunders; Tamblyn R, Reid T, Mayo N, et al. Using medical services claims to assess injuries in the elderly: sensitivity of diagnostic and procedure codes for injury ascertainment. J CLin Epidemiol 2000;53: Singer J, Willet J. Regression diagnostics. In: Applied longitudinal data analysis: modeling change and event occurrence. New York: Oxford University Press; 2003: Orwoll E, Bevan L, Phipps K. Determinants of bone miner- 310 JCOM July 2013 Vol. 20, No. 7
9 Original Research Appendix. ICD-9-CM codes Code Description Code Description Spine 805 VERTEBRL FX W/O CORD INJ FX C6 VERTEBRA-CLOSED FX CERVICAL VERTEBRA-CL FX C7 VERTEBRA-CLOSED FX CERVICAL VERT NOS-CL FX MULT CERVICAL VERT-CL FX C1 VERTEBRA-CLOSED FX DORSAL VERTEBRA-CLOSE FX C2 VERTEBRA-CLOSED FX LUMBAR VERTEBRA-CLOSE FX C3 VERTEBRA-CLOSED FX SACRUM/COCCYX-CLOSED FX C4 VERTEBRA-CLOSED VERTEBRAL FX NOS-CLOSED FX C5 VERTEBRA-CLOSED Hip FX FEMUR INTRCAPS NOS-CL PERTROCHANTERIC FX-CLOS FX UP FEMUR EPIPHY-CLOS TROCHANTERIC FX NOS-CLOS FX FEMUR, MIDCERVIC-CLOS INTERTROCHANTERIC FX-CL FX BASE FEMORAL NCK-CLOS SUBTROCHANTERIC FX-CLOSE FX FEMUR INTRCAPS NEC-CL FX NECK OF FEMUR NOS-CL Other FX OF RIB-CLOSED FX HUMERUS NOS-CLOSED FX RIB NOS-CLOSED FX HUMERUS SHAFT-CLOSED FX ONE RIB-CLOSED FX LOWER HUMERUS-CLOSED FX TWO RIBS-CLOSED FX LOWER HUMERUS NOS-CL FX THREE RIBS-CLOS SUPRCONDYL FX HUMERUS-CL FX FOUR RIBS-CLOSE FX HUMER, LAT CONDYL-CL FX FIVE RIBS-CLOSE FX HUMER, MED CONDYL-CL FX SIX RIBS-CLOSED FX HUMER, CONDYL NOS-CL FX SEVEN RIBS-CLOS FX LOWER HUMERUS NEC-CL FX EIGHT/MORE RIB-CLOSED FX UPPER RADIUS/ULNA-CL FX MULT RIBS NOS-CLOSED FX UPPER FOREARM NOS-CL 808 PELVIC FX FX OLECRAN PROC ULNA-CL FX ACETABULUM-CLOS FX CORONOID PROC ULNA-CL FX OF PUBIS-CLOSED MONTEGGIA'S FX-CLOSED FX OF ILIUM-CLOSED FX UPPER ULNA NEC/NOS-CL FX ISCHIUM-CLOSED FX RADIUS HEAD-CLOSED PELVIC FX NOS-CLOS FX RADIUS NECK-CLOSED FX CLAVICLE-CLOSED FX UP RADIUS NEC/NOS-CL FX CLAVICLE NOS-CLOSED FX UP RADIUS W ULNA-CLOS FX CLAVICLE SHAFT-CLOSED FX RADIUS/ULNA SHAFT-CL FX CLAVICL, ACROM END-CL FX SHAFT FOREARM NOS-CL FX UPPER HUMERUS-CLOSED FX RADIUS SHAFT-CLOSED Appendix Data FX UP Collection END HUMERUS Tool NOS-CL for VAP in Pediatric Post-Acute Care (continued) FX ULNA SHAFT-CLOSED FX SURG NCK HUMERUS-CLOS FX SHAFT RAD W ULNA-CLOS FX ANATOM NCK HUMERUS-CL FX LOWER RADIUS/ULNA-CL Code Description Code Description FX GR TUBEROS HUMERUS-CL FX LOWER FOREARM NOS-CL FX UPPER HUMERUS NEC-CL COLLES' FX-CLOSED FX HUMERUS SHAFT/NOS-CL Other FX DISTAL RADIUS NEC-CL FX DISTAL ULNA-CLOSED FX FEMUR SHAFT/NOS-CLOSE FX LOW RADIUS W ULNA-CL FX FEMUR NOS-CLOSED FX RADIUS/ULNA NOS-CLOSE FX FEMUR SHAFT-CLOSED FX FOREARM NOS-CLOSED FX LOWER END FEMUR-CLOSE FX RADIUS NOS-CLOSED FX LOW END FEMUR NOS-CL FX ULNA NOS-CLOSED FX FEMORAL CONDYLE-CLOSE FX RADIUS W ULNA NOS-CL FX LOW FEMUR EPIPHY-CLOS FX CARPAL BONE NOS-CLOSE SUPRACONDYL FX FEMUR-CL FX NAVICULAR, WRIST-CLOS FX LOW END FEMUR NEC-CL FX LUNATE, WRIST-CLOSED FX UPPER END TIBIA-CLOSE FX TRIQUETRAL, WRIST-CL FX UPPER END FIBULA-CLOS FX PISIFORM-CLOSED FX UP TIBIA W FIBULA-CL FX TRAPEZIUM BONE-CLOSED FX SHAFT TIB/FIB-CLOSED FX TRAPEZOID BONE-CLOSED FX TIBIA/FIBULA NOS-CLOS FX CAPITATE BONE-CLOSED FX CALCANEUS-CLOSE FX HAMATE BONE-CLOSED FX TARSL/METATARS NEC-CL FX CARPAL BONE NEC-CLOSE FX FOOT BONE NOS-CLOSED FX METACARPAL NOS-CLOSED FX ASTRAGALUS-CLOSED FX 1ST METACARP BASE-CL FX NAVICULAR, FOOT-CLOS FX METACARP BASE NEC-CL FX CUBOID-CLOSED FX METACARPAL SHAFT-CLOS FX CUNEIFORM, FOOT-CLOS FX METACARPAL NECK-CLOSE FX METATARSAL-CLOSED MULT FX METACARPUS-CLOSE FX FOOT BONE NEC-CLOSED FX ARM MULT/NOS-CLOSED FX LOWER LIMB NEC-CLOSED FX ARMS W RIB/STERNUM-CLOSED Vol. 20, No. 7 July 2013 JCOM 311
10 Osteoporosis Therapy al density in older men. Osteoporosis Int 2000;11: Ringe J, Dorst A, Faber H, et al. Alendronate treatment of established primary osteoporosis in men: 3-year results of a prospective, comparative, two-arm study. Rheumatol Int 2004;24: Siris E, Harris S, Rosen C, et al. Adherence to bisphosphonate therapy and fracture rates in osteoporotic women: relationship to vertebral and nonvertebral fractures from 2 US claims databases. Mayo Clinic Proc 2006;81: Richards J, Papaloannou A, Adachi J, et al. Effect of selective serotonin reuptake inibitors on the risk of fracture. Arch Intern Med 2007;167: Vestergaard P, Rejnmark L, Mosekilde L. Selective serotonin reuptake inhibitors and other antidepressants and risk of fracture. Calcif Tissue Int 2008;82: Ziere G, Dieleman J, van der Cammen T, et al. Selective serotonin reuptake inhibiting antidepressants are associated with an increased risk of nonvertebral fractures. J Clin Psychopharmacol 2008;28: Bolton J, Metge C, Lix