Lateral tibial plateau autograft in revision surgery for failed medial unicompartmental knee arthroplasty
|
|
|
- Alison Chastity Warren
- 6 years ago
- Views:
Transcription
1 DOI /s z KNEE Lateral tibial plateau autograft in revision surgery for failed medial unicompartmental knee arthroplasty Simone Cerciello 1 Brent Joseph Morris 2 Sebastien Lustig 1 Enrico Visonà 3 Giuliano Cerciello 4 Katia Corona 5 Philippe Neyret 1 Received: 1 November 2014 / Accepted: 16 April 2015 European Society of Sports Traumatology, Knee Surgery, Arthroscopy (ESSKA) 2015 Abstract Purpose Revision surgery for failed unicompartmental knee arthroplasty (UKA) with bone loss is challenging. Several options are available including cement augmentation, metal augmentation, and bone grafting. The aim of the present study was to describe a surgical technique for lateral tibial plateau autografting and report mid-term outcomes. Methods Eleven consecutive patients (median age 69.5 years) affected by posteromedial tibial plateau collapse after medial UKA were enrolled in the present study. The delay between UKA and revision surgery was 21 months (range months). All patients were revised with a cemented posterior-stabilized implant, with a tibial stem. Medial tibial plateau bone loss was treated with an autologous lateral tibial plateau bone graft secured with two absorbable screws. All patients were evaluated with the Oxford Knee Score (OKS), visual analogue scale for pain (VAS), and complete radiographic evaluation. Results At a median follow-up of 60 months (range months), the OKS improved from 21.5 (range * Simone Cerciello simone.cerciello@me.com 1 Albert Trillat Center, Lyon North University Hospital, 103 Grande Rue de la Croix Rousse, Lyon, France 2 Lexington Clinic Orthopedics Sports Medicine Center, The Shoulder Center of Kentucky, Lexington, KY, USA Ospedale di Este, ULSS 17, Este, Italy Casa di Cura Villa Betania, Polo Ospedaliero Santo Spirito, Rome, Italy Science for Health Department, Molise University, Campobasso, Italy 16 26) to 34.5 (range 30 40) (p < 0.01) and the median VAS score improved from 8.0 (range 5 9) to 5.5 (range 3 7) (p < 0.01). No intraoperative complications were recorded. Partial reabsorption of the graft was observed in two cases at final follow-up. Conclusion Lateral tibial plateau bone autograft is an alternative to metal wedge or cement augments in the treatment of medial plateau collapse after UKA. Primary fixation of the tibial plateau autograft can be achieved with absorbable screws and a tibial-stemmed implant. Further comparative studies with a larger series may be helpful to draw definitive conclusions. Level of evidence Case series, Level IV. Keywords Unicompartmental knee arthroplasty Tibial plateau collapse Revision surgery Lateral plateau autograft Introduction Unicompartmental knee arthroplasty (UKA) has emerged in the last decade as an alternative to total knee arthroplasty (TKA) and high tibial osteotomy (HTO) in the treatment of isolated medial compartment osteoarthritis [11]. Unicompartmental knee arthroplasty should not be considered a temporary solution before TKA, because clinical outcomes are not equal to results of a primary knee arthroplasty when revised [20]. The most common cause for a revision of a UKA to TKA is loosening. Loosening accounted for half of all revisions that were performed in the New Zealand Joint Registry [13]. Since aseptic loosening is often asymptomatic initially, it tends to be associated with progressive osteolysis and leads to bone defects that require advanced surgical
2 management in the revision setting [15]. The presence of extensive bone loss at the time of UKA revision is challenging and may require bone grafting [12, 14, 18], the need for stemmed revision components and metal or tantalum augments, or even the need for custom made implants [1]. It is well established that the integration of metal augments with the sclerotic bone of the medial plateau may be difficult and aseptic loosening of the tibia is the most common cause UKA re-revision [8, 13]. Addressing such bone defects with biologic solutions such as autologous bone graft may be advantageous in terms of biologic integration and economic costs. The aim of the present study was to describe a technique for lateral tibial plateau autograft to address the posteromedial tibial plateau collapse in revision surgery for failed UKA and to report the mid-term outcomes in a consecutive series of patients. It was hypothesized that lateral plateau autografting would result in good clinical outcomes and stable radiographic findings at midterm follow-up. Materials and methods Eleven consecutive patients affected by posteromedial tibial plateau collapse after medial UKA were enrolled in the present retrospective cohort study. Medial plateau collapse was detected on lateral radiographs as an increase in posterior inclination of the tibial plateau. Eight patients were female, and three patients were male. The right knee was involved in seven cases, while the left side was involved in four cases. All patients were revised with the same surgical technique, the same cemented posterior-stabilized implant, and by the same senior surgeon (GC). The index procedure was performed in our department for two cases, while the index procedure was performed at outside facilities in nine cases. The median age at the time of revision surgery was 69.5 years (range years). The median delay between UKA and revision TKA was 21 months (15 36 months). The knee flexion was on median 100 (range ), and three patients had a flexion contracture of 7 (range 5 10 ). All patients had significant pain and tibial component loosening with posteromedial bone loss that was evident on serial radiographs. Tibial plateau bone loss was detected with conventional radiographic examination including weight-bearing anteroposterior and lateral views. All patients were evaluated with the Oxford Knee Score (OKS) [5] and a visual analogue scale for pain (VAS). All the methods described in this article were approved by the local ethics committee (Health Director of the Villa Betania Hospital in Rome). Surgical technique All cases were performed with patients in the supine position with the operative leg in a leg holder in order to keep the knee in deep flexion. The tourniquet was inflated at 350 mmhg just prior to the skin incision. The prior surgical incision was utilized and extended distally to reach the inferior border of the tibial tuberosity and proximally around 4 cm proximal to the superior pole of the patella. Medial capsulotomy was performed with electrocautery. Dissection of the anteromedial capsule was completed to improve joint exposure and to achieve partial medial release. The fat pad was excised, and the patella was everted. Complete circumferential osteophyte removal and patellar denervation was performed in all cases. The femoral notch was released, and both anterior and posterior cruciate ligaments were resected. The lateral meniscus was completely resected to allow complete visualization of the lateral compartment. After scar tissue excision, the tibial and femoral components were assessed for stability. The femoral component was well integrated in all cases, but the tibial tray was grossly loose in all cases. Component removal was carried out with sharp osteotomes taking care to preserve the host bone. Tibial resection was performed first. The same instrumentation and implants (Tornier Inc. Montbonnot Saint Martin. France) were used in all cases. This implant has an intramedullary guide for the tibia that controls the tibial slope. The resection was performed with 0 of tibial slope. An extramedullary jig controls varus valgus alignment