L, et al. Fracture risk from psychotropic medications. J Clin Psychopharmacol 2008;28: Lewis C, Ewing S, Taylor B, et al. Predictors of non-spine fracture in elderly men: the MrOS study. J Bone Mineral Res 2007;22: Corley D, Kubo A, Zhao W, et al. Proton pump inhibitors and histamine-2 receptor antagonists are associated with hip fractures among at-risk patients. Gastroenterology 2010;139: FDA Drug Safety Communication. Possible increased risk of fractures of the hip, wrist, and spine with the use of proton pump inhibitors. Available from: drugs/drugsafety/postmarketdrugsafetyinformationforpatientsandproviders/ucm htm. 32. Kaye J, Jick H. Proton pump inhibitor use and risk of hip fractures in patients without major risk factors. Pharmacotherapy 2008;28: Kwok C, Yeong J, Loke YK. Meta-analysis: Risk of fractures with acid-suppressing medication. Bone 2011;48: Yu E, Bauer S, Bain P, Bauer D. Proton pump inhibitors and risk of fractures: A meta-analysis of 11 international studies. Am J Med 2011;124: American College of Rheumatology Ad Hoc Committee on Glucocorticoid-Induced Osteoporosis. Recommendations for the prevention and treatment of glucocorticoid-induced osteoporosis: 2001 update. Arthritis Rheum 2001;44: Eustice C, Eustice R. The facts of corticosteroids (Steroids) ]; Available from com/cs/steroids/a/corticosteroids_2.htm. 37. Vestergaard P, Rejnmark L, Mosekilde L. Anxiolytics, sedatives, antidepressants, neuroleptics and the risk of fracture. Osteoporos Int 2006;17: McClung M, Geusens P, Miller P, et al. Effect of risedronate on the risk of hip fracture in elderly women. N Engl J Med 2001;344: Cree M, Juby A, Carriere K. Mortality and morbidity associated with osteoporosis drug treatment following hip fracture. Osteoporos Int 2003;14: Copyright 2013 by Turner White Communications Inc., Wayne, PA. All rights reserved. 312 JCOM July 2013 Vol. 20, No. 7
CASE 1 WHY IS IT IMPORTANT TO TREAT? FACTS CONCERNS
 4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
Efficacy of risedronate in men with primary and secondary osteoporosis: results of a 1-year study
 Rheumatol Int (2006) 26: 427 431 DOI 10.1007/s00296-005-0004-4 ORIGINAL ARTICLE J. D. Ringe Æ H. Faber Æ P. Farahmand Æ A. Dorst Efficacy of risedronate in men with primary and secondary osteoporosis:
Rheumatol Int (2006) 26: 427 431 DOI 10.1007/s00296-005-0004-4 ORIGINAL ARTICLE J. D. Ringe Æ H. Faber Æ P. Farahmand Æ A. Dorst Efficacy of risedronate in men with primary and secondary osteoporosis:
Chapter 5 Osteoporosis and Bone Health
 Chapter 5 Osteoporosis has been called the silent disease because it typically progresses without symptoms until a fracture occurs. 1 Osteoporosis is age-related and characterized by low bone mass due
Chapter 5 Osteoporosis has been called the silent disease because it typically progresses without symptoms until a fracture occurs. 1 Osteoporosis is age-related and characterized by low bone mass due
Disclosures. Diagnostic Challenges in Osteoporosis: Whom To Treat 9/25/2014
 Disclosures Diagnostic Challenges in Osteoporosis: Whom To Treat Ethel S. Siris, MD Columbia University Medical Center New York, NY Consultant on scientific issues for: AgNovos Amgen Eli Lilly Merck Novartis
Disclosures Diagnostic Challenges in Osteoporosis: Whom To Treat Ethel S. Siris, MD Columbia University Medical Center New York, NY Consultant on scientific issues for: AgNovos Amgen Eli Lilly Merck Novartis
Treatments for Osteoporosis Expected Benefits, Potential Harms and Drug Holidays. Suzanne Morin MD FRCP FACP McGill University May 2014
 Treatments for Osteoporosis Expected Benefits, Potential Harms and Drug Holidays Suzanne Morin MD FRCP FACP McGill University May 2014 Learning Objectives Overview of osteoporosis management Outline efficacy
Treatments for Osteoporosis Expected Benefits, Potential Harms and Drug Holidays Suzanne Morin MD FRCP FACP McGill University May 2014 Learning Objectives Overview of osteoporosis management Outline efficacy
Osteoporosis/Fracture Prevention
 Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Chapter 8 The Skeletal System: The Appendicular Skeleton. Copyright 2009 John Wiley & Sons, Inc.
 Chapter 8 The Skeletal System: The Appendicular Skeleton Appendicular Skeleton It includes bones of the upper and lower limbs Girdles attach the limbs to the axial skeleton The pectoral girdle consists
Chapter 8 The Skeletal System: The Appendicular Skeleton Appendicular Skeleton It includes bones of the upper and lower limbs Girdles attach the limbs to the axial skeleton The pectoral girdle consists
SKELETAL SYSTEM 206. AXIAL SKELETON 80 APPENDICULAR SKELETON 126 (see Figure 6.1) Clavicle. Clavicle. Pectoral girdles. Scapula. Scapula.