and aligns the tibial cut perpendicular to the mechanical axis and also controls the extent of medial bone resection. The resection of medial plateau was performed flush to the residual bone in order to obtain a flat surface perpendicular to the mechanical axis. The difference in height among the medial side and the lateral side could be easily calculated. In fact, on the lateral side, a preliminary orthogonal resection was completed to just below the cartilage level extending medially below the level of the tibial spine. The bony resection was performed in a standard fashion (like for standard primary TKA) 9 mm below the lateral plateau. Once the posterior aspect of the lateral plateau was released, an autograft of around 8 mm was available. Additional bone chips were obtained from the tibial spine. The autograft was prepared to match the medial plateau (Fig. 1). The tibial canal was prepared to host a tibial stem. Size and length of the stem were chosen according to the quality of the metaphyseal bone. The preparation of the metaphysis was performed without the graft in place to avoid any risk of graft fracture, whereas the graft was gently prepared with a luer. Once the match was satisfactorily achieved, the autograft was gently impacted to obtain the same height level for the medial and lateral plateau. The graft was then
3 Fig. 1 Tibial bone graft has a thickness of 8 mm and is prepared with a luer to match with the shape of the medial plateau this goal and to avoid malrotation, the same thickness of the removed implant must be considered when performing the posterior resection. A double check with the epicondylar axis was also performed. Satisfactory ligament balancing was obtained with a (9 mm) polyethylene insert in all cases. The tibial and femoral components were cemented once the stability and the range of movement (ROM) were assessed and deemed to be satisfactory. The tibial stem was not cemented in any case. The tourniquet was released after cementation was completed. The surgical field was irrigated, and bleeding was controlled. A medium drain was placed and left into the joint for the first 24 h. The capsule was closed with a #2 absorbable suture. The subcutaneous layer and skin were sutured in standard fashion. A compressive dressing was applied to the whole leg and left in place for the first 24 h. The physical therapy protocol was the same in all patients. Continuous passive motion was initiated from the first post-operative day and then carried on for the first 3 weeks while increasing knee flexion by 5 daily. Isometric strengthening exercises for the quadriceps strengthening were performed from day 1 as well. Weight bearing was not allowed for the first month. Partial weight bearing was encouraged after one month for 15 more days. Complete weight bearing was allowed 45 days after surgery following radiographic review. Pulsed electromagnetic field therapy (Igea spa, Carpi, Italy) was performed in all patients for the first 45 days after surgery. The duration of follow-up after revision surgery was 60 months (range months). OKS and radiographs were obtained at final follow-up, and an additional subjective evaluation was completed asking the following question: are you very satisfied, satisfied or not satisfied with your functional result? Statistical analysis Statistical analysis of the preoperative and post-operative values was performed using the Wilcoxon signed-rank test: XLSTAT 2009 (G*Power ) setting the alpha value at Fig. 2 Bone graft is gently impacted onto the cancellous bone of the medial plateau and then fixed with two absorbable screws fixed with two 4.5-mm cancellous absorbable poly lactic acid screws with hydroxyapatite coating (Taikron Co Lpt, Japan) (Fig. 2). On the femoral side, distal resection was performed with the aid of an intramedullary cutting guide. The philosophy of this prosthesis is a posterior resection parallel to the plane of the posterior condyles. To achieve Results One patient died 3 years after revision surgery due to natural causes unrelated to the knee replacement. Ten patients were available for both clinical and radiographic evaluation at final follow-up. Tibial plateau bone loss was evaluated radiographically and intraoperatively. A cavitary defect with an intact cortical rim was found in seven cases. In all cases, initial radiographs after UKA revealed an undersized prosthetic tibial tray. The alignment of the tibial component
4 Discussion Fig. 3 AP view shows partial reabsorption of the graft was judged to be correct, with an orientation within 3 to the preoperative joint line in all cases. Serial radiographs demonstrated progressive subsidence of the implant prior to the revision surgery. In the remaining three cases, the defect was segmental with interruption of the cortical rim. In these cases, the sizing of the tibial component was judged to be appropriate. In these cases, the analysis of pre- UKA radiographs revealed that the native posterior tibial slope was not restored. In these circumstances, an insufficient slope may lead to posterior overload during knee flexion with increased risk of tibial tray collapse into the host bone. No intraoperative complications were recorded. At final follow-up, the knee flexion was on median 110 (range ) with one patient having a persistent flexion contracture of 10. The median OKS improved from 21.5 (range 16 26) to 34.5 (range 30 40) (p < 0.01), and the VAS score improved from 8.0 (range 5 9) to 5.5 (range 3 7) (p < 0.01). Three patients were very satisfied with their functional result and six were satisfied. One patient was not satisfied and reported persistent pain under weightbearing conditions. Radiographs revealed complete integration of the graft in eight patients, while partial reabsorption of the graft was present in two cases (Fig. 3). The partial graft reabsorption occurred within the first 6 months, however, in both cases, and the reabsorption was neither symptomatic nor progressive. The most important finding of the present study is the reliable surgical technique of lateral plateau autografting for revision of UKA. To our knowledge, this is the first report on a homogenous population of patients affected by tibial plateau collapse after UKA. The same surgical technique of autologous bone graft from the lateral tibial plateau to address medial plateau bone loss as well as the same implant was utilized in all patients. In the present series, a purely cavitary defect was observed in cases of undersized tibial trays with the posterior aspect sinking into the cancellous bone. Partial involvement of the posterior cortical rim was found in cases of insufficient posterior tibial slope. The bone loss was addressed in all cases with an autograft of the lateral tibial plateau. In fact, the tibial resection, which was performed in the same way as for primary implants, allowed us to harvest an 8 10 mm graft. The primary stability of the graft was secure fixation with two 4.5-mm absorbable screws. To bypass the bone-to-bone interface, a short stem was implanted in all cases and the tibial plateau was cemented as well. The graft was then protected from loading for the first post-operative period, and bone remodelling was stimulated with prolonged pulsed electromagnetic field therapy [19]. Nevertheless, partial reabsorption of the graft was observed in two cases, although it was not clinically symptomatic. No intraoperative complications were reported. Patients were generally satisfied with their functional result with a significant and stable improvement of Oxford and VAS scores even in the two cases that developed a partial reabsorption of the graft. Conversely, the improvement of flexion was not significant. Most of the patients had satisfactory preoperative flexion, and this could be the consequence of the pathologic anatomy. In fact, the posterior involvement of the tibial plateau may have not negatively influenced the preoperative flexion. These positive outcomes may be related to the very strict indications, with limited bone loss exclusively on the tibial side. Revision surgery after failed medial UKA may be technically demanding when bone loss or ligament insufficiency are present [6] leading to outcomes that are generally inferior to primary surgery [20]. The presence of bone loss must be carefully evaluated when dealing with revision of a UKA. It can be contained or segmental. In medial UKA s, bone loss is often attributable to mechanical loosening of the implant. It may be the consequence of technical errors such as excessive varus inclination of the joint line, insufficient posterior tibial slope, or a downsized tibial tray. Finally, additional bone loss may be the result of polyethylene wear [3] or it may be caused at the time of tibial component removal. Different strategies in dealing with bony defects have been described including metal
5 wedges, cement, and allogenic or autologous bone grafting [2, 4, 7, 9, 10, 17, 18, 21]. According to the literature, the use of long stems and wedges is necessary in up to 69 % of the UKA revisions [13, 22]. Currently, no option has been demonstrated to be superior to the others and all these options have shown potential disadvantages. Padgett et al. [12] reported a higher complication rate when cement alone was used to fill the bone defect. Metal wedges are the most common and easiest way to address medial plateau bone loss. Unfortunately, bone sclerosis at the tibial metaphysis can be a problem when metal augments are applied. The excessive stiffness may decrease fixation properties of the implant leading to subsequent loosening of the revision prosthesis [8, 13]. Allografting or autografting may be advantageous in preserving the host bone stock and reproducing the same elasticity of the metaphyseal bone allowing for a physiologic remodelling of the metaphysis. Tibial autograft has several additional advantages. First of all, it is easily accessible during surgery with the possibility of perfect match with the host tibial metaphysis. In addition, autografts offer economic benefits over traditional metal wedges, allografts, or custom implants with the only cost being represented by the two absorbable screws. This is a major issue especially in countries or hospital systems where the budget for revision procedures is limited. However, some doubts may arise regarding the stability of initial fixation of the graft and late integration. Nevertheless, the primary stability of the graft can be increased with absorbable or metallic screws and bypassing the bone-to-bone interface with tibial stems. The integration can be stimulated with external devices such as magnetotherapy or pulsed electromagnetic field therapy [19]. In any case, it is important to highlight the importance of periodic follow-up examination after UKA and the revision surgery. Posterior tibial collapse occurring after UKA may be easily detected in the early phase with radiographic follow-up in symptomatic patients. This is crucial to avoid extensive bone loss that can increase the complexity of revision surgery and affect post-operative outcomes. In a similar way, the presence of tibial reabsorption after revision surgery must be detected and its evolution and clinical impact must be followed with seriate controls. To our knowledge, the study by Pietschmann et al. [14] is the only other one describing a technique of lateral plateau bone grafting. However, in his series of 17 patients, revision surgery was necessary for either an aseptic loosening (tibial, femoral or tibial, and femoral component), progression of osteoarthritis at the lateral compartment or dislocation of the insert and prosthetic fracture. The tibial plateau was fixed with two absorbable pins. At an average follow-up of 3.1 years, no radiographic signs of loosening wear or implant subsidence were observed and significant improvement of all clinical scores was reported. The outcomes of the present study are comparable to those of Pietschmann et al., and both are similar to those reported with metal wedges and augments [14, 16]. The potential biologic and economic advantages make bone autografts an alternative to traditional metal wedges when dealing with bone loss during revision surgery for failed medial UKA s. Our study has several limitations. First of all, the study population was small with strict inclusion criteria and the study was limited to a single centre. Secondly, even though the follow-up was 5 years, this is still relatively short given the expected duration of the implants. Longer-term followup may yield graft complications that were not noticed during the follow-up period. Finally, the series was retrospective and lacked a control group, which makes any definitive conclusions questionable. Conclusion Tibial plateau autograft is an economic and valid alternative to metal wedges in the treatment of medial plateau collapse following UKA. Clinical results and satisfaction rates are encouraging and comparable between the two options. Potential advantages of autograft include preservation of the host bone stock, elasticity, which is similar to the surrounding bone and reduced costs. Partial reabsorption of the graft may be of concern with longer-term follow-up. References 1. Barrett WP, Scott RD (1987) Revision of failed unicondylar unicompartmental knee arthroplasty. J Bone Joint Surg Am 69: Brandes M, Ringling M, Winter C, Hillmann A, Rosenbaum D (2010) Changes in physical activity and health-related quality of life during the first year after total knee arthroplasty. Arthritis Care Res (Hoboken) 63(3): Bruni D, Akkawi I, Iacono F, Raspugli GF, Gagliardi M, Nitri M, Grassi A, Zaffagnini S, Bignozzi S, Marcacci M (2013) Minimum thickness of all-poly tibial component unicompartmental knee arthroplasty in patients younger than 60 years does not increase revision rate for aseptic loosening. Knee Surg Sports Traumatol Arthrosc 21(11): Chakrabarty G, Newman JH, Ackroyd CE (1998) Revision of unicompartmental arthroplasty of the knee. Clinical and technical considerations. J Arthroplasty 13(2): Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Joint Surg (Br) 80(1): Hang JR, Stanford TE, Graves SE, Davidson DC, de Steiger RN, Miller LN (2010) Outcome of revision of unicompartmental knee replacement. Acta Orthop 81(1): Levine WN, Ozuna RM, Scott RD, Thornhill T (1996) Conversion of failed modern unicompartmental arthroplasty to total knee arthroplasty. J Arthroplasty 11(7):