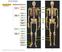 SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 126 (see Figure 6.1) Pectoral girdles 4 Clavicle Scapula 2 2 Clavicle Scapula Humerus 2 Humerus Upper limbs 60 Radius 2 Ulna Carpal bones Metacarpal
SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 126 (see Figure 6.1) Pectoral girdles 4 Clavicle Scapula 2 2 Clavicle Scapula Humerus 2 Humerus Upper limbs 60 Radius 2 Ulna Carpal bones Metacarpal
nogg Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK
 nogg NATIONAL OSTEOPOROSIS GUIDELINE GROUP Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK Produced by J Compston, A Cooper,
nogg NATIONAL OSTEOPOROSIS GUIDELINE GROUP Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK Produced by J Compston, A Cooper,
10/12/2010. Upper Extremity. Pectoral (Shoulder) Girdle. Clavicle (collarbone) Skeletal System: Appendicular Skeleton
 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum (Sternoclavicular
Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum (Sternoclavicular
Module 5 - Speaking of Bones Osteoporosis For Health Professionals: Fracture Risk Assessment. William D. Leslie, MD MSc FRCPC
 Module 5 - Speaking of Bones Osteoporosis For Health Professionals: Fracture Risk Assessment William D. Leslie, MD MSc FRCPC Case #1 Age 53: 3 years post-menopause Has always enjoyed excellent health with
Module 5 - Speaking of Bones Osteoporosis For Health Professionals: Fracture Risk Assessment William D. Leslie, MD MSc FRCPC Case #1 Age 53: 3 years post-menopause Has always enjoyed excellent health with
What is Osteoporosis?
 What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
Prescribing of anti-osteoporotic therapies following the use of Proton Pump Inhibitors in general practice
 Prescribing of anti-osteoporotic therapies following the use of Proton Pump Inhibitors in general practice B. McGowan, K. Bennett, J. Feely Department of Pharmacology & Therapeutics, Trinity Centre for
Prescribing of anti-osteoporotic therapies following the use of Proton Pump Inhibitors in general practice B. McGowan, K. Bennett, J. Feely Department of Pharmacology & Therapeutics, Trinity Centre for
8/6/2018. Glucocorticoid induced osteoporosis: overlooked and undertreated? Disclosure. Objectives. Overview
 Disclosure Glucocorticoid induced osteoporosis: overlooked and undertreated? I have no financial disclosure relevant to this presentation Tasma Harindhanavudhi, MD Division of Diabetes and Endocrinology
Disclosure Glucocorticoid induced osteoporosis: overlooked and undertreated? I have no financial disclosure relevant to this presentation Tasma Harindhanavudhi, MD Division of Diabetes and Endocrinology
A. Incorrect! The appendicular skeleton includes bones of the shoulder, arm, hand, pelvis, leg and foot.
 Anatomy and Physiology - Problem Drill 08: The Skeletal System III No. 1 of 10 1. Which of the following statements about the appendicular skeleton is correct? A. The appendicular skeleton includes bones
Anatomy and Physiology - Problem Drill 08: The Skeletal System III No. 1 of 10 1. Which of the following statements about the appendicular skeleton is correct? A. The appendicular skeleton includes bones
Interpreting DEXA Scan and. the New Fracture Risk. Assessment. Algorithm
 Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Horizon Scanning Technology Briefing. Zoledronic Acid (Aclasta) once yearly treatment for postmenopausal. National Horizon Scanning Centre
 Horizon Scanning Technology Briefing National Horizon Scanning Centre Zoledronic Acid (Aclasta) once yearly treatment for postmenopausal osteoporosis December 2006 This technology summary is based on information
Horizon Scanning Technology Briefing National Horizon Scanning Centre Zoledronic Acid (Aclasta) once yearly treatment for postmenopausal osteoporosis December 2006 This technology summary is based on information
Pectoral (Shoulder) Girdle
 Chapter 8 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum
Chapter 8 Skeletal System: Appendicular Skeleton Pectoral girdle Pelvic girdle Upper limbs Lower limbs 8-1 Pectoral (Shoulder) Girdle Consists of scapula and clavicle Clavicle articulates with sternum
Effective Health Care
 Number 12 Effective Health Care Comparative Effectiveness of Treatments To Prevent Fractures in Men and Women With Low Bone Density or Osteoporosis Executive Summary Background Osteoporosis is a systemic
Number 12 Effective Health Care Comparative Effectiveness of Treatments To Prevent Fractures in Men and Women With Low Bone Density or Osteoporosis Executive Summary Background Osteoporosis is a systemic
Postmenopausal osteoporosis is a systemic
 OSTEOPOROSIS: HARD FACTS ABOUT BONES Steven T. Harris, MD, FACP* ABSTRACT As a consequence of the aging process, osteoporosis affects all men and women. Agerelated loss of bone mass leads to skeletal fragility
OSTEOPOROSIS: HARD FACTS ABOUT BONES Steven T. Harris, MD, FACP* ABSTRACT As a consequence of the aging process, osteoporosis affects all men and women. Agerelated loss of bone mass leads to skeletal fragility
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 8 The Skeletal System: The Appendicular Skeleton The Appendicular Skeleton The 126 bones of the appendicular skeleton are primarily concerned
Principles of Anatomy and Physiology 14 th Edition CHAPTER 8 The Skeletal System: The Appendicular Skeleton The Appendicular Skeleton The 126 bones of the appendicular skeleton are primarily concerned
Appendix. TABLE E-1 Study Variables and Associated ICD-9-CM, HCPCS, and CPT Codes. Codes. (1) Fracture locations
 Page 1 Appendix TABLE E-1 Study Variables and Associated ICD-9-CM, HCPCS, and CPT Codes (1) Fracture locations Vertebral fracture Codes ICD-9-CM Diagnosis codes: 733.13, 805.xx, 806.xx ICD-9-CM Procedure
Page 1 Appendix TABLE E-1 Study Variables and Associated ICD-9-CM, HCPCS, and CPT Codes (1) Fracture locations Vertebral fracture Codes ICD-9-CM Diagnosis codes: 733.13, 805.xx, 806.xx ICD-9-CM Procedure
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Prada D, Zhong J, Colicino E, et al. Association
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Prada D, Zhong J, Colicino E, et al. Association
Skeletal System. Supplementary Information