6 8. Lewold S, Robertsson O, Knutson K, Lidgren L (1998) Revision of unicompartmental knee arthroplasty: outcome in 1,135 cases from the Swedish Knee Arthroplasty study. Acta Orthop Scand 69(5): Martin J, Wallace D, Woods D, Carr AJ, Murray DW (1995) Revision of unicondylar knee replacements to total knee replacement. Knee 2(2): McAuley JP, Engh GA, Ammeen DJ (2001) Revision of failed unicompartmental knee arthroplasty. Clin Orthop Relat Res 392: Niinimäki T, Eskelinen A, Mäkelä K, Ohtonen P, Puhto AP, Remes V (2014) Unicompartmental knee arthroplasty survivorship is lower than TKA survivorship: a 27-year Finnish registry study. Clin Orthop Relat Res 472(5): Padgett DE, Stern SH, Insall JN (1991) Revision total knee arthroplasty for failed unicompartmental replacement. J Bone Joint Surg Am 73: Pearse AJ, Hooper GJ, Rothwell A, Frampton C (2010) Survival and functional outcome after revision of a unicompartmental to a total knee replacement: the New Zealand National Joint Registry. J Bone Joint Surg Br 92(4): Pietschmann MF, Ficklscherer A, Wohlleb L, Schmidutz F, Jansson V, Müller PE (2014) UKA can be safely revised to primary knee arthroplasty by using an autologous bone plate from the proximal lateral tibia. J Arthroplasty 29(10): Revell PA (2008) The combined role of wear particles, macrophages and lymphocytes in the loosening of total joint prostheses. J R Soc Interface 5: Robb CA, Matharu GS, Baloch K, Pynset PB (2013) Revision surgery for failed unicompartmental knee replacement: technical aspects and clinical outcome. Acta Orthop Belg 79: Saldanha KA, Keys GW, Svard UC, White RH, Rao C (2007) Revision of Oxford medial unicompartmental knee arthroplasty to total knee arthroplasty results of a multicentre study. Knee 14(4): Saragaglia D, Estour G, Nemer C, Colle PE (2009) Revision of 33 unicompartmental knee prostheses using total knee arthroplasty: strategy and results. Int Orthop 33(4): Shi HF, Xiong J, Chen YX, Wang JF, Qiu XS, Wang YH, Qiu Y (2013) Early application of pulsed electromagnetic field in the treatment of postoperative delayed union of long-bone fractures: a prospective randomized controlled study. BMC Musculoskelet Disord 19(14): Siddiqui NA, Ahmad ZM (2012) Revision of unicondylar to total knee arthroplasty: a systematic review. Open Orthop J 6(Suppl 2): Springer BD, Scott RD, Thornhill TS (2006) Conversion of failed unicompartmental knee arthroplasty to TKA. Clin Orthop Relat Res 446: Tinius M, Klima S, Marquass B, Tinius W, Josten C (2006) Revision possibilities after failed unicompartmental knee arthroplasty, an analysis of 116 revisions. Z Orthop Ihre Grenzgeb 144(4):
Revision surgery for failed unicompartmental knee replacement : Technical aspects and clinical outcome
 Acta Orthop. Belg., 2013, 79, 312-317 ORIGINAL STUDY Revision surgery for failed unicompartmental knee replacement : Technical aspects and clinical outcome Curtis A. Robb, Gulraj S. Matharu, Khalid Baloch,
Acta Orthop. Belg., 2013, 79, 312-317 ORIGINAL STUDY Revision surgery for failed unicompartmental knee replacement : Technical aspects and clinical outcome Curtis A. Robb, Gulraj S. Matharu, Khalid Baloch,
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up
 Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete
 Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing
 Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Journal of Orthopaedic Surgery 2001, 9(1): 45 50 Bilateral total knee arthroplasty: One mobile-bearing and one fixed-bearing KY Chiu, TP Ng, WM Tang and P Lam Department of Orthopaedic Surgery, The University
Conversion of unicompartmental knee arthroplasty to total knee arthroplasty : The challenges and need for augments
 Acta Orthop. Belg., 2013, 79, 699-705 ORIGINAL STUDY Conversion of unicompartmental knee arthroplasty to total knee arthroplasty : The challenges and need for augments Zeeshan Khan, Syed Z. Nawaz, Steven
Acta Orthop. Belg., 2013, 79, 699-705 ORIGINAL STUDY Conversion of unicompartmental knee arthroplasty to total knee arthroplasty : The challenges and need for augments Zeeshan Khan, Syed Z. Nawaz, Steven
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Minimally invasive unicompartmental knee arthroplasty in treatment of osteonecrosis versus osteoarthritis : a matched-pair comparison
 Acta Orthop. Belg., 2015, 81, 333-339 ORIGINAL STUDY Minimally invasive unicompartmental knee arthroplasty in treatment of osteonecrosis versus osteoarthritis : a matched-pair comparison Qidong Zhang,
Acta Orthop. Belg., 2015, 81, 333-339 ORIGINAL STUDY Minimally invasive unicompartmental knee arthroplasty in treatment of osteonecrosis versus osteoarthritis : a matched-pair comparison Qidong Zhang,
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR
 CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
CLINICAL AND OPERATIVE APPROACH FOR TOTAL KNEE REPLACEMENT DR.VINMAIE ORTHOPAEDICS PG 2 ND YEAR Evolution of TKR In 1860, Verneuil proposed interposition arthroplasty, involving the insertion of soft tissue
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Aseptic Revision Total Knee Surgical Techniques. Andrew Ehmke, DO Chicago, IL May 5, 2018
 Aseptic Revision Total Knee Surgical Techniques Andrew Ehmke, DO Chicago, IL May 5, 2018 I have no disclosures relevant to this talk 3 Phases of Revision 1. Exposure Key to the case!! 2. Component Removal
Aseptic Revision Total Knee Surgical Techniques Andrew Ehmke, DO Chicago, IL May 5, 2018 I have no disclosures relevant to this talk 3 Phases of Revision 1. Exposure Key to the case!! 2. Component Removal
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year
 Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
Cementless Oxford unicompartmental knee replacement shows reduced radiolucency at one year H. Pandit, C. Jenkins, D. J. Beard, J. Gallagher, A. J. Price, C. A. F. Dodd, J. W. Goodfellow, D. W. Murray From
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
Clinical Results of Lateral Unicompartmental Knee Arthroplasty: Minimum 2-Year Follow-up
 Original Article Clinics in Orthopedic Surgery 2016;8:386-392 https://doi.org/10.4055/cios.2016.8.4.386 Clinical Results of Lateral Unicompartmental Knee Arthroplasty: Minimum 2-Year Follow-up Kyung Tae
Original Article Clinics in Orthopedic Surgery 2016;8:386-392 https://doi.org/10.4055/cios.2016.8.4.386 Clinical Results of Lateral Unicompartmental Knee Arthroplasty: Minimum 2-Year Follow-up Kyung Tae
Medium term results of the Miller-Galante unicompartmental knee arthroplasty with 10 year survivorship
 Acta Orthop. Belg., 2013, 79, 197-204 ORIGINAL STUDY Medium term results of the Miller-Galante unicompartmental knee arthroplasty with 10 year survivorship Rajesh Rachha, Karunakar Veravalli, Manoj Sood
Acta Orthop. Belg., 2013, 79, 197-204 ORIGINAL STUDY Medium term results of the Miller-Galante unicompartmental knee arthroplasty with 10 year survivorship Rajesh Rachha, Karunakar Veravalli, Manoj Sood
Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W.
 University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
University of Groningen Alignment of the femoral component in a mobile-bearing unicompartmental knee arthroplasty Kort, N. P.; van Raay, J. J. A. M.; Thomassen, B. J. W. Published in: Knee DOI: 10.1016/j.knee.2007.04.007
Implant Overhang after Unicompartmental Knee Arthroplasty: Oxford Prosthesis versus Miller-Galante II Prosthesis
 Original Article Knee Surg Relat Res 2014;26(2):82-87 http://dx.doi.org/10.5792/ksrr.2014.26.2.82 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Implant Overhang after Unicompartmental
Original Article Knee Surg Relat Res 2014;26(2):82-87 http://dx.doi.org/10.5792/ksrr.2014.26.2.82 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Implant Overhang after Unicompartmental
Mid-Term Results of Oxford Medial Unicompartmental Knee Arthroplasty
 Original Article Clinics in Orthopedic Surgery 2011;3:178-183 http://dx.doi.org/10.4055/cios.2011.3.3.178 Mid-Term Results of Oxford Medial Unicompartmental Knee Arthroplasty Won-Sik Choy, MD, Kap Jung
Original Article Clinics in Orthopedic Surgery 2011;3:178-183 http://dx.doi.org/10.4055/cios.2011.3.3.178 Mid-Term Results of Oxford Medial Unicompartmental Knee Arthroplasty Won-Sik Choy, MD, Kap Jung
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with:
 Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Total Knee Replacement
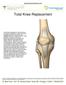 Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Total Knee Replacement A total knee replacement, also known as total knee arthroplasty, involves removing damaged portions of the knee, and capping the bony surfaces with man-made prosthetic implants.
Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system
 Journal of Orthopaedic Surgery 2005:13(3):280-284 Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system S Asif, DSK Choon Department of Orthopaedic Surgery, University of
Journal of Orthopaedic Surgery 2005:13(3):280-284 Midterm results of cemented Press Fit Condylar Sigma total knee arthroplasty system S Asif, DSK Choon Department of Orthopaedic Surgery, University of
Unicompartmental Knee Replacement
 Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
With over 40 years clinical experience, the Oxford Partial Knee is the most widely used, 1 clinically proven 2 partial knee system in the world.
 Oxford Partial Knee A Definitive Implant With over 40 years clinical experience, the Oxford Partial Knee is the most widely used, 1 clinically proven 2 partial knee system in the world. Compared with total
Oxford Partial Knee A Definitive Implant With over 40 years clinical experience, the Oxford Partial Knee is the most widely used, 1 clinically proven 2 partial knee system in the world. Compared with total
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Masterclass. Tips and tricks for a successful outcome. E. Verhaven, M. Thaeter. September 15th, 2012, Brussels
 Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
TOTAL KNEE ARTHROPLASTY (TKA)
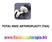 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity
 ORTHOPEDICS May 2009;32(5):360. Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity by John P. Meehan, MD; Mohammad A. Khadder, MD; Amir A. Jamali,
ORTHOPEDICS May 2009;32(5):360. Closing Wedge Retrotubercular Tibial Osteotomy and TKA for Posttraumatic Osteoarthritis With Angular Deformity by John P. Meehan, MD; Mohammad A. Khadder, MD; Amir A. Jamali,
Revision of Unicondylar to Total Knee Arthroplasty: A Systematic Review
 268 The Open Orthopaedics Journal, 2012, 6, (Suppl 2: M2) 268-275 Open Access Revision of Unicondylar to Total Knee Arthroplasty: A Systematic Review Nashat A. Siddiqui *,1 and Zafar M. Ahmad 2 1 Department
268 The Open Orthopaedics Journal, 2012, 6, (Suppl 2: M2) 268-275 Open Access Revision of Unicondylar to Total Knee Arthroplasty: A Systematic Review Nashat A. Siddiqui *,1 and Zafar M. Ahmad 2 1 Department
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
There have been conflicting results reported in the
 Bulletin Hospital for Joint Diseases Volume 61, Numbers 1 & 2 2002-2003 5 Total Knee Replacement Following High Tibial Osteotomy Sanjeev Madan, M.Ch.Orth., F.R.C.S. (Orth), M.Sc.(Orth), M.B.A., R. K. Ranjith,
Bulletin Hospital for Joint Diseases Volume 61, Numbers 1 & 2 2002-2003 5 Total Knee Replacement Following High Tibial Osteotomy Sanjeev Madan, M.Ch.Orth., F.R.C.S. (Orth), M.Sc.(Orth), M.B.A., R. K. Ranjith,
Knee Revision. Portfolio
 Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
Knee Revision Portfolio I use the DePuy Revision Knee System because of its versatility. With this system I can solve nearly any situation I encounter in the OR. Dr. Thomas Fehring, OrthoCarolina Hip and
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty
 Tsukada et al. Journal of Orthopaedic Surgery and Research 2013, 8:36 RESEARCH ARTICLE Open Access Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty Sachiyuki
Tsukada et al. Journal of Orthopaedic Surgery and Research 2013, 8:36 RESEARCH ARTICLE Open Access Metal block augmentation for bone defects of the medial tibia during primary total knee arthroplasty Sachiyuki
Management of Periprosthetic Fracture in Unicompartmental Knee Arthroplasty Patients: A Case Series
 Management of Periprosthetic Fracture in Unicompartmental Knee Arthroplasty Patients: A Case Series Yew Lok Woo, MBBS, Pak Lin Chin, MBBS, FRCS, Ngai Nung Lo, MBBS, FRCS, Shi-Lu Chia, PhD, Darren Keng
Management of Periprosthetic Fracture in Unicompartmental Knee Arthroplasty Patients: A Case Series Yew Lok Woo, MBBS, Pak Lin Chin, MBBS, FRCS, Ngai Nung Lo, MBBS, FRCS, Shi-Lu Chia, PhD, Darren Keng
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Complications of Total Knee Arthroplasty
 Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
Progress in Clinical Medicine Complications of Total Knee Arthroplasty JMAJ 44(5): 235 240, 2001 Shinichi YOSHIYA*, Masahiro KUROSAKA** and Ryosuke KURODA*** *Director, Department of Orthopaedic Surgery,
Tibial & Femoral Opening Wedge Osteotomy System. Surgical Technique
 Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
Tibial & Femoral Opening Wedge Osteotomy System Surgical Technique Opening Wedge Osteotomy Tibial & Femoral Opening Wedge Osteotomy 2 Prior to the osteotomy, a diagnostic arthroscopy is performed to verify
The young patient and the medial unicompartmental knee replacement
 Acta Orthop. Belg., 2015, 81, 283-288 ORIGINAL STUDY The young patient and the medial unicompartmental knee replacement Omar Faour Martín, Jose Antonio Valverde García, Miguel Ángel Martín Ferrero, Aurelio
Acta Orthop. Belg., 2015, 81, 283-288 ORIGINAL STUDY The young patient and the medial unicompartmental knee replacement Omar Faour Martín, Jose Antonio Valverde García, Miguel Ángel Martín Ferrero, Aurelio
Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar
 Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar High Tibial Osteotomy: HTO! Valgisation HTO Intended to transfer the mechanical
Choice of spacer material for HTO! P. Landreau, MD Chief of Surgery Aspetar, Orthopaedic and Sports Medicine Hospital Doha, Qatar High Tibial Osteotomy: HTO! Valgisation HTO Intended to transfer the mechanical
Partial Knee Replacement
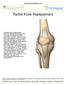 Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Partial Knee Replacement A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Zimmer Unicompartmental High Flex Knee. Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques
 Zimmer Unicompartmental High Flex Knee Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques ZIMMER UNICOMPARTMENTAL HIGH FLEX KNEE INTRAMEDULLARY, SPACER BLOCK
Zimmer Unicompartmental High Flex Knee Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques ZIMMER UNICOMPARTMENTAL HIGH FLEX KNEE INTRAMEDULLARY, SPACER BLOCK
OPERATIVE TECHNIQUE SKS Total Knee Replacement
 OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
THE P.F.C. SIGMA FEMORAL ADAPTER. Surgical Technique
 THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
Stefan Rahm MD University Hospital Balgrist
 Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
Knee Prosthesis Models & Materials, Surgical Techniques and Approaches Stefan Rahm MD University Hospital Balgrist INTRODUCTION VARUS VALGUS 46 Y OLD MALE Pain in the medial compartment left more than
Exposure EXPOSURE. Exposure - Incision. Extend old incision proximally Expose virgin quadriceps tendon
 Exposure Aaron G Rosenberg MD Professor of Orthopedic Surgery Rush Medical College Chicago, Illinois Exposure - Incision Single incision can be used or modified Multiple longitudinal incisions favor the
Exposure Aaron G Rosenberg MD Professor of Orthopedic Surgery Rush Medical College Chicago, Illinois Exposure - Incision Single incision can be used or modified Multiple longitudinal incisions favor the
Unicondylar Knee Arthroplasty
 P R O C E D U R E 1 7 Unicondylar Knee Arthroplasty Ammar Anbari, Craig J. Della Valle, and Brian J. Cole ch017-x4397.indd 259 4/11/2008 10:52:12 AM 260 Contraindications Patients with inflammatory arthritis
P R O C E D U R E 1 7 Unicondylar Knee Arthroplasty Ammar Anbari, Craig J. Della Valle, and Brian J. Cole ch017-x4397.indd 259 4/11/2008 10:52:12 AM 260 Contraindications Patients with inflammatory arthritis
PARTIAL KNEE REPLACEMENT
 PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Autologous bone grafting plus bio-absorbable pin fixation for medial tibial defects in total knee arthroplasty
 Autologous bone grafting plus bio-absorbable pin fixation for medial tibial defects in total knee arthroplasty Showa University Fujigaoka Hospital, Yokohama SHIN KATO, Hiroshi Takagi, Jun Oike, Takayuki
Autologous bone grafting plus bio-absorbable pin fixation for medial tibial defects in total knee arthroplasty Showa University Fujigaoka Hospital, Yokohama SHIN KATO, Hiroshi Takagi, Jun Oike, Takayuki
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Kinematic vs. mechanical alignment: What is the difference?
 Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
Kinematic vs. mechanical alignment: What is the difference? In this 4 Questions interview, Stephen M. Howell, MD, explains the potential benefits of 3D alignment during total knee replacement. Introduction
THE KNEE SOCIETY VIRTUAL FELLOWSHIP
 THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER IX PARTIAL KNEE: MEDIAL, LATERAL AND PFR Revision of Failed Unicompartmental to Total Knee Arthroplasty Presented by: Keith R. Berend, MD COPYRIGHT 2016 THE
THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER IX PARTIAL KNEE: MEDIAL, LATERAL AND PFR Revision of Failed Unicompartmental to Total Knee Arthroplasty Presented by: Keith R. Berend, MD COPYRIGHT 2016 THE
The Knee. The Twin Peg Oxford partial knee replacement: The first 100 cases. Stephen H. White a,, Sharon Roberts a, Peter W.
 The Knee 19 (2012) 36 40 Contents lists available at ScienceDirect The Knee The Twin Peg Oxford partial knee replacement: The first 100 cases Stephen H. White a,, Sharon Roberts a, Peter W. Jones b a Department
The Knee 19 (2012) 36 40 Contents lists available at ScienceDirect The Knee The Twin Peg Oxford partial knee replacement: The first 100 cases Stephen H. White a,, Sharon Roberts a, Peter W. Jones b a Department
The UniSpacer : correcting varus malalignment in medial gonarthrosis
 DOI 10.1007/s00264-009-0908-9 ORIGINAL PAPER The UniSpacer : correcting varus malalignment in medial gonarthrosis Michael Clarius & Justus F. Becker & Holger Schmitt & Joern B. Seeger Received: 20 October
DOI 10.1007/s00264-009-0908-9 ORIGINAL PAPER The UniSpacer : correcting varus malalignment in medial gonarthrosis Michael Clarius & Justus F. Becker & Holger Schmitt & Joern B. Seeger Received: 20 October
Functional Outcomes of Revision Total Knee Arthroplasty Following Failed Unicompartmental Knee Arthroplasty
 Reconstructive Review Volume 4, Number 4, December 2014 ORIGINAL ARTICLE Functional Outcomes of Revision Total Knee Arthroplasty Following Failed Unicompartmental Knee Arthroplasty Chris Ironside MBBS,
Reconstructive Review Volume 4, Number 4, December 2014 ORIGINAL ARTICLE Functional Outcomes of Revision Total Knee Arthroplasty Following Failed Unicompartmental Knee Arthroplasty Chris Ironside MBBS,
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
TOTAL KNEE ARTHROPLASTY SYSTEM
 SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
Massive Varus- Overview. Massive Varus- Classification. Massive Varus- Definition 07/02/14. Correction of Massive Varus Deformity in TKR
 07/02/14 Massive Varus- Overview Correction of Massive Varus Deformity in TKR Myles Coolican Val d Isere 2014 Massive Varus- Classification Classification Intra articular Massive Varus- Classification Classification
07/02/14 Massive Varus- Overview Correction of Massive Varus Deformity in TKR Myles Coolican Val d Isere 2014 Massive Varus- Classification Classification Intra articular Massive Varus- Classification Classification
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique
 ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
The Oxford phase III unicompartmental knee replacement in patients less than 60 years of age Kort, Nanne P.; van Raay, Jos J. A. M.; van Horn, Jim J.
 University of Groningen The Oxford phase III unicompartmental knee replacement in patients less than 60 years of age Kort, Nanne P.; van Raay, Jos J. A. M.; van Horn, Jim J. Published in: Knee surgery
University of Groningen The Oxford phase III unicompartmental knee replacement in patients less than 60 years of age Kort, Nanne P.; van Raay, Jos J. A. M.; van Horn, Jim J. Published in: Knee surgery
S U R G I C A L T E C H N I Q U E David A. McQueen, MD Return to Menu
 S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
S U R G I C A L T E C H N I Q U E David A. McQueen, MD TOTAL KNEE INSTRUMENTS Wichita Fusion Nail Introduction...1 Preoperative Planning...2 Surgical Technique...3-8 Wichita Fusion Nail Surgical Technique
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
SIGMA High Performance Partial Knee. Unicondylar. Surgical Technique
 SIGMA High Performance Partial Knee Unicondylar Surgical Technique Table of Contents Surgical Technique X-ray Templating 3 Approach and Exposure 4 Proximal Tibial Resection 5 Tibial Jig Alignment 7 Tibial
SIGMA High Performance Partial Knee Unicondylar Surgical Technique Table of Contents Surgical Technique X-ray Templating 3 Approach and Exposure 4 Proximal Tibial Resection 5 Tibial Jig Alignment 7 Tibial
Unicondylar Surgical Technique
 Unicondylar Surgical Technique Contents Indications, Contra-indications and X-ray Templating 2 Approach and Exposure 3 Proximal Tibial Resection 4 Tibial Jig Alignment 6 Tibial Sizing 9 Balancing 10 Distal
Unicondylar Surgical Technique Contents Indications, Contra-indications and X-ray Templating 2 Approach and Exposure 3 Proximal Tibial Resection 4 Tibial Jig Alignment 6 Tibial Sizing 9 Balancing 10 Distal
Oxford. Partial Knee
 Oxford Partial Knee Oxford Partial Knee A Definitive Implant The Oxford Partial Knee is the most widely used 38 and clinically proven 22 partial knee replacement (PKR) system in the world, offering industry
Oxford Partial Knee Oxford Partial Knee A Definitive Implant The Oxford Partial Knee is the most widely used 38 and clinically proven 22 partial knee replacement (PKR) system in the world, offering industry
Over 20 Years of Proven Clinical Success. Zimmer Natural-Knee II System
 Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Over 20 Years of Proven Clinical Success Zimmer Natural-Knee II System CSTi Porous Coating Structurally similar to human bone CSTi porous coating combines the excellent biocompatibility of titanium with
Simplifying the Most Clinically Proven Partial Knee in the World. Oxford Partial Knee with Microplasty Instrumentation
 Simplifying the Most Clinically Proven Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty instrumentation
Simplifying the Most Clinically Proven Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty instrumentation
The Survivorship and Clinical Results of Minimally Invasive Unicompartmental Knee Arthroplasty at 10-Year Follow-up
 Original Article Clinics in Orthopedic Surgery 2015;7:199-206 http://dx.doi.org/10.4055/cios.2015.7.2.199 The Survivorship and Clinical Results of Minimally Invasive Unicompartmental Knee Arthroplasty
Original Article Clinics in Orthopedic Surgery 2015;7:199-206 http://dx.doi.org/10.4055/cios.2015.7.2.199 The Survivorship and Clinical Results of Minimally Invasive Unicompartmental Knee Arthroplasty
Uniglide. Unicompartmental Knee Replacement Mk III surgical technique
 Uniglide Unicompartmental Knee Replacement Mk III surgical technique Uniglide Contents Operative summary 4 Pre-operative assessment 6 Preparation 7 Incision 7 Approach 7 Medial procedure 8 Tibial preparation
Uniglide Unicompartmental Knee Replacement Mk III surgical technique Uniglide Contents Operative summary 4 Pre-operative assessment 6 Preparation 7 Incision 7 Approach 7 Medial procedure 8 Tibial preparation
Complications of Medial Unicompartmental Knee Arthroplasty
 Original Article Clinics in Orthopedic Surgery 2014;6:365-372 http://dx.doi.org/10.4055/cios.2014.6.4.365 Complications of Medial Unicompartmental Knee Arthroplasty Jong Hun Ji, MD, Sang Eun Park, MD,
Original Article Clinics in Orthopedic Surgery 2014;6:365-372 http://dx.doi.org/10.4055/cios.2014.6.4.365 Complications of Medial Unicompartmental Knee Arthroplasty Jong Hun Ji, MD, Sang Eun Park, MD,
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique
 POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
Stephen R Smith Northeast Nebraska Orthopaedics PC. Ligament Preserving Techniques in Total Knee Arthroplasty
 Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
Does a minimally invasive approach affect positioning of components in unicompartmental knee arthroplasty? Early results with survivorship analysis
 Acta Orthop. Belg., 2006, 72, 709-715 ORIGINAL STUDY Does a minimally invasive approach affect positioning of components in unicompartmental knee arthroplasty? Early results with survivorship analysis
Acta Orthop. Belg., 2006, 72, 709-715 ORIGINAL STUDY Does a minimally invasive approach affect positioning of components in unicompartmental knee arthroplasty? Early results with survivorship analysis
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
unicompartmental knee SURGICAL TECHNIQUE limacorporate.com
 unicompartmental knee SURGICAL TECHNIQUE limacorporate.com Index INTRAMEDULLARY (IM) SURGICAL PROCEDURE Introduction Page >> 04 Rationale Page >> 05 Preoperative Planning Page >> 07 Patient Preparation
unicompartmental knee SURGICAL TECHNIQUE limacorporate.com Index INTRAMEDULLARY (IM) SURGICAL PROCEDURE Introduction Page >> 04 Rationale Page >> 05 Preoperative Planning Page >> 07 Patient Preparation
Minimally Invasive Surgical Techniques for the Medial Compartment. Intramedullary, Spacer Block and Extramedullary techniques
 Minimally Invasive Surgical Techniques for the Medial Compartment Intramedullary, Spacer Block and Extramedullary techniques Unicompartmental High Flex Knee Intramedullary, Spacer Block and Extramedullary
Minimally Invasive Surgical Techniques for the Medial Compartment Intramedullary, Spacer Block and Extramedullary techniques Unicompartmental High Flex Knee Intramedullary, Spacer Block and Extramedullary
Mædica - a Journal of Clinical Medicine
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Total Knee Arthroplasty Following High Tibial Osteotomy a Radiological Evaluation Horia ORBAN, MD, PhD; Emil MARES, MD; Mihaela DRAGUSANU, MD; Gabriel
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Total Knee Arthroplasty Following High Tibial Osteotomy a Radiological Evaluation Horia ORBAN, MD, PhD; Emil MARES, MD; Mihaela DRAGUSANU, MD; Gabriel
Knee Surg Relat Res 2013;25(1): pissn eissn Knee Surgery & Related Research
 Original Article Knee Surg Relat Res 2013;25(1):13-18 http://dx.doi.org/10.5792/ksrr.2013.25.1.13 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Comparative Study of Two Techniques for
Original Article Knee Surg Relat Res 2013;25(1):13-18 http://dx.doi.org/10.5792/ksrr.2013.25.1.13 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Comparative Study of Two Techniques for
1. Pre-Operative Planning Skin Incision and Arthrotomy
 Stage of Operation 1. Pre-Operative Planning --------------------------1 2. Skin Incision and Arthrotomy ------------------1 3. Femoral valgus angle confirmation ------------2 4. Distal Femur Cutting -----------------------------3