 Skeletal System Supplementary Information COMMON ANATOMICAL TERMS Planes run through the body side to side and front to back eg. median plane Surfaces of the body are also named eg. anterior surface This
Skeletal System Supplementary Information COMMON ANATOMICAL TERMS Planes run through the body side to side and front to back eg. median plane Surfaces of the body are also named eg. anterior surface This
OSTEOPOROSIS IN MEN. Nelson B. Watts, MD OSTEOPOROSIS AND BONE HEALTH SERVICES CINCINNATI, OHIO
 OSTEOPOROSIS IN MEN Nelson B. Watts, MD OSTEOPOROSIS AND BONE HEALTH SERVICES CINCINNATI, OHIO DISCLOSURES Speakers Bureau: Amgen, Radius Consultant: Abbvie, Amgen, Janssen, Radius, Sanofi Watts NB et
OSTEOPOROSIS IN MEN Nelson B. Watts, MD OSTEOPOROSIS AND BONE HEALTH SERVICES CINCINNATI, OHIO DISCLOSURES Speakers Bureau: Amgen, Radius Consultant: Abbvie, Amgen, Janssen, Radius, Sanofi Watts NB et
Assessment and Treatment of Osteoporosis Professor T.Masud
 Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Osteoporosis Screening and Treatment in Type 2 Diabetes
 Osteoporosis Screening and Treatment in Type 2 Diabetes Ann Schwartz, PhD! Dept. of Epidemiology and Biostatistics! University of California San Francisco! October 2011! Presenter Disclosure Information
Osteoporosis Screening and Treatment in Type 2 Diabetes Ann Schwartz, PhD! Dept. of Epidemiology and Biostatistics! University of California San Francisco! October 2011! Presenter Disclosure Information
11/25/2012. Chapter 7 Part 2: Bones! Skeletal Organization. The Skull. Skull Bones to Know Cranium
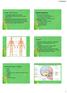 Chapter 7 Part 2: Bones! 5) Distinguish between the axial and appendicular skeletons and name the major parts of each 6) Locate and identify the bones and the major features of the bones that compose the
Chapter 7 Part 2: Bones! 5) Distinguish between the axial and appendicular skeletons and name the major parts of each 6) Locate and identify the bones and the major features of the bones that compose the
Challenging the Current Osteoporosis Guidelines. Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA
 Challenging the Current Osteoporosis Guidelines Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Whom to screen Which test How to diagnose Whom to treat Benefits
Challenging the Current Osteoporosis Guidelines Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Whom to screen Which test How to diagnose Whom to treat Benefits
Biology 218 Human Anatomy. Adapted from Martini Human Anatomy 7th ed. Chapter 7 The Skeletal System Appendicular Division
 Adapted from Martini Human Anatomy 7th ed. Chapter 7 The Skeletal System Appendicular Division Introduction The appendicular skeleton includes: Pectoral girdle Shoulder bones Upper limbs Pelvic girdle
Adapted from Martini Human Anatomy 7th ed. Chapter 7 The Skeletal System Appendicular Division Introduction The appendicular skeleton includes: Pectoral girdle Shoulder bones Upper limbs Pelvic girdle
Bones of Thorax (Rib Cage)
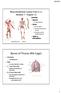 Musculoskeletal System (Part A-2) Module 7 -Chapter 10 Overview Muscles Attachments Bones Bone types Surface features of bones Divisions of the skeletal system Joints or Articulations Susie Turner, M.D.
Musculoskeletal System (Part A-2) Module 7 -Chapter 10 Overview Muscles Attachments Bones Bone types Surface features of bones Divisions of the skeletal system Joints or Articulations Susie Turner, M.D.
Chapter 6 & 7 The Skeleton
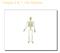 Chapter 6 & 7 The Skeleton Try this Make clockwise circles with your RIGHT foot, while doing this, draw the number 6 in the air with you RIGHT hand what happens to your foot???? Bony Background Adult body
Chapter 6 & 7 The Skeleton Try this Make clockwise circles with your RIGHT foot, while doing this, draw the number 6 in the air with you RIGHT hand what happens to your foot???? Bony Background Adult body
Using the FRAX Tool. Osteoporosis Definition
 How long will your bones remain standing? Using the FRAX Tool Gary Salzman M.D. Director Banner Good Samaritan/ Hayden VAMC Internal Medicine Geriatric Fellowship Program Phoenix, Arizona Using the FRAX
How long will your bones remain standing? Using the FRAX Tool Gary Salzman M.D. Director Banner Good Samaritan/ Hayden VAMC Internal Medicine Geriatric Fellowship Program Phoenix, Arizona Using the FRAX
Denosumab for the prevention of osteoporotic fractures in postmenopausal women
 Denosumab for the prevention of osteoporotic fractures in Issued: October 2010 guidance.nice.org.uk/ta204 NICE has accredited the process used by the Centre for Health Technology Evaluation at NICE to
Denosumab for the prevention of osteoporotic fractures in Issued: October 2010 guidance.nice.org.uk/ta204 NICE has accredited the process used by the Centre for Health Technology Evaluation at NICE to
Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History: History of Fractures Questionnaire
 PhenX Measure: Fracture History (#170900) PhenX Protocol: Fracture History (#170901) Date of Interview/Examination (MM/DD/YYYY): Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History:
PhenX Measure: Fracture History (#170900) PhenX Protocol: Fracture History (#170901) Date of Interview/Examination (MM/DD/YYYY): Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History:
Differentiating Pharmacological Therapies for Osteoporosis
 Differentiating Pharmacological Therapies for Osteoporosis Socrates E Papapoulos Department of Endocrinology & Metabolic Diseases Leiden University Medical Center The Netherlands Competing interests: consulting/speaking
Differentiating Pharmacological Therapies for Osteoporosis Socrates E Papapoulos Department of Endocrinology & Metabolic Diseases Leiden University Medical Center The Netherlands Competing interests: consulting/speaking
Osteoporosis Management
 Osteoporosis Management Lisa Voss PA C, CCD Laura Frontiero NP C, CCD Kaiser Healthy Bones Program San Diego Disclosures: Nothing to disclose www.zazzle.com 1 Overview How to diagnose Osteoporosis FRAX
Osteoporosis Management Lisa Voss PA C, CCD Laura Frontiero NP C, CCD Kaiser Healthy Bones Program San Diego Disclosures: Nothing to disclose www.zazzle.com 1 Overview How to diagnose Osteoporosis FRAX
Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide was developed to assist Primary Care physicians