Stage of Operation 1. Pre-Operative Planning --------------------------1 2. Skin Incision and Arthrotomy ------------------1 3. Femoral valgus angle confirmation ------------2 4. Distal Femur Cutting -----------------------------3
Dora Street, Hurstville 160 Belmore Road, Randwick
 Dr Andreas Loefler www.orthosports.com.au 29 31 Dora Street, Hurstville 160 Belmore Road, Randwick Dr Andreas Loefler Joint Replacement & Spine Surgery CAS or Navigation in TKA New Software for a Full
Dr Andreas Loefler www.orthosports.com.au 29 31 Dora Street, Hurstville 160 Belmore Road, Randwick Dr Andreas Loefler Joint Replacement & Spine Surgery CAS or Navigation in TKA New Software for a Full
A meta-analysis of unicompartmental knee arthroplasty revised to total knee arthroplasty versus primary total knee arthroplasty
 Sun and Su Journal of Orthopaedic Surgery and Research (28) 3:58 https://doi.org/.86/s38-8-859- REVIEW Open Access A meta-analysis of unicompartmental knee arthroplasty revised to total knee arthroplasty
Sun and Su Journal of Orthopaedic Surgery and Research (28) 3:58 https://doi.org/.86/s38-8-859- REVIEW Open Access A meta-analysis of unicompartmental knee arthroplasty revised to total knee arthroplasty
DIFFICULT PRIMARY TKA: VALGUS KNEE
 DIFFICULT PRIMARY TKA: VALGUS KNEE Prof. Stefano Zaffagnini Direttore II Clinica Ortopedica Istituto Ortopedico Rizzoli Università di Bologna EPIDEMIOLOGY MOST FREQUENT DEFORMITY IS FIXED- VARUS: 50 TO
DIFFICULT PRIMARY TKA: VALGUS KNEE Prof. Stefano Zaffagnini Direttore II Clinica Ortopedica Istituto Ortopedico Rizzoli Università di Bologna EPIDEMIOLOGY MOST FREQUENT DEFORMITY IS FIXED- VARUS: 50 TO
Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System
 Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Scandinavian Journal of Surgery 0: 1 8, Department of Surgery, North Karelia Central Hospital, Joensuu, Finland 2
 577022SJS0010.1177/1457496915577022UKA mid-term resultss. S. A. Miettinen et al. research-article2015 ORIGINAL ARTICLE Scandinavian Journal of Surgery 0: 1 8, 2015 Mid-Term Results Of Oxford Phase 3 Unicompartmental
577022SJS0010.1177/1457496915577022UKA mid-term resultss. S. A. Miettinen et al. research-article2015 ORIGINAL ARTICLE Scandinavian Journal of Surgery 0: 1 8, 2015 Mid-Term Results Of Oxford Phase 3 Unicompartmental
The Treatment of Pelvic Discontinuity During Acetabular Revision
 The Journal of Arthroplasty Vol. 20 No. 4 Suppl. 2 2005 The Treatment of Pelvic Discontinuity During Acetabular Revision Scott M. Sporer, MD, MS,*y Michael O Rourke, MD,z and Wayne G. Paprosky, MD, FACS*y
The Journal of Arthroplasty Vol. 20 No. 4 Suppl. 2 2005 The Treatment of Pelvic Discontinuity During Acetabular Revision Scott M. Sporer, MD, MS,*y Michael O Rourke, MD,z and Wayne G. Paprosky, MD, FACS*y
STIFFNESS AFTER TKA PRE, PER AND POST OPERATIVE CAUSING FACTORS
 STIFFNESS AFTER TKA PRE, PER AND POST OPERATIVE CAUSING FACTORS Patrick DJIAN INTRODUCTION Stiffness is one of the most common complications following TKR, causing frustration to both the surgeon and the
STIFFNESS AFTER TKA PRE, PER AND POST OPERATIVE CAUSING FACTORS Patrick DJIAN INTRODUCTION Stiffness is one of the most common complications following TKR, causing frustration to both the surgeon and the
Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design. Adam I. Harris, M.D. & Michelle Ammerman
 Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design Adam I. Harris, M.D. & Michelle Ammerman History: The Total Condylar knee represented a significant advance in
Retrospective Study of Patellar Tracking in an Anatomical, Motion Guided Total Knee Design Adam I. Harris, M.D. & Michelle Ammerman History: The Total Condylar knee represented a significant advance in
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
UDHT08.1.qxd:UDHT /03/08 17:14 Page 1. Surgical. Technique. Elbow Prosthesis. RHS Radial Head System.
 UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 1 Surgical Technique Elbow Prosthesis RHS Radial Head System www.tornier.com UDHT08.1.qxd:UDHT08.1 13/03/08 17:14 Page 2 TABLE OF CONTENTS DESIGN RATIONALE INDICATIONS
Wichita Fusion Nail Surgical Technique. David A. McQueen, MD
 Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Wichita Fusion Nail Surgical Technique David A. McQueen, MD The patented design with a dual advantage Generates compression intraoperatively Innovative compression screw (a) locks femoral and tibial components
Sequential soft tissue release and unconstrained TKA implants in severe varus deformity- Prospective study in 75 knees
 2017; 3(3): 15-20 ISSN: 2395-1958 IJOS 2017; 3(3): 15-20 2017 IJOS www.orthopaper.com Received: 04-05-2017 Accepted: 05-06-2017 Dr. Ranganatha B Thimmegowda MS, DNB, Assistant Professor, ESIC Medical College,
2017; 3(3): 15-20 ISSN: 2395-1958 IJOS 2017; 3(3): 15-20 2017 IJOS www.orthopaper.com Received: 04-05-2017 Accepted: 05-06-2017 Dr. Ranganatha B Thimmegowda MS, DNB, Assistant Professor, ESIC Medical College,
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Outcome of revision total knee arthroplasty with bone allograft in 30 cases
 Acta Orthop. Belg., 2013, 79, 427-434 ORIGINAL STUDY Outcome of revision total knee arthroplasty with bone allograft in 30 cases Katrina F. Franke, Iulian Nusem, Gaugin Gamboa, David A.F. Morgan From Queensland
Acta Orthop. Belg., 2013, 79, 427-434 ORIGINAL STUDY Outcome of revision total knee arthroplasty with bone allograft in 30 cases Katrina F. Franke, Iulian Nusem, Gaugin Gamboa, David A.F. Morgan From Queensland
KneeTec PFJ. Surgical Technique
 KneeTec PFJ KneeTec PFJ Surgical Technique CONTENTS INDICATIONS p.3 CONTRAINDICATIONS p.4 INSTRUCTION FOR USE p.5 Anterior Resection p.6 Sizing and Positioning p.11 Femoral Preparation p.14 Distal and
KneeTec PFJ KneeTec PFJ Surgical Technique CONTENTS INDICATIONS p.3 CONTRAINDICATIONS p.4 INSTRUCTION FOR USE p.5 Anterior Resection p.6 Sizing and Positioning p.11 Femoral Preparation p.14 Distal and
Biomechanics of. Knee Replacement. Mujda Hakime, Paul Malcolm
 Biomechanics of Knee Replacement Mujda Hakime, Paul Malcolm 1 Table of contents Knee Anatomy Movements of the Knee Knee conditions leading to knee replacement Materials Alignment and Joint Loading Knee
Biomechanics of Knee Replacement Mujda Hakime, Paul Malcolm 1 Table of contents Knee Anatomy Movements of the Knee Knee conditions leading to knee replacement Materials Alignment and Joint Loading Knee
Simplifying the Most Clinically Proven 1 Partial Knee in the World. Oxford Partial Knee with Microplasty Instrumentation
 Simplifying the Most Clinically Proven 1 Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty Instrumentation
Simplifying the Most Clinically Proven 1 Partial Knee in the World Oxford Partial Knee with Microplasty Instrumentation 1 Microplasty Instrumentation Innovative, Accurate, Reproducible Microplasty Instrumentation
The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis
 Orthopaedics & Traumatology: Surgery & Research (2011) 97, 410 417 ORIGINAL ARTICLE The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis C. Catier, M.
Orthopaedics & Traumatology: Surgery & Research (2011) 97, 410 417 ORIGINAL ARTICLE The Unispacer TM unicompartmental knee implant: Its outcomes in medial compartment knee osteoarthritis C. Catier, M.