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide was developed to assist Primary Care physicians
A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women
 A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women APHA Conference Washington, DC November 2, 2011 Presenter Disclosures Kathy Schneider, PhD
A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women APHA Conference Washington, DC November 2, 2011 Presenter Disclosures Kathy Schneider, PhD
Bone Mineral Density Studies in Adult Populations
 Bone Mineral Density Studies in Adult Populations Last Review Date: July 14, 2017 Number: MG.MM.RA10aC6 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician
Bone Mineral Density Studies in Adult Populations Last Review Date: July 14, 2017 Number: MG.MM.RA10aC6 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician
Exercise Science Section 2: The Skeletal System
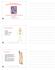 Exercise Science Section 2: The Skeletal System An Introduction to Health and Physical Education Ted Temertzoglou Paul Challen ISBN 1-55077-132-9 Role of the Skeleton Protection Framework Attachments for
Exercise Science Section 2: The Skeletal System An Introduction to Health and Physical Education Ted Temertzoglou Paul Challen ISBN 1-55077-132-9 Role of the Skeleton Protection Framework Attachments for
Men and Osteoporosis So you think that it can t happen to you
 Men and Osteoporosis So you think that it can t happen to you Jonathan D. Adachi MD, FRCPC Alliance for Better Bone Health Chair in Rheumatology Professor, Department of Medicine Michael G. DeGroote School
Men and Osteoporosis So you think that it can t happen to you Jonathan D. Adachi MD, FRCPC Alliance for Better Bone Health Chair in Rheumatology Professor, Department of Medicine Michael G. DeGroote School
1
 www.osteoporosis.ca 1 2 Overview of the Presentation Osteoporosis: An Overview Bone Basics Diagnosis of Osteoporosis Drug Therapies Risk Reduction Living with Osteoporosis 3 What is Osteoporosis? Osteoporosis:
www.osteoporosis.ca 1 2 Overview of the Presentation Osteoporosis: An Overview Bone Basics Diagnosis of Osteoporosis Drug Therapies Risk Reduction Living with Osteoporosis 3 What is Osteoporosis? Osteoporosis:
Meta-analysis: analysis:
 1 Diabetes and TZDs: Risk Factors for Fracture Ann Schwartz, PhD Dept. of Epidemiology and Biostatistics University of California San Francisco July 2010 Osteoporosis CME Presenter Disclosure Information
1 Diabetes and TZDs: Risk Factors for Fracture Ann Schwartz, PhD Dept. of Epidemiology and Biostatistics University of California San Francisco July 2010 Osteoporosis CME Presenter Disclosure Information
Outline. Switching treatment. Evidence from randomized trials. The effects of switching 7/8/2016. When and for whom? Steven Cummings, MD
 Outline Switching treatment When and for whom? Steven Cummings, MD Focus on switching from alendronate or risedronate Evidence about the effects of switching on BMD Purposes of switching Symptoms Poor
Outline Switching treatment When and for whom? Steven Cummings, MD Focus on switching from alendronate or risedronate Evidence about the effects of switching on BMD Purposes of switching Symptoms Poor
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Note: Page numbers of article titles are in boldface type. A Abscess, epidural, 822 824 Achilles tendon rupture, 894 895, 981 982 Acromioclavicular separations, shoulder pain in, 751 753 Adhesive capsulitis,
Disclosures Fractures: A. Schwartz Epidemiology and Risk Factors Consulting: Merck
 Disclosures Fractures: A. Schwartz Epidemiology and Risk Factors Consulting: Merck Ann V. Schwartz, PhD Department of Epidemiology and Biostatistics UCSF Outline Fracture incidence and impact of fractures
Disclosures Fractures: A. Schwartz Epidemiology and Risk Factors Consulting: Merck Ann V. Schwartz, PhD Department of Epidemiology and Biostatistics UCSF Outline Fracture incidence and impact of fractures
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
Exercise 11. The Appendicular Skeleton
 Exercise 11 The Appendicular Skeleton The Appendicular Skeleton The appendicular skeleton contains 126 bones. Consists of the upper and lower limbs, the pectoral girdles, and the pelvic girdles. The pectoral
Exercise 11 The Appendicular Skeleton The Appendicular Skeleton The appendicular skeleton contains 126 bones. Consists of the upper and lower limbs, the pectoral girdles, and the pelvic girdles. The pectoral
PRE-LAB EXERCISES. Before we get started, look up the definitions of these common bone marking terms: Canal: Condyle: Facet: Fissure:
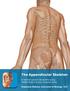 1 PRE-LAB EXERCISES When studying the skeletal system, the bones are often sorted into two broad categories: the axial skeleton and the appendicular skeleton. This lab focuses on the appendicular skeleton,
1 PRE-LAB EXERCISES When studying the skeletal system, the bones are often sorted into two broad categories: the axial skeleton and the appendicular skeleton. This lab focuses on the appendicular skeleton,
Osteoporosis: An Overview. Carolyn J. Crandall, MD, MS
 Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Objectives Review osteoporosis
Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Objectives Review osteoporosis
Chapter 8B. The Skeletal System: Appendicular Skeleton. The Appendicular Skeleton. Clavicle. Pectoral (Shoulder) Girdle
 The Appendicular Skeleton Chapter 8B The Skeletal System: Appendicular Skeleton 126 bones Pectoral (shoulder) girdle Pelvic (hip) girdle Upper limbs Lower limbs Functions primarily to facilitate movement
The Appendicular Skeleton Chapter 8B The Skeletal System: Appendicular Skeleton 126 bones Pectoral (shoulder) girdle Pelvic (hip) girdle Upper limbs Lower limbs Functions primarily to facilitate movement
National Utilization of Calcium Supplements in Patients with Osteoporotic Hip Fracture in Korea
 J Bone Metab 2013;20:99-103 http://dx.doi.org/10.11005/jbm.2013.20.2.99 pissn 2287-6375 eissn 2287-7029 Original Article National Utilization of Calcium Supplements in Patients with Osteoporotic Hip Fracture
J Bone Metab 2013;20:99-103 http://dx.doi.org/10.11005/jbm.2013.20.2.99 pissn 2287-6375 eissn 2287-7029 Original Article National Utilization of Calcium Supplements in Patients with Osteoporotic Hip Fracture
Osteoporosis: A Tale of 3 Task Forces!
 Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Horizon Scanning Centre March Denosumab for glucocorticoidinduced SUMMARY NIHR HSC ID: 6329
 Horizon Scanning Centre March 2014 Denosumab for glucocorticoidinduced osteoporosis SUMMARY NIHR HSC ID: 6329 This briefing is based on information available at the time of research and a limited literature
Horizon Scanning Centre March 2014 Denosumab for glucocorticoidinduced osteoporosis SUMMARY NIHR HSC ID: 6329 This briefing is based on information available at the time of research and a limited literature
Skeletal Manifestations
 Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
The Cost-Effectiveness of Bisphosphonates in Postmenopausal Women Based on Individual Long-Term Fracture Risks
 Volume ** Number ** ** VALUE IN HEALTH The Cost-Effectiveness of Bisphosphonates in Postmenopausal Women Based on Individual Long-Term Fracture Risks Tjeerd-Peter van Staa, MD, MA, PhD, 1,2 John A. Kanis,
Volume ** Number ** ** VALUE IN HEALTH The Cost-Effectiveness of Bisphosphonates in Postmenopausal Women Based on Individual Long-Term Fracture Risks Tjeerd-Peter van Staa, MD, MA, PhD, 1,2 John A. Kanis,
Page 1. Diagnosis and Treatment of Osteoporosis: What s New and Controversial in 2018? What s New in Osteoporosis
 Diagnosis and Treatment of Osteoporosis: What s New and Controversial in 2018? Douglas C. Bauer, MD Professor of Medicine and Epidemiology & Biostatistics University of California, San Francisco What s
Diagnosis and Treatment of Osteoporosis: What s New and Controversial in 2018? Douglas C. Bauer, MD Professor of Medicine and Epidemiology & Biostatistics University of California, San Francisco What s
Citation for the original published paper (version of record):
 http://www.diva-portal.org This is the published version of a paper published in Osteoporosis International. Citation for the original published paper (version of record): Bergman, J., Nordström, A., Nordström,
http://www.diva-portal.org This is the published version of a paper published in Osteoporosis International. Citation for the original published paper (version of record): Bergman, J., Nordström, A., Nordström,
The Appendicular Skeleton
 8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
8 The Appendicular Skeleton PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris 8-1 The Pectoral Girdle The Pectoral Girdle Also called shoulder girdle Connects the
Advanced medicine conference. Monday 20 Tuesday 21 June 2016
 Advanced medicine conference Monday 20 Tuesday 21 June 2016 Osteoporosis: recent advances in risk assessment and management Juliet Compston Emeritus Professor of Bone Medicine Cambridge Biomedical Campus
Advanced medicine conference Monday 20 Tuesday 21 June 2016 Osteoporosis: recent advances in risk assessment and management Juliet Compston Emeritus Professor of Bone Medicine Cambridge Biomedical Campus
Biology 218 Human Anatomy
 Chapter 8 Adapted from Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 203) 1. The appendicular skeleton contains 126 bones that form: i. two pectoral (shoulder) girdles two upper limbs i one pelvic
Chapter 8 Adapted from Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 203) 1. The appendicular skeleton contains 126 bones that form: i. two pectoral (shoulder) girdles two upper limbs i one pelvic
Diagnosis and Treatment of Osteoporosis: What s New and Controversial in ? What s New in Osteoporosis
 Diagnosis and Treatment of Osteoporosis: What s New and Controversial in 2018-19? What s New in Osteoporosis The crisis in treatment and compliance Douglas C. Bauer, MD Professor of Medicine and Epidemiology
Diagnosis and Treatment of Osteoporosis: What s New and Controversial in 2018-19? What s New in Osteoporosis The crisis in treatment and compliance Douglas C. Bauer, MD Professor of Medicine and Epidemiology
The Significance of Vertebral Fractures
 Special Report The Significance of Vertebral Fractures Both the prevalence and the clinical significance of vertebral fractures has been greatly underestimated by physicians. Vertebral fractures are much
Special Report The Significance of Vertebral Fractures Both the prevalence and the clinical significance of vertebral fractures has been greatly underestimated by physicians. Vertebral fractures are much
Impact of varying data quality on statistical analyses of integrated datasets
 Impact of varying data quality on statistical analyses of integrated datasets Eugenio Andraca-Carrera Mathematical Statistician Division of Biometrics VII Office of Biostatistics, CDER, FDA ISCTM 11th
Impact of varying data quality on statistical analyses of integrated datasets Eugenio Andraca-Carrera Mathematical Statistician Division of Biometrics VII Office of Biostatistics, CDER, FDA ISCTM 11th
Osteoporosis Management in Older Adults
 Osteoporosis Management in Older Adults Angela M Cheung, MD, PhD, FRCPC, CCD Professor of Medicine, University of Toronto Disclosures Relationship with Commercial Entities: Honoraria from: Amgen, Eli Lilly,
Osteoporosis Management in Older Adults Angela M Cheung, MD, PhD, FRCPC, CCD Professor of Medicine, University of Toronto Disclosures Relationship with Commercial Entities: Honoraria from: Amgen, Eli Lilly,
OSTEOPOROSIS MANAGEMENT AND INVESTIGATION. David A. Hanley, MD, FRCPC
 OSTEOPOROSIS MANAGEMENT AND INVESTIGATION David A. Hanley, MD, FRCPC There is a huge care gap in the management of osteoporosis in this country. As yet unpublished findings from the Canadian Multicentre
OSTEOPOROSIS MANAGEMENT AND INVESTIGATION David A. Hanley, MD, FRCPC There is a huge care gap in the management of osteoporosis in this country. As yet unpublished findings from the Canadian Multicentre
Download slides:
 Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
Current and Emerging Strategies for Osteoporosis
 Current and Emerging Strategies for Osteoporosis I have nothing to disclose. Anne Schafer, MD Assistant Professor of Medicine Division of Endocrinology & Metabolism December 12, 2014 Outline Osteoporosis
Current and Emerging Strategies for Osteoporosis I have nothing to disclose. Anne Schafer, MD Assistant Professor of Medicine Division of Endocrinology & Metabolism December 12, 2014 Outline Osteoporosis
Male osteoporosis: clinical approach and management in family practice
 Singapore Med J 2014; 55(7): 353-357 doi: 10.11622/smedj.2014085 CMEArticle Male osteoporosis: clinical approach and management in family practice Lay Hoon Goh 1,2, MMed, FCFP, Choon How How 1, MMed, FCFP,
Singapore Med J 2014; 55(7): 353-357 doi: 10.11622/smedj.2014085 CMEArticle Male osteoporosis: clinical approach and management in family practice Lay Hoon Goh 1,2, MMed, FCFP, Choon How How 1, MMed, FCFP,
bio4165 lab quiz 1 Posterior View Anterior View Lateral View Anterior View bio fall.quarter lab.quiz.1...page.1 of 6
 B A Posterior View D C E Lateral View bio.4165...fall.quarter.2005...lab.quiz.1...page.1 of 6 F I G 35 Posterior View H bio.4165...fall.quarter.2005...lab.quiz.1...page.2 of 6 J Posterior View L K Inferior
B A Posterior View D C E Lateral View bio.4165...fall.quarter.2005...lab.quiz.1...page.1 of 6 F I G 35 Posterior View H bio.4165...fall.quarter.2005...lab.quiz.1...page.2 of 6 J Posterior View L K Inferior
Osteoporosis challenges
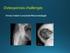 Osteoporosis challenges Osteoporosis challenges Who should have a fracture risk assessment? Who to treat? Drugs, holidays and unusual adverse effects Fracture liaison service? The size of the problem 1
Osteoporosis challenges Osteoporosis challenges Who should have a fracture risk assessment? Who to treat? Drugs, holidays and unusual adverse effects Fracture liaison service? The size of the problem 1
Learning Objectives. Controversies in Osteoporosis Prevention and Management. Etiology. Presenter Disclosure Information. Epidemiology.
 12:45 1:30pm Controversies in Osteoporosis Prevention and Management SPEAKER Carolyn Crandall, MD, MS Presenter Disclosure Information The following relationships exist related to this presentation: Carolyn
12:45 1:30pm Controversies in Osteoporosis Prevention and Management SPEAKER Carolyn Crandall, MD, MS Presenter Disclosure Information The following relationships exist related to this presentation: Carolyn
Osteoporosis: current treatment and future prospects. Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus
 Osteoporosis: current treatment and future prospects Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus Disclosures Consultancy and speaking fees for Gilead, related to development
Osteoporosis: current treatment and future prospects Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus Disclosures Consultancy and speaking fees for Gilead, related to development
Forteo (teriparatide) Prior Authorization Program Summary
 Forteo (teriparatide) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1 FDA Indication 1 : Forteo (teriparatide) is indicated for: the treatment of postmenopausal women with osteoporosis
Forteo (teriparatide) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1 FDA Indication 1 : Forteo (teriparatide) is indicated for: the treatment of postmenopausal women with osteoporosis
Parathyroid Hormone Analog for Osteoporosis Prior Authorization with Quantity Limit Criteria Program Summary
 Parathyroid Hormone Analog for Osteoporosis Prior Authorization with Quantity Limit Criteria Program Summary This prior authorization program applies to Commercial, NetResults A series, NetResults F series
Parathyroid Hormone Analog for Osteoporosis Prior Authorization with Quantity Limit Criteria Program Summary This prior authorization program applies to Commercial, NetResults A series, NetResults F series
Clinical Study Active Referral Intervention following Fragility Fractures Leads to Enhanced Osteoporosis Follow-Up Care
 Osteoporosis Volume 2012, Article ID 234381, 6 pages doi:10.1155/2012/234381 Clinical Study Active Referral Intervention following Fragility Fractures Leads to Enhanced Osteoporosis Follow-Up Care Michelle
Osteoporosis Volume 2012, Article ID 234381, 6 pages doi:10.1155/2012/234381 Clinical Study Active Referral Intervention following Fragility Fractures Leads to Enhanced Osteoporosis Follow-Up Care Michelle
New Developments in Osteoporosis: Screening, Prevention and Treatment
 Osteoporosis: Overview New Developments in Osteoporosis: Screening, Prevention and Treatment Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Risk factors
Osteoporosis: Overview New Developments in Osteoporosis: Screening, Prevention and Treatment Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Risk factors
Fracture=Bone Attack:
 Fracture=Bone Attack: Linking Hip Fractures to Osteoporosis Care Angela M. Cheung, MD, PhD, FRCPC Professor of Medicine, University of Toronto Potential Conflicts of Interests Industry Grants (to UHN)
Fracture=Bone Attack: Linking Hip Fractures to Osteoporosis Care Angela M. Cheung, MD, PhD, FRCPC Professor of Medicine, University of Toronto Potential Conflicts of Interests Industry Grants (to UHN)
Fractures: Epidemiology and Risk Factors. July 2012 CME (35 minutes) 7/24/ July12 1. Osteoporotic fractures: Comparison with other diseases
 Financial Disclosures Fractures: Epidemiology and Risk Factors Research grants, speaking or consulting: Amgen, Lilly, Merck, Novartis, Radius Dennis M. Black, PhD Department of Epidemiology and Biostatistics
Financial Disclosures Fractures: Epidemiology and Risk Factors Research grants, speaking or consulting: Amgen, Lilly, Merck, Novartis, Radius Dennis M. Black, PhD Department of Epidemiology and Biostatistics
Hole s Human Anatomy and Physiology Eleventh Edition. Mrs. Hummer. Chapter 7 Skeletal System
 Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Chapter 7 Skeletal System 1 Chapter 7 Skeletal System Bone Classification Long Bones Short Bones Flat Bones Irregular Bones Sesamoid (Round)
Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Chapter 7 Skeletal System 1 Chapter 7 Skeletal System Bone Classification Long Bones Short Bones Flat Bones Irregular Bones Sesamoid (Round)
July 2012 CME (35 minutes) 7/12/2016
 Financial Disclosures Epidemiology and Consequences of Fractures Advisory Board: Amgen Janssen Pharmaceuticals Inc. Ann V. Schwartz, PhD Department of Epidemiology and Biostatistics UCSF Outline Osteoporotic
Financial Disclosures Epidemiology and Consequences of Fractures Advisory Board: Amgen Janssen Pharmaceuticals Inc. Ann V. Schwartz, PhD Department of Epidemiology and Biostatistics UCSF Outline Osteoporotic
BAD TO THE BONE. Peter Jones, Rheumatologist QE Health, Rotorua. GP CME Conference Rotorua, June 2008
 BAD TO THE BONE Peter Jones, Rheumatologist QE Health, Rotorua GP CME Conference Rotorua, June 2008 Agenda Osteoporosis in Men Vitamin D and Calcium Long-term treatment with Bisphosphonates Pathophysiology
BAD TO THE BONE Peter Jones, Rheumatologist QE Health, Rotorua GP CME Conference Rotorua, June 2008 Agenda Osteoporosis in Men Vitamin D and Calcium Long-term treatment with Bisphosphonates Pathophysiology
Disclosures Fractures:
 Disclosures Fractures: A. Schwartz Epidemiology and Risk Factors Research Funding: GlaxoSmithKline, Merck Ann V. Schwartz, PhD Department of Epidemiology and Biostatistics UCSF Outline Fracture incidence
Disclosures Fractures: A. Schwartz Epidemiology and Risk Factors Research Funding: GlaxoSmithKline, Merck Ann V. Schwartz, PhD Department of Epidemiology and Biostatistics UCSF Outline Fracture incidence
Updates in Osteoporosis. I have no conflicts of interest. What Would You Do? Mrs. C. What s New in Osteoporosis. Page 1
 Updates in Osteoporosis Jeffrey A. Tice, MD Associate Professor of Medicine Division of General Internal Medicine, University of California, San Francisco I have no conflicts of interest What s New in
Updates in Osteoporosis Jeffrey A. Tice, MD Associate Professor of Medicine Division of General Internal Medicine, University of California, San Francisco I have no conflicts of interest What s New in
OSTEOPOROSIS: PREVENTION AND MANAGEMENT
 OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
Coordinator of Post Professional Programs Texas Woman's University 1
 OSTEOPOROSIS Update 2007-2008 April 26, 2008 How much of our BMD is under our control (vs. genetics)? 1 2 Genetic effects on bone loss: longitudinal twin study (Makovey, 2007) Peak BMD is under genetic
OSTEOPOROSIS Update 2007-2008 April 26, 2008 How much of our BMD is under our control (vs. genetics)? 1 2 Genetic effects on bone loss: longitudinal twin study (Makovey, 2007) Peak BMD is under genetic
Osteoporosis. Treatment of a Silently Developing Disease
 Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
Understanding Osteoporosis
 Understanding Osteoporosis Professor Juliet E. Compston Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT NOTICE This book is intended not as
Understanding Osteoporosis Professor Juliet E. Compston Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT NOTICE This book is intended not as
Ch. 5 - Skeletal System
 Ch. 5 - Skeletal System Bones are living, ever-changing structures. This allows them grow and adapt to new situations that the body encounters. The functions of the skeletal system: 1) support bones are
Ch. 5 - Skeletal System Bones are living, ever-changing structures. This allows them grow and adapt to new situations that the body encounters. The functions of the skeletal system: 1) support bones are
Name of Policy: Zoledronic Acid (Reclast ) Injection
 Name of Policy: Zoledronic Acid (Reclast ) Injection Policy #: 355 Latest Review Date: May 2011 Category: Pharmacy Policy Grade: Active Policy but no longer scheduled for regular literature reviews and
Name of Policy: Zoledronic Acid (Reclast ) Injection Policy #: 355 Latest Review Date: May 2011 Category: Pharmacy Policy Grade: Active Policy but no longer scheduled for regular literature reviews and
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 21 July 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 21 July 2010 ACTONEL 5 mg, film-coated tablet B/14 (CIP code: 354 362-3) ACTONEL 30 mg, film-coated tablet B/28 (CIP
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 21 July 2010 ACTONEL 5 mg, film-coated tablet B/14 (CIP code: 354 362-3) ACTONEL 30 mg, film-coated tablet B/28 (CIP
Osteoporosis Treatment Overview. Colton Larson RFUMS October 26, 2018
 Osteoporosis Treatment Overview Colton Larson RFUMS October 26, 2018 Burden of Disease Most common bone disease 9.9 million Americans + 43.1 million Americans have low bone mineral density (BMD) Stealthy
Osteoporosis Treatment Overview Colton Larson RFUMS October 26, 2018 Burden of Disease Most common bone disease 9.9 million Americans + 43.1 million Americans have low bone mineral density (BMD) Stealthy
Prevention of Osteoporotic Hip Fracture
 Prevention of Osteoporotic Hip Fracture Dr Law Sheung Wai 8th July 2007 Associate Consultant Spine team / Orthopedic Rehabilitation Department of Orthopedics and Traumatology NTE Cluster 1 Objectives Problems
Prevention of Osteoporotic Hip Fracture Dr Law Sheung Wai 8th July 2007 Associate Consultant Spine team / Orthopedic Rehabilitation Department of Orthopedics and Traumatology NTE Cluster 1 Objectives Problems
Presenter: 翁家嫻 Venue date:
 FOR THE TREATMENT OF OSTEOPOROSIS IN POSTMENOPAUSAL WOMEN AT INCREASED RISK OF FRACTURES 1 Presenter: 翁家嫻 Venue date: 2018.03.13 PMO: postmenopausal osteoporosis. 1. Prolia (denosumab), Summary of Product
FOR THE TREATMENT OF OSTEOPOROSIS IN POSTMENOPAUSAL WOMEN AT INCREASED RISK OF FRACTURES 1 Presenter: 翁家嫻 Venue date: 2018.03.13 PMO: postmenopausal osteoporosis. 1. Prolia (denosumab), Summary of Product
The NOF & NBHA Quality Improvement Registry
 In collaboration with CECity The NOF & NBHA Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO Practices for
In collaboration with CECity The NOF & NBHA Quality Improvement Registry This registry is approved by CMS as a Qualified Clinical Data Registry (QCDR) for Eligible Professionals and GPRO Practices for
Bone Mass Measurement BONE MASS MEASUREMENT HS-042. Policy Number: HS-042. Original Effective Date: 8/25/2008
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Osteoporosis: How to Manage Long- Term Use of Bisphosphonates AKA Now What? David E Feinstein, DO, CCD November 15 th, 2017
 Osteoporosis: How to Manage Long- Term Use of Bisphosphonates AKA Now What? David E Feinstein, DO, CCD November 15 th, 2017 Introduction A fracture due to OP occurs every 3 seconds around the world. 1
Osteoporosis: How to Manage Long- Term Use of Bisphosphonates AKA Now What? David E Feinstein, DO, CCD November 15 th, 2017 Introduction A fracture due to OP occurs every 3 seconds around the world. 1
